4- Treating TMJ disorders
1/19
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
20 Terms
How are TMJ disorders categorised in 4 groups? (Treatment depends on which category)
1- alterations of condyle disc complex
displacements and dislocations (with/out reduction)
2- structural incompatibility
morphological alterations
adhesions
subluxation
spontaneous dislocation
4- inflammatory disorders
synovitis/capsulitis
retrodiscitis
arthritis
5- associated structures
temporal tendinitis
stylomandibular ligament
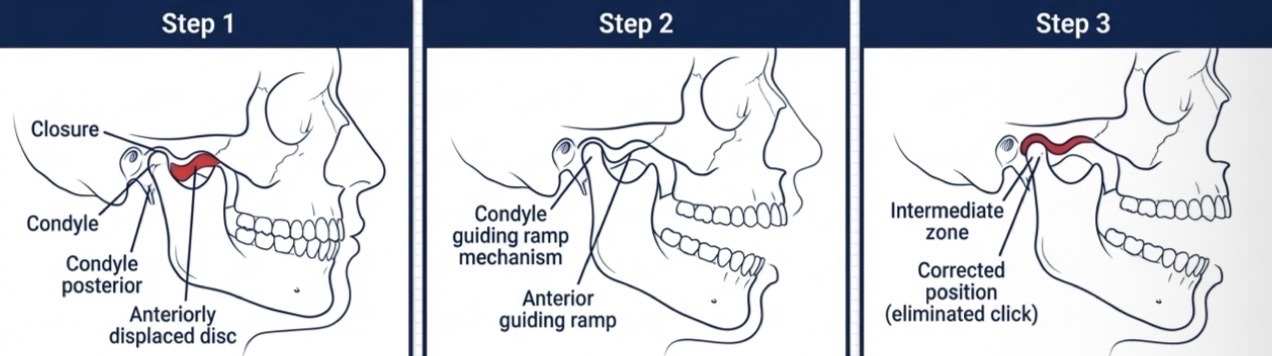
What is disc displacement with reduction- define, etiology, causal factors, diagnosis?
Initial phase of disc alteration- condyle recovers position on disc during opening
Elongation of discal/capsular ligaments and thinning of intermediate zone of disc
Direct or chronic microtrauma (hypoxia-reperfusion, bruxism)
Normal mandibular range of motion, pathological prescience of reciprocal joint noise (click)
How to treat disc displacement?
Re-establish condyle-disc relationship to eliminate painful load
Orthopaedic technique- anterior repositioning device- eliminates click
Mainly use at night to promote tissue adaption without altering occlusion permanently
Therapies- voluntary movement restrictions soft diet and temp analgesia
How can morphological alteration of adhesions cause structural incompatibility?
Morphological changes to smooth surface of disc or bony structures due to trauma or chronic overload
Temporary union (simple adhesion) or permanent (fibrotic ct) between articular surfaces
What is the etiology, clinical manifestation and invasive treatment of structural incompatibility?
Post macrotrauma hemarthrosis or prolonged static loading (eccentric bruxism/clenching)
Single, dry click when opening (temp adhesion) or severe limited opening without noises
Manually manipulate under anesthesia, arthrocentesis or arthroscopy of conservative management fails
What is subluxation?
Sudden displacement of condyle anterior to eminence
Causes dull sound (thud) at end of MO
can do opposing exercises, intraoral limiters and voluntary restriction
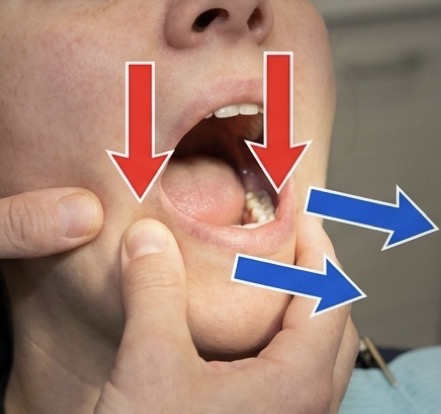
What is spontaneous dislocation?
