EXAM 4 Lecture
1/141
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
142 Terms
Urinary System functions
Kidneys regulate blood volume and composition, blood pressure, pH, glucose and produces hormones, filter wastes
Ureters transport urine from kidneys to urinary bladder
Urinary bladder stores urine and expels it into urethra
Urethra discharges urine from bod
What do the kidneys regulate?
blood volume and composition, blood pressure, pH, glucose
What do the Ureters do?
transport urine from kidneys to urinary bladder
What does the Urinary bladder do?
stores urine and expels it into urethra
What does the Urethra do?
discharges urine from body
What are the functions of the kidney? (8)
- Regulation of blood ionic composition
- Regulation of blood pH
- Regulation of blood volume
- Regulation of blood pressure
- Maintenance of blood osmolarity
- Production of hormones
- Regulation of blood glucose
- Waste removal
What makes up the blood’s ionic composition
Na+, K+, Ca2+, Cl-, HPO42
How does kidneys regulate blood volume?
Can choose whenever or not to conserve or eliminate water
How does the kidneys regulate blood pressure?
They can secret renin that then actives the renin-angiotensin-aldosterone pathway.
what is blood osmolarity
measures the concentration of all chemical particles found in the plasma. ( Water vs electrolytes: ions K+, Na+, Ca2+, Cl-, HPO42-)
How does the kidneys maintain blood osmolarity?
Primarily by adjusting the excretion or conservation of both water and electrolytes
Draw the The Renin-Angiotensin-Aldosterone System (RAAS)
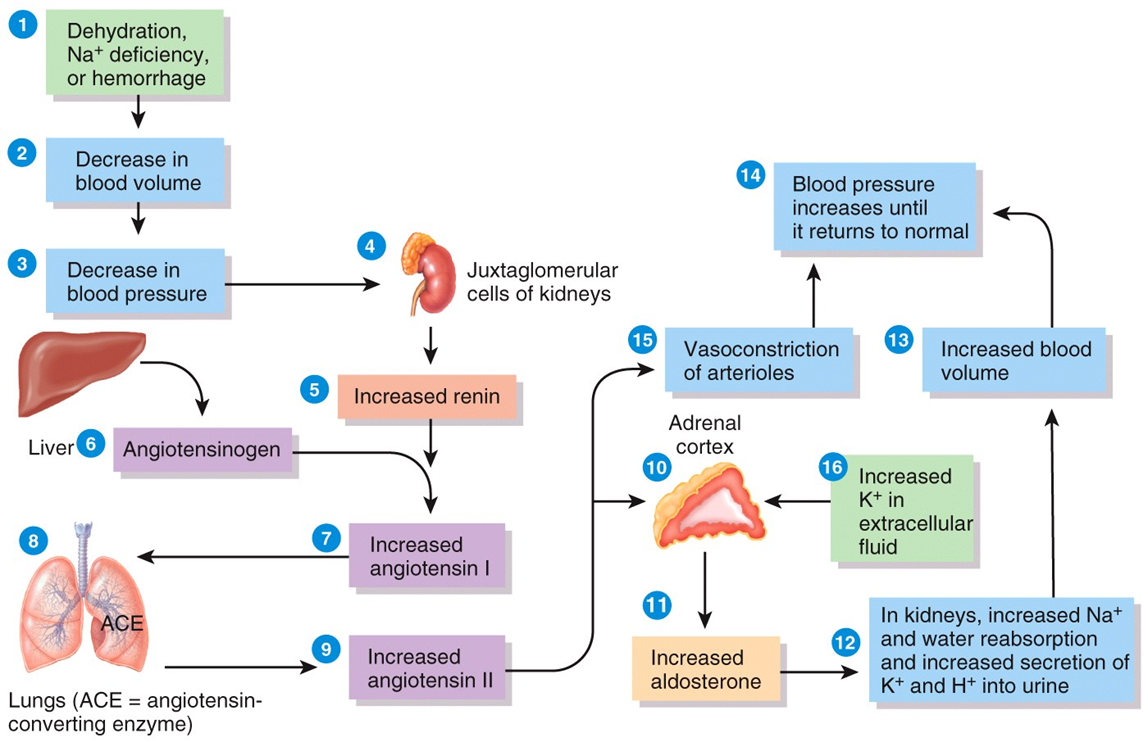
What hormones do the kidney produce?
calcitriol hormone and erythropoietin hormone
What does the calcitriol hormone do?
It’s the active form of vitamin D. It increases Ca2+ absorption in large intestines, maintain calcium levels
What does the •erythropoietin hormone do?
Increases erythrocyte formation
How do the kidneys reglue blood glucose levels?
It uses glutamine (amino acid) to preform gluconeogenesis (synthesizes new glucose from non-carbohydrate precursors,)
What is waste in blood defined as?
Substances that have no useful function in the body. Some result from metabolic reactions in the body.
Where do Ammonia and Urea come from?
Deamination of amino acids
Where does Urobilin come from?
Catabolism of hemoglobin
Where does creatinine come from?
From the breakdown of creatine phosphate in muscle fibers
Where does Uric acid come from?
Catabolism of nucleic acids
What other wastes might be excreted in urine besides Ammonia, Urea, Urobilin, Creatinine, and Uric acid
Foreign substances from the diet, such as drugs or environmental toxins.
What are the primary waste products of metabolic reactions that the kidneys excrete in urine, and which metabolic processes produce them?
Ammonia and urea from deamination of amino acids
Urobilin from catabolism of hemoglobin
Creatinine from the breakdown of creatine phosphate in muscle fibers
Uric acid from catabolism of nucleic acids
What kidney is slightly lower?
