H/O Lecture 1-2: Anemias | Quizlet
1/114
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
115 Terms
Anemia
group of diseases characterized by a decrease in hemoglobin or lack of RBCs which lead to a decreased oxygen carrying capacity
What is the typical lifespan of an RBC?
120 days
What are the s/sx of iron deficiency anemia?
Fatigue
SOB
Dizziness
Pallor
RLS
Tongue inflammation
Lip inflammation
Pica
Ice eating
Concave nails
What labratory values should be drawn to assess the presence and type of anemia?
CBC
Reticulocyte count
Iron profile
Folate
B12
Fecal occult blood test
Hemoglobin (Hb)
protein within RBCs that are responsible for oxygen delivery to tissues
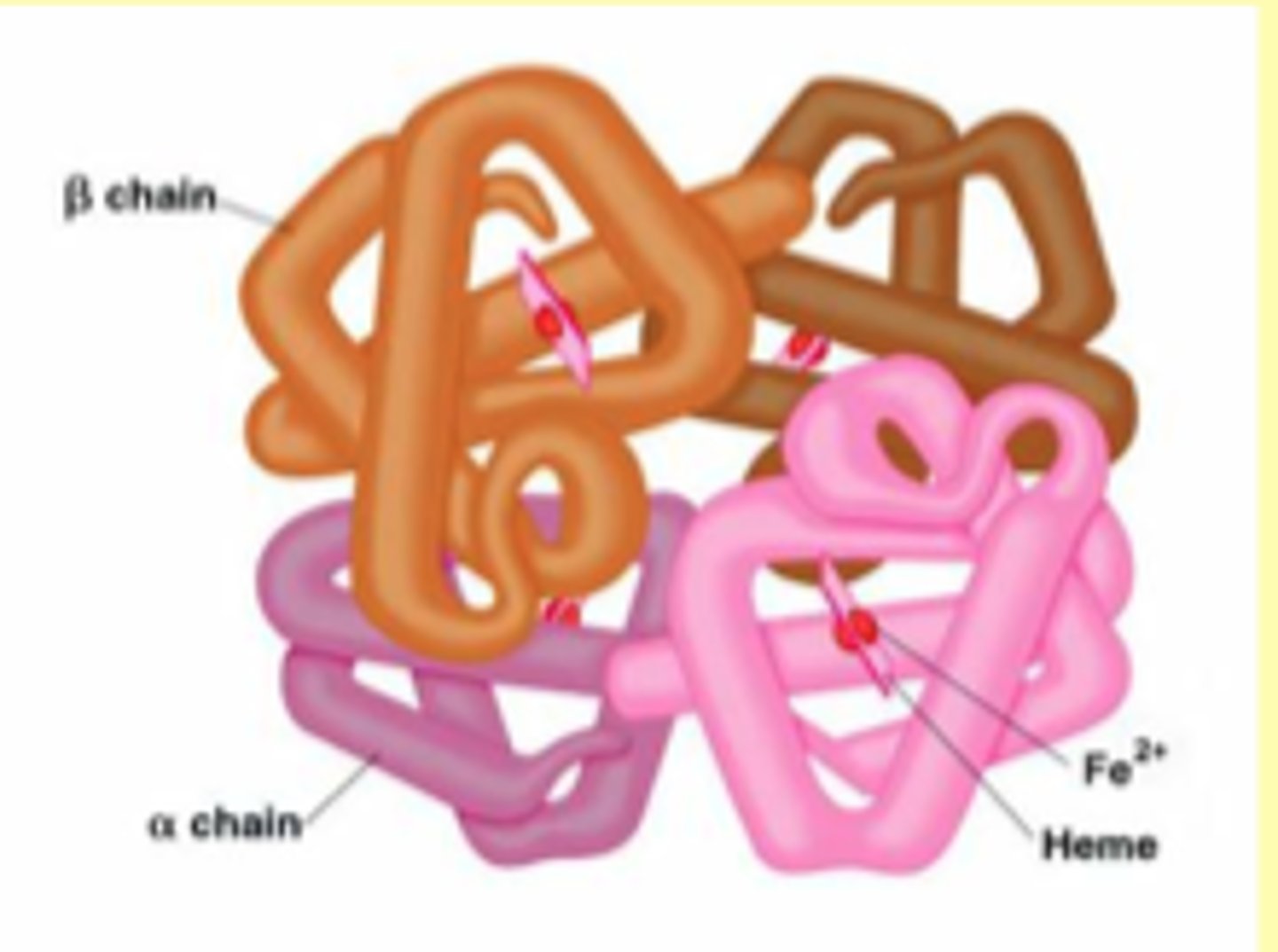
What Hb levels indicate anemia?
