Kidney/Urinary
1/76
Earn XP
Description and Tags
Intg. Organ Phys, Exam 3
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
77 Terms
What are the six functions of the kidneys?
Regulation of ECF volume and BP (integrated system w/ Cardiovascular system)
Regulations of blood osmolarity (~290 mOsm)
Maintenance of ion balance (Na, Ca2, K)
Homeostatic reg of pH (regulates H+ and HCO3- conc. w/ lungs.)
Excretion of waste
Production of hormones.
What hormones does the kidneys produce?
Erythropoietin, renin, conversion of Vitamin D to its active form.
What metabolic wastes does the kidneys excrete?
Creatinine, urea/uric acid, urobilinogen,
Where are the kidney’s located?
Retroperitoneally (behind peritoneal cavity) along lower ribs.
What surrounds the kidneys?
Capsule.
What is the outer part of the kidney?
Cortex
What is the inner part of the kidney?
Medulla.
What are the functional units of the kidneys?
Nephrons.
How does urine leave nephrons?
Flows into renal pelvis and out the ureter.
How much cardiac output does the urinary system receive?
20-25%
Sequence nephron structure.
Glomerulus in Bowman’s Capsule —> Proximal tubule —> Loop of Henle —> Distal tubule —> Collecting ducts.
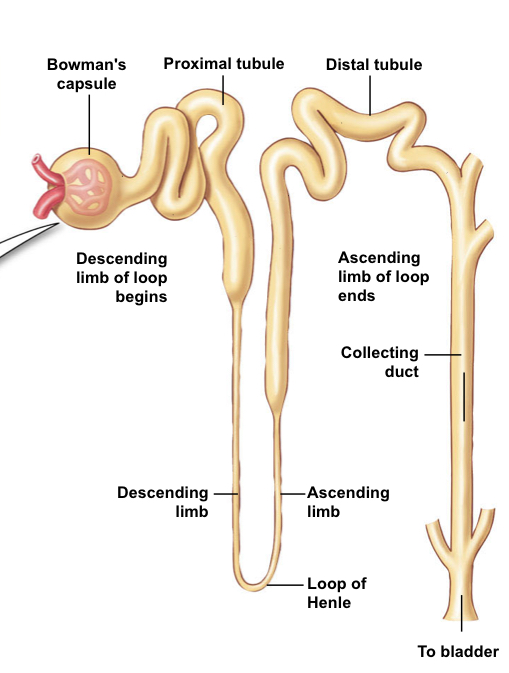
What are nephrons comprised of?
Two arterioles and two sets of capillaries that form a portal system.
What does the cortex of the kidneys contain? (nephron structure)
Bowman’s capsule, proximal and distal tubules.
What does the medulla of the kidney contain? (nephron structure)
Loops of Henle, collecting ducts.
What is filtrate? How much of it is filtered each day?
Filtration of blood into the lumen of the nephron; 180 L.
Excretion Equation:
Excretion = Filtration - Reabsorption + Secretion
Glomerular Filtration
Fluid pressure created by fluid in Bowman’s capsul.
Only 20% of the plasma passes through the glomerulus filtered.
Less than 1% of filtered fluid is excreted.
What are the Glomerular Filtration Driving Forces?
Capillary pressure causes filtration.
Hydrostatic pressure (BP)
Colloid osmotic pressure.
Sequence vascular elements pathway in the kidneys:
Afferent arteriole —> glomerulus —> efferent arteriole —> Peritubular capillaries —> vasa recta —> renal vein.
What process of the kidney occurs in Bowman’s capsule?
Filtration.
What process of the kidney occurs in proximal tubule?
Reabsorption and Secretion.
What process of the kidney occurs in Loop of Henle?
Reabsorption.
What process of the kidney occurs in the distal tubules?
Reabsorption and secretion.
What process of the kidney occurs in collecting duct?
Reabsorption and secretion.
Sequence tubular element pathways in the kidneys:
Bowman’s capsule —> Proximal tubule —> Loop of Henle —> Distal tubule —> collecting duct —> bladder and external environ.
Sequence renal excretion:
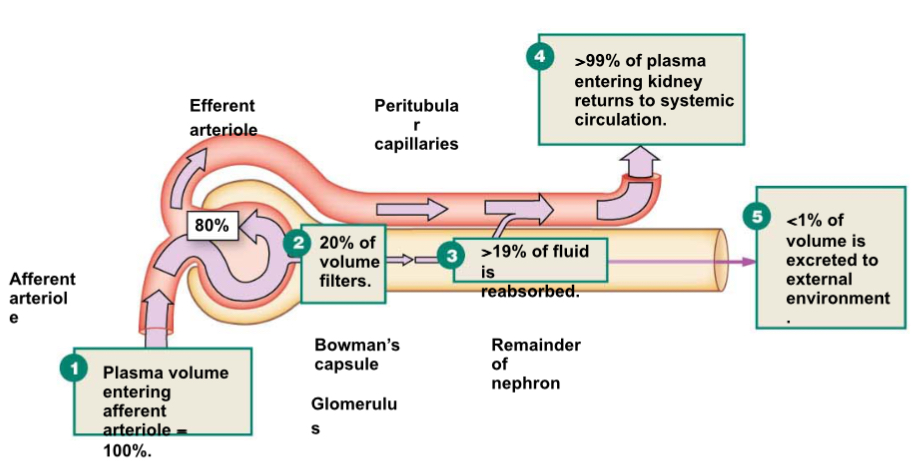
What are podocytes?
