BIO 300 Lecture7B.IntroToHematopoieticSystem Review
1/45
Earn XP
Description and Tags
BIO 300 Pathophysiology
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
46 Terms
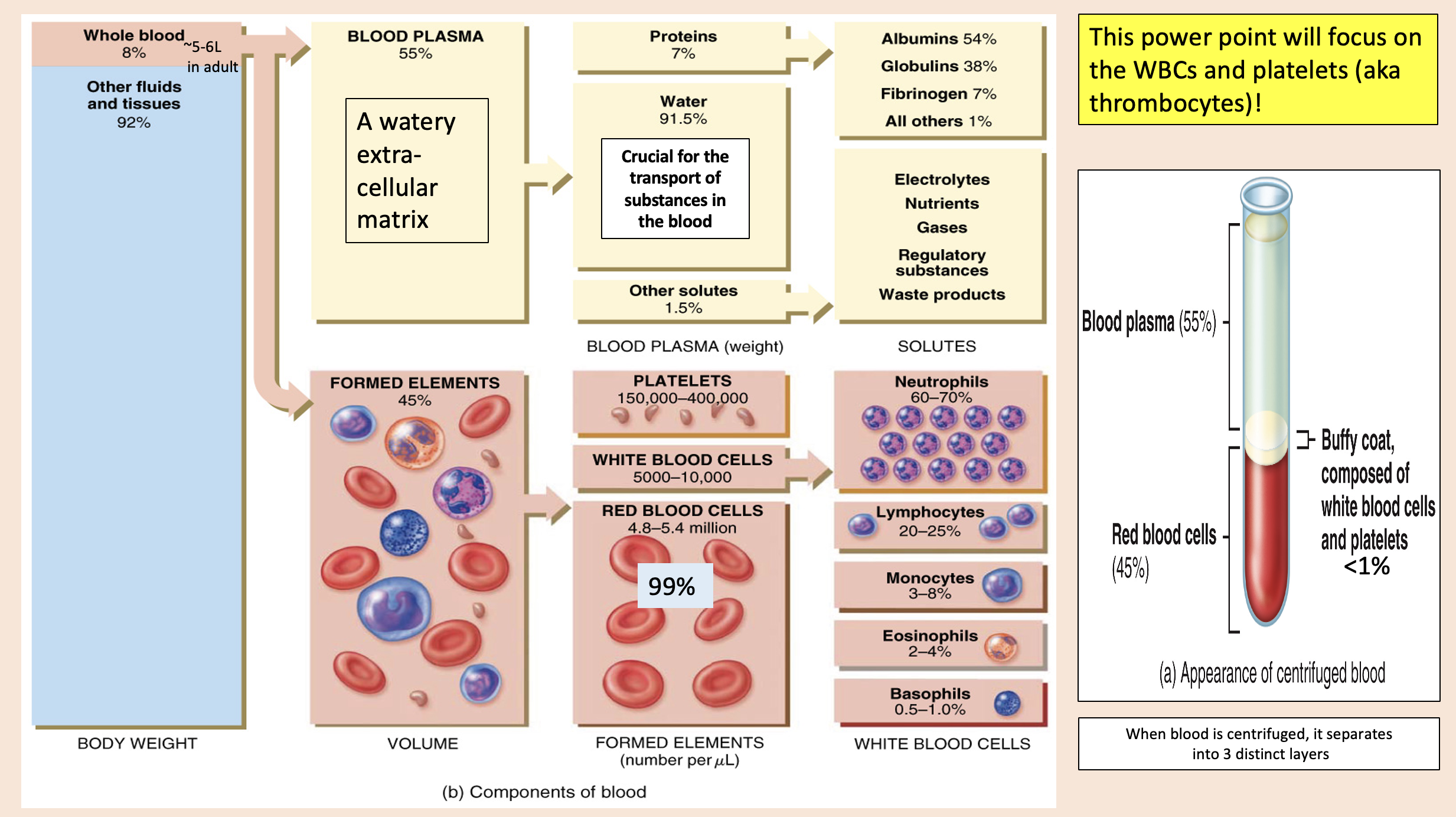
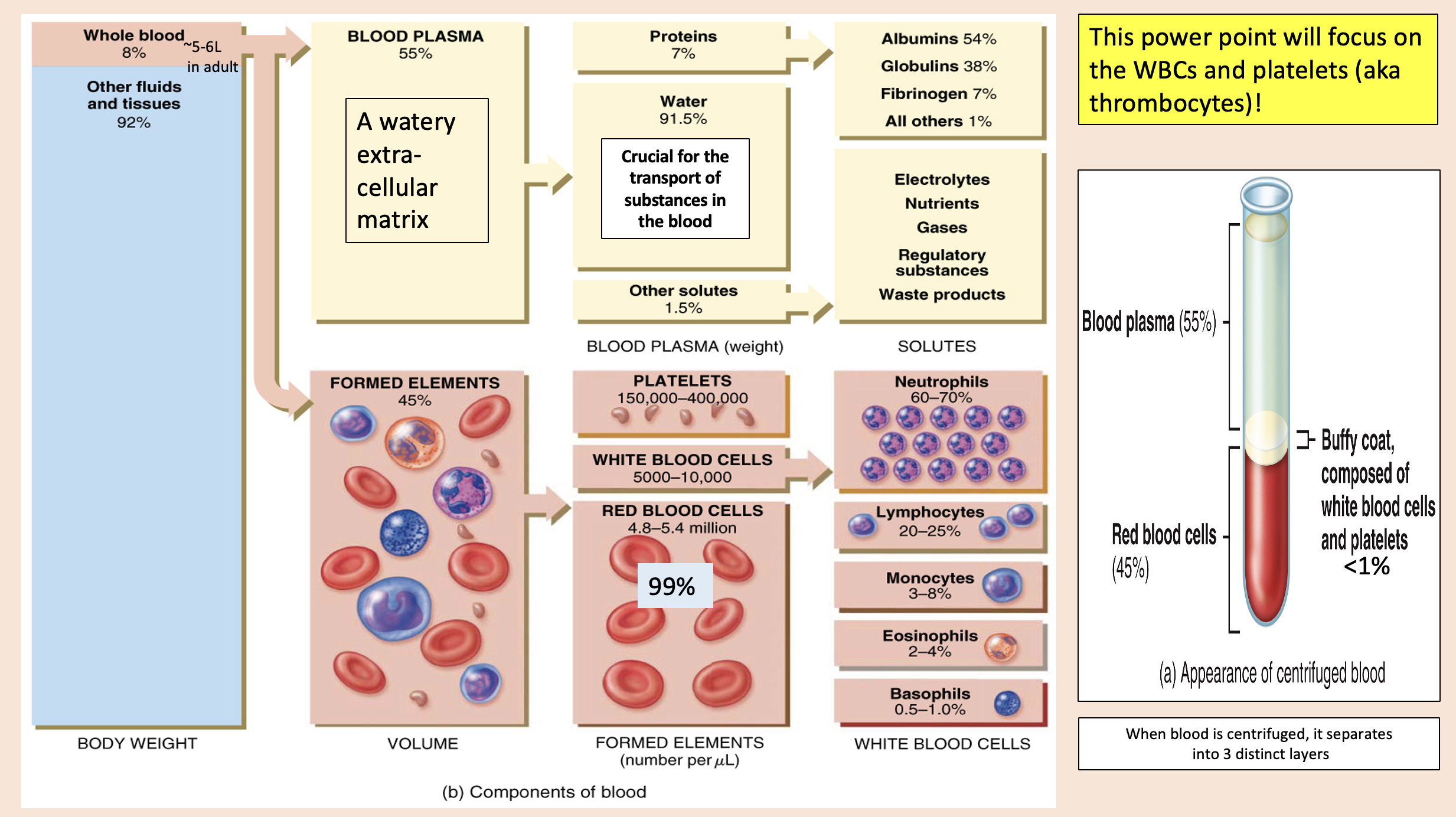
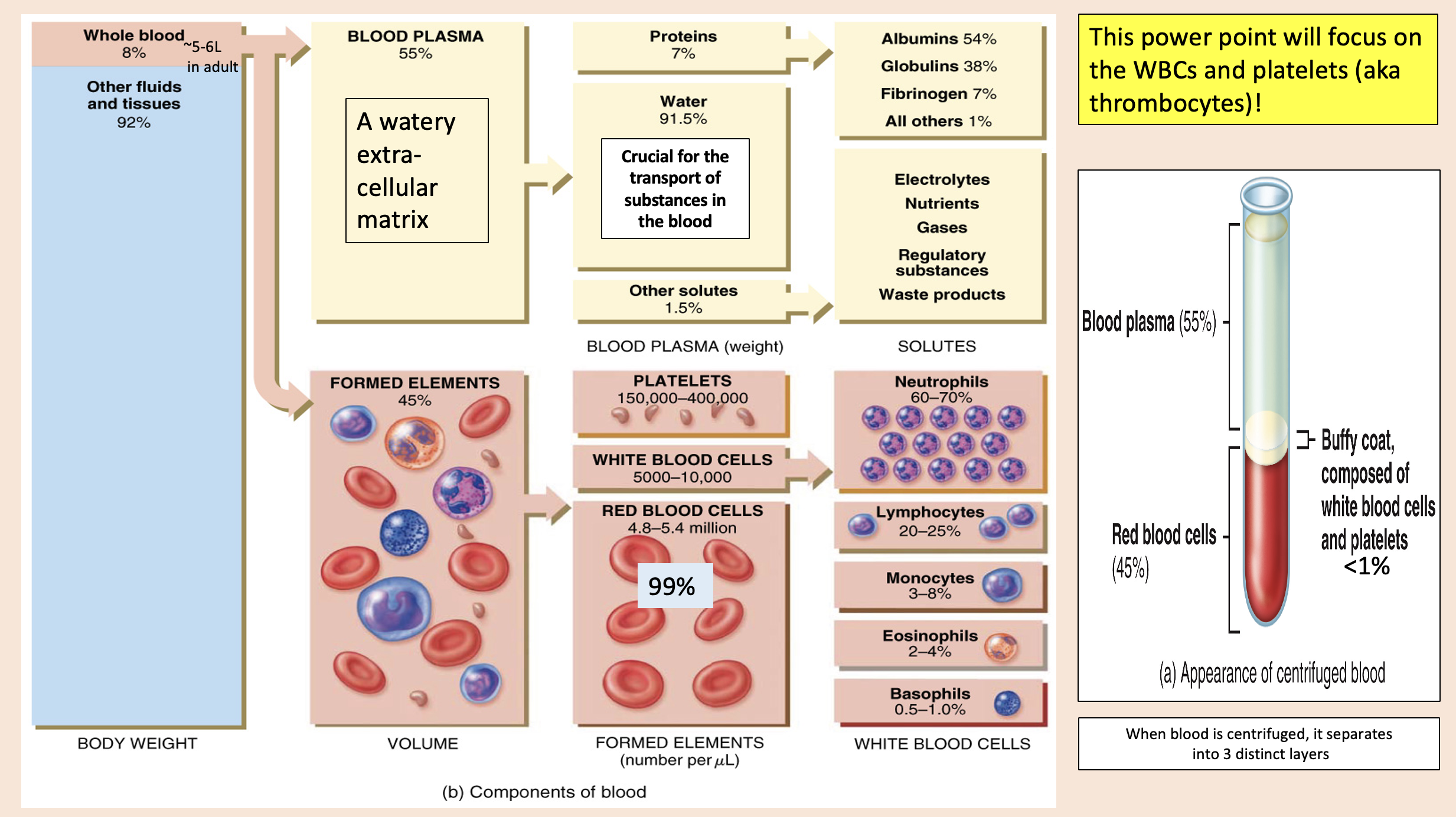
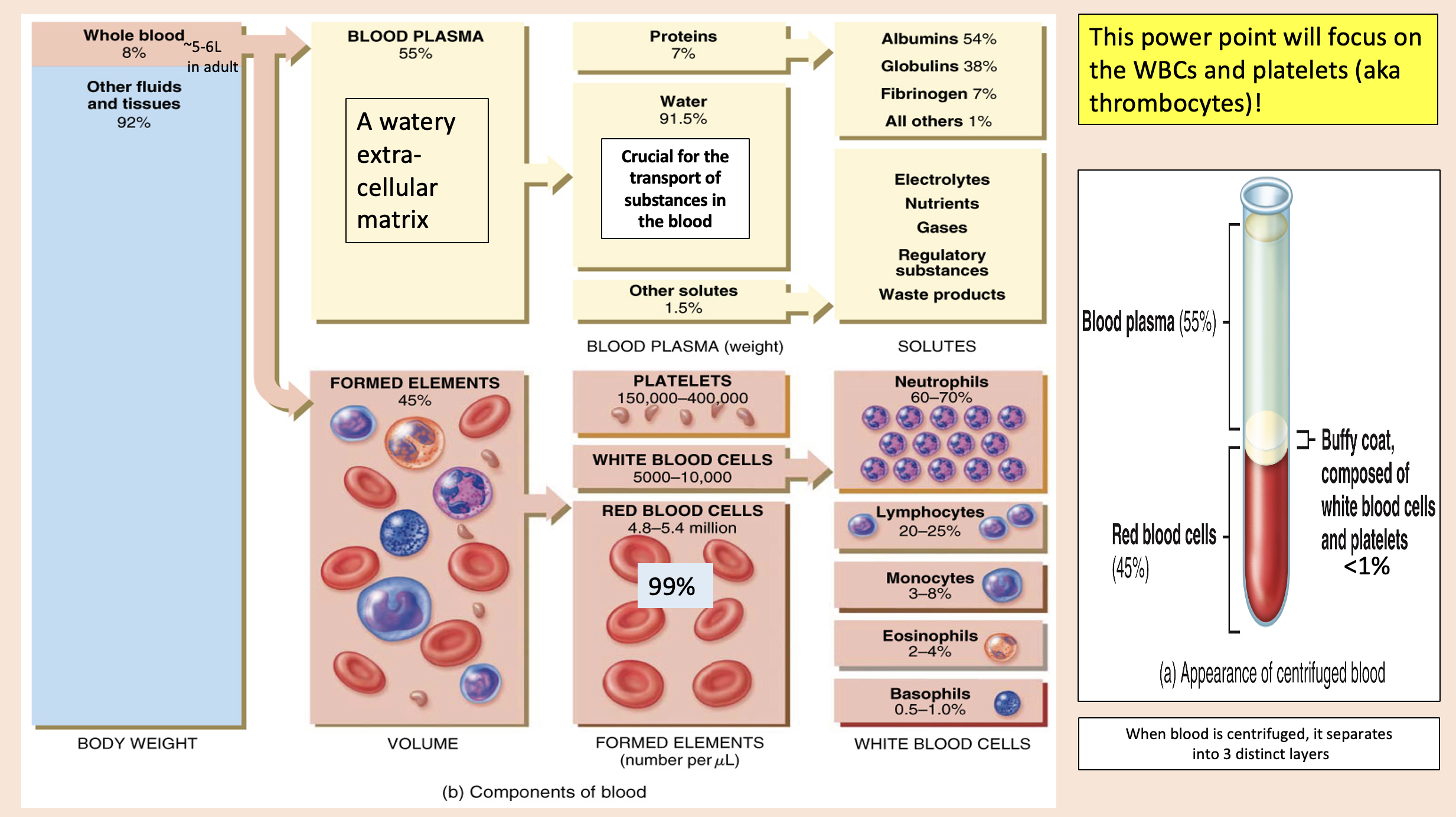
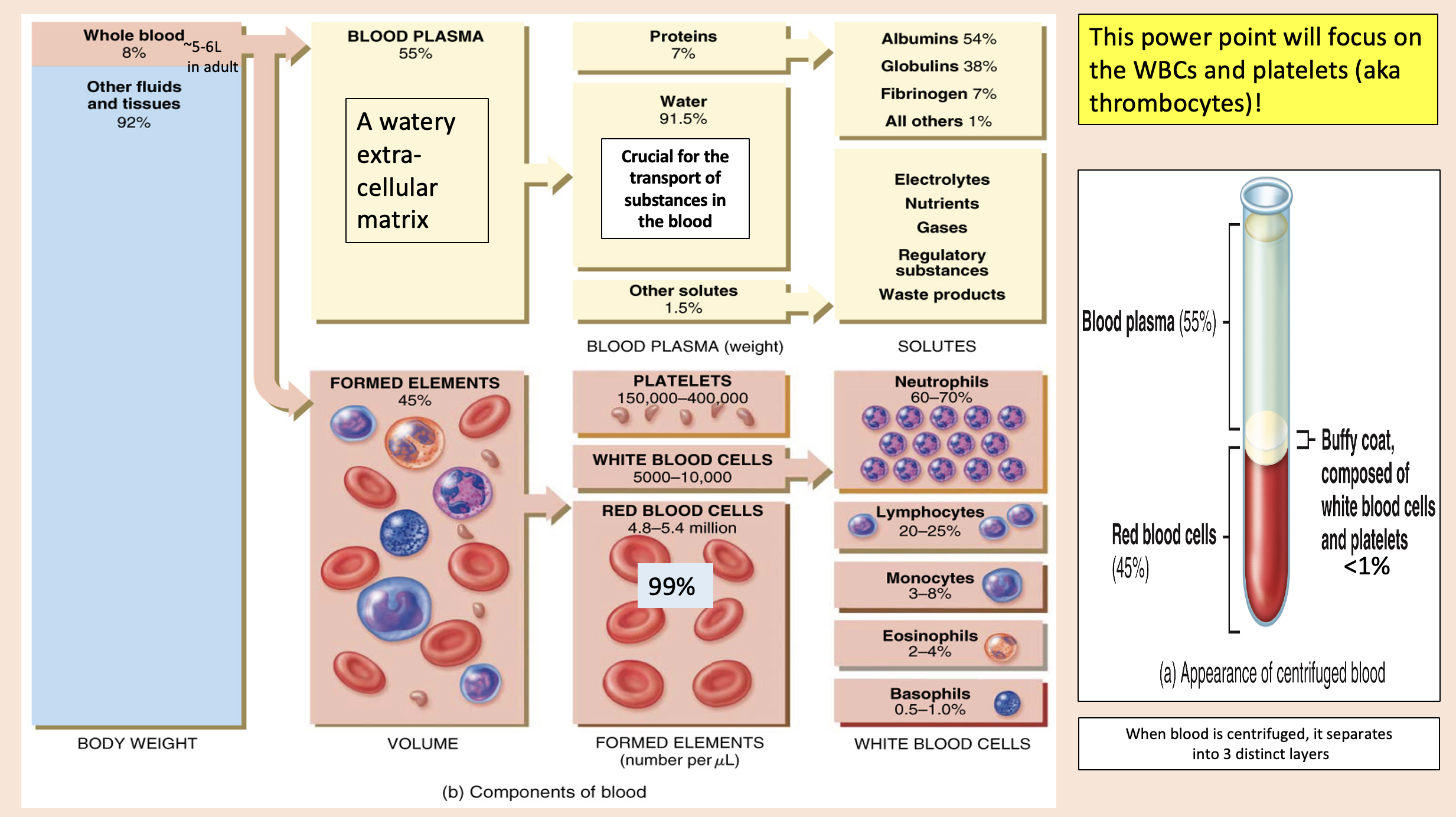
A watery extra- cellular matrix.
blood plasma
