Immunity and lymphatic system
1/41
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
42 Terms
What is blood?
A (liquid) connective tissue composed of cells and a fluid extracellular matric
It performs transport, regulatory and protective functions
Label the components inside the blood
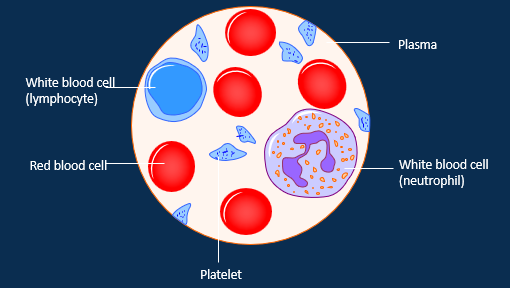
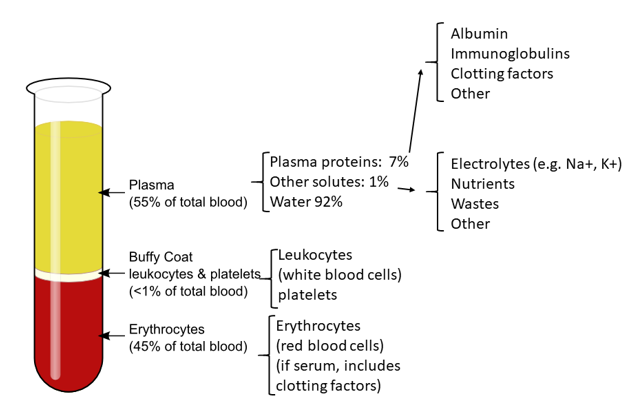
What are the percentages of the compotents of blood?
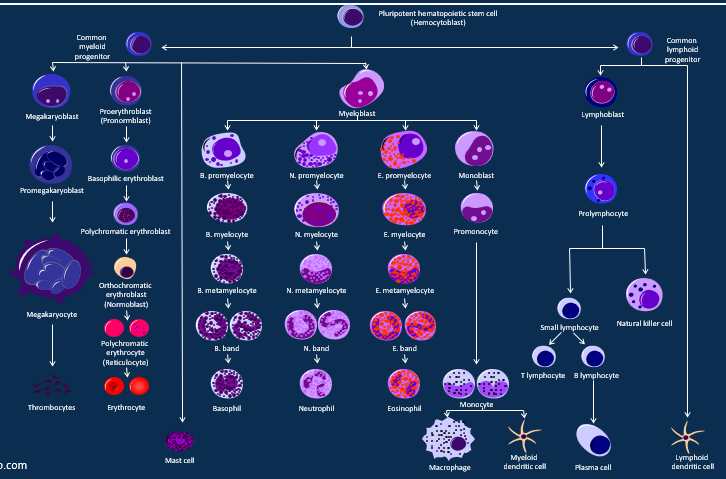
Describe haemopoiesis
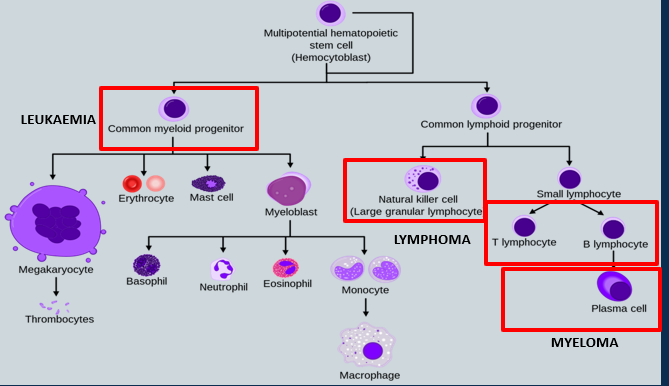
What is leukaemia
common myeloid progenitor
(a multipotent stem cell in the bone marrow that differentiates into non-lymphoid blood cells, including red blood cells, platelets, and most white blood cells)
What is lymphoma
- natural killer cell (large granular lymphocyte)
What cells count as myelomas?
