BioL Exam 3: Cardiovascular
1/112
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
113 Terms
mediastinum of thoracic cavity
where is the heart located?
pericardium
what is the serous membrane that covers and protects the heart? (has 2 layers)
outer fibrous, inner serous pericardium
what are the two layers of the pericardium?
parietal, visceral
what are the two layers of the inner serous pericardium?
outer fibrous pericardium
outer most layer of pericardium
dense irregular connective tissue that encloses and protects the heart
attached to the diaphragm inferiorly and the pulmonary trunk and aorta superiorly
parietal layer of serous pericardium
middle layer pericardium
inner serous pericardium
composed of simple squamous epithelium and areolar connective tissue that fuses to the fibrous pericardium
The visceral and parietal layers are separated by the serous cavity, a fluid-filled space
visceral layer of serous pericardium, parietal layer of serous pericardium, outer fibrous pericardium
list the layers of the pericardium from innermost to outermost
endocardium, myocardium, epicardium
list the three layers of the heart from innermost to outer most
epicardium
innermost layer of the serous pericardium and the outermost layer of the heart wall
myocardium
middle layer of the heart
thickest & contains cardiac muscle
pumps blood through heart to major arteries
endocardium
innermost layer of the heart, lining the heart chambers and heart valves
composed of endothelium reinforced with a thin layer of connective tissue that binds to the myocardium
myocardium
which layer of the heart is the thickest?
specialized cardiac muscle tissue
responsible for contraction/ relaxation cycle throughout the body
right atrium, right ventricle, left atrium, left ventricle
list the four chambers of the heart
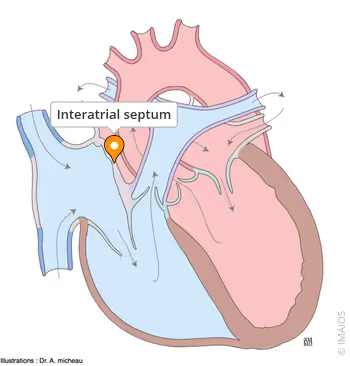
interatrial septum
what divides the right and left atrial chambers?
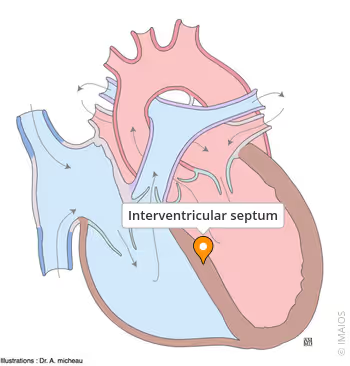
interventricular septum
what divides the right and left ventricles?
atrium
upper or receiving chamber of the heart that pumps blood into the lower chambers just prior to their contraction
contains pectinate muscles
muscular ridges
smaller chamber
