SelfCare: Ophthalmic, Otic, & Oral (Exam I)
1/108
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
109 Terms
dry eye
multifactorial disease of the ocular surface characterized by a loss of homeostasis of the tear film, and accompanied by ocular symptoms, in which tear film instability and hyperosmolarity, ocular surface inflammation and damage, and neurosensory abnormalities play etiological roles
tears
those with dry eye experiences either decreased production of ______, or increased evaporation of ocular lubrication
humidity
common exacerbating environmental factors of dry eye can be dry or dusty environment, heating/AC, or reduced ______
beta blockers
drugs that can cause dry eye are antihistamines, decongestants, diuretics, and _______
ocular
when patients present to the pharmacy to treat dry dry eye, it can be characterized as a normal appearing sclera or mildly red eye, patient may complain of a sandy or gritty feeling or feeling of something is in the eye, and/or there is potential initial presentation of excessive tearing: dry eye can lead to _____ tissue damage if untreated so it is important we treat patients when they come to the pharmacy with their concerns
tissue damage
the treatment goals of dry eye is to alleviate dryness of the ocular surface, relieve symptoms of irritation, and prevent possible corneal and noncorneal _______
eye pain
exclusions for treating those with dry eye include if the patient is experiencing ______, blurred vision not associated with use of ophthalmic ointments, or sensitivity to light
contact lens
exclusions for treating those with dry eye include if the patient has a history of ________ wear, blunt trauma to the eye, or any chemical exposure affecting the eye
72
exclusions for treating those with dry eye include if the patient's eye has been exposed to heat excluding sun exposure, or if symptoms have persisted for longer than ____ hours
lubricants
the general treatment approach for dry eye is ocular ______ and nonpharmacy recommendations like removing themselves from dry conditions, not sleeping with fan directly in face, etc.
low
if the patient is experiencing mild discomfort dry eye symptoms, we will recommend ____ viscosity artificial tears 1-2 times a day (follow up in 1 week)
high
if the patient is experiencing moderate discomfort dry eye symptoms, we will recommend low viscosity artificial tears 3-4 times a day OR a _____ viscosity solution (follow up in 1 week)
preservative-free (PF)
if the patient is experiencing severe discomfort dry eye symptoms, we will recommend _____ artificial tears every hour as needed AND a night time eye ointment (follow up in 1 week)
evaporation
nonpharmacologic therapy to treating dry eye includes avoidance of environments that promote _______ of tear film: to do this you can use a humidifier or reposition work areas away from air vents
computer screens
nonpharmacologic therapy to treating dry eye includes avoiding prolonged use of _______ or the use of eye protection in windy outdoor environments
warm
nonpharmacologic therapy to treating dry eye includes eyelid function improvement like applying a ____ compress, discontinuing offending agent, and maintaining good eyelid hygiene
dietary
nonpharmacologic therapy to treating dry eye includes ______ modification: omega-3 oils and flaxseed oils can be used as supplements
less
the less viscous a pharmacologic therapy is, the _____ contact time it will have with the eye
more
the more viscous a pharmacologic therapy is, the ______ contact time it will have with the eye
solution
is the dosage form of artificial tears that has the shortest contact time but causes the smallest amount of blurred vision
gel
is the dosage form of artificial tears that has the second shortest contact time but causes the second smallest amount of blurred vision
ointment
is the dosage form of artificial tears that has the longest contact time but causes the largest amount of blurred vision
suspension
if your eye drop is in the form of a _______, you must shake before use
5
if you are combining multiple eye drop solutions, you should wait at least ____ minutes before instilling the next drop combination of drops and ointments
10
if you are combining multiple eye drop ointments, you should instill the drops at least ____ minutes before the ointment: if you add drops after ointments, the drop would never reach the sclera due to the ointment acting as a protective agent
pouch
when administrating an eye drop, you should look up to the ceiling and pull down on the lower eyelid with the non-dominant hand to create a _____, then instill the drop with your dominant hand
blink tears
Active Ingredient: Polyethylene Glycol 400 0.25% — acts as an eye lubricant to hydrate and soothe dry eyes.
Use: For temporary relief of burning, irritation, and discomfort due to dry eyes or exposure to wind/sun; helps protect the eye surface from further irritation by restoring tear balance.
Refresh Optive - Preservative Free
Active Ingredients: Carboxymethylcellulose Sodium (0.5%) and Glycerin (0.9%) — both act as eye lubricants to moisturize and relieve dryness.