T lymphocytes
B lymphocytes
Plasma cells
Label the diagram of hemocytobasts/ blood cancers
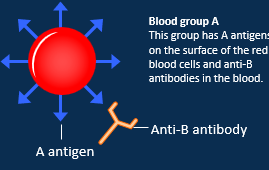
Describe A blood group
A antigens on its surface
anti-B antibodie in the blood
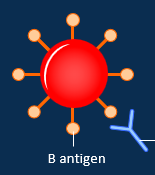
Describe B blood group
B antigens on its surface
anti-A antibodies in the blood
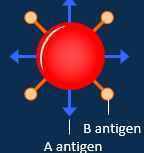
Describe AB blood group
Has both A and B antigens on its surface
No antibody on the surface
Rarest blood group
Describe O blood group
No red blood cell antigens on its surface
Anti-A and anti-B antibodies in the blood
most common

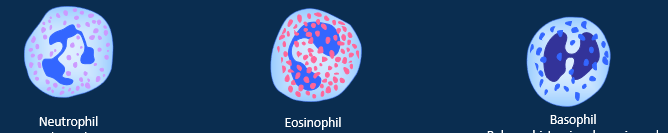
What are the granular types of leucocytes
Neautrophil= first responders, phagocytosis and release toxins
Eosinophil= manages allergic reactions and parasitic infections, releases cytotoxins, proteins and lysozymes
Basophil= releases histamine, heparin and serotonin during inflammation and allergic reactions. closely related to mast cells
What are the agranular types of leucocytes
Monocyte= macrophage, fixed and wandering. Transform into phagocytes when active.
Lymphocytes= T cell, B cell and Natural Killer cell which control adaptive immune response. develop in primary lymph organs (red bone marrow and thymus) and undertake functions in secondary lymph organs (spleen, lymph nodes, tonsils, appendix and other lymphoid tissues)

Describe the lymphatic system
• It drains excess interstitial fluid, transports dietary lipids/ fat-soluble vitamins, and facilitates immune responses
• Lymph vessels have permeable walls and valves.
• Lymph drains into the thoracic duct and right lymphatic duct before returning to the blood circulation.
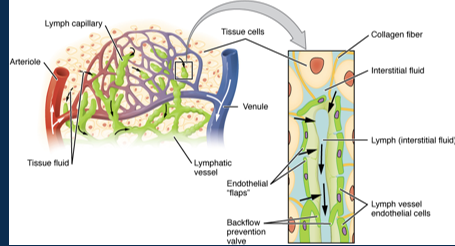
Label the lympathic system on the body
•Lymphatic system drains excess interstitial fluid, transports dietary lipids/ fat-soluble vitamins, and facilitates immune responses
•Lymph vessels have permeable walls and valves.
•Lymph drains into the thoracic duct and right lymphatic duct before returning to the blood circulation. Relies on skeletal muscle and respiratory pumps.
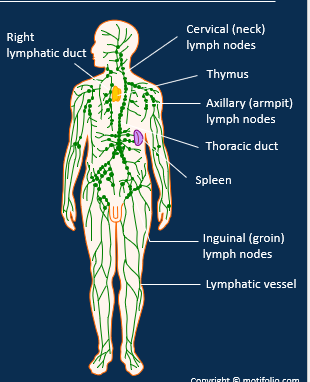
Where does the lymph drain out to?
Thoracic duct
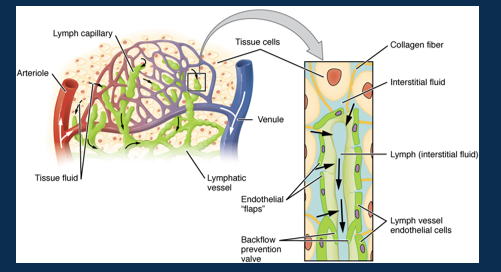
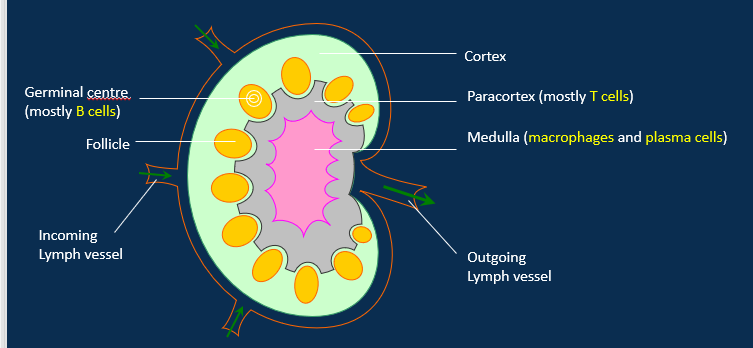
Label the structure of the kidney and it’s lymph vessels
Describe the spleen
•Rich blood supply and filters blood through white and red pulp.
