BIO 300 Lecture12.CardiacDisorders.Part2.pptx
1/58
Earn XP
Description and Tags
BIO 300 Pathophysiology
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
59 Terms
is the leading cause of death in men and women in the U.S.
cardiac disease

Most common heart disease in the U.S.
coronary artery disease

Typically takes years to develop.
Coronary system becomes deficient in supplying blood, oxygen, & nutrients to the heart (aka impaired coronary blood flow).
Triggered by subtle physical or chemical “insults” to the endothelial cell layer of arteries.
coronary artery disease (CAD)

Most common cause for coronary artery disease
atherosclerosis

Says that the earliest event in atherogenesis is injury to the endothelium of vessels.
Injury is triggered by any number of insults, either alone or in combination.
The "Response to Injury Theory"

Physical injury or stress as a result of direct trauma or hypertension.
Turbulent blood flow.
Circulation of reactive free radicals [from smoking, air pollutants, diet, etc.].
Hyperlipidemia (high blood concentrations of LDL or VLDL).
Chronically elevated blood glucose levels.
The "Response to Injury Theory" include
Results from an inherited metabolic defect that leads to very high levels of the homocysteine
homocysteinemia

A metabolite of methionine [from animal protein]; high concentrations are toxic to the endothelium.
homocysteine

Provokes an inflammatory response & other responses
injury to endothelial cells
Monocytes and T-lymphocytes adhere to the endothelium and then migrate beneath it by squeezing between the endothelial cells.
Other circulating monocytes and T-lymphocytes are then attracted to the sites.
coronary artery disease inflammatory response
Endothelial cells change shape = tight junctions between cells loosen = increased permeability = fluid, lipids, LDL, & more leukocytes enter area.
The monocytes differentiate into macrophages and begin to “eat” the LDL.
coronary artery disease other responses
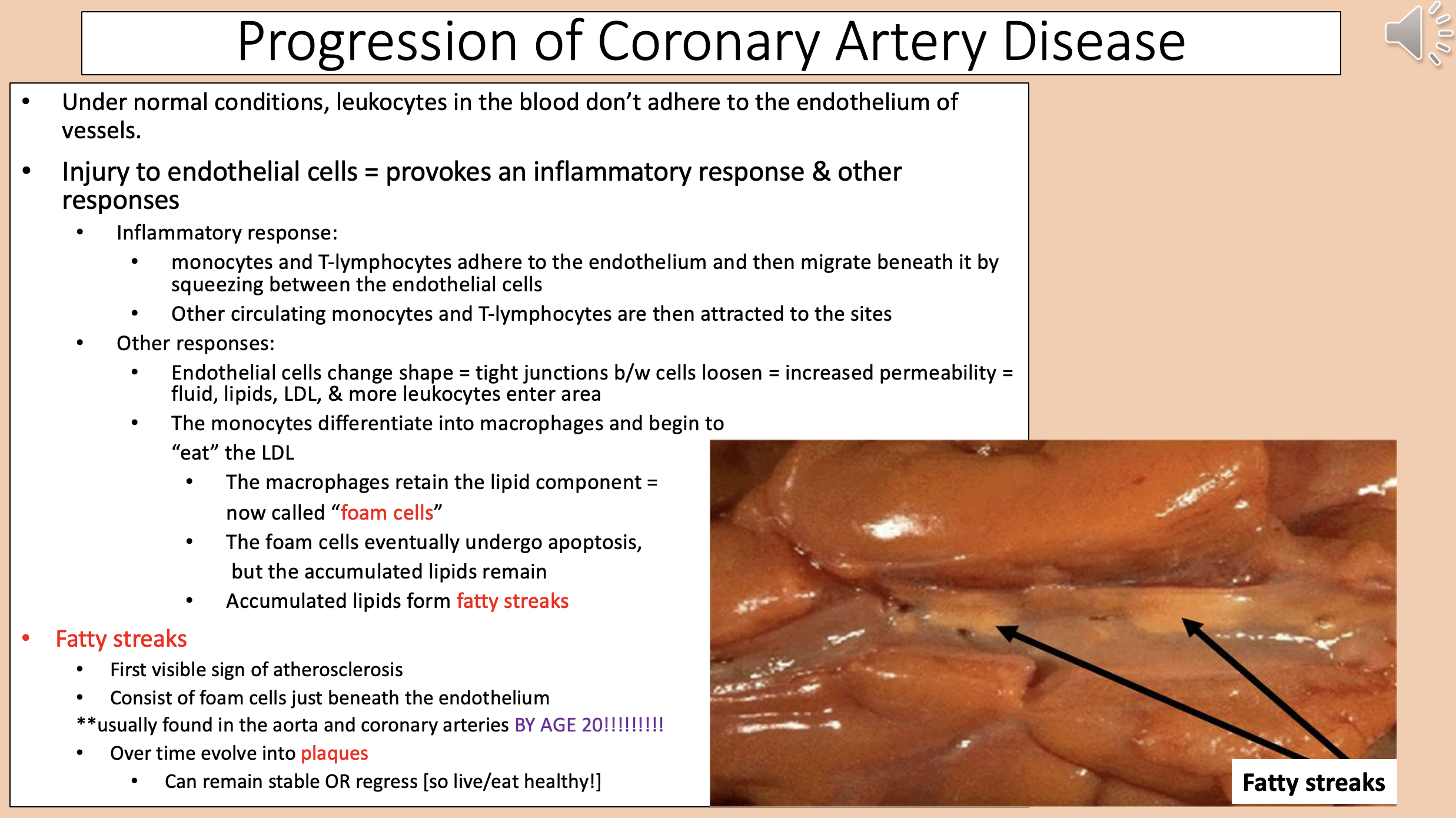
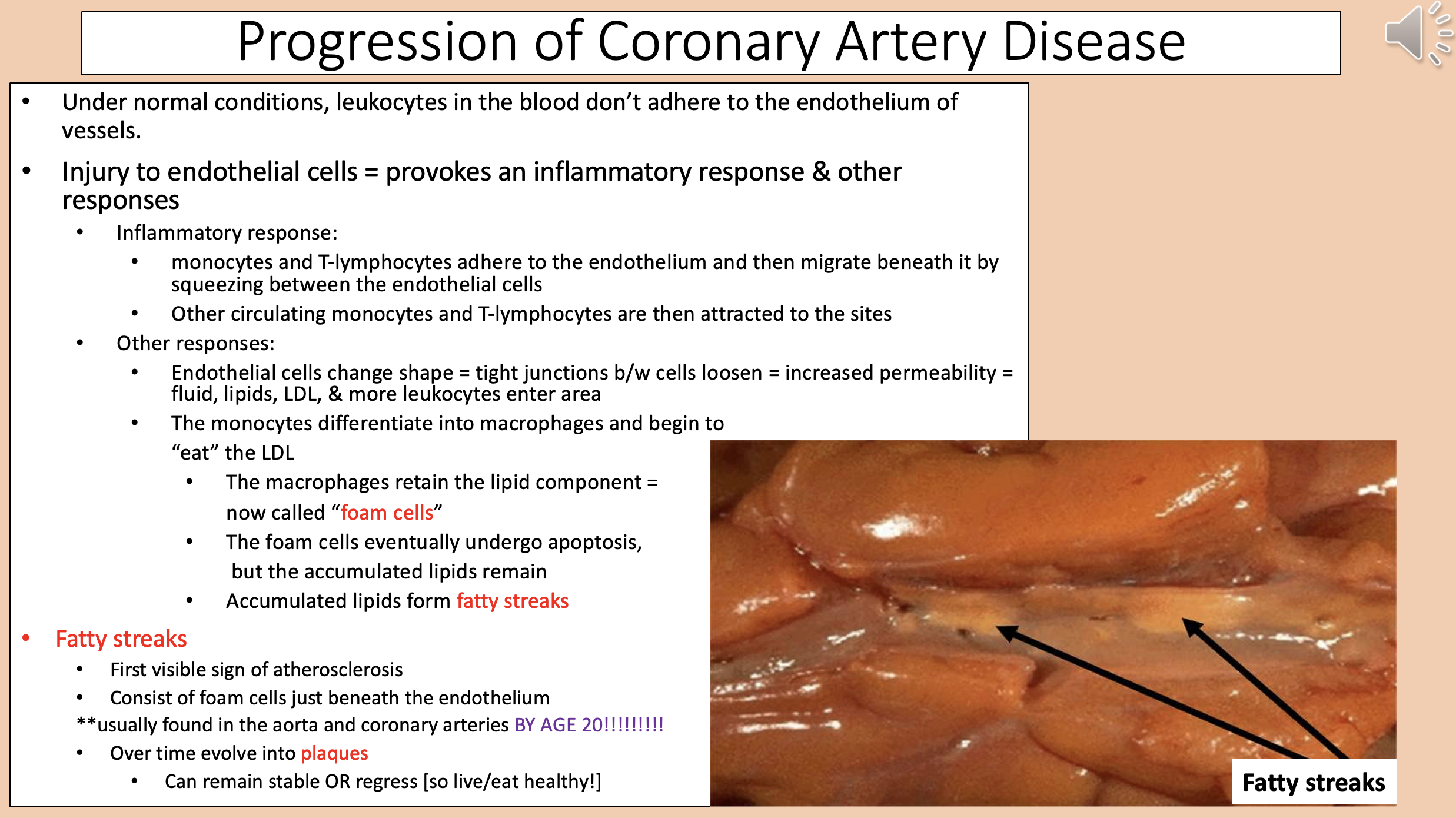
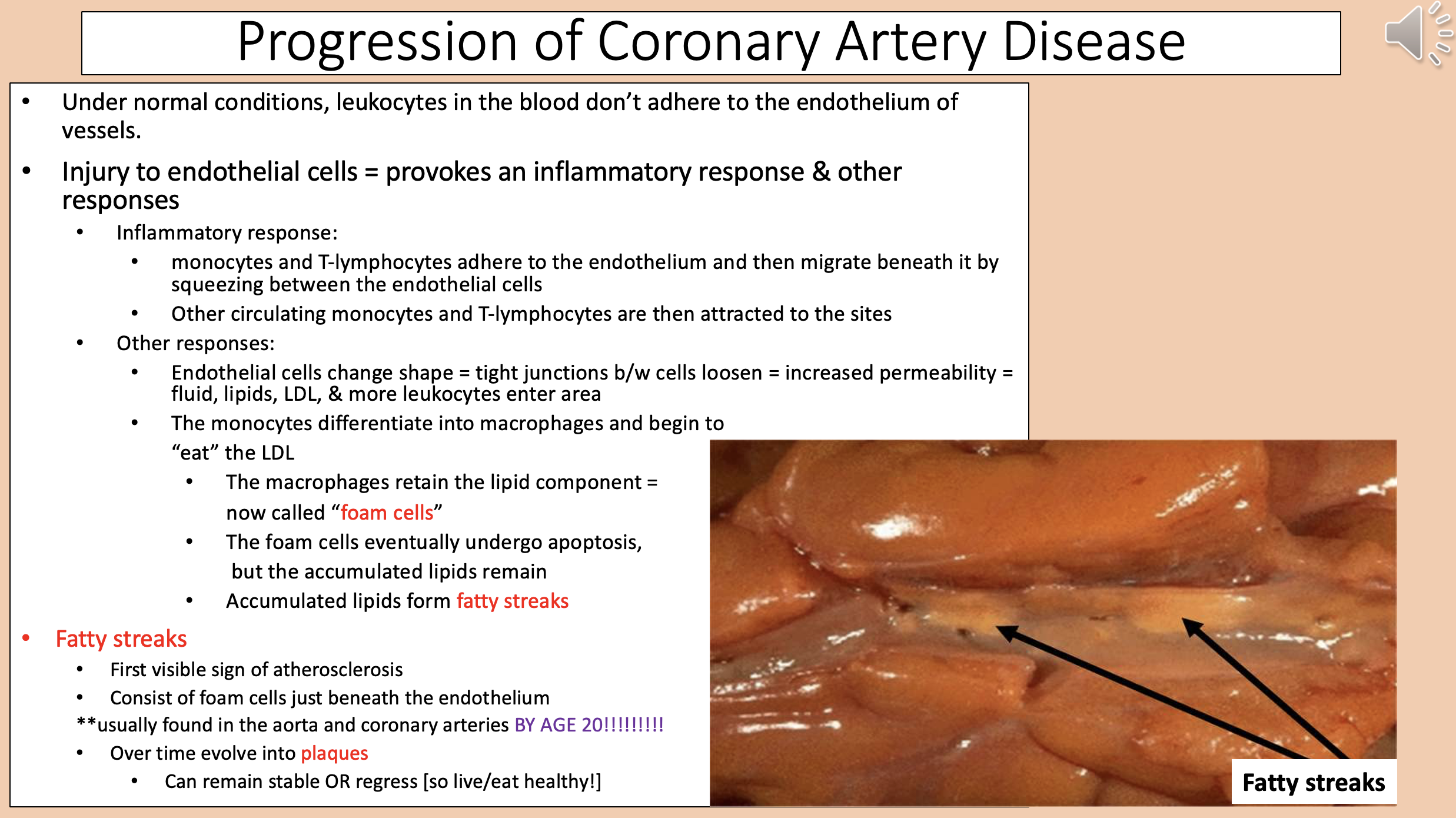
The macrophages retain the lipid component
foam cells
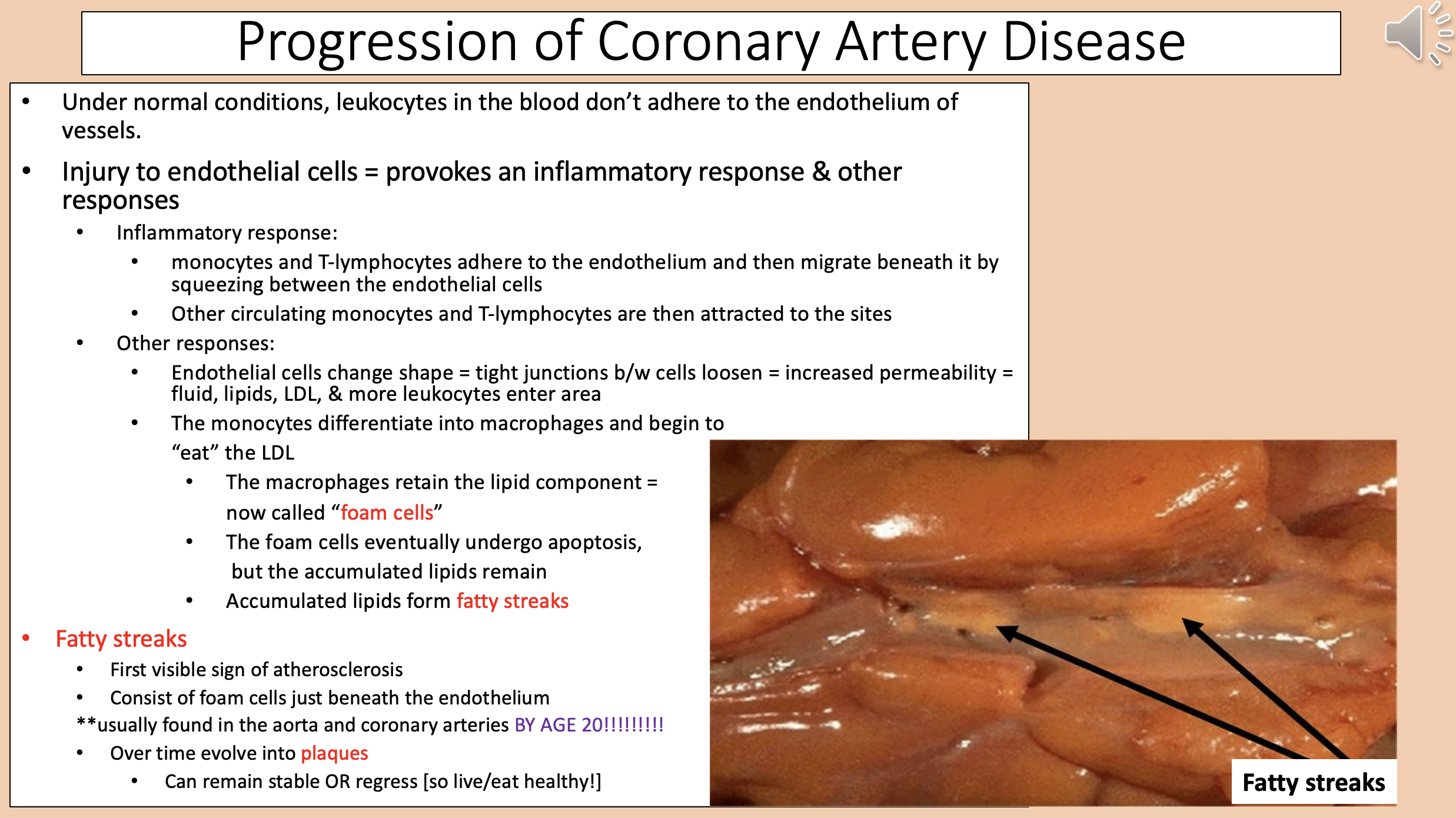
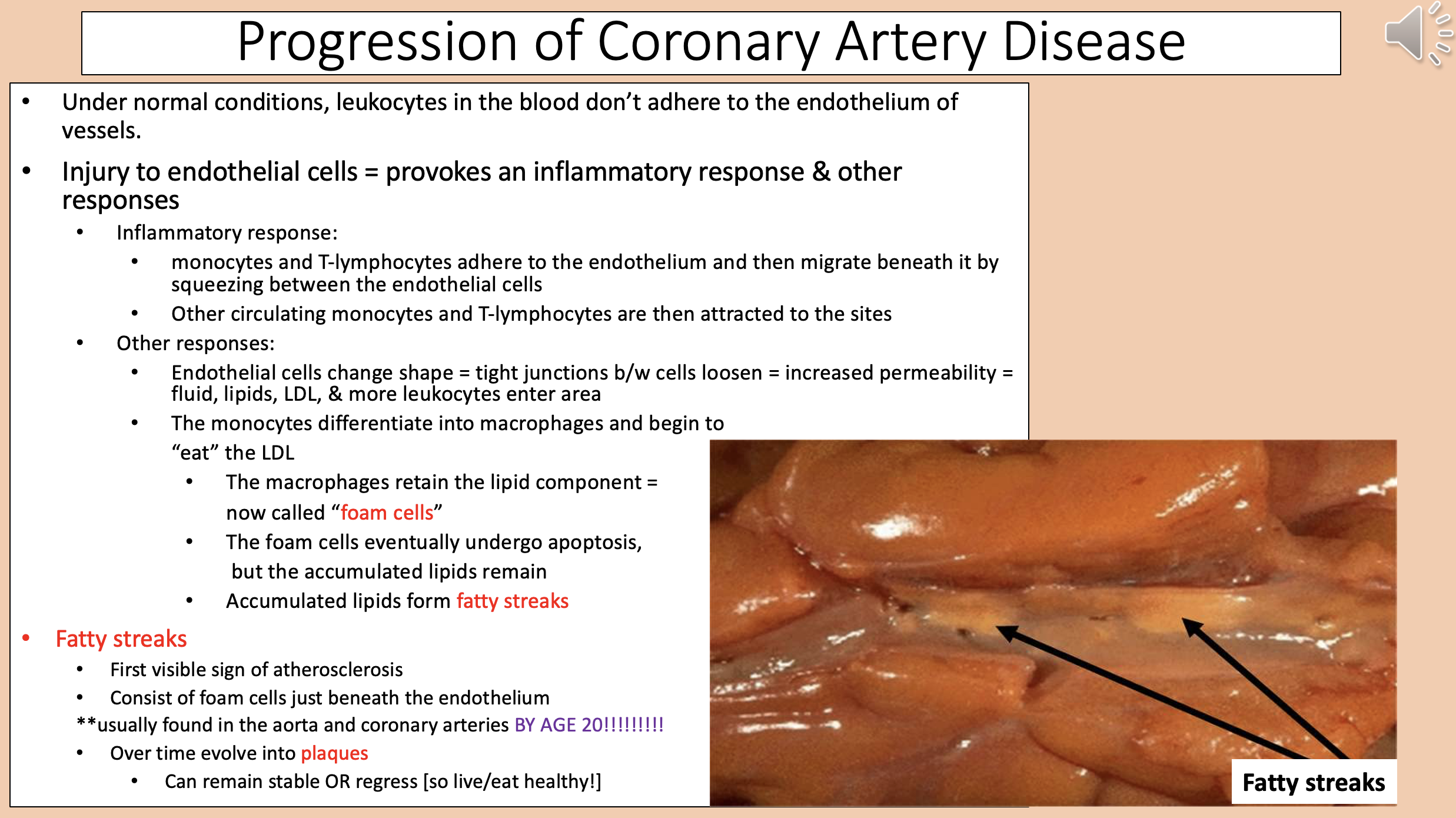
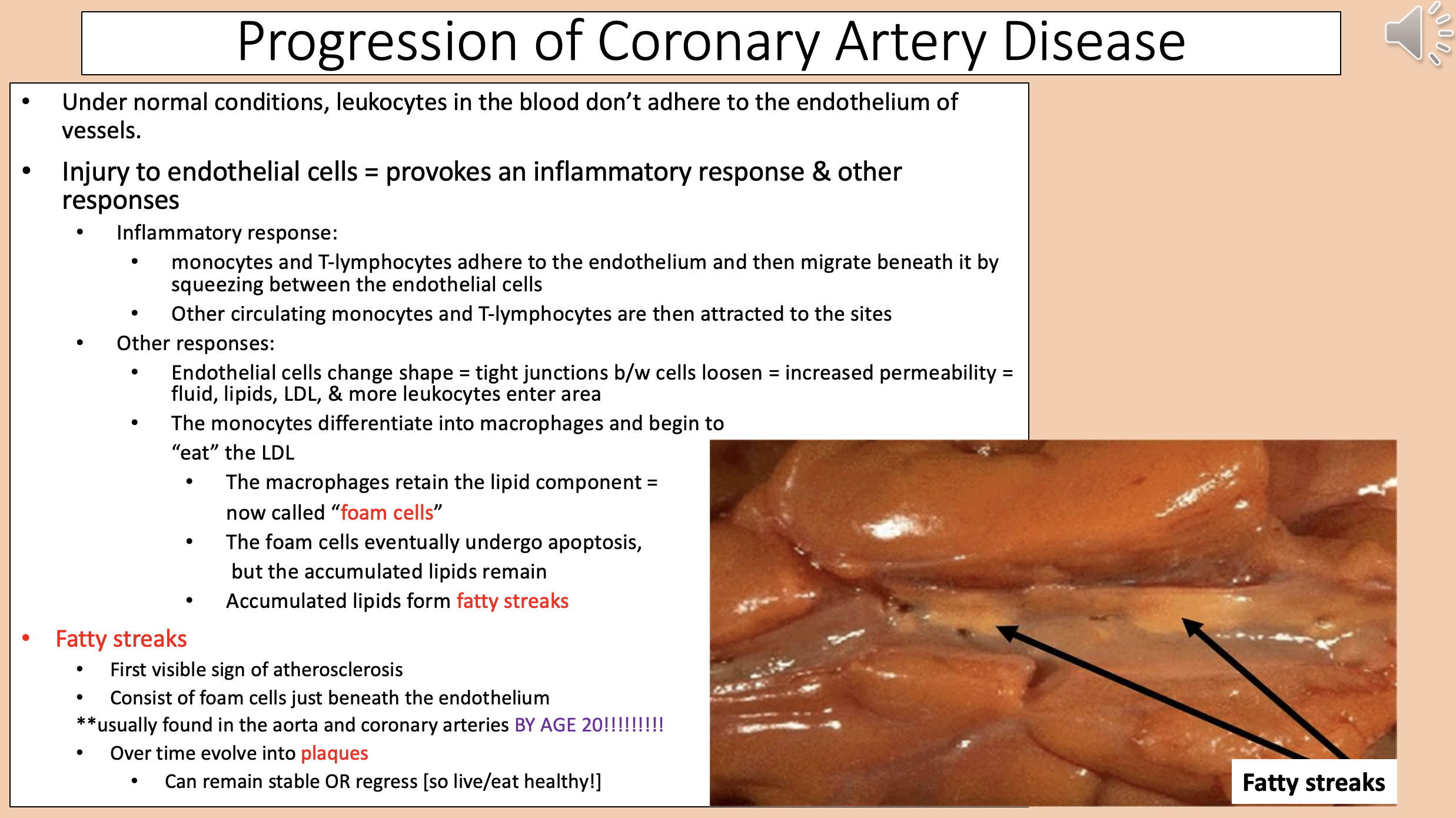
Accumulated lipids form
fatty streaks
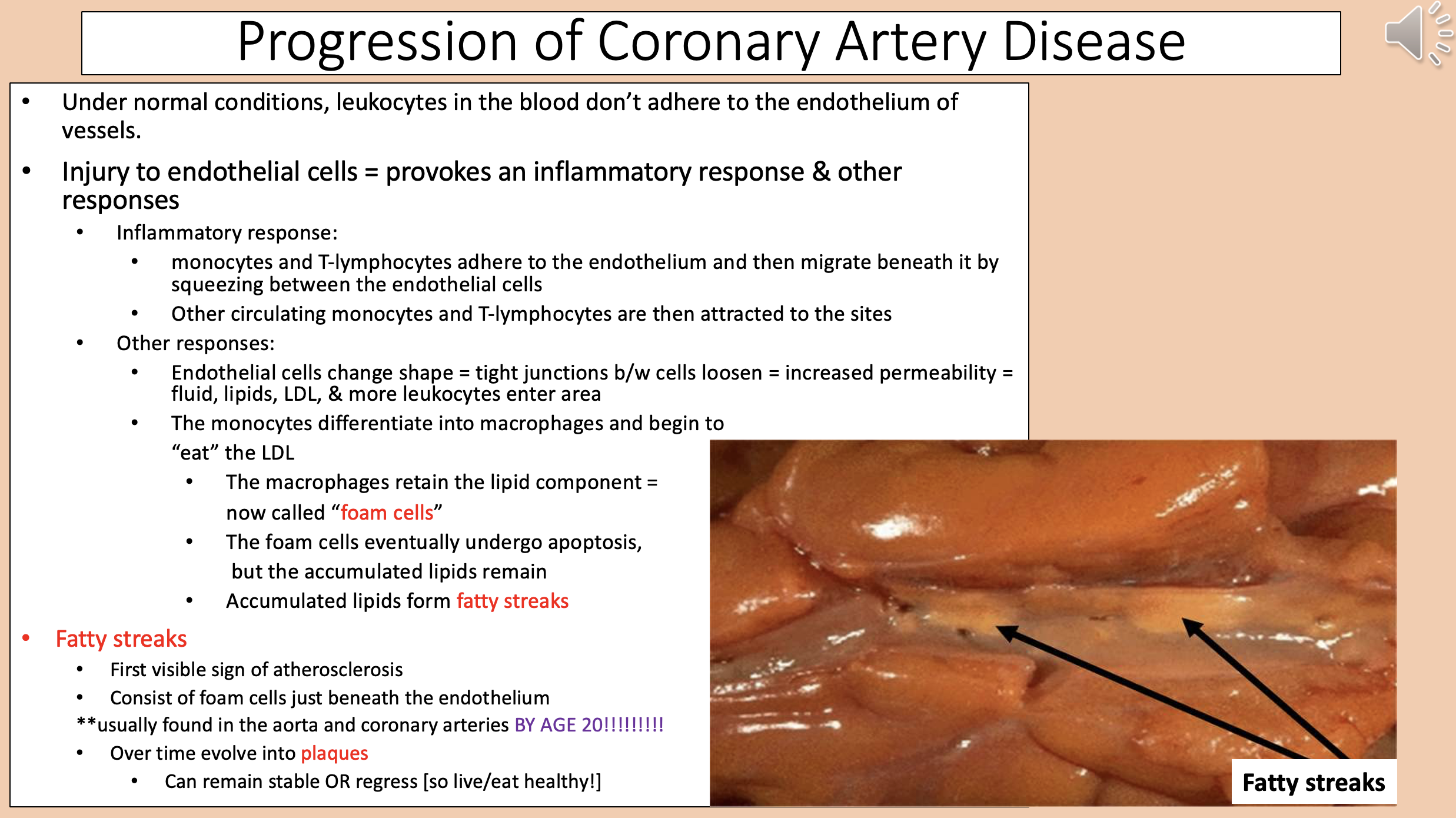
First visible sign of atherosclerosis.
Consist of foam cells just beneath the endothelium.
Usually found in the aorta and coronary arteries BY AGE 20.
fatty streaks
