Test 1 Physiology
1/291
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
292 Terms
Net charge of the inside of a neuron
Negative
Net charge of the outside of a neuron
Positive
Passive channels
Always open - leak channels
Active/gated channels
Open and close in response to specific stimuli
Leak channels (passive)
Allows ions to move freely via diffusion
Active (gated) channels
Opening of these channels can change the membrane potential by a brief increase or decrease in the membrane permeability of an ion
Chemically gated ion channel
Chemical binds to a gate to open it
Voltage gated ion channel
Changes in voltage causes the gate to open by changing its structure
Mechanically gated ion channel
Pressure causes the gate to open by changing its structure
Graded potential
Small, local and temporary change in membrane potential
Depolarization
Increase in membrane potential
Hyperpolarization
Decrease in membrane potential
Action potential
Strong stimulus activated when the membrane potential becomes less than -55mV or -60mV
Unmyelinated axons
Continuous propagation
Myelinated axons
Faster propagation of an action potential
Chemical communication
An action potential passes from one neuron to a second neuron at a synapse via chemical messages called neurotransmission
Electrical synapse
Direct physical contact between two cells at a gap junction, action potential (information) is transmitted quickly and efficiently
Chemical synapse
Communication between two neurons or a neuron to another cell, information is transmitted by chemicals called neurotransmitters
