Unit 2: ICR
1/34
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
35 Terms
Cerebral Perfusion Pressure
pressure needed to ensure blood flow, oxygen, and nutrients to the brain
cerebral perfusion pressure is impacted by….
Increased ICP
pushes on the blood vessels in the brain, limiting/constricting blood flow and oxygen and nutrient supply to the brain
increased ICP → reduces CPP & leads to tissue and brain ischemia, leading to brain tissue death
How does autoregulation help maintain constant cerebral perfusion pressure?
increased ICP → vasodilation to increase cerebral blood flow to deliver oxygen to brain tissues (can also exacerbate and contribute to increasing ICP)
decreased ICP → vasoconstriction of cerebral blood vessels to decrease cerebral blood flow
hypoxia & hypercapnia → leads to vasodilation to increase cerebral blood flow
hypocapnia → causes vasoconstriction; decreases cerebral blood flow
overcompensation can cause cerebral edema & contribute to increased ICP
level of consciousness
pt is aware of self and the environment; is able to respond appropriately to stimuli
mental status
assessment of pt’s cognitive, affective, and behavioral state
have to be conscious and awake first in order to assess mental status
cognition includes:
thought processes
memory
perception
communication
problem solving
emotion
what can loss of autoregulation lead to?
Cushing’s Triad
s/s of cushing’s triad
systolic hypertension where there is a large difference between the systolic and diastolic pressure
low HR with bounding pulse
irregular/decreased RR
s/s of ICP
weakness
lethargy
headaches
vomiting
blurred vision
changes in behavior
purpose of treatment for increased ICP
to decrease ICP and restore blood flow
effects of impaired ICP
elevated ICP leads to the brain being compressed d/t increased blood flow/injury/trauma/mass
leads to herniation risk
effects of impaired cerebral perfusion
limited blood flow to brain tissue can lead to brain ischemia and tissue damage
effects of impaired neuronal integrity
caused by damaged or inflamed neurons from trauma, infection, stroke, or neurodegenerative diseases
effects of impaired neuro-transmission
disrupted neurotransmitter release or uptake, leading to issues like seizures or impaired cognition.
effects of impaired cerebral metabolism
hypoxia, hypercapnia, or hypoglycemia can lead to energy deficits, neuronal damage, or brain cell death.
3 direct consequences of impaired ICR
Herniation or displacement of brain tissue due to severe increased intracranial pressure
Permanent physical, cognitive, or psychological disabilities due to cellular damage
Brain death or systemic failure due to severe intracranial dysregulation.
5 functional consequences of impaired ICR
consciousness → decreased LOC, coma
motor control → motor deficits, speech & language impairment
sensory processing → sensory deficits, vision & hearing loss
cognitive functions → altered mental status, impaired memory, impaired thought process
autonomic functions → dysregulation of HR, BP, temp, and RR
assessing LOC
assess for:
level of alertness
response to stimuli (AVPU)
concerning cues during a LOC assessment
sudden change in LOC; early sign of impaired ICR
assessing cognitive function
assess for:
level of orientation
memory
concerning cues during a cognitive function assessment
disorientation
confusion
forgetfulness
concerning cues during a vision assessment
blurred vision
loss of vision
papilledema
impaired eye movement
assessing language function
assess for:
communicating speech
understanding speech
concerning cues during a language function assessment
slurred speech (dysarthria)
aphasia (no speech)
incoherent speech
assessing pupils (reflexes)
assess for:
PERLA
concerning cues during a pupil assessment
unequal pupil size *late sign for impaired ICR
assessing sensory function
assess for:
sensation in the extremities
concerning cues during a sensory function assessment
numbness
tingling
loss of sensation
assessing motor function
assess for:
strength
coordination
concerning cues during a motor function assessment
weakness
paralysis
discoordination (ataxia)
assessing autonomic function
assess for:
heart
lungs
BP
concerning cues during an autonomic function assessment
irregular respirations
vomiting (esp. w/o nausea)
hypertension with bradycardia (indicates cushing’s triad; *late sign)
Babinski reflex
Positive = dorsiflexion of the big toe and fanning of the other toes when the lateral aspect of the sole of the foot is stroked
in infants/newborns → normal
abnormal in those >2 years old
in adults → concerning; indicates damage to CNS
decorticate
flexed, indicates damage to the cerebral cortex
indicates severe brain damage
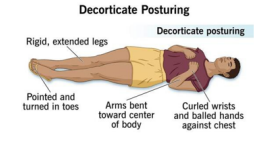
decerebrate
extended, more severe, indicates damage to the midbrain or lower brainstem
indicates severe brain damage
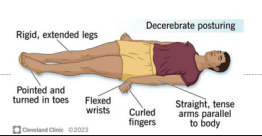
interventions to prevent increasing ICP
monitor VS; look for s/s of Cushing’s Triad
monitor LOC
I/Os - limit fluid intake
reduce stimuli + promote energy conservation + reduce brain metabolism
raise HOB 30-40 degrees
initiate seizure precautions
avoid valsalva maneuvers (ie. coughing, sneezing, straining (like pooping))
monitor ICP/CCP