•White pulp of T and B lymphocytes and macrophages perform immune clearance of pathogens.
•Red pulp maintains red blood cell health.
- macrophages remove old erythrocytes
- stores iron
- stores platelets
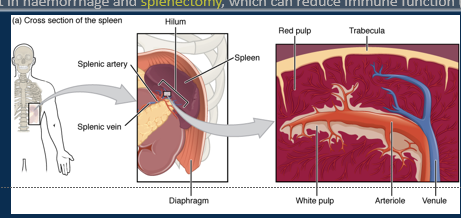
What happens if the spleen goes under trama?
•Trauma can result in haemorrhage and splenectomy, which can reduce immune function (may require prophylactic antibiotics).
What are the two types of immune defences?
Innate defences
Adaptive immunity
Describe innate defences
1st line= Physical barriers created by skin and mucus membranes
2nd line= antimicrobials, natural killer cells, phagocytes, fever, inflammation.
Describe adaptive immunity
T lymphocytes= cell-mediated response by cytotoxic/ memory T cells, helper T cells, and suppressor T cells.
B lymphocytes= antibody-mediated response by Plasma and Memory B cells.
Describe the 1st line of innate adaptation around the body
Eyes= tears from glands in the eyelids wash away dirt + have antiseptic substance
Mouth= glands produce saliva, a mixture of mucus and enzymes that cleans the mouth
Respiratory tract= mucus traps pathogens and cilia sweep mucus to the throat
Stomach= hydrochloric acid, kills most organisms
Intestines= goblet cells produce mucus, which protects the lining from digestive chemicals and harmful organisms.
Genital and urinary tract= “Harmless” bacteria within the genital tract and the flushing action of urine in the urinary tract both help prevent the growth of harmful organisms.
Skin= protected by sebum , and sweat. Both of these are mildly antiseptic. Hair provides a protective coat.
Describe the 4 elements of the 2nd line of the innate immune system
Anticrobials= interferons, iron-binding proteins & complement.
Natural killer cells= immunological surveillance, direct attack upon a range of microbes, infected and cancerous cells
Phagocytes= phagocytosis of pathogens. Secrete wastes and display fragments for antigen recognition.
Fever= pyrogens increase temperature set-point. Increase metabolism, immune function and makes inhospitable environment for pathogens.
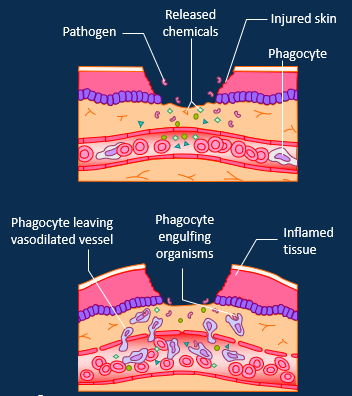
Describe inflammation as a 2nd line innate immune system step
Inflammation is a protective response but causes local tissue swelling, erythema, heat and pain.
1. Vasodilation and capillary permeability.
Mast cells release histamine and heparin.
2. Migration of phagocytes.
Neutrophils engulf pathogens and secrete cytokines which attract monocytes (transform into macrophages) by chemotaxis. Fibrin network prevent spread of microbes.
3. Tissue regeneration.
Healing and fibroblasts secrete collagen to form a scar.
C-Reactive Protein (CRP) is a non-specific biochemical maker of inflammation.
Inflammatory process stimulates the adaptive immune system.
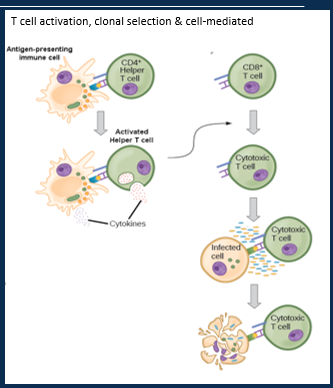
Describe T lymphocytes (cell-mediated) role in the adaptive immune system
Three types of T cell:
1.- Cytotoxic T cell/ Memory T cell (CD8+)
2.- Helper T cell (CD4+)
3.- Suppressor T cell
T cells detect antigens presented by MHCs at the cell surface.
