Lids & Lashes (Full)
1/343
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
344 Terms
How many times do we blink per minute?
12-20x
(so there has to be some lid laxity because it is in constant motion)
sebaceous glands found in the eyelid skin near eyelashes
glands of Zeis
sweat glands found in the eyelid skin near eyelashes
glands of Moll
critical barrier between the orbit & lid tissues that provides rigidity to eyelids and prevents orbital fat protrusion, edema, hemorrhage, & infection
orbital septum
trichiasis
EYELASH ABNORMALITY
--eyelid is in normal position
--eyelashes grow out of right place but in the wrong direction
CAUSES:
--trauma (chemical burns)
--trachoma
--inflammation (blepharitis, VKC)
--epiblepharon
--herpes zoster blepharitis
--autoimmune diseases (OCP, SJS/TEN)
TREATMENT:
--lubrication
--contact lenses
--epilation via forceps every 6-10 weeks
--entropion repair
--surgery/lasers
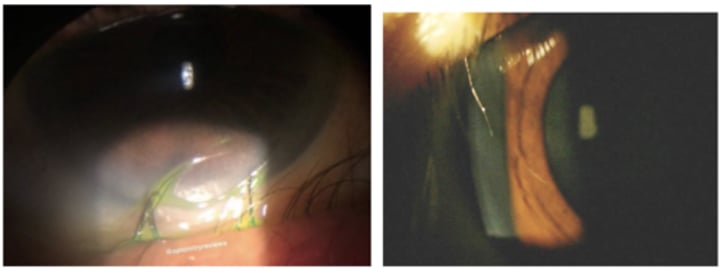
8 most common causes of trichiasis
trauma (chemical burns), trachoma, blepharitis, VKC, epiblepharon, herpes zoster, OCP, SJS/TEN
epiblepharon
LID ABNORMALITY LEADING TO TRICHIASIS
--congenital and relatively common bilateral condition
--common in Asians and Native Americans
CAUSES:
--no definitive cause
--may be due to extra horizontal fold of tissue that overrides the lid margin
--may also be due to absent insertion of lower lid retractors to the skin and orbicularis, or insertion that's too close to the lid margin
TREATMENT:
--can resolve with facial bone growth by 2 years old
--surgical repair can fix, though it can recur
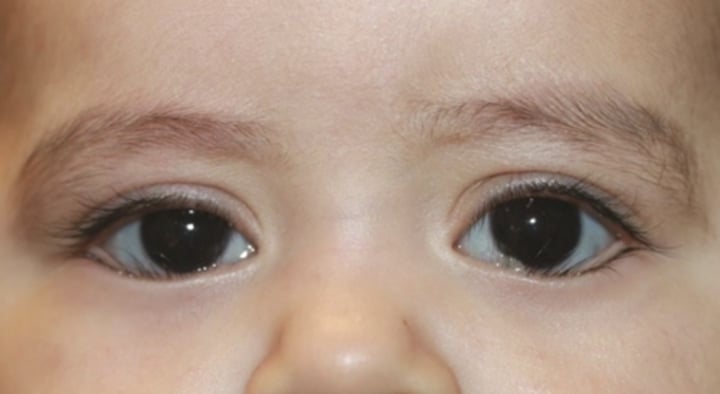
There is no definitive cause of epiblepharon. What are 3 possible causes?
1. extra horizontal fold of tissue that overrides the lid margin
2. no insertion of lower lid retractors to skin/muscle
3. lid retractors inserted too close to lid margin
How do we fix epiblepharon and thus the accompanying trichiasis?
resolves on its own with facial bone growth, but might need surgery
What are 5 treatments for trichiasis?
lubrication, CLs, epilation, cryotherapy, entropion repair/other forms of surgery
distichiasis
EYELASH ABNORMALITY
--additional lashes grow from the wrong place
--double row of eyelashes
CAUSES:
--congenital: isolated, associated with ptosis or strabismus
--acquired: entropion, chronic inflammation, chemical burns
TREATMENT:
--monitor
--epilation
--surgery/lasers
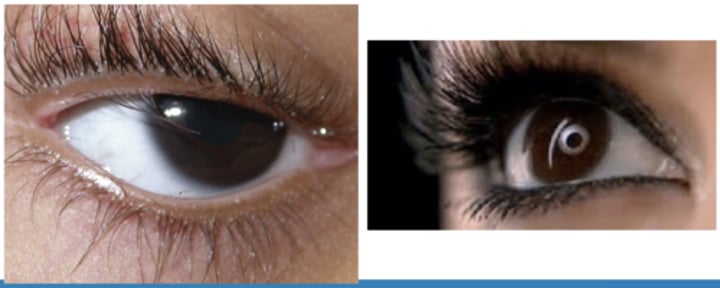
Distichiasis may be congenital, associated with a ptosis or strabismus. However, it can also be acquired - what are 3 causes of acquired distichiasis?
entropion, chronic inflammation, chemical burns
We monitor distichiasis to see if it warrants further treatment. If it does, what are 3 forms of treatment?
epilation, cryotherapy, trephination/other forms of surgery
In addition to trauma, tumors, and cosmetic related causes like a makeup reaction/eyelid tattooing, chronic inflammation can also be a cause of madarosis. What are 2 forms of chronic inflammation that can cause it?
blepharitis, allergy
In addition to trauma, tumors, and cosmetic related causes like a makeup reaction/eyelid tattooing, systemic conditions can also be a cause of madarosis. What are 7 examples of systemic (hint: some autoimmune) conditions where madarosis is seen?
alopecia, SLE, scleroderma, psoriasis, thyroid disease, HIV/AIDS, sickle cell disease
In addition to trauma, tumors, and cosmetic related causes like a makeup reaction/eyelid tattooing, medications can also be a cause of madarosis. What are 4 examples of medications that can cause madarosis?
miotics, cholesterol, anticoagulants, Botox
poliosis
EYELASH ABNORMALITY
--abnormality of hair melanin
--white eyelashes
CAUSES:
--VKH Syndrome
--Waardenburg Syndrome
--chronic blepharitis
--topical medications: prostaglandins
--melanoma
--autoimmune disease: sarcoidosis
TREATMENT: none
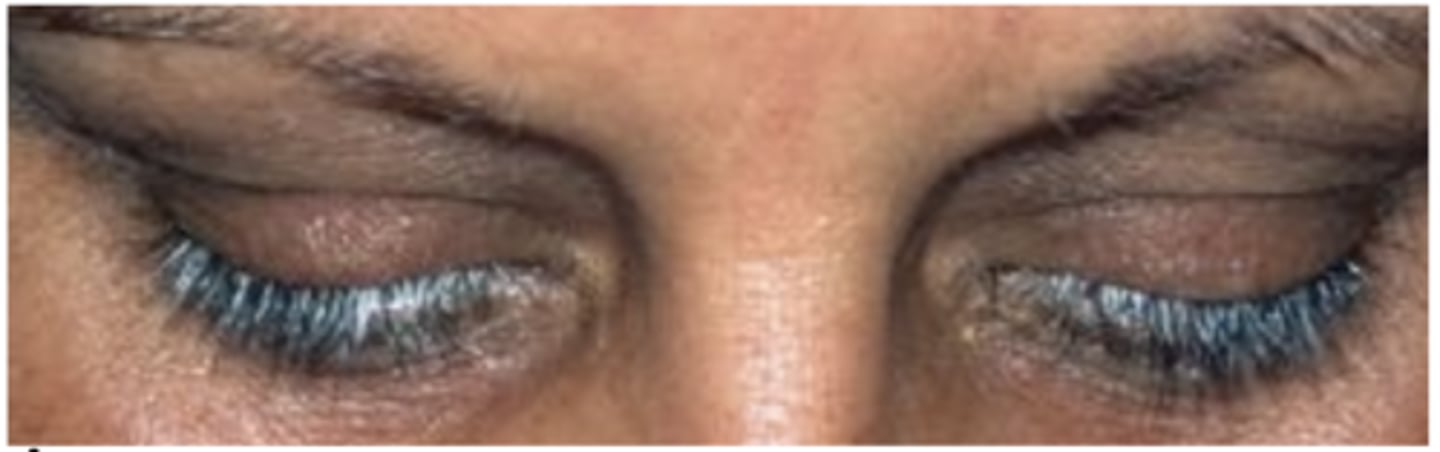
What are 6 conditions/factors associated with poliosis?
VKH syndrome, Waardenburg syndrome, chronic blepharitis, melanoma, autoimmune disease, chronic blepharitis
entropion
ABNORMAL LID POSITION
--eyelid turns inward
--appears as pseudotrichiasis
--may be involutional (senile), cicatricial, spastic, or congenital
SYMPTOMS:
--FB sensation
--tearing
--photophobia
--redness
--pain
--corneal staining, infection, scarring
TREATMENT:
--lubrication
--bandage CL
--lash epilation
--lid taping
--Botox
--sutures
--eyelash removal
--membrane grafts
--antibiotics or immunosuppressives
--surgery
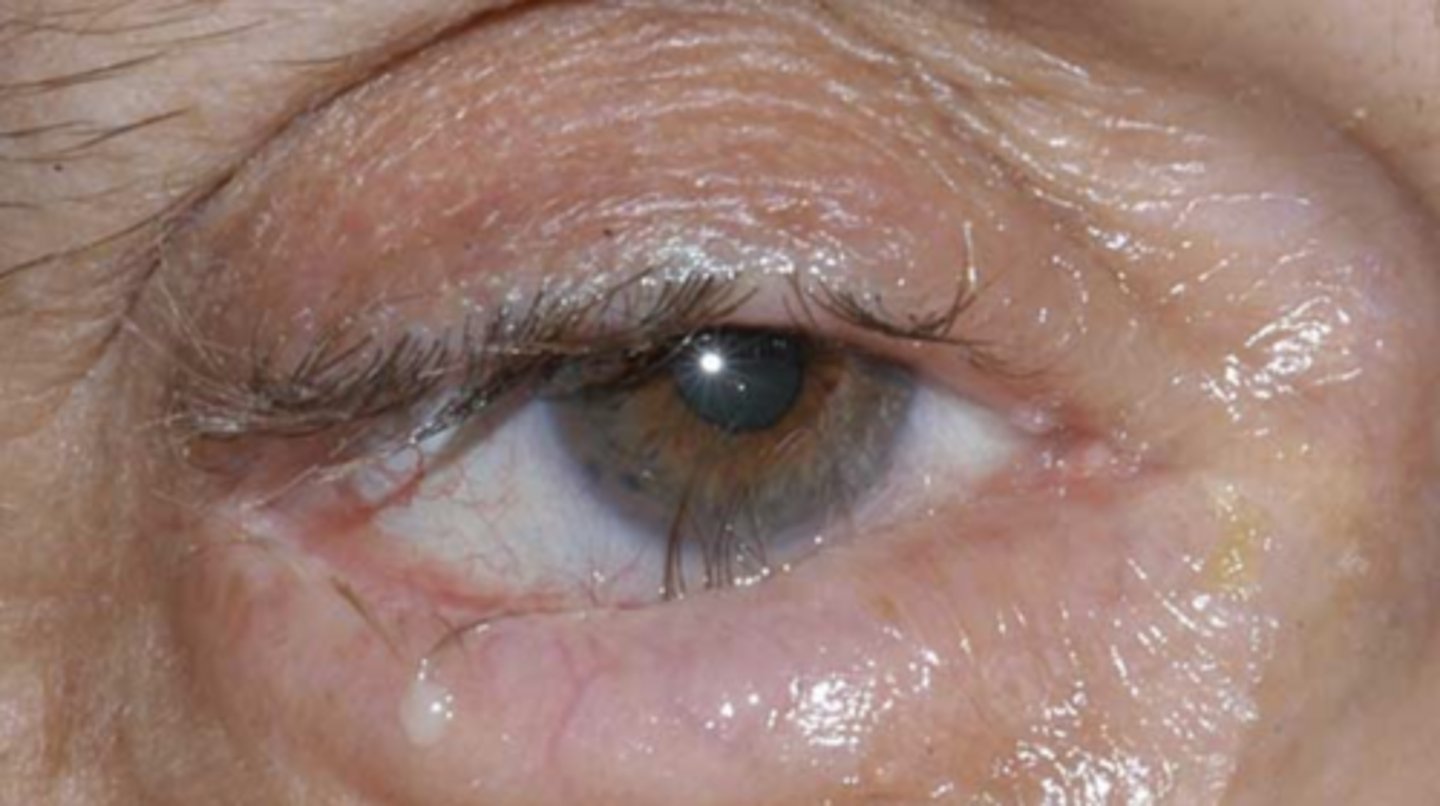
What are 6 symptoms that a patient may experience with entropion?
