Immunology or Licensed to Kill
1/143
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
144 Terms
What is an antigen?
A molecule recognized by the immune system as foreign or unique. Can be a protein, polysaccharide, lipid (like cardiolipin), or nucleic acid. Not all antigens trigger an immune response.
What cells or molecules recognize antigens?
A: B-cell receptors, T-cell receptors, and antibodies.
What does antigenic specificity mean?
A: The ability of the immune system to recognize an antigen as unique and distinguish it from other molecules precisely (like a lock-and-key).
Example
Your body sees a flu virus protein.
It makes an antibody that only binds to that flu virus protein.
That antibody won’t bind to a cold virus protein, even though it’s also foreign.
What is antigenicity?
A: The ability of an antigen to bind specifically to immune system products (antibodies or T-cell receptors).
Antigen example
Blood group antigens (A, B)
Found on your red blood cells.
Your body can make antibodies against blood types you don’t have.
Example: If you’re type A, your body can recognize B antigens as foreign.
Bacterial surface proteins (e.g., flagellin)
Bacteria have proteins on their surface, like flagellin, which makes their “tails” move.
Your immune system can detect these proteins as foreign.
Viral capsid proteins (e.g., HBsAg)
Viruses are covered by proteins called capsid proteins.
Example: Hepatitis B surface antigen (HBsAg) is the protein on hepatitis B virus that the immune system recognizes.
Allergens (e.g., pollen proteins)
These are usually harmless proteins from things like pollen or pet dander.
Some people’s immune systems see them as foreign and overreact, causing allergies.
What is an antigenic determinant?
Also called an epitope
It’s a tiny, specific part of an antigen that the immune system actually recognizes and binds to.
This is bound by an antibody, B or T receptors
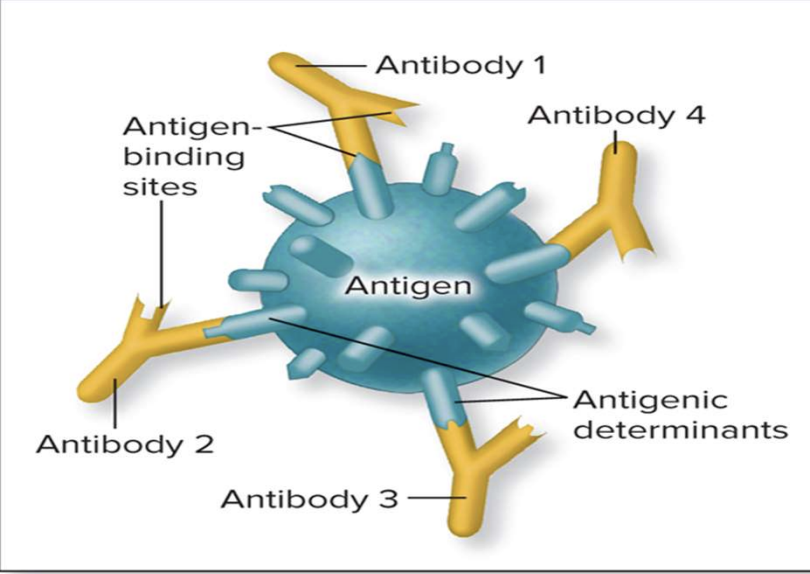
NOTE:
Epitope = exact spot on the antigen that the immune system “sees.”
2. Important points
Each epitope has a unique shape, like a key that fits one lock.
A pathogen (like a virus or bacteria) can have many epitopes, so the immune system has many targets.
NOTE:
Epitope = exact spot on the antigen that the immune system “sees.”
2. Important points
Each epitope has a unique shape, like a key that fits one lock.
A pathogen (like a virus or bacteria) can have many epitopes, so the immune system has many targets.
Vaccines - Connection to antigenic determinants
Vaccines are designed to show your immune system the key epitopes of a pathogen.
Your body then makes protective antibodies that recognize those epitopes.
Example: COVID-19 vaccines show your immune system the spike protein’s epitope so it can recognize the real virus later.
Monoclonal antibodies - Connection to antigenic determinants
These are lab-made antibodies that are designed to bind one specific epitope.
Example: Rituximab binds the CD20 epitope on B cells to treat certain diseases.
Key idea: targeting a specific epitope can turn off or destroy specific cells or molecules.
Autoimmunity - Connection to antigenic determinants
Sometimes, the immune system accidentally targets your own body’s epitopes.
These are called self-epitopes, and attacking them causes autoimmune diseases.
Example: in type 1 diabetes, the immune system attacks epitopes on insulin-producing cells.
