DISORDERS OF GROWTH
1/55
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
56 Terms
what are the major types of disorders of growth
too much
too little
wrong type
wrong place
what are the reasons for disorders of growth
developmental/ congential
between life and death
congenital: pre natal period
reactive/ adaptation e.g. to offer more protection
short term response
diagram showing cell proliferation and differentiation
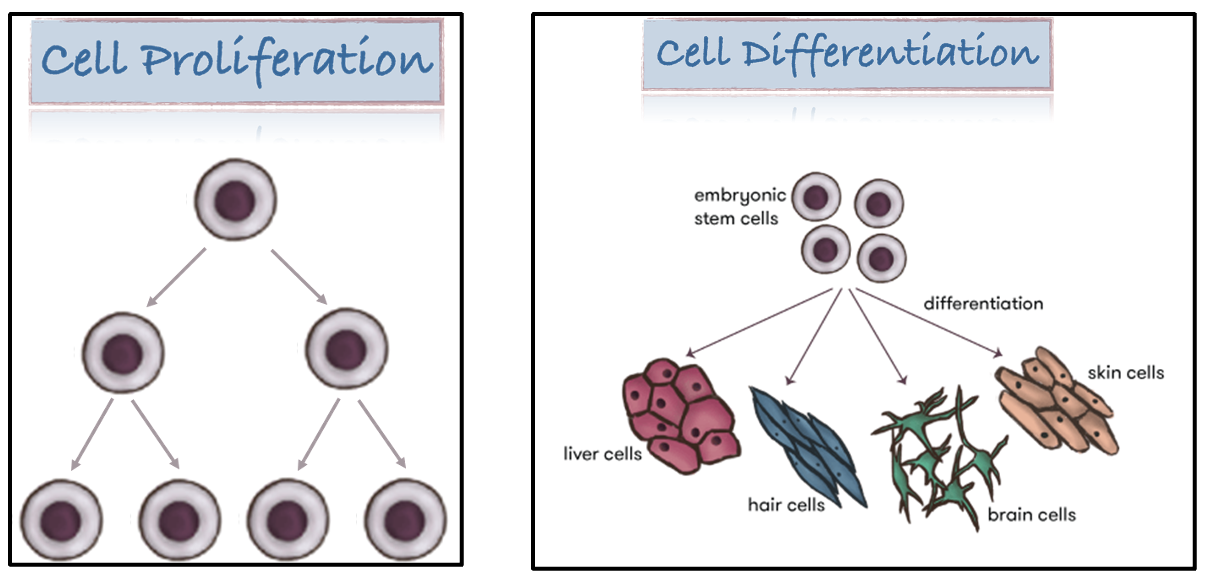
how do disorders of growth arise
stress » adaptation » disorders of growth
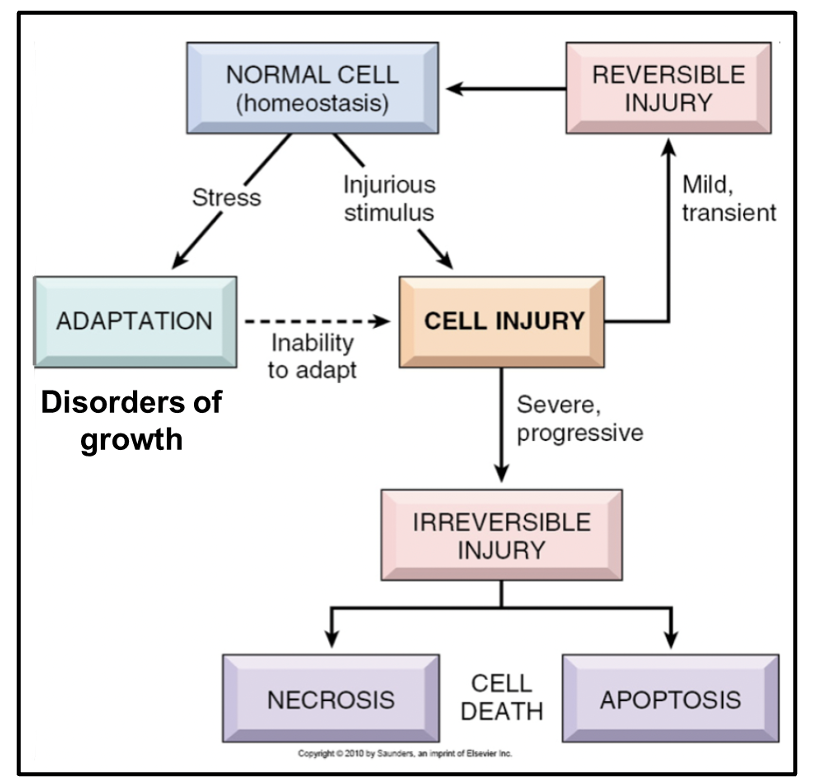
give examples of disorders of growth
stress (chronic trauma) on oral epithelial mucosal cells » increase in cell number
stress (more effort) on skeletal muscle cells » increase in size e.g. going to the gym
what does the prefix hyper mean
hyper = increased
what does the prefix hypo mean
hypo = decreased
what does the suffix trophos mean
trophos = nutrition/ metabolism (increase/ decrease cell size)
what does the suffix plasis mean
plasis = growth (cell number)
what does the prefix meta mean
meta = changed (different cell type)
what does the prefix dys mean
dys = bad
what does the prefix neo mean
neo = new
give an example of a type of developmental/ congenital disorder of growth
hamartoma: benign growths in specific tissues