Mandible locks in full opening, closure impossible
Very painful due to elevator muscle spasm
Firm continuous downward pressure on lower molars then a gentle backward push treats it
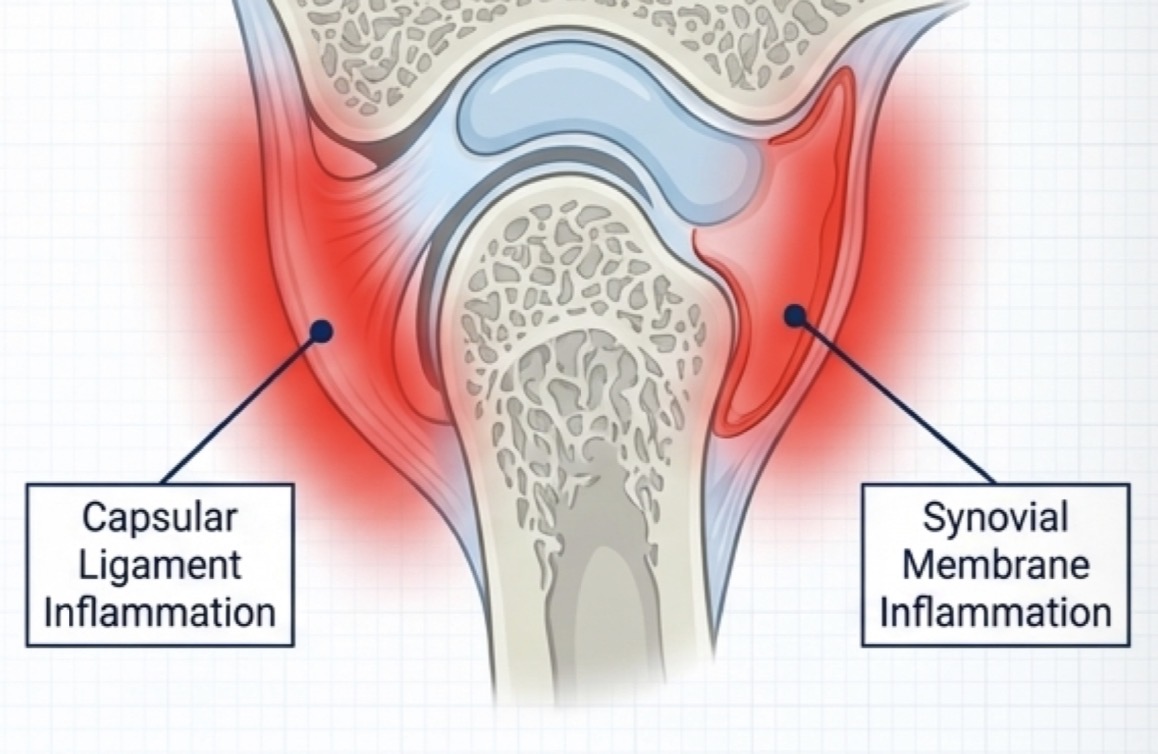
What is synovitis and cpasulitis?
Canst distinguish between these without arthroscopic access
Inflammation of synovial intima or capsular ligament
Due to single macro trauma (direct blow to chin) or many micro traumas from muscle hyperactivity
What is the biomechanical diagnosis of synovitis and capsulitis, clinical palpation and treatment protocol?