Axon terminal
Presynaptic cell
Dendrite
Postsynaptic cell
Excitary neurotransmitter
Promotes the generation of an action potential in the postsynaptic cell
Inhibitory neurotransmitters
Inhibits the generation of an action potential in the postsynaptic cell
Neuromuscular junction
Transfer of information from a motor neuron to a skeletal muscle fibre
Reflex
Brief, rapid, involuntary response triggered by stimulus
Cerebrum
Controls all conscious thoughts and intellectual functions, processes sensory and motor information
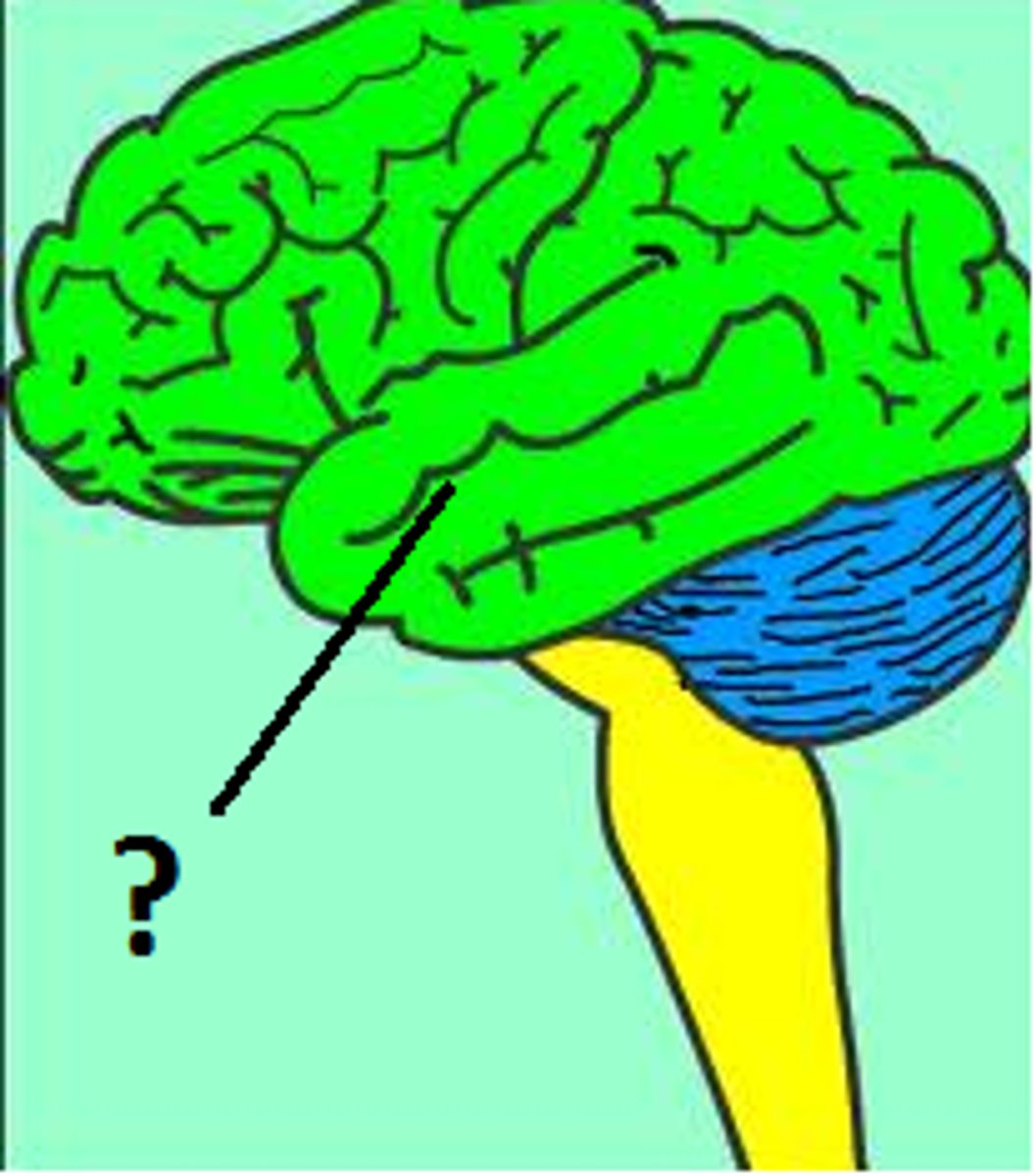
Function of cerebrum
Memory, cognition, control of skeletal muscle contractions, processing/interpreting sensory information
Cerebellum
