Exam 2 Cmbined
1/147
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
148 Terms
In general, how does an action potential occur?
when a stimulus of suffecient strength depolarizes the cell
What’s the all or none law?
once a nerve impulse is initiated, it will travel the length of the neuron
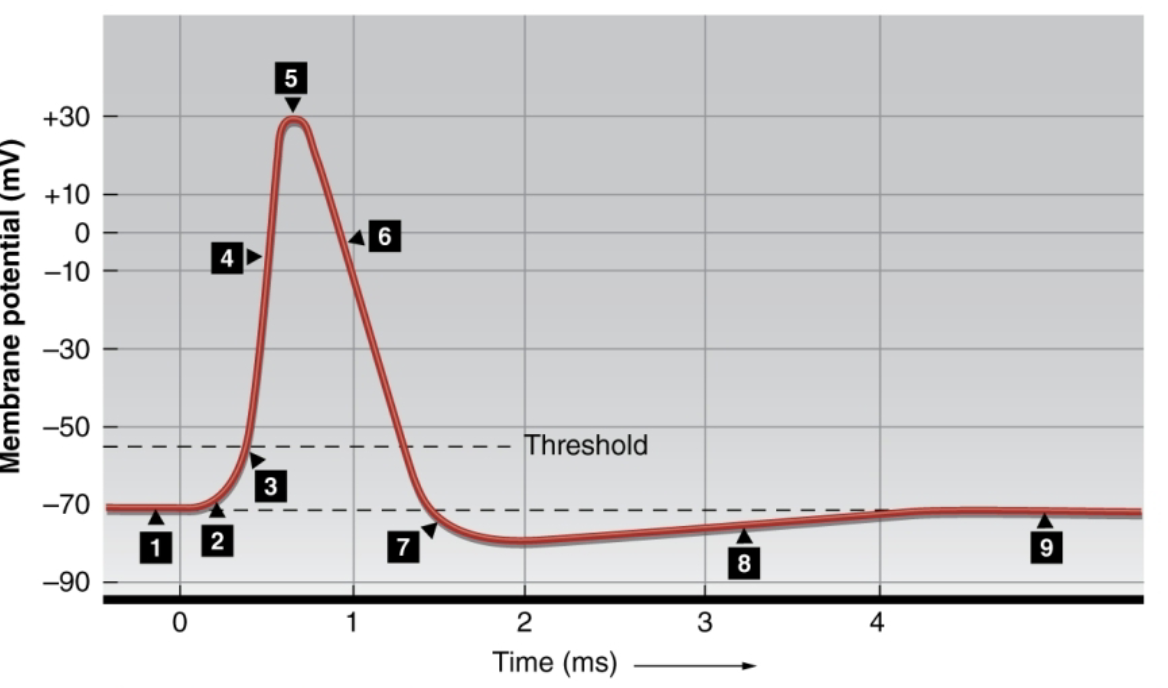
Describe what’s happening at 1-3?
1: resting membrane potential remains constant around -70mV due to fixed anions and sodium potassium pumps, 2: a depolarizing stimulus shifts the membrane towards threshold, 3: the membrane depolarizes to threshold (-55mV), opening all voltage gated NA+ channels
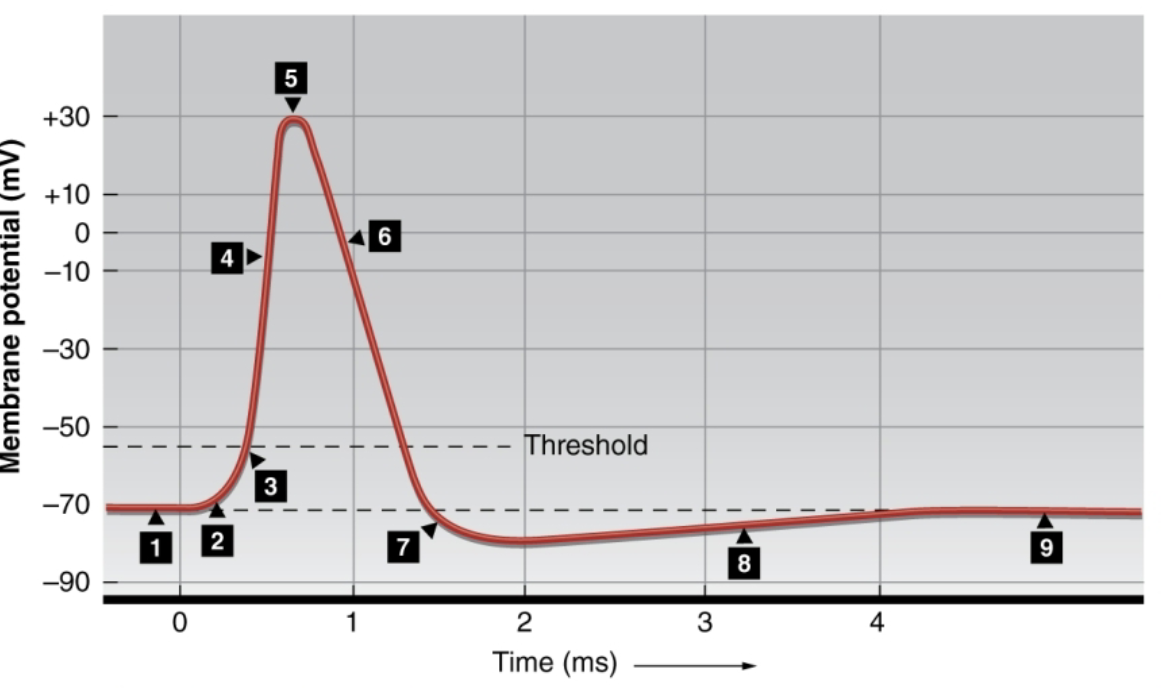
What happens at 4?