Right is lower because the liver is there
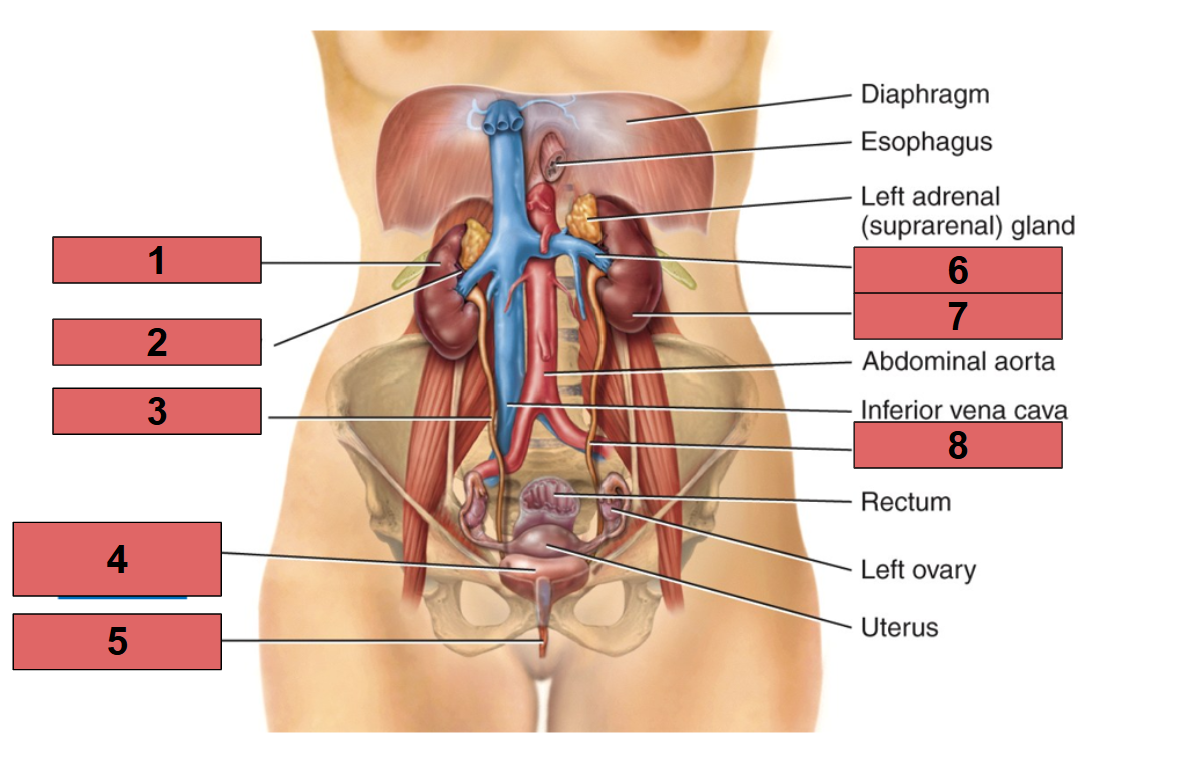
Label this picture
1- Right kidney
2- rental artery
3- Right ureter
4- urinary bladder
5- urethra
6- left renal vein
7- left kidney
8- left ureter
What are the three layers of tissue around kidney?
renal capsule, adipose capsule, and the renal fascia
What is the renal capsule?
The outer surface of the kidney
What is the tissue of the renal capsule like?
Smooth, transparent sheet of dense irregular connective tissue, continuous with the outer coat of the ureter.
What is the adipose capsule?
Mass of fatty tissue surrounding the renal capsule
What does the adipose capsule do?
holds the kidney in place and protects from trauma
What is Nephroptosis?
floating kidney that is more common is women
What is the renal fascia?
The outer most layer of the kidney
What kind of tissue is the renal fascia?
Thin layer of dense irregular connective tissue
What does the renal fascia do?
Anchors kidney to abdominal wall and other surrounding structures
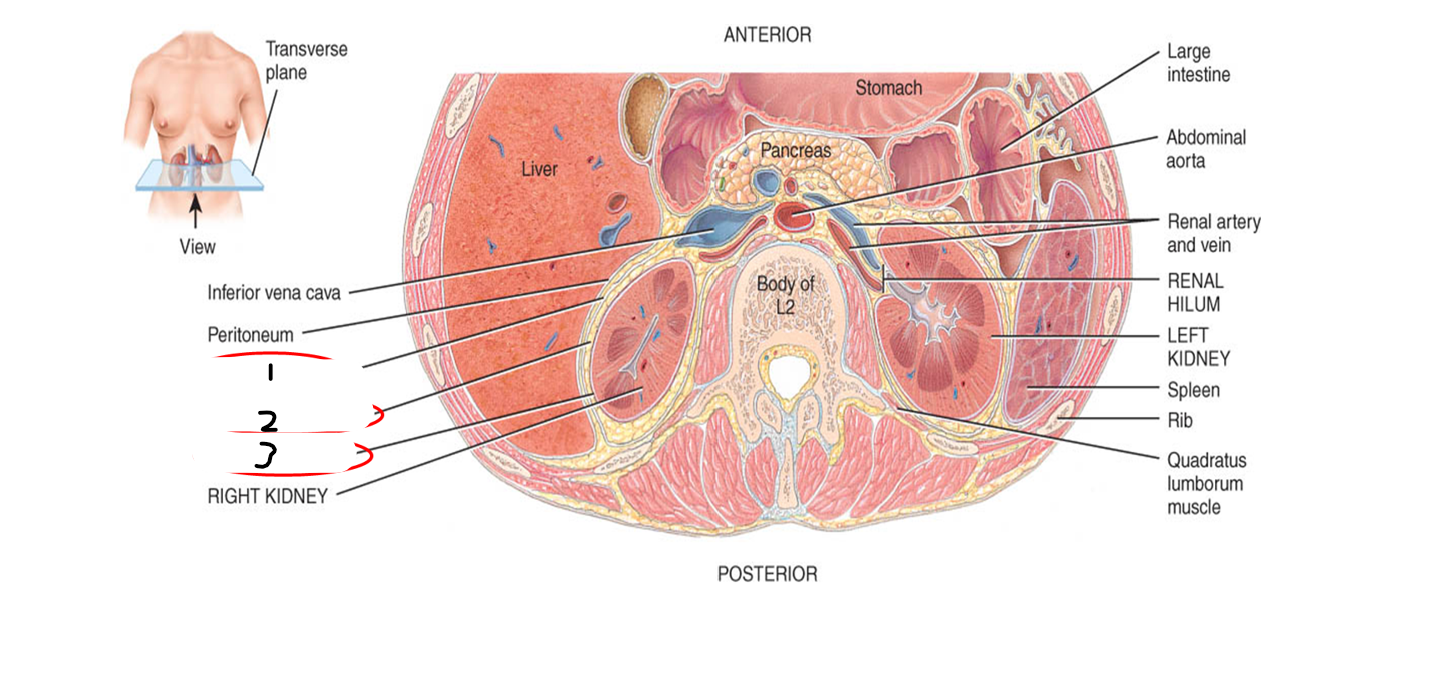
label this picture of the external anatomy of kidneys
1- renal fascia
2- adipose capsule
3- renal capsule
What is the External Anatomy of Kidneys
Three layers of tissue around kidney
Renal capsule is the outer surface of kidney.