Monitors and adjust ongoing movement information
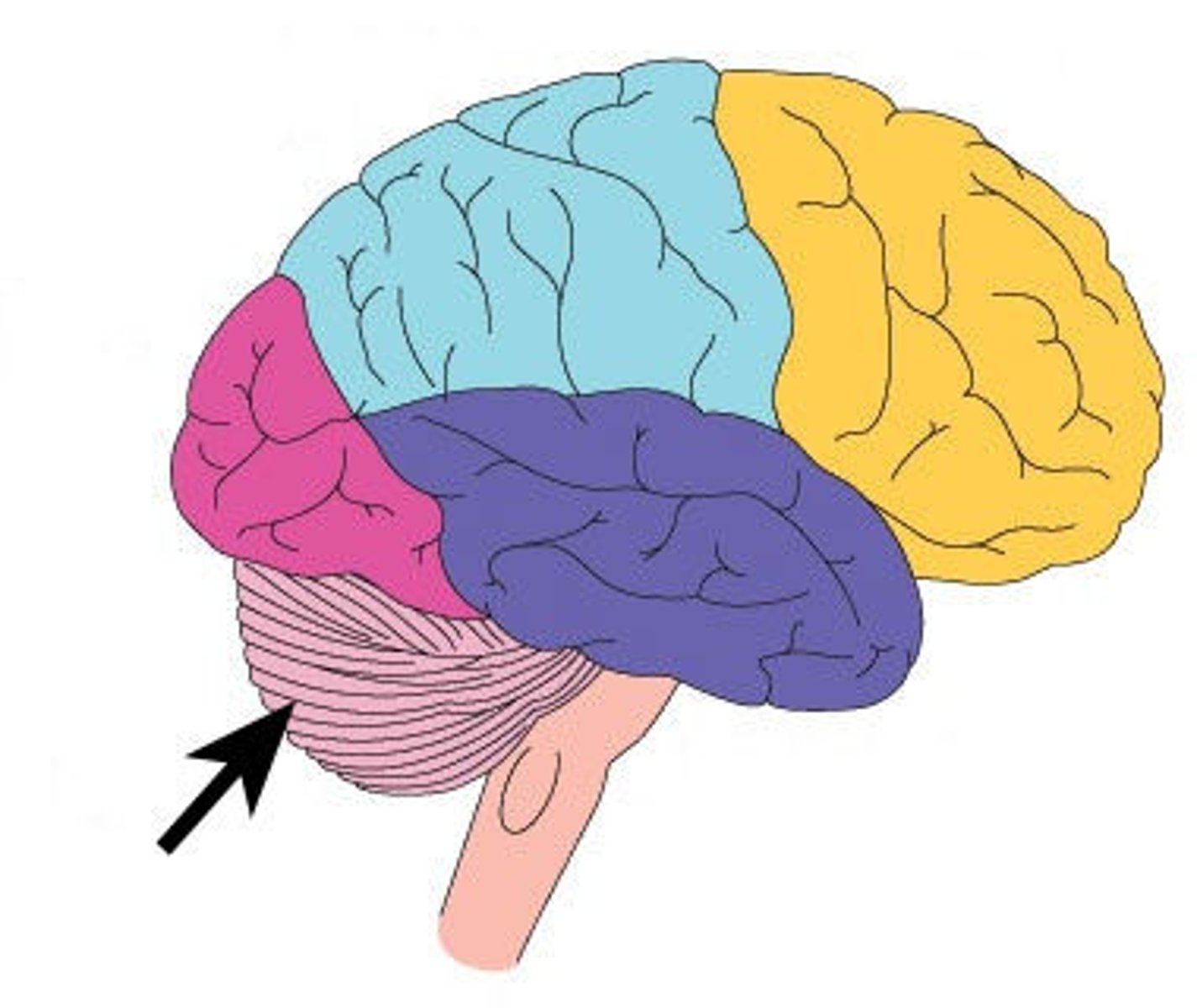
Spinal cord
Transfers information between the brain and the body
Thalamus
Filters and relays sensory information to the cerebral cortex
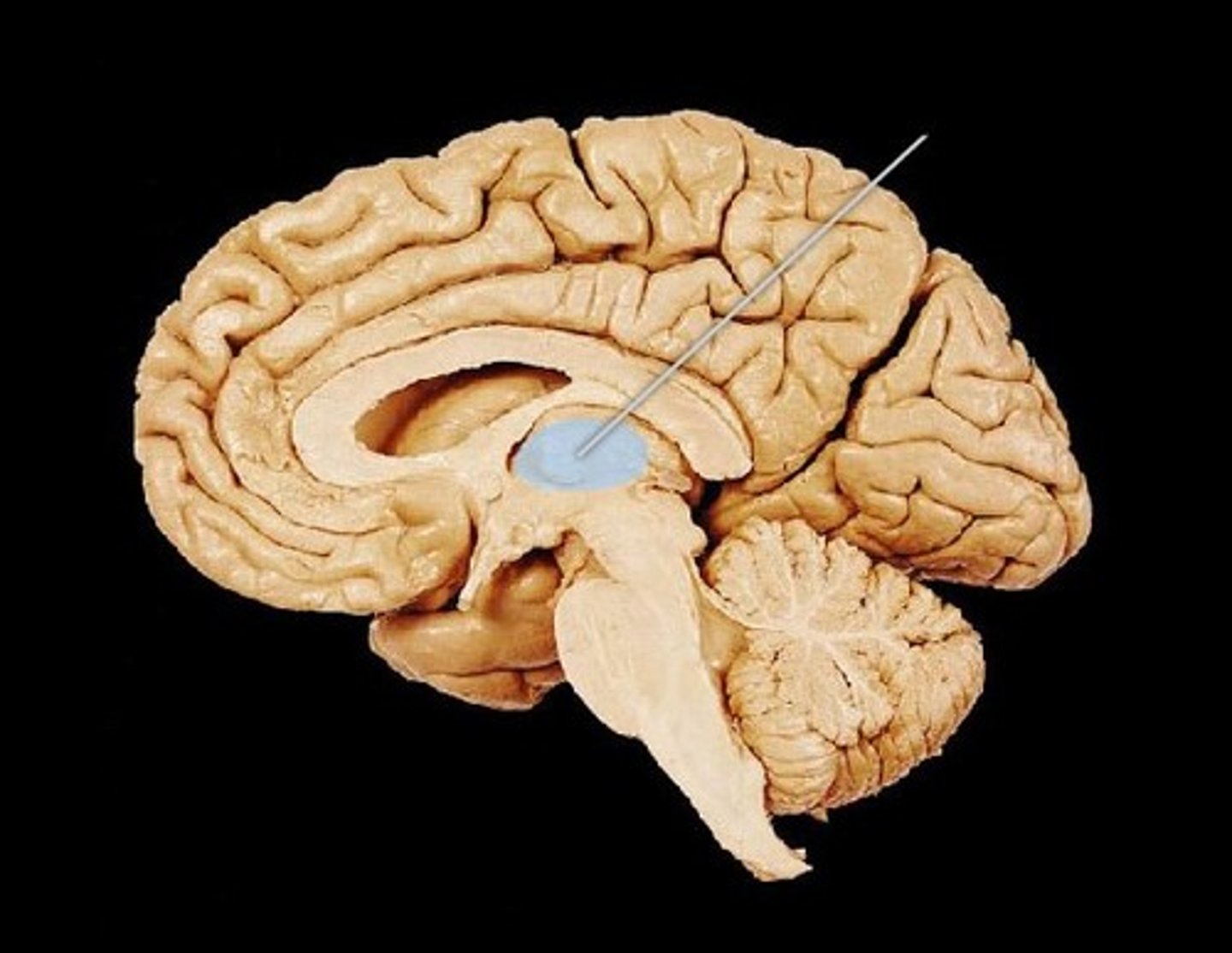
Hypothalamus
Major regulator of homeostasis
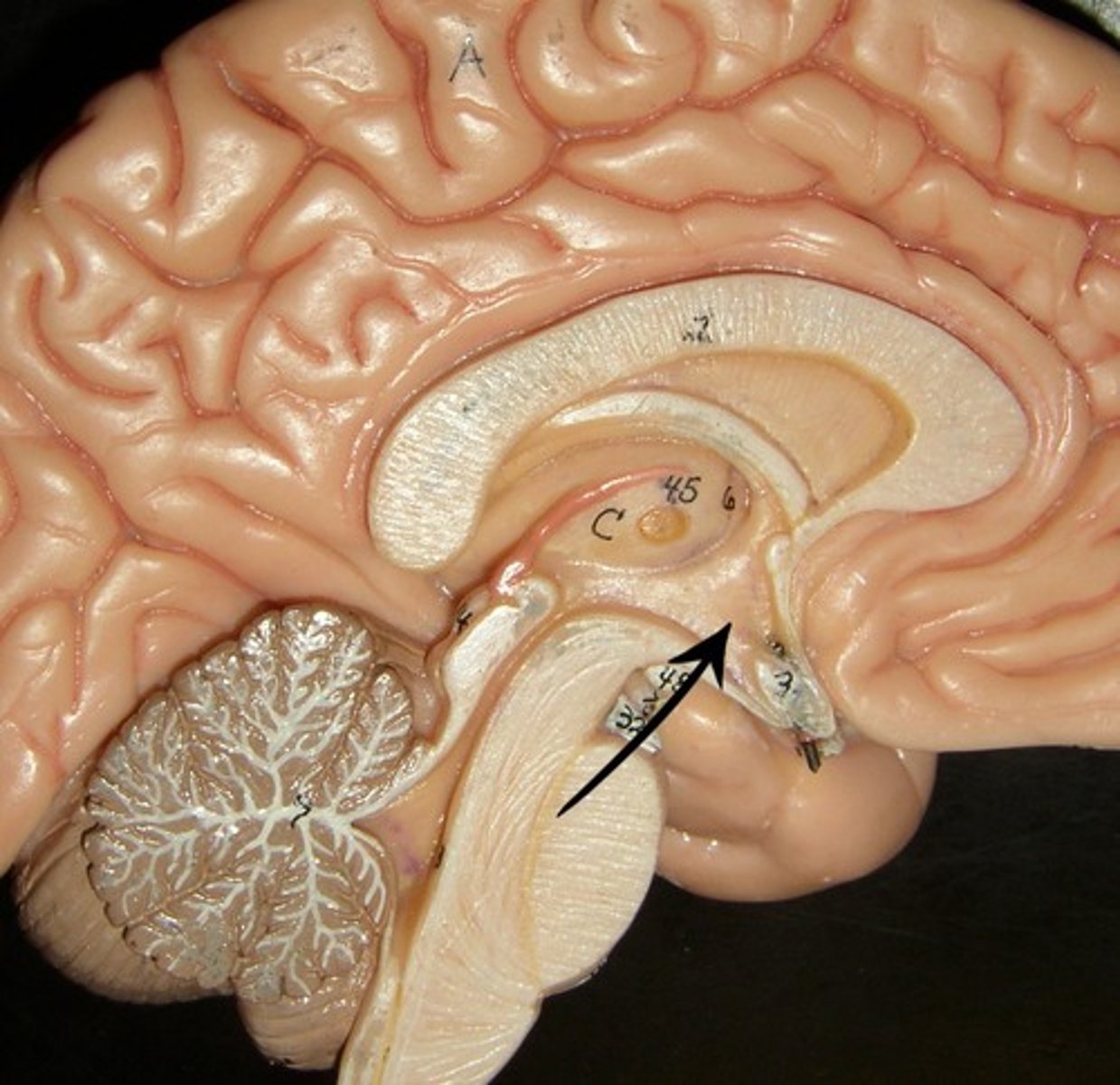
Midbrain
Processes visual and auditory information
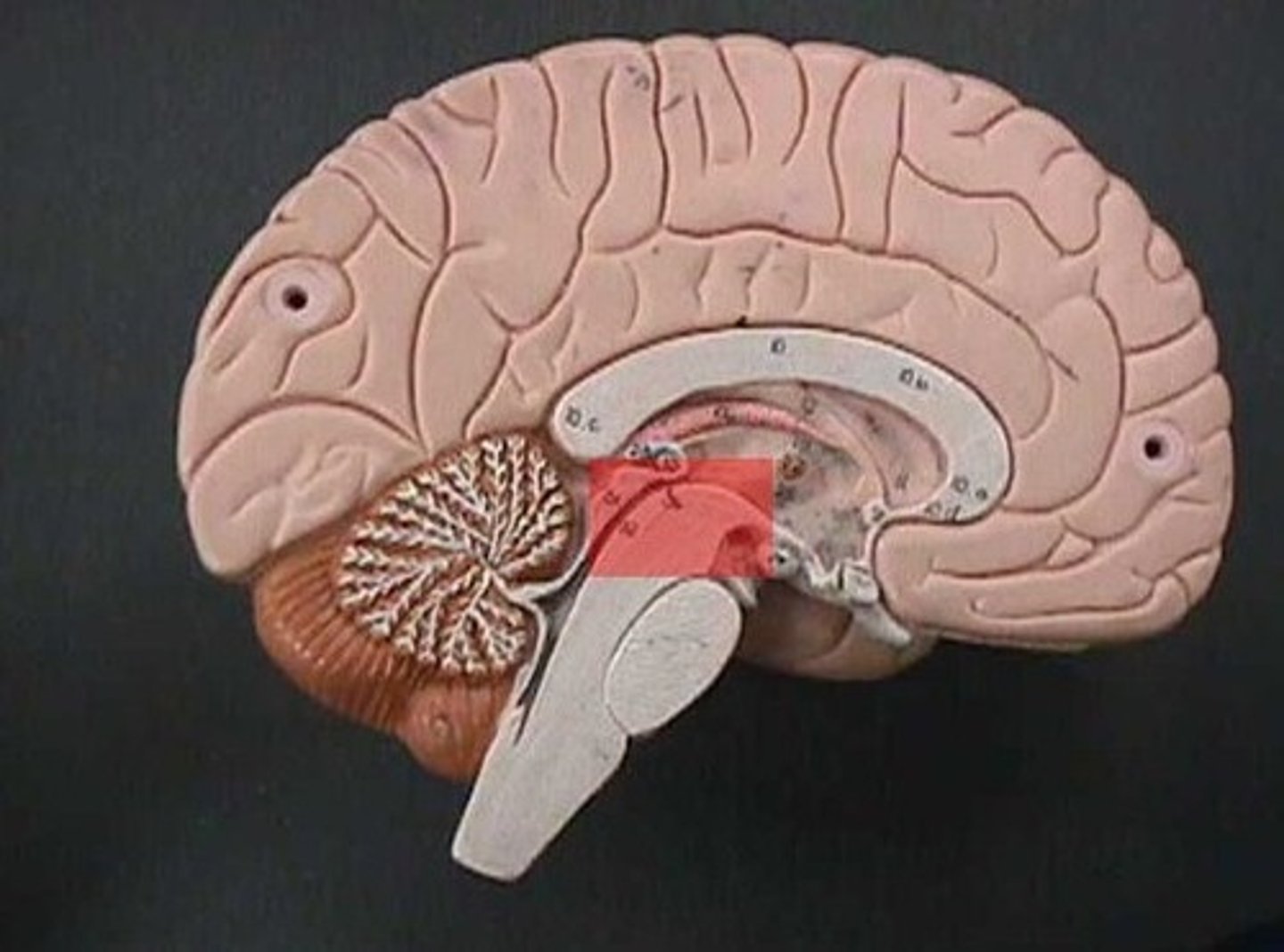
Pons
Subconscious control of skeletal muscle and smooth muscle in organs
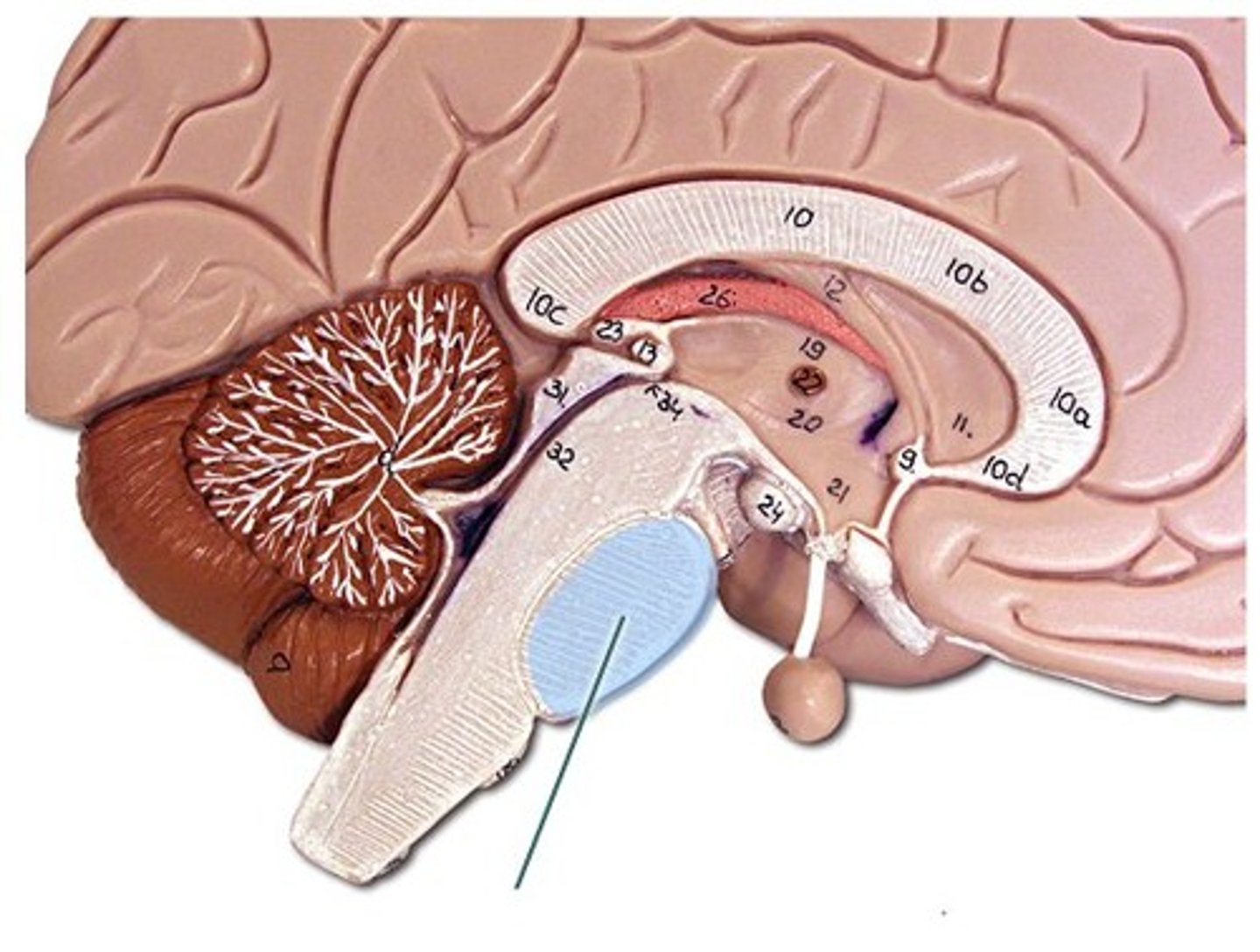
Medulla oblangata
Regulation of the cardiovascular, respiratory and digestive systems
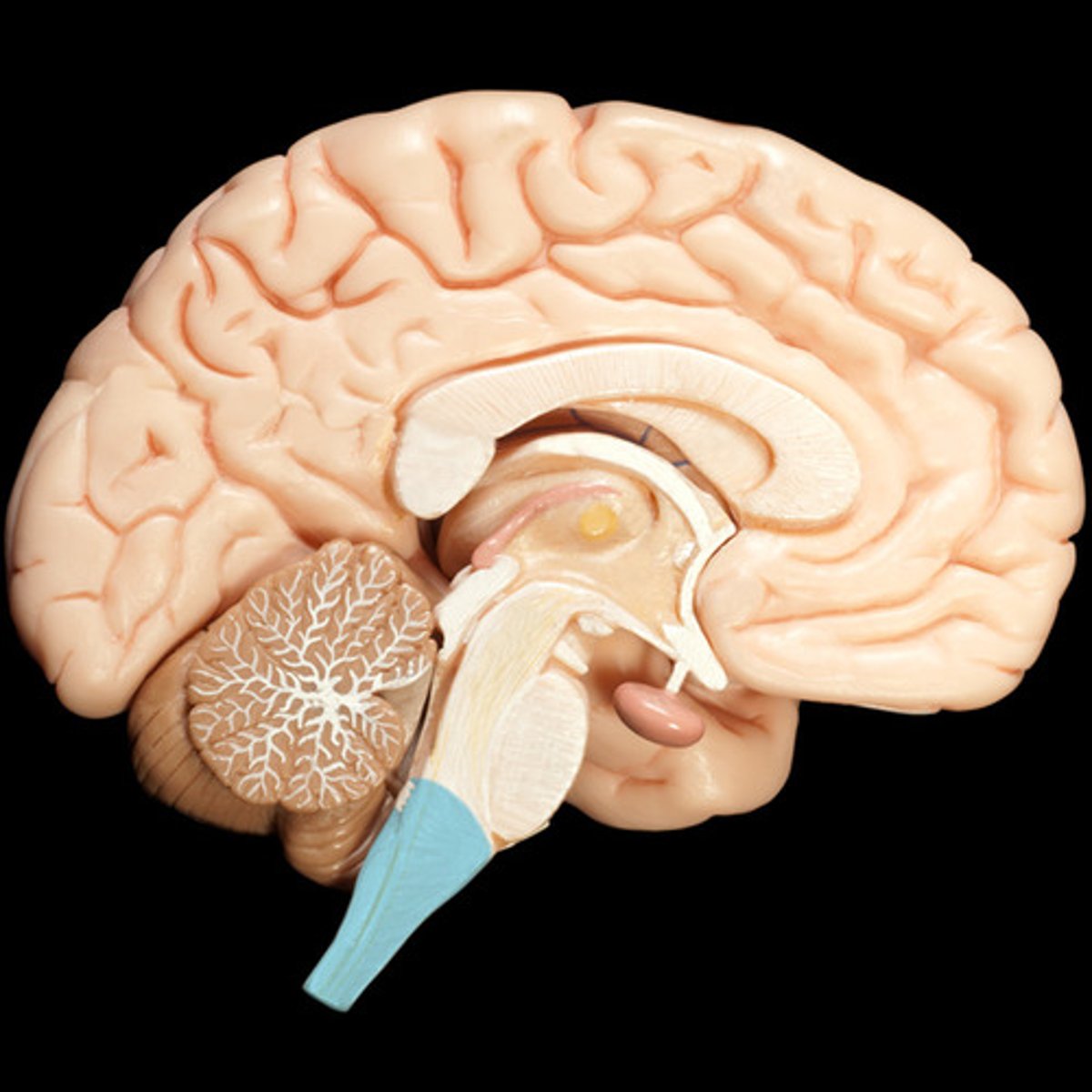
Afferent
Sensory information travelling into the CNS through a dorsal root
