Mod 11: Block theory
1/110
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
111 Terms
What is the main function of the accessory digestive organs? (3)
Aquire nutrients from food
Provide enzymes for breakdown of food
produce bile for digestion of dietary fat
What are 3 accessory digestive organs
Liver
Gallbladder
Pancreas
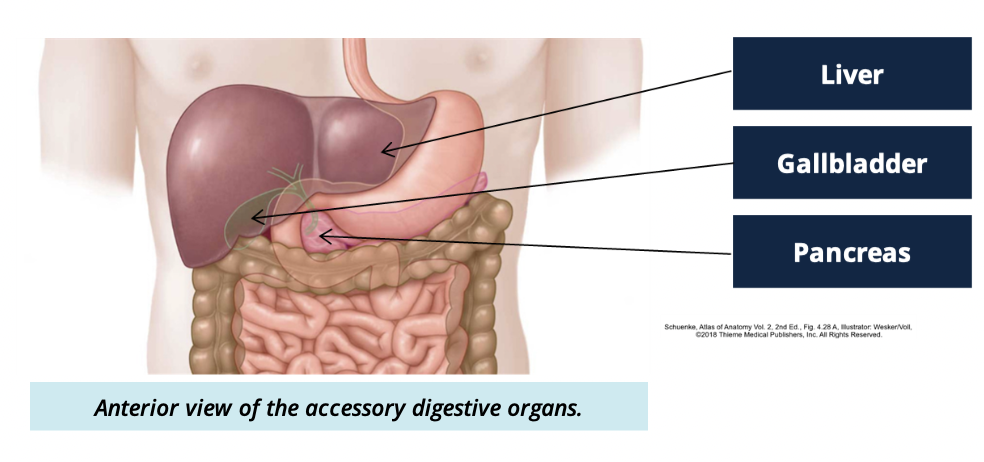
Liver functions (3)
produces bile for digestion of fats
stores dietary glucose as glycogen
so it can later be broken down + used for energy
role in metabolism of toxins, durgs, and alcohol in blood
What is the gallblader
a small organ underneath the liver
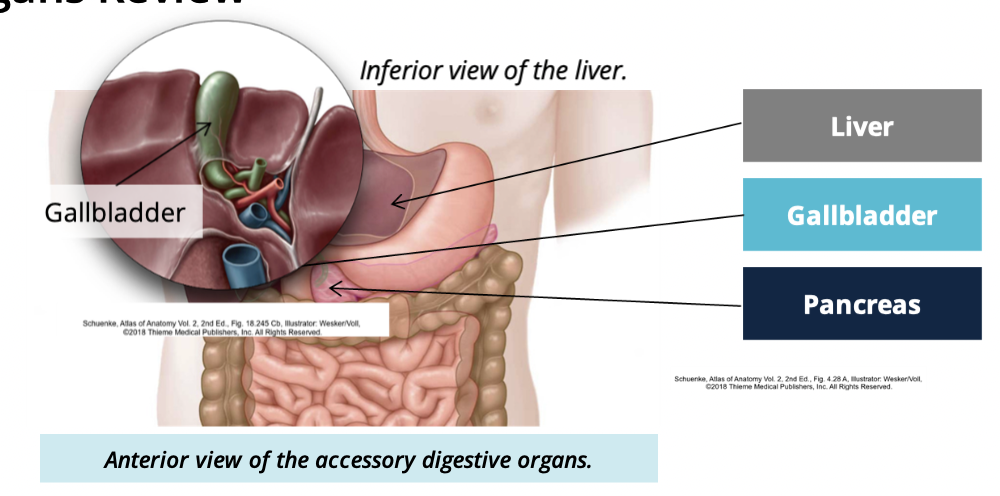
Gallbladder function
storage + release of bile in the digestive system
What is the pancreas? what does that mean?
A mixed gland
has both endocrine + exocrine functions
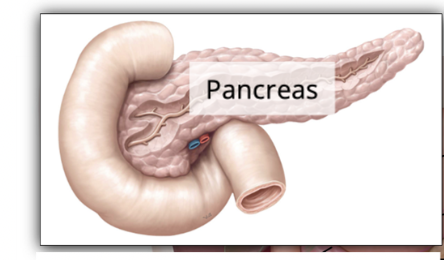
Pancreas functions
Endocrine: controls levels of blood glucose
Exocrine: secrete digestive enzymes into intestine
Where is the liver found?
sit in the upper right abdominal quadrant
inferior to diaphragm
anterior to vena cava
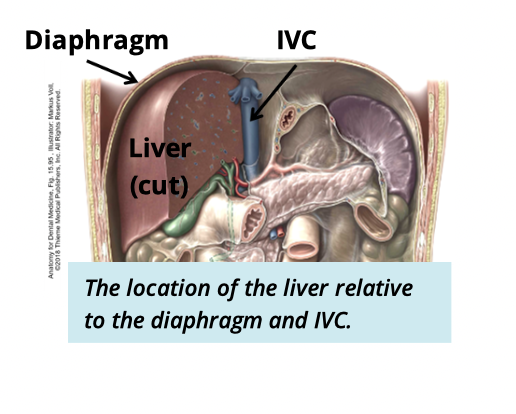
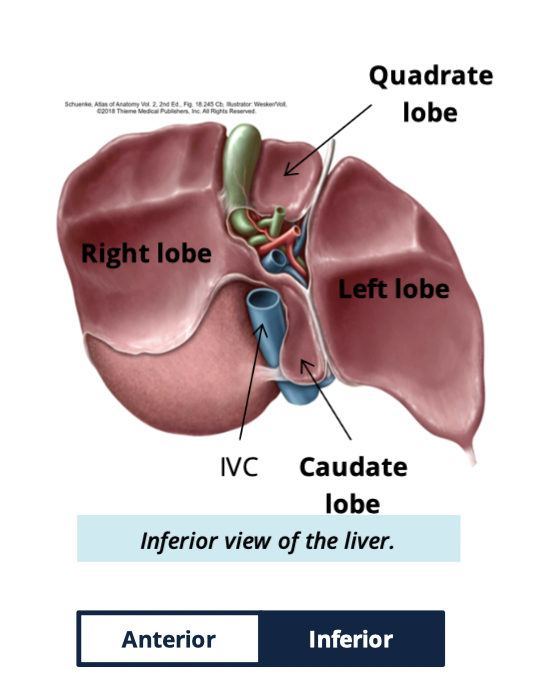
Liver has what four lobes
right
left
caudate
quadrate
What is the purpose of ligaments of the liver
attaches the liver to surrounding abdominal peritoneum and the diaphragm
what seperates the left and right lobes of the liver
Falciform
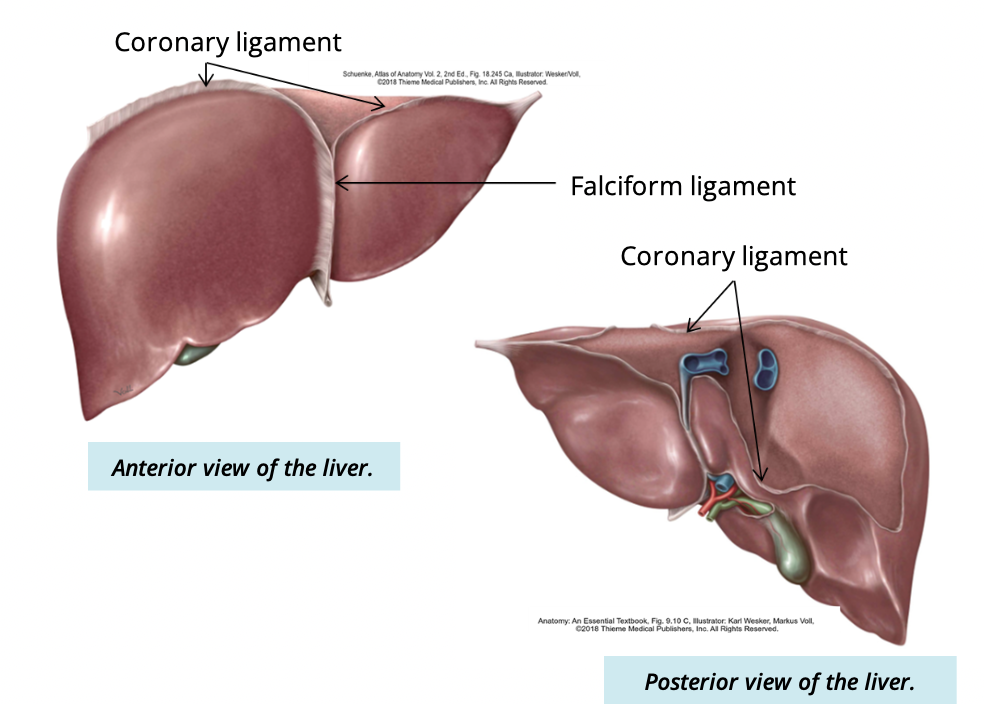
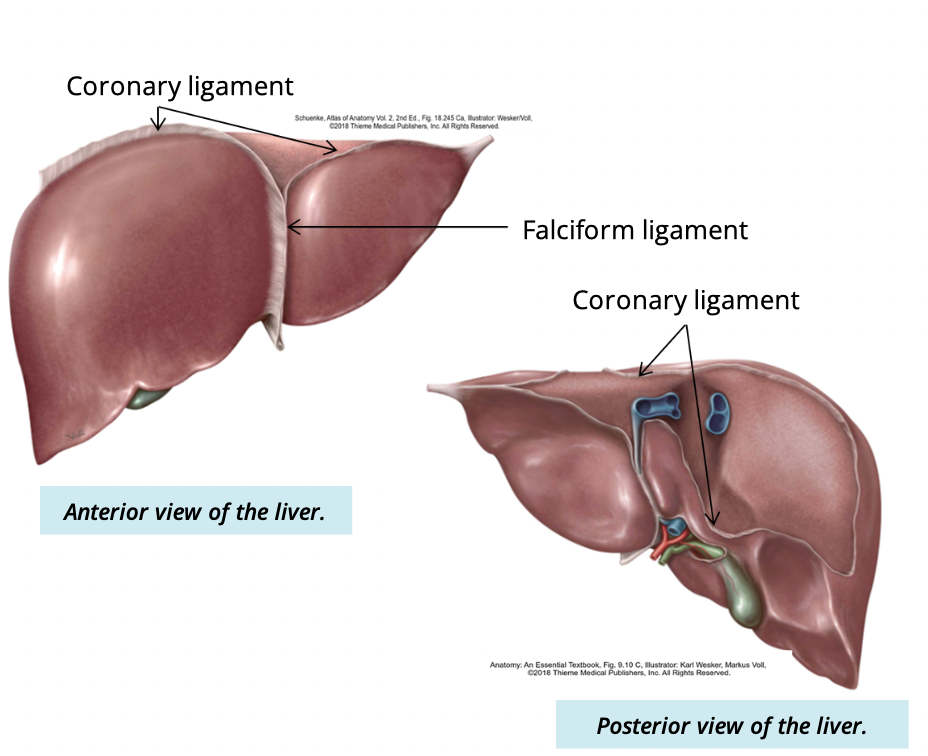
purpose of coronary ligament
suspends the liver from the inferior surface of the diaphragm
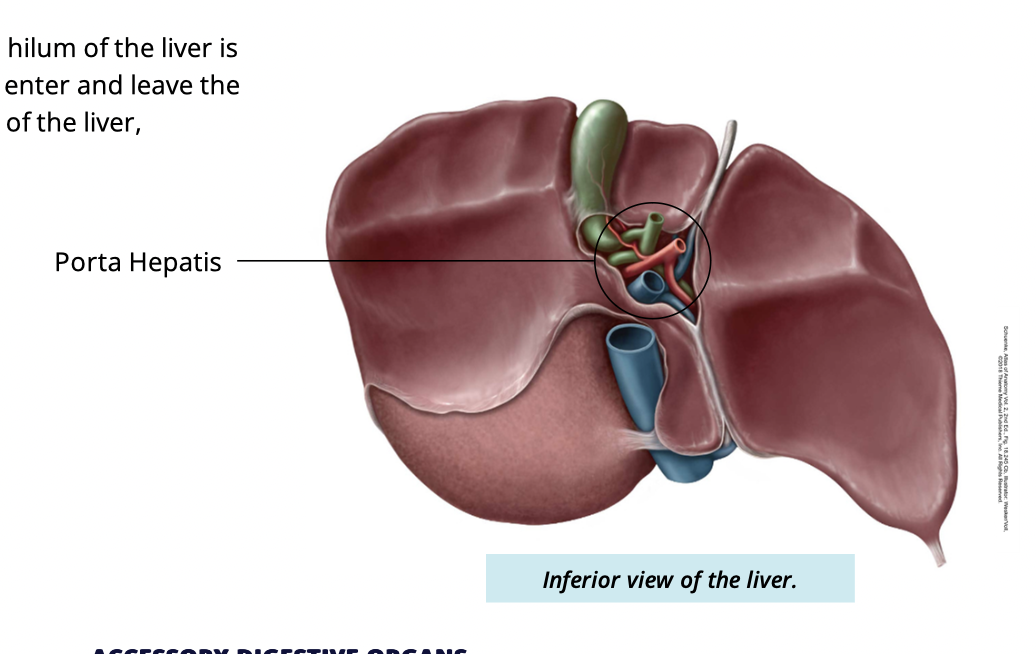