Adipose capsule is a mass of fatty tissue surrounding the renal capsule; holds the kidney in place and protects from trauma
Renal fascia is a more superficial layer that anchors kidney to abdominal wall
Where is the renal cortex located and look like?
Inside of kidneys, superficial, light in color, and between / above renal pyramids
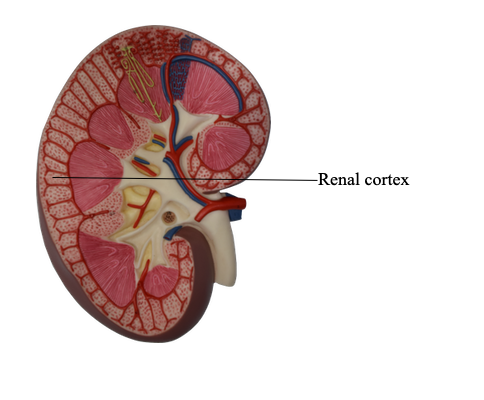
Where is the renal medulla and what does it look like?
deep part of the kidney, dark reddish-brown
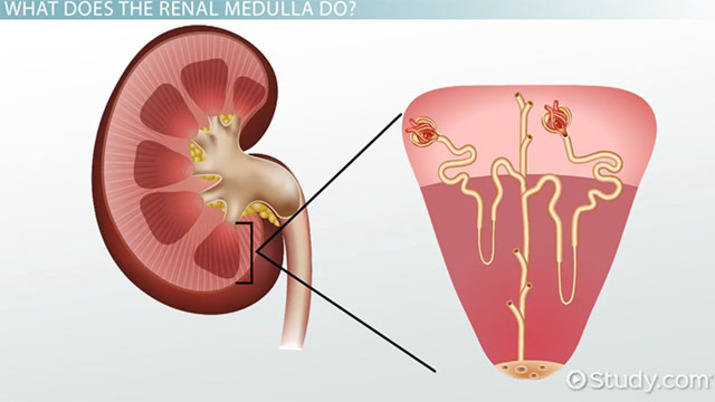
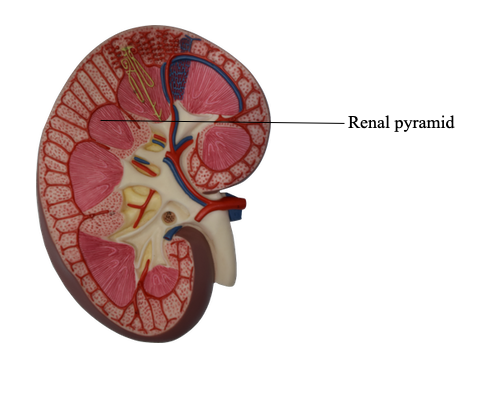
What are renal pyramids?
cone-shaped structures in the renal medulla
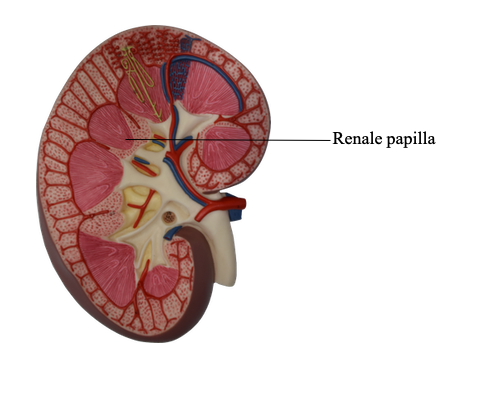
What are renal papilla?
Concave portion, where ureter, vessels and nerves converge
What is a Renal lobe?
