Unit 3: Lymphatic System
1/61
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
62 Terms
what is the function of the lymphatic system?
three primary functions: maintain fluid balance in the tissues, transport absorbed fat from the small intestine to the blood, and protect the body from infection and disease (working in close association with the venous system but still separate and unique)
what is the direction of fluid flow in the lymphatic system, and where are lymphatics located?
flows from the peripheral to the central system, located throughout the body except for the CNS and avascularized tissues slightly more superficially than the veins
how much of the fluid volume that perfuses tissues is returned to the heart via the lymphatic system?
10%, since 90% is reabsorbed with venous capillary network
what is the interstitial space?
The interstitial space is the area between cells in tissues that contains interstitial fluid, providing a medium for the exchange of nutrients and waste between blood vessels and cells.
what is the function of the lymph nodes?
filter, trap, and hold bacteria, cancer cells, and large protein molecules, produces lymphocytes, purify and thicken the lymph before it enters the blood stream, and is places alongside the inside of the lymph vessels
how many lymph nodes does the body have in total?
600-700
what structures are involved in the lymphatic system?
superficial and deep lymph vessels and nodes, bone marrow, thymus, spleen, tonsils, peyer patches in the small intestine, and lymph fluid (should be clear ideally)
what is the pathway of lymph through the lymphatic vessels?
start at the lymph capillaries to the precollectors, to the lymph collectors, to the lymph nodes, to the lymph trunks, to the thoracic and R lymphatic duct, and then re-enters the blood (mostly through the veins)
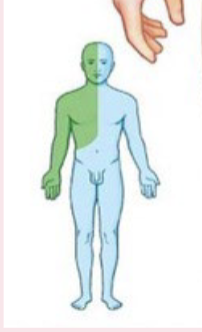
which duct is responsible for drainage of the green area, and which is responsible for the blue area?
green is drained by the R lymphatic duct, and the blue is by the thoracic duct
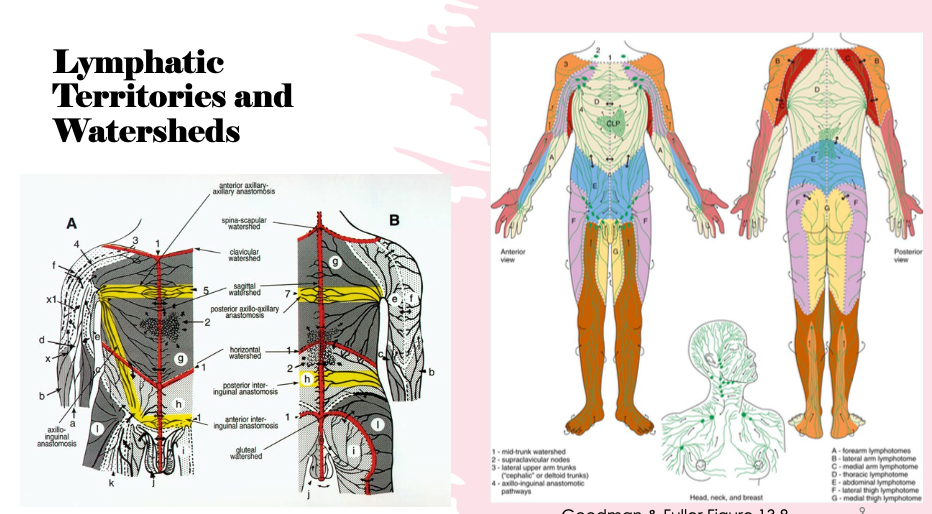
what are the lymphatic territories versus the watersheds?
Lymphatic territories refer to distinct areas of lymphatic drainage in the body, while watersheds are the linear boundaries that separate these territories, serving as areas where lymph flow is re-routed or redistributed.(in image watersheds are on the left and territories on the right)
what concepts are involved in fluid dynamics of the lymphatic system?
pressure driven system based on principles of osmotic diuresis, laws of basic fluid dynamics, and starling’s law
what is the transport capacity?
