RN Maternal Newborn Online Practice 2023 A
1/54
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
55 Terms
A nurse is assessing the newborn of a client who took a selective serotonin reuptake inhibitor (SSRI) during pregnancy. Which of the following manifestations should the nurse identify as an indication of withdrawal from an SSRI?
Large for gestational age
Hyperglycemia
Bradypnea
Vomiting
Bradypnea
Newborns exposed to selective serotonin reuptake inhibitors (SSRIs) in utero may experience SSRI withdrawal syndrome, which manifests as:
Respiratory distress (including bradypnea or tachypnea)
Irritability, jitteriness, and tremors
Hypoglycemia
Poor feeding and weak cry
Hypothermia
Large for gestational age (LGA): SSRI use is not associated with excessive fetal growth. LGA is more common in maternal diabetes or gestational diabetes.
Hyperglycemia: Neonatal withdrawal from SSRIs is more likely to cause hypoglycemia, not hyperglycemia.
Vomiting: While newborns may have poor feeding due to withdrawal, vomiting is not a primary symptom of SSRI withdrawal.
A nurse in a family planning clinic is caring for a client who requests an oral contraceptive. Which of the following findings in the client's history should the nurse recognize as a contraindication to oral contraceptives? (Select all that apply.)
Cholecystitis
Hypertension
Human papillomavirus
Migraine headaches
Anxiety disorder
Migraine headaches
Cholecystitis
Hypertension
Certain conditions increase the risk of complications with oral contraceptive (OC) use, particularly due to the estrogen component, which can contribute to thromboembolic events and other cardiovascular risks.
Cholecystitis – Oral contraceptives increase cholesterol levels and can contribute to gallbladder disease by slowing bile flow, which may worsen conditions like cholecystitis or a history of gallstones.
Hypertension – Estrogen in combined oral contraceptives (COCs) can cause fluid retention and increase blood pressure, leading to stroke or cardiovascular complications. Women with uncontrolled or severe hypertension should avoid OCs.
Migraine headaches – Women who experience migraines with aura are at increased risk for stroke with estrogen-containing contraceptives due to the potential for vasoconstriction and thrombotic events.
Human papillomavirus (HPV) – HPV is not a contraindication for oral contraceptives. OCs do not worsen HPV infections or increase the risk of cervical cancer progression. However, regular Pap smears are still advised.
Anxiety disorder – Anxiety does not affect the safety of oral contraceptives. OCs may even help with premenstrual mood fluctuations, though they do not treat anxiety directly.
Erb-Duchenne (Erb’s) palsy Nursing Actions
Educate the parents to begin range of motion exercises on the affected arm after 1 week. – Indicated
Early passive range of motion (ROM) exercises are essential to prevent contractures and promote recovery. These exercises typically start after the first week to allow initial healing.
Assess for grasp reflex in the affected extremity. – Indicated
The grasp reflex should remain intact because Erb’s palsy affects only motor function, not sensory or reflex functions of the hand. A diminished grasp reflex may indicate a more severe injury, such as Klumpke’s palsy (lower brachial plexus injury).
Immobilize the arm across the abdomen by pinning the newborn’s sleeve to their shirt. – Indicated
Immobilization in the adducted, flexed position prevents further stretching of the injured nerves, allowing them to heal. Pinning the sleeve to the newborn’s shirt helps prevent excessive movement while promoting gradual nerve recovery.
Instruct parents to limit physical handling for 2 weeks. – Contraindicated
Limiting physical handling is not recommended because passive ROM exercises and gentle movement are encouraged to prevent stiffness and muscle atrophy. Instead, parents should be taught proper handling techniques to avoid putting pressure on the affected arm.
A nurse is admitting a client to the labor and delivery unit when the client states, "My water just broke." Which of the following interventions is the nurse's priority?
Perform Nitrazine testing.
Assess the fluid.
Check cervical dilation.
Begin FHR monitoring.
Begin FHR monitoring.
Step-by-Step Nursing Actions:
Immediately assess FHR using external fetal monitoring or Doppler to detect signs of distress (e.g., variable decelerations due to cord compression).
Assess the amniotic fluid for color, odor, and amount to check for meconium-stained fluid (which may indicate fetal distress).
Perform Nitrazine or ferning test if needed to confirm ROM, but this is not the first priority.
Check cervical dilation to determine labor progress, but this is secondary to fetal monitoring.
Graphic Record Blood pressure 130/78 mm Hg Respiratory rate 20/min Heart rate 90/min
Diagnostic Results Hemoglobin 12 g/dL (11 to 16 g/dL) Hematocrit 34% (33% to 47%) 1-hr glucose tolerance test 120 mg/dL (less than 180-190 mg/dL)
Progress Notes Fundal height 30 cm Good fetal movement Not experiencing headache, dizziness, blurred vision, or vaginal bleeding Fetal heart rate 110/min
A nurse in an antepartum clinic is providing care for a client who is at 26 weeks of gestation. Upon reviewing the client's medical record, which of the following findings should the nurse report to the provider?
The nurse should report the fetal heart rate (FHR) of 110 beats per minute (bpm) to the provider.
An FHR of 110 bpm is at the lower limit of normal and could indicate fetal bradycardia or potential fetal distress.
Blood pressure (130/78 mmHg) → Within normal limits for pregnancy.
Respiratory rate (20/min) and heart rate (90/min) → Normal.
Hemoglobin (12 g/dL) and hematocrit (34%) → Within the expected range for pregnancy.
1-hour glucose tolerance test (120 mg/dL) → Well below the threshold for gestational diabetes screening (typically 180-190 mg/dL).
Fundal height (30 cm) → Slightly above the expected range for 26 weeks (fundal height usually correlates with gestational age in cm). However, this alone is not necessarily alarming if fetal growth has been consistently normal.
No symptoms of preeclampsia or bleeding → The absence of headaches, dizziness, blurred vision, or vaginal bleeding is reassuring.
neonatal abstinence syndrome (NAS(
A withdrawal syndrome that occurs in newborns when their mothers have used certain drugs during pregnancy, most commonly opioids.
Symptoms
Irritability and excessive crying
Tremors and jitteriness
Seizures
Poor feeding and weight gain
Sleep disturbances
Diarrhea and vomiting
Fever
High-pitched cry
Vital Signs
Day 2, 0900:
Heart rate 174/min
Respiratory rate 88/min
Temperature 36.1° C (97.0° F)
Oxygen saturation 97% on room air
Diagnostic Results
Day 1, 0800: Newborn results
Blood type: A+
Urine toxicology screen: positive marijuana
Day 2, 0800: Newborn results
Total bilirubin 10 mg/dL (1.0 to 12.0 mg/dL)
Day 2, 0915:
Blood glucose: 38 mg/dL (expected value greater than 40 to 45 gm/dL
Nurses Notes
Day 2, 0900:
Newborn awake, alert, and crying. Loosely wrapped in one blanket. Mild tremors noted. Yellow discoloration of mucus membranes and sclera noted. Respirations 88/min, no retractions, grunting, or nasal flaring noted. Diaper changed for small amount of urine and transitional stool.