Escape Mutants - Connection to antigenic determinants
Viruses like HIV or Influenza can change their epitopes slightly over time.
This is called antigenic drift, and it helps the virus evade recognition by your antibodies.
That’s why you can get the flu more than once, and why flu vaccines are updated each year.
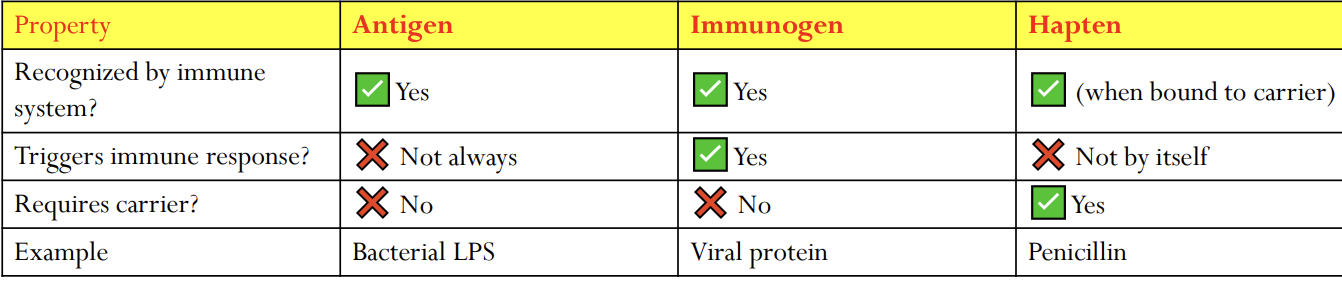
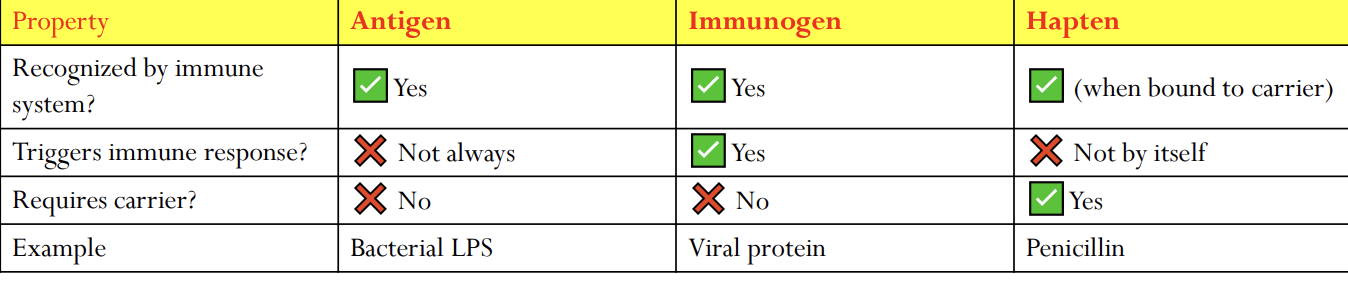
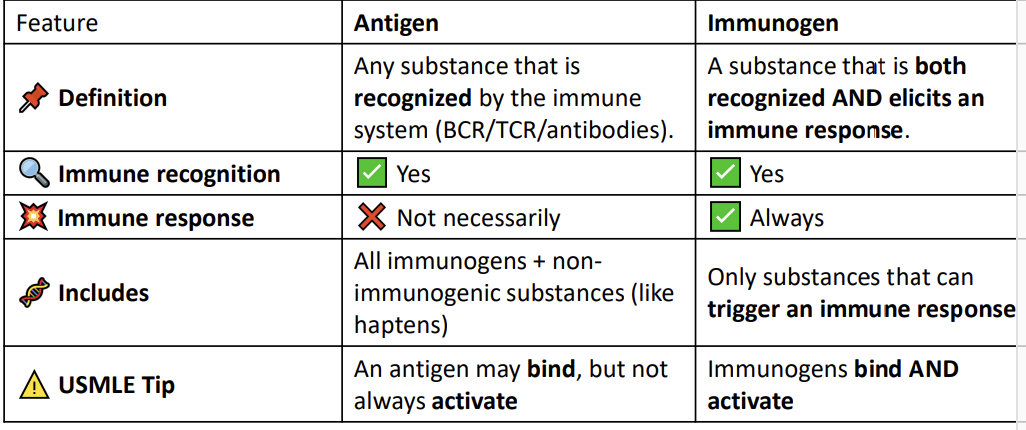
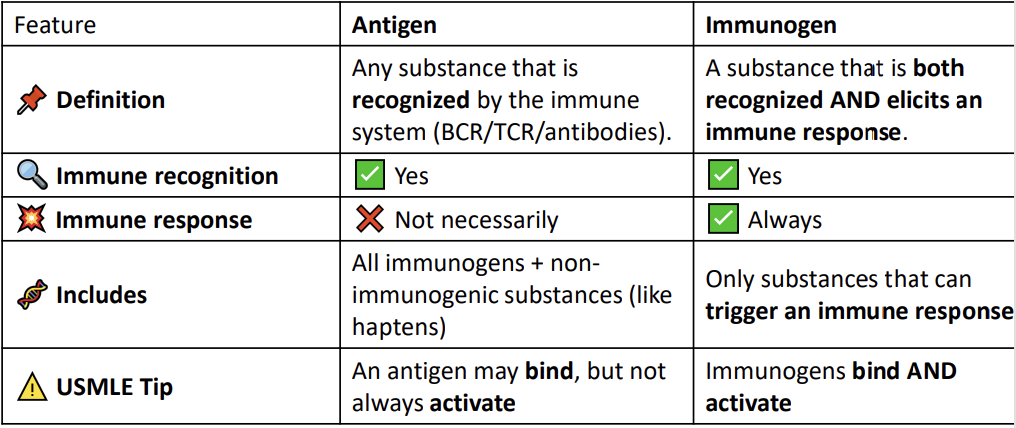
What is an Immunogen?
An immunogen is a substance that can actually trigger an immune response.
Key point: All immunogens are antigens, but not all antigens are immunogens. (Some antigens are recognized but don’t cause a response.)
Immunogenicity
Definition: The ability of a substance to induce an immune response—either:
Humoral immunity → antibodies from B cells
Cell-mediated immunity → T cells attacking infected cells
NOTE: “Immunogen = Initiates immunity.”
NOTE: “Immunogen = Initiates immunity.”
NOTE:
Antigen: Anything your immune system can recognize.
Immunogen: An antigen big and complex enough to make your immune system act.
NOTE:
Antigen: Anything your immune system can recognize.
Immunogen: An antigen big and complex enough to make your immune system act.
Tetanus toxoid - immunogen examples
A modified toxin from Clostridium tetani
Used in vaccines
Stimulates your body to make protective antibodies without causing disease
Viral spike proteins (e.g., SARS-CoV-2 spike) - immunogen examples
Protein on the surface of the virus
Target of mRNA vaccines
Trains the immune system to recognize and fight the real virus
Bacterial exotoxins (e.g., diphtheria toxin) - immunogen examples
Toxins secreted by bacteria
Stimulates adaptive immunity
Can be used in vaccines when inactivated (toxoids)
NOTE: “Hapten = Half-antigen” — needs a partner (carrier protein) to spark a response.
NOTE: “Hapten = Half-antigen” — needs a partner (carrier protein) to spark a response.
What is a hapten?
A hapten is a tiny molecule that is too small to trigger an immune response on its own.
Alone → not immunogenic (your immune system ignores it).
When attached to a larger carrier protein → becomes an immunogen and can trigger immunity.
Key idea:
Hapten + carrier protein = can provoke an immune response
A hapten is a tiny molecule that is too small to trigger an immune response on its own.
Alone → not immunogenic (your immune system ignores it).
When attached to a larger carrier protein → becomes an immunogen and can trigger immunity.