rapid NA+ entry (influx) depolarizes the cell
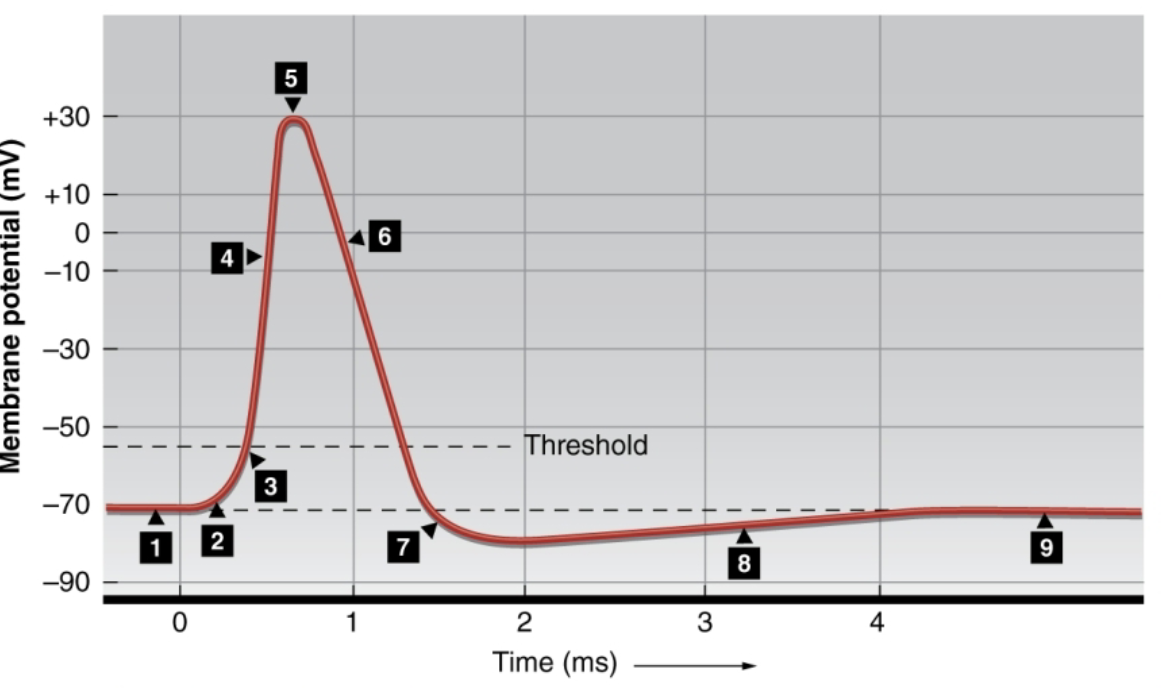
What happens at 5?
Na channels close and slow K channels open
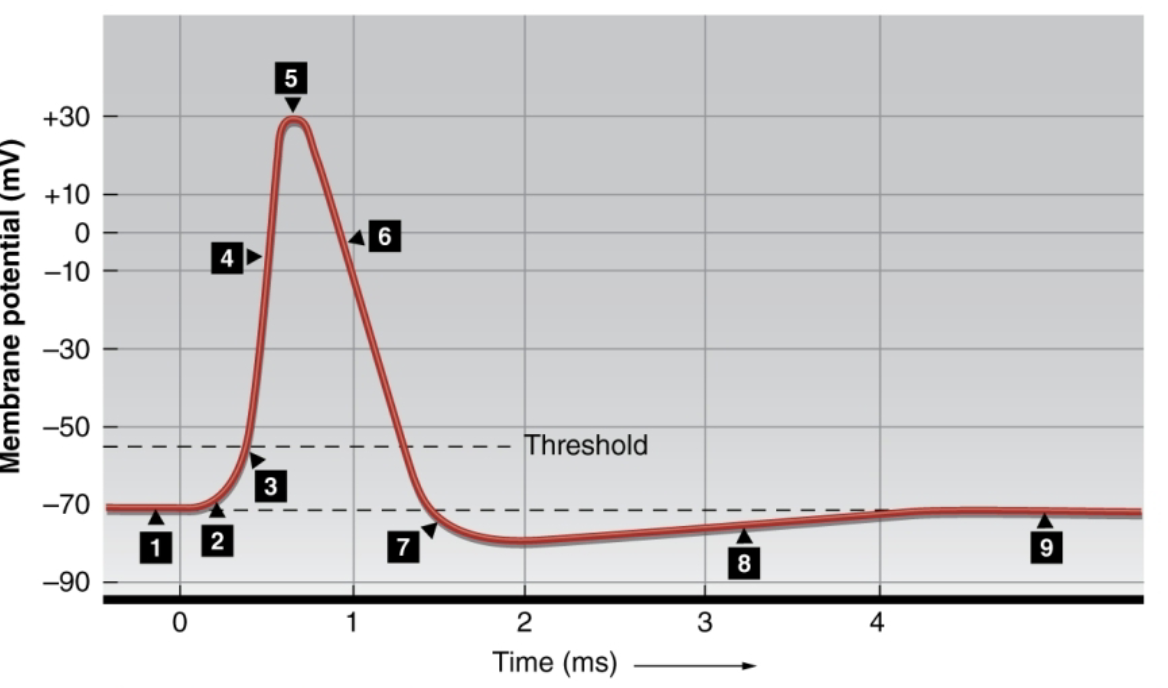
What happens at 6?
