Clinical and pathological changes seen in fungal infections
1/32
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
33 Terms
What are the major tissue reactions seen with fungal infections?
1. Acute suppurative inflammation + micro-abscess formation
2. Chronic inflammation -( pyogranulomatous or granulomatous)
3. Necrosis - if fungi invade blood vessels we see infarction and tissue death
what kind of inflam is seen in acute fungal infections
(Predominantly neutrophilic inflammation)
what happens in chronic inflam in fungal infection
The complex molecules of fungal walls do not fully degrade when phagocytosed, so not totally removed by acute inflammation
→ fungal material released into tissues when phagocytes die → recruitment of additional macrophages to remove debris → Activated → produce chemokines and cytokines → recruit more macrophages
Repeated cycles → granulomatous inflammatory response
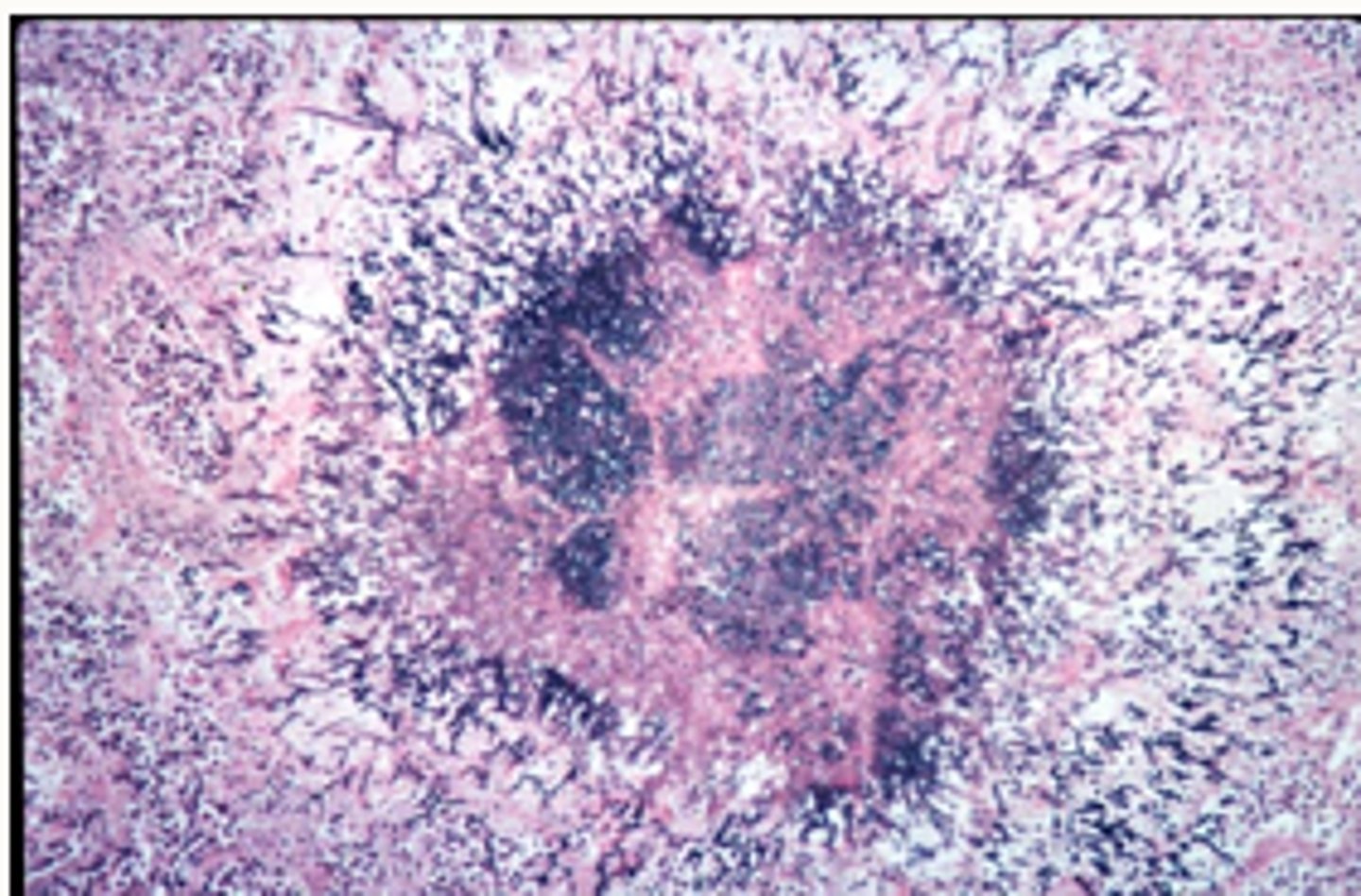
Well-demarcated fungal granuloma
fungal organisms in middle
How might an animal present with dermatophytosis?
-alopecia, claw disease, papules and pustules
How might an animal present with Malassezia infection?
