CM3 5.5 Wound Management
1/54
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
55 Terms
What should be clarified if a patient says they are unable to move a wounded body part?
Are they truly unable to move it or will they not move it because it hurts?
What are the elements of contamination?
- Time (from injury to initial cleansing; from injury until presentation)
- Initial Wound Care (prior to ED arrival)
- Causative agent (glass, wood, etc.)
- Cleanliness (of body & environment at the time of injury and after)
What are some H&P clues that there is foreign body potential in a wound?
- Object broke/ shattered
- FB Sensation
- Removal of a portion of the object
What are some chronic medical conditions that can increase the likelihood of poor wound healing / increase risk of infection?
Age, nutritional status
Diabetes, Steroids
Immunocompromised
( also Thin Skin
Keloids/ Hypertrophic scar formation)
What is the difference between a hypertrophic scar and a keloid?
Hypertrophic scar stays within the confines of original injury, keloid goes beyond.
When preparing a wound for closure, what must be done (and documented) prior to anesthetizing?
functional & neurovascular exam / status
Which of the following bacteriostatic skin disinfectants are recommended for wound preparation?
A. Chlorhexidine
B. Betadine
C. Povidone-Iodine
A. Chlorhexidine
(Betadine is not recommended; Povidone Iodine IS recommended but is bactericidal and partially fungicidal/ virucidal)

When prepping a wound, a patient's hair is impair ability to properly close. Which is the next best option?
A. Choose different suture material
B. Shave the hair
C. Trim the hair
C. Trim the hair
(FYI can also utilize abx ointment to part hair and keep from getting into the wound; DO NOT SHAVE - Increases infection risk 10x)

T/F Most studies show that prophylactic antibiotics are generally NOT needed for wound care
True (except high risk wounds)

Though the volume of irrigant required for initial wound care is not known, what is the common recommendation?
Anywhere from 60-200 mL/cm of wound length
T/F sufficient pressures for irrigating can be generated using a bulb syringe or fluid from IV bag
False

What are the components of wound preparation?
- Sterile Technique
- Anesthesia
- Hemostasis
- FB consideration
- Skin disinfectant
-+/- Hair "removal"
- +/- prophylactic abx
- Debridement
- Irrigation
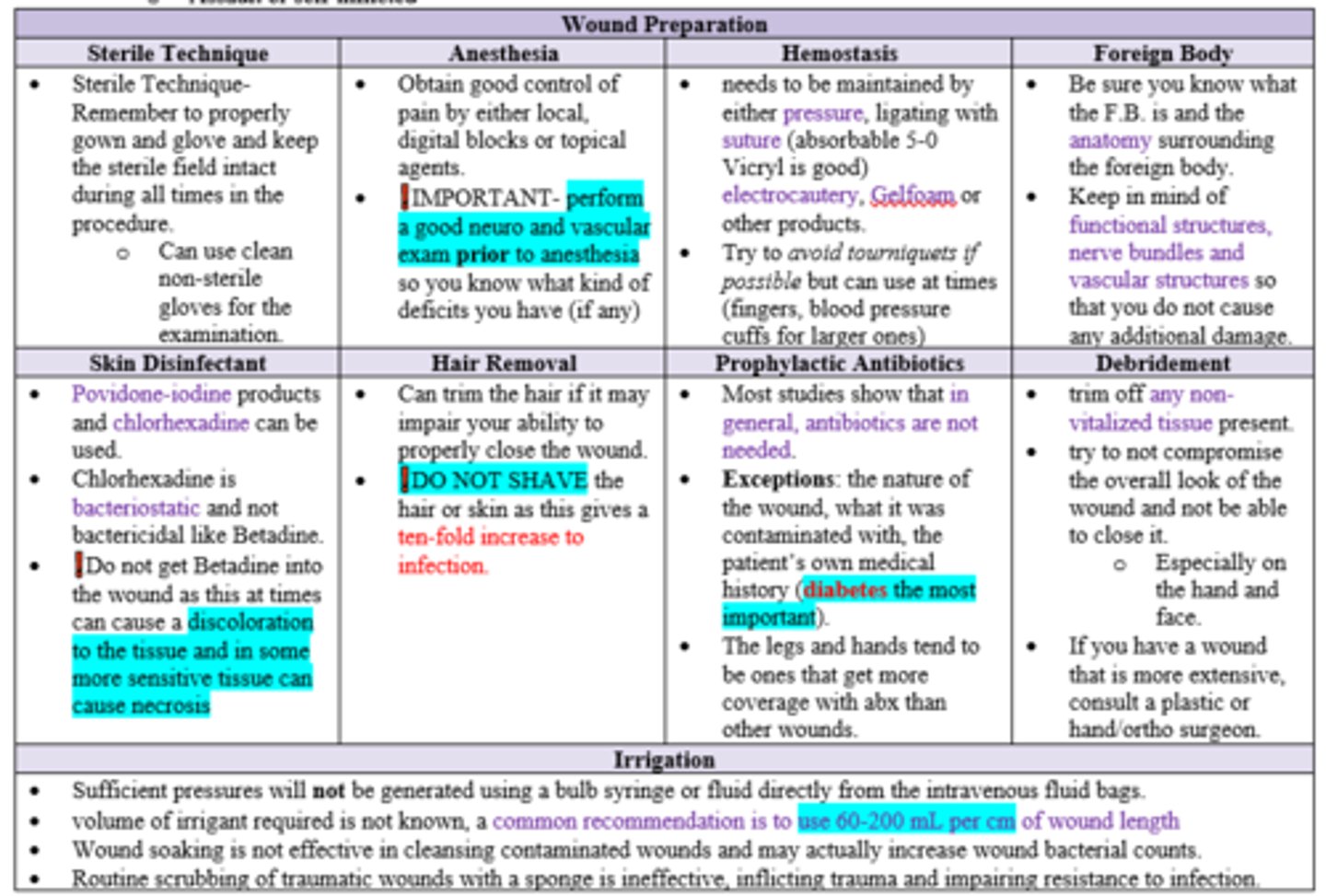
Which of the following is NOT a component of an ideal local anesthetic?
A. Rapid onset & offset of action
B. Potent
C. Vasoconstrictor action or compatible with VC
D. Reversible action
A. Rapid onset & offset of action (We want rapid onset but we also want sufficient duration of action)
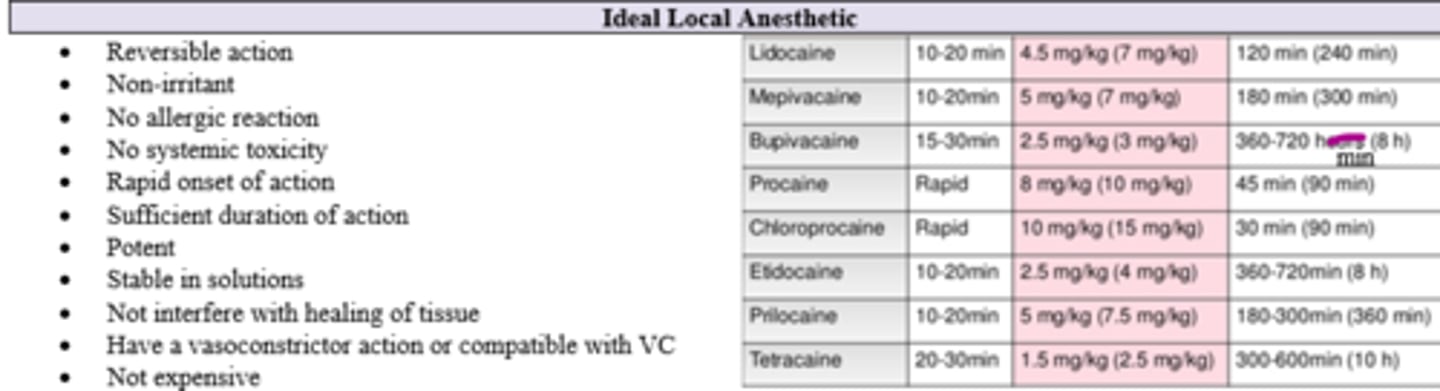
Of the following local anesthetics listed in the lecture, which has the longest duration of action?
