1019DOH - Applied Oral Biology (ORAL HISTOLOGY)
1/125
Earn XP
Description and Tags
hello! this is for the real ones lmao:) please study these unshuffled! they're meant to be in sequence. we got this YEAHH
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
126 Terms
what is the stomodeum?
the small distance between the heart and head in an embryo of 5-6 weeks in utero
stomodeum alternative name
primitive oral cavity
3 germ layers of the 5-6 WIU embryo (WIU = weeks in utero)
ectoderm
mesoderm
endoderm
ectoderm germ layer of the embryo
external lining of the body and oral cavity later on
epithelial in origin
anything we can touch (eg. eyes, hair, nails, skin) is this
mesoderm germ layer of the embryo
connective tissue in origin (eg. blood, bone, cartilage, muscle)
anything inbetween guts and epithelium is this
endoderm germ layer of the embryo
lines internal organs (guts)
not supposed to be exposed to the external environment
anything related to the GI (gastrointestinal) system is this
starts from pharynx and travels down
all 3 ____ ______ are needed for an embryo to develop
germ layers
what are the different embryonic origins of the tissues found in the oral cavity?
enamel) external layer, epithelial in origin ∴ ectoderm
dentin, pulp, cementum, PDL, alveolar bone) connective tissue ∴ mesoderm
NO ENDODERM (no guts in teeth lol)
what 2 layers form the ectoderm? (think microscopically)
what does the ectoderm lay above?
a layer of superficial flat cells
a layer of lower columnar cells
ectoderm rests on a basement membrane and then a lower layer of connective tissue (mesoderm)
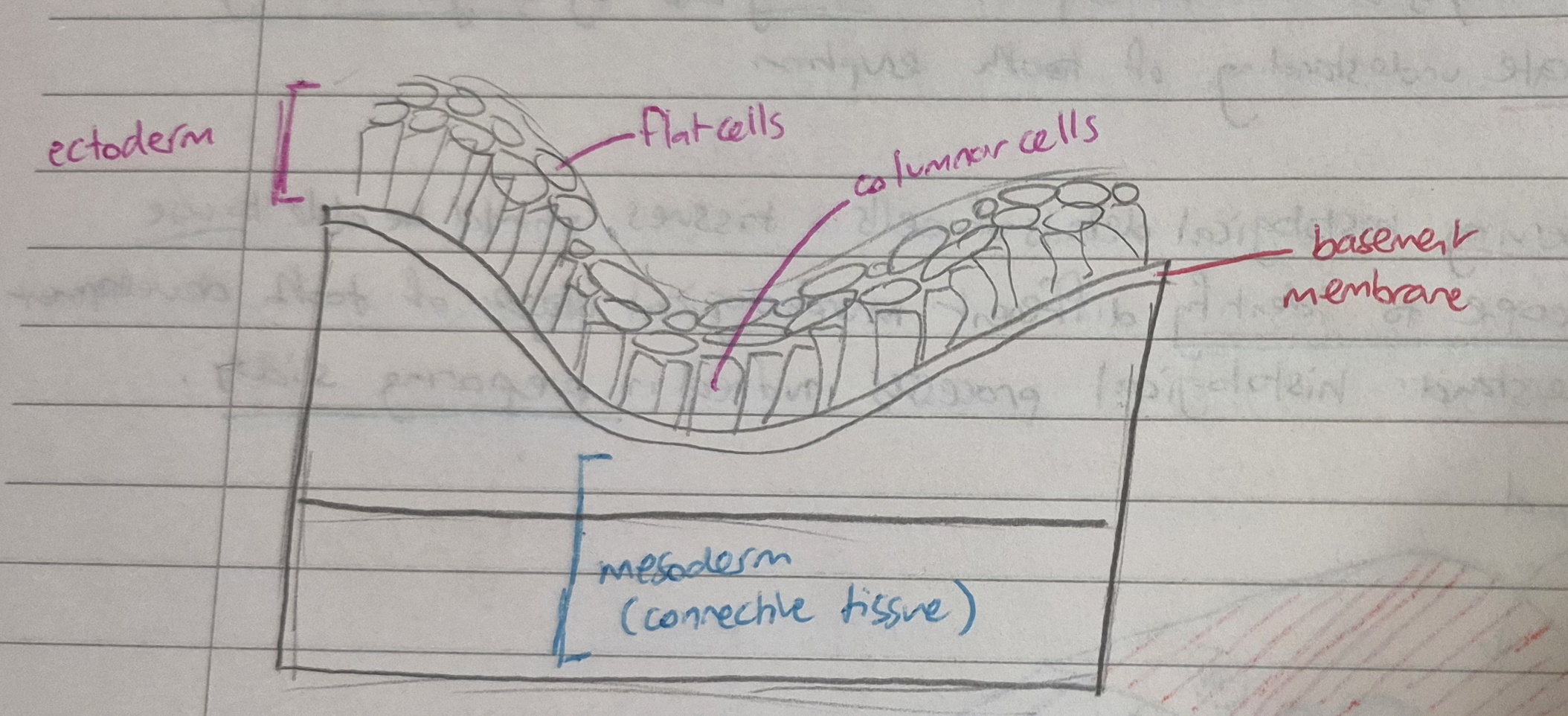
what does it mean if the basement membrane breaks?