Over time fatty streaks evolve into.
Can remain stable OR regress.
plaques
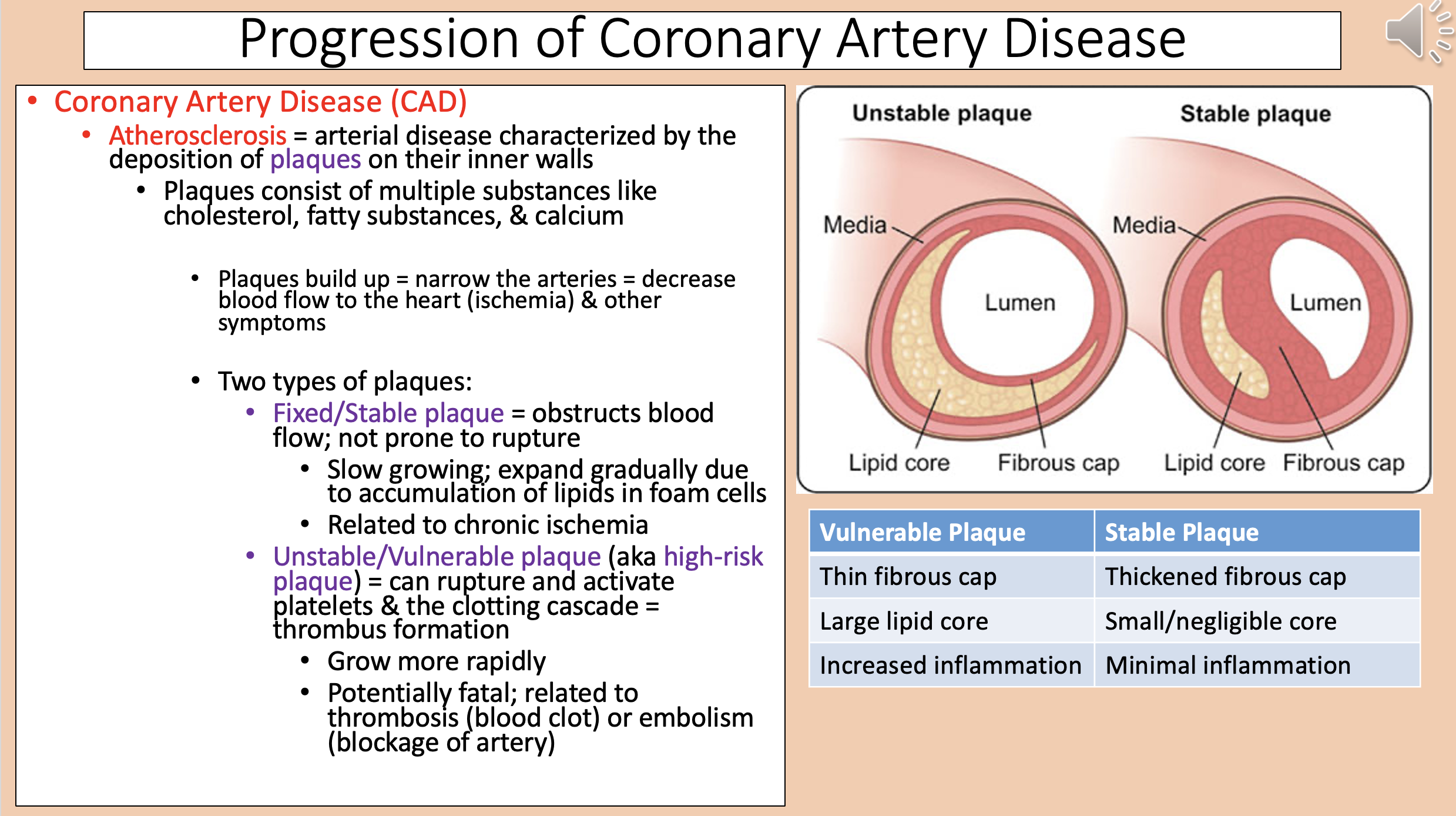
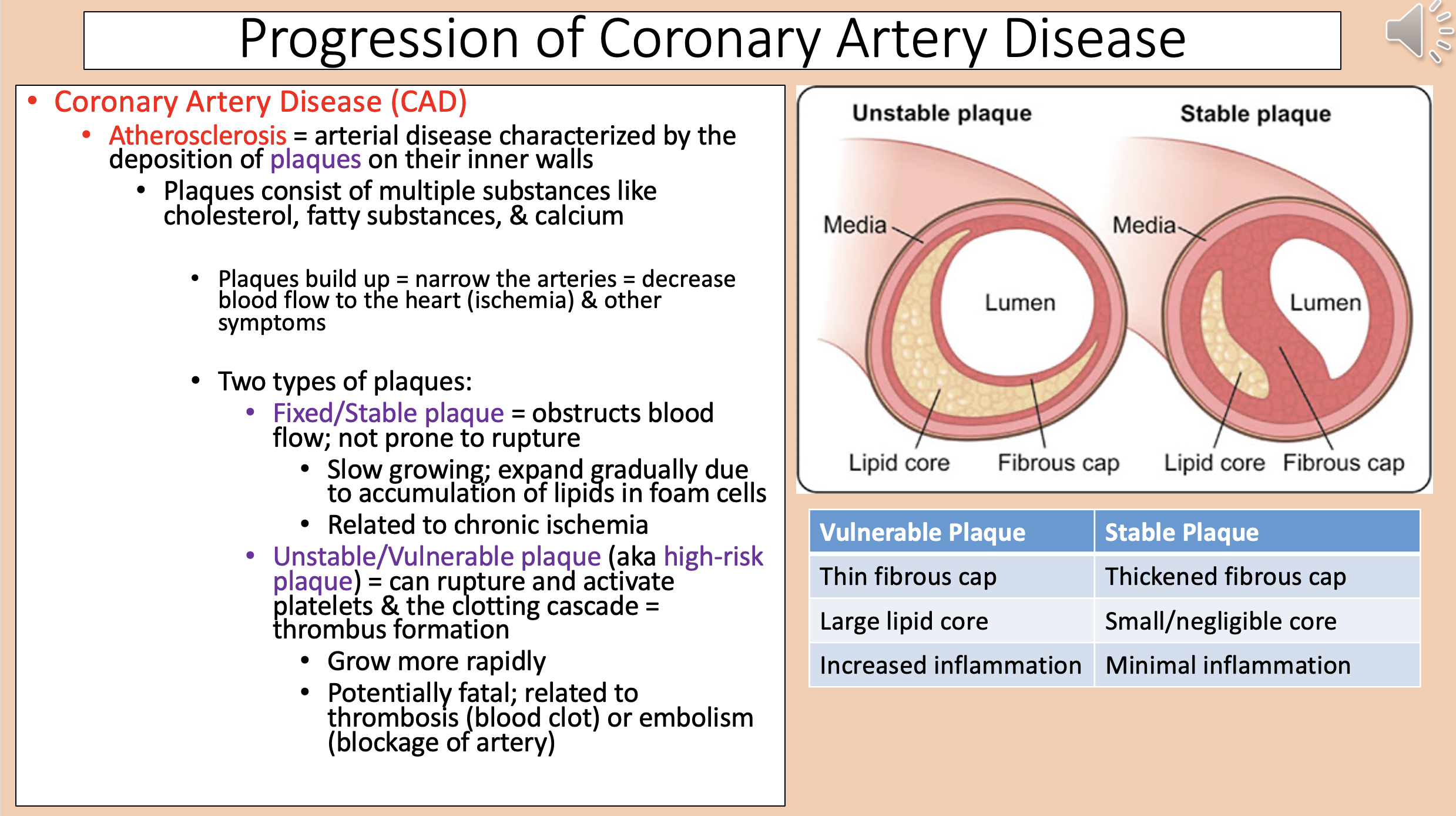
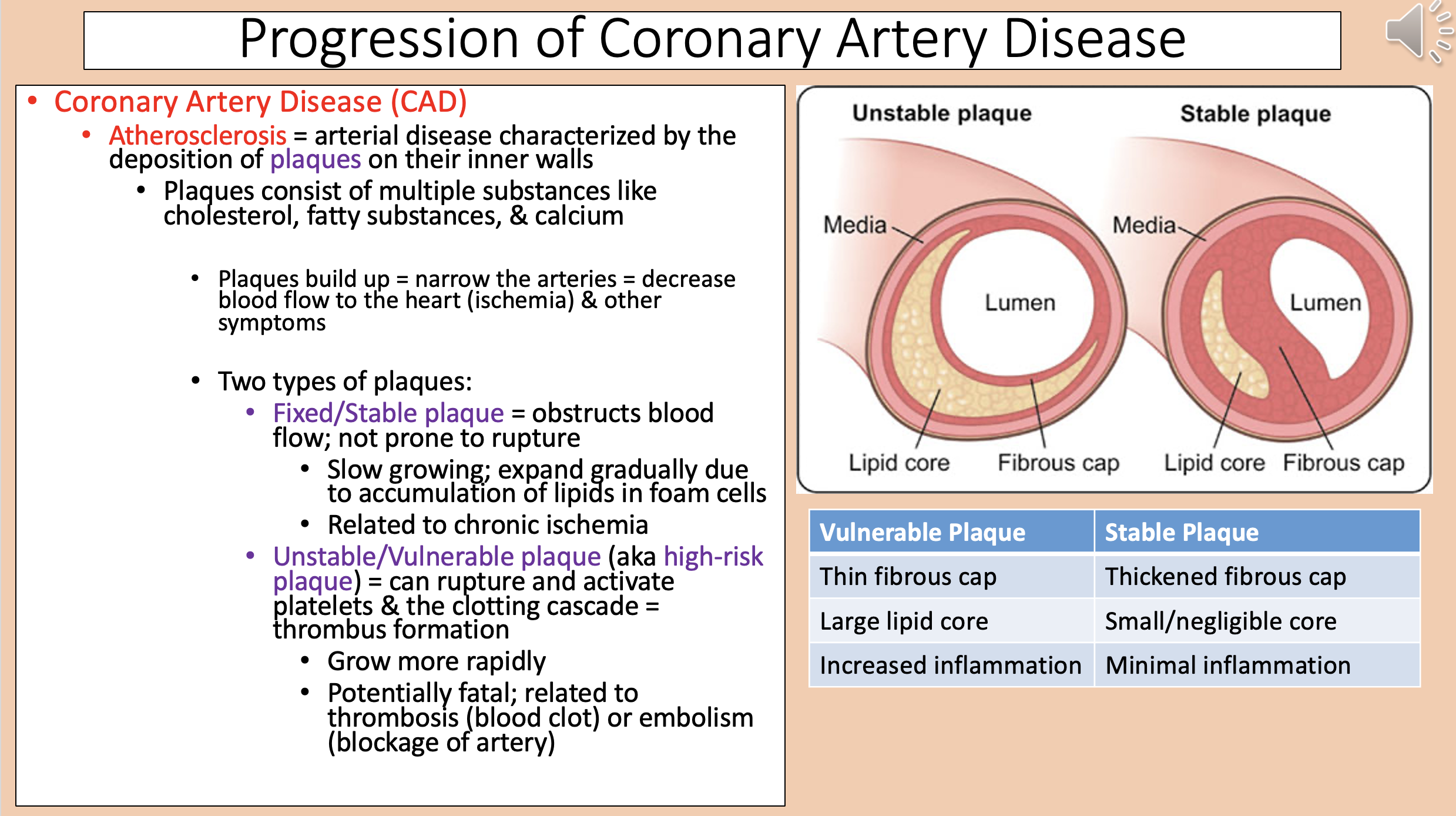
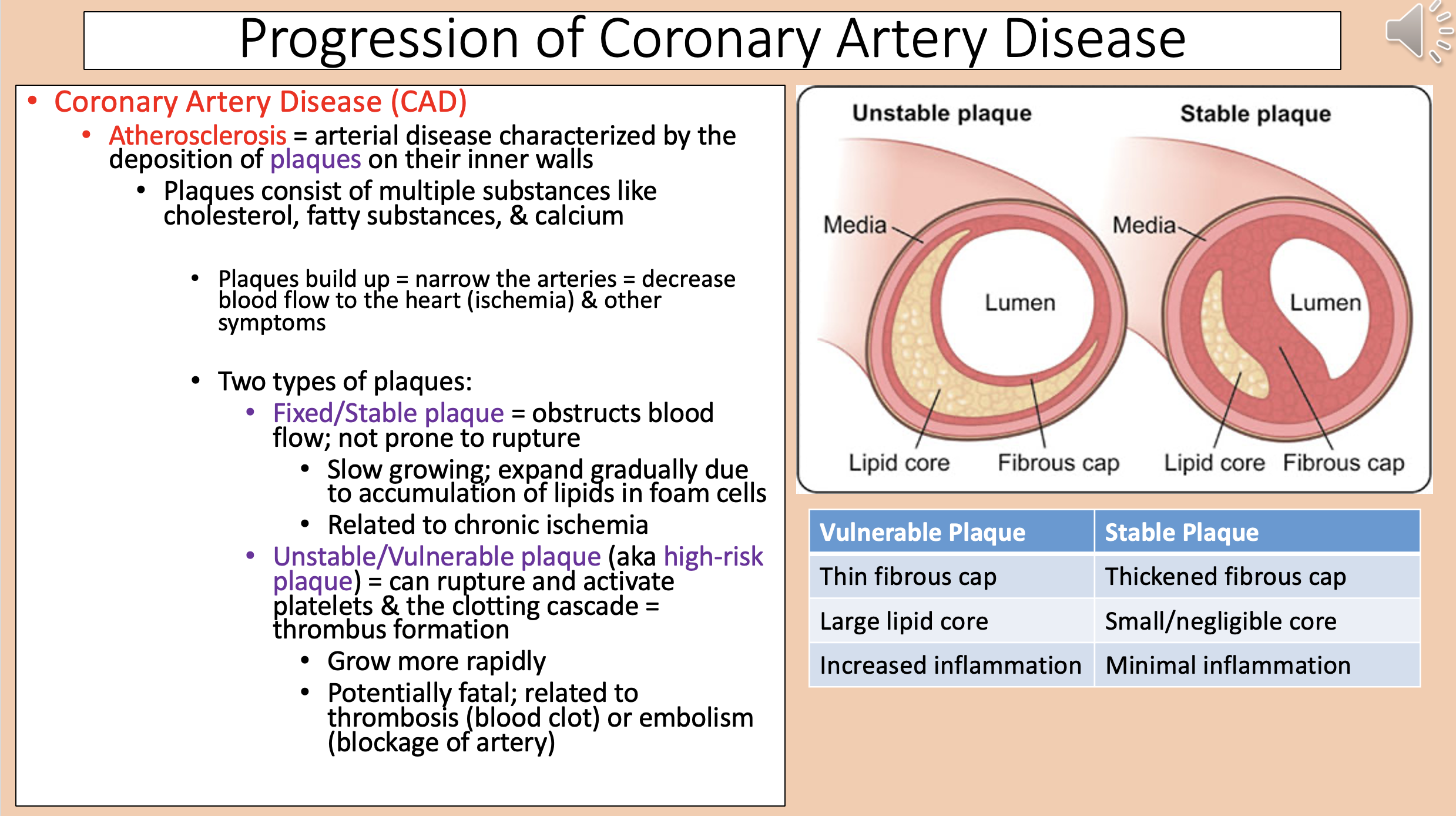
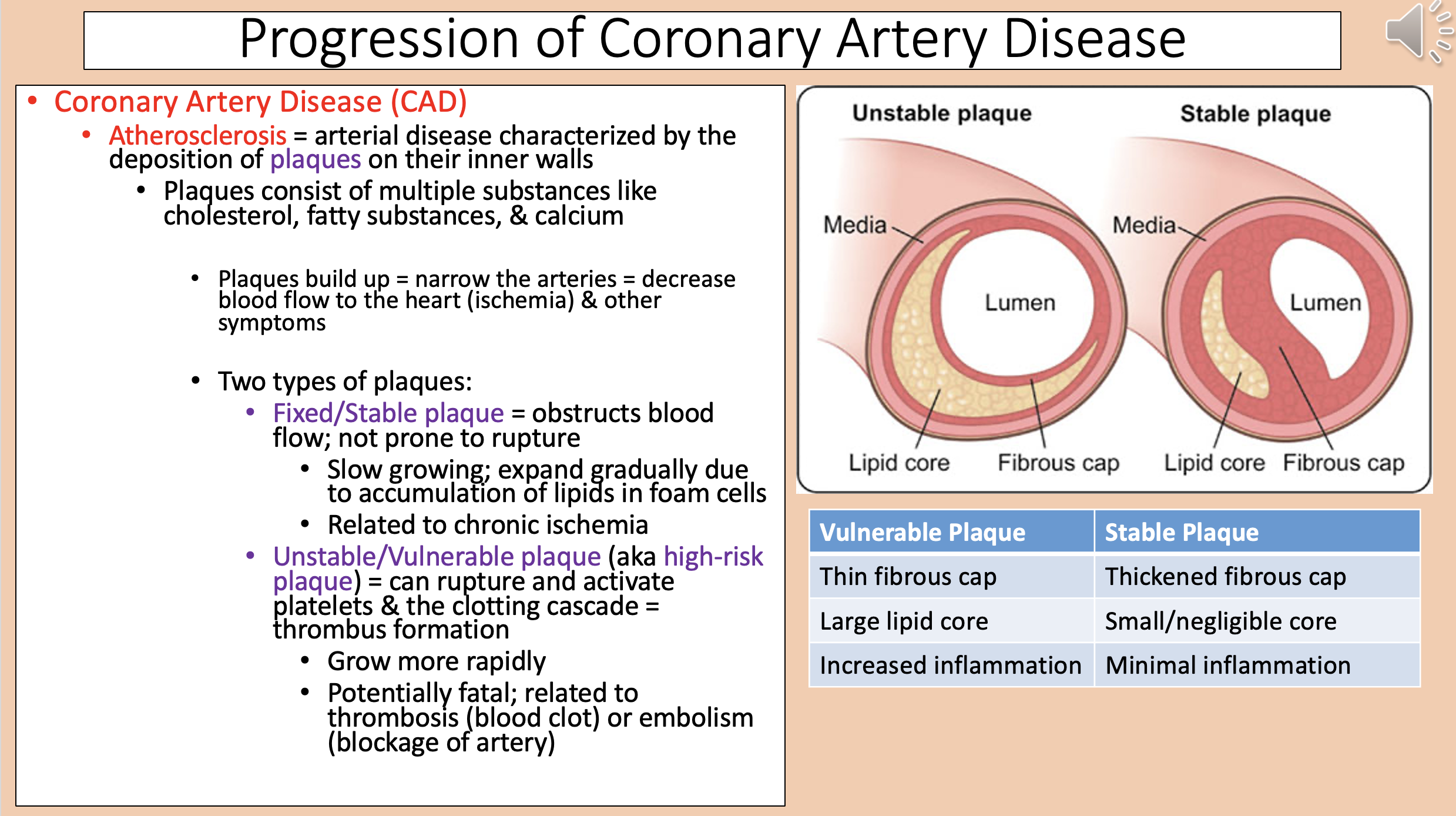
Arterial disease characterized by the deposition of plaques on their inner walls
atherosclerosis
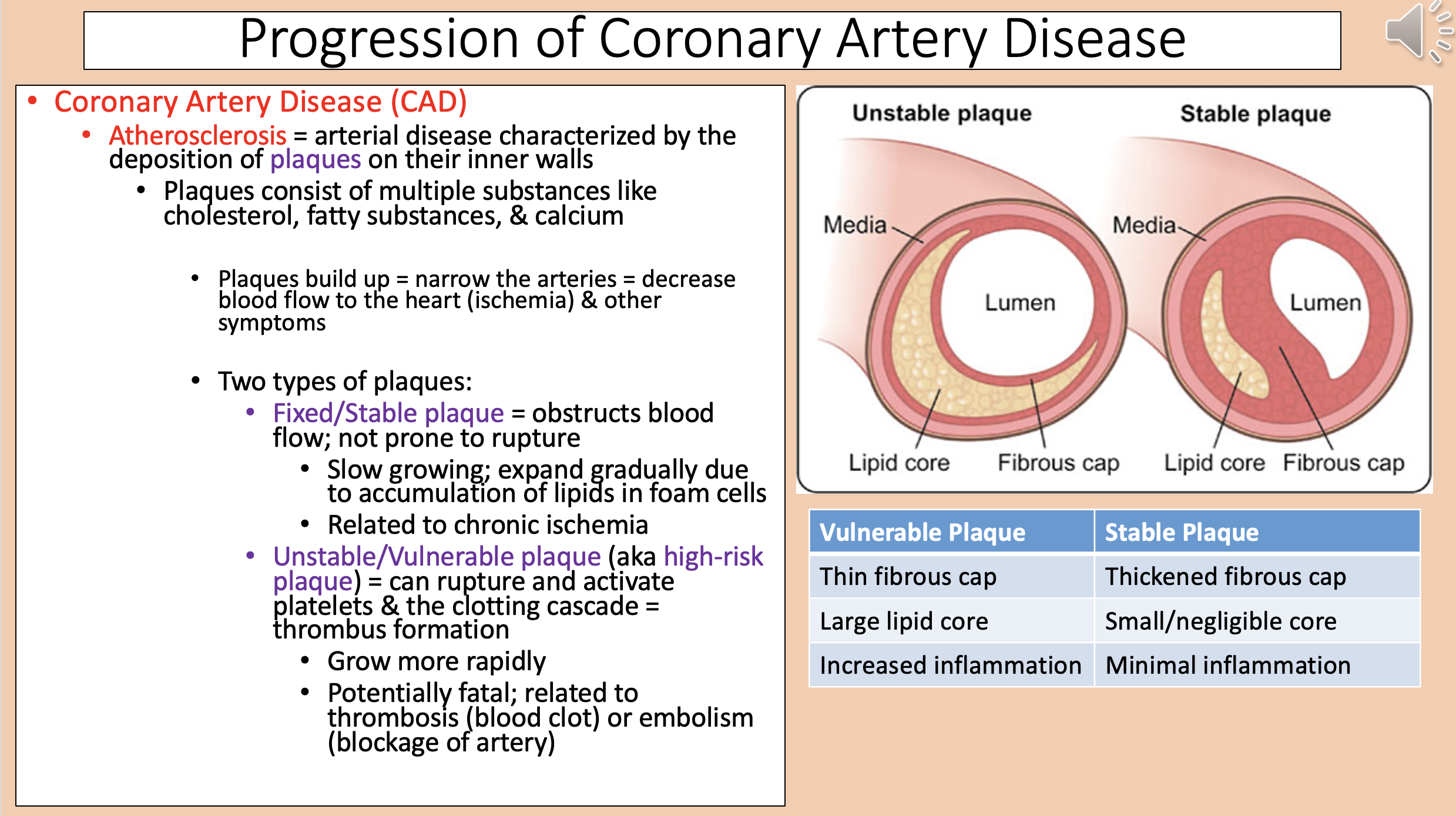
Narrow the arteries = decrease blood flow to the heart (ischemia) & other symptoms
Plaques build up
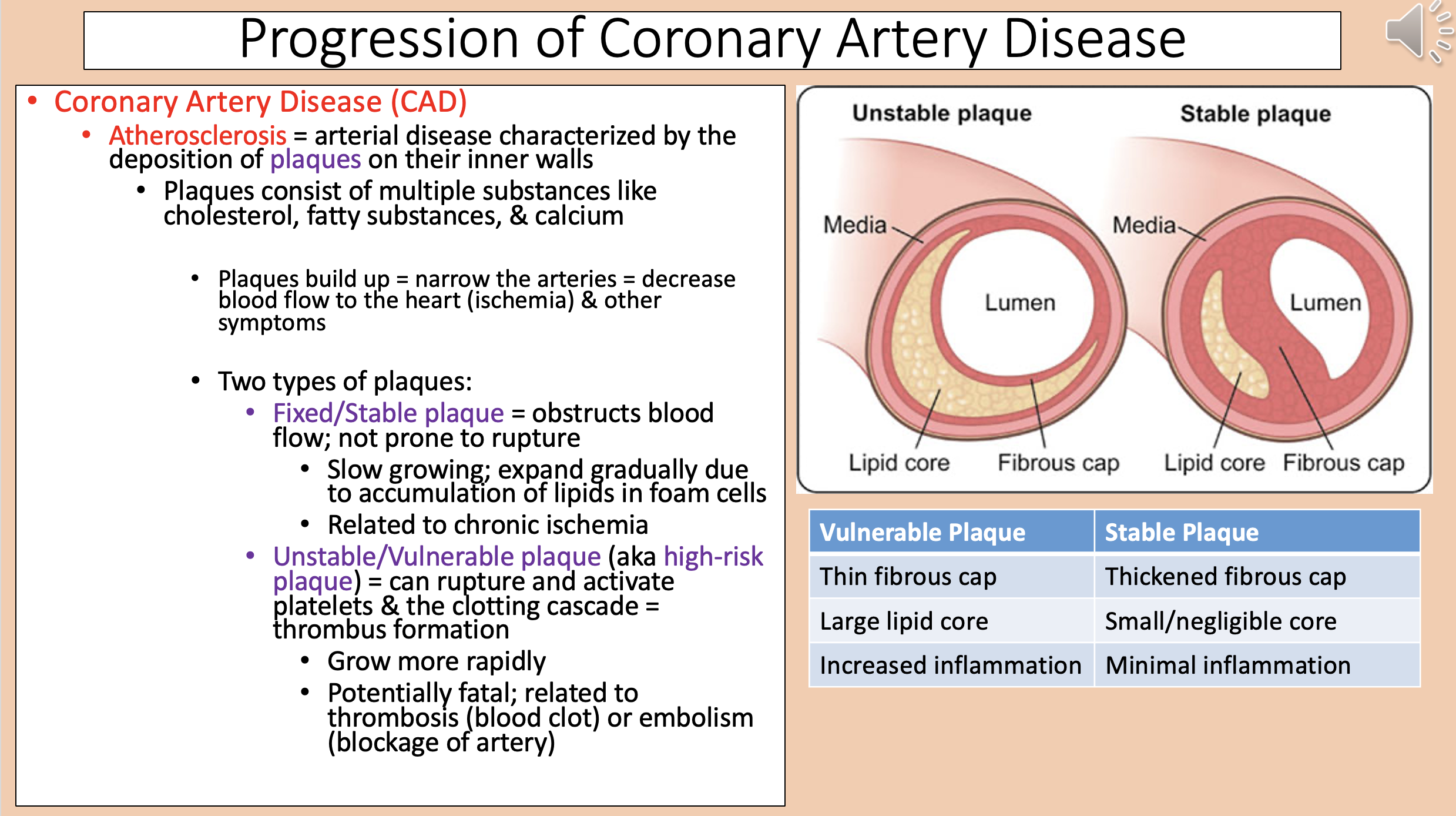
Two types of plaques
fixed/stable plaque and unstable/vulnerable plaque
Obstructs blood flow; not prone to rupture
fixed/stable plaque
Slow growing; expand gradually due to accumulation of lipids in foam cells.
Related to chronic ischemia.
fixed/stable plaque
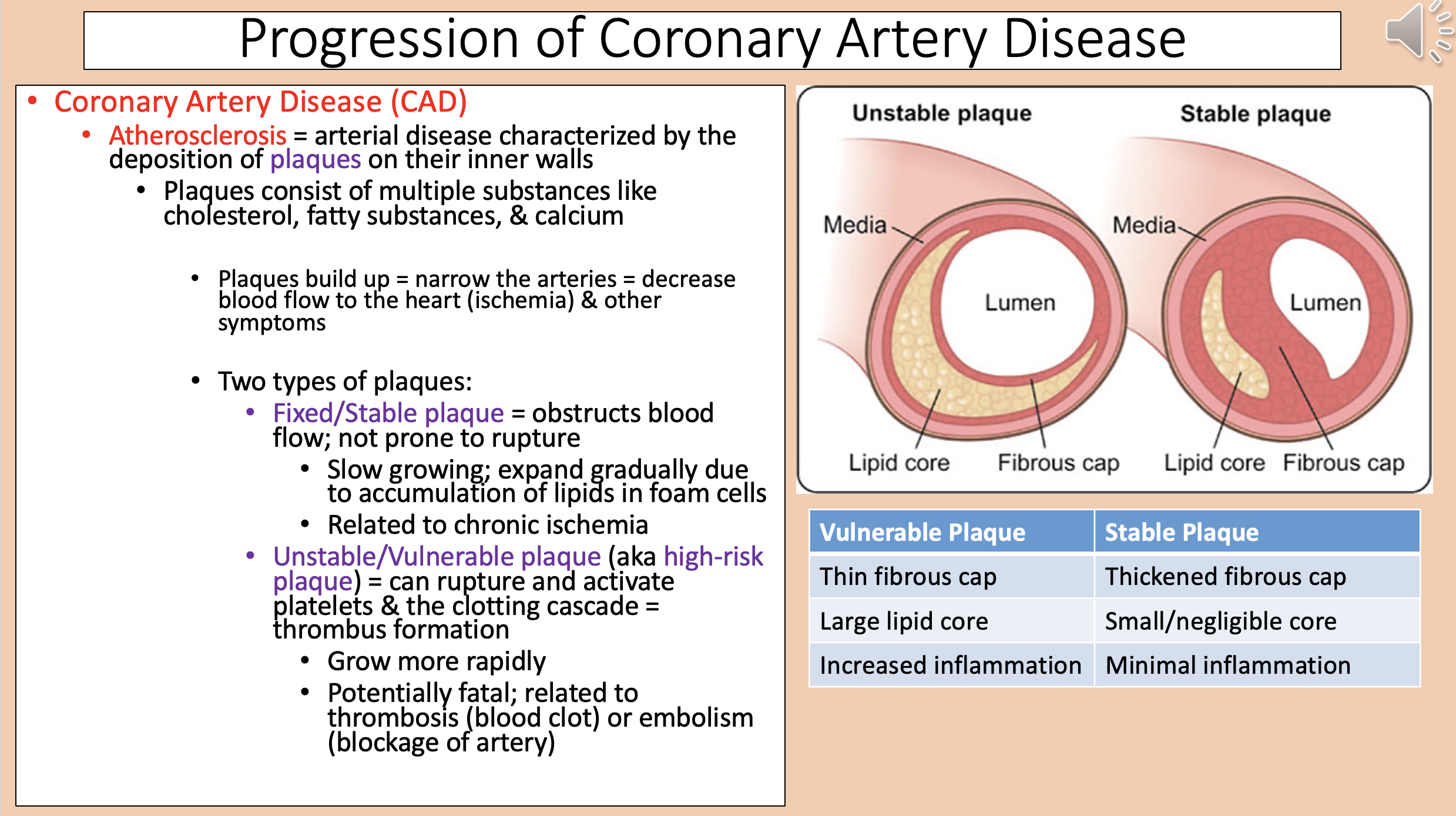
aka high-risk plaque
unstable/vulnerable plaque
Can rupture and activate platelets & the clotting cascade = thrombus formation
unstable/vulnerable plaque
Grow more rapidly.
Potentially fatal; related to thrombosis (blood clot) or embolism (blockage of artery).
unstable/vulnerable plaque
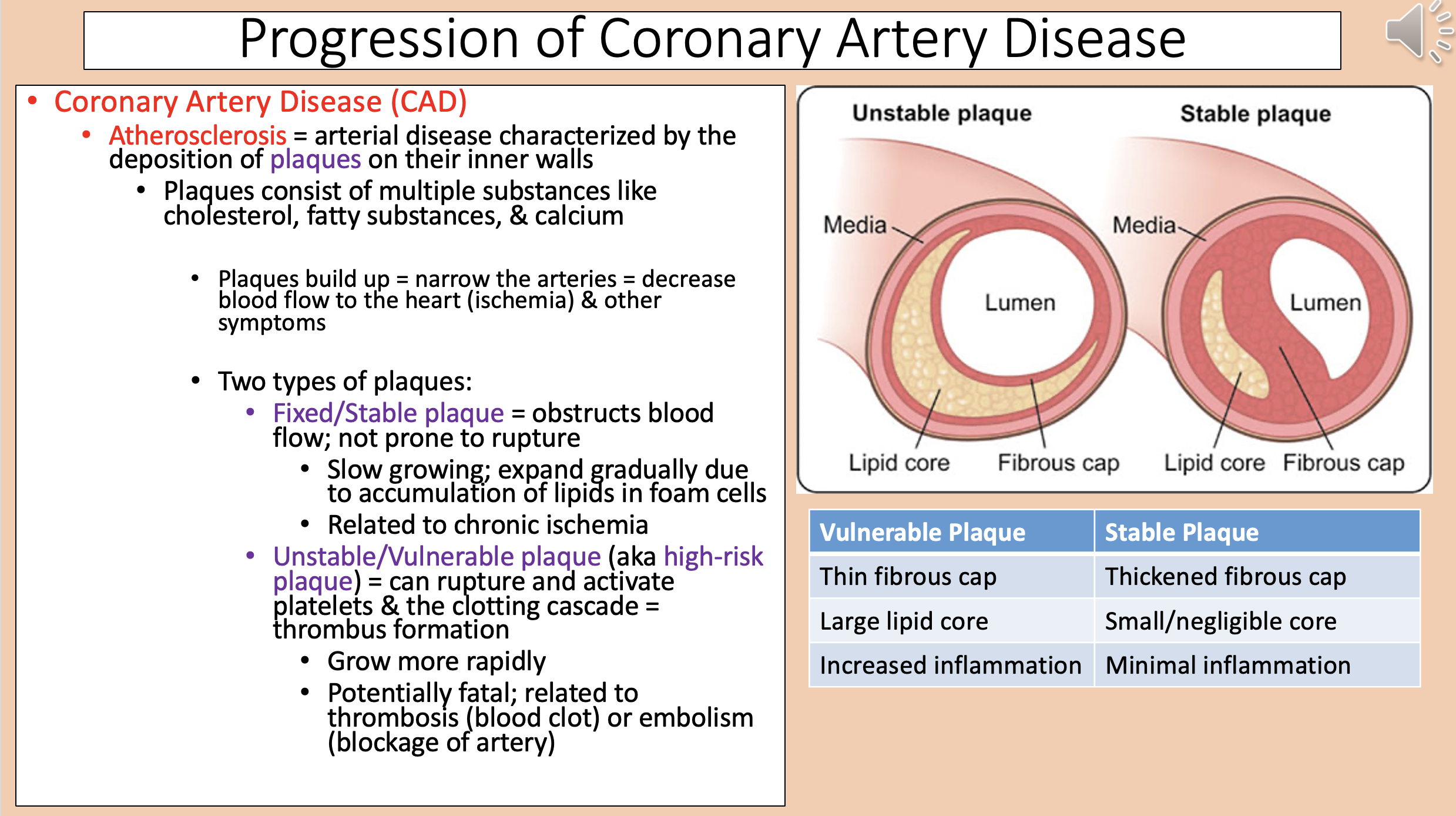
Vulnerable Plaque
Thin fibrous cap.
Large lipid core.
Increased inflammation.