Specialized cells that wrap around glomerular capillaries.
What limits the filtration of molecules in the kidneys?
Glomerular capillary endothelium
Glomerular basement membrane/basal lamina
Specialized podocytes.
What makes up the glomerular capillary endothelium
Fenestration that allows passage smaller than RBCs.
Luminal surface lined with negatively-changed proteins of a glycocalyx.
What makes up Glomerular basement membrane/basal lamina.
Layers of extra cellular matrix containing negatively charged glycoproteins, collagen, and other protein.
What makes up specialized podocytes?
Contains long cytoplasmic extensions called foot processes that wrap around the capillaries and interlace to form filtration slits closed by a salt diaphragm.
How does podocyte foot process work?
The surround each capillary, leaving slits through which filtration takes place.
What do mesangial cells do?
alter surface area of filtration slits and secrete immune modulators such as cytokines
What is the glomerular filtration rate (GFR) determined by? How would you describe the rate of GFR?
Filtration pressure
Filtration coefficient (slit SA and filtration barrier permeability.)
Constant.
Filtration pressure equation:
Hydrostatic pressure - colloid osmotic pressure - capsule fluid pressure.
What causes filtration (force).
BP.
Vasoconstriction of the ____ arteriole effects what and how?
AFFERENT;
increases resistance
decreases renal blood flow, capillary BP (PH), and GFR
What doe increased resistance of the _____ arteriole effect and how?
Efferent;
Decrease renal blood flow
Increases PH and GFR
What regulates GFR?
Myogenic response
Tubuloglomerular feedback (paracrine control)
Hormones and autonomic neurons.
What is the myogenic reponse? What is it used in?
intrinsic ability of vascular smooth muscle to respond to pressure changes; regulation of GFR.
How do hormones and autonomic neurons regulate GFR?
By changing resistance in arterioles, and by altering the filtration coefficient.
What do macula densa cells do? What is it involved in?
Sense distal tubule flow and release paracrine factors that affect AFFERENT arteriole diameter.
Involved in tubuloglomerular feedback.
Sequence Tubuloglomerular Feedback and GFR:
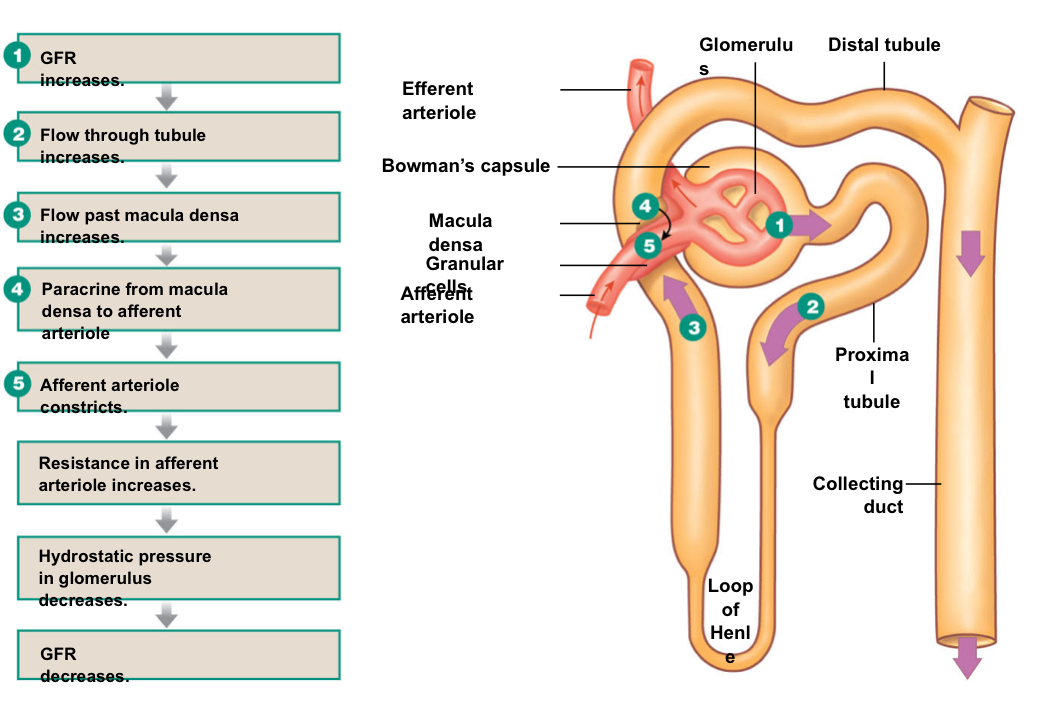
What makes up the Juxtaglomerular Apparatus (JGA)?