K+ leaves the cell rapidly, repolarizing the membrane
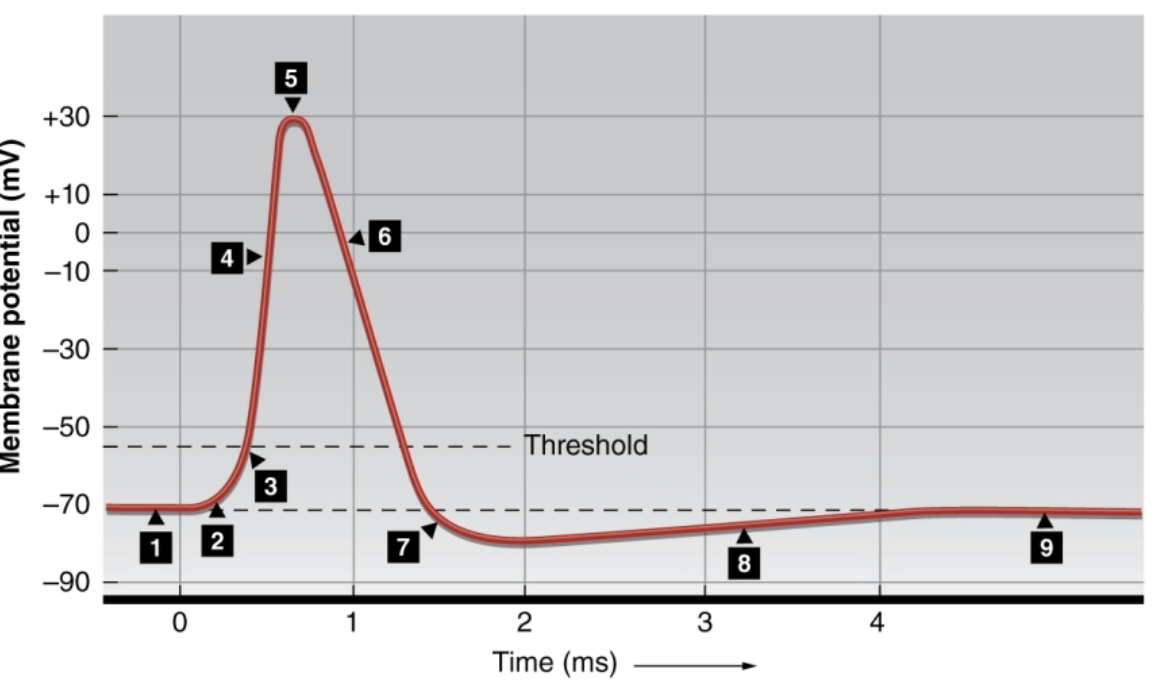
What happens at 7-9?
7: K+ channels remain open and extra K+ leaves the cell, hyperpolarizing it, 8: voltage gated K+ channels close while a bit of K+ still leaks out, 9: resting membrane potential and membrane permeability is restored
What two major factors influence the velocity of an AP?
myelination (saltatory conduction) and size principle (axon diameter)
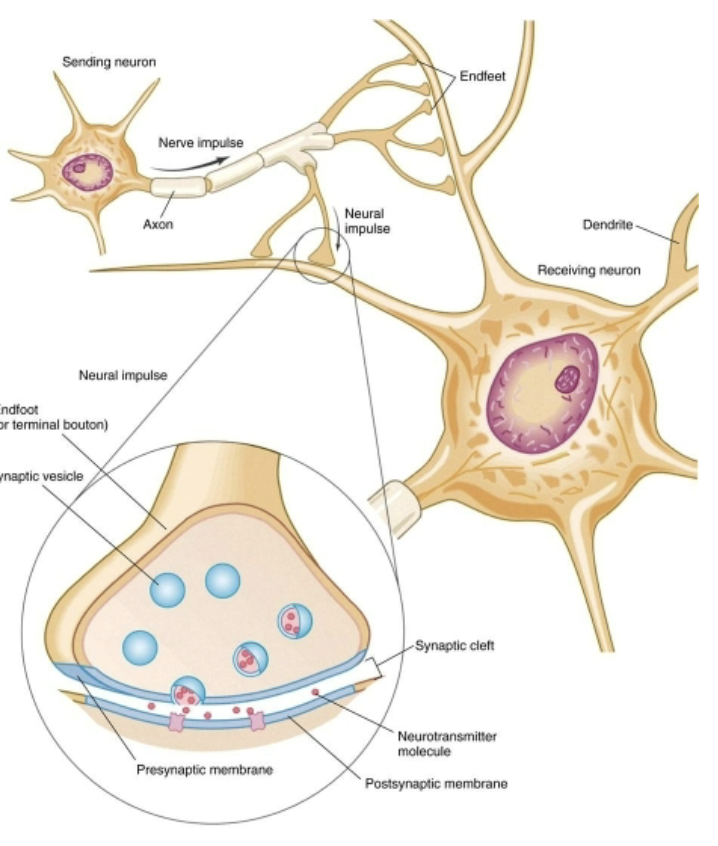
What’s a neurotransmitter?
a chemical messenger released from the presynaptic neuron, which binds to receptors on the postsynaptic membrane, causing depolarization or repolarization of the postsynaptic membrane
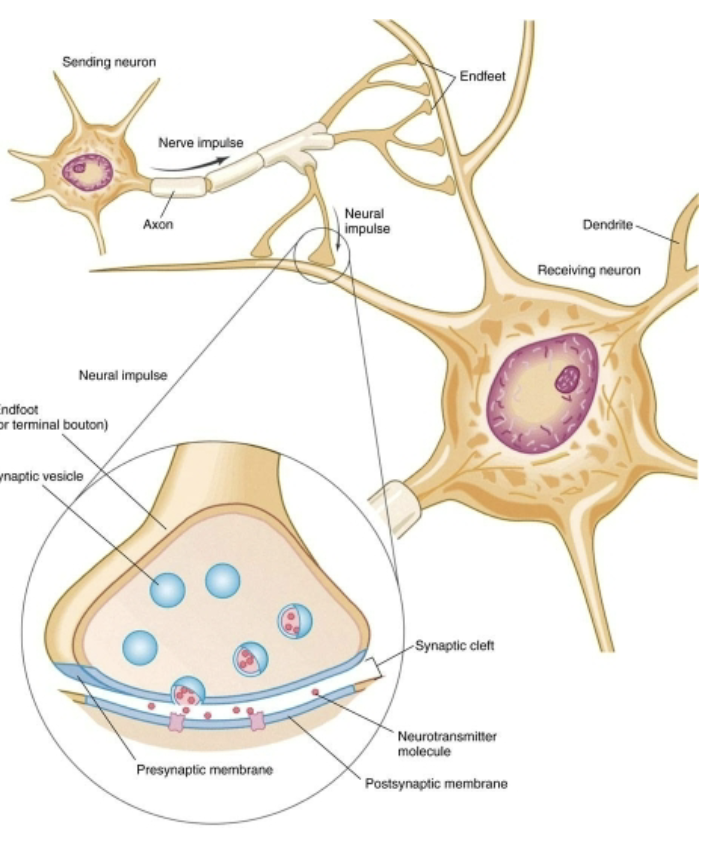
What’s an EPSP and what two factors influence it?
