Bordetella pertussis / Whooping cough MCDB 132
1/65
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
66 Terms
What disease does Bordetella pertussis cause in infants?
Whooping cough
What is the reservoir for B. pertussis?
Humans
What is the transmission for B. pertussis?
air droplets/ coughing person to person
What disease does B. pertussis cause in adults?
Mild persistent cough
What can complications with B. pertussis lead to?
Secondary pneumoniae; death
What are the symptoms of B. pertussis?
Severe cough
Is B. pertussis Gram - or Gram +?
Gram -
What shape is B. pertussis?
Coccobaccillus
Is B. pertussis aerobic or anaerobic?
It is an obligate anaerobe.
Is B. pertussis motile or non-motile?
It is non-motile.
What is the nickname for B. pertussis infections?
100-day cough
What are the 3 stages of B. pertussis disease?
Catarrhal stage
Paroxysmal stage (toxemic stage)
Convalescent stage
What happens during the Catarrhal stage of B. pertussis disease?
Week 0-2
URT colonization
Bug is very contagious
Intense cough, but no whooping sound
Bug presence in throat cultures increases
Antibiotics are able to lower the severity and duration of the disease
What happens during the Paroxysmal stage (toxemic stage) of B. pertussis disease?
Week 2-8
Cough severity increases with whooping sound
Bug presence in throat culture decreases
Antibiotics are not able to lower disease symptoms because of toxins
What happens during the Convalescent stage of B. pertussis disease?
Week 8-12
Gradual recovery
Susceptible to other respiratory infections (pneumonia)
What are the main symptoms during the Catarrhal stage for B. pertussis?
Runny nose, low-grade fever, mild and occasional cough, highly contagious.
What are the main symptoms during the Paroxysmal stage for B. pertussis?
Fits of numerous and rapid coughs followed by “whoop” sound, vomiting and exhaustion after coughing fits (called paroxysms)
What are the main symptoms during the Convalescent stage for B. pertussis?
Coughing lessens but fits of coughing may return. Susceptible to many other respiratory infections.
What are the general steps of B. pertussis pathogenesis?
Inhale bugs
Bugs attach to cilia of respiratory epithelial cells
Toxins are produced
Ciliated cells stop beating
What is the first step to Pertussis pathogenesis?
Inhalation of the bacteria Bordetella perussis.
What is the main function of cilia in respiratory epithelial cells (nasopharynx)?
They trap particles in mucin and push them out. Cilia in URT push down into throat, cilia in LRT push up towards throat.
What do the toxins of B. pertussis do once they are produced by B. pertussis attached to cilia of nasopharynx?
They paralyze the cilia, causing inflammation of respiratory tract. This interferes with clearing of pulmonary secretion. Cilia cells stop beating (paralyzed) so they can’t clear debri, leading to coughing fits.
What part of the body is the nasopharynx?
The nose and throat.
What are the two general categories of virulence factors in B. Pertussis?
Adhesins and toxins.