Medical History
Apgars: 7 at 1 min and 8 at 5 min of age
Birth weight: 3,515 g (7 lb 12 oz)
Maternal blood type: O+
Uncomplicated pregnancy. Maternal use of marijuana during pregnancy
Client who gave birth plans to breastfeed.
Based on the assessment findings, the newborn is most likely experiencing Neonatal Abstinence Syndrome (NAS) due to maternal marijuana use and Acute Bilirubin Encephalopathy due to elevated bilirubin levels and jaundice.
Potential Condition to Select:
Neonatal Abstinence Syndrome (NAS)
Supporting Findings:
Neurological Signs: Mild tremors
Respiratory Findings: Tachypnea (88/min)
Metabolic Instability: Low blood glucose (38 mg/dL)
Jaundice: Yellow discoloration of mucus membranes and sclera
Maternal History: Marijuana use in pregnancy (although marijuana is not the most common cause of NAS, withdrawal symptoms may still occur)
Actions to Take:
Perform neonatal abstinence system scoring.
This helps quantify withdrawal severity and determine treatment needs.
Encourage birthing parent to breastfeed.
Breastfeeding can help stabilize blood glucose and provide comfort to the newborn experiencing withdrawal symptoms.
Parameters to Monitor:
Blood glucose level
The newborn is hypoglycemic (38 mg/dL). Frequent monitoring is needed.
Bilirubin level
The newborn is jaundiced with a bilirubin level of 10 mg/dL. Monitoring bilirubin levels will help assess the risk of hyperbilirubinemia progression.
A nurse is caring for a client who is at 22 weeks of gestation and is HIV positive. Which of the following actions should the nurse take?
Administer penicillin G 2.4 million units IM to the client.
Instruct the client to schedule an annual pelvic examination.
Tell the client they will start medication for HIV immediately after delivery.
Report the client's condition to the local health department.
Report the client's condition to the local health department.
HIV is a reportable disease in all states, meaning healthcare providers are required to notify the local health department to ensure proper tracking, treatment, and public health measures. This is important for monitoring trends, preventing further transmission, and ensuring that the client has access to resources.
Administer penicillin G 2.4 million units IM
This treatment is used for syphilis, not HIV. While individuals with HIV may have co-infections like syphilis, penicillin G is not a standard treatment for HIV.
Instruct the client to schedule an annual pelvic examination
Women with HIV should have more frequent pelvic exams and Pap smears due to an increased risk of HPV and cervical cancer. Annual screening alone may not be sufficient.
Tell the client they will start medication for HIV immediately after delivery
Incorrect because HIV treatment should start immediately, not after delivery. Antiretroviral therapy (ART) should be initiated during pregnancy to reduce maternal viral load and decrease the risk of vertical transmission (mother-to-baby transmission).
A nurse is caring for a client who is at 10 weeks of gestation. Which of the following findings should the nurse report to the provider?
Frequent vomiting with weight loss of 3 lb in 1 week
Reports of mood swings
Nosebleeds occurring approximately 3 times per week
Increased vaginal discharge
Frequent vomiting with weight loss of 3 lb in 1 week
Frequent vomiting accompanied by significant weight loss (≥ 5% of pre-pregnancy weight or ~3 lb in 1 week) during early pregnancy could indicate hyperemesis gravidarum, a condition that requires medical evaluation. This condition can lead to dehydration, electrolyte imbalances, and nutritional deficiencies, potentially harming both the mother and fetus. The nurse should report this finding to the provider so that appropriate interventions, such as IV fluid replacement and antiemetics, can be initiated.
Reports of mood swings
Mood swings are a common physiological response to hormonal changes, particularly increased progesterone and estrogen in early pregnancy. No immediate intervention is needed unless symptoms suggest severe depression or anxiety impacting daily functioning.
Nosebleeds occurring approximately 3 times per week
Increased blood volume and vascular congestion from hormonal changes can cause nasal congestion and nosebleeds during pregnancy. While frequent nosebleeds should be monitored, they are not typically an emergency unless accompanied by severe bleeding, high blood pressure, or signs of anemia.
Increased vaginal discharge
Increased vaginal discharge (leukorrhea) is a normal finding in pregnancy due to increased estrogen levels and cervical mucus production. The discharge should be clear or white and odorless. However, the provider should be notified if it is foul-smelling, green, yellow, or associated with itching or pain, as this may indicate an infection.
A nurse is assessing a newborn who is 16 hr old. Which of the following findings should the nurse report to the provider?
Substernal retractions
Acrocyanosis
Overlapping suture lines
Head circumference 33 cm (13 in)
Substernal retractions
A nurse is assessing a late preterm newborn. Which of the following manifestations is an indication of hypoglycemia?
Hypertonia
Increased feeding
Hyperthermia
Respiratory distress
Respiratory distress
Hypoglycemia in a late preterm newborn can present with respiratory distress, including tachypnea, grunting, nasal flaring, retractions, or apnea. Low blood glucose levels impact the newborn’s energy supply, leading to poor respiratory effort and increased oxygen consumption. Late preterm newborns (34-36 weeks gestation) have immature glucose regulation, making them more prone to hypoglycemia.
Hypertonia (Increased muscle tone) ❌
Hypoglycemia typically causes hypotonia (poor muscle tone or lethargy) rather than hypertonia. The newborn may appear floppy, weak, or have poor reflexes due to the lack of available glucose for muscle function.
Increased feeding ❌
Hypoglycemic newborns often have poor feeding due to weak suck, jitteriness, or lethargy. Increased feeding is not a direct sign of hypoglycemia but may occur if the baby is experiencing hunger from normal glucose fluctuations.
Hyperthermia (High body temperature) ❌
Hypoglycemia is more commonly associated with hypothermia (low body temperature) rather than hyperthermia. Newborns rely on glucose for thermoregulation, so low glucose can lead to cold stress, not fever.
A nurse is assessing a client who gave birth vaginally 12 hr ago and palpates their uterus to the right above the umbilicus. Which of the following interventions should the nurse perform?
Reassess the client in 2 hr.
Administer simethicone.
Assist the client to empty their bladder.
Instruct the client to lie on their right side.
Assist the client to empty their bladder.
A nurse is developing a plan of care for a newborn who is to undergo phototherapy for hyperbilirubinemia. Which of the following actions should the nurse include in the plan?
Feed the newborn 1 oz of water every 4 hr.
Apply lotion to the newborn's skin three times per day.
Remove all clothing from the newborn except the diaper.
Discontinue therapy if the newborn develops a rash.
Remove all clothing from the newborn except the diaper.
