Case 7: Mary Jane Morrison
1/53
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
54 Terms
Cervix Anatomy
Uterus neck
Sections:
Internal Os: Opening into uterus
Cervical canal
External Os: Opening into vagina
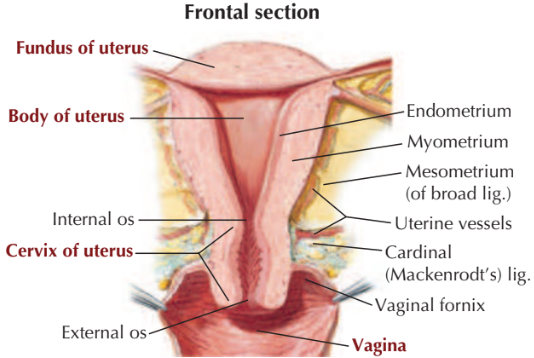
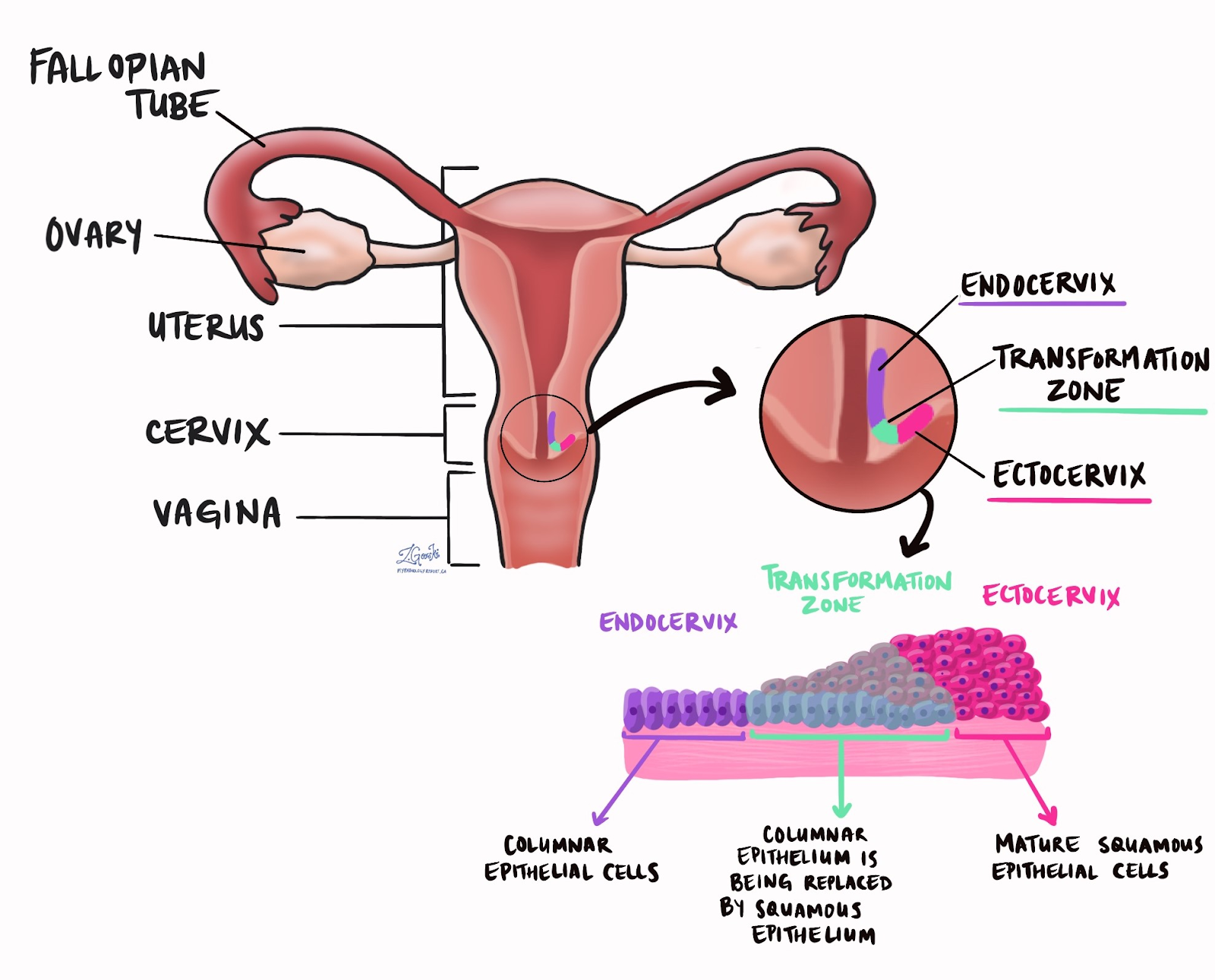
Cervix: Histology
Endocervical Mucosa: Simple columnar epithelium
Inside canal
Exocervical Mucosa: Stratified squamous epithelium
Around external os → Upper vagina (continuous)
Transformation Zone: Squamous-columnar epithelium
Transition between endo and exocervical mucosa
Around external os
Vaginal environment exposure = Reprogram epithelial stem cells = Neoplasia
Chlamydia: Pathogen + Transmission
Chlamydia trachomatis (bacteria)
Transmission:
Sexual contact
Vertical transmission
Chlamydia: Pathophysiology
Bacteria into urogenital tract = Infect endocervical epithelium (female) or urethral epithelium (male)
Chlamydia: Clinical Presentation
Asymptomatic: Most women
Symptomatic:
Urethritis (dysuria, polyuria)
Proctitis (rectal inflammation)
Female:
Vaginal discharge
Postcoital/intermenstrual bleeding
Dyspareunia
PID
Male:
Urethral discharge
Epididymitis
Prostatitis
Chlamydia: Treatment
Antibiotics
Axithromycin (1g x 1 dose)
Doxycycline
Levofloxacin
Abstinence
7 days after treatment
Chlamydia: Prevention
Safe sex (barrier contraception)
Screening:
Sexually active women: Annual for ≥ 25 years + STI risk factors
Prenatal: STI risk factors
Gonorrhea: Pathogen + Transmission
Neisseria gonorrhoeae (bacteria)
Transmission:
Sexual contact
Perinatal (before and after birth)
Gonorrhea: Pathophysiology
Bacteria invade epithelium cells = Inflammation + phagocyte recruitment = Tumor necrosis factor from phagocytes damage epithelial cells = Deeper infection
Gonorrhea: Clinical Presentation
Urethritis
Discharge
Dysuria
Increase urinary frequency
Cervicitis