tissues are normal for the site but they are excessive
grows in patient’s growth period then stops growing
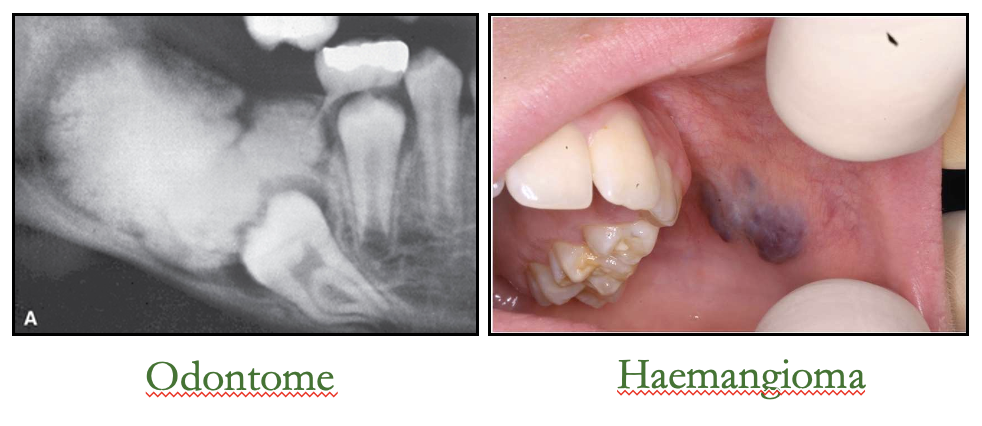
what are examples of hamartomas
congenital pigmented naevi - excessive melanin production
haemangioma - excessive vascularisation
odontomes
histology of odontome
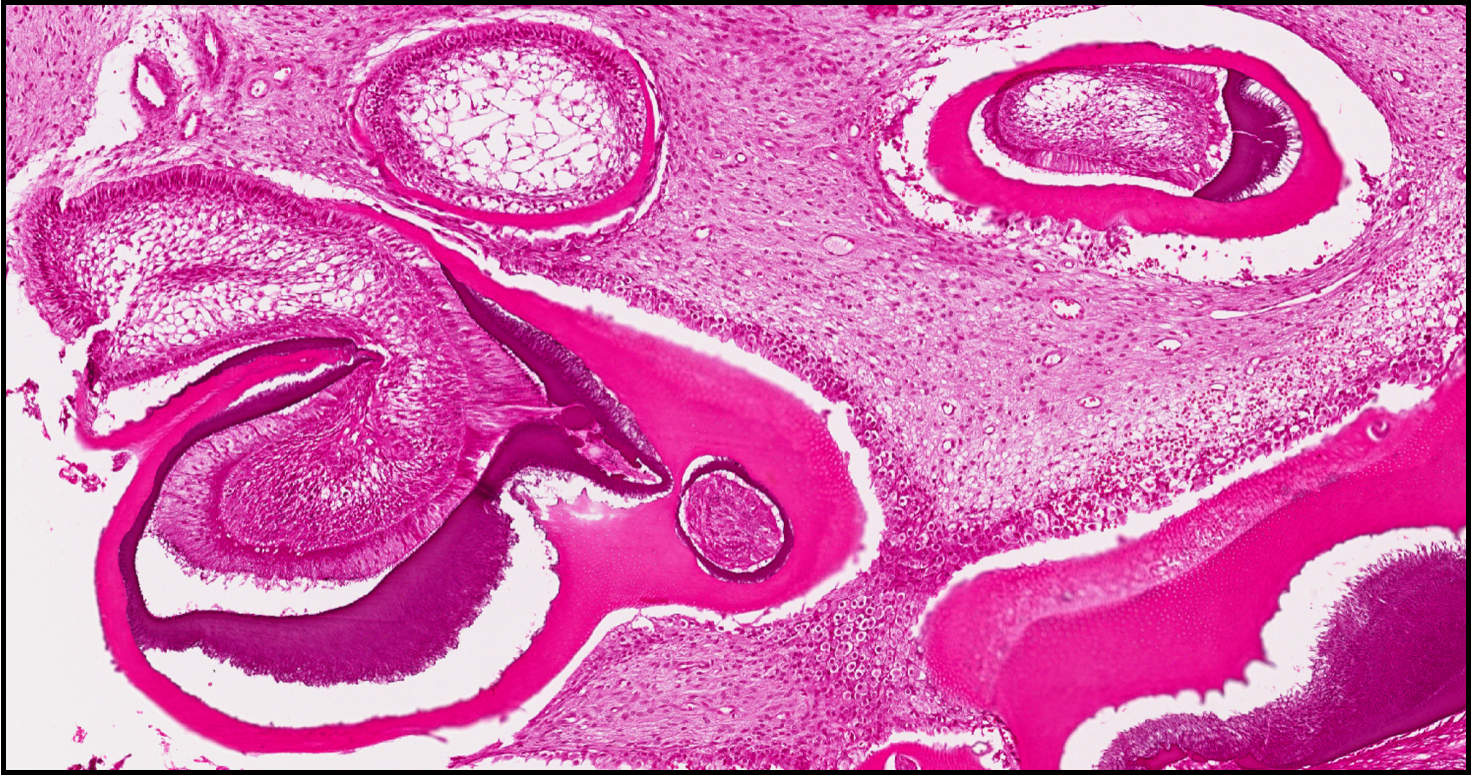
give examples of types of reactive/ adaptive disorders of growth
hyperplasia - increase in cell number
hypertrophy - increase in cell size
outline hyperplasia
hyperplasia: increase in cell number
in response to a stimulus
can be physiological or pathological
stops once stimulus is removed
give an example of a physiological VS pathological hyperplasia
physiological: breast enlargement during puberty
pathological: thyroid enlargement
give an oral example of pathological hyperplasia
denture-induced hyperplasia (Epulis fissuratum)
usually related to ill-fitting complete denture
benign lump: smooth pink surface lying parallel with the alveolar ridge
what is the management for Epulis fissuratum
relieve the denture flange and wait for regression
if it does not regress within 2-3 weeks the lump should be excised
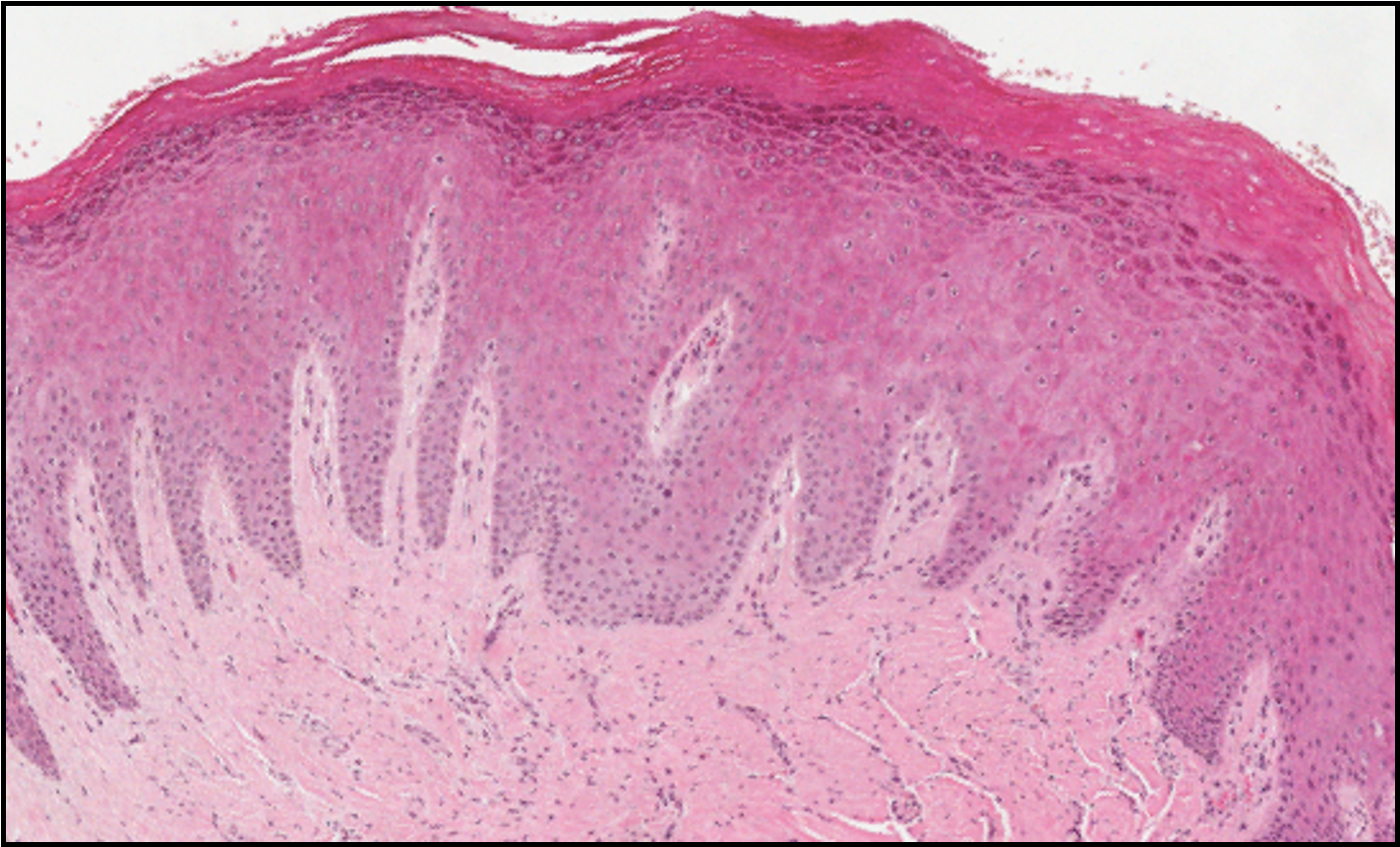
describe this histological image
LHS = normal epithelium
RHS = hyperplasia