Men: <13 g/dL
Women: <12 g/dL
Hematocrit
volume of RBCs compared to the total volume of blood
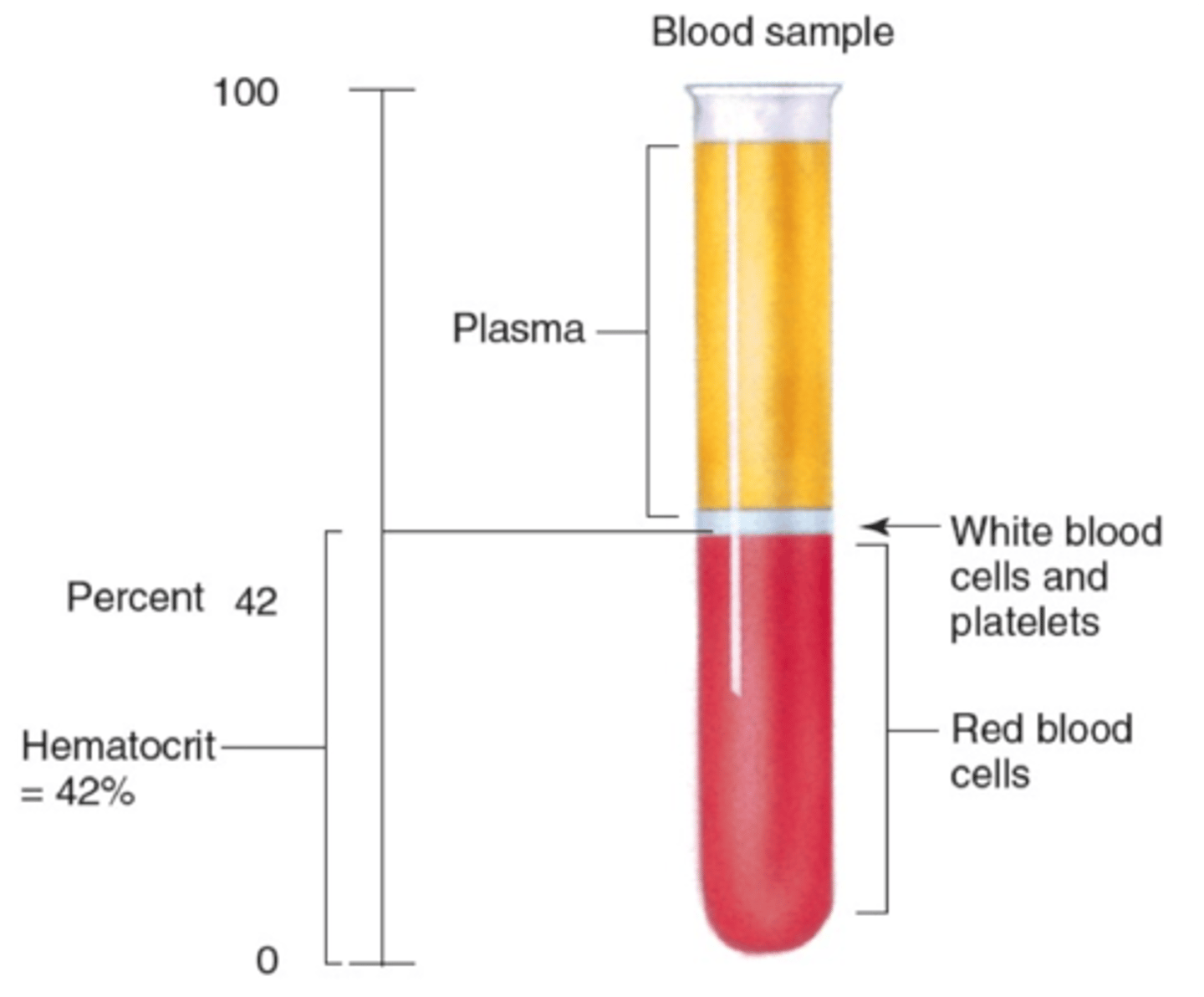
What are the normal levels of hematocrit?
