Communication, Homeostasis and Energy
1/147
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
148 Terms
What abiotic and biotic stresses does a plant have to deal with?
Abiotic:
Changes in day length
Changes in temperature + freezing
Drought + excess of water
Changes in soil water salinity
Winds
Biotic:
Herbivory (being eaten)
Being touched
Competition with other plants
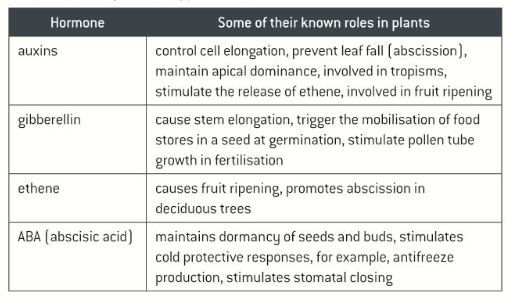
What processes/changes are different plant hormones involved in?
How and why do deciduous plants respond to drops in temperature and shorter day lengths in the winter?
Deciduous plants drop their leaves (abscission, controlled by ethene) in the winter and remain dormant until spring
This is because:
Day lengths decrease
This means plants are able to photosynthesize for a smaller proportion of the day
This reaches a point where the glucose produced by photosynthesis is less than the glucose needed for respiration and for producing antifreeze chemicals
Trees with leaves are also more likely to be damaged due to winds in winter
Dropping temperatures can also freeze the soils so that it is difficult to absorb water for transpiration, and can deactivate enzymes in the cells so leaves become less functional
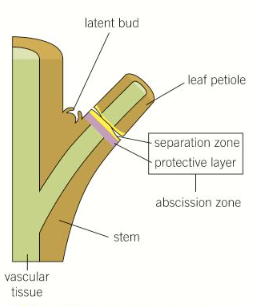
How does leaf abscission happen?
Auxin levels drop and ethene is produced as the day length shortens and temperatures drop
This activates a layer of cells at the base of the leaf stalks, causing them to produce enzymes that break down the cell walls in the abscission zone
The vascular bundles are sealed off and the fatty material suberin is deposited to form a waterproof protective scar layer preventing pathogen entry when the leaf falls
How can plants respond to day length?
Photoperiodism is involved in many seasonal changes in plants, such as opening dormant leaf buds, flowering, and the formation of tubers
The light-sensitive phytochrome pigment switches between two forms, Pr (red light) and Pfr (far-red light), depending on the light available at different times of day, and the ratio of these two forms measures the night length
How can plants respond to water stress?
When water is unavailable, the hormone abscisic acid (ABA) is produced, which causes the stomata to close
ABA binds to cell surface receptors on guard cells, causing them to lose ions, increasing the water potential so that water leaves the cells by osmosis
This reduces the turgor of the guard cells, closing the stomata
What are the chemical defences to herbivory in plants?
They can produce:
Nitrogenous chemicals called alkaloids (eg. caffeine + nicotine), which are bitter-tasting or act as metabolic poisons to deter or kill herbivores
Polyphenol chemicals called tannins, which are bitter-tasting and toxic to herbivores, by binding to and deactivating the digestive enzymes in saliva
Plants can release pheromones- these can warn nearby plants of the same species that they are under attack and trigger their defences, and can attract the herbivore’s natural predators
How do some unique plants respond to touch?
Mimosa pudica leaves rapidly fold when touched
Physical stimulus causes ion movement that changes the water potential and triggers the movement of water by osmosis to affect turgidity, closing the leaves
This acts to dislodge small herbivorous insects and scare off others
What tropisms can plants show?
Phototropism- light- shoots grow towards light (positive) and roots grow away (negative), maximising photosynthesis and root growth
Gravi/geotropism- gravity- shoots grow up against gravity (negative) and roots grow down with it (positive), ensuring shoots and roots grow in the correct direction regardless of seed orientation
Hydrotropism- water- roots grow towards damper soil (positive) maximising water access
Thigmotropism- touch- allows climbing plants to detect a support and curl around it (positive) , which can help them grow upwards more energy efficiently
Chemotropism- chemicals- some plants respond directionally to chemicals eg. pollen tubes growing towards the ovules (positive) in response to chemicals it releases
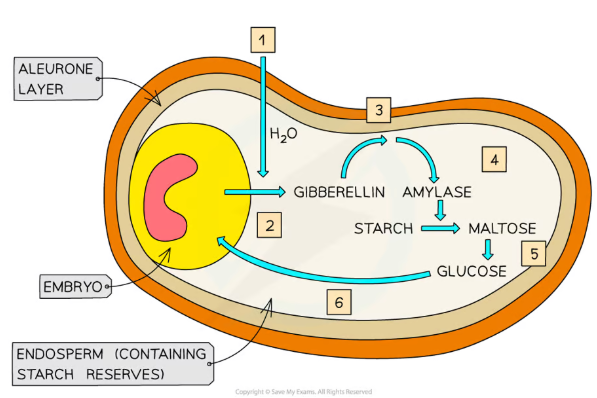
How are hormones involved in seed germination?
Gibberellins trigger seed germination, while abscisic acid (ABA) inhibits it (they are antagonistic hormones)
In the correct germination conditions, the seed starts to absorb water and the embryo produces gibberellins
The gibberellins switch on the genes coding for amylase and proteases, so that they are produced
These enzymes break down the food stores (found in the cotyledons of dicot seeds and the endosperm of monocot seeds), producing glucose that is used for respiration
The ATP produced is used for embryo growth, to break through the seed coat
ABA, on the other hand, inhibits amylase production
How are gibberellins involved in stem elongation?
They increase the length of the internodes (regions of a stem between two leaves)
What is the experimental evidence for the involvement of gibberellins in seed germination and stem elongation?
Seeds which have been bred not to produce gibberellins, and seeds exposed to gibberellin biosynthesis inhibitors never germinate, unless gibberellins are applied and the inhibition removed
Dwarf plant varieties have been bred which produce very low levels of gibberellins, which grow to the same height as normal varieties when treated with gibberellins
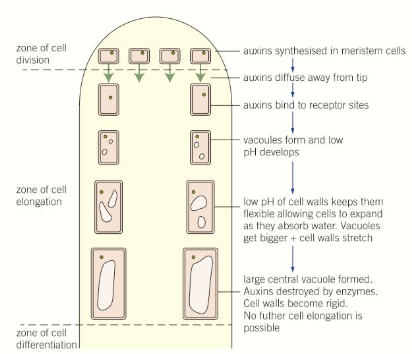
How are auxins involved in cell elongation and phototropism?
Auxins are produced in the tips of apical (main) shoots and bind to receptors in the cell membranes of meristematic cells, which drops the pH to around 5
This is the optimum pH for enzymes which maintain the flexibility and plasticity of cell walls, so the cells can elongate more easily
As the cells mature, enzymes destroy auxin, and the pH rises again, so that the cell walls become more rigid and fixed
In phototropism, the auxins move to the shaded side of shoots, causing this process of cell elongation so the shoot bends towards the light
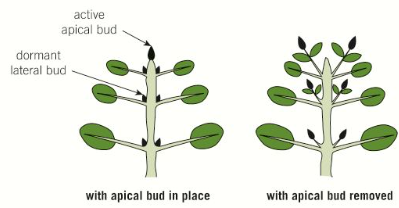
How are auxins involved in apical dominance?
High concentrations of auxins stimulate the growth of apical shoots and inhibit the growth of lateral shoots, resulting in apical dominance
This prioritises upward growth of the shoot to reach more light for photosynthesis
Further down the stem, the auxin concentrations are lower, meaning lateral growth is less inhibited (results in the conical shape of conifer trees)
If the apical shoot tip is cut off, preventing the production of auxins, the lateral shoots grow faster, and if auxins are artificially applied their growth is suppressed again
How can plant hormones be used commercially?
Selective weed killers- auxins
Applying synthetic auxins to weeds in high enough concentrations can cause such rapid growth that the plant can’t sustain, causing it to die
We can do this because most weeds are broad-leaved dicots and most crops are narrow-leaved monocots so the weeds are more susceptible and die off
Rooting powders- auxins
Dipping plant cuttings in rooting powders containing auxins can stimulate them to grow new roots
Controlling ripening- ethene
Ethene can be used to stimulate fruits to ripen at the correct time
This is particularly for bananas and avocados (climacteric fruits), so that they can be harvested unripe, then ripened artificially after transport, so they aren’t damaged or wasted, and are ripe for sale
How is the nervous system organised structurally and functionally?
Structurally, the nervous system can be divided into the:
Central nervous system (CNS) – the brain and the spinal cord
Peripheral nervous system (PNS) – all of the nerves in the body
Functionally, the nervous system can be divided into the:
Somatic nervous system- voluntary actions
Autonomic nervous system- involuntary actions (eg. heart rate)
The autonomic system can be further divided into the:
Sympathetic nervous system- ‘fight or flight’ responses
Parasympathetic nervous system- ‘rest + digest’ functions
What neurotransmitters do the parasympathetic and sympathetic nervous systems use?
Parasympathetic - acetylcholine (ACh)
Sympathetic- noradrenaline (NA) and norepinephrine (NE)
What is the structure of the brain?
