Chapter 21 - Skin & Eye Diseases
1/73
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
74 Terms
Epidermis
Thin outer portion of skin; composed of layers of epithelial cells
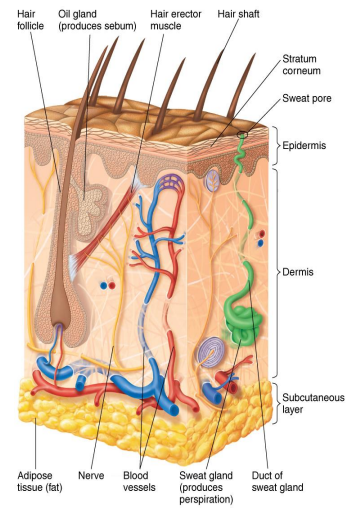
Keratin
Waterproofing protein coating outer layer of epidermis
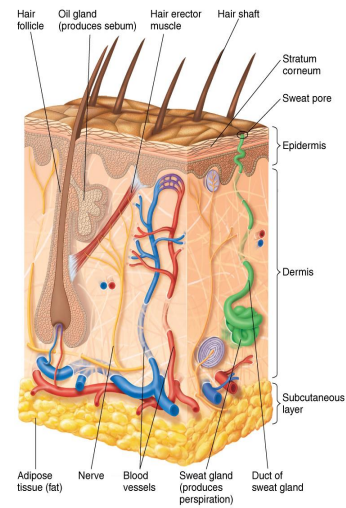
Dermis
Inner, thick portion of skin; composed mainly of connective tissue
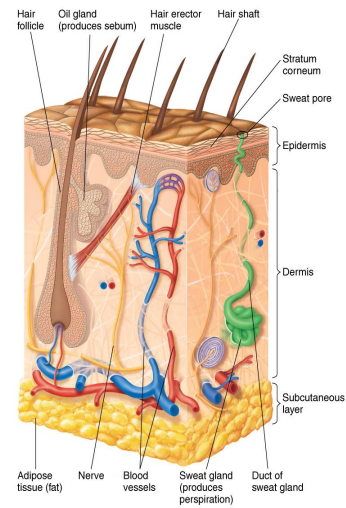
What does perspiration do?
Provides moisture and nutrients for growth
Contains salt that inhibits microorganisms
Antimicrobial peptides
Short proteins in innate immunity that destroy microbes by disrupting their cell membranes
Sebum
Oily secretion by oil glands containing fatty acids that inhibit pathogens
Mucous Membranes
Line the body cavities open to the exterior
Tightly packed epithelial cells attached to an extracellular matrix
cells secrete mucous
some cells have cilia
Often acidic
Membrane of eyes washed by tears containing lysozyme
Often folded to maximize surface area
Normal Microbiota of the Skin
Resistant to drying and high salt concentration
Large numbers of gram positive cocci
Staphylococci & micrococci
Areas with moisture have higher populations
Metabolize sweat and contribute to body odor
Staphylococci
Spherical gram-positive bacteria; form irregular clusters
Many produce coagulase
Enzyme that clots fibrin in the blood
Used to identify types of staphylococci
Staphylococcus epidermidis
Ninety percent of normal skin microbiota
Healthcare-associated pathogen
Produces biofilm on catheters
Coagulase-negative
Staphylococcus aureus
Carried in the nasal passages of 20% of the population
Golden-yellow colonies
Coagulase-positive
May produce damaging toxins and cause sepsis
Avoids host defenses in the skin
Secretes proteins and toxins that kill phagocytic cells
MRSA strains are antibiotic-resistant
Folliculitis (staph)
Infections of the hair follicles
Sty (staph)
Folliculitis of an eyelash
Furuncle (boil) (staph)
A type of abscess; localized region of pus surrounded by inflamed tissue
Carbuncle (staph)
Damage and inflammation of deep tissue from a spreading furuncle
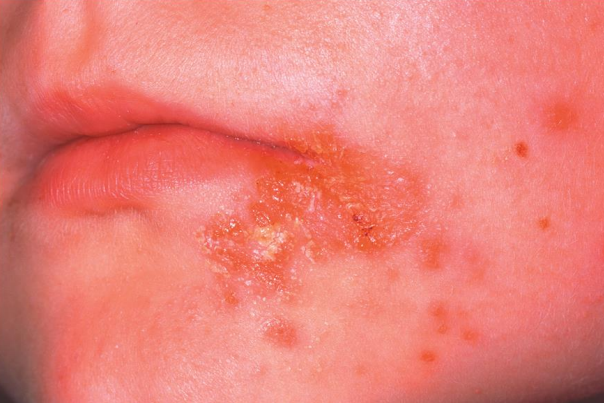
Impetigo (staph)
Pathogen → Staph aureus
Portal of entry → Skin
Symptoms → Crusting (nonbullous) sores, spread by autoinoculation