early signs of malignancy
mixture of ectoderm and mesoderm is very bad (except in some embryological events)
from both ectoderm and mesoderm, the ____1___ (derived from mesoderm) is formed, which all __2___ and ___ ___3______ are formed from.
mesenchyme
teeth
oral structures
the development of ______ ____ ______ is the only development that precedes tooth development
neural crest cells
when do neural crest cells appear….
during embyrological development?
physically on the embryo?
during CNS development (CNS = central nervous system)
at the top of neural grooves (at the crest of the groove)
neural crest cell properties
(note: neural crest cells will be referred to as NCC’s from now on)
ectodermal in origin
ability to migrate to other tissues
can differentiate into other cell types
can send signals to neighbouring tissues and tissues they migrate to
why are NCC’s important?
act as a leader during embryological development
have different abilities (eg, ectodermal in origin like nervous tissue and can move and migrate like stem cells)
when they move, they send signals to migrated to and surrounding tissues
NCC’s migrate from the __1__ surface of the embryo to the ___2____, where they reside in the ____3____ to change it to the _____4______.
dorsal
stomodeum
mesenchyme
ectomesenchyme
after NCC’s migrate to the mesenchyme, where will they reside?
below the basement membrane
when NCC’s migrate to the mesenchyme, why does the name change from mesenchyme to ectomesenchyme?
NCC’s are ectodermal in origin - ‘ecto’ in ectomesenchyme refers to this
mesoderm (mesenchyme) is pure connective tissue
but because the NCC’s have travelled there it isn’t pure connective tissue anymore
this is why the name changes
ectomesenchyme is needed to develop a tooth. why?
enamel is ectodermal in origin
PDL, alveolar bone, periodontal ligament, cementum, pulp and dentin are all mesodermal (connective tissue) origin
ectomesenchyme is both ectoderm and mesoderm which is why it is needed to develop all above structures
once NCC’s reside in the ectomesenchyme, what do they do and what does this affect?
start sending signals to migrated to and surrounding tissues
signals therefore affect not only the mesenchyme but the ectoderm on top too
the embryo is flattened ____-_______
dorso-ventrally
what are branchial arches?
six finger-like projections that extend from the ectoderm of the foregut to the outer ectodermal lining
lined by ectoderm on outside, endoderm on inside and mesoderm inbetween
ONLY FIRST BRANCHIAL ARCH LINED BY ECTODERM ON THE INSIDE AND OUTSIDE
contain all information for developing organs
why is the first branchial arch lined by ectoderm on the inside and outside?
because the first branchial arch develops into all structures in the head
endoderm is for guts, and the head doesn’t need it
this is why its lined by ectoderm on the inside and outside
what do the 2nd, 3rd/4th, 5th/6th branchial arches contain the information for?
2nd: neck
3rd/4th: thorax
5th/6th: anything below (guts/lower limbs)
what are clefts in branchial arches? what are they lined by?
depressions between branchial arches from the outside
lined by ectoderm