FBS, tearing, photophobia, redness, pain, corneal involvement
What are 4 types of entropion? What is the most common?
involutional (senile), cicatricial, spastic, congenital
involutional is most common
involutional entropion
ABNORMAL LID POSITION - type of ENTROPION
--eyelid turned inward due to age
--occurs with lower lid only
--happens due to "O'HARE"...
--Overaction of palpebral part of orbicularis oculi muscle
--Horizontal lid laxity caused by stretching of cantonal tendons
--Atrophy of tarsal plate
--Retractor dehiscence of the lower eyelid retractors
--Enopthalmos of the globe
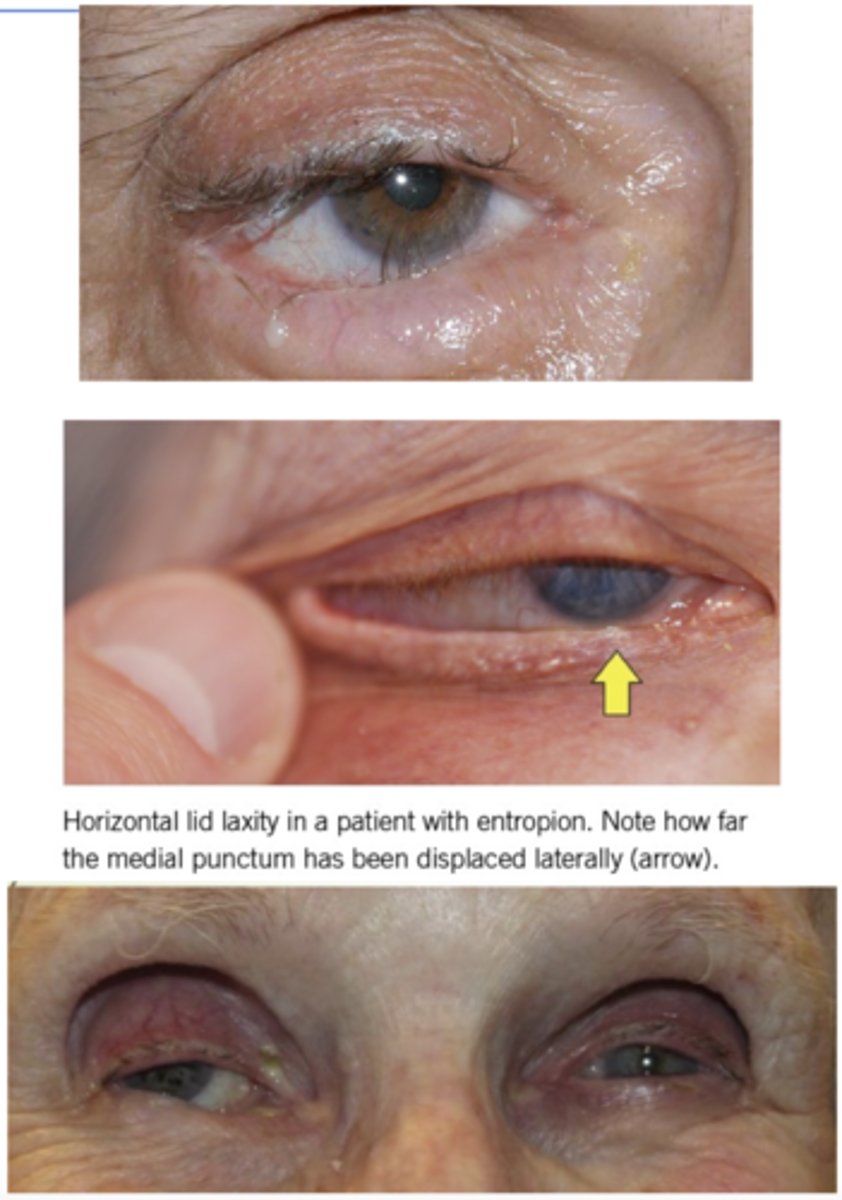
What are 5 contributing factors to involutional (senile) entropion? (hint: "OHARE")
1. overreaction of palpebral part of orbicularis oculi
2. horizontal lid laxity
3. atrophy of tarsal plate
4. retractor dehiscence of lower eyelid retractors
5. enophthalmos
cicatricial entropion
ABNORMAL LID POSITION - type of ENTROPION
--eyelid turned inward due to conjunctival fibrosis shrinking the posterior lamellae
--can occur with upper and lower lids
--difficult to treat, high recurrence
CAUSES:
--infectious (trachoma, herpetic disease)
--inflammatory (OCP, SJS/TEN)
--chronic use of glaucoma drops
--trauma (chemical burn, post surgical, radiation)
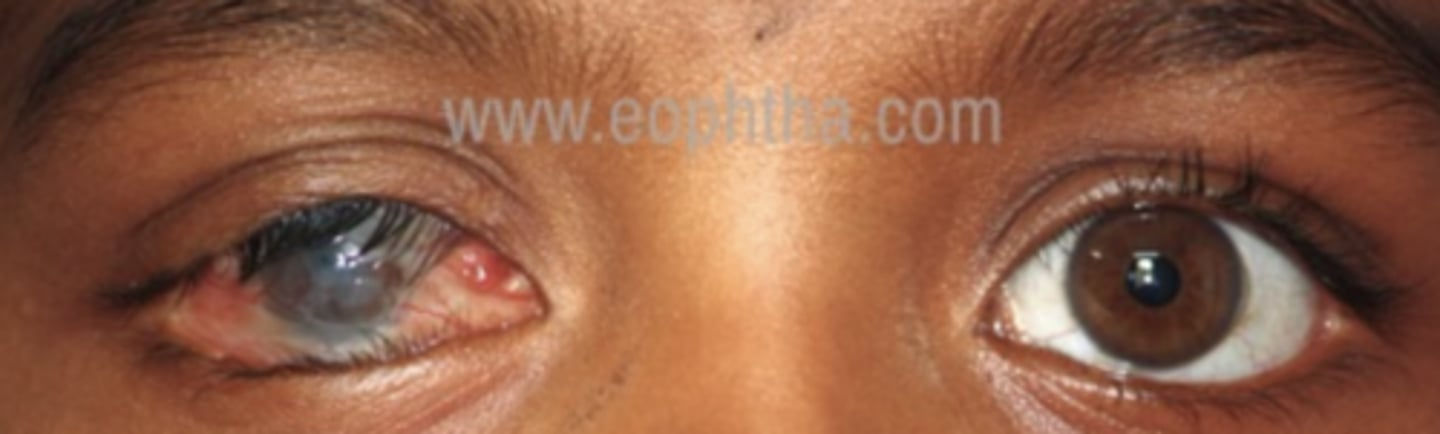
What are 5 causes of cicatricial entropion?
trachoma, OCP, SJS/TEN, chronic use of glaucoma drops, trauma (chemical burn, post-surgical, radiation)
ocular cicatricial pemphigoid (OCP)
AUTOIMMUNE DISEASE - cause of CICATRICIAL ENTROPION
--type II hypersensitivity reaction
--rare, bilateral, chronic
--relapsing autoimmune disease
--more common in females, 60+
--vision threatening
--treated with systemic immunomodulators
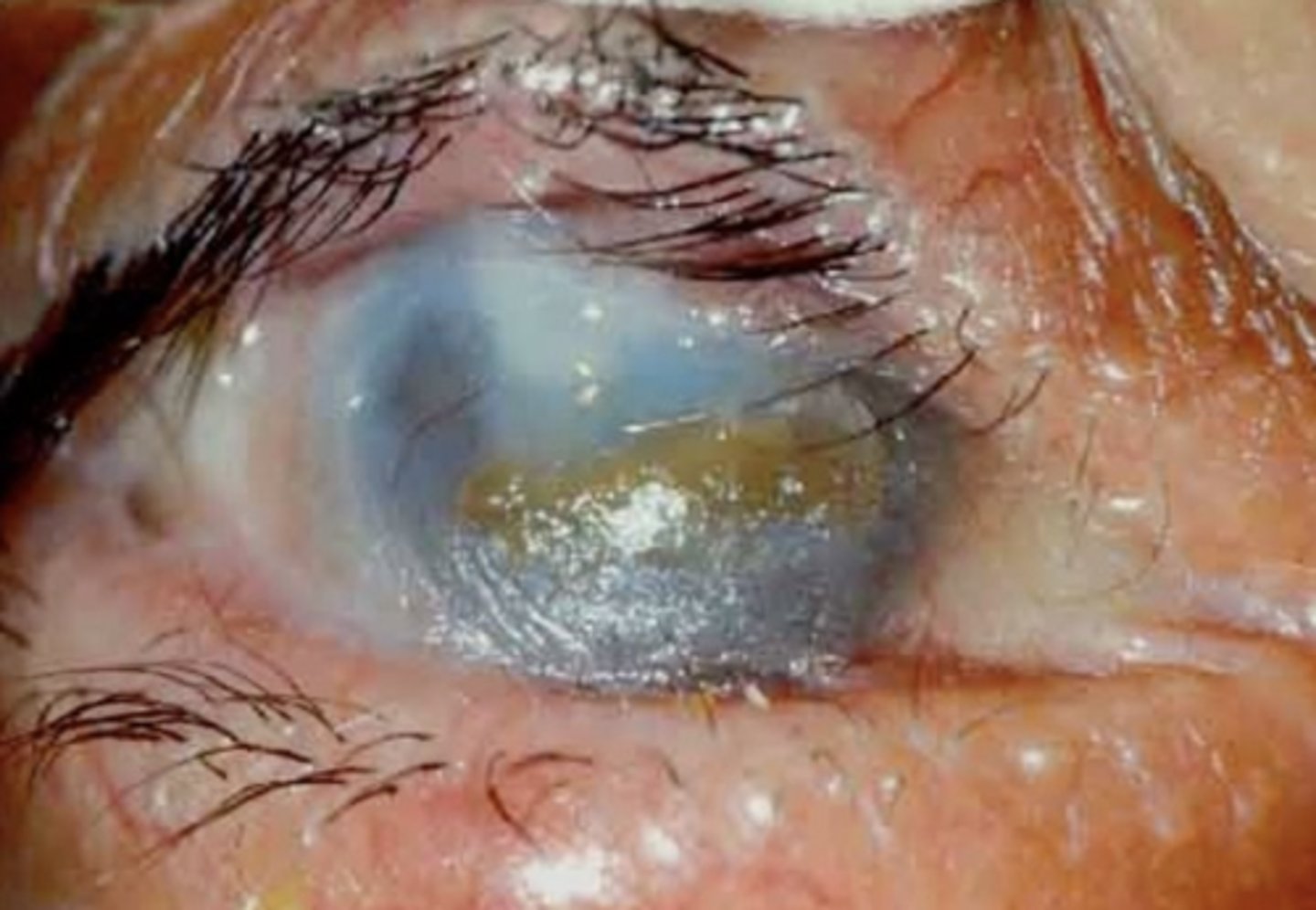
Stevens-Johnson Syndrome & toxic epidermal necrolysis (SJS/TEN)
