Combined Set BOC 7th
1/2239
Earn XP
Description and Tags
everything but lab ops, pls shuffle!
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
2240 Terms
Vasoconstriction is caused by several regulatory molecules, which include:
a. fibrinogen and vWF
b. ADP and EPI
c. thromboxane A2 and serotonin
d. collagen and actomyosin
c. thromboxane A2 and serotonin
Warfarin is classified as a vitamin K antagonist. The factors that are impacted by warfarin therapy are:
a. VIII, IX, and X
b. I, II, V, and VII
c. II, VII, IX, and X
d. II, V, and VII
c. II, VII, IX, and X
When a patient is placed on warfarin therapy, the first factor that will be decreased is:
a. factor II
b. factor V
c. factor VII
d. factor VIII
c. factor VII
A patient with a positive family history of bleeding presents to the ED with the results shown in the table.
The patient is not on any medication and so is likely to be deficient in factor:
a. II
b. V
c. VII
d. VIII
c. VII

Hageman factor (XII) is involved in each of the following reactions except:
a. activation of C1 to C1 esterase
b. activation of plasminogen
c. activation of factor XI
d. transformation of fibrinogen to fibrin
d. transformation of fibrinogen to fibrin
The most potent plasminogen activator in the contact phase of coagulation is:
A. kallikrein
B. streptokinase
C. HMWK
D. fibrinogen
A. kallikrein
The activation of plasminogen to plasmin resulting in the degradation of fibrin occurs by:
a. PAI-1
b. alpha-2 antiplasmin
c. tPA
d. alpha-2 macroglobulin
c. tPA
How does tissue factor pathway inhibitor inhibit coagulation?
a. inhibition of tissue factor-factor VIIa-factor Xa complex
b. conversion of thrombin to prothrombin
c. uncoupling factor XIII dependent crosslinking of fibrin
d. binding and hiding tissue factor on the endothelial surface
a. inhibition of tissue factor-factor VIIa-factor Xa complex
An inhibitor of plasmin activity is:
a. tPA
b. PAI-1
c. alpha-2 antiplasmin
d. plasminogen
c. alpha-2 antiplasmin
Antithrombin inhibits factors:
a. IIa and Xa
b. Va and VIIIa
c. VIIa and XIIa
d. IXa and Va
a. IIa and Xa
The propagation phase of the in vivo coagulation model includes:
a. a final burst of thrombin
b. activation of platelets
c. feedback mechanism to thrombin
d. activation of factor Va and factor VIIIa
a. a final burst of thrombin
In the cell-based model of coagulation the intrinsic pathway operates on the:
a. activated platelet surface to produce the burst of thrombin
b. tissue factor bearing cell to initiate and amplify coagulation
c. proteolytic digestion of fibrinogen
d. activation of the contact pathway
a. activated platelet surface to produce the burst of thrombin
A new oral anticoagulant apixaban has been given to a patient who was previously on warfarin. This drug directly inhibits:
a. vitamin K dependent factors
b. factor IIa
c. factor Xa
d. both factor IIa and Xa
c. factor Xa
The anticoagulant that directly inhibits thrombin is:
a. LMWH
b. argatroban
c. warfarin
d. rivorxaban
b. argatroban
A patient who presents with renal impairment is being started on oral anticoagulant therapy. The DOAC that should be avoided would be:
a. dabigatran
b. apixaban
c. rivaroxaban
d. warfarin
a. dabigatran
In secondary hemostasis, coagulation proteins become activated to form a fibrin clot. Prior to these proteins being activated, their inactive proenzymes are known as:
a. serine proteases
b. cofactors
c. zymogens
d. substrates
c. zymogens
Alpha granules are found on the platelet in the:
a. peripheral zone
b. sol gel zone
c. organelle zone
d. membranes
c. organelle zone
Which of the following best represents the 3 steps of normal hemostasis (in order)?
a. decreased heart rate, adhesion of platelets, plug formation
b. platelet aggregation, formation of FXIII, fibrin plug
c. vasoconstriction, platelet aggregation, fibrin formation
d. vascular damage, stasis, endothelial injury
c. vasoconstriction, platelet aggregation, fibrin formation
Which of the following platelet antigens act as the receptor for collagen?
a. GPIb/V/IX complex
b. GPIIb/IIIa complex
c. GPIa/IIa complex
d. GPIV/X complex
c. GPIa/IIa complex
Which platelet surface antigen acts as the receptor for fibrinogen?
a. GPIb/V/IX
b. GPIIb/IIIa
c. GPIa/IIa
d. GPIc/IIa
b. GPIIb/IIIa
How does GPIb become activated in vivo and in vitro, respectively?