what are pouches in branchial arches? what are they lined by?
depressions between branchial arches form the inside
lined by endoderm (except between 1st and 2nd arches where lined by ectoderm - no need for endoderm in the whole head area including the oral cavity)
flip card over for transverse section of a branchial arch
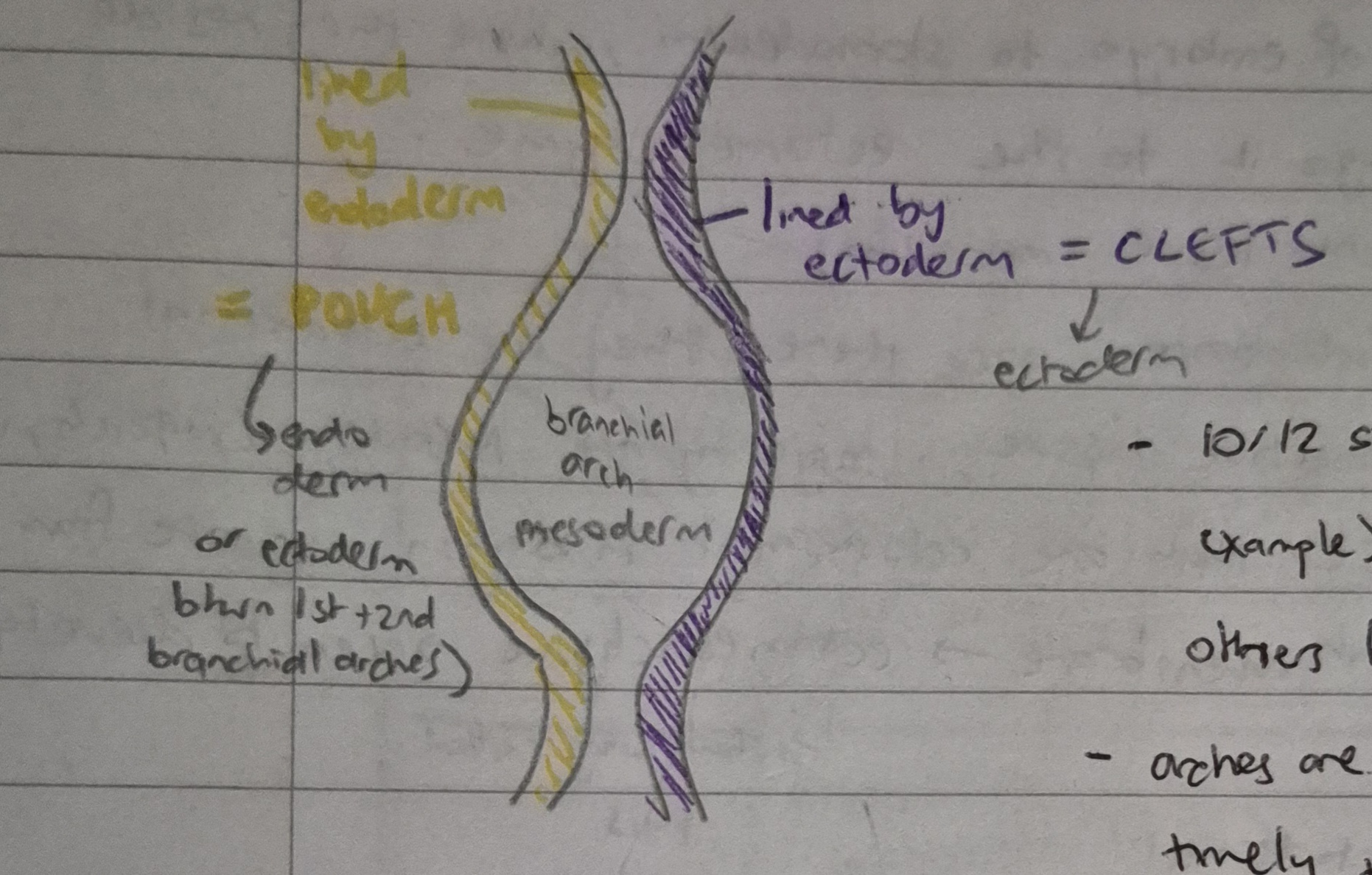
6 derivatives of the first branchial arch (mandibular arch)
mandible and maxilla
lower lip, part of upper lip and cheek
all teeth
all salivary glands
all masticatory muscles
anterior 2/3rds of the tongue
all structures derived from the same branchial arch will share the same…
nerve and blood supply
how many branchial arches (and therefore, how many nerve supplies) form the tongue?
3 branchial arches form the tongue
therefore, there are 3 nerve supplies
structures from the first branchial arch are supplied by the ____1____ nerve or a branch of this nerve, therefore, the first branchial arch can also be called the _______2_ ____
mandibular
mandibular arch
the first branchial arch is directly below the…
stomodeum (primitive oral cavity)
the anterior 2/3rds of the tongue is formed from the first branchial arch. which nerve is its sensory nerve supply?
the lingual nerve (branch of mandibular nerve)
what is Meckel’s cartilage?
runs from where to where
guides development of…
remnants will leave how may ligaments and bones behind?
Meckel’s cartilage is the cartilage within the mesodermal part (centre) of the mandibular arch
runs from the middle ear to the mandible ( ∴ follows shape and structure of mandible)
guides development of mandible but doesn’t contribute that much to it (can still develop a mandible without Meckel’s cartilage)
remnants will leave 2 ligaments and 4 bones behind
list the structures derived from Meckel’s cartilage remnants
incus and malleus
lingula of the mandible (spiky bit on inner side of mandible - guards entrance of mandibular foramen)
mental ossicles (at midline, aka genial tubercles, are 4 little bones on lingual side of mandible)
sphenomandibular ligament
fill this in:
1st branchial arch (_____1____ arch) → ____2__ nerve (or branch of)
2nd branchial arch (__3___ arch) → __4___ nerve (or branch of)
mandibular
mandibular
hyoid
facial
name the stages in tooth development in order
dental lamina
bud
cap
bell
eruption
describe the formation of dental lamina
(this is step 1 of tooth development)
note: phrase highlighted in yellow is something you need to include when you start any stage of tooth development (will appear from this card onward when describing tooth formation steps, so keep an eye out 👀)
under influence of the NCC’s, downward proliferation of ectoderm forms two dental laminae
dental laminae appear as band-like structures
NCC’s do this by sitting in the mesenchymal area and signalling to the ectoderm to proliferate downwards
one lamina carries the upper deciduous teeth
the other lamina carries the lower deciduous teeth
describe the bud stage
(this is step 2 of tooth development)
under influence of the NCC’s, 10 rounded projections/buds (enamel organs) appear on the labial surface of the dental lamina (corresponding to 10 deciduous teeth!)
