BIO110: PHYSIOLOGY QUIZ 2 GUIDE
1/71
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
72 Terms
DEFINE TENDON
muscle to bone
define ligament
attaches bone to bone
define motor unit
One motor neuron plus all of the muscle fibers it innervates
define thick filament
aka myosin
attaches to actin using the “myosin head”, ATP + P attaches onto the head to begin the attachment. Once attached the ATP + P is released and slides the actin to the center of the sacromere
define thin filament
aka ACTIN
Allows the myosin to attach onto actin to allows the actin to slide into the center of the sarcomere
define sacromere & draw the diagram
the smallest functional unit of skeletal muscles
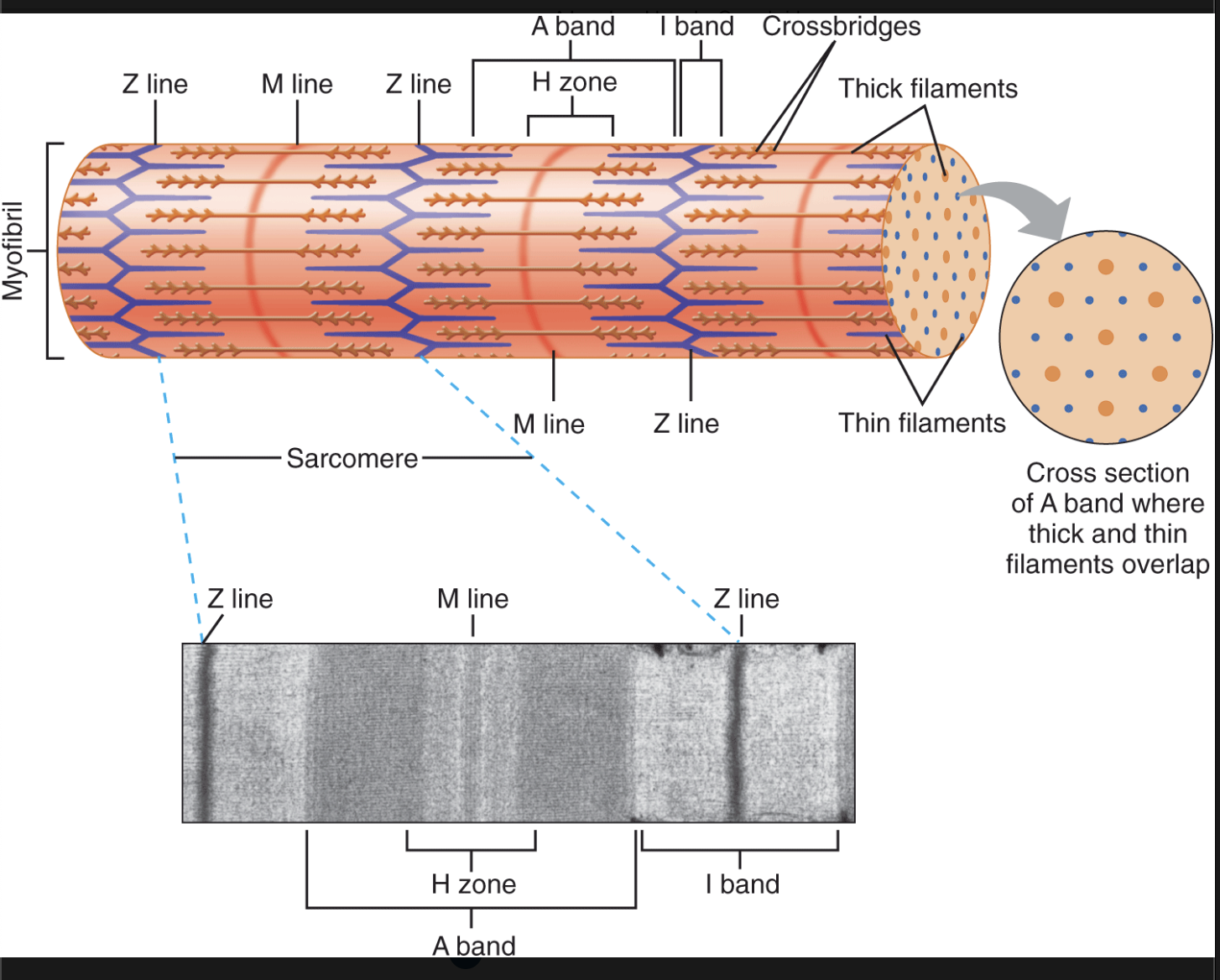
define origin and insertion of muscles
Origin: part of the muscle that does not move joint
Insertion: part of muscle that does move joint
define creatine kinase
Creatine Kinase is the enzyme that catalyzes creatine phosphate + ADP to make ATP. It is reversible as well
First source of energy for skeletal muscle
what is the function of T-tubules
AKA transverse tubules: carry electrical signals deep into the muscle fibers. Triggers the sarcoplasmic reticulum to release calcium, the calcium allows the muscle to contracts
Bring action potential inside the cell
what is the function of myoglobin
Stores oxygen in the muscle
Hemoglobin stores o2 into the rbc
where is calcium stored in muscle cells and how is it released during contracton?