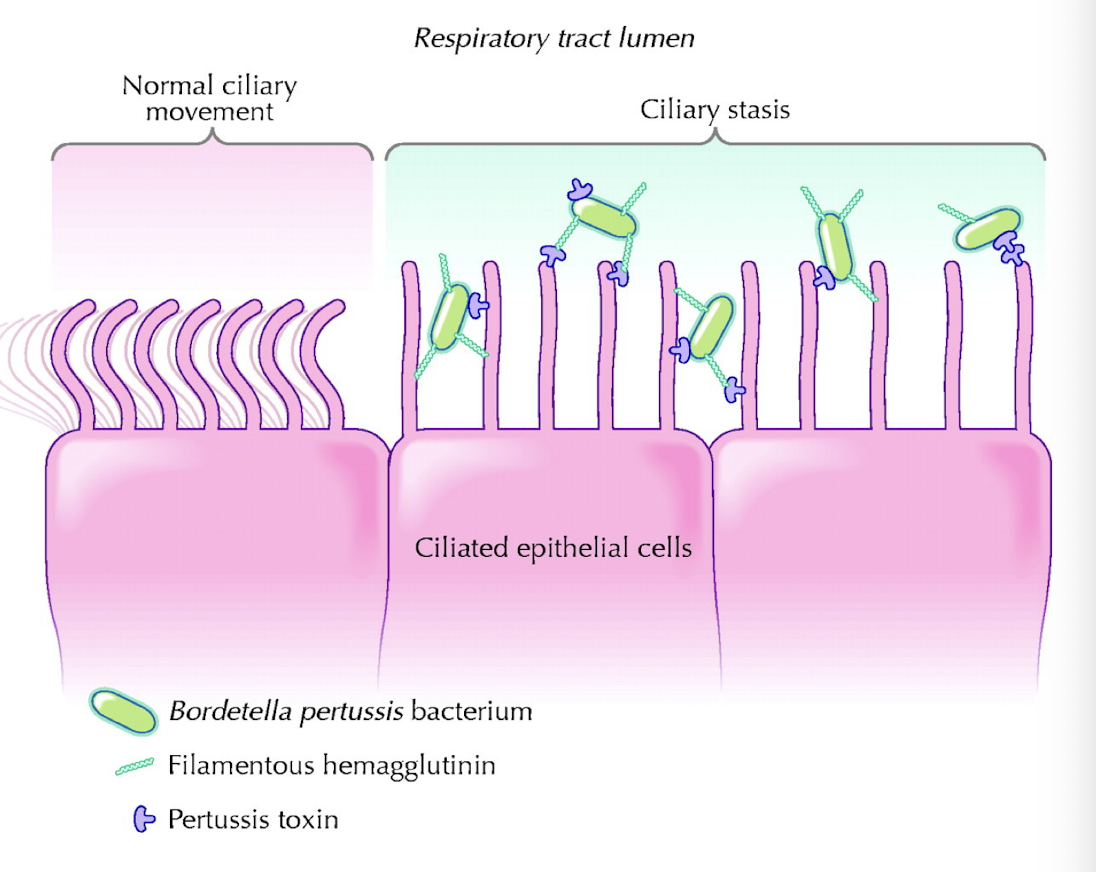
What does FHA stand for?
Filamentous hemagglutinin
What is the primary adhesin of B. pertussis?
Filamentous hemagglutinin (FHA)
What does FHA (Filamentous hemagglutinin) do?
It binds ciliated cells and phagocytes.
What does PT stand for in the context of B. Pertussis pathogenesis?
Pertussis Toxin
What is the role of PT?
It acts as a secondary adhesin, anchoring B. pertussis to host cell surfaces.
What type is cell-bound PT?
A1B5 Type
What are the six subunits of PT?
A (active) subunit → S1
B (binding) subunits → S2-S5
there are two S4 subunits, they act as the “glue” for the pentamer
What does subunit S2 of PT do?
Binds to ciliated cells
What does the subunit S3 of PT do?
Binds to phagocytes
Does B. pertussis invade the blood? If not, what does it do?
It does not invade the blood. Instead, it adheres to the respiratory epithelium cells and produces toxins to damage tissue and evade the immune system.
What is the general role of the A subunit of bacterial exotoxins?
A is for Active. It usually has enzymatic activity to disrupt host cell.
What is the general role of the B subunit of bacterial exotoxins?
B is for Binding. B subunits are responsible for identifying the target cell, binding to its receptors, and facilitating the entry of the A subunit.
What is the role of the S1 subunit of PT (pertussis toxin)?
S1 is an enzyme that ADP-ribosylates (ADPR) a G protein (Gi), inactivating it from turning off Adenylate Cyclase (ACase), leading to uncontrolled increase in cyclic AMP (cAMP).
What are the effects of PT?
rise in cAMP (ATP + ACase = cAMP)
inactivates (ADPR) G proteins (in WBCs)
lowers phagocyte killing
sensitizes cough neurons (cough reflex)
blocks neuronal cough inhibition, leads to violent coughing
What does ACT stand for in the context of B. Pertussis pathogenesis?
Adenylate Cyclase Toxin
What is ACT?