each bud is surrounded by a mesenchymal condensation (which is the dental papilla and the dental sac)
each lamina (from step 1) have 10 tooth buds each
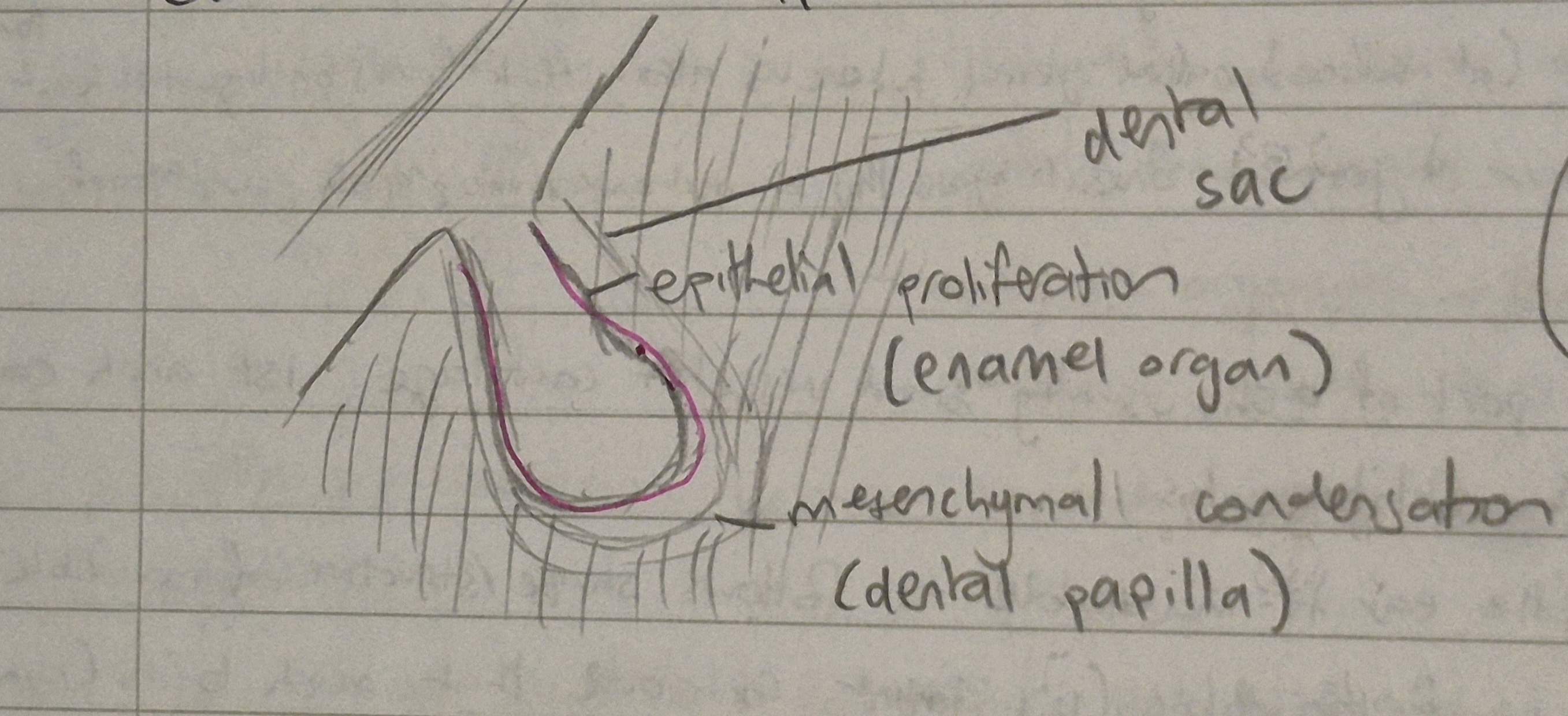
the enamel organ in the bud stage of tooth formation is the __1_dermal part, and eventually forms the ___2___
ecto
enamel ;)
in the bud stage, the dental papilla (mesenchymal condensation) eventually forms what under the influence of the NCC’s?
the dental papilla forms dentin and pulp of the tooth
the dental sac in the bud stage is ________/________ in origin, and forms what 3 structures to connect the tooth to the outside environment?
mesenchymal/mesodermal
cementum, PDL and alveolar bone
the tooth germ is formed of three parts. what are they? what are their dermal origins?
enamel organ (ectoderm in origin)
dental papilla (mesodermal in origin)
dental sac (mesodermal in origin)
what is the difference between the enamel organ and the tooth germ?
