BI315 Unit 3
1/144
Earn XP
Description and Tags
Lectures 19-Lecture 26
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
145 Terms
Internal transport fluid that is pumped through the circulatory system.
Transports dissolved and suspended substances
Composed of various cells suspended in plasma
Blood
Type of blood cells responsible for the gas exchange of O2 and CO2 in the blood via their expression of hemoglobin.
Red Blood Cells (Erythrocytes)
Type of blood cells that are specialized for immune functions.
Leukocytes (White blood cells)
Cell fragments important in blood clotting/wound healing.
Platelets
Percentage by volume of RBCs in the blood.
Hematocrit
A low hematocrit would indicate what?
A decreased percentage of RBCs, indicating low blood oxygen circulation (anemia).
Hematocrit is largely regulated by this hormone, which is secreted when O2 delivery to the kidneys is low.
Erythropoietin (EPO)
Illustrate the hormonal feedback loop resulting from low oxygen.
Low O2 —→ High EPO Secretion —→ High Plasma EPO —→ High Production of RBCs —→ High Blood Hb (hemoglobin) Concentration —→ High Blood O2-carrying capacity —→ Restoration of O2 Delivery
Path that blood moves through the circulatory system, starting with the right atrium of the heart:
Right atrium —→ Right AV Valve —→ Right Ventricle —→ Pulmonary Semilunar Valve —→ Pulmonary Circulation—→ Left Atrium —→ Left AV Valve —→ Left Ventricle —→ Aortic Semilunar Valve —→ Systemic Circulation
Gas exchange of O2 and CO2 occurs in the ___________, which carries blood from the ____________ to the ____________.
pulmonary circuit | right ventricle | left atrium
Oxygenated blood is circulated via the ____________, which carries blood from the ________ to the _____________.
systemic circuit | left ventricle | right atrium
Path that blood moves as it is passing through the pulmonary circuit:
Right ventricle —→ Pulmonary valve —→ Pulmonary trunk —→ Pulmonary arteries —→ Pulmonary arterioles —→ Capillaries of lungs —→ Pulmonary venules —→ Pulmonary veins —→ Left atrium
Path that blood moves as it is passing through the systemic circuit:
Left ventricle —→ Aortic valve —→ Aorta —→ Systemic arteries —→ Systemic arterioles —→ Capillaries of body —→ Systemic venules —→ Systemic veins —→ Venae cavae —→ Right atrium
Movement of blood away from the heart is facilitated by…
Arteriolar circulation
Movement of blood towards the heart is facilitated by…
Venous circulation
The flow of blood to and from the tissues of the heart muscle, supplying oxygen and nutrients while removing waste products.
Coronary Circulation
Major differences between cardiac myocytes and skeletal myocytes:
Cardiac myocytes are electrically couple to each other via gap junctions.
Cardiac myocyte contractions are initiated by the electrical activity of other cardiac myocytes.
Cardiac myocytes express receptors for multiple hormones and neurotransmitters.
Cardiac action potentials are prolonged, cardiac twitches do not summate.
Specialized intercellular connections that facilitate electrical and metabolic communication between adjacent cardiac myocytes.
Gap junctions
Specialized cells in the heart that regulate the heartbeat by generating electrical impulses, primarily located in the sinoatrial node; control timing and rhythm of heart contractions.
Pacemaker cells
Path that leads to heart contraction:
SA node cells fire action potentials —→ Depolarization of atrial cardiac myocytes —→ AV node cells fire action potentials —→ Depolarization down the bundle of His —→ Depolarization spreads through ventricular cardiac myocytes
Hormones that speed up bursting frequency of SA node cells, increasing heart rate.
Norepinephrine and epinephrine
Hormones that slow the bursting frequency of SA node cells, decreasing heart rate.
Acetycholine
Streamlined Pulmonary Circuit pathway:
Right ventricle —→ Pulmonary semilunar valve —→ Pulmonary Artery—→ Lungs —→ Pulmonary veins —→ Left atrium
Streamlined Systemic Circuit Pathway:
Left Ventricle —→ Aortic semilunar valve —→ Aorta —→ Body tissues —→ Right atrium
Wigger’s Diagrams tell us…
the relationship between pressure, volume, and heart sounds during the cardiac cycle
Term used to refer to periods on the Wigger’s Diagram when blood is being pumped out and into circulation.
Systole
Term used to refer to periods on the Wigger’s Diagram where blood is being pumped into the heart.
Diastole
During systole, the pressure of the ___________ is approximately equal to the pressure of the ______.
left ventricle | aorta
During systole, the volume of the left ventricle is ____________, as blood is flowing from ____________ to _________.
decreasing | the left ventricle | the aorta
On a Wigger’s Diagram, what does the electrocardiogram tell us?
SA Node firing an action potential.