pair of AUTOIMMUNE DISEASES - cause of CICATRICIAL ENTROPION
--rare, severe skin reaction triggered by medications
--damages mucous membranes
--potentially vision and life threatening
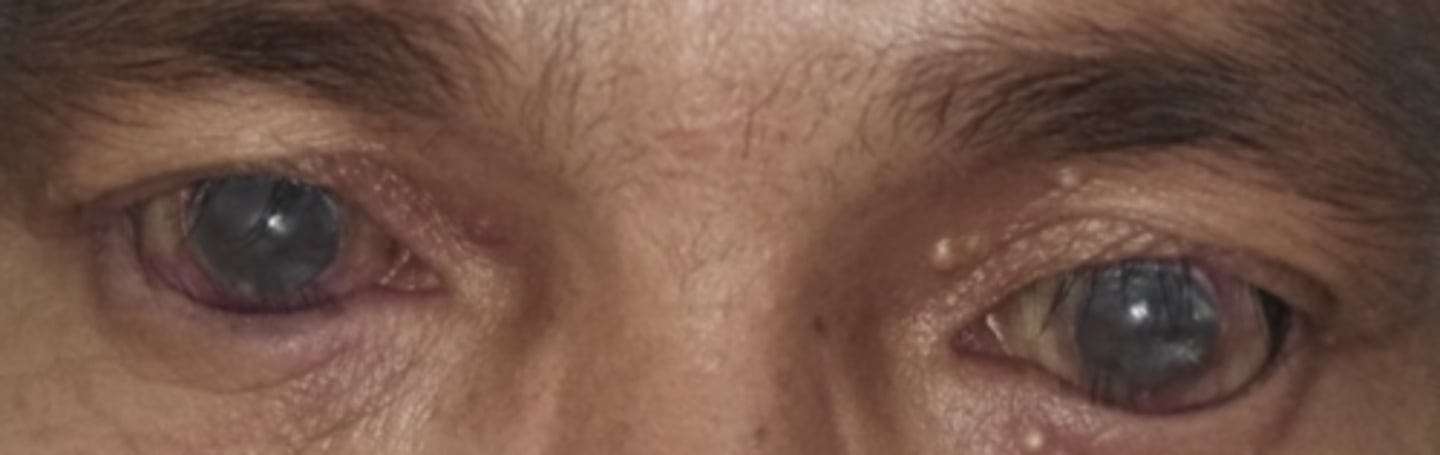
spastic entropion
ABNORMAL LID POSITION - type of ENTROPION
--eyelid turned inward that occurs intermittently
--often associated with involutional entropion
CAUSES:
--blepharospasm or hemifacial spasm
--post ocular surgery
--inflammatory ocular conditions

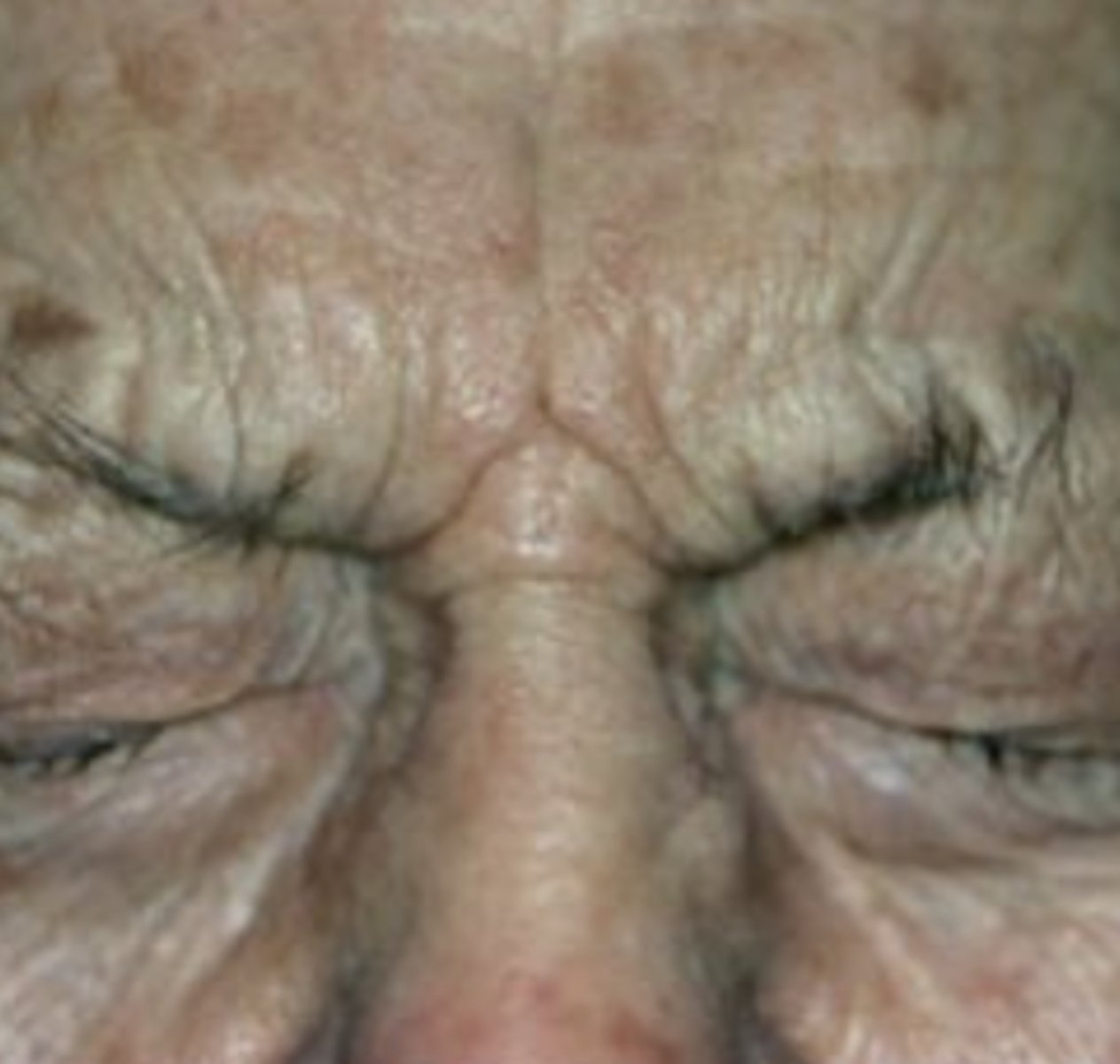
blepharospasm
ABNORMAL LID CONDITION - cause of SPASTIC ENTROPION
--involuntary, tonic, spastic bilateral lid closure
--type of dystonia
--can also cause pseudoptosis
--more common in females, 50+
--cause: idiopathic, Parkinson's, psychotropic meds
--treatment: anti-cholinergic meds, Botox
What are 2 forms of treatment commonly used for blepharospasm which can also treat spastic entropion?
anti-cholinergic meds, Botox
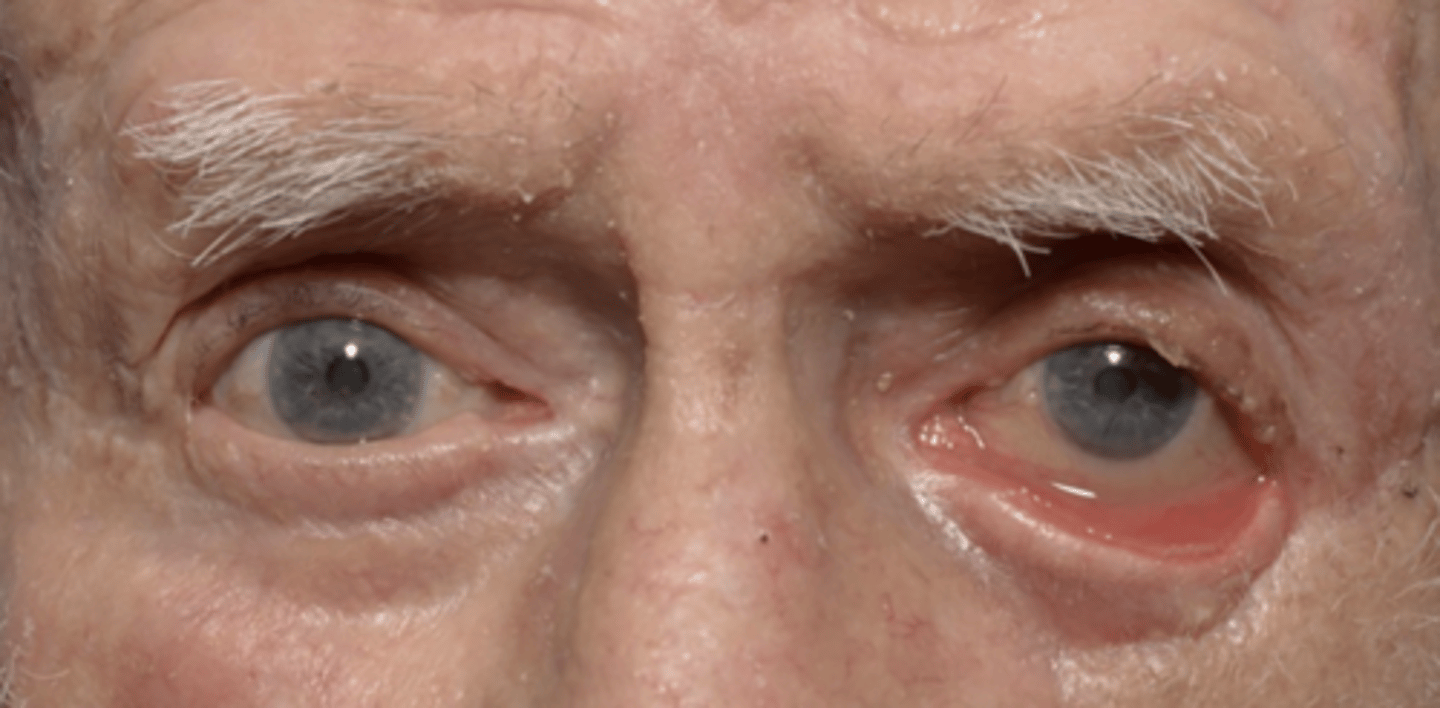
ectropion
ABNORMAL LID POSITION
--eyelid turns outward
--may be involutional, cicatricial, paralytic, inflammatory, mechanical, or congenital
SYMPTOMS:
--epiphora
--redness
--dryness
--FB sensation
--irritation
--conjunctiva is thickened, hyperemic, possibly keratinized
--punctal malposition & stenosis
--corneal exposure, staining, neurotrophic
--infection
TREATMENT:
--treat the underlying condition
--lubrication
--bandage CL
--lid taping
--tarsorrhaphy (glue, suture)
--surgical repair
What are 5 symptoms indicating that a patient may be experiencing ectropion?
epiphora, redness, dryness, FBS, irritation
What are 5 consequences that may result from a patient having ectropion?
thickened/hyperemic conj, possible keratinization of conj, punctal malposition, corneal involvement, infection
What are the 6 types of ectropion?
