17 - liver symposium
1/67
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
68 Terms
what are the enteric hepatitis'
A and E
what are the parenteral hepatitis'
B, C and D
what are the self limiting acute hepatitis'
A and E
what hepatitis' cause chronic disease
B, C, D
what is the only DNA hepatitis
hepatits B
transmission of hep A
faecal oral
what hepatitis' are the only ones with a vaccine available
A and B
treatment of hepatitis A
supportive - self limiting acute virus
hepatitis B transmission
blood and body fluids
treatment of hepatitis B
antivirals (NOT curative)
supportive
transmission of hepatitis C
bloodborne
treatment of hepatitis C
direct acting antivirals
transmission of hepatitis D
alongside hep B
treatment of hep D
pegylated interferon alpha
hepatits E transmission
faecal oral
treatment of hepatitis E
supportive - self limiting same as A
what can hepatitis A cause
cholestasis
pruritis
significant jaundice
flu like symptoms
nausea and vomiting
dark urine
pale stool
Is hepatitis A acute or chronic?
acute
is hepatitis A symptomatic or asymptomatic
asymptomatic (especially in children) but can cause symptoms
what is diagnosis of hepatitis A based on
IgM antibodies
what is a rare complication of hepatitis A
acute liver failure (fulminant hepatitis)
how does vertical transmission occur in hepatitis B
infection passed on from mother to child during childbirth
- most children recover within 2 months
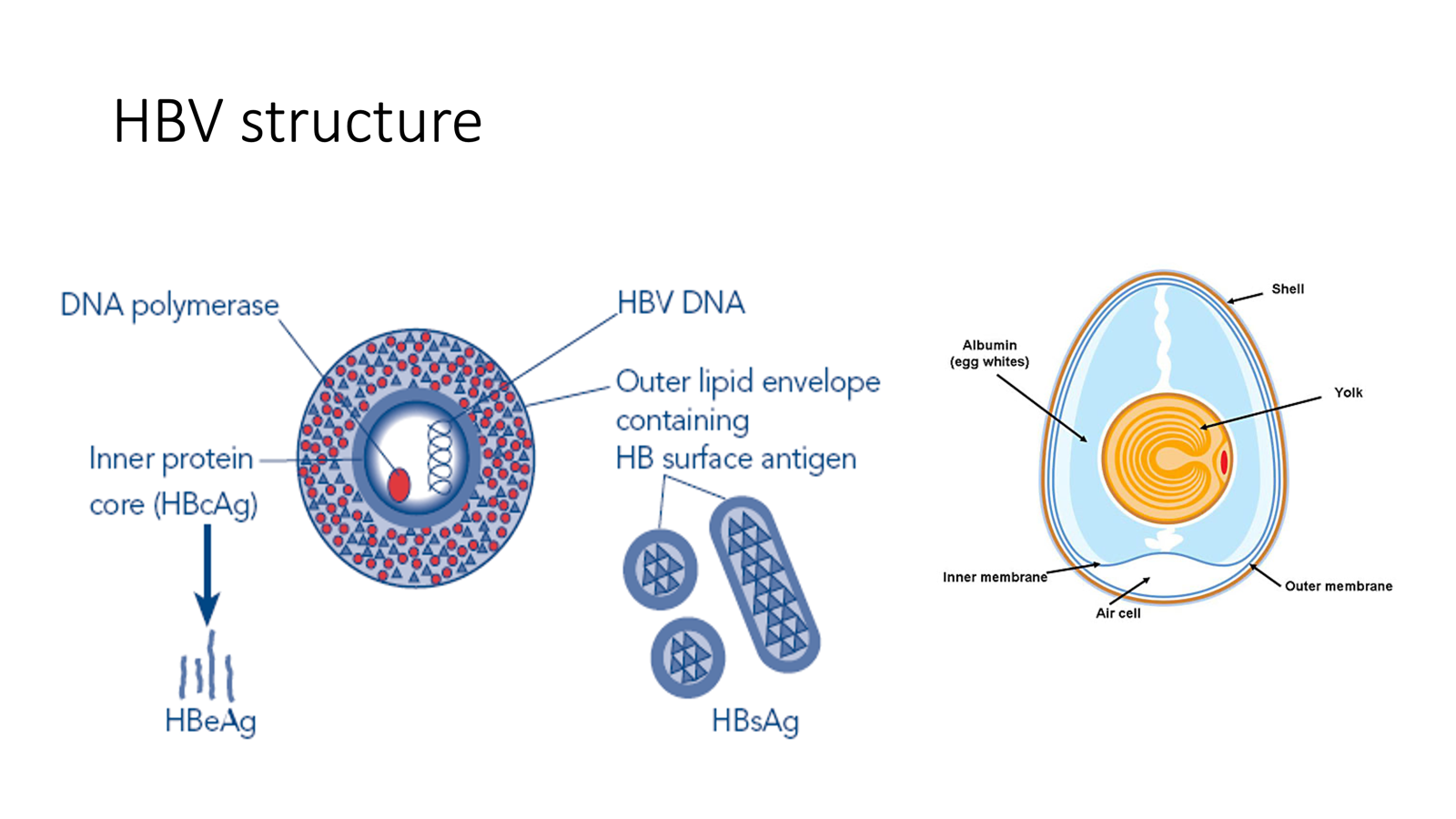
what is the hepatitis B structure
HBV DNA
outer lipid envelope with antigens (HBsAg)
inner protein core (HBeAg)
DNA polymerase
markers of hep B (Ag)
- HBsAg indicates....