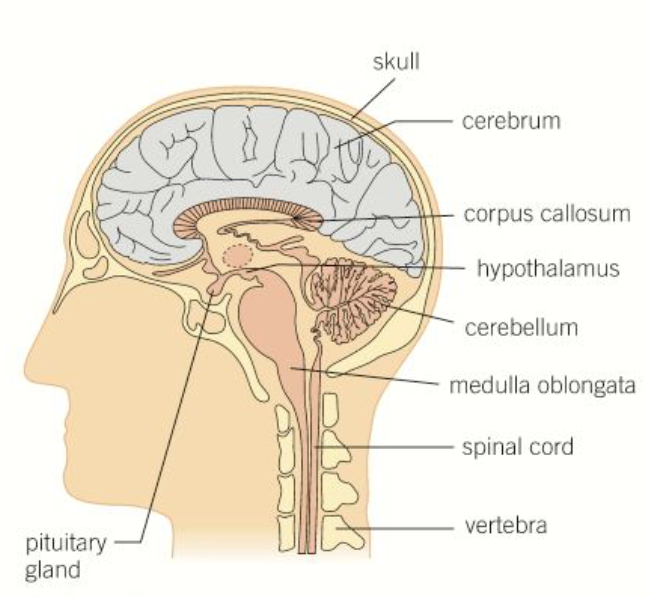
Describe the structure and function of the cerebrum/cerebral cortex
Carries out a large variety of functions involved with conscious activities, including:
Vision
Hearing
Speech
Thinking
Memory
Divided into two halves, the cerebral hemispheres, joined together by a band of nerve fibres known as the corpus callosum
Describe the function of the hypothalamus
Found just above the pituitary gland
Involved in homeostasis by monitoring the blood that flows through it and responding
It also produces hormones and triggers the pituitary gland to release hormones
Regulates:
Body temperature
Water retention by the kidneys (osmoregulation)
Digestion and hunger
Describe the structure and function of the pituitary gland
Found just below the hypothalamus
Secretes hormones that control many body processes
Divided into two sections:
Anterior pituitary - produces and releases hormones (mainly sex hormones such as FSH)
Posterior pituitary - stores and releases hormones produced by the hypothalamus
Describe the function of the cerebellum
Controls motor coordination, movement and balance
Describe the function of the medulla oblongata
Connected to the brain stem
Controls involuntary + unconscious processes, including:
Heart rate
Blood pressure
Breathing rate
Coughing
Vomiting
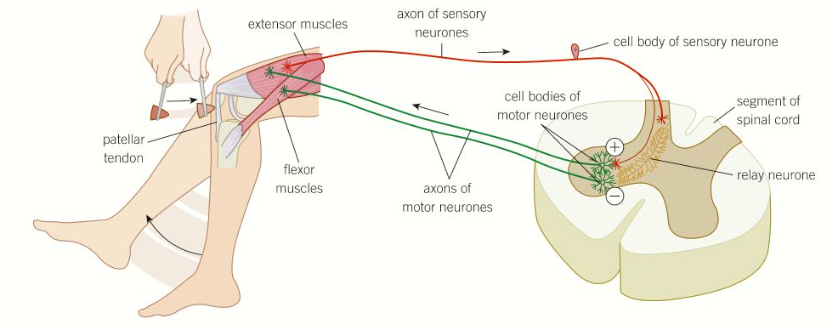
What is the knee-jerk reflex and how does it work?
The knee-jerk reflex is a spinal reflex often used by doctors to check that the nervous system is functioning properly
When the leg is tapped just below the kneecap, an impulse is generated that travels to the spinal cord, simultaneously triggering the extensor muscle to contract and the flexor muscle to relax- this makes the leg kick quickly and involuntarily
This reflex is used by our bodies to maintain posture and balance
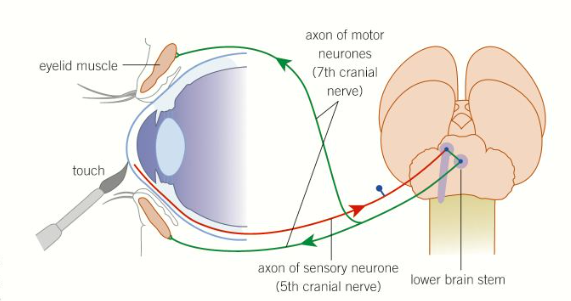
What is the blinking reflex and how does it work?
The blinking reflex is a cranial reflex often used by doctors to check that unconscious patients aren’t brain dead
When the cornea of the eye is irritated, an impulse is generated that travels to the lower brain stem, triggering both eyes to close quickly and involuntarily
This reflex is used by our bodies to prevent damage to the eyes eg. from dust
What is the overall structure and function of skeletal muscle?
Skeletal muscles are involved in voluntary, conscious movement of bones
They are striated (have stripes), tubular and multinucleated
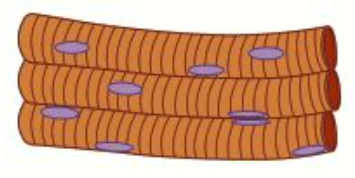
What is the structure and function of cardiac muscle?
Cardiac muscles are involved in involuntary, myogenic (without stimulus) contraction of the heart to pump blood
They are faintly striated (have stripes), branched and uninucleated
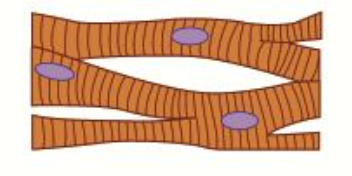
What is the structure and function of smooth muscle?
Smooth muscles are involved in involuntary control of many different parts of the body, including vasoconstriction in the walls of blood vessels, and peristalsis (movement of food) in the digestive tract
They are non-striated (don’t have stripes), spindle-shaped and uninucleated
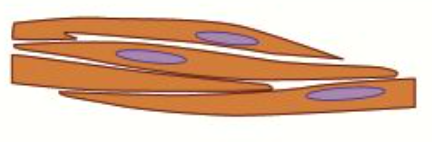
What is the detailed structure of skeletal muscle?
Skeletal muscles are made up of many muscle fibres
Muscle fibres are like long cells that contain:
Mitochondria
Multiple nuclei
Contractile myofibrils
Sarcoplasmic reticulum (like an ER, which contains calcium ions for muscle contraction)
Sarcoplasm (cytoplasm)
All are enclosed by the sarcolemma (cell membrane)
T-tubules (thin projections of the sarcolemma that point inwards, and spread electrical impulses across the whole sarcoplasm so all the myofibrils can contract at once)
The myofibrils contain thick filaments made of myosin and thin filaments made of actin- these slide past each other to make the muscle fibres contract
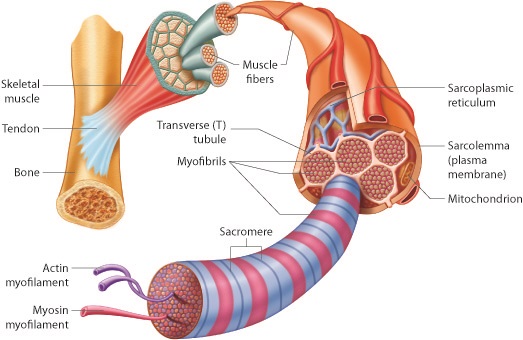
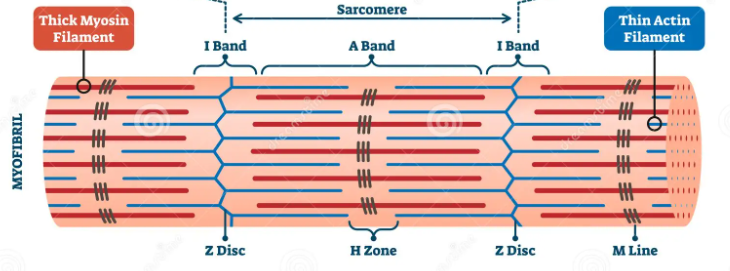
What is the structure of a myofibril?
The myofibrils contain thick filaments made of myosin and thin filaments made of actin arranged in an interlocking pattern- these slide past each other to make the muscle fibres contract
The M line is where thick myosin filaments attach
The Z line is where the thin actin filaments attach
A sarcomere is the section between two Z lines
The A (dark) band is the length of the thick myosin filaments
The H band is where only thick myosin filaments are present
The I (light) band is where only thin actin filaments are present
What is a neuromuscular junction?
The space between a motor neurone and a muscle, which functions in the same way as a cholinergic synapse, except the receptor proteins for acetylcholine are found on the sarcolemma (the muscle fibre membrane)
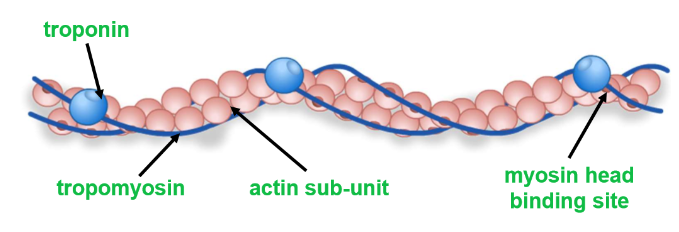
What proteins are involved in the sliding filament model?
In a myofibril, the thick filaments are made of fibrous myosin proteins with hinged globular heads
The thin filaments are made of two globular actin protein chains, which twist together
Two fibrous tropomyosin proteins twist around the actin chains, blocking their myosin head binding sites
Troponin proteins hold tropomyosin in place, and have calcium ion binding sites that allow it to change shape
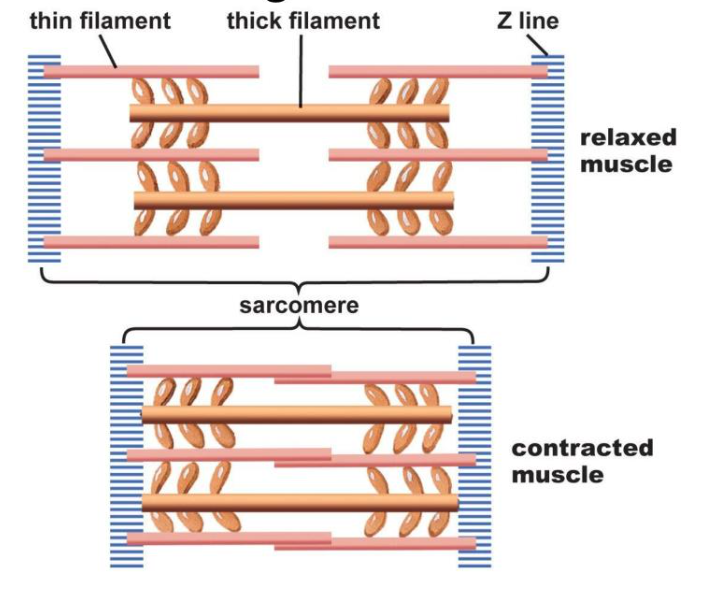
What is the sliding filament model and how does it work?