Use: Temporarily relieves burning, irritation, and discomfort due to dryness; helps protect against further irritation.
NO Preservative: without preservatives, it's gentler and safer for frequent or daily use, especially for sensitive eyes or after surgery
Sooth Allergy + Dry Eye
Active Ingredients: Ectoine 2% (protects cells and may reduce allergic inflammation) and Sodium Hyaluronate 0.24% (a natural lubricant to hydrate the eye surface).
Use: For relief of dry eye symptoms and allergy-related irritation — soothes dryness while helping protect against allergens that can cause inflammation and discomfort.
Refresh Optive
Active Ingredients: Carboxymethylcellulose Sodium (0.5%) and Glycerin (0.9%) — both act as eye lubricants to moisturize and relieve dryness.
Use: Temporarily relieves burning, irritation, and discomfort due to dryness; helps protect against further irritation.
Preservative: Some multi-dose bottles contain preservatives like Purite® or benzalkonium chloride (BAK) — gentler options exist and may be better for sensitive eyes, but PF is preferred for frequent use.
preservative-free (PF)
_______ ophthalmic agents have a higher risk of contamination and must be packaged as single use products
Benzalkonium chloride (BAK)
common ophthalmic preservative: for long-term use associated with conjunctival and corneal damage
Mercury
common ophthalmic preservative: patients who become sensitized to thimerosal can develop contact blepharitis or conjunctivitis after several weeks of exposure and must discontinue the use of products that contain this ingredient
Chlorobutanol
common ophthalmic preservative that is less effective than BAK as an antimicrobial preservative: breaks down in bottles with prolonged storage
P-hydroxybenzoic acid derivatives
common ophthalmic preservative like Methylparaben and Propylparaben: is unstable at high pH and can induce allergic reactions
Sodium perborate (GenAqua)
common ophthalmic preservative: disappearing preservative (dissociates to hydrogen peroxide which rapidly dissociates to oxygen and water), amount of hydrogen peroxide formed is so small that it does not cause irritation
Stabilized oxychloro complex
common ophthalmic preservative like Purite and OcuPure: another disappearing preservative (breaks down to water and sodium chloride with UV exposure)
allergens
common _____ of allergic conjunctivitis are pollen, animal dander, and topical eye preparations: clinical presentation includes red eye, watery discharge, pruritis, and may also present with seasonal allergic rhinitis
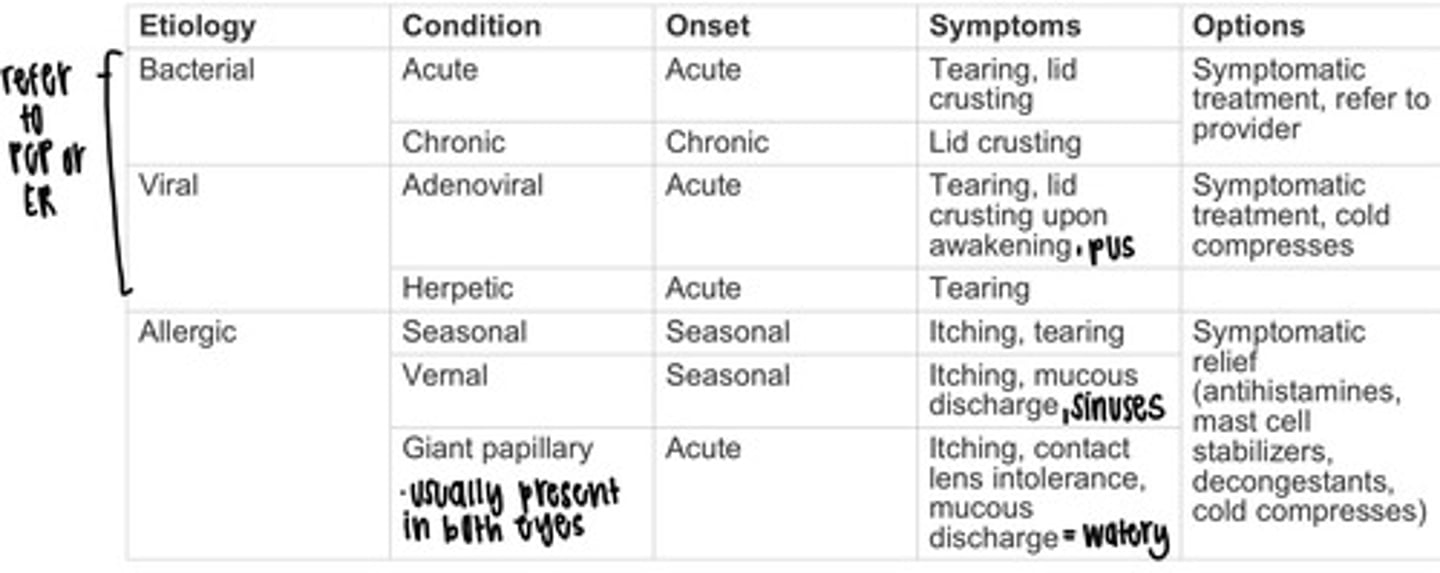
symptomatic relief
treatment goals of allergic conjunctivitis is to remove or avoid the allergen, limit or reduct the severity of the allergic reaction, provide _______, and to protect the ocular suface
cold
nonpharmacologic therapy for treating allergic conjunctivitis includes allergy removal/avoidance (check pollen count, keep doors/windows closed, hypoallergenic bedding, wash clothes frequently, bathing before bedtime, use of air filters, wear sunglasses), ______ compress application 3-4x a day, and removal of contact lenses until symptom resolution
artificial tears
the first line pharmacologic treatment for treating allergic conjunctivitis is ________
antihistamine
the next consideration pharmacologic treatment for treating allergic conjunctivitis is ophthalmic ______ or mast cell stabilizer
decongestant
to reduce redness in allergic conjunctivitis, and ophthalmic ______ or alpha-adrenergic agonists should be recommended
oral
if systemic allergic symptoms are presents, an _____ antihistamine may be considered for treating allergic conjunctivitis
72
you should refer a patient with allergic conjunctivitis to their PCP if symptoms have not been relieved after _____ hours of therapy
Zaditor