thicker granular layer because producing more keratohyaline granules »
more keratin at surface
connective tissue is slightly pinker due to overproduction of collagen
outline hypertrophy
hypertrophy: increase in cell size
often associated with hyperplasia
in response to a stimulus
can be physiological (increase in skeletal muscle size when going to the gym) or pathological
what is pure hypertrophy
increase in the size of skeletal and cardiac muscle
give examples of physiological hypertrophy
there is physiological hypertrophy of the uterus during pregnancy
left ventricular hypertrophy also occurs
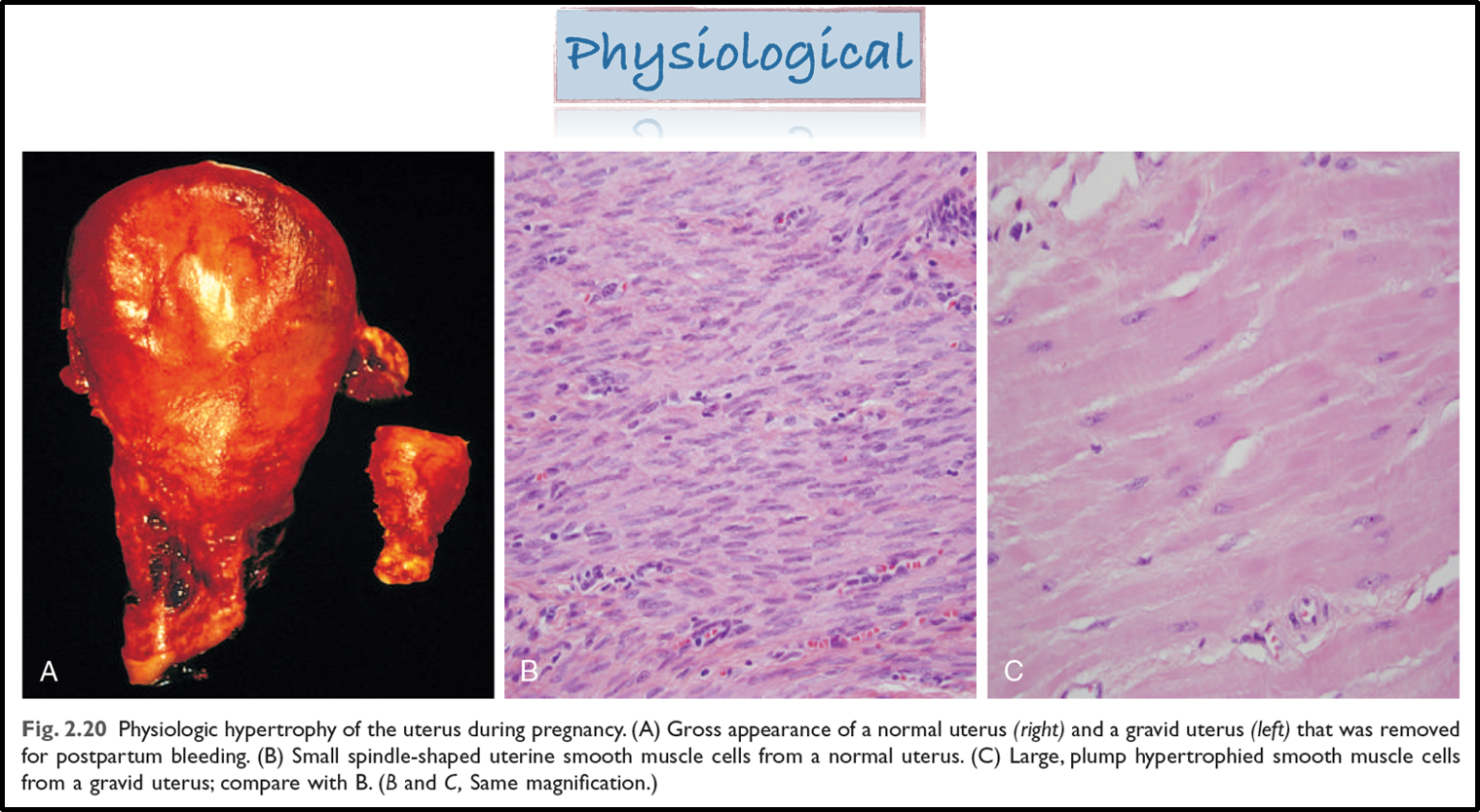
give an example of pathological hypertrophy
hypertension - also left ventricular hypertrophy
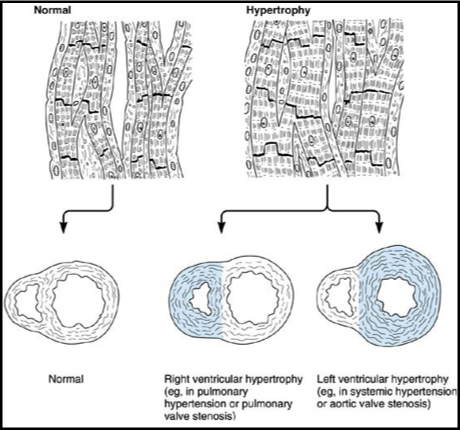
diagram showing why left ventricular hypertrophy may occur
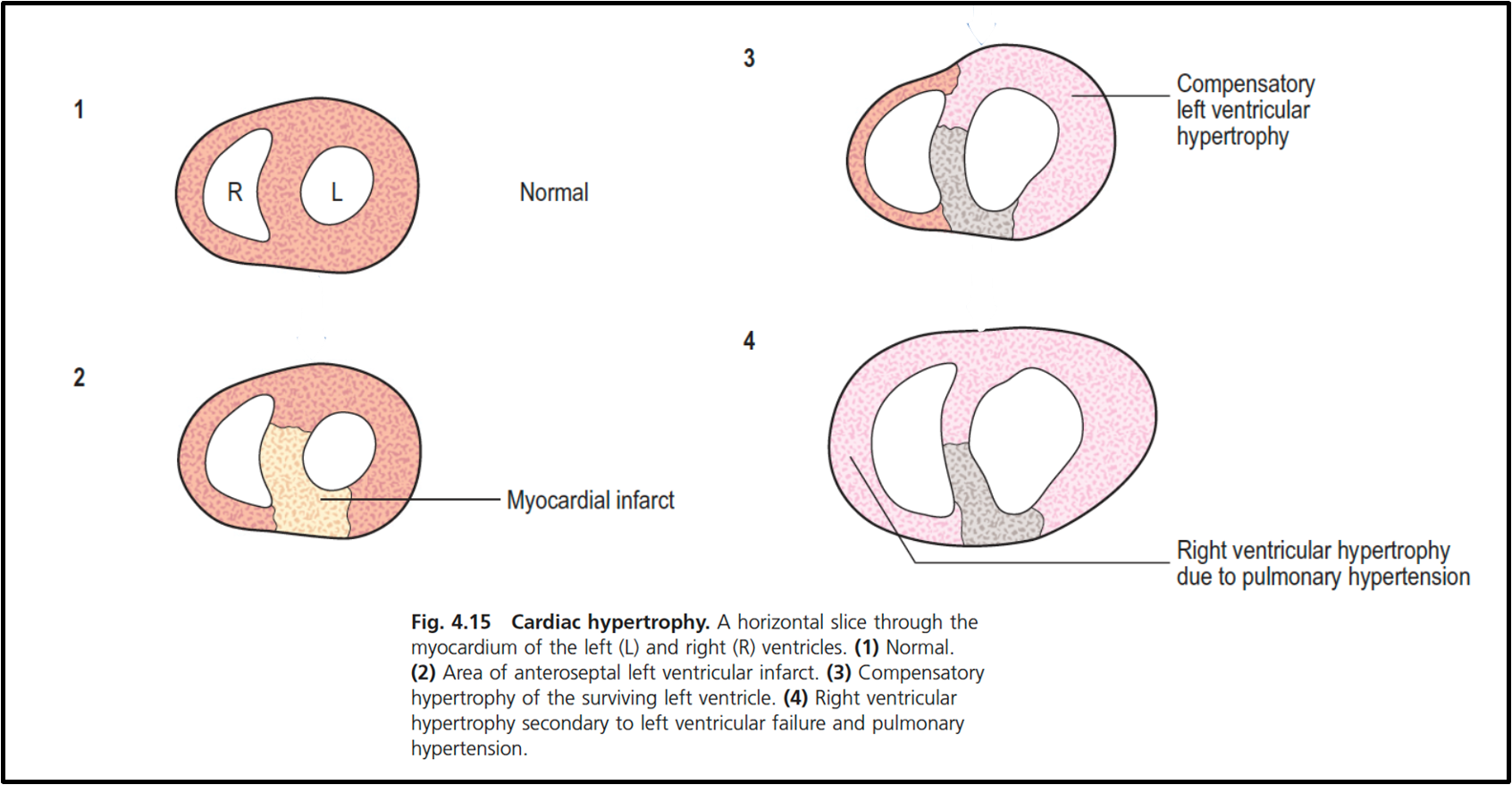
hypertrophy and hyperplasia diagram
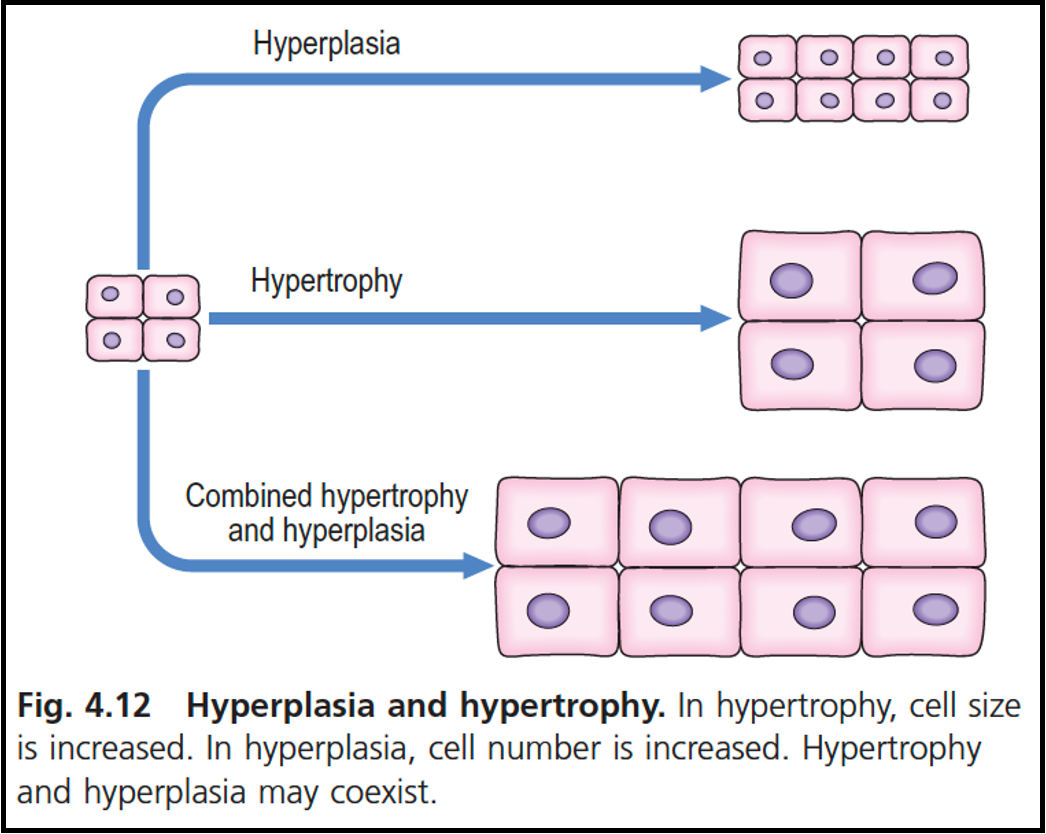
give another example of compensatory physiological hyperplasia/ hypertrophy
compensatory physiological hyperplasia/ hypertrophy is a type of regenerative growth
usually occurs after organ damage, removal or malfunction
growth can be a result of increased cell size (compensatory hypertrophy) or increased cell division (compensatory hyperplasia)