Feed the newborn 1 oz of water every 4 hr. ❌
Water supplementation is NOT recommended for newborns undergoing phototherapy.
Breast milk or formula should be provided frequently (every 2-3 hours) to promote bilirubin excretion through stools and urine.
Giving water displaces nutrient-rich milk and does not help in eliminating bilirubin effectively.
Apply lotion to the newborn's skin three times per day. ❌
Lotions or ointments should NOT be applied to the newborn’s skin during phototherapy.
The heat from phototherapy can increase skin breakdown and absorption of chemicals from lotions, potentially causing irritation or burns.
Discontinue therapy if the newborn develops a rash. ❌
A mild rash (transient maculopapular rash) is a common side effect of phototherapy and is not a reason to stop treatment.
Phototherapy should only be discontinued if there are severe adverse effects, such as dehydration, excessive lethargy, or worsening bilirubin levels.
A nurse is planning care for a client who is to undergo a nonstress test. Which of the following actions should the nurse include in the plan of care?
Maintain the client NPO throughout the procedure.
Place the client in a supine position.
Instruct the client to massage the abdomen to stimulate fetal movement.
Instruct the client to press the provided button each time fetal movement is detected.
Instruct the client to press the provided button each time fetal movement is detected.
A nurse is providing dietary teaching to a client who has hyperemesis gravidarum. Which of the following statements by the client indicates an understanding of the teaching?
"I will eat foods that taste good instead of balancing my meals."
"I will avoid having a snack before I go to bed each night."
"I will have a cup of hot tea with each meal."
"I will eliminate products that contain dairy from my diet."
"I will eat foods that taste good instead of balancing my meals."
A nurse is teaching a client who is at 10 weeks of gestation about nutrition during pregnancy. Which of the following statements by the client indicates an understanding of the teaching?
"I should increase my protein intake to 60 grams each day."
"I should drink 2 liters of water each day."
"I should increase my overall daily caloric intake by 300 calories."
"I should take 600 micrograms of folic acid each day."
"I should take 600 micrograms of folic acid each day."
regnant clients should consume 600 mcg (0.6 mg) of folic acid daily to help prevent neural tube defects (e.g., spina bifida, anencephaly) in the developing fetus. Folic acid is crucial for DNA synthesis and fetal development, especially in the first trimester when the neural tube is forming.
"I should increase my protein intake to 60 grams each day." ❌
While protein is essential for fetal growth, the recommended daily intake during pregnancy is 71 grams per day, not 60 grams.
Protein-rich foods include lean meats, eggs, dairy, legumes, and nuts.
"I should drink 2 liters of water each day." ❌
Pregnant clients should aim for at least 3 liters (8–12 cups) of fluids per day to support increased blood volume, amniotic fluid, and kidney function.
Dehydration can lead to preterm contractions and other complications.
"I should increase my overall daily caloric intake by 300 calories." ❌
The recommended caloric intake depends on gestational age:
First trimester: No additional calories are needed.
Second trimester: Increase by ~340 kcal/day.
Third trimester: Increase by ~450 kcal/day.
The client is at 10 weeks (first trimester), so this statement is incorrect.
A nurse is preparing to administer oxytocin to a client who is postpartum. Which of the following findings is an indication for the administration of the medication? (Select all that apply.)
Flaccid uterus
Cervical laceration
Excess vaginal bleeding
Increased afterbirth cramping
Increased maternal temperature
Flaccid uterus
Excess vaginal bleeding
A nurse is teaching a client who is at 35 weeks of gestation about manifestations of potential pregnancy complications to report to the provider. Which of the following manifestations should the nurse include?
Shortness of breath when climbing stairs
Swelling of feet and ankles at the end of the day
Headache that is unrelieved by analgesia
Braxton Hicks contractions
Headache that is unrelieved by analgesia
A persistent headache that does not improve with analgesia can be a sign of preeclampsia, a serious pregnancy complication characterized by hypertension, proteinuria, and possible organ damage. Severe preeclampsia can progress to eclampsia, which includes seizures. Other warning signs include blurred vision, right upper quadrant pain, and sudden swelling of the face or hands.
A nurse is teaching a postpartum client about steps the nurses will take to promote the security and safety of the client's newborn. Which of the following statements should the nurse make?
"The nurse will carry your baby in their arms to the nursery for scheduled procedures."
"We will document the relationship of visitors in your medical record."
"It's okay for your baby to sleep in the bed with you while in the hospital."
"Staff members who take care of your baby will be wearing a photo identification badge."
"Staff members who take care of your baby will be wearing a photo identification badge."
"The nurse will carry your baby in their arms to the nursery for scheduled procedures." ❌
Incorrect because nurses should transport newborns in a bassinet, not in their arms.
This policy ensures safe transport and prevents accidental drops or abduction risks.
"We will document the relationship of visitors in your medical record." ❌
While visitor check-ins are important, hospitals do not routinely document every visitor’s relationship in the medical record.
Instead, security protocols like visitor wristbands, ID checks, or newborn tagging systems help ensure safety.
"It's okay for your baby to sleep in the bed with you while in the hospital." ❌
Co-sleeping is NOT safe in the hospital due to the risk of suffocation or accidental falls.
The baby should always be placed in a bassinet next to the mother’s bed, following safe sleep guidelines to prevent Sudden Infant Death Syndrome (SIDS).
A nurse is assessing a client who is at 30 weeks of gestation during a routine prenatal visit. Which of the following findings should the nurse report to the provider?
Swelling of the face
Varicose veins in the calves
Nonpitting 1+ ankle edema
Hyperpigmentation of the cheeks
Swelling of the face
Facial swelling is a potential sign of preeclampsia, a serious pregnancy complication characterized by hypertension, proteinuria, and possible organ damage. Swelling of the hands, face, or generalized edema should be reported to the provider immediately, as it may indicate worsening preeclampsia and increased risk for complications such as eclampsia, HELLP syndrome, or placental abruption.
Varicose veins in the calves ❌
Normal finding in pregnancy due to increased blood volume and pressure on leg veins from the growing uterus.
Encouraging elevation of legs, compression stockings, and avoiding prolonged standing can help.
Nonpitting 1+ ankle edema ❌
Mild ankle swelling is common in the third trimester due to fluid retention and decreased venous return.
Concerning edema would be sudden, severe, generalized swelling or pitting edema extending beyond the ankles.
Hyperpigmentation of the cheeks (Melasma or "mask of pregnancy") ❌
Common, harmless skin change due to hormonal shifts increasing melanin production.
It typically fades postpartum and does not require medical intervention.