A. Lidocaine
B. Procaine
C. Prilocaine
D. Bupivacaine
D. Bupivacaine (360-720 minutes; FYI Etidocaine has the same onset and duration)
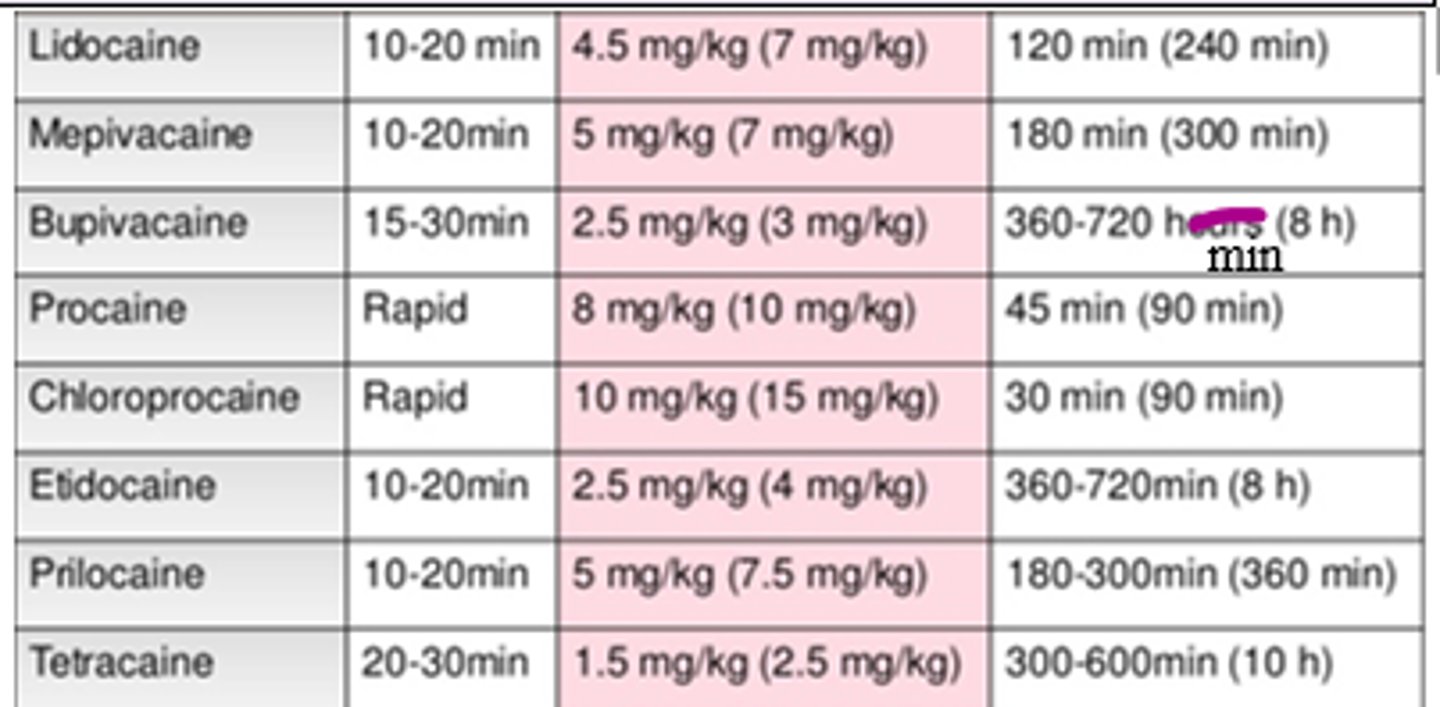
Of the following local anesthetics listed in the lecture, which has the shortest onset of action?
A. Tetracaine
B. Lidocaine
C. Procaine
D. Bupivacaine
C. Procaine (Rapid; other rapid onset is Chloroprocaine)
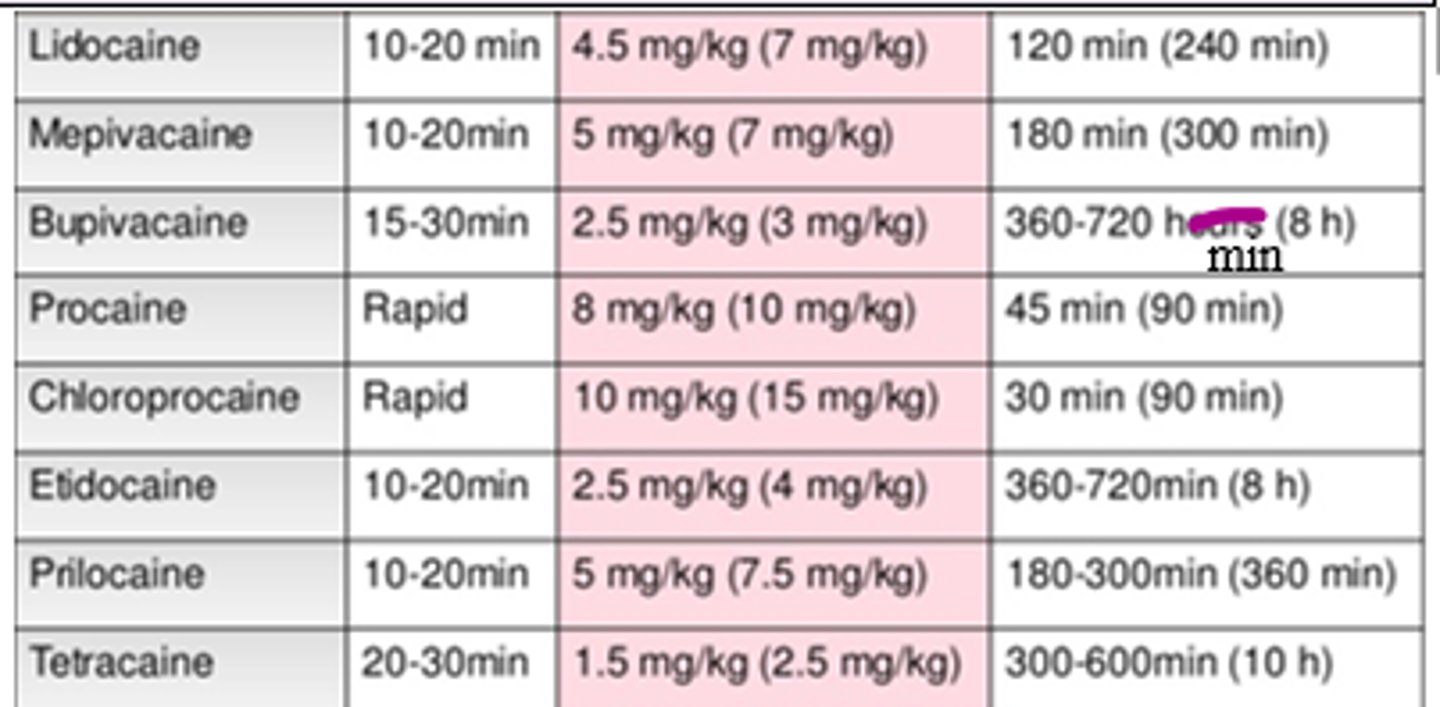
What is the onset, max dose, and duration of Lidocaine?
Onset: 10-20m
Max dose: 4.5 mg/kg (7 mg/kg w epi)
Duration: 120m (240m)
The order of the sensory function blockade is the (same/reverse) order of functional recovery?
Reverse

What is the order of sensory function blockade?
1. Pain
2. Cold
3. Warmth
4. Touch
5. Deep pressure
6. Motor
Elderly, malnourished, and connective tissue disorders pose what for wound risk?
Poor wound repair
What are the 4 methods of wound closure?
1. Sutures (mc)
2. Staples
3. Adhesive tapes
4. Cyanoacrylate Tissue Adhesive
Unless on the face, a wound >____ hours old poses a higher risk of infection?
14
What are the types of wound healing?
Primary
Delayed Primary (Tertiary)
Secondary (if infection risk is high)
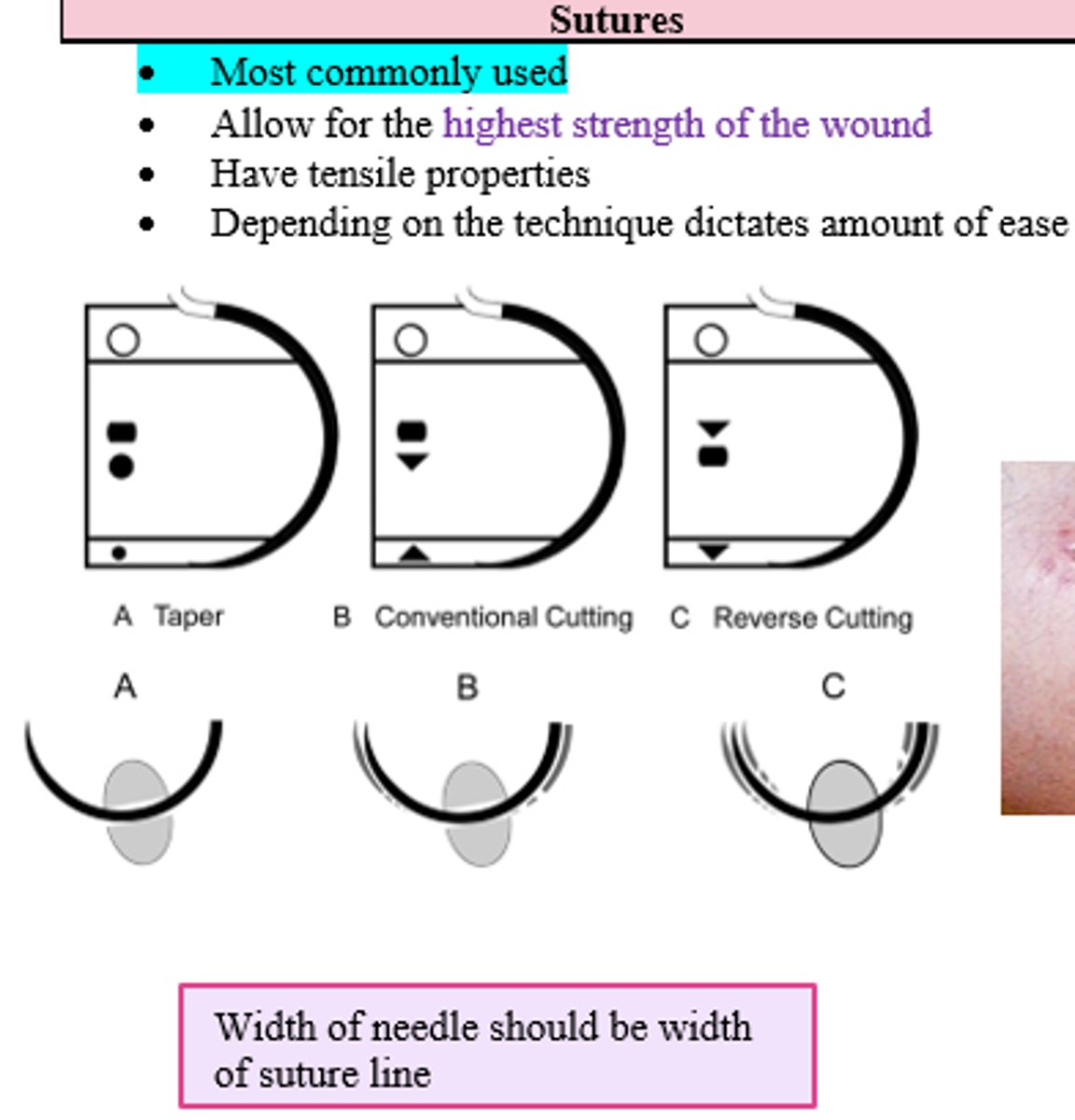
Width of the needle should be (less than/same as/ greater than) the width of the suture line
same as
Which type of wound closure is the most commonly used and allows for the highest strength of the wound?