the enamel organ is 1 of 3 parts forming the tooth germ
the tooth germ is all 3 parts
which tissue in the tooth germ (bud stage) is ectodermal in origin?
the enamel (derived from the enamel organ)
describe the early cap stage
(this is step 3 of tooth development)
note: there’s 2 parts to this stage and this is the first. the second part of this stage will be called the ‘late cap stage’
under influence of NCC’s, the enamel organ of the bud stage undergoes unequal growth to change in shape from a bud to a cap
enamel organ during this stage has its inner surface lined by columnar cells, called inner enamel epithelium or the inner dental epithelium
the outer surface is lined by cuboidal cells and is called the outer enamel epithelium or the outer dental epithelium
inner and outer dental epithelium meet at the cervical loop
what structures form above and below the cervical loop?
above the loop: crown of the tooth
below the loop: root/s of the tooth
true or false?
the inner and outer epithelium have the same functions as each other (cap stage)
false
they have different functions
in the cap stage of tooth formation, are the tissues hard or soft?
all tissues are soft tissue in this stage
what is morphal differentiation? (cap stage)
the convexity of the outer surface and the overall morphological change to a cap shape
what is histo-differentiation? (cap stage)
in bud stage, you have 2 layers of ectoderm (flat and columnar cells)
but in cap stage, there are more layers. the inner surface is lined by different cells than the outer surface
in the early cap stage, which surface grows at a lower rate?
the inner surface grows at a slightly lower rate than the outer surface
describe the late cap stage
(this is step 3.2 of tooth development)
note: this is the second and final part of the cap stage
polyhedral cells in the middle of the enamel organ change into star-shaped cells called stellate reticulum, due to secretion of a hydrophilic substance called glucosaminoglycans (GAG’s) produced by polyhedral cells
lots of cytoplasm/tissue fluids will be attracted to the polyhedral cells
with no escape route for the fluid, cells change shape to star-like forms (stellate reticulum cells) and form long processes to occupy space and prevent bursting.
desmosomes connect stellate reticulum cells and form a tight network between them
note: the enamel organ is still surrounded by dental papilla and dental sac-like in the bud stage
3 functions of the stellate reticulum cells (cap stage)
resist against physical trauma (as filled with tissue fluid/cytoplasm)
help enamel mineralisation/maturation
distribution of calcium to newly formed enamel
list and describe the 2 transient structures in the cap stage
note: these structures appear in this stage only!
enamel knot and enamel cord
rounded cells that connect inner and outer enamel epithelium
KNOT) thought to determine the future site of the cusp/incisal ridge
CORD) may give rise to another type of cells called stratum intermedium
cell free zone
thin area between enamel organ and dental papilla
separates dental papilla from inner surface of enamel organ
helps cells perform their function
elongate during early and late bell stage
enamel knot and cord and stratum intermedium cells (late cap stage and transient structures)
the enamel knot and cord will eventually disappear (as they are only present in the cap stage)
after the enamel knot and cord pull the inner enamel epithelium to the future site of the cusp/ridge, they will leave remnants
these remnants are called stratum intermedium cells
these cells appear rounded and flat
they appear on top and work with the inner enamel epithelium and help it perform its function
