Urinary System A and P II
1/136
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
137 Terms
Main job of the system?
Filter blood to make urine
What do kidneys do
filter
What do the ureters do?
carry urine
What does the bladder do
store urine
What does the urethra do?
Relase urine
Where are the urinary system organs located
retroperitoneal
Important Kidney functions?
Balance chemicals
Control pH
Control blood pressure
Make hormones
Remove drugs and hormones
How does the urinary system control pH?
Acid-base balance, adjust H+ and bicarbonate (HCO3)
How does the urinary system control blood pressure?
Release or keep water, release renin (increase BP)
What does the hormone EPO and Calcitrol do?
EPO: makes red blood cells, Calcitrol: absorb calcium
Hilum of Kidney
entry and exit for blood vessel and ureter
layers around kidney
Fibrous capsule: protective layer, inner
Perinephric fat: cushion and support
Renal Fascia: holds kidney in place
Paranepheric fat: outer cushion
Renal cortex is located
outer
Renal medulla is located
inner
Renal Pyramid
structures within the renal medulla that contain nephron loops and collecting ducts, involved in urine formation.
Renal papilla
the tip of the renal pyramid that drains urine into the minor calyx.
Renal lobe
functional unit to make urine, cortex + medulla +collum
Renal collum
cortex tissue between pyramids
Renal sinus made of and does what?
made up of minor and major calyx and pelvis, open space for urine drainage
The minor calyx drains one
pyramid/medulla
Renal pelvis is merged
major calyces and mergers at medial edge with ureter
minor calyx merges to form>…. them merges with→ …
major calyxand then the renal pelvis.
What is the nephron composed of (2 things)?
renal corpuscle and renal tubule
Border between cortex and medulla called?
cortical medullary junction
What is a nephron?
microscopic filtration unit that makes filtrate
Renal corpuscle description and components
bulbus region for filtration site, afferent and efferent arterioles, glomerulus
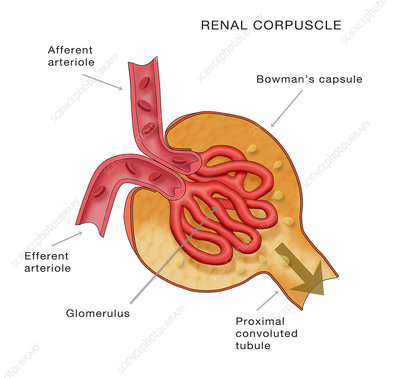
Glomerulus is a ball of what?
capillary ball
What are the capsules of the glomerulus and what is their permeability
visceral layer (permeable inner), parietal layer (impermeable), capsular space in between
The afferent arteriole is always going to be … than the efferent arteriole
larger
What happens at the renal tubule of the nephron?
Processing
3 parts of renal tubule and their cells types
PCT (proximal convoluted tubule): simple cuboidal epithelium with micro villi (high surface area)
Nephron loop: descending and accessing limb, simple cuboidal and simple squamous
Distal convoluted tubule: simple cuboidal without microvilli that goes to collected tubule
Types of nephrons and amount
cortical (85%) and juxtamedullary (15%)
Describe cortical nephrons
short loop, with renal corpuscles near peripheral cortex
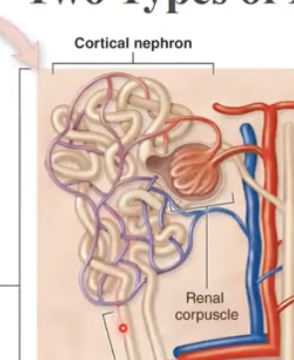
Describe juxtmedullary nephron
next to the medulla, long loop, forms salt gradient in intersitial space
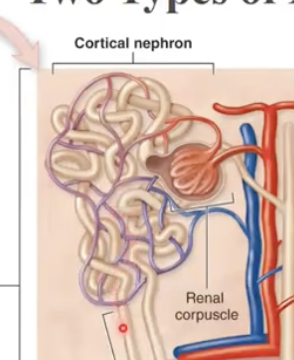
Orders nephrons drain into (3 parts)
collecting tubule→ collecting duct→papillary duct
2 specialized cells in tubule/duct
principal cells and intercalated cells
Principal cells
hornone control for don’t pee, ADH and aldosterone
intercalated cells
regulate pH of blood and urine, type A: remove acid (H) and type B: remove base (HCO3)
Specialized juxtaglomerular apparatus cells
Granular cells
Macula densa cells
extraglomerular cells
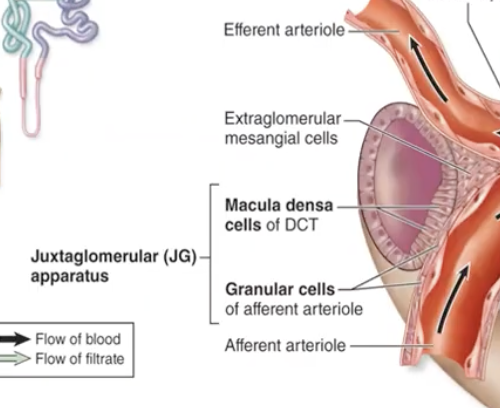
Granular cells location and their function
in afferent arteriole, contract with sympathetic stimulations, dont pee signal (renin!)