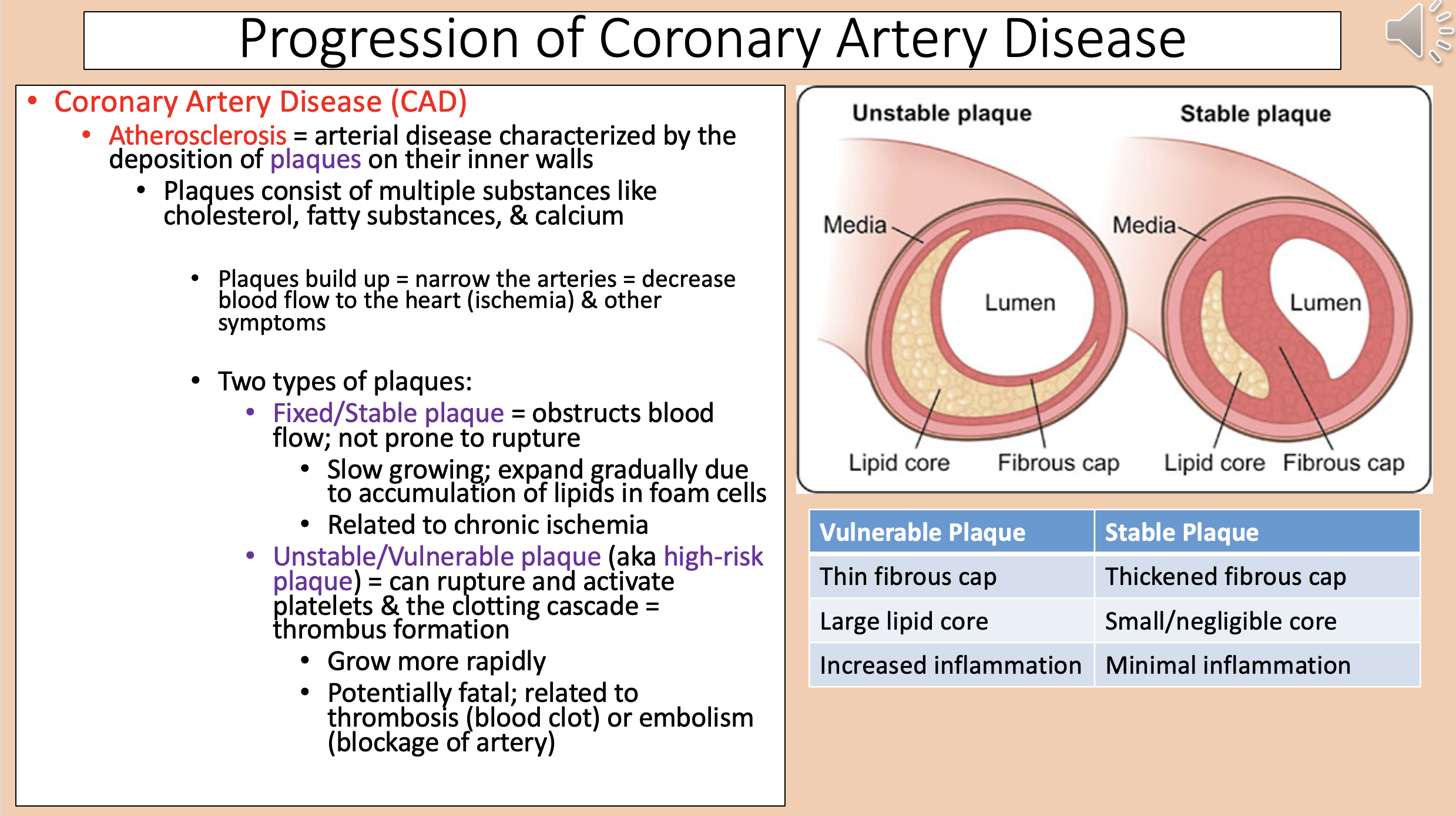
Stable Plaque
Thickened fibrous cap.
Small/negligible core.
Minimal inflammation.
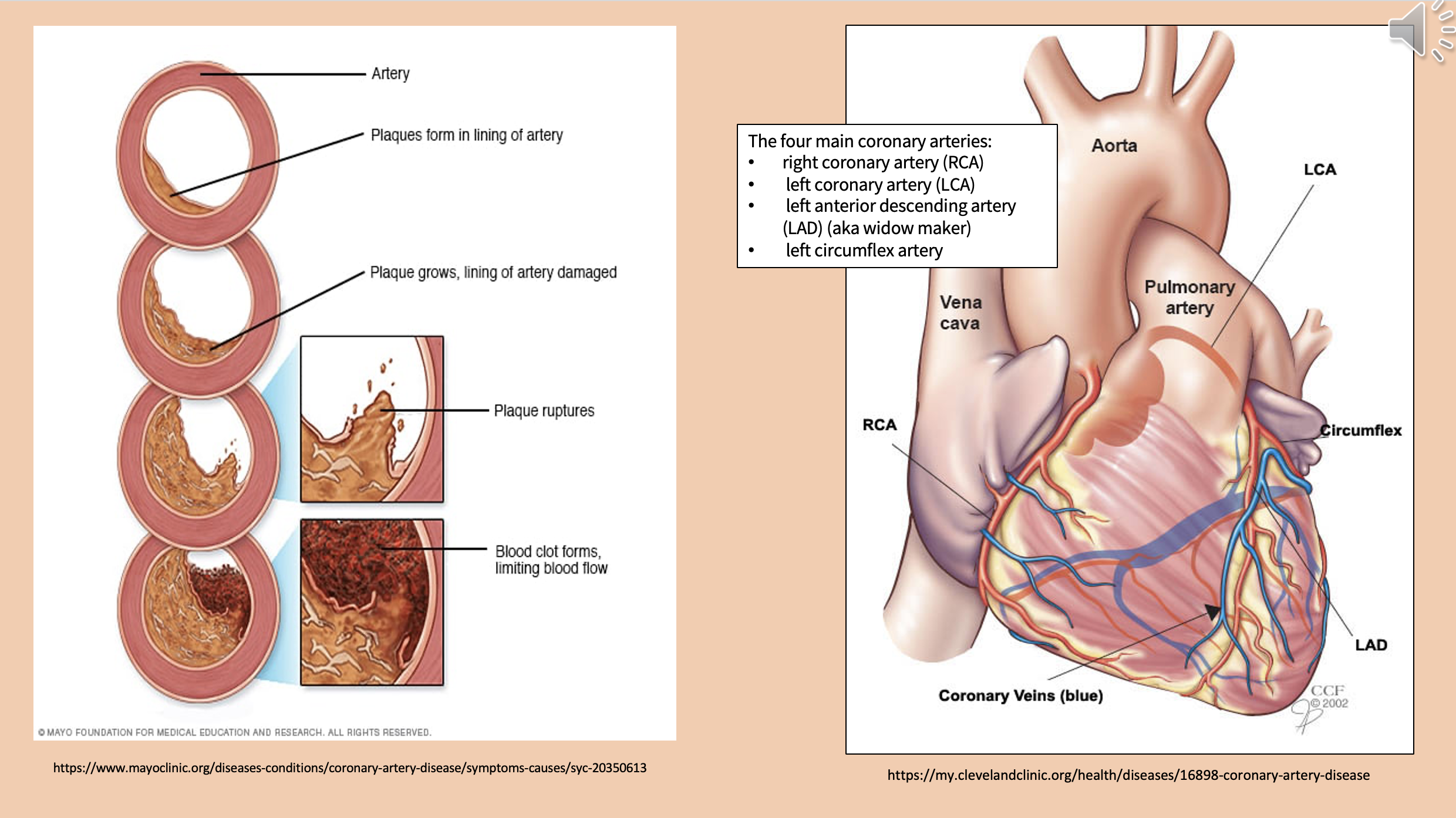
The four main coronary arteries
right coronary artery (RCA).
left coronary artery (LCA).
left anterior descending artery (LAD).
left circumflex artery
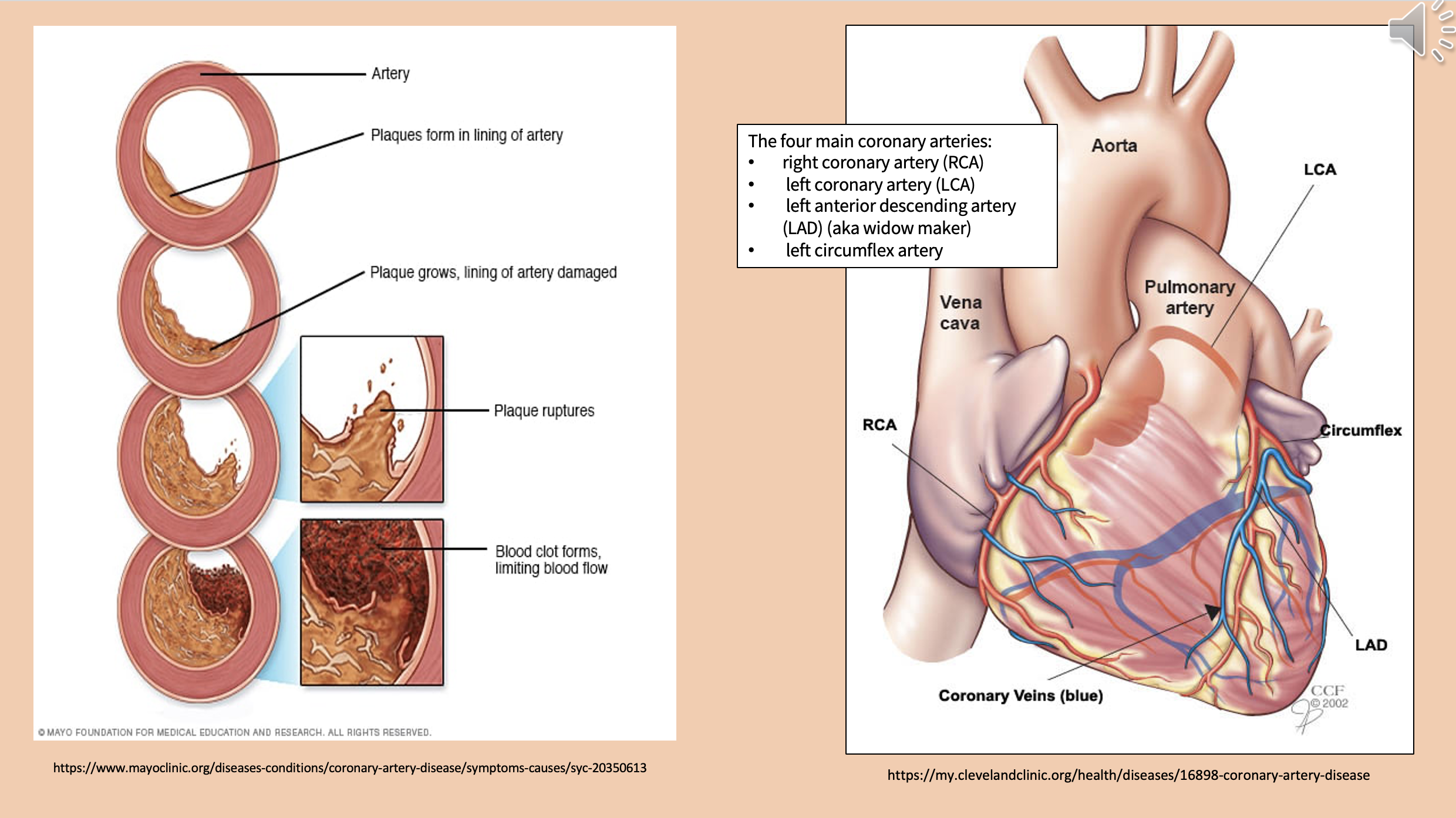
aka widow maker
left anterior descending artery
coronary artery disease (CAD) early stages
asymptomatic
Angina/chest discomfort.
Arrhythmias.
Myocardial Ischemia.
Ischemic damage to other areas (muscle cramping, etc).
Dyspnea/shortness of breath.
coronary artery disease symptoms
Heart failure.
Heart attack.
Cardiac arrest/death.
coronary artery disease potential long-term complications
Age.
Gender (men have higher risk)(risk for women increases after menopause).
High blood pressure.
High LDL cholesterol.
Low HDL cholesterol.
Obesity.
Physical inactivity.
Dietary choices.