Activated by antigen recognition and co-stimulation by Helper T cells.
T cells undergo clonal selection to produce Cytotoxic T cells and Memory T cells.
Cytotoxic T cells attack pathogens using perforin, granzymes, lymphotoxin and stimulating apoptosis.
Memory cells enable a much quicker secondary response on exposures to the same antigen, while Suppressor T cells stop the response to protect healthy tissues from damage.
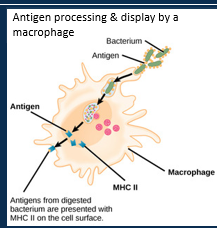
Describe T lymphocytes (cell-mediated) role in the adaptive immune system picture
Describe B lymphocytes (antibody/humoral) role in the adaptive immune system picture
•B cells do a chemical attack on pathogens using antibodies
•They are activated by specific antigen and co-stimulation of T Helper cells
•Undergo clonal selection to produce active plasma cells and memory cells.
•Plasma cells secrete antibodies or immunoglobulins (IgG, IgE, IgD, IgM, IgA).
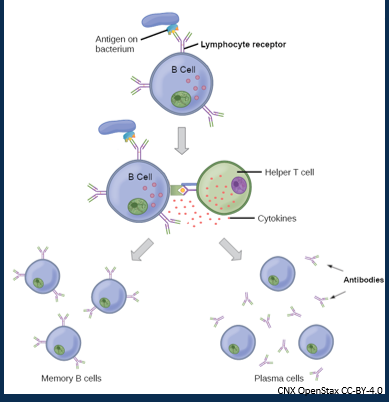
What are the functions of antibodies
1. Neutralise pathogens
2. Agglutination (clumping of pathogens)
3. Activates the complement system
4. Attracts phagocytes
5. Opsonisation (allow phagocytes to attach)
6. Stimulates inflammation
7. Prevents pathogen adhesion to skin and mucus membranes
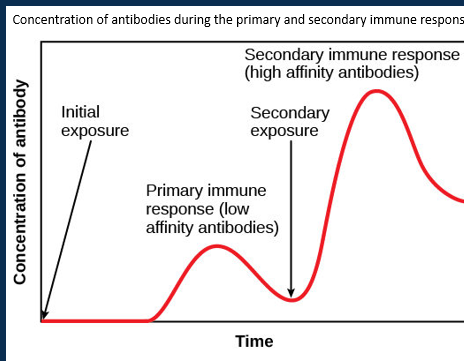
Describe immunological memory
•Development of memory T and B cells during a primary immune response allow a much faster and more powerful secondary immune response on exposure to the same antigen.
•This avoids disease by creating naturally-acquired active immunity.
•Vaccines use this principle, and provide artificially-acquired active immunity.
•Passive immunity through the transfer of antibodies can be naturally- (placenta/ breastfeeding) or passively- (clinical therapy) acquired.
What does non-pathogenic mean
They dont cause disease and can be beneficial
Label bacterial structure
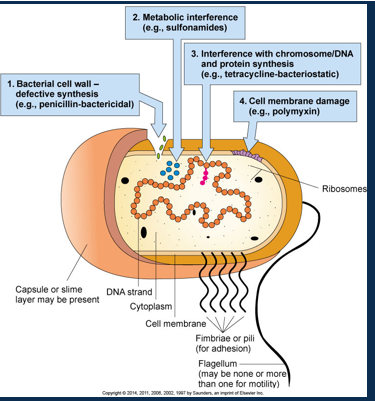
What are multi-resistant infectios
Happens when micro-organisms change when they are exposed to antimicrobial drugs. Micro-organisms that develop this are referred to as ‘superbugs’.
•The ability to prevent and treat a range of infections is threatened.
•Antimicrobial resistance can occur naturally over time but its known that the overuse or misuse of antibiotics can accelerate the process.