Continuous pain exaggerated only by elongating the capsular ligament (at MO or translation)
Acute pain just anterior to tragus and at lateral pole of condyle
Soft diet, schedules NSAIDs, thermotherapy (moist heat) and ultrasound
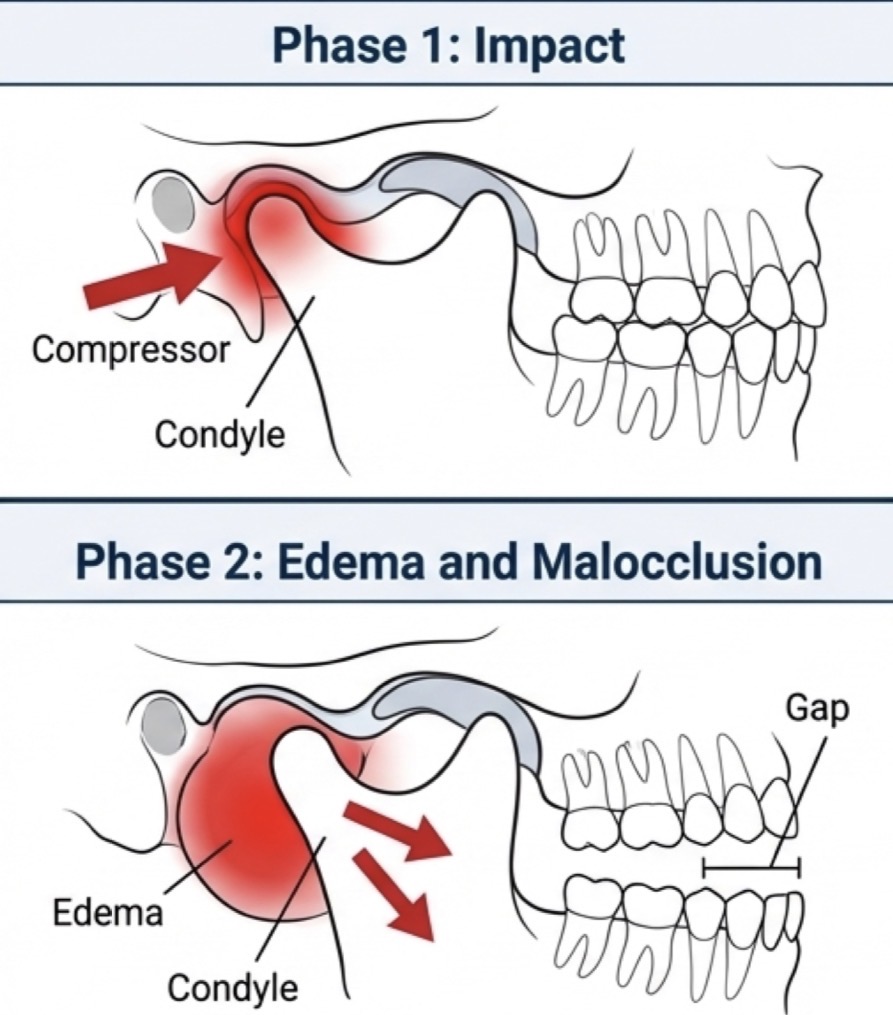
What is retrodiscitis?
Inflammation off retro disc tissue related to suppression of TMJ cavity
Diagnostic key- severe edema in retrodiscal space pushes condyle down and forwards- causes acute loss of ipsilateral posterior occlusal contact (malocclusion)
Extrinsic etiology- trauma (whiplash or blow to chin) impacts condyles into posterior zone
Intrinsic- chronic anterior disc dislocation, condyle repeatedly compresses retrodiscal bed