Efferent
Command information travelling through out of the CNS through a ventral root
Components of the somatic nervous system
Skeletal muscles, skin and joints
Components of the autonomic nervous system
Glands, smooth muscle, cardiac muscle and adipose tissue
Sympathetic nervous system
Increase heart rate, blood rate and glucose mobilisation. Decrease digestion
Parasympathetic nervous system
Facilitates digestion, energy storage, growth and immune response
Enteric nervous system
Network of neurons in the digestive tract that operate without instructions from the CNS
How many bones in the human body?
206
Osteocytes
mature bone cell that maintains bone matrix
osteoblasts
immature bone cell that produces new bone matrix in a process called ‘ossification’ or ‘osteogenesis’. differentiates to become osteocytes.
osteoclasts
absorb and remove bone matrix. large.
osteogenic
stem cells that become osteoblasts. more rare
Osteon
Basic functional unit of mature compact bone
endochondral ossification
Formation, growth, and remodelling. Occurs in most bones. Involves replacing hyaline cartilage with bone.
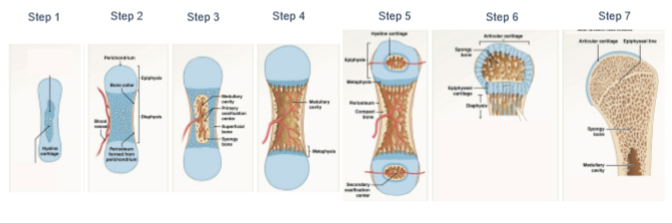
endochondral ossification steps.
cartilage model formation
growth and calcification
blood vessel penetration and spongy bone production
Bone formation (osteoblasts) spreads and remodelling (osteoclasts) occurs
secondary ossification centre created in epiphyses.
epiphyses fill with spongy bone and epiphyseal plate separates epiphysis and diaphysis.
epiphyseal cartilage gets narrower and disappears at puberty.
How do long bones get longer?
endochondral ossification
two types of ossification
endochondral and intramembranous
difference between endochondral and intramembranous ossification
endochondral: occurs in most bones, involves replacing of hyaline cartilage with bone.
intramembranous: occurs in clavicles, mandibles, and flat bones of skull, begins when osteoblasts differentiate in mesenchymal (stem) cells or fibrous connective tissue.
What is bone made up of?
Organic collagen matrix: formed from chains, triple helices, and fibrils.
How do bones support our body weight?
Handle compressive forces via transferring force to compact bone. Tension on lateral side of bone shaft, and compression on the medial side of shaft.