a. shear force, ristocetin
b. ristocetin, compression
c. activation of ADP receptor, ristocetin
d. binding vWF, epinephrine
a. shear force, ristocetin
A patient is on aspirin 100 mg/day to prevent the formation of clots caused by platelets. The mechanism in which aspirin impairs platelet function is by:
a. inactivating cyclooxygenase which blocks thromboxane A2
b. impairs vWF via GPIb/IX/V receptor
c. decreased amounts of arachidonic acid
d. inactivation of ADP and phospholipase A2
a. inactivating cyclooxygenase which blocks thromboxane A2
A patient is diagnosed with a factor V Leiden mutation. The factor V activity level should be:
a. shortened
b. prolonged
c. undetectable
d. within reference range
d. within reference range
The ISI is determined by comparing the PT results of the manufacturer's reagent against:
a. rabbit thromboplastin
b. micronized silica
c. tissue factor
d. human brain thromboplastin
d. human brain thromboplastin
A coagulation reagent should be sensitive to factor deficiencies. A reagent is considered sensitive to a factor when the level of factor activity is approximately:
a. 30%
b. 40%
c. 50%
d. 60%
a. 30%
What factors are considered heat labile?
a. II and IX
b. V and VIII
c. VII and XI
d. X and XII
b. V and VIII
What factors serves as a carrier for factor VIII?
a. factor V
b. factor IX
c. tissue factor
d. von Wililebrand factor
d. von Wililebrand factor
Patients may present with either a bleeding or thrombotic event in"
a. dysfibrinogenemia
b. hypofibrinogenemia
c. afibrinogenemia
d. hyperfibrinogenemia
a. dysfibrinogenemia
The key enzyme of the fibrinolytic system is:
a. plasmin
b. thrombin
c. urokinase
d. strptokinase
a. plasmin
The major serine protease responsible for clot breakdown is:
a. TPA
b. alpha 2 antiplasmin
c. streptokinase
d. PAI-1
a. TPA
What subendothelial structural protein triggers coagulation through activation of factor VII?
a. thrombomodulin
b. nitric oxide
c. tissue factor
d. silica
c. tissue factor
Protein C and its cofactor protein S proteolytically inactivate factors:
a. IIa and Xa
b. Va and VIIIa
c. VIIIa and IXa
d. XIa and XIIa
b. Va and VIIIa
Arterial thrombosis is caused by:
a. RBC & platelets
b. fibrin & WBC
c. thrombin & FXIII
d. WBC & platelets
d. WBC & platelets
The 2 factors that differentiate liver disease from vitamin K deficiency are:
a. II and VII
b. IX and VII
c. VIII and IX
d. V and VII
d. V and VII
In a patient diagnosed with liver disease, which one of the following factors typically shows an increase?
a. factor VII
b. factor VIII
c. factor IX
d. factor X
b. factor VIII
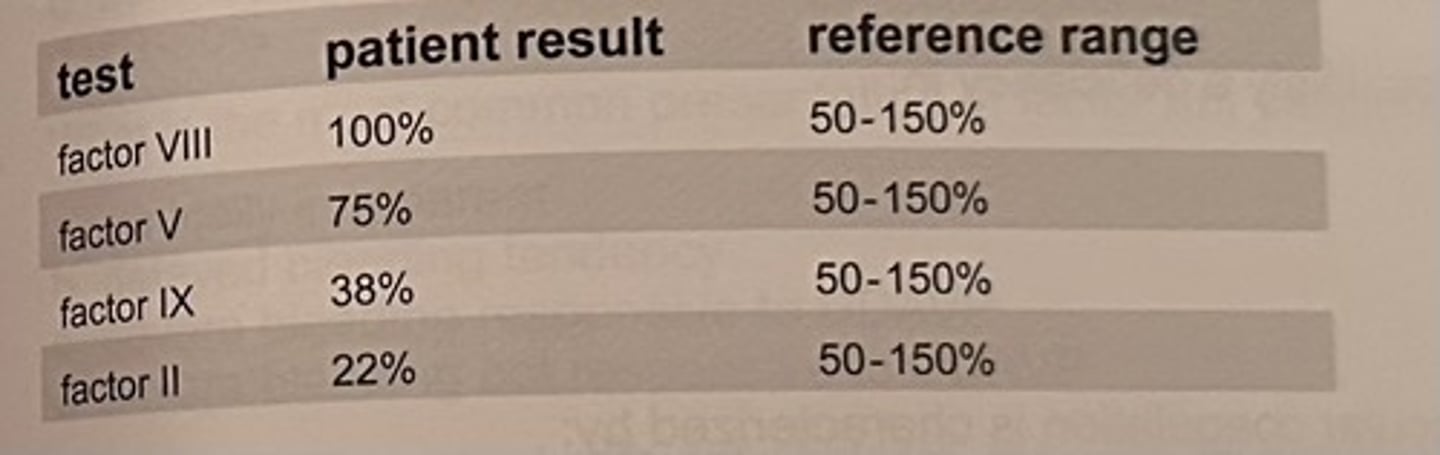
A 4-year-old boy presents with chronic ear infections and is on prophylactic antibiotics. He also presents with a bleeding diathesis. Factor assay results are shown in the table.