ophthalmic antihistamine/mast cell stabilizer thats; active ingredient is Ketotifen 0.025% and should be used for ages 3 and up: 1-2 drops every 8-12 hours
Pataday Once Daily Relief Extra Strength
ophthalmic antihistamine/mast cell stabilizer thats; active ingredient is Olopatadine 0.7% for ages 2 and up: 1 drop every 24 hours
Pataday Once Daily Relief Original Strength
ophthalmic antihistamine/mast cell stabilizer thats; active ingredient is Olopatadine 0.2%: 1 drop every 24 hours
Pataday Twice Daily Relief
ophthalmic antihistamine/mast cell stabilizer thats active ingredient is Olopatatdine 0.1%: 1 drop every 12 hours
vasoconstriction
the general mechanism of action of ophthalmic decongestants/alpha-adrenergic agonists is to reduce redness via _________: it does not address allergic responses!!
hypertension
ophthalmic decongestants/alpha-adrenergic agonists agents are used in cautions in patients with _______, arteriosclerosis, cardiovascular disease, diabetes, or hyperthyroidism
72
except for Brimonidine, decongestants should not be used for more than _____ hours due to rebound congestion
Brimonidine
______ is a decongestant that may be used for up to 4 weeks due to minimal rebound congestion
rebound congestion
_____ is less likely with the use of naphazoline or tetrahydrozoline as compared to oxymetazoline or phenylephrine
Clear Eyes Redness Relief
ophthalmic decongestants/alpha-adrenergic agonists thats active ingredient is Naphazoline 0.012%: 1-2 drops up to 4 times a day
Lumify
ophthalmic decongestants/alpha-adrenergic agonists thats active ingredient is Brimonidine tartrate 0.025%: 1 drops every 6 to 8 hours up to 4 times a day
Visine Advanced Redness + Irritation Relief
ophthalmic decongestants/alpha-adrenergic agonists thats active ingredient is Tetrahydrozoline HCl 0.05%: 1-2 drops every 4 hours
Visine A
antihistamine + decongestant eye drop thats active ingredient is Pheniramine maleate 0.3% & Naphazoline HCl 0.025%: 1-2 drops 3-4 times a day
ocular irrigant
if loose foreign substances enter the eye, remove the foreign substance with an ______: if unavailable, flush with copious amounts of water
refer
we should _____ a patient if foreign substance is a fragment of wood or metal, if substance is not removed by irrigation, or if there is pain, changes in vision, continued redness, or worsening of condition after irrigation
tooth hypersensitivity
experiences of oral pain from hot, cold, sweet, sour, and/or spicy foods: pain can range from mild discomfort to sharp, excruciating pain
toothpaste
the goals of therapy for treating tooth hypersensitivity is to repair the damaged tooth surface using appropriate ______ and to replace aggressive or improper toothbrushing practices with optimal technique
toothache
exclusions for treating a patient presenting with tooth hypersensitivity is if they are experiencing a _______, mouth soreness associated with poor fitting dentures, presence of fever or swelling, loose teeth, bleeding gums in the absence of trauma, broken or knocked out teeth, severe tooth pain triggered or worsened by hot, cold, or chewing, and/or trauma to the mouth with bleeding, swelling, and soreness
soft-bristled
one general treatment approach for tooth hypersensitivity is the use of a ______ toothbrush and standard toothpaste with fluoride then follow up in 7 days
desensitizing
another general treatment approach for tooth hypersensitivity is twice daily use of _______ toothpaste with a soft-bristled toothbrush then follow up in 14 days: if unresolved after day 14, a dental referral is required
acidic
nonpharmacologic therapy for treating tooth hypersensitivity includes avoiding aggressive brushing, avoiding brushing within 30-60 minutes of consuming _____ foods, and to use a soft-bristled toothbrush
potassium nitrate & sodium fluoride
pharmacologic therapy for treating tooth hypersensitivity includes desensitizing toothpastes containing ______, and avoidance of abrasive toothpaste (ex: whitening, stain removal)