Key idea:
Hapten + carrier protein = can provoke an immune response
NOTE:
Hapten = tiny tag that alone can’t alert the immune system
Carrier protein = big “flagpole” that makes the immune system notice the hapten
Together → immune system reacts
NOTE:
Hapten = tiny tag that alone can’t alert the immune system
Carrier protein = big “flagpole” that makes the immune system notice the hapten
Together → immune system reacts
Common hapten examples
Penicillin: binds host proteins → triggers immune reaction in some people
Nickel (Ni²⁺): binds skin proteins → causes contact dermatitis
Urushiol (poison ivy): binds skin proteins → triggers T-cell response
Dinitrophenol (DNP): experimental hapten used in immunology research
Common hapten examples
Penicillin: binds host proteins → triggers immune reaction in some people
Nickel (Ni²⁺): binds skin proteins → causes contact dermatitis
Urushiol (poison ivy): binds skin proteins → triggers T-cell response
Dinitrophenol (DNP): experimental hapten used in immunology research
The most immunogenic bacteria
Shigella
8/10 will get you sick
Type I Hypersensitivity (Immediate / Allergic)
Who can get it: Anyone (genetic predisposition can increase risk)
How fast: Immediate reaction, usually minutes after exposure
Mediated by: IgE antibodies
Example:
Hay fever (pollen allergy)
Peanut allergy
Bee sting allergy
Mechanism: IgE binds allergens → triggers mast cells → release histamine → symptoms like swelling, itching, or anaphylaxis
Type IV Hypersensitivity (Delayed / Cell-mediated)
Who can get it: Usually after repeated exposure
How fast: Delayed, 24–72 hours after exposure
Mediated by: T cells (not antibodies)
Example:
Contact dermatitis (poison ivy, nickel)
Some drug reactions
Mechanism: T cells recognize antigen (or hapten-carrier complex) → release cytokines → inflammation and tissue damage
Only people who have been previously sensitized react; it doesn’t happen immediately like allergies (Type IV)
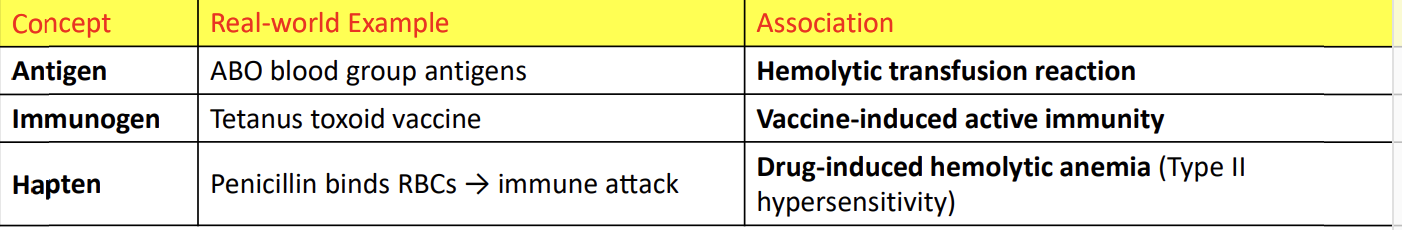
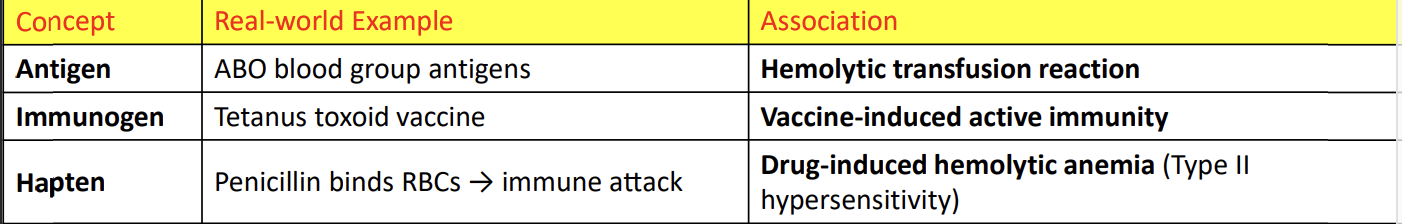
“Vaccines use immunogens, not just antigens.”
Vaccines don’t just show your immune system something it can recognize (antigen).
They show something that is big or complex enough to actually trigger an immune response (immunogen).
Example: Tetanus toxoid in the tetanus vaccine → recognized AND provokes immunity.
2. “Hapten-carrier model helps explain Type I and Type IV hypersensitivity.”
Some small molecules (haptens) cannot trigger immunity alone.
When they attach to larger carrier proteins, they become immunogenic.
This process explains some allergic reactions (hypersensitivities):
Type I: Immediate allergy (like penicillin-induced reactions)
Type IV: Delayed-type allergy (like poison ivy dermatitis)
. “Contact dermatitis, drug-induced hemolysis, and autoimmune hemolytic anemia can involve hapten formation.”
In these conditions, small molecules bind to your own proteins → form hapten-carrier complexes.
Your immune system sees the combination as foreign → attacks it, causing:
Contact dermatitis: nickel, poison ivy
Drug-induced hemolysis: penicillin or other drugs bind RBC proteins
Autoimmune hemolytic anemia: immune system destroys red blood cells because of hapten formation
What is shigella
Very dangerous:
Shigella is a highly invasive bacteria that can cause serious gastrointestinal illness.
“You have it from red cells / bloody diarrhea”:
Infection causes bloody diarrhea (dysentery) because it damages the intestinal lining, leading to blood in stool.
“It will destroy your GI completely”:
Shigella invades and destroys epithelial cells in the gut, causing ulcers and inflammation.