Smoking.
Diabetes.
coronary artery disease risk factors
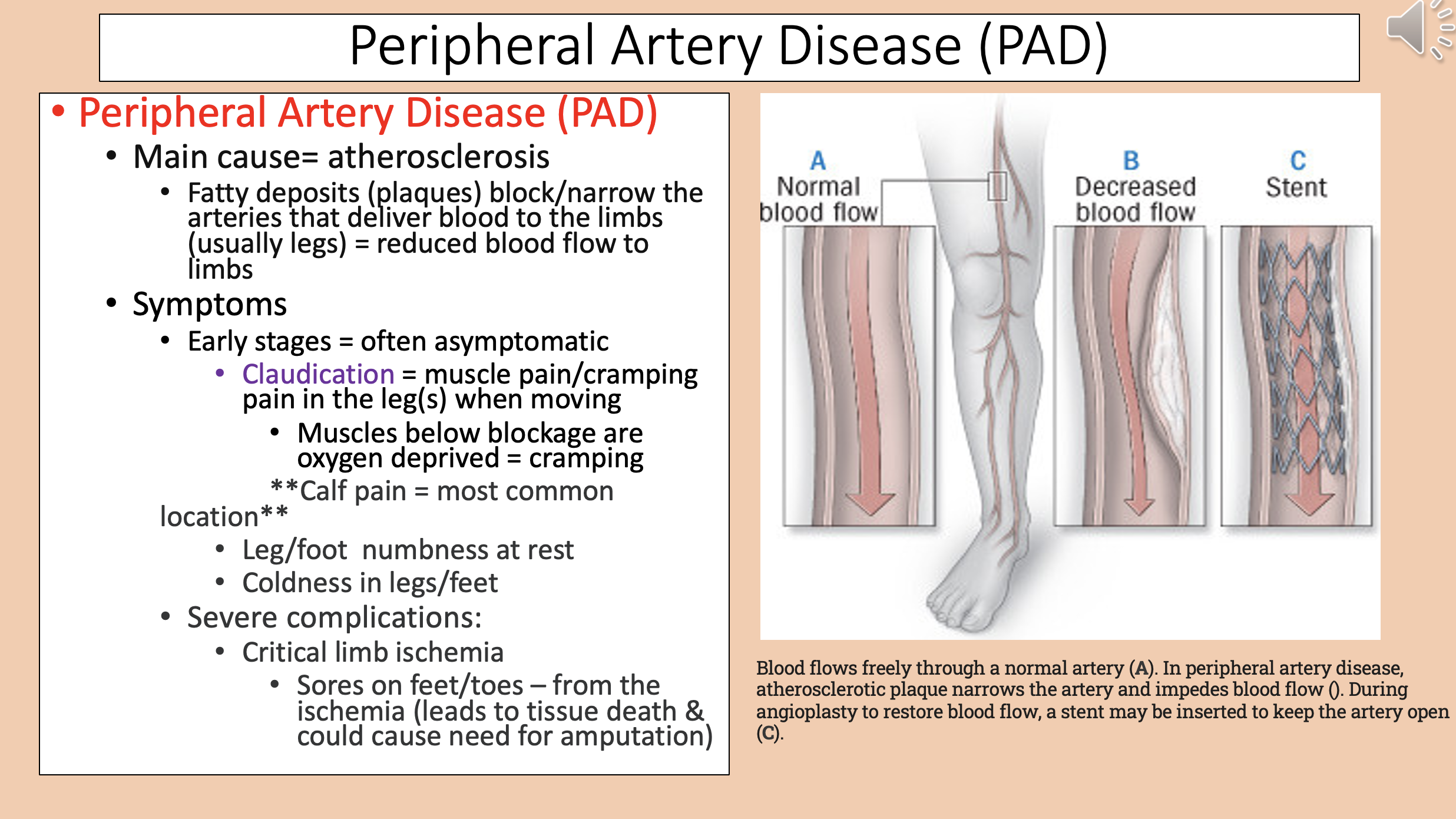
Peripheral Artery Disease (PAD) main cause
atherosclerosis
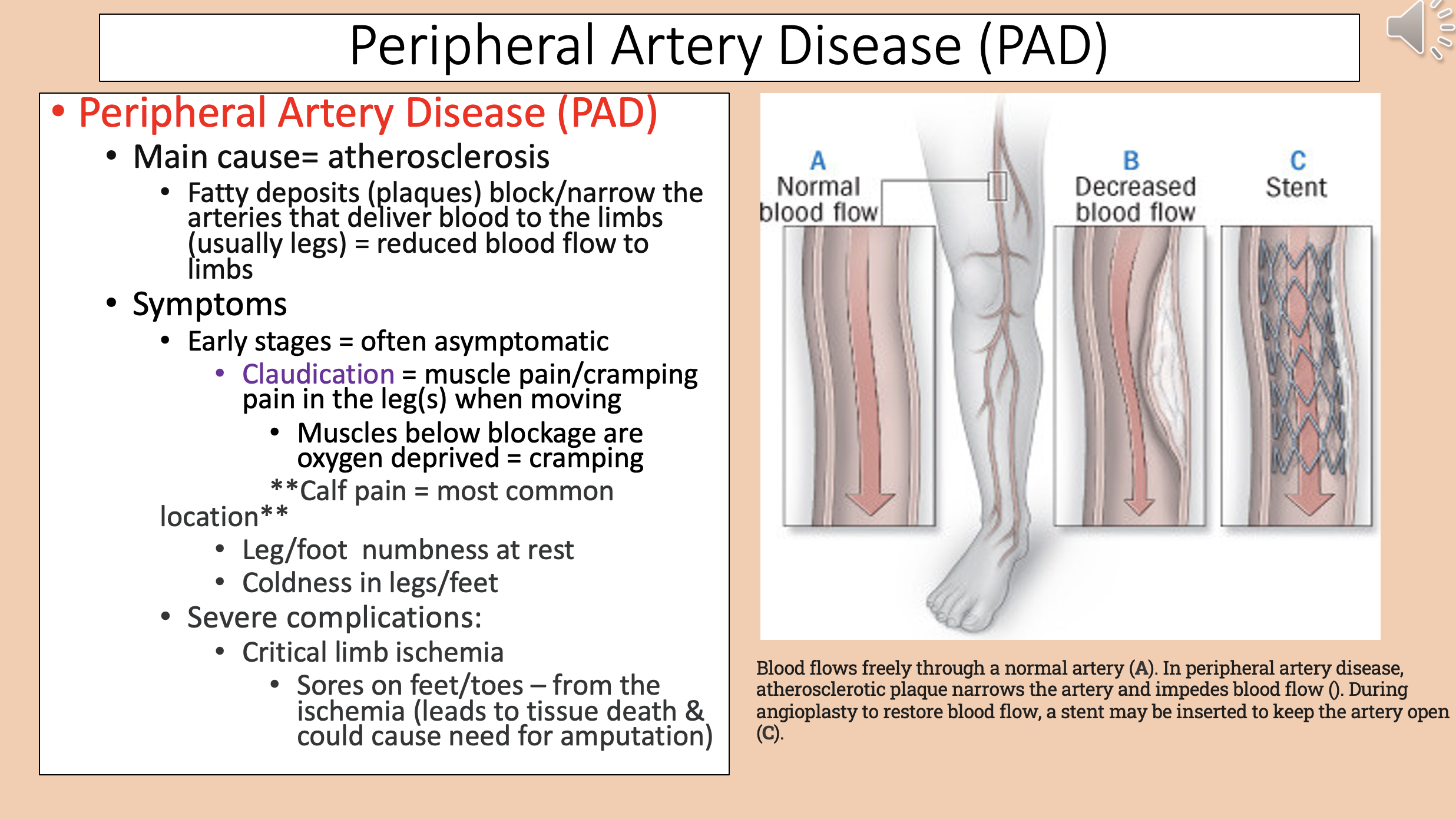
Peripheral Artery Disease (PAD) early stages
asymptomatic
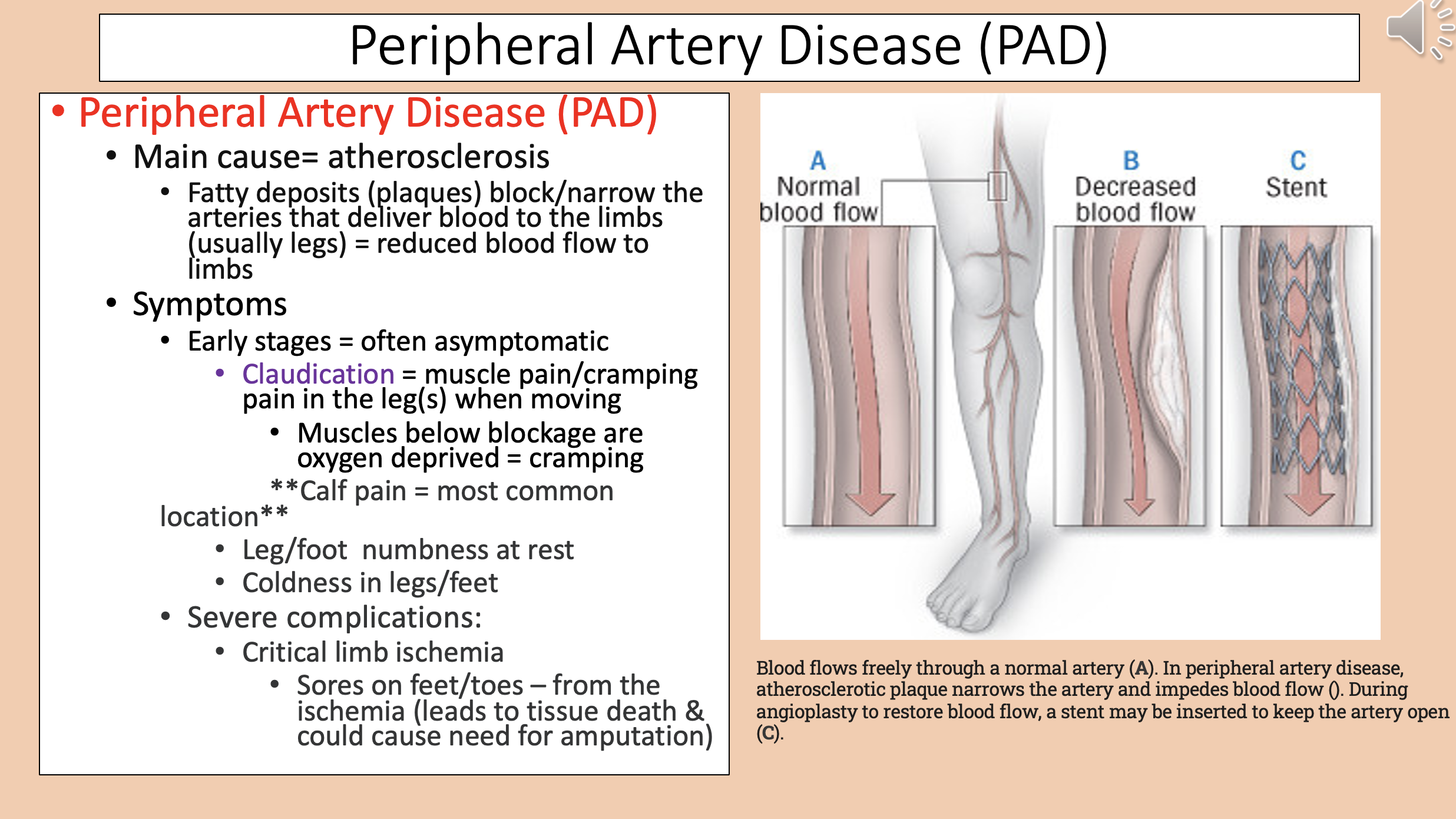
Muscle pain/cramping pain in the leg(s) when moving
claudication
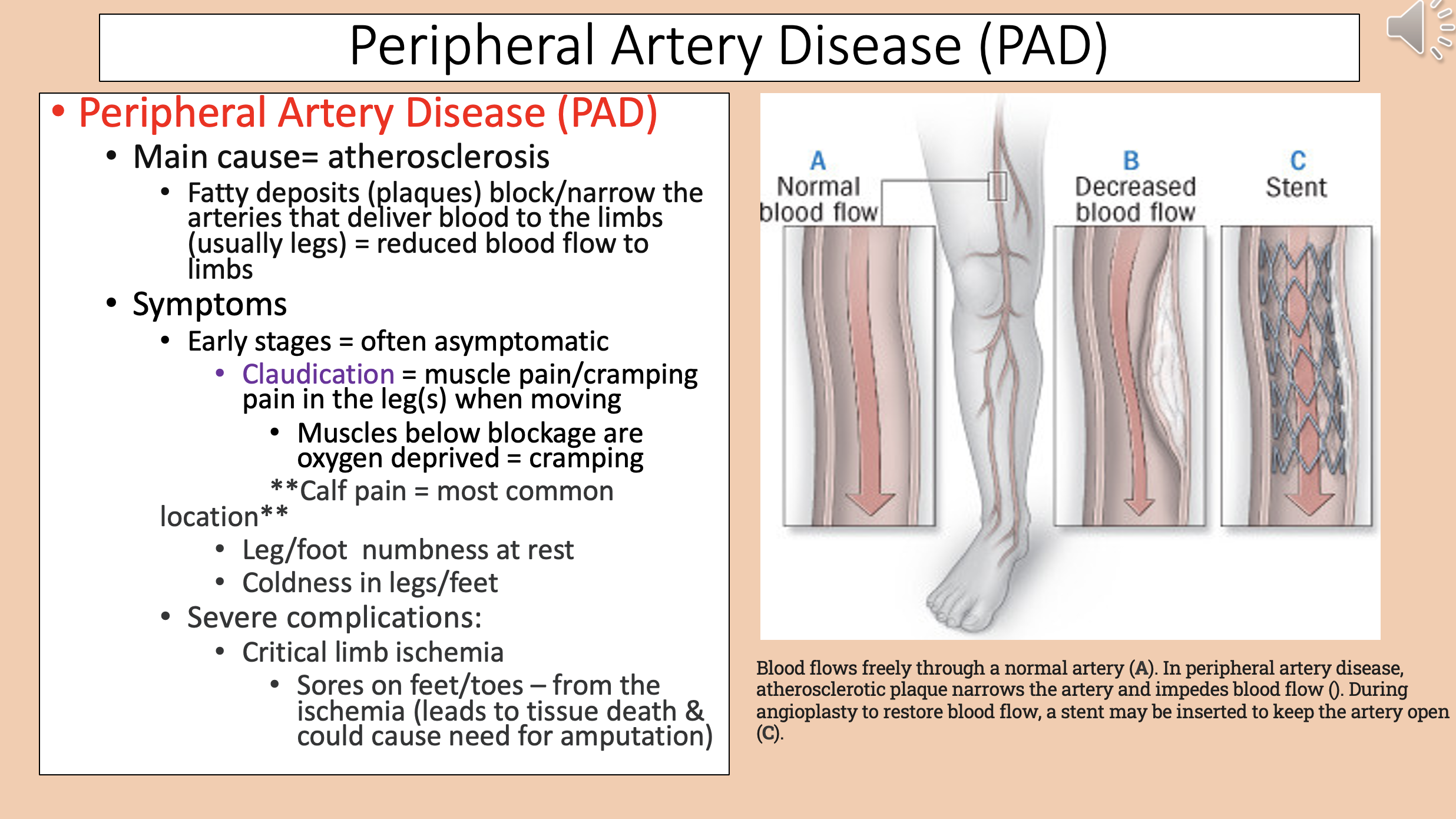
Muscles below blockage are oxygen deprived
cramping
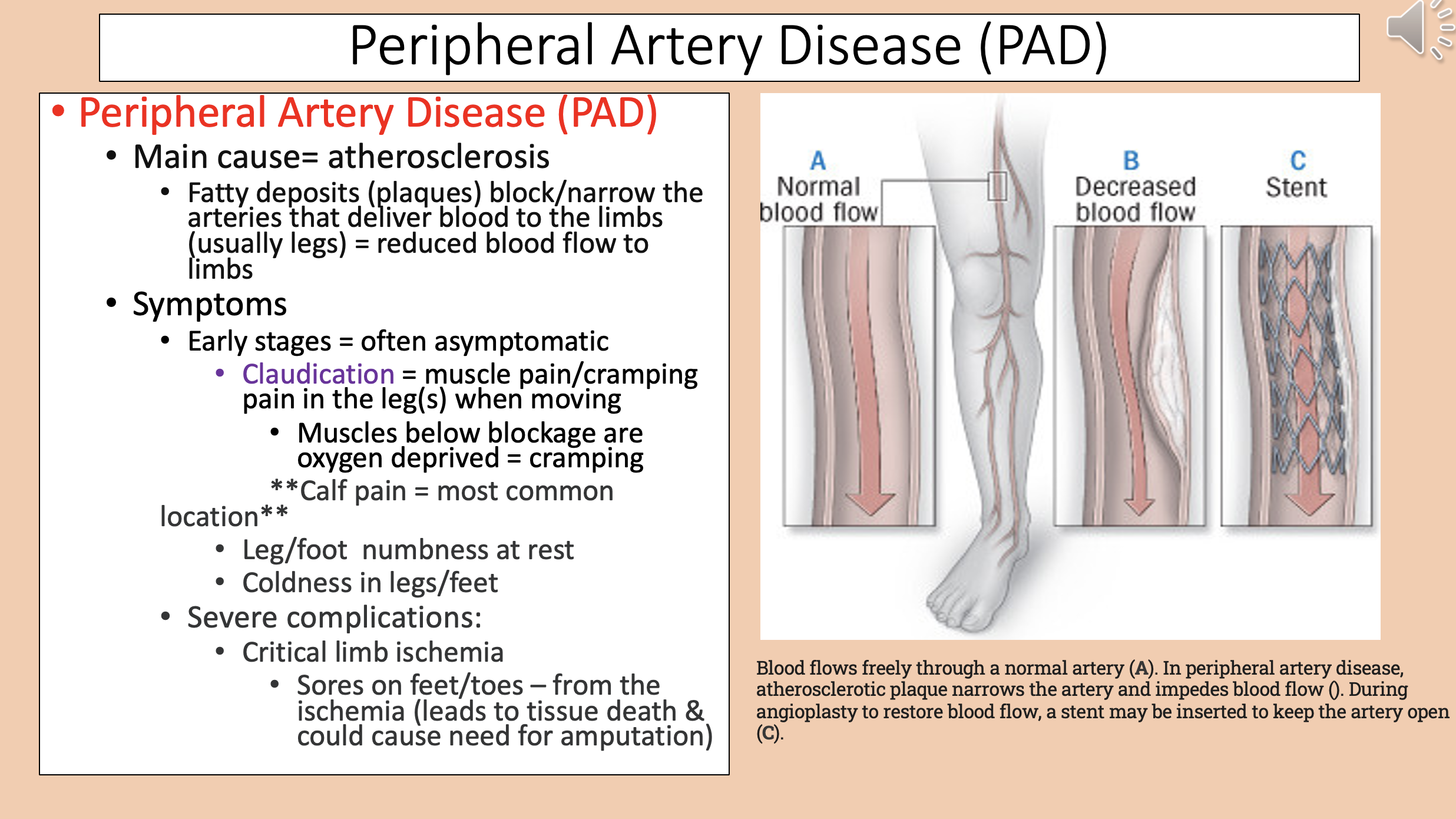
Peripheral Artery Disease (PAD) most common location
calf pain
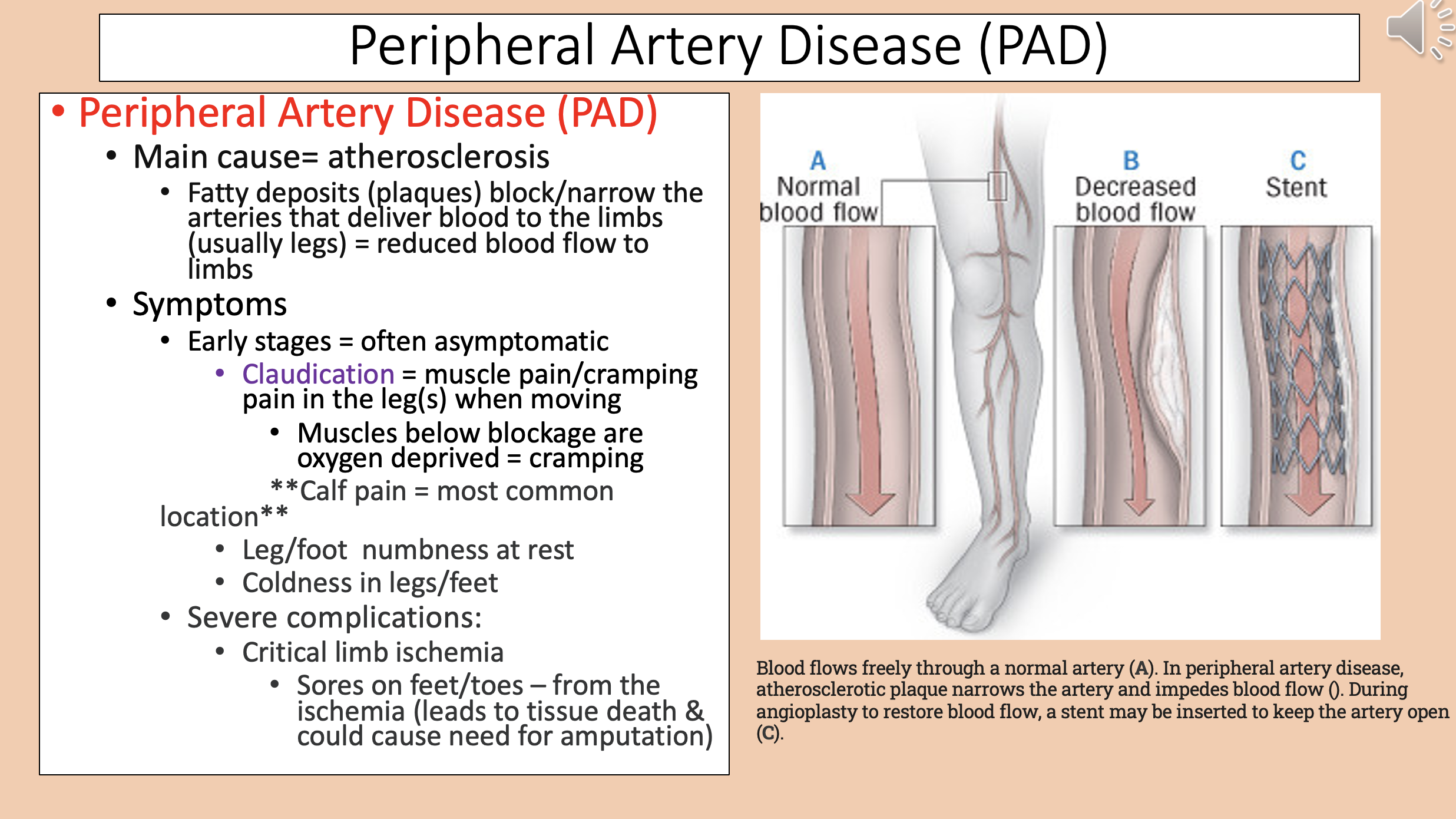
Peripheral Artery Disease (PAD) severe complications
critical limb ischemia
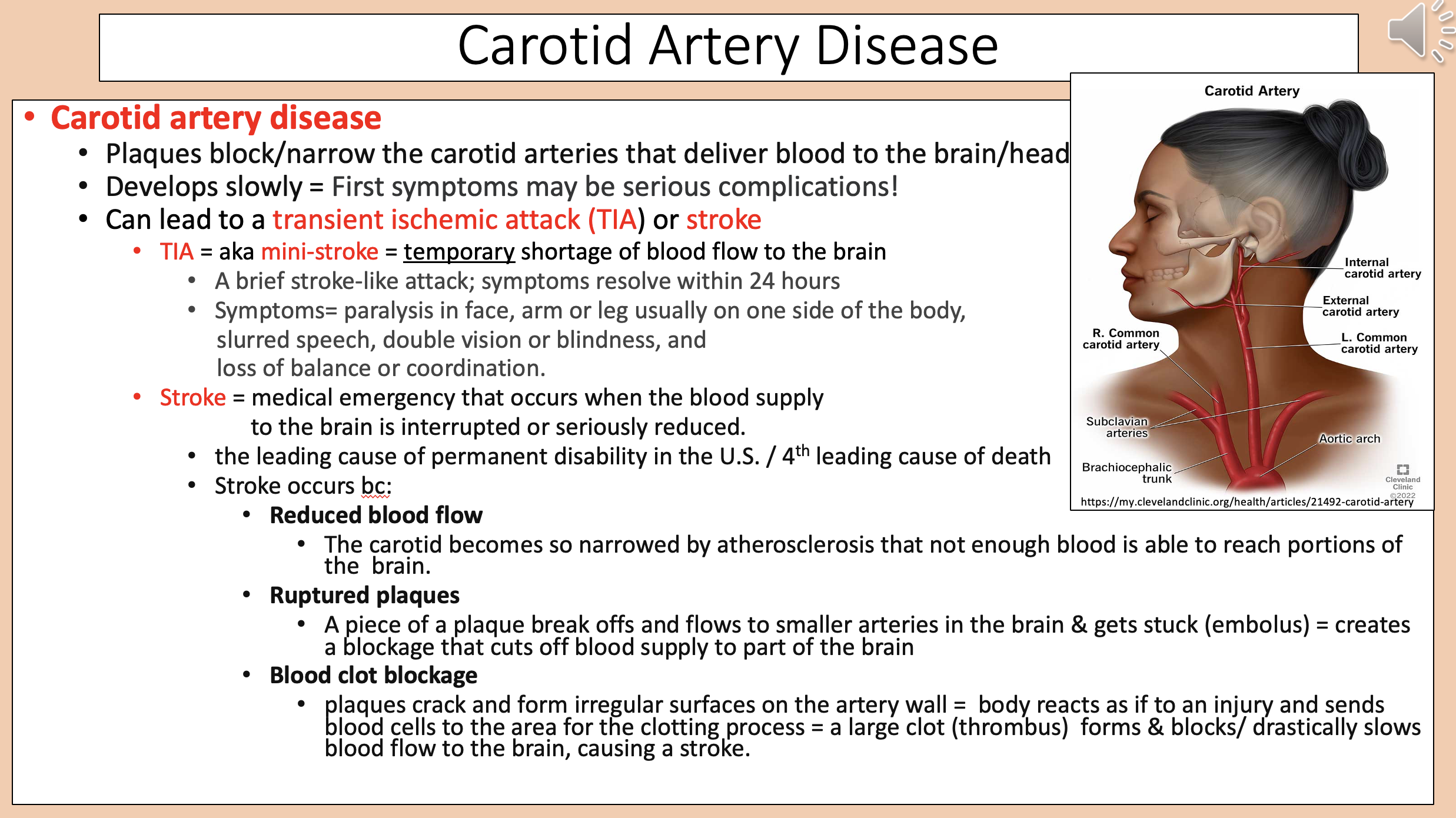
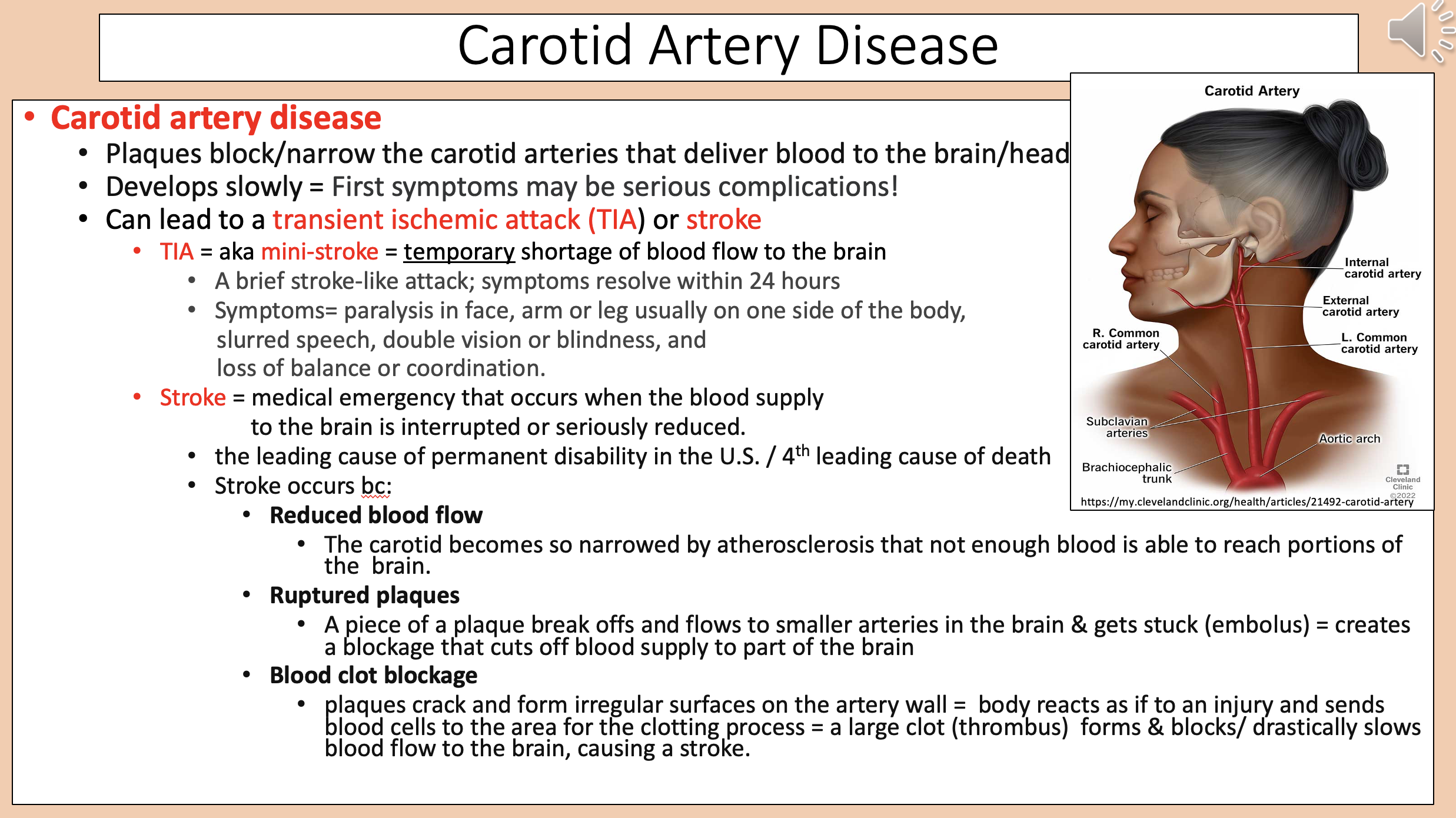
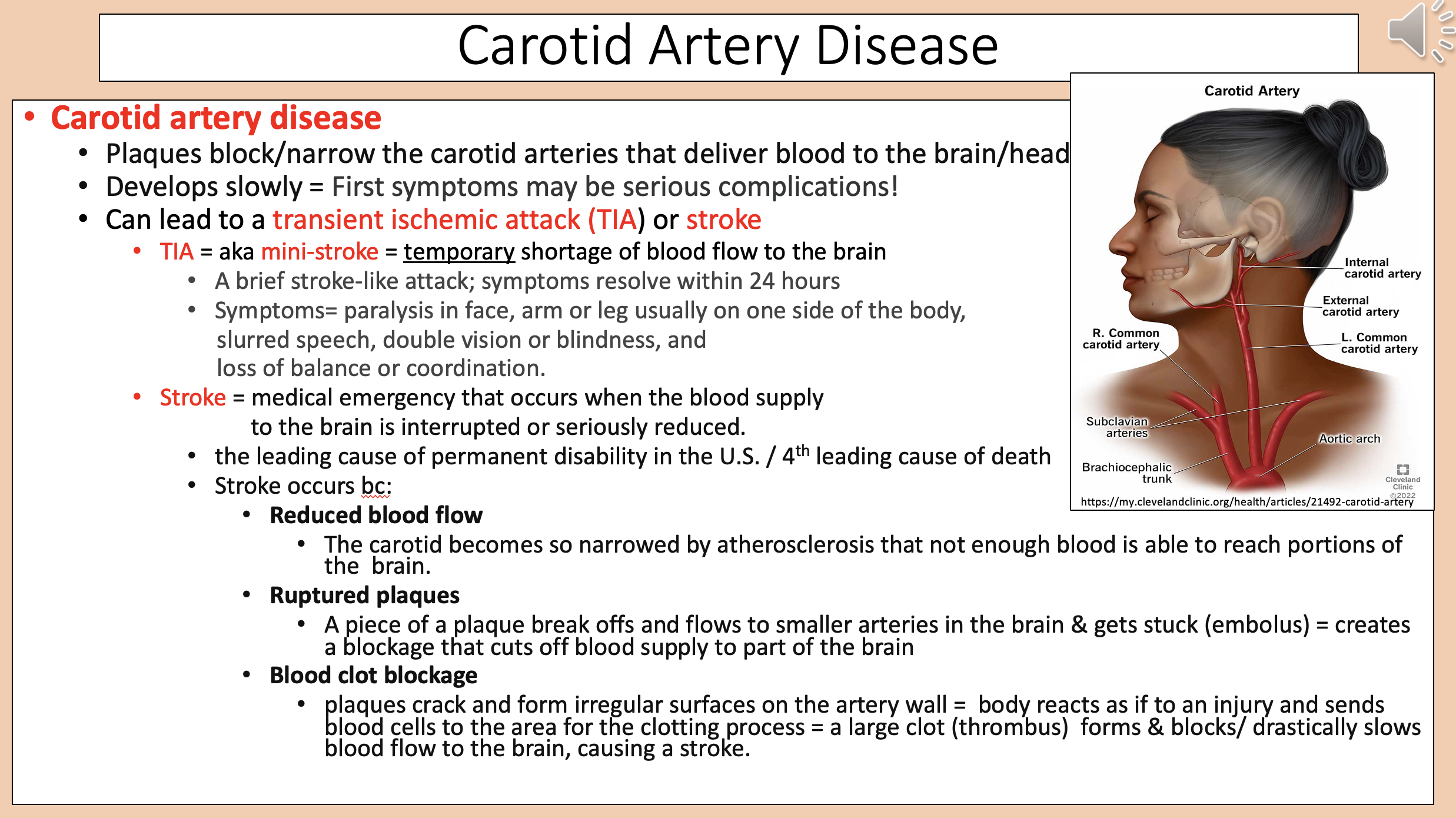
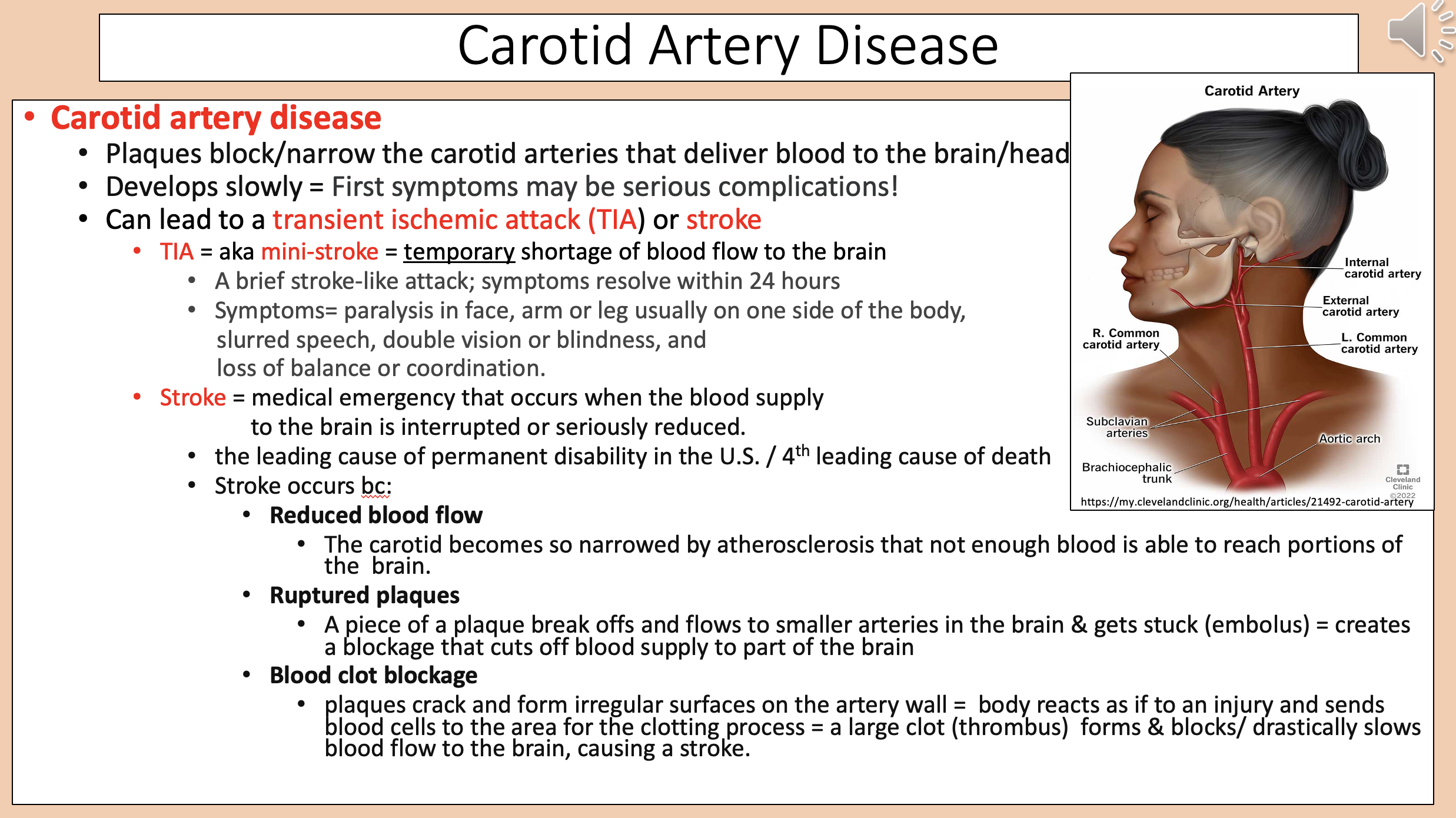
Plaques block/narrow the carotid arteries that deliver blood to the brain/head.
