becoming swallowing experts
1/161
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
162 Terms
Dysphagia
Difficulty moving food from the mouth to the stomach.
Swallowing/Disordered Swallowing can be impacted by
- cognitive awareness
- level of alertness
- awareness of food and smell to increase salivation
- behavioral, sensory, and preliminary motor acts in preparation of the swallow
Define aspiration
Unwanted material below the vocal folds
Define penetration
Unwanted material that travels to the vocal folds but does not enter the trachea
Define transient
The term used when material goes to the vocal folds but goes in and out
Residue/retention/stasis
material that hangs out (either orally or pharyngeally) after the swallow is complete
Regurgitation/reflux/backflow
food from the esophagus flows back into the pharynx and/or from the pharynx into the nasal cavity
Define MBSS
Radiology procedure where the patient is given barium in a variety of consistencies and is observed swallowing under x-ray so that anatomic and physiological function can be evaluated
List some examples of conditions that may co-occur with or cause dysphagia
- congenital abnormalities
- structural damage
- CVA
- tumors
- closed head injury
- degenerative diseases (PD, Dementia, etc)
- any patient with weakness (such as due to a severe infection like sepsis)
- esophageal disorders
What are three types of esophageal disorders?
- Dysmotility Disorders
- Structural Disorders
- GERD
What are examples of dysmotility disorders?
Presbyesophagus, diffuse esophageal spasm, nutcracker esophagus
What are examples of structural esophageal disorders?
Esophageal strictures
Zenker's diverticulum
Tortioned esophagus (corkscrew esophagus)
Hypertonic upper esophageal sphincter (UES)
Bezoar
List the symptoms of esophageal disorders?
Pain/pressure (pt. may identify that it feels like food is stuck in a specific spot)
Copious secretions
Lots of belching
History of GERD
What are options for treating esophageal disorders?
- Positioning
- Feeding techniques
- Providing information about a diet that will decrease symptoms
- Cricopharyngeal dilation exercises
What are the four stages of swallowing?
1. Oral preparatory phase
2. Oral stage
3. Pharyngeal swallow phase
4. Esophageal phase
What are some signs/symptoms of dysphagia?
Unable to recognize food
Coughing before, during, after a swallow
Frequent coughing at the end of or right after a meal
History of pneumonia
Weight loss
Wet vocal quality
Increased secretions (oral and/or pharyngeal)
Watery eyes while eating
Temperature spikes
Patient is struggling
How are evaluation and screening different?
Screening = identifying pathology to refer a patient for an evaluation
Evaluation = in-depth physiologic assessment of swallowing mechanism to ID the underlying anatomic or physiologic abnormalities so that effective treatment can be planned
What are possible complications of dysphagia?
Pneumonia/respiratory failure
Malnutrition
Dehydration
(Death)
Name one sensory/behavioral action that has to happen to prepare for a safe swallow
Determining the necessary mouth posture (e.g. the mouth posture you use to eat a hamburger vs. take a sip of water is going to be different)
Define presbyesophagus
Esophagus gets stretched out with age and is now less able to achieve sufficient peristalsis to get food to move downwards efficiently
Define Diffuse Esophageal Spasm
the squeezing motion for peristalsis is non-rhythmic/non-ordered, so the bolus moves up and down
Define nutcracker esophagus
- an area of tightness in the esophagus where the bolus cannot easily pass through
* this is the most common motility disorder
Define esophageal stricture
An abnormal narrowing of the esophagus that typically will cause difficulty swallowing
Define Zenker's diverticulum
A gap in the tissue of the upper PE segment creating a kind of "swimming pool" where material can get caught
Define Bezoar
Something blocking the lower esophageal sphincter (may be any material, class examples were a tooth or hair)
Define GERD
Gastroesophageal Reflux Disease - persistent reflux of gastric contents into the esophagus.
*patient may report pain somewhere in the esophagus but be unable to ID exactly where the pain is
What is "globus sensation"
pain that is in an unrelated or a general area...this is common with the esophagus because it is a poor localizer of pain (since there aren't lots of nerve endings there, we feel the pain somewhere else or generally)
Why is it important to understand the esophagus/esophageal disorders if it's outside our scope of practice?
If you notice something atypical related to the esophagus, you can note it and refer to a doctor for further investigation.
What is the oral preparatory stage?
starts when food enters your mouth, includes chewing, gathering food, and preparing to swallow it
What is the oral stage?
bolus/liquid starts to move back towards the pharynx
What is the pharyngeal swallow phase?
starts when the larynx rises (watch the hyoid bone), bolus is in the lingual-mandibular line, and the swallow reflex is triggered
What are the evaluation tools commonly used to assess dysphagia?
- Bedside swallow evaluation (this would be done with an oral motor exam, assessment of breath support/airway protection, assessment of cognition)
- Modified barium swallow study
- FEES-fiber optic endoscopic evaluation of swallow
Research shows that only what % of patients who aspirate are correctly identified after clinical examination?
60-70%
How much can a patient safely aspirate?
Trick question - there is no data on this because it depends on patient's health level
But, if a patient is aspirating >10% per bolus even with interventions, they should be advised not to eat that consistency by mouth (Logemann)
Who are other professionals who might be on a dysphagia patient's treatment team?
PT, OT, nursing, MD, dietician, CNAs, radiologist, pharmacist, psychiatrist
What makes up the oral cavity?
Lips anteriorly, teeth, hard palate, soft palate, uvula, mandible, anterior and posterior faucial arches, and palatine tonsils
Muscles/nerves in chewing
-Temporalis, masseter, and medial pterygoid muscle -
Depresses, opens and protrudes the mandible and moves it laterally
-Lateral pterygoid
All innervated by the trigeminal nerve (CN V)
Labial muscles of chewing
•Function-To hold food in contact with the teeth.
-Orbicularis Oris,
-Zygomaticus
-Buccinator
•These are innervated by the facial nerve (CN VII)
Oral Cavity: roof, floor, lateral walls and posterior limit
•Roof: Hard and soft palates
•Floor: Geniohyoid muscles and muscular diaphragm (mylohyoid muscles)
•Lateral walls: Dental arches
•Posterior limit: Isthmus of fauces (contains palatine tonsils between palatoglossal and palatopharyngeal arches, marks the transition to oropharynx)
Hyoid bone
is embedded in the base of the tongue and does not articulate with other bones.
What suspends the hyoid bone
soft tissue and the posterior belly of the digastric and stylohyoid muscles. Both of these muscles attach posterolateral from the region of the temporal bone
What is the larynx suspended by?
The hyoid bone
Mylohyoid Muscle
-Origin
•Inner surface of the body of the mandible anteriorly.
