Kidney to Bladder
1/33
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
34 Terms
The two upper urinary tract organs are…
Kidneys
Ureters
The two lower urinary tract organs are…
Bladder
Urethra
Give main characteristics of the kidneys
They are bilateral bean-shaped organs, reddish-brown in Color, and surrounded by smooth fibrous capsule
Between 5th and 9th week of gestation, the kidneys typically ascend from the pelvis to a position high on the posterior abdominal wall (typically extend from T12-L3)
Right kidney is often lower due to liver
Retroperitoneal
Surrounded by perinephric fat which extends into the renal sinuses
Which two nerves run posterior to the kidneys?
Iliohypogastric nerve
Ilioinguinal nerve
_______________ sit atop each kidney. What do they do?
Suprarenal / Adrenal Glands
Release catecholamines and steroids
Plays a role in blood pressure regulation
Function as part of the endocrine system, completely separate in function from the kidneys
Separated by the kidneys by fascial septum
Name and describe the parts of the kidney
Hilum/Hilus : area where vessels, lymphatics, and nerves enter and leave the kidneys; continuous with renal sinus
Renal cortex: continuous band of pale tissue that completely surrounds the renal medulla
Renal medulla: between the renal cortex and renal sinus
Renal sinus: area between the renal medulla and pelvis/hilum
Renal columns: internal extensions of the renal cortex — divides the renal medulla into renal pyramids
Renal papilla: apical openings of the pyramids projecting into the renal sinus
Minor calyx: receive urine from the papillary ducts (contained in renal papilla)
Major calyx: when 2-3 minor calyx unite
Renal pelvis: when 2-3 major calyx unite → ureter
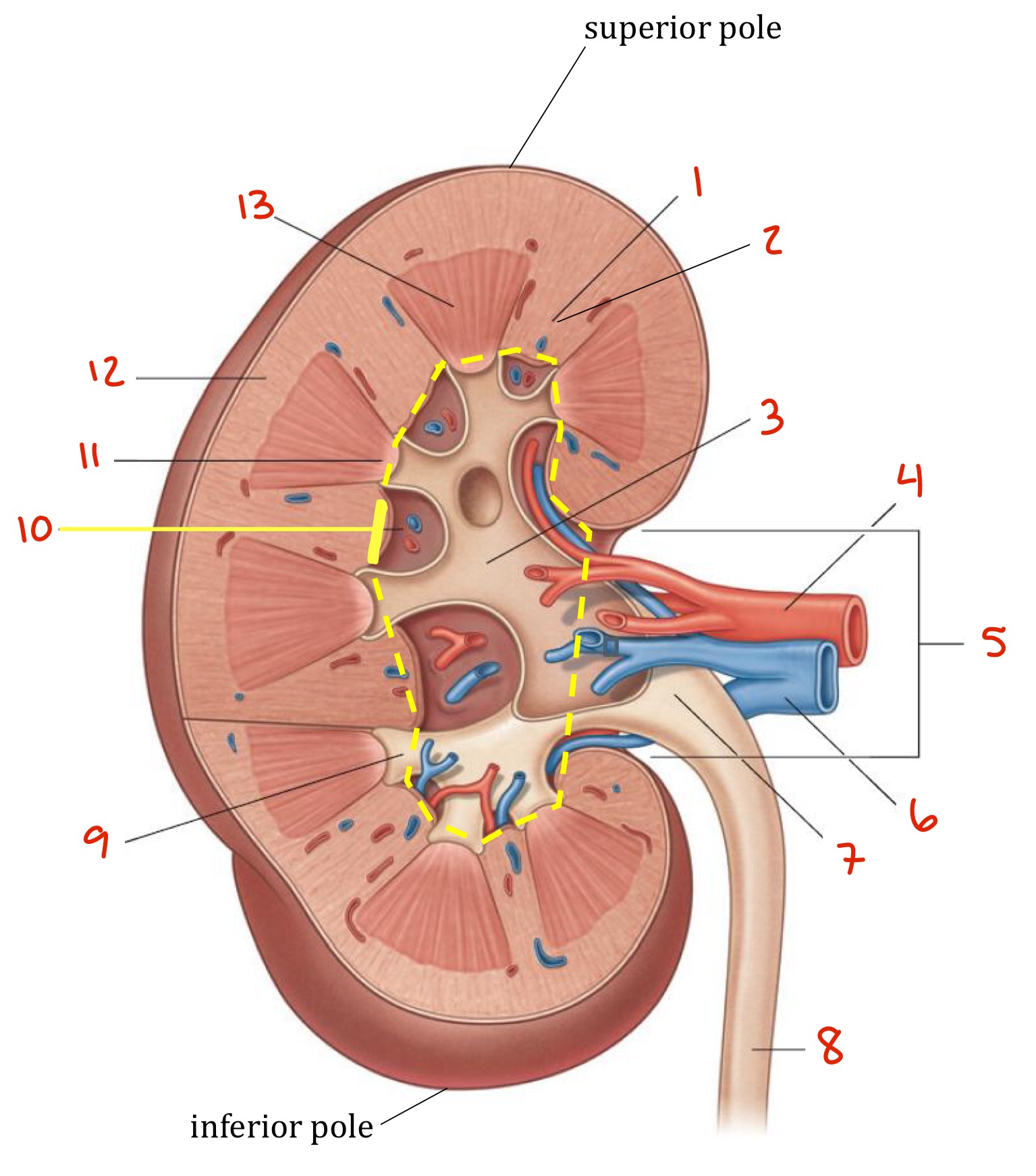
Identify
Renal column
Renal column
Major calyx
Renal artery
Hilum