Albumins.
Globulins.
Fibrinogen.
All others.
proteins
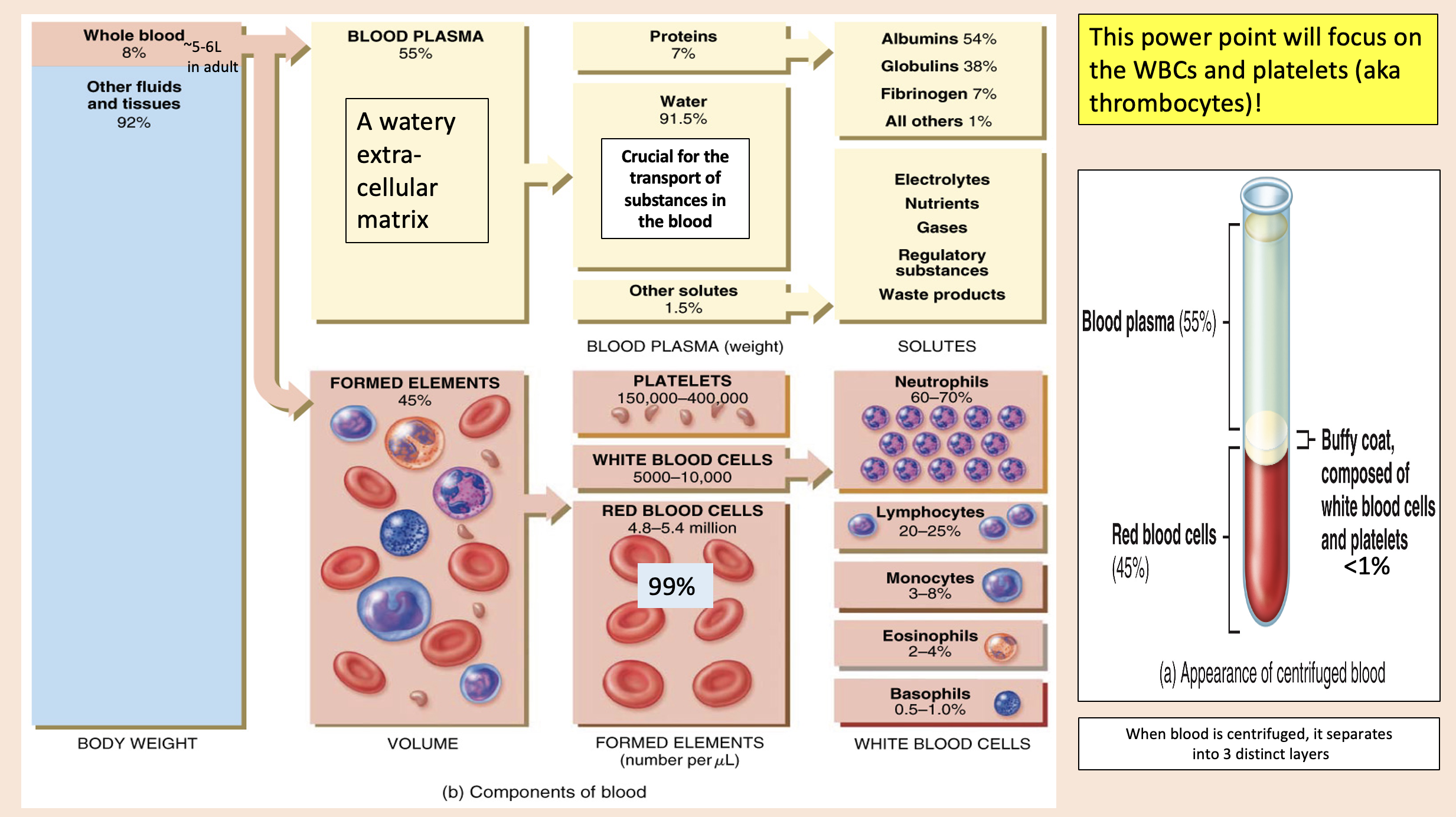
Crucial for the transport of substances in the blood
water
Electrolytes.
Nutrients.
Gases.
Regulatory substances.
Watery products.
other solutes
Neutrophils.
Lymphocytes.
Monocytes.
Eosinophils.
Basophils.
white blood cells
Platelets.
White Blood Cells.
Red Blood Cells 99%.
formed elements
aka White Blood Cells
leukocytes