-Insertion
•Body of the hyoid bone inferiorly and posteriorly
-Function:
•Elevates the floor of the mouth
•Depresses jaw when hyoid bone is in fixed position
-Innervation
• Trigeminal Nerve
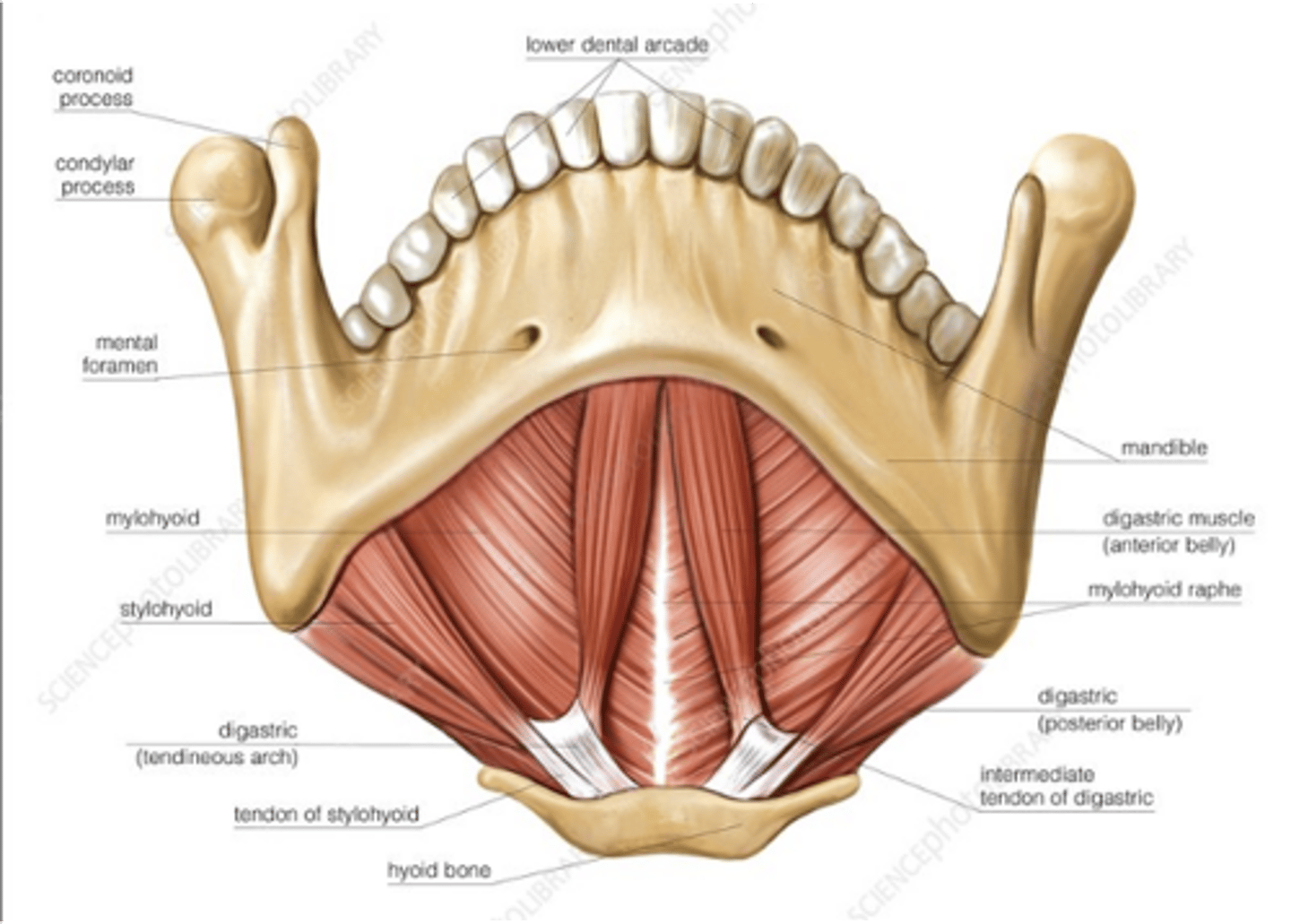
What are the suprahyoid muscles?
mylohyoid
geniohyoid
digastric
hyoglossus
stylohyoid
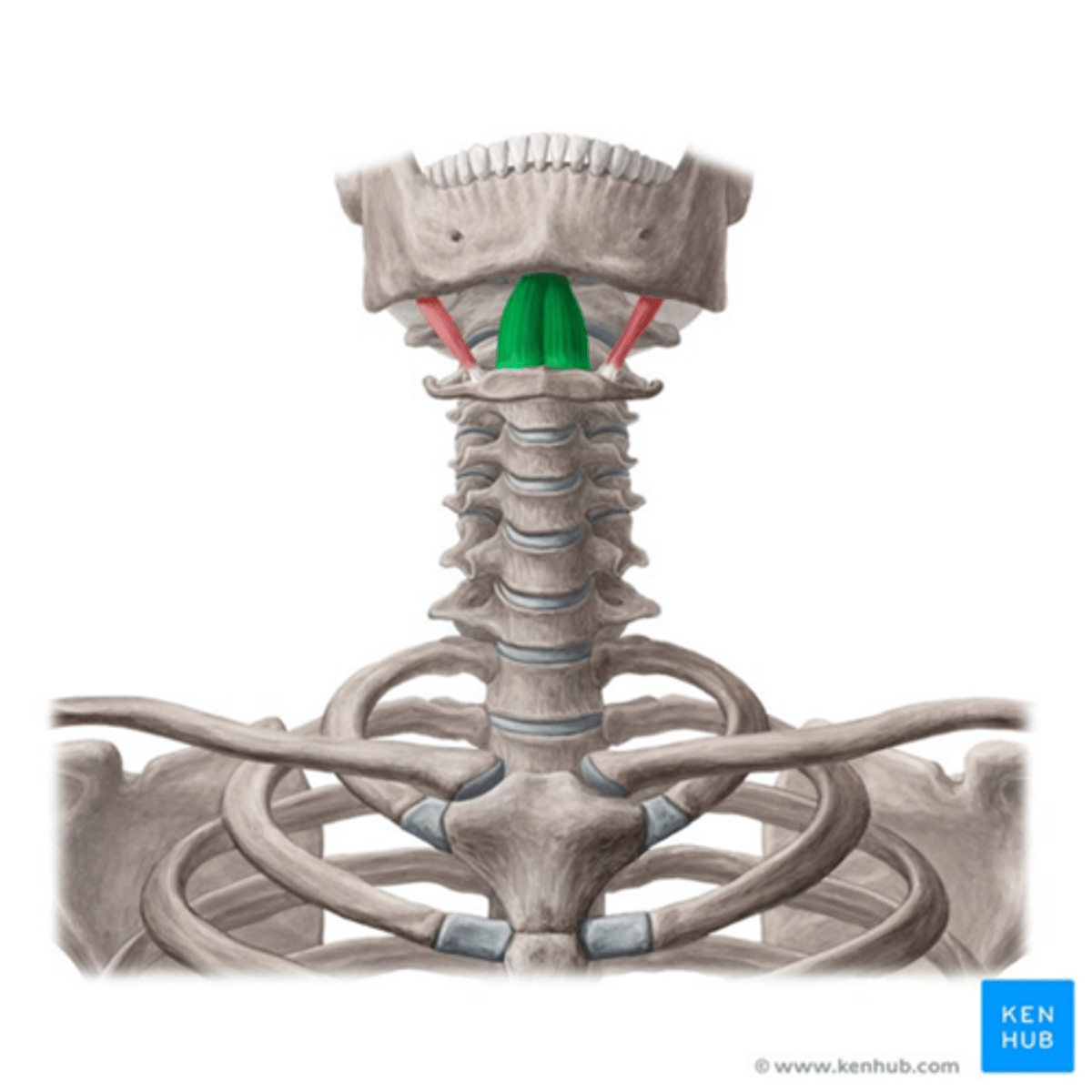
geniohyoid muscle
•Origin
- Mental Spine of the Mandible
•Insertion
- Body of the hyoid
•Function
-Elevates the hyoid and pulls in anteriorly
•Innervation
•Hypoglossal
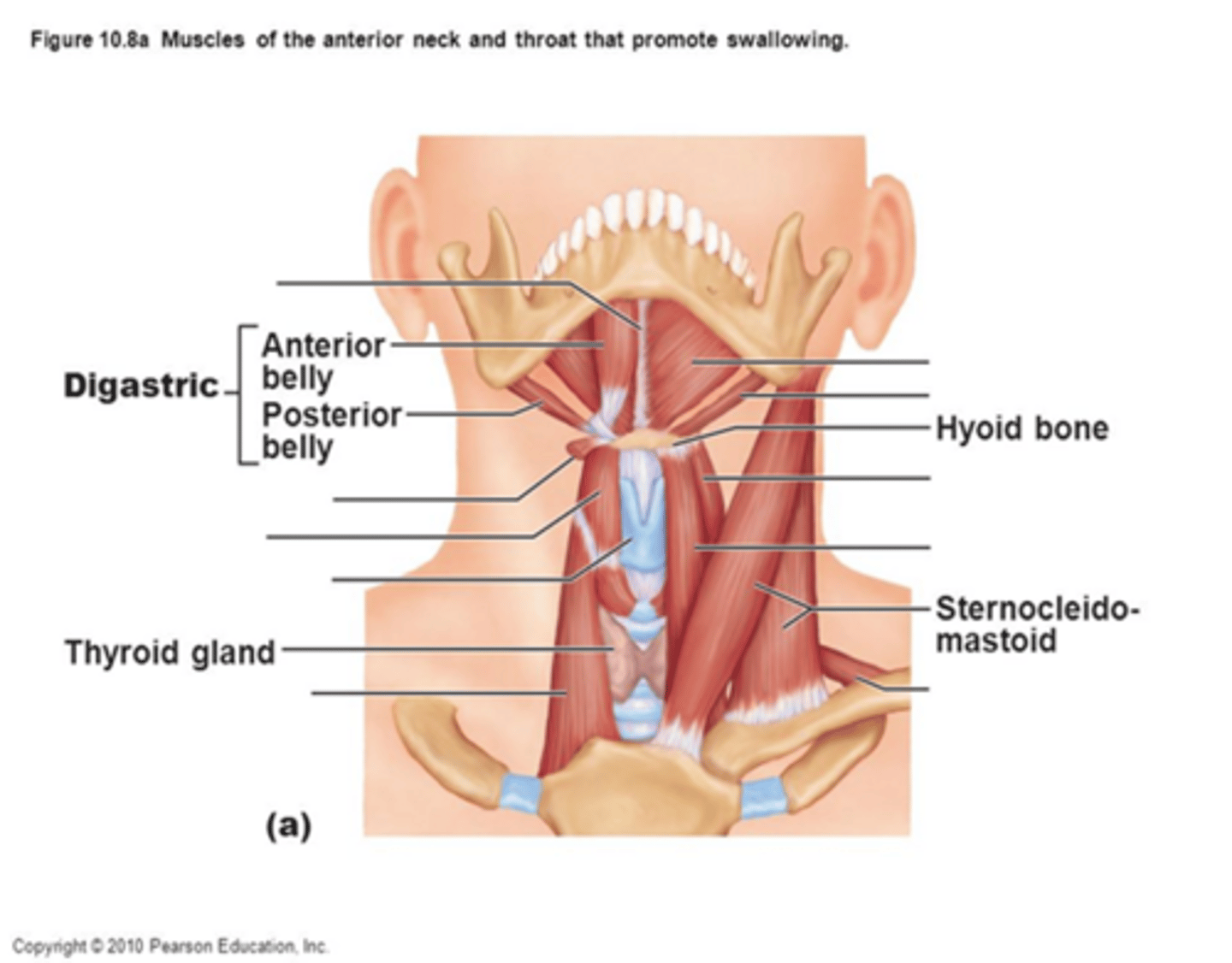