a small depolarization of the postsynaptic membrane making it more likely to generate an AP, influenced by spatial and temporal summation
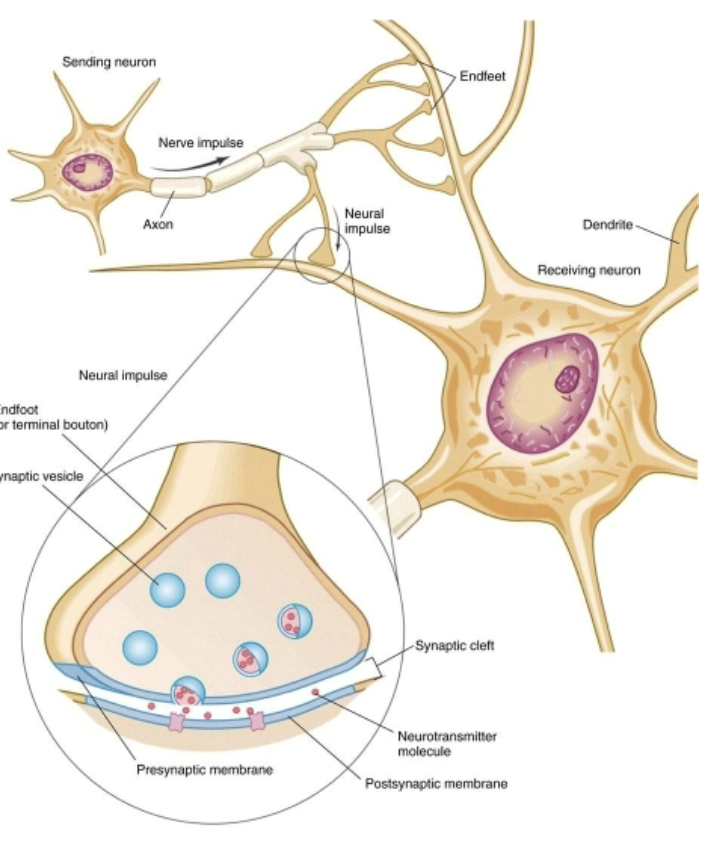
What’s an IPSP?
change in the postsynaptic membrane that makes it less likely to generate an action potential
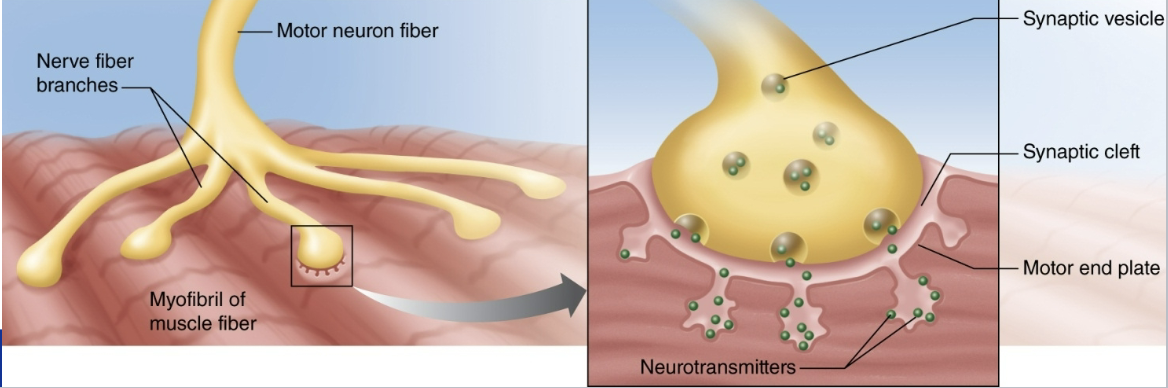
What’s the NMJ?
area between a motor neuron and a muscle fiber for a motor unit
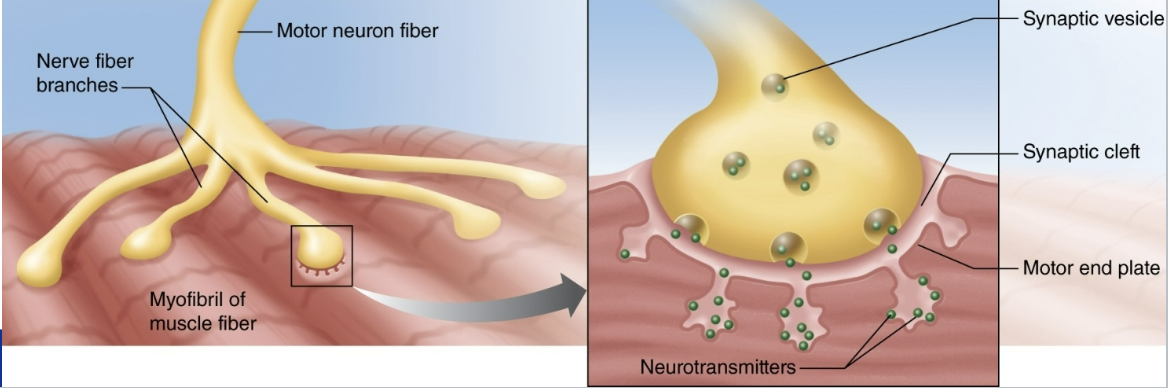
What’s a motor end plate?