involutional (senile), cicatricial, paralytic, inflammatory, mechanical, congenital
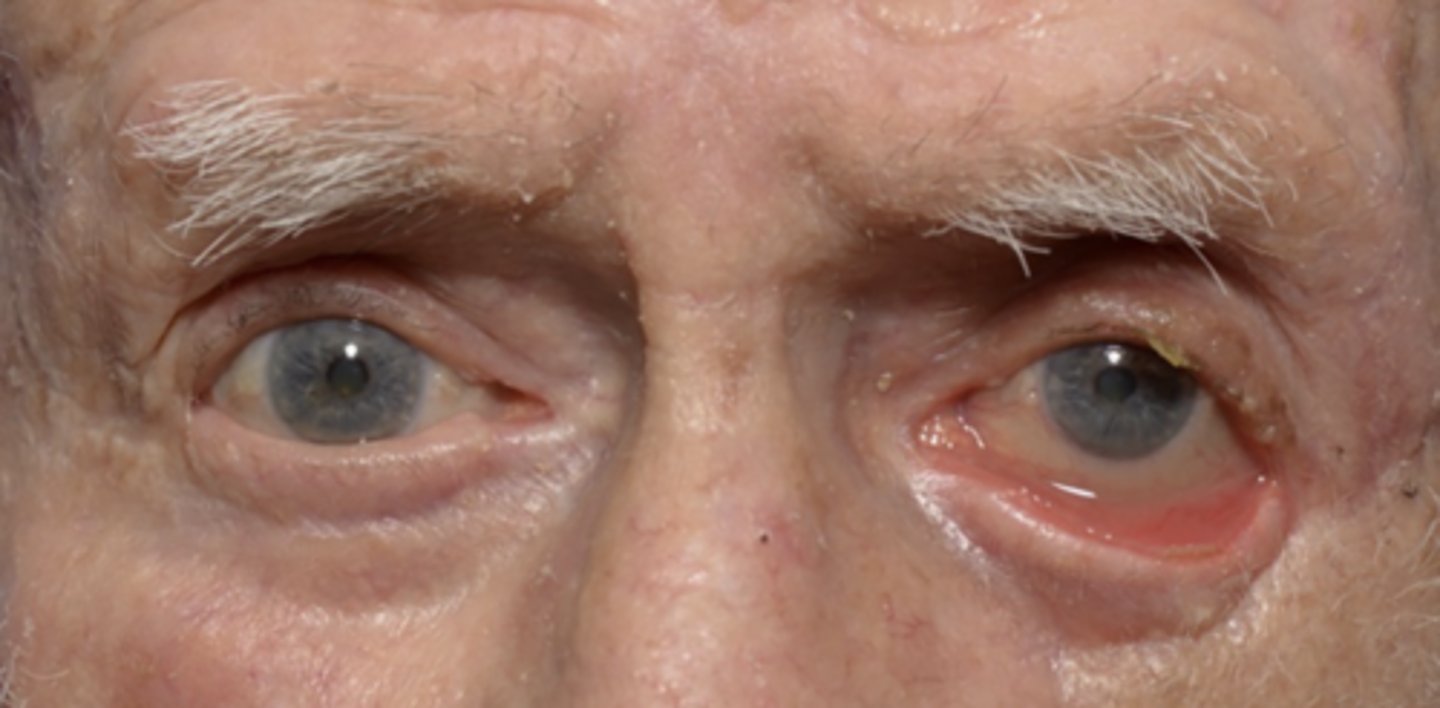
involutional ectropion
ABNORMAL LID POSITION - type of ECTROPION
--eyelid turned outward due to age
--caused by weakness of the pre-tarsal portion of the orbicularis oculi
--also results from laxity of canthal ligaments & punctual malposition
What causes involutional ectropion? (2)
weakness of pretarsal portion of orbicularis oculi & laxity of canthal ligaments
cicatricial ectropion
ABNORMAL LID POSITION - type of ECTROPION
--eyelid turned outward due to trauma, ichthyosis, or herpes zoster ophthalmicus
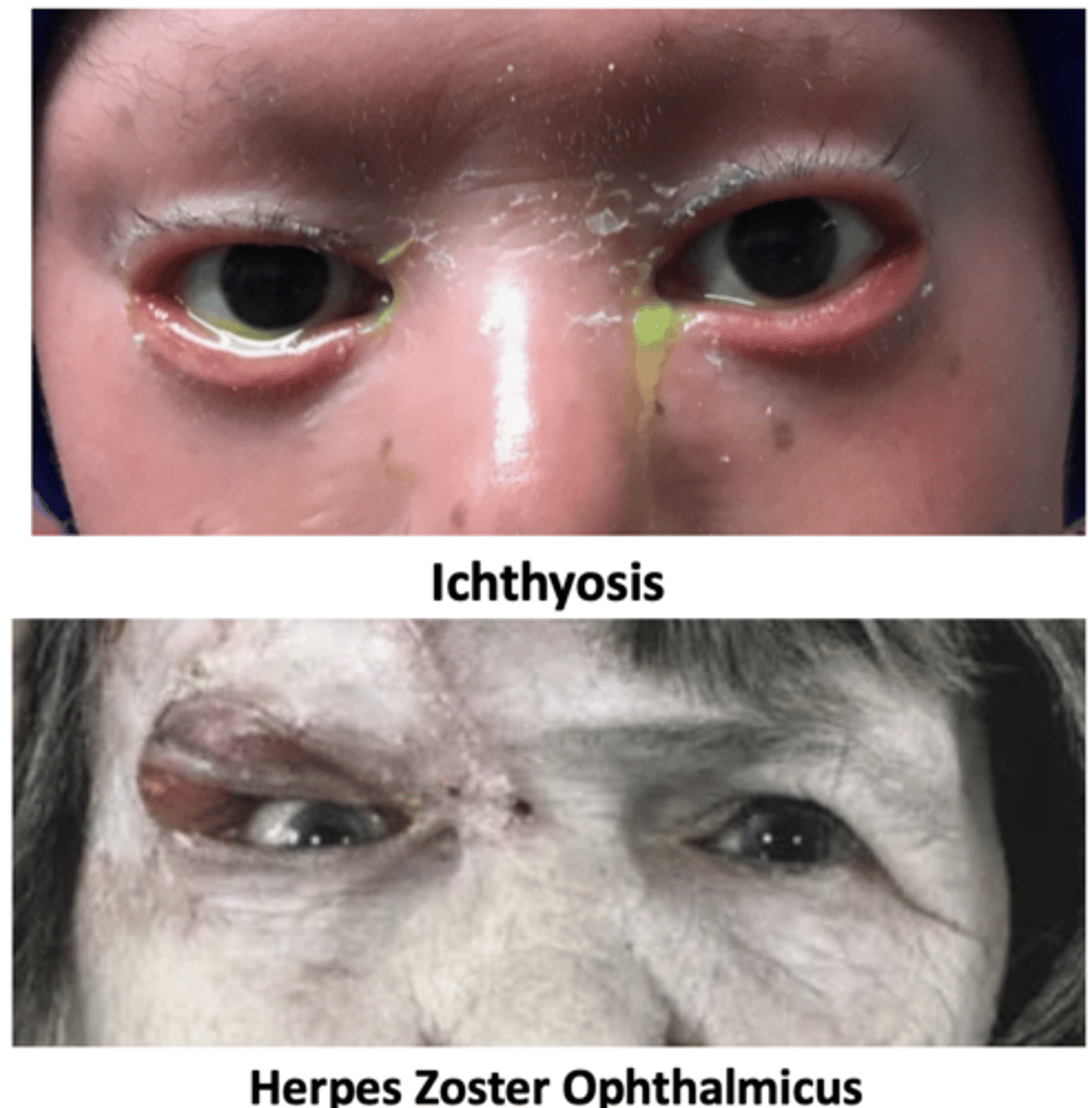
What are 3 possible causes of cicatricial ectropion?
trauma, ichthyosis, herpes zoster
paralytic ectropion
ABNORMAL LID POSITION - type of ECTROPION
--eyelid turned outward due to a CN VII palsy, stroke, tumor, or surgery

In addition to a stroke, tumor, or some form of surgery, another form of paralytic ectropion could be what form of CN palsy?
CN VII palsy
inflammatory ectropion
ABNORMAL LID POSITION - type of ECTROPION
--eyelid turned outward due to eczema, rosacea, psoriasis dermatitis, or certain medications
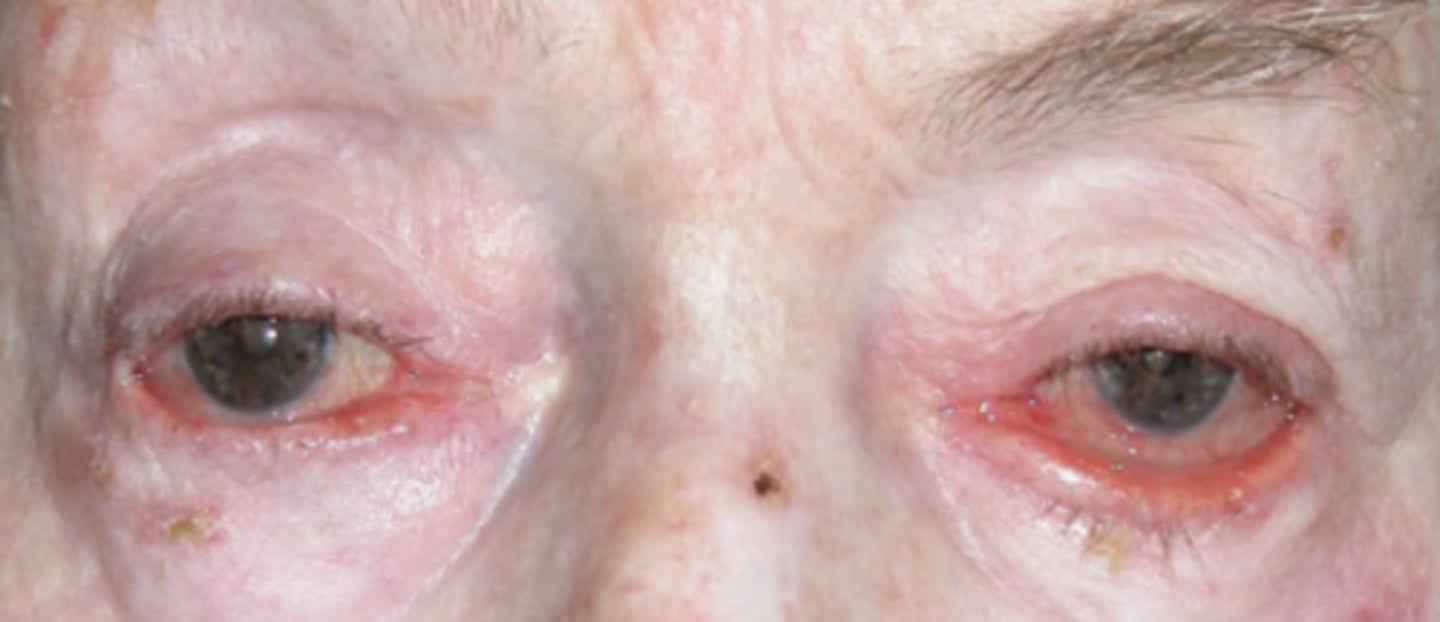
mechanical ectropion
ABNORMAL LID POSITION - type of ECTROPION
--eyelid turned outward due to a tumor, chalazion, dermatochalasis, or orbital fat herniation
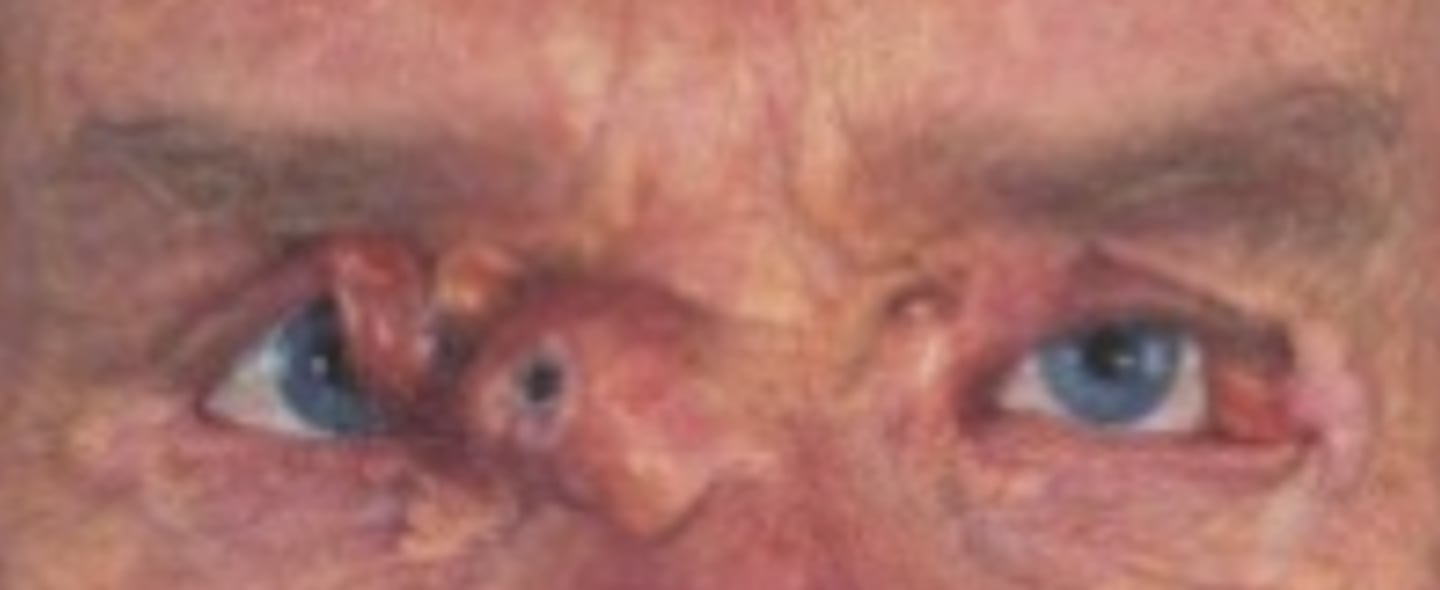
congenital ectropion
ABNORMAL LID POSITION - type of ECTROPION
--eyelid turned outward due to blepharophimosis or Down's Syndrome
--patient is born with ectropion
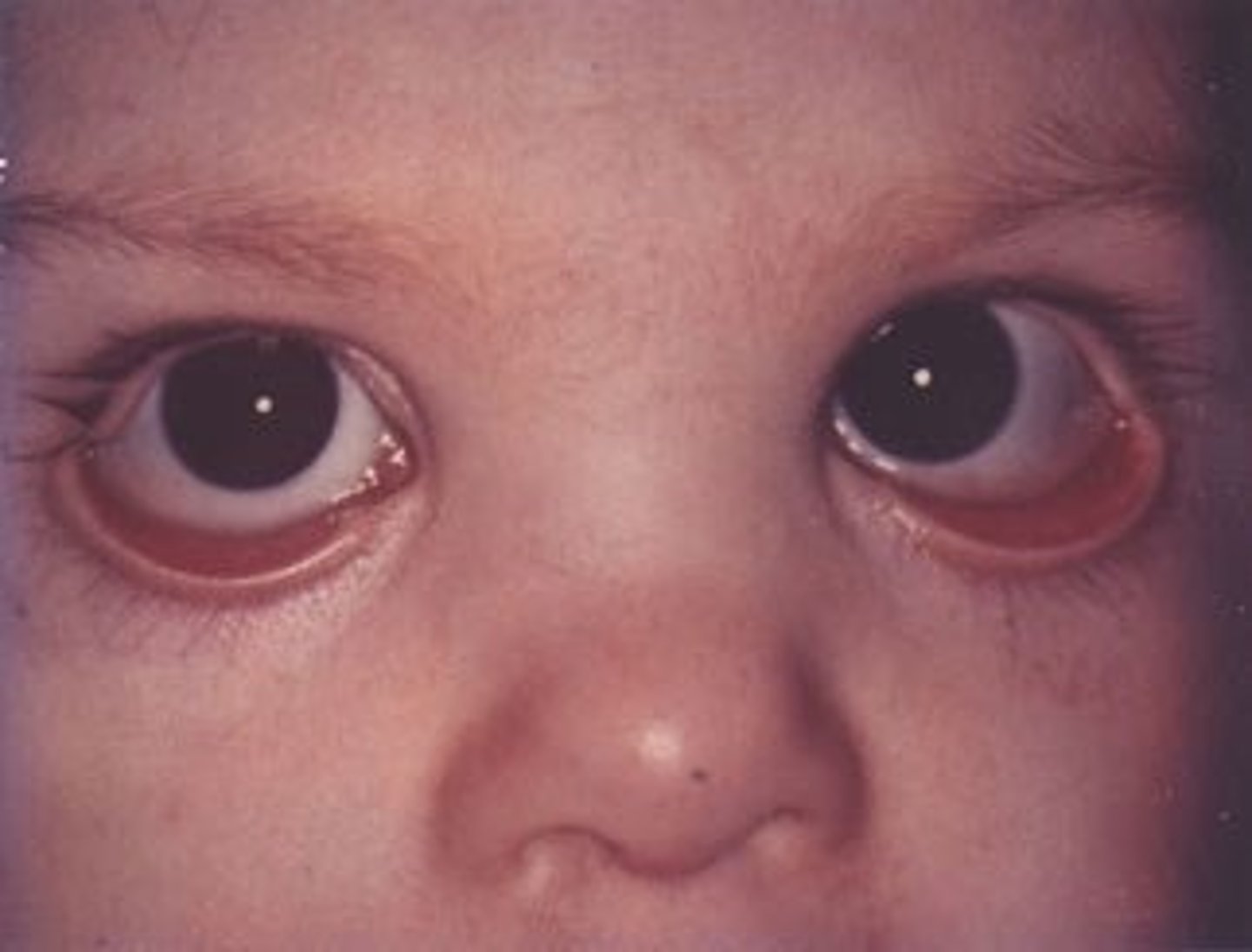
What are 2 conditions a child can be born with that would cause them to have congenital ectropion?