Possible causes are:
a. factor II deficiency
b. lupus anticoagulant
c. hemophilia
d. vitamin K deficiency
d. vitamin K deficiency
A hemophilic male and a normal female can produce a:
a. female carrier
b. male carrier
c. male hemophiliac
d. normal female
a. female carrier
Hemophilia B is a sex-linked recessive disorder that presents with a decrease in factor:
a. VIII
b. IX
c. X
d. XI
b. IX
To distinguish between hemophilia and von Willebrand disease, a patient with von Willebrand will present with which of the following test results?
a. result a
b. result b
c. result c
d. result d
c. result c

A patient presents with bleeding 48 hours after tooth extraction. Results are shown in this table.
The cause of bleeding is most likely a deficiency in:
a. plasminogen
b. factor XIII
c. alpha-2 antiplasmin
d. factor XII
b. factor XIII
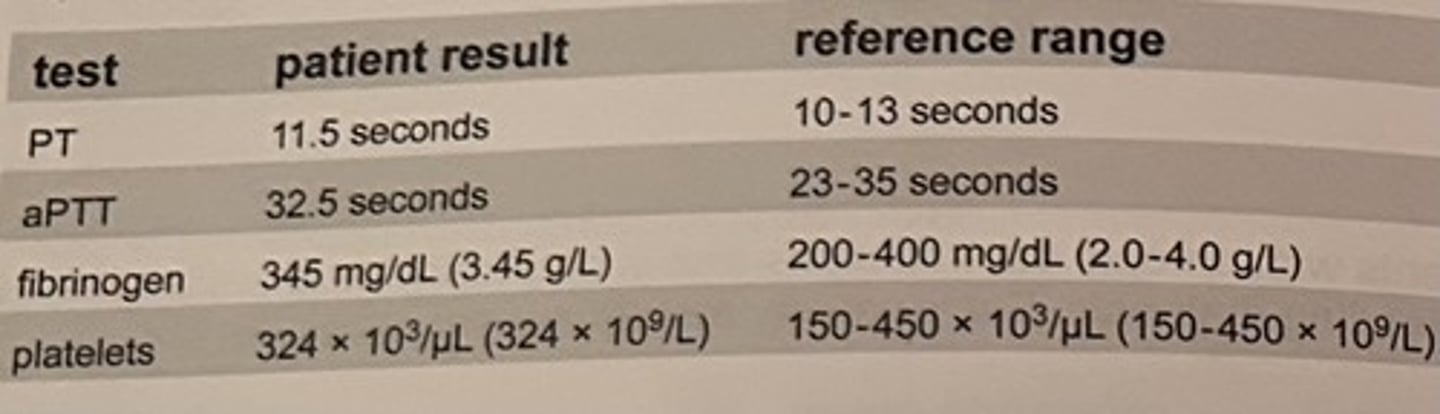

Acute DIC is characterized by:
a. hypofibrinogenemia
b. thrombocytosis
c. negative D-dimer
d. shortened thrombin time
a. hypofibrinogenemia
A patient develops unexpected bleeding and test results shown in the table are obtained.
What is the most probable cause of these results?
a. familial afibrinogenemia
b. primary fibrinolysis
c. DIC
d. liver disease
c. DIC