The sliding filament model describes how sarcomeres shorten to contract muscles:
An action potential arrives at the neuromuscular junction and causes calcium ions to be released from the sarcoplasmic reticulum
These diffuse through the sarcoplasm and bind to troponin molecules, causing troponin and tropomyosin to change shape
This exposes the myosin binding sites on the actin molecules, and the globular heads of myosin proteins bind, forming cross bridges between the thick and thin filaments
The heads bend (the power stroke), pulling the actin filaments in towards the M line, which shortens the sarcomere
ATP binds, making the myosin heads detach and act as an ATPase enzyme to hydrolyse ATP into ADP and Pi, releasing energy to return to their original position
The myosin heads then bind to a new site further along the thin filament, and this process repeats multiple times, shortening the sarcomere further to contract the muscle
How is energy supplied to muscles?
Mitochondria can respire aerobically to produce ATP but this is slow and requires a good supply of oxygen, so it is used more for long periods of low intensity exercise
Aerobic respiration produces much less ATP, and causes the build up of lactic acid, but can be used for short bursts of high intensity exercise, when the blood can’t supply enough oxygen for aerobic respiration
Creatine phosphate is stored in muscles, which can act as a small reserve supply of phosphate to combine with ADP and produce ATP quickly, so it can be used for short bursts of vigorous exercise before it is used up
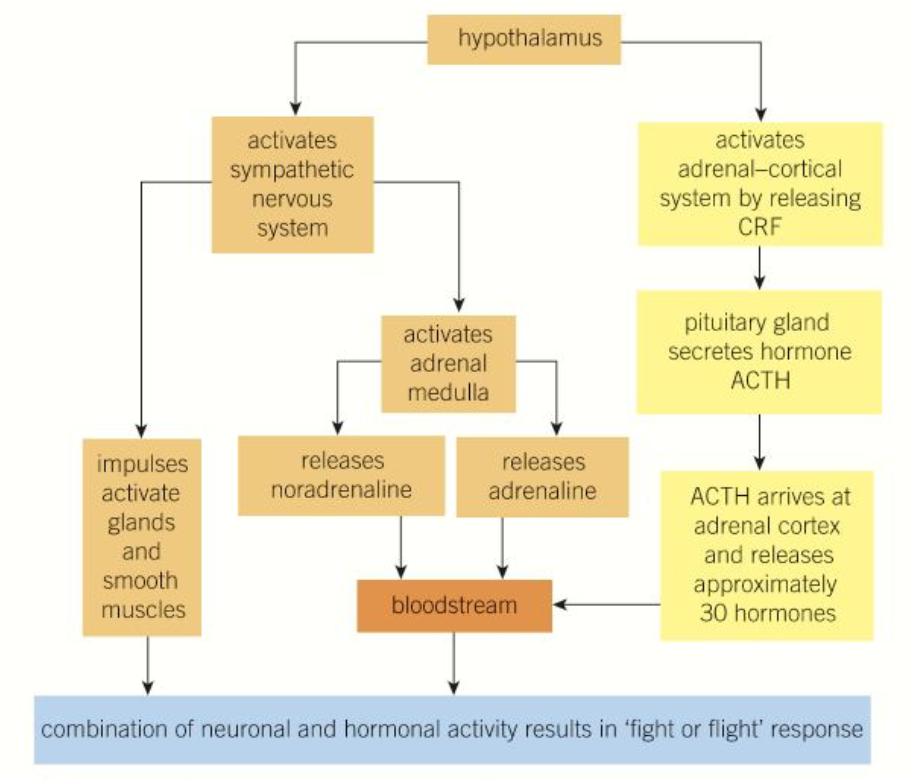
How is the fight or flight response brought about?
A stimulus is detected, causing the hypothalamus to activate the sympathetic nervous system and the adrenal-cortical system (by releasing CRF, cortisol releasing hormone):
The sympathetic nervous system sends impulses to activate glands and smooth muscles, and activated the adrenal medulla to release adrenaline and noradrenaline into the blood stream
The adrenal-cortical system stimulates the pituitary to release ACTH, which reaches the adrenal cortex and causes 30 different hormones to be released
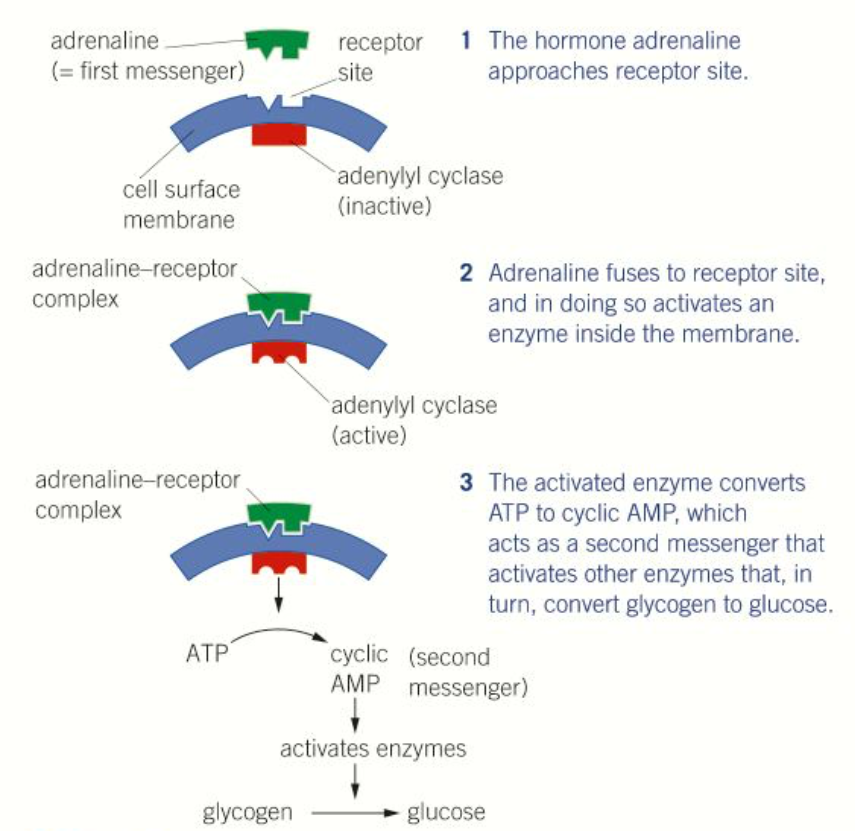
How does adrenaline trigger glycogenolysis?
Adrenaline, the first messenger, binds to the membrane of liver cells, which causes the adenylyl cyclase enzyme to activate
This converts ATP into cyclic AMP (cAMP), the second messenger
This activates enzymes to trigger a reaction cascade converting glycogen into glucose
How does the autonomic nervous system speed up the heart rate?
The acceleratory centre of the medulla oblongata is activated
This causes the frequency of the action potentials sent down the accelerator nerve (part of the sympathetic nervous system) to increase
These travel to the sino-atrial node (SAN) and cause the heart rate to increase
How does the autonomic nervous system slow down the heart rate?
The inhibitory centre of the medulla oblongata is activated
This causes the frequency of the action potentials sent down the vagus nerve (part of the parasympathetic nervous system) to decrease
These travel to the sino-atrial node (SAN) and cause the heart rate to decrease
How do baroreceptors influence the heart rate?
When blood pressure gets too low, impulses are sent to the medulla oblongata, which triggers the heart rate to increase
When blood pressure gets too high, impulses are sent to the medulla oblongata, which triggers the heart rate to decrease
How do chemoreceptors influence the heart rate?
When the respiratory rate increases, CO2 levels in the blood increase, which causes the pH to decrease due to the production of carbonic acid- this causes chemoreceptors to send impulses to the medulla oblongata, which triggers the heart rate to increase (so that CO2 can be removed more quickly)
When the respiratory rate decreases, CO2 levels in the blood decrease, which causes the pH to increase- this causes chemoreceptors to send impulses to the medulla oblongata, which triggers the heart rate to decrease (back to its normal level)
What are the long-term adverse effects of stress?
Continually high blood pressure (from increased heart rate) can lead to cardiovascular problems
Continually high blood glucose (from glycogenolysis) can lead to diabetes
Suppression of the immune system results in a higher susceptibility to disease/infection
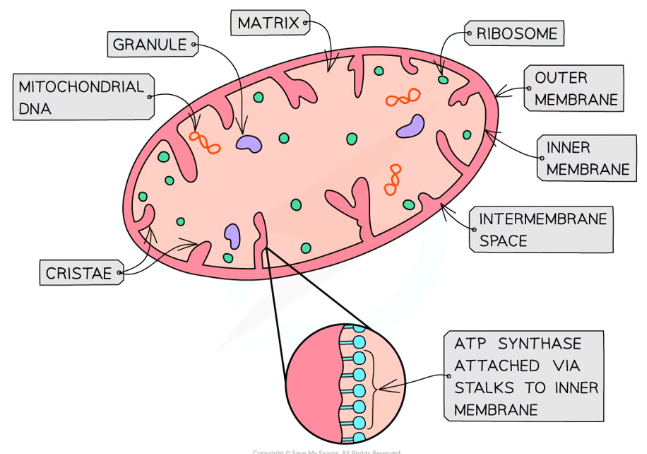
What is the structure of mitochondria?
Mitochondria have two membranes, a smooth outer one and an inner one which is folded up into cristae, projections which point inwards (high surface area)
Between these is the intermembrane space, which has a low pH (high proton concentration)
The inner membrane contains the matrix (like cytoplasm), itself containing 70S ribosomes, enzymes and circular mitochondrial DNA
What are the stages of aerobic respiration? Where do they each take place?
Glycolysis- in the cytoplasm
The Link reaction (oxidative decarboxylation)- in the mitochondrial matrix
The Krebs cycle- in the mitochondrial matrix
Oxidative phosphorylation (electron transport chain)- at the mitochondrial inner membrane
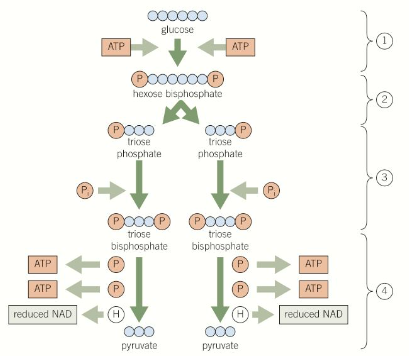
What is the process of glycolysis?