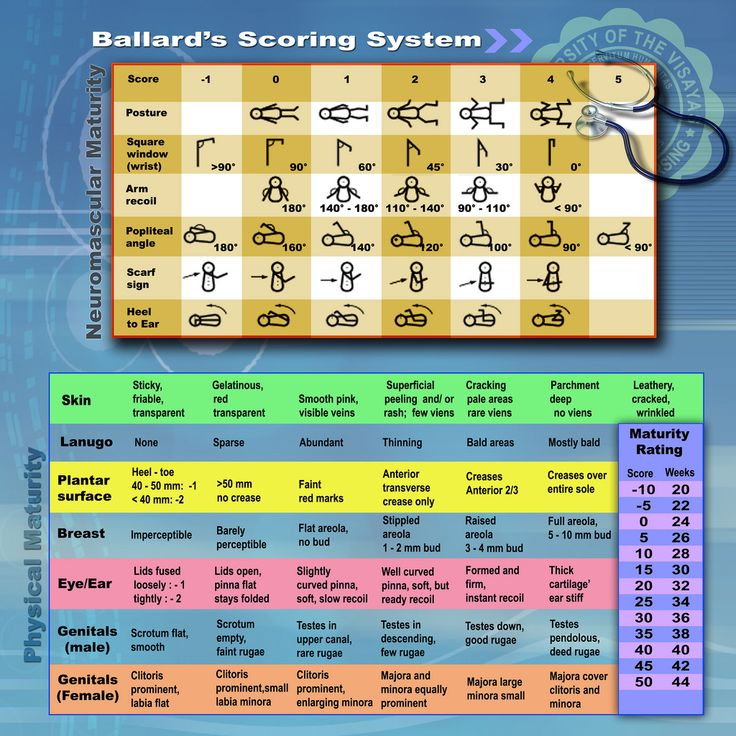
A nurse is assessing a newborn who was born at 26 weeks of gestation using the New Ballard Score. Which of the following findings should the nurse expect?
Minimal arm recoil
Popliteal angle of 90°
Creases over the entire foot sole
Raised areolas with 3 to 4 mm buds
Minimal arm recoil
A newborn born at 26 weeks of gestation is considered extremely preterm and will exhibit low muscle tone and poor flexion due to immature neuromuscular development. Minimal arm recoil is expected because preterm infants have decreased muscle strength and underdeveloped passive flexor tone.
Popliteal angle of 90° ❌
A preterm infant has a greater degree of joint extension due to reduced muscle tone.
A 26-week newborn would likely have a popliteal angle much greater than 90°, meaning the leg extends easily.
A popliteal angle of 90° is seen in more mature infants closer to term.
Creases over the entire foot sole ❌
Preterm infants have smooth soles or very few creases.
Sole creases develop progressively with gestational age, and full foot creases are seen in term newborns (≥37 weeks).
Raised areolas with 3 to 4 mm buds ❌
Breast tissue development occurs later in gestation.
At 26 weeks, the areola is barely visible, flat, or slightly raised, and the breast bud is either absent or very small.
Raised areolas with 3 to 4 mm buds are typically found in full-term newborns (≥37 weeks).
New Ballard Score
Neuromuscular Maturity
Each category is scored from -1 to 5 based on the level of maturity.
Posture
More flexion = higher score
Less flexion = lower score (preterm)
Full-term infants maintain a well-flexed posture.
Square Window (Wrist Flexion)
Measures wrist flexibility by bending the hand toward the forearm.
Preterm infants (>90° wrist angle) = low score.
Full-term infants (<30° wrist angle) = high score.
Arm Recoil
Measures passive extension and recoil of the arms.
Full recoil (return to flexed position) = higher maturity.
Minimal recoil or slow return = prematurity.
Popliteal Angle
Measures knee flexion.
Smaller angle (more flexion) = higher score.
Larger angle (more extension) = lower score.
Scarf Sign
Measures how far the arm can be pulled across the chest.
Preterm infants can pull across easily (low score).
Term infants have resistance (high score).
Heel to Ear
Measures flexibility of the hip.
More resistance = higher score.
Less resistance (heel reaches ear easily) = lower score.
Physical Maturity
Each category is scored based on developmental characteristics of the newborn.
Skin
Preterm: Sticky, fragile, red, or gelatinous.
Term: Peeling, parchment-like, or cracked.
Lanugo (Fine Hair)
Preterm: None or sparse.
Midterm: Abundant.
Term: Mostly bald.
Plantar Surface Creases
Preterm: Few creases.
Term: Creases over the entire sole.
Breast Tissue Development
Preterm: Flat or barely noticeable.
Term: Raised areola with a well-developed bud.
Eye/Ear Development
Preterm: Loose, soft, folds easily.
Term: Firm, developed cartilage with strong recoil.
Genitals (Male and Female)
Male: Testes descend and rugae (wrinkles) develop.
Female: Labia cover the clitoris and minora as gestation progresses.
Maturity Rating (Gestational Age Estimation)
The total score is matched with the corresponding gestational age in weeks:
Score -10 = 20 weeks gestation
Score 0 = 24 weeks gestation
Score 10 = 28 weeks gestation
Score 20 = 32 weeks gestation
Score 30 = 36 weeks gestation
Score 40 = 40 weeks gestation
Score 50 = 44 weeks gestation
A nurse is caring for a client who is in labor and reports increasing rectal pressure. They are experiencing contractions 2 to 3 min apart, each lasting 80 to 90 seconds, and a vaginal examination reveals that their cervix is dilated to 9 cm. The nurse should identify that the client is in which of the following phases of labor?
Passive descent
Active
Early
Descent
Active
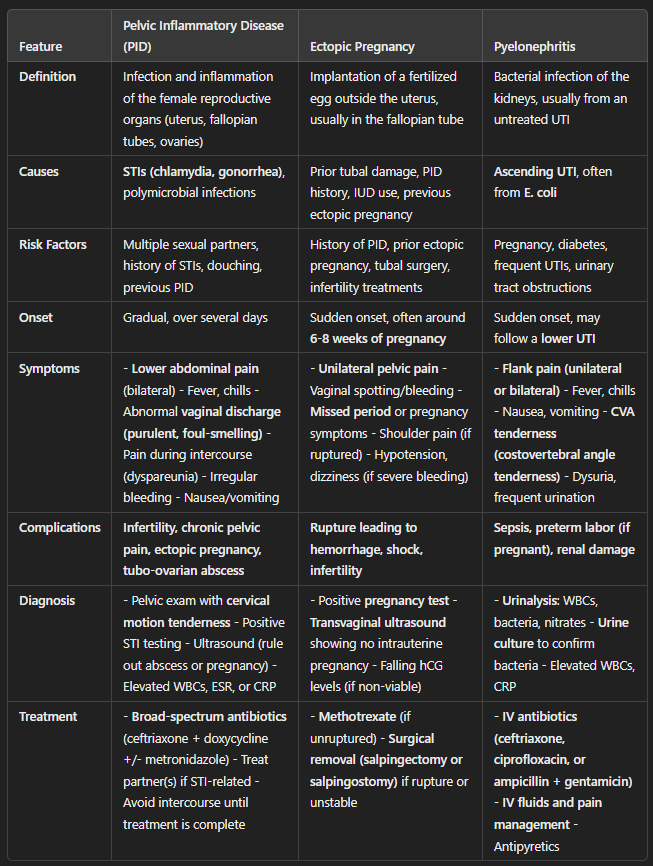
Comparison of Pelvic Inflammatory Disease (PID), Ectopic Pregnancy, and Pyelonephritis (Table)
Key Differences:
Pelvic Inflammatory Disease: Infection-related, often from an STI, leading to bilateral lower abdominal pain and abnormal vaginal discharge.
