FNH 351 - Bone Nutrients: Vitamin D
1/45
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
46 Terms
What are the chemical forms of vitamin D that are physiologically relevant?
ergocalciferol (vitamin D2)
cholecalciferol (vitamin D3)
what do the physiologically forms of vitamin D differ in? Which one can be converted to the active form?
differ only in side chains. both can be converted to active form and have same metabolic activity
what is vitamin D derived from?
steroids
what is the active form of vitamin D?
1,25-(OH)2-cholecalciferol (or 1,25-(OH)2-vitamin D3) = calcitriol
what examples of food sources of vitamin D?
Fatty fish, liver, shitake mushrooms, fortified products (milk, orange juice)
what forms of vitamin D is found in food?
animal products – vitamin D3 / cholecalciferol
plants – vitamin D2 / ergosterol
what forms of vitamin D are found in supplements and fortified foods?
vitamin D2 / ergocalciferol
vitamin D3 / cholecalciferol (more effective in increasing vitamin D status)
explain the digestion of vitamin D
there is none required
where does vitamin D absorption occur?
mostly jejunum
how is vitamin D absorbed?
Absorbed in micelles by passive diffusion
Incorporated into chylomicrons in enterocyte
Chylomicrons → lymph → blood → vitamin D to extrahepatic tissues
Chylomicron remnants → remaining vitamin D to the liver
what form of vitamin D is synthesized endogenously? what is it synthesized from?
vitamin D3 (cholecalciferol). synthesized from 7-dehydrocholesterol in skin upon exposure to UVB light
what prevents overproduction of vitamin D?
generation of inactive metabolites
what does endogenous synthesis of vitamin D depend on?
Sunblocks and sunscreen use
Skin pigment (lower with darker skin pigment)
Aging (vitamin D synthesis decreases with age)
Time of day
Season
Latitude
explain the transport of different forms of vitamin D
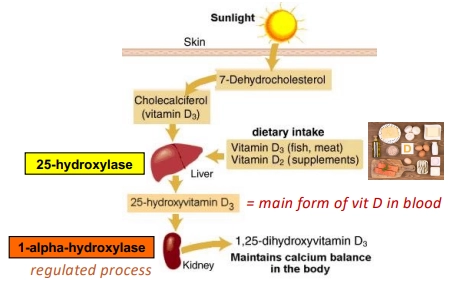
what happens to vitamin D in the liver?
most vitamin D gets converted. 25-hydroxylase converts vitamin D to active form (vitamin D3) - 25-hydroxyvitamin D3 (25-(OH)-D) and secreted into the blood circulation
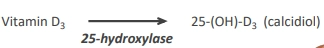
what is the major circulating form of vitamin D?
Plasma 25-(OH)-D
how is 25-(OH)-D transported?
has to be bound to vitamin-D binding protein (DBP)
what is the major storage site of vitamin D?
blood
what is vitamin D converted to in the kidney?
converted into 1,25-(OH)2-D = active form of vitamin D (= hormone) by 1-alpha-hydroxylase
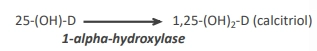
what regulates the conversion of vitamin D that occurs in the kidney?
↑ stimulated by parathyroid hormone (PTH), and low serum phosphate
↓ inhibited by higher concentration of 1,25-(OH)2-D, FGF23 hormone, and high serum phosphate
how is 1,25-(OH)2-D transported?
Loosely bound to vitamin-D-binding protein (facilitates tissue uptake). It has a short half-life.
what are 1,25-(OH)2-D’s target tissues?
bone, intestine, kidney, and also heart, muscle, pancreas, and central nervous system
what are other metabolites of vitamin D?
1,24,25-(OH)3 D via 24-hydroxylase
24R,25-(OH)2 D via 24-hydroxylase
Calcitroic acid
what is the major excretory product of vitamin D and how is vitamin D excreted?