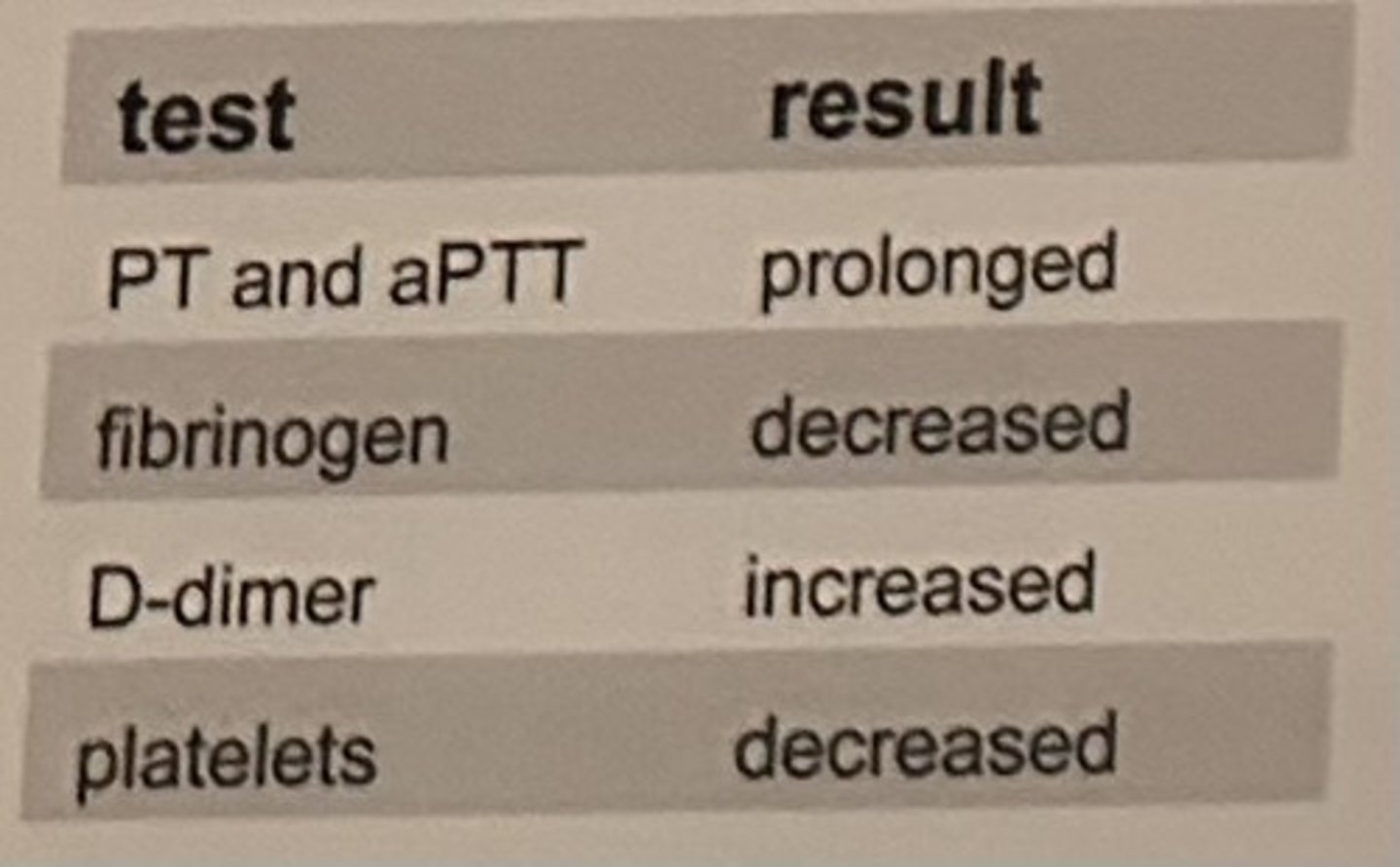
A patient presents with the results shown in the table.
These results are characteristic of:
a. dysfibrinogenemia
b. increased D-dimer
c. fibrin monomer-split product complexes
d. therapeutic heparinization
a. dysfibrinogenemia

Only an abnormal aPTT would be seen in the following disorder:
a. deficiencies of factors X, V, and II
b. DIC
c. liver disease
d. anti-FVIII antibodies
d. anti-FVIII antibodies
What is usually the factor VIII level in a hemophiliac patient with spontaneous bleeding?
a. <1%
b. 5-10%
c. 20-30%
d. 50-60%
a. <1%
What is the most common presentation of factor XIII deficiency?
a. clinically inapparent
b. delayed bleeding tendency
c. severe bleeding responsive to DDAVP
d. severe bleeding not responsive to DDAVP
b. delayed bleeding tendency
A patient is diagnosed with amyloidosis, they will be deficient in which of the following factors?
a. factor II
b. factor V
c. factor VII
d. factor X
d. factor X
Which of the following tests are the most beneficial tool to aid in the diagnosis of DIC?
a. fibrinogen, aPTT, FDP
b. FDP, aPTT, reptilase
c. thrombin time, fibrinogen
d. thrombin time, D-dimer, fibrinogen
d. thrombin time, D-dimer, fibrinogen
Results of a factor X assay are shown in the table.