or both
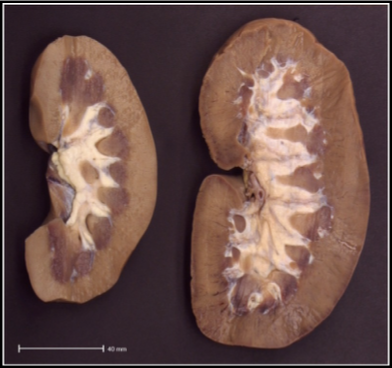
what does this image show
LHS: pig born with both kidneys
RHS: pig born with one kidney
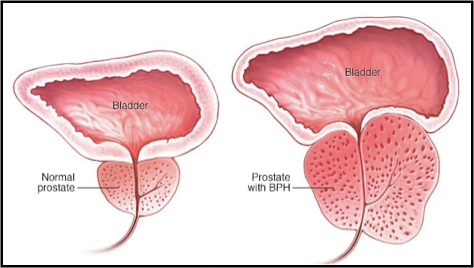
give another example of pathological hyperplasia
benign prostatic hyperplasia (BPH)/ prostate gland enlargement
common condition in older men
as the gland enlarges it can squeeze the urethra
state congenital changes of too little growth
agenesis: does not develop at all
aplasia: fails to develop normal structure
hypoplasia: less tissue is formed
outline tooth agenesis
tooth agenesis: congenital absence of one or more teeth
8s > 5s > 2s
hypodontia - agenesis of one to six teeth (excluding 8s)
oligodontia - absence of more than 6 teeth (excluding 8s)
anodontia - complete absence of teeth
outline aplasia (achrondroplasia)
achondroplasia i.e. dwarfism
random event, but the gene change can also be inherited
defect in converting cartilage into bone
most common type of restricted growth
normally occurs in limbs, hence stunted growth
outline dental enamel hypoplasia
dental enamel hypoplasia
enamel is deficient in quantity
affected region = area of ameloblastic activity at the time of injury
areas of coronal discolouration or actual pits and irregularities
increased risk of caries
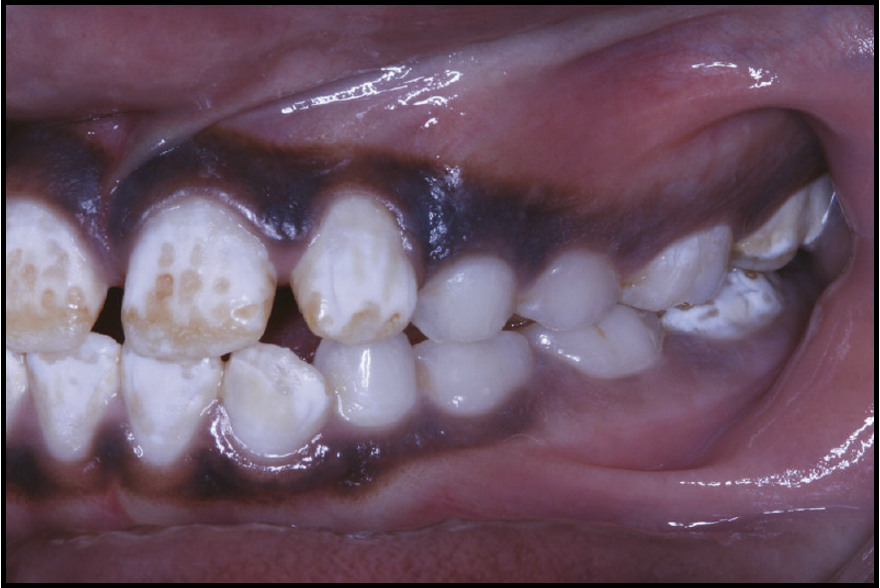