right atrium
receives blood from the superior and inferior vena cava and the coronary sinus (systemic circuit) that flows into the right ventricle
left atrium
receives blood from the pulmonary veins that flows into the left ventricle
ventricles
contains trabeculae carneae
ridges of muscle covered by endocardium
one of the primary pumping chambers of the heart located in the lower portion of the heart
left ventricle
the major pumping chamber on the lower left side of the heart that ejects blood all over the body (systemic circuit) via the aorta and receives blood from the left atrium
much thicker
right ventricle
the major pumping chamber on the lower right side of the heart that ejects deoxygenated blood into the lungs (pulmonary circuit) via the pulmonary trunk and receives blood from the right atrium
contains chordae tendineae
string-like extensions of tough connective tissue that extend from the flaps of the atrioventricular valves to the papillary muscles
chordae tendinae
string-like extensions of tough connective tissue that extend from the flaps of the atrioventricular valves to the papillary muscles
left
which side of the heart
receives blood rich in oxygen and poor in carbon dioxide from the lungs
pumps it to rest of the body
right
which side of the heart
receives blood poor in oxygen and rich in carbon dioxide from the body
pumps it to lungs
right atrioventricular, left atrioventricular, pulmonary semilunar, aortic semilunar valves
list the 4 valves of the heart
tricuspid valve
what is another name for the right atrioventricular valve
bicuspid/ mitral valve
what is another name(s) for the left atrioventricular valve
tricuspid valve
what valve is between the right atrium and the right ventricle
bicuspid/ mitral valve
what valve is between the left atrium and the left ventricle
pulmonary semilunar valve
localized in between the right ventricle and the pulmonary trunk
aortic semilunar valve
between the left ventricle and the aorta
valves
keeps the blood moving in only one direction and then they close to prevent the back flow of blood
atrioventricular valves
valves that prevent back flow from the ventricles into the atria
semilunar valves