These results indicate the presence of:
a. factor deficiency
b. clotted sample
c. inhibitor
d. bad draw
c. inhibitor

A patient that has a lupus anticoagulant may bleed due to:
a. factor VIII deficiency
b. drugs
c. antibodies to prothrombin
d. infection
c. antibodies to prothrombin
Patients with factor XIII deficiency have:
a. an abnormal aPTT
b. delayed bleeding
c. tissue damage
d. joint bleeds
b. delayed bleeding
In hemolytic disease of the newborn, babies present with:
a. hyperbilirubinemia
b. thrombocytosis
c. hyperalbuminemia
d. leukocytosis
a. hyperbilirubinemia
Occasional spontaneous bleeding may occur in a hemophiliac who is classified as:
a. acquired
b. mild
c. moderate
d. severe
c. moderate
In liver disease patients present with decreased synthesis of:
a. common pathway factors
b. intrinsic pathway factors
c. fibrinogen pathway factors
d. vitamin-K-dependent factors
d. vitamin-K-dependent factors
Alloantibodies are found in:
a. congenital hemophilia
b. acquired hemophilia
c. congenital von Willebrand disease
d. acquired von Willebrand disease
a. congenital hemophilia
When there is a disparity between the results of the fibrinogen antigen and the activity, the most likely diagnosis is:
a. dysfibrinogenemia
b. hypofibrinogenemia
c. hyperfibrinogenemia
d. afibrinogenemia
a. dysfibrinogenemia
Bleeding doesn't correlate well with factor levels in a deficiency of:
a. factor VIII
b. factor IX
c. factor XI
d. factor VII
c. factor XI