§Erythema, scale, hair loss, lichenification with chronicity. Also involved in otitis
What would be seen in candida infection?
§Very rare in small animals
§Affects skin, mucosae
§Ulcers/erosions covered with tenacious yellow/grey exudate
What would be seen in subcutaneous (deep) mycoses?
•Present as cutaneous papules or s/c nodules +/- ulceration, discharging tracts
•Usually due to traumatic implantation of fungus - most commonly on feet/limbs or head
•Regional lymphadenopathy common
•Occasionally disseminate to other organs
What will be seen in systemic mycoses?
•Granulomas/pyogranulomas/necrosis in organs affected - can affect any organ system
•causes systemic illness
Describe Aspergillosis
-A common soil saprophyte with occasional pathogenic effects
-A fungal that can show more than one manifestation of tissue invasion such as through inhalation, local inoculation and haematogenous spread from Gi tract
Describe inhalation route of aspergillus
-Most common
§Local respiratory infection, esp birds
§Guttural pouch mycosis (horses)
§Nasal aspergillosis (dolicocephalic dogs)
Describe local inoculation route of aspergillus
-Ocassional
§Keratitis (horse)
§Mastitis (cattle - via contaminated intra-mammary tubes)
Describe haematogenous spread from GI tract of aspergillus
§Mycotic placentitis/abortion (cattle)
How does mycotic placentitis manifest?
Causes necrosis of placenta and abortion
How will mycotic abortion present?
Hyperkeratotic skin lesions on aborted foetus
What are the diagnostic tests for mycoses?
-Direct microscopic examination
-fungal culture
-histopathology
-Other test: PCR and Wood’s lamp for dermatophytosis, Latex agglutination test for cryptococcal capsular antigen in serum/CSF/urine, ELISA for Sporothrix schenkii antibodies
Describe direct microscope examination?
Examine hair plucks/scale: For dermatophytosis
Cytology stained e.g. with Diff Quick such as
Malassezia - stained direct/indirect impression smears or acetate tape strips
Cryptococcus spp - see yeasts in CSF or aspirates/direct smears of cutaneous lesions/nasal exudate
Describe fungal culture
hair, dry skin scrapings/scale, coat brushings - for dermatophytes
tissue culture (from biopsy or PM material) - for subcutaneous/deep mycoses
Sabauraud dextrose agar for most; some require specialised/enriched media
Incubation times/temps vary between fungi
potential for false +ve results due to carriage/contamination
Can speciate based on
Asexual spore type
Colony appearance
Features of vegetative hyphae
Describe histopathology
§Generally used for subcutaneous/systemic infections - on biopsy or PM material
§Histological demonstration of fungi within tissues confirms infection, c.f. carriage/contamination - occasionally used for dermatophytes
§Request special fungal stains,
what stains for fungi for histopathology
e.g. Periodic acid-Schiff (PAS), Grocott-Gomori methenamine silver (GMS)
what other tests can be done for fungi
PCR and Wood’s lamp for dermatophytosis – see later teaching
Latex agglutination test for cryptococcal capsular antigen in serum/CSF/urine
ELISA for Sporothrix schenkii antibodies
Give 2 examples of mycotoxicosis
-Aflatoxicosis (aflatoxins)
-Ergotism (ergotamine)
What are the clinical findings of aflatoxicosis?
-hepatotoxicity
-immunosuppression
mutagenesis/teratogenesis,
ill-thrift
what fungus causes aflatoxicosis and what doe sit affect
aspergillus
grown on grain so affects animals consuming grain
cattle, pigs, poultry, dogs, trout
What are the clinical findings of Ergotism?
Neurotoxicity and perinatal deaths in lambs and calves
what fungus causes ergotism and what doe sit affect
Claviseps sp
seedheads of ryegrass/other grasses/cereals
grown on grain seed heads → cattle pigs, poultry, deer, sheep horses
what does the severity and recovery of mycotoxicosis depend on
Severity depends on amount of toxin ingested
Recovery rate depends on duration of exposure
What are the epidemiological feature of mycotoxicosis/
Outbreaks, usually seasonal and sporadic, +/- associated with certain batches of food
how to confirm mycotoxicosis
-To confirm must find mycotoxin in feed of concern as clinical signs often just present as immunosuppression
what type of hypersensitivity is it usually
type 1
What are the clinical changes seen with hypersensitivity fungal induced disease?
fungi/moulds in chronic pulmonary disease/recurrent airway obstruction
causes chronic cough, nasal discharge, occ resp distress
environmental fungi/moulds in canine atopic dermatitis
causes pruritus
skin Malassezia
causes pruritus
what can be done for induction of hypersensitivity due to fungi
Once clinical investigations have shown potential allergy to exist, IgE serology or intradermal testing can be carried out if want to investigate causal allergens
what is the main clinical effect of fungal disease
tissue mycosis
less commonly mycotoxicosis and fungal hypersensitivity