Stores: sarcoplasm reticulum
released: action potential created by acetylcholine
what is the cross-bridge cycle
Actin attaches to myosin and contracts the muscle
what happens to the sacromere during contraction?
What specifically changes
Z lines move closer together
I band gets smaller
H zone gets smaller or disappears
A band stays the same length
Why this happens
Actin (thin filaments) slide over myosin (thick filaments).
The sarcomere gets short / small
what is the difference between fast and slow muscle fibers?
fast / slow myosin ATPase
Fast fibers contain fast ATPase. It splits ATP rapidly, allowing cross bridge repeat quickly, it is faster but tire easily
Slow fibers contain slow ATPase. It splits the ATP slowly, allowing the cross bridge to repeat slowly. It is slower but lasts longer
When oxidative phosphorylation is not sufficient, what becomes the source of energy and what is the byproduct?
Phosphorylation of ADP by creatine phosphate
Oxidative phosphorylation of ADP in mitochondria
Anaerobic glycolysis
What type of neuron causes skeletal muscle contraction
motor neuron / alpha motor
define polycythemia
increased erythrocytes
define hypoxia
low oxygen in the tissue
define hypoxemia
low oxygen in arterial blood
define anemia
A reduction of amount of oxygen/hemoglobin a red blood cell can carry or lack of production in RBC
Decrease oxygen carrying capacity
define hematocrit
The fractional amount of erythrocytes to the blood is called the hematocrit
define hemoglobin
a protein in red blood cells that carries oxygen and carbon dioxide
define albumin
where is albumin produced in
Albumin is the most abundant protein in blood plasma.
Maintains osmotic pressure → helps keep fluid in blood vessels
keeps water into veins/B.V. away from tissue
made from liver
define EPO
Erythropoietin
hormone released from the kidney in response to low oxygen; stimulates the synthesis of erythrocytes
What is/are endothelium and endothelial cells
where can you find them?
Endothelial cells: The individual cells that make up the inner lining of blood vessels and the heart.
Endothelium: The layer formed by endothelial cells. It is the continuous lining inside blood vessels and the heart.
lining blood vessels of the heart
define nitric oxide
Produced at: endothelium
Function: dilates blood vessels and prevent platelet aggregation / clumping
Stops clot formation
define hemostasis
stop blood loss
what is the life cycle and lifespan of red blood cells
Lives 120 days
Cycle:
kidney sends EPI > bone marrow to produce red blood cell
When young, RBC is flexible. When old, it gets hard and brittle > spleen (which is narrow) = young will thrive but old will be brittle and break into parts. In the spleen RBC will break into Globin + heme into bilirubin + iron
Bilirubin > liver & turn into bile
Bile > kidney > urine
Bile > digestive > poop
what substance gives urine and feces their yellow colour?
biliburin
what are the function of the spleen?
Removes waste and damaged RBC
what is fibrinogen and what role does it play in clot formation?
Fibrinogen is synthesized by the liver and is a key substance in the formation of blood clots.
what converts fibrinogen into fibrin?
thrombin
what is hematocrit and what is the normal range?
What is hematocrit and what is the normal range?
percentage of RBC present in Total Blood volume
Men: 42-52%
Women 37-47%
around 45%
which organ produces the most clotting factors?
liver
what are the function of hemoglobin?
protein in the RBC that Produces oxygen and carbon dioxide
what is pernicious anemia
condition is due to a lack of vitamin B12
What is jaundice and which substance causes it when elevated?
Yellowing of eyes and skin due to increased bilirubin
define cardiac output?
Cardiac output is the amount of blood the heart pumps per minute.
CO = SV × HR
define stroke volume and what is normal range?
Stroke volume is the amount of blood ejected by the left ventricle of the heart in one heartbeat.
70ml
define mean arterial pressure
Mean arterial pressure (MAP) is the driving force for blood flow through the systemic circulation.
MAP = 1SBP + 2 DBP / 3
AVERAGE IS 90
define TPR
TOTAL PERIPHERAL RESISTANCE
in the systemic circuit (blood flow L heart > body > R heart), the combined resistance (resistance determines how hard the heart must pump) of all the blood vessels
Example: Narrower or more numerous pipes → higher resistance, All the pipes together = total resistance in the system
TPR=MAP/CO
DEFINE EJECTION FRACTION
Ejection fraction is the percentage of blood pumped out of the ventricle with each heartbeat.
EF = STROKE VOLUME / END-DIASTOLIC VOLUME * 100
SV: BLOOD EJECTED PER BEAT
EDV: BLOOD IN VENTRICLE BEFORE CONTRACTION
Normal: ~55-70% (54%)
DEFINE COMPLIANCE
ability for b.v. to stretch
arteries = low compliance
veins = increased compliance
define PP
“pulse pressure”
PP = SYSTOLIC PRESSURE - DIASTOLIC PRESSURE
define ischemia
decreased blood flow to a tissue / organ
define arterial baroreceptors
pressure receptors in the artery that senses presusre change in the blood
define role does MAP play in systemic circulation?