A newborn baby boy is known to have a homozygous protein C deficiency. This puts him at a risk for:
a. DVT
b. warfarin induced skin necrosis
c. increased risk of thrombosis
d. purpura fulminans
d. purpura fulminans
Protein S forms a reversible complex with:
a. C4b binding protein
b. protein C
c. total protein S
d. Fc receptors
a. C4b binding protein
A 48-year-old male is screened pre-operatively. He has a positive family history for bleeding. The patient is of Ashkenazi Jewish descent. His results are shown in the table.
Based on this history and results of the tests, this patient's most likely diagnosis is a deficiency in factor:
a. VIII
b. IX
c. XI
d. XII
c. XI

Unregulated and excessive formation of thrombin and plasmin is seen in:
a. liver disease
b. vitamin K deficiency
c. hemolytic disease of the newborn
d. disseminated intravascular coagulation
d. disseminated intravascular coagulation
A patient presents with a factor VIII level of 2%. The vWF activity (ristocetin cofactor) is <1% with a vWF antigen of 3%. The most likely diagnosis is:
a. hemophilia A
b. hemophilia B
c. type II vWD
d. type II vWD
d. type II vWD
A patient with a clot presents with the results shown in the table.
The most likely diagnosis is:
a. DIC
b. hypofibrinogenemia
c. dysfibrinogenemia
d. afibrinogenemia
c. dysfibrinogenemia
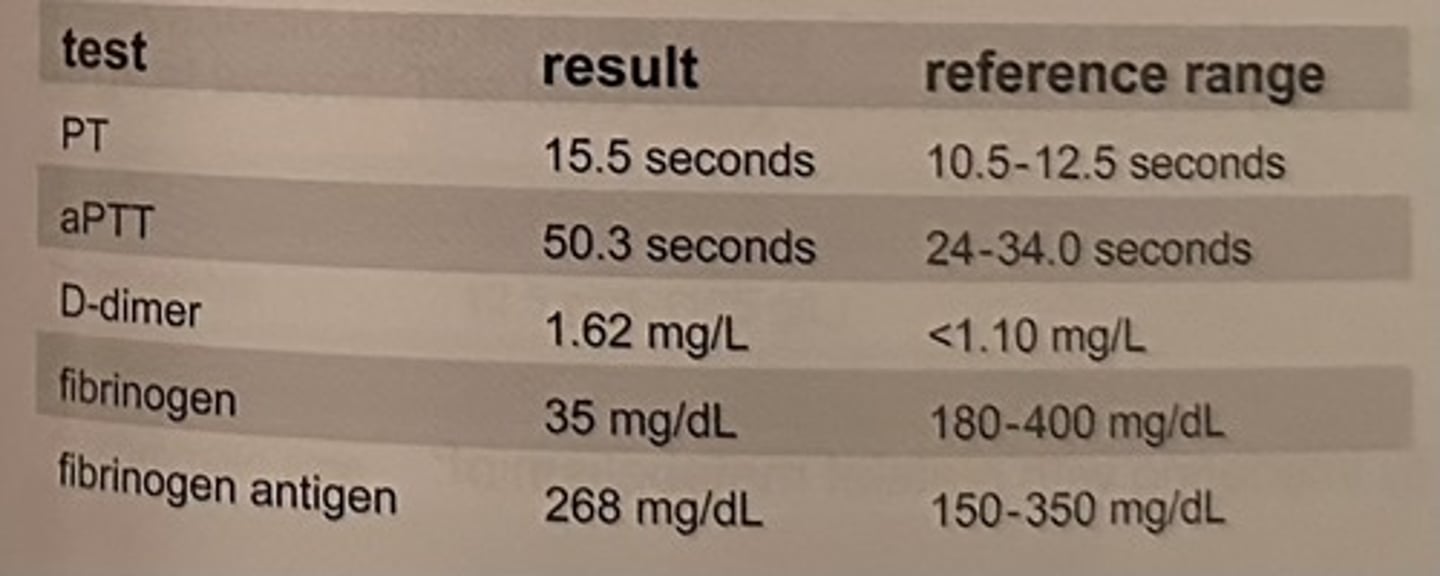

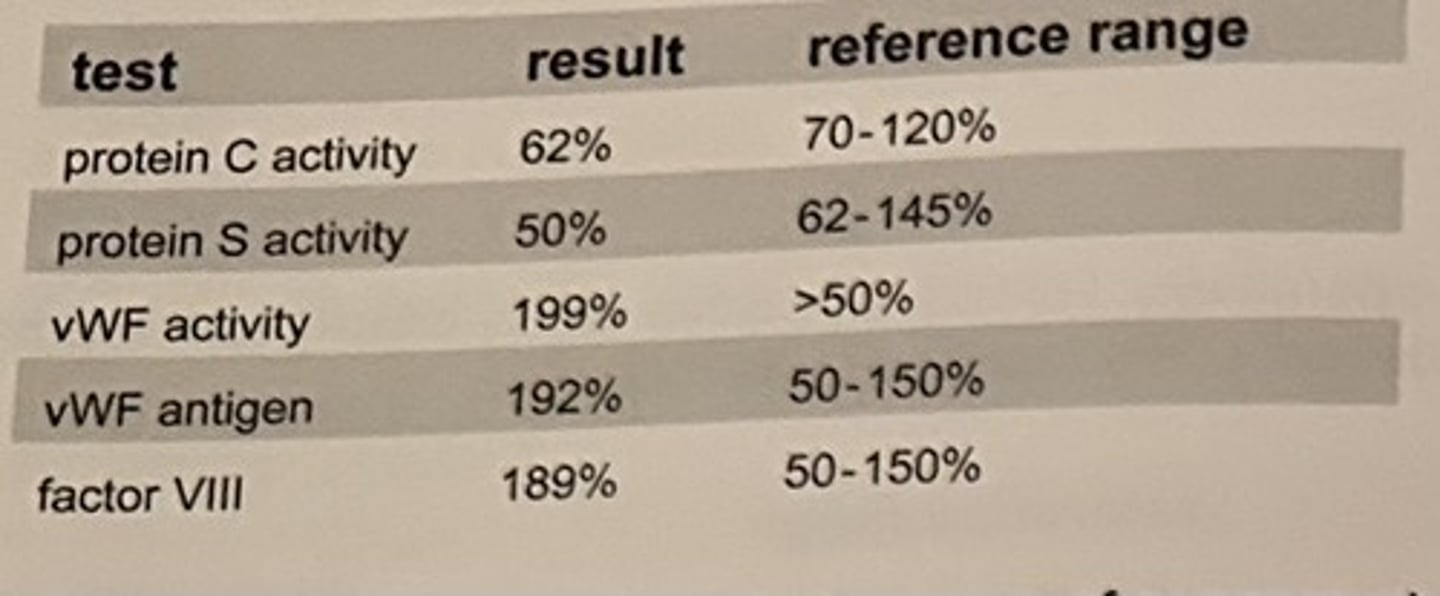
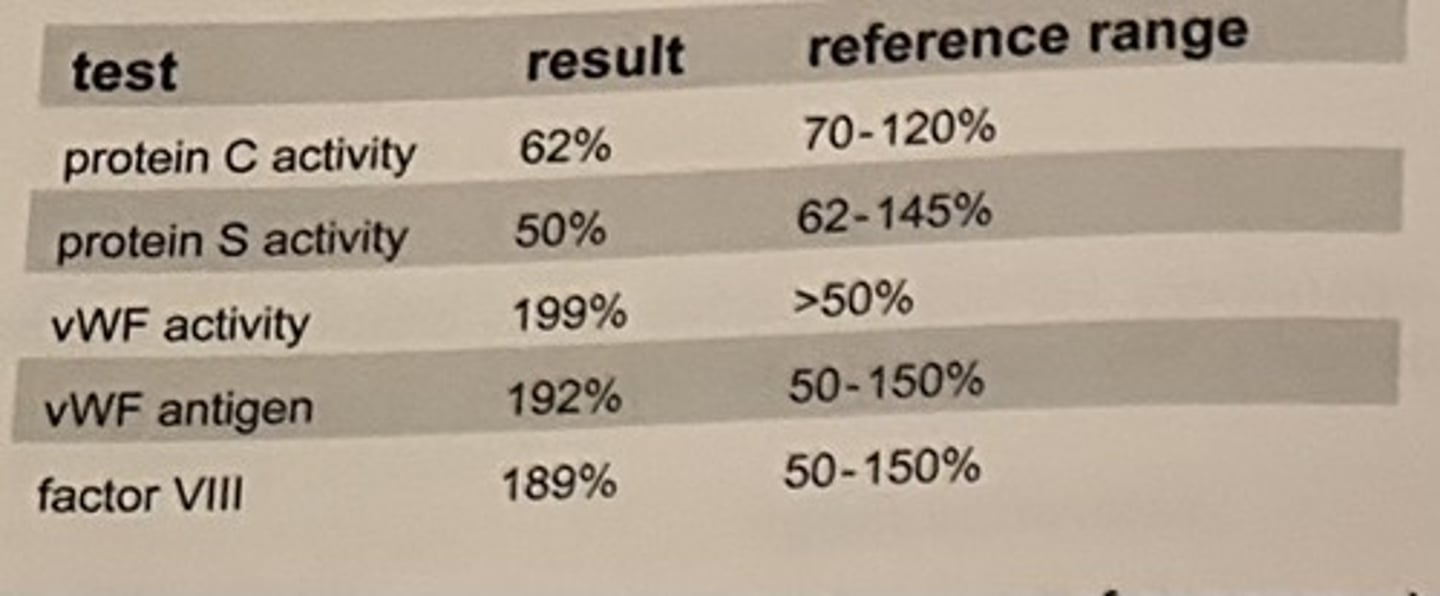
The following results are obtained on a pregnant woman who is short of breath.