Macula densa cells location and function
in DCT, sends signals to granular cells based on NACL concentrations
Extraglomerular mesangial cells location and function
contract!, inbetween afferent arteriole and DCT
Steps of artery flow through kindey
in: renal artery→segmental artery→interlobar artery→arcuate artery→interlobular artery→afferent arteriole→glomerulus→efferent arteriole
flow of filtrate starts where?
capsular space
What is fluid called when it can no longer be acted on?
urine!
What happens in glomerular filtration?
Substances are moved from blood within the glomerulus into the capsular space
What happens during tubular reabsorption?
bring back in body, substances move from tubular fluid back to blood
What happens during tubular secretion?
stuff your body wants to get rid of (out of body), substance from blood go to tubular fluid
Filtration membrane of glomerular characteristics
pours, thin, negatively charged
3 layers of filtration membrane (glomerular)
Endothelium (inner)
Basement membrane
Visceral layer
Endothelium of glomerulus description
fennestrated, allows plasma and dissolved substances to be filtered
Basement membrane of glomerulus description
glycoprotein and proteogylcan molecules
visceral layer of glomerular capsules description
outermost, pedicels, flirtation slits and podocytes
Podocytes what are they and what do they do?
extensions of pedicels wrap around glomerular capillaries, thin spaces called filtration slides, don’t allow most small proteins in
What gets through filtration membrane mostly?
water, glucose, amino acids, ions, very small amounts of protein (no big stuff and no charge)
What cannot get through filtration membrane?
Large proteins and different blood cells (white and red)
3 types of substance in blood and description
Freely filtered (small stuff get through easy)
Not filtered (larger stuff doesn’t enter like blood cells)
Limited Filtration (normally blocked, small medium proteins maybe no charge stuff)
Mesangial cells in filtrate of glomerulus
squeeze afferent arteriole to regulate blood flow and glomerular filtration rate.
glomerular hydrostatic pressure increases with increased
blood pressure
blood colloid osmotic pressure (OPg) is and does what?
osmotic pressure exerted by dissolved solutes, pulls fluid into glomerulus
Capsular hydrostatic pressure is and does what?
The push back in from pressure in capsule does to filtrate, stops additional fluid movement
Glomerular hydostatic pressure is and does what?
the blood pressure inside glomerulus, pushes water and some solutes out of glomerulus
Glomerular hydrostatic pressure has a … blood pressure than systematic capillaries
higher
What is net filtration pressure and what does it determine?
the difference between driving and opposing forces, determines if filtration occurs
If net filtration pressure is positive what happens?
filtrate turns into tubular fluid (push overcomes pull back in)
GFR is the rate of
which filtrate is formed
If your blood pressure increases your … increase
NFP
intrinsic controls what is it and 3 diff types
happening in the kidney maintain constant bp and GFR
1.Myogenic response
Tubuloglomeruluar feedback mechanism
Myogenic response
intrinsic control of smooth muscles in arteriole, decrease bp→ vessels dilate more blood in glomerulus (opposite for increased)
Tubuloglmerular feedback mechanism
backup to myogenic response if bp is increased really high, NaCL in tubular fluid increases so vasoconstriction will occur even more!
If you dilate afferent arteriole, you make … urine
more!
Extrinsic controls are
neural and hormonal control
What is the effect of sympathetic stimulation on GFR?
↓ GFR → ↓ urine → ↑ blood volume (renin release)
How does sympathetic stimulation affect renal arterioles?
Vasoconstriction (afferent & efferent)
What triggers ANP release?
↑ heart chamber stretch
Effect of ANP on kidneys?
↑ GFR → ↑ urine → ↓ blood volume (no renin release)
Maintaining GFR is what kind of regulation?
Intrinsic auto regulation
Parasympathetic increases or decreases GFR
increases
Substgances are … when moved from blood to nephron
secreted
substances are … when they move from nephron back to blood
reabsorbed
What ever is not reabsorbed back to blood is excreted as …
urine
Where does the most reaborptiuon occur
PCT
What is paracellular transport?
movement between epithelial cells
What is transcellular transport?
movement of substances through epithelial cells
Transcellular transport uses:
pumps
pumps work … concentration gradient
against
Channels goes … concentration gradient
with
Carriers use energy from other
ions
How much of glucose do you reabsorb?
100%
How much of proteins do you reabsorb?
100%
How much of sodium is reabsorbed in the PCT
65%
How much of sodium is reabsorbed in nephron loop?
25%
How much of sodium is reabsorbed in DCT?
5%
What hormone causes the insertion of pumps?
Aldosterone
What hormones increase Sodium reabsorption?
aldosterone, cortisol, estrogen, growth hormone, thyroid hormone, insulin
What hormones decrease NA reabsorption?
ANP, progesterone, parathyroid hormone, glucagon
What are aquaporins?
Water channels
Common substances that are reabsorbed
potassium, calcium and phosphate, hydrogen ions and bicarbonate ions
What are calcium and phosphate regulated by .. and does what?
parathyroid hormone (releases phosphate and reabsorb calcium)
What secretes potassium?
aldosterone and principal cells