Have nuclei and organelles.
Larger than RBCs.
NO Hb (bc their role is not to transport oxygen).
Can live for hours or days – & some for years (lymphocytes).
white blood cells

Combat inflammation.
Immune response.
Identify & destroy cancer cells.
leukocytes functions

Leukocytes are generally classified a (based on presence or absence of granules in their cytoplasm)
granular or agranular

Basophils.
Eosinophils.
Neutrophils.
granular

Lymphocytes.
Monocytes.
agranular

aka polymorphonuclear leukocytes or PMNs.
aka segs [bc of segmented nucleus].
neutrophil
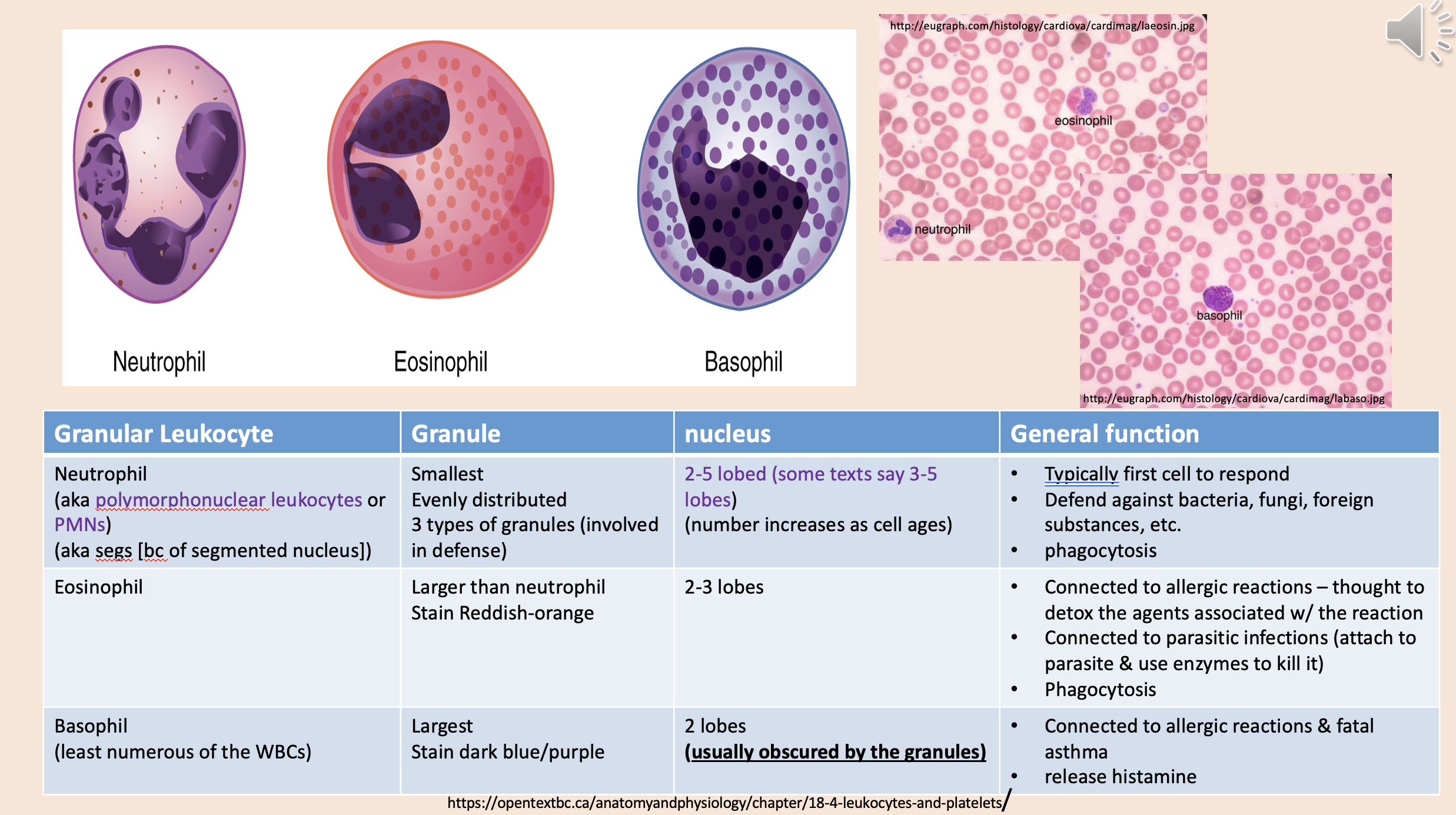
Typically first cell to respond.
Defend against bacteria, fungi, foreign substances, etc.
Phagocytosis.