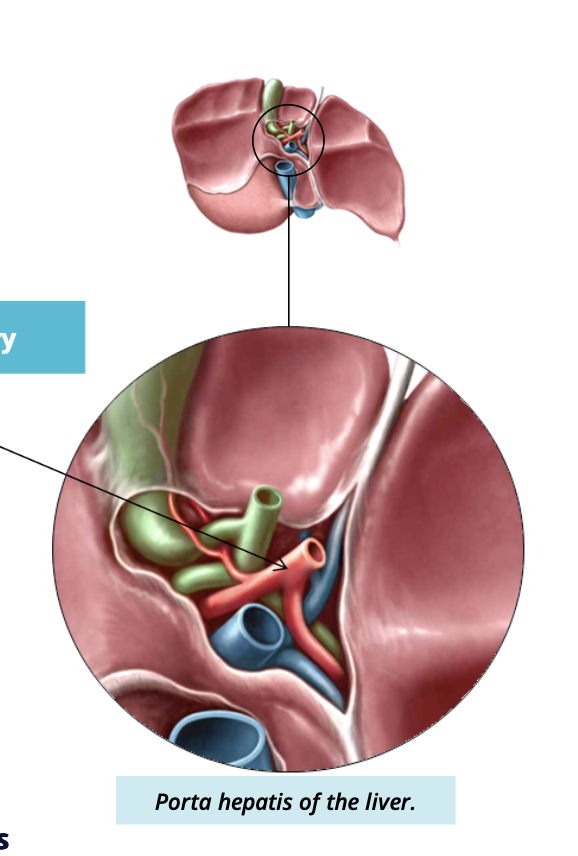
What is the porta hepatis/hilum of liver
where hepatic vessels and ducts enter and leave the liver
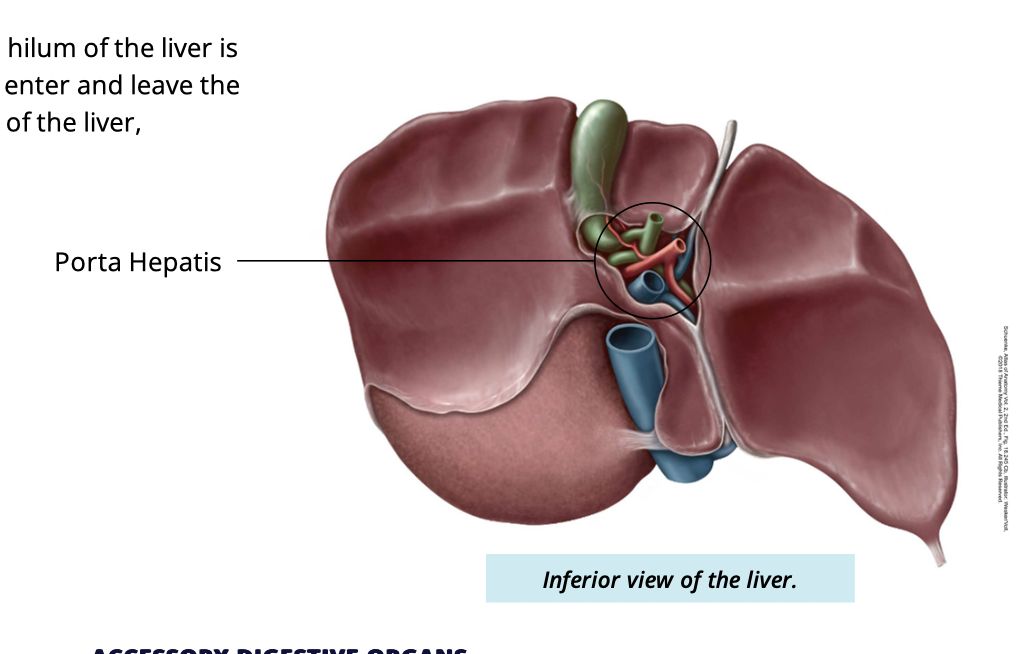
Where is the portal hepatic located
inferior side of liver
surrounded by four lobes
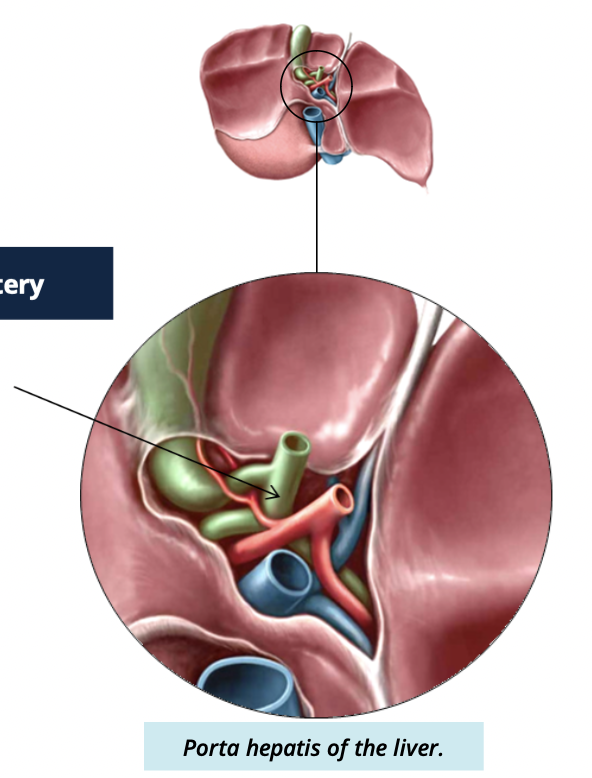
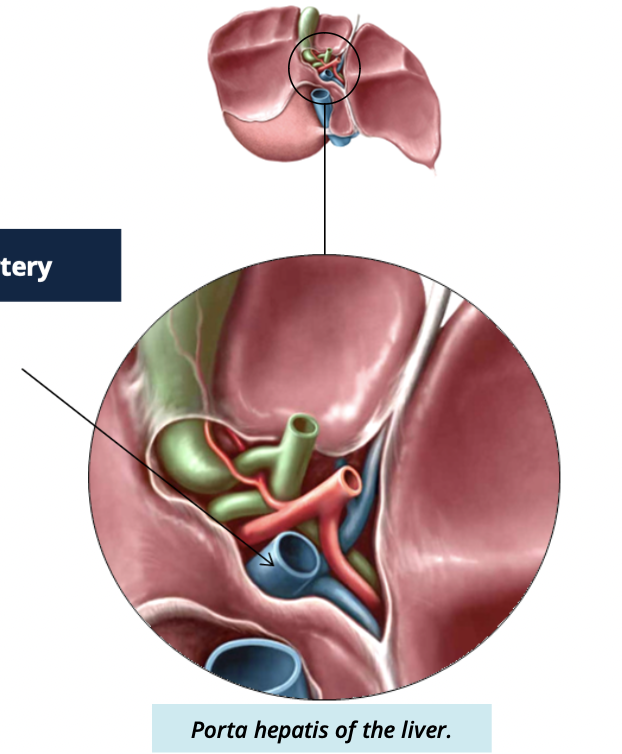
what 3 structures enter and leave the portal hepatis
Common hepatic duct
portal vein
hepatic artery
Function of common hepatic duct
drains bile produced in the liver
joins w/ cystic duct of the gallbladder to form the common bile duct
Describe portal vein function
carries nutrient rich blood from digestive system → liver
toxins/drugs travel through this vessel into the liver to be metabolized
Describe function of hepatic artery
carries oxygenated blood to the liver
branches to supply each lobe
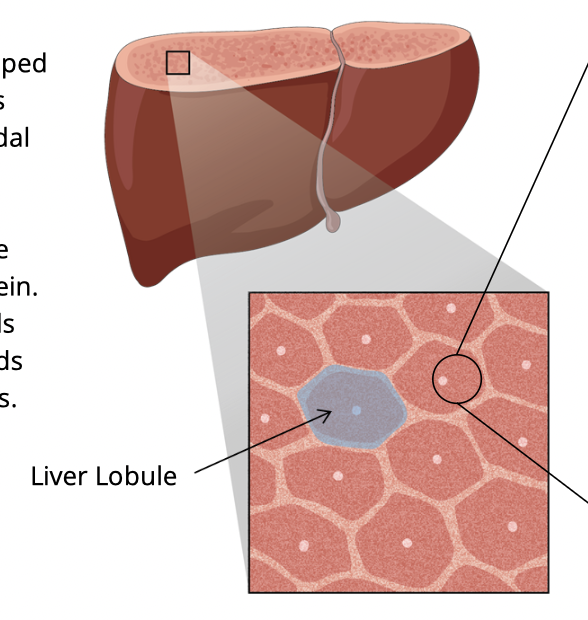
What is the functional unit of the liver?
Liver lobule (hexagonal structure)
What cells make up the liver lobule
Simple cuboidal cells called hepatocytes
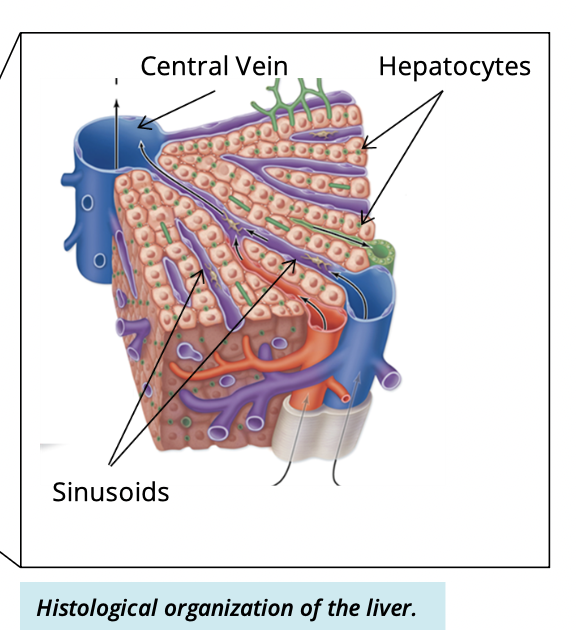
How are hepatocytes arranged
In plates (cords) radiating from a central vein
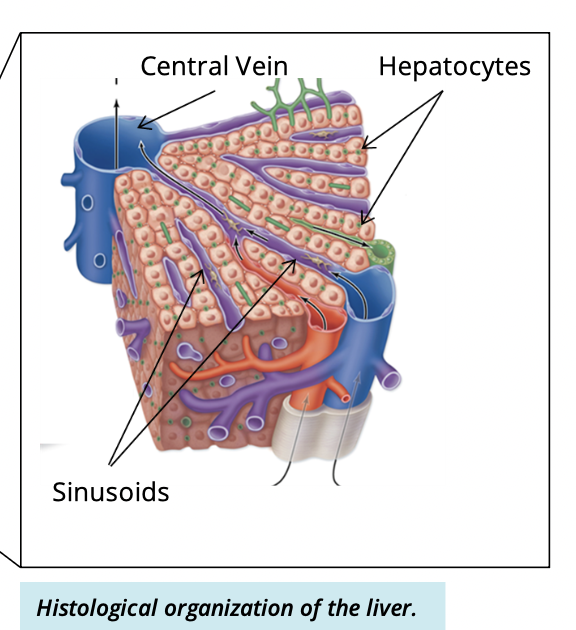
What are sinusoid?
spaces between hepatocyte plates where venous blood flows
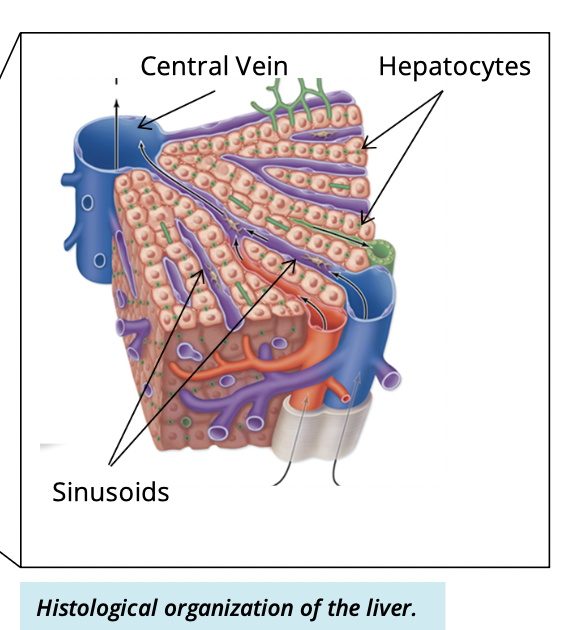
What structures make up the portal (hepatic) triad
branches of the:
hepatic artery
poral vein
common hepatic duct
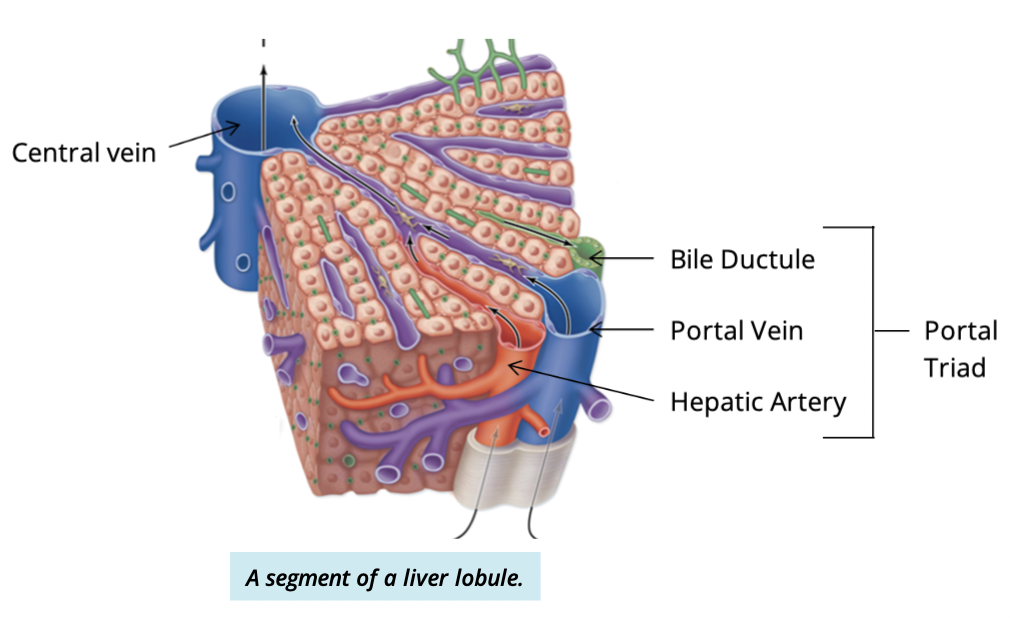
Where are portal triads lcoated in the liver lobule?
each lobule is surrounded by 6 travels
one at each corner of the hexagon
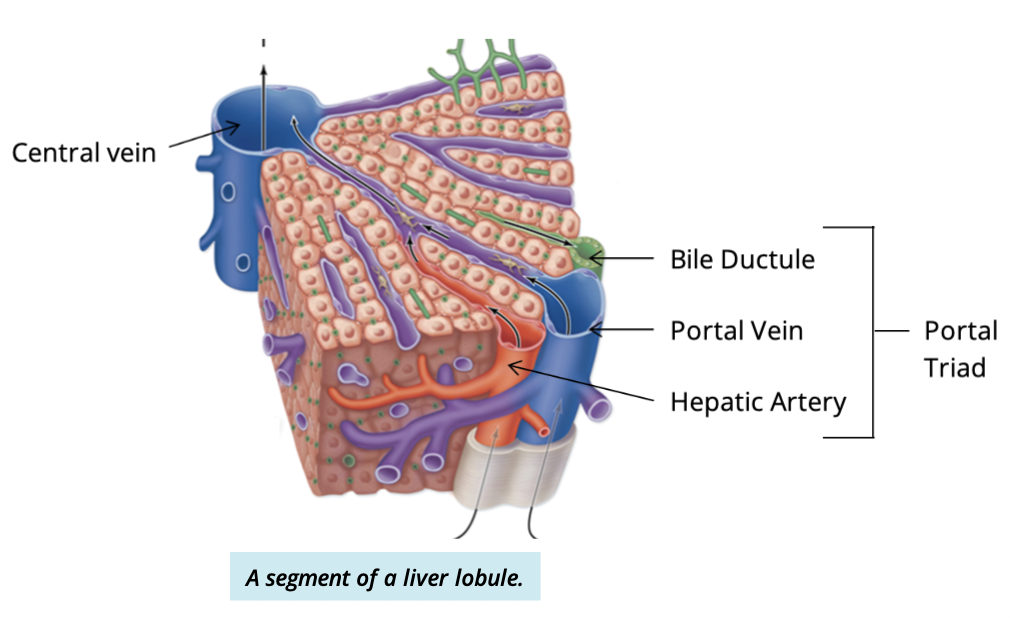
What happens in the sinusoid?