Diagrastric muscle
•Origin
-Intermediate tendon by loop of fascia to hyoid bone
•Insertion
-Lower border of the mandible
•Function
-Raises hyoid bone if jaw is in fixed positions.
-Depresses jaw if hyoid bond is in fixed position
•Innervation
- Trigeminal
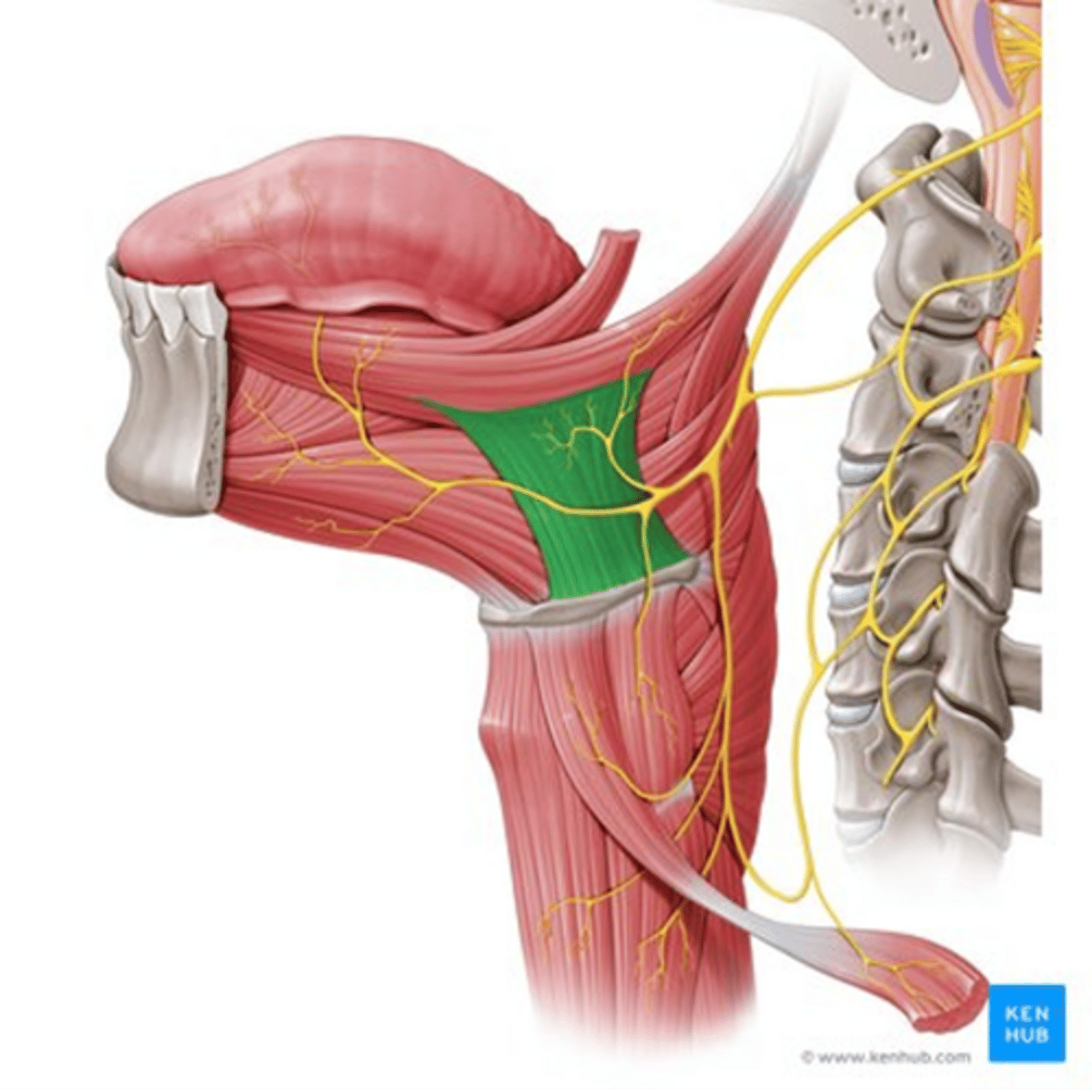
Hypoglossus Muscle
•Origin
-Greater horn of the hyoid
•Insertion
- Side of the tongue
•Function
- Depresses the tongue to the floor of the mouth
•Innervation
-Hypoglossal
Stylohyoid Muscle
•Origin
-Stylohyoid process of the temporal Bone