“They get inside the cell, go into epithelial tissue, find macrophages, but it won’t react”:
Shigella enters intestinal epithelial cells to hide and replicate.
It can evade macrophages (immune cells), so the bacteria can survive without being immediately destroyed.
A 30-year-old man develops a rash after receiving penicillin. The drug binds to host proteins and is recognized by the immune system. What is the best classification of penicillin in this context?
A. Immunogen
B. Antigen
C. Epitope
D. MHC molecule
E. Cytokine
Answer: B. Antigen Penicillin acts as a hapten — not immunogenic alone, but becomes an antigen when bound to a protein.
“Antigen = ANTIbody GENerator”
It generates a response that leads to antibody production.
“Antibody = Anti-BODYguard”
Acts as a defender that neutralizes invaders (antigens)
Antigen
Definition: A molecule that is recognized by the immune system (B cells, T cells, antibodies)
Function: Triggers an immune response (can be self or foreign)
Structure: Can be any substance – proteins, polysaccharides, lipids
Origin: Comes from pathogens, toxins, allergens, or even self-tissue
Recognition: Has epitopes that are recognized by antibodies or T/B cell receptors
Reusability: May appear multiple times (e.g., virus spike protein)
Antibody
Definition: A protein produced by B cells (plasma cells) in response to an antigen
Function: Neutralizes, marks, or eliminates antigens
Structure: Y-shaped glycoprotein (immunoglobulins: IgG, IgA, etc.)
Origin: Made by activated B lymphocytes (plasma cells)
Recognition: Has paratopes that bind specifically to epitopes
Reusability: Produced in response to each unique epitope
A patient receives a vaccine containing viral protein. Several weeks later, their serum contains high levels of specific IgG molecules. Which of the following best describes the relationship between the protein and the IgG?A. The IgG is an antigen and the protein is an antibody
B. The IgG is an antibody and the protein is an antigen
C. Both are antigens
D. Both are antibodies
E. The protein is a cytokine
Correct Answer: B The viral protein is the antigen that stimulated the immune system to produce IgG antibodies.
Hepatitis B - Antigen/body role
Antigen role: HBsAg (Hepatitis B surface antigen) – shows up in the blood and acts as a diagnostic marker (tells doctors you’re infected).
Antibody role: Anti-HBs – antibodies your body makes against HBsAg. Provides protective immunity (prevents infection if exposed later).
Systemic Lupus (SLE) - Antigen/body role
Systemic Lupus Erythematosus (SLE)
Antigen role: Nuclear antigens – parts of the cell’s nucleus that are recognized as foreign in autoimmune disease.
Antibody role: Anti-dsDNA antibodies – produced against nuclear antigens; used as a diagnostic marker for SLE.
Rh Incompability - Antigen/body role
Antigen role: Fetal Rh⁺ red blood cells – act as antigens when they enter a Rh⁻ mother’s bloodstream.
Antibody role: Maternal anti-Rh antibodies – can attack and destroy fetal RBCs, leading to hemolytic disease of the newborn.
Cytokines Definition
Small proteins that regulate and control immune system activity.
Act as chemical messengers between cells.
Who Produces Cytokines
Cells from the innate immune system
Cells from the adaptive immune system
Some non-immune cells (example: neurons)
How Cytokines Work
Released by one cell and bind to receptors on target cells.
Trigger intracellular signaling pathways.
This causes changes in gene expression and cell behavior.
Ways Cytokines Signal
Autocrine: act on the same cell that released them
Paracrine: act on nearby cells
Endocrine: travel through the blood to distant cells
NOTE: Key Characteristics
Short half-life (they don’t last long in the body)
Work through specific receptors on target cells
NOTE: Key Characteristics
Short half-life (they don’t last long in the body)
Work through specific receptors on target cells
What does it mean that cytokines must have “balanced production and regulation”?
The body must produce the right amount of cytokines at the right time.
This allows the immune system to fight infections effectively.
Too many cytokines can cause excessive inflammation and tissue damage.
Proper balance prevents immune-mediated damage to the body.
NOTE: Cytokines are like volume control on the immune system:
Too little → weak immune response
Too much → excessive inflammation and tissue damage
Balanced → healthy immune defense
NOTE: Cytokines are like volume control on the immune system:
Too little → weak immune response
Too much → excessive inflammation and tissue damage
Balanced → healthy immune defense
Cytokine Characteristics (What they are like)
Small soluble proteins
→ Tiny proteins that move easily through body fluids.Produced by innate and adaptive immune cells
→ Both early defense cells (like macrophages) and specific immune cells (like T cells) make them.Released from one cell and bind to receptors on another cell
→ One cell sends the signal and another cell receives it using receptors.Action similar to hormones
→ Like hormones, they send signals that control cell behavior.