TC is the total workload of the system
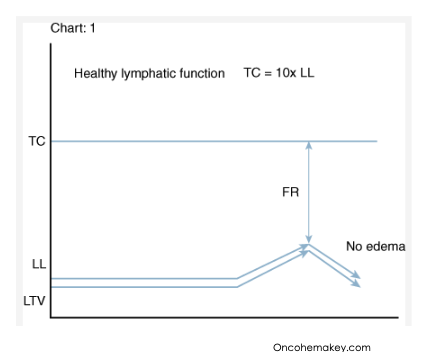
what is the lymphatic load (LL)?
The lymphatic load (LL) refers to the total amount of fluid, proteins, and cells that must be transported by the lymphatic system from the interstitial space to the bloodstream.
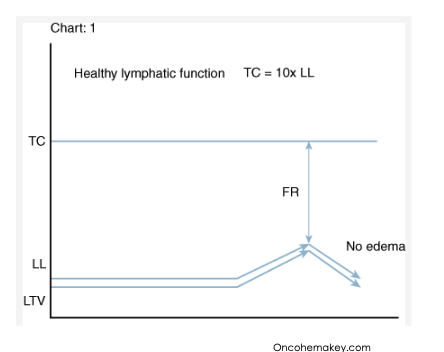
what is the lymph time volume?
amplitude and frequency of intrinsic contractions
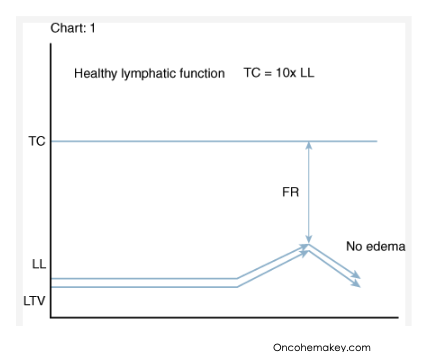
what is the functional reserve?
difference between TC and LL
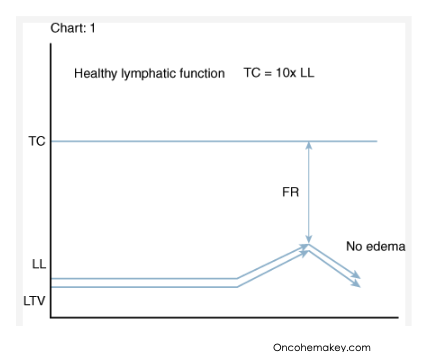
what is dynamic instability
TC (transport capacity) is normal, no FR (functional reserve), LL (lymphatic load) exceeds the TC, and TC = max LTV (see venous edema)
what is mechanical insufficiency?
TC reduced, no FR, LL exceeds TC, and TC = max LTV (leads to lymphedema)
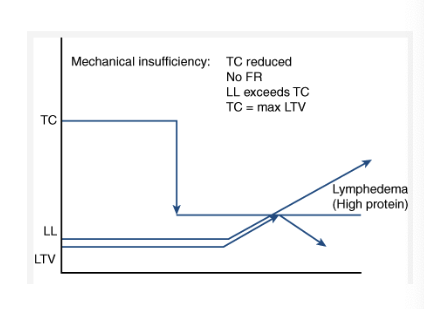
what type of insufficiency is demonstrated by the image?
mechanical insufficiency
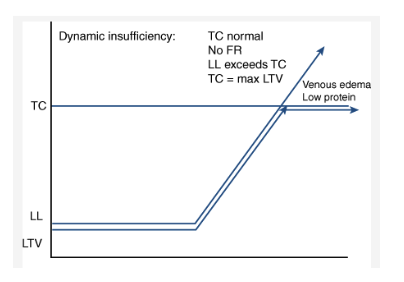
what type of insufficiency is demonstrated by the image?
dynamic insufficiency
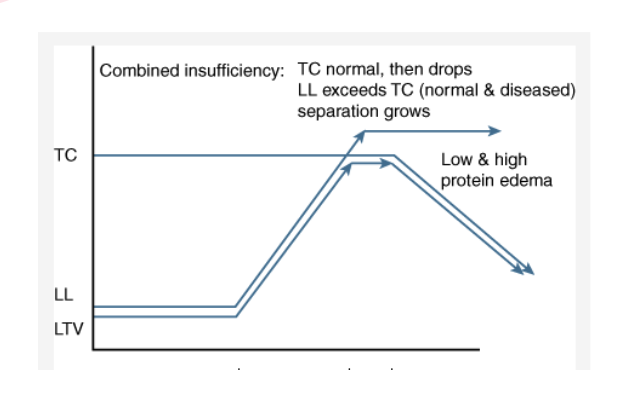
what is combined insufficiency?