Ectopic Pregnancy: Unilateral pelvic pain with missed period and vaginal spotting. If ruptured, can cause hypovolemic shock.
Pyelonephritis: Flank pain, fever, chills, and CVA tenderness, often following a UTI.
Nursing Priorities:
PID: Treat with antibiotics, educate on STI prevention, encourage partner treatment.
Ectopic Pregnancy: Monitor for rupture, provide methotrexate or prepare for surgery, and watch for signs of shock.
Pyelonephritis: Administer IV antibiotics, fluids, and pain management, and monitor for sepsis.
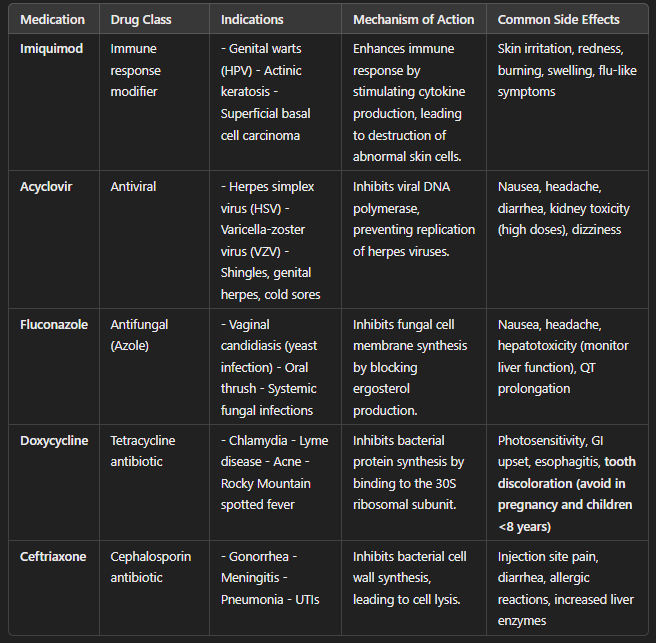
Comparison of Medications: Imiquimod, Acyclovir, Fluconazole, Doxycycline, and Ceftriaxone (Table)
Key Differences:
Imiquimod is used for HPV-related genital warts and works by stimulating the immune system.
Acyclovir is an antiviral that treats herpes infections by stopping viral replication.
Fluconazole is an antifungal used for yeast infections by disrupting fungal cell membranes.
Doxycycline is a broad-spectrum antibiotic that treats chlamydia and other bacterial infections, but should be avoided in pregnancy.
Ceftriaxone is a strong antibiotic often given as an IM injection for gonorrhea.
Nursing Considerations:
Imiquimod: Educate about possible skin irritation; apply at bedtime.
Acyclovir: Increase fluid intake to prevent kidney toxicity.
Fluconazole: Monitor liver function for long-term use.
Doxycycline: Take with plenty of water to prevent esophagitis; avoid sunlight.
Ceftriaxone: Check for penicillin allergies before administration.
💡 Remember:
Acyclovir for viruses, Fluconazole for fungi, Doxycycline & Ceftriaxone for bacteria, Imiquimod for immune response stimulation!
A nurse is reviewing the medical record of a newly admitted client who is at 32 weeks of gestation. Which of the following conditions is an indication for fetal assessment using electronic fetal monitoring?
Oligohydramnios
Hyperemesis gravidarum
Leukorrhea
Periodic tingling of the fingers
Oligohydramnios
A nurse is assessing a client who is postpartum and has idiopathic thrombocytopenia purpura (ITP). Which of the following findings should the nurse expect?
Decreased platelet count
Increased erythrocyte sedimentation rate (ESR)
Decreased megakaryocytes
Increased WBC
Decreased platelet count
idiopathic thrombocytopenia purpura (ITP)
Condition where the body's immune system mistakenly attacks and destroys platelets, leading to a low platelet count (thrombocytopenia)
Causes purple bruises
A nurse is caring for a client who is at 15 weeks of gestation, is Rh-negative, and has just had an amniocentesis. Which of the following interventions is the nurse's priority following the procedure?
Check the client's temperature.
Observe for uterine contractions.
Administer Rho(D) immune globulin.
Monitor the FHR.
Monitor the FHR.
LEOPOLDS
Palpate the fundus to identify the fetal part.
Determine the location of the fetal back.
Palpate for the fetal part presenting at the inlet.
Identify the attitude of the head.
A nurse is caring for a postpartum client who is receiving heparin via a continuous IV infusion for thrombophlebitis in their left calf. Which of the following actions should the nurse take?
Administer aspirin for pain.
Elevate the affected leg.
Massage the affected leg every 12 hr.
Apply cold compresses to the affected calf.
Elevate the affected leg.
A nurse in a prenatal clinic is assessing a group of clients. Which of the following clients should the nurse see first?
A client who is at 11 weeks of gestation and reports abdominal cramping
A client who is at 15 weeks of gestation and reports tingling and numbness in right hand
A client who is at 20 weeks of gestation and reports constipation for the past 4 days
A client who is at 8 weeks of gestation and reports having three bloody noses in the past week
A client who is at 11 weeks of gestation and reports abdominal cramping.
Abdominal cramping in the first trimester could indicate a threatened miscarriage (spontaneous abortion) or an ectopic pregnancy, both of which are urgent concerns. Ectopic pregnancy can lead to rupture and hemorrhage, while miscarriage may require intervention to prevent complications like excessive bleeding or infection.
Why the other options are not the priority:
A client who is at 15 weeks of gestation and reports tingling and numbness in the right hand:
Not an emergency. Likely carpal tunnel syndrome, which is common in pregnancy due to fluid retention causing median nerve compression.
Management includes wrist splinting, avoiding repetitive movements, and elevation of the hand.
A client who is at 20 weeks of gestation and reports constipation for the past 4 days:
Not urgent. Constipation is common in pregnancy due to progesterone-induced smooth muscle relaxation and uterine pressure on the intestines.
Management: Increase fiber, fluids, and physical activity. Stool softeners (e.g., docusate) may be used if necessary.
A client who is at 8 weeks of gestation and reports having three bloody noses in the past week:
Not urgent. Epistaxis (nosebleeds) are common in pregnancy due to increased blood volume and hormonal effects on nasal mucosa.