renal pyramid, renal cortex, ½ of renal columns to either side
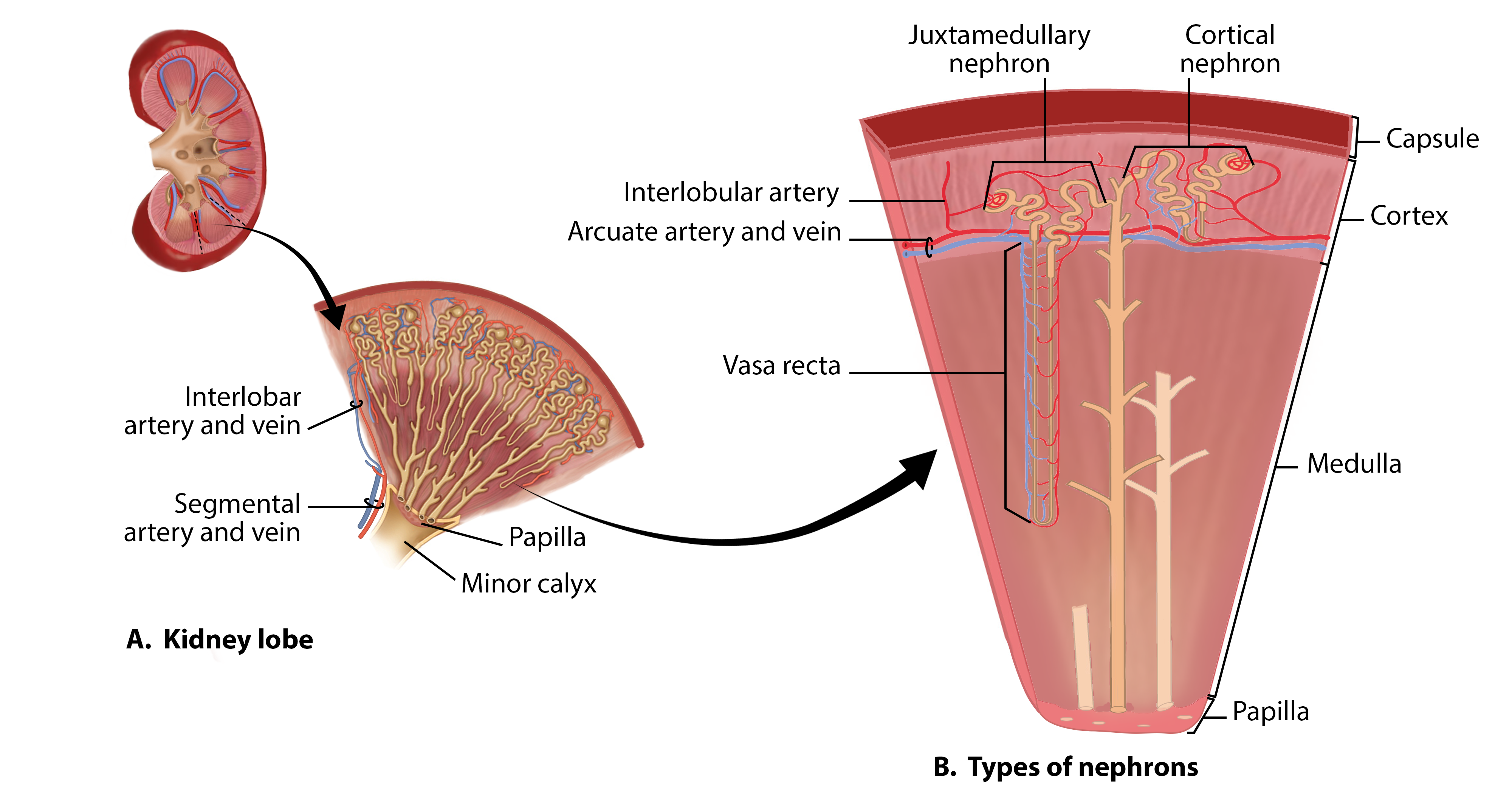
What is the Minor Calyx?
Chamber in the kidney that collects urine from the renal pyramid
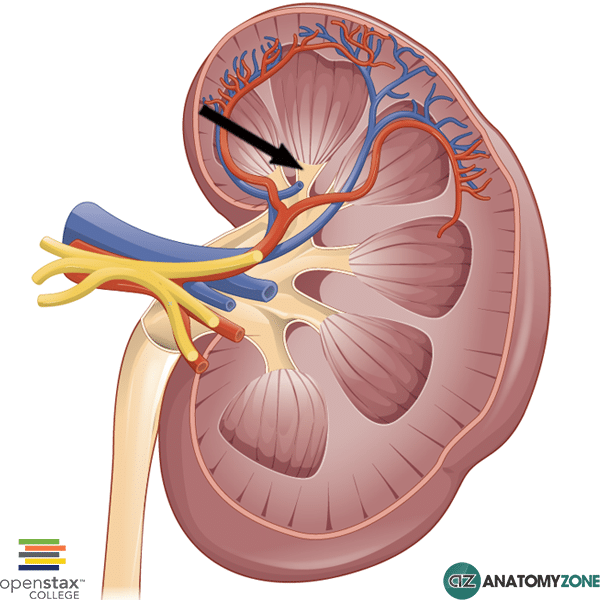
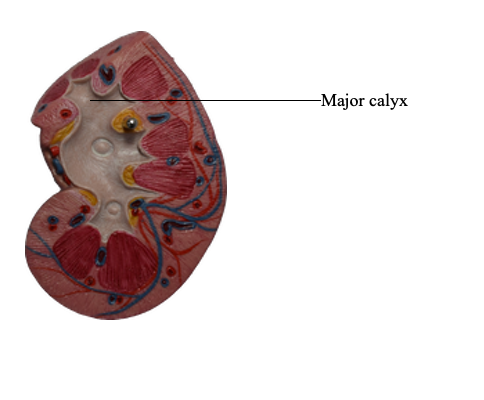
What is the Major Calyx?
A large, funnel-shaped structure in the kidney that collects urine from several smaller minor calyces
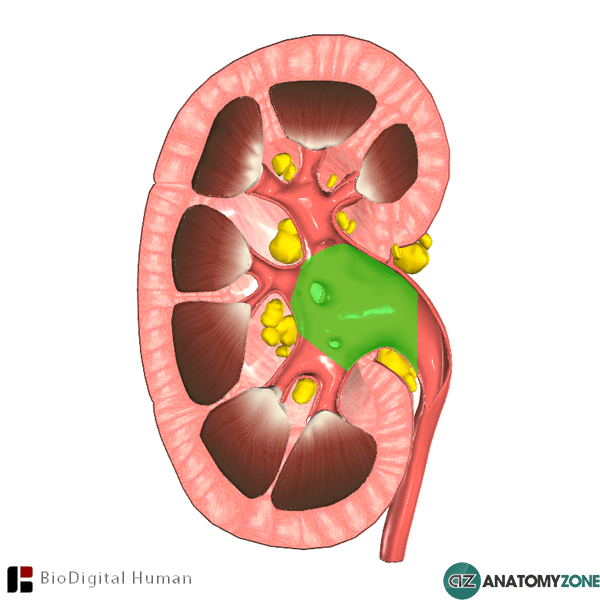
What is the Renal Pelvis?
Central collecting chamber within the kidney
What is the Parenchyma?
It’s the only functional portion of the kidney. It’s made up of the renal cortex, renal pyramids, and nephrons (all the brownish parts of the kidney)
What is a Nephron?
The the basic structural and functional unit of the kidney.
