Filtration, Reabsorption, Secretion
1/62
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
63 Terms
mechanisms of urine formation:
the kidneys filter the body’s entire plasma volume ____ times each day
60
mechanisms of urine formation:
the filtrate contains ______
all plasma components except proteins
mechanisms of urine formation:
the filtrate loses _____ to become urine
water, nutrients, and essential ions
mechanisms of urine formation:
the urine contains _____ and _____
metabolic wastes and unneeded substances
mechanisms of urine formation:
urine formation and adjustment of blood composition involves three main processes
glomerular filtration, tubular reabsorption, secretion
glomerular filtration:
principles of ____ that account for _____ in all capillary beds apply to the glomerulus as well
fluid dynamics, tissue fluid
glomerular filtration:
the glomerulus is more efficient than other capillary beds because (3)
filtration membrane more permeable
higher blood pressure
higher net filtration pressure
glomerular filtration:
______ are not filtered and are used to maintain ______ of the blood
plasma proteins, oncotic pressure
______ is the pressure responsible for filtrate formation
net filtration pressure (nfp)
NFP equals the
glomerular hydrostatic pressure minus the oncotic pressure of glomerular blood combined with the capsular hydrostatic pressure
NFP equation
NFP = HPg - (OPg + HPc)
pressure is the force that drives the movement of water molecules from a region of ____ solute concentration to a ____ concentration
low, high
____ pressure is the force exerted by _____ in the blood that ______ into the blood vessels
oncotic, proteins, draws water
glomerular filtration rate (GFR)
total amount of filtrate formed per minute by the kidneys
factors governing filtration rate at the capillary bed are (3)
total surface area available for filtration
filtration membrane permeability
net filtration pressure
GFR is _____ to the NFP
directly proportional
changes in GFR normally result from changes in _____
glomerular blood pressure
if the GFR is too _____, needed substances cannot be _____ quickly enough and are lost in ____
high, reabsorbed, urine
if the GFR is too _____, everything is _____, including _____ that are normally disposed of
low, reabsorbed, wastes
regulation of glomerular filtration:
three mechanisms control the GFR
renal autoregulation (intrinsic system), neural controls, hormonal mechanism (the renin-angiotensin system)
intrinsic controls:
under normal conditions, _____ maintains a nearly ____ glomerular filtration rate
renal autoregulation, constant
intrinsic controls:
autoregulation entails two types of control
myogenic and flow-dependent tubuloglomerular feedback
intrinsic controls:
myogenic responds to
changes in pressure in the renal blood vessels
intrinsic controls:
flow-dependent tubuloglomerular feedback senses changes in the
juxtaglomerular apparatus
extrinsic controls:
when the sympathetic nervous system is at rest, renal blood vessels are _____
maximally dilated
extrinsic controls:
when the sympathetic nervous system is at rest, _____ mechanisms prevail
autoregulation
extrinsic controls:
under stress, ______ is released by the sympathetic nervous system
norepinephrine
extrinsic controls:
under stress, ____ is released by the adrenal medulla
epinephrine
extrinsic controls:
under stress, ____ constrict and ____ is inhibited
afferent arterioles, filtration
extrinsic controls:
the sympathetic nervous system also stimulates the ____
renin-angiotensin mechainsm
renin-angiotensin mechanism:
triggered when the _____ release renin
JG cells
renin-angiotensin mechanism:
renin acts on _____ to release _____
angiotensinogen, angiotensin I
renin-angiotensin mechanism:
angiotensin I is converted to _____
angiotensin II
renin-angiotensin mechanism:
angiotensin II causes ______ to rise
mean arterial pressure
renin-angiotensin mechanism:
angiotensin II stimulates the _____ to release ____
adrenal cortex, aldosterone
renin-angiotensin mechanism:
as a result, both ____ and ____ rise
systemic and glomerular hydrostatic pressure
renin-angiotensin mechanism flow
enzyme reaction, angiotensin I, enzyme reaction, angiotensin II, stimulates, adrenal cortex to secrete, aldosterone
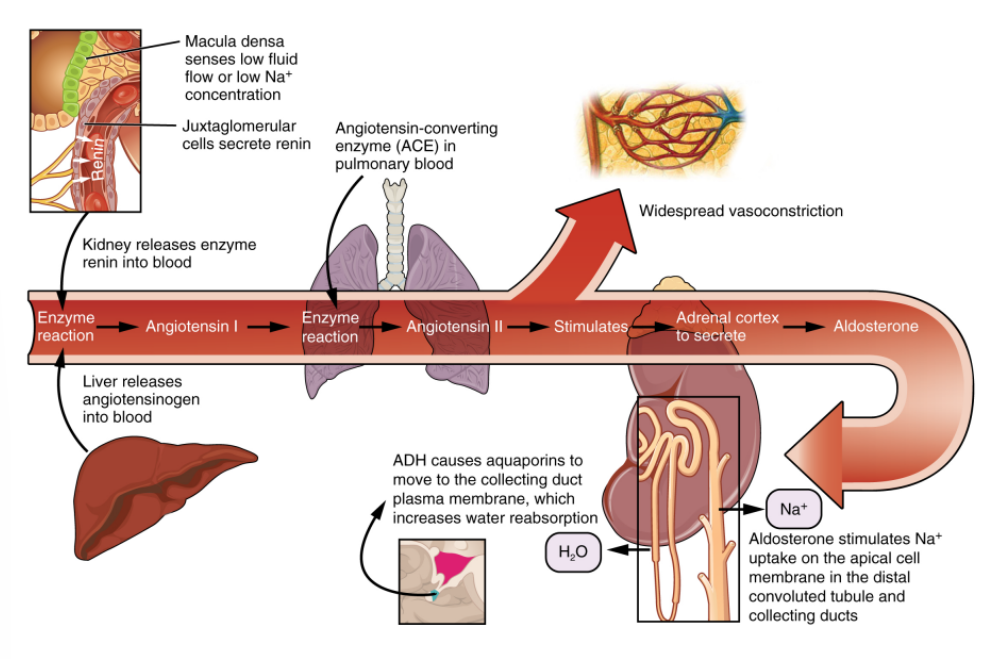
renin-angiotensin mechanism:
____ releases angiotensinogen into blood
macula dense sense ____ or ____
juxtaglomerular cells secrete ____
____ releases enzyme renin into blood
____ in pulmonary blood
aldosterone stimulates ____ on the apical cell membrane in the ____ and ____
liver
low fluid flow or low Na+ concentration
renin
kidney
angiotensin-converting enzyme
Na+ uptake, distal convoluted tubule, collecting ducts
renin release is triggered by ______ of the granular JG cells
reduced stretch
renin release is triggered by stimulation of the JG cells by
activated macula densa cells
renin release is triggered by direct stimulation of the JG cells via
beta-adrenergic receptors by renal nerves