Management: Humidifiers, increased hydration, saline nasal spray, and avoiding nasal trauma (e.g., excessive nose blowing).
A nurse is caring for a client who is to receive oxytocin to augment their labor. Which of the following findings contraindicates the initiation of the oxytocin infusion and should be reported to the provider?
Late decelerations
Moderate variability of the FHR
Cessation of uterine dilation
Prolonged active phase of labor
Late decelerations
A nurse is caring for a newborn who was transferred to the nursery 30 min after birth because of mild respiratory distress. Which of the following actions should the nurse take first?
Confirm the newborn's Apgar score.
Verify the newborn's identification.
Administer vitamin K to the newborn.
Determine obstetrical risk factors.
Confirm the newborn's Apgar score.
A nurse is planning care for a client who is in labor and is requesting epidural anesthesia for pain control. Which of the following actions should the nurse include in the plan of care?
Place the client in a supine position for 30 min following the first dose of anesthetic solution.
Administer 1,000 mL of dextrose 5% in water prior to the first dose of anesthetic solution.
Monitor the client's blood pressure every 5 min following the first dose of anesthetic solution.
Ensure the client has been NPO 4 hr prior to the placement of the epidural and the first dose of anesthetic solution.
Monitor the client's blood pressure every 5 minutes following the first dose of anesthetic solution.
Epidural anesthesia can cause maternal hypotension, leading to decreased placental perfusion and fetal oxygenation. Frequent blood pressure monitoring (every 5 minutes) after the first dose helps detect and manage hypotension early by administering IV fluids or positioning the client appropriately.
"Place the client in a supine position for 30 min following the first dose of anesthetic solution."
Incorrect. Supine positioning can cause supine hypotensive syndrome due to the uterus compressing the inferior vena cava, reducing venous return and cardiac output.
Correct Positioning: The client should be in a lateral (side-lying) position or semi-Fowler’s position with a tilted pelvis to avoid vena cava compression.
"Administer 1,000 mL of dextrose 5% in water prior to the first dose of anesthetic solution."
Incorrect. Dextrose 5% in water (D5W) is not the preferred fluid because it can cause maternal hyperglycemia, which can lead to fetal hypoglycemia after birth.
Correct Fluid: A bolus of 500-1,000 mL of lactated Ringer’s (LR) or normal saline (NS) is administered before epidural placement to prevent hypotension.
"Ensure the client has been NPO 4 hr prior to the placement of the epidural and the first dose of anesthetic solution."
Incorrect. Laboring clients do not need to be NPO before epidural placement.
Light oral intake (clear liquids, ice chips) is usually permitted to maintain hydration and prevent ketosis. Strict NPO is more relevant for general anesthesia (e.g., emergency C-section) to prevent aspiration.
A nurse in the antepartum clinic is assessing a client's adaptation to pregnancy. The client states that they are "happy one minute and crying the next." The nurse should interpret the client's statement as an indication of which of the following?
Emotional lability
Focusing phase
Cognitive restructuring
Couvade syndrome
Emotional lability
Couvade syndrome
Condition where the partner of a pregnant woman experiences physical and psychological symptoms similar to pregnancy, even though they are not pregnant themselves
A nurse is transporting a newborn back to the parent's room following a procedure. Which of the following actions should the nurse take prior to leaving the newborn with their parent?
Ensure that the parent's identification band number matches the newborn's identification band number.
Ask the parent to verify their name and date of birth.
Check the newborn's security tag number to ensure it matches the newborn's medical record.
Match the newborn's date and time of birth to the information in the parent's medical record.
Ensure that the parent's identification band number matches the newborn's identification band number.
A nurse is caring for a client who has preeclampsia and is receiving a continuous infusion of magnesium sulfate IV. Which of the following actions should the nurse take?
Restrict hourly fluid intake to 150 mL/hr.
Have calcium gluconate readily available.
Assess deep tendon reflexes every 6 hr.
Monitor intake and output every 4 hr.
Have calcium gluconate readily available.
Magnesium sulfate is given to clients with preeclampsia to prevent and manage seizures (eclampsia) by acting as a CNS depressant. However, magnesium toxicity is a serious risk and can cause respiratory depression, loss of deep tendon reflexes (DTRs), cardiac arrest, and decreased urine output.
Calcium gluconate is the antidote for magnesium sulfate toxicity and should be readily available at the bedside to reverse its effects immediately in case of overdose.
"Restrict hourly fluid intake to 150 mL/hr."
Incorrect. Fluid intake should be limited to 100-125 mL/hr to prevent fluid overload and pulmonary edema, which is a complication of magnesium sulfate therapy.
Excessive IV fluids can increase the risk of pulmonary edema, especially in preeclamptic clients who may already have endothelial dysfunction and leaky capillaries.
"Assess deep tendon reflexes every 6 hr."
Incorrect. Deep tendon reflexes (DTRs) must be checked every 1-2 hours, not every 6 hours.
Diminished or absent DTRs are an early sign of magnesium toxicity and must be monitored closely to prevent progression to respiratory depression and cardiac arrest.
"Monitor intake and output every 4 hr."
Incorrect. Urinary output should be assessed hourly, as oliguria (less than 30 mL/hr) is an early sign of magnesium toxicity.
Magnesium is excreted by the kidneys, and decreased urine output increases the risk of toxic accumulation.
magnesium sulfate IV.
also used for pediatric acute nephritis and to prevent seizures in severe pre-eclampsia, eclampsia, or toxemia of pregnancy.
A nurse is assessing a newborn 12 hr after birth. Which of the following manifestations should the nurse report to the provider?
Acrocyanosis
Transient strabismus
Jaundice
Caput succedaneum
Jaundice
Jaundice within the first 24 hours of life is abnormal and may indicate pathologic jaundice, often caused by conditions such as hemolytic disease of the newborn (Rh or ABO incompatibility), sepsis, or liver dysfunction. This requires immediate evaluation and potential treatment (e.g., phototherapy) to prevent bilirubin encephalopathy (kernicterus), which can cause permanent neurological damage.
A nurse is providing teaching for a client who has a new prescription for combined oral contraceptives. Which of the following findings should the nurse include as an adverse effect of this medication?
Depression
Polyuria
Hypotension
Urticaria
Depression
Depression is a known adverse effect of combined oral contraceptives (COCs) due to the hormonal influence on neurotransmitters such as serotonin and dopamine. Some individuals may experience mood changes, irritability, or depressive symptoms while taking COCs. If the symptoms become severe, an alternative form of contraception should be considered.
Polyuria (excessive urination)
Not a common side effect.
COCs do not directly cause polyuria. Instead, they can sometimes lead to fluid retention or bloating rather than excessive urination.
Hypotension (low blood pressure)
Not a common side effect.
COCs are more likely to cause mild hypertension (high blood pressure) rather than hypotension.
Women with uncontrolled hypertension may need to avoid COCs due to an increased risk of cardiovascular complications.