neutrophil function
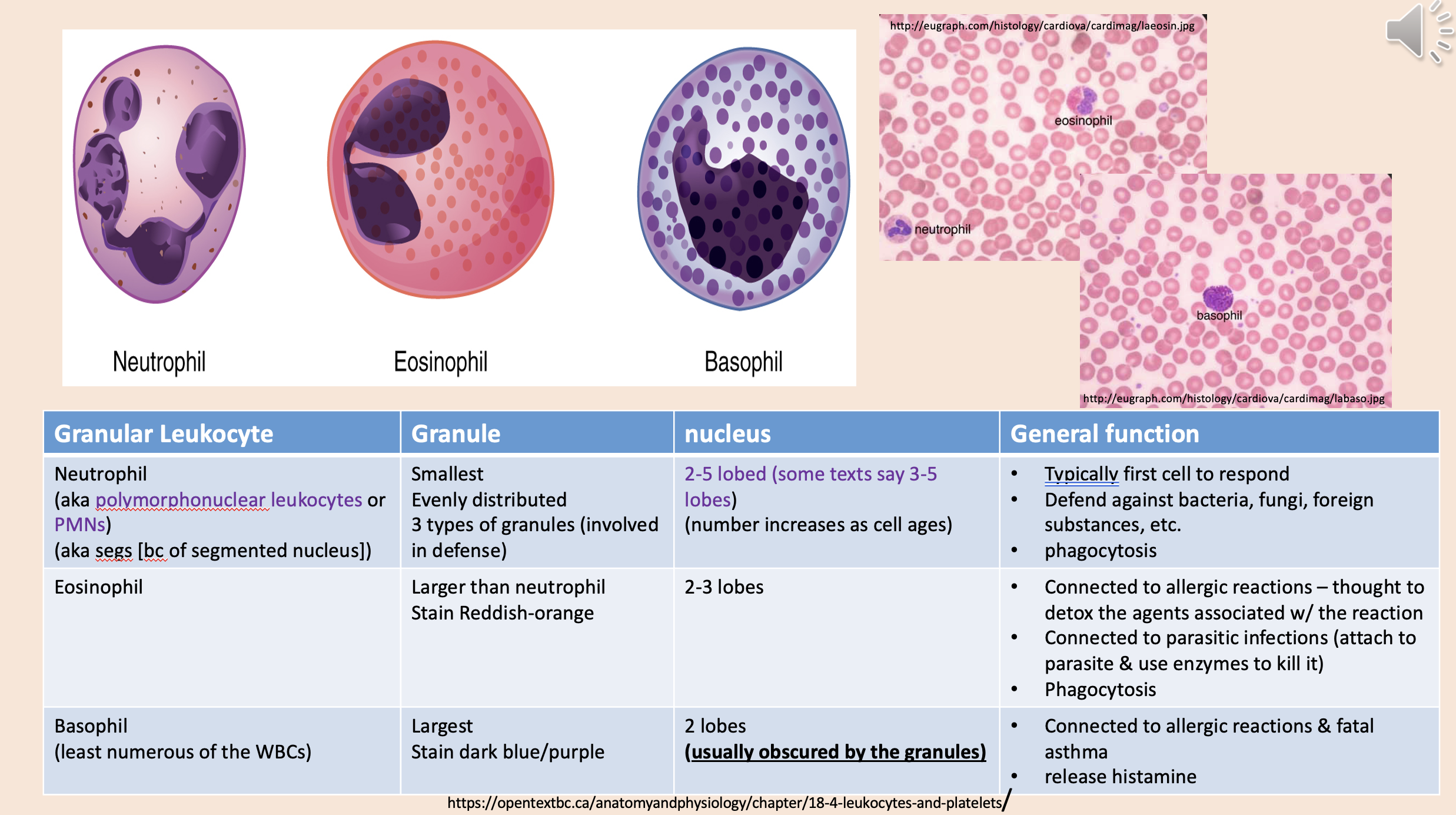
Connected to allergic reactions – thought to detox the agents associated w/ the reaction.
Connected to parasitic infections (attach to parasite & use enzymes to kill it).
Phagocytosis.
eosinophil
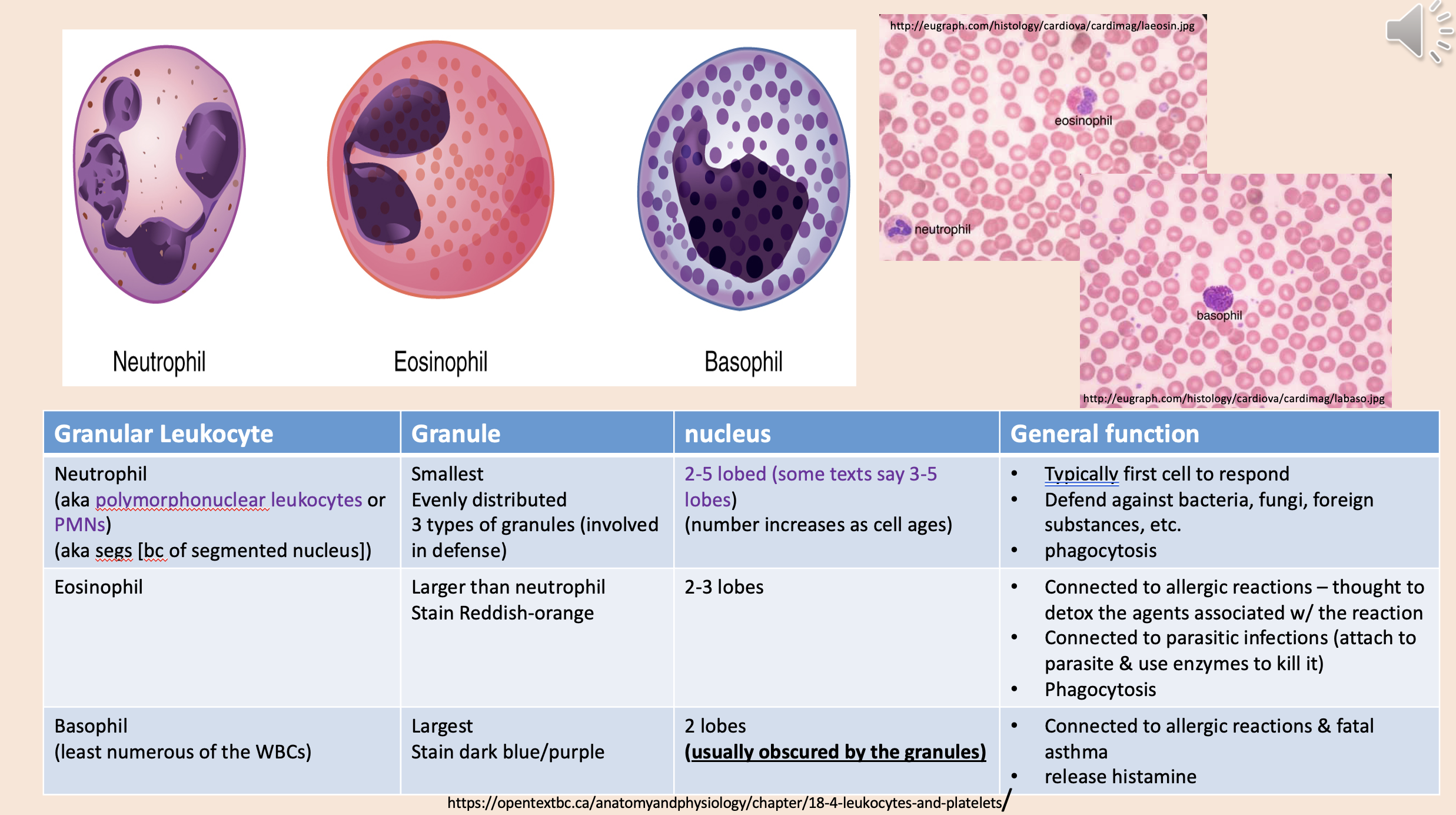
Connected to allergic reactions & fatal asthma.
Release histamine.
basophil
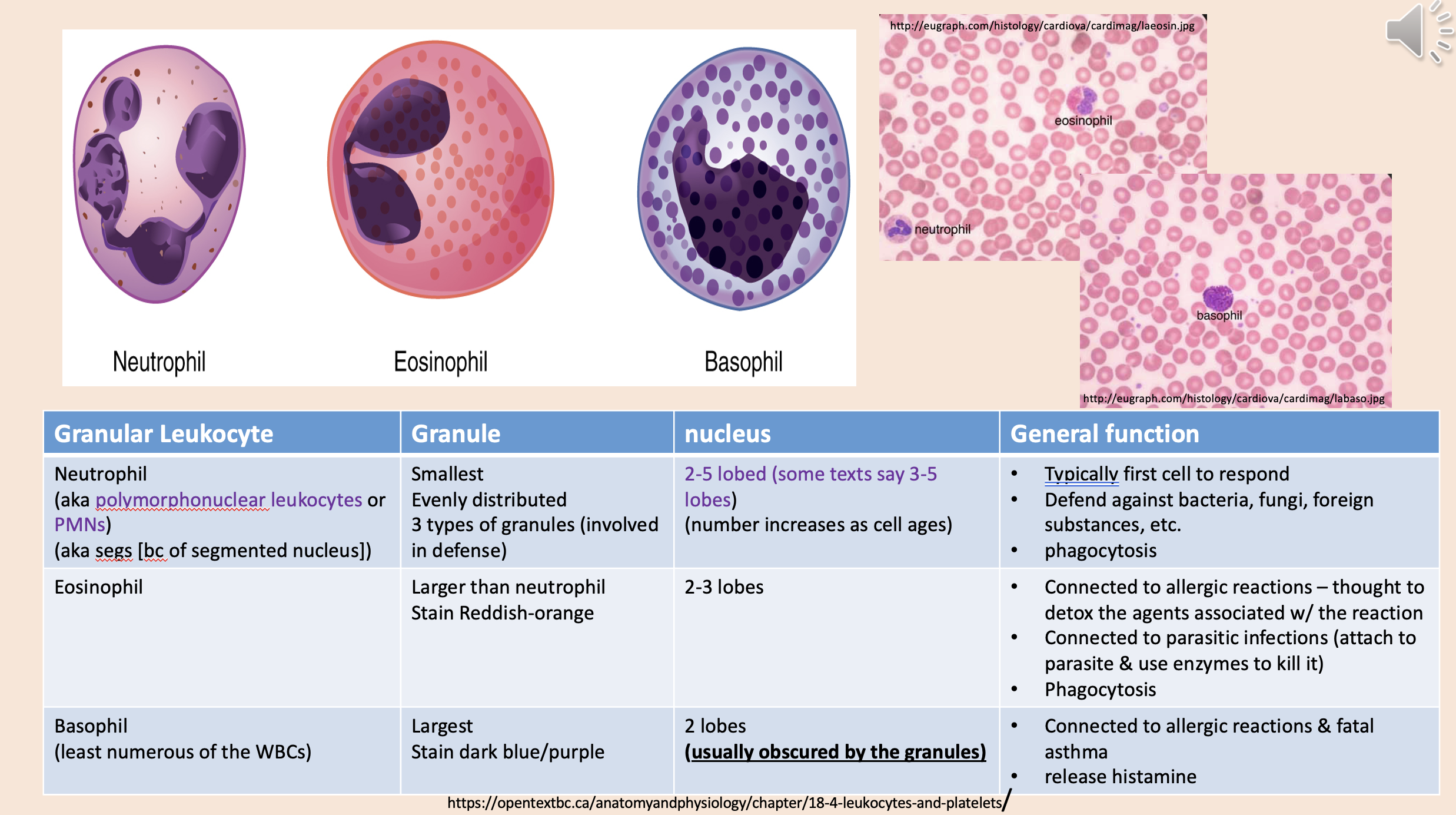
Least numerous of the WBCs
basophil
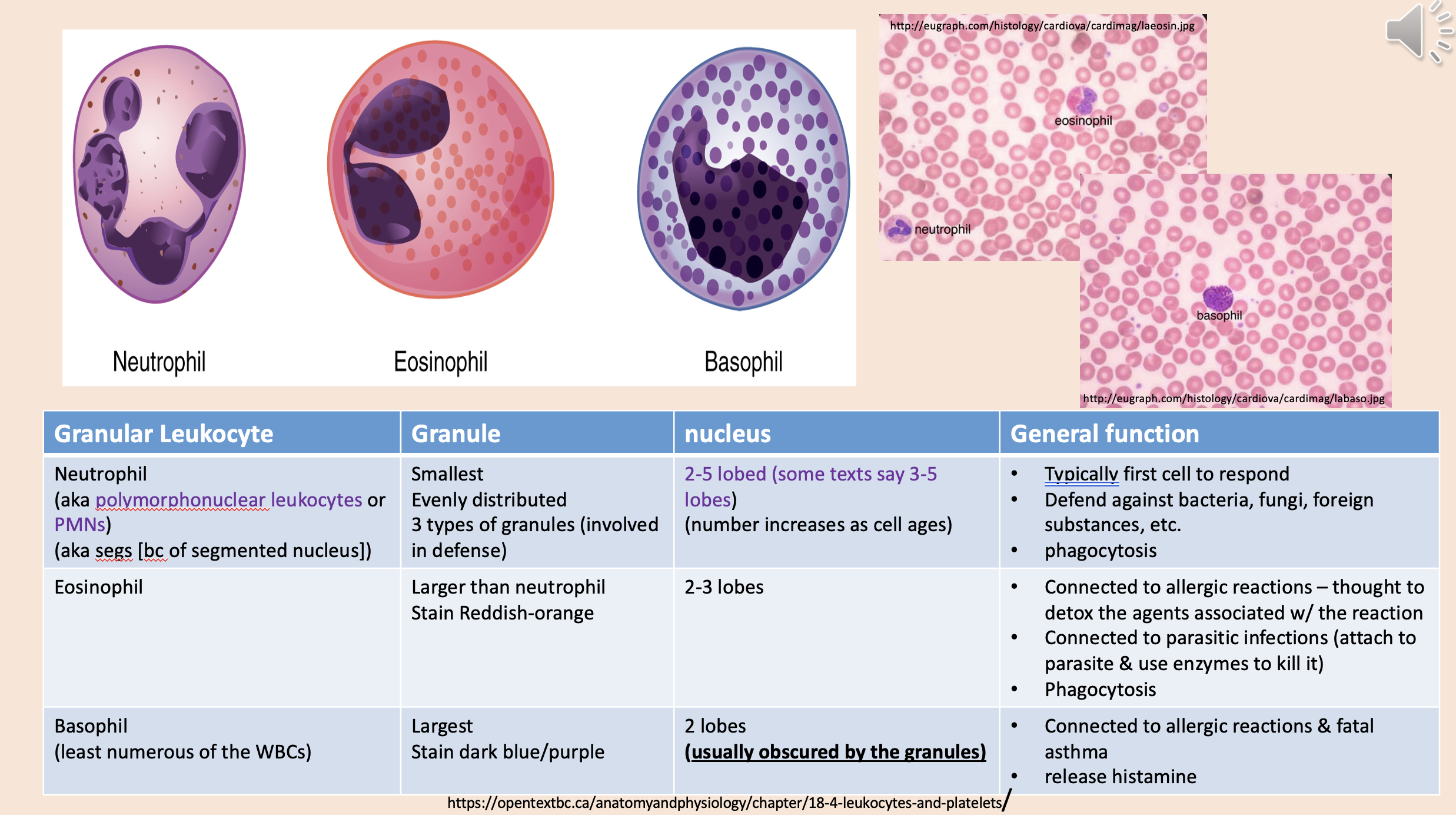
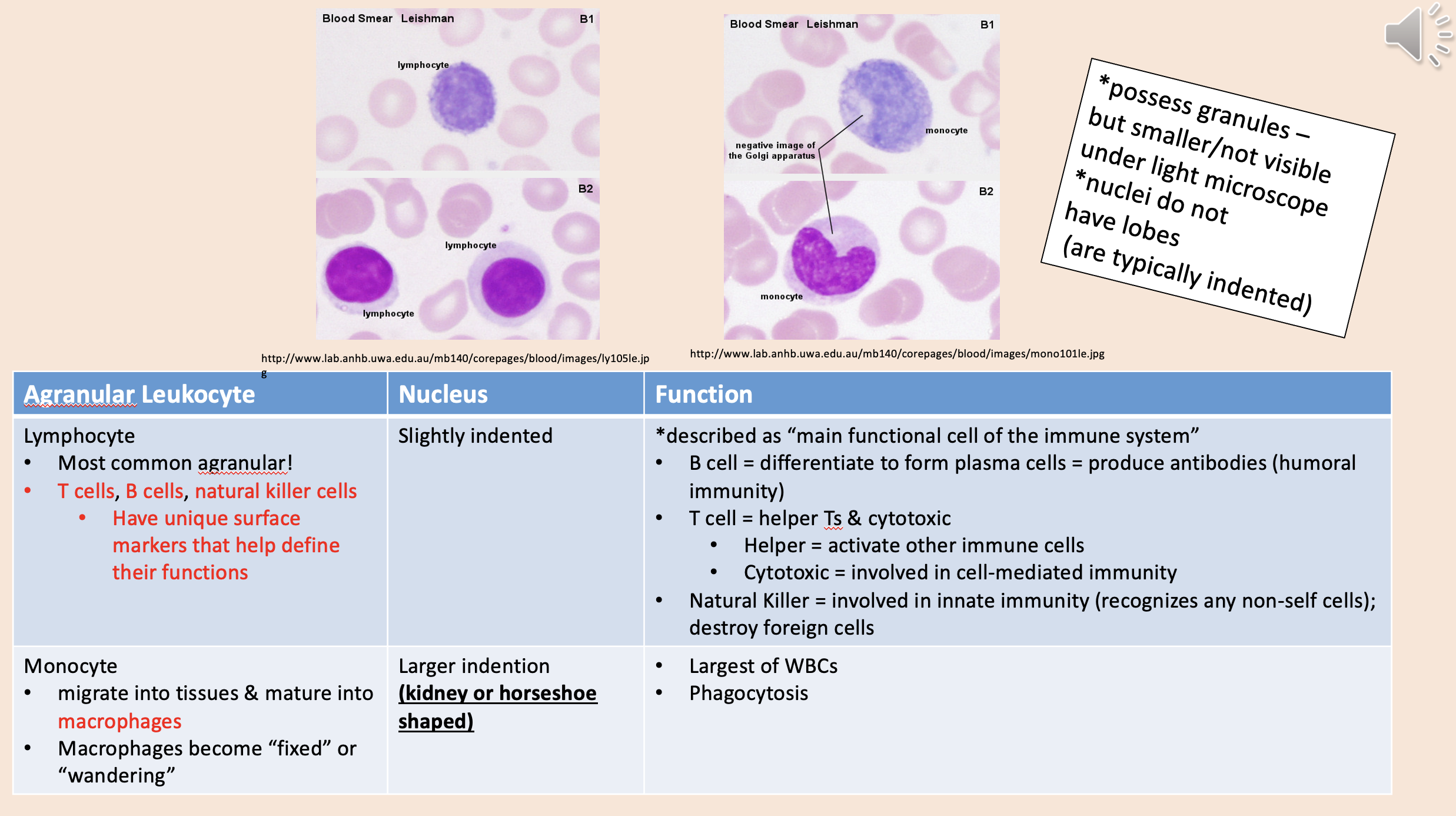
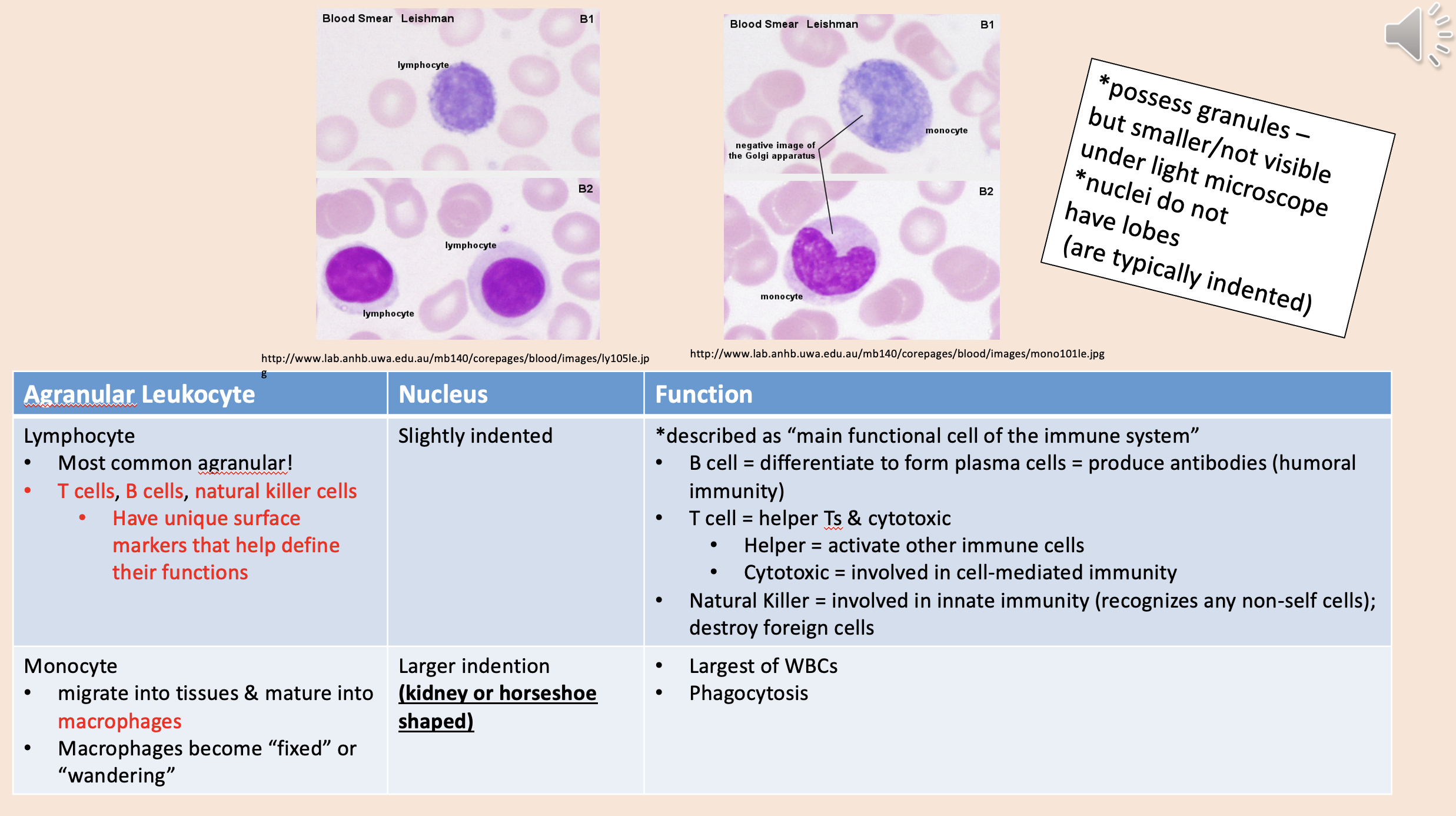
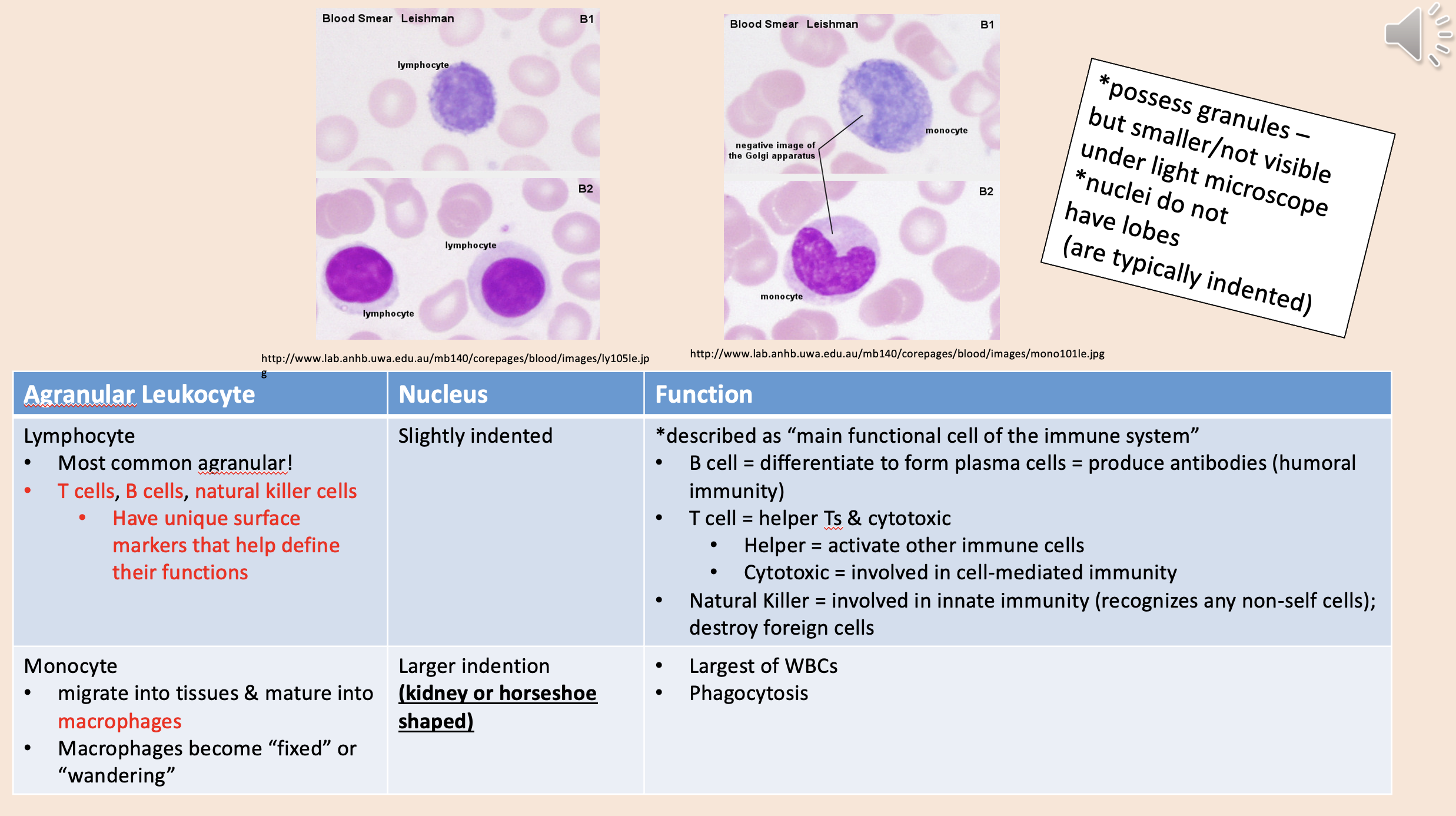
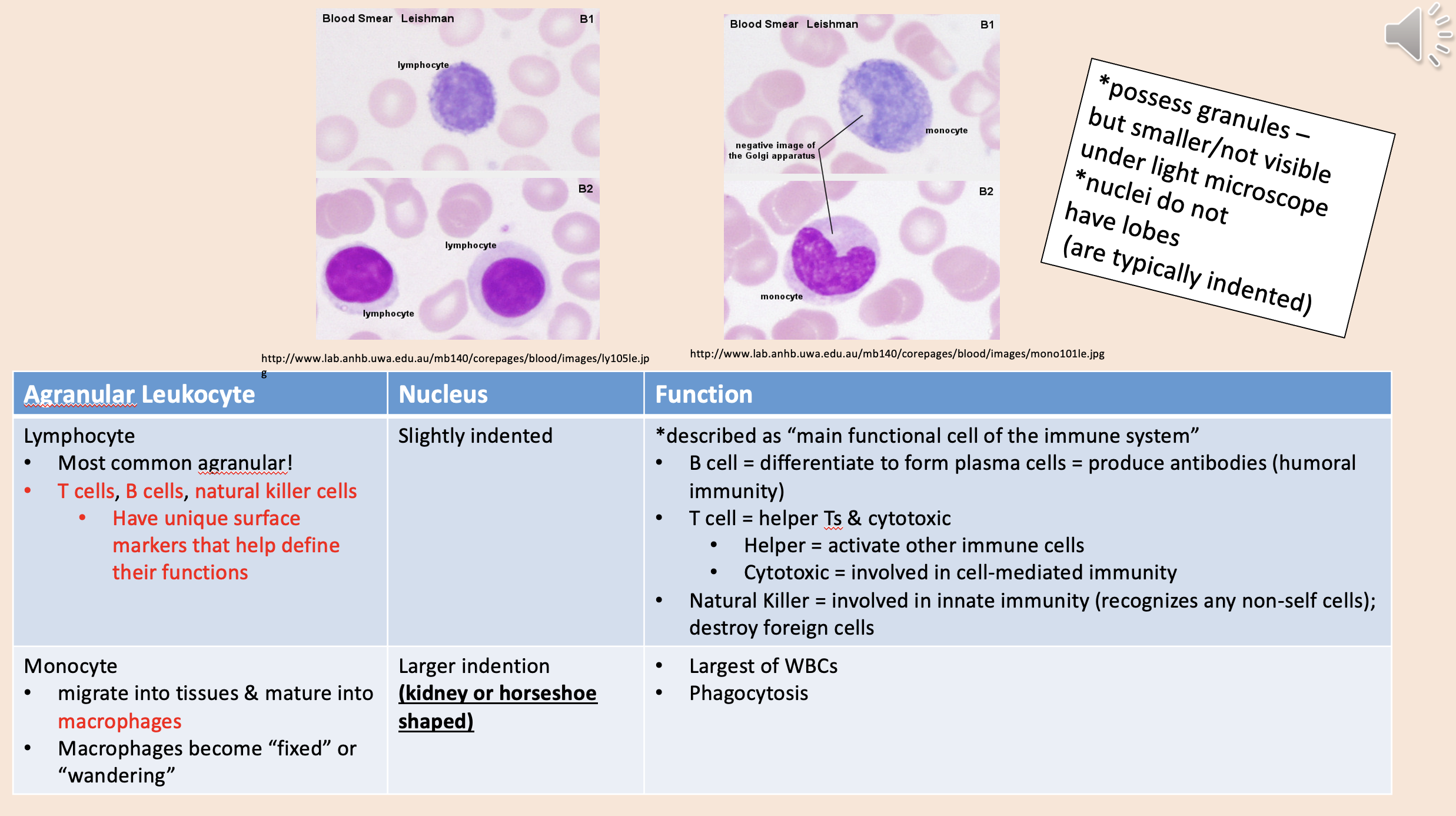
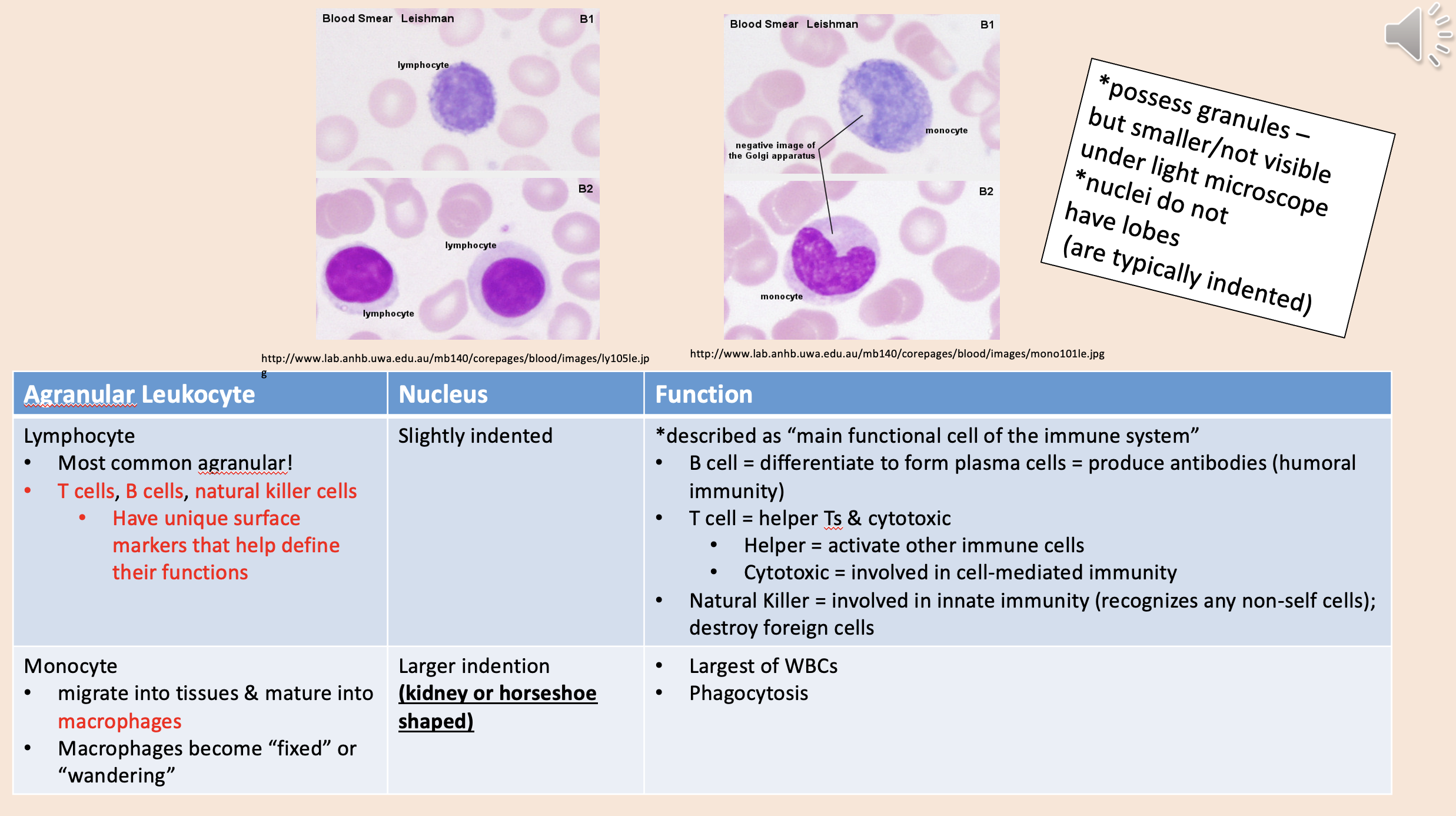