ACT (Adenylate Cyclase Toxin) is itself an ACase (adenylate cyclase enzyme) release by B. Pertussis. It requires host calmodulin (a protein) to become active. Once active, it converts ATP into cAMP, driving up cAMP levels.
What is meant by ATP + ACase = cAMP?
This represents a single-step biochemical pathway where the ACase enzyme converts ATP into cAMP.
How does excessively high levels of cAMP effect phagocytes?
Too high levels of cAMP overstimulates/ intoxicates phagocytes, impairing their ability to kill bacterial invaders.
What does the tracheal cytotoxin (TCT) do in B. Pertussis pathogenesis?
It kills ciliated cells which impairs their ability to clear debris (stop beating), resulting in an increase of nitric oxide (NO) which is toxic. This leads to mucus build up and coughing fits.
What does the lethal toxin do in B. Pertussis pathogenesis?
It causes inflammation and local necrosis (irreversible death of cells) at sites near bugs.
What are the two adhesin pertussis virulence factors?
PT (cell-bound) B subunits
FHA (filamentous hemagglutinin)
What are the four toxin pertussis virulence factors?
PT (S1 subunit)
ACT - adenylate cyclase toxin
Tracheal cytotoxin (TCT)
Lethal toxin
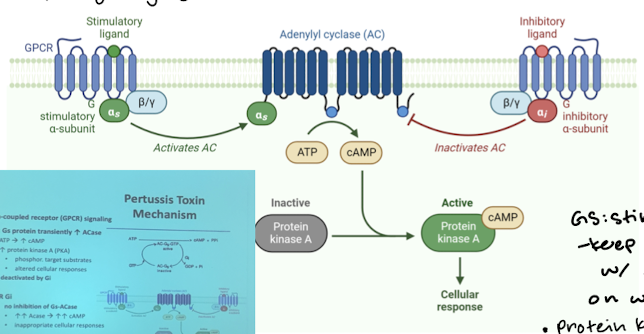
What is the normal mechanism of the G protein-coupled receptor (GPCR) signaling? (unaffected by PT)
Gs (stimulatory) protein transiently increases ACase which with ATP creates cAMP. cAMP activates protein kinase A (PKA). PKA phosphorylates different proteins, enzymes, and receptors, eliciting cellular response. This process is naturally regulated by Gi (inhibitory) which inactivates the whole process.
☆ On with Gs, Off with Gi
What does ADPR (ADP-ribolsylation) of Gi by PT do?/ What is the mechanism of PT?
It prevents Gi from regulating Gs-ACase system, leading to high levels of ACase and therefor high levels of cAMP. This results in inappropriate cellular responses.
What are the three methods of detection of B. Pertussis?
Culture
PCR
Serology
How long does it take for the test results of culture for B. Pertussis infection to come in?
0-2 weeks
How long does it take for the test results of PCR test for B. Pertussis infection to come in?
0-4 weeks
How long does it take for the test results of serology for B. Pertussis infection to come in?
2-8 weeks
What is the main treatment for B. Pertussis?
Antibiotics within 1-2 weeks of symptoms. Antibiotics given any later will not prevent illness or spread.
What are the vaccines/ strategies to prevent B. Pertussis infection?
DTaP vaccine
PT toxoid + FHA + other adhesins
Tdap booster every 10yr
Tdap during each pregnancy (3rd trimester)
to protect the baby in the first few weeks of its life (???)
What are the three diseases/ bacteria that DTaP is used to prevent?
Diphtheria, Tetanus, and Pertussis.
Why can’t you treat pertussis infections with antibiotics after 1-2 weeks of symptoms?
Because after that time the bugs have gone away but the damage to host cells done by pertussis toxin (paralyzation of ciliated cells, inflammation in airways) is irreversible by antibiotics. Pertussis is a toxin-mediated disease so even if there is no bacteria, pertussis toxins can still cause disease. Antibiotics are only effective if given at the catarrhal stage.
Even though antibiotics are ineffective at lessening symptoms after the catarrhal stage of a pertussis infection, why are they still given to patients?
To limit transmission and disease spread.