One molecule of glucose (6C) is phosphorylated to form one molecule of hexose bisphosphate (6C), using 2 ATP (producing 2 ADP)- this makes it more reactive
The hexose bisphosphate splits into two molecules of triose phosphate (3C) by lysis
Each triose phosphate is phosphorylated to form a triose bisphosphate molecule (3C) (using free phosphate ions from the cytoplasm)
Each triose bisphosphate molecule is then dehydrogenated (oxidised) to reduce the coenzyme NAD into NADH, and dephosphorylated to convert 2 ADP into 2 ATP (4 total)- this produces two pyruvate (3C) molecules
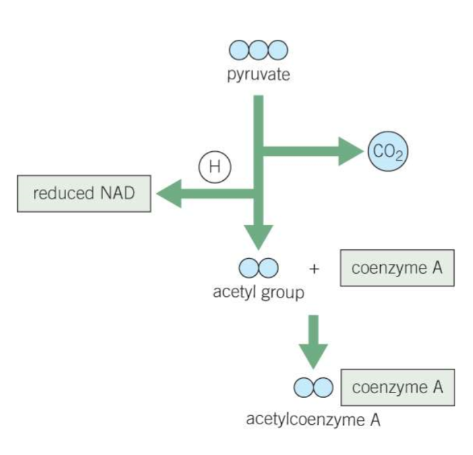
What is the process of the Link reaction?
Pyruvate is actively transported from the cytoplasm across the double membrane of the mitochondria into the matrix
Pyruvate (3C) is decarboxylated by losing a carbon dioxide molecule, and oxidised by losing a hydrogen, which reduces NAD into NADH
This produces an acetyl group (2C), which binds with coenzyme A to form acetylcoenzyme A (acetyl coA)
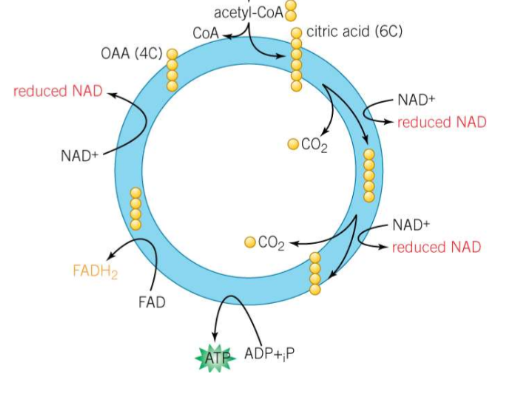
What is the process of the Krebs cycle?
Acetylcoenzyme A (2C) is joined with oxaloacetate (4C) to form citrate (6C), releasing the coenzyme A
The citrate is decarboxylated twice by losing two carbon dioxide molecules, producing a 4C compound
This compound is dehydrogenated (oxidised) by losing 5 hydrogens to reduce 3 NAD and 1 FAD to NADH and FADH2
The compound loses a phosphate group to form ATP from ADP (substrate-level phosphorylation)
This process regenerates the oxaloacetate molecule
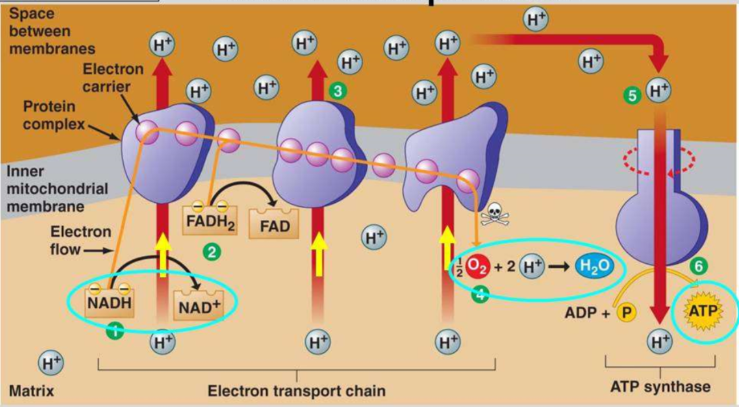
What is the process of oxidative phosphorylation?
NADH and FADH2 produced in the Krebs cycle are oxidised by losing hydrogen atoms, which split into H+ ions (protons) and electrons
These high energy electrons enter the electron transport chain, releasing energy as they move down levels
This energy is used to transport protons from the mitochondrial matrix into the intermembrane space, creating a proton gradient
The protons return to the matrix via facilitated diffusion through ATP synthase channel proteins, which converts ADP into ATP (this is chemiosmosis)
The protons and electrons at the end of this process combine with oxygen (the final electron acceptor) to form water
What are the reactants and end products of each step of aerobic respiration?
Glycolysis- one glucose molecule is converted into two pyruvate molecules, producing 2 NADH and net 2 ATP (2 used up, 4 produced)
The Link reaction- one pyruvate is converted into acetylcoenzyme A, producing NADH and one CO2 molecule
The Krebs cycle- one acetylcoenzyme A molecule is used to produce 3 NADH, FADH2, ATP, 2 CO2 and a coenzyme A molecule, regenerating oxaloacetate which is reused in the cycle
Oxidative phosphorylation- hydrogen atoms from NADH and FADH2 are used to produce ATP and water
How do cristae in mitochondria increase respiration?
The cristae greatly increase the surface area of the inner mitochondrial membrane, which provides more area for the facilitated diffusion of protons through ATP synthase, to increase the rate of chemiosmosis in oxidative phosphorylation
Why are coenzymes important for respiration?
Coenzyme A is used to transport the acetyl group from the Link reaction to the Krebs cycle
NAD and FAD can accept hydrogen atoms (get reduced) and transfer them from different stages (mainly the Krebs cycle) to the electron transport chain for oxidative phosphorylation to occur
How does a lack of oxygen impact respiration?
No final electron acceptor at the end of the electron transport chain, so it stops functioning
This means no more ATP is produced by oxidative phosphorylation
NADH and FADH2 can’t be oxidised by donating hydrogen atoms to the electron transport chain
This means no NAD and FAD are available for the Krebs cycle, so it stops
In this case, anaerobic respiration is used to supplement ATP demand
What are the three types of organism in terms of aerobic an anaerobic respiration?
Obligate anaerobes- can’t survive in the presence of oxygen (eg. some bacteria)
Facultative anaerobes- can switch between anaerobic and aerobic depending on whether oxygen is present or not (eg. yeast)
Obligate aerobes- can’t survive in the absence of oxygen (eg. mammals)
Even though mammals can use anaerobic respiration to produce ATP, they are not facultative anaerobes as they can’t survive without oxygen- anaerobic respiration can only be used for short periods supplementing aerobic respiration, when oxygen is low
How does anaerobic respiration work?
Anaerobic respiration only involves glycolysis (same as in aerobic respiration), producing small amounts of ATP- 2 per glucose molecule
Some cells are able to reoxidise the NADH produced so that the process can continue:
Yeast cells (and some plant cells) can use ethanol fermentation
Mammalian muscle cells can use lactate fermentation
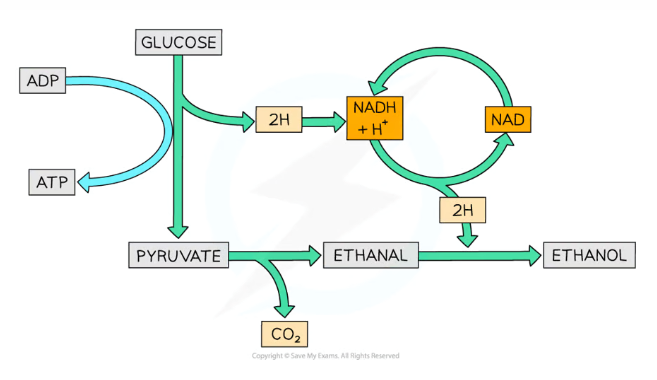
What is the process of ethanol fermentation by yeast (and some plant cells)?
Glucose is converted into two pyruvate molecules during glycolysis, also producing 2 ATP and NADH
The pyruvate is then decarboxylated to ethanal, catalysed by the enzyme pyruvate decarboxylase, producing CO2
The ethanal is reduced to ethanol by NADH (reforming NAD)
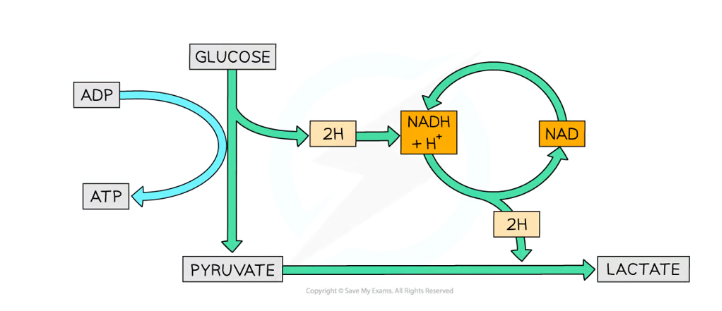
What is the process of lactate fermentation in mammals?
Glucose is converted into two pyruvate molecules during glycolysis, also producing 2 ATP and NADH
The pyruvate is then reduced to lactate by NADH (reforming NAD), catalysed by the enzyme lactate dehydrogenase
The lactate is converted back into glucose (metabolised) in the liver, requiring lots of oxygen (causing oxygen debt)
This is a reversible reaction
How are different respiratory substrates used in respiration?
Triglycerides (lipids) are hydrolysed into fatty acids, which are converted into acetyl CoA and enter the Krebs cycle, and glycerol, which is converted into pyruvate and enters the Link reaction
Proteins are hydrolysed into amino acids, which have to be deaminated (removing amine group) and converted into pyruvate which enters the Link reaction
Why do different respiratory substrates have different relative energy values?
Lipids release the most energy when they are broken down, compared to carbohydrates and proteins, which are roughly equal
This is because lipids contain more hydrogens, meaning more hydrogen atoms are available to form a proton gradient during chemiosmosis, producing more ATP
What is the respiratory quotient? What are the values for carbohydrates, proteins and lipids?