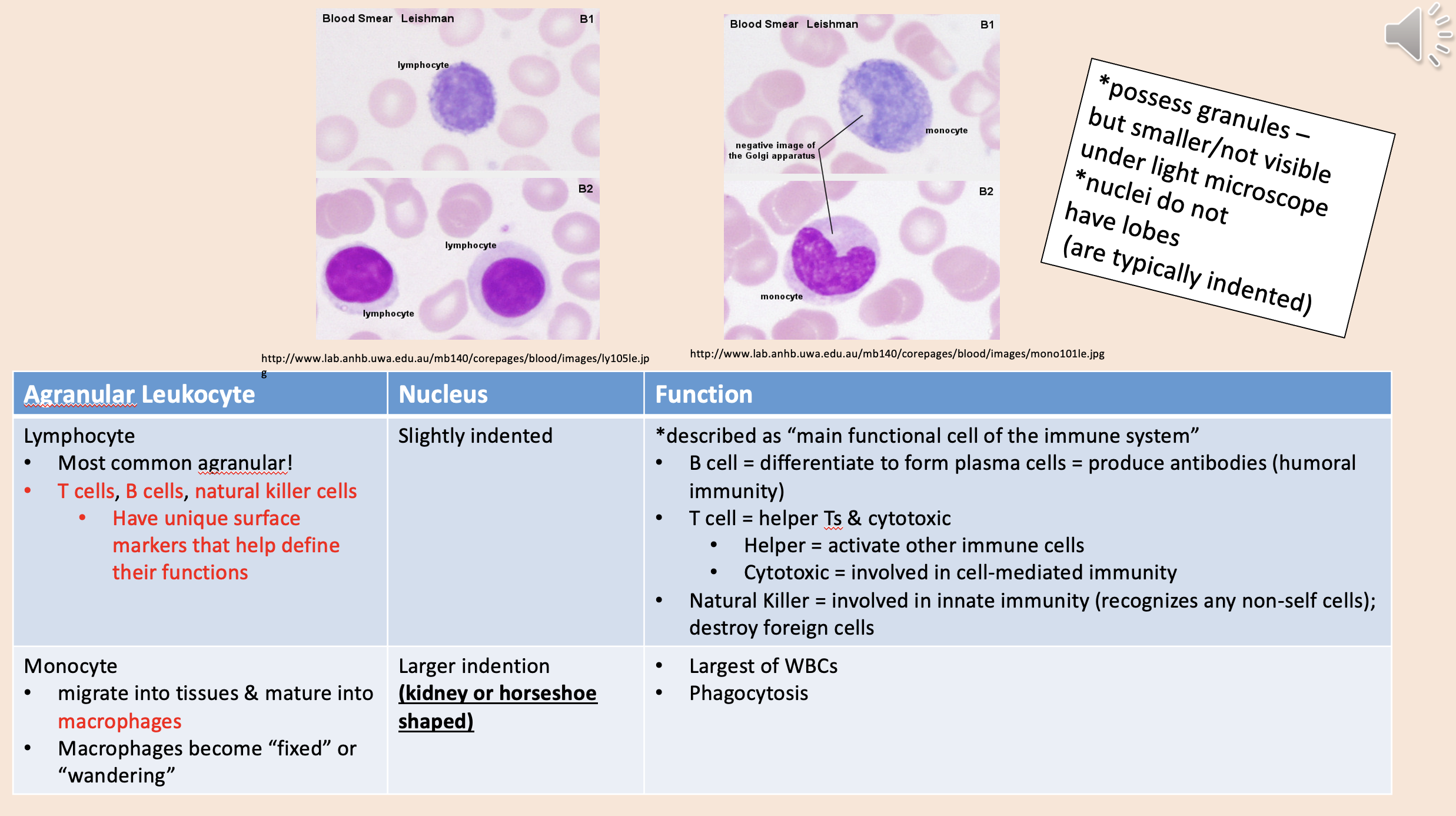
Most common agranular!
T cells, B cells, natural killer cells.
Described as “main functional cell of the immune system.
lymphocyte
Differentiate to form plasma cells = produce antibodies (humoral immunity)
B cell
Helper Ts & cytotoxic
T cell
Activate other immune cells
helper
Involved in cell-mediated immunity
cytotoxic
Involved in innate immunity (recognizes any non-self cells); destroy foreign cells.
natural killer
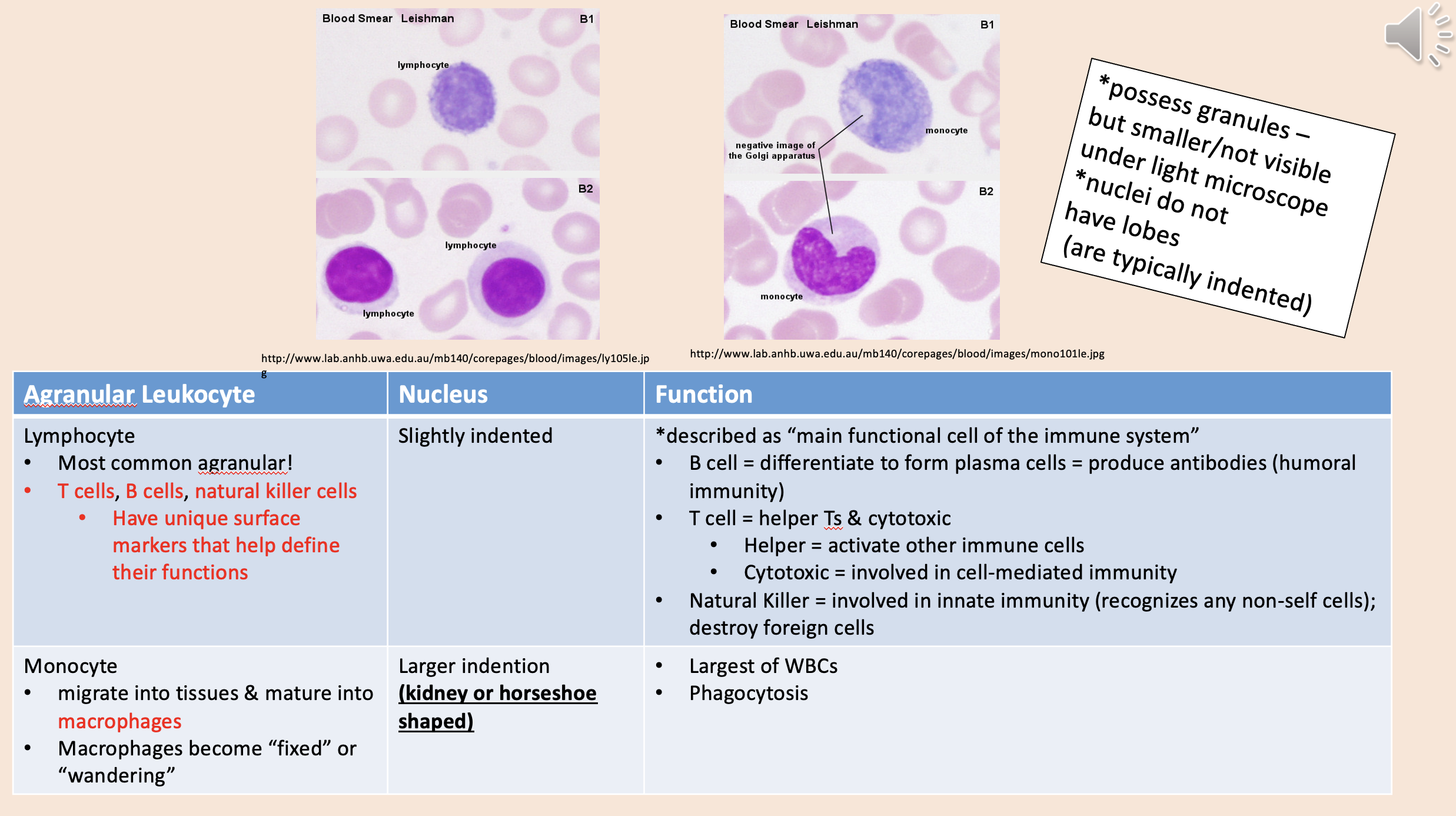
Migrate into tissues & mature into macrophages.
Macrophages become “fixed” or “wandering”.
monocyte
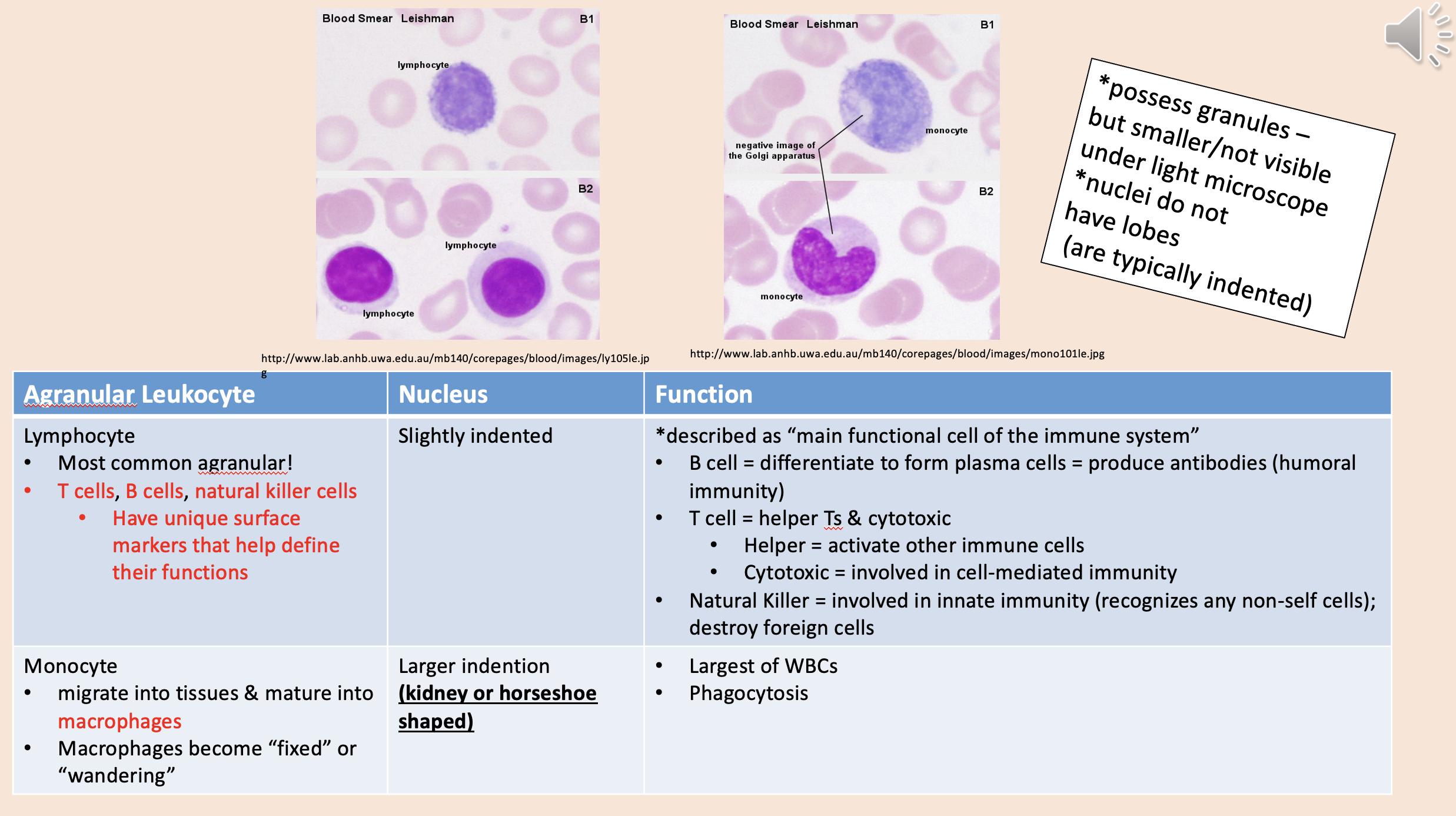
Largest of WBCs.
Phagocytosis.
monocyte function
aka platelets
thrombocytes