Men: 40-54%
Women: 36-48%
RBC Count
count of RBCs per unit of blood
What is the normal RBC count?
Males: 4.7-6.1 x10^6
Females: 4.1-5.1 x10^6
Mean Corpuscular Volume (MCV)
average WBC size
What is the normal value of MCV?
80-100 fL
Mean Corpuscular Hemoglobin (MCH)
hemoglobin amount per red blood cell
What is the normal value of MCH?
27-31 pg/cell
What is the normal value of MCHC?
32-36 g/dL
Mean Corpuscular Hemoglobin Concentration (MCHC)
concentration of Hb per volume of cells
Why is the MCV lab value helpful?
determines whether cells are macrocytic, normocytic, or microcytic
What does the MCH value tell us?
helps determine microcytosis or macrocytosis
What does the MCHC value tell us?
helpful for distinguishing microcytosis vs. hypochromia
Reticulocyte count
measurement of erythrocyte precursors to measure ability of the body to produce new RBCs
When would a reticulocyte count be high?
acute blood loss
hemolytic anemia
When would a reticulocyte count be low?
Iron deficiency
B12 deficiency
Renal insufficiency
RBC Distribution Width (RDW)
measures the variety of how much and what size of RBCs
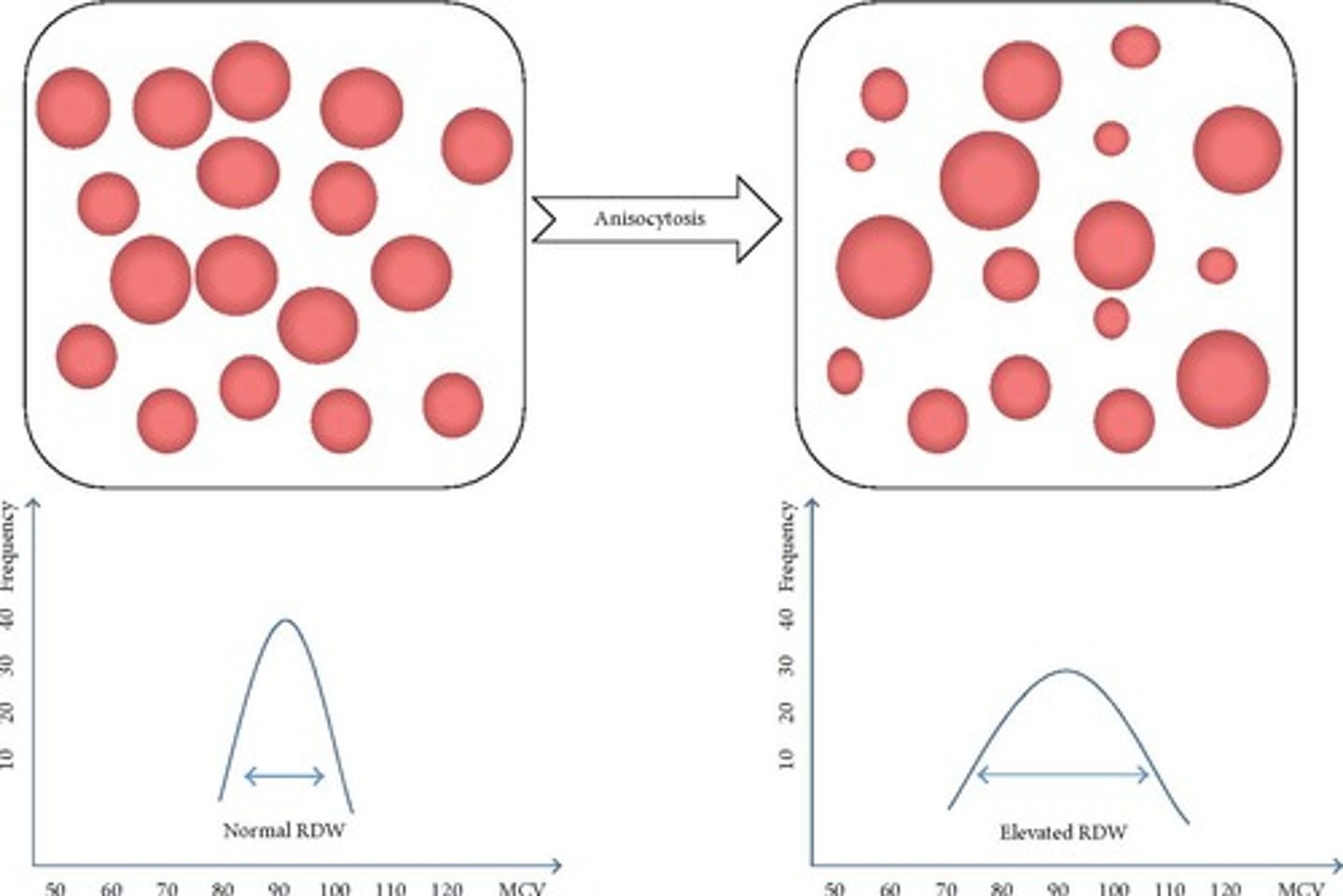
What is the normal RDW?