RQ = CO2 produced / O2 consumed
Eg. For glucose, C6H12O6 +6 O2 → 6 CO2+ 6 H2O, so the RQ = 6/6 = 1.0
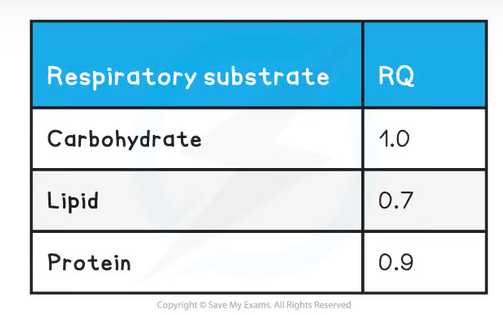
How is carbon dioxide produced in the body and what effect does it have on the body if not excreted as a waste product?
Produced by the decarboxylation of respiratory substrates during aerobic respiration
Carbon dioxide is converted into carbonic acid (dissociates to form hydrogen carbonate ions) to be transported in the blood, so it decreases the blood pH in high concentrations, which can damage cells (acidosis)
How is ammonia produced in the body and what effect does it have on the body if not excreted as a waste product?
Produced by the deamination of excess amino acids in the liver
Ammonia is converted into urea, both of which are toxic nitrogenous waste, which diffuses into cells, decreasing the water potential so that they absorb water by osmosis and burst
What is the gross structure of the liver?
The liver receives oxygenated blood from the heart via the hepatic artery, and the deoxygenated blood returns via the hepatic vein
It also receives blood from the duodenum (small intestine) via the hepatic portal vein, so it can use the reabsorbed nutrients
It is connected to the gall bladder, which stores the bile the liver produces, then secretes it into the bile duct to the duodenum
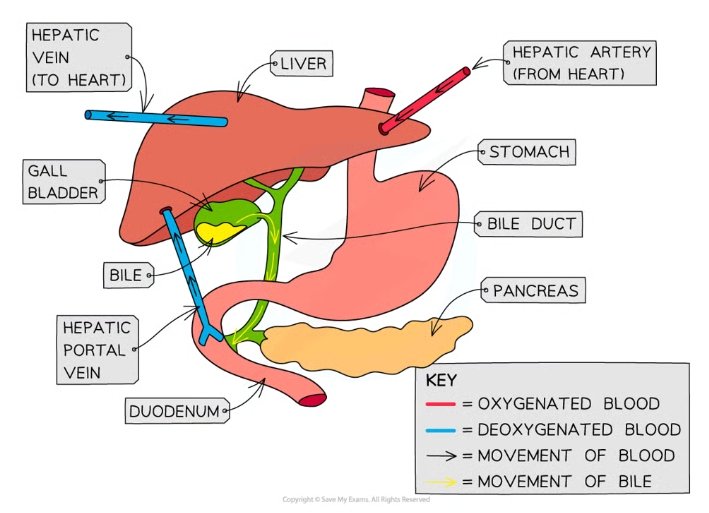
What is the histology of the liver?
Hepatocytes (liver cells) are arranged into lobules, containing channels called sinusoids
At the corners of lobules are branches of the hepatic portal vein and hepatic artery, which supply oxygenated blood and nutrients to the liver, and branches of the bile duct, which receives the bile (waste products) produced
At the middle of each lobule is a branch of the hepatic vein, which receives the deoxygenated blood produced
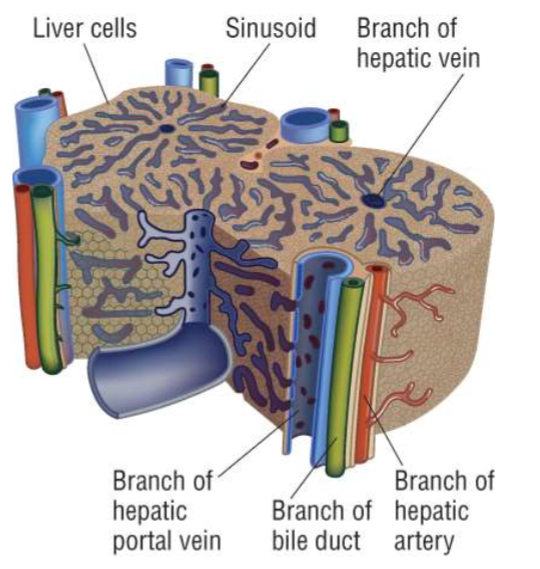
How do sinusoids work?
Oxygenated blood from the branch of the hepatic artery and nutrient-rich deoxygenated blood from the branch of the hepatic portal vein mix, and flow towards the central branch of the hepatic vein
The hepatocytes (liver cells) use this oxygen to metabolise the nutrients and process waste products in the blood, and the deoxygenated blood produced exits via the branch of the hepatic vein
Kupffer cells in the sinusoids are resident macrophages (phagocytes), which engulf and break down foreign bodies and pathogens
The hepatocytes produce bile, which they secrete into the bile canaliculi, which flow the opposite direction towards the branch of the bile duct
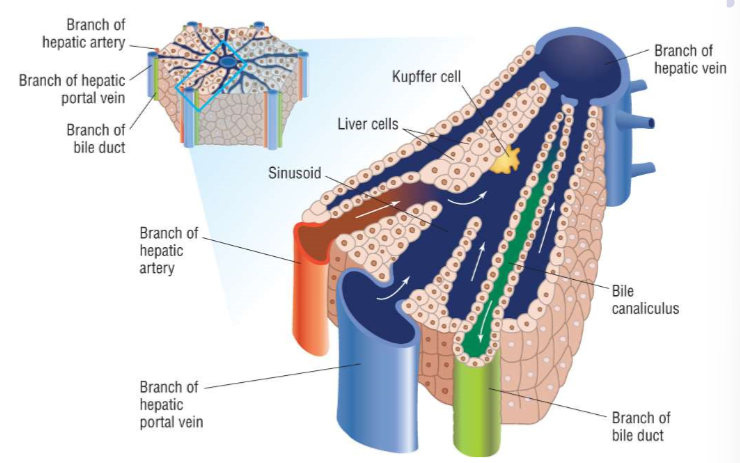
What are the three functions of the liver?
Glycogenesis, and the storage of glycogen in hepatocytes
Formation of urea from excess amino acids, by deamination and the ornithine cycle
Detoxification of alcohol, hydrogen peroxide and lactate
What is the process of urea production by the liver?
Deamination of excess amino acids, removing the amine group (NH2) and a hydrogen to form ammonia (NH3)
This also produces a keto acid, which can enter the Krebs cycle to be respired, or be converted into glycogen or lipids for storage
The ammonia is toxic and so is converted into the less toxic urea by combining it with carbon dioxide in the ornithine cycle
What is the process of the detoxification of alcohol by the liver? How can this cause liver problems?
In the hepatocytes, ethanol is converted into ethanal by the enzyme ethanol dehydrogenase
Ethanal is converted into ethanoate by ethanal dehydrogenase, which can then enter the Krebs cycle to be respired
This produces ATP, which causes the liver not to metabolise as much stored fats, which can lead to fatty liver condition
This can worsen and lead to cirrhosis (scaring) of the liver due to excessive alcohol consumption
What is the gross structure of the kidney?
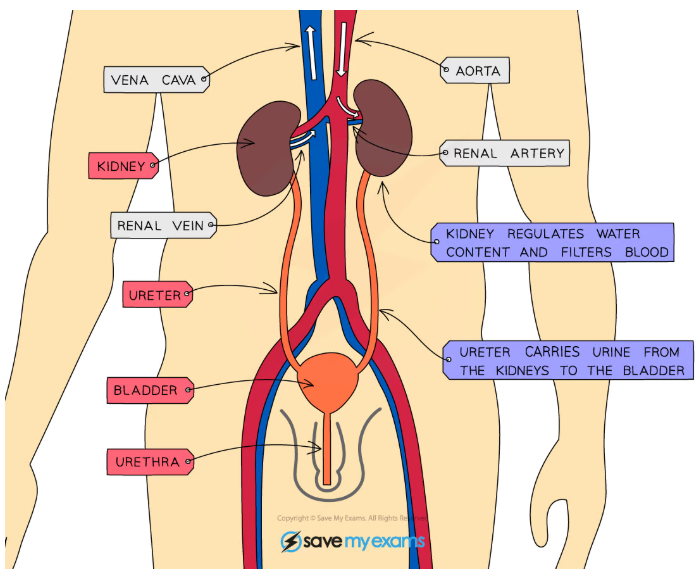
What is the histology of the kidney?
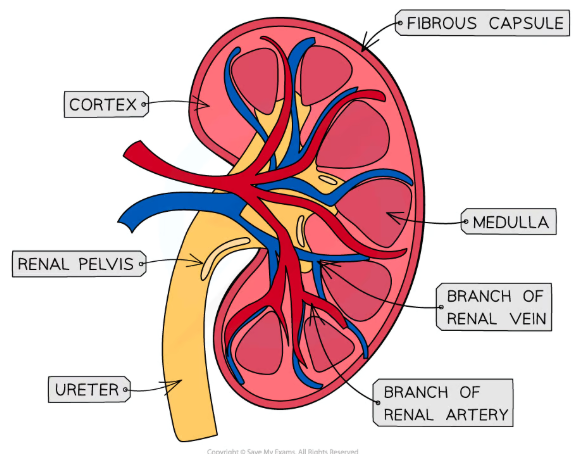
What is the basic structure of a nephron and where are they found?