IFN-γ (Interferon-gamma)
Activates macrophages
Enhances antigen presentation
Promotes Th1 T-cell differentiation
Important for strong cellular immune responses
IFN-β (Interferon-beta)
Antiviral effects
Enhances MHC Class I expression
Helps regulate immune responses
IFN-α (Interferon-alpha)
Antiviral effects
Increases MHC Class I expression (helps immune cells recognize infected cells)
Activates Natural Killer (NK) cells
Interferons (IFN)
Cytokines mainly involved in defense against viruses.
Colony-Stimulating Factors (CSF)
Cytokines that stimulate the bone marrow to produce immune cells.
Example: Granulocyte CSF (G-CSF)
Increases production of granulocytes (a type of white blood cell)
Helps the body replace immune cells during infection
Tumor Necrosis Factor (TNF)
Cytokines involved in inflammation and immune defense.
Example: TNF-α
Promotes inflammation
Causes fever
Stimulates acute-phase proteins in the liver
In severe infections can contribute to septic shock
Interleukins (IL)
Cytokines that help immune cells communicate with each other.
Mostly produced by white blood cells.
Example: IL-2
Stimulates T cell growth and activation
Helps immune cells multiply during an infection
NOTE: Cytokine Categories
IL → immune cells talk to each other
TNF → inflammation
CSF → make more immune cells
IFN → fight viruses
NOTE: Cytokine Categories
IL → immune cells talk to each other
TNF → inflammation
CSF → make more immune cells
IFN → fight viruses
What are hybridomas?
A: Hybrid cells made by fusing an antibody-producing B cell with a tumor cell, allowing scientists to continuously produce a specific monoclonal antibody.
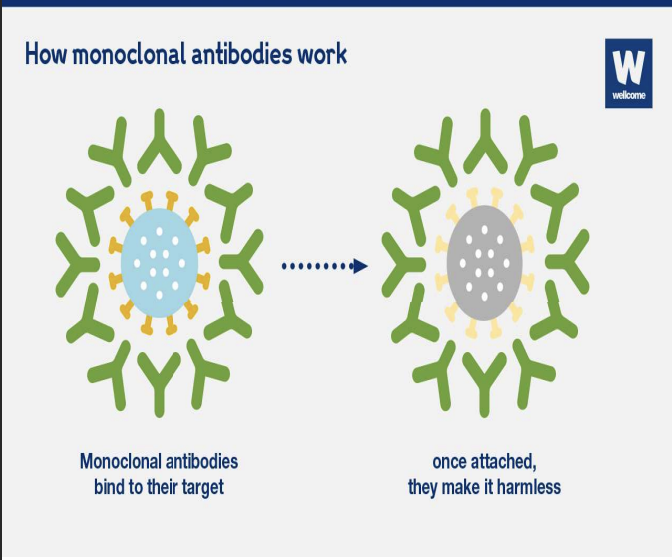
What are monoclonal antibodies
Monoclonal antibodies are lab-made antibodies that target specific cancer cells and help the immune system destroy tumors, making them an important tool in cancer immunotherapy.
The invaders
Bacteria
Viruses
Parasites, protista and worms
Fungi
Prion
Bacteria
Millions live on the skin and billions live in the gut.
Many are beneficial (“good bacteria”) and help the body.
They help by:
Helping digest food
Producing useful substances
Competing with harmful microbes
If they grow too much or the wrong types dominate, they can cause problems.
Some harmful bacteria can become resistant to antibodies or immune defenses.
Viruses
Very small infectious particles.
Contain DNA or RNA inside a protective coat.
They cannot reproduce on their own.
They infect cells by:
Entering the cell
Injecting their genetic material
Using the cell to make more viruses
Often destroying the cell when new viruses are released.
Parasites
Organisms that live in or on a host and take nutrients from it.
Some parasites are worms acquired from contaminated food or water.
They can cause nutrient loss, digestive problems, or disease.
In severe infections, parasites may consume nutrients meant for the host.
Fungi
Microorganisms such as yeasts and molds.
Can infect skin, nails, or deeper tissues.
Some fungi produce toxins.
Nail fungal infections can be difficult to treat because the fungus can persist deep in the nail tissue.