The patient's obstetrician calls because of concern about the patient's clotting risk. Based on the pregnancy status of this patient, the results appear:
a. elevated
b. the patient is at risk for bleeding
c. that the patient is at risk for clotting
d. normal
d. normal
A 65-year old male with metastatic pancreatic carcinoma shows elevated PT and aPTT, platelet count 15x10^3/uL (15x10^9/L) and elevated D-dimer. A blood smear would show:
a. Howell-Jolly bodies
b. macro-ovalocytes
c. schistocytes
d. target cells
c. schistocytes
A 25-year old male with celiac disease presents with occult positive stools. What vitamin deficiency should be considered?
a. vitamin A deficiency
b. vitamin D deficiency
c. vitamin E deficiency
d. vitamin K deficiency
d. vitamin K deficiency
vWF antigen can be found in which of the following?
a. myeoblasts
b. monoblasts
c. lymphoblasts
d. megakaryocytes
d. megakaryocytes
The life span of a platelet is:
a. 5 days
b. 10 days
c. 20 days
d. 30 days
b. 10 days
Aspirin affects platelet function by interfering with platelet metabolism of:
A. cyclooxygenase
B. lipids
C. carbohydrates
D. nucleic acids
A. cyclooxygenase
In patients who present with bleeding disorders caused by platelets, the most common type of bleeding is:
a. mucosal bleeding
b. hemarthrosis
c. delayed bleeding
d. deep hematomas
a. mucosal bleeding
The anticoagulant that is best directed against platelets is:
a. argatroban
b. hirudin
c. tirofiban
d. dabigatran
c. tirofiban
How do ticlopidine and clopidogrel inhibit platelets?
a. binding von Willebrand factor
b. ADP mediated platelet aggregation
c. inhibit GPIIb/IIIa
d. depletion of platelet alpha granule content
b. ADP mediated platelet aggregation
von Willebrand factor mediates platelet adhesion by binding to platelet receptor:
a. GPIb/IIa
b. GPIb/GPIX/GPV
c. GPIIb/IIa
d. GPIb/GPIIIa/GP X
b. GPIb/GPIX/GPV
The disease state that presents with a quantitative platelet disorder is:
a. von Willebrand disease
b. hemophilia A
c. Glanzmann thrombasthenia
d. May-Hegglin anomaly
d. May-Hegglin anomaly
A patient presents with a very low platelet count and is diagnosed with acute idiopathic thrombocytopenia purpura (ITP). Which statement is associated with acute ITP?
a. it is found primarily in adults
b. spontaneous remission usually occurs within several weeks
c. women are more commonly affected
d. peripheral destruction of platelets is decreased
b. spontaneous remission usually occurs within several weeks
The most common cause of bleeding in patients is:
a. qualitative platelet defect
b. qualitative abnormality of fibrinogen
c. quantitative abnormality of fibrinogen
d. quantitative abnormality of platelets
d. quantitative abnormality of platelets
A 53-year-old man is in recovery following a triple bypass operation. Oozing is noted from his surgical wound. The lab data shown in the table are obtained.
The most likely cause of bleeding would be:
a. dilution of coagulation factors due to massive transfustion
b. intravascular coagulation secondary to microaggregates
c. hypofibrinogenemia
d. dilutional thrombocytopenia
d. dilutional thrombocytopenia

ADAMTS13 deficiency is responsible for thrombocytopenia found in:
A. TTP
B. DIC
C. HUS
D. ITP
A. TTP
Heparin induced thrombocytopenia (HIT) is an immune mediated complication associated with heparin therapy. Antibodies are produced against:
a. ACLA
b. PF4
c. AT
d. B2GP1
b. PF4
In PV, the platelet count is:
a. elevated
b. normal
c. decreased
d. variable
a. elevated
A 60-year-old man has a painful right knee and a slightly enlarged spleen. Hematology results included in the table.