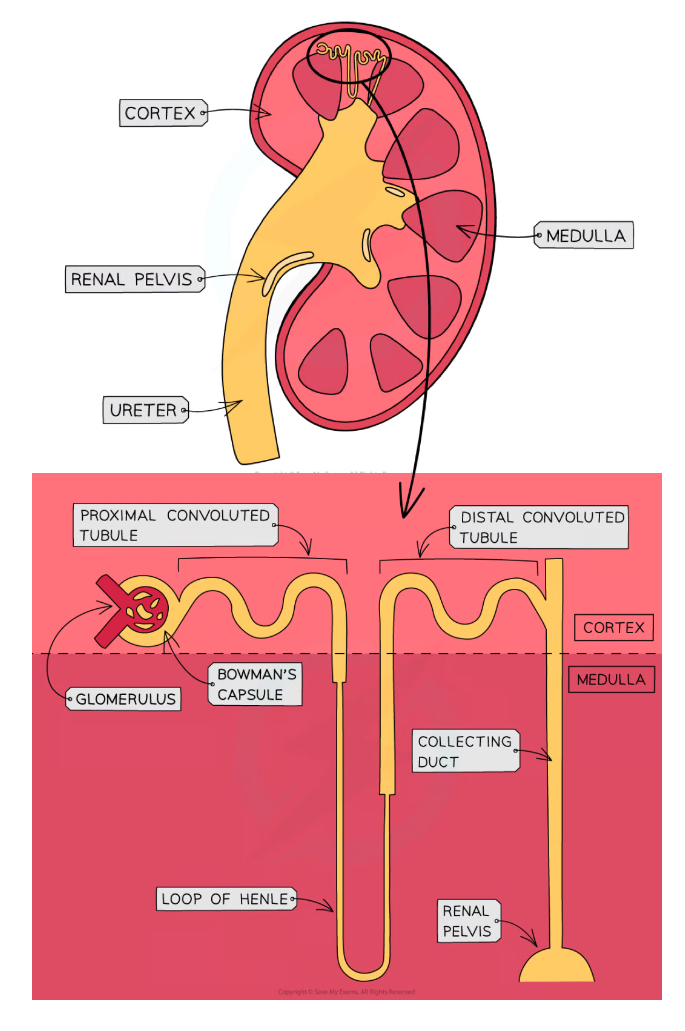
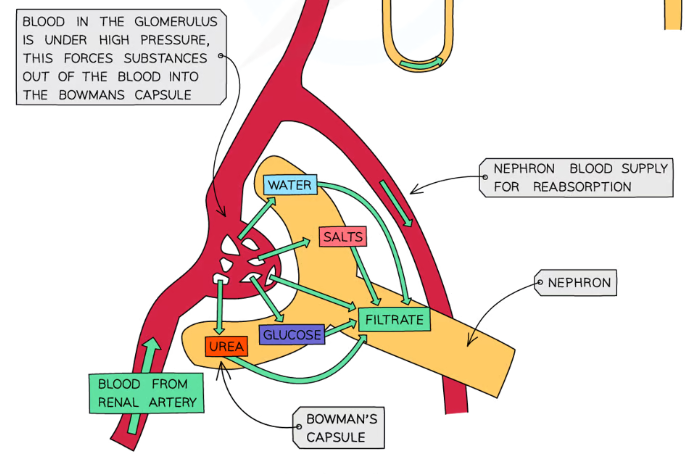
How are nephrons supplied with blood?
Oxygenated blood from the renal artery enters the glomerulus in the Bowman’s capsule through the afferent arteriole
The filtered blood leaves the glomerulus through the efferent arteriole
This is divided in a network of capillaries running along the rest of the nephron
The deoxygenated blood in these capillaries join up and leave through the renal vein
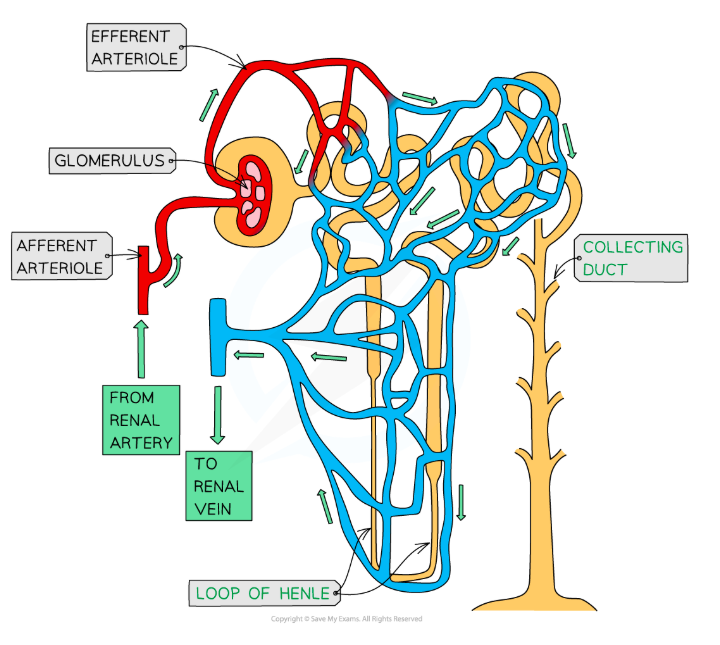
What substances are filtered out during ultrafiltration ad what substances stay in the blood?
Everything with a molecular mass smaller than 69,000 passes through the Bowman’s capsule
Small soluble molecules, including water, glucose, urea, inorganic ions (from salts) and amino acids are filtered out into the proximal convoluted tube of the nephron
Larger materials including red and white blood cells, plasma proteins and platelets can’t be filtered out and stay in the blood of the efferent arteriole
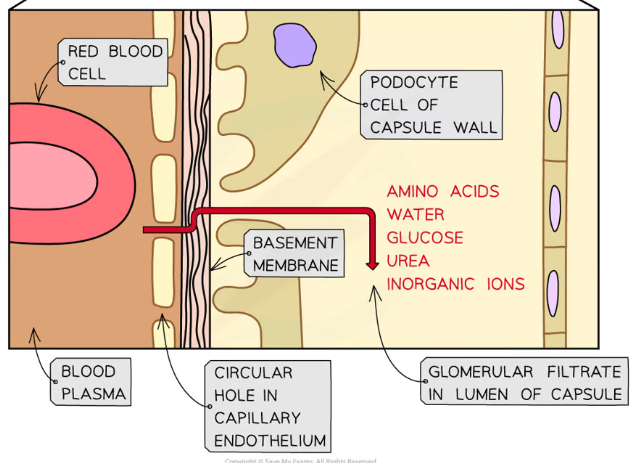
What layers are substances filtered through in the glomerulus and the Bowman’s capsule?
The first is the endothelium of the capillary, which has fenestrations (pores) between endothelial cells, for substances to leave through
The next is the basement membrane, which is made up of collagen and glycoproteins
The last is the epithelium of the Bowman’s capsule, which is made up of podocyte cells that have thin projections forming a web
Substances that can be filtered through these layers enter the lumen (space) of the Bowman’s capsule
How is the blood forced through the Bowman’s capsule?
During ultrafiltration, the blood is at very high pressures allowing the blood to be filtered effectively
This high pressure is achieved by the efferent arteriole (leaving the capsule) having a much smaller lumen than the afferent arteriole (entering the capsule)
How are solutes selectively reabsorbed in the proximal convoluted tube (pCT)
Sodium-potassium pumps in the basal membranes (side facing the capillaries) of pCT epithelium cells actively transport Na+ ions into the blood
This lowers their concentration inside the cells, maintaining a concentration gradient
This gradient causes Na+ ions in the filtrate to diffuse through the luminal membranes (side facing the pCT lumen) into the epithelium cells
They can only diffuse in through co-transporter proteins, transporting another solute (eg. glucose/an amino acid) at the same time
The solutes can then diffuse into the capillaries through transport proteins in the basal membranes
The filtrate at the end of the pCT contains no glucose, amino acids or vitamins, and about 85% of the water and Cl- ions are passively reabsorbed
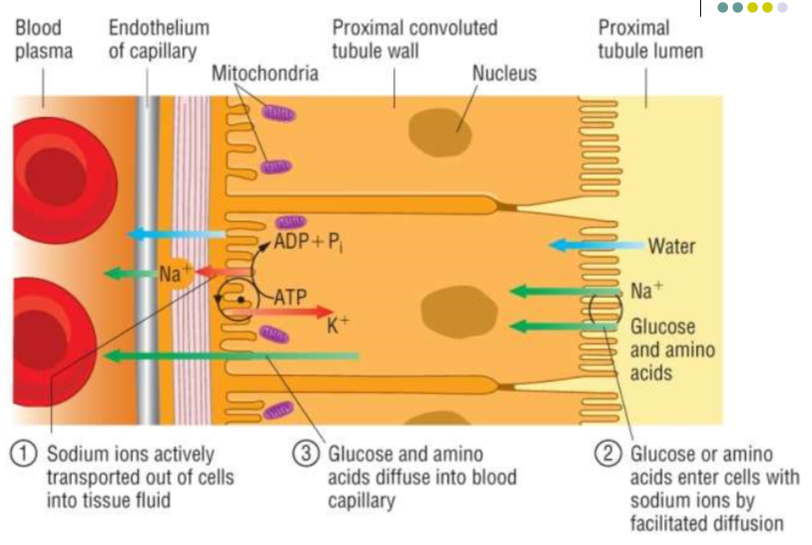
How is the proximal convoluted tubule (pCT) adapted for selective reabsorption?
Microvilli line the epithelium of the pCT, increasing the surface area
The epithelium contains co-transporter proteins, which allow specific large molecules to pass through into the blood (eg. glucose/amino acids)
The cells of the pCT contain many mitochondria, providing energy by respiration for sodium-potassium pumps in the basal membranes
Cells are tightly packed together, so no fluid passes between them
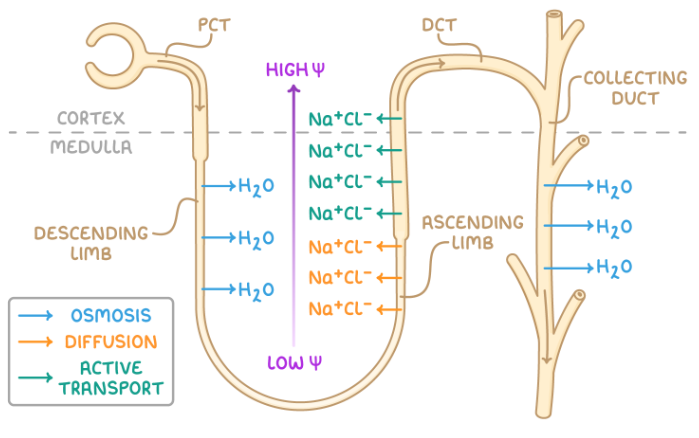
How does water and ion transport work in the loop of Henle?