valves that prevent back flow from the arteries into the ventricles
pulmonary circulation
movement of blood from the right side of the heart to the lungs, and back to the left side of the heart
systemic circulation
movement of blood from the left side of the heart to the systemic cells (make up bodily tissue) of the body and then back to the right side of the heart
deoxygenated blood
what type of blood enters the heart through the right inferior and superior vena cava into the right atrium
tricuspid valve
opens allowing deoxygenated blood flow from right atrium into right ventricle
right ventricle
contracts to send deoxygenated blood through pulmonary valve & artery to lungs for oxygenation
oxygenation of blood
Air enters the lungs, traveling down to the tiniest air sacs, the alveoli, which are surrounded by a network of tiny capillaries
Oxygen molecules move from the alveoli (high concentration) across the thin respiratory membrane into the blood capillaries (low concentration)
lungs
where does oxygenated blood come from to re-enter the heart
pulmonary veins
what structures does oxygenated blood go through to re-enter the left atrium
arteries, arterioles, capillaries
what three blood vessels does the aorta branch into from largest to smallest/ highest to lowest pressure
to carry oxygenated blood away from the heart
coronary arteries
transport blood rich in oxygen to the muscle of the heart (myocardium)
coronary veins
transport blood poor in oxygen away from the muscle of the heart (myocardium)
cardiac veins
carries deoxygenated blood to the coronary sinus
Great cardiac vein – drains areas supplied by the left coronary artery
Middle cardiac vein – drains areas supplied by the posterior interventricular branch
Small cardiac vein – drains right atrium and right ventricle
Anterior cardiac vein – drains right ventricle and opens directly into the right atrium
anastomosis
the area where two or more arteries supplying blood to the same region connect
area where vessels unite to allow blood to circulate even if there may be partial blockage in another branch
collateral anastomosis
alternative routes provided by anastomosis
blood vessels