Asymptomatic
Discharge
Pain
PID
Discharge
Fever
Pain
Fitz-Hugh-Curtis syndrome (RUQ from hepatitis)
Epididymitis
Orchitis
Swollen/tender testicles
Gonorrhea: Treatment
Antibiotics
Ceftriazone
Complicated: + doxycycline and metronidazole
Treat partners
Abstinence
7 days after treatment
Symptoms resolved
Gonorrhea: Prevention
Barrier contraception
Antibiotic prophylaxis (sexual assault)
Screening:
Sexually active women: Annual for ≥ 25 years + STI risk factors
Prenatal: STI risk factors
HPV: Pathogen + Transmission
Human papillomavirus
Transmission:
Sexual contact
Fomites
Vertical transmission (rare)
HPV: Pathophysiology
HPV express oncoproteins E6 and E7 = Epidermal hyperplasia + hyperkeratosis = Warts
HPV: Clinical Presentation
Warts
Anogenital
Cutaneous
HPV: Treatment
NO CURE
Spontaneously resolve in < 2 years
Wart removal
HPV: Prevention
Barrier contraception
HPV vaccine (gardasil) → 11-12 years
Circumcision
Screening:
> 25 years = Every 5 years
Syphilis: Pathogen + Transmission
Treponema pallidum (bacteria)
Transmission:
Sexual contact (mucocutaneous lesions)
Vertical transmission
Blood transfusion + organ donation (rare)
Syphilis: Pathophysiology
Bacteria bind endothelial cells = Inflammatory reaction = Endarteritis (artery intima proliferation + inflammation)
Syphilis: Clinical Presentation
Localized primary lesions (chancre)
Lymphadenopathy
Syphilis: Treatment
Penicillin G (first-line)
Allergy:
Allergen desensitization + penicillin
Doxycycline
Ceftriaxone
Syphilis: Prevention
Barrier contraception
Doxycyline PEP
Circumcision
Screening: Annual
HIV infection
MSM
Pregnancy
HBV: Pathogen + Transmission
Hep B virus (HBV)
Transmission:
Sexual contact (mucocutaneous lesions)
Parenteral (needles, blood transfusion, organ transplant)
Vertical transmission
HBV: Pathophysiology