active infection
Hepatitis B surface antigen
markers of hep B (Ag)
- E antigen HBeAg
marker of viral replication - high infectivity
markers of hep B (Ab)
- HBcAb
Hepatitis B core antibody
past or current infection
markers of hep B (Ab)
- IgM high titre
ACUTE
IgM low titre in hep B
chronic
markers of hep B (Ab)
- IgG
CHRONIC or past infection if HBsAg is negative
markers of hep B (Ab)
- HBsAb
Hepatitis B surface antibody
implies vaccination OR past infection
HBV DNA
indicates active replication of virus, direct count of viral load
- used for monitoring treatment
what is done if there is a hep B positive mother and you want to reduce the risk of the baby contracting Hep B at birth
neonates are given
- hep B vaccine
- hep B immunoglobulin infusion
MUST BE DONE WITHIN 24 HOURS
pathway of chronic hepatitis B
acute turns chronic
normal liver
- 2 pathways
1. no further progression
2. cirrhosis
cirrhosis can develop into HCC or end stage liver disease
treatment options for hepatitis B
oral antivirals
pegylated interferon
complications of hepatitis C
liver cirrhosis
HCC
when do symptoms appear in hepatitis C
when it develops to cirrhosis
what is the problem with vertical transmission of hep C
antivirals are unsafe in pregnancy and there are no additional measures such as vaccination to reduce risk of transmission
hep C testing
Anti-HCV, HCV RNA to confirm diagnosis
- calculate viral load
- identify genotype
how does hepatitis D survive in patients
patients who have a hep B infection as D is attached to HBsAg
what is the problem with hepatitis D in terms of hep B
increased complications and severity of hep B
treatment regime of hepatitis D
pegylated interferon alpha over 48 WEEKS
what is the issue with pegylated interferon alpha
not very effective and significant side effects
what can drugs cause in terms of drug induced liver disease
toxic necrosis
acute hepatitis
chronic hepatits
cholestasis
mixed pattern hepatocellular/cholestasis
hepatic vein thrombosis
veno-occlusion disease
steatosis
granulomatous hepatitis
what is the antidote for paracetamol
N-acetylcysteine (NAC)
standard administration of NAC
3 stage IV infusion
- 150mg/kg over 1 hour
- 50mg/kg over 4 hours
- 100mg/kg over 16 hours
characteristics of NAFLD
excessive fat in liver cells esp triglycerides interfering with function
4 stages of NAFLD
NAFLD
non alcoholic steatohepatitis (NASH)
fibrosis
cirrhosis
risk factors for NAFLD
middle age
obesity
poor idet
low activity
type 2 diabetes
high cholesterol
HTN
smoking
investigations for NAFLD
LFTs
liver ultrasound
enhanced liver fibrosis blood test
NAFLD fibrosis score
FIB-4 score
transient elastography (fibroscan)
liver biopsy - GOLD STANDARD, tells extent of steatosis and if fibrosis or no fibrosis
LFTs findings in NAFLD
raised AST - 1st indication
ultrasound findings in NAFLD
hepatic steatosis - increased echogenicity
what is the first line investigation or assessing fibrosis in NAFLD
enhanced liver fibrosis blood test
markers in enhanced liver fibrosis blood test
HA
PIIINP
TIMP-1
10.51 or more in enhanced liver fibrosis blood test
ADVACNED fibrosis
under 10.51 in ehanced liver fibrosis test
fibrosis unlikely - check every 3 years
low risk fibrosis points on NAFLD fibrosis score
<45yo
no diabetes
BMI <30
AST:ALT <1
platelet count >150 normal
albumin normal >34
high risk fibrosis points on NAFLD fibrosis score
>45yo
diabetic
BM >30
AST:ALT >1
low platelet count <150
low albumin <34
FIB-4 score <1.45
no advanced cirrhosis
FIB-4 score >3.25
cirrhosis
How is FIB-4 calculated?
age (years) x AST/platelet count x square root ALT
what does an AST:ALT ratio greater than 1.5 suggest
alcoholic liver disease
treatment of NAFLD
weight loss
healthy diet
exercise
avoid/limit alcohol
stop smoking
control diabetes, BP and cholesterol
refer patients with advanced fibrosis to specialists
specialist treatment of NAFLD
bariatric surgery
liver transplant
vitamin E
pioglitazone
tests of liver disease
cytokeratin-18 - elevated CK18 levels correlate with the severity and progression of NAFLD and NASH.
fibroscan - diagnoses scarring
MR/CT
MR spectroscopy - quanitfy fat
medication for autoimmune hepatitis
long term azathioprine
medication for primary biliary cholangitis
UDCA (Ursodeoxycholic acid) treatment of choice
treatment for primary sclerosing cholangitis
liver transplant
biliary stents
When is liver transplant given
chronic liver disease with poor survival
chronic liver disease with poor quality of life
hepatocellular carcinoma
acute liver failure
genetic diseases