nutrient rich blood from the portal veins travels into the sinusoids
inside, the nutrients from the blood is taken up into hepatocyte
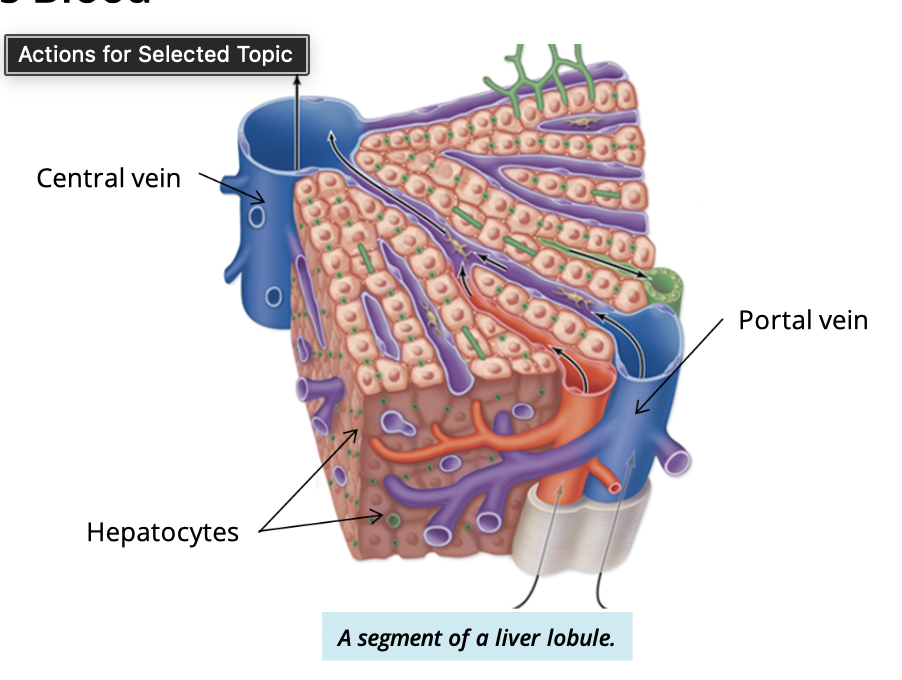
What is the path of blood flow after sinusoid?
Sinusoids → central vein → hepatic vein → inferior vena cava → heart
note: this is oxygen poor blood
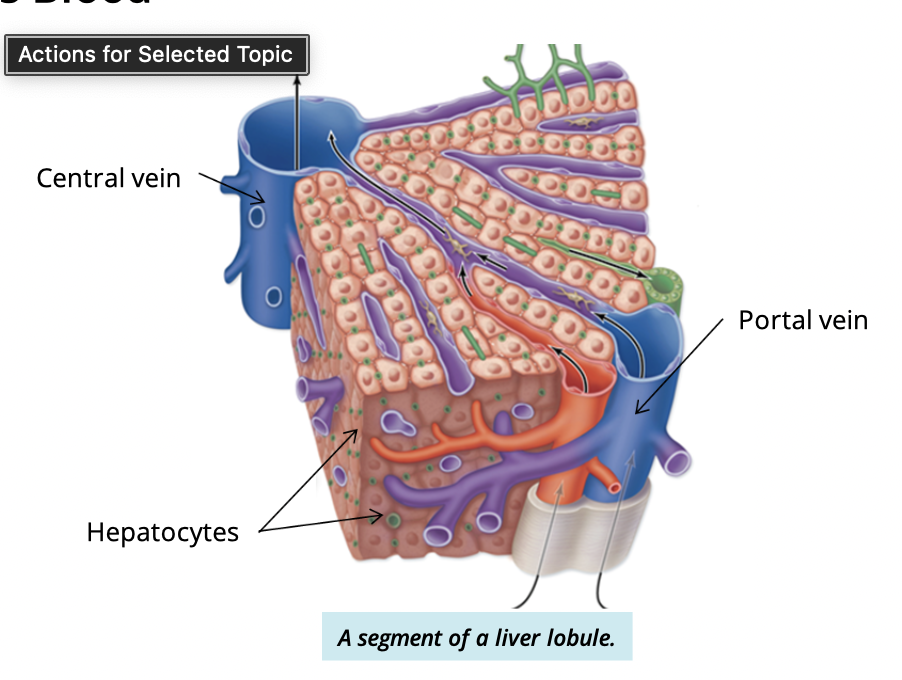
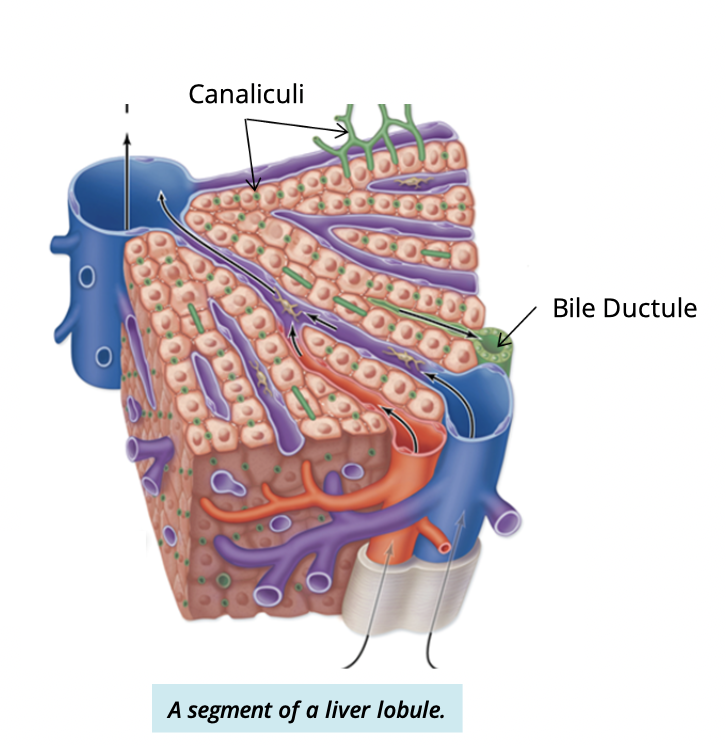
What is the pathway of bile flow in the liver?
Hepatocytes → canaliculi → bile ductules (portal triad) → hepatic ducts → common hepatic duct
what is liver cirrhosis?
a slow, progressive disease
healthy liver tissue is replaced by scar tissue
prevents liver from functioning normally
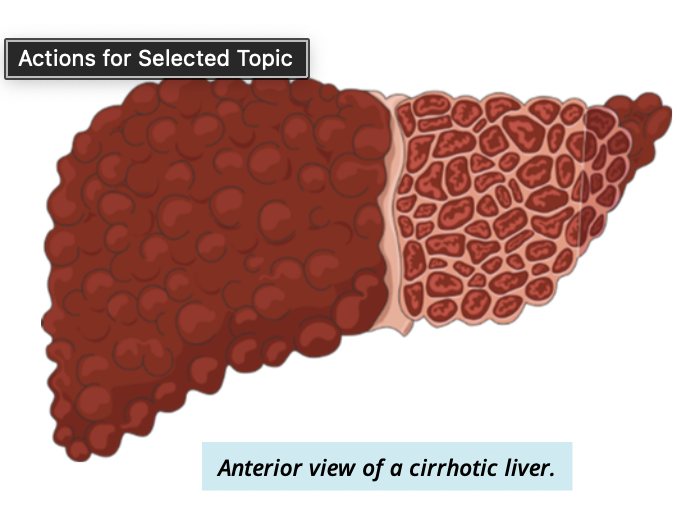
Symptoms/dysfunctions in a patient with cirrhosis
jaundice of skin
distended abdomen (bloated look)
Describe the gallbalder shape and location
peer-shaped muscular sac
lies inferior to the right lobe of the liver
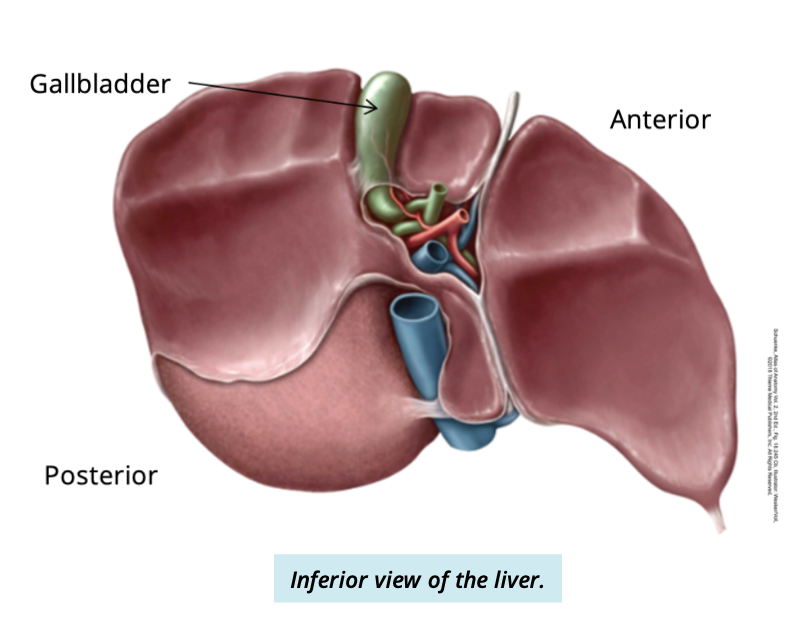
Gallbladder function
store + concentrate bile not immediately required for digestion
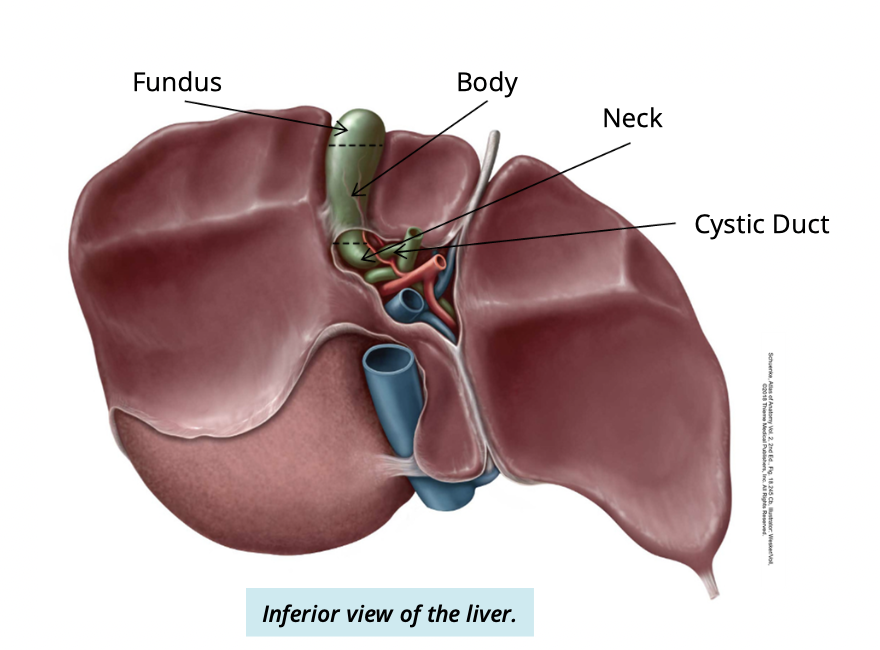
Describe and identify the 3 regions of the gallbladder
Fundus:
found anteriorly
Body:
between fundus + neck
Neck:
found posteriorly
connected to cystic duct
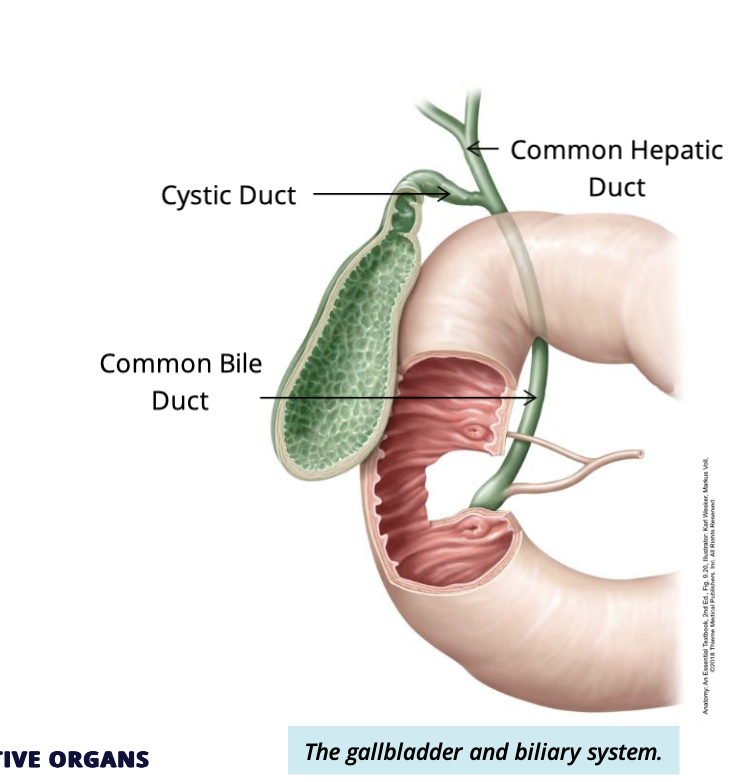
What does the biliary system consist of?
interconnected ducts that connect the liver and gallbladder
what does the duct system do?
stores and drains bile into the duodenum
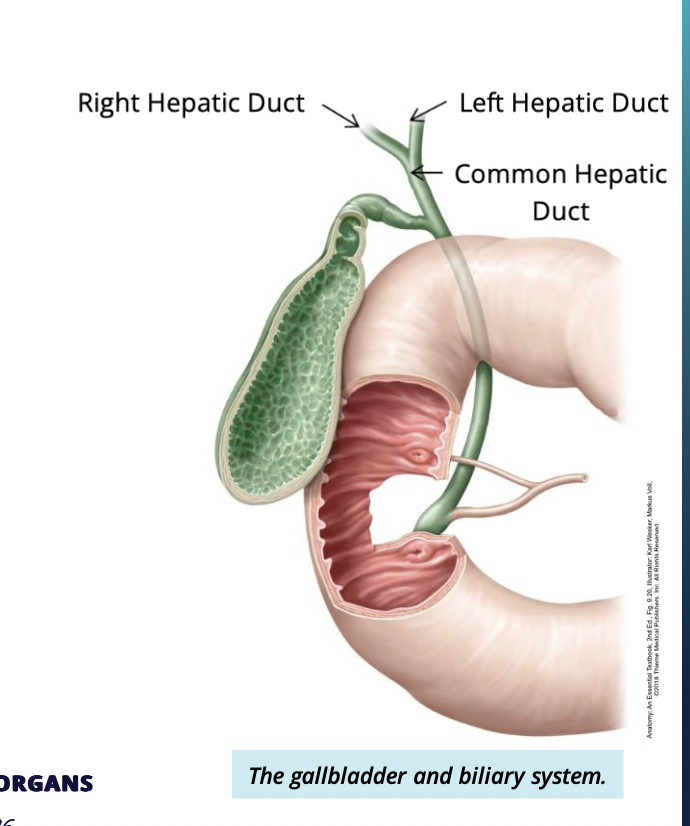
what are the ducts of the biliary system?
