Extrinsic and Immune Hemolytic Anemias: Pathophysiology, Types, and Laboratory Features
1/48
Earn XP
Description and Tags
credit to tyler
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
49 Terms
What is microangiopathic hemolytic anemia?
A group of potentially life-threatening disorders characterized by RBC fragmentation and thrombocytopenia.
What causes microangiopathic hemolytic anemia?
Mechanical shearing of RBC membranes as cells pass through turbulent areas of small blood vessels.
What are schistocytes?
Distorted and rigid fragments of RBCs resulting from mechanical shearing.
What laboratory findings are associated with microangiopathic hemolytic anemia?
Decreased hemoglobin level, increased reticulocyte count, increased serum indirect bilirubin, and presence of schistocytes.
Name a major type of microangiopathic hemolytic anemia.
Thrombotic thrombocytopenic purpura (TTP).
What characterizes Thrombotic Thrombocytopenic Purpura (TTP)?
Abrupt appearance of microangiopathic hemolytic anemia, severe thrombocytopenia, and elevated serum lactate dehydrogenase.
What enzyme deficiency causes TTP?
A deficiency of the von Willebrand factor-cleaving protease known as ADAMTS-13.
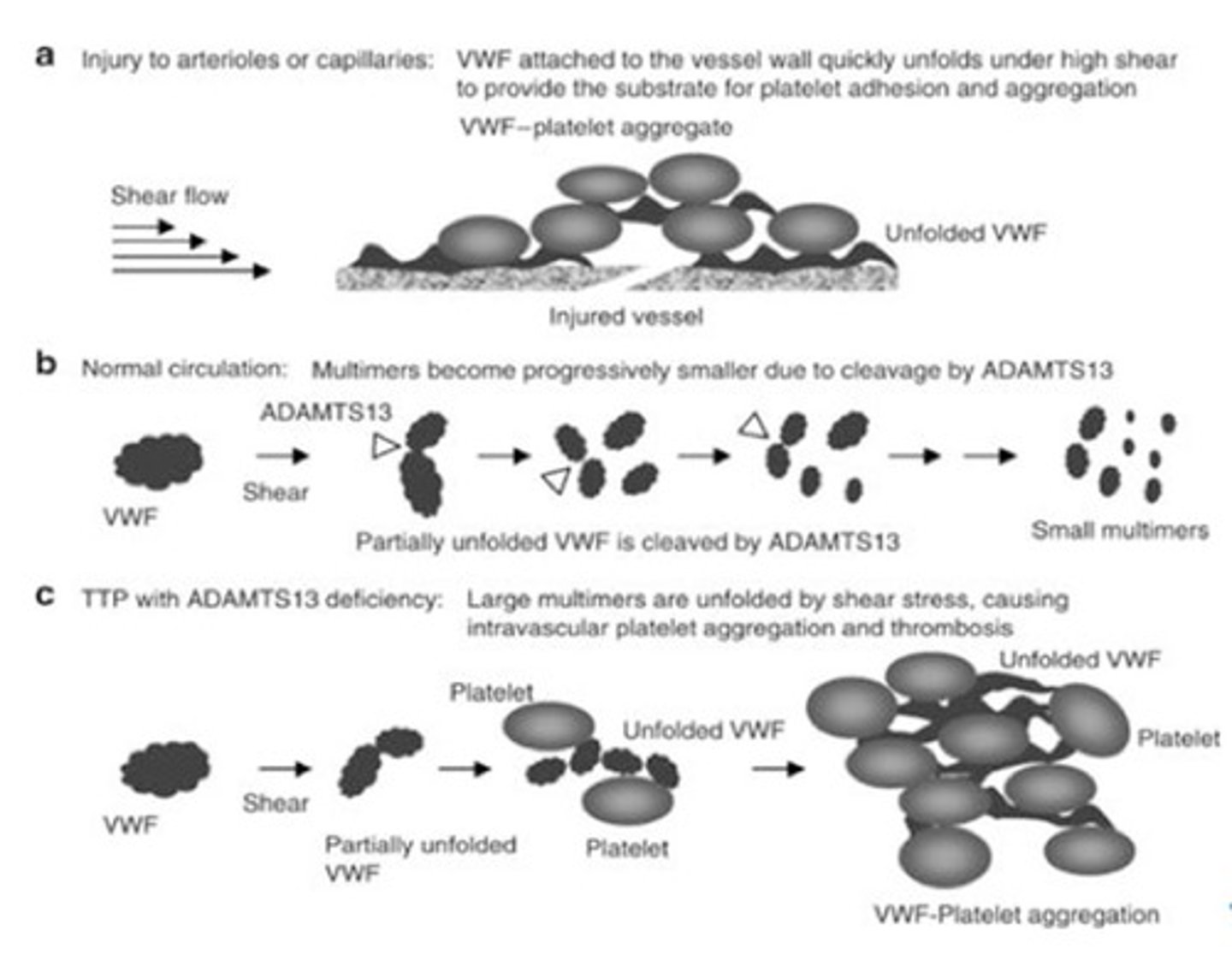
What are typical laboratory findings in TTP?