Colgate Sensitive
Toothpaste designed to relieve tooth sensitivity by helping block exposed dentin tubules and protecting nerves from triggers like cold, heat, sweets, or brushing. Often contains potassium nitrate or stannous fluoride to reduce sensitivity while also preventing cavities and strengthening enamel.
Sensodyne Pronamel
Toothpaste specifically formulated for sensitive teeth that also helps strengthen and protect enamel from acid erosion. Uses fluoride to remineralize enamel while providing gentle sensitivity relief, making it useful for people with acid-related enamel wear and tooth sensitivity.
recurrent aphthous stomatitis (RAS)
painful epithelial ulcer or mucosa of the mouth also known as canker sores: round or val, flat or with a depressed center, gray or yellowish gray, cannot be cured (symptom relief only)
10-14
most cases of recurrent aphthous stomatitis (RAS) peak onset is 10-19 years of age and may spontaneously resolve after _____ days: though to be primarily idiopathic
secondary infections
the treatment goals of recurrent aphthous stomatitis (RAS) is to relieve pain and irritation to enable lesion healing and prevention of complications such as _______
14
exclusions for self treatment of recurrent aphthous stomatitis (RAS) is if the lesions are associated with underlying pathology, if lesions are present for more than _____ days, if the patient has frequently systemic illness, symptoms of systemic illness, and/or failure of prior appropriate self-treatment
vitamin supplement
nonpharmacologic treatment for treating recurrent aphthous stomatitis (RAS) includes a ______ if cause if vitamin deficiency (iron, folate, B12), avoid spicy or acidic food, avoid sharp textured food, and applying ice in 10 minute increments, but no more than 20 minutes per hour
oral debriding
the 1st line pharmacologic treatment for treating recurrent aphthous stomatitis (RAS) is using _____ and wound-cleaning agents
Hydrogen peroxide
oral debriding and wound-cleaning agent pharmacologic treatment for treating recurrent aphthous stomatitis (RAS): mix with an equal amount of water before rinsing for at least 1 minute
Carbamide peroxide
oral debriding and wound-cleaning agent pharmacologic treatment for treating recurrent aphthous stomatitis (RAS): place a few drops on the tongue, mix with saliva, and swish in the mouth for 1 minute
7
the max duration of oral debriding and wound-cleaning agent pharmacologic treatment for treating recurrent aphthous stomatitis (RAS) therapy is _____ days: it can result in transient tooth sensitivity due to decalcification of enamel
3
when using oral debriding and wound-cleaning agent pharmacologic treatment for treating recurrent aphthous stomatitis (RAS), use after meals, avoid eating or drinking for at least ____ minutes, and do not swallow
topical oral anesthetics
pharmacologic treatment for treating recurrent aphthous stomatitis (RAS) includes _______ like benzocaine and benzyl alcohol for ages 2 and up
topical oral protectants
pharmacologic treatment for treating recurrent aphthous stomatitis (RAS) includes ________ like denture adhesive used to coat and protect the ulcerated area and patches are also available
oral rinses
pharmacologic treatment for treating recurrent aphthous stomatitis (RAS) includes _____ like saline rinse (1-3 teaspoons of salt in 4-8 ounces of warm tap water then swish & spit), and listerine
systemic analegsics
pharmacologic treatment for treating recurrent aphthous stomatitis (RAS) includes ______ like NSAIDs or acetaminophen but in appropriate dosage form (no powders)
7
you should refer a patient presenting with recurrent aphthous stomatitis (RAS) when lack of resolution after ____ days of therapy, canker sores are present for more than 14 days from initial presentation, and/or if there are signs of systemic infection