Develops slowly.
carotid artery disease
carotid artery disease can lead to
transient ischemic attack (TIA) or stroke
aka mini-stroke
TIA
Temporary shortage of blood flow to the brain
TIA
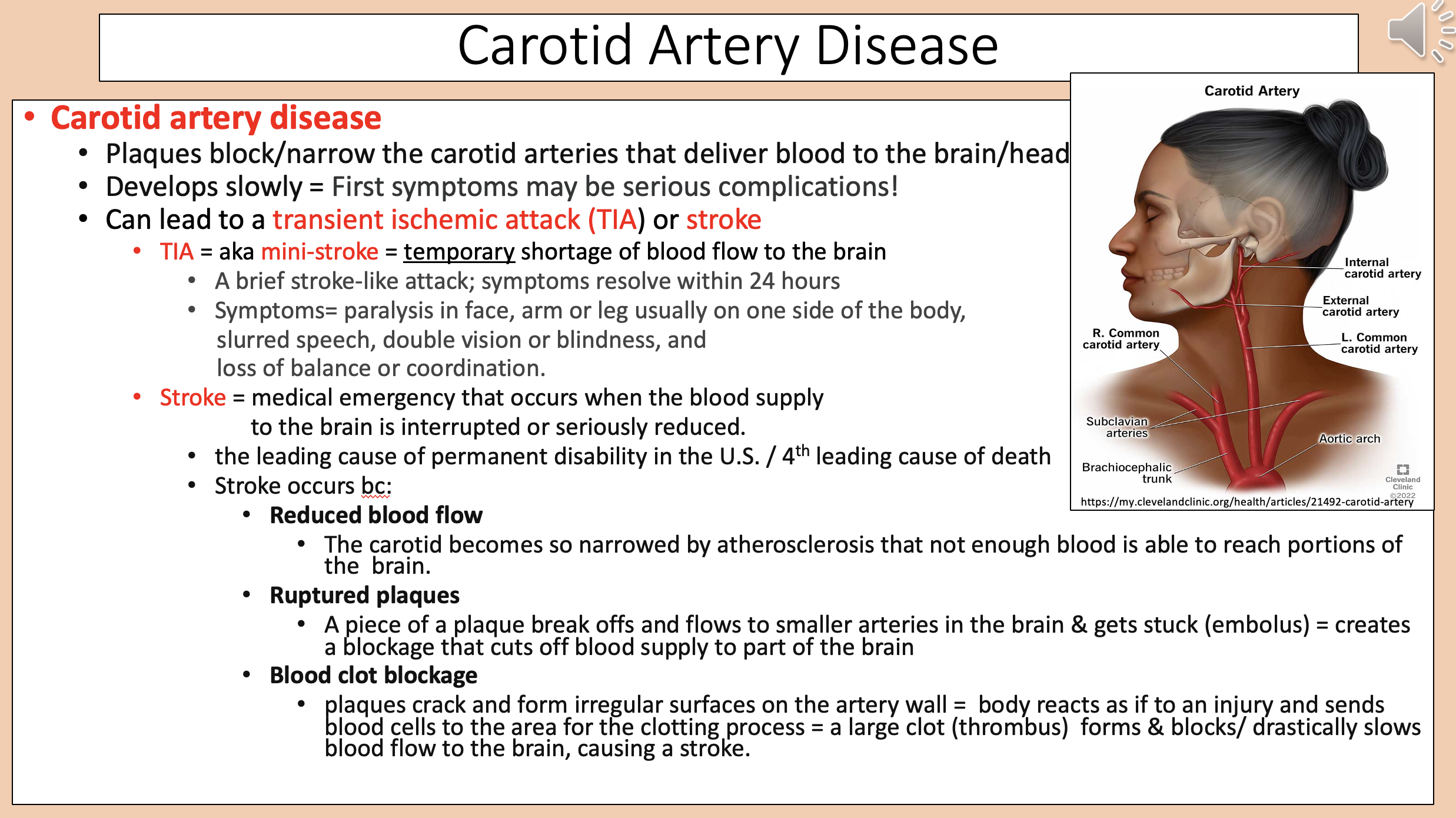
Paralysis in face, arm or leg usually on one side of the body.
Slurred speech.
Double vision or blindness.
Loss of balance or coordination.
carotid artery disease symptoms
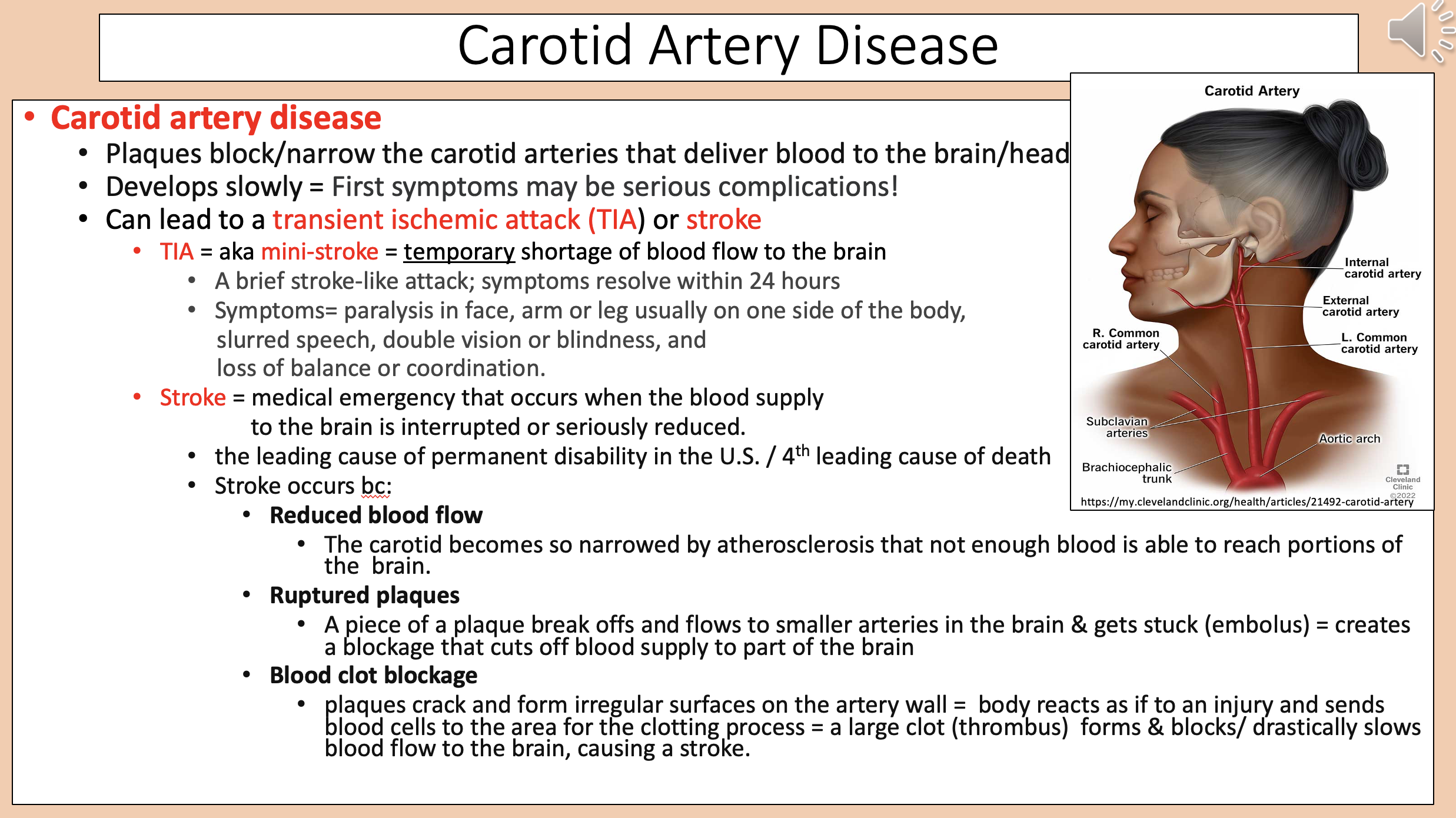
Medical emergency that occurs when the blood supply to the brain is interrupted or seriously reduced
stroke
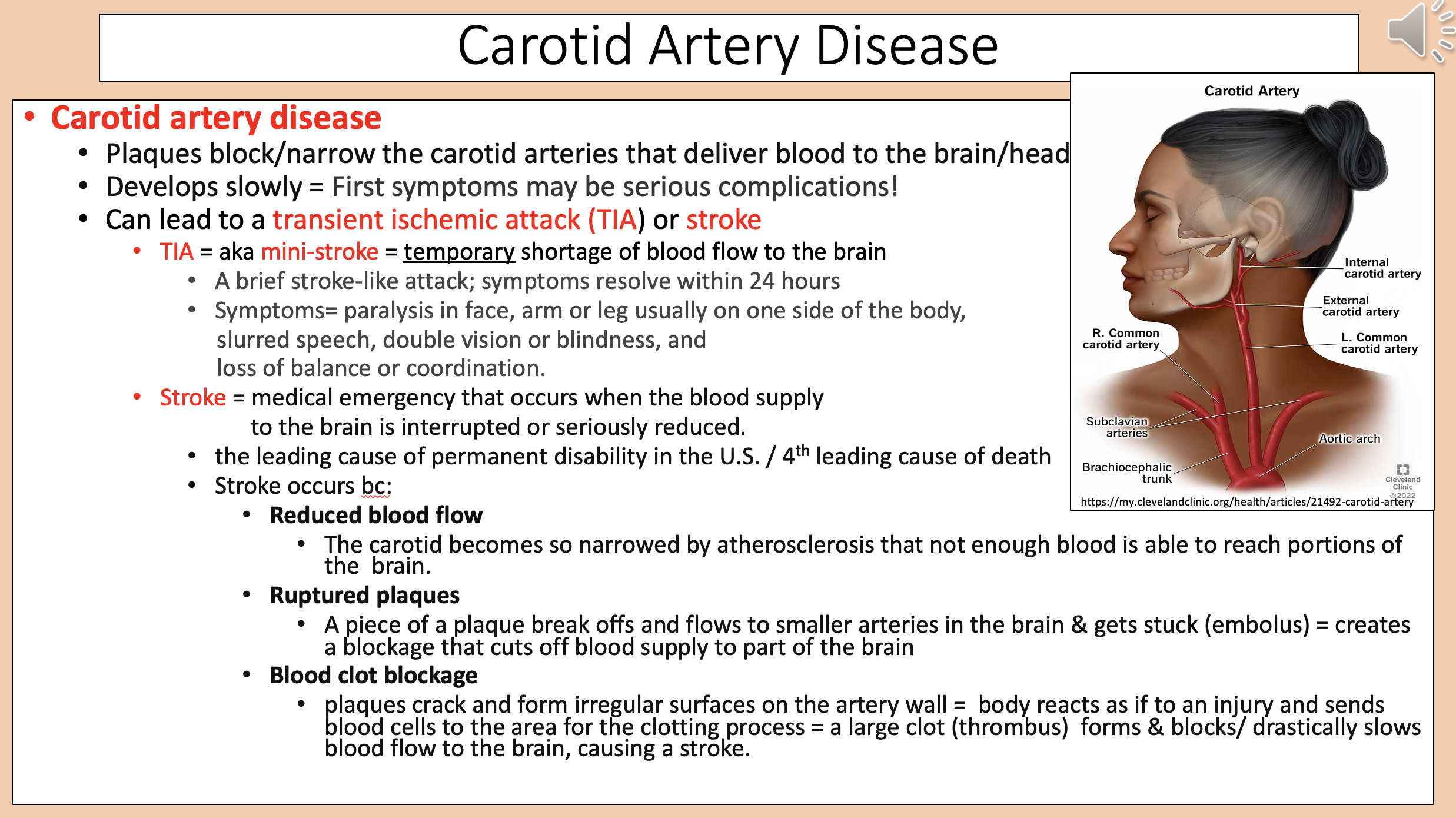
The leading cause of permanent disability in the U.S.
4th leading cause of death.
stroke
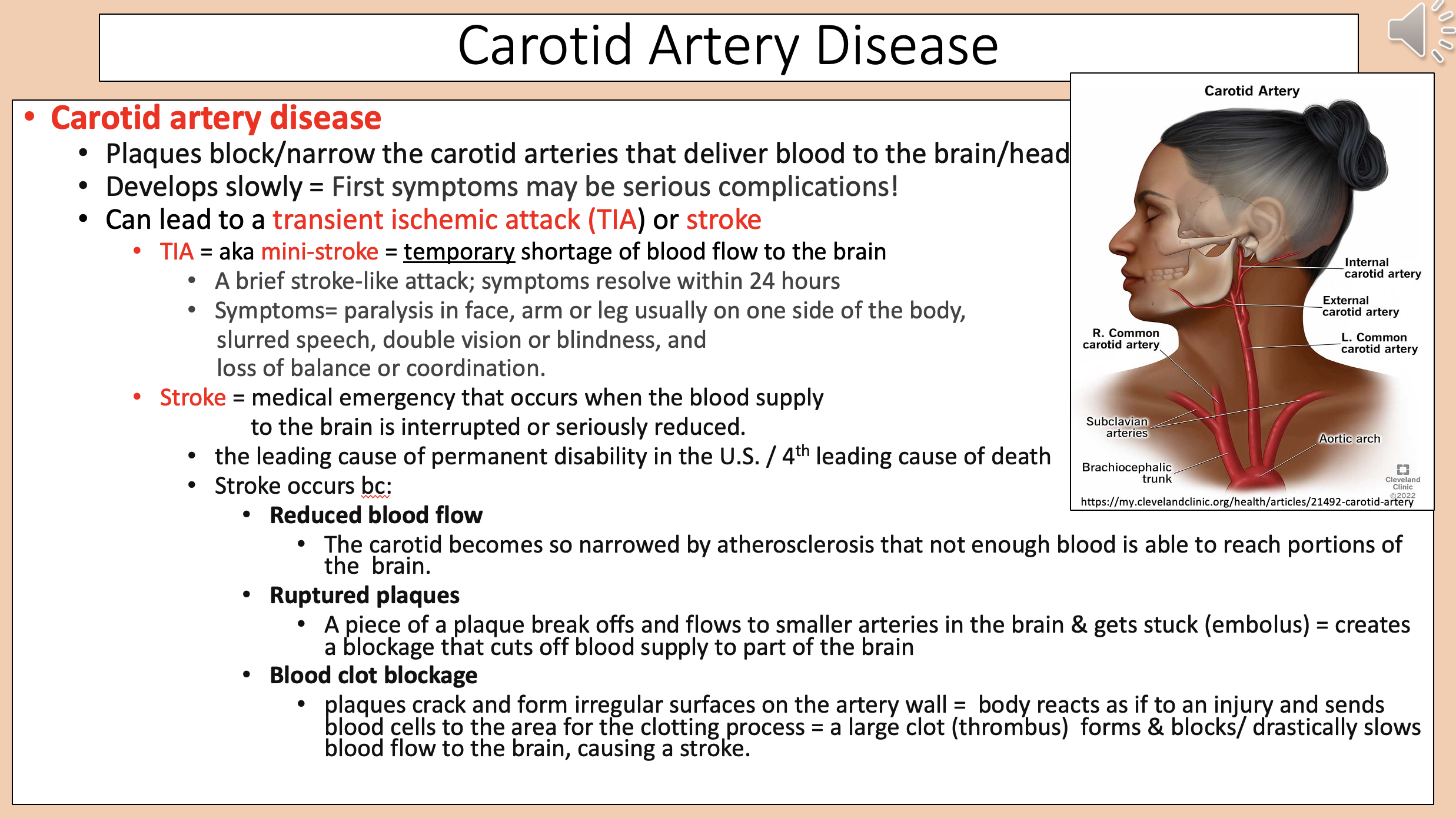
Stroke occurs because
Reduced blood flow.
Ruptured plaques.
Blood clot blockage.