11.5-14.5%
Serum iron
circulating iron bound to transferrin
Serum ferritin
iron stored in the liver, spleen, and bone marrow
What are the normal serum ferritin levels?
Males: 20-300 ng/mL
Females: 15-200 ng/mL
What is the normal serum iron levels?
Males 65-176 mcg/dL
Females: 50-170 ng/mL
Total Iron Binding Capacity (TBIC)
measures the capacity of transferrin to bind iron
Transferrin Saturation (TSAT)
ratio of serum iron to TBIC - indicated how much iron-binding sites are occupied on transferrin
What is the normal TBIC levels?
250-450 mcg/dL
What is the normal TSAT levels?
20-50%
What MCV value indicates microcytic anemia?
<80 mg/dL
What MCV value indicates normocytic anemia?
80-100 mg/dL
What MCV value indicates macrocytic anemia?
>100 mg/dL
What is the most common cause of microcytic anemia?
Iron deficiency
Who is at high risk for IDA?
Children <2 y/o
>65 y/o
Adolescent girls
Pregnant/lactating
Bloos loss
Altered gut absorption
Low meat diet
Iron deficiency anemia (IDA)
prolonged periods of iron deficiency from increased demand, blood loss, or decreased dietary intake/absorption of iron
Ferritin
HIGHLY soluble form of iron that is stored in the liver, spleen, serum, and bone marrow
Hemosiderin
INsoluble form of iron that is primarily stored in the liver and bone marrow
What are the stages of IDA?
1. Decreased bone marrow stores
2. Impaired erythropoesis
3. Hgb falls below normal limits
4. Microcytosis and hypochromia develop
5. Iron deficiency and low hemoglobin affect the body
As transferrin increases, what happens to serum iron levels?
decrease
As transferrin decreases, what happens to serum iron levels?
increases
What is used to rule IN IDA?
Ferritin <30 ng/mL
What is used to rule OUT IDA?
Ferritin >100 ng/mL
What lab values are DECREASED in IDA?
Hgb/Hct
MCV
Serum Fe (low or normal)
Ferritin
TSAT
What lab values are INCREASED in IDA?
TBIC -
What is the PO iron therapy recommendation for IDA?
120mg of elemental iron per day for 3 months
What shows an adequate response to PO iron therapy?
Hgb increase of 1 g/dL after 1 month
Normal ferritin levels
Men: 20-500 mg/dL
Women: 20 -200 mg/dL
ADRs of PO iron therapy
Dark Stools
GI upset
Nausea
Diarrhea/constipation
What is the amount of elemental iron in ferrous sulfate?
20%
What is the amount of elemental iron in ferrous gluconate?
12%
What is the amount of elemental iron in ferrous fumarate?
33%
What foods should be avoided with PO iron?
Milk
Calcium
High fiber foods
Caffeine
Can PO iron be taken with food?
Yes, but decreases absorption by ~40%
What medications decrease the absorption of PO iron?
Tetracyclines
Fluoroquinolones
Antacids/PPIs/H2 blockers
Multivitamins
What can help to increase the absorption of PO iron?
Vitamin C
Empty stomach
Every other day dosing
Which drugs are affected by iron?