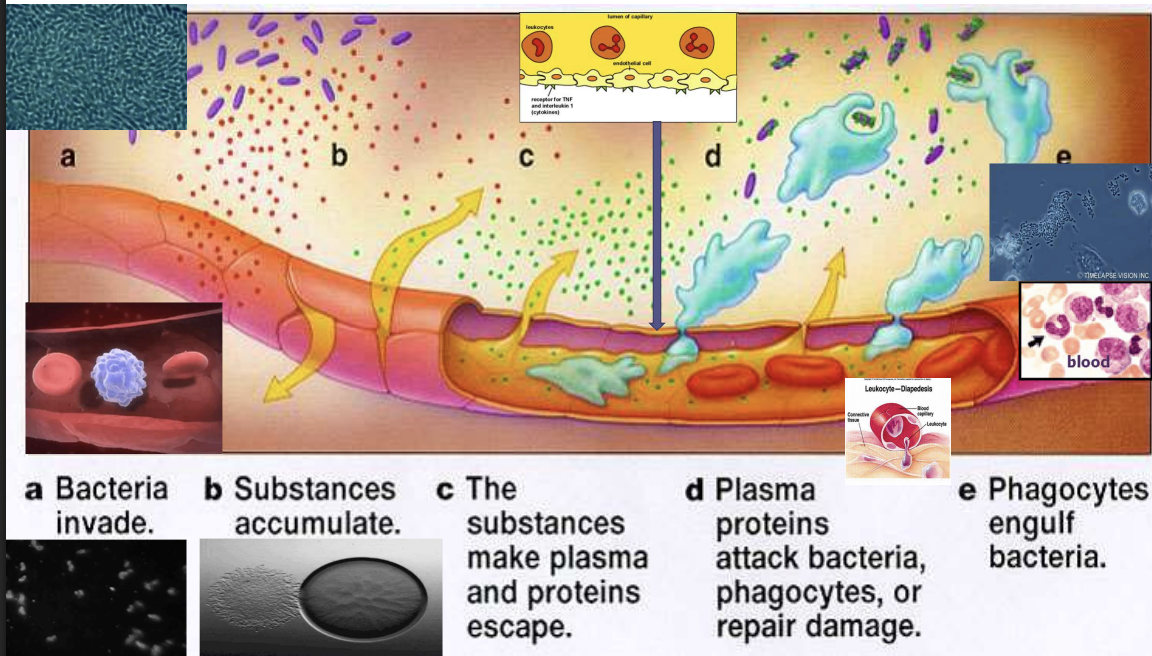
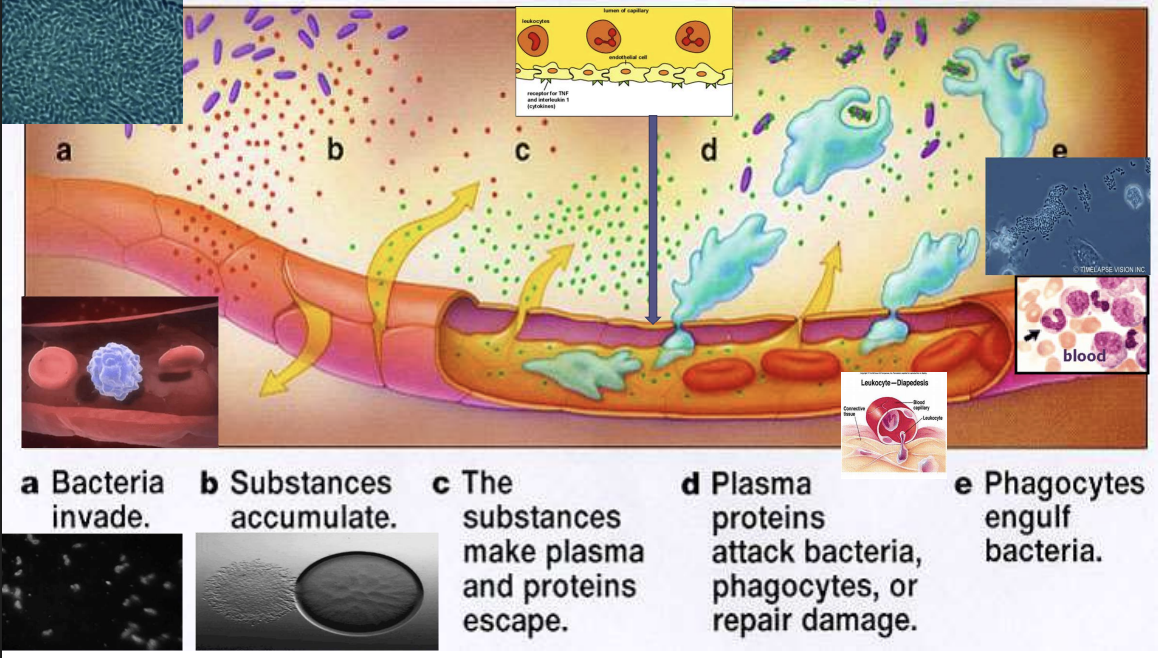
What happens first in a bacterial infection in tissue?