Platelet count of 10 to 30 × 10^9/L, schistocytes on blood film, and markedly elevated serum lactate dehydrogenase.
What is the treatment for idiopathic TTP?
Plasma exchange therapy to remove ADAMTS-13 autoantibody and infuse replacement ADAMTS-13 enzyme.
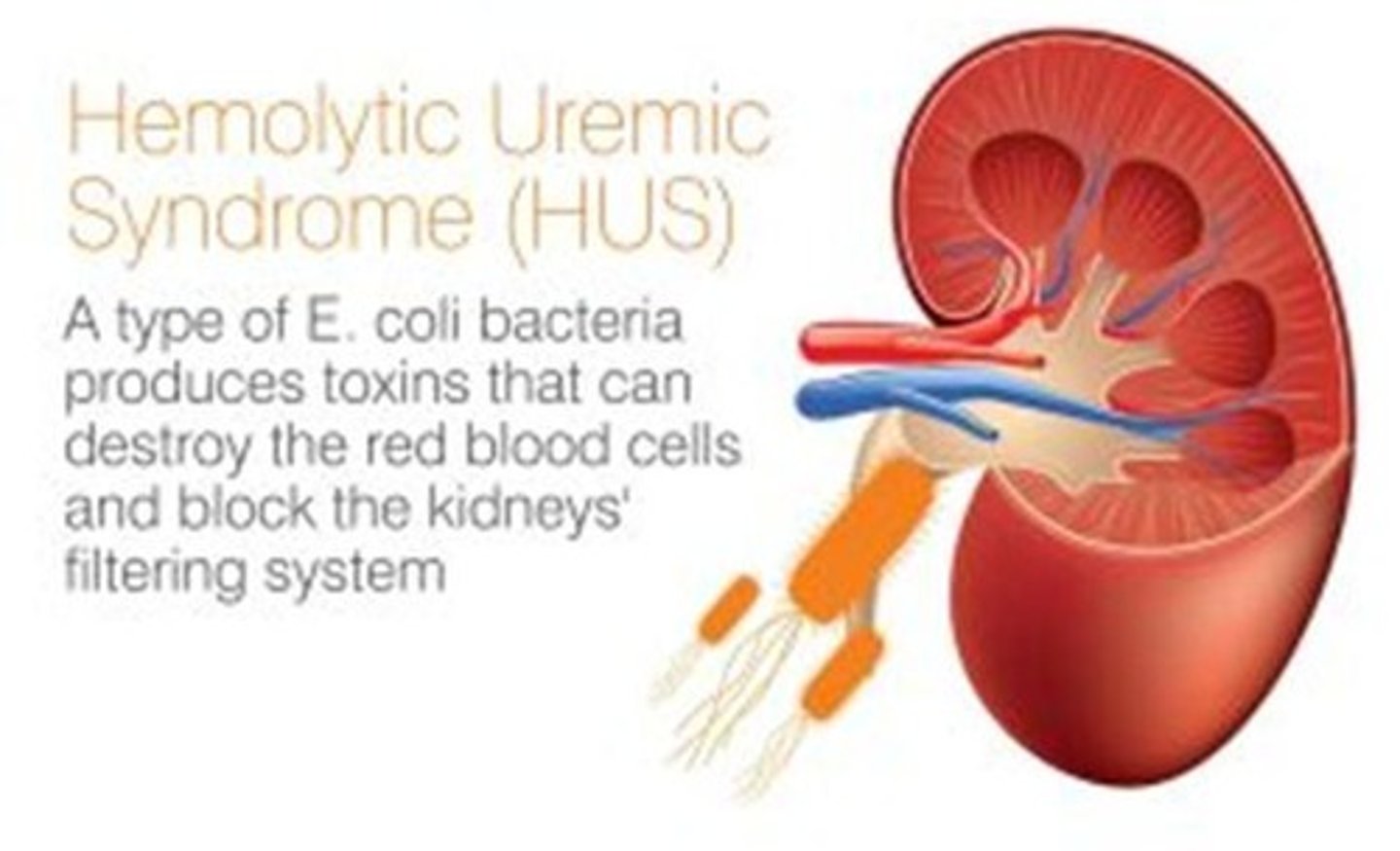
What is Hemolytic Uremic Syndrome (HUS)?