Method of transmission → Direct contact
Treatment → Topical antibiotics
Scaled skin syndrome (staph)
Bullous impetigo
Toxin B causes exfoliation
Pemphigus neonatorum: impetigo of the newborn
Toxic Shock Syndrome (TSS) (staph)
Fever, vomiting, shock, and organ failure caused by toxic shock syndrome toxin 1 (TSST-1) in the bloodstream
Streptococcal Skin Infections
Gram-positive cocci in chains
Produce hemolysins that lyse red blood cells
Beta-hemolytic streptococci often cause disease
Streptococci differentiated into groups A through T based on antigenic cell wall carbohydrates
Group A streptococci (GAS) → Streptococcus pyogenes
Eighty immunological types
Produce virulence factors:
Streptolysins: lyse RBCs
M proteins: external to the cell wall; allow adherence and immune system avoidance
Hyaluronidase: dissolves connective tissue
Streptokinases: dissolve blood clots
Erysipelas (strep)
S. pyogenes infects the dermal layer of the skin
Causes local tissue destruction and sepsis
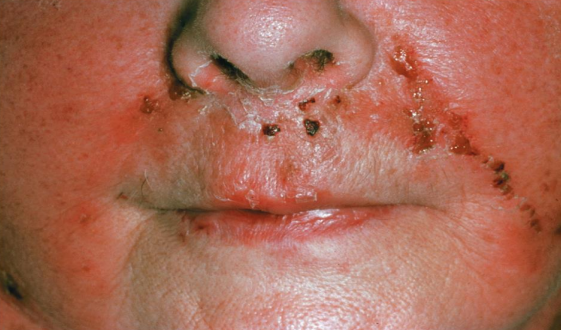
Necrotizing fasciitis (strep)
“Flesh-eating” disease
Exotoxin A produced by S. pyogenes acts as a superantigen
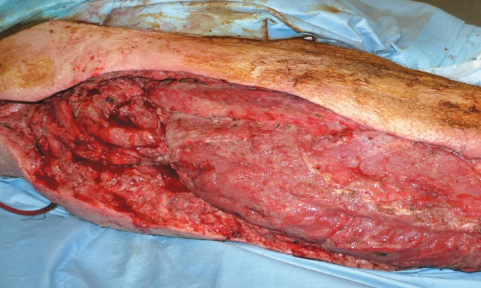
Infections by Pseudomonads
Pseudomonas aeruginosa
Gram-negative, aerobic rod (water)
Pyocyanin produces a blue-green pus.
Produces exo- and endotoxins; grows in biofilms
Pseudomonas dermatitis
Self-limiting rash acquired in swimming pools
Otitis externa
“Swimmer’s ear”
Opportunistic in burn patients
Resistant to many antibiotics
Buruli Ulcer
Caused by Mycobacterium ulcerans
Produces the toxin mycolactone
Enters via a break in the skin or an insect bite
Causes deep, damaging ulcers
May require amputation
Primarily found in western and central Africa
Acne
Most common skin disease in humans
Skin cells shed in the hair follicles and combine with sebum
Causes blockages
Sebum formation is affected by hormones, not diet
Comedonal (mild) Acne
Easily treated with topicals
Inflammatory (moderate) Acne
Caused by Propionibacterium acnes
Metabolizes sebum; fatty acids produce an inflammatory response
Treated with antibiotics and benzoyl peroxide
Nodular Cystic (severe) Acne
Inflamed lesions with pus deep in the skin
Most common route for skin diseases to be transmitted:
Respiratory routes
Warts
Papilloma → Small skin growths
Transmitted via contact