The descending limb is permeable to water and impermeable to Na+ and Cl- ions, while the ascending limb is impermeable to water and permeable to ions
At the bottom of the ascending limb of the loop of Henle, Na+ and Cl- ions diffuse out of the filtrate into the interstitial space of the medulla
This establishes a low water potential in the interstitial space
Further up the ascending limb, as the water potential in the filtrate itself becomes higher, the ions must be actively transported out
This low water potential in the interstitial space encourages water to diffuse by osmosis out of the descending limb at the start of the loop of Henle
From the interstitial space, the water diffuses into the capillaries
The water leaving the descending limb lowers the water potential of the filtrate, in turn allowing the ion transport at the bottom of the ascending limb to be passive
This is known as a counter-current multiplier system, as the low water potential achieved deeper in the medulla allows water to diffuse out of the whole collecting duct, as there is always a water potential gradient, producing very concentrated urine
What does the distal convoluted tubule (DCT) do?
The cell membranes of DCT epithelium cells have many ion pumps and transporter proteins for active transport and facilitated diffusion of any remaining ions and other solutes
How is the water content of the blood controlled?
By osmoregulation
Osmoreceptors (sensory neurones) in the hypothalamus monitor the water potential of the blood
If the water potential drops, the osmoreceptors signal the release of more anti-diuretic hormone (ADH, produced in the hypothalamus) from the posterior pituitary gland
ADH travels through the blood to the collecting ducts in the kidneys
Here they cause the collecting duct cells to become more permeable to water
This means that more water will be reabsorbed into the blood, increasing the water potential and producing a smaller volume of more concentrated urine
(Vice versa for when water potential becomes too high- it is always fluctuating in a negative feedback loop)
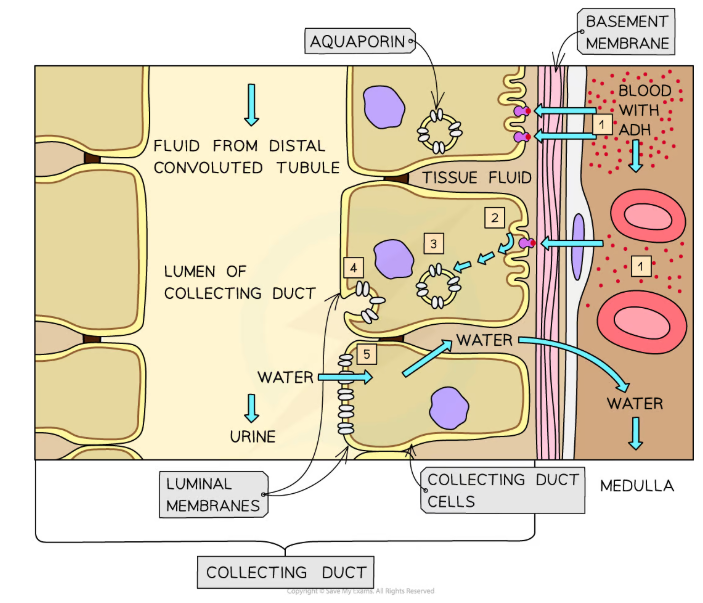
How does ADH make the collecting ducts more permeable to water?
ADH binds to receptors on the collecting duct cells, triggering a reaction cascade that causes the activation of aquaporin proteins in vesicles
This makes the vesicles fuse with the luminal membrane (facing the filtrate) of the collecting duct cells, depositing aquaporins
Aquaporin molecules are water-permeable channels, so the membrane permeability increases
How can urine samples be used in medicine?
Testing for glucose in the urine to diagnose diabetes- all the glucose should be reabsorbed in the PCT, but if the blood glucose concentration is too high some may still be excreted
Pregnancy test sticks- monoclonal antibodies are used to detect the presence of hCG, a hormone only found in pregnant women’s urine
Testing for drugs/alcohol and for anabolic steroid use, ‘doping’ in athletes- using mass spectrometry and gas chromatography of urine
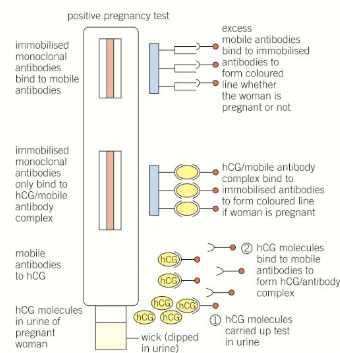
How do pregnancy tests work and how are they produced?
When the human embryo implants it releases the hCG hormone
A mouse is injected with hCG, causing an immune response where it produces B-cells that make the specific antibody
These are removed and fused with a myeloma cancer cell to produce a hybridoma cell that divides very rapidly and also produces the monoclonal antibodies
Pregnancy tests contain immobilised monoclonal antibodies, attached to coloured beads so that when hCG is present in the urine they are activated and a coloured line shows up
A second line is always formed regardless of whether the woman is pregnant, to make sure that the test is working
What problems can arise from kidney failure?
Less blood is filtered by the glomerulus, causing the glomerular filtration rate (GFR) to decrease- this leads to a build-up of urea, water (leading to high blood pressure), salts and toxins in the blood
The electrolyte balance in the blood is also disrupted (the concentrations of sodium, potassium and chloride ions are not maintained)- this causes osmotic imbalances
How can glomerular filtration rate be measured?
The concentration of creatinine in the blood is measured
Creatinine is a product of the natural breakdown of muscles, which should normally be filtered out of the blood
This means that a high creatinine concentration signals poorly functioning/failed kidneys
(It has to be taken into account that creatinine concentrations are typically higher in men and increas with age)
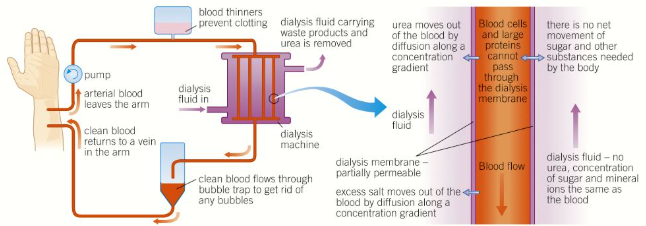
How does haemodyalisis work?
A patient’s blood (containing a blood thinner preventing clots) passes through a dialysis machine
Here it is filtered through partially permeable membranes into a dialysis fluid in a countercurrent system
This fluid has the same concentration of glucose as the patient’s blood, a typical concentration of mineral ions, and no urea
This means that all the urea is filtered out by diffusion, some mineral ions are filtered out to restore the electrolyte balance, and no glucose is lost
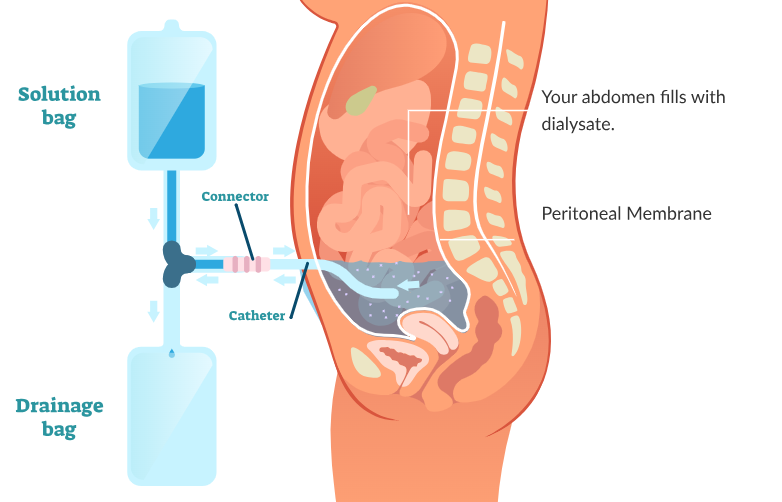
How does peritoneal dialysis work?
Dialysis is conducted across the peritoneum, the membrane which lines the abdomen of the patient
Dialysis fluid is introduced into the abdomen via a catheter and left for several hours
Urea and excess mineral ions in the blood cross the peritoneal membrane into the dialysis fluid, which is then drained out
How do kidney transplants work?
One healthy donor kidney is surgically transplanted to replace both of a patient’s non-functioning kidneys
This requires finding a donor with a compatible blood group
To prevent rejection the patient must still take immunosuppressants their whole lives (which leaves them more vulnerable to infections)
Give the function and structure of each of the neurones
Sensory- carry impulses from the receptors to the CNS, cell body branches off from the middle of the axon
Relay- connect sensory and motor neurones, short axon and dendrites branch out from the cell body
Motor- carry impulses from the CNS to the effectors, cell body at one end of the axon with dendrites branching off
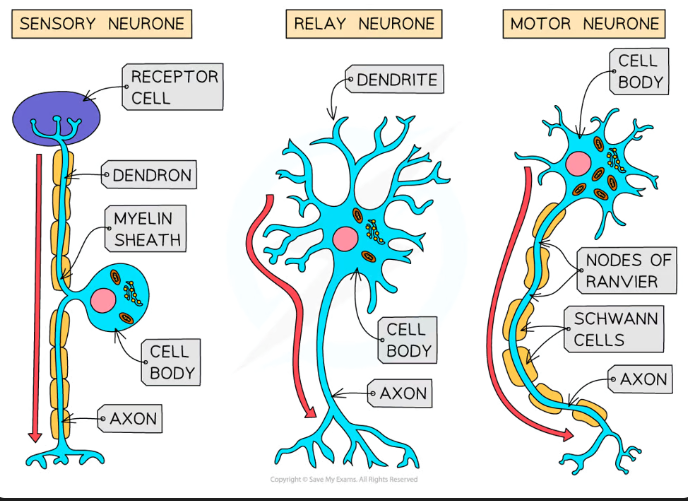
What is the structure of the myelin sheath? What benefits does it have?
Specialised Schwann cells wrap around the axon multiple times, which builds up layers of phospholipid bilayer
Between the Schwann cells there are small uninsulated sections called nodes of Ranvier
The electrical impulse in myelinated neurones will ‘jump’ between these nodes instead of travelling the whole length of the axon (saltatory conduction), which greatly speeds up the transmission compared to unmyelinated neurones
Why are sensory receptors referred to as transducers?
