Week 3: Chapter 48 - (Exam 1) - NRSE 2212 Cox/Rice/Saunders
1/90
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
91 Terms
Why should all wounds not be cleaned with chlorhexidine prior to obtaining a culture?
Antiseptic solutions like chlorhexidine may damage healthy tissue and delay wound healing
What is aseptic technique?
A procedure used by medical staff to prevent the spread of infection
Before collecting a wound culture sample, what must you clean the skin with?
Normal Saline
Should wound culture samples be taken from old drainage?
No!
Pressure sores, ulcers, decubitus ulcers, and bedsores are now referred to as...?
Pressure Injuries
What are the 6 layers of the skin and underlying structures?
1. Epidermis
2. Dermis
3. Subcutaneous layer
4. Fascia of Muscle
5. Muscle
6. Bone
What is the straum corneum?
The outermost layer of the epidermis, acting as the primary barrier against the environment by protecting against dehydration, pathogens, and UV radiation.
What is the straum germinativum?
Aka, the stratum basale.
- The deepest layer of the epidermis (outer skin) where new skin cells are constantly generated through cell division (mitosis) to replace old cells, making it crucial for skin renewal and repair.
What are the 5 layers of the skin?
stratum corneum, stratum lucidum, stratum granulosum, stratum spinosum, stratum basale
Come Let's Get Sun Burnt
In the older adult, the skin becomes ... what? (5)
- Less elastic
- Drier
- Reduced collagen
- Areas of hyperpigmentation
- More prone to injury
Why are infants just as prone to skin injuries as older adults?
Their skin is thinner and more permeable than that of adults, which predisposes infants to skin breakdown.
Which patients are the most at risk for pressure injuries?
Those with immobility, friction and shear, moisture, incontinence, poor nutrition, perfusion, age, skin conditions, and altered LOC.
What is impaired mobility?
decreased/restricted mobility, but not completely immobile
What is the best location to check skin turgor on an older adult?
Clavicle.
Adequate levels of ... what .. maintain the skin, repair minor defects, and preserve intravascular volume
Protein!
Impaired arterial circulation aka tissue perfusion does what...?
- Restricts activity
- Produces pain
- Leads to muscle atrophy
- Development of thin tissue that is prone to ischemia and necrosis
Impaired venous circulation does what...?
- Engorged tissues with high levels of metabolic waste
- Edema
- Ulcerations
- Skin breakdown
What certain types of drugs are more notorious for causing reactions?
- Allopurinol
- Anticonvulsants
- Antipsychotics
- PCN and Sulfa Drugs
- Pain Relievers
- Digoxin NSAIDs
What is skin maceration?
Softening of skin from prolonged contact with moisture
What does the skin need to regenerate cells from maceration?
O2
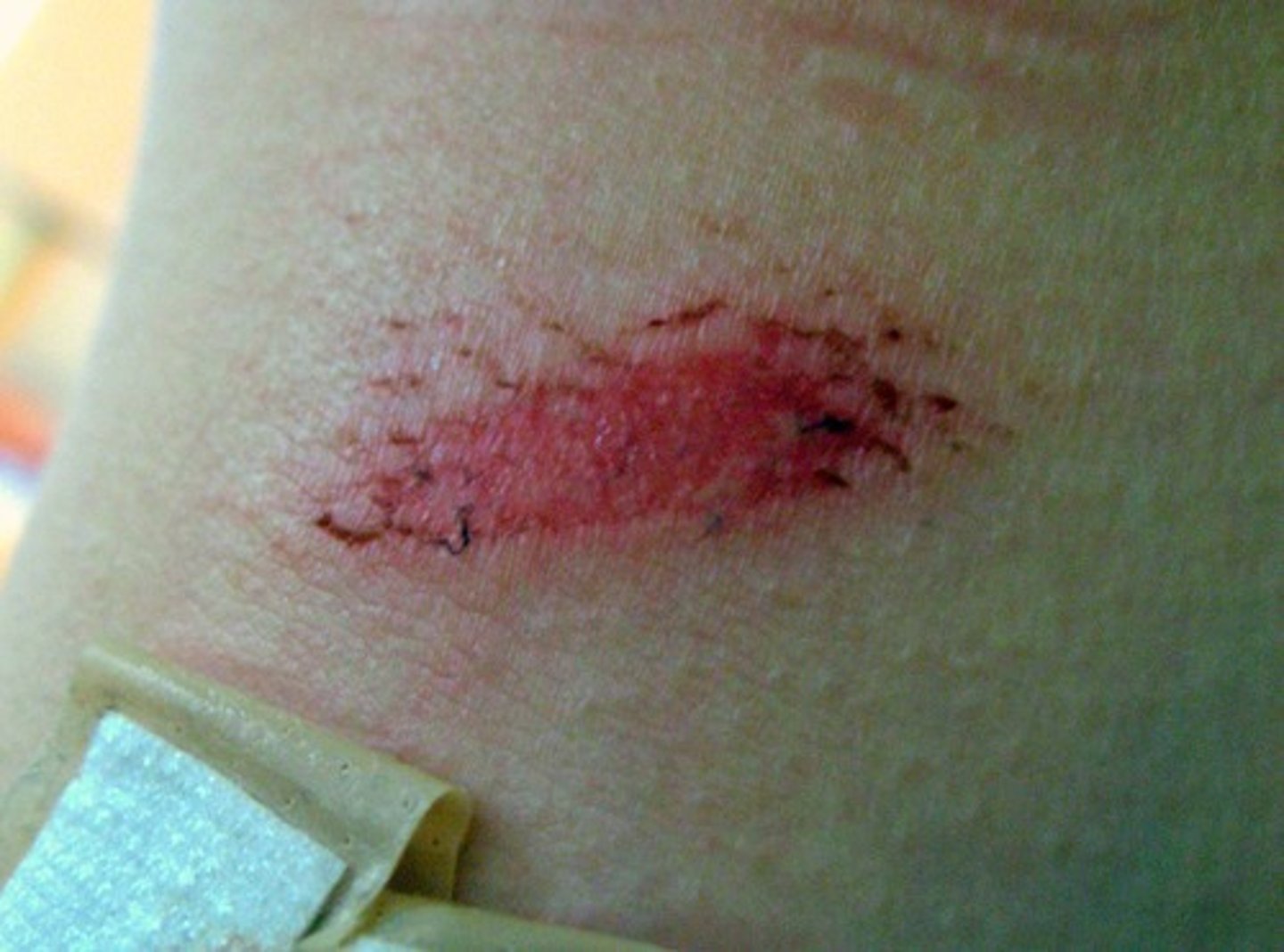
What is an abrasion?
a scrape of the superficial layers of the skin; usually unintentional but may be performed intentionally for cosmetic purposes to smooth skin surfaces
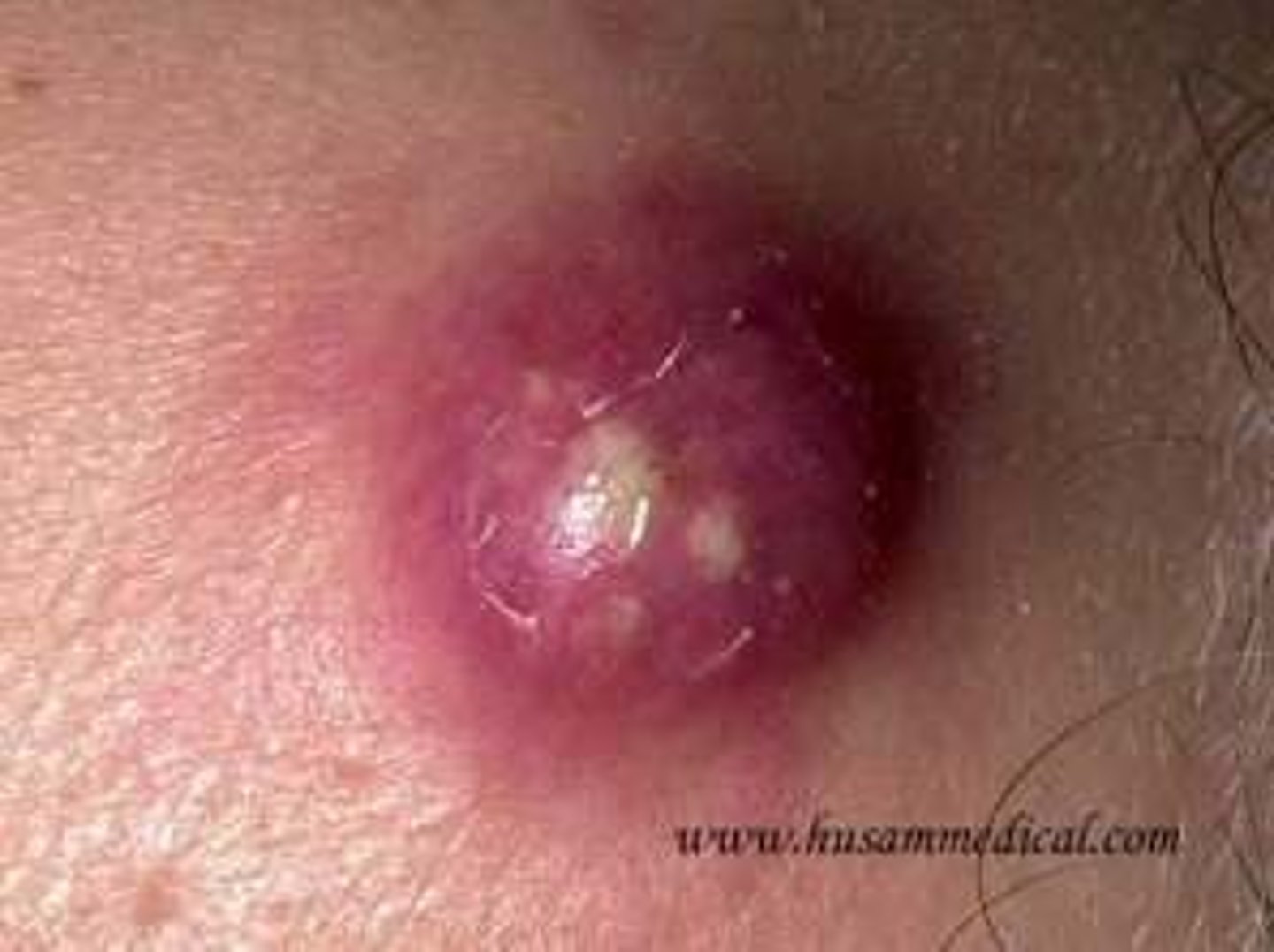
What is an abscess?