Renal vein
Renal pelvis
Ureter
Minor calyx
Renal sinus
Renal papilla
Renal cortex
Renal pyramid
The _______ artery carry unfiltered blood into the kidney: it is a lateral branch of the __________ that usually arise just _______ to the origin of the SMA. The left artery is ______ and originates _______ than right artery. The right artery is ______ and passes _________ to the inferior vena cava. Tha arteries are _________ to the veins.
Renal, abdominal aorta, inferior, shorter, higher, longer, posterior, posterior
The _______ veins carry filtered blood out of the kidneys; they are formed by many smaller veins at the ______. They are ________ to the renal arteries; the left vein is _________ than the right, crosses ________ to the abdominal aorta and __________ to the SMA.
Renal, Hilum, anterior, longer, anterior, posterior
The kidneys receive _______% of the cardiac output of blood
20-25
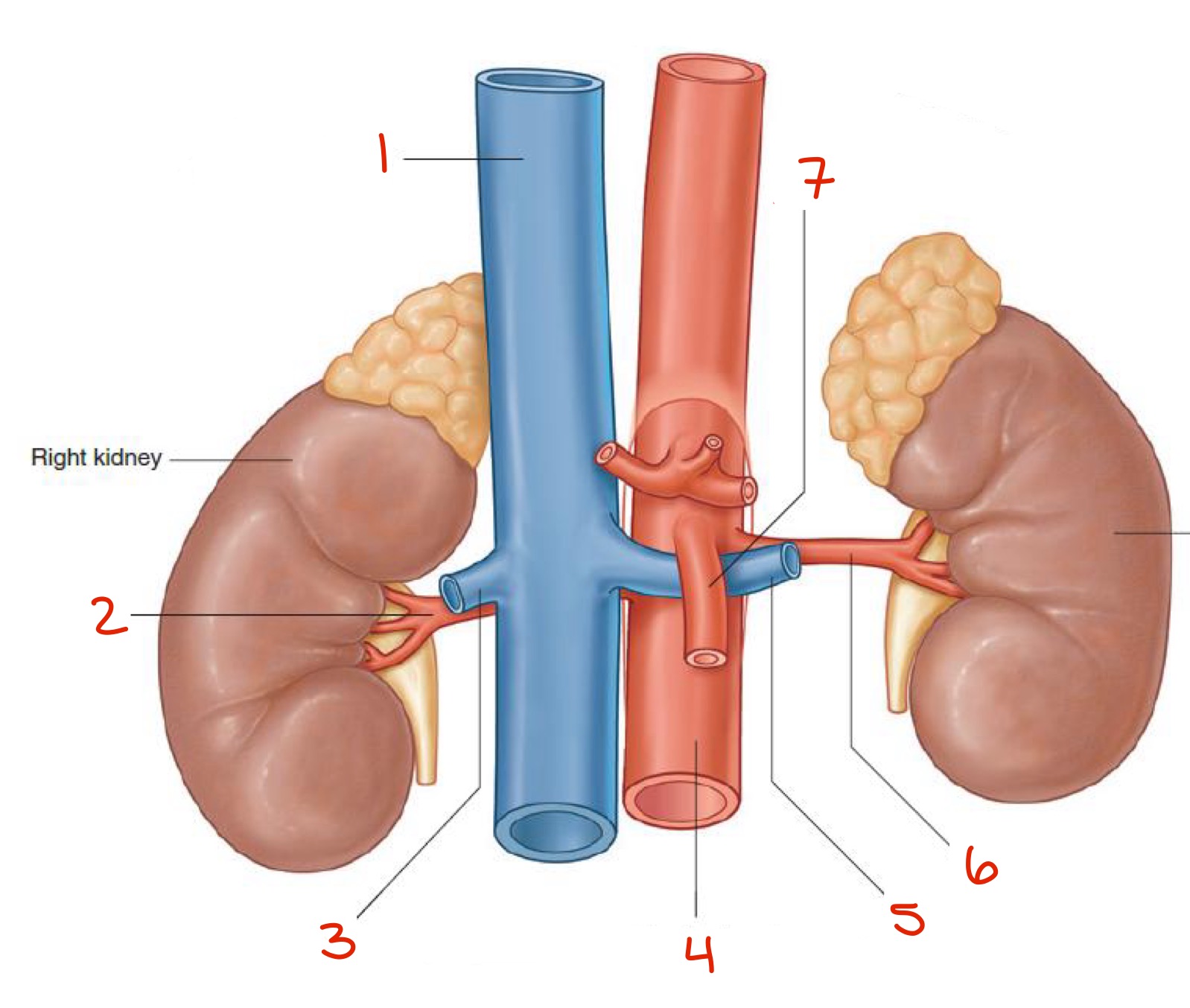
Identify
Inferior vena cava
Right renal artery
Right renal vein
Abdominal aorta
Left renal vein
Left renal artery
Superior Mesenteric Artery
What are the 3 main functions of the kidneys? Describe each one slightly (covered more in physiology)
Produces urine — excretion of waste, excess medicine, organic materials
Filters blood — most of the contents of the blood goes back to the bloodstream, some is excreted as urine
Regulates aspects of homeostasis: blood pressure, water balance, balancing of electrolytes, acid-base balance, RBC production, activation of vitamin D
Essential to clear bacterial components and cytokines from the blood
What are nephrons? (answer very general, again covered in physiology)
They are the functional unit of the kidneys
1-2 million in each kidney
Important in filtration, reabsorption, and secretion
Starts in the cortex and loops down into medulla
What is defined as a kidney lobe?