these structures ensures that the heart receives the needed nutrients and oxygen to keep pumping blood through its chambers
the heart wall is too thick and does not allow the diffusion of oxygen and nutrients to the heart
conduction system
a specialized network of cells in the heart that generates and transmits electrical impulses, controlling the timing, rate, and rhythm of the heartbeat
Cardiac muscle cells repeatedly generate spontaneous action potentials that then trigger heart contractions
autorhythmicity
ability of cardiac muscle to initiate its own electrical impulse that triggers the mechanical contraction that pumps blood at a fixed pace without nervous or endocrine control
sinoatrial node
1st set of nodal cells
known as the pacemaker, a specialized clump of myocardial conducting cells located in the superior portion of the right atrium that has the highest inherent rate of depolarization that then spreads throughout the heart
Initiates sinus rhythm (normal heart rate)
initiates action potential
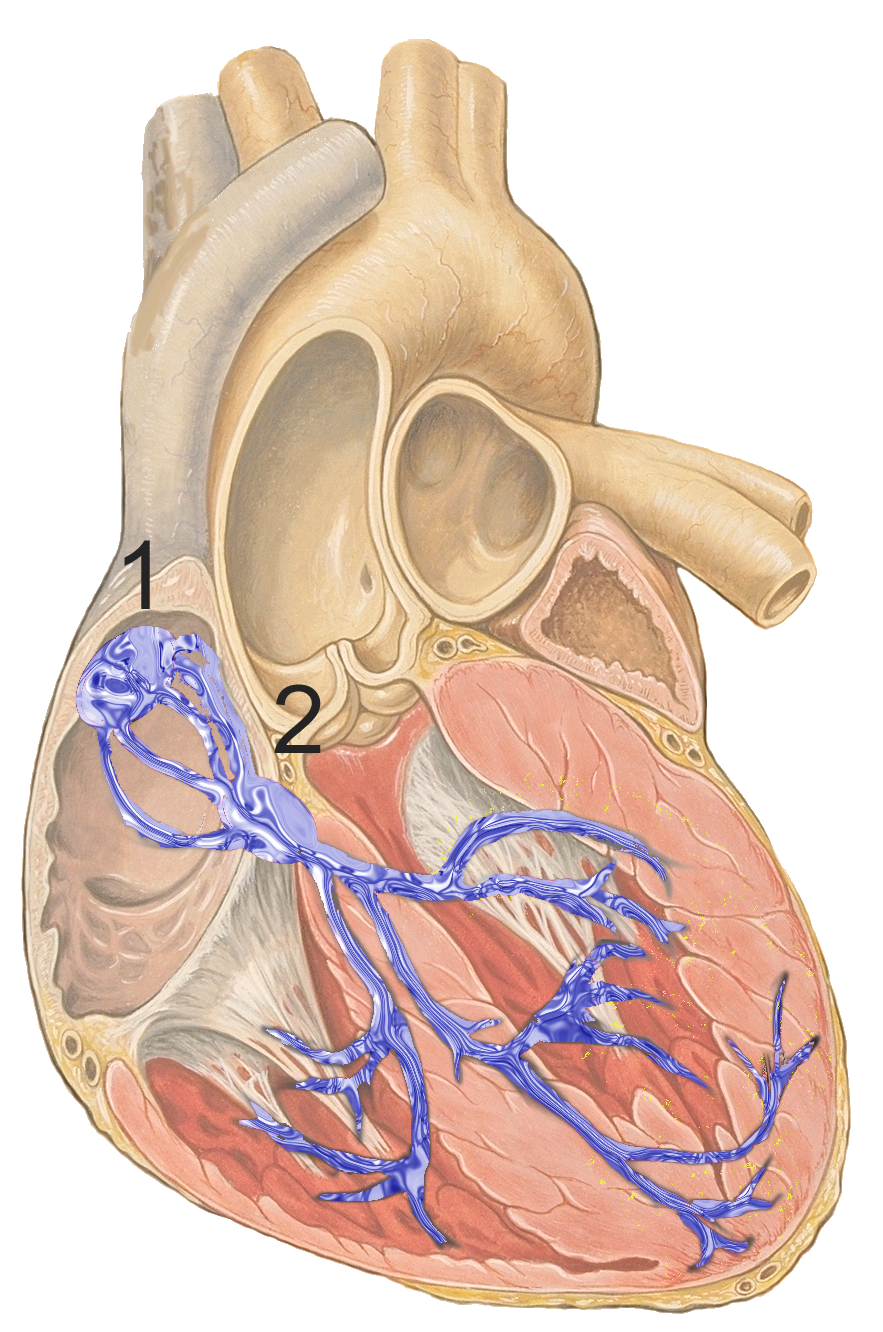
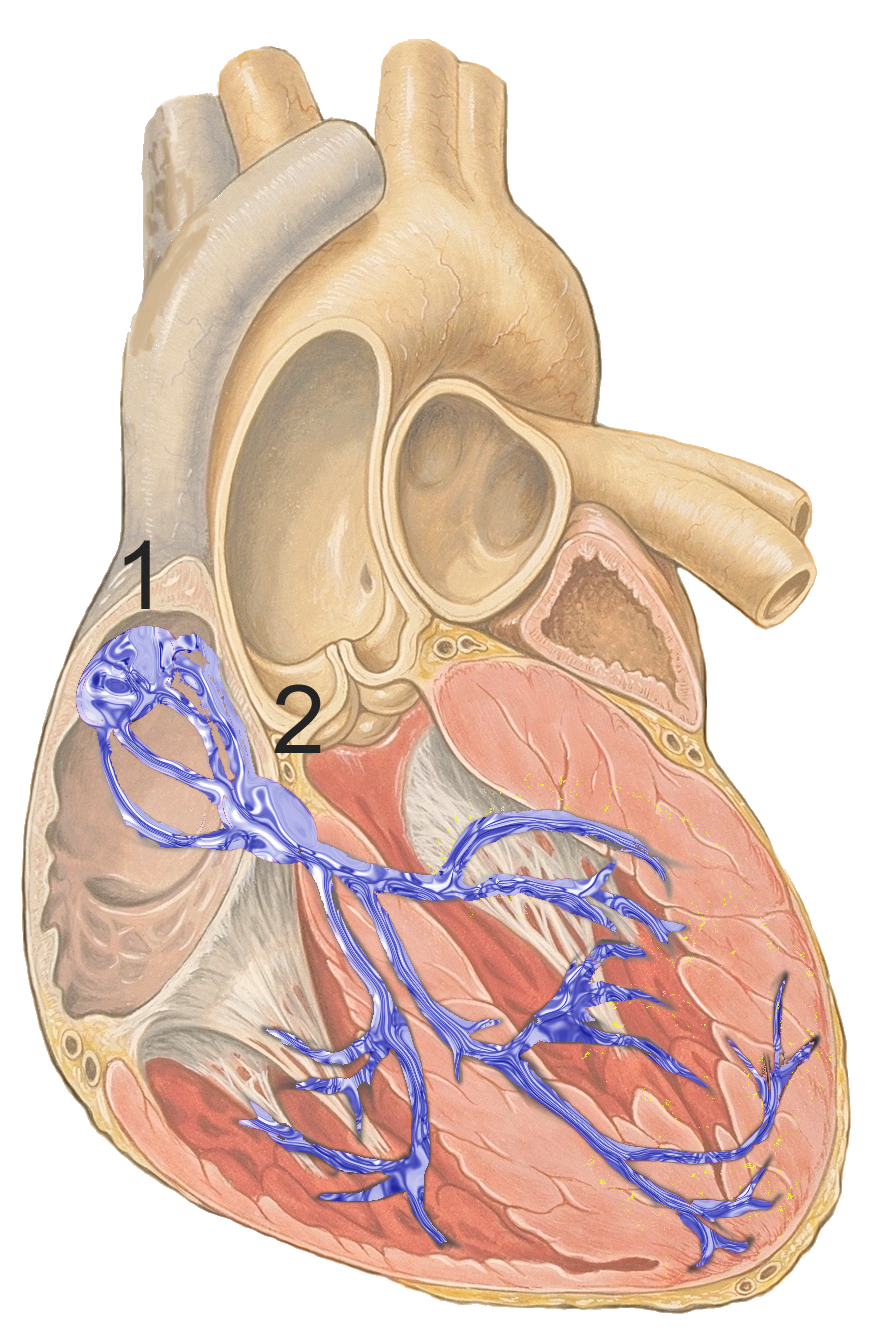
atrioventricular node
2nd set of specialized nodal cells
clump of myocardial cells located in the inferior portion of the right atrium within the atrioventricular septum; receives the impulse from the SA node, pauses, and then transmits it into specialized conducting cells within the interventricular septum
The septum prevents the impulse from spreading directly to the ventricles without passing through the AV node
atrioventricular bundle
group of specialized myocardial conductile cells that transmit the impulse from the AV node through the interventricular septum; form the left and right atrioventricular bundle branches
“Bundle of His”
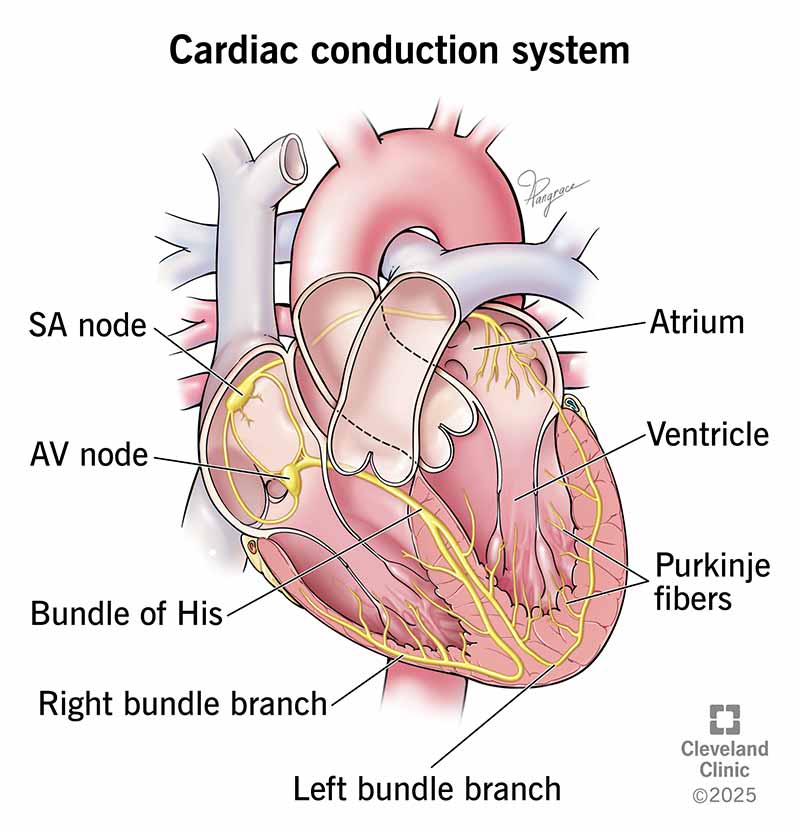
atrioventricular bundle branches
specialized myocardial conductile cells that arise from the branches of the atrioventricular bundle and pass through the interventricular septum
lead to the Purkinje fibers and also to the right papillary muscle via the moderator band
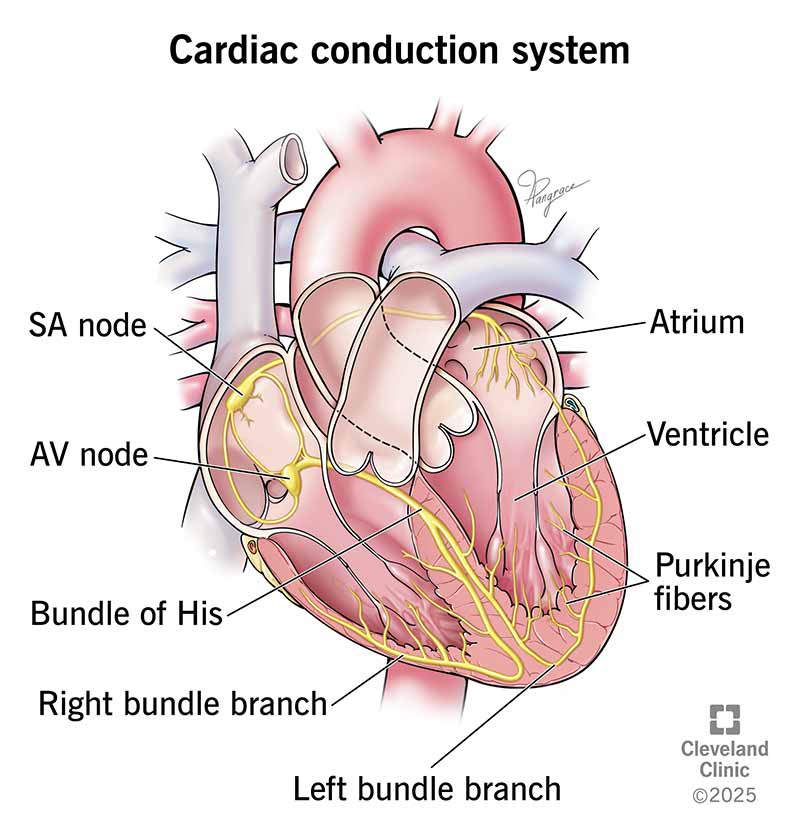
purkinje cells
final component of conduction system
are specialized cardiac muscle cells located in the inner ventricular walls (subendocardium) that conduct electrical impulses rapidly, ensuring synchronized contraction of the ventricles