Levodopa
Methyldopa
Levothyroxine
Quinolones
Tetracyclines
Doxycycline
How should medications that interact with iron be taken?
separate by at least 2 hours
Levothyroxine - separate by 4 hours
What is the percentage of elemental iron in ferric maltol?
100%
When is IV iron preferred over PO iron?
Intolerance to PO
Impaired iron absorption
Rapid blood loss
CKD
Why is IV iron superior to oral iron?
sustained Hb response and reducing the need for blood transfusions
What are the biggest ADRs of IV iron?
Infusion related reactions
Anaphylactic reactions
Which IV iron formulation requires test doses due to high rates of anaphylaxis reactions?
Iron Dextran (BBW)
Which IV iron formulation is given in a series of small doses over days to weeks?
Iron sucrose
Which IV iron formulation is commonly used in dialysis patients?
sodium ferric gluconate
Which IV iron formulation can be infused quickly?
Ferumoxytol
Which IV iron formulation needs to be infused over 1 hour?
Sodium ferric gluconate
IV Iron formulations
Iron sucrose (Venofer)
Iron Dextran (Infed)
Sodium ferric gluconate
Ferumoxytol
PO Iron formulations
Ferrous sulfate
Ferrous gluconate
Ferrous fumarate
Ferric maltol
What are the best markers for detecting iron deficiency in heart failure?
TSAT <20%
<10% of bone marrow erythroblasts containing iron
Which iron formulations are preferred in heart failure?
Iron sucrose
Ferric carboxy maltose
Ferric gluconate
What are the caues of microcytic anemia?
Iron deficiency
Sideroblastic anemia
Thalassemia
Lead poisoning
What are the caues of macrocytic anemia?
Vitamin B12 deficiency
Folate deficiency
Liver disease
Drugs
What are the caues of normocytic anemia?
Anemia of CKD
Sickle cell
Aplastic anemia
Hemorrhage
Where are folate and vitamn B12 absorbed?
Small intestine
Jejunum (folate)
Terminal ilium (B12)
Pernicious anemia
autoimmune disorder where autoantibodies target intrinsic factor
Which drugs can cause folate deficiencies?
Methotrexate
Bactrim
Which drugs can cause B12 deficiencies?
Metformin
PPIs
H2 Receptor blockers
Chemotherapy
What can cause folate deficiencies?
Alcohol
Poor diet
Bariatric surgery
Celiac
Methotrexate
Bactrim
Pregnancy
What can cause B12 deficiencies?
Vegan
Pernicious anemia
Bariatric surgery
Celaic
Metformin
PPI
H2RAs
Pernicious anemia can cause what deficiency?
Vitamin B12
What labs can be used to differentiate between folate and vit B12 anemias?
Folic acid
Methylmalonic Acid
How do the folic acid levels differentiate between vit B12 and folate deficiency anemias?
Folate - decreased levels
B12 - normal levels
How do the methylmalonic acid levels differentiate between vit B12 and folate deficiency anemias?
Folate - normal levels
B12 - increased levels
What are the s/sx of folate deficiency anemia?
Fatigue
Oral Ulcers
Neural tube defects in fetus
Neuropsych changes
What are the s/sx of B12 deficiency anemia?
Glossitis (tongue inflammation)
Reduced sensation/ tingling
Decrased cognitive function
What is the onset of folate and B12 deficiencyes?
Folate - weeks to months
B12 - years
What is the treatment of B12 deficiency anemia?
Vitamin B12 (IM, SQ, or PO)
ADRs of B12
Headache
Infection (if injection)
Fatigue
What is the treatment for folate deficiency?
folic acid
What is the repletion dose of folic acid?
1000-5000 mcg PO QD
What is the maintenance dose of folic acid?
400 mcg PO QD
Why is it important to supplement with folate in pregnancy?
risk of neural tube defects
What is the recommendation of folate supplementation in pregnancy?
400-800 mcg PO QD
Why does chronic kidney disease cause normocytic anemia?
decreased erythropoietin production
Can blood transfusions be used in CKD patients with anemia?
should be avoided to minimize risk of rejection (HLA sensitization)
When would a transfusion be allowed for an anemic CKD patient?
when the patient requires stabilization
Erythropoiesis Stimulating Agents (ESAs)
Epoetin Alfa
Darbepoetin alfa