Treat- temp stabilisation appliance to offload tissue (extrinsic) or anterior repositioning device (intrinsic)
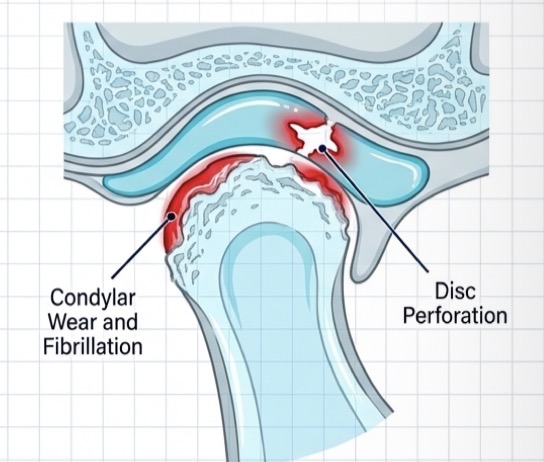
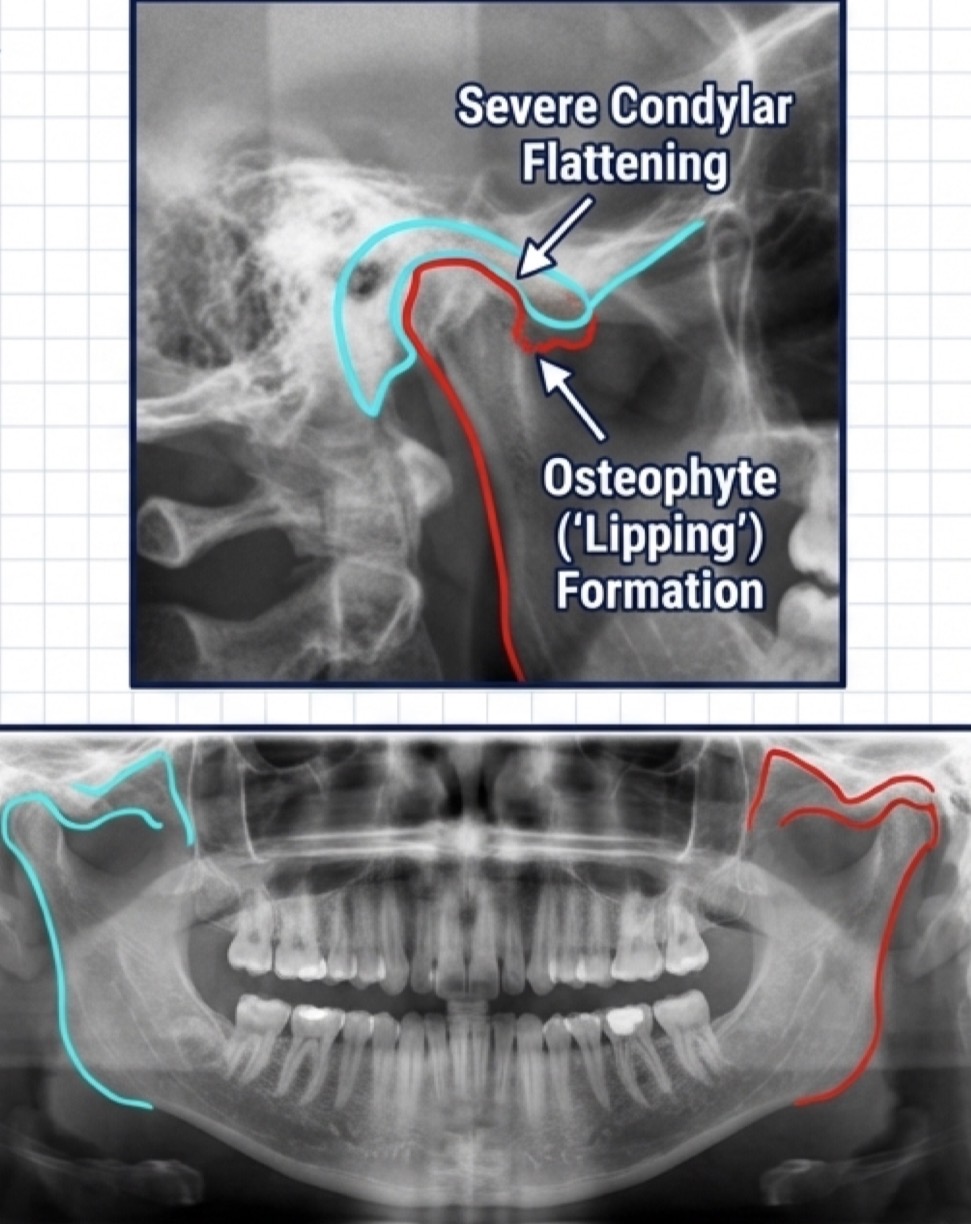
What is osteoarthritis- degenerative arthropathy- define, etiology, clinical symptoms, x ray, management?
Destructive disorder of subarticularbone and articular surfaces- not mainly inflam initially
Chronic overload (freq dislocations) excess capacity for cellular adaptation
Unilateral joint pain (worsens at end of day), crepitus (sand like noise) and soft end feel
Severely flat condyle, osteophyte (lipping) formation and cortical erosion
Radical reduction of mechanical load via occlusal appliances, soft diet and NSAIDs
What are the 3 natural self limiting stages of osteoarthritis?
