Anatomy CH 11.5: Cardiovascular system - Blood Vessels
1/147
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
148 Terms
blood vessels
network of:
arteries
arterioles
capillaries
venules
veins
that carries blood away from the heart, to the cells, and back again
arteries
strong elastic vessels adapted for carrying high-pressure blood
transports blood away from the heart
pressure driven
become smaller as they divide and lead to arterioles
arterioles
small branches of an artery that leads to capillaries
get thinner as they approach capillaries
larger arterioles have walls like arteries —> consists of three layers
smaller arterioles have only endothelium, small # of muscle cells, thin layer of CT
lumen
area where blood flows
in both arteries and veins
what is the difference in lumen between veins and arteries
veins are wider
arteries are more narrow
endothelium
in both veins and arteries
layer closest to the lumen
what kind of tissue is the endothelium layer
simple squamous epithelial
tunica media
smooth muscle and elastic fiber
thicker in arteries
precapillary sphincter
regulates pressure when shifting to capillaries
opens capillary beds of skeletal muscles via vasodilation and relaxation during exercise
lessens the blood flow to capillary beds of less important areas of body in order to give blood somewhere else via vasoconstriction and contraction
capillaries
BV with the smallest diameter
connect small arterioles to small venules
only a layer of endothelium
Permeability varies from one tissue to the next due to the size of the openings between cells
density varies from body part
areas with high metabolic activity have higher densities
allows nutrients, gases, and wastes to be exchanged between the blood and tissue fluid
exchange in capillaries
constant exchange of respiratory gases, nutrients, metabolic wastes between capillaries and tissue via diffusion, filtration, and osmosis
depends on concentration gradient
typically goes from high to low
more fluid leaves capillaries by filtration than return via osmosis
lymphatic vessels
pick up excess tissue fluid that is not picked up by capillaries and returned into circulation
blood flow in capillaries
blood with a high concentration of oxygen + nutrients enters capillaries
these things diffuse into tissues
plasma stays in the blood bc of large size
what is diffused INTO capillaries
carbon dioxide (CO2) and metabolic wastes diffuse from tissue fluid into capillaries
hydrostatic pressure
How things enter capillaries
occurs from the pumping of the heart
generates force for the filtration of substances through capillaries
opposite pressure of colloid osmotic pressure
when is BP higher than colloid osmotic pressure in capillaries
at the arteriolar end of capillaries
this means filtration occurs the most here
when is BP lower than colloid osmotic pressure in capillaries
at venular ends of capillaries
reabsorption is greater here
where are capillary openings larger
kidney
intestines
endocrine glands
where are capillary openings smaller
muscle tissues
colloid osmotic pressure
pressure caused by the presence of plasma proteins that stay in the blood and draw water into capillaries
opposite force of hydrostatic pressure
three types of capillaries
continuous
fenestrated
sinusoidal
continuous capillaries
found in skin (dermis/hypodermis), muscles, NS
small gaps that allow small molecules to pass through
fenestrated capillaries
found in kidneys, small intestine, endocrine glands (hormones)
filters
has small pores that allow small molecules to pass through
sinusoidal capillaries
found in liver, spleen, lymph nodes, bone marrow, endocrine glands
has large gaps and pores that allow blood cells through
venules
lead from capillaries merge to form larger veins that return blood to heart
veins
carries blood back to the heart
blood is low in oxygen
different from arteries because it has valves to prevent backflow of blood
BP is lower than artery
functions as blood reservoirs
vasoconstriction of veins in times of blood loss can restore normal BP even after 25% of blood being lost to a hemorrhage
type of wall - artery
thick + strong
3 layers
endothelial lining
middle layer of smooth muscle + elastic CT
outer layer of CT
type of wall - arteriole
thinner wall than artery
3 layers
smaller arterioles have an endothelial lining + smooth muscle tissue + small amount of CT
type of wall - capillary
single layer of squamous epithelium
type of wall - venule
thinner wall than arteriole
less smooth muscle + elastic CT
type of wall - vein
thinner wall than artery but similar layers
middle layer is thinner
has valves
blood pressure
force blood exerts against inner walls of blood vessels
moves through lumen of arteries and arterioles
decreases with distance from heart
arteries > arterioles > capillaries > veins
exists all throughout the cardiovascular system
refers to systemic arterial pressure (blood vessel pressure)
increases with age
where is BP highest? lowest?