Back: Bacteria enter the body through a cut or damaged tissue and begin multiplying
What attracts white blood cells to the infection site?
Back: Chemical signals released by damaged cells and bacteria attract immune cells to the area.
Why do plasma and immune proteins leave the blood vessel during infection?
Back: Blood vessels become more permeable, allowing plasma and immune proteins to enter the tissue to fight bacteria.
What do phagocytes (macrophages and neutrophils) do during infection?
Back: They engulf and digest bacteria using enzymes in a process called phagocytosis.
What is pus and why does it form?
Back: Pus = dead bacteria + dead white blood cells + tissue debris that accumulates during infection
Why don’t antibodies work well in an abscess?
Back: The wall around the abscess blocks antibodies and immune cells from reaching the bacteria.
Why do doctors sometimes drain pus from an abscess?
Back: To remove trapped bacteria and pus, allowing the immune system and treatments to work better
What are lymphocytes?
Back: A type of white blood cell involved in the immune response
What are the three main types of lymphocytes?
Back: B-lymphocytes, T-lymphocytes, and NK (natural killer) cells.
What do B-lymphocytes do?
Back: Produce antibodies that bind to and help eliminate antigens.
What do T-lymphocytes do?
Back: Recognize infected or abnormal cells and help control the immune response.
What do NK (natural killer) cells do?
Back: Directly kill virus-infected cells and tumor cells without needing prior activation.
Where are most leukocytes located?
Back: Most leukocytes are found in body tissues rather than circulating in the bl
What are secondary lymphatic structures?
Back: Structures that house and support immune cells, where immune responses are often initiated.
Which immune cells are found in secondary lymphatic structures?
Back: T-lymphocytes, B-lymphocytes, macrophages, dendritic cells, and NK cells.
Which immune cells are found in secondary lymphatic structures?
Back: T-lymphocytes, B-lymphocytes, macrophages, dendritic cells, and NK cells.
What are examples of secondary lymphatic structures?
Back: Lymph nodes, spleen, tonsils, MALT, and lymphatic nodules.
What organs house macrophages?
Back: Certain organs contain macrophages that may be permanent residents or migrating immune cells.
What are location-specific macrophages?
Back: Macrophages named based on the tissue where they permanently live (example: alveolar macrophages in the lungs).
What is the first layer of defense in the immune system?
Back: The epithelium (skin and mucous membranes), which acts as a physical barrier to stop pathogens from entering the body.
What are the three main phagocytic cells in the blood that eat bacteria and antigens?
Back:
Neutrophils
Monocytes (which become macrophages)
Dendritic cells
What do phagocytic cells do?
Back: They engulf and digest bacteria, pathogens, and antigens through phagocytosis.
Where are dendritic cells commonly found?
Back: In the epithelial layers of the skin and mucosal membranes.
Where do dendritic cells usually come from?
Back: They are usually derived from monocytes.
What do dendritic cells do when they encounter pathogens?
Back: They engulf pathogens and migrate into the lymph to help activate the immune response.
Where are mast cells located in the body?
Back: In connective tissue, especially near small blood vessels.
In which tissues are mast cells especially abundant?
Back: In the dermis of the skin and mucosa of the respiratory, gastrointestinal (GI), and urogenital tracts.
Where else can mast cells be found in the body?
Back: In connective tissue of organs, such as the endomysium of muscle.
NOTE: • Mast cells typically in close proximity to small blood vessels
NOTE: • Mast cells typically in close proximity to small blood vessels
What does the body use to protect itself in the nonspecific (innate) immune response?
Back: Cellular and chemical defenses that attack pathogens without targeting a specific organism.
What immune cells are involved in nonspecific defense?
Back: Phagocytes and natural killer (NK) cells.
What are antimicrobial proteins?
Back: Proteins in blood and tissue fluid that help destroy or inhibit microbes.
What happens during the inflammatory response?
Back: Macrophages, mast cells, white blood cells, and chemicals are recruited to fight infection.
What are the two main types of lymphocytes in adaptive immunity?
Back: B lymphocytes and T lymphocytes.
What type of immunity do B lymphocytes control?
Back: Humoral immunity, which involves antibody production.