Renal pyramid + surrounding cortical tissue
Cortical nephrons are primarily responsible for ___________ whereas juxtamedullary nephrons are primarily responsible for ____________.
Excretion and regulation, concentrating and diluting urine
Define and describe (generally) what a glomerulus is
The filtering unit of the kidney
A unique bundle of capillaries lined by delicate fenestrated endothelia, a complex mesh of protein that serve as the glomerular basement membrane, and specialized cells that form the slit diaphragms between interdigitating foot processes
Enclosed in the renal corpuscular capsule, or Bowman’s capsule
What are juxtaglomerular cells?
Cells located in the walls of the afferenr arterioles, that act as baroreceptors, sensing changes in blood pressure, and respond to low BP, low salt diets, and sympathetic stimulation
Ureters are _____peritoneal muscular tubes that transport urine from the ________ to the _______. They are about 25cm long, and 3 mm thick. They are made up of _______ muscle arranged in spiral, longitudinal, and circular bundles
Retro, kidneys, bladder, smooth
The renal pelvis becomes continuous with the ureter at the ______________. The ureter then descends onto the antero-medial aspect of the _________, then cross anteriorly over the ____________, at the division of _________ and _________ to enter the pelvic cavity. The ureter then enters on the postero-lateral wall of the _______
Ureteropelvic junction, psoas major, common iliac artery, external and internal iliac arteries, bladder
How does urine go from the kidneys to the bladder (I.e. what happens)
An increase in pressure (in the kidneys) initiates a peristaltic contraction beginning in the pelvis and spreading downward along the ureter to force urine toward the bladder
What arteries provide blood supply to the ureters?