highest in arteries
lowest in veins
highest farther away from heart
lower closer to heart
systolic level
top number
force of heart pump
pumping out blood
maximum arterial pressure during contraction
normal: <= 120 mmHg
diastolic level
bottom number
heart filling up with blood
minimum arterial pressure during relaxation
<= 80 mm Hg
prehypertension
highest risk of high BP
120-139 mmHg / 80-89mmHg
hypertension stage 1
high BP
140-159 / 90-99
hypertension stage 2
severe high BP
>160 / >100
hypertensive
emergency condition
>=180 / >110
hypertensive crisis
leads to heart attack/stroke/death
hypertension / high BP
silent killer —> 1/3 people don’t know they have —>no symptoms
uncontrollable risk factors
primary and secondary types
uncontrollable risk factors of hypertension
genetics
age
primary hypertension
aka essential HT
the cause in unknown
idiopathic
secondary hypertension
results of medical problems or meds
kidney or liver diseases
physical or physiological
atherosclerosis
blood viscosity
caused by dehydration / EPO
heart function
increase HR leads to increase chance of stroke
volume
amount of blood that the heart out per beat
what contributes to high BP
diet
high sodium
stress/trauma
obesity
smoking tobacco
nicotine
caffeine
excessive alcohol
poor sleep
sleep apnea
arterial blood pressure
rises and falls according to pattern established by cardiac cycle
systolic + diastolic
measured by sphygmomanometer
hypotension
<90/60 mmHg
dehydration
rapid position changes (orthostatic / sudden drop)
pregnancy (preeclampsia)
heart failure
severe infection (sepsis)
allergic reactions
meds
diuretics (water loss - pee a lot)
beta blockers
anti depressants
nutritional deficiencies
lack B12 or B9
food rich in potassium help
APICAL pulse
pulse at the heart
needs the stethoscope
pulse
if pulse is normal: count for 30s and multiply by 2 OR 15s and multiply by 4
normal: 60-100 bpm
