Lecture 17. Infections of the Urogenital System 5
1/40
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
41 Terms
what is a UTI
bacterial colonization urine or any urinary tract organ (except distal urethra)
UTIs
what disease can this pathogen cause
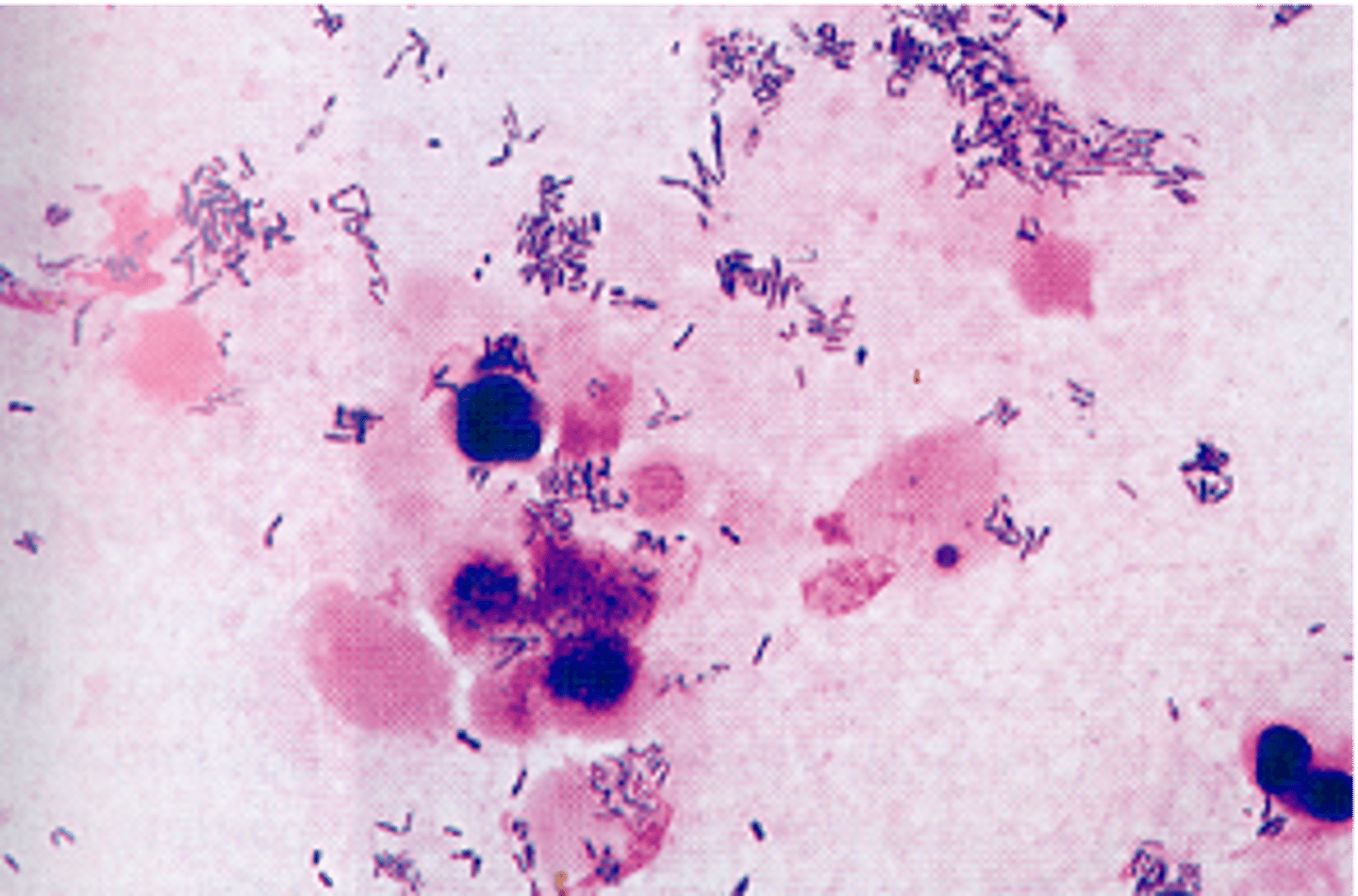
what gram negative rod bacteria is urease negative
E. coli
what gram negative coccobacilli is rapid urease positive
Proteus spp.