when the TC is normal but then drops, LL exceeds the TC (normal then drops) and separation grows, see low and high protein edema
what is edema?
excess levels of interstitial fluid accumulation, low protein swelling, dynamic insufficiency. is a symptom that can be caused by several conditions such as CHF, venous insufficiency, immobility, pregnancy, trauma, may affect the whole body or certain parts (generalized or localized)
what is lymphedema?
swelling of the soft tissues resulting from the accumulation of protein rich fluid (lymph), a disease where components of lymphatic system are not function sufficiently, is mechanical insufficiency, most commonly is seen in the extremities but can be seen in the head, neck, abdomen and genitalia
what is lymphangitis ?
inflammation of a lymphatic vessel
what is lymphadenitis?
inflammation of one or more lymph nodes
what is lymphadenopathy?
enlargement of the lymph node (s)
how is lymphedema classified?
primary (idopathic) or secondary (acquired)
what are some causes of primary lymphedema?
may be unknown. hereditary, developmental abnormality, aplasia, hypolasia, hyperplasia
what are secondary lymphedema causes?
filariasis, surgery, trauma, chronic venous insufficiency, immobility, infection, primary or metastatic neoplasm, obesity, medication, lipedema, paralysis, HIV/AIDS
what is filariasis?
the #1 cause of secondary lymphedema world wise, caused by a parasitic infection spread by infections
what is the most common cause of secondary lymphedema in the US?
cancer surgery and radiation
epidemiology of lymphedema?
affects approx 10 million people in the US, about 6-70% of patients with breast cancer, and there is a higher risk with lymph removal and increased BMI (23% of patients with gynecologic cancer and 34% of men after prostate cancer)
populations at risk of lymphedema?
populations undergoing treatment for malignancy (mastectomy, chemotherapy, radiation), and prior medical history (trauma to the affected limb or infections in the affected limb)
what is the stage 0 of lymphedema?
no swelling but subjective complaints, reduced TC yet remains sufficiency to manage normal LL
what is the stage 1 of lymphedema?
considered reversible/fluctuating, see soft pitting edema, elevation reduces swelling, and increases with activity, heat, and humidity
what is stage 2 lyphedema?
spontaneously irreversible: non-pitting edema, moderate changes to severe swelling skin changes that alter the texture (lumps, fibrosis), and symptoms can be managed but not cured
what is stage 3 lymphedema?
severe, non-pitting fibrotic edema, severe skin changes (hardening, deep skin folds, skin papillomas, etc), elephantiasis
when might people get head and neck lymphedema and what might it look like?
head and neck tumors, tonsillectomies, see image

what are evidence based predictors of breast cancer related lymphedema?
extent of the axillary dissection, BMI over 25, seroma, regional node radiation, post-surgical infection (lymphangitis)
what are probable/possible predictors of breast cancer related lymphedema?
when greater than 5 nodes are removed, taxane chemotherapy after surgery, inactivty, genetic and physiological predisposition
what is the clinical presentation of lymphedema?
see asymmetry, swelling distal to or adjacent to the area, pitting edema early on, non-pitting lateral stages, fibrotic changes in the dermis, dermal abnormalities, increased susceptibility to infection, loss of mobility and ROM, and impaired wound healing
what are the symptoms of lymphedema?
feelings of fatigue, heaviness, pressure, or tightness in the affected region, numbness and tingling, discomfort or pain varying from mild to intense, decrease flexibility, clothing and jewelry are tight
how can lymphedema be diagnosed?
since there is no gold standard diagnostic criterion, diagnosed clinically: diagnosis of exclusion so make sure to exclude everything it isn’t first! take a thorough history, signs and symptoms with systems review, lymphatic system damage or deformity, may or may not need imaging (lymphography, doppler/duplex ultrasound, MRI, CT scan)
what the Stemmer sign?