pocket formed around a motor neuron by the sarcolemma of a muscle fiber
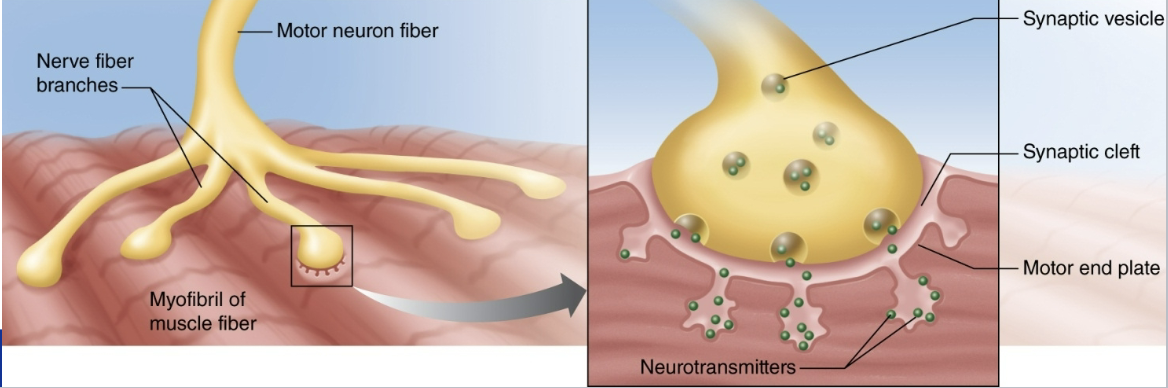
How does a motor neuron create a muscular AP?
Ach is released from the motor neuron which causes an end plate potential (EPP), which moves down into the T-tubles
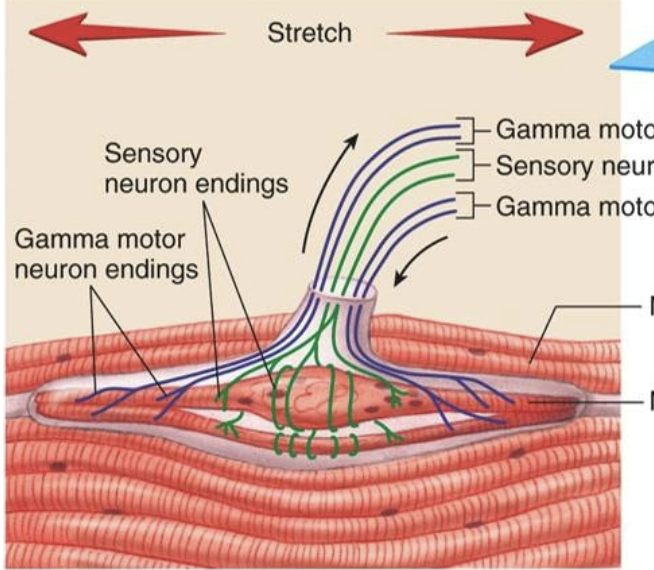
What’s a muscle spindle?
sensory receptor inside skeletal muscle which respond to changes in muscle length
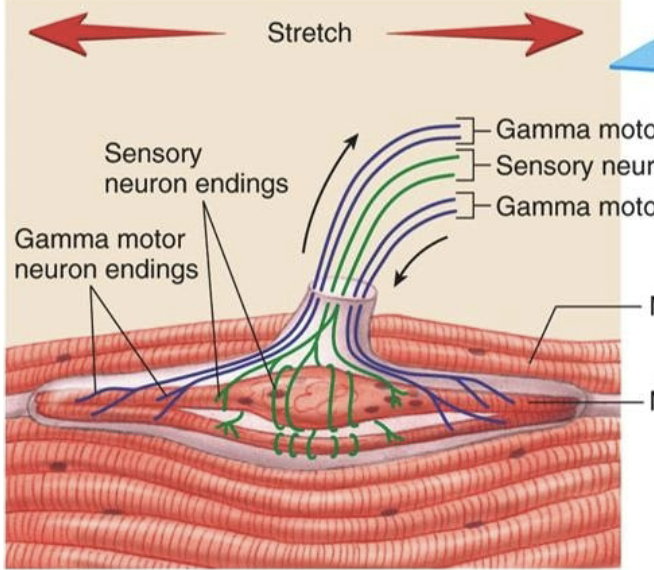
What are intrafusal fibers?
part of a muscle spindle, run parallel to normal fibers
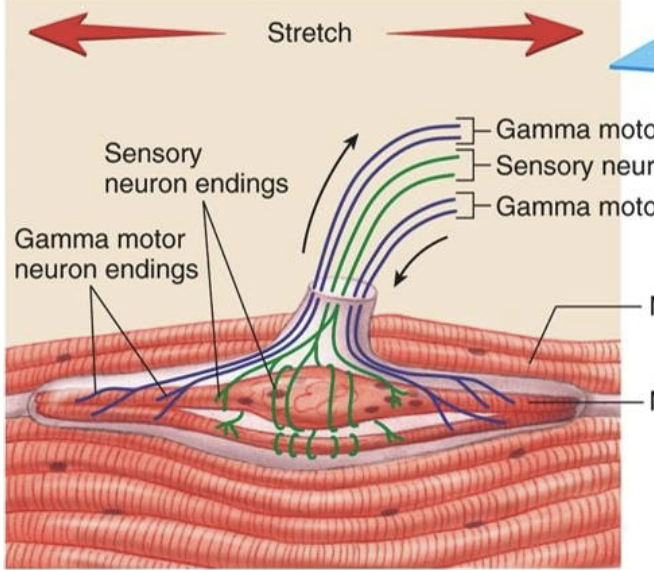
What are gamma motor neurons?