blepharophimosis, Down's syndrome
What are 4 common forms of entropion/ectropion testing?
orbicularis override test, MRD 2, snap back test, lid distraction test
How do we conduct the orbicularis override test to look for entropion/ectropion?
ask patient to forcibly blink and look for internal rotation of lid or lagophthalmos
There are many measurements that we can take involving the pupil, lid margins, and palpebral fissure in general, but one that is important for entropion/ectropion testing is MRD 2. How do we measure this?
from corneal reflex in pupil to lower lid margin
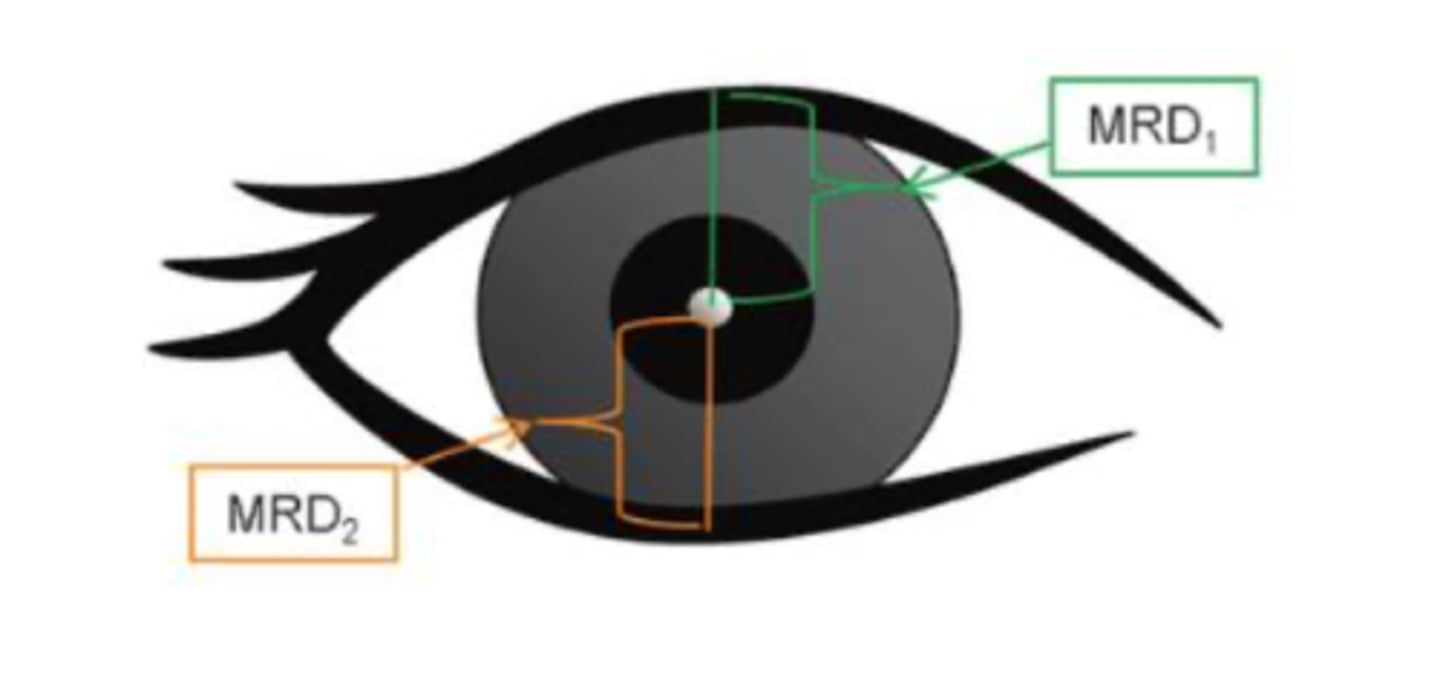
What is a normal approximate MRD 2 value?
5 mm
How do we conduct the snap back test to look for entropion/ectropion?
pull patient's lower lid down then let go and evaluate how soon it returns to normal position
You perform the snap back test on your patient to evaluate for possible entropion/ectropion and it returns to position immediately. What grade do we give their lid?
normal
You perform the snap back test on your patient to evaluate for possible entropion/ectropion and it returns to position after 2-3 seconds. What grade do we give their lid?
grade 1
You perform the snap back test on your patient to evaluate for possible entropion/ectropion and it returns to position after 4-5 seconds. What grade do we give their lid?
grade 2
You perform the snap back test on your patient to evaluate for possible entropion/ectropion and it returns to position after 5 seconds and requires blinking. What grade do we give their lid?
grade 3
You perform the snap back test on your patient to evaluate for possible entropion/ectropion and it returns slightly but continues hanging down. What grade do we give their lid?
grade 4
How do we conduct the lid distraction test to look for entropion/ectropion?
pull the lid away from the globe and measure how far it can be pulled out
What is considered abnormal for the lid distraction test?
>6 mm
What are 6 temporary fixes for entropion?
lubrication, bandage CLs, lid taping, lash epilation, Botox, Quickert sutures
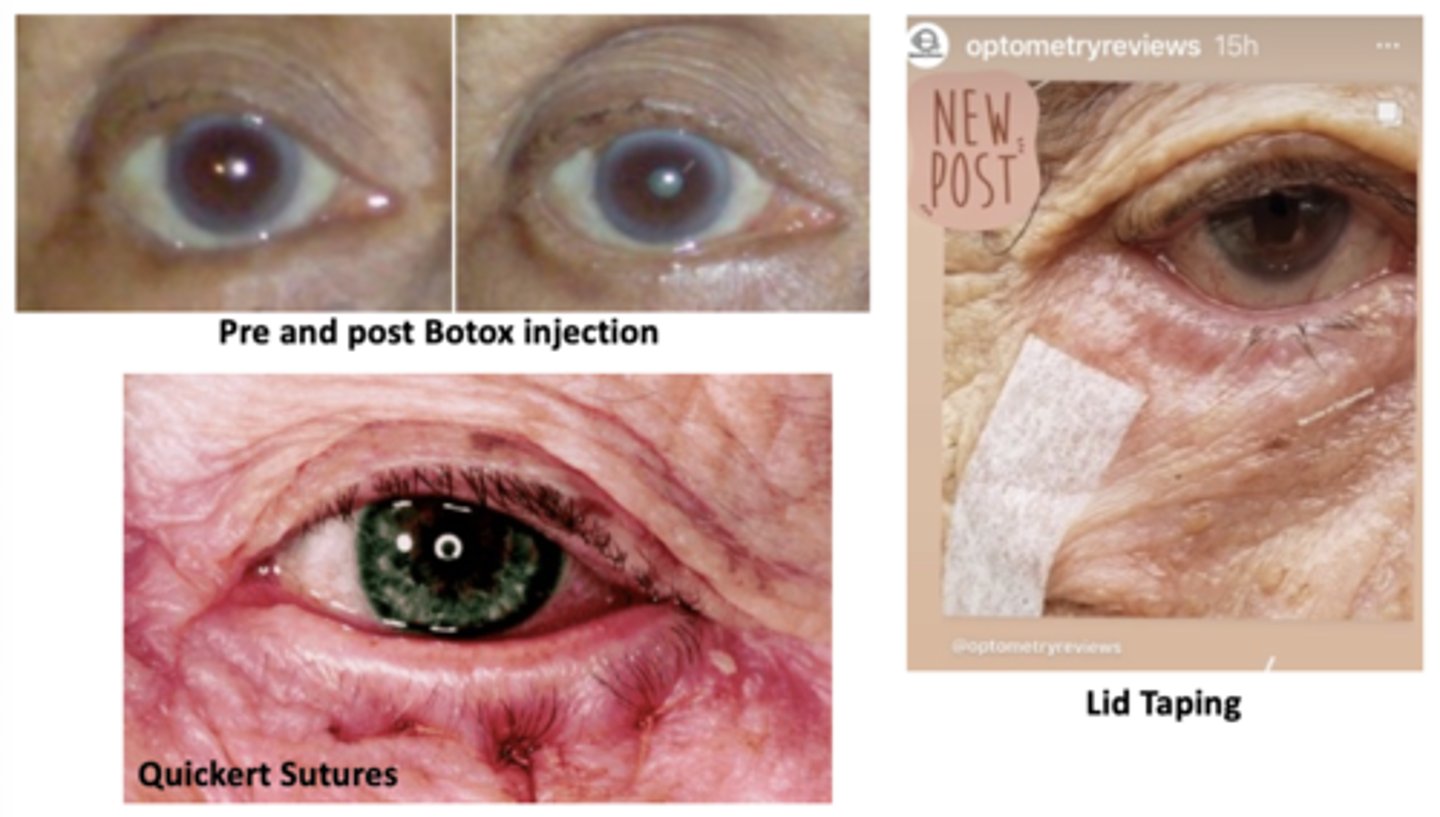
What are 4 permanent fixes for entropion?
eyelash removal, membrane grafts, antibiotics or immunosuppressives to treat underlying cause, surgery
What are 4 temporary fixes for ectropion?
lubrication, bandage CLs, lid taping, tarsorrhaphy
What are 2 permanent fixes for ectropion?
tarsorrhaphy, surgery
ptosis
ABNORMAL LID POSITION
--droopy eyelid
--may be congenital or acquired
--"pseudo" if caused by something that makes the lid droop that is NOT a muscle issue
EVALUATION:
--levator function
--marginal limbal distance
--marginal crease distance
--Bell's phenomenon
--Hering's law
--fatiguability test
--ice pack test
--visual field
TREATMENT:
--monitor via cosmetic appearance and visual fields
--assess for underlying systemic issue
--eyelid taping
--alpha adrenergic eyedrops (Upneeq)
--ptosis crutch built in to glasses
--scleral lenses
--surgery
What is the difference between ptosis and pseudoptosis?