if irregular check pulse for one minute
athletes: 40-60bpm
tachycardia
bradycardia
irregularity
Arrythmia
which finger has its own pulse
thumb
do not use when checking pulse
tachycardia
high pulse
resting over 100bpm
caused by:
infection
dehydration
cardiac condition
bradycardia
low pulse
resting below 60 bpm
caused by:
drugs
not athlete
irregularity
Arrhythmia
skipping beats
uneven beats
pulse pressure
difference between systolic + diastolic
normal difference is 40 mmHg
indirect measurement of cardiac output
diastolic - systolic
low pulse pressure
<25-30
BASH
BASH
low pulse pressure
B LEEDING (hemorrhage)
A ORTIC (largest artery)
S TENOSIS (narrowing of BV)
H EART FAILURE
high pulse pressure
>40
AFAR
high pulse pressure
A THROSCLEROSIS
F EVER
A ORTIC
R REGURGE
what artery is used to measure blood pressure
brachial artery
sphygmomanometer
listens to sound
release pressure = first sound = systolic
after sound = diastolic
3 layers of artery
tunica interna
tunica medai
tunica externa
tunica interna
innermost endothelial layer of artery
prevents platelet aggregation/clumping
secretes substances to regulate blood flow
tunica media
thick middle layer of artery
composed of smooth muscle
tunica externa
outermost CT layer of artery
thin
attaches artery to tissues
sympathetic impulses
innervate the smooth muscle in the walls of arteries + arterioles via vasomotor fibers
vasomotor fibers
autonomic nerve fibers that innervate the vascular smooth muscle of blood vessels to regulate their diameter
constriction
dilation
controls blood flow
sympathetic stimulation
causes muscle contraction
results in vasoconstriction of arteries
vasoconstriction
the constriction of arteries
increases peripheral resistance + BP
vasodilation
vasomotor impulses are inhibited
dilation of arteries occur
decreases peripheral resistance and BP
arterial blood pressure points
radial artery
temporal artery