From start to end, one systole period is equal to ____________.
one heart beat
During diastole, what is happening in the left ventricle?
The left ventricle is passively filling with blood, preparing for the next contraction.
What is the purpose of the atria contracting right at the end of diastole?
To push remaining blood into the ventricles, optimizing filling.
At the very beginning of systole, what is true of the valves?
All of them are closed.
The _______ must contract first, before the ________ can contract in the heart.
atria | ventricle
A phase of the cardiac cycle where the ventricles contract without a change in volume, leading to increased pressure.
Occurs at the peak of Systole
Isometric Volume
A valve located between the right ventricle and the pulmonary artery that prevents blood from flowing back into the heart after it has been pumped to the lungs.
Pulmonary Semilunar valve
A valve situated between the left ventricle and the aorta that prevents backflow of blood into the heart after it has been pumped into the systemic circulation.
Aortic semilunar valve
Valve, also known as the tricuspid valve, located between the right atrium and right ventricle, preventing backflow during ventricular contraction.
Right AV
Valve, also known as the mitral valve, situated between the left atrium and left ventricle, preventing backflow during ventricular contraction.
Left AV
Heart valves enforce two-way flow, blood can flow in either directional without consequence.
False
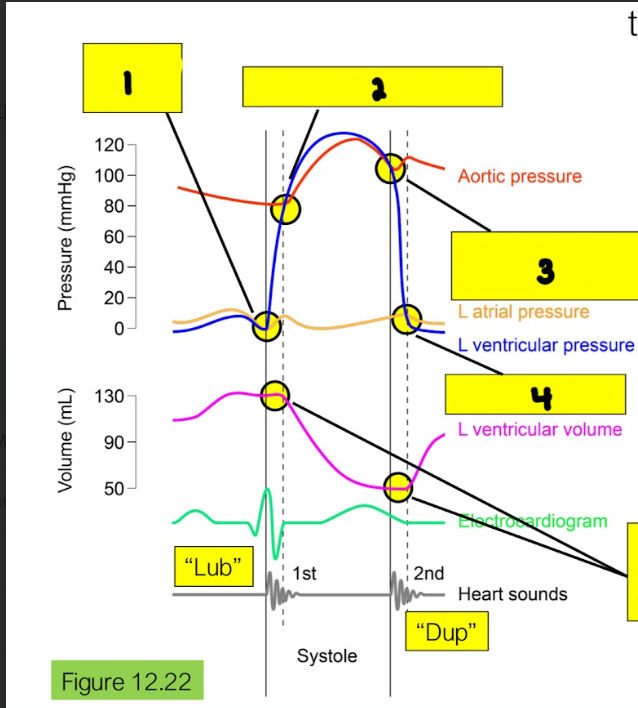
What is happening in box 1?
Left AV Closes
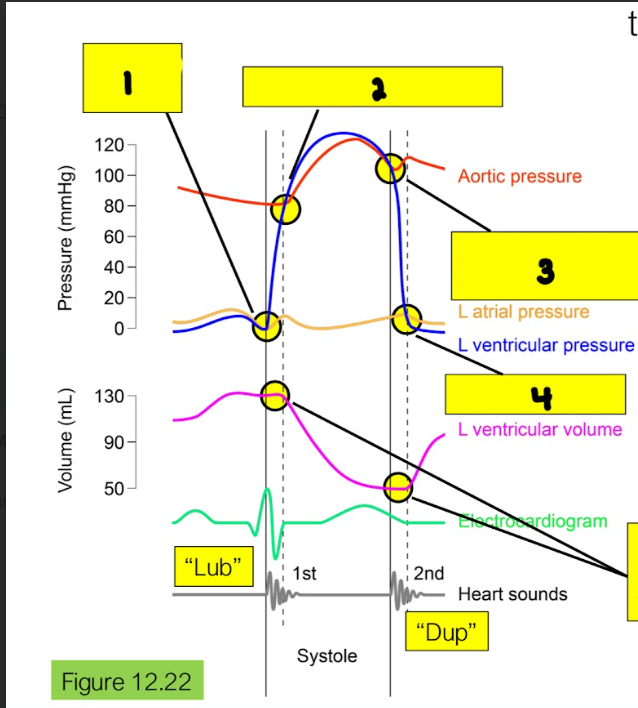
What is happening in box 2?