Sutures
What is the most common closure type?
Simple Interrupted Suture
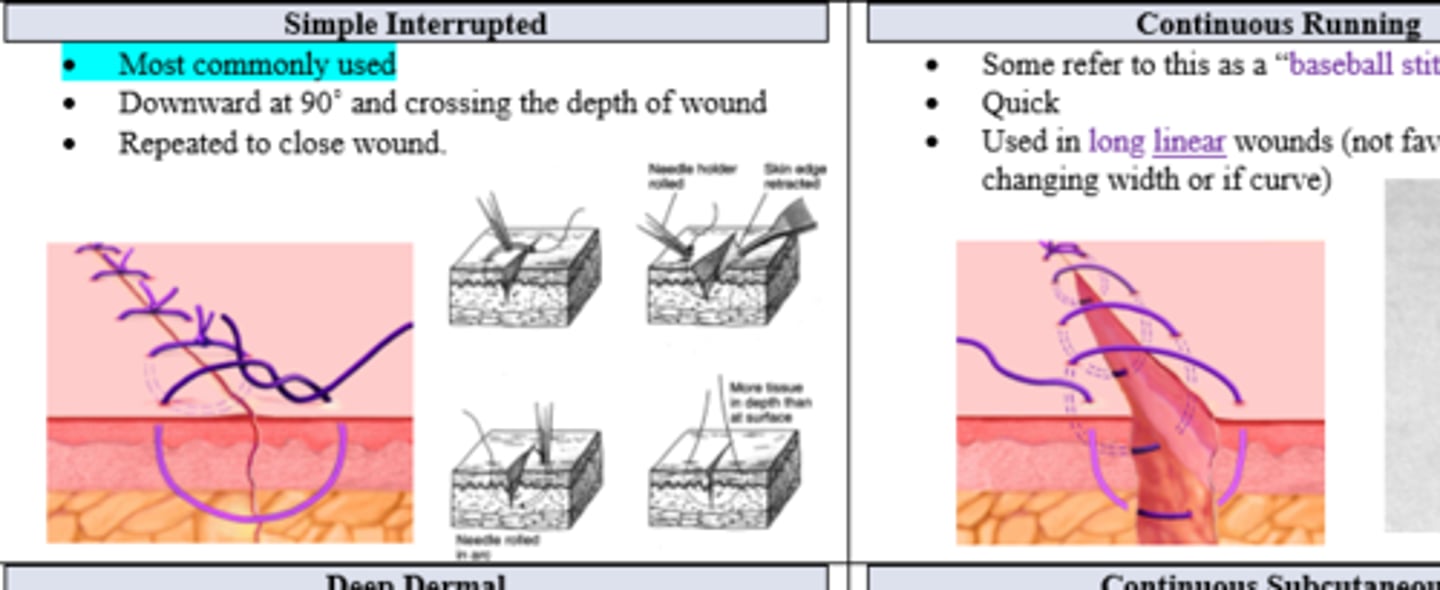
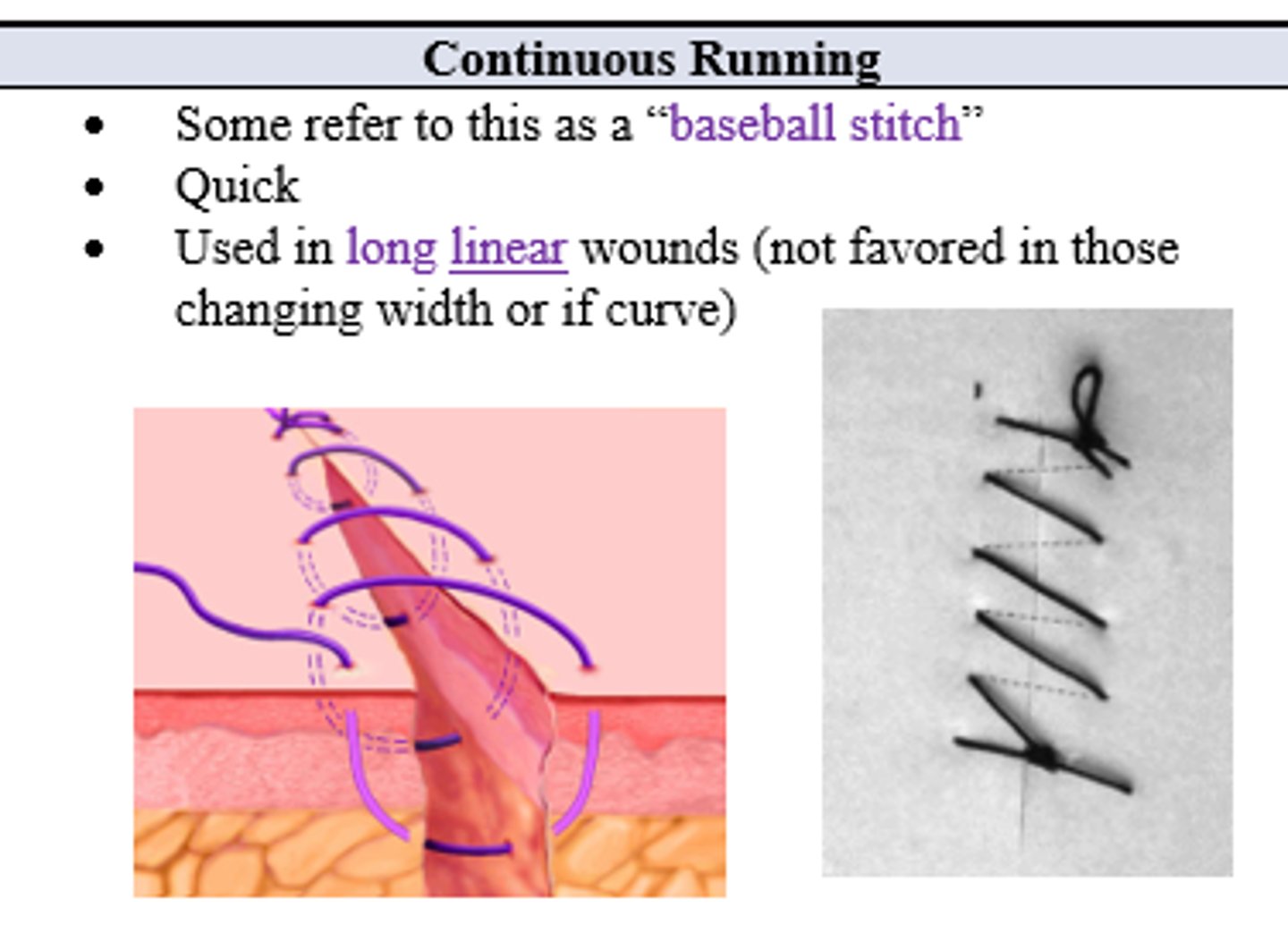
Patient has a long, linear wound that you'd like to close quickly. What stitch, commonly referred to as a baseball stitch, should you use?
Continuous running
What stitch, most commonly used in surgery, requires even "bites" on each side of the wounds with absorbable suture material.