A localized collection of pus resulting from invasion from a pyogenic bacterium or other pathogen; must be opened and drained to heal
What is a contusion?
bruise
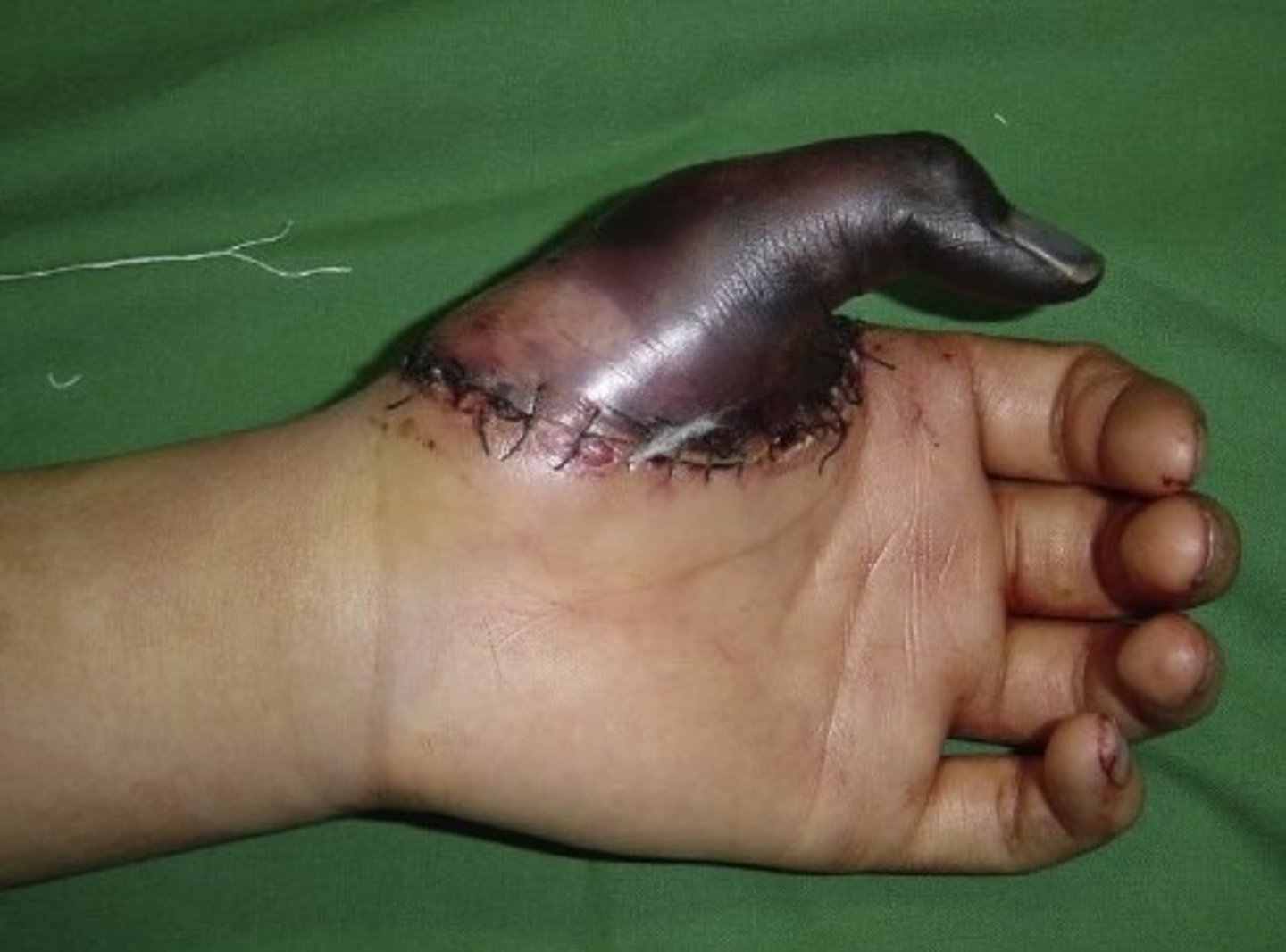
What is a crushing wound?
wound caused by force leading to compression or disruption of tissues
What is wound excoriation?
a skin injury where the top layer of skin is scraped, torn, or worn off, creating an abrasion, scratch, or linear erosion, often from mechanical force like scratching with fingernails or using tools, leading to open sores, scabs, or potential infection.
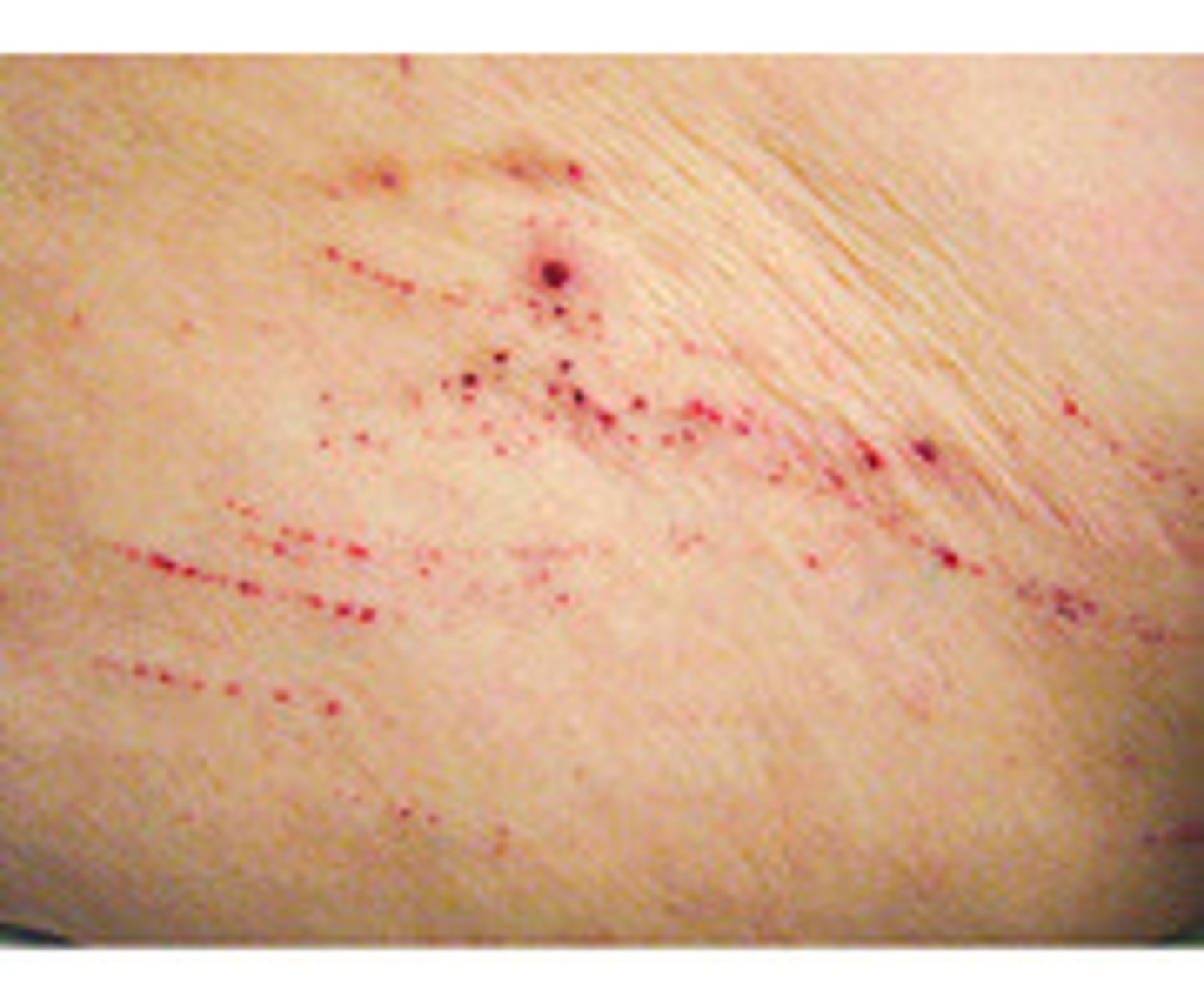
What is an incision?
A sharp, smooth cut.