Virus invade hepatocytes = Produce viral DNA = CD8+ T cells attack infected hepatocytes = Liver inflammation + destruction
HBV: Clinical Presentation
Fever
Fatigue
Myalgia
Nausea
Jaundice
RUQ pain
HBV: Treatment
Supportive care
Avoid hepatotoxic meds
Stop alcohol
AVT: Chronic infection
HBV: Prevention
HBV vaccine
At birth OR childhood
Circumcision
Screening:
18+: 1 time
Pregnant: 1 time
Tissue/blood donors
HCV: Pathogen + Transmission
Hep C virus (HCV)
Transmission:
Parenteral
Vertical transmission
Sexual contact (rare)
HCV: Pathophysiology
Virus invade hepatocytes = Produce viral RNA = Host immune response cause liver inflammation + destruction
HCV: Clinical Presentation
Asymptomatic
Symptomatic:
Fever
Malaise
Myalgia
RUQ pain
Nausea/vomiting
Jaundice
HCV: Treatment
AVT: All patients
Supportive care
Avoid hepatotoxic drugs
Stop alcohol
HCV: Prevention
NO VACCINE OR PREP
Education
PPE
Needle sharing
Screening:
18+: 1 time
Pregnancy: 1 time
STI Testing/Screening Methods
Nucleic acid amplification testing (NAAT): PCR
Vaginal swab (pap smear) or urine
Serology
BBI (HBV, HCV, HIV, syphilis)
STI Test of Cure
F/U diagnostic test to determine if STI (chlamydia, gonorrhea) cleared from treatment
Failure Reasons:
Poor compliance
Reinfection from untreated partner
Antibiotic resistance
STI Complications
PID
Fitz-Hugh-Curtis syndrome
Sepsis
Infertility
Ectopic pregnancy
Cervical cancer (HPV)
STI Complications: PID
Ascending bacterial infection infecting structures above cervix
Endometrium
Fallopian tubes
Ovaries
Peritoneum
PID Management
Empiric antibiotics
Parenteral: Cephalosporin + doxycycline
Oral: Switch after 24-48 h improvement
Partner treatment
Test + treat chlamydia and gonorrhea
STI screening
Education
Stop intercourse until treatment complete
Barrier contraception
PID Complication
Infertility
Increased from…
Chronic chlamydia
Failure to treat
Severe inflammation → Fallopian tube scarring