This is most compatible with:
a. congenital spherocytosis
b. RA with reactive thrombocytosis
c. myelofibrosis
d. idiopathic thrombocythemia (essential or primary)
d. idiopathic thrombocythemia (essential or primary)

The type of bleeding that is the most characteristic in patients with platelet disorders is:
a. deep muscle hemorrhages
b. retroperitoneal hemorrhages
c. mucous membrane hemorrhages
d. severely prolonged clotting times
c. mucous membrane hemorrhages
When reviewing platelet morphology on a blood smear, the presence of giant platelets is noted. This may indicate:
a. Bernard-Soulier
b. von Willebrand Disease
c. Glanzmann thrombasthemia
d. Ehler-Danlos
a. Bernard-Soulier
A patient with multimer pattern that has all bands present but in decreased concentrations would be diagnosed with:
a. hemophilia
b. type 1 vWD
c. type 2 vWD
d. type 3 vWD
b. type 1 vWD
Which characteristic of Bernard-Soulier syndrome helps distinguish it from von Willebrand disease?
a. concomitant storage pool defects in platelets
b. giant platelets
c. thrombocytosis
d. thrombocytopenia
b. giant platelets
Which of the following characteristics are common between Hermansky-Pudlak and Chediak-Higashi syndromes?
a. giant inclusion granules in granulocytes
b. alpha granule storage pool defects
c. inclusions in macrophages
d. oculocutaneous albinism
d. oculocutaneous albinism
Patients with wiscott-aldrich syndrome present with:
a. thrombocytosis, giant platelets
b. thrombocythemia, eczema
c. thrombocytopenia, giant platelets
d. thrombocytopenia, eczema
d. thrombocytopenia, eczema
When evaluating a patient for von Willebrand disorder, the ABO blood type that has the lowest level of vWF is:
a. O
b. A
c. B
d. AB
a. O
Which subtype of von Willebrand disease is most common?
a. type 1
b. type 2A
c. type 2B
d. type 3
a. type 1
Which of the following types of von Willebrand disease should not be treated with DDAVP?
a. type 1
b. type 2A
c. type 2B
d. type 3
c. type 2B
TTP presents with a pentad of symptoms which doesnt include:
a. fever
b. anemia
c. thrombocytopenia
d. liver failure
d. liver failure
A 40-year-old female has pinpoint hemorrhages on her legs, with an Hct of 43% and a platelet count of 19x10^3/uL (19x10^9/L). Steroids fail to increase platelet count. The patient's diagnosis is:
a. decreased platelet production
b. suppressed pluripotent stem cells
c. immune thrombocytopenic purpura
d. defective platelet endothelial interaction
c. immune thrombocytopenic purpura
A 60-year-old female presents with blurred vision, confusion, and petechiae with a platelet count of 29x10^3/uL (29x10^9/L).
The CBC RBC morphology shows schistocytes. The differential diagnosis should include:
a. ITP
b. TTP
c. HUC
d. DIC
b. TTP

One of the main difference between TTP and HUS is:
a. neurological involvement
b. kidney dysfunction
c. thrombocytopenia
d. microangiopathic hemolytic anemia
b. kidney dysfunction
Several hours after birth an infant develops petechiae, purpuric hemorrhages and a platelet count of 21x10^3/uL (21x10^9/L). The most likely diagnosis is:
a. drug induced immune thrombocytopenia
b. thrombotic thrombocytopenic purpura
c. autoimmune neonatal thrombocytopenia
d. neonatal idiopathic thrombocytopenia
c. autoimmune neonatal thrombocytopenia
In TTP, a deficiency of ADAMTS13 causes clotting because of:
a. increased vW factor
b. inability to cleave ULVWM
c. increased production of thrombin
d. inability to produce antibodies to prevent platelet aggregation
b. inability to cleave ULVWM
An orthopedic patient who is on heparin has a platelet count of 50x103/uL (50x10^9/L); his platelet count the previous day was 120x10^3/uL (120x10^9/L). The patient is tested for HIT and has a positive result. The first step in the treatment of HIT is:
a. start LMWH
b. stop heparin
c. switch to warfarin
d. give platelets
b. stop heparin
In HELLP syndrome patients present with:
a. normal liver enzymes
b. elevated platelets
c. high blood pressure
d. hemochromatosis
c. high blood pressure
von Willebrand factor serves as a stabilizer for:
a. platelets
b. factor IX
c. ristocetin
d. factor VIII
d. factor VIII
The platelet disorder in which the abnormality is due to a defect in platelet aggregation is:
a. Glanzmann thrombasthenia
b. von Willebrand disease
c. storage pool disease
d. Bernard-Soulier syndrome
a. Glanzmann thrombasthenia