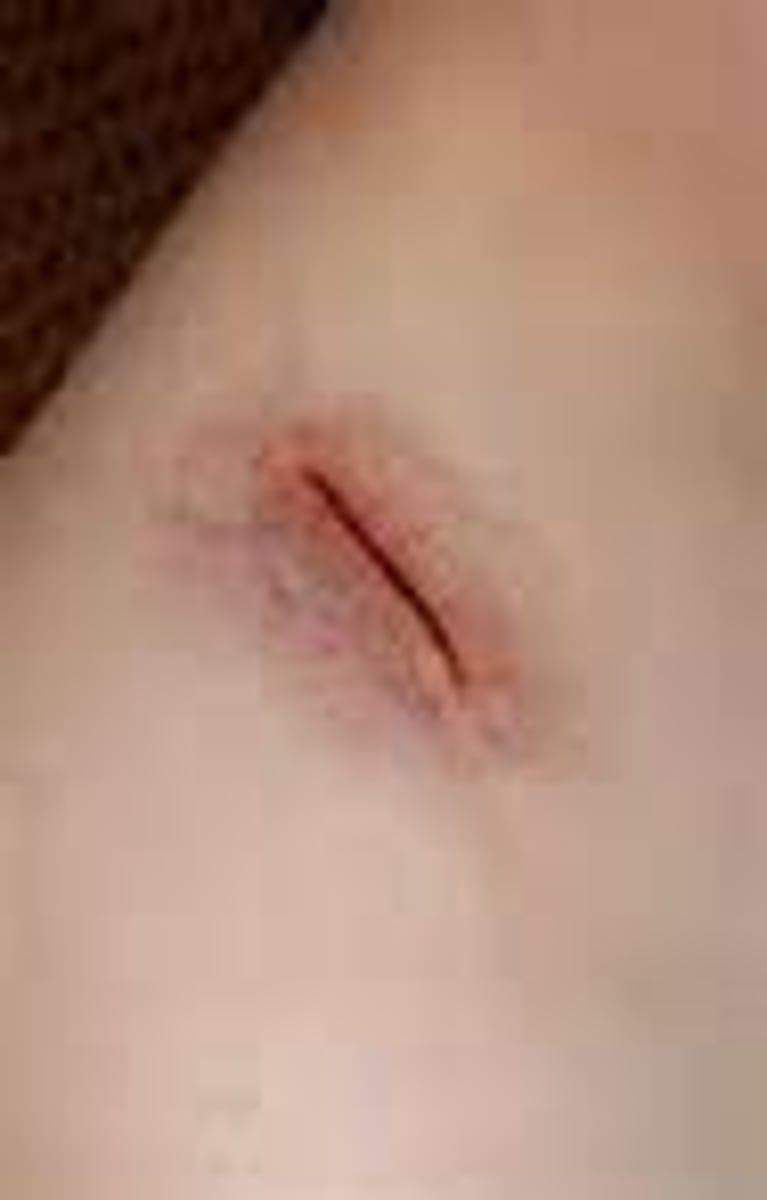
What is a laceration?
a deep cut or tear in skin or flesh.
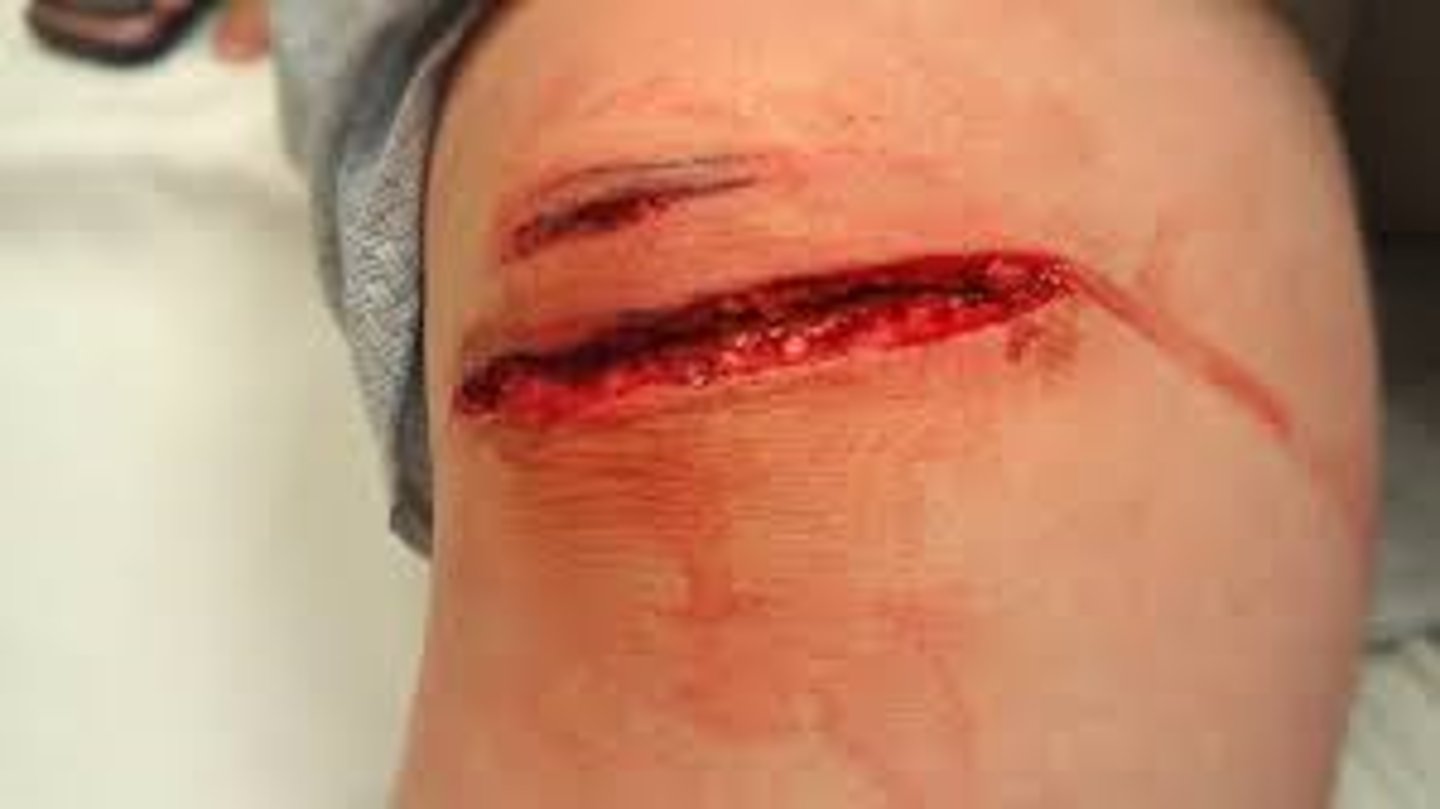
What is a penetrating wound?
Like a puncture wound, but the item remains embedded in the tissue.
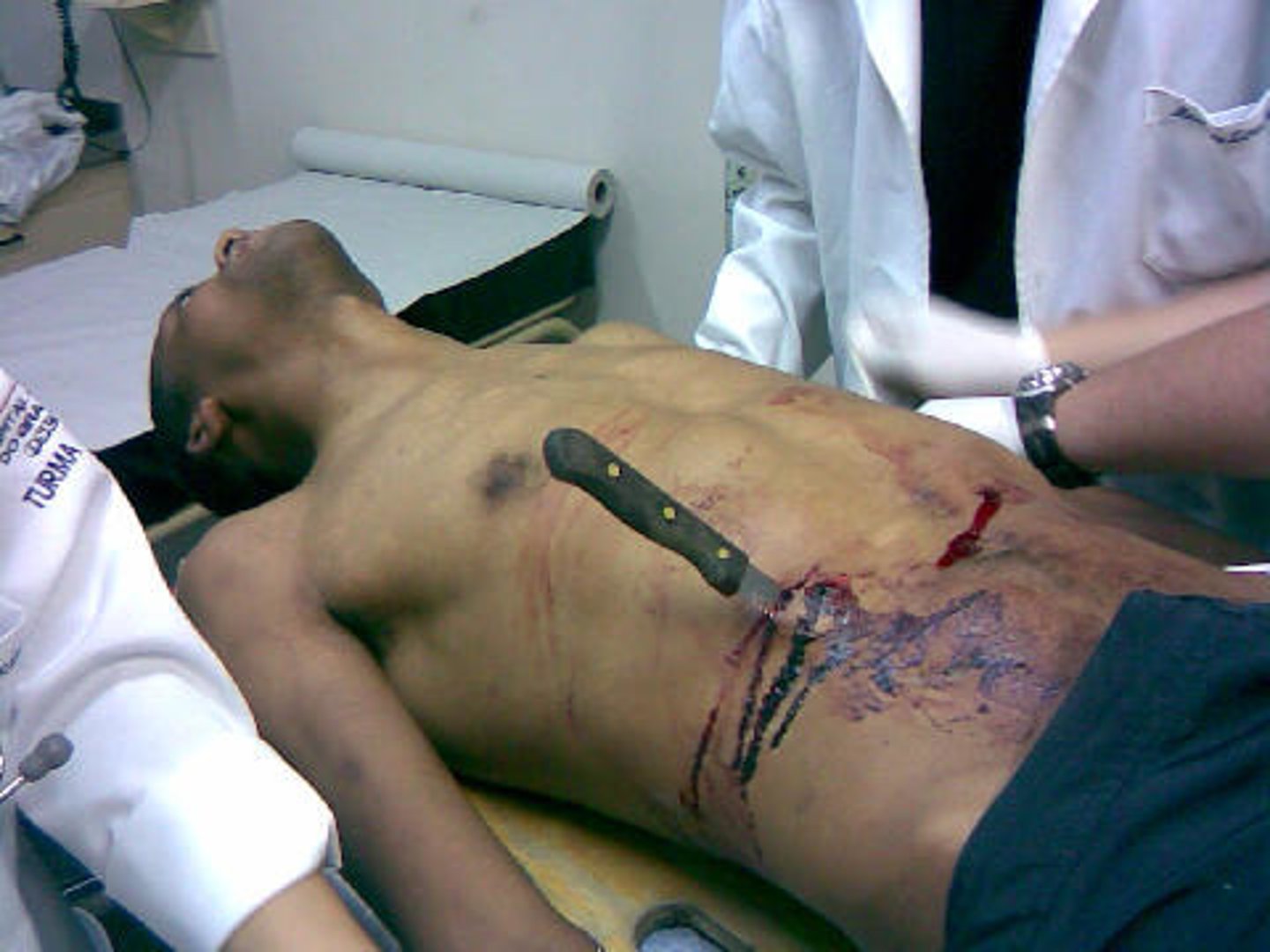
What is a puncture wound?