Fragments of cells
mgakaryocytes.

Release chemicals used for blood clotting when necessary form a
platelet plug

Platelet plug formation is a key step in
hemostasis

Sequence of responses to stop bleeding/prevent hemorrhage
hemostasis

Hemostasis sequence of responses
vascular constriction/spasms.
platelet plug formation.
blood clotting.

aka gel formation or coagulation
blood clotting

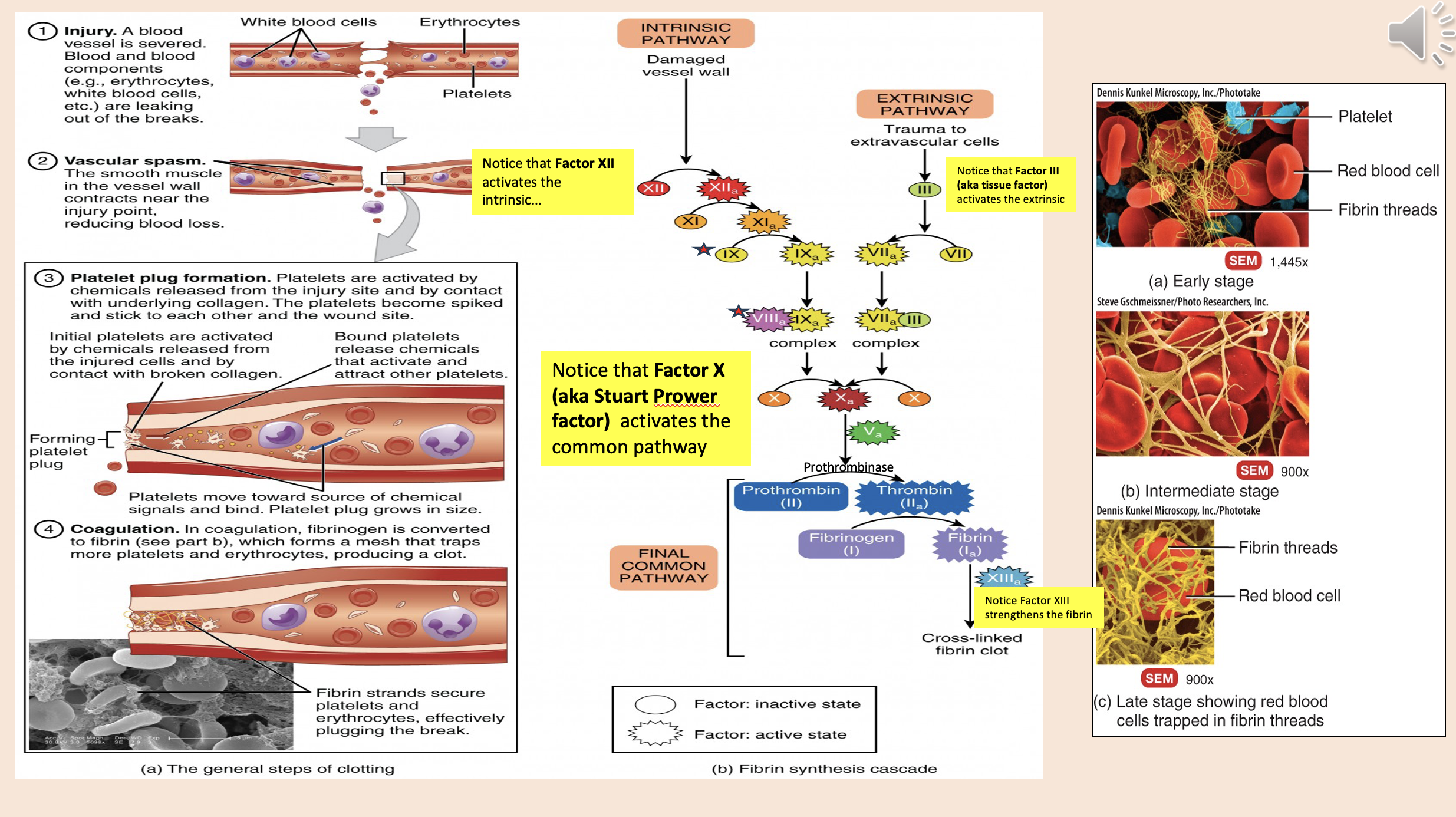
Factor XII activates
intrinsic
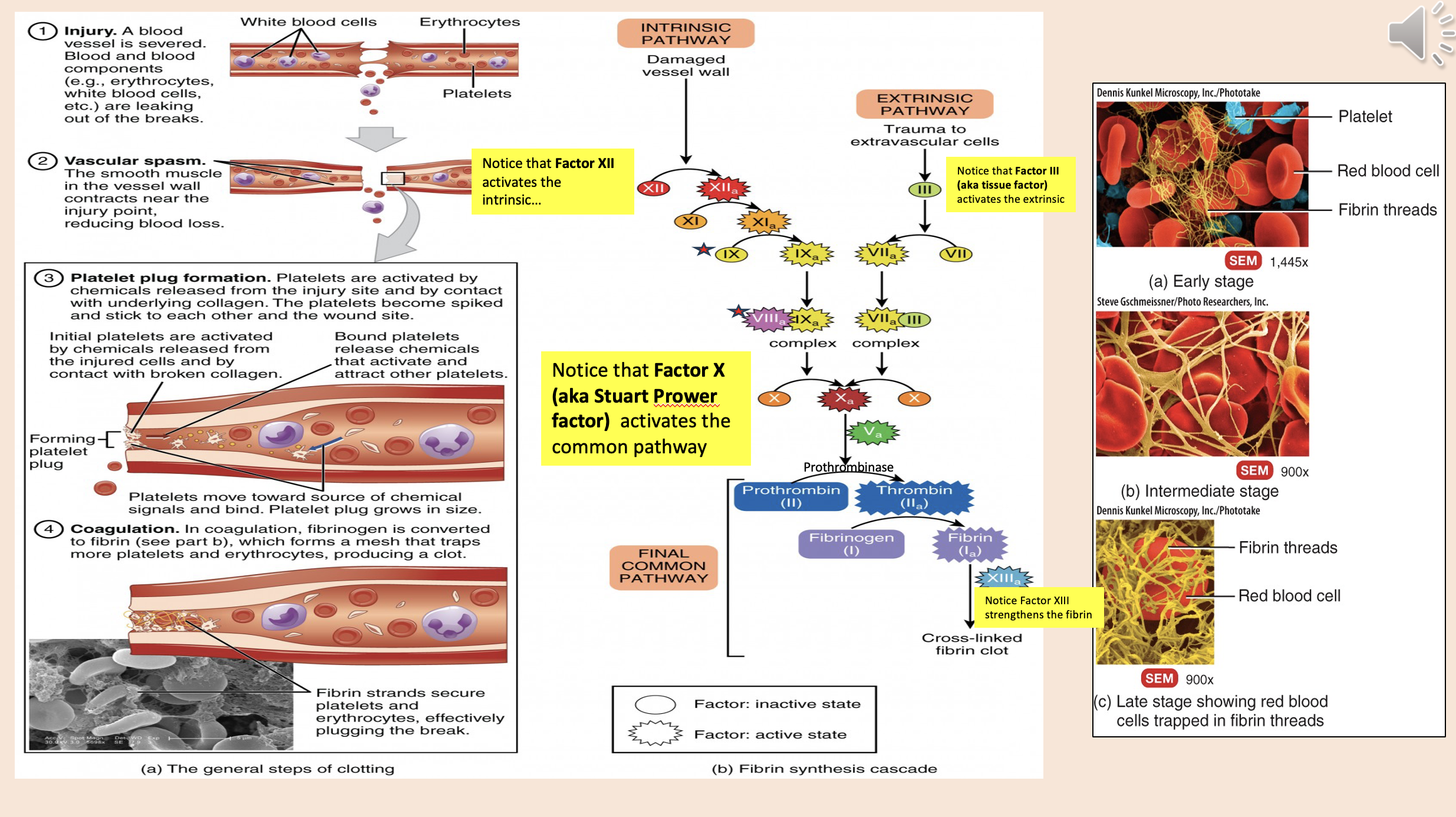
Factor X (aka Stuart Prower factor) activates
common pathway
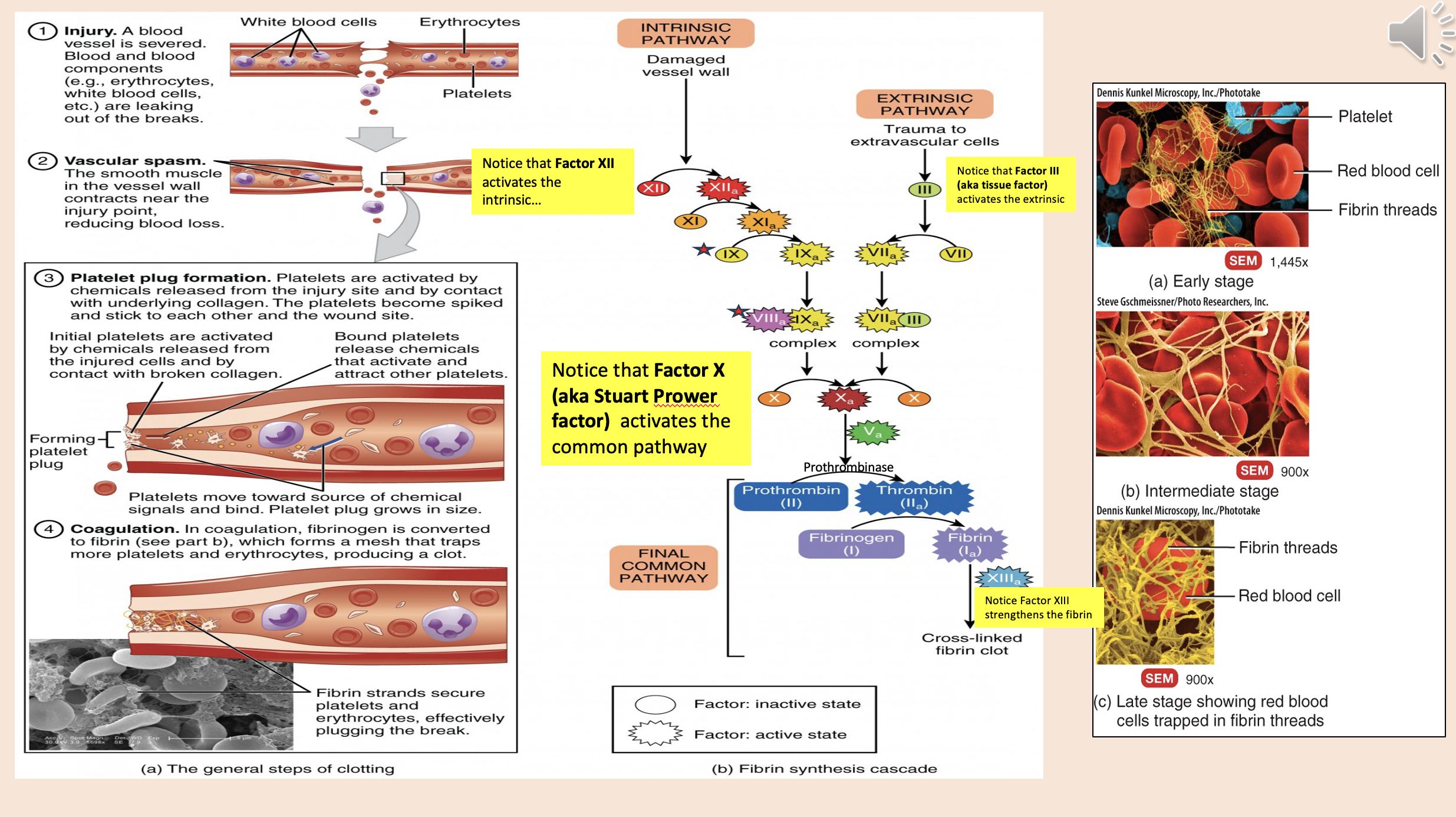
Factor III (aka tissue factor)
extrinsic
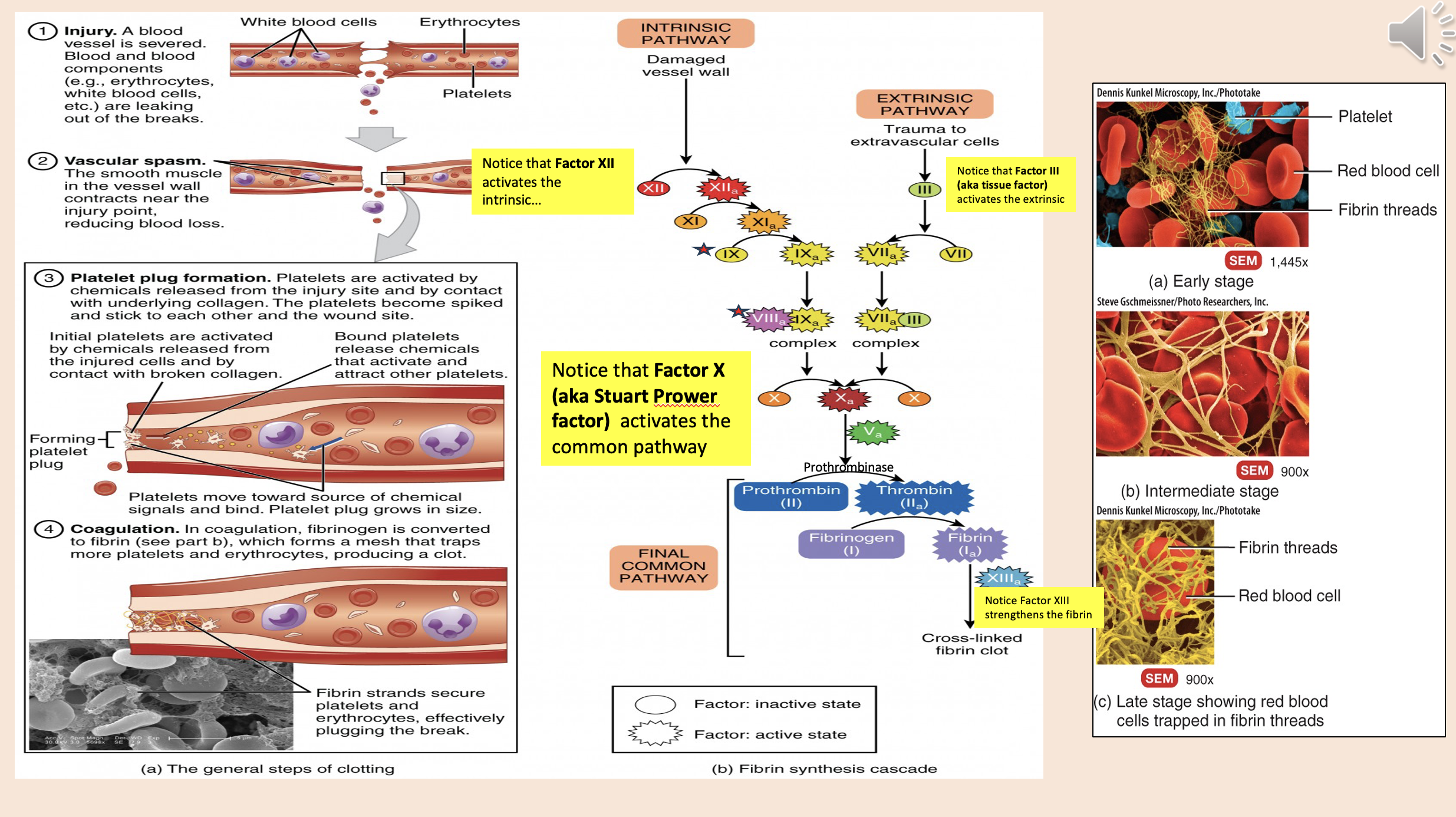
Factor XIII strengthens the
fibrin
The regression in size of the blood clot & pulling of vessel edges together
clot retraction