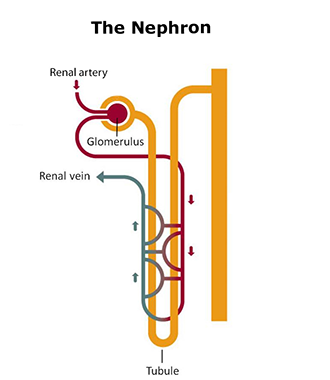
What makes up a nephron?
It’s made up of renal corpuscle and a renal tubule.
What is the renal corpuscle?
The initial filtering unit of the kidney nephron, located in the renal cortex.
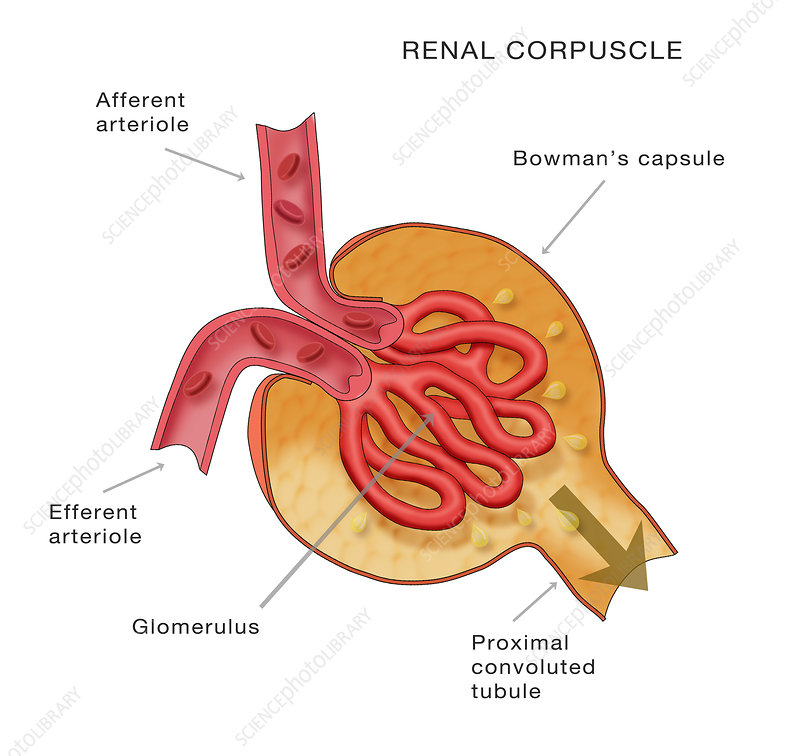
What does the renal corpuscle do?
Blood plasma filtered. The initial site of blood filtration in the nephron, responsible for separating water, ions, and waste from blood plasma to form filtrate
What is the renal tubule?
a tiny, long tube within the kidney's nephron that filtered fluid passes into this
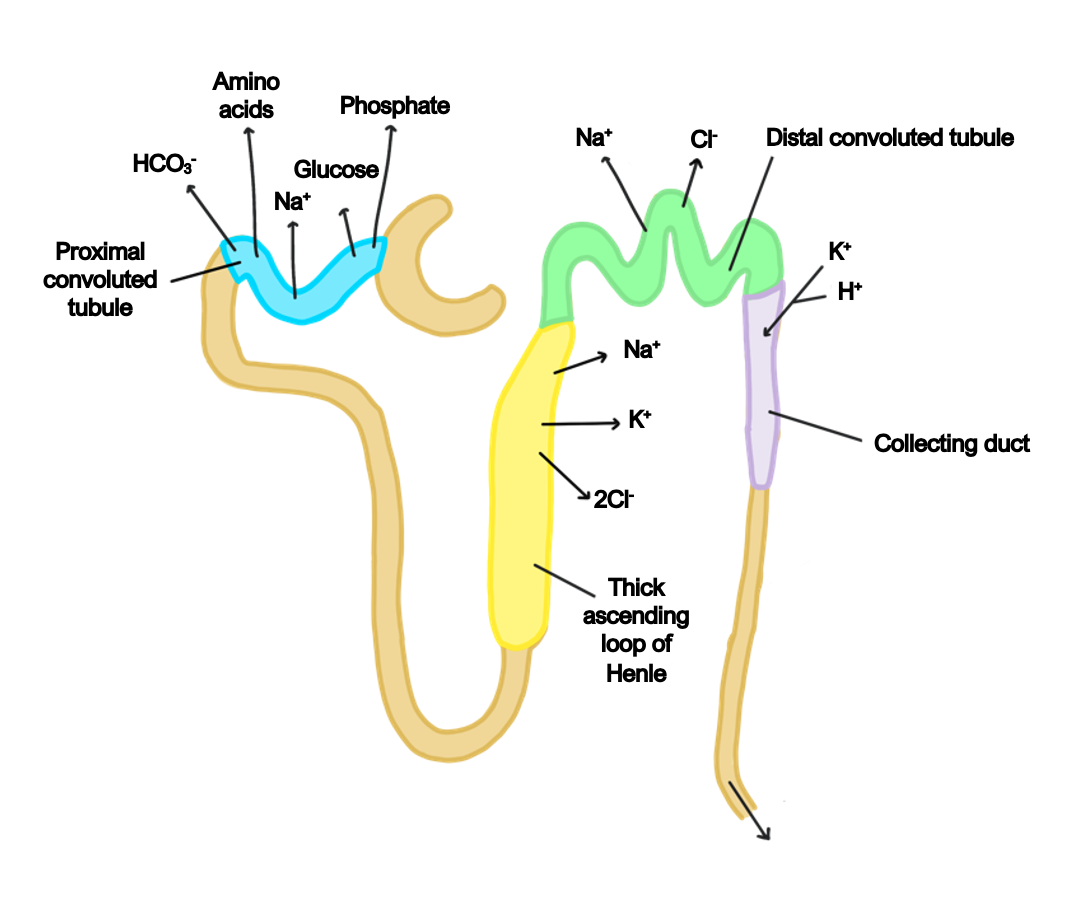
What is the glomerulus?
A tiny, specialized cluster of capillaries located within the nephron.