When blunt or sharp object punctures the skin
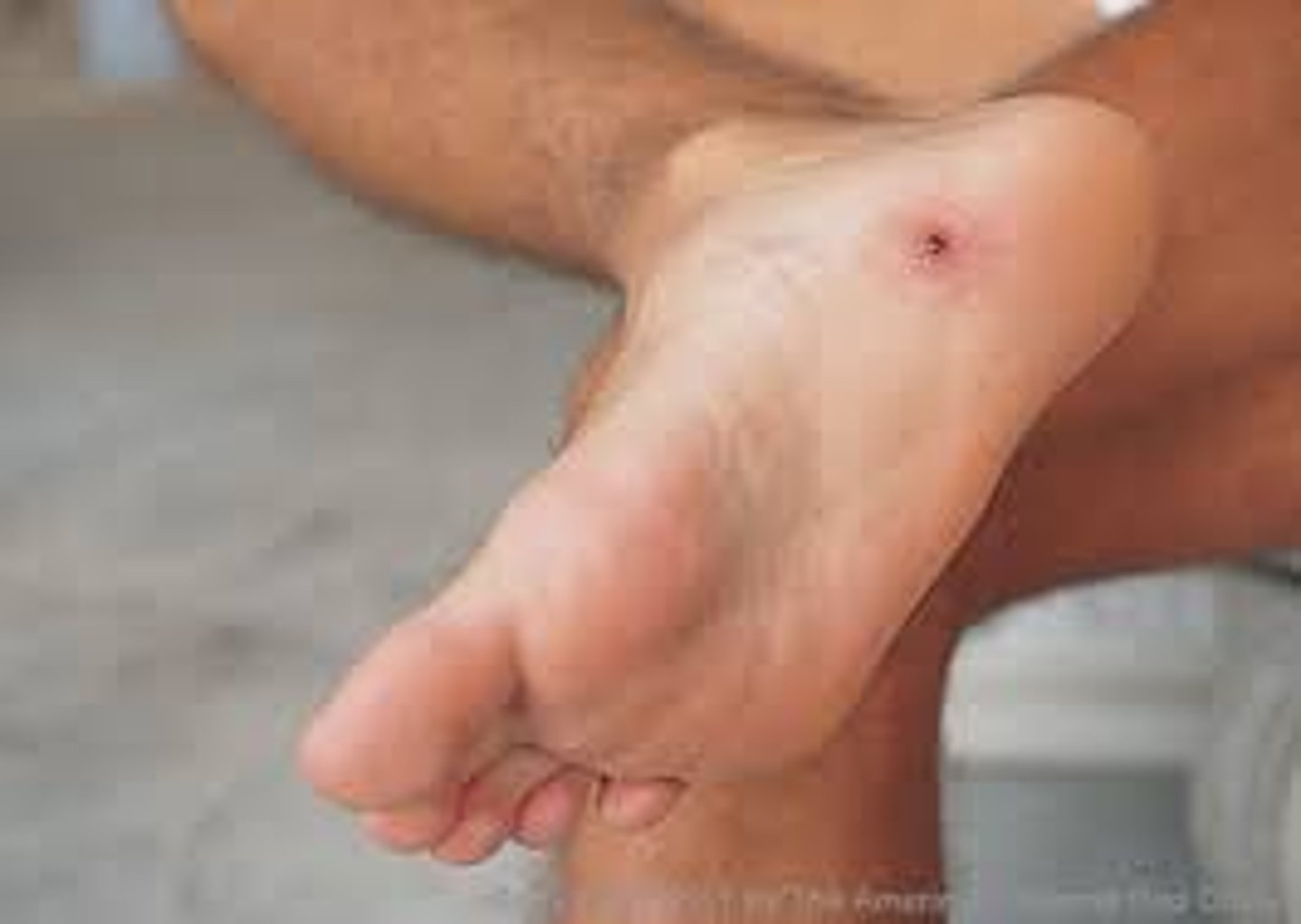
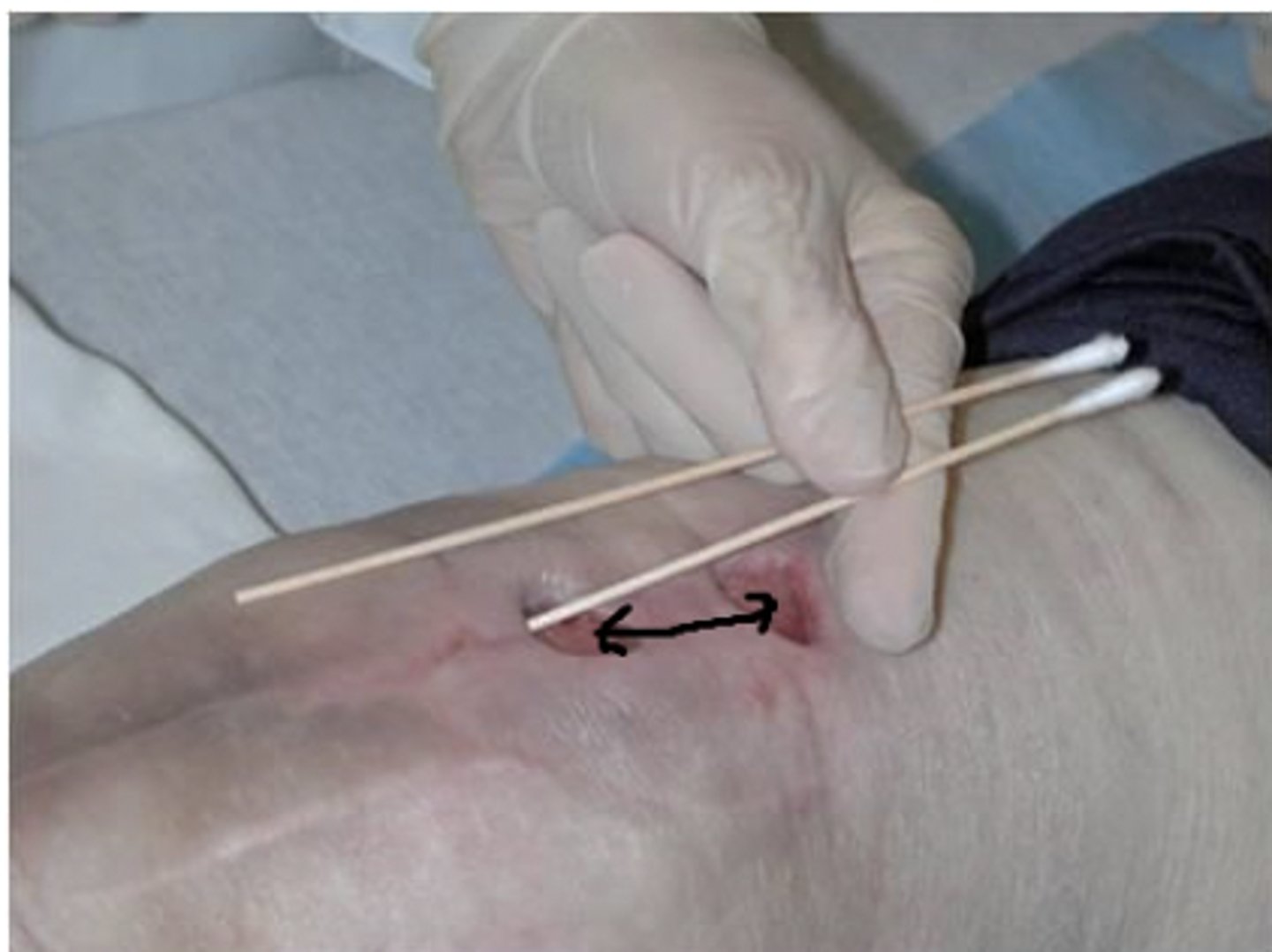
What is a tunnel wound?
a wound with an entrance and exit site
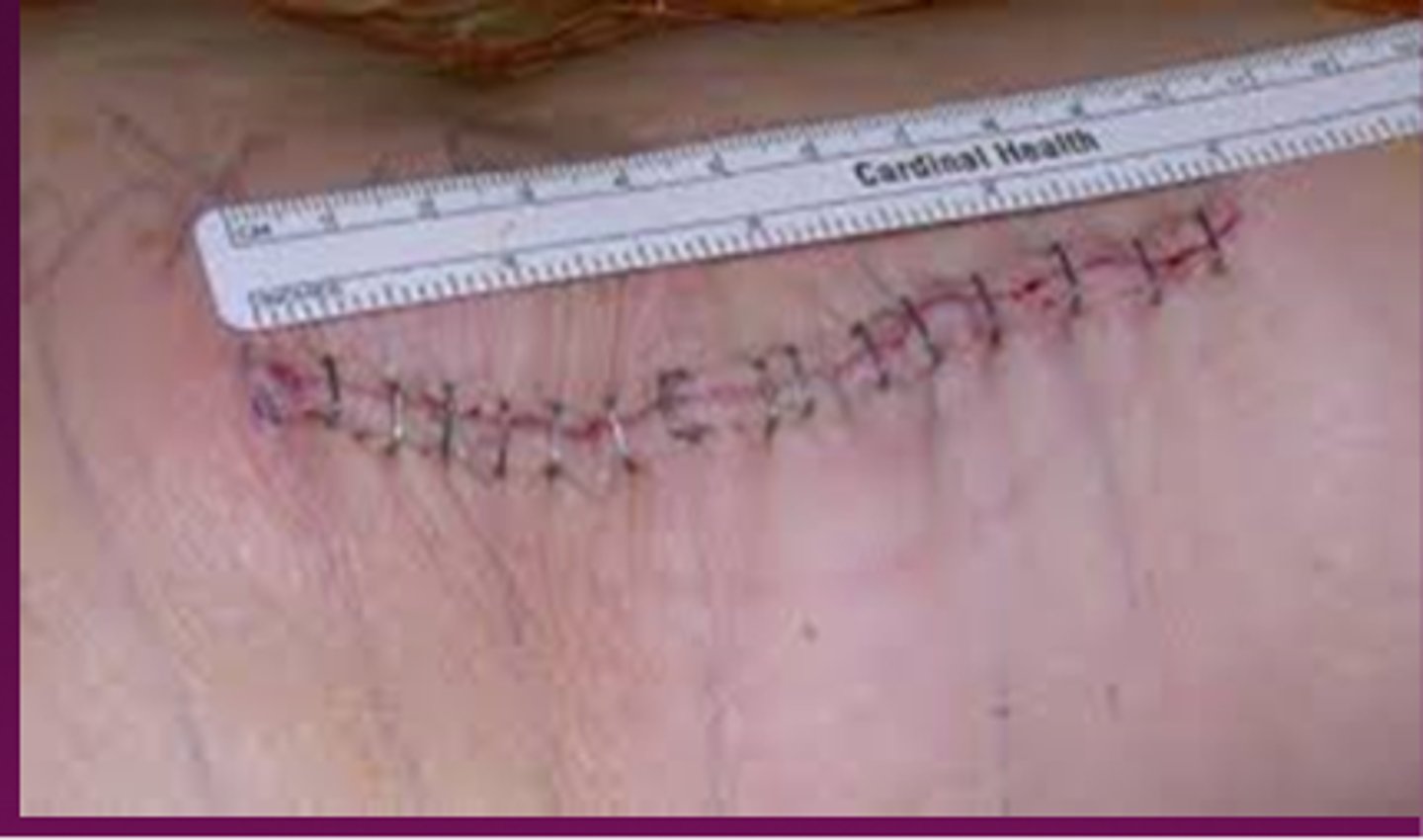
What is a primary wound?