Hepatic ducts
cystic duct
common bile duct
Describe the hepatic duct
2 parts:
left + right hepatic ducts each coming from left or right lobe respectively
drain bile into the common hepatic duct
Describe Cystic duct
attaches to the common depatic duct
functions to transport bile to + from the gallbladder
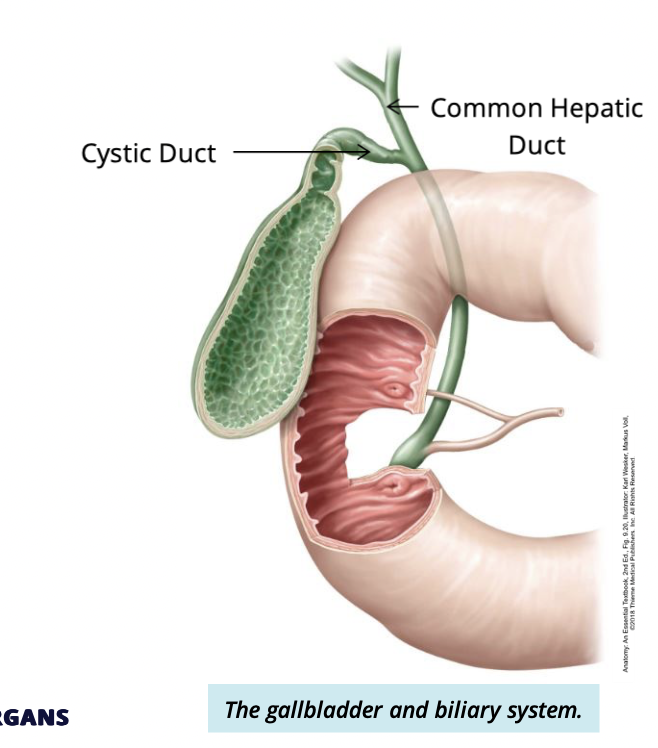
Describe the common bile duct
the common bile duct meets with the cystic duct to drain bile into the common bile duct, which enter the duodenum
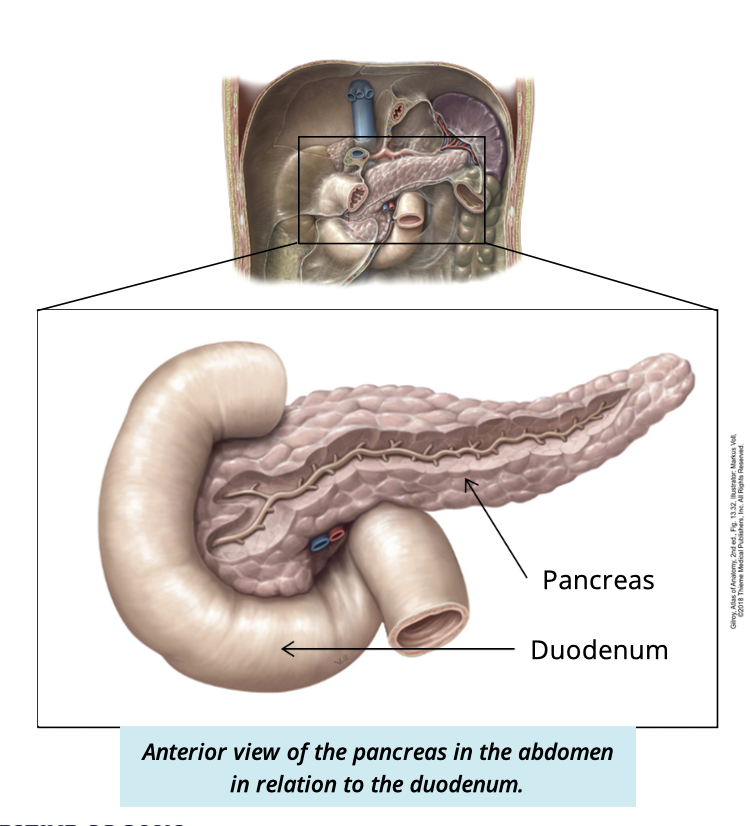
Describe the pancreas (2)
lobular organ → lies deep to the stomach
both exocrine + endocrine functions
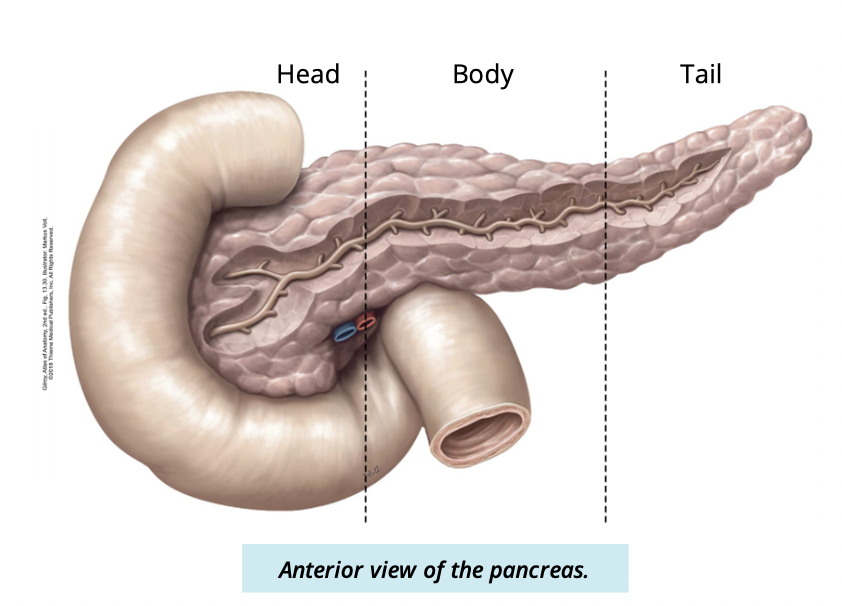
Describe and identify the parts the the pancreas is divided into (3)
head
sits in the concavity of the duodenum
body
passes behind the stomach
tail
abuts the medial side of the spleen
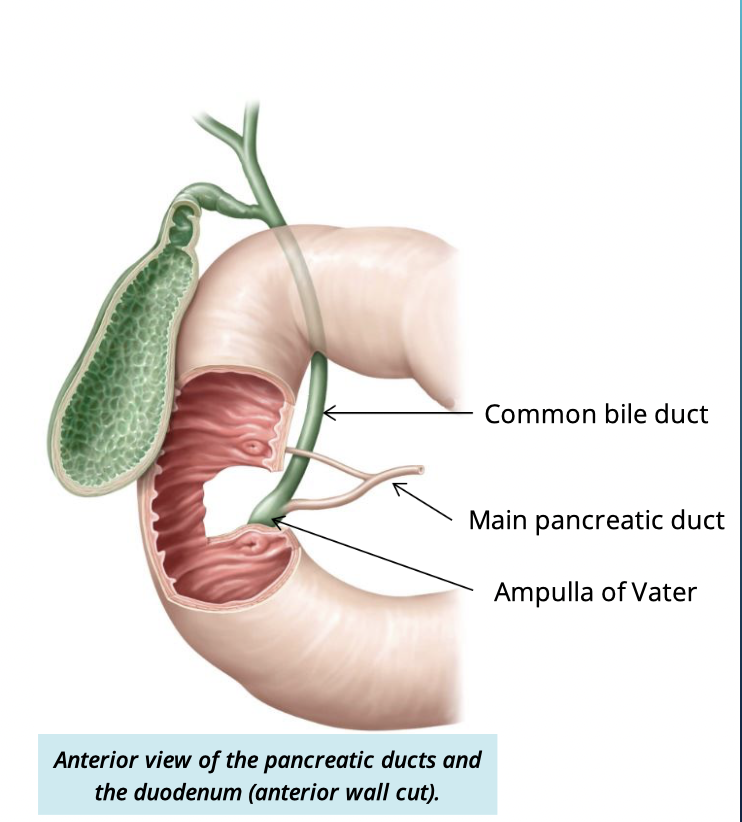
function of the main pancreatic duct
Collects the exocrine products of the pancreas
fuses w/ comon bile duct to empty into the duodenum at the hepatopancreatic ampulla of vater
Pancreas composition
99% exocrine
1% endocrine
islets of langerhans scattered within this portion
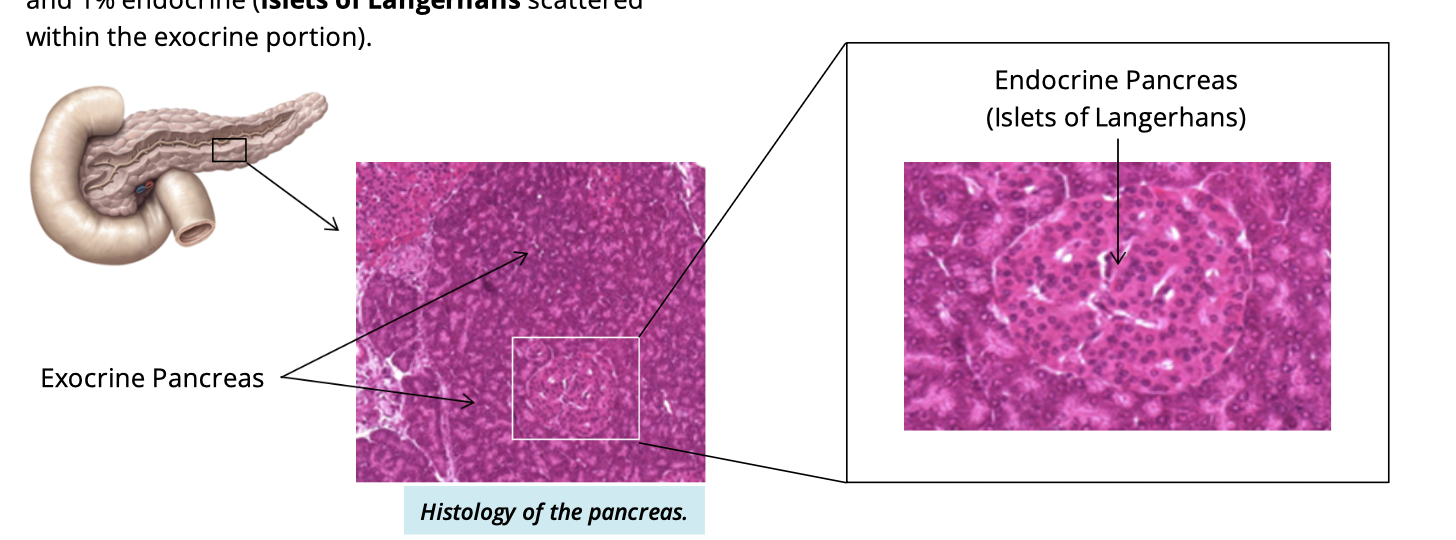
The exocrine functions of the pancreas
secretion of pancreatic juices from the pancreatic acini into the duodenum
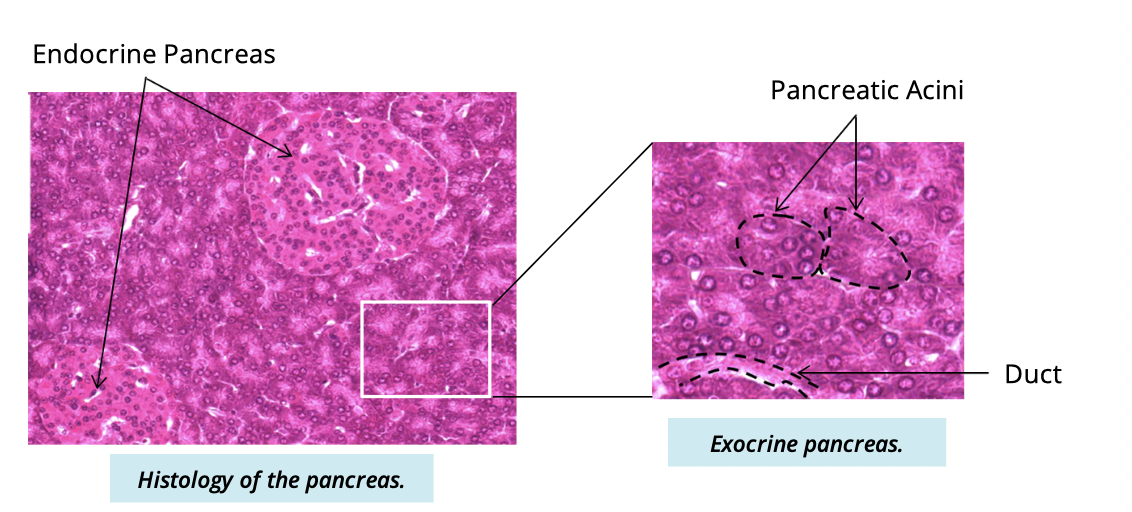
Describe pancreatic juices
rich in digestive enzymes
contain bicarbonate ions to neutralize acid from the stomach

fill using anatomical terms

Functions of the kidneys (3)
filter blood to produce urine
balance ion concentration + body fluid volume
produce erythropoitin
homrone that stimulates red blood cell production
what system do the kidneys belond to?