•Insertion
-Body of the hyoid at the greater cornu
•Function
-Elevates hyoid and tongue base
•Innervation
-Facial nerve
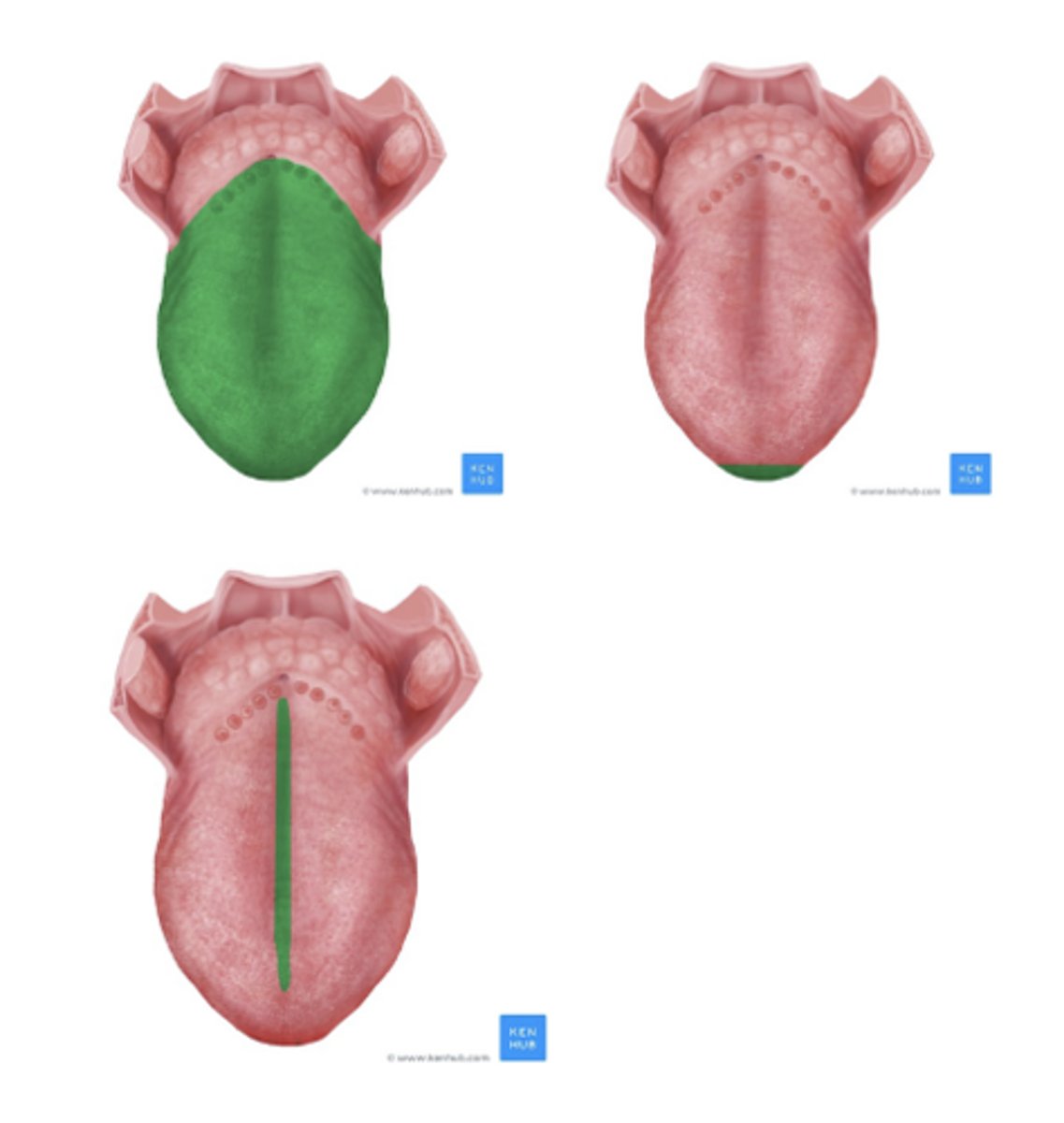
What makes up the oral vs pharyngeal tongue
Oral tongue is the tip, blade, front, center, and back. ends at the Vallate Papillae (volitional control)
Pharyngeal tongue the tongue base to the hyoid bone (neural control)
What are landmarks of the body of the tongue?
The body of the tongue, apex, and median sulci
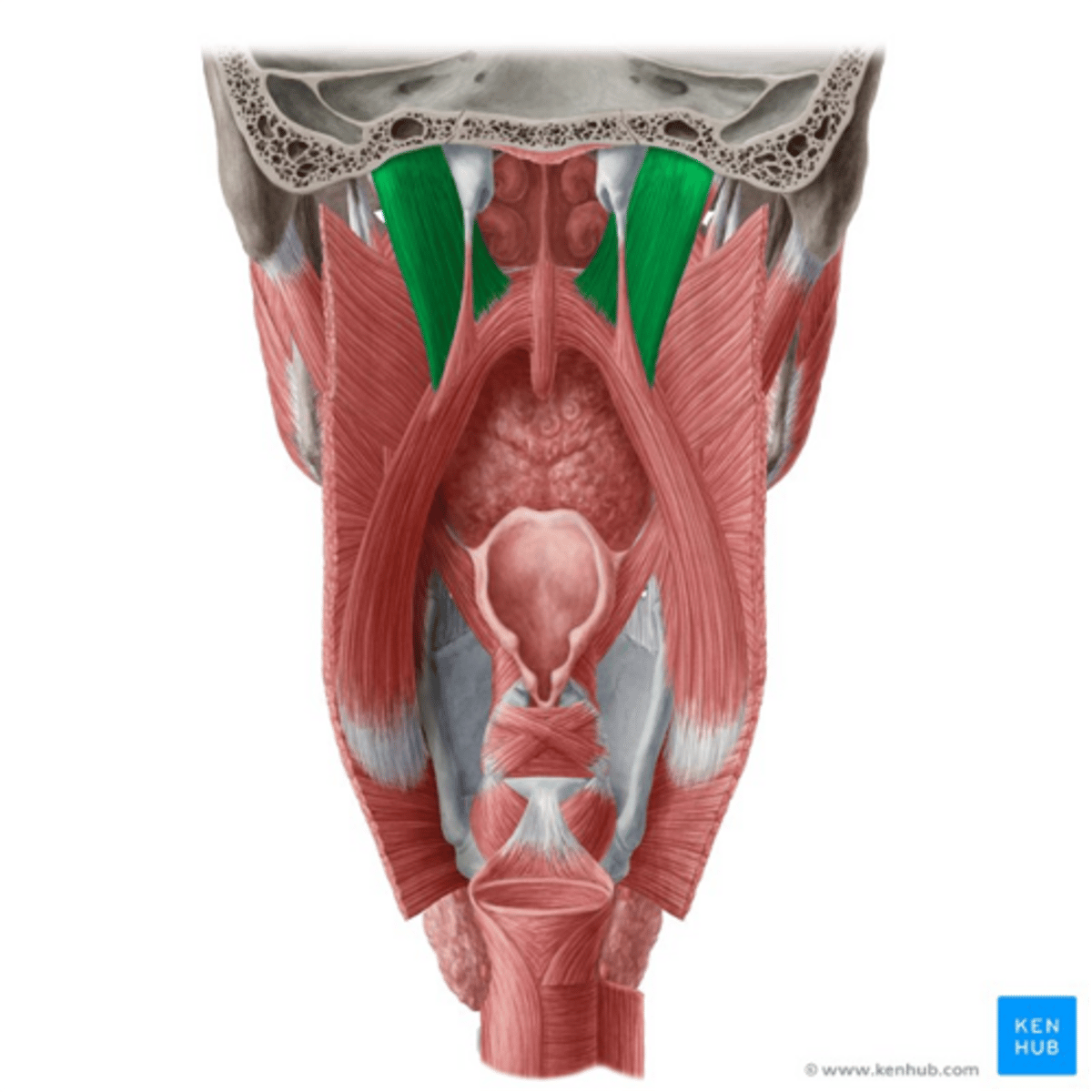
What are the muscles of the soft palate?