flip card over for a visualiser of the cap stage
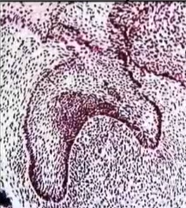
describe the early bell stage
(this is step 4 of tooth development)
note: there’s 2 parts to this stage and this is the first. the second part will be called the ‘late bell stage’
under influence of NCC’s (by giving signals), the IEE align themselves on the future dentino-enamel junction (or, cervical line)
this is so the shape and type of the tooth can be determined during this stage
lingual to the enamel organ of the deciduous tooth, a downward proliferation from the main dental lamina appears, called successional dental lamina, which carries the permanent successor
all changes that occur here are morphal differentiation
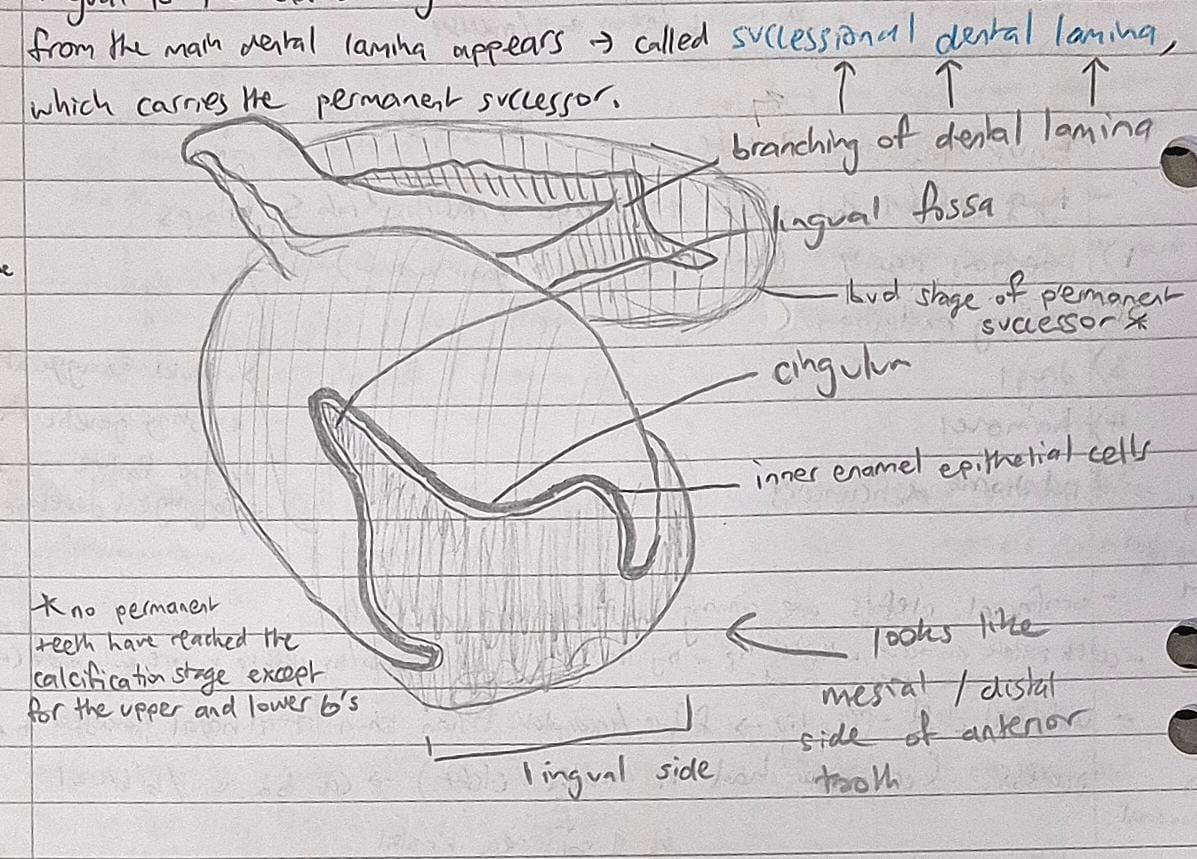
clinical significance of the early bell stage
sometimes kids will have 2 rows of teeth
this happens because the permanent tooth has erupted and the deciduous one hasn’t been shed yet
as a clinician, you should remove the dec. tooth and keep the permanent one
the succession of the dental lamina will always be LINGUAL to the deciduous one.
if there are 2 rows of teeth, which should you pull, the labial or the lingual one?
always pull the labial one
the permanent erupts lingual to the deciduous (dec in front)
you can also look for mamelon presence, do an x-ray or look for size difference to tell as well
this phenomenon occurs more often on the lower jaw around the incisor area
where does histo-differentiation (histological change) take place in during the early bell stage?
in the cells of the enamel organ
describe the histological changes that take place during the early bell stage
the inner enamel epithelium becomes longer
rearrangement of the organelles take place - called repolarisation
these cells are now called preameloblasts (which are ready for enamel matrix formation)
the IEE elongate toward the cell-free zone, leading to its disappearance, so…
preameloblasts come into contact with the peripheral layer of the dental papilla (lots of signalling molecules as ectomesenchyme has inducive properties), leading to the induction of odontoblasts
the odontoblasts start forming dentin matrix
once they create the first few layers, they realise that the preameloblasts haven’t done anything (no enamel matrix is formed)
so they start reciprocal induction to ‘wake up’ the preameloblasts again
stratum intermedium
present 2-3 layers above the preameloblasts
arise from enamel knot and cord (remnants of transient structures)
preameloblasts
rich in alkaline phosphatase
this is an enzyme that helps preserve mineralised tissue and stop reabsorption
_______ formation is always ahead of enamel formation
dentin
what is the reverse of functional polarity?
also known as repolarisation
certain organelles move toward the upper pole/end of the cell while others move downwards
the nucleus and mitochondria move to the top of the cell
while the other organelles move to the bottom of the cell, close to the basement membrane
a '-blast’ cell is a _______ cell
a ‘-clast’ cell is a _______ cell
formative
destructive
describe the physical characteristics of the cell types in the early bell stage (OEE, stellate, DP and DS)
outer enamel epithelium - cuboidal cells (like in cap stage) but shorter
stellate reticulum - same as cap stage but longer processes and smaller cell body
dental papilla - same as cap stage but cell-free zone disappears after elongation of IEE
dental sac - same as cap stage
which two cell types are important for secreting alkaline phosphatase, which is necessary for enamel maturation/calcification?
stratum intermedium
stellate reticulum
what are the 3 differences between the early and late bell stage?