Urinary system
kidneys mark the beginning of the urinary system
Why is urine production important?
removes waste and excess ions from the body
Where are the kidneys located?
on either side of the spine (T12-L2)
against the posterior abdominal wall
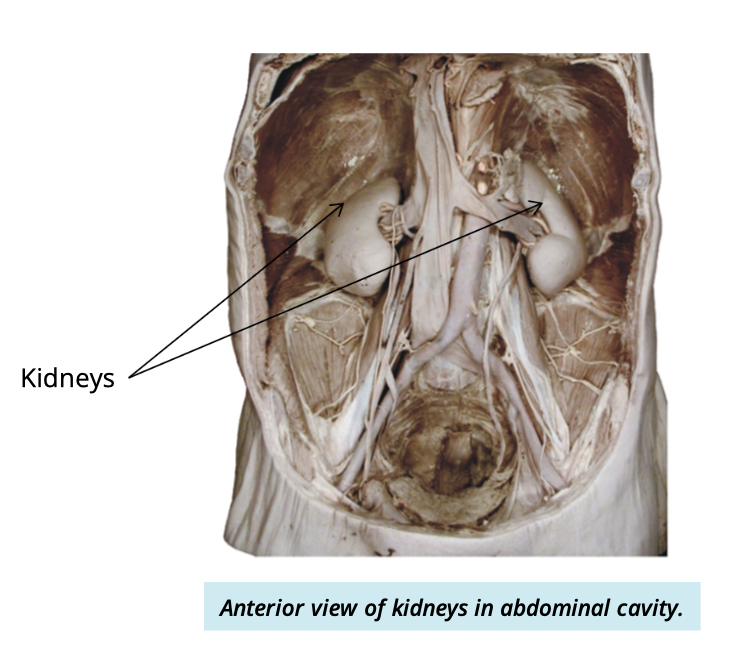
What is the shape and general size of the kidneys
bean shaped
fist sized
12cm length
6.6cm width
2.5cm thick
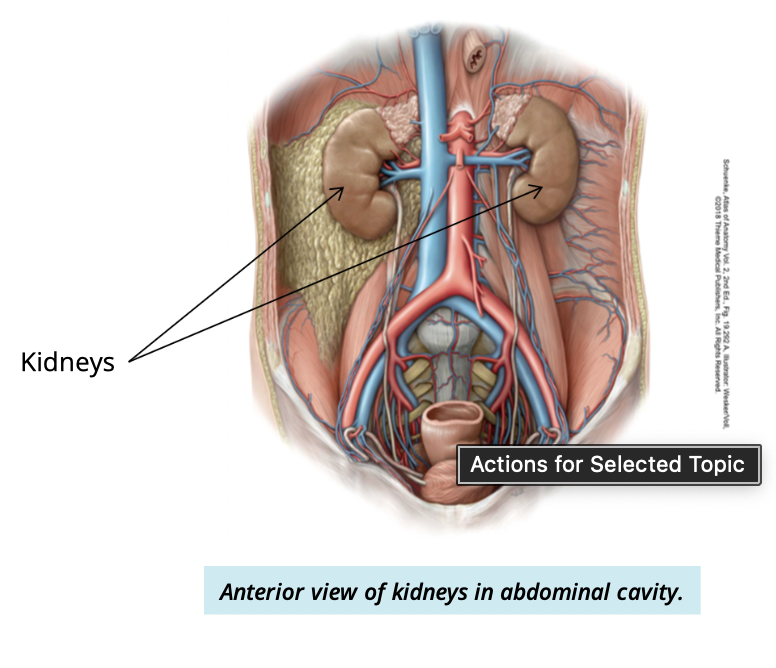
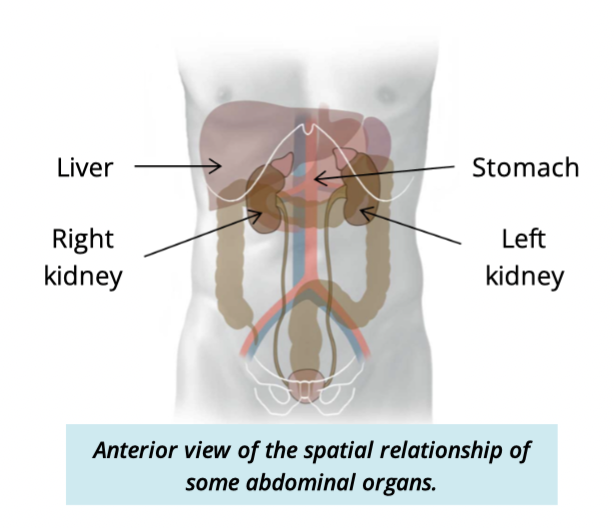
Which kidney is lower and why?
Right kidney sits lower
due to large size of liver
What is the hilum of the kidney?
the medial concave surface where vessels, nerves, and ureter enter/exit
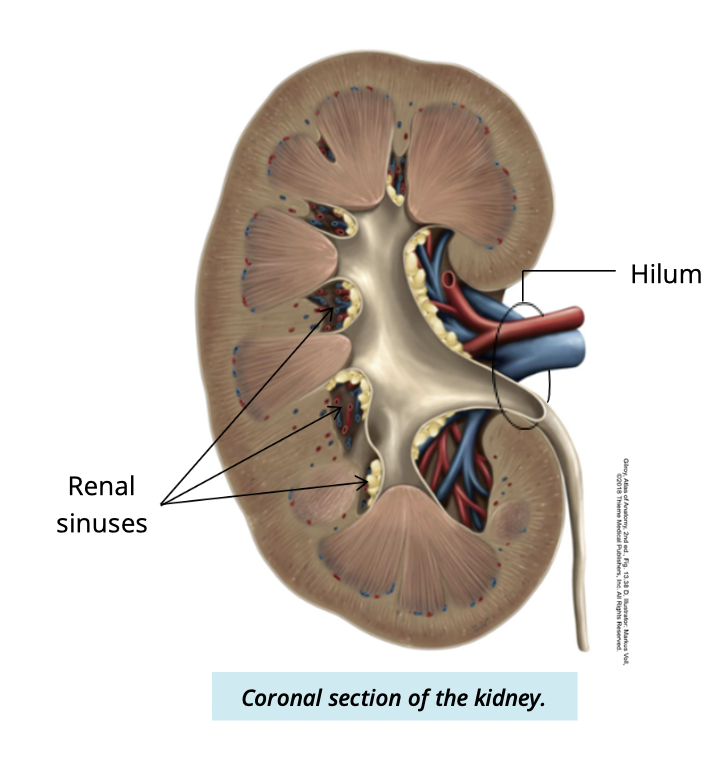
what structures pass through the hilum?
Enter:
Renal artery + nerves → enter
Exit:
renal vein + ureters -→ exit
what is the renal sinus
An internal space continous with the hilum
filled w/ fatty tissue
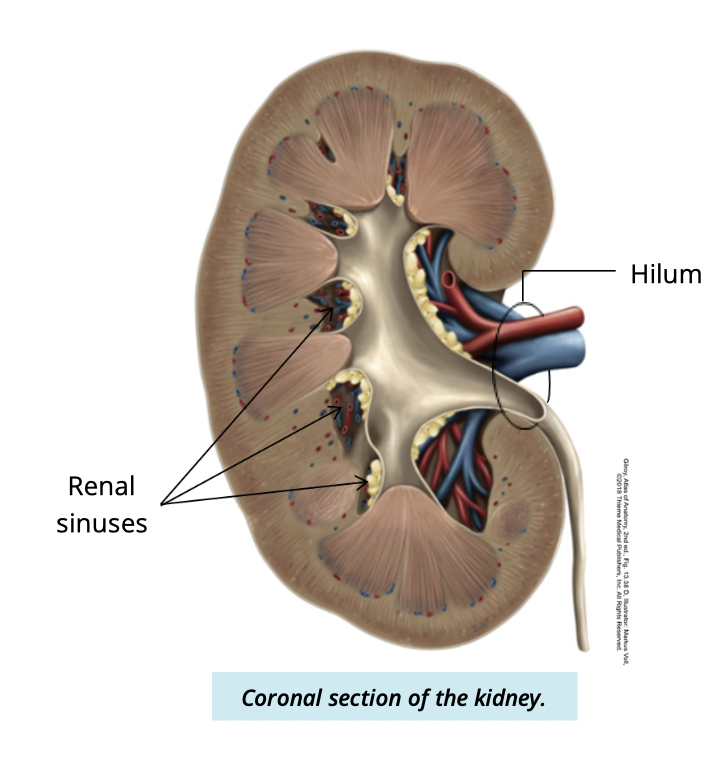
What is the renal capsule?
A fibrous layer covering the kidney
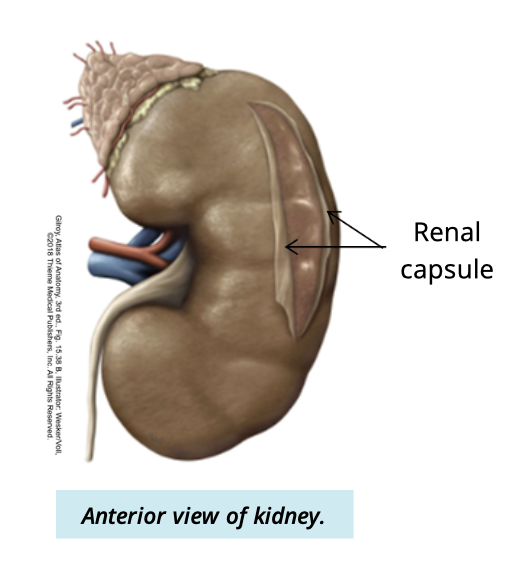
What type of tissue is renal capsule made of?
dense irregular CT
what are the functions of the renal capsule?
protects from injury/pathogens
maintains kidney shape
What is the adipose capsule?
layer of adiopose tissue external to the renal capsule
adipose capsule function
cusion + protection
completely surrounds kidney
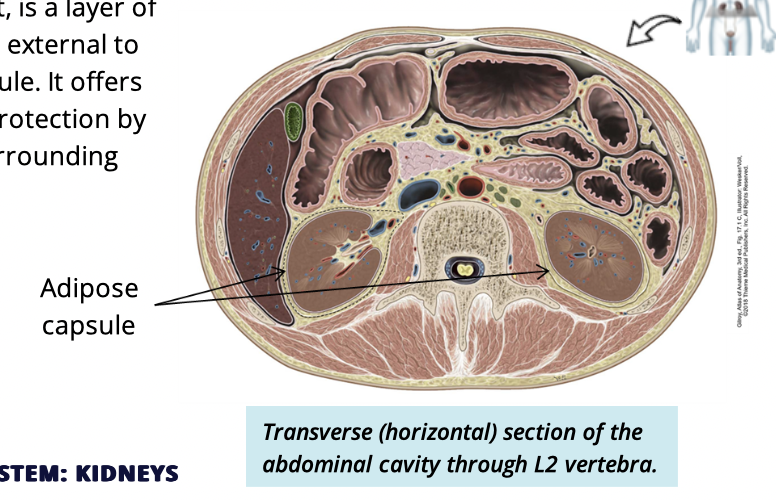
what are the two supportive tissue layers of the kidney
renal capsule
adipose capsule
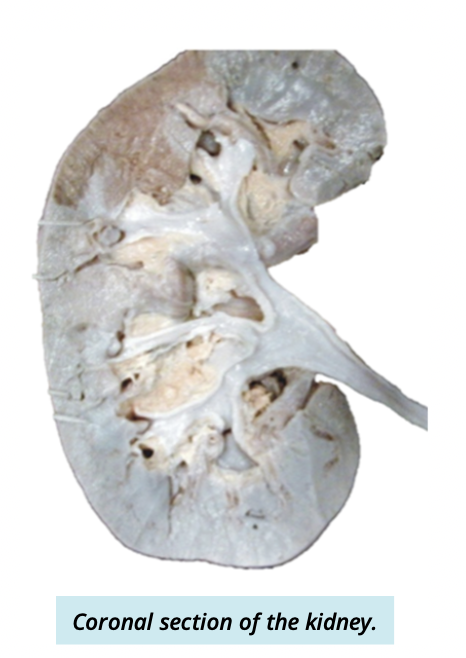
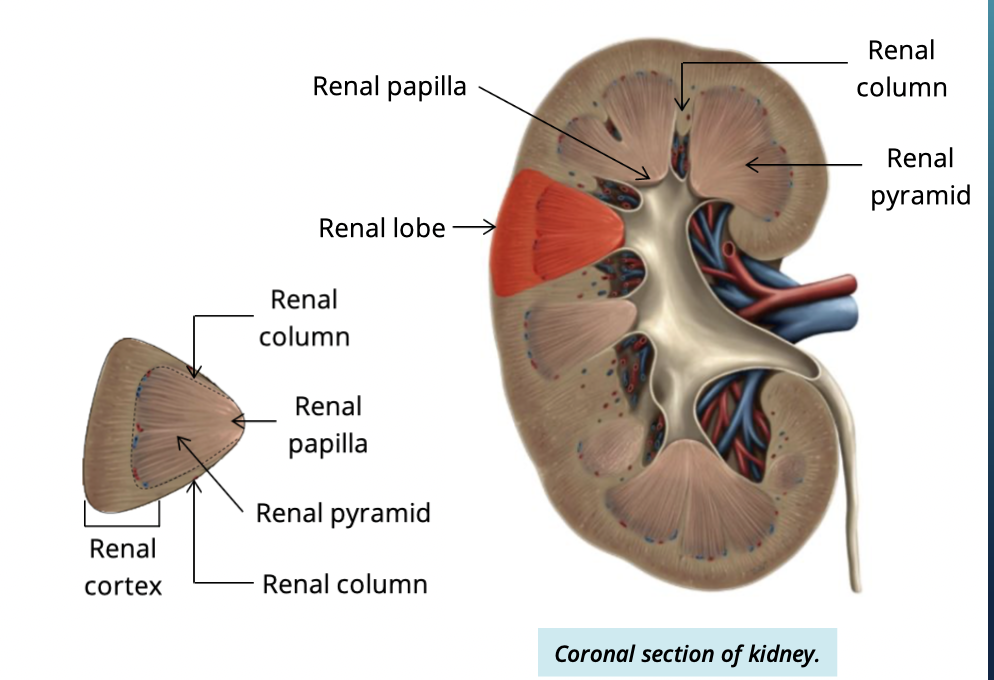
Describe + identify the two internal anatomy of the kidney
cortex
outer layer of kidney
medulla
deep to cortex
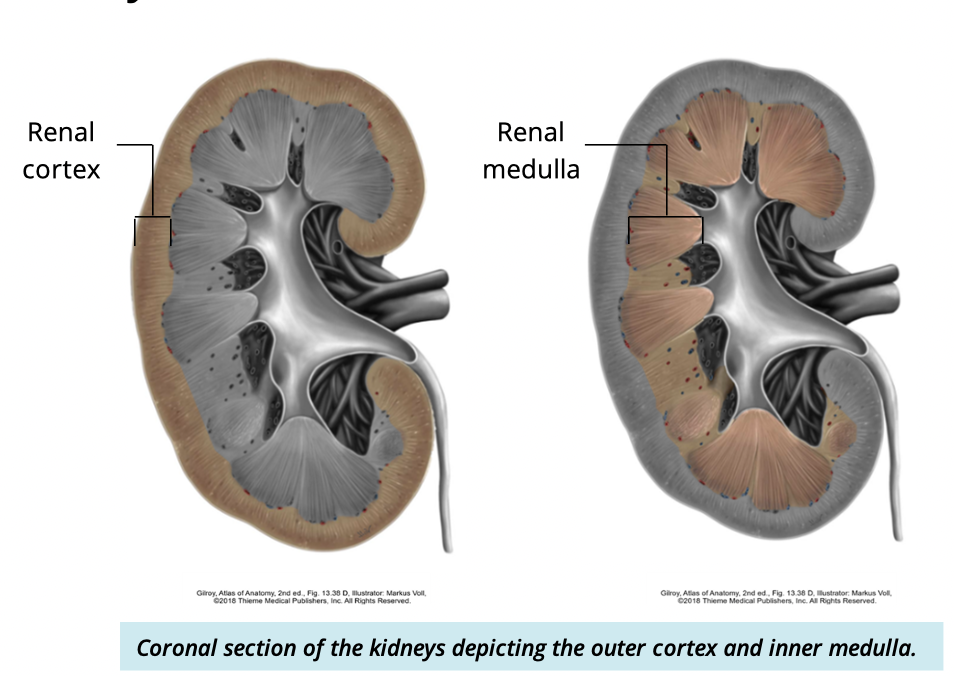
what is the function of the cortex and medulla
filter blood to make urine
what are renal columns?