The nephron loops back on itself so that the distal tubule is adjacent to the glomerulus; allows for paracrine signaling.
What’s transcelluar transport?
Substances cross apical and basolateral membranes of the tubule epithelial cell; uses transporter carrier and pumps.
What’s the paracelluar pathway?
Substances pass through the tight junctions between two adjacent cells
ID primary active transporters:
Directly coupled to an E source, moves chemicals up a conc. gradient.
ID secondary active transporters:
Coupled to ions (Na+ or H+) gradient. Commonly uptake transporters.
Sequence tubular reabsorption of slutes:
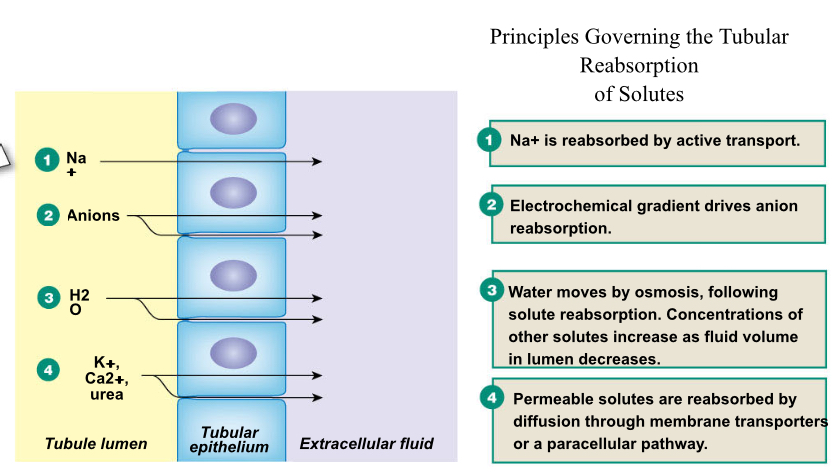
Sequence sodium reabsorption:
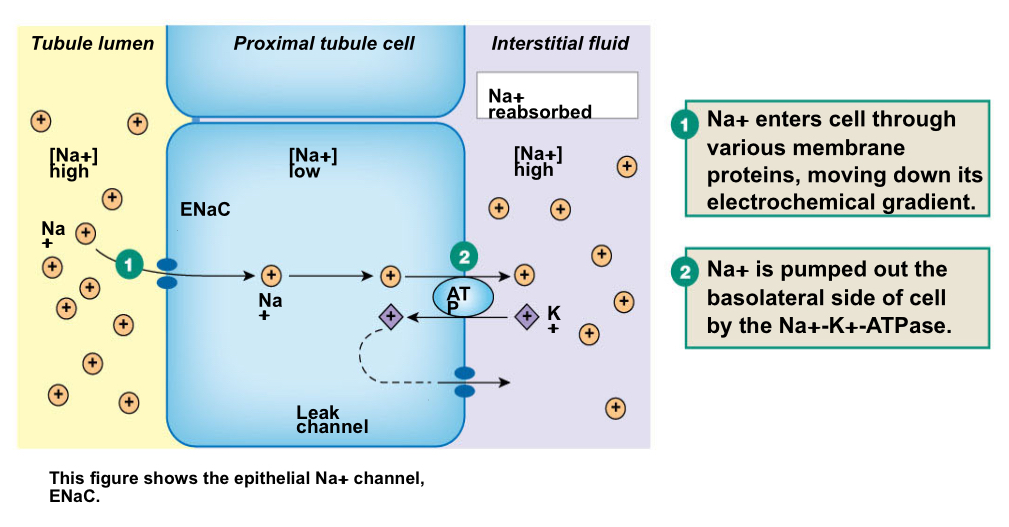
Sequence sodium-linked glucose reabsorption:
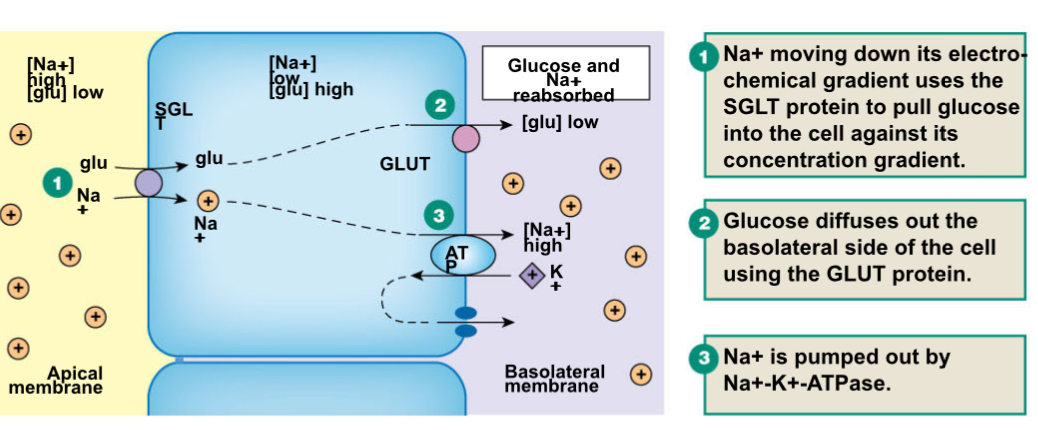
What is filtration of glucose proportional to?