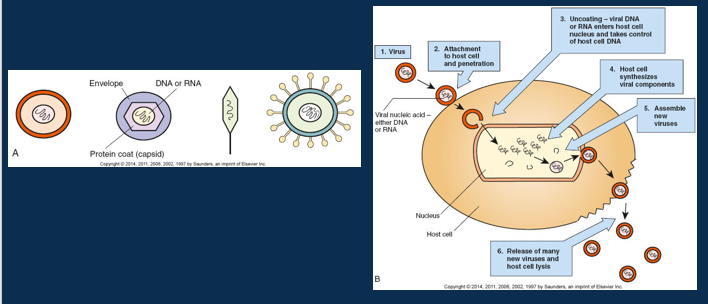
Describe viral structure and replication
What is immunosuppression
a reduction in the efficiency of the body’s immune system, resulting in a weakened ability to fight infections and diseases.
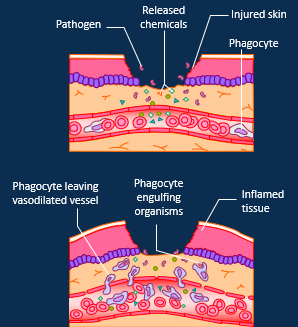
Describe how a local inflammation is dealt with
Pathogenic antigens/ cell damage detected
Mast cells release histamine and heparin, causing vasodilation and increased vessel permeability
Clotting factors and complement proteins migrate into interstitial space. Phagocytosis and release of cytokines. Fibrin network forms to trap microbes.
Monocytes attracted to the area – transform into phagocytic macrophages and release proinflammatory cytokines (e.g. IL-1, IL-6 and TNF). Recruitment of lymphocytes
Fibroblasts secrete collagen to form a supportive scar as tissue heals and remodels.
Describe sepsis
“Sepsis is a dysregulated response to infection”
Improvement in outcomes relies on early identification and treatment.
Complex syndrome of pathophysiological pathways which can present with a range of non-specific symptoms, making diagnosis challenging.
Usually happens of patients that are already sick
What are the risk factors of sepsis
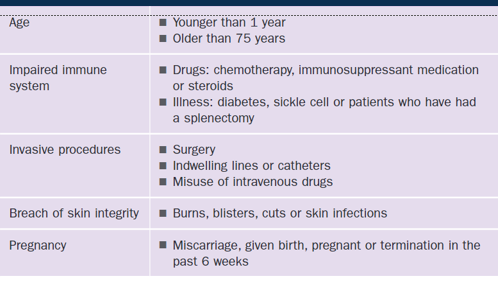
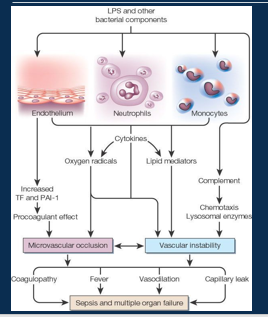
Pathophysiology of sepsis
•Sustained inflammatory signals/ bacterial challenge can lead to systemic (rather than localised) inflammation
•Activated white blood cells and build up of cytokines damage blood vessel endothelium.
•Damaged endothelium releases nitric oxide (NO) which causes further vasodilation and permeability, as well as more cytokines, complement and activated clotting.
•Procoagulant states (called disseminated intravascular coagulation - DIC) can result in microemboli and further tissue ischemia.
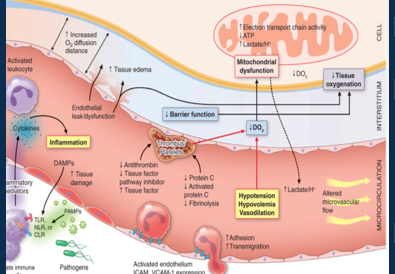
What is a septic shock
sepsis causes dangerously low blood pressure and cellular abnormalities
Hypotension results in hypoperfusion of tissues and build-up of wastes.
Cells are starved of oxygen/ glucose and resort to anaerobic respiration, generating lactate. Results in lactic (metabolic) acidosis.
Cell function is affected and intracellular salts accumulate. Fluid shifts from intravascular to interstitial and then intercellular space
Damaged cells leak enzymes which injuries other neighbouring cells.
•Viscous cycle of cell dysfunction leads to multi-organ failure.
•Diagnosed when: serum lactate >2mmol/L and vasopressors are required to maintain mean arterial pressure (MAP) ≥65mmHg.
What do you have to do when Sepsis happens