used to test for lymphedema, observing for skin fold thickness on the second toe or finger. will see inability to pinch the skin at the dorsum of the second toe indictates a positive sign. helps to distinguish lymphedema from other forms of swelling (trauma, renal disease, CHF). will be positive in stage 2 and 3
what other tests and measures can be used to measure for lymphedema?
circumferential measurements (compared between limbs), limb volume measurements, skin elasticity, bioelectric spectroscopy, BMI, sensory integrity, and pain assessment
what are some differential diagnosis for lymphedema?
chronic venous insufficiency, lipedema, cardiac dysfunction, DVT, phlebo-lymphostatic edema, lipo-phlebo-lymphedema, renal impairement, protein imbalances, malignant lymphedema
what is lipedema?
symmetrical swelling of both legs, extending from the hips to the ankles, caused by deports of subcutaneous adipose tissue, fatty bulges in the buttocks, medial proximal and distal thigh, with foot sparing, complain of pitting edema as the day progresses
what are the PT implications of lipedema?
sympomatic relief, improve trunk and LE function
how can lymphedema be treated?
begin ASAP, complete decongestive therapy (CDT) is the gold standard, goal is to control and reduce swelling, prevent progression, and improve QOL (done is phases)
what is done in Phase 1 of Lymphedema treatment?
decongestion: see manual lymphatic drainage, multilater/compression bandages, remedial exercises, skin and nail care, limb elevation, self care education, usually daily treatments and see average of 2-3 weeks for UE and 2-4 for LE but will depend on the pt
what is done in phase 2 of lymphedema treatment?
maintenance and homecare phase, use of garments, bandaging, exercise, skin and nail hygeine, self-MLD, follow up with certified lymphedema therapist
what is manual lymph drainage?
A specialized massage technique used to stimulate lymphatic flow (Vodder technique), reduce swelling, and promote relaxation. gentle, light, lower pressure slow massage that starts distally, repetitive and rhythmic, stimulates the lymph vessels by providing mild mechanical stretches on the wall of the lymph
describe compression bandaging for lymphedema
a method that uses elastic bandages to apply consistent pressure on affected areas, helping to reduce swelling and promote lymphatic drainage. Short stretch compression bandages have low resting pressure to exert minimal pressure on the skin but high working pressure to increase lymph uptake and increased pumping of the collecting lymphatics when the muscles are contracting. should have multilayer with padding and sometimes a foam layer to help soften fibrotic/hardened tissue
what are alternative compression tools instead of bandages?
garments, velcro devices, pumps (since bandages are bulky, expensive, and time consuming)
what kinds of exercises will help with lymphedema?
remedial exercises that are slow, low exertion, rhythmic. SHould be performed while in bandages/compression. work the trunk first followed by limb muscles, used DIAPHRAGMATIC breathing and work proximal to distal. These exercises will support lymph flow
what education should be given to patients with lymphedema?
education on long term management, skin assessment and hydration, nail care and hygiene, nutrition, diaphragmatic breathing, self massage and bandaging, infection prevention, garment and bandaging care, emotional support, and remind them to not use BP cuff on affected limbs or to draw blood from those limbs
if a patient is post surgical, what should be considered?
lymphedema education, exercise recommendation and precautions (drain precautions and physician orders), avoid exercises that may strain/stress the incision site
what are the contraindications to CDT? (complete decongestive therapy)
acute DVT, cardiac edema (need cardiac clearance), acute infection, acute bronchitis, malignancies, renal failure
what things may cause poor outcomes with CDT?
malignant lymphedema bc the system is obstructed, morbid obesity, insufficient treatment, associated illnesses, lack of compliance, faulty diagnosis
what are some surgical interventions for lymphedema?
lymphovenous anastamosis surgical procedure, vascularized lymph node transfer, suction assisted protein lipectomy (SAPL) for lipedema, and debulking surgeries tho these are largely ineffective
what is key to reduce risk of chronic lymphedema and to have better outcomes?
prospective surveillance- screen all the at risk patients, baseline girth/volume, questionaries, periodic measurements/interviews, education
what are the barriers to treatment of lymphedema?
insurance, availability of resources, self management or family support, misdiagnosed or misunderstood, prognosis: progressive, lifelong, and no cure
what act made it that medicare now covers lymphedema care?
the lymphedema treatment act (passes in 2023)