what are causes of dental enamel hypoplasia
nutritional deficiency
prematurity
allergic diseases
trauma
state another term for developmental/ pathological changes of too little growth
atrophy: decrease in cell size and/ or number
outline atrophy
mechanisms:
imbalance of cell loss and production
reduced proliferation
increased cell loss (apoptosis > necrosis)
reduction in structural components of the cell i.e. cell volume
generalised VS localised
outline generalised atrophy
nutritional e.g. in starvation
age related (senile)
endocrine: release of hormones into the blood produces a dysregulated signalling pathway » systemic atrophy
bone: osteoporosis (linked with endocrine dysregulation)
outline localised atrophy
ischaemia: lack of blood supply can lead to localised atrophy and cell death
pressure » localised atrophy
disuse » localised atrophy
neuropathic changes » localised atrophy
immune mediated: e.g. atrophic gastritis (own immune system attacks stomach lining)
idiopathic: unclear cause » localised atrophy
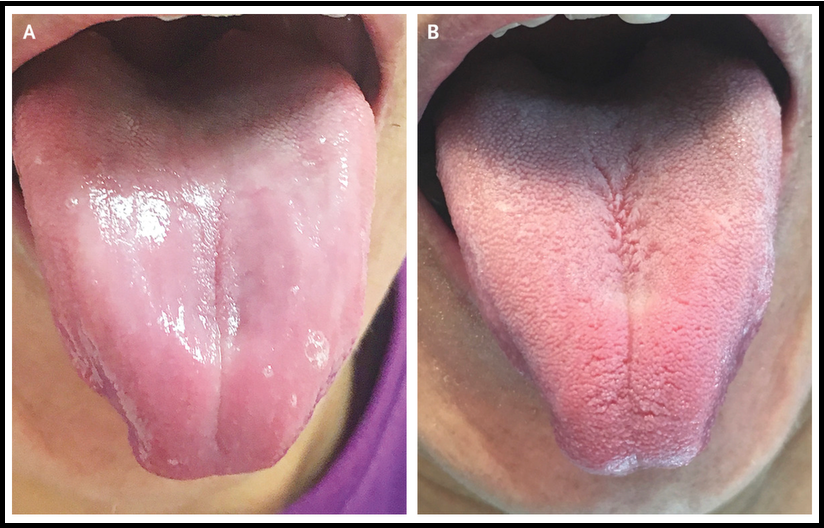
outline atrophic glossitis
partial or complete absence of filiform papillae on the dorsal surface of tongue
diabetes is a comorbidity of atrophic glossitis
list causes of atrophic glossitis
deficiencies of major nutrients incl.