Herpes Simplex Labialis (HSL)
caused from the Herpes Simplex Virus (HSV) commonly called the cold sore
prodromal phase
the _____ of Herpes Simplex Labialis (HSL) is 2-48 hours prior to lesion appearance: burning, itching, numbness is common presentation and other potential symptoms at this stage includes pain, fever, localized bleeding, swollen lymph nodes, and malaise
transmission
treatment goals for Herpes Simplex Labialis (HSL) is to relieve pain and irritation while wounds are healing, prevent secondary infections, and to minimize _______
14
exclusions for self-treatment is if the lesions are present for more than _____ days, increased frequency of outbreaks (may need to be prescribed anti-viral over any OTC medications), immunocompromised, symptoms of infections, no previous diagnosis of cold sore, and/or frequency recurrence
moisturizing
nonpharmacologic therapy for Herpes Simplex Labialis (HSL) is handwashing and _____
Docosanol 10% (Abreva)
only FDA-approved OTC product for cold sores: reduces severity and duration of symptoms, only improves healing time by 1 day, inhibits direct fusion between the herpes virus and the human cell plasma membrane preventing viral replication, apply at first sign of outbreak 5 times per day for a max of 10 days
Oragel
topical anesthetic that can also be used to treat Herpes Simplex Labialis (HSL): follow up in 14 days
Xerostomia
dry mouth
loose teeth
exclusions for self-treatment of xerostomia is tooth erosion and decay, candidiasis, gingivitis, periodontitis, reduced denture-wearing time, mouth soreness associated with poor-fitting dentures, presence of fever or swelling, ______, bleeding gums in absence of trauma, broken or knocked-out teeth, severe tooth pain triggered by hot cold, or chewing, trauma to the mouth, Sjogren's syndrome, and/or salivary gland stones
salivary flow
a nonpharmacologic treatment for xerostomia is to help prevent a reduction in _______ by avoiding the use of cigarettes and smokeless tobacco and not drinking or using products that contain alcohol (including mouth rinses) or medications that cause depletion of salivary flow
caffeine
a nonpharmacologic treatment for xerostomia is to avoid food or drinks that contain _____, avoid hot spicy foods, limit consumption of sugary, starchy, and acidic foods: do not suck on hard candy or lozenges sweetened with sugar, if desired chew gum sweetened with sugar alcohol such as xylitol to help increase flow of saliva
fluoridated
a nonpharmacologic treatment for xerostomia is if possible take medications 1 hour before meals so that the natural saliva flow caused by food can counteract any mouth dryness, use a very soft toothbrush to reduce abrasion of the teeth, drink plenty of water especially if it is ______, and/or to use a cool mist humidifier at home to help moisten the air
carboxymethyl or hydroxyethylcellulose
pharmacologic therapy by xerostomia includes artificial saliva with active ingredients of _______: not a cure, only provide replacement therapy and use as needed
sugarless gum
dental hygiene counseling points include: brush at least twice daily, floss at least once daily, replace toothbrushes at least every 3 months, chewing _____ for 20 minutes after meals decreasing tooth decay by increasing saliva, toothpastes containing baking soda, brush with mildly abrasive toothpaste and soft-brush toothbrush to minimize enamel erosion, and/or supervise children under the age of 12 when using fluroride-containing products to minimize swallowing
excessive or impacted cerumen (EOC)
commonly called ear wax: function is to clean, protect, and lubricate the external auditory canal (EAC)
removed
a common myth about excessive or impacted cerumen (EOC) or ear wax is that is should be _______: inappropriate removal can push wax deeper into the ear, damage the EAC or tympanic membranes, and can potentially result in otitis media