high glycogen
nodal/ conducting cells
where do cardiac action potentials originate
nodal/ conducting cells
cells that initiate and propagate the action potential (the electrical impulse) that travels throughout the heart
sinoatrial node
atrioventricular node
bundle of his
atrioventricular bundle branches
Purkinje cells
contractile cells
conduct impulses and undergo contractions that pump blood through the body
they are striated, involuntary, and branched cells that use a long-lasting calcium-driven action potential and sarcomere sliding filaments to produce coordinated, forceful contractions, relying on high oxygen consumption
99% of cardiac muscle cells
cardiomyocytes
ECG
surface recording of the electrical activity of the heart that can be used for diagnosis of irregular heart function
the overall electrical signal from the action potentials that initiate the cardiac contraction
aka: EKG
p wave, qrs complex, t wave
list the three ECG peaks
p wave
what ekg wave indicates atrial systole (depolarization)
atria begin contracting and wave represents the depolarization of the atria where Na+ (sodium) is entering the cell
AV close
larger wave could indicate an enlargement of the atria
qrs complex
what ekg wave indicates ventricular systole (depolarization)
represents the depolarization of the ventricles and includes, as a component, the repolarization of the atria
contraction of ventricles follows
t wave
ventricular diastole (repolarization)
represents the repolarization of the ventricles
semilunar valves close
cardiac cycle
consists of the contraction and relaxation of both atria, rapidly followed by contraction and relaxation of both ventricles
systole
period of contraction that pumps blood into circulation
diastole
period of time when the heart muscle is relaxed and the chambers fill with blood
depolarization
the electrical activation process where cardiac cells transition from a resting (polarized) negative state to a positive state
causes ion exchange (sodium ions Na+ flowing in, potassium ions K+ flowing out) across the cell membrane, triggering muscle contraction and propelling blood.