Calcitroic acid is the major excretory product
Conjugation and excretion via the bile (happens in liver)
what are the metabolic functions of vitamin D?
genomic action - regulation of gene expression, e.g., calcium homeostasis
non-genomic action - activation of signal transduction pathways, physiological responses
vitamin D is involved in the regulation of > __ genes, including:
regulation of > 200 genes, including:
Calbindin, Ca-channel transporter, Ca2+-ATPase, osteocalcin (all of which are proteins that are important for absorption of calcium in the intestine)
what does calcitriol do in terms of gene expression and how does it do it?
it enhances gene expression by binding to vitamin D receptor (VDR) at the VDR/RXR complex, triggering the vitamin D response element to enhance gene expression
what are some effects of vitamin D genomic action on cells?
Increased expression of proteins needed to maintain calcium homeostasis
Promotes differentiation of white blood cells, intestinal epithelial cells and osteoclasts
Reduces cell proliferation of fibroblasts and keratinocytes
what is the non-genomic action of vitamin D?
Activation of signal transduction pathways via VDR or MARRS protein on cell membranes, leading to physiological responses.
What physiological processes may non-genomic actions of vitamin D affect?
Calcium absorption
Regulation of calcium channels in muscle
Maintenance of blood calcium homeostasis
what happens when blood calcium level is low?
Stimulates parathyroid hormone (PTH) release
PTH increases 1,25-(OH)₂-D synthesis in the kidney
Leads to:
Increased kidney calcium reabsorption
Increased intestinal absorption of calcium and phosphorus
Increased bone resorption of calcium and phosphorus
NET RESULT: Increased blood calcium
what are the nutrient-nutrient interactions with vitamin D?
calcium and phosphorus
dietary lipids (FAs)
vitamin A
vitamin A, E, and K
what is the nutrient-nutrient interaction with vitamin D and calcium & phosphorus?
Absorption and serum levels of calcium and phosphorus regulated by vitamin D
what is the nutrient-nutrient interaction of vitamin D with dietary lipids?
improve absorption of vitamin D
what is the nutrient-nutrient interaction of vitamin D with vitamin A
Gene expression control requires calcitriol and retinoic acid for vitamin D response element to exert its function
what is the nutrient-nutrient interaction of vitamin D with vitamins A, E, and K?
Vitamin D may compete for incorporation into micelles
What is the status biomarker for vitamin D?
Most commonly used indicator: plasma/serum 25-(OH)-D concentration
strong correlation with dietary vitamin D intake
What does vitamin D deficiency cause in infants and children?
rickets which is a disorder of failed bone mineralization, defective mineralization of cartilage in the epiphyseal growth plate, and bowing of legs with weight-bearing
What does vitamin D deficiency cause in adults?
Osteomalacia
Osteoporosis
what is osteomalacia?
impaired bone remineralization (“softening” of bones), and prolonged elevation of blood PTH
Why does vitamin D deficiency cause osteomalacia?
bc causes decrease in Ca absorption and decrease serum Ca → decrease Ca for bone mineralization. Also causes a decrease in phosphorus absorption. As bone turnover occurs, the bone matrix is preserved while bone mineralization is impaired
what is osteoporosis?
reduced total bone mass (density)
what are the risk factors for developing osteoporosis?
Non-modifiable
estrogen deficiency
ethnicity
family history
Potentially modifiable
Vitamin D deficiency
Excess alcohol
Smoking
Malnutrition, incl. calcium, phosphorus, magnesium
Physical inactivity
what are the potential causes of vitamin D deficiency?
Insufficient exposure to sunlight with inadequate intake
Limited time outside, use of sun protection (clothing, sunscreen), higher latitudes
Fat malabsorption and inadequate endogenous synthesis
what are the populations at risk for vitamin D deficiency?
Older adults: typically have lower intake and lower synthesis
Human milk fed infants: human milk low in vitamin D, infants most protected from sun exposure
what are symptoms of vitamin D excess?
Hypercalcemia
Calcification of soft tissues
Impaired renal function