mandibular artery
axillary artery
carotid artery
brachial artery
femoral artery
APICAL pulse
dorsalis pedis artery
factors that influence arterial BP
cardiac output
blood volume
peripheral resistance
blood viscosity
cardiac output
directly affects BP
total volume of blood the heart pumps per minute
stroke volume x heart rate
average CO = 70mL/beat x 72 beats/min = 5040mL/min
if stroke volume or heart rate increases, so does the cardiac output
stroke volume
amount of blood discharged from each ventricle with each contraction
about 70mL
heart rate
number of heart beats per min
average is 72 beats/min
cardioinhibitory reflex arc
cardiac output increases
BP increases
baroreceptors in aortic arch + carotid sinuses are stimulated
sensory impulses to cardiac center
parasympathetic impulses to heart
SA node inhibited
heart rate decreases
BP returns normal (ish)
baroreceptors
sense changes in Bp
located in aortic arch + carotid arteries
cardioinhibitory reflex
in arterial BP increases, baroreceptors send impulses to cardiac center of medulla oblongata
parasympathetic impulses are sent to sinoatrial node to slow heart rate + decrease CO and BP
sinoatrial node
the heart's natural pacemaker
cardioaccelerator reflex
if arterial BP decreases, medulla oblongata sends sympathetic impulses to increase heart rate + CO + BP
some other factors that cause change in BP
emotionally upset
exercise
rise in temperature
peripheral resistance
controls BP
the resistance to blood flow determined by the diameter of small arterioles
changes in arteriolar diameter changes BP
Symphathetic nerves change diameter in response to BP changes
smaller diameters will provide greater resistance + increase BP
some chemical can impact by affecting precapillary sphincters + smooth muscle
what chemicals affect peripheral resistance
increase CO2 and decreased O2 and decreased pH cause vasodilation in tissues with high metabolic needs