A condition characterized by microangiopathic hemolytic anemia, thrombocytopenia, and acute renal failure.
What typically causes typical HUS?
Infection with Shiga toxin-producing Escherichia coli (STEC), often preceded by gastroenteritis.
What is HELLP syndrome?
A serious pregnancy complication characterized by hemolysis, elevated liver enzymes, and low platelet count.

What are the major diagnostic criteria for HELLP syndrome?
Low platelet count (<100 × 10^9/L), elevated serum lactate dehydrogenase, and elevated aspartate aminotransferase.
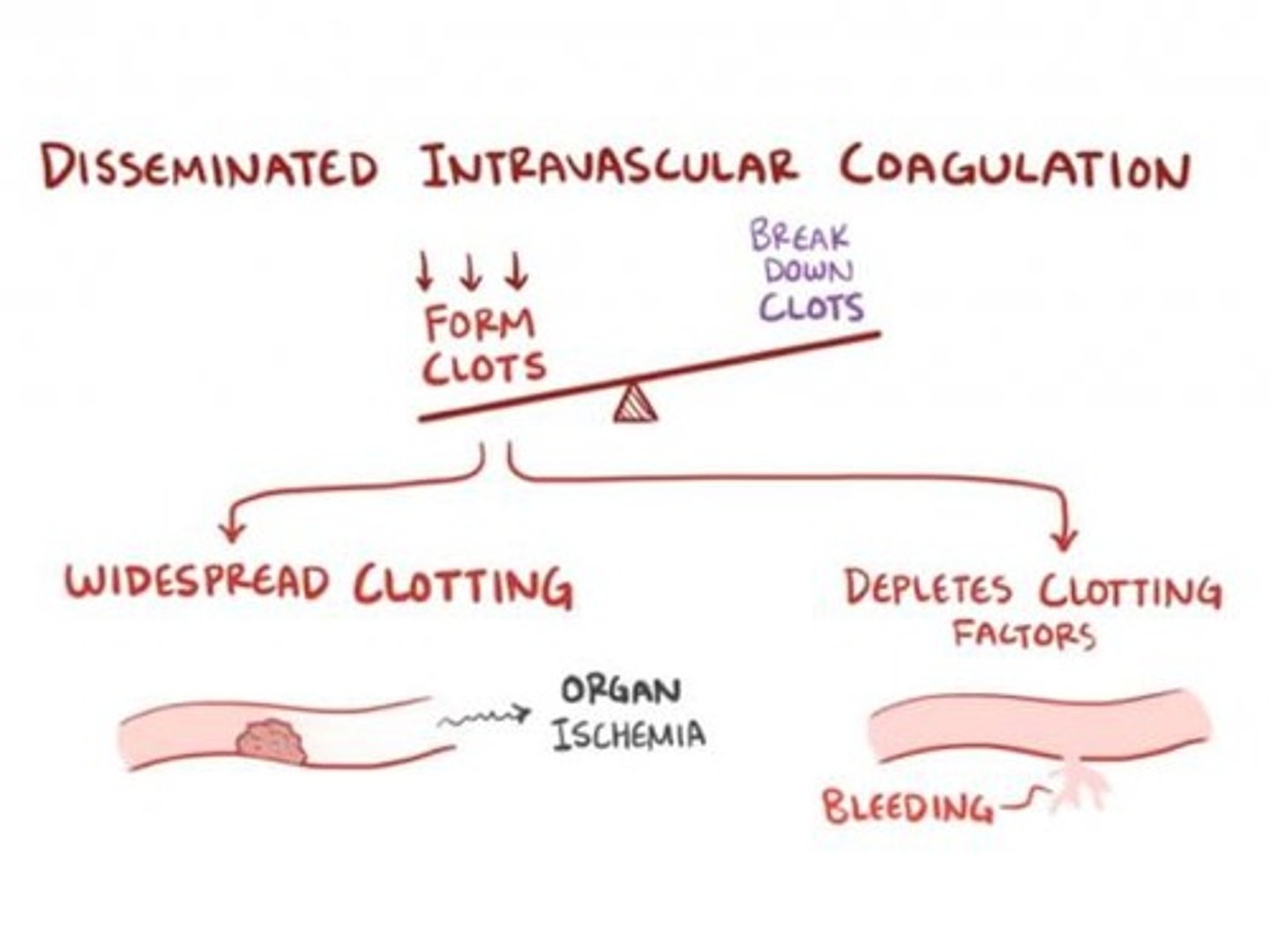
What is Disseminated Intravascular Coagulation (DIC)?
A condition characterized by widespread activation of the hemostatic system, leading to fibrin thrombi formation.
What are common causes of extrinsic hemolytic anemias?
Infectious agents, drugs, chemicals, venoms, and extensive burns.
What distinguishes extrinsic hemolytic anemias from intrinsic ones?
In extrinsic hemolytic anemias, RBCs are structurally and functionally normal but are prematurely hemolyzed due to external factors.
What is the role of microthrombi in microangiopathic hemolytic anemia?
They partially block small blood vessels, causing mechanical injury to RBCs as they pass through.
What is the prognosis for patients with HELLP syndrome?
Worse prognosis is indicated by platelet counts falling below 50 × 10^9/L.
What are the two general types of HUS?
Typical HUS (Shiga toxin-associated) and atypical HUS (caused by unregulated complement activation).