riboflavin, niacin, pyridoxine, vitamin B12, folic acid, iron, zinc, vitamin E
protein-calorie malnutrition
can be due to infiltration of various fungi e.g. Helicobacter pylori
candidiasis
xerostomia
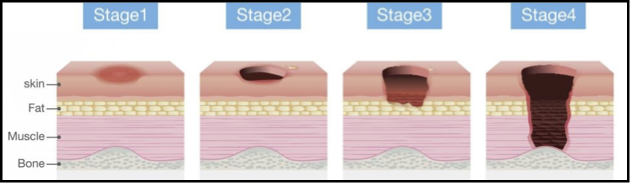
outline pressure as a cause of localised atrophy
most commonly from being bed ridden » bed sores (huge issue for NHS)
pressure points » ulceration
pressure stops the delivery of nutrients into that area of tissue
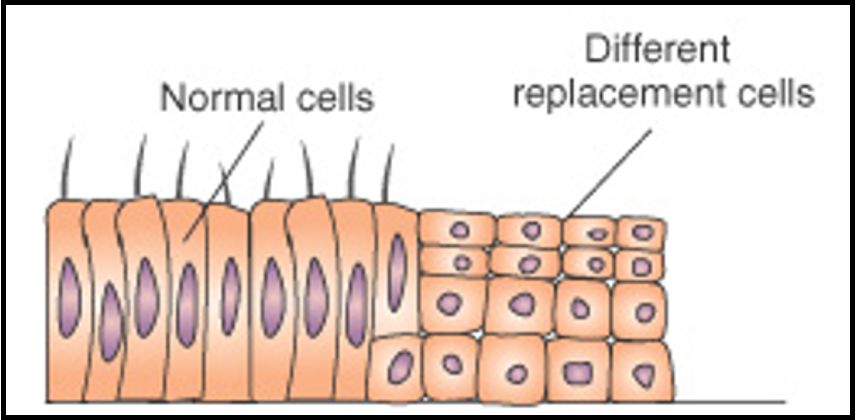
outline metaplasia
metaplasia change in which one adult cell type (epithelial or mesenchymal) is replaced by another adult cell type (wrong type)
this is an adaptive response
sensitive cell type is replaced by another cell type better suited to withstand the adverse environment
however it often results in the loss of the original tissue’s specialised function
can be a precursor to dysplasia and cancer
what is the most common type of metaplasia
epithelial metaplasia
table showing types of metaplasia
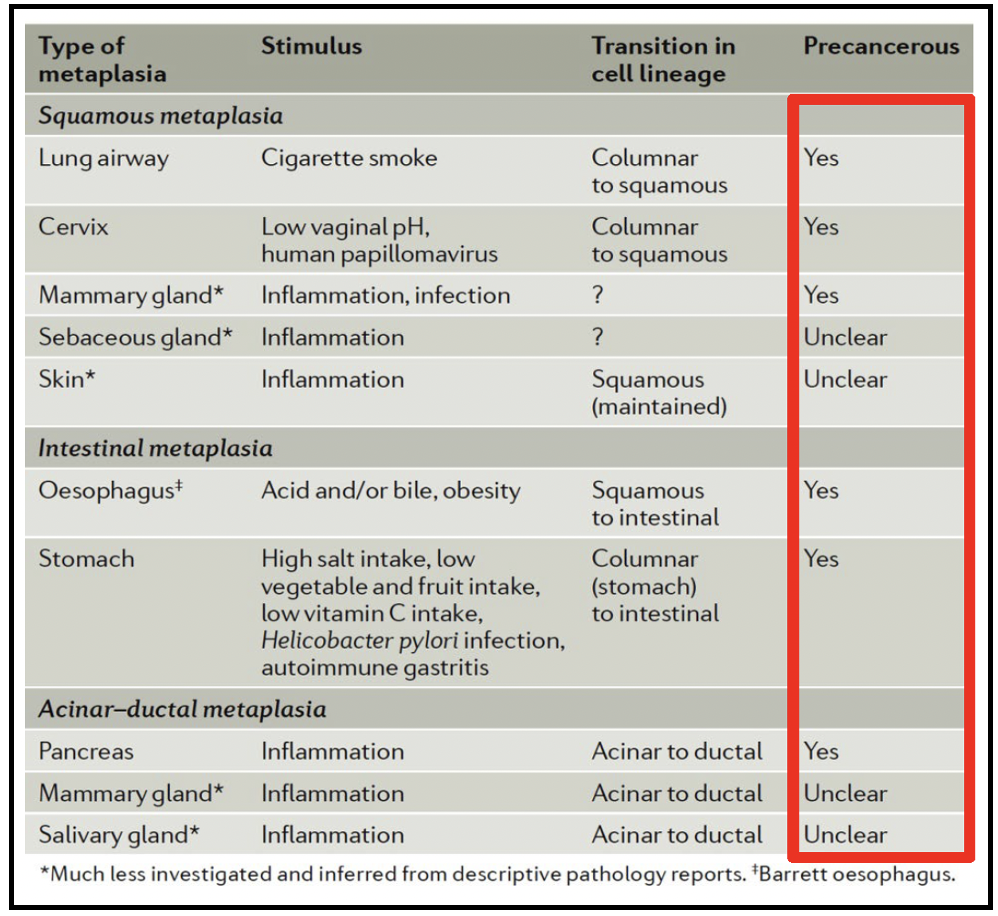
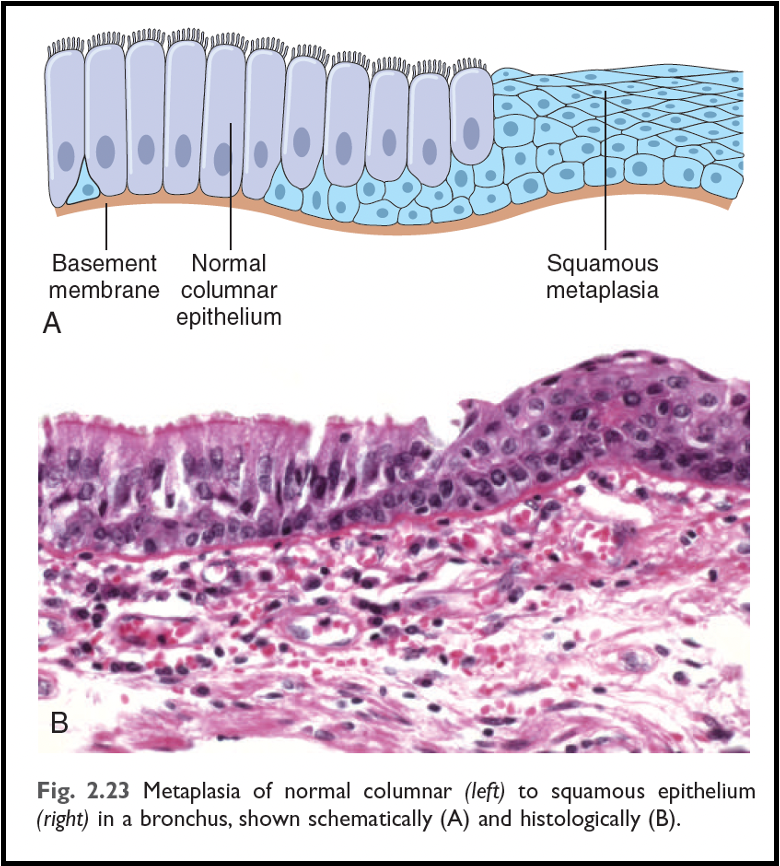
outline squamous metaplasia