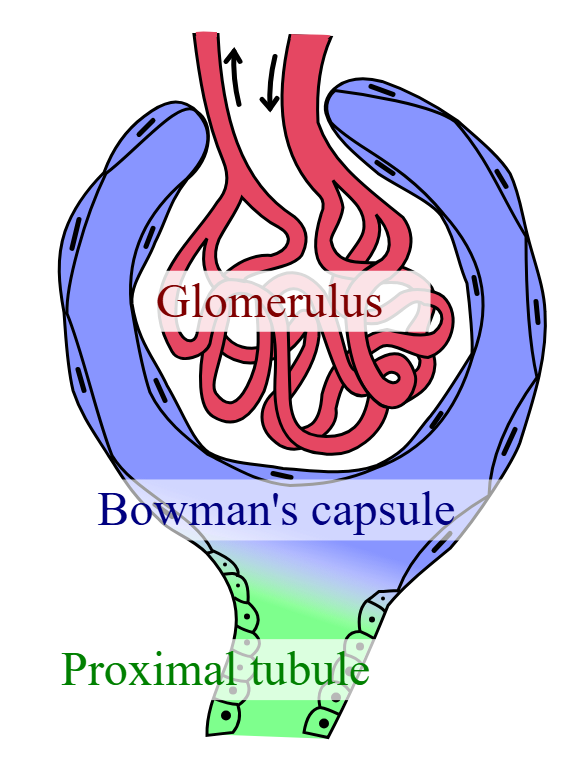
What is the glomerular (Bowman’s) capsule?
epithelial layers that surround capillaries
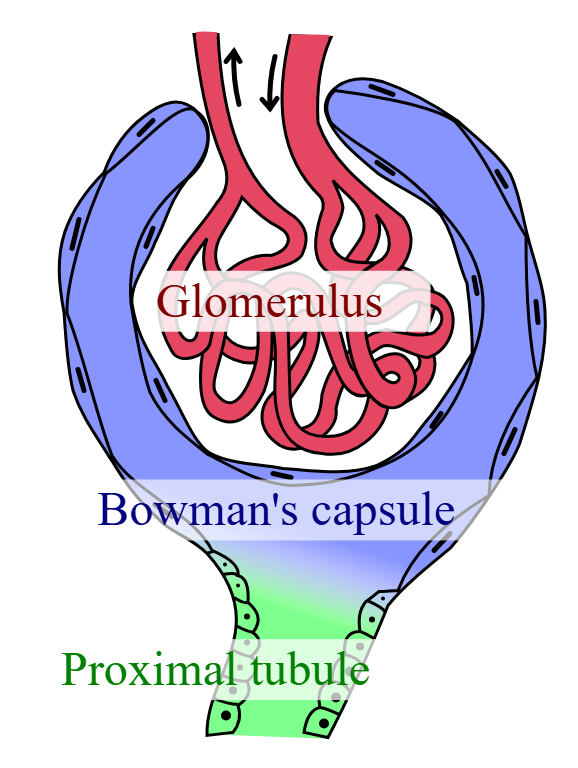
What are the Steps of Filtration?
1. Blood plasma filtered in glomerular capsule
2. Fluid passes into renal tubule
3. Fluid leaves distal convoluted tubule and empties into collecting duct.
What are the 3 sections of the renal tubule?
-Proximal convoluted tubule
-Loops of Henle
-Distal convoluted tubule
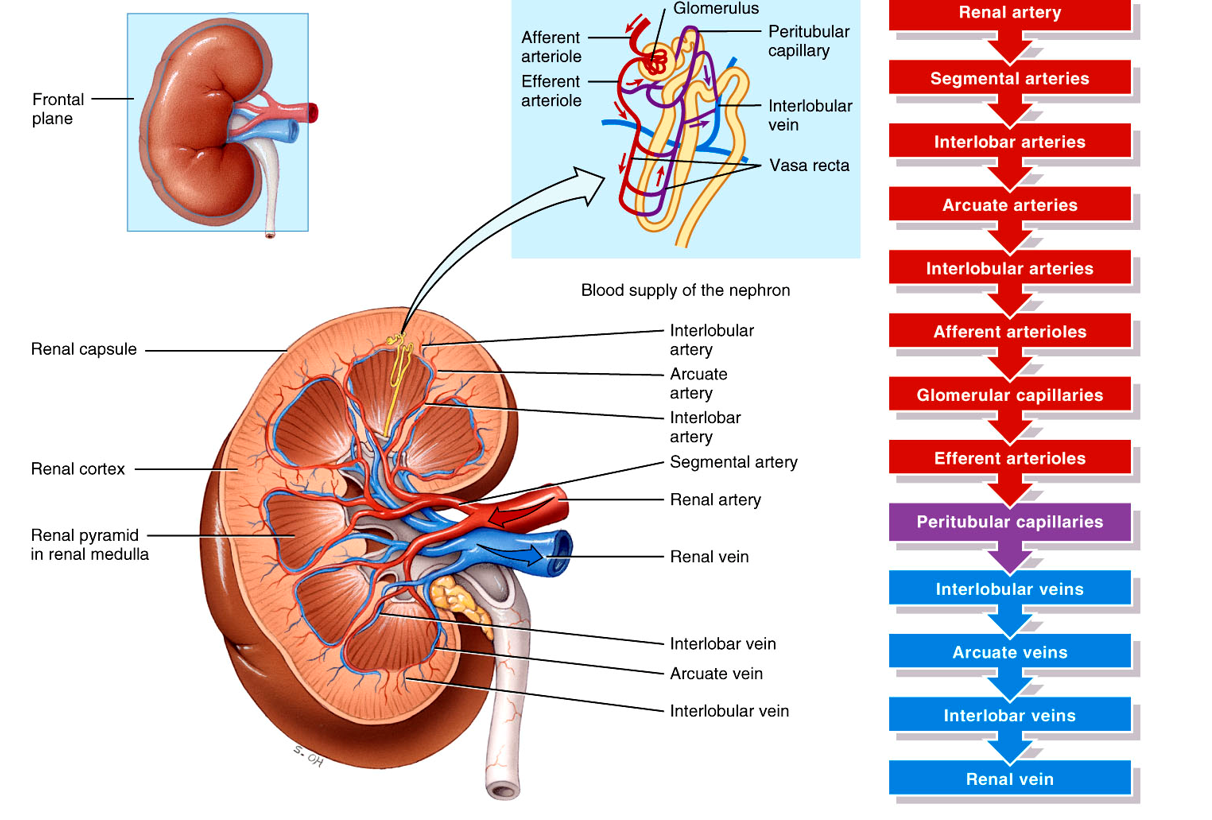
Whats the order of blood supply to the kidneys?