levator veli palatini, tensor veli palatini, palatoglossus, palatopharyngeus
levator veli palatini
•Origin
-Temporal bone
•Insertion
-Palatine aponeurosis of soft palate
•Function
-Raises the velum
•Nerve
-Vagus and Accessory
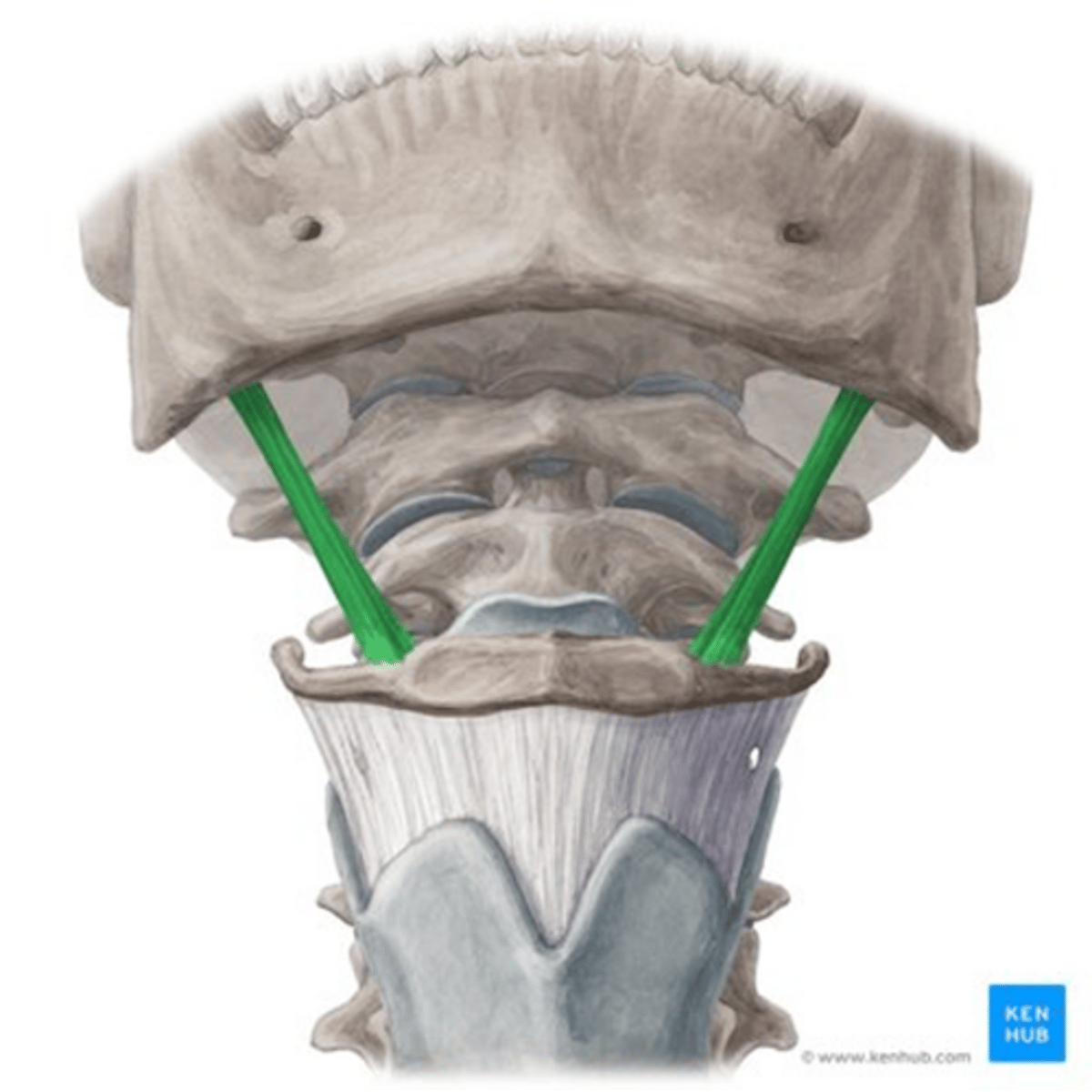
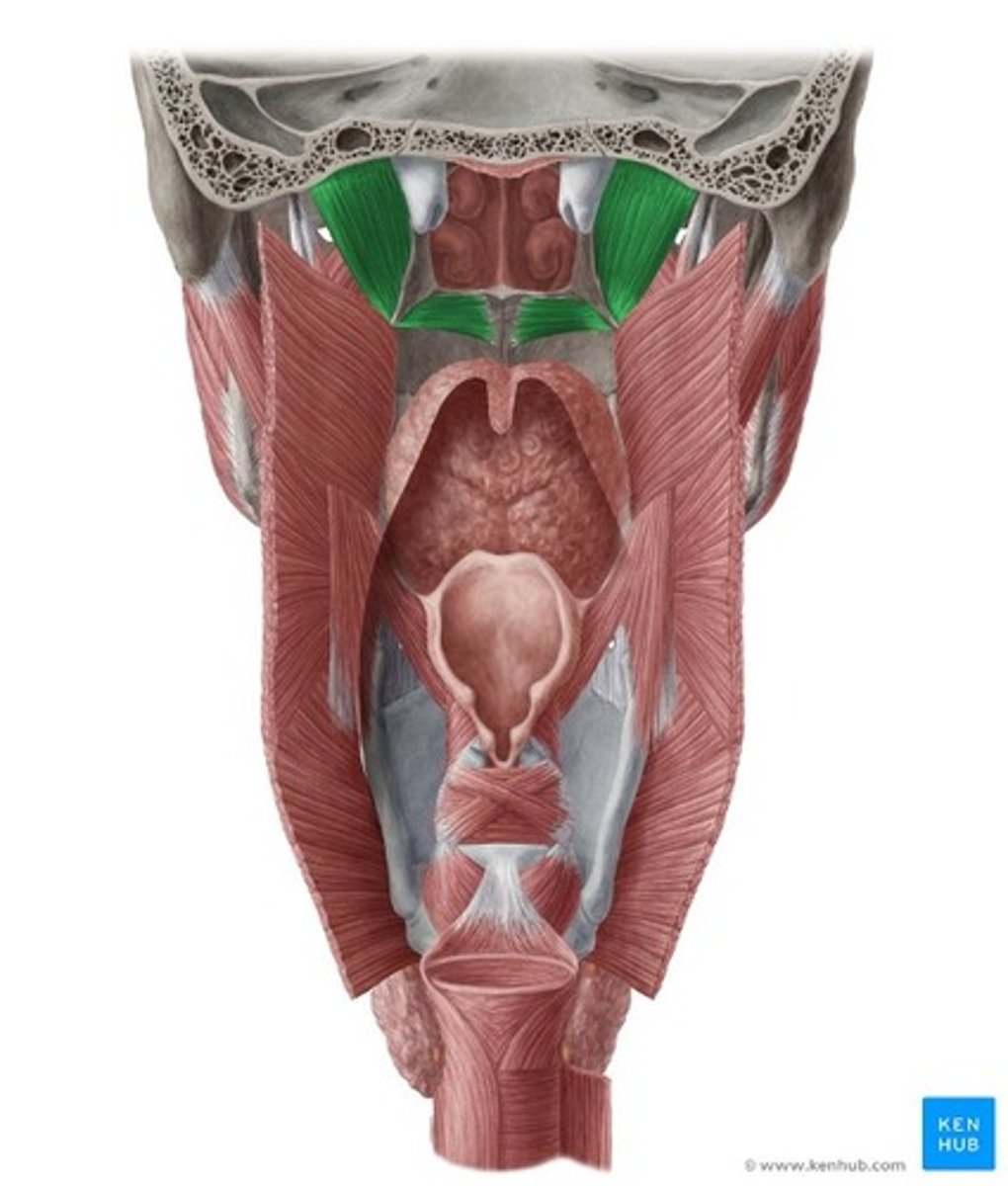
Tensor Veli Palatini
•Origin/Insertion
-Pterygoid fossa of skull
•Function
-The tensor veli palatini muscles stretches the soft palate producing the tension during oral and swallowing. This enables the tongue to press against the soft palate
-Opens eustachian tube
•Nerve
-Trigeminal
palatoglossus
•Origin
-Anterior surface of the Soft Palate
•Insertion
-Dorsum of the tongue
•Function
-Narrows fauces and elevates the tongue or pulls soft palate to the tongue
•Innervation
-Glossopharyngeal, vagus, and accessory