pseudoptosis is caused by something that makes the lid droop but not a muscle issue, whereas ptosis is more of an underlying nerve/muscle issue
dermatochalasis
TYPE OF PSEUDOPTOSIS
--age related "sagging" skin of the upper & lower lids
--more common in males
ASSOCIATED WITH:
--poor cosmesis
--eyelash ptosis
--VF defect
--dry eye
--epiphora
TREATMENT: lid surgery
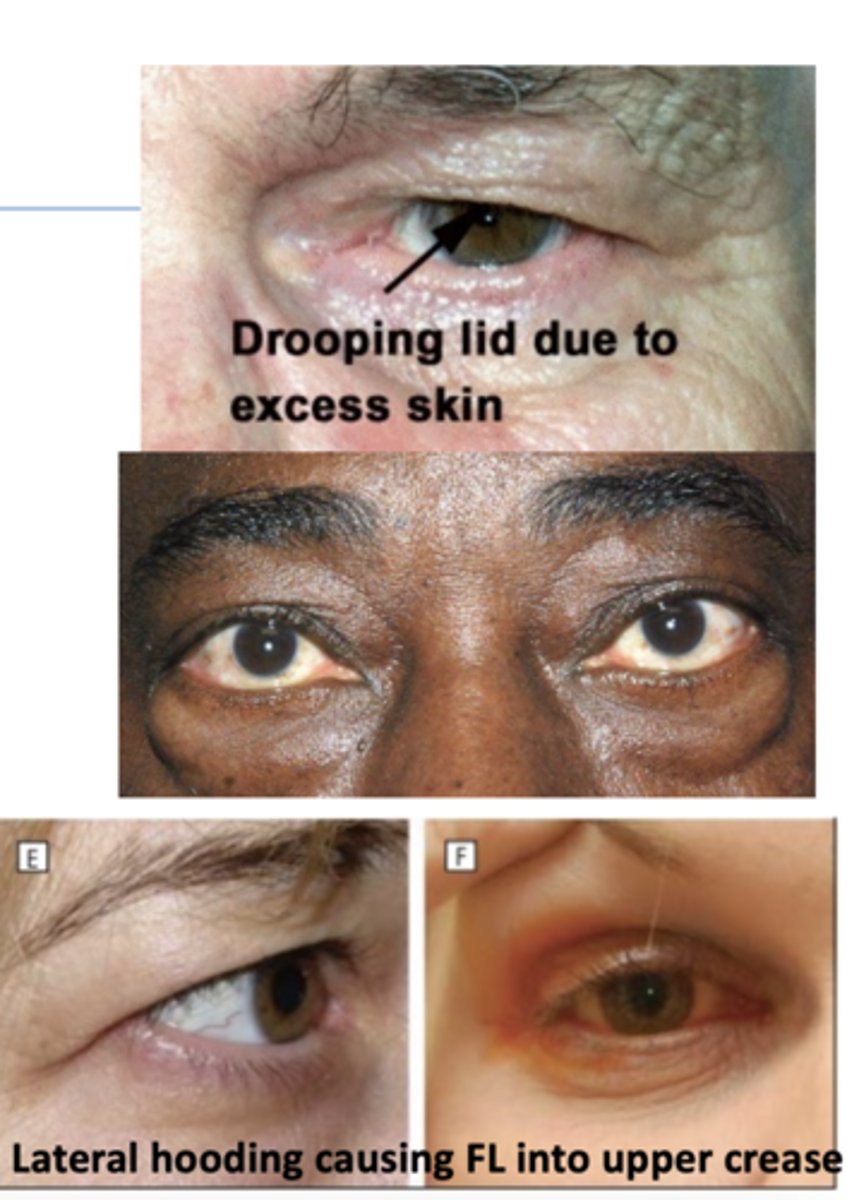
Who gets dermatochalasis more commonly: males or females?
males
What are 5 issues commonly associated with dermatochalasis?
poor cosmesis, eyelash ptosis, VF defect, dry eye, epiphora
How do we treat dermatochalsis to improve a patient's pseudoptosis?
lid surgery
blepharochalasis
TYPE OF PSEUDOPTOSIS
--intermittent, painless upper lid edema
--spontaneous resolution
--thin, wrinkled "tissue paper" lids with discolored periorbital skin
--unknown triggers and pathogensis
--starts in childhood, improves with age
--no gender predilection
--leads to aponeurotic disinsertion
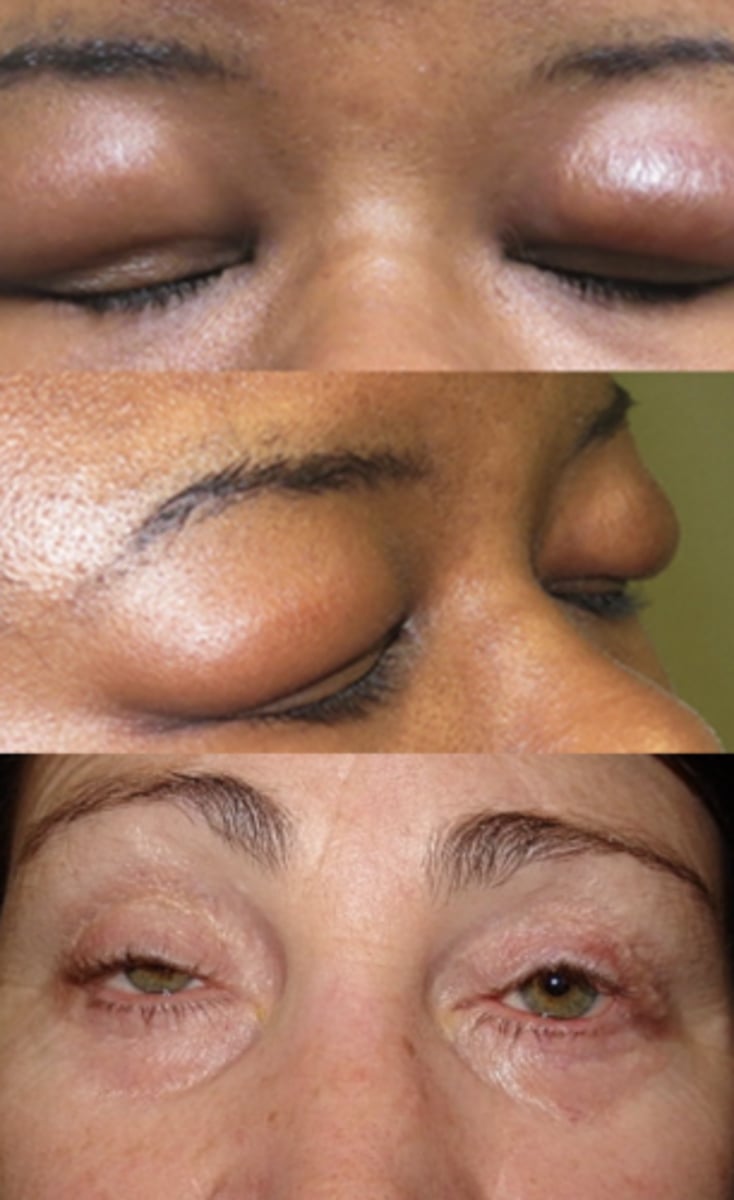
floppy eyelid syndrome
TYPE OF PSEUDOPTOSIS
--generalized laxity of lid tissues
--associated with sleep position if unilateral
SYMPTOMS:
--easy superior lid eversion
--mechanical irritation (pap. conjunctivitis or dry eye)
--lid and eyelash ptosis
--ropy discharge
--lagophthalmos
--ectropion
ASSOCIATED WITH:
--obstructive sleep apnea (in obese, middle aged men)
--alcohol use
--keratoconus
--glaucoma
--non-arteritic anterior ischemic optic neuropathy
TREATMENT:
--treat ocular surface disease
--overnight shield
--lid tape
--eyelid surgery
--treat obstructive sleep apnea

Other than obstructive sleep apnea (OSA), what are 4 other associations with FES?
alcohol use, keratoconus, glaucoma, NA-AION (non-arthritic anterior ischemic optic neuropathy)
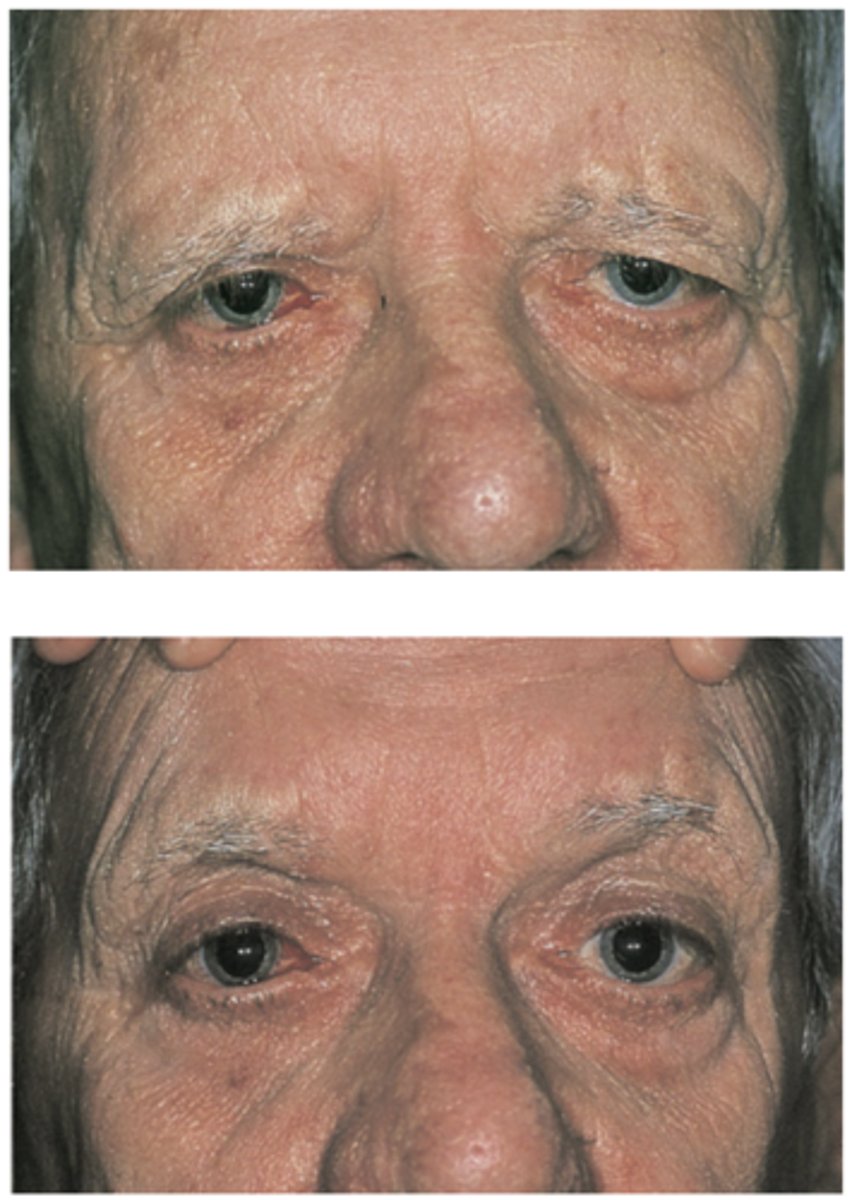
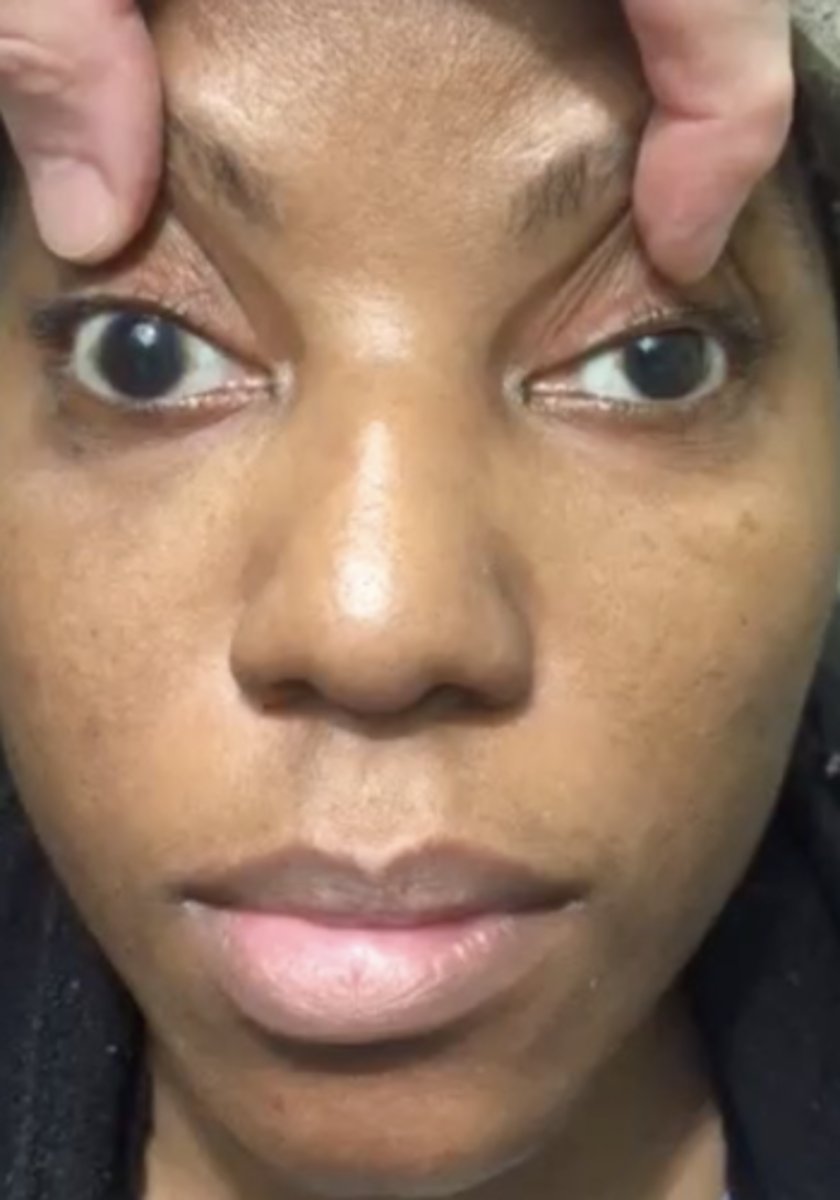
brow ptosis
TYPE OF PSEUDOPTOSIS
--laxity of the connective tissue or skin of the frontalis muscle
--causes descent of the brow fat pad
--more noticeable temporally
--associated with dermatochalasis and ptosis (lift brow to differentiate)
--typically acquired due to age or trauma
TREATMENT:
--fillers/Botox
--brow lift
What are some temporary and permanent fixes for brow ptosis? (3)
fillers and Botox for temporary fix, brow lift for permanent solution
myokymia
TYPE OF PSEUDOPTOSIS
--eyelid "twitch"
--painless, involuntary, fine, continuous, undulating contractions
--involuntary misfiring of the neurons that innervate the orbicularis oculi and Muller's muscle
--usually benign, self limiting unless it involves other facial muscles (sign of intracranial mass)
--occurs in younger patients
CAUSES:
--fatigue, stress, physical exertion
--caffeine or alcohol
--tobacco
--post COVID
TREATMENT:
--remove offending agent
--reassurance
--antihistamines
--Botox
--possibly tonic water?