Renal arteries — upper part
Gonadal and common iliac arteries — middle part
Branches of the internal iliac arteries — lower part
Give characteristics of the bladder, in general
Is the most anterior element of the pelvic viscera
Sub/Infra peritoneal
Shaped like a 3 sided pyramid that has tipped over to lie on one of its margins
Becomes a pelvic organ after puberty — in the newborn, it’s small and cannot concentrate urine
Hollow, muscular organ that stores urine
Expels urine through the urethra
Describe the anatomy of the bladder
Rugae: folds in the wall of the bladder when it is empty; allows for expansion (they disappear as it expands)
Has 4 layers: mucous coat, sub-mucous coat, muscular coat (contains transitional epithelium and detrusor muscle), and serous coat)
Detrusor muscle: interlaced smooth muscle fibers of the muscular coat — forms the internal urethral sphincter, innervated by parasympathetic fibers (that causes contraction)
T/F:
The cellular thickness of the bladder changes based on how much urine it holds
The bladder most often holds about 1L of urine before the need to urinate (micturition) emerges
True
False → it may hold up to 1L of urine, but the urge to urinate occurs once it contains 200mL (in adults, the normal urge to urinate usually occurs as the bladder exceeds 500 mL)
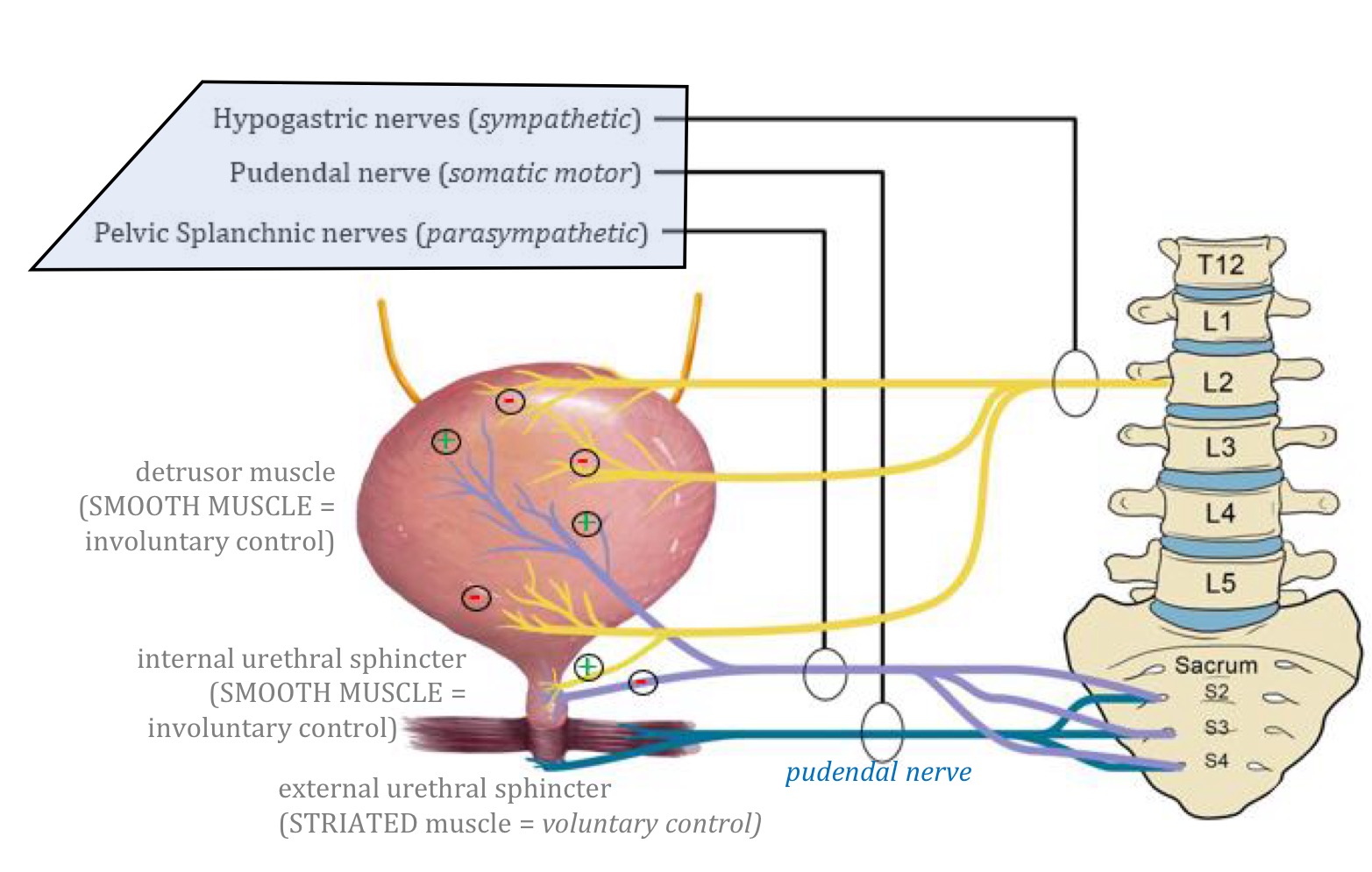
What nerves innervate the detrusor muscle?