Multiple infections
STI Complications: Fitz-Hugh-Curtis Syndrome
Perihepatitis: Liver capsule inflammation → RUQ + right shoulder pain
STI Prevention
Primary: Decrease risk factors
Behavioural counselling
PrEP
Vaccines
AVT
Secondary: Early detection
Screening
Pap: ≥ 25 years + sexually active → Every 3 years
PEP
Antibiotics
ARVT
STI Reporting
Chlamydia
Gonorrhea
Syphilis
HBV
HCV
HIV/AIDS
Infectious Vulvovaginitis
Yeast infection (vulvovaginal candidiasis)
Bacterial vaginosis (BV)
Trichomoniasis
Yeast Infection: Pathogen
Candida albicans (fungus)
Yeast Infection: Pathophysiology
Fungal overgrowth
Risk factors:
Pregnancy
Immune deficiency
Antimicrobials
Yeast Infection: Clinical Presentation
Vaginal discharge
White
Crumbly
Sticky
Vulvovaginal erythema
Vaginal burning + pruritis
Dysuria
Dyspareunia
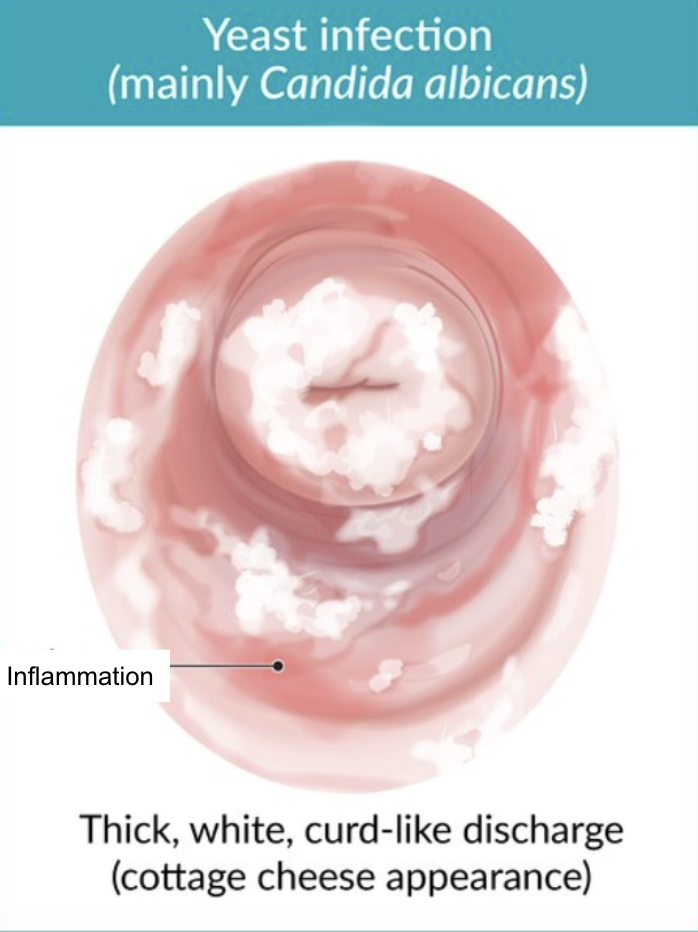
Yeast Infection: Treatment
Antifungals
Topical azole
BV: Pathogen
Gardnerella vaginalis
Atopobium vaginae
Prevotella spp.
Mobiluncus spp.
BV: Pathophysiology
Low bactobacillus in vagina = Pathogenic bacteria overgrowth
NO inflammation
Risk factors:
Sexual intercourse
IUD
Vaginal douching
Pregnancy
BV: Clinical Presentation
Asymptomatic
Vaginal discharge
Grey
Milky
Fishy odour

BV: Treatment
Antibiotics: For symptoms
Oral/intravaginal metronidazole
Intravaginal clindamycin
Trichomoniasis: Pathogen
Trichomonas vaginalis (parasite)
Sexual contact transmission
Trichomoniasis: Pathophysiology
Parasite attach to genital epithelium (cytotoxic) = Epithelial cell lysis
Trichomoniasis: Clinical Presentation
Vaginal discharge
Yellow-green
Purulent
Frothy
Foul-smelling
Vulvovaginal pruritis
Vaginal burning
Dyspareunia
Dysuria
Strawberry cervix (erythema + petechiae)
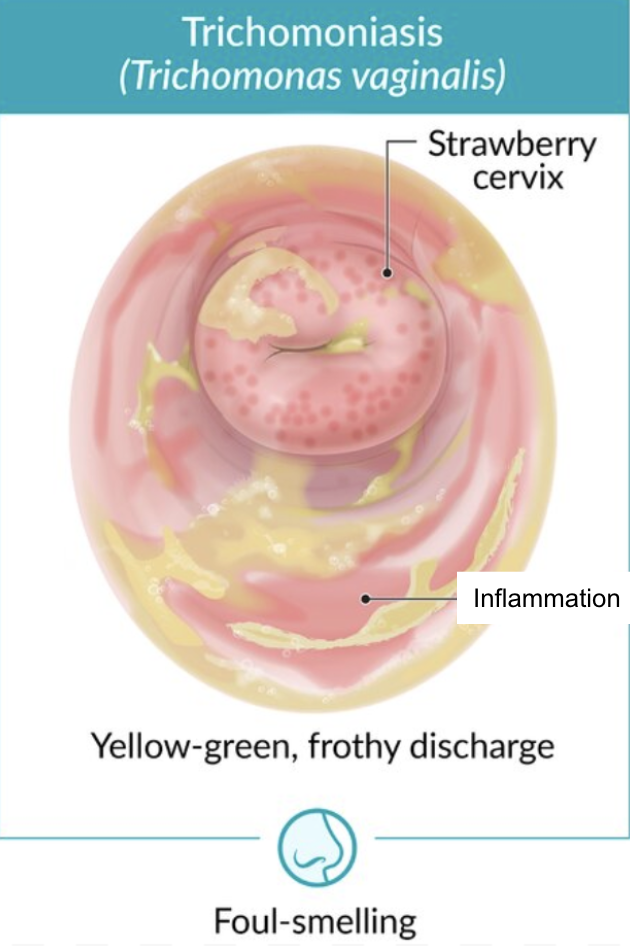
Trichomoniasis: Treatment
Antimicrobial
Oral metronidazole
Oral tinidazole
Treat partners