A 21 y/o patient comes in complaining of an "annoying eyelid twitch" (no other involvement). Confident in what you've learned in Anterior Segment, you tell her that this is simply just myokymia, an involuntary misfiring of the neurons that innervate the orbicularis oculi and Muller's muscles, and that it is nothing to worry about. She doesn't really know what any of that means and just wants to know what is causing it. What are 5 common causes of myokymia?
fatigue/stress, caffeine, alcohol, tobacco, COVID
Your patient with myokymia just wants to know how to get rid of her twitch and go about her day. What are 4 possible treatment options you can tell her about?
antihistamines, Botox, tonic water, remove offending agents (get better sleep, relieve stress better, less caffeine, etc.)
A congenital ptosis may be isolated or the result of cranial dysinnervation disorders. If it is isolated, then what is the typical cause?
unilateral, abnormal development of LPS (and maybe Muller's muscle too)
Will you still see an upper lid crease with an isolated congenital ptosis?
no
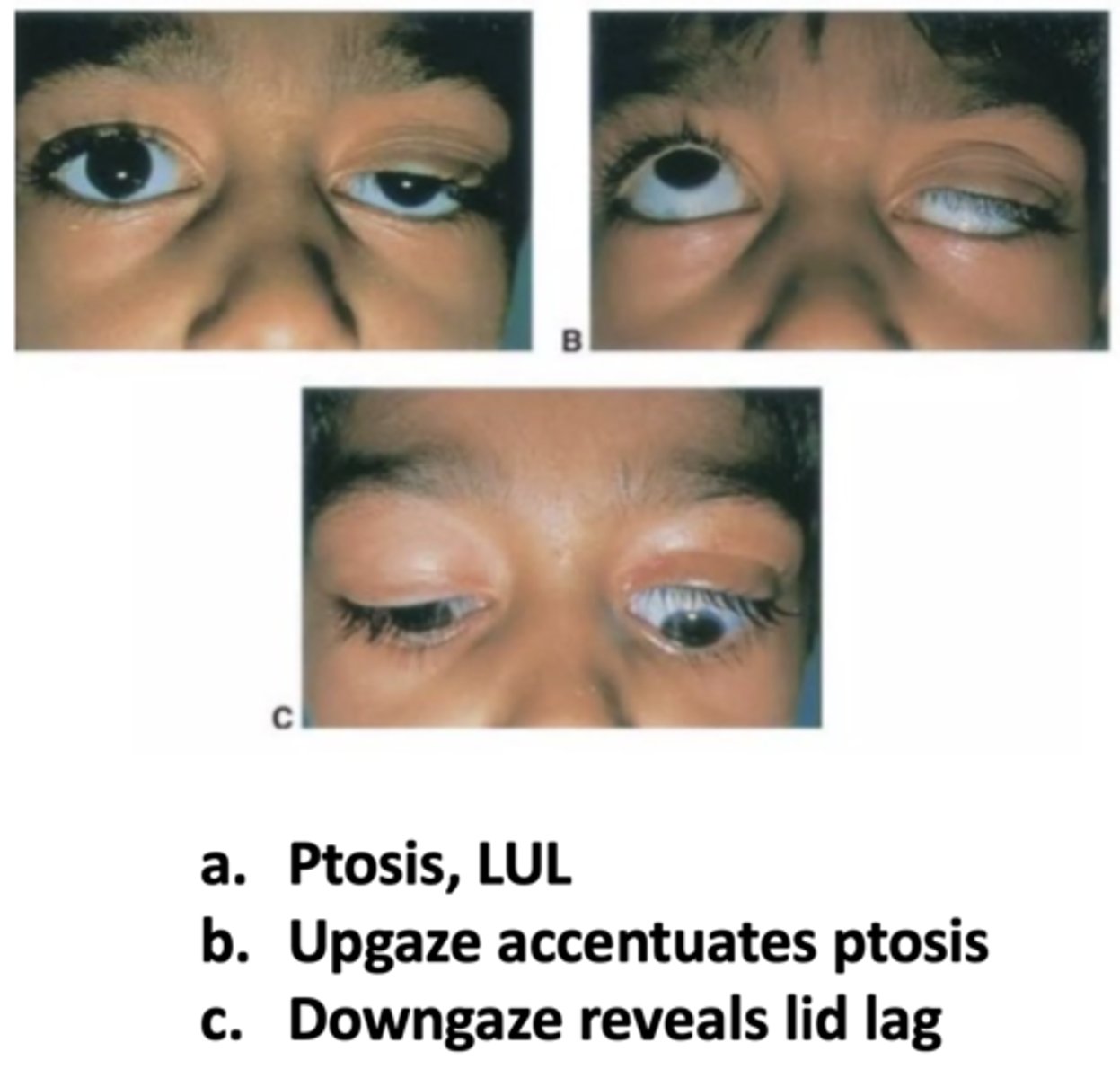
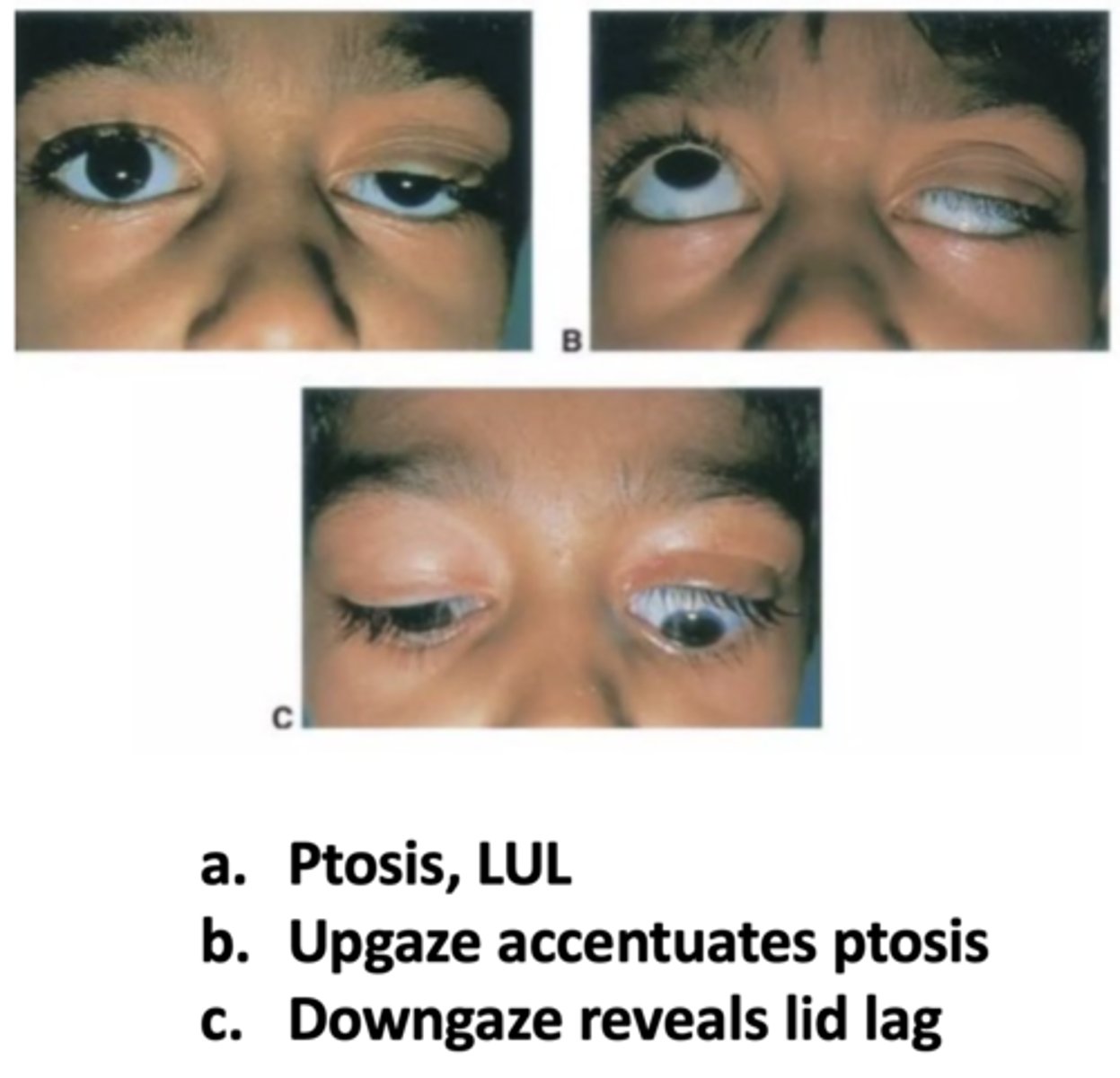
If a patient has an isolated congenital ptosis, how will it appear in upgaze?