part of a muscle spindle, stimulate intrafusal fibers to contract with extrafusal (normal) fibers via aplha motor neuron
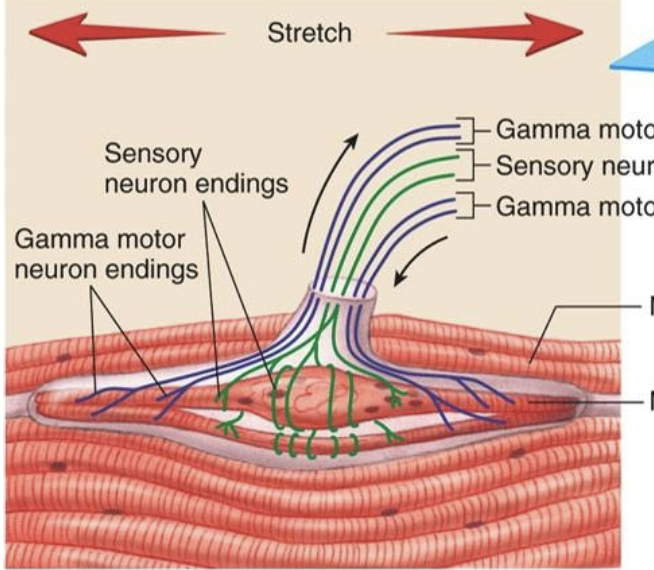
What is the GTO?
a sensory receptor embedded in tendons, which monitors tension in muscles and prevents muscle damage during excessive force production
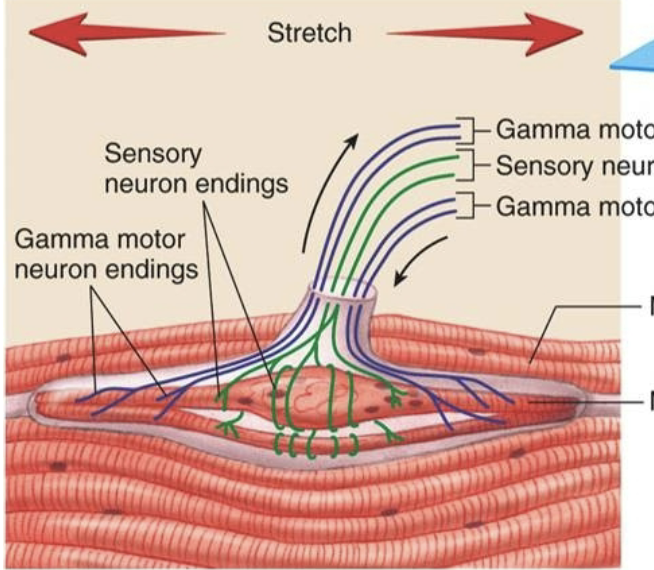
What do GTO’s do when stimulated by excessive tension?
inhibit agonists, excite antagonists to rpevent excessive tension in the muscle/tendon
What are the three major functions of skeletal muscle?
force production for locomotion and breathing, force production for postural support, heat production during cold stress
What is an isometric contraction?
muscle exerts force without changing length, ex: postural muscles
What is a concentric muscle contraction?
muscle shortens during force production
What is an eccentric muscle contraction?
muscle produces force while length increases, associate with fiber damage
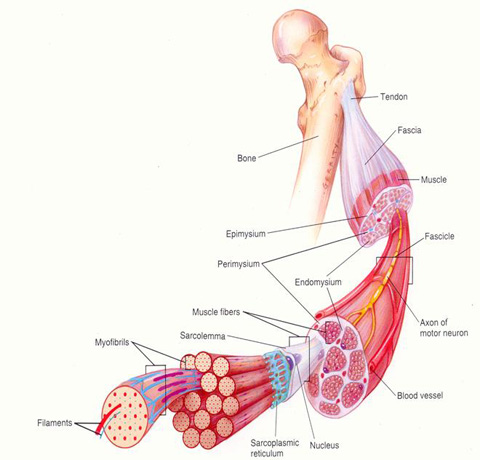
What is epimysium?
the CT layer that surrounds an entire muscle
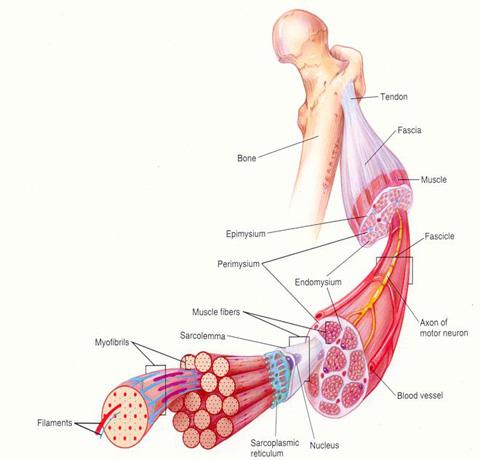
What’s fascia?
a tough CT layer that is broad and can cover multiple muscles
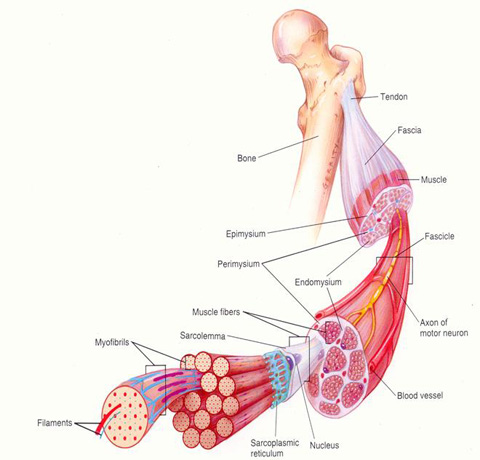
WHat’s perimysium?