Rental artery – Segmental arteries – Interlobar arteries – Arcuate Arteries – Interlobular Arteries – Afferent Arterioles – Glomerular Capillaries – Efferent Arterioles – Peritubular capillaries – Interlobular veins – arcuate veins – interlobar veins – renal veins
Renal artery
Enters the kidney and Supplies kidney with blood
Afferent arteriole
Arteries that enters the glomerulus
Glomerular capillaries
Network of capillaries where filtration occurs
Efferent arterioles
Arteries that exits glomerulus
Peritubular capillaries
Exchange with tubules
What is filtrate?
. It’s the the fluid filtered from blood plasma into the Bowman's capsule of nephrons. It is formed from water and solutes
What is not filtered out in the Renal corpuscle?
cells and protein are not filtered out
Where does kidney filtration take place?
In the glomerulus
What main functions occur in the Renal tubules?
Reabsorption and secretion
What is fluid called in the Renal tubules?
tubular fluid
What reabsorption happens in renal tubules ?
99% of water and many solutes are returned from the tubular fluid to the blood (Peritubular capillaries)
What secretion happens in the renal tubules?
Wastes, drugs, excess ions secreted from the blood into the tubular fluid.
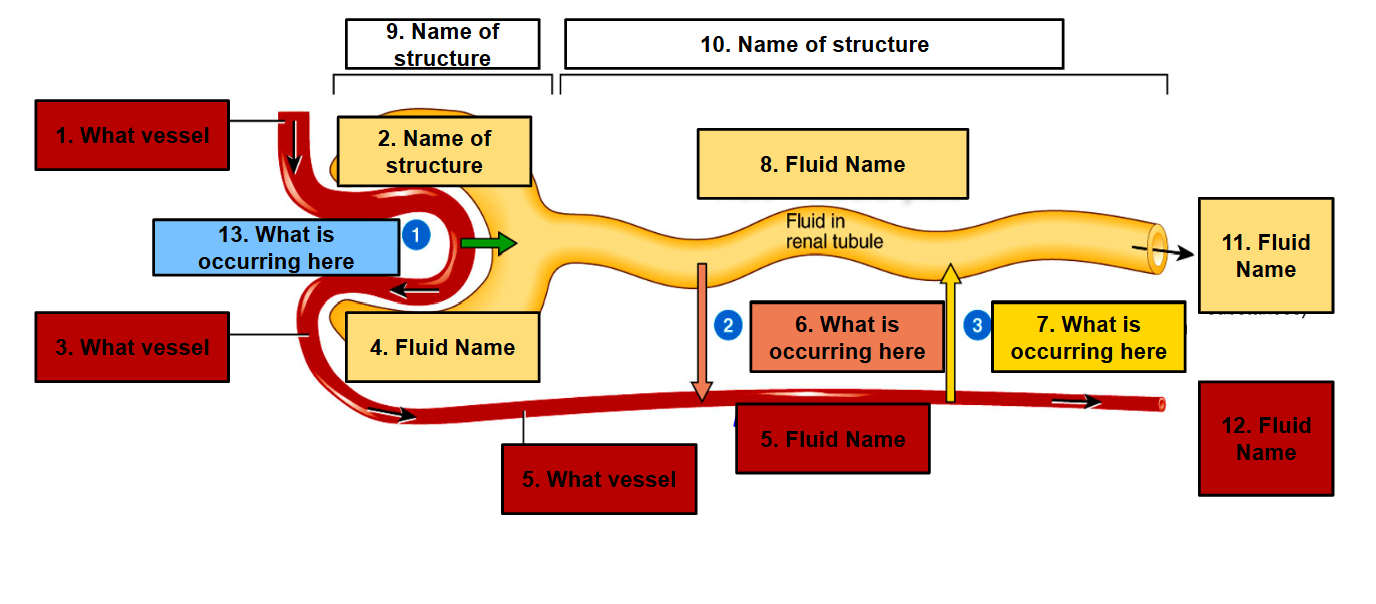
Label this picture
1- Afferent Arteriole
2- Glomerular Capsule
3- Efferent Arteriole
4- Filtrate
5- Pertiublar Capiilaries
6- Tubular reabsortion from tubular fluid into blood
7- tubular secretion from blood into tubular fluid
8- Tubular fluid
9- Renal corpuscle
10- Renal tubule
11- Urine
12- Blood
13- Filtration from blood plasma into nephron
What happens in the Collecting ducts ?
Excretion
What is Excretion?
filtration + secretion - reabsorption
What is the fluid in the Collecting duct called?