How does exercise affect bone growth and maintenance?
More physical activity —> more applied force/stress to bones —> more bone production by osteoblasts.
Less physical activity —> less applied force/stress to bones —> bone mass loss (up to 1/3 of mass)
Factors that affect bone growth and maintenance.
Nutrition, hormones, and exercise.
Calcitriol
Regulates calcium via homeostasis.
Found in kidneys. Increases calcium and phosphate ion absorption by the intestines of the digestive tract.
Parathyroid hormone.
Regulates calcium via homeostasis. Stimulates osteoclast (and osteoblast) activity, increases the blood calcium ion level
Calcitonin
Regulates calcium via homeostasis.
In pregnant and breastfeeding women, decreases blood calcium ion level and aids calcium ion transfer to fetus.
Calcium homestasis (which hormones)
Calcitriol, parathyroid hormone, and calcitonin regulate level of calcium ions.
Why is calcium homeostasis important to be maintained?
Variations in usual calcium levels (1-2kg of calcium) affects cellular function. (eg neurons and muscle cells)
factors that decrease blood calcium ion level
Thyroid gland secretes calcitonin. triggers a bone response (osteoclast activity decreases), intestinal response (intestinal absorption of calcium decreases), and kidney response (kidneys excrete less calcium ions, leading to calcium loss in urine)
Bone blood cell production
Hemopoiesis: production of platelets, red blood cells, and white blood cells. occurs in red bone marrow.
Cartilage structure
Supportive connective tissue consiting of matrix (firm gel) and cells (chondrocytes) Avascular.
Cartilage types
Fibrocartilage, hyaline, and elastic
Fibrocartilage location and function
Location: meniscus in knee, pubic symphysis, and intervertebral discs
Function: resists compression, limits movement
Hyaline cartilage location and function
Location: synovial joints
Function: Reduces friction between articular bony surfaces, stiff yet flexible support
Ligaments structure
Dense regular connective tissue consting mostly of collagen fibres. avascular.
Examples of cells in ligaments
Fibroblasts: secrete protein subunits to form collagen.
Fibrocytes: maintain collagen fibres
Types of ligaments
Extracapsular: outside joint capsule
Intracapsular: inside joint capsule
Ligament function
Connects bone to bone, supports, strengthens and reinforces synovial joints.
Affects of aging on bones
Osteoporosis: decreased bone mass and/or density
Arthritis: joint inflammation and damage to articular cartilage.
What is the name of the process that converts DNA to mRNA?
Transcription
What is the name of the process that converts mRNA to protein?
Translation
Secretory vesicle
Fuse to membrane and empty contents into extracellular space
Membrane renewal vesicle
Add new proteins and lipids to plasma membrane
Passive transport
Requires no energy expenditure
Active transport
Requires the cell to expend energy
Diffusion
Net movement of a substance from an area of higher concentration to an area of lower concentration (passive)
Concentration gradient
Difference between high and low concentration
Down the concentration gradient
Movement of a substance from an area of higher concentration to an area of lower concentration
Osmosis
Diffusion of water across a semi-permeable membrane (passive)
Facilitated diffusion
Integral proteins bind specific ions or organic substrates and carry them across the plasma membrane via carrier-mediated/facilitated diffusion
Active transport (type of transport)
Integral proteins bind specific ions and carry them across the plasma membrane via carrier-mediated transport (active)
Exocytosis
Small membrane sac fuses with the plasma membrane to move substances out of the cell (active)
Endocytosis
Extracellular materials are packed in vesicles at the plasma membrane and transported into the cell (active)
Receptor-mediated endocytosis
Movement of hormones
Pinocytosis
Movement of nutrients
Phagocytosis
Movement of bacteria
Intercellular communication
Communication between cells
Endocrine communication
Occurs when a cell releases a chemical message into the bloodstream to affect the activity of specific cells in another part of the body
Paracrine communication
Occurs when a cell releases a chemical message into the extracellular fluid to transfer information from cell to cell, primarily with a single tissue
Autocrine communication
Occurs when the chemical messages affect the same cells that secrete them
Synaptic communication
Occurs when a neuron releases a chemical message at a chemical synapse with a target cell
Direct communication
Occurs between two cells of the same type and the cells must be in physical contact
How do somatic cells divide?
Mitosis
How do sex cells divide?
Meiosis
Tissue
A group of cells working together to perform specific functions
Connective tissue
Fills internal spaces, provides structural support, stores energy
Epithelial tissue
Covers exposed surfaces and forms glands
Nervous tissue
Carries information from one part of the body to another in the form of electrical impulses