Urticaria (hives, itchy rash)
Rare side effect.
While allergic reactions to COCs can occur, urticaria is not a typical adverse effect. If a client develops hives or an allergic reaction, they should discontinue use and consult their provider.
A nurse is caring for a client who is at 41 weeks of gestation and has a positive contraction stress test. For which of the following diagnostic tests should the nurse prepare the client?
Percutaneous umbilical blood sampling
Amnioinfusion
Biophysical profile (BPP)
Chorionic villus sampling (CVS)
Biophysical profile (BPP)
A positive contraction stress test (CST) indicates that the fetus experienced late decelerations with uterine contractions, which suggests uteroplacental insufficiency and potential fetal distress. The biophysical profile (BPP) is the next step to further evaluate fetal well-being by assessing:
Fetal breathing movements
Gross body movements
Fetal tone
Amniotic fluid volume
Nonstress test (NST) results
A BPP score of 8 to 10 is reassuring, whereas a score below 6 may indicate fetal compromise and the need for delivery.
Percutaneous Umbilical Blood Sampling (PUBS)
This test directly samples fetal blood from the umbilical vein to check for fetal anemia, infections, or genetic conditions.
Not indicated for a positive CST, as fetal distress is typically evaluated with BPP or further monitoring.
Amnioinfusion
This procedure infuses fluid into the amniotic sac via an intrauterine catheter to relieve cord compression or dilute meconium-stained fluid.
Not a diagnostic test and not used to assess fetal distress after a positive CST.
Chorionic Villus Sampling (CVS)
This test is used early in pregnancy (10-13 weeks) to diagnose genetic or chromosomal abnormalities.
Not relevant at 41 weeks or for a positive CST.
A nurse is teaching a client who is at 37 weeks of gestation and has a prescription for a nonstress test. Which of the following instructions should the nurse include?
"The test should take 10 to 15 minutes to complete."
"You will lay in a supine position throughout the test."
"You should not eat or drink for 2 hours before the test."
"You should press the handheld button when you feel your baby move."
"You should press the handheld button when you feel your baby move."
A school nurse is providing teaching to an adolescent about levonorgestrel contraception. Which of the following information should the nurse include in the teaching?
"You should take the medication within 72 hours following unprotected sexual intercourse."
"You should avoid taking this medication if you are on an oral contraceptive."
"If you don't start your period within 5 days of taking this medication, you will need a pregnancy test."
"One dose of this medication will prevent you from becoming pregnant for 14 days after taking it."
"You should take the medication within 72 hours following unprotected sexual intercourse."
Levonorgestrel (Plan B, Emergency Contraception Pill) is most effective when taken within 72 hours (3 days) after unprotected intercourse. The sooner it is taken, the higher the effectiveness in preventing pregnancy. It primarily works by:
Preventing or delaying ovulation
Altering the uterine lining to prevent implantation
While it can still be taken up to 5 days (120 hours) after intercourse, its effectiveness decreases significantly after 72 hours.
"You should avoid taking this medication if you are on an oral contraceptive." ❌
Incorrect because levonorgestrel can be taken by individuals who are on oral contraceptives.
It is meant for emergency use only and should not replace regular birth control.
"If you don't start your period within 5 days of taking this medication, you will need a pregnancy test." ❌
Incorrect because Plan B can alter the menstrual cycle by causing early, late, or heavier/lighter periods.
A pregnancy test is recommended if the period is delayed by more than a week, not just 5 days.
"One dose of this medication will prevent you from becoming pregnant for 14 days after taking it." ❌
Incorrect because levonorgestrel only works for the specific act of unprotected intercourse before taking it.
It does not provide ongoing protection, so additional contraception should be used for subsequent sexual activity.
A nurse is planning care for a client who is in labor and is to have an amniotomy. Which of the following assessments should the nurse identify as the priority?
O2 saturation
Temperature
Blood pressure
Urinary output
Temperature
An amniotomy is an artificial rupture of membranes (AROM) performed to induce or augment labor. The priority assessment after an amniotomy is monitoring the client's temperature because ruptured membranes increase the risk for infection, particularly chorioamnionitis (infection of the amniotic sac).
After an amniotomy, the nurse should assess maternal temperature every 2 hours to detect early signs of infection.
A temperature ≥100.4°F (38°C) suggests infection and should be reported immediately.
Prolonged rupture of membranes (>18 hours) further increases the risk of infection.
Oxygen Saturation (O₂ Sat) ❌
Not the priority because amniotomy does not directly affect maternal oxygenation.
O₂ saturation would be important if fetal distress or maternal respiratory issues were present, but this is not the primary concern here.
Blood Pressure (BP) ❌
Not the priority unless there are complications like preeclampsia or excessive bleeding.
Amniotomy does not typically affect BP, unlike epidural anesthesia, which may cause hypotension.
Urinary Output ❌
While monitoring urinary output is important for overall maternal hydration and kidney function, it is not the priority immediately after an amniotomy.
Urinary retention is more of a concern after epidural administration, not after amniotomy.
A nurse on an antepartum unit is caring for four clients. Which of the following clients should the nurse identify as the priority?
A client who has gestational diabetes and a fasting blood glucose level of 120 mg/dL (less than 95 mg/dL)
A client who is at 34 weeks of gestation and reports epigastric pain
A client who is at 28 weeks of gestation and has an Hgb of 10.4 g/dL (11 to 16 g/dL)
A client who is at 39 weeks of gestation and reports urinary frequency and dysuria
A client who is at 34 weeks of gestation and reports epigastric pain.
Epigastric pain in the third trimester is a potential sign of severe preeclampsia, HELLP syndrome (Hemolysis, Elevated Liver enzymes, Low Platelets), or liver involvement, which can quickly progress to life-threatening complications.
Epigastric pain (right upper quadrant pain) is due to liver swelling and irritation from severe hypertension and preeclampsia.
Other concerning signs include headaches, visual disturbances, proteinuria, and high blood pressure.
HELLP syndrome can lead to liver rupture, stroke, placental abruption, and maternal/fetal death if not treated immediately.
A client who has gestational diabetes and a fasting blood glucose level of 120 mg/dL (normal: <95 mg/dL) ❌
Elevated glucose is a concern but not immediately life-threatening.
The nurse should notify the provider for insulin adjustments, but this is not an urgent situation compared to possible severe preeclampsia.
A client who is at 28 weeks of gestation and has an Hgb of 10.4 g/dL (normal: 11-16 g/dL) ❌
Mild anemia is common in pregnancy due to hemodilution.
This client may need iron supplementation, but it is not an emergency.
A client who is at 39 weeks of gestation and reports urinary frequency and dysuria ❌
This suggests a urinary tract infection (UTI), which can lead to complications like pyelonephritis and preterm labor if untreated.