Urine
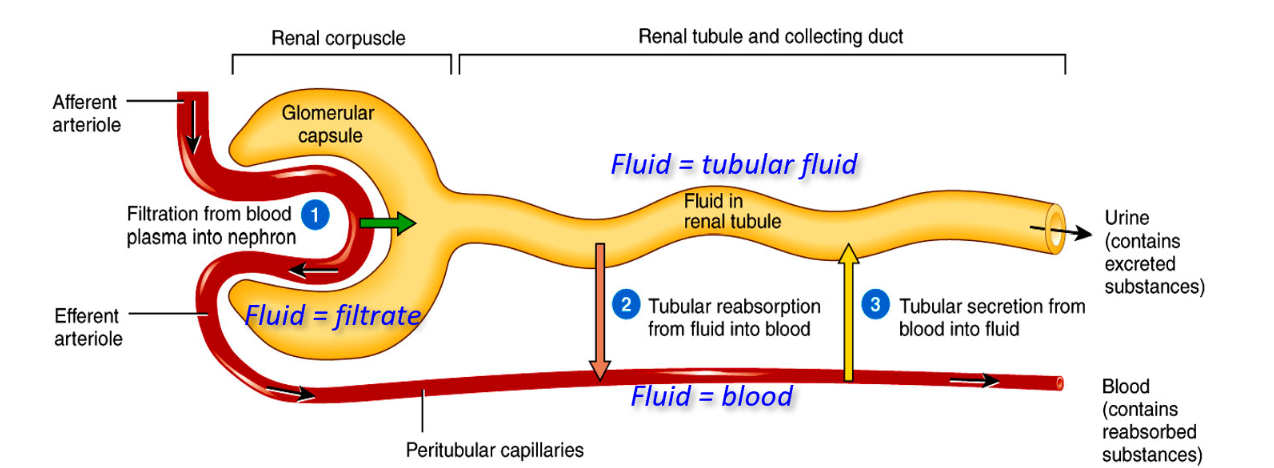
What is fluid called in the Glomerular capsule, Proximal Convoluted Tubule, Loop of Henle, Distal Convoluted Tubule, Collecting Duct, Peritubular Capillaries called?
Glomerular capsule- Filtrate
PCT,LOH,DCT - Tubular Fluid
Collecting Duct - urine
Peritubular Capillaries - Blood Plasma
What percentage of filtrate is reabsorbed?
About 99% is reabsorbed.
What is the Body Fluid Composition of Blood Plasma?
( No Blood Cells)
Protein
Glucose
Amino Acids
Na+
H+
Urea
What is the Body Fluid Composition of Blood
Blood Cells
Protein
Glucose
Amino Acids
Na+
H+
Urea
What is the Body Fluid Composition of Filtrate?
( No Blood Cells or Proteins)
Glucose
Amino Acids
Na+
H+
Urea
What is the Body Fluid Composition of Tubular Fluid?
( No Blood Cells or Proteins)
Glucose
Amino Acids
Na+
H+
Urea
What is the Body Fluid Composition of Urine?
(No Blood Cells Proteins, Glucose, or Amino Acids)
Na+
H+
Urea
What is the fluid composition difference between Filtrate &Tubular fluid vs Urine
Filtrate and tubular fluid have Glucose and Amino Acids while urine does not.
What is the fluid composition difference between Blood Plasma and Filtrate &Tubular fluid
Blood plasma has proteins while Filtrate &Tubular fluid does not
What precent of filtrate returns after reabsorption?
99%
Is Glomerular Filtration selective or nonselective?
nonselective
What are the layers to Glomerular (Bowman’s) capsule?
Visceral layer, Parietal layer, and Capsular space
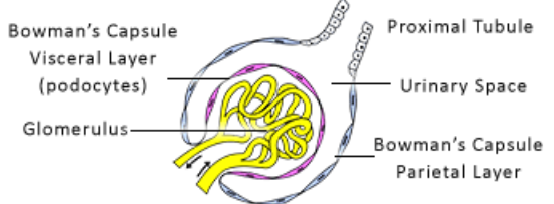
What is the Visceral layer of the Glomerular (Bowman’s) capsule?
The Inner most layer that is made of Podocytes. The Podocytes wrap around glomerular capillaries.
What tissue type is the Visceral layer of the Glomerular (Bowman’s) capsule?
Simple squamous epithelium ( made of podocytes)
What is the Parietal layer of the Glomerular (Bowman’s) capsule?
Outer layer Simple squamous epithelium.
What is the Capsular (Bowman’s) space?
The Space between the visceral and parietal layers where filtrate collects
What causes the large volume of filtrate?
Large surface area
Thin, porous filtration membrane.
High glomerular capillary blood pressure
What contributes to the Large surface area for filtrate to be produced
Highly branched network of glomerular capillaries
what are the layers and features of the glomerular capillaries?
Endothelium - Fenestrations
Basal lamina – negative charge and repels proteins
Filtration slits - Spaces between the podocytes
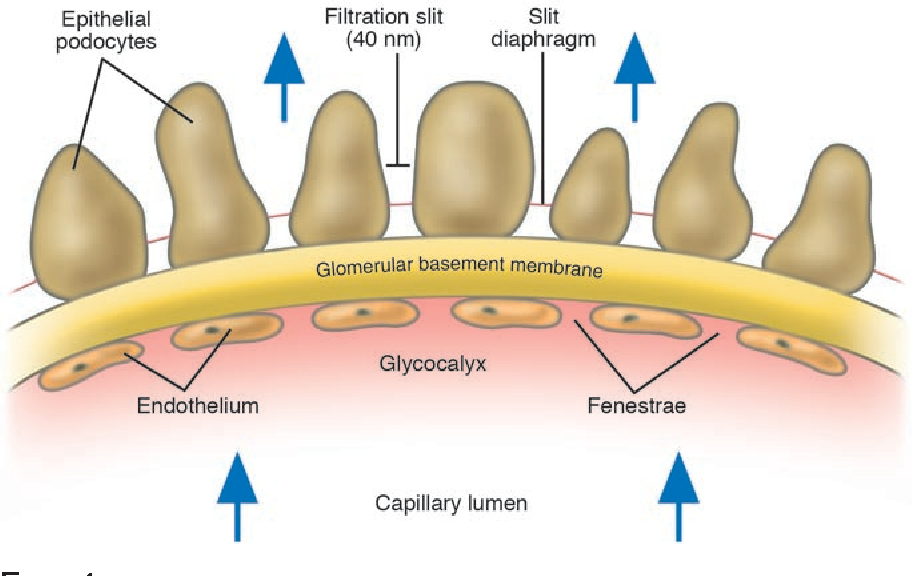
What are the Fenestrations of glomerular endothelium?
Inner most layer with large pores.
What is the Basal lamina layer of the glomerular capillaries
Connective tissue (Acellular material) that is negative charge and repels proteins
What are Filtration slits?
Spaces between the podocytes of the visceral layer of the glomerular capsule
What is NOT filtered in Glomerular Filtration?
plasma proteins and blood cells