occurs in smokers
normal ciliated columnar epithelial cells of the trachea and bronchi is replaced by stratified squamous epithelial cells
SSE is more resistant to noxious chemicals in cigarette smoke and vapes
important protective mechanisms like mucous secretion and ciliary clearance are lost
squamous metaplasia VS epithelial dysplasia diagram
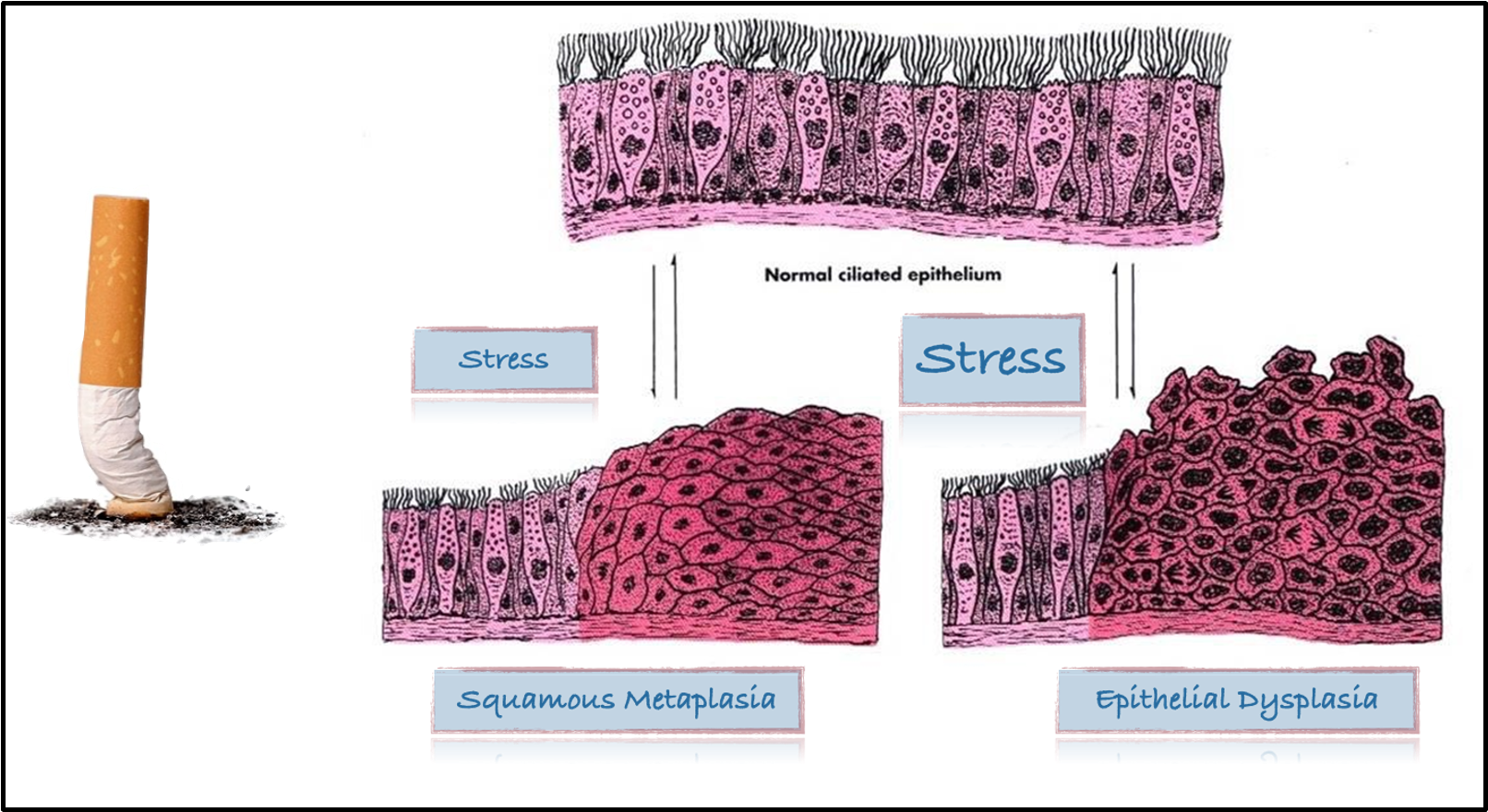
outline intestinal metaplasia
chronic gastric reflux
stomach is producing acid (stressor) which flows into and damages oesophagus
normal SSE of lower oesophagus undergo metaplastic transformation to gastric or intestinal-type columnar epithelia
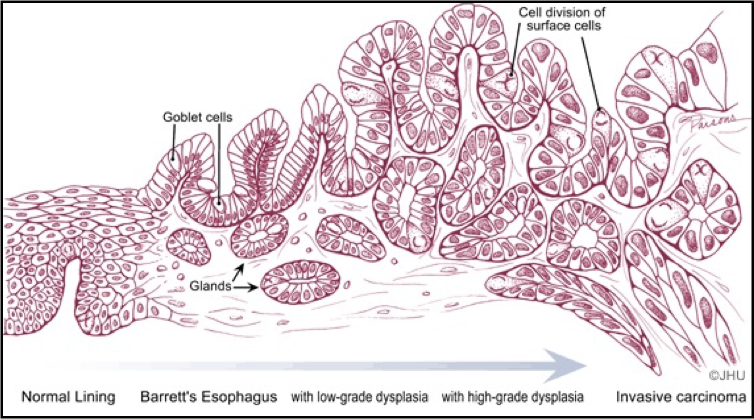
what does intestinal metaplasia lead to
Barrett’s oesophagus
premalignant lesion of oesophageal adenocarcinoma
10% rate of malignant transformation » oesophageal carcinoma
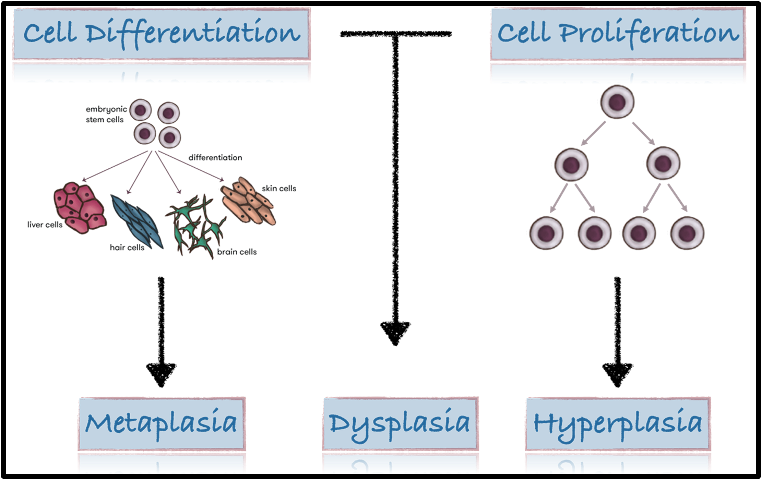
outline (epithelial) dysplasia
epithelial dysplasia: abnormal growth and differentiation in a tissue, with abnormal cells and tissue architecture
has the potential to become a malignant tumour (neoplasia)