original/main dental lamina has degenerated in the late bell stage
there are 2 types of cells in the dental lamina in the early bell stage. in the late bell stage, epithelial rests of serres or serres pearls appear
they mostly do nothing
in some cases under certain stimulation they multiply and form an eruption cyst
the epithelial rests are remnants of the dental lamina
teeth start developing at the cusps/incisal edges and go down. in the late bell stage, you can see the first few drops of the dentin matrix.
even one drop of dentin matrix changes the early bell stage into the late bell stage
what is the clinical significance of dentin formation being ahead of enamel formation?
if there is a developmental abnormality (eg dentinogenesis imperfecta), then there is a high chance that the enamel will be affected to (amelogenesis imperfecta)
but not vice versa! the stimulus that caused the imperfection may have started during enamel formation period and not dentin, so therefore will ONLY affect the enamel
describe what happens in the late bell stage
(this is step 4 of tooth development)
note: this is the second and last step of the bell stage
the deposition of the 1st layer of the hard dental surface occurs - dentin
the enamel organ loses its connection to the dental lamina
the remnants of the dental lamina are called epithelial rests of serres, or serres pearls
inner enamel epithelium - preameloblasts elongate more to form ameloblasts through reciprocal induction
the stratum intermedium is the same as in the early bell stage
the outer enamel epithelium becomes flat and its plasma membrane becomes folded
this is to increase the surface area available for obtaining nutrition from the dental sac
nutrition from the dental papilla cannot be obtained after deposition of the hard dental structures (enamel + dentin)
as the OEE is epithelial in origin (avascular), it relies on underlying connective tissue for nutrients (ectomesenchyme/mesoderm)
some small blood vessels/capillaries are present here
dental papilla + dental sac are the same as in the early bell stage
what is the clinical significance of serres pearls?
they sometimes can produce a pathology/cyst called an eruption cyst
where and when does root formation start?
starts after complete formation of the crown
i.e) when enamel + dentin formation reaches the future CEJ
starts at the cervical loop
what is the epithelial diaphragm?
a horizontal proliferation formed of IEE and OEE
leads to a primary close of the apex (no calcification yet)
secondary closure takes place through deposition of dentin and cementum at the apex
what is the epithelial root sheath of Hertwig (ERSH)?
a vertical proliferation formed of IEE and OEE that forms the length and shape of the root
a proliferating zone of dental papilla occurs with epithelial diaphragm and ERSH
the peripheral layer of dental papilla is differentiated into ________. these start formation of dentin, and when this occurs, ____ is degenerated.
odontoblasts
ERSH
what are epithelial rests of malassez?
the remnants of ERSH after dentin formation occurs
what happens after the ERSH is degenerated?
dentin is exposed to the dental sac, so UMC’s (undifferentiated mesenchymal cells) differentiate into…
cementoblasts (lay down cementum matrix)
fibroblasts (form periodontal ligaments)
osteoblasts (form alveolar bone matrix)
in most cases the epithelial rests of malassez will do nothing, but under certain circumstances they form…
a pathology/cyst called a periodontal cyst
in case of bi-rooted teeth, _ tongue-like projections develop at the level of bifurcation
in case of tri-rooted teeth, _ tongue-like projections develop at the level of bifurcation
2
3
what are accessory root canals?
caused by early degeneration of ERSH before odontoblasts differentiate
can also form as a result of:
blood vessels interrupting the course of ERSH
failure of fusion of tongue-like projections in multi-rooted teeth (more common)
what are enamel pearls?
caused by late degeneration of ERSH after complete formation of the whole thickness of dentin
leads to enamel formation on the root - an enamel pearl
can also occur in localised places - doesn’t have to be the whole root
IEE will be in contact with dentin for a very long time and will pursue the process of crown formation. why?
IEE will become preameloblasts, then ameloblasts, then enamel along that area
very common on cervical 1/3 of root and around bi/trifurcation area
will appear glowing on an x-ray
when scaling may initially seem like some stubborn calculus under the gingival margin
what is intermediate cementum?
a tissue that has intermediate properties between dentin and cementum
occurs due to degeneration of ERSH after odontoblasts differentiate and before complete thickness of dentin is formed.
(should degenerate after dentin is formed not before)
dentin and cementum are not meant to be forming at the same time during root formation
seen as an anatomical variation
what is dilaceration?
describes teeth with severe curvature of the root
occurs due to trauma of a deciduous tooth pushing the developing tooth germ and bending the ERSH
can happen after the tooth has erupted because roots aren’t fully developed yet
if extracting, will need to break tooth and remove parts separately
root canal - instruments don’t bend severely so will be difficult to do
will need x-rays before procedure
what are the physical properties of enamel?