What is the most common cause of typical HUS?
Infection with Shiga toxin-producing Escherichia coli (STEC), particularly serotype O157:H7.
What laboratory findings indicate hemolysis in HELLP syndrome?
Anemia, biochemical evidence of hemolysis, and presence of schistocytes on blood film.
What is the typical platelet count in patients with TTP?
10 to 30 × 10^9/L.
What is the significance of elevated serum lactate dehydrogenase in TTP?
It indicates intravascular hemolysis and extensive tissue ischemia.
What are the major clinical manifestations of hemolytic anemia?
Organ damage due to obstruction of microvasculature and bleeding from consumption of platelets and coagulation factors.
What causes hemolytic anemia in malaria?
Direct lysis of infected RBCs, immune destruction of both infected and noninfected RBCs, and inhibition of erythropoiesis.
Which protozoan parasite is responsible for malaria?
Plasmodium.
What is the most common cause of babesiosis in the United States?
Babesia microti.
What are common symptoms of babesiosis?
Fever, chills, headache, sweats, nausea, arthralgias, myalgia, anorexia, and fatigue.
How is babesiosis diagnosed?
By demonstrating the parasite on Wright-Giemsa stained thin peripheral blood films.
What can cause hemolytic anemia due to drug and chemical exposure?
Oxidative denaturation of hemoglobin leading to methemoglobin and Heinz bodies.
What is the effect of extensive burns on red blood cells?
It induces RBC fragmentation and budding, leading to acute hemolytic anemia.