Caused by Papilomavirus
more than 50 types
some cause cancers
Smallpox (Variola)
Caused by an orthropoxvirus
Two forms of the disease
Variola major has 20-60% mortality
Variola minor has <1% mortality
Transmitted via the respiratory route, moves into the bloodstream, and infects the skin
Method of transmission → Aerosol
Completely eradicated from the human population by vaccination
Potential bioterrorism agent
Monkeypox
Pathoe=gen → Monkeypox virus
Portal of Entry → Respiratory tract
Related to smallpox
Endemic to small animals in Africa
Jumps from animals to humans
Prevention by the smallpox vaccination
Chickenpox (varicella)
Pathogen → Herpesvirus varicella-zoster (human herpesvirus 3)
Transmitted via the respiratory route
Causes pus-filled vesicles
Reye’s syndrome: severe complications of chickenpox; vomiting and brain dysfunction
Aspirin use increases risk
Virus becomes latent in the central nerve ganglia
Prevented by a live attenuated vaccine
Breakthrough varicella can occur if previously vaccinated
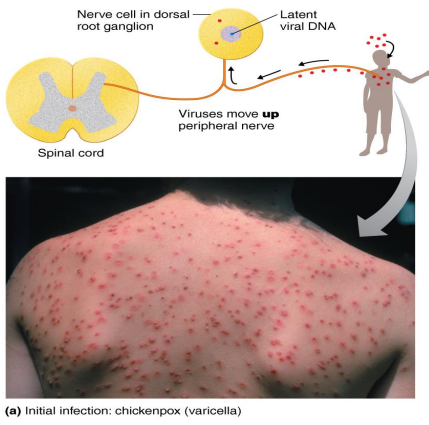
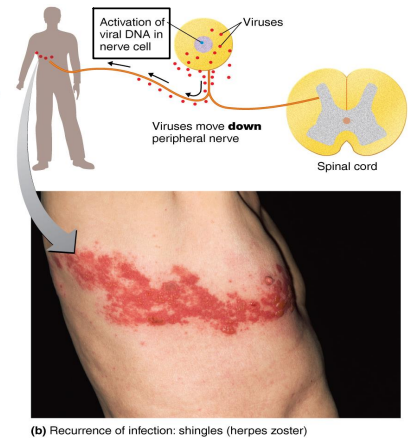
Shingles (herpes zoster)
Pathogen → HHV-3
Reactivation of the latent varicella-zoster virus (chickpox) that moves along peripheral nerves to the skin
Due to stress or lowered immunity
Follows the distribution of affected cutaneous sensory nerves
Limited to one side of the body
Postherpetic neuralgia
Prevention via the zoster vaccine
Antiviral drugs may lessen symptoms.
Human herpesvirus 1 (HSV-1) and 2 (HSV-2)
HSV-1 is spread primarily by oral or respiratory routes
90% of U.S.
Remains latent in trigeminal nerve ganglia
Outbreaks are triggered by the sun, stress, or hormonal changes
HSV-2 is spread primarily sexually
Remains latent in sacral nerve ganglia (spine)
Herpes gladiatorum (wrestling)
Vesicles on the skin
Herpetic whitlow (doctors and nurses)
Vesicles on the fingers
Herpes encephalitis
Virus spreads to the brain
Treated with acyclovir
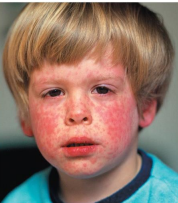
Measles (Rubeola)
Viral disease transmitted by the respiratory route
Cold-like symptoms, macular rash
Pathogen → Morbillivirus
Method of transmission → Aerosol
Koplik’s spots
Red spots on the oral mucosa opposite the molars
Prevented by the MMR vaccine (No treatment)
Children under 1 year old cannot receive the vaccine.