Platelet contractile proteins pull on the fibrin = fibrin contracts = fibrin twists and knots form
reduced clot size

Degradation of the fibrin clot while macrophages consume the platelets
fibrinolysis

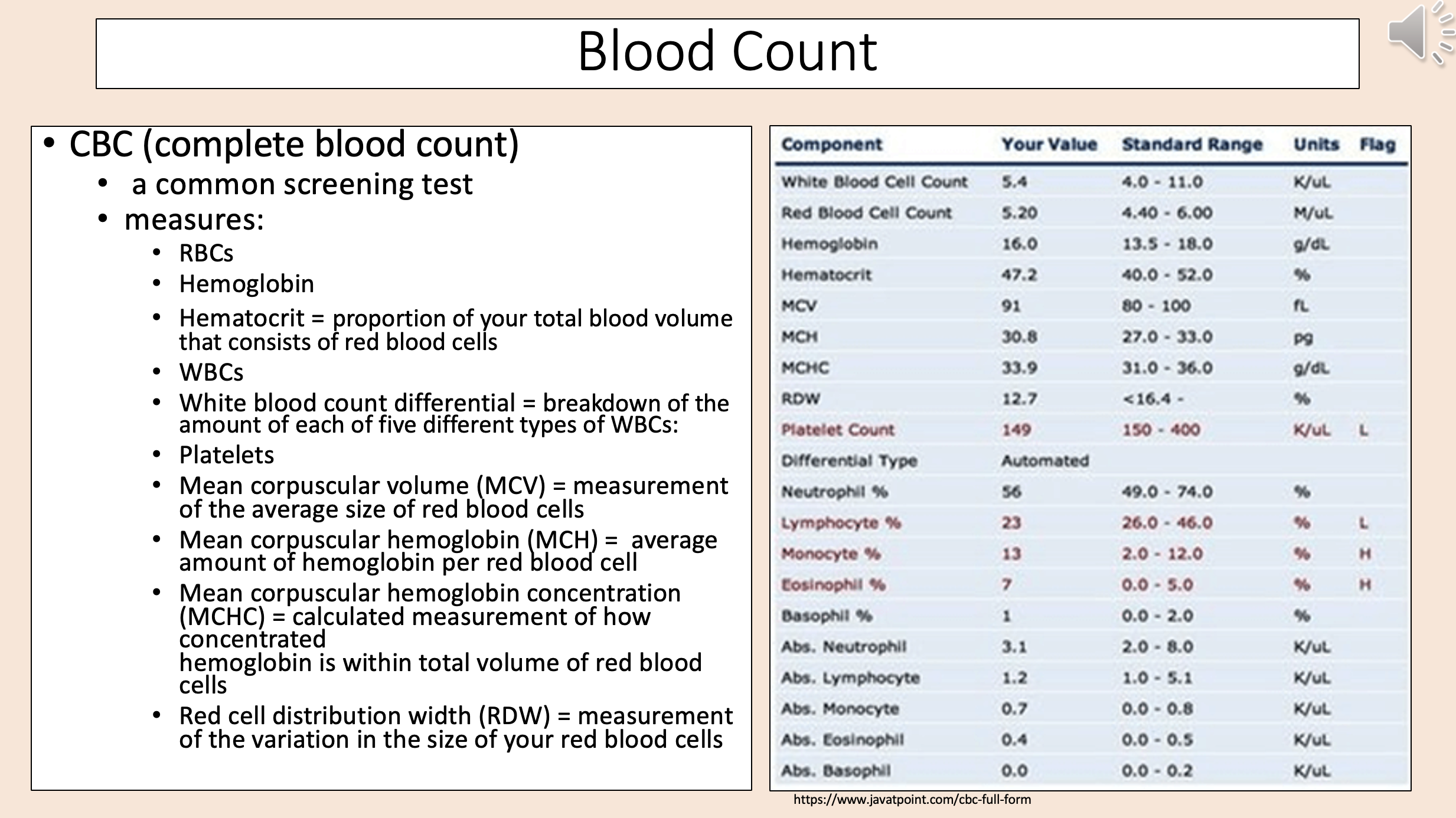
CBC
complete blood count
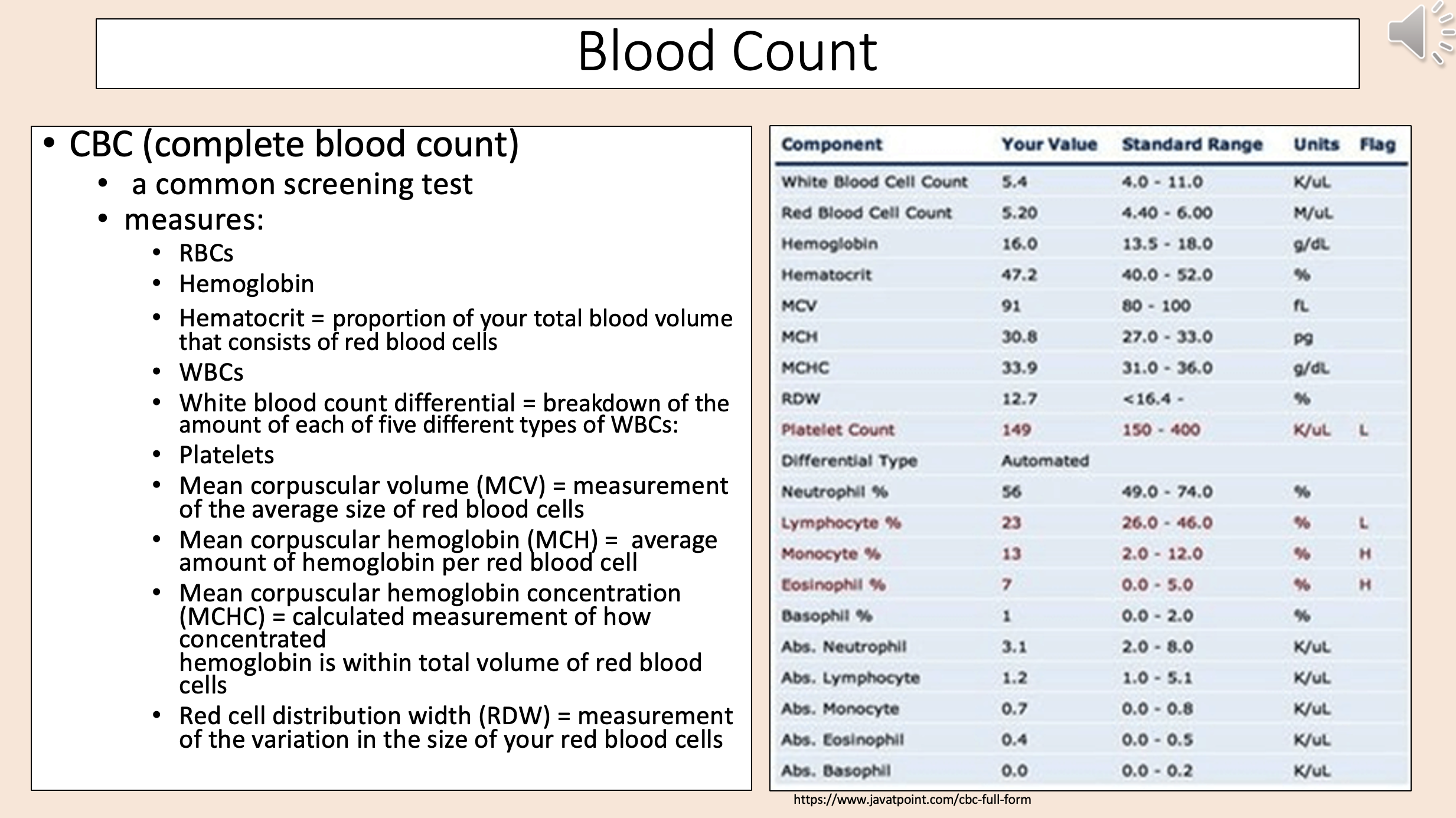
Proportion of your total blood volume that consists of red blood cells
hematocrit
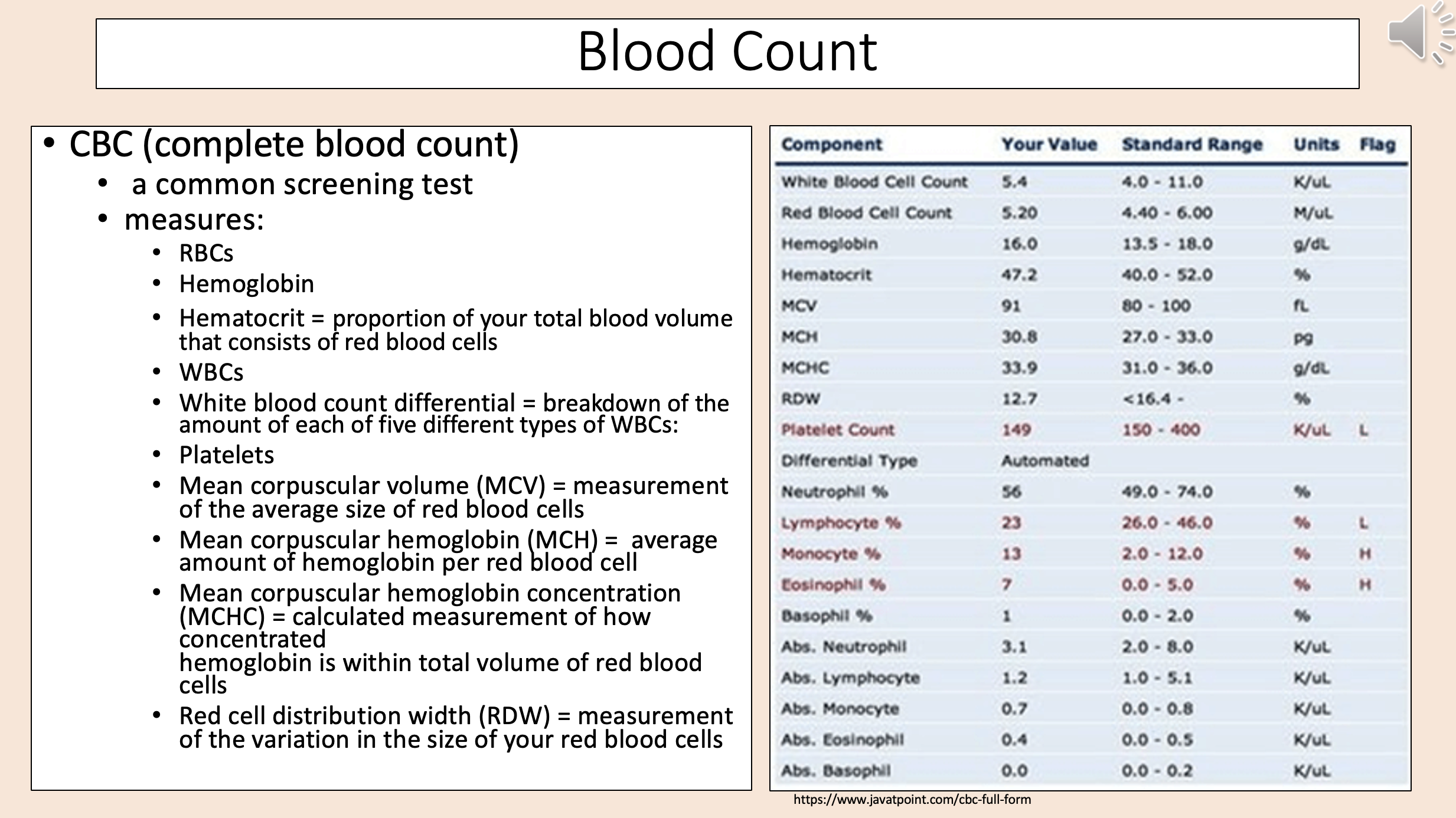
Break down of the amount of each of five different types of WBCs
white blood count differential