wound that is closed with edges clean and intact ex: trauma or surgical incision
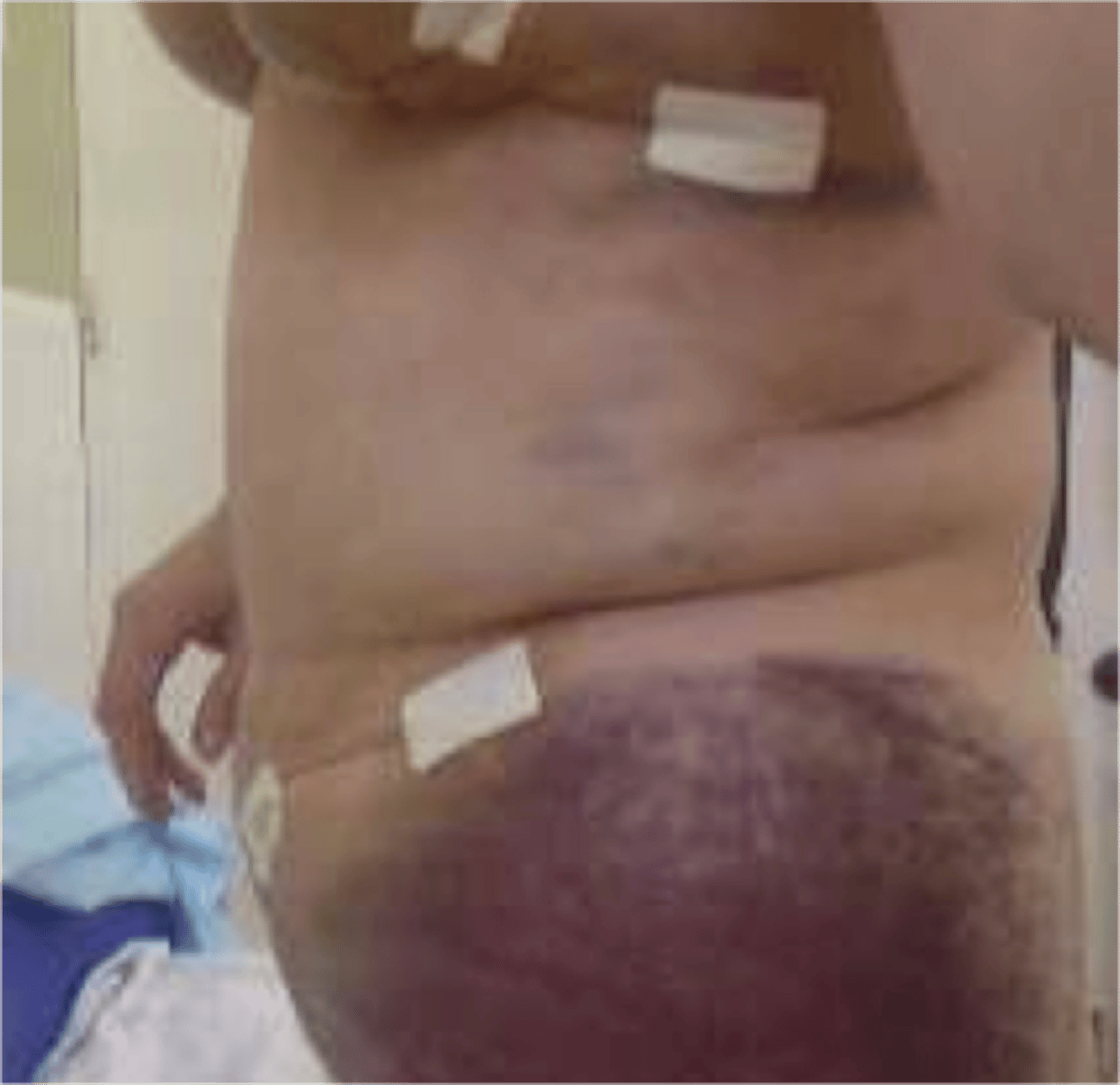
What is a secondary wound?
wound edges not approximated ex: surgical wounds that have tissue loss or contamination
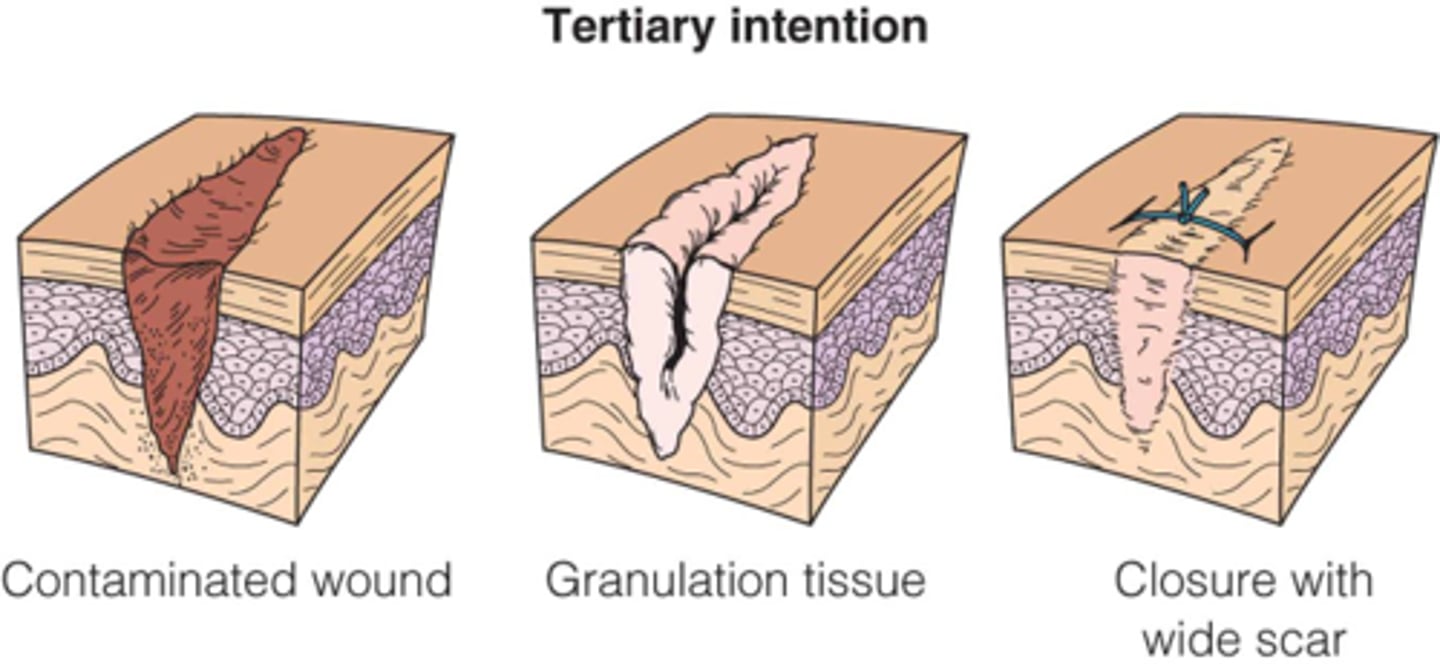
What is tertiary intention?
when a wound is allowed to remain open for a time and then closed, allowing for debridement and other wound care - to reduce bacterial counts prior to closure
Acute vs chronic injury
immediate injury caused by trauma vs an injury resulting from overuse caused by repetitive activity
Where do pressure ulcers typically occur?