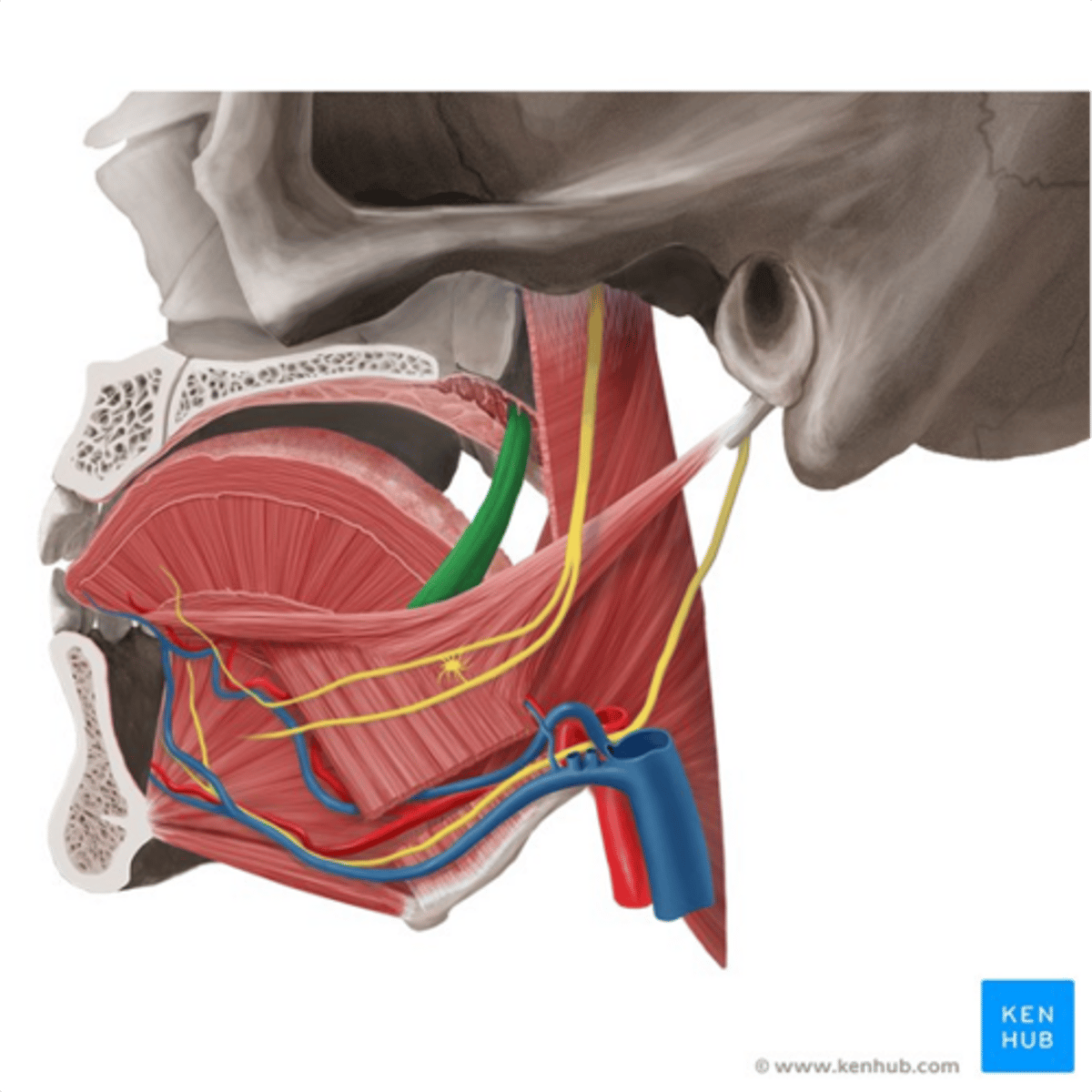
Palatopharyngeus
•Origin
–Soft Palate
•Insertion
–Pharyngeal Wall
•Function
–Elevates pharynx superiorly, anteriorly and medially (shortening it to swallow)Innervation
–Close during pharyngeal phase of swallow
Vagus and accessory
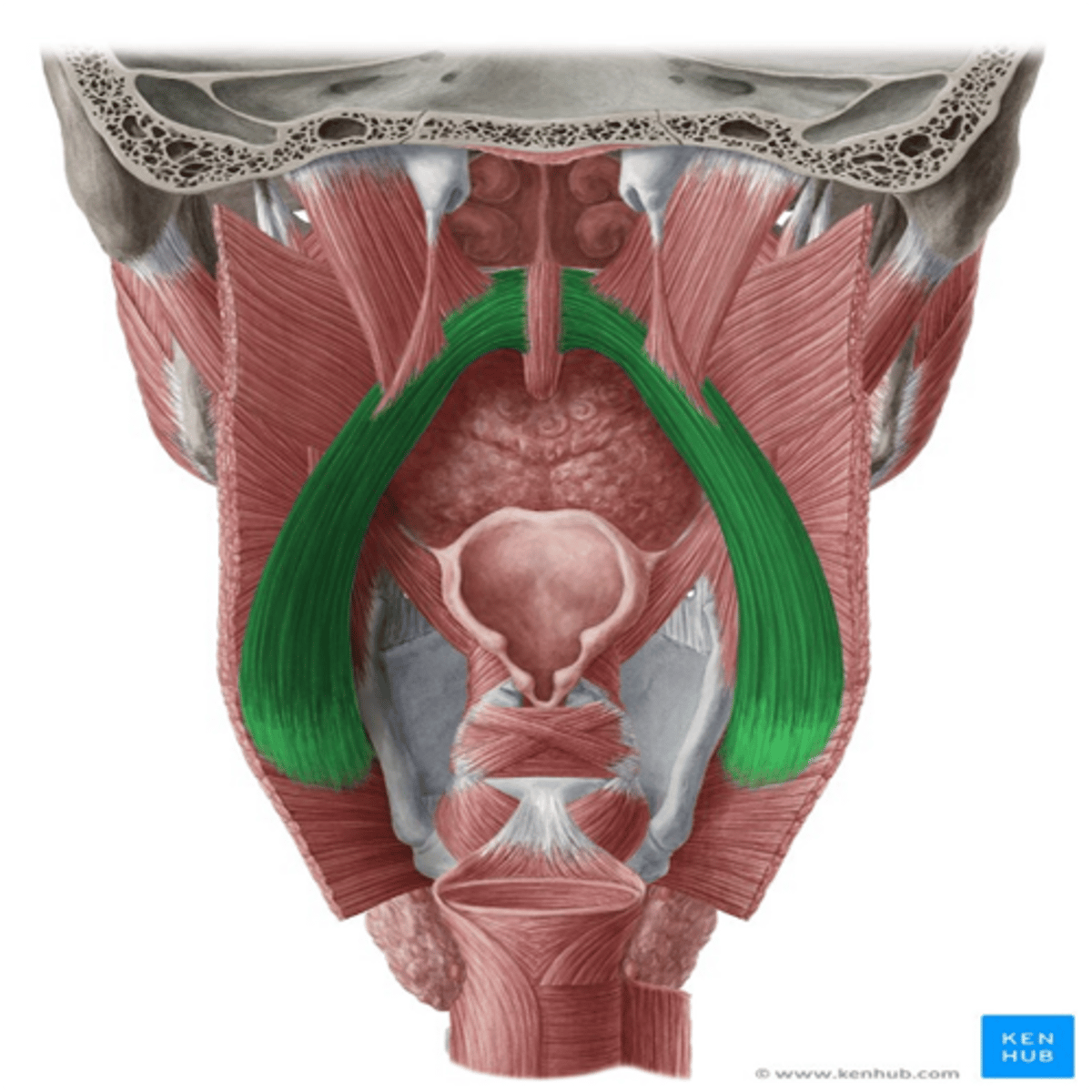
What muscle produces the tension of the soft palate during swallowing?
The tensor veli palatini (it enables the tongue to press against the soft palate and move the bolus to the oropharynx
What muscles elevate the velum
the levator veli palatini and the palatoglossal muscle. this closes the nasopharynx preventing food from getting in
What muscle tenses the velum?
Tenor veli palatini (Fun Fact: responsible for opening the eustachian tube but not during the oral phase)
What muscle depresses the tongue, approximates the palate or pharyngeal fold?