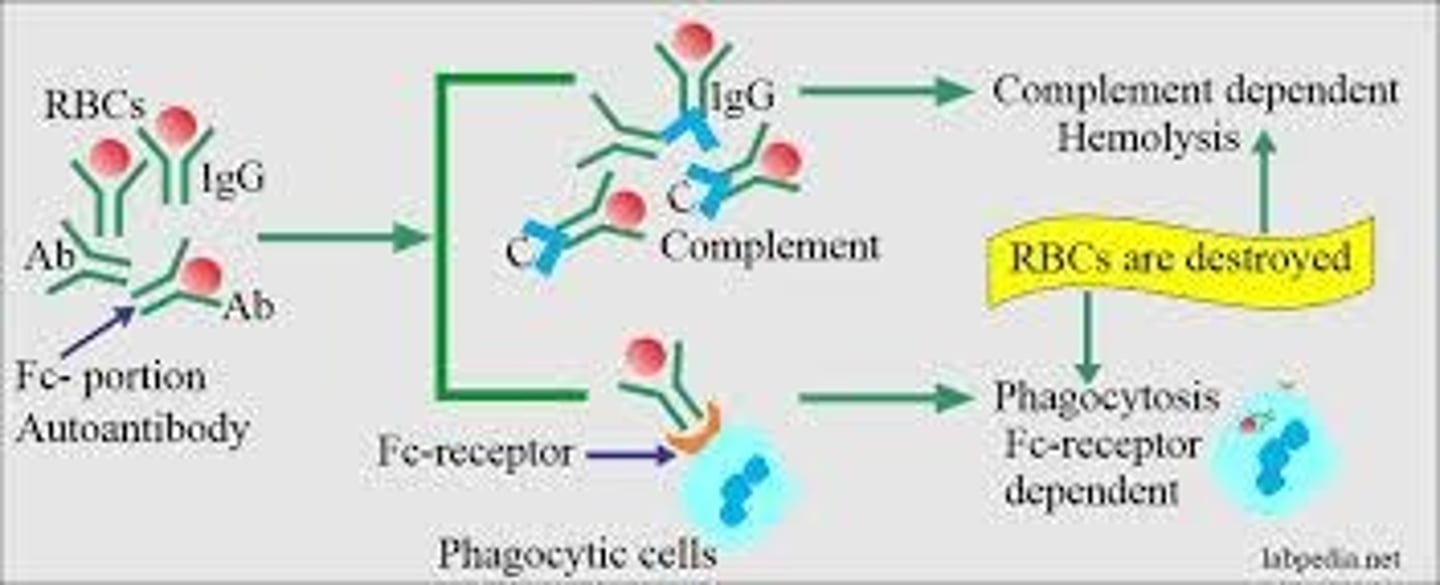
What are the two classes of antibodies involved in immune hemolytic anemias?
Immunoglobulin G (IgG) and Immunoglobulin M (IgM).
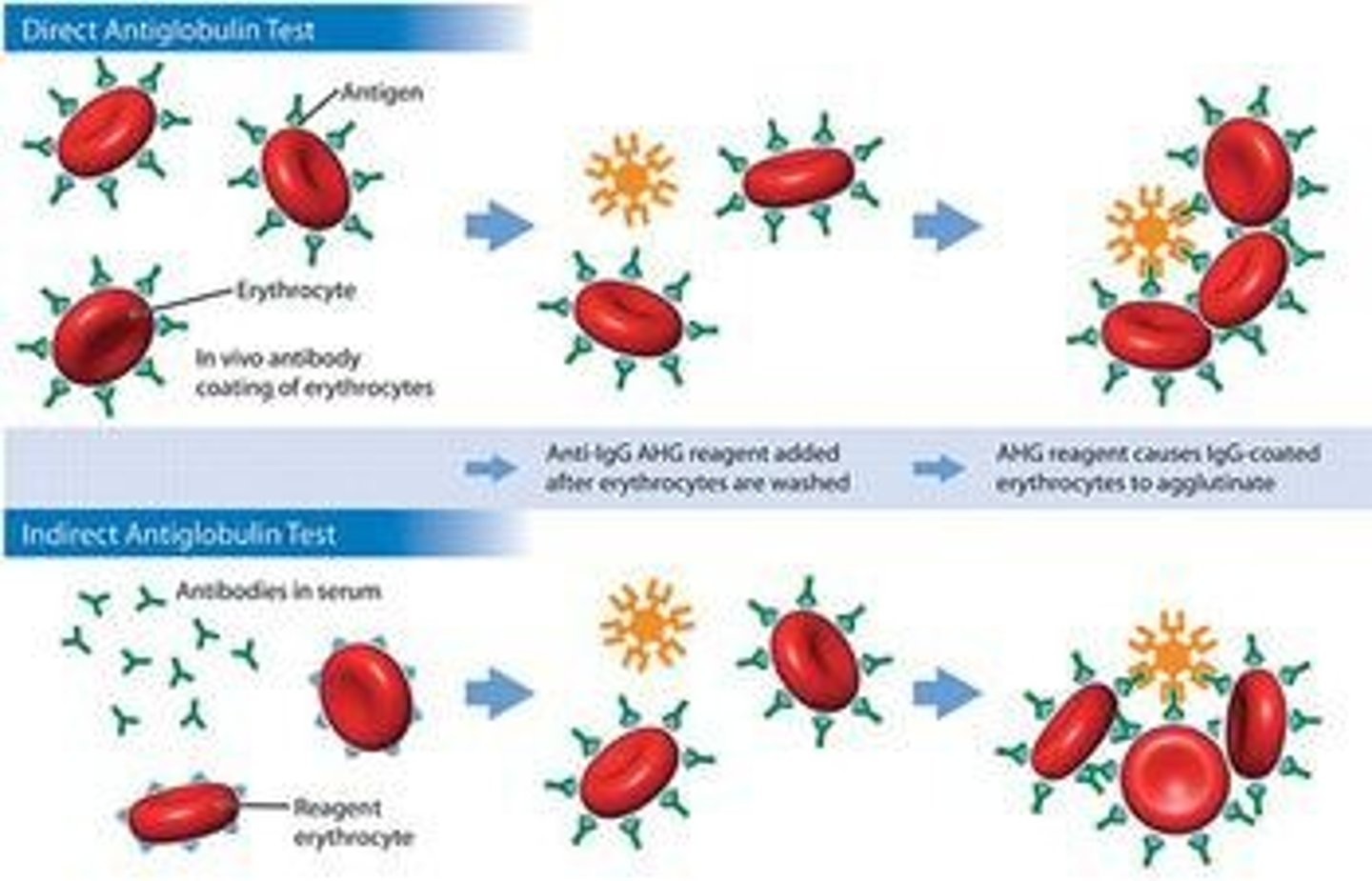
What does a positive Direct Antiglobulin Test (DAT) indicate?
In vivo sensitization of RBC surface by IgG, C3b, or C3d.
What is Warm Autoimmune Hemolytic Anemia (WAIHA)?
The most common autoimmune hemolytic anemia, where autoantibodies react optimally at 37°C.
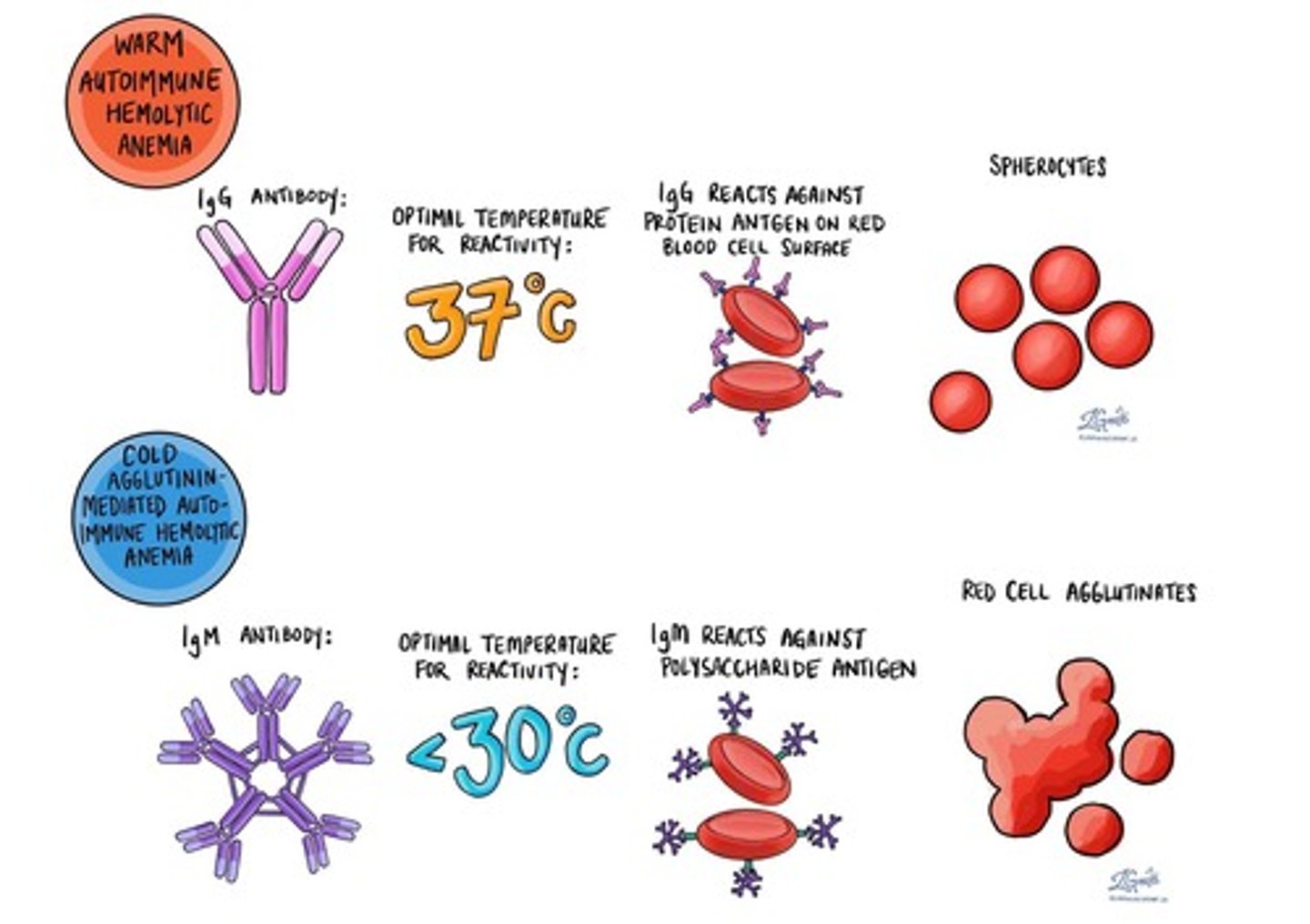
What percentage of WAIHA cases are idiopathic?
Approximately 70% are idiopathic.
What laboratory findings are associated with WAIHA?
A positive DAT in over 95% of patients, with approximately 85% having IgG.
What is the significance of warm autoantibodies in WAIHA?
They are usually panreactive, agglutinating all screening and panel cells.