extensions of the cortex that seperate renal pyramids
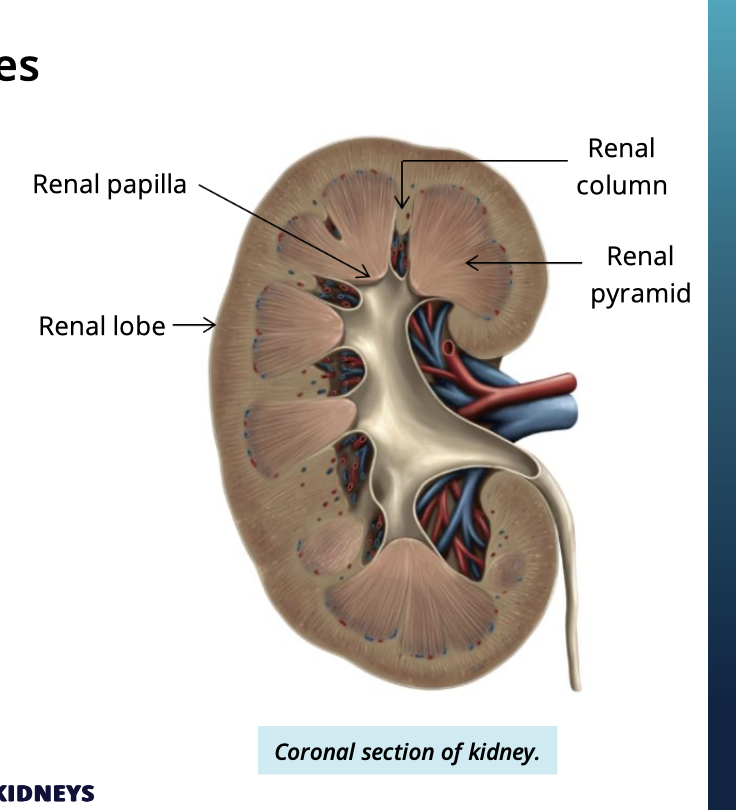
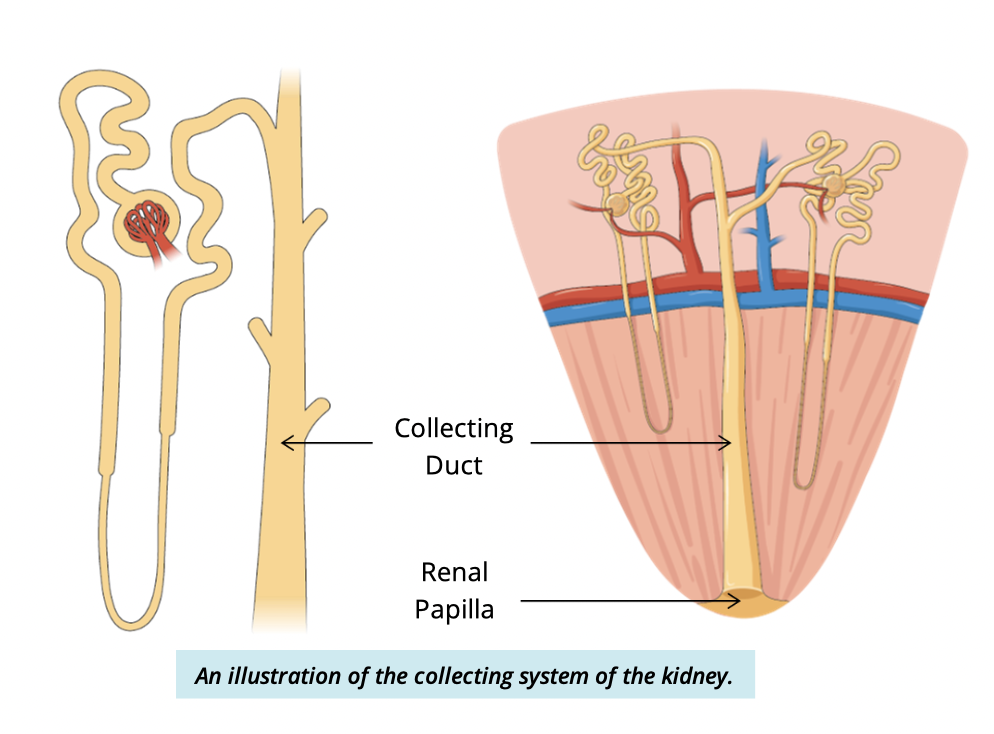
what is the renal papilla?
The apex (tip) of the renal pyramid
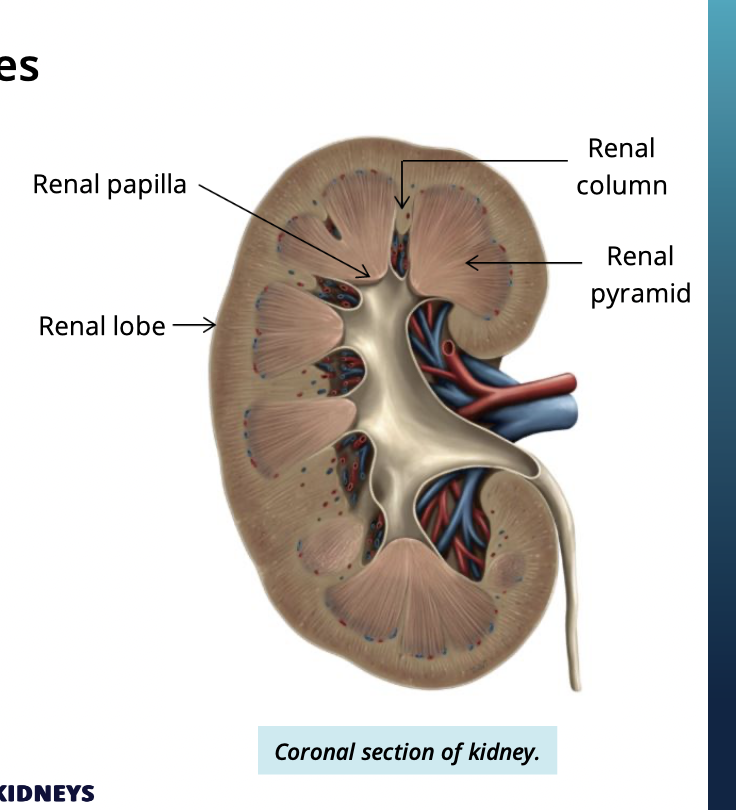
What makes up each renal lobe of the kidney? (3)
the kidney is divided into renal lobes.. each lobe has:
renal pyramid
overlying cortex
surrounding renal column
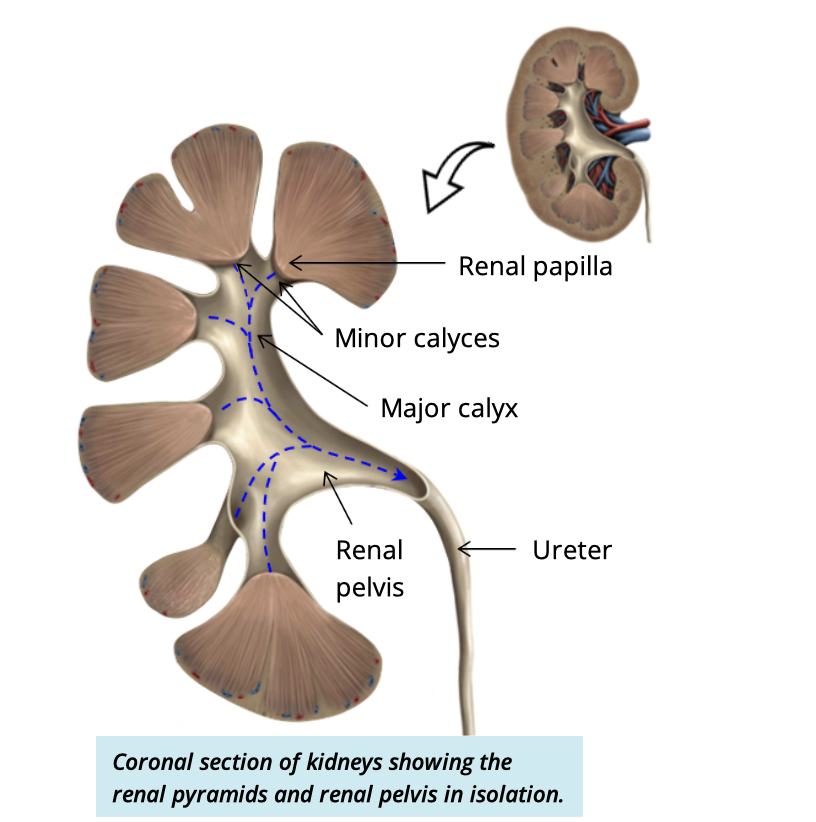
what ist he pathway of urine
kidney → renal papilla → minor calyx → major calyx → large renal pelvis → ureters
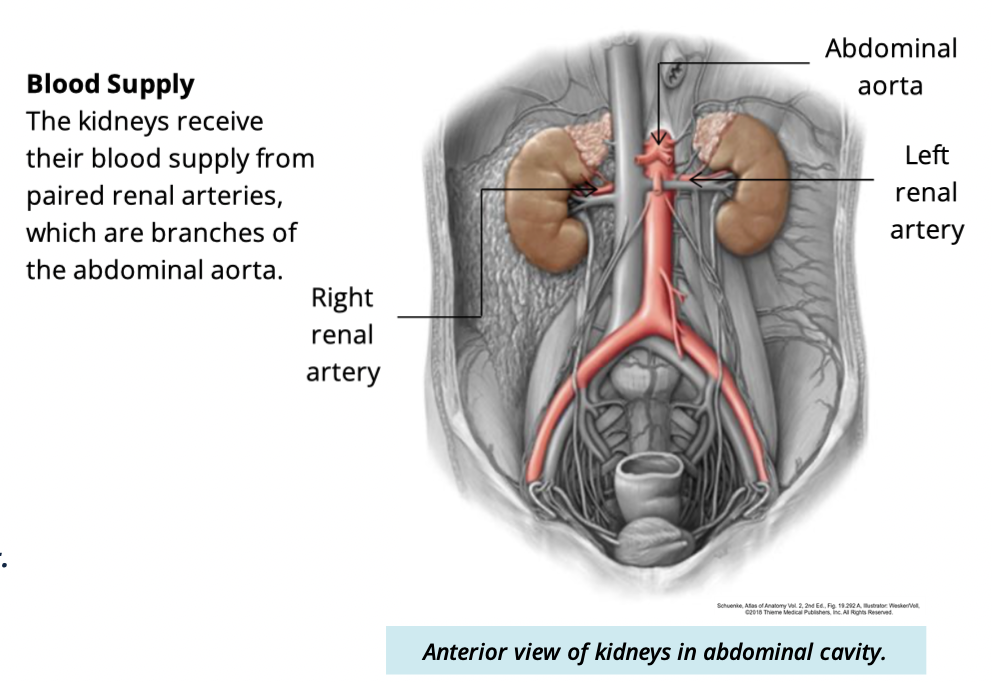
kidneys recieve their blood supply from what?
paired renal arteries
branches of the abdominal aorta
Kideys are drained by what?
Renal veins
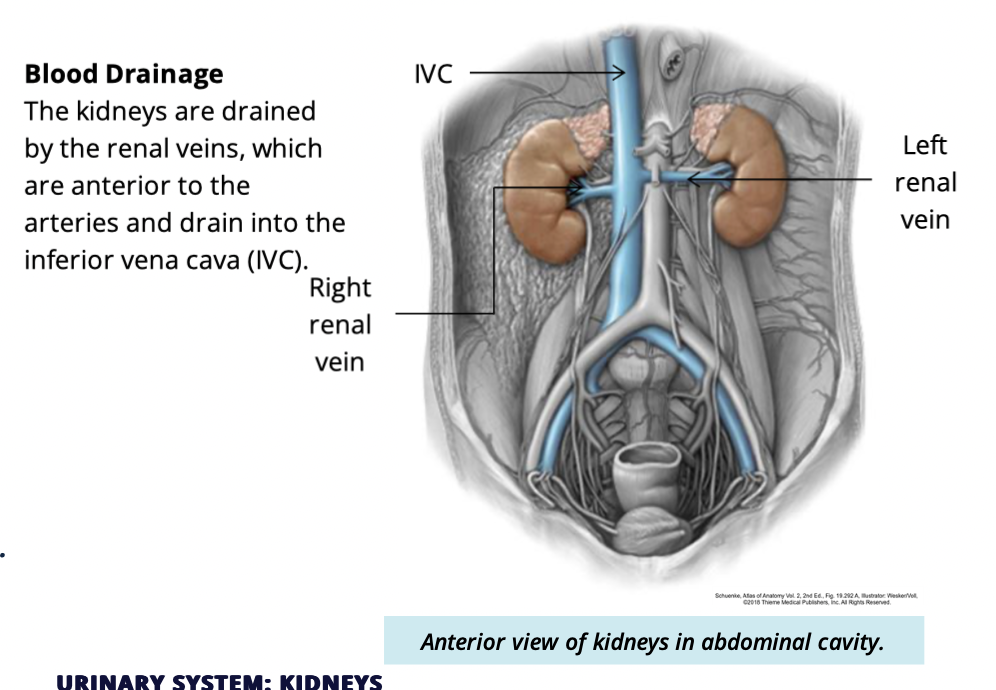
which renal artery is longer and why?
Right renal artery
bc descending aorta is on the left, so it must travel further to reach the right kidney
WHhich renal vein is longer and why?
