infection prevention and control
1/15
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
16 Terms
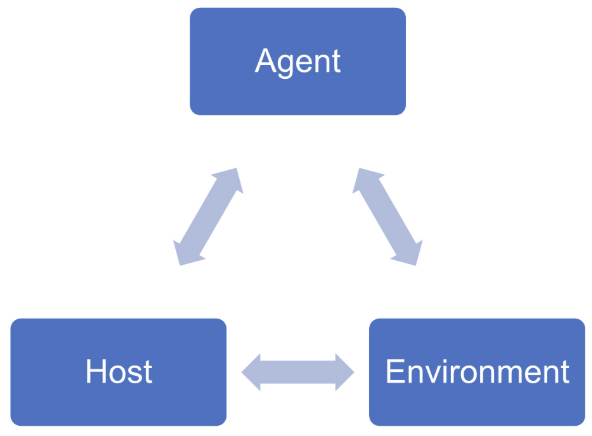
what is the epidemiological triad
three components that must interact for infection to occur
agent → organism that causes the disease, reside in humans, animals or environmental surfaces
host → target of the disease
environment → the surroundings and conditions external to the host, which allows transmission of the disease
the transmission pathways can be direct or indirect
what is route of transmission
organism moving from one host to another. can occur through direct contact to the susceptible host via
contaminated surfaces
respiratory droplets
airborne droplets
susceptible host is typically an individual with compromised immunity e.g. patients that are
elderly
have undergone surgery
have chronic illness
what are the different routes of transmission
Contact Transmission → via direct touch or indirectly through contaminated surfaces and medical equipment.
Droplet Transmission → large respiratory droplets traveling short distances during coughing or sneezing
Airborne Transmission → smaller particles that remain suspended and travel long distances in the air.
what are the different ways we can control the spread of infection
behaviour change → condoms to reduce STDs, regular handwashing, healthy diet, use of insect repellants
vaccines → reduction and eradication of diseases, herd immunity
medication → treat infection, prevent infection before or after exposure to a disease (pre and post-exposure prophylaxis)
surveillance → monitor disease and characterise disease patterns to detect outbreaks and guides the prioritisation development and evaluation of disease control programs in countries, also guides formularies
environment → control or eradicate mosquitoes, safe supply of water, improving sanitation and hygiene
infection control → sterilisation pf equipment, PPE, isolating infectious patients
why is hospital environment important
hospital is where serious illnesses are treated and also where antibiotic-resistant infections are particularly likely to develop and spread.
Infections acquired in hospitals and other health-care facilities are called nosocomial infections
Resistant bacteria exert a heavy toll in terms of illness and mortality, as well as added direct and indirect costs.
the key to limiting risk is the intense measures for the prevention and control of infection
what are infection prevention and control (IPC) measures
prevent the spread of pathogens, including those with AMR, within and between health-care facilities, and from facilities to the community
there is a legal requirement to implement “The Code of Practice on the prevention and control of infections” → trusts must have clear arrangements for the effective prevention, detection and control of Healthcare associated infection (HAI), including the procedures to be taken in the event of an outbreak of infection.
In addition to the standard IPC measures, there are specific recommendations concerning AMR pathogens.
importance of containing Healthcare Associated Infections, HAI
HAIs can develop either as a direct result of healthcare interventions such as medical or surgical treatment, or from being in contact with a healthcare setting.
HAI covers a wide range of infections. The most well-known include those caused by methicillin-resistant Staphylococcus aureus (MRSA) and Clostridium difficile (C. difficile).
HAIs pose a serious risk to patients, staff and visitors. They can incur significant costs for the NHS and cause significant morbidity to those
infected.
importance of screening and prevention for colonisation
Screening for Multidrug-Resistant Organisms
Screening identifies carriers of multidrug-resistant organisms like MRSA and CPE (Carbapenemase-Producing Enterobacterales) upon hospital admission to prevent spread.
Difference Between Colonisation and Infection
Colonisation means presence without symptoms, while infection involves symptomatic disease requiring treatment.
Benefits of Early Detection
Early detection enables isolation precautions, reducing transmission risk and preventing outbreaks.
Impact on Patient Safety and Costs
Screening protects vulnerable patients and reduces healthcare costs by minimising treatment and containment needs
what are standard infection and control measures
Hand Hygiene
Respiratory Hygiene (when coughing or sneezing)
Personal Protective Equipment → using the right gloves, gown, mask and eye protection from the pathogen you are protecting yourself and the patient from
Occupational Exposure management including Sharps
Management of Care Equipment
Safe Care of Linen including Uniforms
Control of Environment
Safe Waste Disposal
what is isolation of patients
isolating patients who are colonised or infected with resistant organisms
involves application of specific contact precautions/personal protective equipment
Group several similarly affected patients in a bay. However, isolation in single rooms is not always feasible.
what is Clostridioides difficile infection (CDI)
usually develops when you're taking antibiotics, or when you've finished taking them within the last few weeks. The most common symptoms are:
watery diarrhoea, which can be bloody
painful tummy cramps
feeling sick
signs of dehydration, such as a dry mouth, headaches and peeing less often than normal
a high temperature (fever) of above 38C (100.4F)
loss of appetite and weight loss
what are the risk factors for C dificil
Have been treated with broad-spectrum antibiotics or several different antibiotics at the same time, or those taking long-term antibiotics
Have had to stay in a healthcare setting, such as a hospital or care home, for along time
Are over 65 years old
Have certain underlying conditions, including inflammatory bowel disease (IBD), cancer or kidney disease.
Have a weakened immune system
Taking a PPI
Have had surgery on their digestive system
How is Clostridium difficile contracted?
found in the digestive system of about 1 in every 30 healthy adults. the bacteria often live harmlessly because the other bacteria normally found in the bowel keep it under control
Antibiotics can interfere with the balance of bacteria in the bowel, which can lead to C. difficile bacteria multiplying and produce toxins
C. difficile can spread easily to other people because the bacteria are passed out of the body in the person's diarrhoea.
Once out of the body, the bacteria turn into resistant cells called spores.
These can survive for long periods on hands, surfaces (such as toilets), objects and clothing unless they're thoroughly cleaned.
Infectious until at least 48 hours after symptoms have cleared up
summary of roles and activities at hospital level

what are the typical activities of the IPC team
core members generally include
Director of Infection Prevention & Control (DIPC): senior figure, often a Chief Nurse or Consultant, who leads the overall strategy.
Consultant Microbiologists/Virologists: Medical doctors who provide expert clinical and laboratory advice.
Infection Prevention and Control Lead Nurses/Specialist Nurses/Practitioners: A team of nurses dedicated to implementing policies, providing education, conducting surveillance, and managing outbreaks.
Surveillance Officers/Analysts: Staff responsible for collecting, analysing, and reporting infection data
what are the responsibilities of the infection control team
Staff education and training
Policy and guideline development e.g. MRSA Screening
Producing patient information leaflets and visiting patients on request
Co-ordinating the annual infection prevention and control audit
Surveillance of specific healthcare associated infections (HAI) e.g. MRSA bloodstream infections and Clostridium difficile infection
Investigating outbreaks and co-ordinating control measures
Working closely on issues related to cleanliness of environment and equipment
Participating in evaluation of new technology link and supporting national infection prevention and control collaborative projects.