Nerve Control of Circulation
1/10
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
11 Terms
What is blood pressure and how are changes regulated?
Blood pressure is the driving force of blood flow. Changes in blood pressure are detected by baroreceptors and regulated by altering cardiac output and/or the total peripheral resistance:
Mean arterial pressure (MAP) = cardiac output (CO) x total peripheral resistance (TPR)
Vasodilation → decreased blood pressure
Vasoconstriction → increased blood pressure
How is cardiac output influenced?
CO is changes by either heart rate or stroke volume:
Cardiac output (CO) = heart rate (HR) x stroke volume (SV)
Therefore, changes in HR & SV help maintain the MAP.
How is heart rate influenced?
HR is driven by pacemaker cells, which are heavily influenced by the autonomic nervous system:
Sympathetic activation → increased HR
Parasympathetic activation → decreased HR
Why is it important to have a stable blood pressure?
Too low BP can cause fainting due to inadequate O2 delivery to tissues. Too high BP can lead to stroke/heart attack.
Normal BP: 120/80 mmHg (systolic/diastolic)
What is a normal cardiac output?
5 L/min for each ventricle
Total is 10 L/min for systemic and pulmonary circulation combined
Both ventricles pump the same volume to avoid blood accumulation. However, pulmonary circulation operates under lower pressure due to lower resistance.
How is high blood pressure regulated through the baroreflex (short-term)?
Baroreceptors are located in the aortic arch and carotid sinus, and act instantaneously on change in blood pressure.
Stimulus: increase in MAP or physical pressure
Baroreceptors detect the change and increase their firing rate of action potentials, which get integrated in the medulla (brainstem)
Effector response:
Increased parasympathetic activity via vagus nerve to signal the SA node to decrease HR
Decreased sympathetic activity signals heart to decrease SV & HR; peripheral vessels vasodilate, decreasing TPR
Results in BP decreasing back towards set point
How does the orthostatic reflex work?
The orthostatic reflex involves the body adjusting to blood pressure quickly in response to postural changes, e.g. when standing up.
Blood pools in the lower extremities due to gravity
Venous return to heart decreases due to decreased SV, also causing drops in CO and HR
Cerebral perfusion is reduced, causing dizziness
Baroreceptors detect the drop and start their firing
Brain reponds by increasing sympathetic output and decreasing parasympathetic output
Results in vasoconstriction (due to increased TPR) and increased HR, quickly restoring blood pressure
In elders, this baroreflex sensitivity decreases, leading to slower BP recovery, which increases risk of fainting
What is the autotransfusion mechnaism?
It is a response that compensates for haemorrhage (blood loss) by shifting interstitial fluid into the capillaries to restore blood volume and blood pressure until RBCs and plasma proteins can replace. Drinking water enhances this process as it increases total body fluid, aiding in further reabsorption.
Describe the control of the cardiovascular system during exercise.
The input comes from:
Mechanoreceptors in the muscles that detect movement
Chemoreceptors that detect metabolic changes (i.e., increased CO2 production)
Reset arterial baroreceptors that are adapted to new, higher pressure range
In response, adjustments are coordinated by “exercise centres” in the brain and the medullary cardiovascular centre to increases sympathetic activity and decrease parasympathetic output, leading to:
Increased HR via sympathetic activation
Increased SV via enhanced contractility
Vasoconstriction in non-essential organs (kidney, gut)
Vasodilation in skeletal muscles and skin (thermoregulation)
Since blood pressure increases during exercise, why do the baroreceptors not oppose?
Baroreceptors are reset during exercise. This tells the system that the higher pressure is appropriate, accepting the new “normal” so that the baroreceptors don’t trigger compensatory decrease in HR or vasodilation
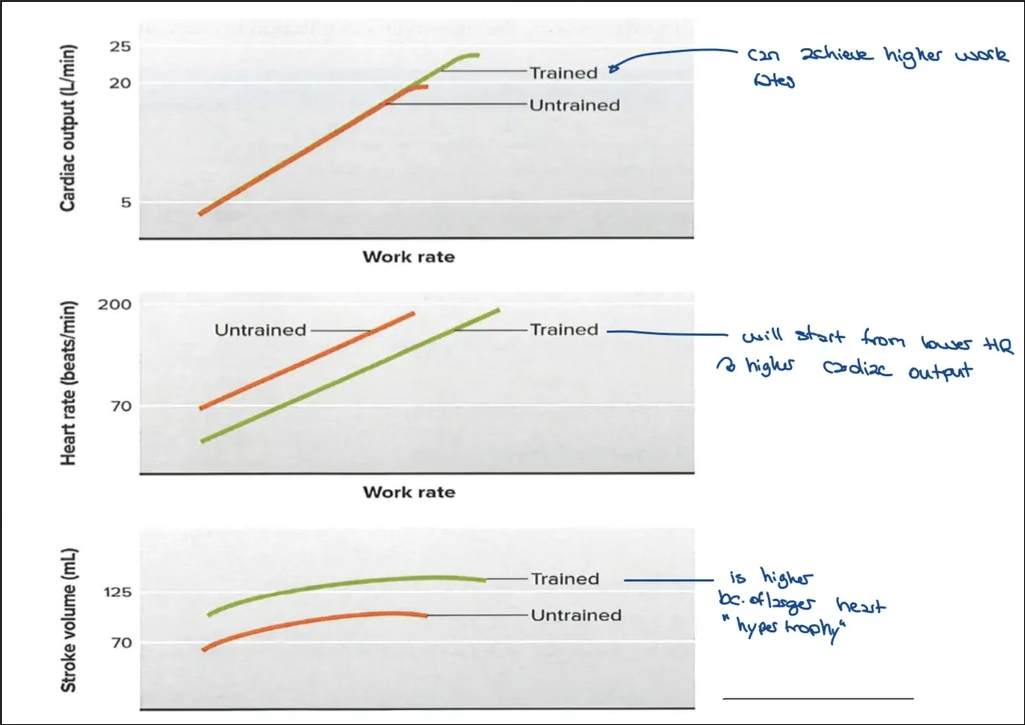
What happens to the relationship of CO, HR, and SV with training?
Cardiac output increases with work rate
Heart rate starts from a lower point
Stroke volume is higher due to hypertrophy