‘dysplasia’ also used to name different pathological conditions e.g. renal dysplasia, bone dysplasia
outline neoplasia
neoplasia: uncontrolled growth which does not stop and persists after the stimulus is removed
outline ectopia
ectopia (wrong place)
developmental abnormality
normal tissue
abnormal site
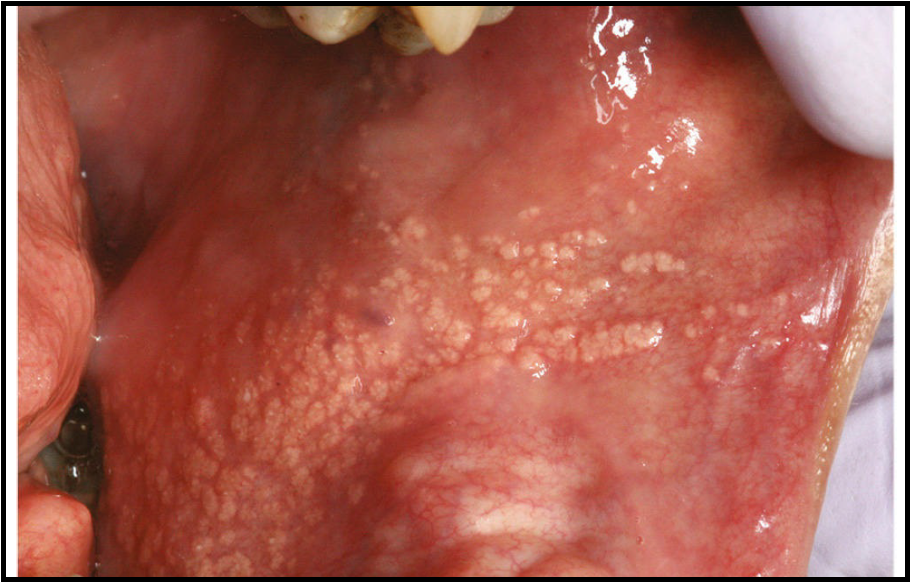
give an example of ectopia in the oral cavity
ectopic sebaceous glands
i.e. Fordyce spots
soft yellowish granules seen in upper lip and buccal mucosa
80% of population
rarely evident in infants
increase during puberty
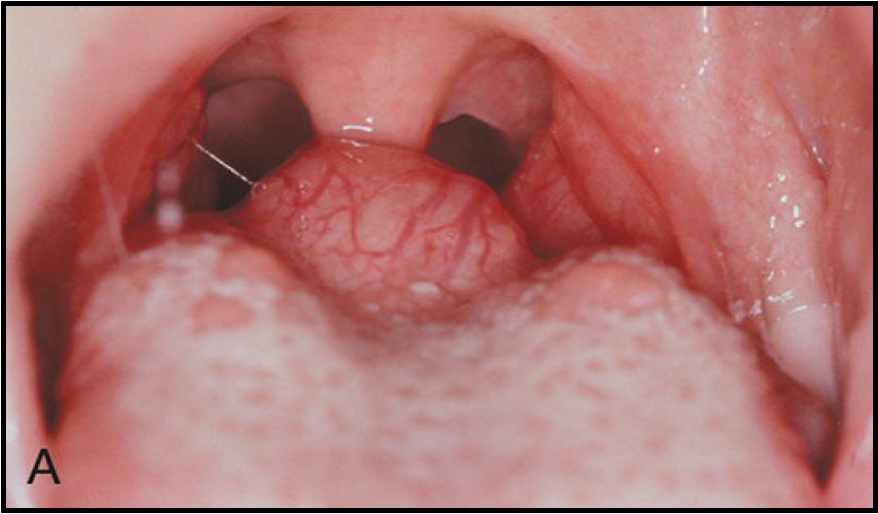
give an example of ectopia elsewhere in the body
ectopic thyroid tissue
e.g. lingual thyroid
lack of descent of thyroid tissue during development - true incidence not known
90% of all ectopic thyroid tissue is associated with dorsum of the tongue
usually not clinically evident
when clinically evident it is largely asymptomatic/ associated with hypothyroidism
what leads to adaptation
stress
how does potential carcinogenesis result from stress
chronic stress » metaplasia » dysplasia » potential carcinogenesis