S2-S4 parasympathetic fibers via the pelvic splanchnic nerves
What is the trigone?
An area of increased sensitivity to stretch
Triangle formed by two ureteral openings and internal urethral sphincter
Give some differences between the external and internal urethral sphincters
Location: internal is at base of the trigone/bladder, external is in the deep perineal space of the urogenital diaphragm
Muscle type: internal is smooth muscle (involuntary), external is striated muscle (voluntary)
Innervation: sympathetic innervation for internal, autonomic innervation (pudendal nerve S2-4) for external
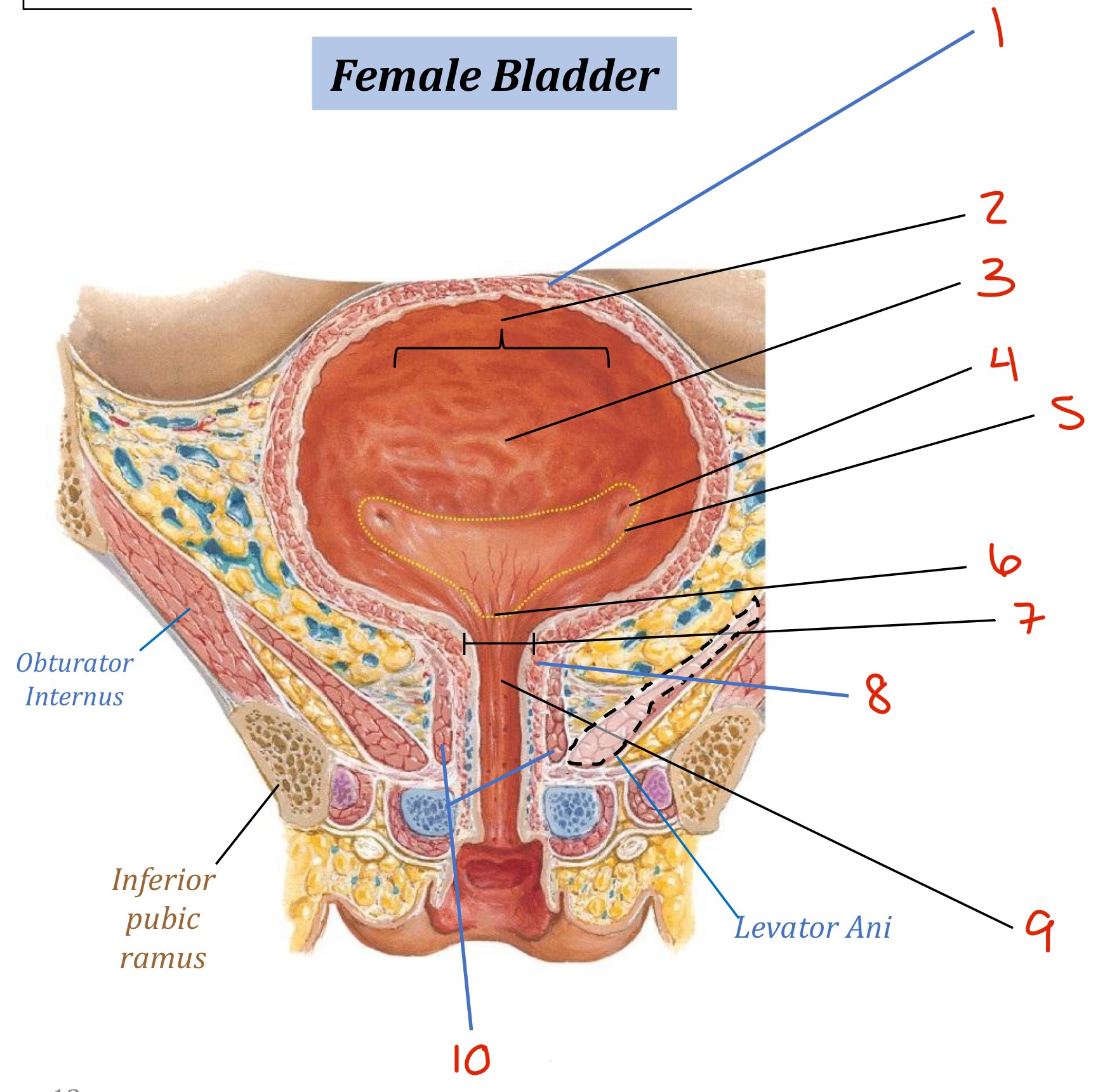
Identify
Detrusor muscle
Body of the bladder
(Urothelium) Rugae
Ureteral opening
Trigone
Urethral opening
Bladder neck
Internal Urethral Sphincter
Urethra
External Urethral Sphincter
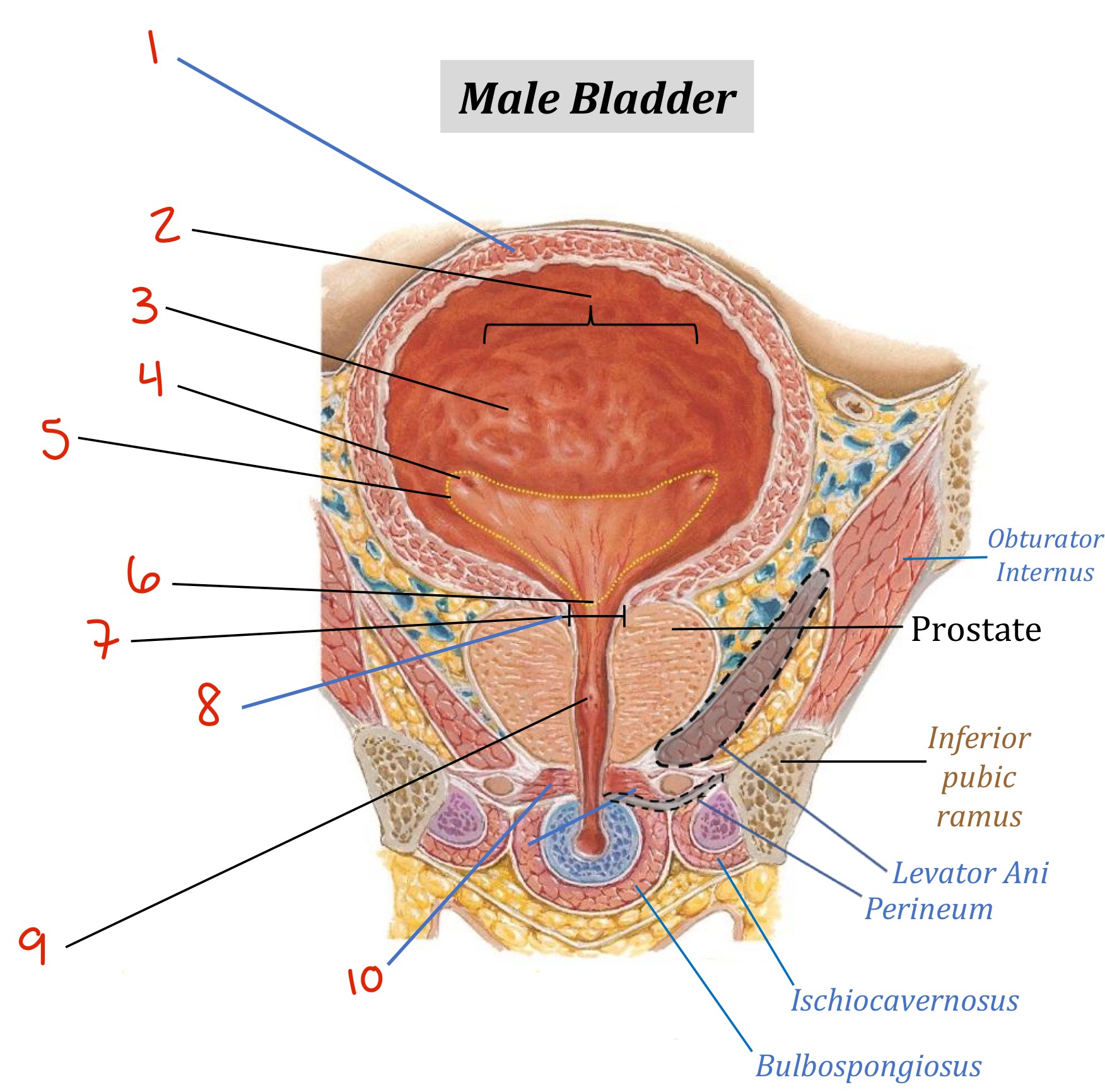
Identify
Detrusor muscle
Body of the bladder
(Urothelium) Rugae
Ureteral opening
Trigone
Urethral opening
Bladder neck
Internal Urethral Sphincter
Urethra
External Urethral Sphincter
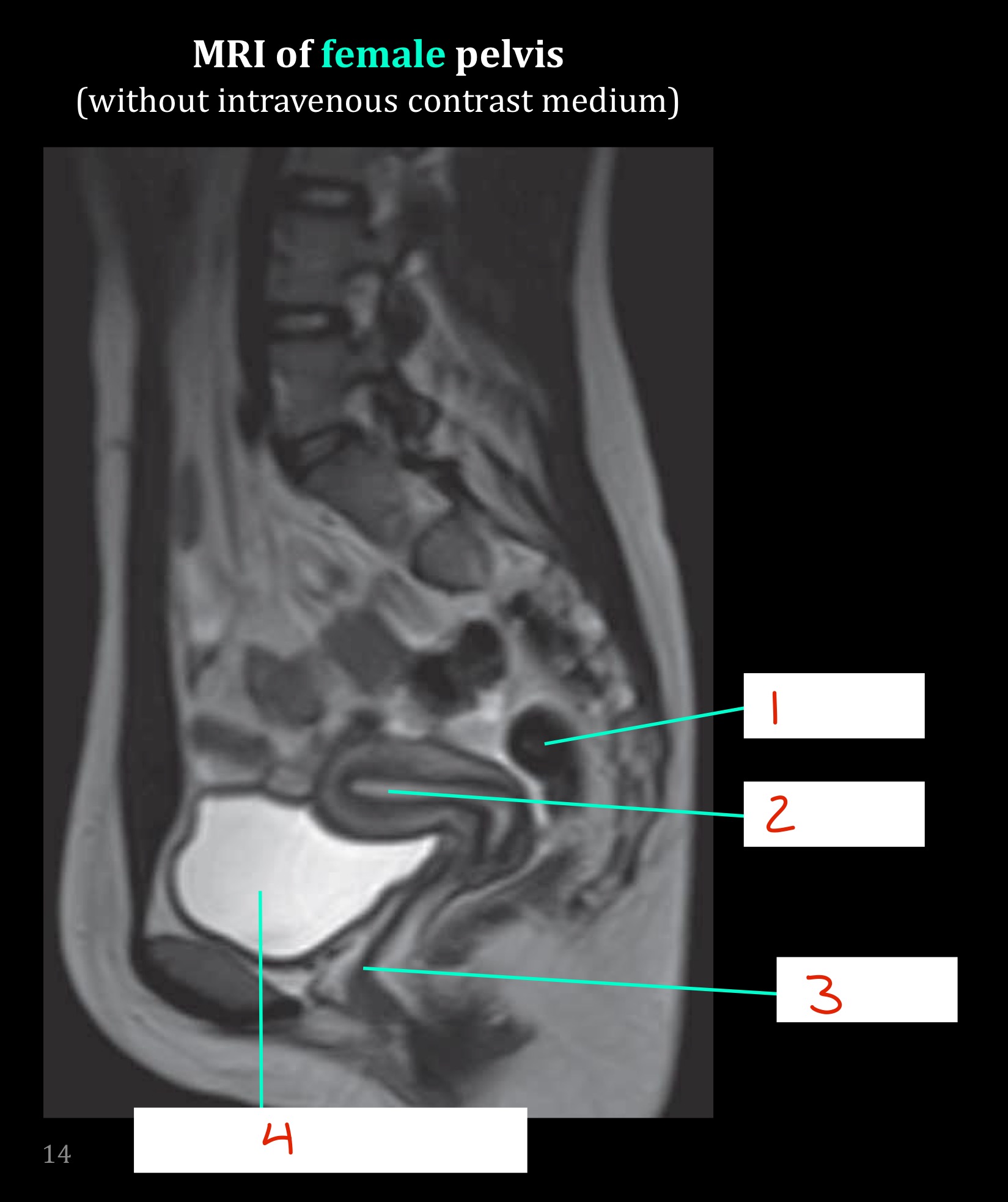
Identify
Rectum
Uterus
Vagina
Urinary bladder