Palatopharyngeus
What muscle shortens the velum?
Musculus uvulae
What does saliva do?
•Maintains oral moisture/lubrication
•Reduces tooth decay
•Assists in digestion
•Natural neutralizer of stomach acid that may reflux into the esophagus (why we need copious secretions)
•Immune defense
•Taste transmission.
How much saliva does an average adult make a day?
1.5 liters
What are the salivary glands?
parotid, submandibular, sublingual
Sublingual gland
mucous gland only, secretes viscous fluid
parotid gland and duct
Serous gland-only. makes a thinner type of fluid
submandibular gland
mixed gland - makes both viscous and serous type of fluid (both thick and thin)
structures involved in deglutition (swallowing)
-Superior, medial, and inferior pharyngeal constrictors (innervated by the Vagus nerve)
•These muscles form posterior and lateral walls of the pharynx (outer most walls)
-Point of Insertion for all muscles above
•Median (Pharyngeal) Raphae Pharyngeal raphae-middle of the pharyngeal wall
-Point of Origin
•Various structures, bony and soft tissue structures located anteriorly (pterygoid plate, sphenoid bone, soft palate, base of the tongue, mandible, and hyoid bone, and thyroid and cricoid cartilages
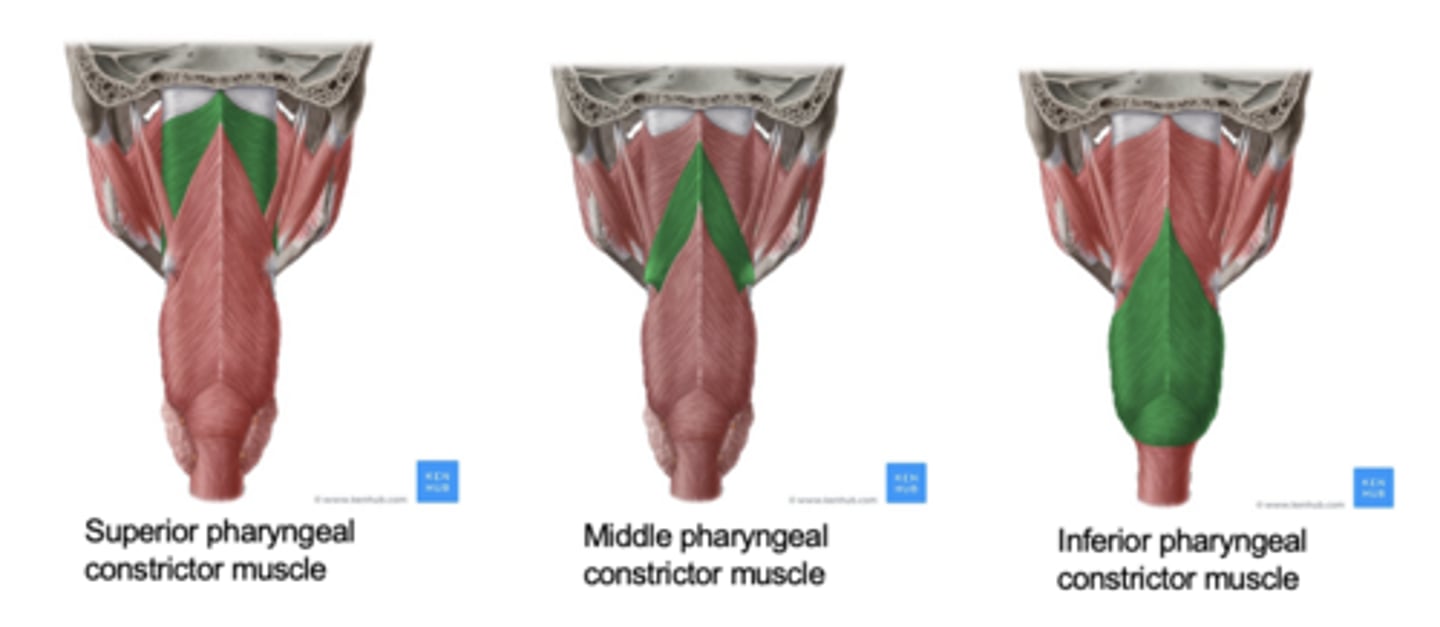
Inferior fibers OF THE superior constrictor
–Attach to the base of the tongue and sometimes are called sometimes called the Glossopharyngeus muscle
•This muscle is important because it is PROBABLY responsible for tongue base retraction and simultaneously anterior bulging of the posterior pharyngeal wall at the tongue base level (very important in pharyngeal clearance during the actual swallow)
Inferior constrictor muscle
•Point of Insertion-Median Raphe (pharyngeal raphe)
•Attachment-To the either side of the thyroid cartilage anteriorly
•These muscles form the walls of pyriform sinus
•End at the upper esophageal sphincter muscle
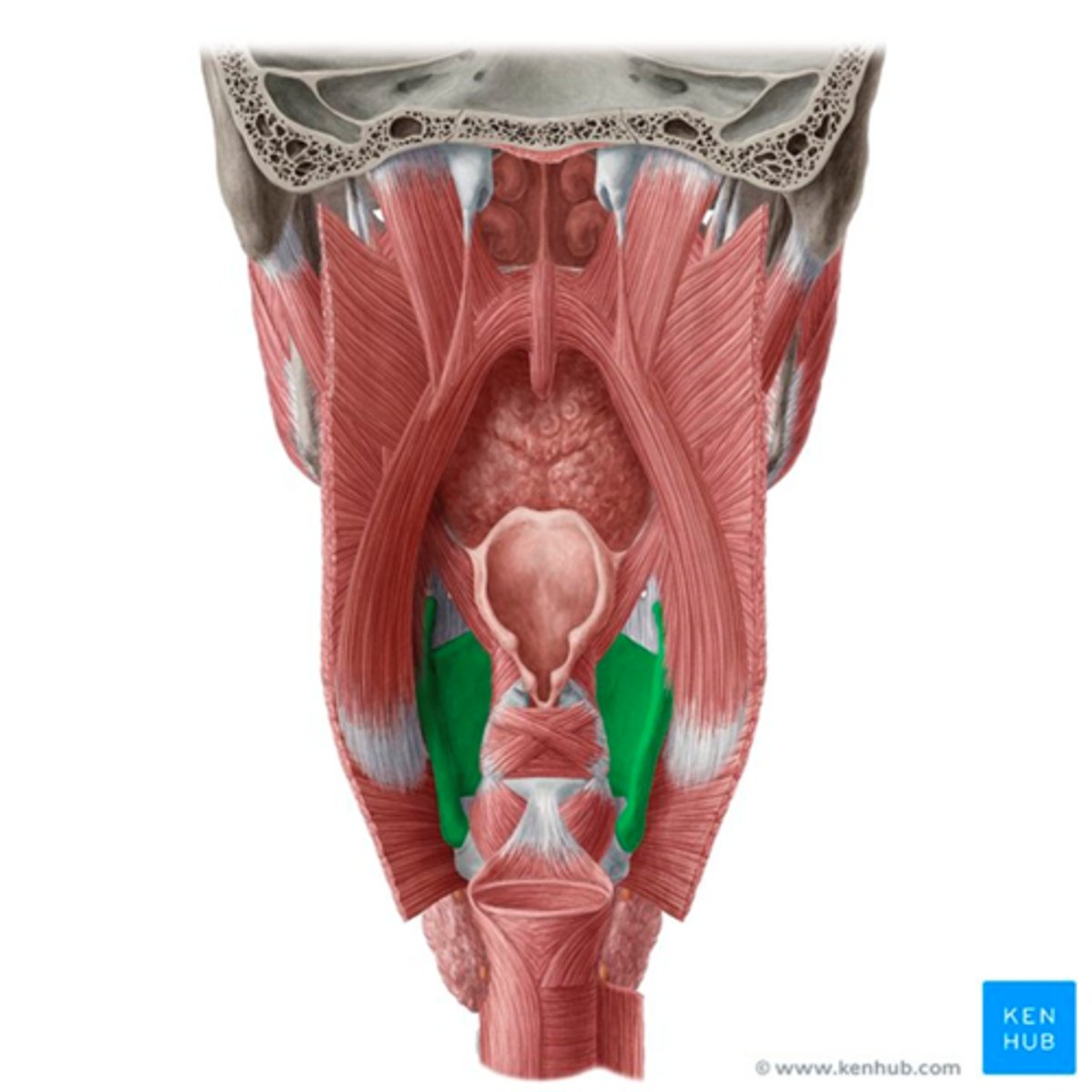
the cricopharyngeus muscle is also known as
the UES and PES
Cricopharyngeus muscle
•May or may not be part of the inferior constrictor muscle
•Point of attachment- posterolateral surface of the cricoid lamina
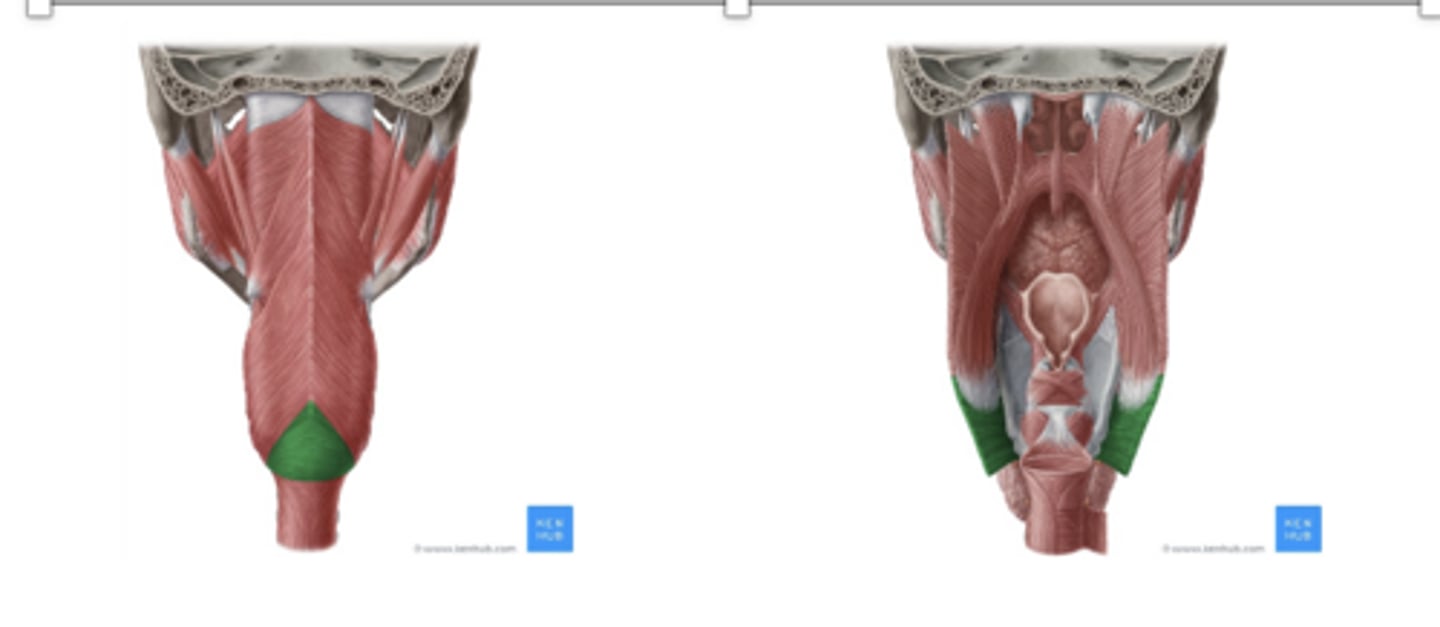
What does the UES muscle do when an adult is awake? Why?
•Tonic contraction, mild, at rest in an awake adult
-prevents air from entering in during respiration
-Secondary role-prevents backflow into the pharynx
-The pressure will is equivalent to holding 11cc of water in the esophagus.
-It's peak pressure occurs immediately prior to the swallow
What does the UES do when asleep?
It is relaxed
What is the esophagus?
•Collapsed tube 23-25 cm long with a sphincter at both ends UES and LES (lower esophageal sphincter) which empties into the stomach
What does the LES do?
prevents reflux of acidic gastric contents back into the esophagus
What are the 2 types of muscle in the esophagus?
-Inner circular and outer longitudinal
•Striated "type" muscle upper 1/3
•Smooth and striated muscle middle 1/3
•Smooth muscle lower 1/3
How many levels of sphincters are in the larynx?
3 levels
What muscles does the trigeminal nerve (CN V) innervate?
Innervates the chewing muscles (temporalis, masseter, medial, and lateral pterygoid)
What is the function of the trigeminal nerve (CN V)