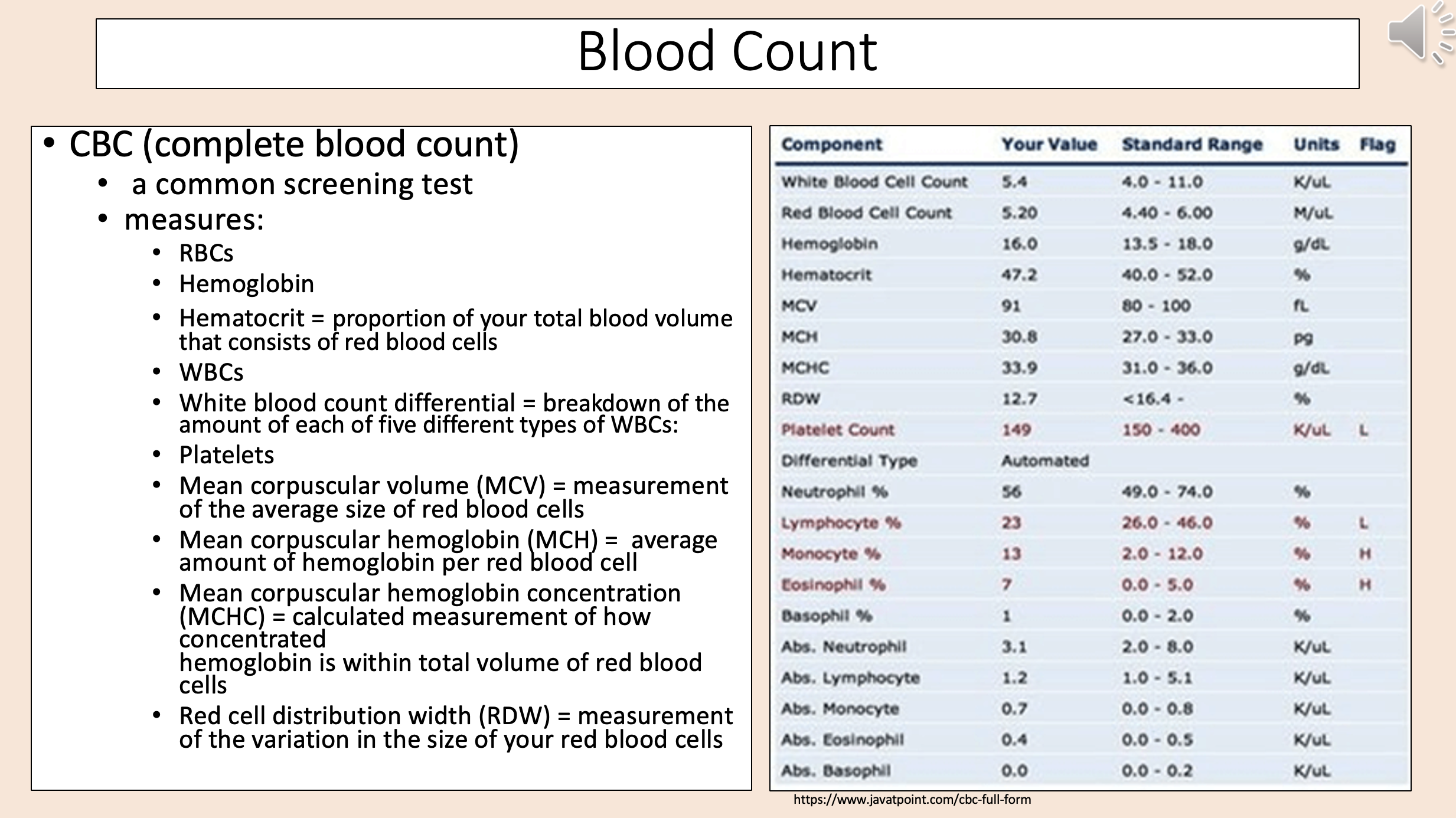
Measurement of the average size of red blood cells
mean corpuscular volume (MCV)
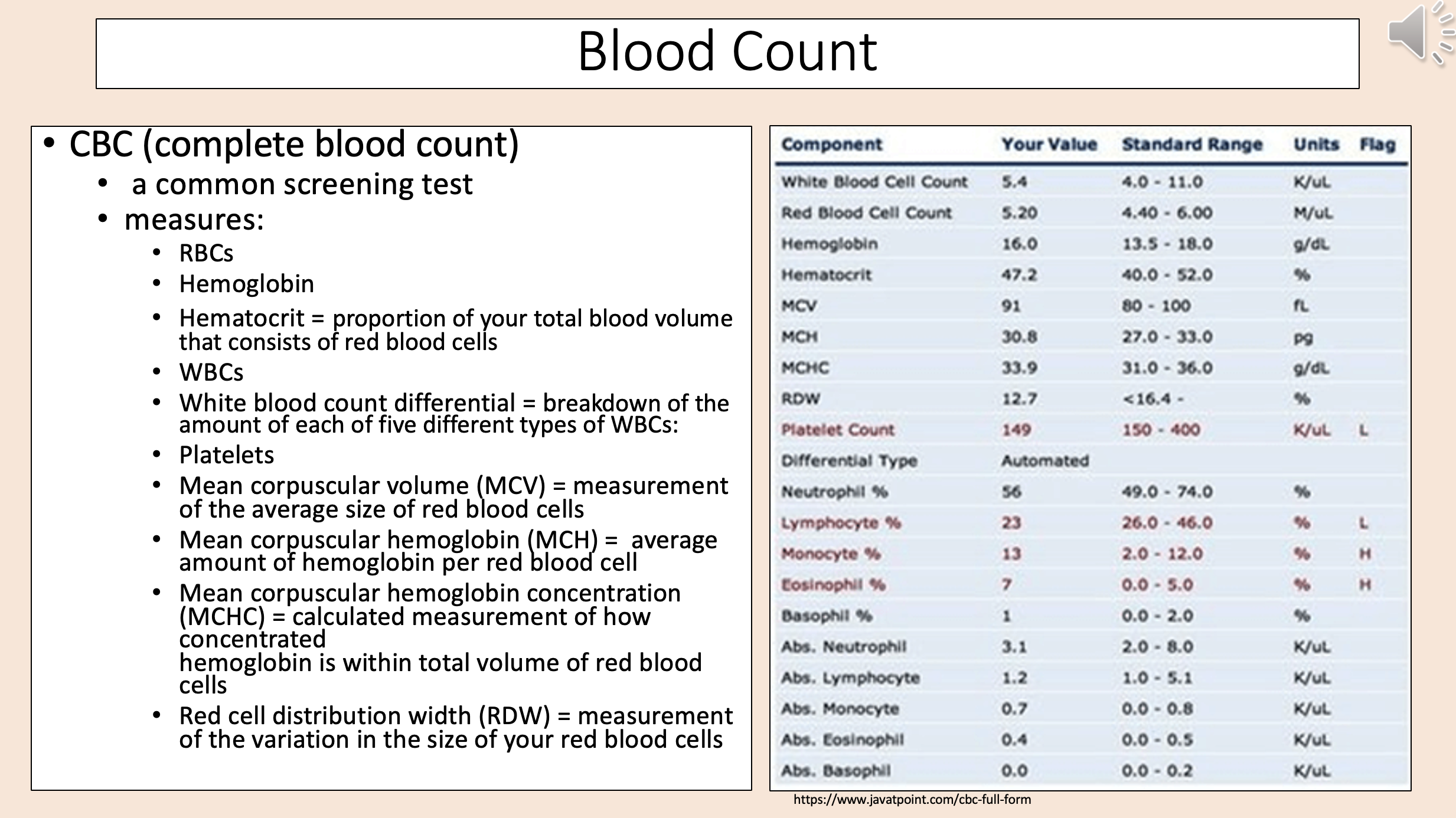
Average amount of hemoglobin per red blood cell
mean corpuscular hemoglobin (MCH)
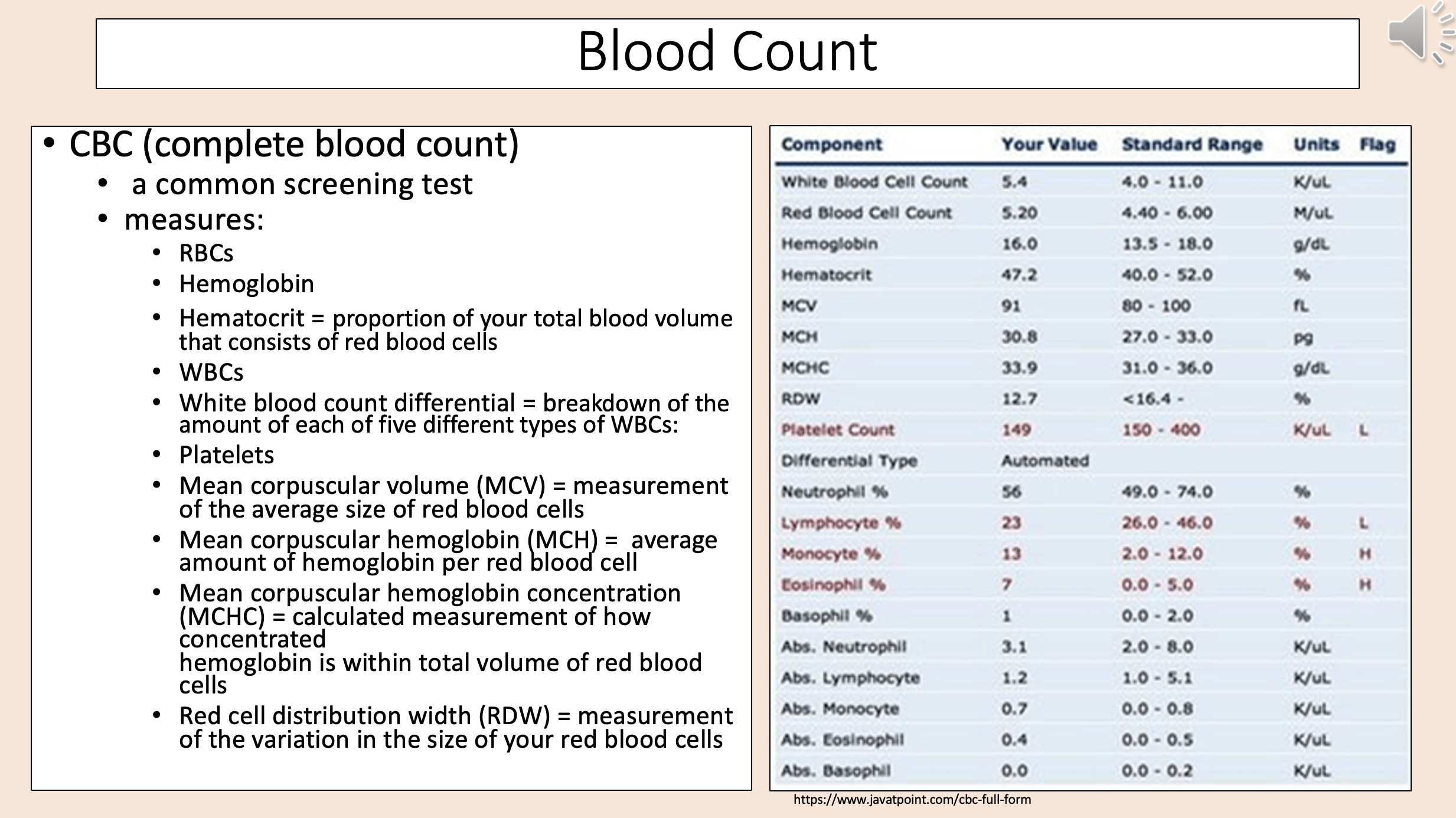
Calculated measurement of how concentrated
mean corpuscular hemoglobin concentration (MCHC)
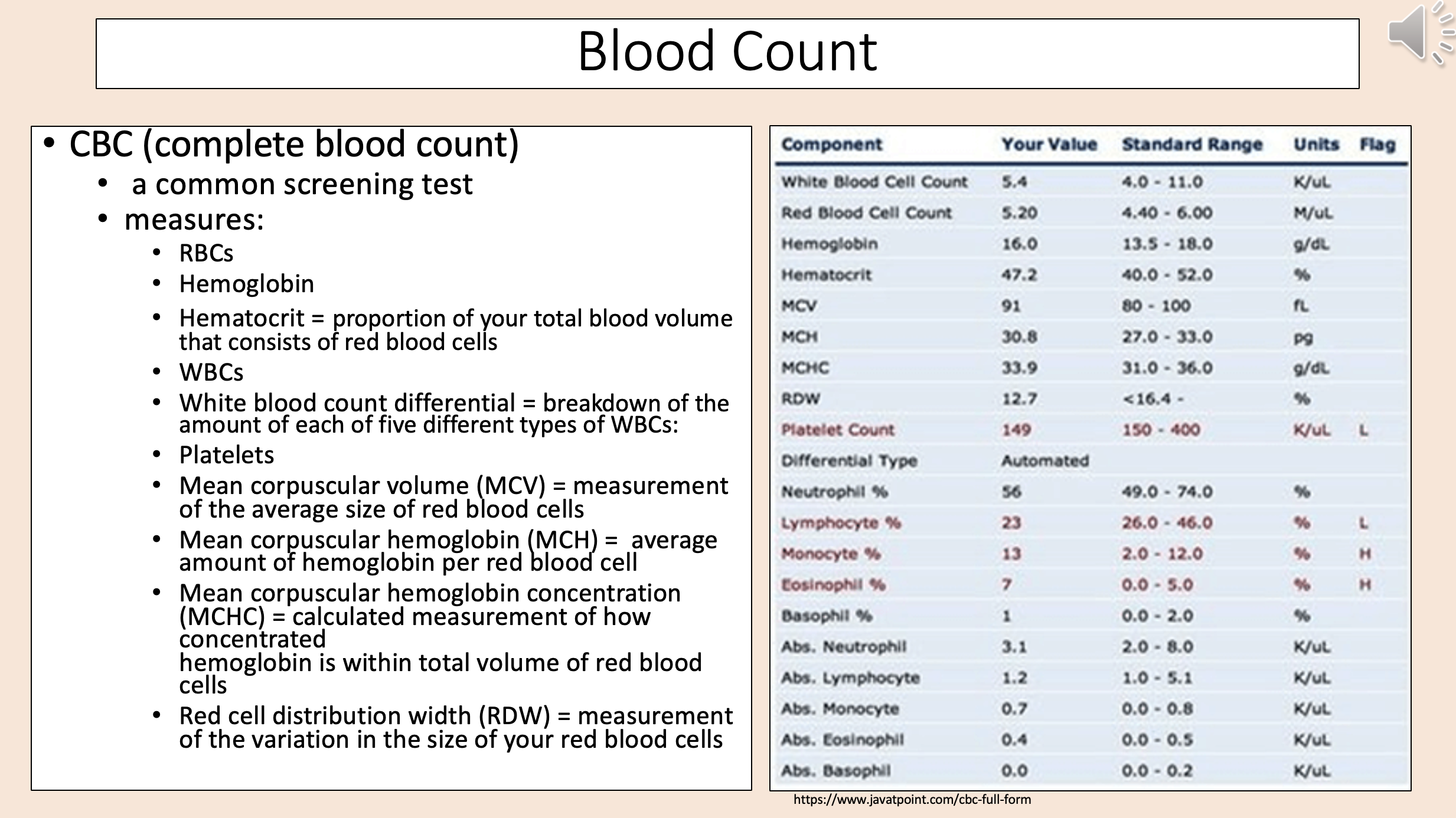
Measurement of the variation in the size of your red blood cells
red cell distribution width (RDW)