Continuous subcutaneous

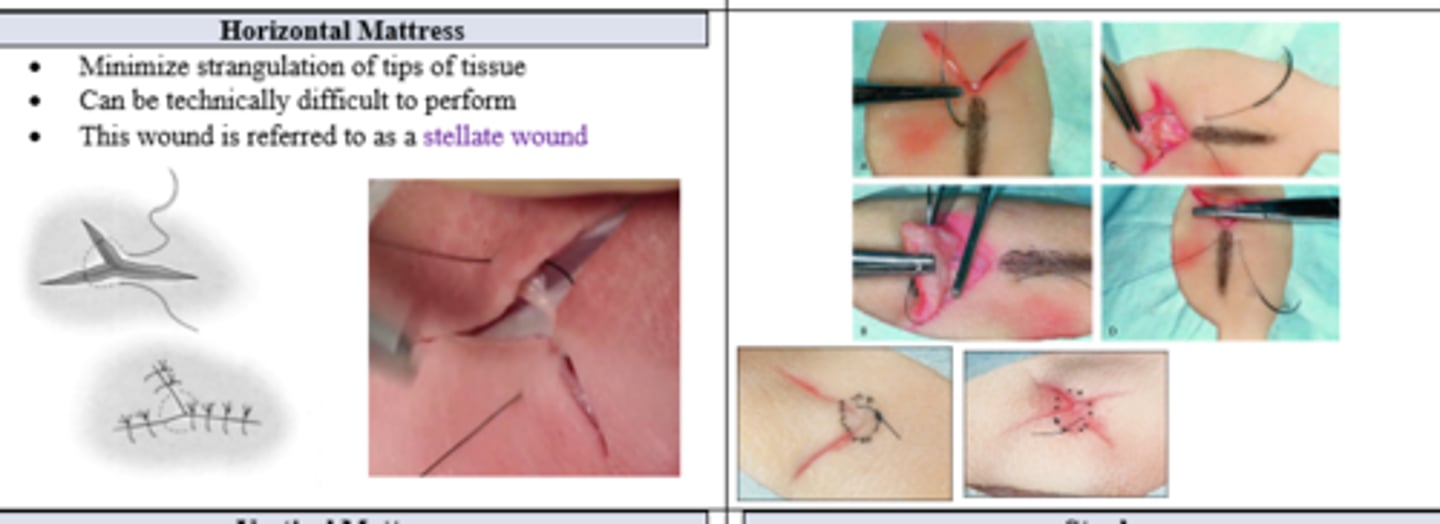
Which stitch can minimize strangulation of tips of tissue in stellate wounds?
Horizontal Mattress (technically a modified corner stitch)
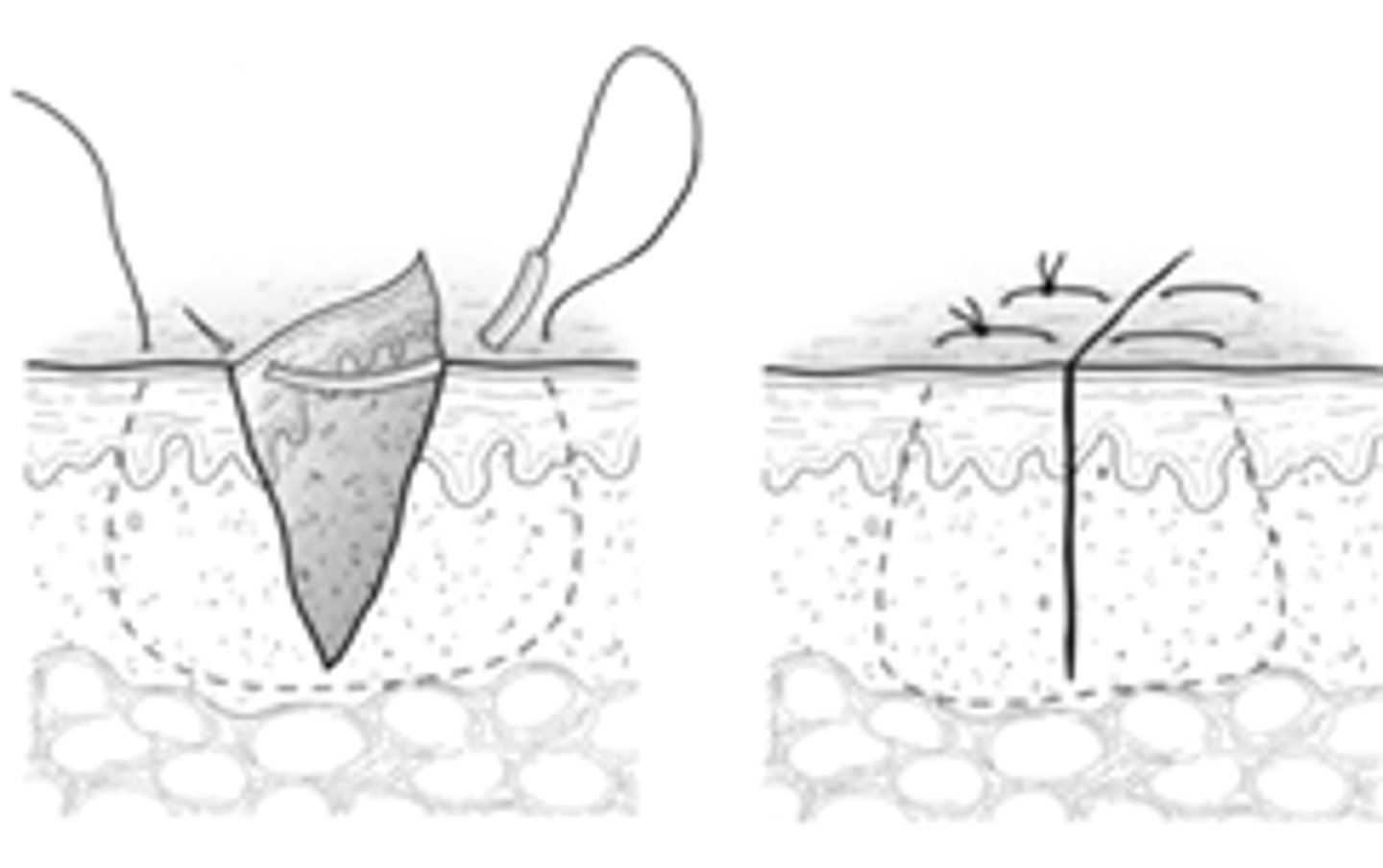
What stitch combines deep and percutaneous closure which is excellent for wound eversion, but care should be taken to not apply too much tension?
Vertical Mattress
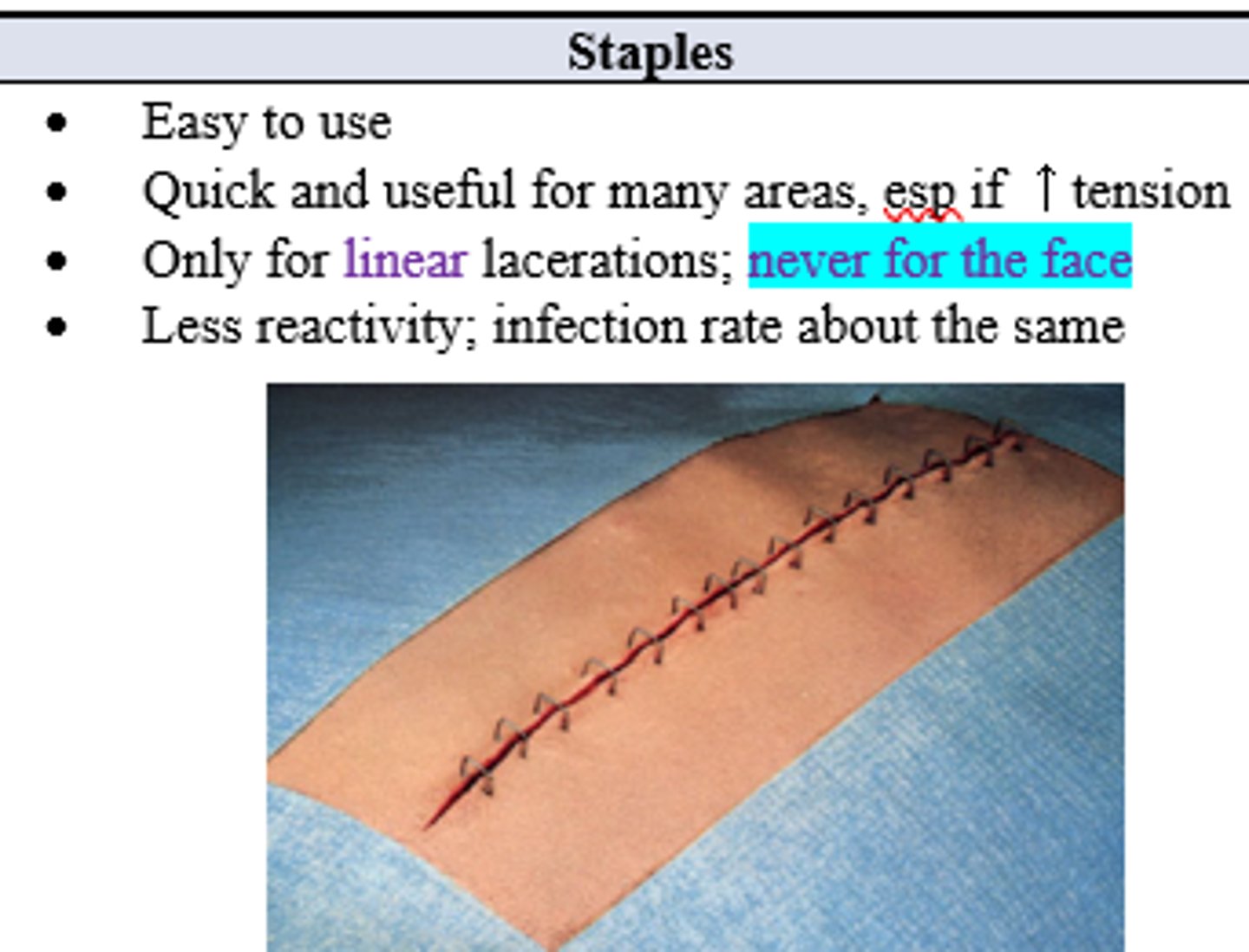
What closure choice is useful for linear lacs, has less reactivity, and is especially useful if there is high tension (but should NEVER be used on the face)?