Aortic semilunar valve opens
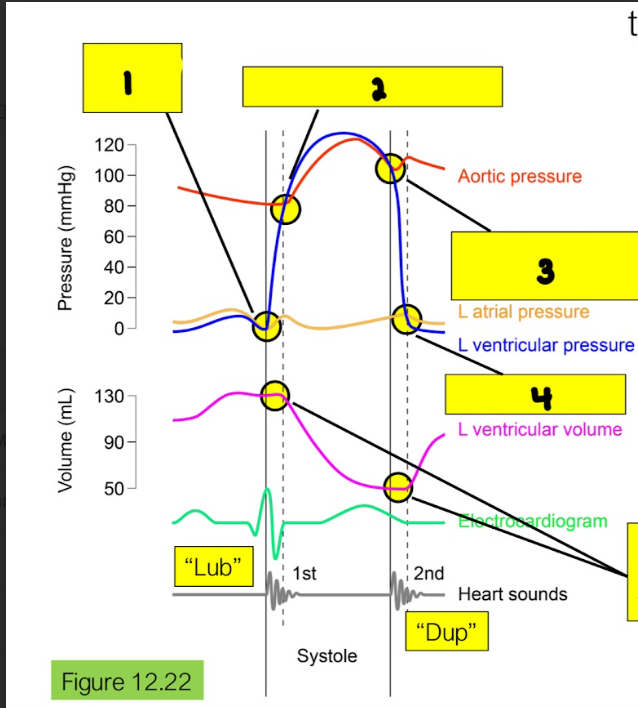
What is happening in box 3?
Aortic semilunar valve closes
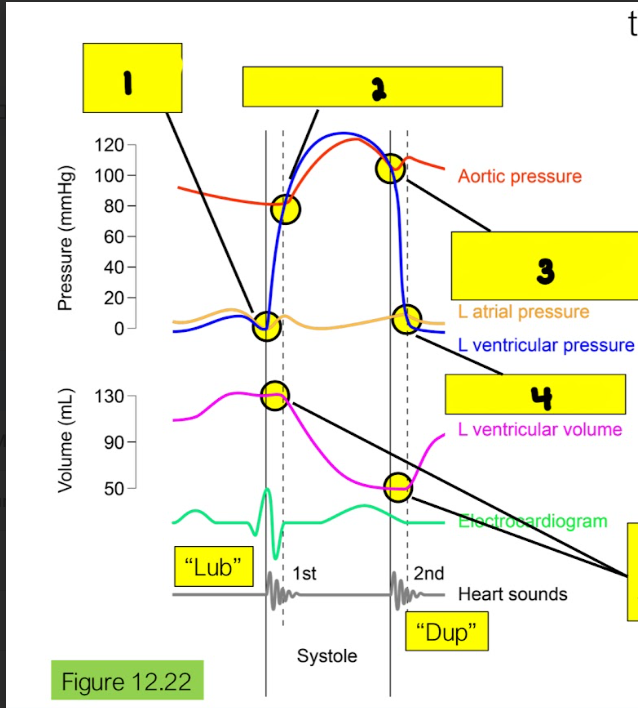
What is happening in box 4?
Left AV opens
Amount of blood pushed out into circulation.
Stroke Volume (SV)
Determines the rate at which the circulatory system delivers blood to the capillary beds; determines rate at which cells get oxygen; variable.
Cardiac Output (CO)
Equation for Cardiac Output
CO = HR x SV (HR is heart rate)
A condition resulting from reduced blood flow to tissues, leading to a shortage of oxygen and nutrients necessary for cellular metabolism.
Ischemia
Severe ischemia can lead to heart tissue damage called…
myocardial infarction.
A process where tissue dies due to a lack of blood supply, typically resulting in significant damage to the affected organ.
Infarction
A type of pain that originates from the internal organs, often described as deep, squeezing, or diffuse, and is usually associated with autonomic responses.
Visceral Pain
Pain perceived at a location different from the source, often due to shared afferent pathways.
Referred Pain
Irregular heartbeats that may disrupt normal blood flow, leading to various symptoms such as palpitations, dizziness, or even fainting.
Cardiac Arrythmia
Heart condition where the heart beats slower than normal.
Bradycardia
Heart condition where the heart beats faster than normal.
Tachycardia
A serious cardiac arrhythmia characterized by rapid, ineffective contractions of the ventricles, leading to loss of pulse and cardiac output. It is a medical emergency that requires immediate treatment.
Ventricular Fibrillation
Highly irregular, uncoordinated activity of myocytes that prevents normal chamber contraction.
Atrial Fibrillation
Sudden ventricular fibrillation caused by chest impact.
Commotio cordis
Medical device useful for bradycardias or other issues where normal pacemaking by the SA node is affected.
Pacemakers
Medical device useful for rescuing the heart from fibrillation events.
Defibrillators
Vessel types that make up the vasculature:
Arteries
Veins
Capillaries
Blood vessels that carry deoxygenated blood back to the heart, except for the pulmonary ____, which carry oxygenated blood from the lungs.
Veins
Blood vessels that carry oxygenated blood away from the heart, except for the pulmonary _____, which carry deoxygenated blood from the heart to the lungs.
Arteries
Smallest blood vessels that facilitate the exchange of oxygen, carbon dioxide, nutrients, and waste products between blood and tissues.