Over bony prominences
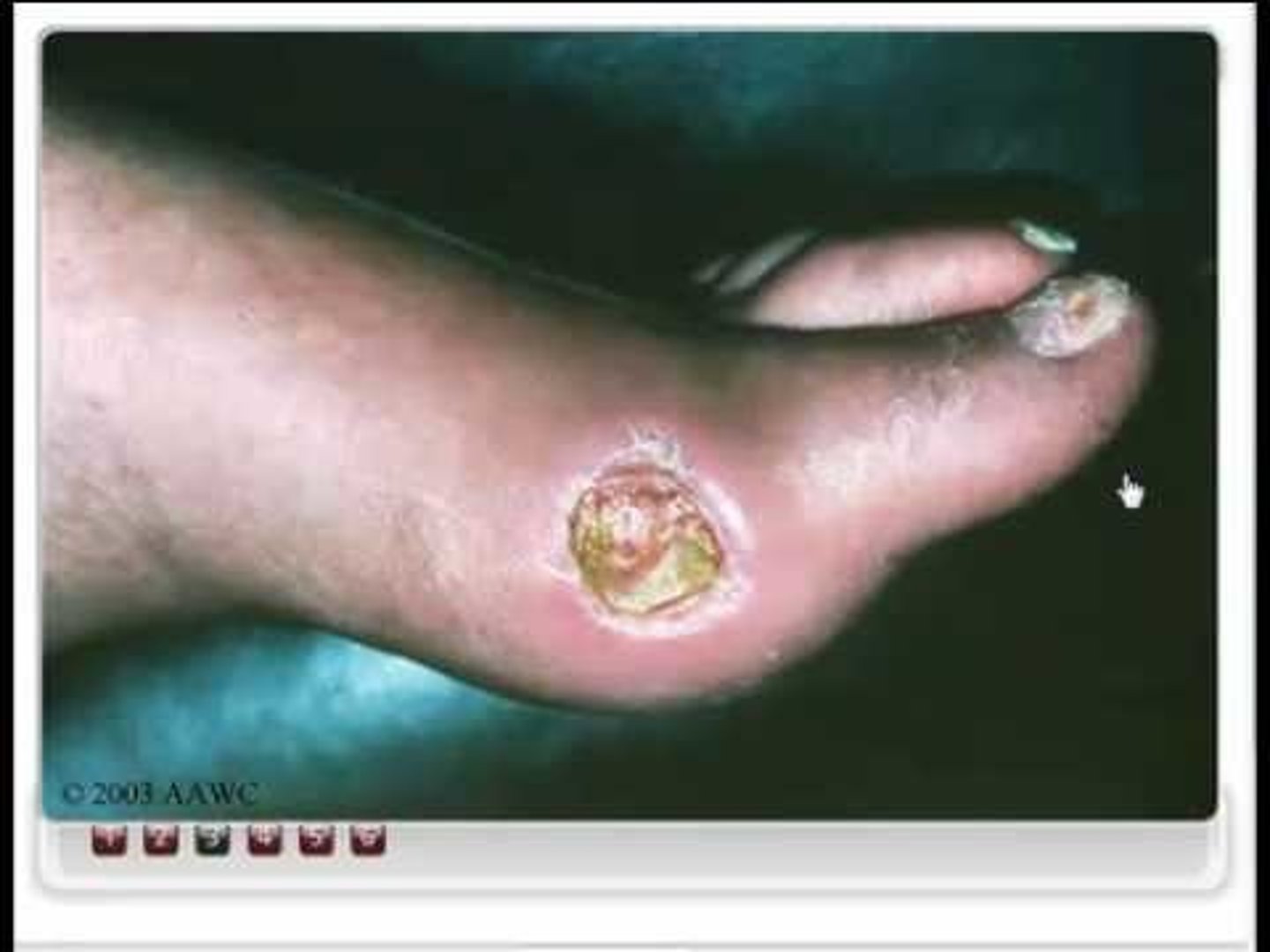
What is a diabetic foot ulcer?
Narrowing of the arteries, reduced oxygenation to the feet result in delayed wound healing and tissue necrosis.
Where do diabetic foot ulcers typically occur?
Plantar surfaces and toes (ball of foot and underside of toes)
What are arterial ulcers?
Ulcers occurring due to damage to the arteries caused by lack of blood flow to tissues.
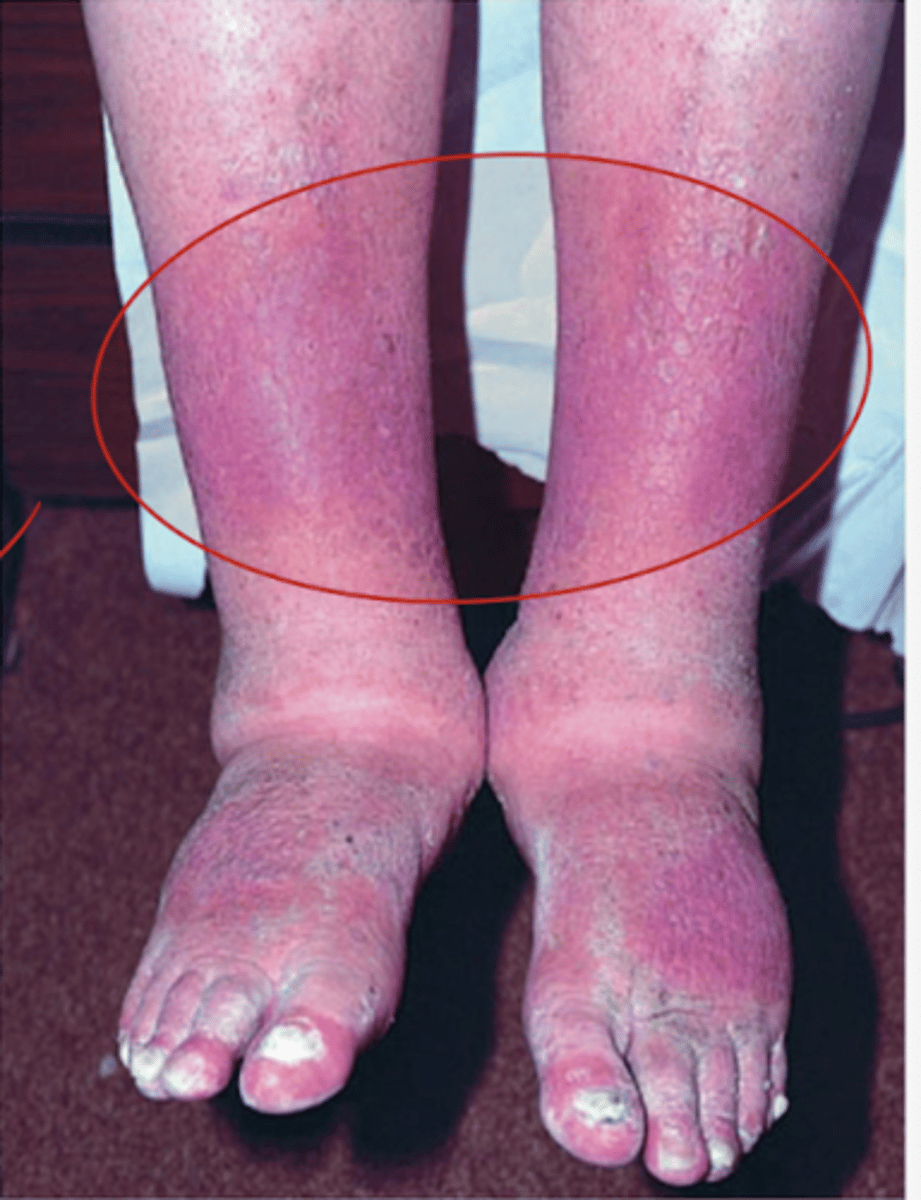
What are venous stasis ulcers?
found near lateral or medial malleolus assoc with lower extremity edema
Where does wound regeneration happen?
In epidermal wounds, leaves no scar
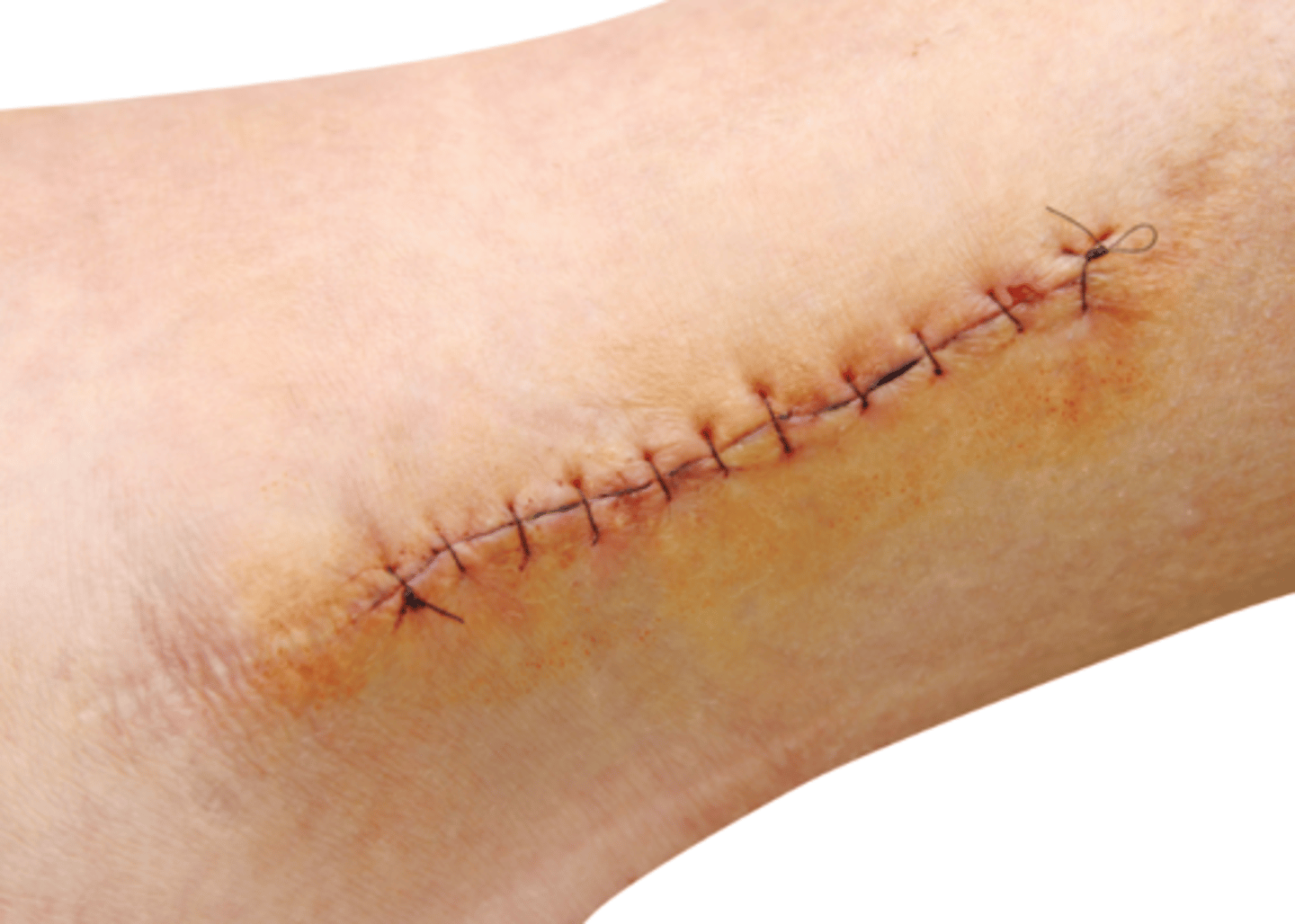
What is primary intention wound healing?
when the edges of a clean wound are closed in some manner immediately (i.e. suture, steri strips, staples)
What is secondary intention wound healing?