more apparent
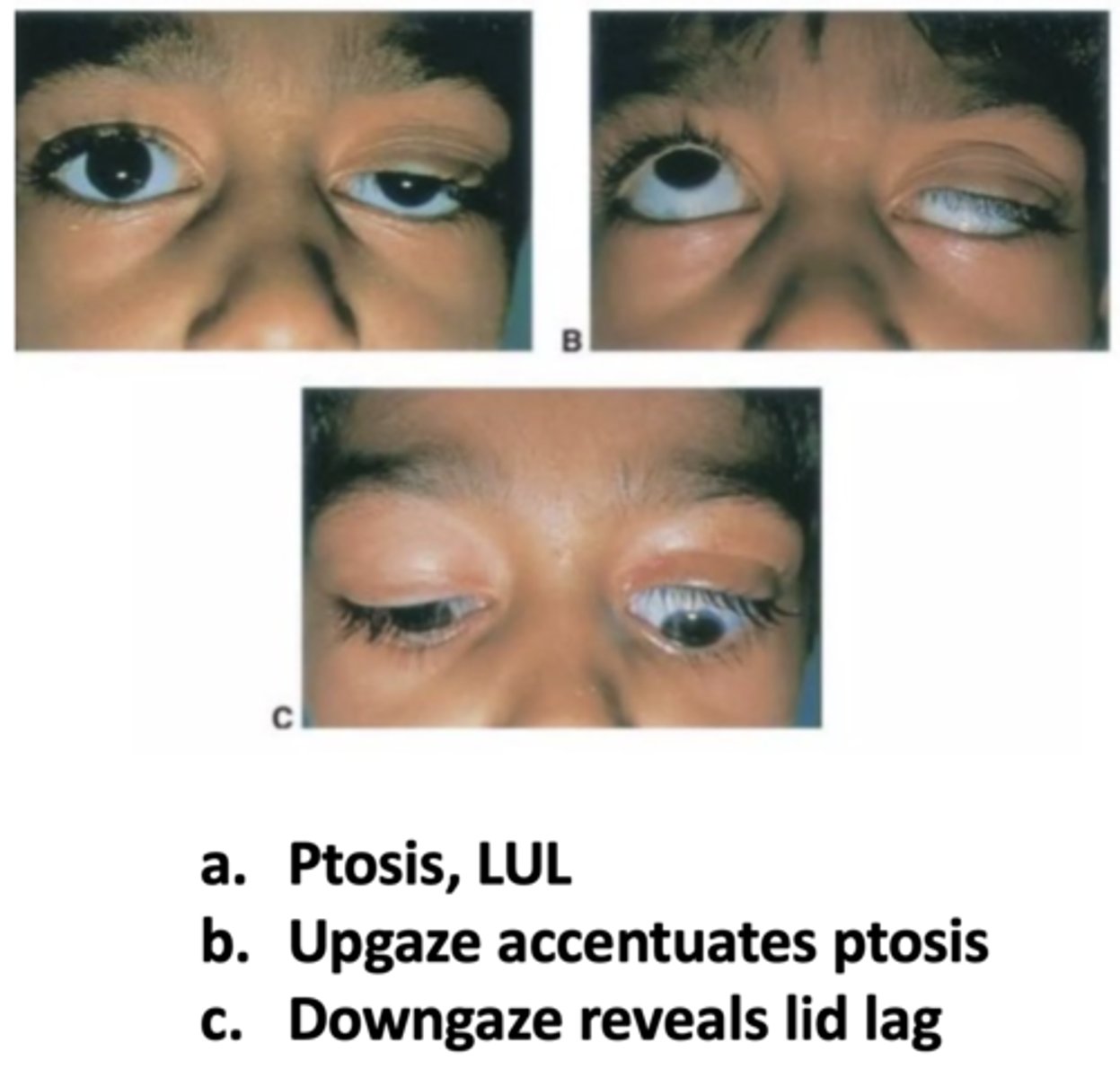
If a patient has an isolated congenital ptosis, how will it appear in downgaze?
lid lag
blepharophimosis, ptosis, & epicanthus inversus syndrome (BPES)
CAUSE OF CONGENITAL PTOSIS
--caused by maldevelopment of brainstem and/or cranial nerves
--non-progressive
--causes ptosis, narrow fissure, wide set eyes, and poorly developed nasal bridge and superior orbital rims
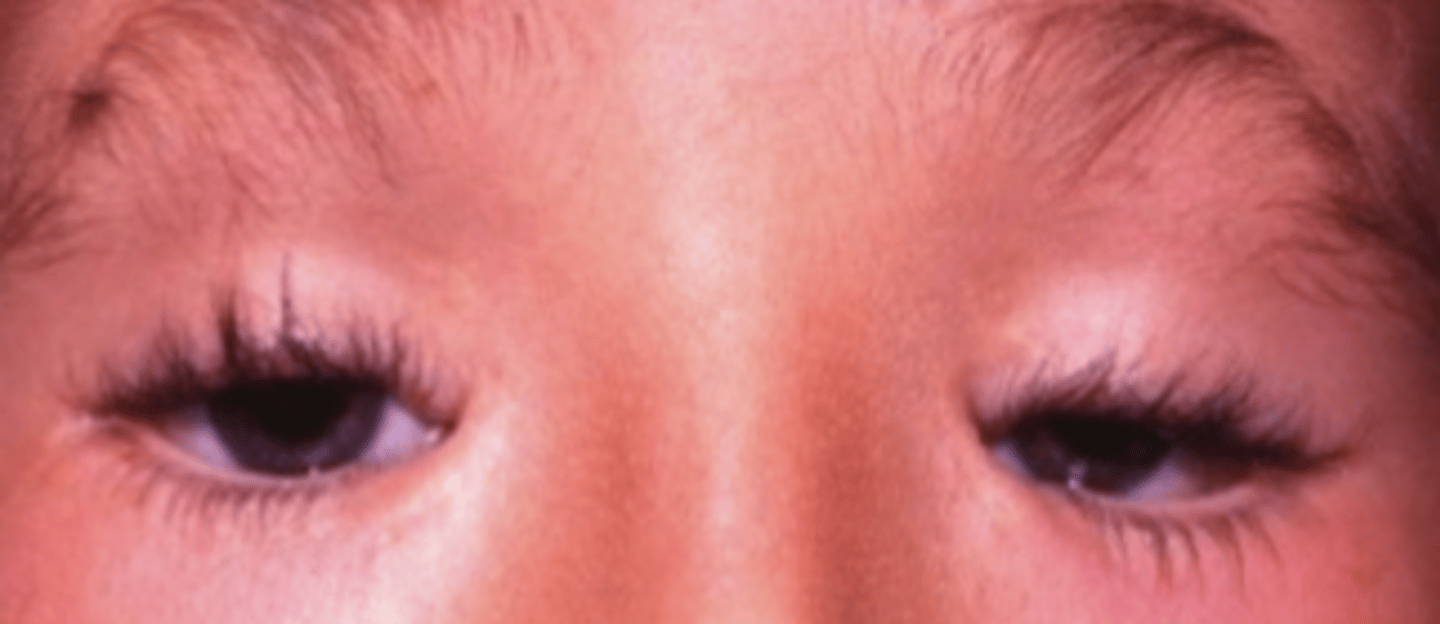
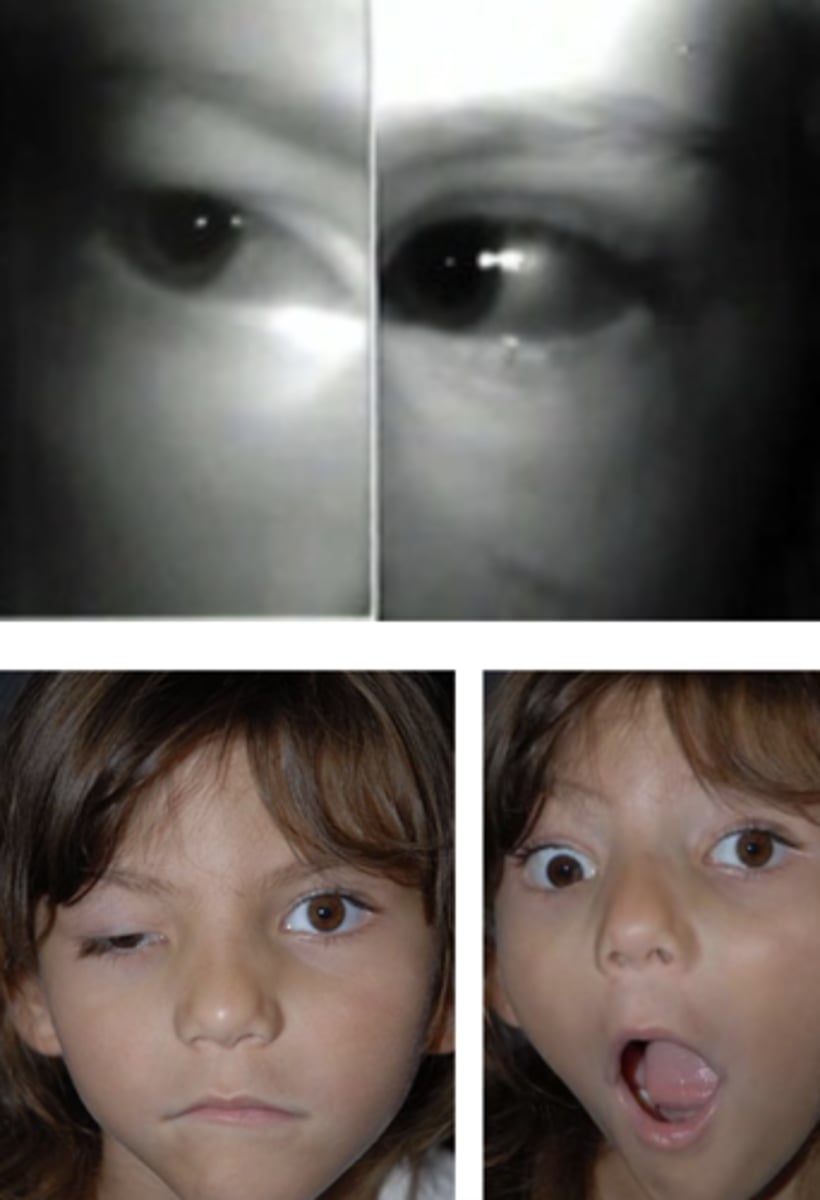
Marcus-Gunn jaw winking syndrome
CAUSE OF CONGENITAL PTOSIS
--aberrant innervation of the LPS by CN V3
--elevation of the ptotic lid with chewing, sucking, or opening of mouth
--kid opens mouth = eye elevates
--doesn't improve with age
TREATMENT: surgery if it interferes with vision or for cosmesis
What are the 5 types of acquired ptosis?
aponeurotic, traumatic, mechanical, myogenic, neurogenic
If LPS function is normal in aponeurotic ptosis, then what causes the eyelid to droop?
LPS aponeurosis is inserted improperly or loosened from its tarsal attachment
What might cause the LPS aponeurosis to loosen/disinsert from its tarsal attachment, causing aponeurotic ptosis? (4)
CL wear, eye rubbing, trauma, surgery
What is characteristic of the ipsilateral eyebrow in aponeurotic ptosis?
elevated
(causing high or absent lid crease)
Such as in someone with isolated congenital ptosis, is there a lid lag in downgaze for someone with acquired aponeurotic ptosis?
no
myogenic ptosis
CAUSE OF ACQUIRED PTOSIS
--dysfunction of LPS
--also includes restricted EOMs and facial expressions
--may result from MG, CPEO, or myotonic dystrophy
How is myogenic ptosis different from aponeurotic ptosis?
myogenic is caused by dysfunctional LPS itself, aponeurotic is improper LPS aponeurosis attachment to tarsal plate
What are 3 examples of diseases that can demonstrate myogenic ptosis as a sign?
MG, CPEO, myotonic dystrophy
Who most commonly gets MG?
young females, older men
What is a characteristic ocular sign of MG that accompanies ptosis?
Cogan's lid twitch
If a patient has a ptosis and (+) Cogan's lid twitch, 1) what should you suspect that they have? 2) What do you see with this lid twitch?
MG, overshoot in upgaze after downgaze (lid twitches when looking back up after looking down)
chronic progressive external ophthalmoplegia (CPEO)
HEREDITARY MYOPATHY - cause of MYOGENIC PTOSIS
--mitochondrial myopathy that may be hereditary or sporadic
--no treatment
--bilateral, symmetric ptosis
--no diplopia
--eye muscles are vulnerable due to large volume of mitochondria
--atrophy of facial muscles leads to "masked face"
--possible variant: Kearns-Sayre
Is a bilateral ptosis caused by CPEO symmetrical or asymmetrical?
symmetrical
Is a ptosis caused by CPEO unilateral or bilateral?
bilateral
Do patients with CPEO experience diplopia?
no
Why are eye muscles so vulnerable to CPEO?
they have lots of mitochondria to be messed up
Why do we see a "masked face" with CPEO?
patient has atrophy of facial muscles
myotonic dystrophy
GENETIC DISEASE -- cause of MYOGENIC PTOSIS
--autosomal dominant
--failure of the muscles to relax after contraction
--most common form of adult onset muscular dystrophy
--type 1 (out of 2) is more common and more severe
SYMPTOMS:
--results in bilateral ptosis
--flat facial expression
--early Christmas tree cataract
--frontal baldness, testicular atrophy, DM

Is ptosis caused by myotonic dystrophy unilateral or bilateral?
bilateral
Because myotonic dystrophy causes the muscles to fail to relax after contraction, how does the patient's face appear?
flat facial expression