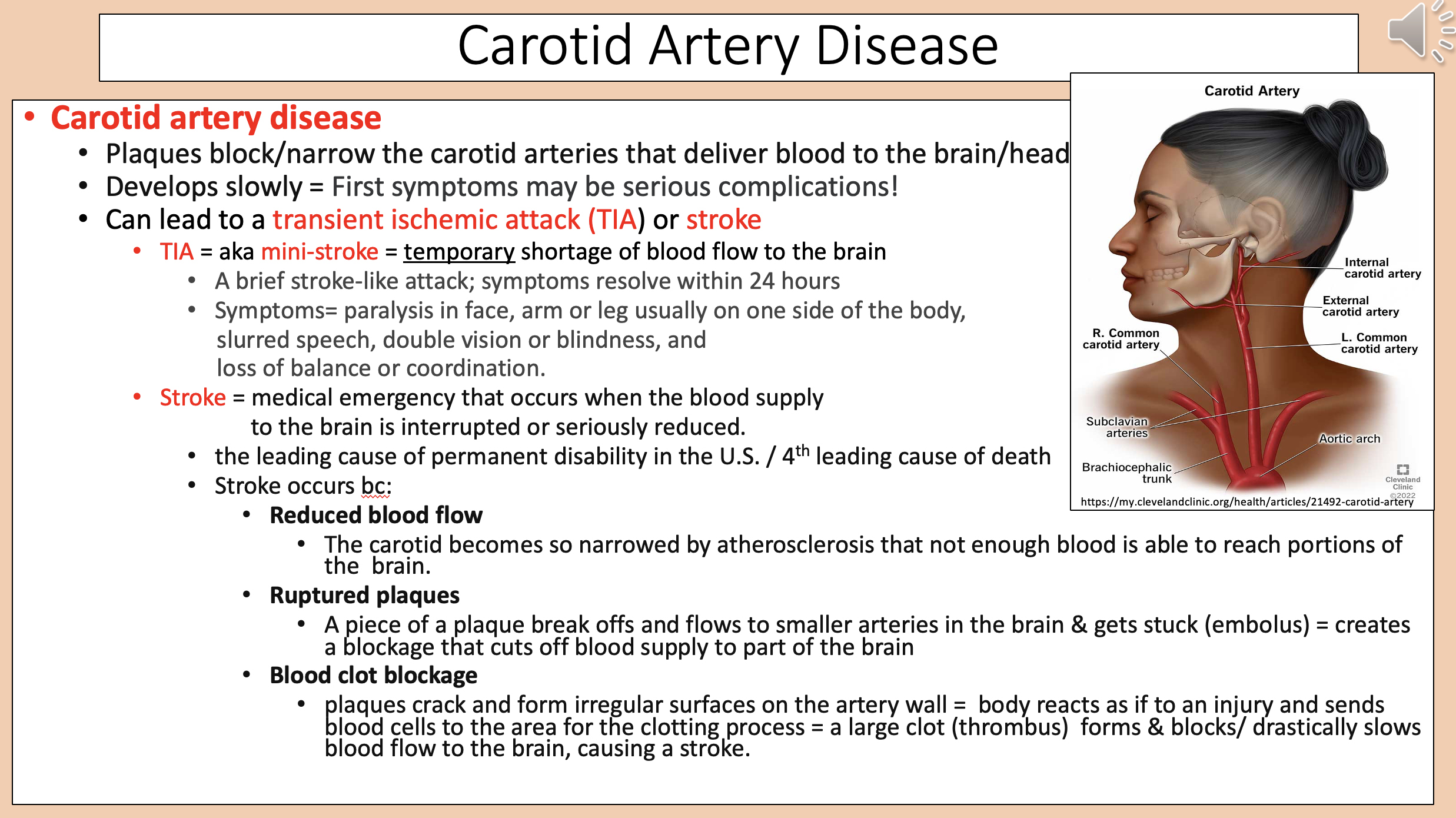
The carotid becomes so narrowed by atherosclerosis that not enough blood is able to reach portions of the brain
reduced blood flow
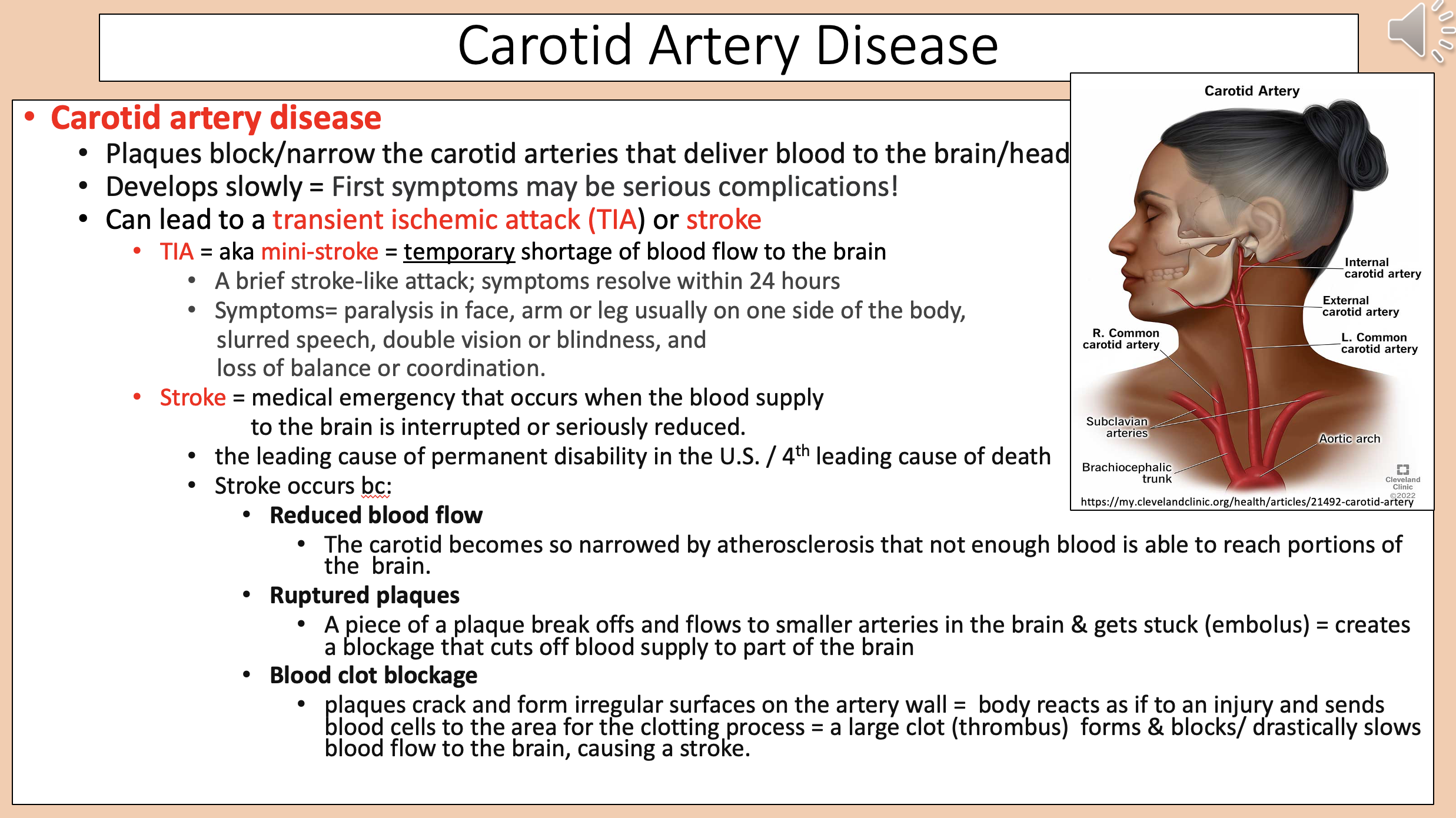
A piece of a plaque break offs and flows to smaller arteries in the brain & gets stuck (embolus) = creates a blockage that cuts off blood supply to part of the brain
ruptured plaques
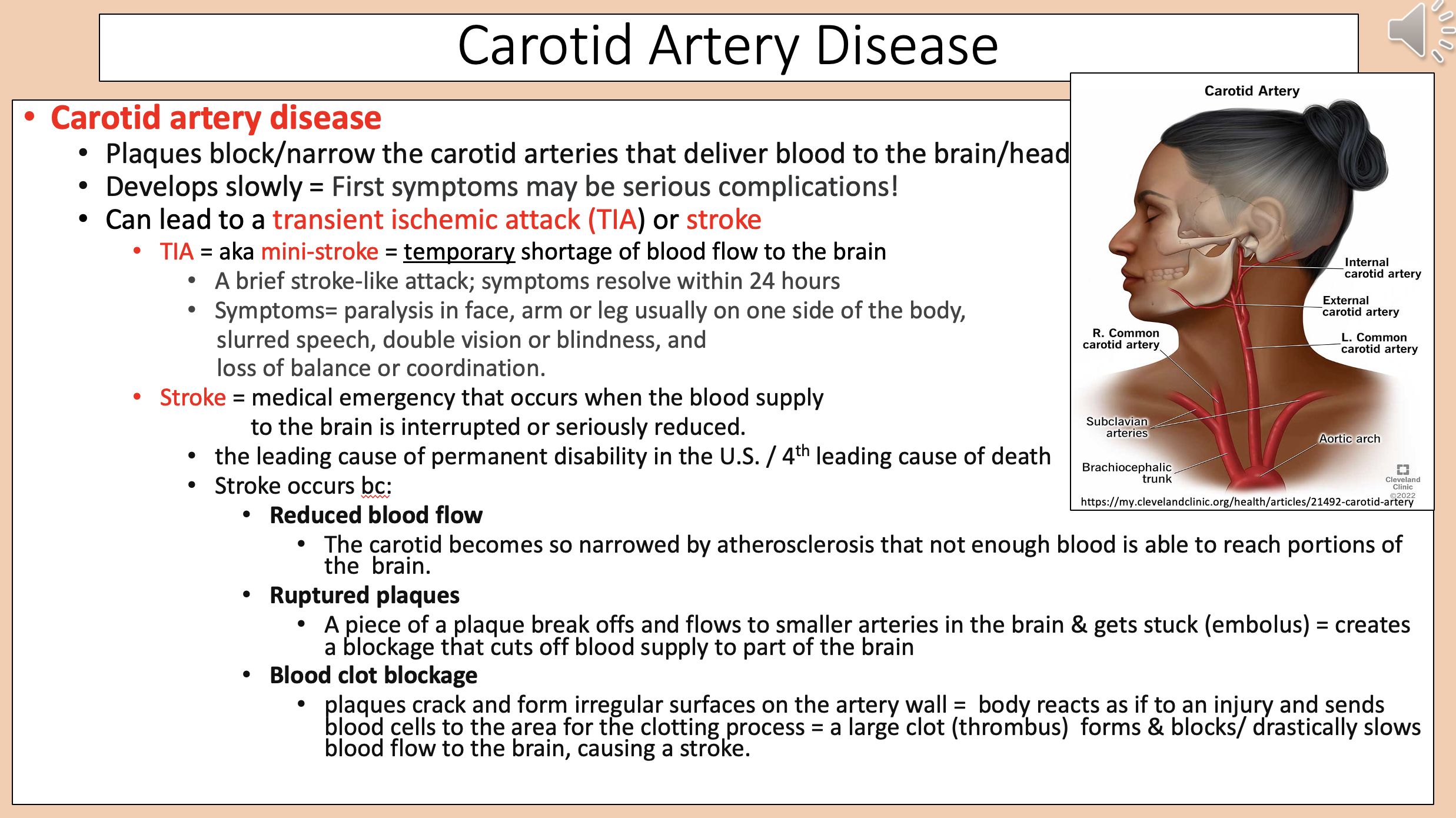
Plaques crack and form irregular surfaces on the artery wall = body reacts as if to an injury and sends blood cells to the area for the clotting process = a large clot (thrombus) forms & blocks/ drastically slows blood flow to the brain, causing a stroke
blood clot blockage
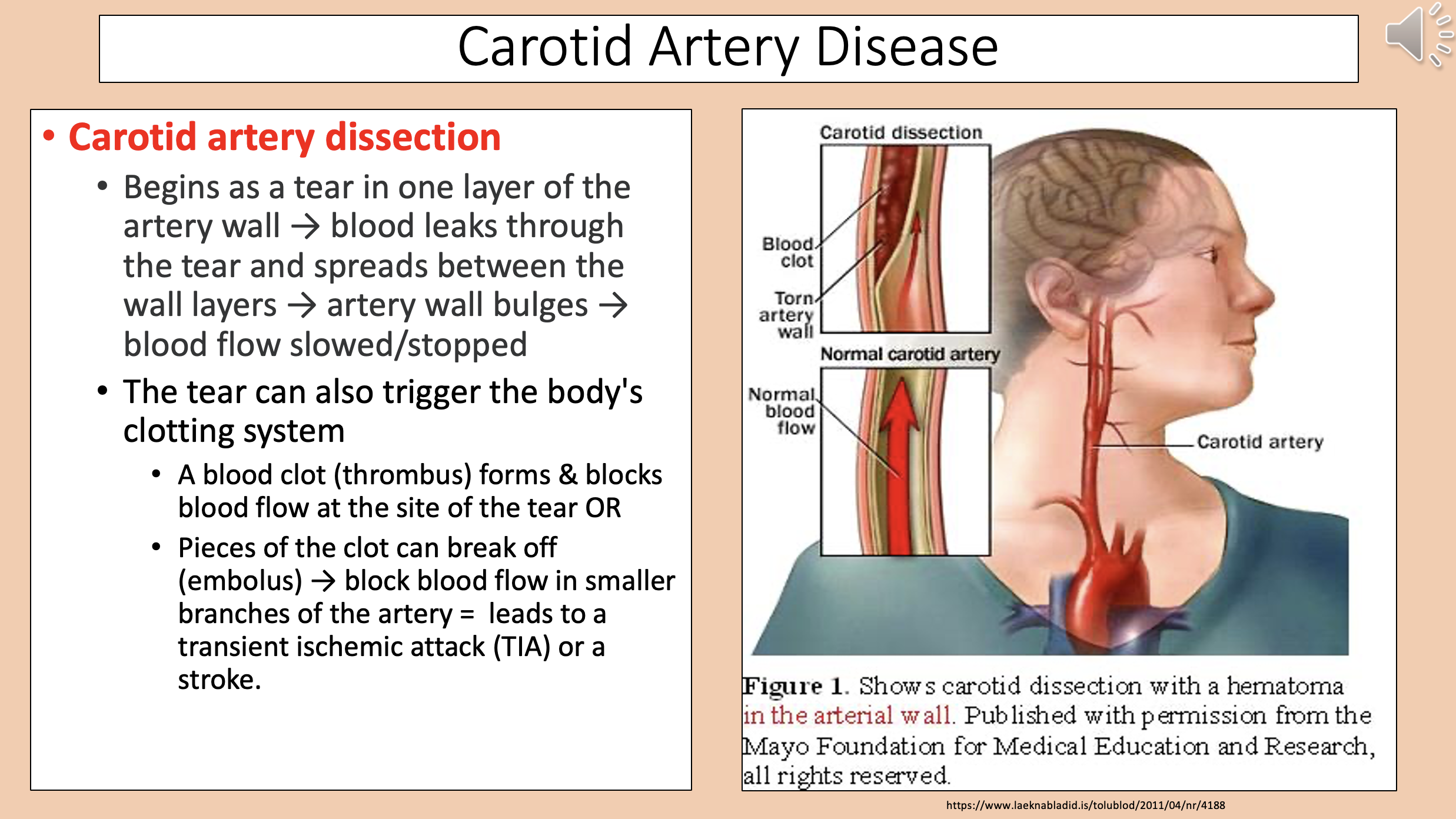
Begins as a tear in one layer of the artery wall → blood leaks through the tear and spreads between the wall layers → artery wall bulges → blood flow slowed/stopped.
The tear can also trigger the body's clotting system.
carotid artery dissection
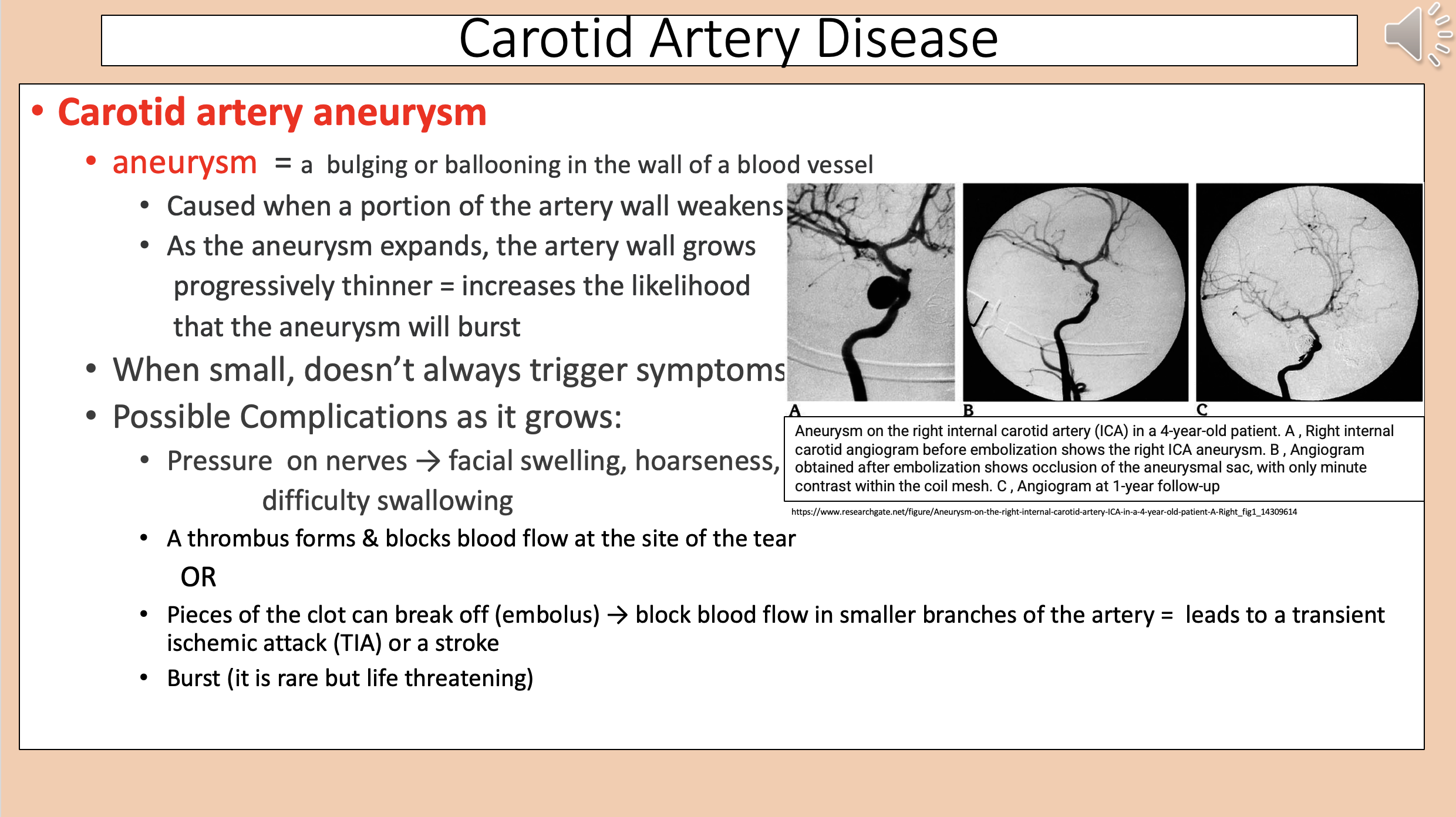
A bulging or ballooning in the wall of a blood vessel
aneurysm
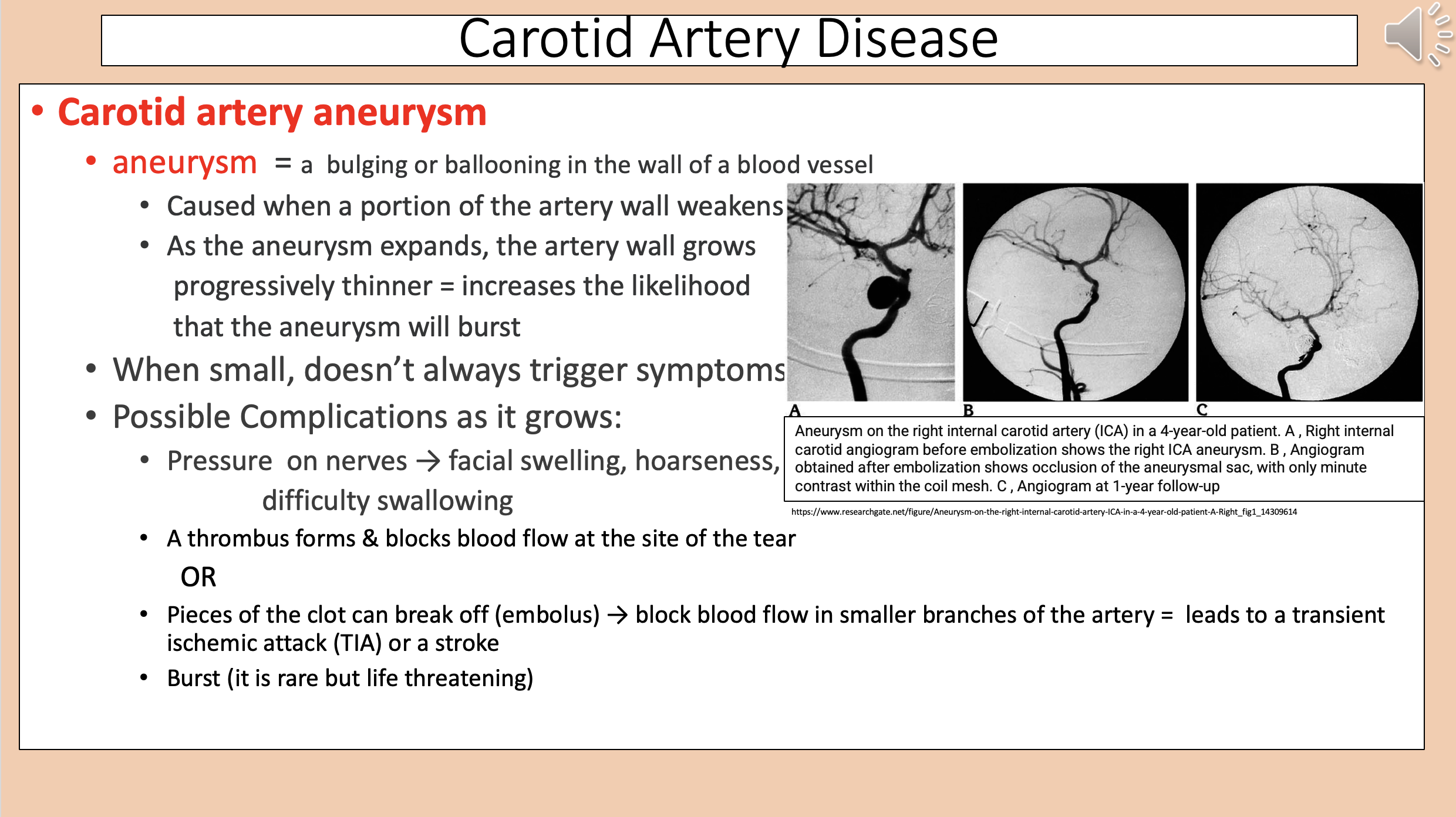
Caused when a portion of the artery wall weakens.