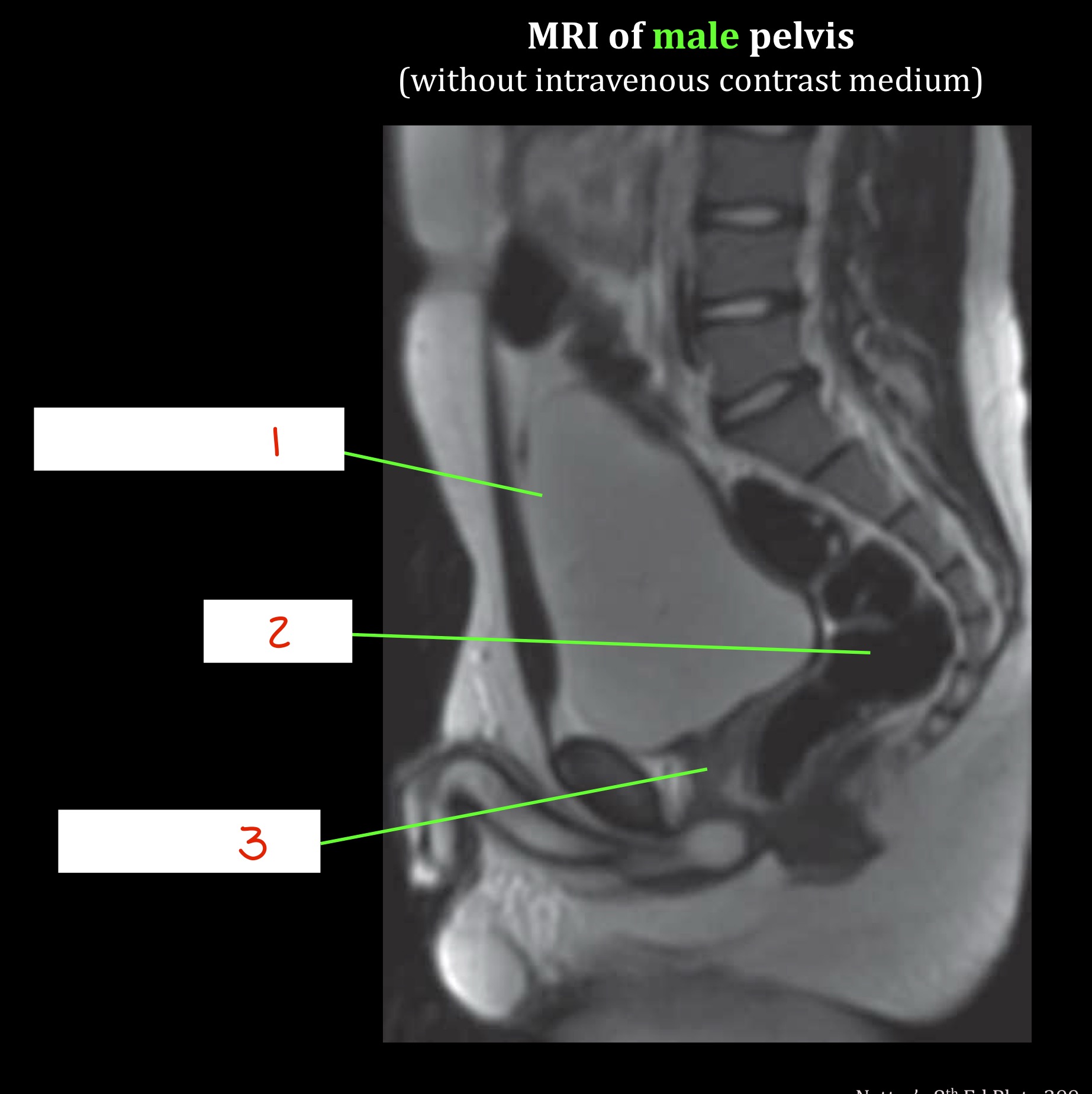
Identify
Urinary bladder
Rectum
Prostate gland
What artery/ies provide the primary and supplementary supply of blood to the female bladder ?
Primary: superior vesical artery (from internal iliac (anterior trunk) → umbilical →)
Supplementary: vaginal artery, obturator artery, inferior gluteal artery
What artery/ies provide the primary and supplementary supply of blood to the female bladder ?
Same as female, but vaginal artery → inferior vesical artery
Describe the innervation of the bladder
Pelvic splanchnic nerves primarily relay somatic sensory information regarding bladder wall stretch
Parasympathetic Fibers :
S2-S4 spinal cord via the pelvic splanchnic nerves and inferior hypogastric plexus
Provide MOTOR innervation the the detrusor muscle = promotes contraction of the detrusor muscle
Inhibit contraction of the internal urethral sphincter
Sympathetic Fibers:
Conveyed from lower thoracic and upper lumbar spinal cord via the sacral splanchnic nerve to the hypogastric plexus and nerves
Promotes contraction of the internal urethral sphincter
Helps inhibit detrusor contraction during early filing phase