Staples
Which closure choice tends to slough off with tension or moisture and is most frequently used for reinforcement of sutures?
Adhesive tapes

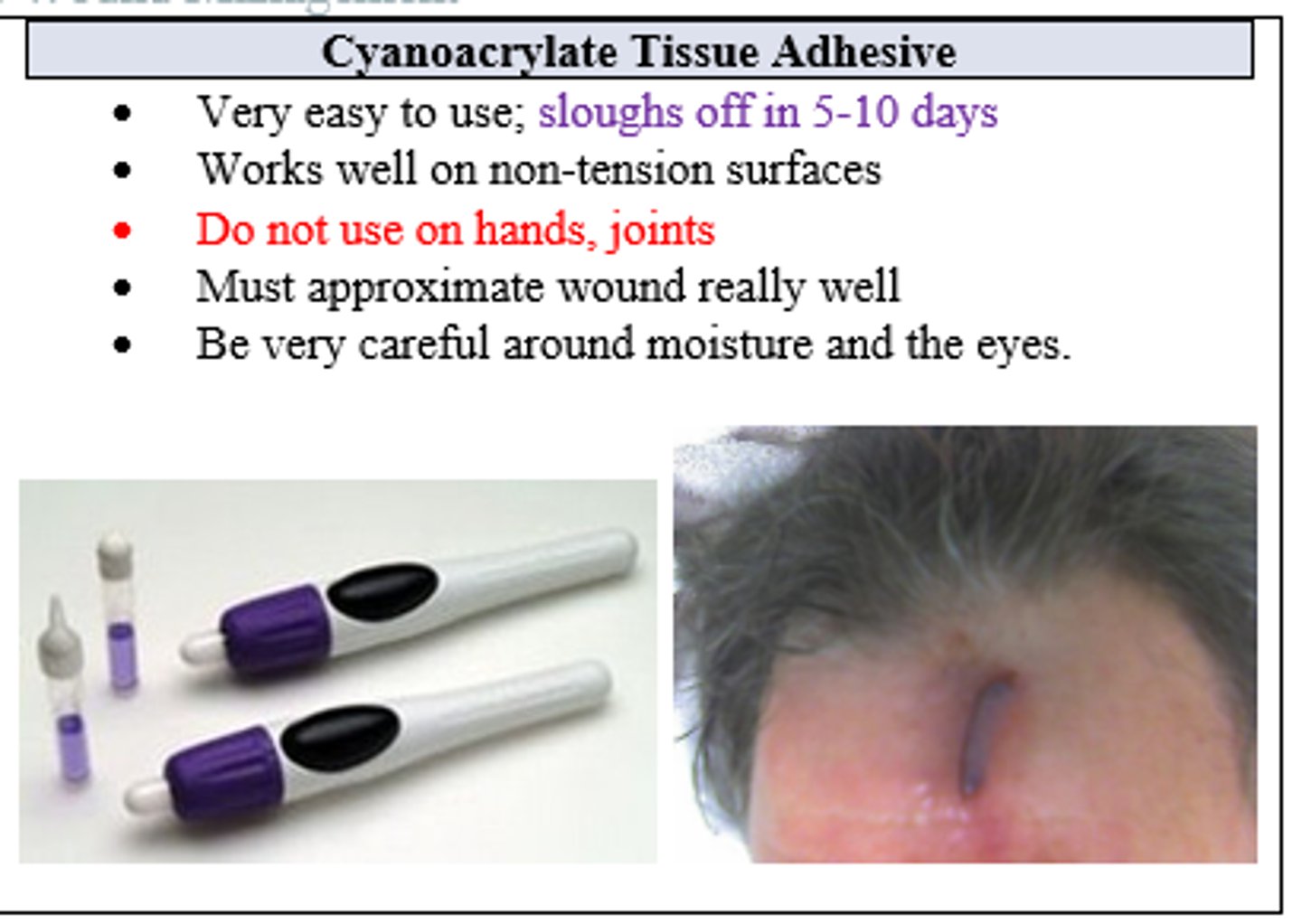
Which closure choice sloughs off in 5-10 days, works well on non-tension surfaces, and should NOT be used on hands or joints?
Cyanoacrylate Tissue Adhesive
Facial and scalp lac's account for ____% of all wounds in the ED
50

When should CT be used as an imaging modality for soft tissue FBs?
Reserved for failed exploration or infection
What imaging modality should be used for all of the following potential FBs:
Bone, Fish spines, metal/aluminum, and teeth?
Radiography

What imaging modality might be first used for all of the following potential FBs:
Glass, metal, pencil graphite, some plastic, stone, wood
US (can also see these on radiography if US is negative)

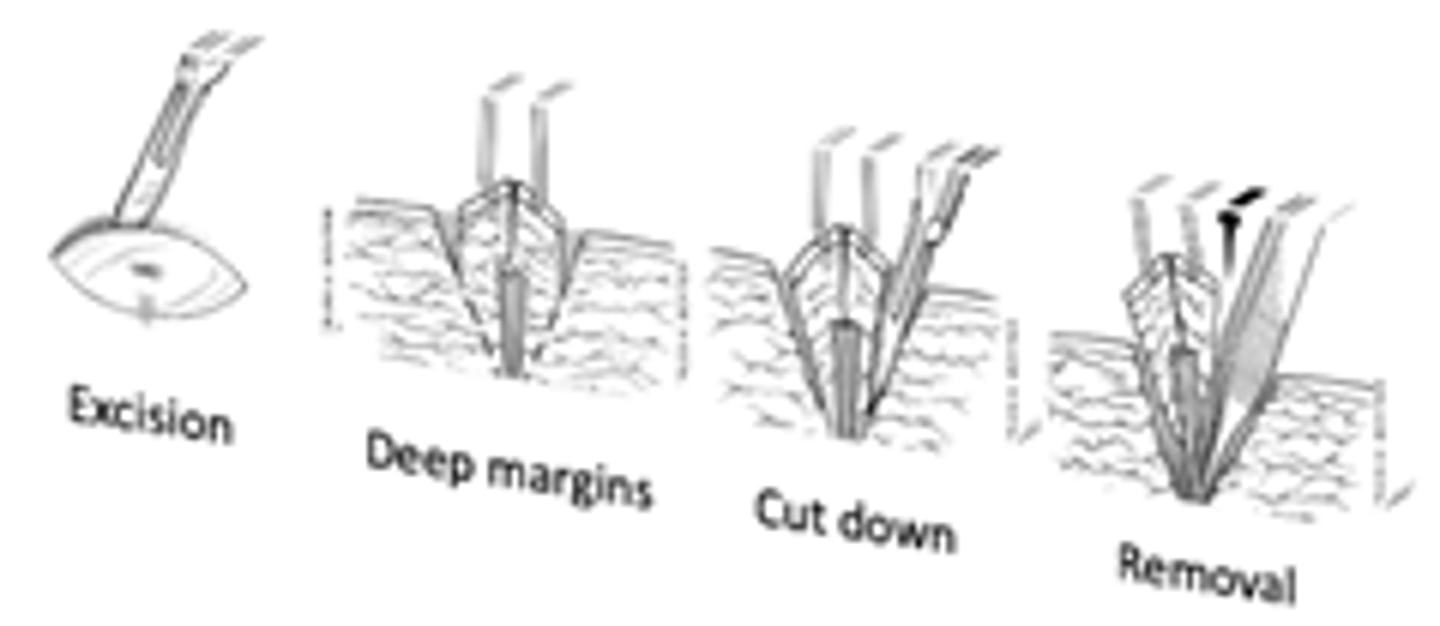
What are the steps for removing a FB?
Excision, deep margins, cut down, removal
What should be considered in a scalp wound?