Wound margins are not well approximated; larger wound area requires the formation of granulation tissue to fill in the gap. A longer period of time is needed to heal.
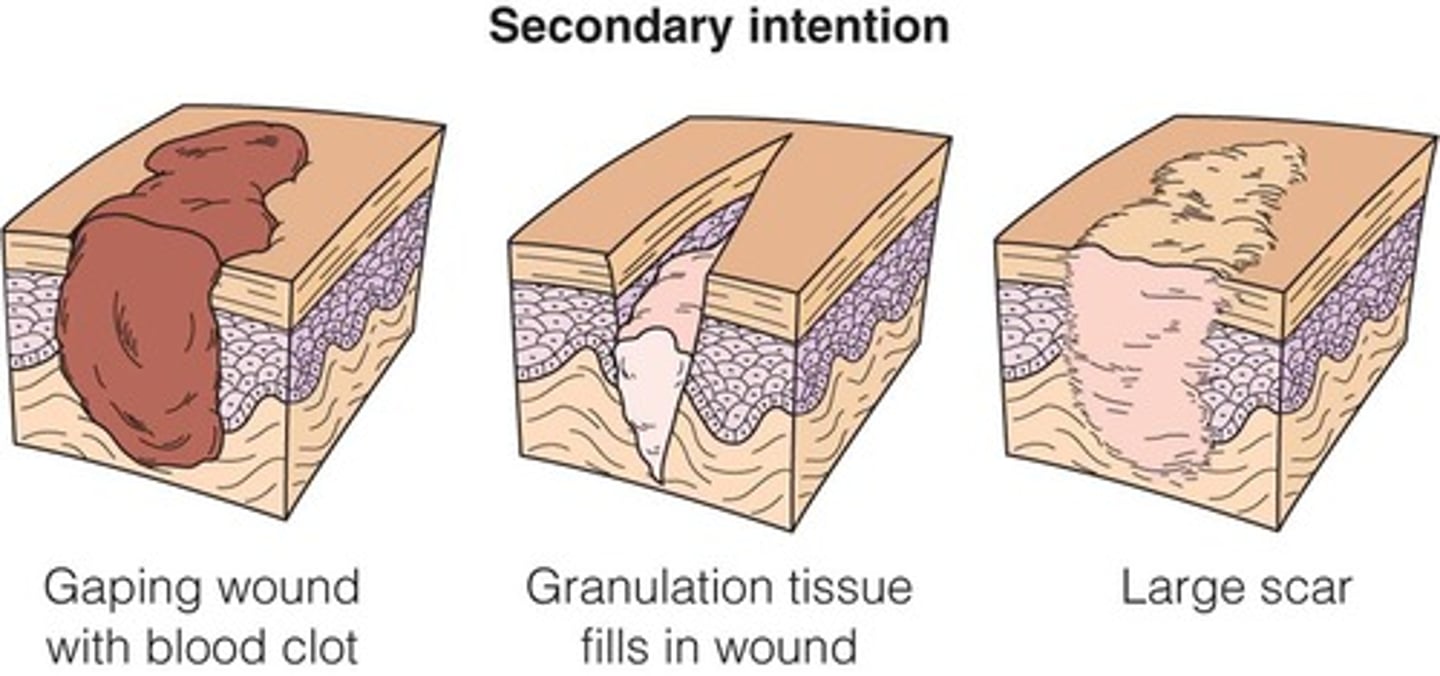
What is tertiary intention wound healing?
Wound healing is delayed and occurs when the wound that was previously open is now closed. This process is usually associated with large infected and contaminated wounds.
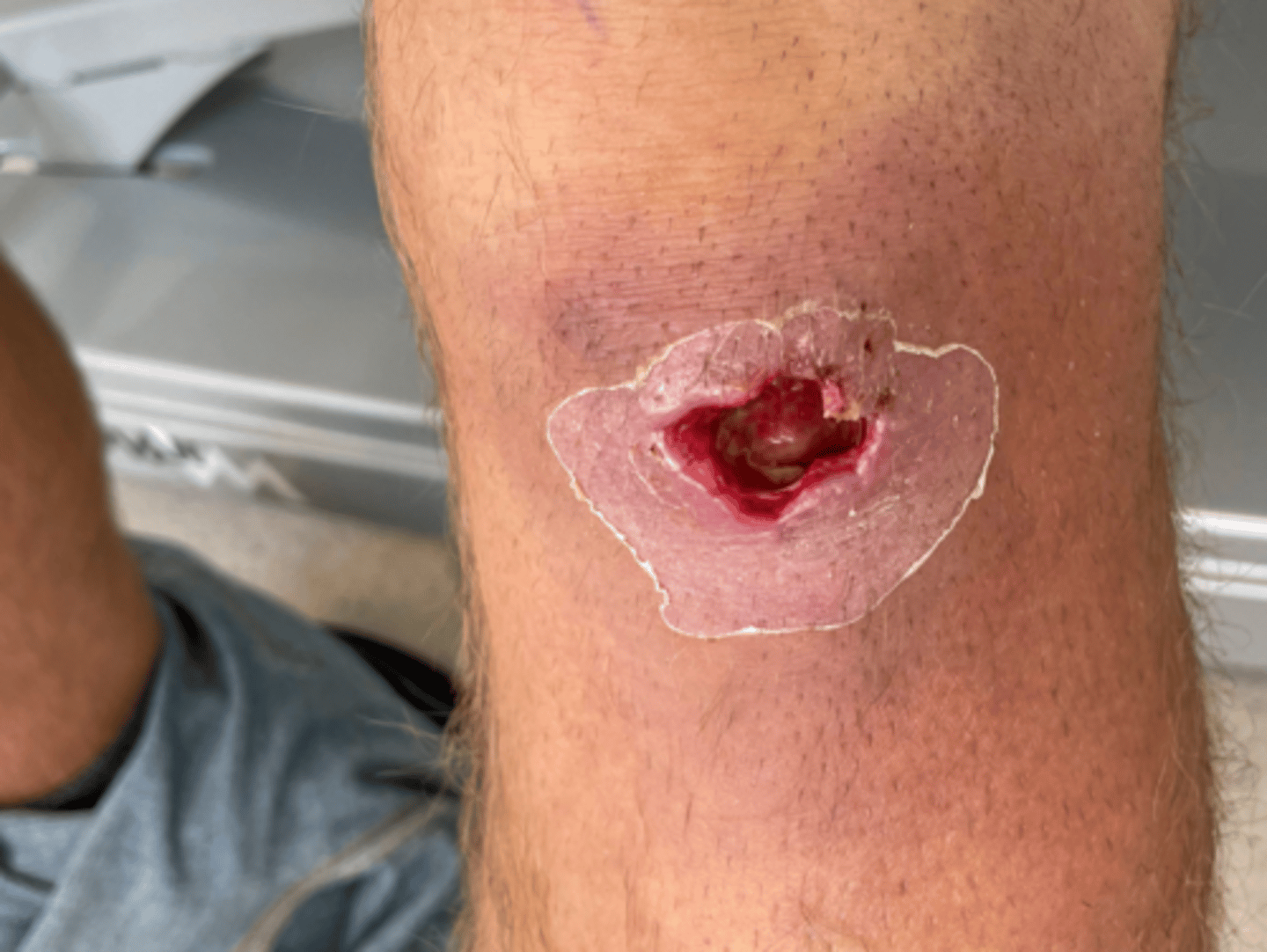
What are the 4 phases of wound healing?
1. Hemostasis
2. Inflammation
3. Proliferation
4. Maturation
What happens during the hemostasis phase of wound healing?
At the time of injury, tissue and capillaries are destroyed, causing blood and plasma to leak into the wound. Area vessels constrict to limit blood loss. Platelets aggregate (clump together) to slow bleeding. At the same time, the clotting mechanism is activated to form a blood clot.
What happens during the inflammatory phase of wound healing?
The inflammatory reaction is characterized by edema, erythema, pain, temperature elevation, and migration of white blood cells into the wound tissues. Within 24 hours, macrophages begin engulfing bacteria (phagocytosis) and clearing debris. Along with plasma proteins and fibrin, they form a scab on the wound surface, which seals the wound and helps prevent microbial invasion.
What happens during the proliferative phase of wound healing?
This phase occurs from days 5 to 21. Cells develop to fill the wound defect and resurface the skin. Fibroblasts (connective tissue cells) migrate to the wound where they form collagen, a protein substance that adds strength to the healing wound. New blood and lymph vessels sprout from the existing capillaries at the edge of the wound. The result is the formation of granulation tissue, a beefy red tissue that bleeds readily and is easily damaged. As the clot or scab is dissolved, epithelial cells begin to grow into the wound from surrounding healthy tissue and seal over the wound (epithelialization).
What happens during the tissue remodeling phase of wound healing?