the CT layer that surrounds bundles of muscle fibers (fascicles)
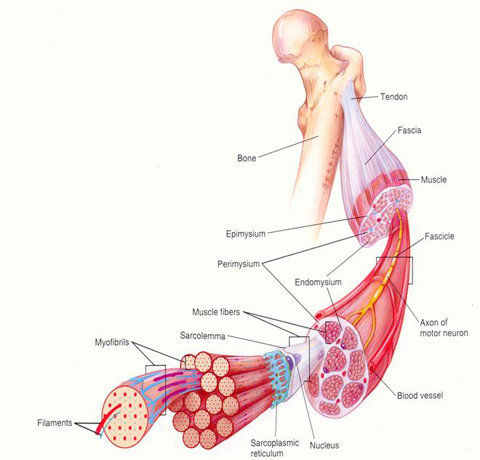
What’s endomysium?
CT layer that surrounds individual muscle fibers
What is the sarcolema?
muscle cell membrane
What’s a sarcoplasm?
the cytoplasm of a muscle fiber
What do satellite cells do?
play a role in muscle growth and repair by increasing the number of nuclei
What is a myonuclear domain?
The region of cytoplasm controlled by a single nucleus in a muscle fiber
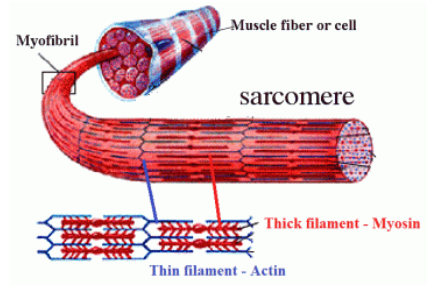
What is a myofibril?
repeating segments of sarcomere which make up a muscle fiber
What are the two contractile proteins of myofibrils?
actin (thin filament) and myosin (thick filament)
What is a sarcomere?
the basic contractile unit of a muscle, includes a Z line, M line, H zone, A band, I band, and another Z line
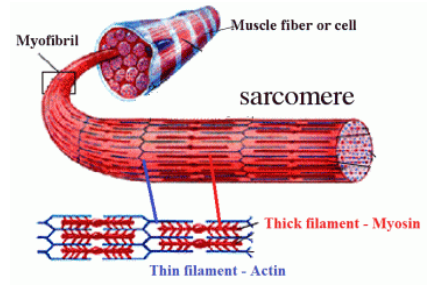
What is myosin?
thick filament which interacts with actin on myosin heads
What is nebulin?
a protein that binds actin and controls it’s length
What is titin?
elastic protein that connects z discs to the M-line and is responsible for muscle stiffness/elasticity
What’s tropomyosin?
blocks actin-myosin interaction
What is troponin?
part of actin which binds to Ca++
What is the importance of the SR?
intramuscular storage cite for calcium which releases it during contraction
What are t-tubules?
tubes that extend from the sarcolemma to the SR, which allow and action potential to propagate deep into muscle fibers
In general, what is characteristic of type IIa muscle fibers?
an intermediate fiber with both glycolytic and oxidative metabolism, “fast-oxidative glycolytic fibers”, medium red color
In general, what is characteristic of type IIx muscle fibers?
rarely uses for everyday activity, short high intensity exercise, “fast-glycolytic fibers”, lightest white color
In general, what’s characteristic of type I muscle fibers?
high aerobic metabolism for endurance, “slow-oxidative fibers”, darkest red color
What defines maximal muscle fiber force production?
force per unit of cross-sectional area
What is muscle fiber contraction speed (Vmax) dependent on?
myosin ATPase activity
What’s the relative number of mitochondria for Type IIx fast glycolytic fibers?
low: fully glycolytic so no aerobic capacity
What’s the relative number of mitochondria for Type IIa fast-oxidative glycolytic fibers?
moderate to high: mix of both energy systems
What’s the relative number of mitochondria for Type I slow oxidative fibers?
high: slow endurance fibers, purely aerobic metabolism
What’s the fatigue resistance in Type IIx muscle fibers?
low: max explosive/force fibers, not sustainable
What’s the fatigue resistance in Type IIa fibers?
moderate-high
What’s the fatigue resistance in Type I fibers?
high: long endurance aerobic fibers
What’s the predominant energy system for Type IIx fibers?
anaerobic (glycolysis)
What’s the predominant energy system for Type IIa fibers?
mix of aerobic/anaerobic metabolism
What’s the predominant energy system for Type I fibers?
aerobic oxidative phosphorylation
What’s the relative ATPase activity (correlates to shortening velocity) for Type IIx fibers?
highest: fastest contractions, most powerful
What’s the relative ATPase activity (correlates to shortening velocity) for Type IIa fibers?
high
What’s the relative ATPase activity (correlates to shortening velocity) for Type I fibers?
low: slowest fiber type, least powerful
What is the relative efficiency (ability to use Fat/CHO for fuel) of Type IIx fibers?
low: minimal fat oxidation, almost purely glycolysis to produce fast ATP
What is the relative efficiency (ability to use Fat/CHO for fuel) of Type IIa fibers?
moderate: can use both based on intensity of ex
What is the relative efficiency (ability to use Fat/CHO for fuel) of Type I fibers?
high: able to fully oxidize fat and highly efficient at utilizing O2
What is the capillary density for Type Iix fibers?
low: anaerobic
What is the capillary density for Type IIa fibers?
moderate
What is the capillary density for Type I fibers?
high
What’s the myoglobin content for Type IIx fibers?
low
What’s the myoglobin content for Type IIa fibers?
moderate
What’s the myoglobin content for Type I fibers?
high
What’s an example of an activity that relies heavily on Type IIx fibers?
max effort sprint 30-60m, 1-3 RM Lift
What’s an example of an activity that relies heavily on Type IIa fibers?
