Serology Lab final
1/13
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
14 Terms
What are 4 key points about influenza?
• It’s a contagious respiratory illness.
• It ranges from mild to severe, with possible complications.
• It spreads mainly via droplets (when people cough, sneeze, or talk).
• Annual vaccination is the best way to prevent it. 
What are common symptoms of influenza and who is at higher risk for complications?
• Symptoms: fever, chills, cough, sore throat, runny or stuffy nose, muscle aches, fatigue, headache, sometimes vomiting or diarrhea.
• Higher-risk groups: young children, people 65 and older, pregnant people, those with chronic conditions (like lung or heart disease), and immunocompromised individuals. 
What’s the difference between antigenic drift and antigenic shift in influenza?
• Antigenic drift: small, gradual mutations in the virus → leads to seasonal flu changes.
• Antigenic shift: a major, sudden change → can cause new virus strains and potentially pandemics.
⸻
What are 3 key points about EBV?
• Very common virus.
• Spread through saliva.
• Can cause infectious mononucleosis (“mono”).
Who is at risk for EBV, what does latency mean, and how does EBV spread?
• Risk: Teens, young adults, immunocompromised people.
• Latency: EBV remains dormant in B cells, even after symptoms resolve.
• Spread: Through saliva (kissing, sharing drinks/food), also possibly through other body fluids.
What are three simple prevention strategies for EBV?
• Avoid sharing utensils, cups, or toothbrushes.
• Avoid deep kissing with someone who has mono.
• Practice good hygiene (wash hands, don’t share saliva-contaminated items).
What do the EBV antibodies VCA IgM, VCA IgG, EA, and EBNA indicate?
• VCA IgM: Indicates a recent or acute EBV infection.
• VCA IgG: Indicates a past or current infection.
• EA (Early Antigen): Suggests active viral replication (acute).
• EBNA (Epstein-Barr Nuclear Antigen): Usually appears later and indicates past infection.
What is the Monospot test, and what are its limitations?
• Detects heterophile antibodies, which are produced in response to EBV.
• Limitations: Less reliable in young children; false negatives possible.
⸻
How is HIV transmitted and how is it not transmitted?
• Transmitted by: blood, sexual contact, shared injection equipment (needles), breast milk, perinatal transmission (mother → child).
• Not transmitted by: casual contact (hugging, shaking hands), sharing food, mosquitoes, saliva (in general), or tears/sweat.
What are the three stages of HIV infection?
• Acute HIV infection: Flu-like symptoms, very high viral load.
• Chronic (latent) HIV infection: Virus is active but reproduces at lower levels; can last many years.
• AIDS: Defined by CD4 count < 200 cells/mm³ or presence of AIDS-defining illness.
What types of HIV tests exist and what are their pros and cons?
• Antibody-only tests: Cheap, fast; but they have a longer “window period.”
• 4th-generation antigen/antibody tests: Detect p24 antigen + antibodies → shorter window, more sensitive.
• NAT / PCR (viral load) tests: Detect HIV RNA directly → most sensitive, but expensive and not routine for screening.
What are ART, PrEP, and PEP in HIV care?
• ART (Antiretroviral Therapy): Daily treatment to suppress HIV.
• PrEP (Pre-Exposure Prophylaxis): Medicine taken before exposure by HIV-negative people to prevent infection.
• PEP (Post-Exposure Prophylaxis): Emergency HIV prevention taken after potential exposure, must be started within ~72 hours.
What are 5 fast, important facts about HIV?
• Higher viral load = greater risk of transmission.
• ART reduces viral load, potentially to undetectable levels. 
• U = U (“Undetectable = Untransmittable”) — people with sustained undetectable viral load do not sexually transmit HIV. 
• With treatment, people with HIV can live long, healthy lives. 
• Prevention (PrEP/PEP) + regular testing are extremely effective in reducing new HIV infections. 
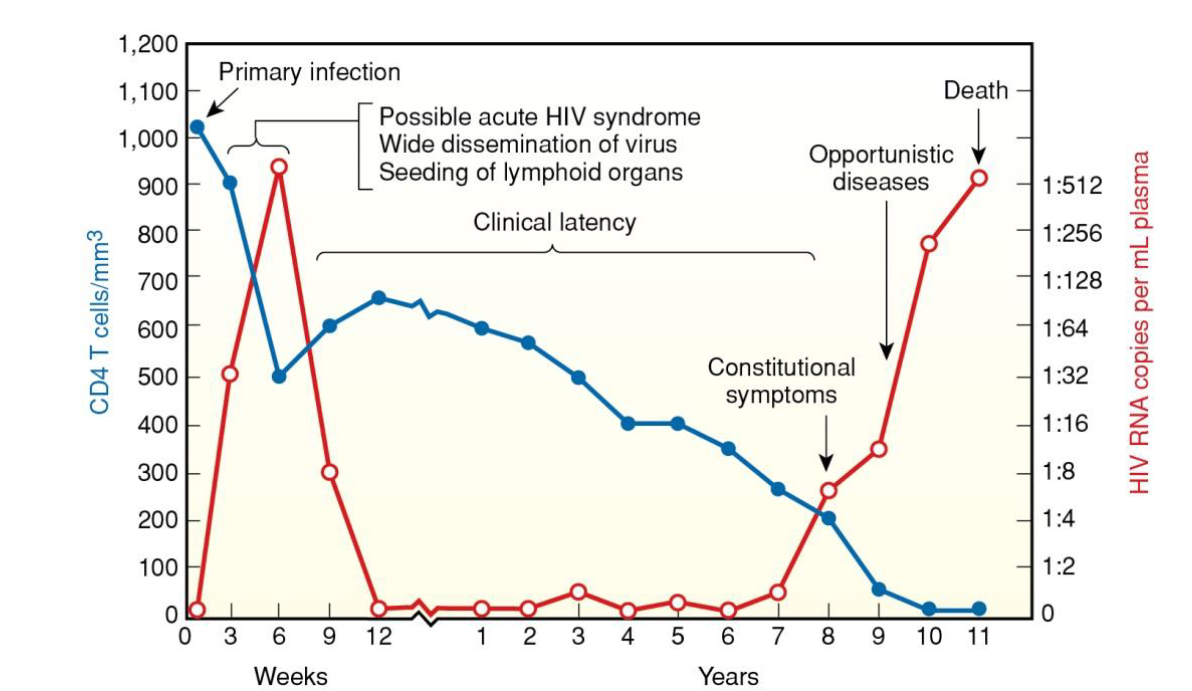
What does the CD4 count / viral load graph show throughout HIV infection?
• Acute phase: Viral load spikes; CD4 count drops.
• Chronic phase: Viral load drops (if untreated, stable-ish), and CD4 declines slowly.
• AIDS: Viral load rises again; CD4 falls below ~20