- Note if galea is injured
- if hematoma present, evacuate so it won't scar down

skin tension lines are (perpendicular/ parallel) to facial lines
perpendicular
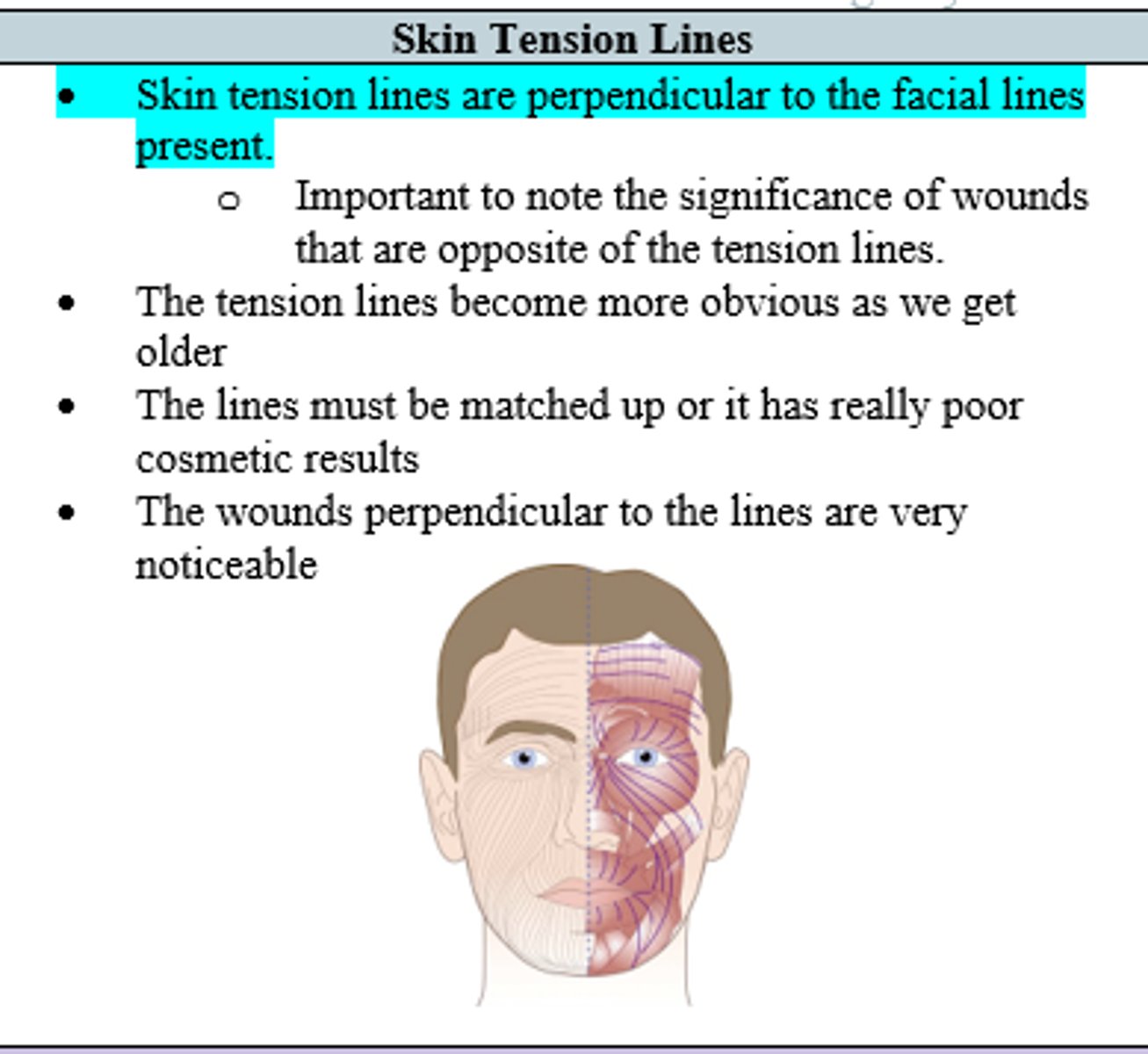
When closing a forehead wound, what needs to be repaired first?
lines in the face

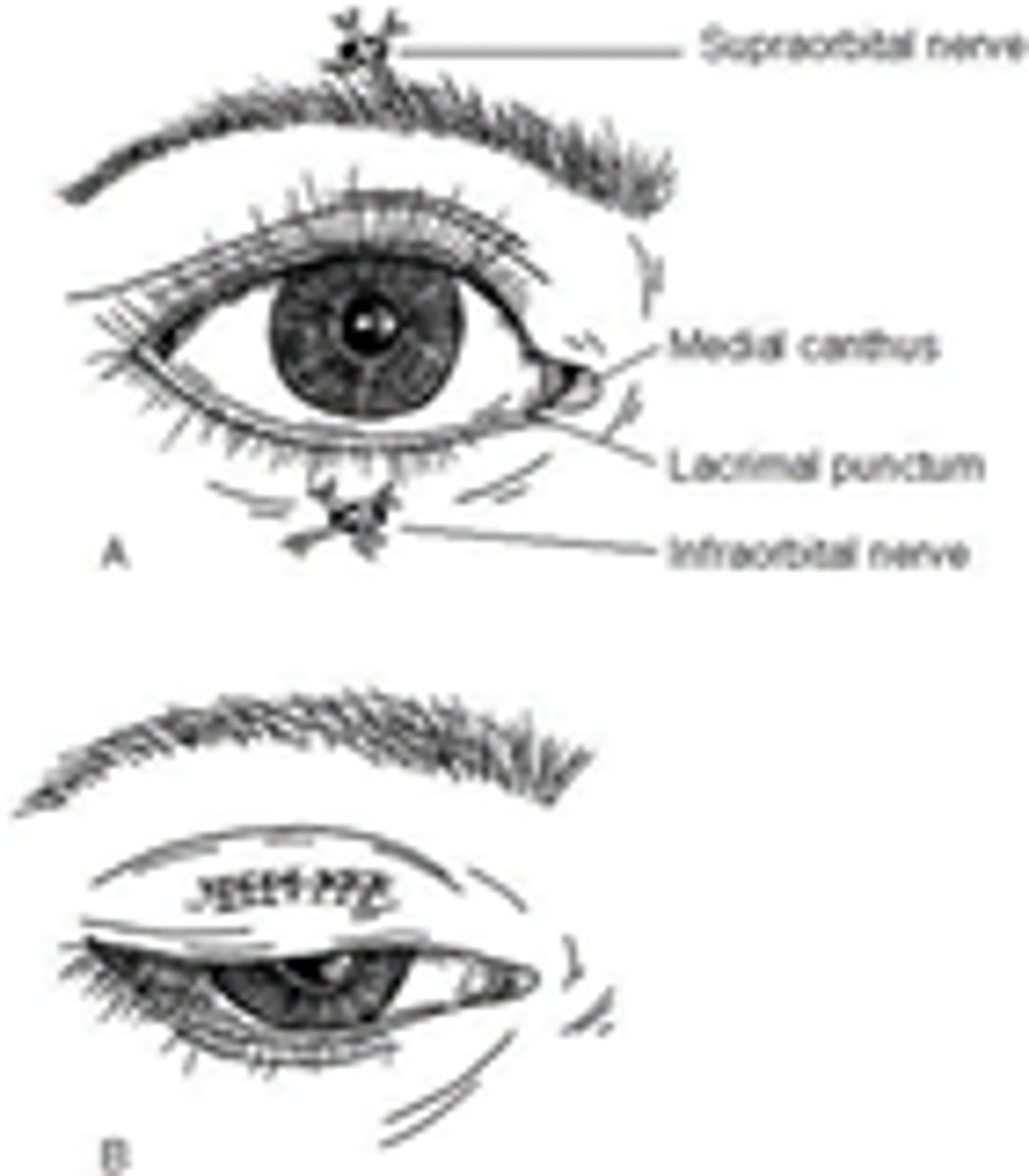
Pt has lid lac that needs to be repaired. How do you proceed?
-Exam to check all associated structures
- Evert the lid to see if went all the way through (if so, do thorough globe exam)
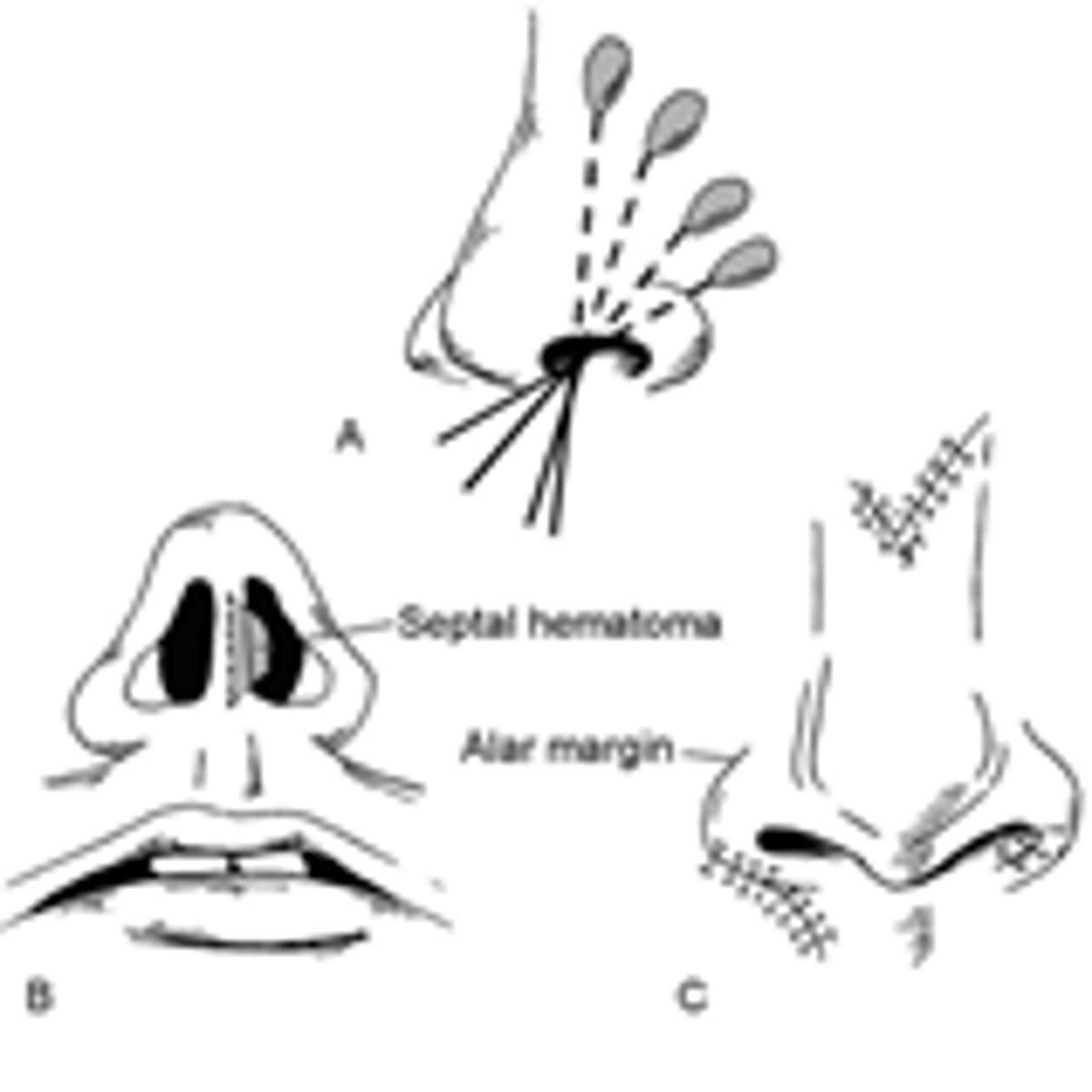
Pt has a through and through lac of their nose. How do you proceed?