Rubella
German measles
Pathogen → Rubivirus
Macular rash and light fever
Method of transmission → Aerosol
Transmitted via the respiratory route; 2- to 3-week incubation
Prevented by the MMR vaccine (No treatment)
Not recommended for pregnant women
Fifth Disease (erythema infectiosum)
Pathogen → Human parvovirus B19
Mild flulike symptoms; “slapped-cheek” facial rash
Method of transmission → Aerosol
No treatment
Roseola
Roseolovirus (HHV-6, HHV-7)
Respiratory tract
High fever; body rash; recovery within 1 to 2 days
Method of transmission → Aerosol
No treatment
Hand-foot-and-mouth Disease
Pathogen → Enteroviruses
Spread via mouth mucous or saliva (children)
Fever and sore throat; rash on hands, feet, mouth, and tongue
Method of transmission → Aerosol
No treatment
Mycosis
Fungal infection of the body
Cutaneous Mycoses
Colonize the hair, nails, and outer epidermis
Metabolize keratin
Dermatomycoses
Informally known as tineas or ringworm
Tinea capitis: scalp ringworm
Tinea cruris: jock itch
Tinea pedis: athlete’s foot
Tinea unguium: ringworm of nails
Fungi involved in Cutaneous Mycoses
Trichophyton
Microsporum
Epidermophyton
Treatment = topicals (miconazole & clotrimazole)
Subcutaneous Mycoses
More serious than cutaneous mycoses; penetrate the stratum corneum
Usually caused by fungi that inhabit the soil
Sporotrichosis (subcutaneous mycoses)
Caused by Sporothrix schenkii; dimorphic fungus
Enters a wound; forms a small ulcer
Treated with potassium iodide
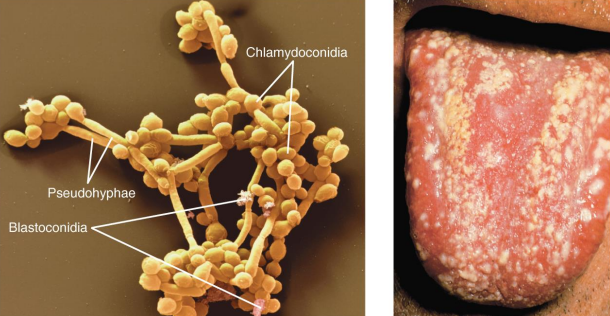
Candidiasis
Overgrowth of Candida albicans (yeast)
Forms pseudohyphae, making it resistant to phagocytosis
Occurs in the skin and mucous membranes of the genitourinary tract and mouth
Thrush: C. albicans infection of the oral cavity
Results when antibiotics suppress competing bacteria or a change occurs in the mucosal pH
Fulminating disease in the immunosuppressed
Treatment → Miconazole & clotrimazole topically
Scabies
Caused by Sarcoptes scabiei mites
Burrow in the skin to lay eggs
Causes inflammatory skin lesions
Transmitted via intimate contact
Treatment with permethrin
Pediculosis (Lice)
Pediculus humanus capitis (head louse)
P. h. corporis (body louse)
Feed on blood from the host
Lay eggs (nits) on the hair and attach to the shafts
Treatment with topical insecticides (permethrin or pyrethrin)
Malathion, lindane, or ivermectin are used in cases of resistance
Inflammation of the Eye Membranes: Conjunctivitis
An inflammation of the conjunctiva
Also called red eye or pinkeye
Commonly caused by Haemophilus influenzae, which is a bacterium unassociated with influenza infections
Also caused by adenoviruses
Can be caused by pseudomonads associated with unsanitary contact lenses
Ophthalmia Neonatorum
Caused by Neisseria gonorrhoeae
Large amount of pus forms; ulceration of corneas results
Untreated cases may lead to blindness.
Transmitted to a newborn’s eyes during passage through the birth canal
Prevented by treating a newborn’s eyes with antibiotics
Inclusion Conjunctivitis
Caused by Chlamydia trachomatis
Bacterium that grows as an obligate intracellular parasite
Transmitted to a newborn’s eyes during passage through the birth canal
Spread also through swimming pool water
Treated with tetracycline
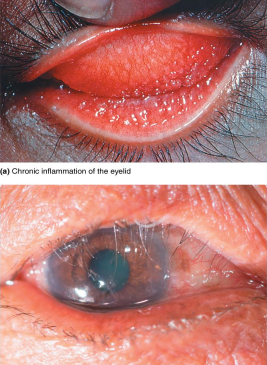
Trachoma
Caused by some serotypes of Chlamydia trachomatis
Leading cause of blindness worldwide
Transmitted via hand contact or flies
Infection causes permanent scarring; scars abrade the cornea, leading to blindness
Secondary infections can also be a factor.
Oral azithromycin is used in treatment.
Keratitus
Inflammation of the cornea
Bacterial (United States) → Contact lenses
Fusarium and Aspergillus (Africa and Asia)
Herpetic keratitis
Caused by herpes simplex virus 1 (HSV-1)
Infects cornea and may cause blindness
Treated with trifluridine
Acanthamoeba keratitis
Ameba transmitted via water and soil
Associated with unsanitary contact lenses
Mild inflammation followed by severe pain
Treatment with 2% chlorhexidine and propamidine isethionate eye drops or topical neomycin
May require a corneal transplant
Strategies to reduce incidence of neglected tropical diseases:
Preventive chemotherapy
Innovative, intensified disease management
Veterinary care
Vector control
Improved sanitation and hygiene services
Subacute sclerosing panencephalitis
Rare; Occurring 1 to 10 years after measles recovery
Congenital rubella syndrome
Fetal damage, deafness, heart defects, mental retardation in 35% of cases
15% mortality within first year of life