Left renal vein
bc Inferior vena cava is on the right, so the left vein has to travel further
Relative positions of renal veins + arteries
renal vein is ANTERIOR to renal arteries
what ist he functionality unit of the kidney? what is its function
Nephrons (millions per kidney)
filters blood + produced urine
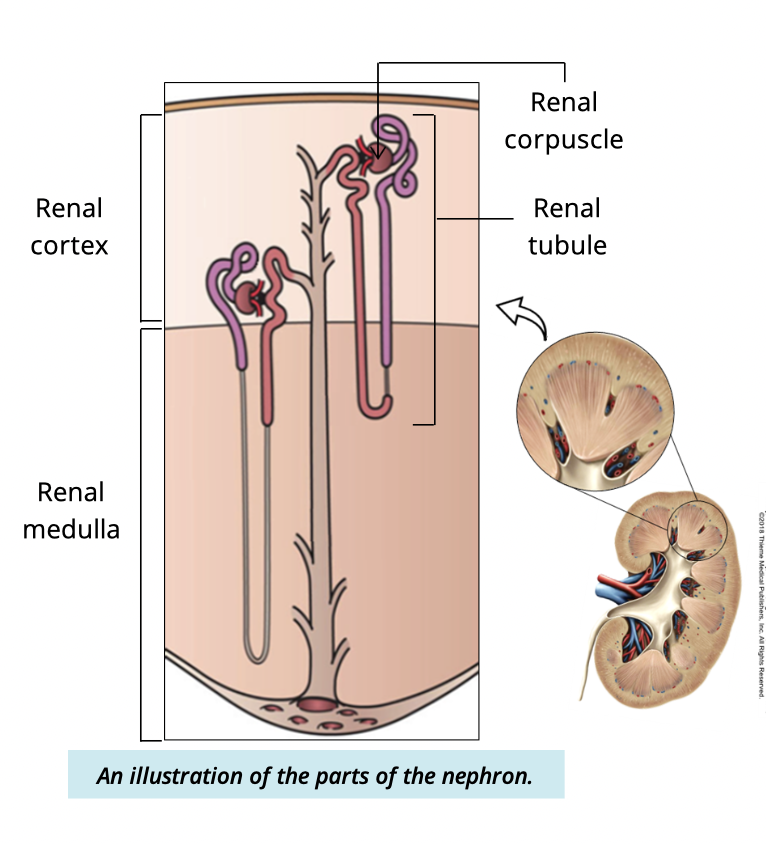
What are the two main parts of a nephron
renal corpuscle
renal tubule
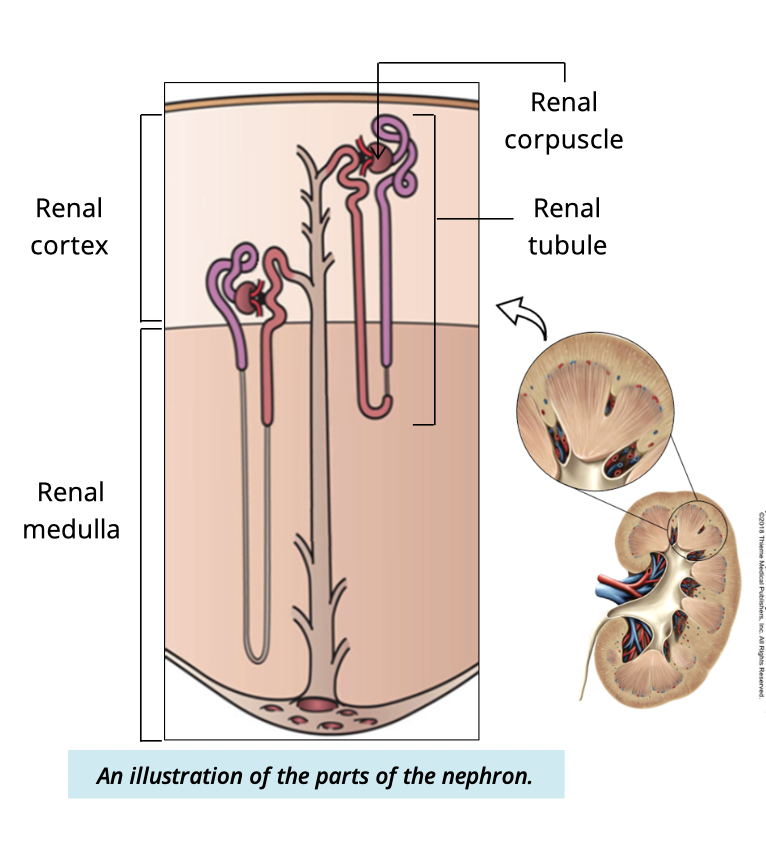
What two structures make up the renal corpuscle?
Glomerulus capsule
glomerular (Bowmans) capsule
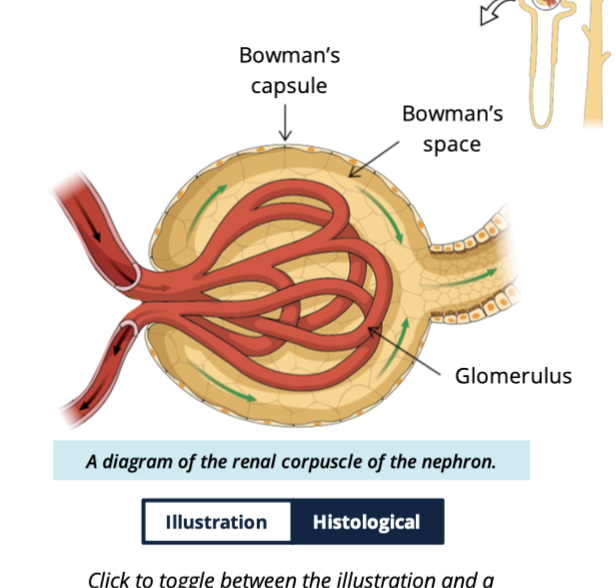
what does the glomerulus consist of?
bundles of capillaries
enclosed within the glomerular space
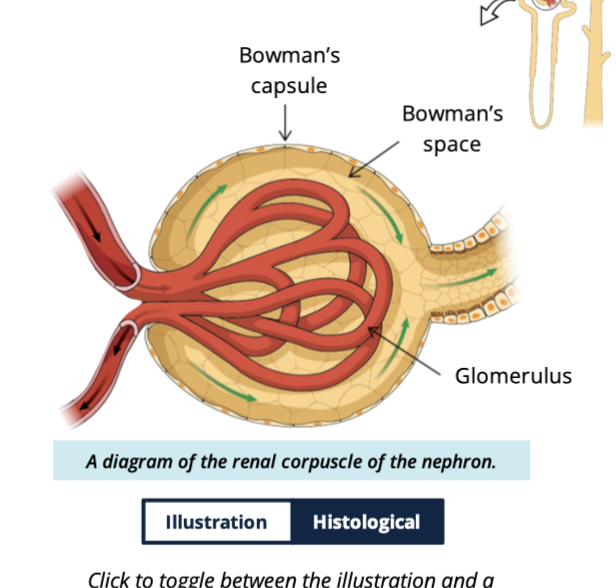
What is the capsular (Bowman’s) space?
Space between the glomerular capillaries and the capsule walls
how is filrate formed in the kidney?
Blood enters the glomerular capillaries → components of blood are filtered into bowmans space → this filtered fluid is called filtrate
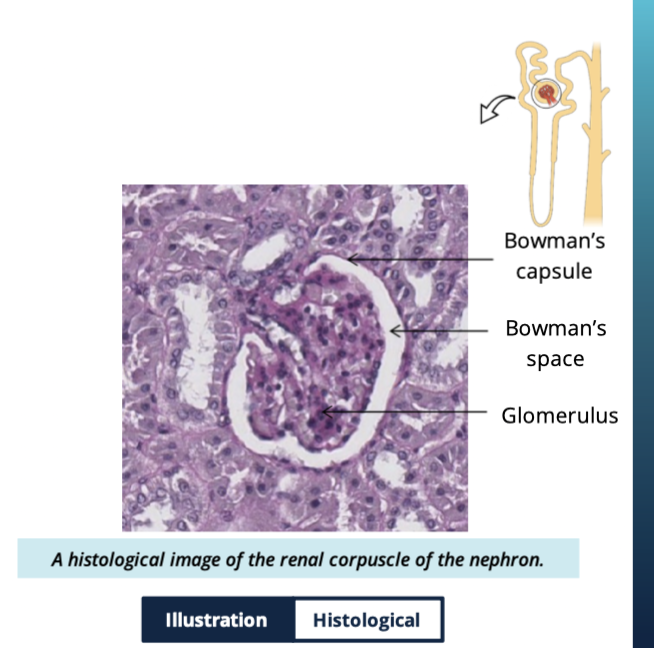
what feature of glomerular capillaries allows filtration?
Fenestrations (small holes) that let water, ion, and small molecules pass
What are podocytes?
specialized cells that wrap around glomerular capillaries, forming filtration slits
What do filtration slits do?
permit water and salts to pass while restricting proteins
What are the three sections of the renal tube?
Proximal convoluted tubule → loop of henle —> distal convoluted tubule
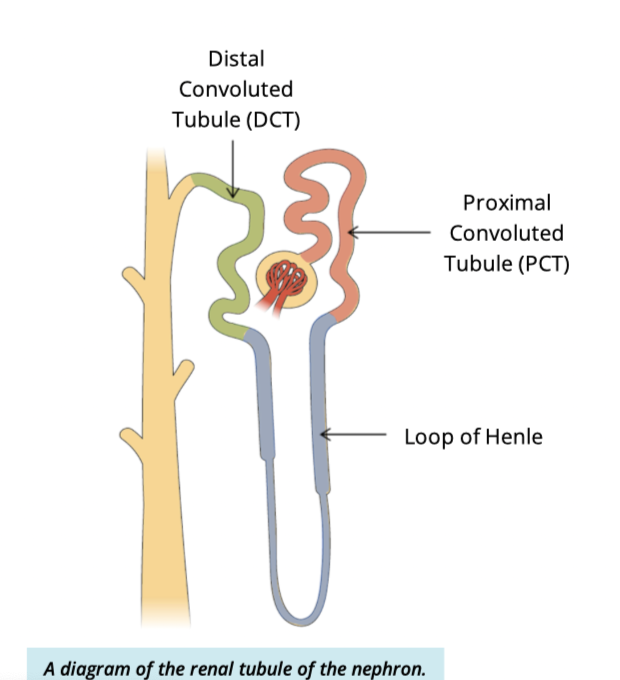
What is the main function of the renal tubule?
reabsorption + secretion of ions, water, and other substances to modify filtrate
Where does filtrate go after the renal tubules?
Into collecting tubules →
collecting ducts in the renal medulla
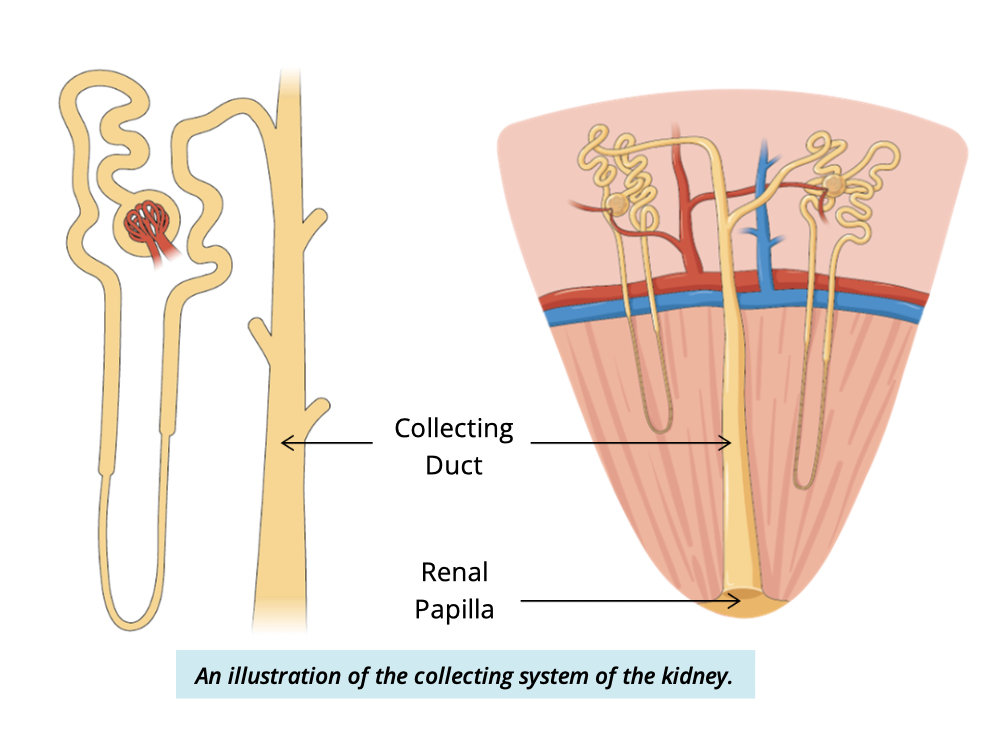
What happens in the collecting ducts?
Final processing/modification of filtrate occurs
When does filtrate become urine?
Once it leaves the collecting duct at the renal papilla
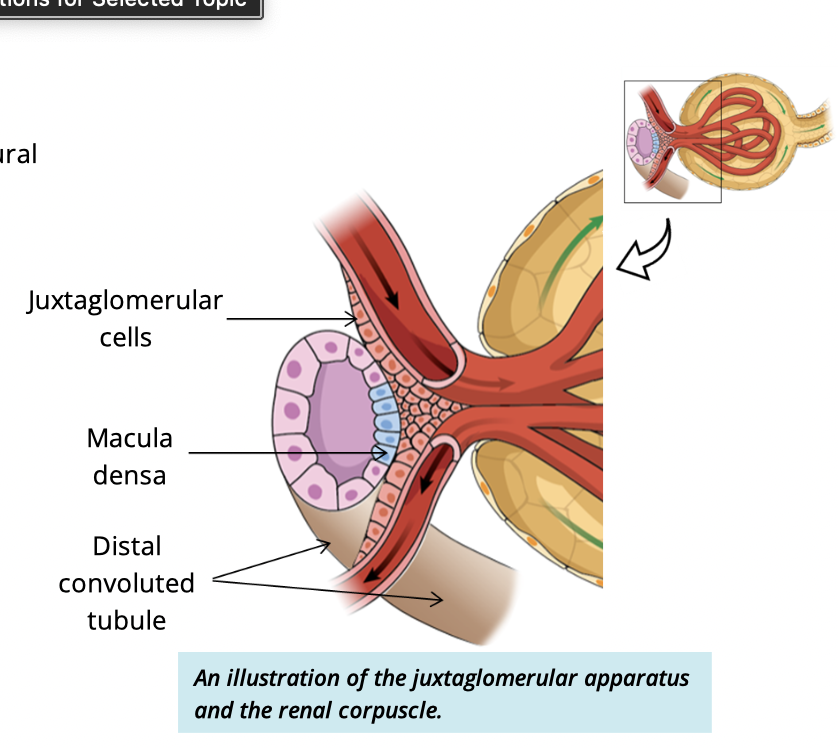
What is the function of the juxtaglomerular apparatus (JGA)?