800m–1500m run or tempo intervals (e.g., 3–5 min hard efforts)
What’s an example of an activity that relies heavily on Type I fibers?
long distance steady state easy pace running (eg: 45-90min)
What is fatigue?
the inability to maintain power output or force during repeated muscle contractions
What are the major divisions of fatigue?
central fatigue and peripheral fatigue
What’s central fatigue?
fatigue of the central nervous system
What is peripheral fatigue due to?
neural factors, mechanical factors, energetics of contraction
What are the 5 major causes of fatigue?
energy delivery, elevated temp, lactate/H+ accumulation, failure of muscle’s contractile mechanism, alteration in the nervous system
What are the 3 areas of fatigue within the body’s energy systems?
PCr depletion, decline in blood glucose, glycogen depletion
Name some signs of hypoglycemia (blood glucose <45 mg/dl)?
shakiness, dizziness, sweating, hunger, headache, fatigue, pale skin, mood changes, decrease in performance
What is meant by “running out of glycogen”?
depletion of muscle glycogen stores which reduces ATP production and decreases performance
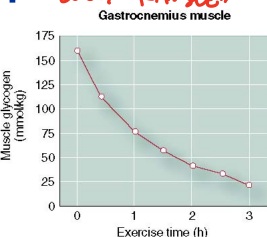
How is glycogen depletion selective?
only muscles that are actively involved in exercise experience lots of glycogen depletion (local fatigue)
What’s the role of lIver glycogen during exercise?
helps maintain blood glucose levels
How does liver glycogen depletion affect muscle glycogen utilization?
once liver glycogen stores decrease, muscle rely more on their own glycogen stores, thus increasing the use of muscle glycogen
What is the key enzyme responsible for muscle glycogen breakdown during exercise?
phosphorylase
What extracellular factor influences muscle glycogen breakdown?
increases epinephrine in response to exercise which forms cyclic AMP which activates phosphorylase
What intercellular factors influence muscle glycogen breakdown?
increased levels of intercellular calcium from the SR which activate calmodulin which in turn activates phosphorylase
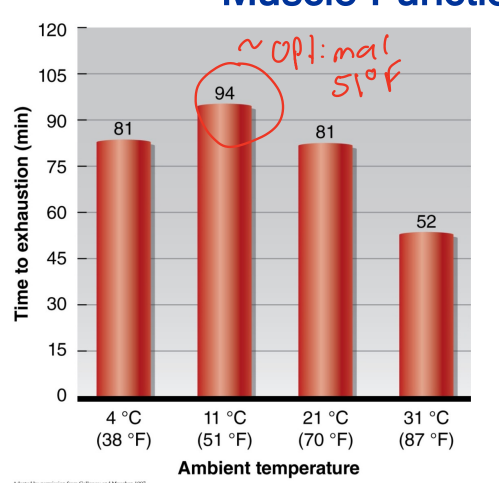
Describe the relationship between heat and fatigue?
there is an optimal temp for exercise (~51F ambient temp) slightly higher than body temp which aids in enzyme activity, contractile function, and nerve conduction. heat also leads to faster dehydration and therefore decreased blood plasma volume which has negative impacts on the CV system
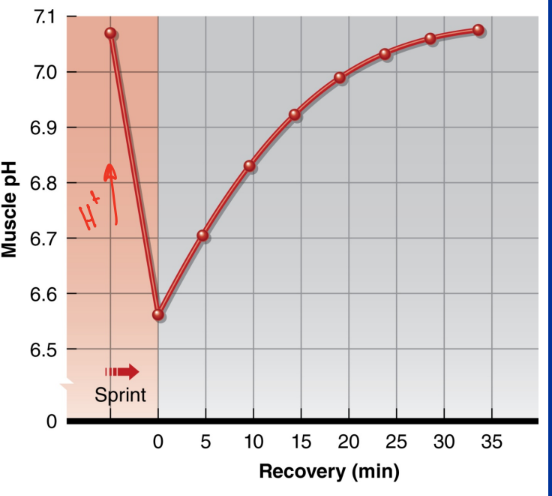
What is the effect of low pH from metabolic byproducts on fatigue?
H+ inhibits PFK (rate limiting enzyme for glycolysis), interferes with calcium binding to troponin, interferes with calcium reuptake
How does ACh contribute to neuromuscular fatigue?
Neuromuscular fatigue occurs when ACh signaling is disrupted. This can happen if less ACh is released from the motor neuron, if ACh is broken down too quickly by acetylcholinesterase, or if receptors are blocked
How do membrane excitability and potassium contribute to neuromuscular fatigue?
potassium can leave the intracellular space and decrease membrane potential below resting values, making it harder to depolarize the muscle
What is central fatigue in neuromuscular fatigue?
reduction in neural drive from the central nervous system that limits motor unit recruitment and force production
What is direct calorimetry?
a way to measure energy expenditure through body heat production (substrate production)
What’s indirect calorimetry?
a way to measure energy expenditure from the ratio of CO2 produced to O2 consumed
What are a couple other ways of calculating energy expenditure?
Carbon13 and Doubly labeled water
What’s the energy requirements/O2 consumption at rest?
100% aerobic metabolism, 0.25 L/min, 3.5 ml/kg/min, 1 MET
What is RMR?
minimum amount of energy required by the body to sustain basic cellular function
What 3 things make up TEE?
RMR, Thermic Affect of Food, Physical Activity
How does age affect RMR?
gradually decreases mainly due to less fat-free mass (muscle)
How does body temp affect RMR?
increases with increasing body temp
How does stress increase RMR?
stress activates sympathetic nervous system which increases RMR
How do hormones affect RMR?
thyroxine from thyroid and epinephrine both increase RMR
In general, hoe does body surface area affect RMR?
linear increase