- Anesthetize w liquid cocaine
- Start at rim of ala and work way out
- Ensure septal hematoma is not present
When repairing lip lac, what process do you perform to anesthetize prior to repair?
Nasolabial blocks bilaterally (above canine into mucosal surface)
In order for the best cosmetic result, how do you close a lip lac?
Approximate vermillion border first and place suture
Then start from outside and work down
(mucosal tissues heal quickly, the main focus should be final cosmetic appearance of lip)
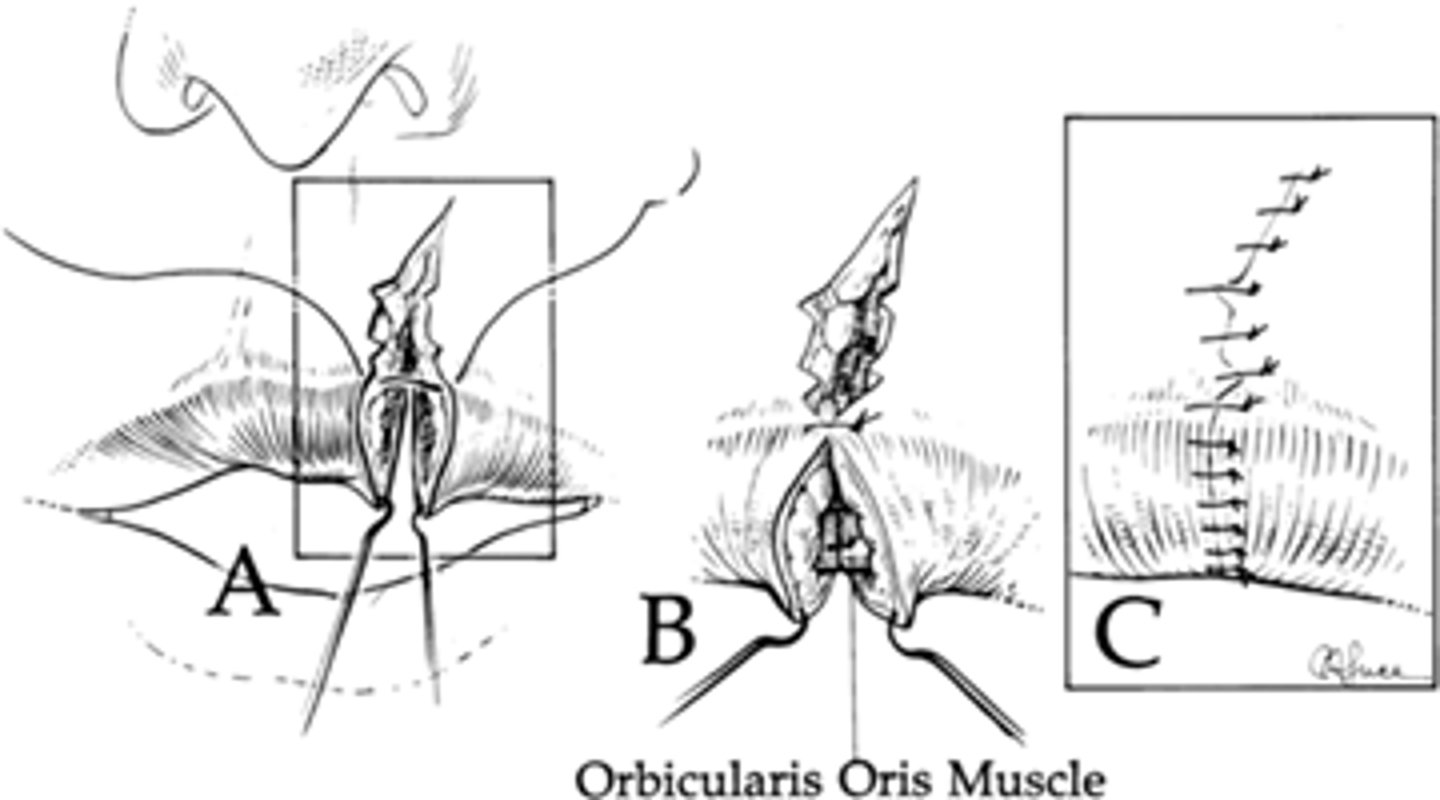
What should be focus of care when a lac is through ear cartilage?
Management of wound after repair
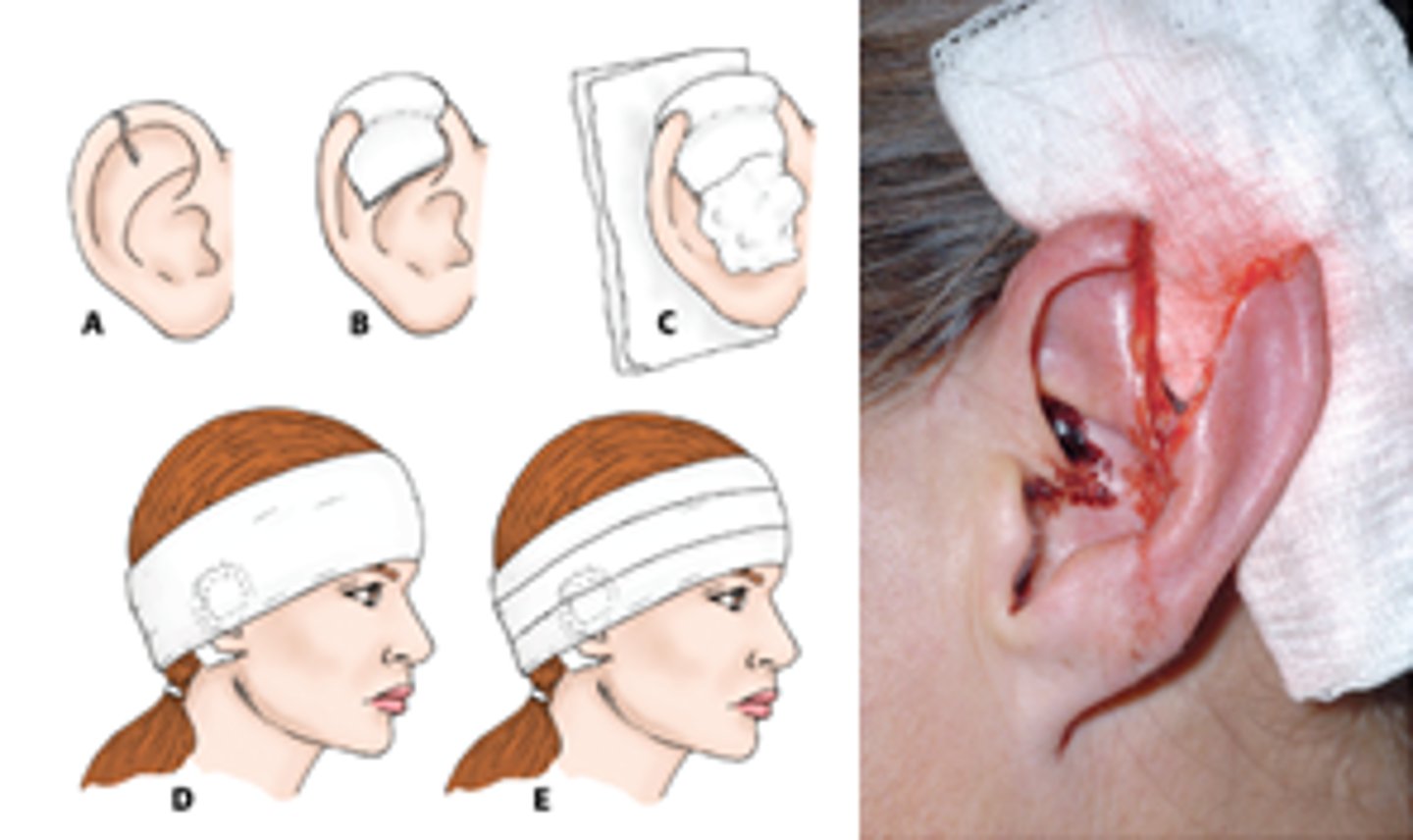
How do you close a ear lac through the cartilage?