Plasma concentration. Filtration does not saturate.
What is reabsorption of glucose proportional to?
Plasma concentration until the transport maximum is reached.
What is excretion of glucose proportional to?
Nothing! Glucose excretions is zero until the renal threshold is reached.
Excretion equation:
Filtration - Reabsorption + secretion
Increasing secretion enhances what?
Nephron excretion.
What is secretion (kidney).
Transfer of molecules from extracellular fluid into lumen of the nephron
Sequence anion secretion:
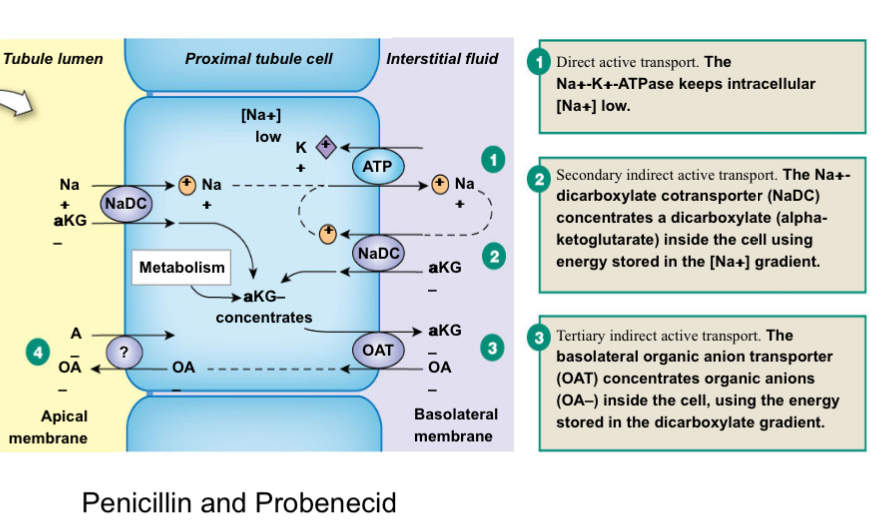
What is clearance?
Rate at which a solute disappears from the body by excretion or by metabolism; Noninvasive way to measure GFR
What is used to measure GFR?
Insulin and creatinine.
If filtration and excretion are the same, then…
there’s no net reabsorption or secretion; clearance of a substance equals the GFR.
Filtered load of X equation:
[X]plasma * GFR
Filtered load of insulin equation:
excretion rate of inulin
GFR equation (insulin clearance ed.)
excretion rate of inulin/[inulin]plasma = inulin clearance
What happens during glucose clearance?
Normally all glucose that’s filtered is reabsorbed.
What happens during urea clearance?
Net absorption.
What is net absorption?
When filtration is greater than excretion.
What happens during penicillin clearance?
Net secretion.
What is net secretion?
When excretion is greater than filtration.
What is micturition?
The process of urination.
What path does micturition take?
Ureter —> Bladder —> Urethra
Does urine change it’s composition?
No.
What in the bladder walls send signals to the spinal cord?
Stretch receptors.
What makes up micturitions?
Internal sphincter (smooth muscle)
external sphincter (skeletal muscle) between bladder and urethra
Sequence micturition pathway:
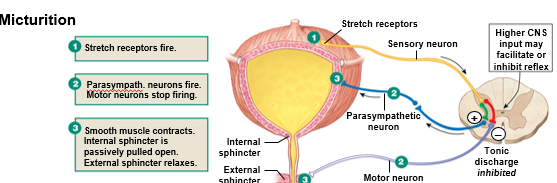
When the bladder is at rest. the internal sphincter is _____.
Passively contracted.
When the bladder is at rest. the external sphincter _____.
Stays contracted.