1- click/joint lock
2- rigid lock + acute pain
3- fibrotic adaptation (pain stops, crepitus persists, opening recovers)
What is infectious arthritis?
Barrial invasion via penetrating trauma or adjacent extension, needs ATB
What is Hyperuricemia (gout)?
Precipitation of monosodium urate crystals, DD via serum analysis
What is rheumatoid arthritis?
Systemic AI disease, aggressive, bilateral presentation in TMJ
How do you treat systemic polyarthritic disorders in TMJ?
NSAIDS
Localised heat
Muscle relaxation
Must refer to rheumatology
Contraindications- correcting open bite with orthodontics during acute phases
Difference between osteoarthritis and rheumatoid polyarthiritis
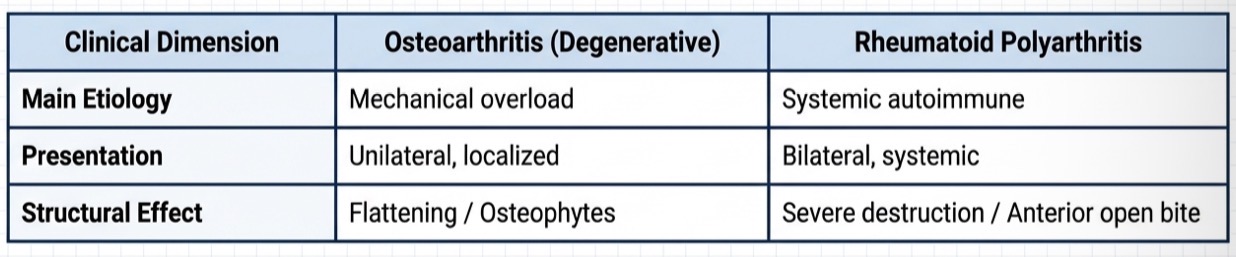
What is temporal tendinitis? (DD)
Inflammation of distal insertion of temporal muscle on coronoid process
Secondary to hyperactivity (bruxism)
Causes referred retro orbital pain
Direct intraoral palpation produces sharp pain
Treat- maxillary rest, control parafunctions with splints and analgesics
What is the stylomandibular liagment?(DD)
Chronic inflammation of ligament
Pain at mandibular angle radiating to ear
Worsens with protrusive movements
Treat- maxillary rest, control parafunctions with splints and analgesics
A diagnostic block injecting LA without vasoconstrictor into muscular/ligament insertion will relieve symptoms
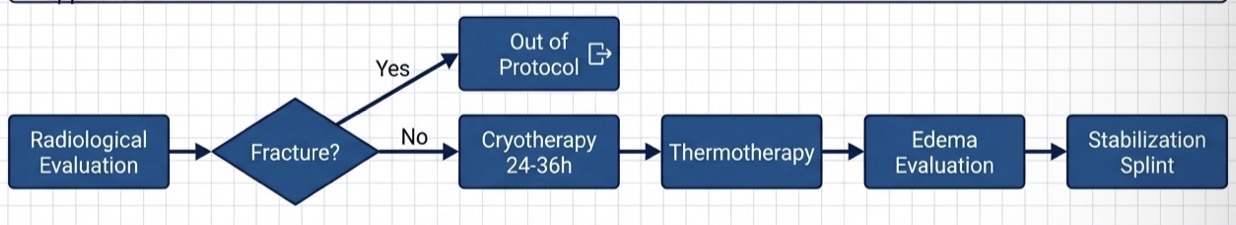
Clinical considerations in acute trauma- initial triage, conservative vs acute management and mechanical support?
Radiographs (opg or transcranial) to rule out maxilofacial or condylar fractures
Soft diet, total restricted mastication for 2 weeks, no aggressive pharmacological intervention
Repeated cryotherapy (first 24-36 hrs) for vasoconstriction , then thermatherapy to remove exudates