ID: ch 17 and 18, fri 13th class
1/29
Earn XP
Description and Tags
going through audio recorded lecture - all done
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
30 Terms
Six ways to avoid being killed by phagocytes
Talks and release, opsonization prevented (e.g. protein produced, which prevents interaction between opsonizing antibody and phagocyte), contact with phagocyte prevented (e.g. through a capsule), phagolysosome fusion inhibited (eg TB YUHH), escape into the cytoplasm (from the phagolysosome), resistance to killing (eg by producing antioxidants)
example of viral pathogen that evades TLR based innate defense & how they do it
Herpes - avoids ICP0 which tags immune proteins for degradation via the proteasome (tags them with ubiquitin), destroys IFN pathways - curbs virus response
example of bacterial pathogen that evades adaptive defense & some more details on the pathogen
salmonella - gram-, 2% of patients die, foodborne infection, bacteria hides in gallbladder with biofilm formation
strategies to evade adaptive defenses (4)
hiding places, mimicry, antigenic variation, immune interference
strategies to evade adaptive defenses: hiding places (2 + 1)
cyst: worm cyst in liver eg, or cytoplasm cyst by listeria monocytogenes
host genome: eg retroviral DNA integration
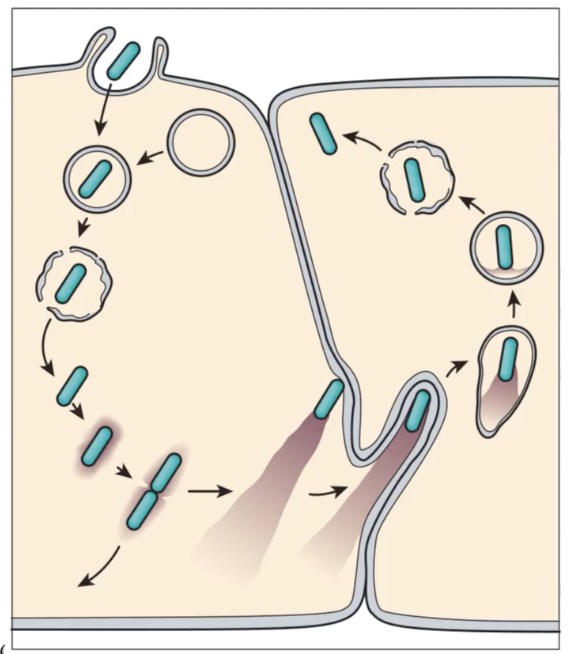
what is this image showing
cytoplasm as hiding place, cell to cell spread
strategies to evade adaptive defenses: mimicry more detail, 1 eg
not very effective, of host proteins, eg TB, risk of cross-reacting antibodies for host (eg step throat)
strategies to evade adaptive defenses: antigenic variation I example
influenza virus: genome has 8 ss RNA segments (separated), has 2 predominant surface proteins (haemaglutinin- attaches to sugars that project from the airway epithelium; Neuraminidase- cleaves bond between haemaglutinin and sialic acid (viral release));
4 types of influenza - A most relevant for humans and clinitiancs, and then H and N have diff variants; also can be low and high pathogenic avian influenza
most scary influenza variant rn
H5N1 avian flu (HPAI)
what organ system does influenza attack in birds vs mammals
mammals: respitatory tract
birds: gastrointestinal tract
antigenic shift vs antigenic drift
antigenic shift is a sudden major change, antigenic drift is a gradual process (usually a single mutation)
reasons for differences in death rate in avian flue SE asia vs US? (4)
surveillance bias (mild cases detected), different virus strains, different exposure intensity, earlier treatment
why does the H5N1 virus spread easily among birds but not humans?
H5 - binds to alpha 2,3linkage between sialic acid and galactose - deep in lungs, more deadly, spreads more difficult
H1 - eg seasonal virus, binds to alpha2,6 linkage - in upper respirator tract - much less fatal but easier spread
worries with H5N1 avaian virus
antigenic drift: and bind to 2,6 sialic acid-galactose
antigenic shift: mix of deadly avian virus and easily spreadable human virus- coinfection in one host and reassortment
what happens w/ influenza coinfection
the diff ss DNA strands - reassort and mix different fragments together, reassortment, sudden major change in properties
strategies to evade adaptive defenses: antigenic variation II descr.
gene switching, eg coat switching in parasite that causes sleeping sickness, through variant surface glycoproteins (VSG)
strategies to evade adaptive defenses: antigenic variation III descr.. eg
gene conversion, eg gonorrhoeae - their pili can change their shape - silent copy recombinded with expressed copy, changes it
strategies to evade adaptive defenses: immune interference I
Th1/Th2 balance - Th1 promote macrophages to become M1 (warmongers), Th2 promote macrophages to become M2 (peacekeepers)
strategies to evade adaptive defenses: immune interference II
suppression, eg HIV
strategies to evade adaptive defenses: immune interference III
modulators like superantigens (Sag) - forces MHCII and TCR apart - no recognition of antigen but huge stimulation of T cells, bind outside the conventional antigen-binding site
results of Sag
uncoordinated/ineffective immune response (20% vs 0.01%), cytokine storm, toxic shock syndrome, overwhelming inflammatory response
pathogen related to toxic shock syndrome
staphylococcus aureus - common if you have tampons in for too long, gram+ cocci
immune sensing in (intestinal) epithelia (4)
toll-like receptors, PRR in cytoplasm: cytosolic nucleotide binding domain and leucine rich repeat containing receptors (assemble inflammosomes- danger sensing proteins), nucelic acid receptors (eg RIG-I), can sense PAMPs and DAMPs
imflammosome more in depth
danger-sensing proteins, detect when cells become infected or damaged, become activated and bind tgt forming inflammosomes, cleave active proteins into their dormant form - dormanr forms can then create pores in cells - pyroptosis
how does toxic shock syndrome happen
outside-in signaling mechanism, cell lysis by alpha toxn, epithelium dissolves, cell death by pyroptosos
strategies to evade adaptive defenses: immune interference IV
persistent infections, latent to patent (eg TB!!)
pathology of infectious diseases (6)
endotoxin (pathogen antigens), exotoxin (released agent), inflammation, immune response, allergies, oncogenesis
endotoxin descr
fingerprint structural molecules of the pathogens, powerful activators of immune and inflammatory responses
4 hypersensitivities
IgE mediated: allergic/anaphylactic shock, IgG mediated cytoytoxic - autoimmune disease, Ab against skin, immune-complex mediated - inflammation around blood vessels, cell mediated eg nicket hypersensitivity - landerhans cells cause T cell inflammation
cancer and ID
6 possible ID, usually viruses, eg HPV - causes papilloma virus, vaccine greatly helps!!