epinephrine and norepinephrine causes vasoconstriction of systemic vessels which increase PR and BP
vasomotor center
in medulla oblongata
adjusts sympathetic impulses of smooth muscles in arterioles
adjusts BP
contractions of skeletal muscles - vein blood flow
squeeze blood back up veins one section at a time
respiratory movements - vein blood flow
creates differences in thoracic + abdominal pressures which draw blood back up the veins
venoconstriction - vein blood flow
returns blood to heart
initiated by sympathetic reflexes when BP in veins is low
aorta
body’s largest diameter artery
principal branches of aorta
ascending aorta
aortic arch
descending aorta
thoracic aorta
abdominal aorta
ascending aorta
first portion
extends out of left ventricle
aortic sinuses are opposite of the valve cusps
region/organ supplied: heart

branch of ascending aorta
right + left coronary arteries

aortic arch
bend of aorta
after ascending aorta
3 branches

3 branches of aortic arch
brachiocephalic trunk
left common carotid artery
left subclavian artery
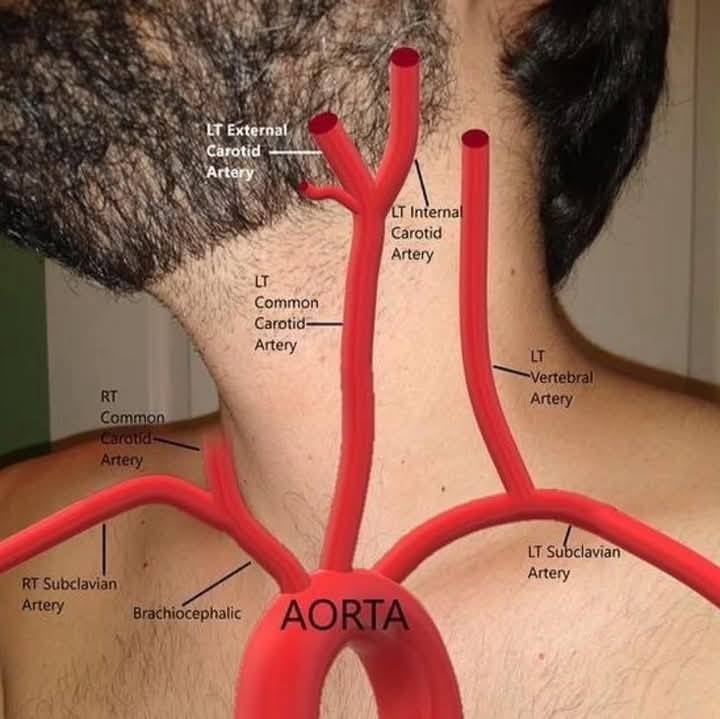
brachiocephalic trunk region/supplies
right upper limb, right side of head
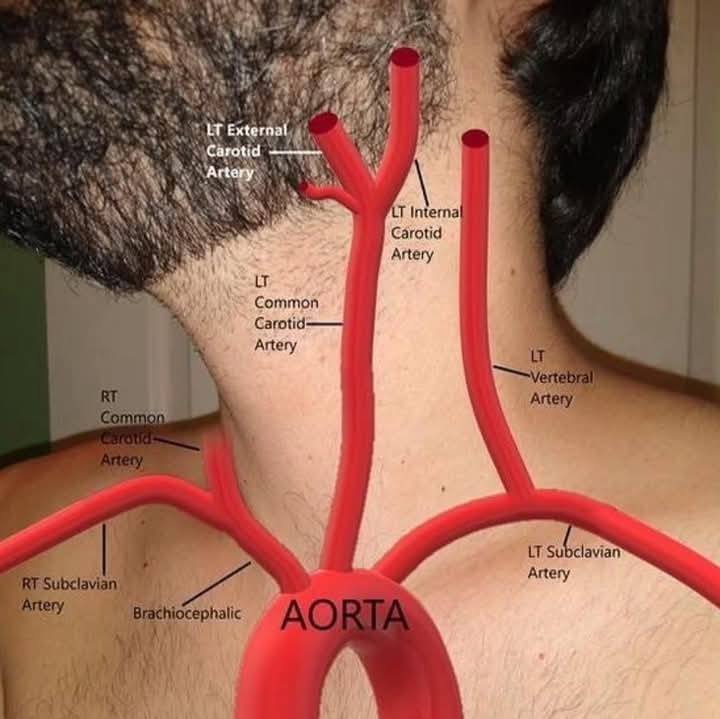
left common carotid artery region/supplies
left side of head
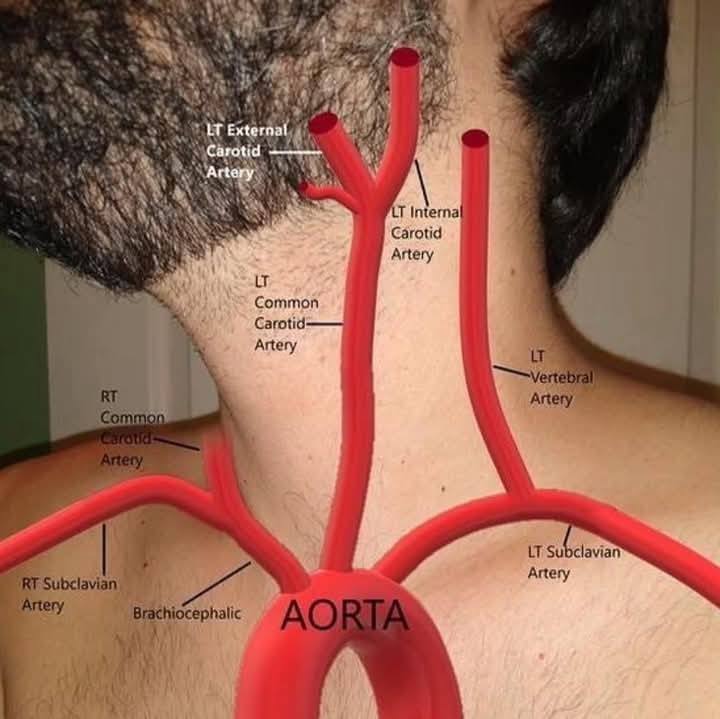
left subclavian artery region/supplies
left upper limb
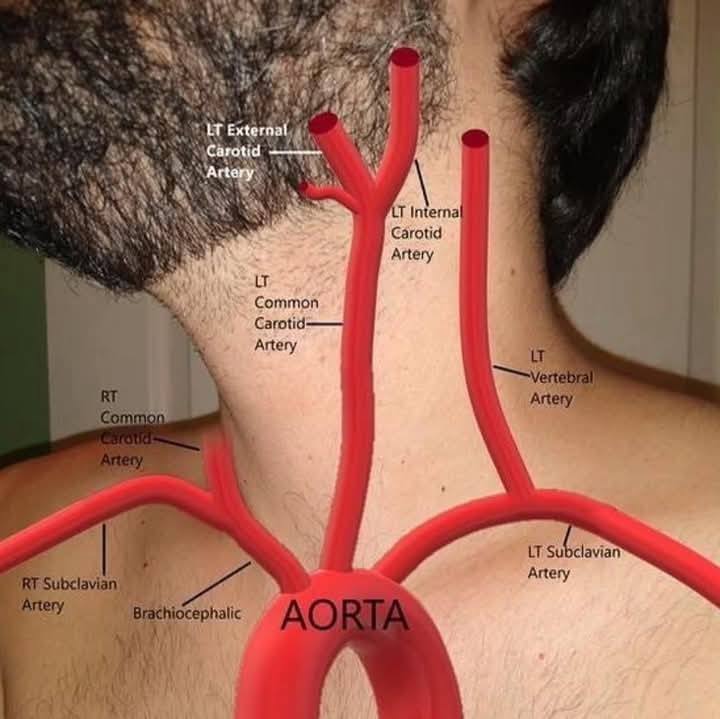

descending aorta
follows arch
extends down the anterior to the vertebral column
consists of thoracic aorta and abdominal aorta
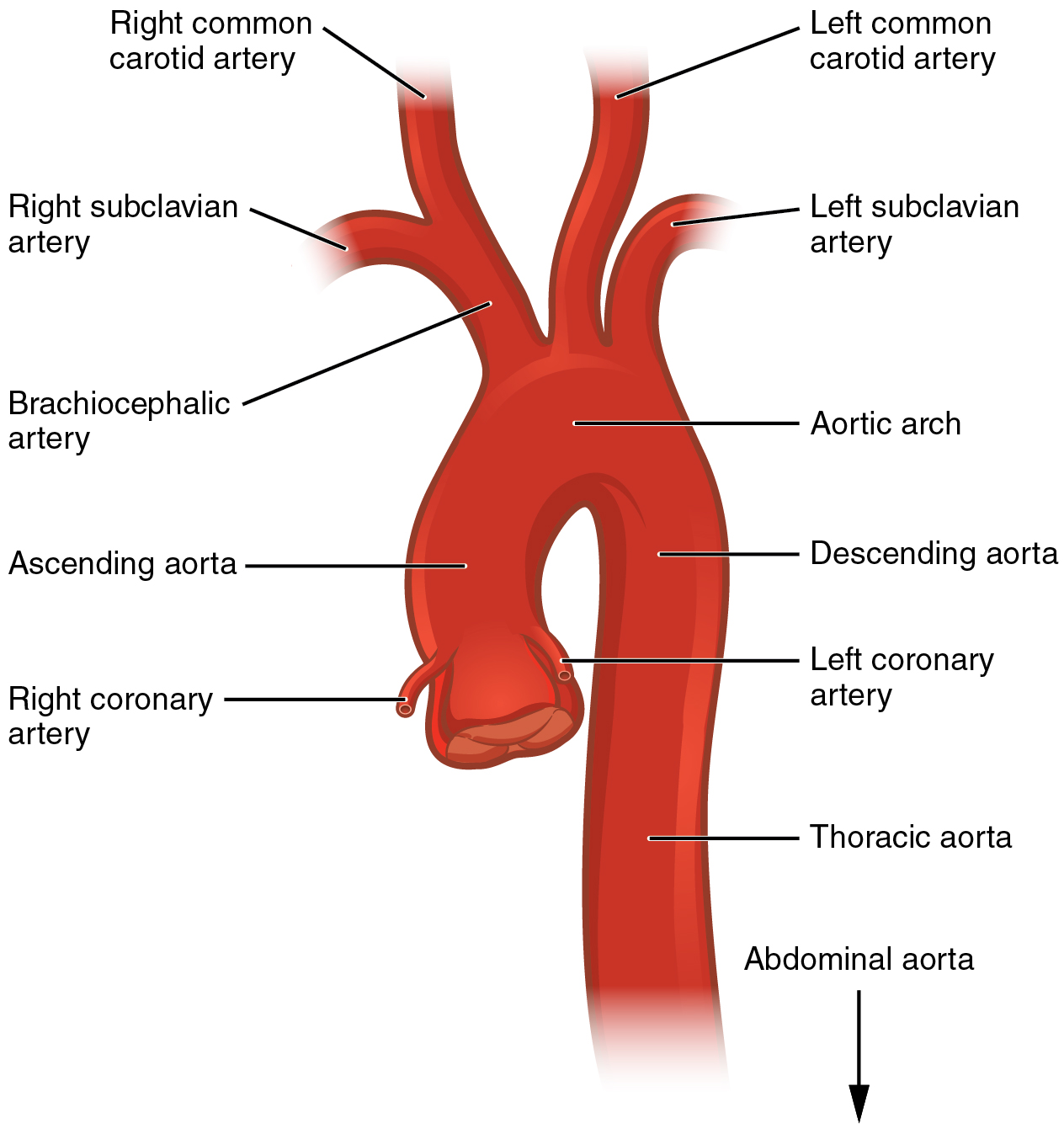
thoracic aorta
portion above diaphragm
allows for small arteries to supply thoracic wall and viscera
thoracic aorta branches
bronchial
pericardial
esophageal
mediastinal
posterior intercostal
bronchial artery
thoracic aorta
supplies bronchi
pericardial artery
thoracic aorta
supplies pericardium