Use 5.0-6.0 vicryl and approximate using cartilage rings of pinnae
pad the ear extensively and wrap head after to distribute pressure evenly so there is minimal risk of hematoma/ necrosis
What historical components are important to consider when patient comes in with arm, hand, finger, or nail wound?
- Mechanism
- Handedness
- Medical hx (esp. DM)
- Occupation
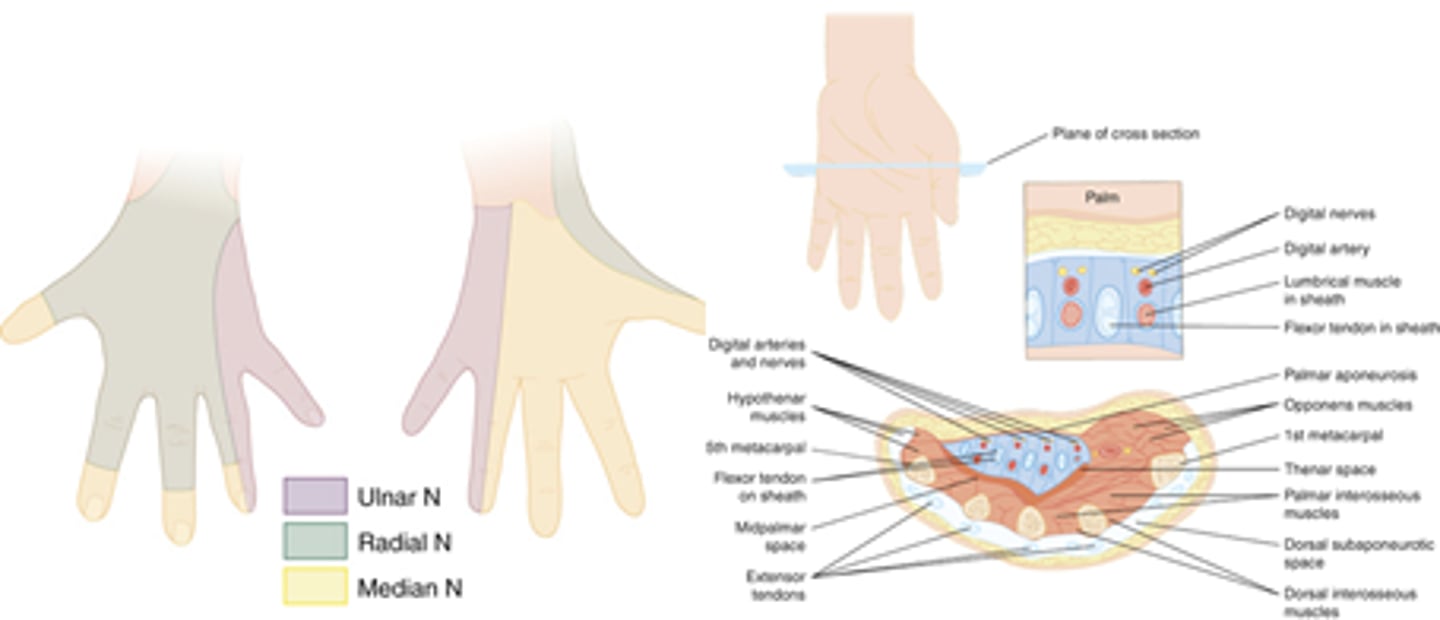
What nerves innervate the hand and where?
Median n (palmar aspect of digits 1-3 and 1/2 of 4 and corresponding nails)
Ulnar n (palm/volar aspect of other half 4 and all 5)
Radial n (volar aspect, minus median distribution, of digits 1-3 + 1.2 4)
When should tendon lacs be repaired?
Flexor: 24-48h
Extensor: up to 1 week
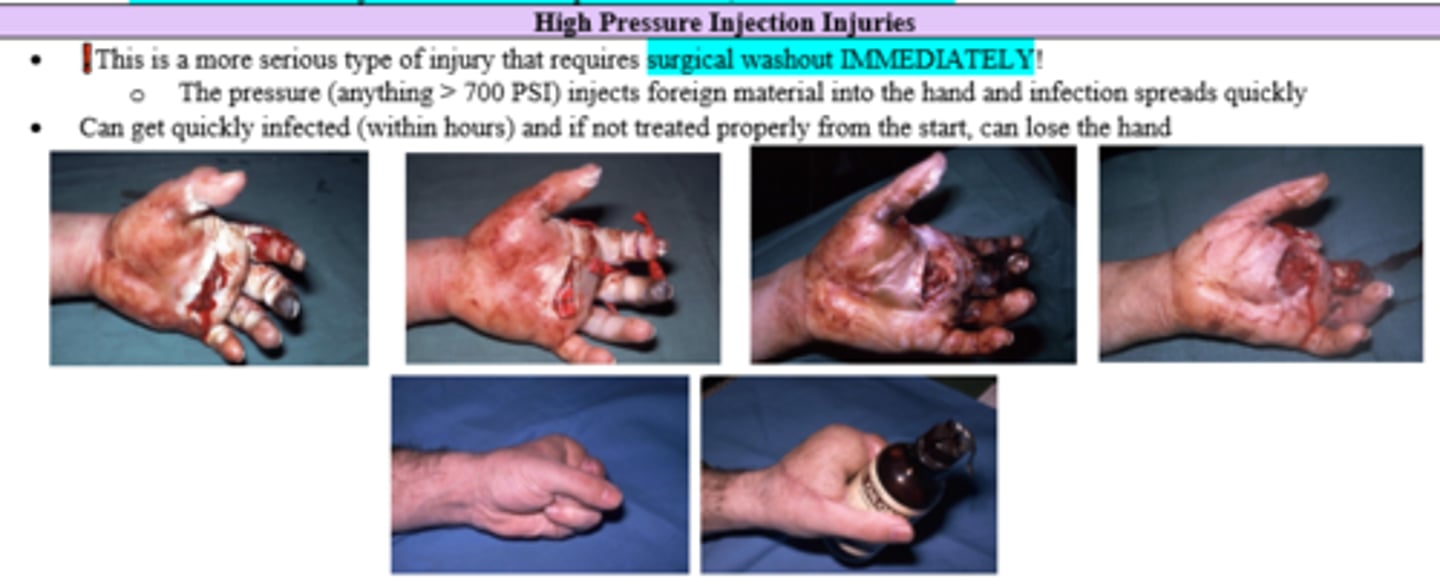
Patient comes to ER after sustaining a hand wound when he was trying to check the pressure of a 700psi spray paint bottle. What should be done immediately?
Surgical wash out (gets infected within hours)
Patient comes to ER after family found her with horizontal cut marks on her anterior wrists. What should be done prior to wound anesthesia?
Thorough neurovascular check (also consider ?suicidal attempt or gesture; FYI can close with 4-0 or 5-0 nylon or prolene)
At which point should a hand surgeon be consulted for f/u dt extensor tendon lac?
When ~50% lac'd
What should be used when anesthetizing distal cuts on the fingers?
Digital block

Which bite wounds should get antibiotic coverage?
all
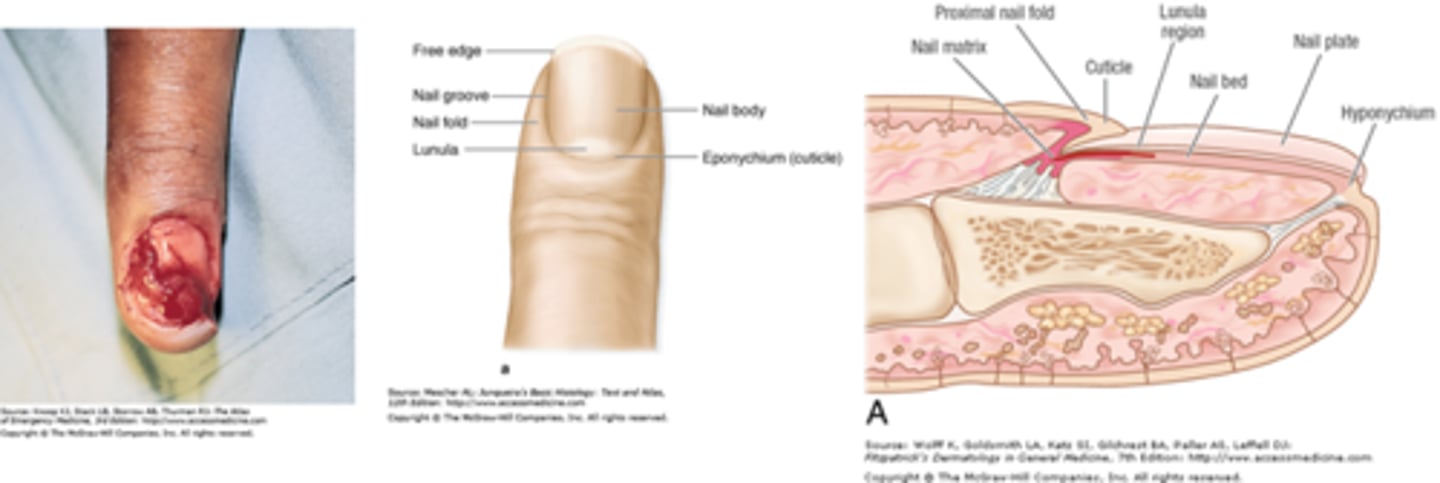
What should be considered with fingernail injury?
Ensure distal phalanx is not fractured (if so, it is considered OPEN fracture)