However, this is not immediately life-threatening compared to severe preeclampsia/HELLP syndrome in the 34-week client.
A nurse is assessing a newborn following a circumcision. Which of the following findings should the nurse identify as an indication that the newborn is experiencing pain?
Decreased heart rate
Chin quivering
Pinpoint pupils
Slowed respirations
Chin quivering
A nurse is performing a routine assessment on a client who is at 18 weeks of gestation. Which of the following findings should the nurse expect?
Deep tendon reflexes 4+
Fundal height 14 cm
Blood pressure 142/94 mm Hg
FHR 152/min
FHR 152/min
Deep tendon reflexes (DTRs) 4+ ❌
Abnormal. Hyperreflexia (4+ DTRs) is a sign of central nervous system (CNS) irritability, which can occur with preeclampsia.
Normal DTRs in pregnancy should be 2+ (brisk but normal).
If 4+ DTRs were present, the nurse should assess for other preeclampsia signs (hypertension, proteinuria, headaches, visual disturbances).
Fundal height 14 cm ❌
Too low for 18 weeks.
Fundal height (in cm) should approximately match the gestational age in weeks ±2 cm.
At 18 weeks, the fundal height should be ~16-22 cm, around the midway point between the symphysis pubis and umbilicus.
A 14 cm fundal height suggests growth restriction or incorrect dating.
Blood pressure 142/94 mm Hg ❌
High blood pressure in pregnancy (≥140/90 mmHg) before 20 weeks may indicate chronic hypertension.
Gestational hypertension and preeclampsia typically develop after 20 weeks.
The nurse should monitor BP closely and assess for signs of preeclampsia (headaches, proteinuria, vision changes, epigastric pain, hyperreflexia).
A nurse is caring for a client who becomes unresponsive upon delivery of the placenta. Which of the following actions should the nurse take first?
Determine respiratory function.
Increase the IV fluid rate.
Access emergency medications from cart.
Collect a maternal blood sample for coagulopathy studies.
Determine respiratory function.
When a client becomes unresponsive after placental delivery, the nurse should first assess airway, breathing, and circulation (ABCs). Checking for respiratory function (breathing effort, airway patency, and oxygenation) is the priority action to ensure the client is receiving adequate oxygen.
Unresponsiveness postpartum can indicate massive postpartum hemorrhage, amniotic fluid embolism, or cardiopulmonary collapse, all of which require immediate assessment of breathing and circulation.
If respiratory arrest is confirmed, immediate resuscitation (CPR, oxygen support, and emergency intervention) is required.
A nurse is caring for a client who has hyperemesis gravidarum and is receiving IV fluid replacement. Which of the following findings should the nurse report to the provider?
Blood pressure 105/64 mm Hg
Heart rate 98/min
Urine output of 280 mL within 8 hr
Urine negative for ketones
Blood pressure 105/64 mm Hg
A nurse is assessing four newborns. Which of the following findings should the nurse report to the provider?
A newborn who is 26 hr old and has erythema toxicum on their face
A newborn who is 32 hr old and has not passed a meconium stool
A newborn who is 12 hr old and has pink-tinged urine
A newborn who is 18 hr old and has an axillary temperature of 37.7° C (99.9° F)
A newborn who is 32 hr old and has not passed a meconium stool
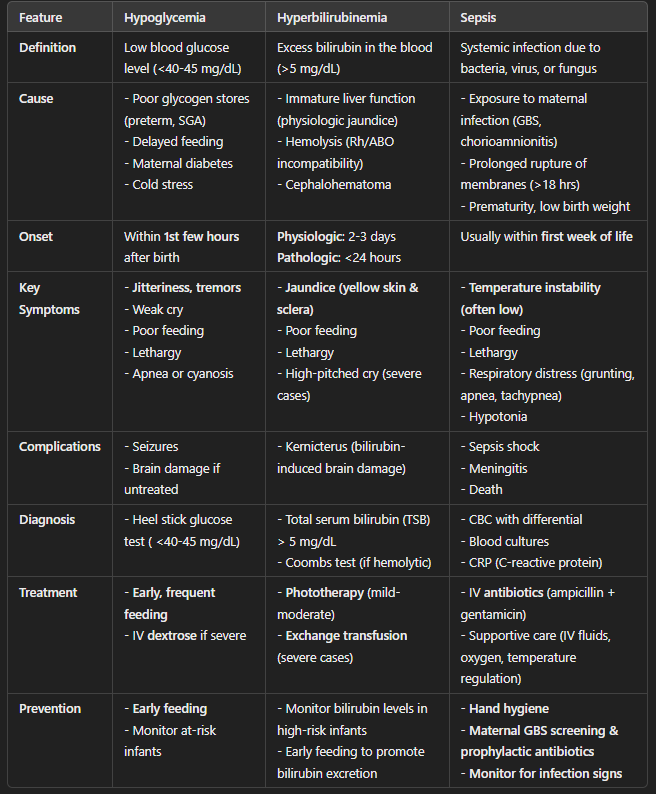
Comparison of Hypoglycemia, Hyperbilirubinemia, and Sepsis in Newborns (Table)
Key Differences:
Hypoglycemia: Occurs immediately after birth, presents with jitteriness, poor feeding, and lethargy, and is treated with early feeding or IV glucose.
Hyperbilirubinemia: Develops over 2-3 days, presents with yellow skin/sclera, and is treated with phototherapy or exchange transfusion.
Sepsis: Can occur at birth or within the first week, presents with temperature instability, poor feeding, and respiratory distress, and requires IV antibiotics.
💡 Remember:
Hypoglycemia → Jittery + Weak Cry → Feed or Give Glucose
Hyperbilirubinemia → Yellow Skin → Phototherapy
Sepsis → Temperature Instability + Lethargy → IV Antibiotics
A nurse is teaching a client who has pregestational type 1 diabetes mellitus about management during pregnancy. Which of the following statements by the client indicates an understanding of the teaching?
"I will need to increase my insulin doses during the first trimester."
"I should engage in moderate exercise for 30 minutes if my blood glucose is 250 or greater."
"I will continue taking my insulin if I experience nausea and vomiting."
"I will ensure that my bedtime snack is high in refined sugar."
"I will continue taking my insulin if I experience nausea and vomiting."
Clients with pregestational type 1 diabetes mellitus must continue taking insulin even if they are nauseous or vomiting to prevent diabetic ketoacidosis (DKA), which can be life-threatening during pregnancy. Glucose monitoring and ketone testing should be done frequently, and small, frequent carbohydrate-rich meals or liquids should be consumed to maintain blood glucose levels. If vomiting persists, the provider should be notified.
A nurse is caring for a client following an amniocentesis at 18 weeks of gestation. Which of the following findings should the nurse report to the provider as a potential complication?
Increased fetal movement
Leakage of fluid from the vagina
Upper abdominal discomfort
Urinary frequency
Upper abdominal discomfort