As the aneurysm expands, the artery wall grows progressively thinner = increases the likelihood that the aneurysm will burst.
carotid artery aneurysm
Most common type of aneurysm
aortic aneurysm
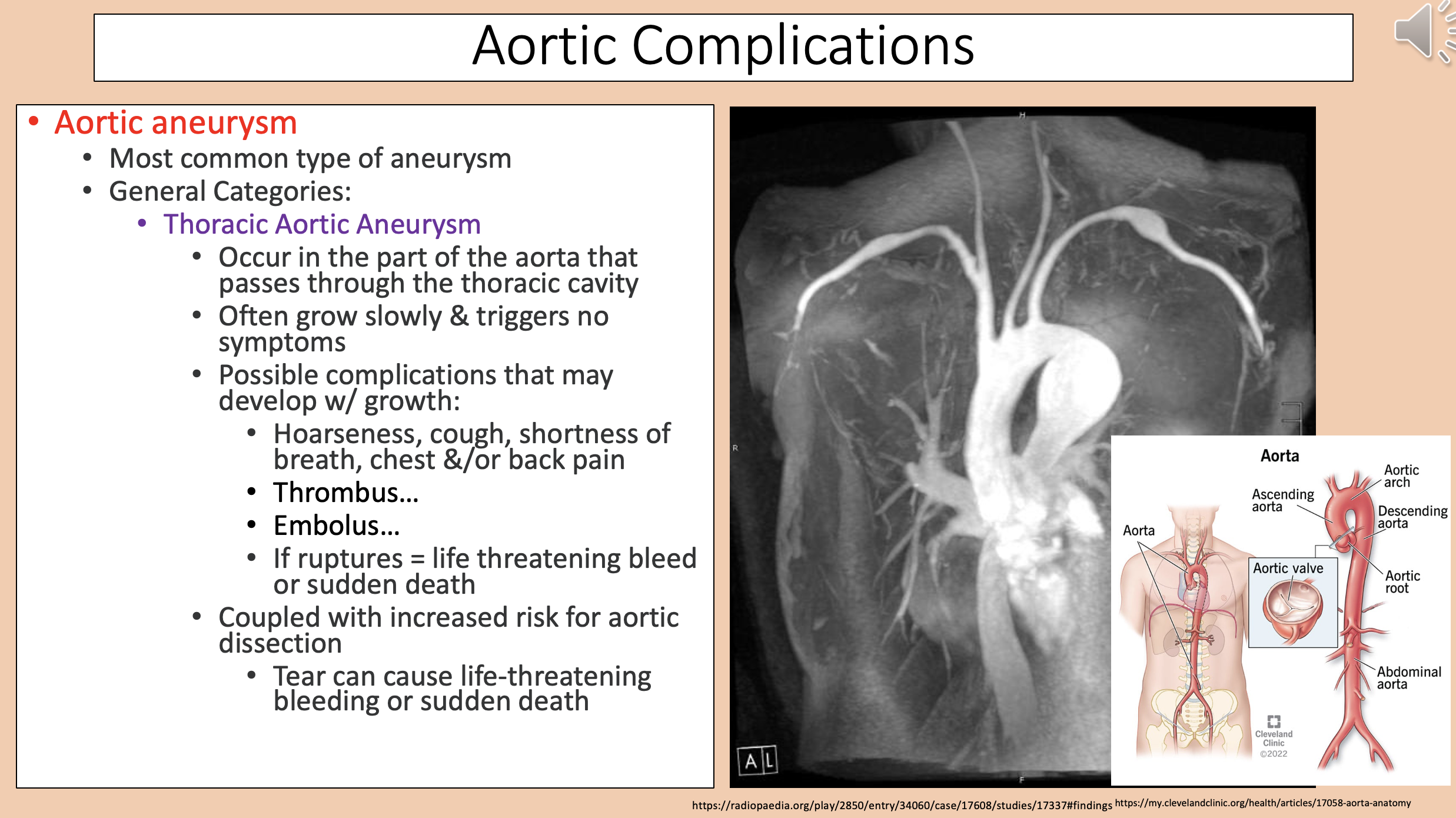
aortic aneurysm general categories
thoracic aortic aneurysm and abdominal aortic aneurysm
Occur in the part of the aorta that passes through the thoracic cavity.
Often grow slowly & triggers no symptoms.
thoracic aortic aneurysm
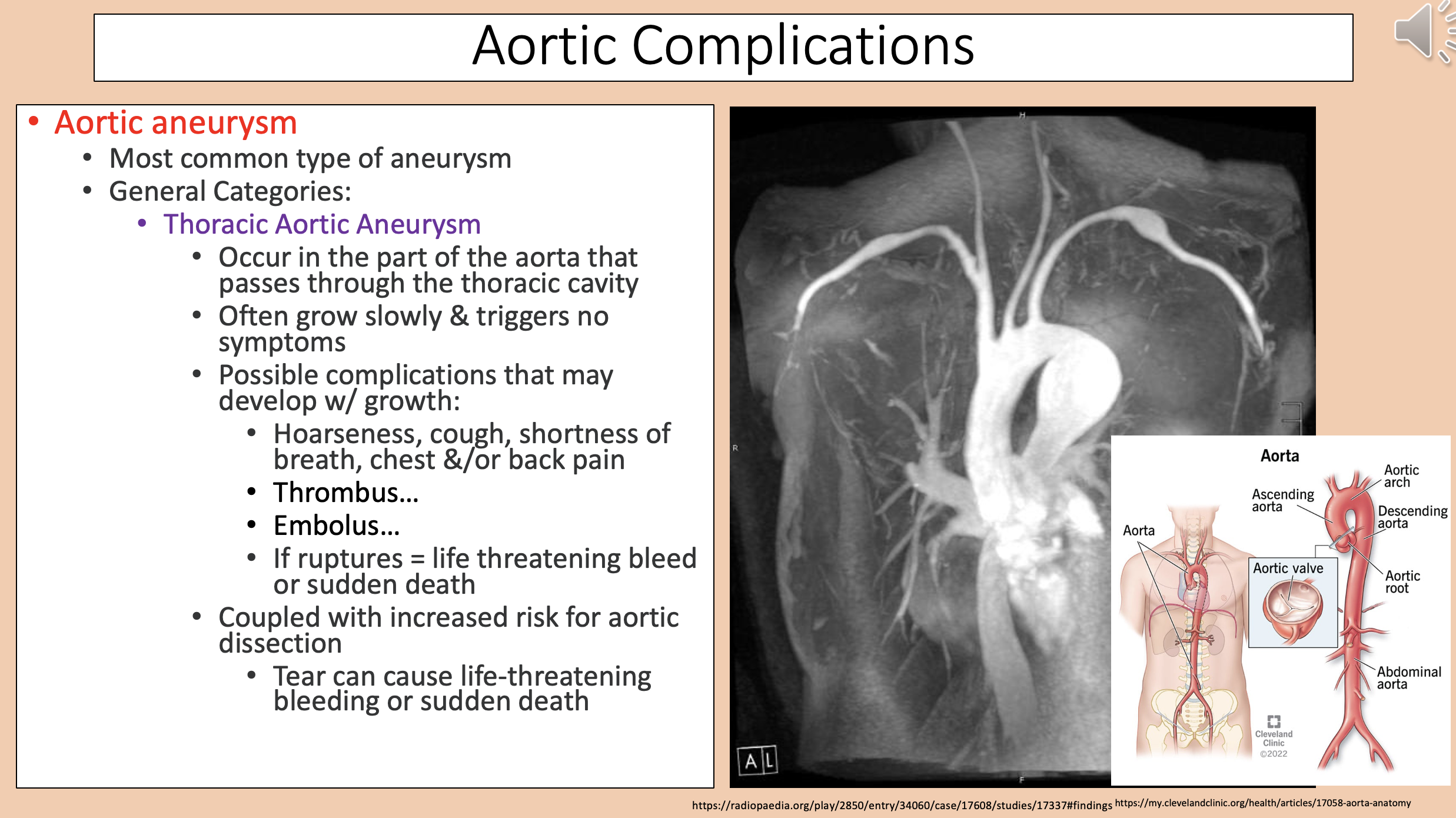
Hoarseness, cough, shortness of breath, chest &/or back pain.
Thrombus...
Embolus...
If ruptures = life threatening bleed or sudden death.
thoracic aortic aneurysm complications
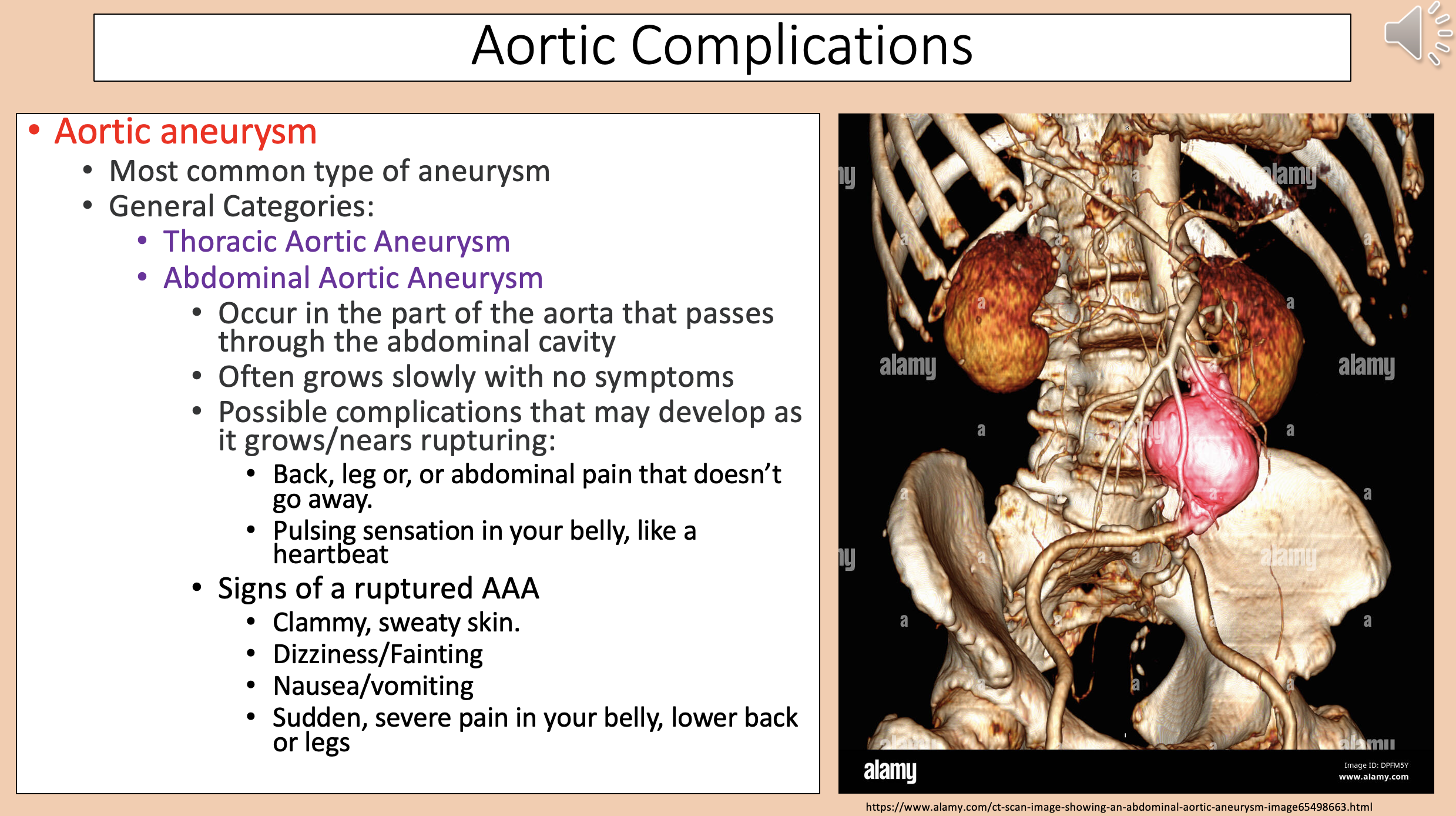
Occur in the part of the aorta that passes through the abdominal cavity.
Often grows slowly with no symptoms.
abdominal aortic aneurysm
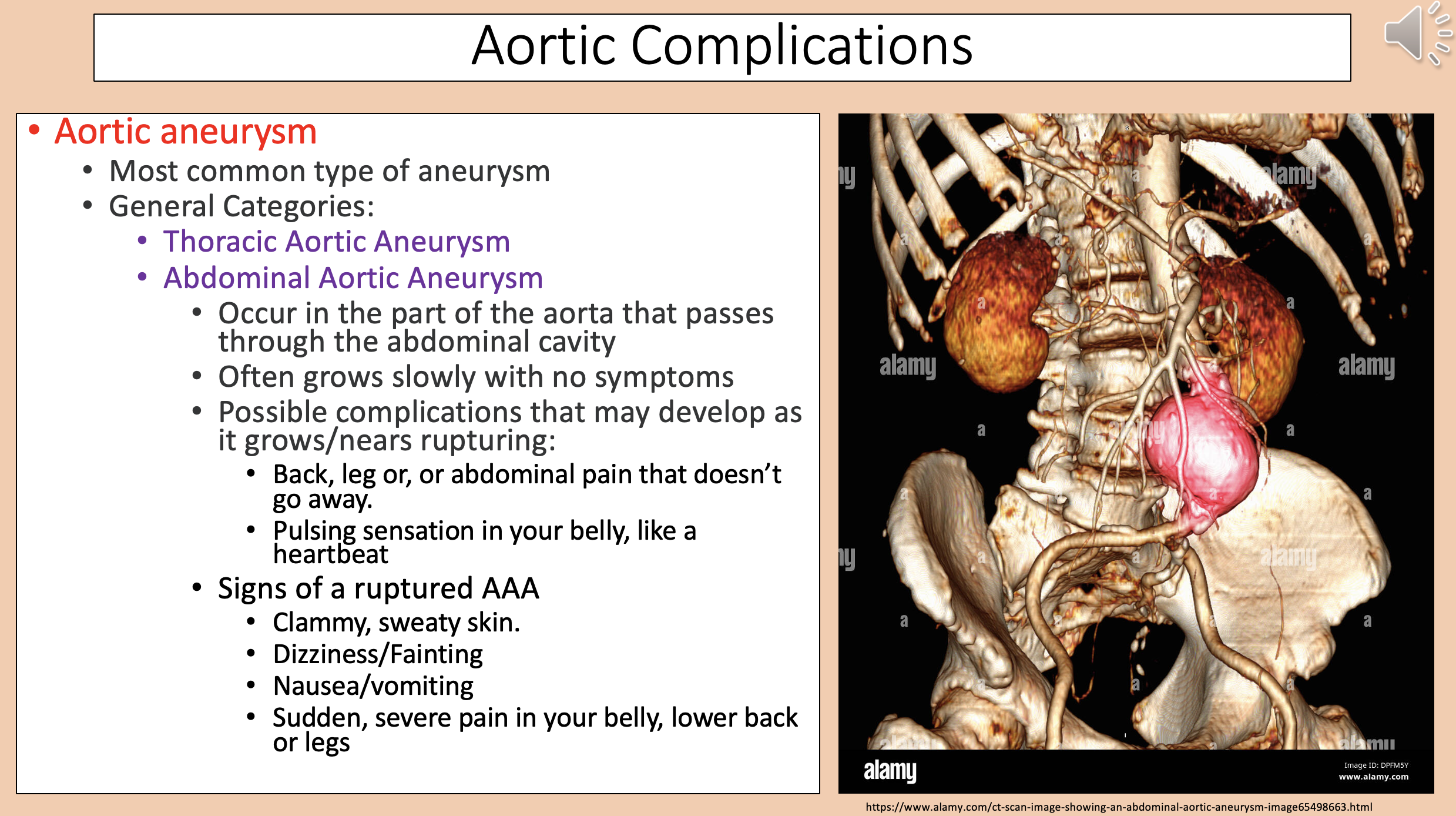
Back, leg or, abdominal pain that doesn’t go away.
Pulsing sensation in your belly, like a heartbeat.
abdominal aortic aneurysm complications
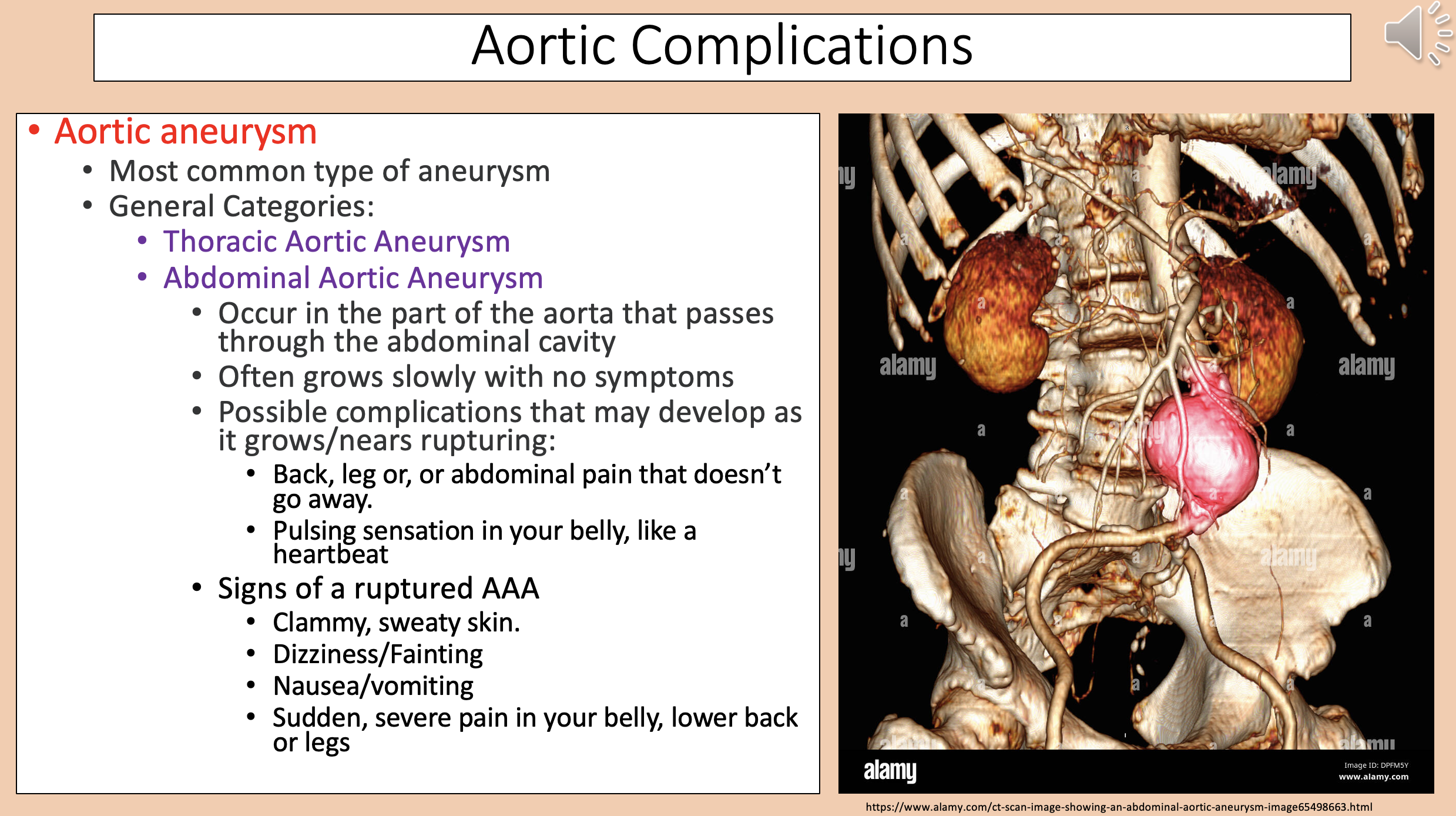
Clammy, sweaty skin.
Dizziness/Fainting.
Nausea/vomiting.
Sudden, severe pain in your belly, lower back or legs.
Signs of a ruptured AAA
Treatment for thoracic and aortic aneurysms
Monitoring.
Medications.
Surgery.