p wave & qrs complex
sodium ions, potassium ions
what ions exchange during depolarization (flowing in, flowing out)
repolarization
the biological process where a cell, particularly muscle or nerve cells, returns to its negative resting state after depolarization (contraction or excitation)
sodium channels close while potassium channels open, allowing positive potassium ions to leave the cell, restoring the negative charge inside
T wave
sodium, potassium
what channels close, open (allowing positive ions out) during repolarization
lub
S1
the sound created by the closing of the atrioventricular valves during ventricular contraction (systole)
dub
S2
the sound of the closing of the semilunar valves during ventricular diastole (relaxation)
cardiac output
the amount of blood pumped out by each ventricle in one minute
a measure of how effective the cardiovascular system is in performing its function of moving blood throughout the body to deliver nutrients and remove wastes
cardiac output (CO) = stroke volume (SV) x heart rate (HR)
stroke volume
the volume of blood pumped out by one ventricle with each beat (ml/beat)
at rest: 70 ml/beat
= end diastolic volume - end systolic volume
heart rate
the number of times your heart beats per minute (beats/min)
at rest: 75 beats/minute
end diastolic volume, end systolic volume
what two things control stroke volume
end diastolic volume
the amount of blood that collects in a ventricle during diastole (relaxation)
end systolic volume
the volume of blood that remains in a ventricle after it has contracted
preload, contractility, afterload
stroke volume and cardiac output depend on what three factors?
preload
the degree to which cardiac muscle cells are stretched before they contract
higher = higher the stroke volume
contractility
the contractile strength achieved at a given muscle length or the ability to produce a contraction (generate force)
afterload
the pressure that the ventricles must overcome to eject blood or the back pressure that the arterial blood exerts on the aortic and pulmonary valves
Hypertension (high blood pressure) will reduce the ability of the ventricles to eject blood and result in a lowered SV
chronotropic agents
what are factors that can change heart rate called
The sympathetic division of the autonomic nervous system
The parasympathetic division of the autonomic nervous system
Hormones
Drugs
tunica intima, tunica media, tunica externa
what are the three layers in most blood vessels from innermost to outermost
tunica intima
innermost layer of a blood vessel
single layer of squamous endothelium surrounded by subendothelial layer of areolar connective tissue
tunia media
middle layer of a blood cell
circular arrangement of smooth muscle cells with elastic fibers
vasoconstriction: narrows lumen to increase blood pressure
tunica externa
outer most layer of a blood vessel
areolar connective tissue with collagen and elastic fibers
fibers anchor to surrounding organs
vasa vasorum: smaller arteries that feed wall of larger blood vessels
arteries, veins, capillaries
list the three different blood vessel types
elastic/ conducting, muscular/ distributing, arterioles
list the three types of arteries
arteries
moves blood from heart to capillaries
thicker tunica media
narrower lumen
more resilient and resistant to blood pressure changes
(elastic, muscular, arterioles)
elastic arteries
Nearest to the heart
Conduct blood from heart to smaller branches
Largest arteries (1-3cm)
Contains lots of elastic fibers
Stretch to receive blood
Recoil to deliver blood to muscular arteries
E.g. aorta, pulmonary trunk, common carotid, common iliac
muscular arteries
3mm-1cm in size
More elastic fibers than other arteries
Internal lamina between tunica intima and media
External lamina between tunica media and externa
E.g. brachial, coronary
arterioles
Smallest arteries (10 μm-3 mm)
Larger arterioles have all 3 tunics
Smaller arterioles have thin endothelium and single layer of smooth muscle cells
Resistance vessels
veins
Conducts blood toward the heart
Thicker tunica externa
Larger lumen vs arteries
Fewer elastic and collagen fibers
Collapse when no blood
May contain valves
venules/ veins as blood reservoir
venules, veins as blood resevoir
list the two types of veins
venules
Smallest veins (8 to 100 μm)
Receive blood from thoroughfare channels and capillary beds
Larger have 3 tunics
Merge to form veins
veins as blood reservoir
At rest, 30% of blood volume is in pulmonary circulation and heart chambers
70% in systemic circulation
55% of total blood volume in veins, 15% in arteries/capillaries
capillaries
Connect arterioles to venules
Tunica intima does not have subendothelial layer
Thin walls allow for perfusion (rapid exchange of gas/nutrients)
Smallest vessels
continuous, fenestrated, sinusoidal
continuous capillaries
Most common type of capillary
No breaks or spaces between cells
Tight junctions connect adjacent cells
Intercellular clefts between cells are large enough for small molecules to cross blood to interstitial fluid