Sensory receptors are transducers because they convert stimuli (light, heat and sound energy) into electrical impulses within sensory neurones
What are the main sensory receptors, what stimuli do they do detect, and where are they found?
Photoreceptors- light- cone cells in the eye
Thermoreceptors- heat- the skin
Chemoreceptors- chemicals (tastes and smells)- the nose and tongue
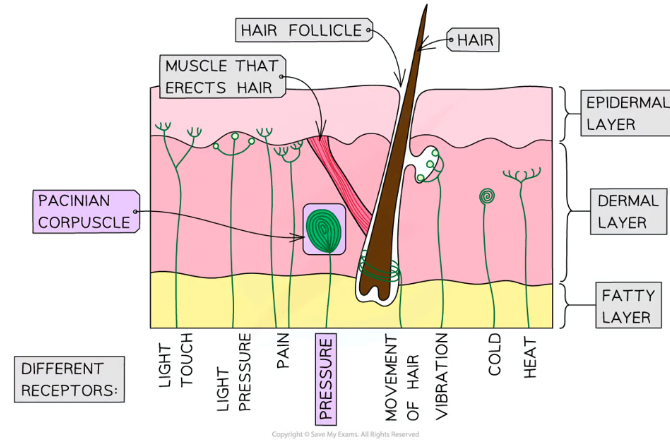
Mechanoreceptors- pressure + movement- pacinian corpuscle in the skin
What are pacinian corpuscles where are they found?
Pacinian corpuscles are mechanoreceptors found deep in the skin, which respond to pressure changes
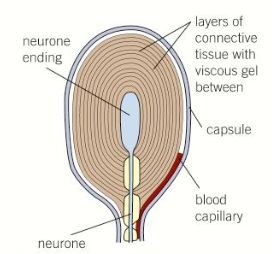
What is the structure of pacinian corpuscles?
Layers of connective tissue separated by a gel surround the end of a sensory neurone dendrite
The gel contains Na+ ions, but the sensory neurone doesn’t, giving it a negative charge (resting potential)
The membrane of the sensory neurone contains stretch-mediated sodium ion channels which change width based on pressure changes
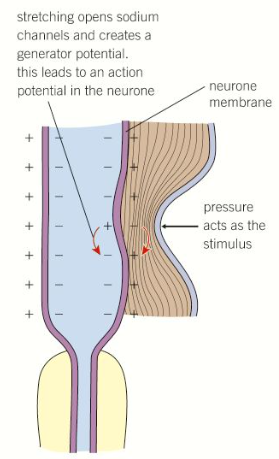
What happens at pascinian corpuscles to generate an impulse?
Stretch-mediated sodium ion channels in the sensory neurone membrane are too narrow for sodium ions to diffuse through into the sensory neurone, which gives it a negative charge (the resting potential)
When pressure is applied, the membrane is distorted, causing the stretch-mediated sodium ion channels to widen so that sodium ions can diffuse into the sensory neurone
This depolarises the neurone (the generator potential), which creates an impulse (the action potential) that can travel down the neurone
What is a resting potential and how is it established in a neurone?
At rest, the inside of a neurone has a negative electrical potential compared to the outside, called the resting potential, which is about -70mV
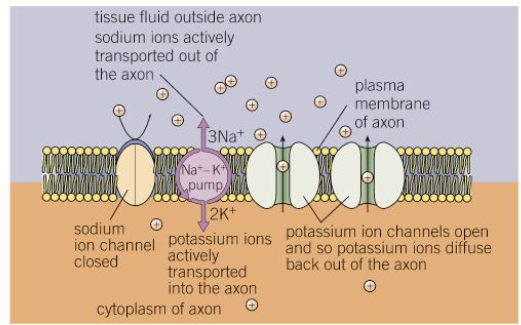
To establish this, sodium-potassium pumps in the membranes of neurones actively transport (using ATP) 3 Na+ ions out of the neurone, in exchange for 2K+ ions in
Some potassium ion channel proteins are open, allowing K+ ions to leave the neurone by facilitated diffusion down their electrochemical (concentration) gradient
The sodium ion channels are closed, blocking the diffusion of Na+, so positive ions will build up outside the neurone, giving it a relative negative charge
How are action potentials generated in nuerones?
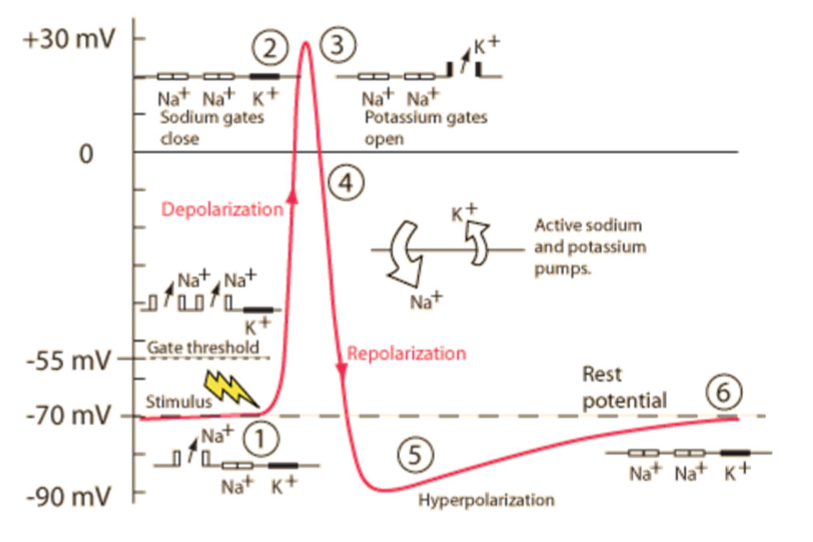
A stimulus causes some sodium ion channels to open, so that Na+ ions can diffuse into the neurone down their electrochemical gradient, making the charge less negative
If this reaches a threshold of about -55mV, the voltage-gated sodium ion channels open, so more Na+ ions can diffuse in, causing the neurone to depolarise to +40mV (this is positive feedback)
At this point, the sodium ion channels close and the potassium ion channels open (negative feedback), allowing K+ ions to diffuse out and lower the charge again, through repolarisation
The potassium ion channels are slow to close, meaning too many K+ ions end up diffusing out, causing the neurone to be hyperpolarised
The potassium ion channels close and sodium-potassium pumps restore the resting potential
How is an action potential transmitted down a neurone?
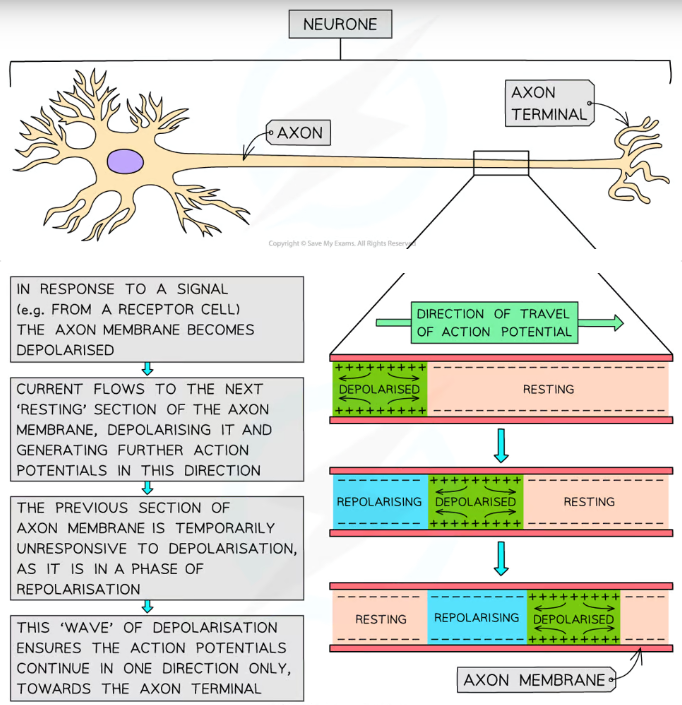
An action potential in one section of a neuron acts as a stimulus for sodium ion channels to open further along, depolarising the next section, moving like a wave
This forces the impulse to travel in only one direction, as the previous section is in a refractory period, where it is repolarising and is unresponsive to stimulus
What is the all-or-nothing principle?
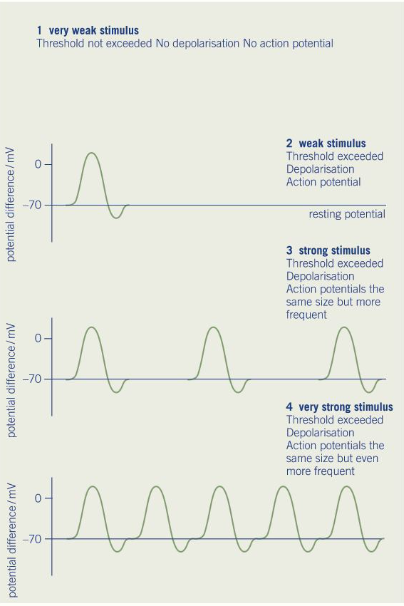
An impulse is only generated if the initial stimulus is sufficient to reach the threshold (-55mV) at which the voltage-gated sodium ion channels will open
If the threshold is reached, the magnitude of the action potential will always be the same (+40mV), and will not be proportionate to the magnitude of the stimulus
However, stronger stimuli increase the frequency of the action potential
What is saltatory conduction?
In myelinated neurones the nodes of Ranvier, the gaps between Schwann cells, are the only points where sodium ions can diffuse through the membrane
This means the axon can only depolarise at these points, so the action potential ‘jumps’ between them
This is significantly faster, so myelinated neurones have a higher speed of transmission than non-myelinated neurones
What factors affect the speed of impulse transmission?
Myelination- speeds up transmission due to saltatory conduction
Axon diameter- greater diameters result in greater surface area for ion diffusion, speeding up transmission
Temperature- warmer temperatures result in faster diffusion of ions due to higher kinetic energy, speeding up transmission, however when the temperature gets too high the ion channel proteins denature and prevent/slow transmission
What is a cholinergic synapse?
A synapse (gap between two neurones) that uses acetylcholine as a chemical neurotransmitter