colour
thickness
hardness
brittleness
permeability
describe physical property 1 of enamel (colour)
yellowish/greyish white (not supposed to be stark white)
canines being darker than incisors is normal
in some teeth, the cervical 1/3 of the tooth is darker than the incisal 1/3 which is more translucent
the darker the enamel the stronger they are (more calcium)
whitening teeth weakens enamel
describe physical property 2 of enamel (thickness)
2-2.5mm at cusp tips/incisal edges (stress bearing areas) - relatively thin
becomes thinner to end as a feather/knife edge on the cervical line
enamel is the highest mineralised/calcified tissue in the human body
structure of enamel based on mineral content and complexity of enamel structure, not thickness
describe physical property 3 of enamel (hardness)
enamel is the hardest calcified tissue in the body due to:
high mineral content (30% more than any other tissue)
complex crystal orientation
note: enamel of permanent teeth is stronger than enamel of deciduous teeth
describe physical property 4 of enamel (brittleness)
very brittle due to large amount of minerals
most hard things are brittle (but doesn’t chip easily because of dentin
dentin, which is less mineralised and brittle compensates for enamel and is necessary as a support for enamel (more elastic, flexible) - acts as a shock absorber
part of the longevity of enamel depends on health/preservation of dentin layers
describe physical property 5 of enamel (permeability)
acts as a semi-permeable membrane for certain ions (especially fluoride ions in saliva)
bigger molecular weight substances won’t pass through the enamel but things with smaller weight can
this property is both good and bad
fluoride ions in water and saliva can absorb through enamel rods/crystals and strengthen the tooth (GOOD)
but sugars - especially if in liquid form - can also penetrate through the enamel (BAD)
describe the chemical composition of enamel
96% inorganic
mainly hydroxyapatite crystals (basic structure of any mineralised tissue as well)
loose hydroxyl group present at the end (both good and bad thing)
good - replaceable with fluoride and end up with fluorapatite - more resistant to decay and doesn’t dissolve in acids that easily (inc. resistance by 30-40%)
bad - hydroxyl group can be easily broken by acids/sugars/toxins and then the hydroxyapatite crystals get broken
what are the 2 types of histological preparations for examination of hard tissues?
describe them
what about tissues that are nearly equal in organic - soft - (35%) and inorganic - hard - (65%) content, like dentin?
DECALCIFIED SECTIONS
best for soft tissues
removes calcium from the tooth structure
GROUND SECTIONS
tooth is ground until very thin layer is made
the grinding creates lots of friction and heat, so that tissues with less minerals become more burnt than others, creating a dark appearance
darker = softer, lighter = harder
this is put on a slide without any staining and examined
DENTIN
can use both methods to examine dentin as the amount of inorganic and organic material is significant enough to be seen in either section
describe the enamel rod
basic structural unit of enamel
may be hexagonal or prism-like in cross-section
rods don’t have a fixed regular geometric outline
both ‘enamel rod’ and ‘enamel prism’ terms can be used interchangeably
smallest tooth (lower perm. central incisor) has ≃ 5 million rods
largest tooth (upper perm. first molar) has ≃ 12 million rods
each enamel rod contains hundreds of thousands of hydroxyapatite crystals
what’s the difference between ‘direction’ and ‘course’?
direction - describes going from point A to point B
for example, going from the gold coast to brisbane, the direction is to brisbane
course - describes the ways to get there
could go through the suburbs, go through motorway, fly there etc
describe the direction of permanent enamel
enamel arrangement is better than deciduous, because its supposed to last longer - in cervical 1/3rd, follows the shape of the tooth and ends up as a knife edge, blends in perfectly with the CEJ
describe the course of enamel
wavy course except at the incisal edges/cusp tips where enamel rods have a complex course (gnarled enamel)
this is to withstand masticatory forces
enamel rods twist around each other, making the course more complex - and more strong
what are the two patterns that appear in a cross section of enamel?
keyhole pattern
fish scale pattern
what is the difference between the enamel rods/prisms and the interrod/interprismatic substance?
the angulation of the crystals
eg if rods were 45 degrees, the interrod substance would be 90 degrees (different angulation)
what are the 3 tissues the body can’t regenerate
(i actually don’t know if we need to know this but bakr mentioned it, so…)
enamel
pericardium (heart muscle)
brain cells
why do ameloblasts have a life history and not a life cycle?
the ameloblasts serve a purpose before the tooth erupts and degenerates when the tooth is erupting
the process of enamel formation stops so there’s no need for ameloblasts anymore
what are the 6 different stages the ameloblasts go through?
differentiating (presecretory) stage
secretory stage
transitional stage
maturative stage
protective stage
desmolytic stage
give details about stage 1 of ameloblasts (presecretory/differentiation stage)
ameloblasts differentiate from IEE
in early bell stage, IEE is separated from DP by cell-free zone
IEE cells elongate at the expense of cell-free zone - comes into contact with the DP
now they are preameloblasts
preamel. induce the formation of odontoblasts by a process called induction (from the peripheral layer of dental papilla)
the cells are columnar, but shorter in comparison to what the secretory/mature ameloblasts will look like