Mean arterial pressure (MAP) is the driving force for blood flow through the systemic circulation.
MAP = 1SBP + 2 DBP / 3
AVERAGE IS 90
what is the driving force of blood in a closed system
MAP
what is the compliance of arteries versus veins
Compliance is how easily a blood vessel can stretch when pressure increases.
Arteries
Stiffer (low compliance)
Can maintain high pressure
Veins
Stretchy (high compliance)
Can store large volumes of blood
what is total peripheral resistance and how is it calculated
in the systemic circuit (blood flow L heart > body > R heart), the combined resistance (resistance determines how hard the heart must pump) of all the blood vessels
TPR = MAP / CO
in which type of vessels does the largest drop in arterial pressure occur
arterioles because they provide the greatest resistance to blood flow.
which vessels have the greatest total cross-sectional area
Capillaries have the greatest total cross-sectional area, allowing slow blood flow for exchange with tissues.
which artery is most commonly used to measure blood pressure
Blood pressure is most commonly measured in the brachial artery of the upper arm.
at rest where is most of the blood in circulatory system found and why?
At rest, most blood is in the veins (60%) because they are compliant and serve as blood reservoirs.
is atrial fibrillation usually fatal?
Atrial fibrillation is usually not fatal on its own, but it increases the risk of stroke and heart failure. Often managed with medications (rate/rhythm control, anticoagulants)
What is the myogenic response?
IF BLOOD VESSELS STRETCH, IT RECOILS
define diffusion, filtration, and reabsorption in capillaries
Capillaries are thin-walled vessels where substances move between blood and tissues. There are three main mechanisms:
Diffusion Definition: Movement of molecules from high concentration → low concentration.
Filtration Definition: Movement of fluid from blood to interstitial
Reabsorption Definition: Definition: “Movement of fluid from interstitial to blood”
what are the different types of capillaries
Continuous capillaries:
Most common type
Small gaps between endothelial cells; allow for watersoluble substances; if larger than water-soluble molecules, it is more difficult to pass through
Fenestrated capillaries
Large gaps between endothelial cells forming pores or fenestrations (windows)
Allow proteins, and in some cases blood cells, to move through
define the function of veins
large blood vessels that carry blood toward the heart
called "volume reservoir”
blood remain in veins and moves only by the muscle of the veins
keeps 60% of blood
define active vs reactive hyperemia
Active: increased blood flow in response to increased metabolic activity
Steady state:
O2 is delivered as fast as it is consumed
CO2 is removed as fast as it is produced
Increased metabolic rate
O2 is consumed faster than it is delivered
CO2 is produced faster than it is removed
Reactive: increased blood flow in response to a previous reduction in blood flow
Blockage of blood flow to tissues
Metabolites increase and oxygen decreases
Vasodilation
When blockage is released
ncreased blood flow due to low resistance
Metabolites removed, oxygen delivered
define effect nitric oxide has on blood vessels
causes vasodilation by relaxing vascular smooth muscle
stops clot formation
define general function of adrenergic receptors
Alpha:
1) Blood Vessels
2) CNS
Beta:
1) heart
2) lungs
3) adipose
The general function of cholinergic receptors
Muscarinic:
All organs
Nicotinic
Neuromuscular junction
which adrenergic receptor are found mosly in blood vessels
alpha 1
what are arterial baroreceptors
pressure receptors that senses pressure changes in BP
which of the central nervous system controls the cardiovascular centers?
The brainstem controls the cardiovascular centers specifically the medulla oblongata acting to regulate the HR and BP.
what is filtration and reabsorption
Filtration: Movement of fluid/solutes across a membrane due to pressure.
example: fluid from the blood stream enters the tubules of the kidneys
Reabsorption: refers to movement of filtered solutes and water from the lumen of the tubules back into the plasma.
what is the function of endothelium
Endothelium: The layer formed by endothelial cells. It is the continuous lining inside blood vessels and the heart. Think of it as the “tissue,” while endothelial cells are the “building blocks.
what is the role of EPO in oxygen regulation
EPO = erythropoietin
Erythropoietin is released from certain cells in the kidney in response to low oxygen levels in blood.
bands of sarcomere
A Band: measures the length of thick filaments, contains thick & thin filaments
H zone: part of the A-band, contains ONLY thick filaments
I band: contains only thin filaments
M band: links thick filaments together
Z line: links thin filaments
what are the 3 sources of ATP?
creatine phosphate
aka “energy on tap” does not depend on body state or food. DEPENDS NO FACTORS
on set / right away
does not last long (30 seconds - 60 seconds)
Oxidative phosphorylation
Burns food to make ATP
Reliant on body state and food
The primary source
Limited by oxygen
anaerobic glycolysis
becomes dominant source when oxygen is low
break down glucose without affecting o2
problem: produces lactic acid