Capillaries
Equation for Flow Rate and what each variable stands for:
Flow Rate= (Pin-Pout)/R
where Pin is the inlet pressure, Pout is the outlet pressure, and R is the resistance to flow.
In the equation R (resistance of flow) what is the only appreciably change?
Radius of blood vessel
Changes in blood vessel diameter that regulate blood flow and blood pressure. These responses can lead to vasodilation or vasoconstriction.
Vasomotor Responses
Capillaries have a _______ flow rate because there are so many of them.
slow
Equation for Mean Arterial Pressure:
MAP = CO x TPR (total peripheral resistance)
Combined resistance to flow of all the systemic arterial blood vessels.
Total Peripheral Resistance (TPR)
The circulation of blood in the blood vessels of the heart muscle, supplying oxygenated blood and nutrients while removing waste products.
Coronary Circulation
The process by which deoxygenated blood returns to the heart through the veins after delivering oxygen and nutrients to the body's tissues.
Venous Circulation
A mechanism that assists venous return to the heart by contracting skeletal muscles, which compress veins and propel blood towards the heart.
Skeletal Muscle Pump
A mechanism that aids venous return to the heart by creating pressure changes in the thoracic cavity during inhalation and exhalation, which helps pull blood back towards the heart.
Respiratory Pump
Mechanism describing the relationship between the volume of blood filling the heart (preload) and the subsequent force of contraction, whereby an increased volume leads to a stronger heart contraction.
Frank-Starling Mechanism
Equation for Flow Rate of any given organ:
Floworgan=MAP/Rorgan
The increase in blood flow to an organ or tissue in response to increased metabolic activity, ensuring adequate oxygen and nutrient delivery during heightened demand.
Active Hyperemia
Cascade of Active Hyperemia:
Increased Metabolic Activity of Organ —→ Decreased O2, Increased metabolites in organ interstitial fluid —→ Vasodilation of arterioles —→ Increased blood flow to organ
Vasomotor responses are controlled by…
Local Controls
Extrinsic Controls
Interoceptors that monitor MAP (blood pressure) and contribute to its homeostatic regulation.
Baroreceptors
All else constant, if there is an increase in the firing rate of baroreceptors, then the firing rate of ___________ nerves to the heart would be predicted to ____________ as part of the homeostatic control of MAP.
sympathetic, decrease
Vasodilation will lead to an increase in all of the following, except…
Total Pressure Resistance
The process by which blood flows through the capillaries. It is essential for the exchange of oxygen, nutrients, and waste between blood and tissues.
Capillary Perfusion
The process of delivering nutrient- and oxygen-rich blood through the circulatory system to tissues and organs
Perfusion
The movement of fluid and solutes across the capillary wall driven by pressure differences. It facilitates the transfer of substances between blood and interstitial fluid.
Faster than diffusion
Requires energy input by pump
Bulk Flow
Where does gas/nutrient exchange occur with tissues?
Capillary beds
Transport processes at play in capillary beds:
Diffusion
Active Transport
Transcytosis
Ultrafiltration
Endocytosis and exocytosis through an endothelial cell.
Usually reserved for larger molecules, like protein hormones.
Transcytosis
Bulk flow of water and small solutes through clefts/fused-vesicle channels caused by pressure differences between the blood and interstitial fluid.
Can impact different solutes differently due to the filtering properties of the pores through the cells and the presence of the endothelial glycocalyx.
Ultrafiltration
What are the two classes of force that govern filtration across the epithelia?
Hydrostatic pressure
Osmotic pressure
Across the capillary, the hydrostatic pressure is ____________ the osmotic pressure, so the net filtration rate flows from the ________ to the _________.
greater than | plasma | interstitial fluid
The forces that predict the movement of fluid across capillaries, including hydrostatic and osmotic pressures, affecting filtration and absorption.
Starling Forces
Similarities Between Cardiovascular System & Respiratory System
Integrated gas exchange system
Internal transport systems that move a fluid by bulk flow
Flow rate = P/R
Terminal tubes are finely branched, increasing surface area and thus diffusion
The flow of air in and out of the lungs during respiration, involving both inhalation and exhalation; flowing in and out of the same tube.
Tidal Flow
The main airway that conducts air into the lungs, branching into bronchi, and is supported by cartilage to keep it open.
Trachea
The major air passages that branch from the trachea into each lung, leading to smaller bronchioles. They play a crucial role in air conduction and respiratory function.
Bronchi
The smaller air passages that branch off from the bronchi, leading to alveoli, where gas exchange occurs. They regulate airflow and are vital for respiratory function.
Bronchioles
Tiny air sacs in the lungs where gas exchange occurs, allowing oxygen to enter the blood and carbon dioxide to be expelled. They increase the surface area for efficient respiration.
Alveoli
What makes up the conducting zone in the respiratory system?
Trachea
Bronchi
Bronchioles
Terminal Bronchioles