What can cause secondary WAIHA?
Lymphoproliferative diseases, nonlymphoid neoplasms, autoimmune disorders, immunodeficiency disorders, and viral infections.
What are schistocytes, spherocytes, and microspherocytes?
Types of red blood cell abnormalities observed in hemolytic anemia.
What is the role of the spleen in hemolytic anemia?
It removes damaged or senescent red blood cells from circulation.
What is the impact of venom from snakes or insects on red blood cells?
It can induce hemolytic anemia, potentially leading to renal failure and death.
What is the primary mechanism of immune hemolytic anemia?
Antibody-mediated destruction of red blood cells.
What are the clinical consequences of severe babesiosis?
Acute respiratory failure, congestive heart failure, renal shutdown, liver failure, CNS involvement, or disseminated intravascular coagulation.
What is the effect of malaria on noninfected RBCs?
Infected parasites shed proteins that modify noninfected RBCs, enhancing their removal by the spleen.
What is the significance of Heinz bodies in hemolytic anemia?
They indicate oxidative damage to hemoglobin due to drugs or chemicals.
How does the DAT procedure work?
Polyspecific antihuman globulin is added to patient RBCs to detect sensitization.
What is the typical duration of symptoms in babesiosis?
Symptoms can last from several weeks to months.
What is the relationship between RBC temperature and WAIHA?
WAIHA autoantibodies react optimally at body temperature (37°C).
What is the role of the immune system in hemolytic anemia?
It mediates the destruction of red blood cells through antibody binding.