what gram negative small rod is delayed urease positive
Klebsiella spp. (think a kurb causes a delay in traffic)
what gram positive cocci in bunches is urease positive
(looks like grape clusters P fror positive and purple)
Staphylococcus spp.
what gram positive cocci in chains is urease negative
(think strep like stretched out)
Streptococcus spp.
what is the primary pathogen involved with canine UTIs
E. coli, proteus, klebsiella
what is the primary pathogen found in cats with UTI
E. coli, Proteus, Staphylococcus aureus, Pasteurella multocida
what are the most common species found in horse UTIs
E. coli, Staphylococcus aureus, Streptococcus
what are the most common species found in cattle/sheep/goats UTIs
E. coli, Trueperella pyogens, and Corynebacterium spp.
UTI pathogens are typically a normal flora of the lower UT and are considered...
opportunistic infections
what determines the outcome of a UTI
virulence factors and host defense
what is the most common method of entry for a UTI
ascension into the urethra
what are some of the host defenses against UTIs
1. urine flow (number 1)
2. anti-adherence mechanisms
what is the role of the urinary oligosaccharide anti-adherence mechanism
coat bacteria to prevent receptor binding
what is the role of the bladder glycosaminoglycan anti-adherence mechanism
coat transitional epi
what is the role of the epithelial cell exfoliation anti-adherence mechanism
removed even if they bind
what is the role of the urine osmolality anti-adherence mechanism
bacteriostatic effects
what conditions can decrease urine osmolality
renal failure, cushing's, diabetes mellitus
what are some of the risks for host defense mechanisms
urinary stasis, foreign body, epi surface damage, and pressure from uterus during gestation
what are the C/s associated with UTI
1. pollakiuria (increased frequency)
2.stranguria (straining to urinate)
3. dysuria (irregular urination)
what is the most common rule out of dysuria
urethrocystitis
what can recurrent cystitis lead to
PN or prostatitis
what are the main ways to Dx. UTIs
1. urinalysis
2. quantitative culture
what is observed on urinalysis that indicates a UTI
1. PE: red/brown, turbid, foul odor
2. chemical: protein (+), glucose (+), occult blood, acidic pH
3. microscopic bacteria + pyuria
red/brown urine
what c/s is shown to indicate UTIs

turbid w/ leukocytes/bacteria/crystals
what c/s is shown to indicate UTIs

what is the best way to collect urine for a culture
cystocentesis
why is catheterization not an ideal way to collect urine for a culture
risk of contamination
a culture showing >100,000/mL w/ signs likely indicates...
UTI
a culture showing <1,000/mL likely indicates...
contamination
what does culture interpretation include
species (multiple = contamination), numbers, consistent urinalysis results
what pathology is associated with UTIs
hematuria, pyuria, bacteriuria
when it comes to antibiotic selection...
antibx. sensitivity may not reflect susceptibility in UT
since the urinary tract is a conditionally susceptible site antibiotics must be...
concentrated
how often do antibiotics have to be given for UTIs
10-14 days
when administering antibiotics it is important to consider...
toxicity
when treating UTIs w/ antibiotics it is important to...
re-culture @48hrs to check for bacteria growth
if antibiotics fail to treat UTIs, it can lead to recurrent cystitis due to...
1. relapse: infection w/ same organism
2. reinfection: infection w/ new organism
in a case of chronic bacterial cystitis antibiotics may be needed...
4-6wks and recultured @48hrs and every 6mo till 24mo