This phase, also known as remodeling, is the final phase of the healing process. It begins in the second or third week and continues even after the wound has closed. Over the next 3 to 6 months, the initial collagen fibers that were laid in the wound bed during the proliferative phase are broken down and remodeled into an organized structure (e.g., scar tissue), increasing the tensile strength of the wound.
Partial-thickness wounds have how many stages of healing?
3
Full thickness wounds have how many stages of healing?
4
What are Steri-strips used for?
to reinforce a subcuticular skin closure, or to approximate wound edges of small incisions.
What are sutures used for?
bringing the edges of a wound together in order to speed wound healing and reduce scar formation
What are surgical staples used for?
Made of lightweight titanium, surgical staples provide a fast, easy way to close an incision. They are also associated with a lower risk of infection and tissue reaction than are sutures. The downside of staples is that some wound edges are more difficult to align. The most common sites for wound stapling are arms, legs, abdomen, back, scalp, or bowel. Wounds on the hands, feet, neck, or face should not be stapled.
What is surgical glue used for?
safe for use in clean, low-tension wounds. It is an ideal wound closure method for skin tears
What is serous exudate?
Watery exudate: indicates early inflammation
What is sanguineous exudate?
bloody drainage
What is serosanguineous exudate?
Pale, pink, watery; mixture of clear and red fluid
What is purulent exudate?
Pus: indicates a bacterial infection
What is purosanguineous exudate?
red tinged pus
What is wound hemorrhage?
slipped suture, dislodged clot at wound site, infection, or the erosion of a blood vessel by foreign body
if its internal a hematoma is formed
What is wound infection?
infection in operative wound
What is wound dehiscence?
Disruption of previously joined wound edges due to an infection, too tight sutures, or injury to wound
What is wound evisceration?
protrusion of internal organs thru the wall of an incision. placing them in low fowlers with the knees bent helps reduce the tension on the wound
What is a wound fistula?
abnormal passage connecting two body cavities or a cavity and the skin. Fistulas often result from infection. An abscess forms, which breaks down surrounding tissue and creates the abnormal passageway. Chronic drainage from the fistula may lead to skin breakdown and delayed wound healing. The most common sites where fistulas form are the gastrointestinal and genitourinary tracts.
What is the Braden scale?
an evidence-based tool that looks at various factors that put patients at risk for developing a pressure ulcer. Includes:
sensory perception
moisture
activity
mobility
nutrition
friction
shear
A score of below... is at risk for injury. A score of below... is at very high risk for injury.
<16 indicates "at risk"
<9 indicates "very high risk"
What are the most common laboratory assessments related to skin integrity?
- Protein levels
- CBC
- ESR
- Glcuose
- Thyroid
- Iron
What is wound swabbing?
The most common and most noninvasive method to obtain a culture is with a swab. Swab specimens have been shown to be acceptably accurate in representing bacteria counts biopsied from a wound.
What is needle aspiration?
involves insertion of a needle into the tissue to aspirate tissue fluid. Organisms present in the tissue fluid can then be detected. Needle aspiration is an invasive procedure.
What is tissue biopsy?
Different type such as punch, incision, excision, and shave. When skin lesions are suspected to be malignant
The nursing diagnosis: "Impaired Skin Integrity" is appropriate for patients who have experienced damage to the ..?
- Epidermis or Dermis
- Stage 1 or 2 Pressure injury
The nursing diagnosis: "Impaired Tissue Integrity" is appropriate for patients who have experienced damage to the ..?
- SQ Tissue, muscle, bone
- Stage 3 or 4 Pressure Injury
What is a JP drain?
Jackson Pratt
Closed drainage system attached to a suction bulb
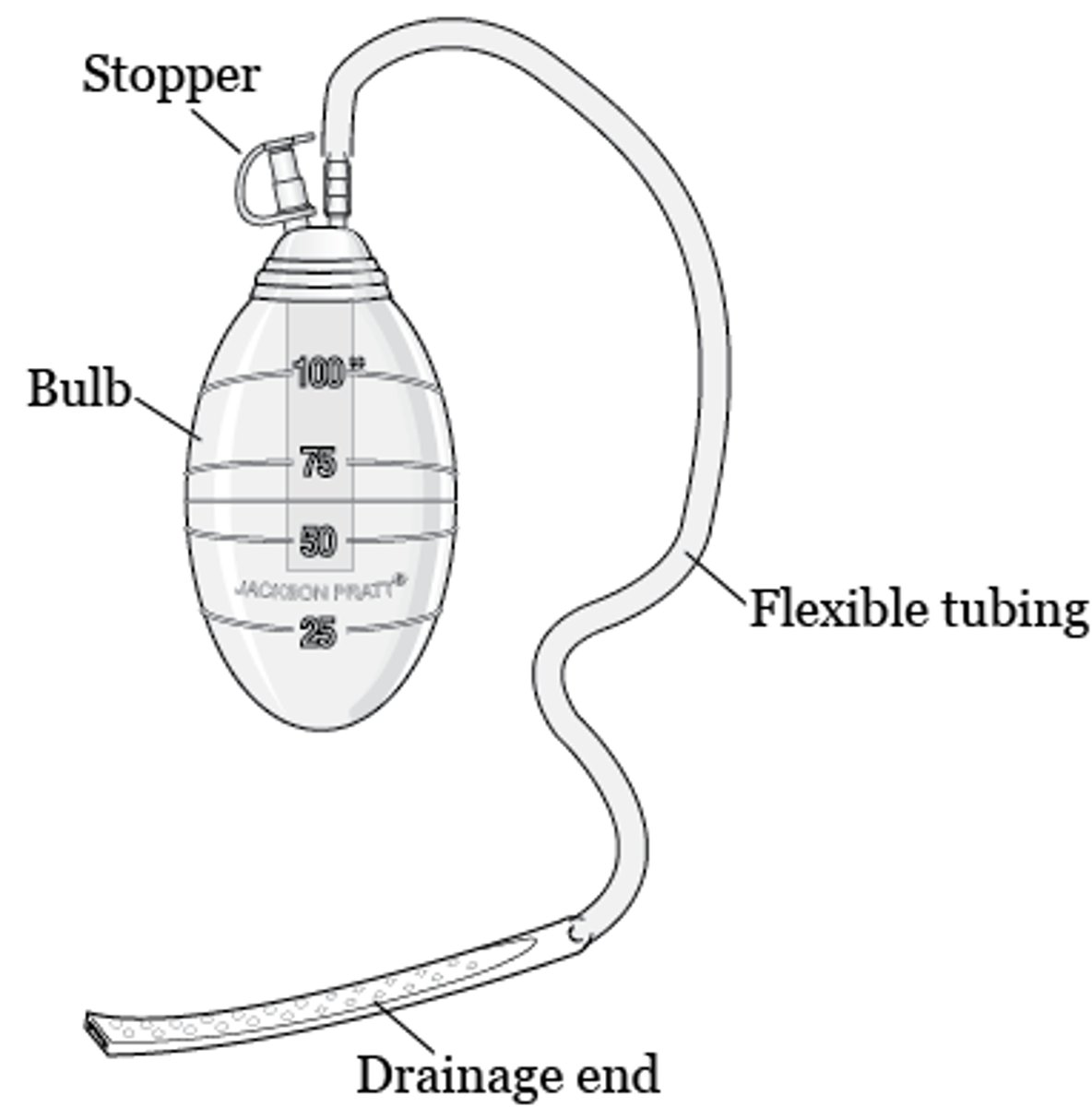
What is debriding a wound?
•the removal of devitalized tissue or foreign material from a wound.
It also helps remove cells that are alive but not functioning (senescent) from the wound bed and edges.
important because Removal of necrotic tissue, exudate, and infective material helps stimulate wound healing and prepare the wound bed for advanced therapies or biological agents.
ways to debrid: sharp, mechanical, enzymatic, autolysis, biotherapy
What is sharp debriding?
is the use of a sharp, sterile instrument, such as scalpel or scissors, to remove devitalized tissue. This method provides an immediate improvement of the wound bed and preserves granulation tissue
What is mechanical debridement?
done with wet-to-dry saline dressing placed in the wound that absorbed necrotic tissue and is allowed to dry
What is enzymatic debridement?
chemical debridement in which enzymes are used to break down necrotic tissue without targeting viable tissue
What is autolysis debridement?
debriding is the use of an occlusive, moisture-retaining dressing and the body's own enzymes and defense mechanisms to break down necrotic tissue. This process takes more time than the other techniques, but it is tolerated better
Do you cover an active area of bleeding with a warm application?
No! Bleeding will continue and possibly get worse! Contraindication!
What is the contraindication to cold therapy?
If the site of injury is edematous. The cold could FURTHER retard circulation to the area and prevent the absorption of the interstitial fluid.
Pressure injuries affect what % of hospitaloized clients?
15%
What are some intrinsic factors of pressure injury development?
- Immobility
- Impaired sensation
- Poor nutrition
- Dehydration
- Aging
- Fever, infection
- Edema
What are some extrinsic factors of pressure injury development?
- Friction
- Pressure
- Shearing
- Moisture
Compare friction and shear
Friction is the rubbing of two surfaces against one another.
Shear is a combination of friction and gravity that can compress vessels and skin and cause breakdown.
What is hyperemia?
increased blood flow
What is reactive hyperemia?
Increased blood flow to an organ in response to a period of reduced blood flow
What is blanching hyperemia?
press finger over affected area --> skin turns lighter in color --> removal of finger --> redness present
Do you massage bony prominences?
NEVER!
What is protective positioning?
intentionally arranging a patient's body to ensure safety, comfort, and clinical benefit, such as improving oxygenation or preventing skin breakdown.
How do you measure the depth of a pressure injury?
By using a sterile, saline moistened, cotton tipped applicator.
What is the ABCDE skin assessment?
A: Asymmetry
B: border irregularity
C: color variegation
D: diameter greater than 6mm
E: evolving changes