other factors affecting glomerular filtration:
prostaglandins (PGE2 and PGI2) are ______ produced in response to ____ and _____
vasodilators, sympathetic stimulation, angiotensin II
other factors affecting glomerular filtration:
prostaglandins (PGE2 and PGI2) are thought to prevent ____ damage when _____ is ____
renal, peripheral resistance is increased
other factors affecting glomerular filtration:
_____ is vasodilator produced by the vascular endothelium
nitric oxide
other factors affecting glomerular filtration:
____ is a vasoconstrictor of renal vasculature
adenosine
other factors affecting glomerular filtration:
endothelin is a powerful _____ secreted by ____
vasoconstrictor, tubule cells
sodium reabsorption is almost always by
active transport
sodium reabsorption:
_____ enters the tubule cells at the _____
Na+, luminal membrane
sodium reabsorption:
is actively transported out of the tubules by a
Na+ K+ ATPase pump
sodium reabsorption:
from there it moves to peritubular capillaries due to (2)
low hydrostatic pressure and high osmotic pressure of the blood
sodium reabsorption:
Na+ reabsorption proves the energy and means for ____
reabsorbing most other solutes
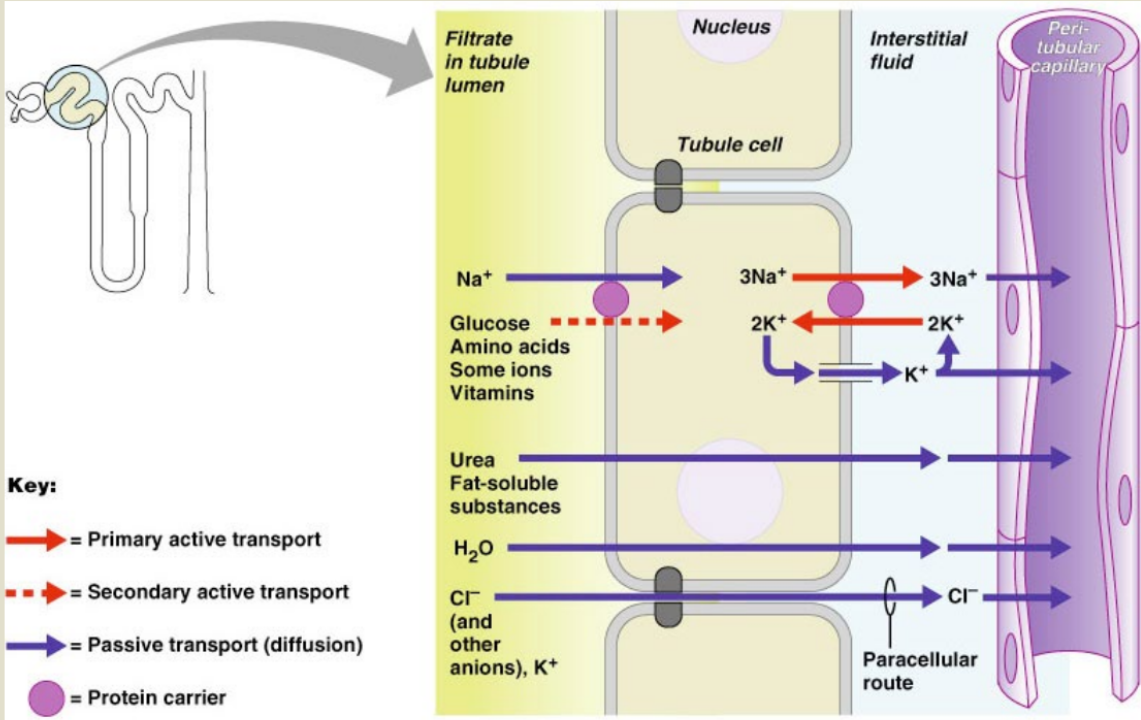
reabsorption by pct cells:
active pumping of Na+ drives reabsorption of
water by osmosis, aided by water-filled pores called _____
_____ and _____ by diffusion
organic nutrients and selected cations by _____
aquaporins
cations and fat-soluble substances
secondary active transport
substances are not reabsorbed if they (3)
lack carriers, are not lipid soluble, are too large to pass through membrane pores
(3) are the most important nonreabsorbed substances
urea, creatinine, uric acid
tubular reabsorption:
all _____ are reabsorbed
organic nutrients
tubular reabsorption:
water and ion reabsorption is _____ controlled
hormonally
tubular reabsorption:
reabsorption may be an ______ or _____ process
active (primary/secondary) or passive
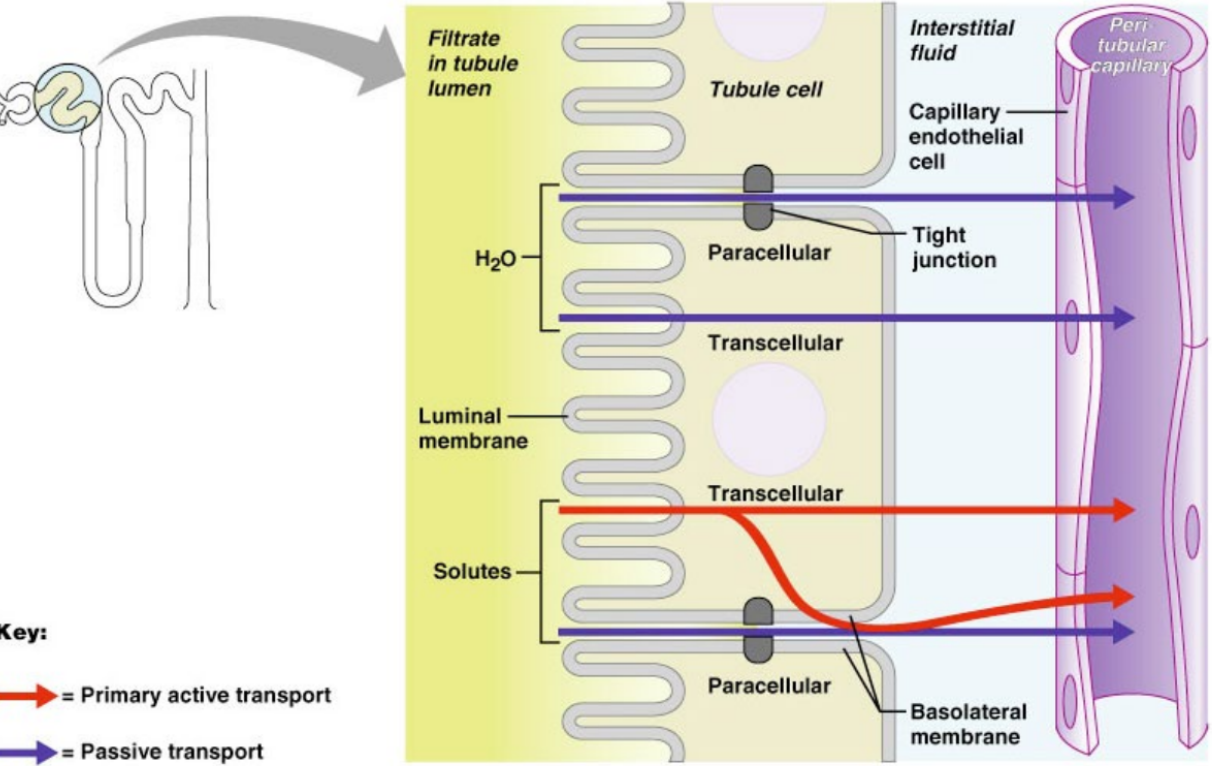
routes of water and solute reaborption
read
tubular secretion:
essentially reabsorption in reverse, where substances move from _____ into _____
peritubular capillaries or tubule cells into filtrate
tubular secretion is important for disposing of
substances not already in the filtrate
tubular secretion is important for eliminating undesirable substances such as
urea and uric acid
tubular secretion is important for ridding the body of
excess potassium ions
tubular secretion is important for controlling
blood pH