1. Assists the glossopharyngeal nerve in raising the larynx and pulling it forward during swallow
2. Gives all sensation besides taste for anterior 2/3 of tongue.
What muscles does the facial nerve (CN-VII) innervate for?
Innervates the lip muscles (buccinator, obicularis oris, and zygomaticus)
What is the function of facial nerve (CN-VII)
1. (Motor) Innervates w/ the lip muscles to keep food in contact with the teeth.
2. (Sensory) Carries information about taste from the anterior 2/3 of tongue.
What does the glossopharyngeal nerve (CN IX) innervate?
Innervates the 3 salivary glands in the mouth
AND
the upper pharyngeal constrictor muscles & stylopharyngeus (with vagus X)
What is the function of the glossopharyngeal nerve (CN IX)
1. Moistens mouth, prevents tooth decay, aids in protecting esophagus from reflux of stomach acid.
2. Elevates the larynx and pulls it forward during the pharyngeal swallow phase (helps relax & open the UES)
3. Mediates all sensation (including taste) from posterior 1/3 of tongue
4. Sensation from velum & superior part of the pharynx
Can I guess the rest?
nope, keep studying --> Emilyyyyy, are you sure? I'm thinking: yes, no, maybeee?? - pri lol :)
3 multiple choice options
A lesion on the glossopharyngeal nerve may cause what?
Impaired gag reflex unilaterally
What does the Vagus Nerve (CN X) innervate?
1. Glossopalatine and levator veli palatini muscles
2. pharyngeal constrictor muscles
3. intrinsic musculature of larynx
4. cricopharyngeous
5. nerves involved in esophageal stage of swallow & muscles of respiration
What sensory function is the Vagus Nerve (CN X) responsible for?
sensory information from the velum and posterior & inferior larynx
What does the Spinal Accessory nerve (CN XI) innervate?
palatopharyngeus muscle
& muscularis uvula
What is the function of the muscularis uvula?
Raising the velum
What does the Hypoglossal Nerve (CN XII) innervate?
all extrinsic and intrinsic tongue muscles
What are the four phases of the swallow?
oral preparatory, oral phase, pharyngeal phase, esophageal phase
How many times a day, on average, does a person swallow?
580
When we sleep, how much time can pass, on average, between swallows?
20 minutes
Some types of swallows do not involve all components of the swallow. Give an example of a time this is true.
When we swallow saliva, we don't usually chew it
The oral preparatory phase begins with what step
recognizing the food, this helps us determine what the mouth will do with the liquids (is it a lot of food, what kind, is it a drink so you need to not open your mouth as wide, etc)
The first labial seal during the oral preparatory phase is important to prevent what
Losing material anteriorly (out the mouth)
A labial seal during oral prep requires what?
the nasal airway has to be open for breathing
Describe what a "tipper" is
Food is held between the midline of the tongue & the hard palate with the tongue tip elevated and touching the alveolar ridge
Describe what a "dipper" is, and what % of people are "dippers"
Food is held on the floor of the mouth and the front of the tongue.
20% of people are dippers
What is an abnormal pre-swallow position in adults?
When the tongue is held between the bolus & anterior teeth - this is a tongue thruster