Regulates blood pressure by monitoring ion concentrations in the filtrate
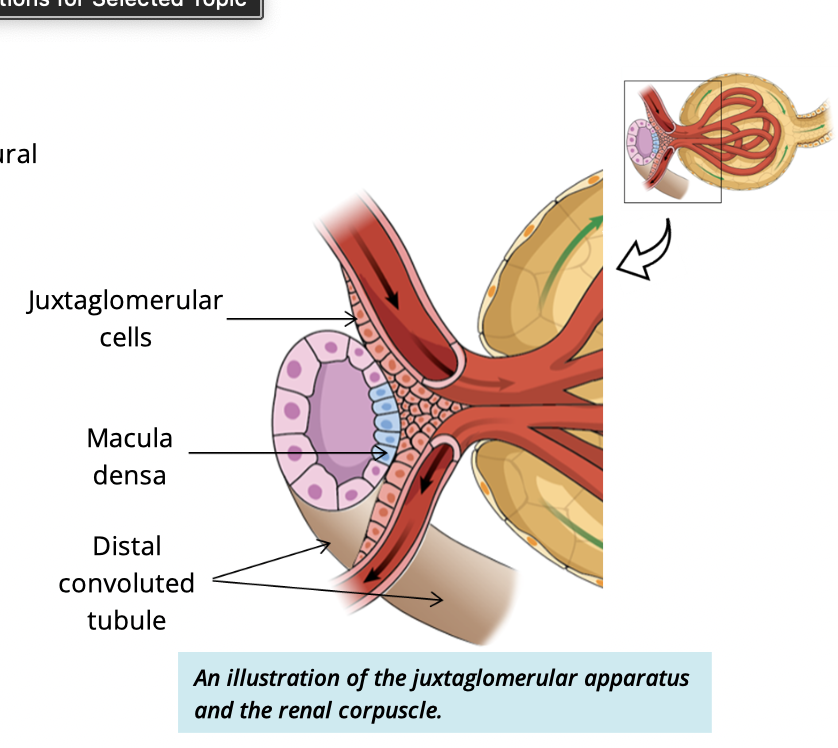
What are juxtaglomerular cells?
Modified smooth muscle cells of the afferent arteriole
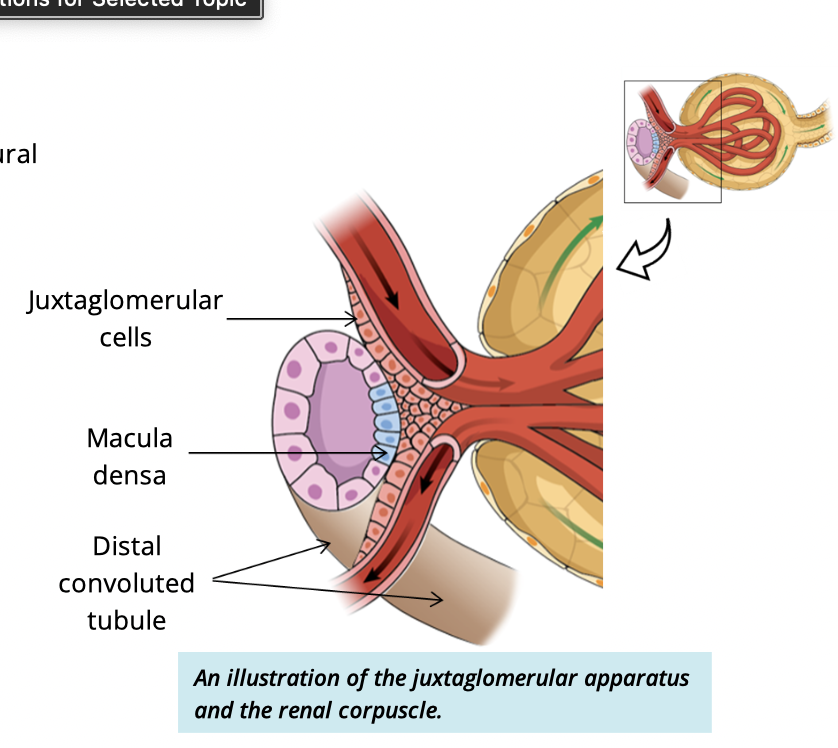
What is the macula densa?
Modified cuboidal cells of the distal convoluted tubule
Function of the urinary tract
transfers + stores the urine produced by the kidneys until its ready for excretion
3 parts of the urinary tract
ureters
bladder
urethra
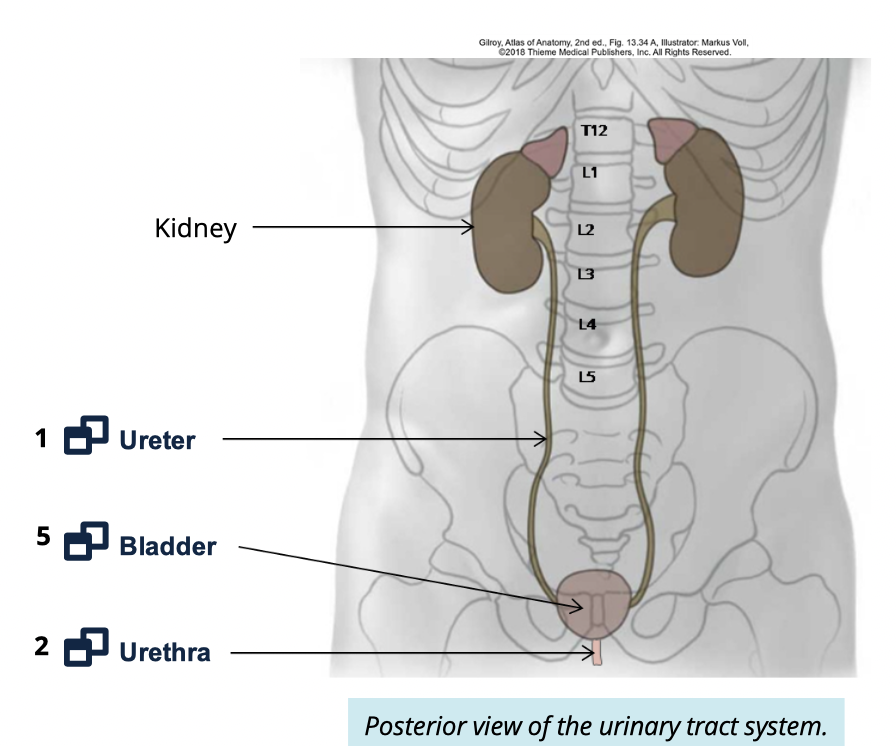
Describe the ureters (4)
2 long, thin, muscular tubes
connects kidney w/ bladder
begin as a contuation of the renal pelvix
extends toward pelvic cavity where they penetrate the posterior wall of the bladder
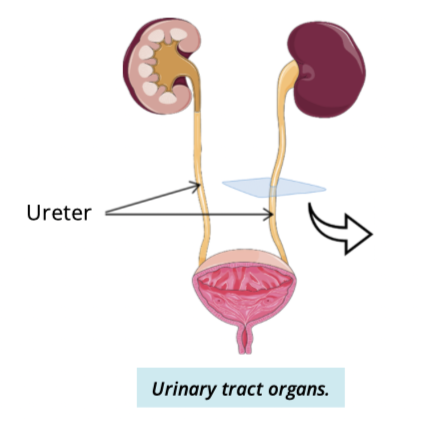
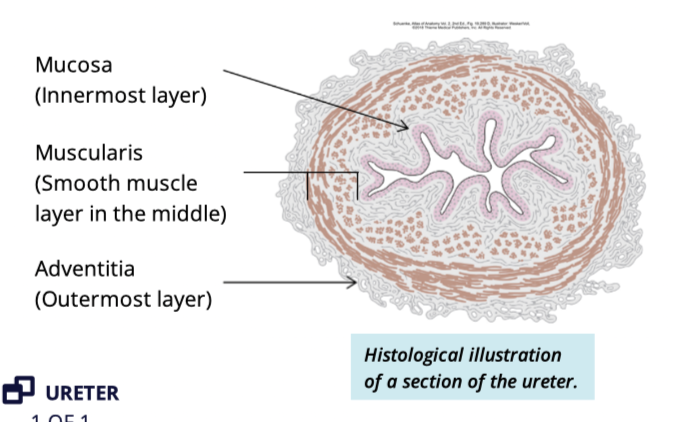
Describe the histological layers of the ureter
adventitia
muscularis
smooth muscle
mucosa
transitional epithelium
What is the function of the urinary bladder?
Temporarily stores urine
What is the trigone of the bladder
A smooth triangular area at the base of the bladder
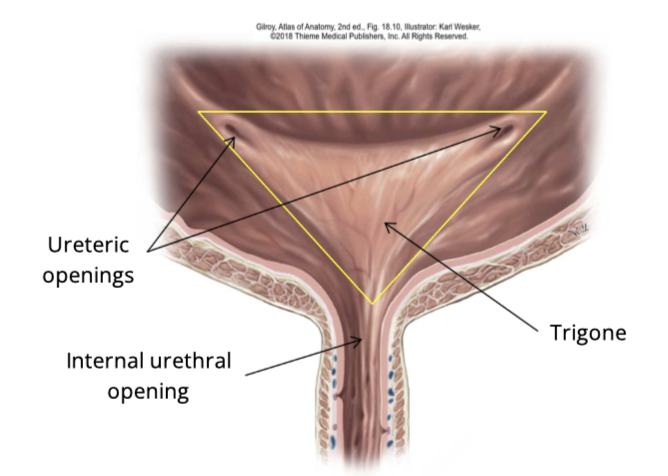
What structures define the trigone?
Two ureter openings (superior)
internal urethral opening (inferior)
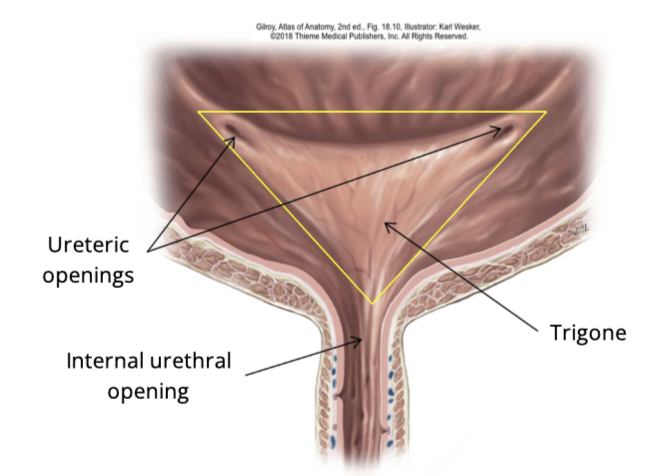
what is the function of the trigone?
Funnels urine into the urethra + signals urge to void
Describe the neck of the urinary bladder
constricted portion
connected to the urethra inferiorly
surrounded by an internal urethral sphincter
made up of smooth muscle
involuntary control
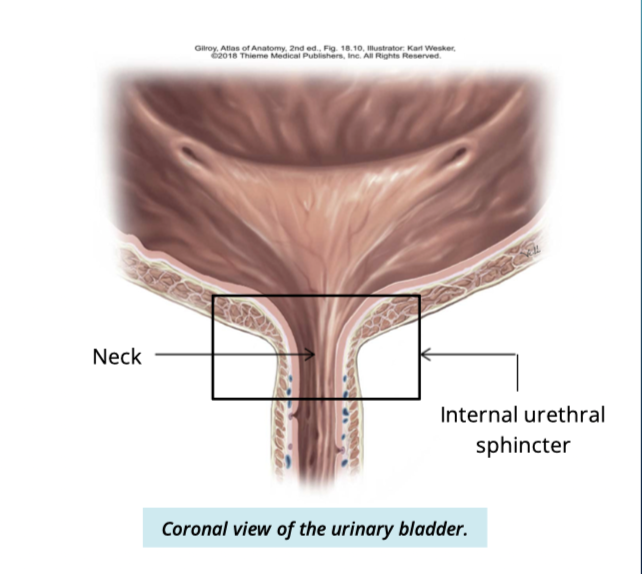
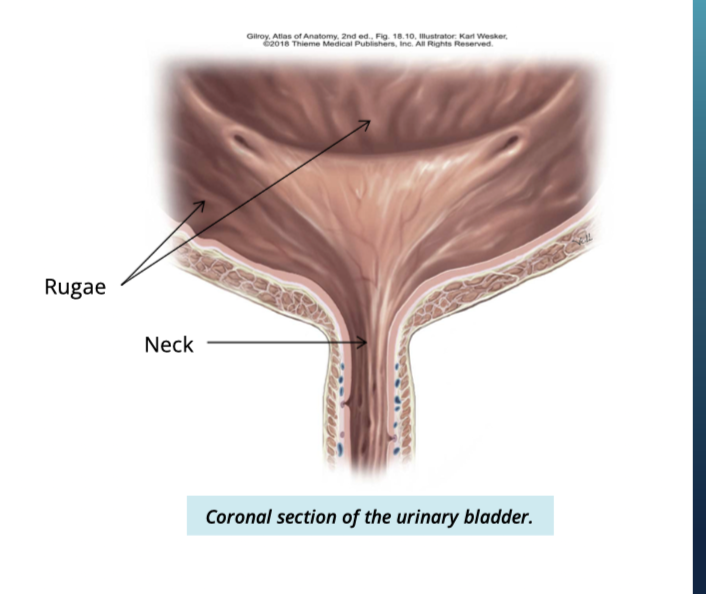
Describe the interior of the bladder
Rugae → folded appearance
allows bladder to expand
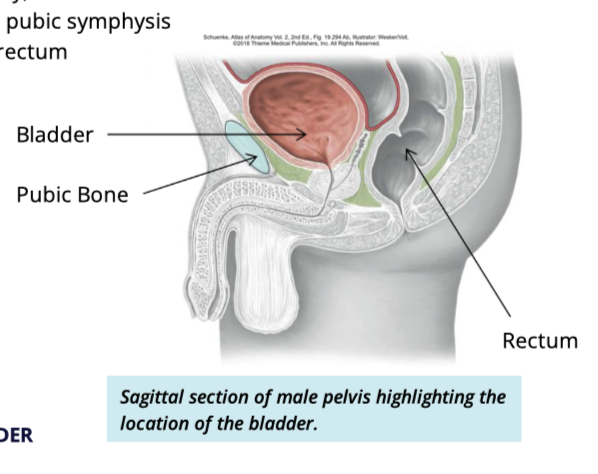
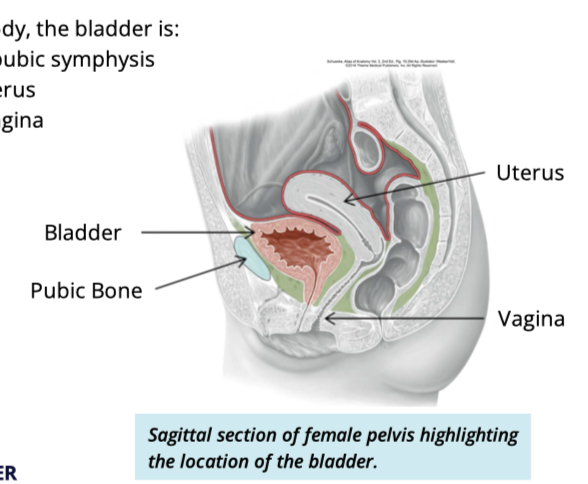
Bladder location in females
posterior to pubic symphysis
inferior to uterus
anterior to vagina
Bladder location in males
posterior to pubic symphysis
anterior to rectum