Fundamentals Exam #3
1/173
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
174 Terms
What are the four principles of pharmacokinetics?
Absorption, distribution, metabolism, and excretion.
How does blood flow affect medication absorption?
Greater blood supply at the site of administration leads to faster absorption.
Why is sublingual medication absorption rapid?
Due to the high density of blood vessels located under the tongue.
How does body surface area influence absorption?
A larger surface area allows for faster absorption.
What is the primary factor that allows medications to pass the blood-brain barrier?
Lipid solubility.
What is the primary site of medication metabolism in the body?
The liver.
What is the process of biotransformation?
The use of enzymes to detoxify, break down, and remove active chemicals from medications.
What is the primary organ responsible for medication excretion?
The kidneys.
What is a therapeutic effect?
The expected or predicted physiological response to a medication.
How does an adverse effect differ from a side effect?
An adverse effect is unintended and undesirable, whereas a side effect is a predictable and unavoidable secondary response.
What is an idiosyncratic reaction?
An unpredictable response where a patient overreacts, underreacts, or has a reaction different from the norm.
What is a synergistic drug interaction?
An interaction where the combined effect of two medications is greater than the effect of either given separately.
Define polypharmacy.
The use of five or more medications at home, often involving multiple doctors and increasing the risk of adverse drug events.
Who is most at risk for polypharmacy?
Older adults, due to multiple disease processes.
Can a nurse delegate medication administration to assistive personnel?
No.
What is the nurse's role as the 'last line of defense' in medication administration?
To verify that orders are correct and safe before administering, as the nurse is responsible for errors even if the provider prescribed it.
List the required components of a complete medication order.
Patient's full name, date/time of order, medication name, dosage, route, frequency, and provider signature.
What is a medication error?
Any avoidable event that could result in incorrect medication use or patient injury.
What is the first action a nurse should take if a medication error occurs?
Assess the client's condition.
What should a nurse do after a medication error is identified and the patient is assessed?
Report the error, even if no harm occurred.
How does protein binding affect medication distribution?
Medications bound to serum proteins like albumin are typically not pharmacologically active.
Why might a provider decrease a medication dose for a patient with renal impairment?
Because the kidneys are unable to adequately excrete the medication, leading to potential toxicity.
What is a toxic effect?
A response caused by the accumulation of medication in the bloodstream.
What is one common factor that contributes to medication errors in a clinical setting?
Interruptions during the preparation or administration process.
What are the rights of medication administration?
Right medication, right dose, right client, right route, right time, right indication, and right documentation.
What does the TACTIS acronym stand for in medication assessment?
Therapeutic effect, Action, Contraindications, Toxic effects, Interventions, and Safe dose.
What are the three checks for medication administration?
1. Compare stock to EMAR at the supply source, 2. Compare to EMAR after entering the client's room, 3. Compare medication labels to EMAR at the bedside while scanning.
When should medication reconciliation be performed?
At admission, transitions of care, and discharge.
What are the three main categories of medication administration routes?
Enteral, parenteral, and topical.
What factors influence a provider's choice of medication route? (6)
Client condition, adherence, medication attributes, location of desired effect, speed of response, and dosage accuracy.
What are the advantages of the oral (enteral) route?
It is the safest, most convenient, and most preferred by patients for self-administration.
What safety steps are required when administering medication via an NG or PEG tube?
Use liquids when possible, crush pills and mix with warm water, and flush tubing before, between, and after administration.
What are the primary complications associated with tube medication administration?
Clogged tubing and misconnected tubing.
What safety precaution must be taken before applying a new transdermal patch?
Ask the patient if they have an existing patch and wear clean gloves.
How should transdermal patch application be documented?
Document the location on the EMAR and on the patch itself.
What are the safety rules for ophthalmic medication instillation?
Avoid the cornea, do not touch the eye or eyelid with the dropper, use only on the affected eye, and never share medications.
What must be checked before administering otic (ear) drops?
Check with the provider for eardrum rupture if the patient has ear drainage.
What temperature should otic drops be when administered?
Room temperature.
What risk is associated with the overuse of nasal decongestant sprays?
The rebound effect.
How are intravaginal suppositories versus foams/creams typically administered?
Suppositories are inserted with a gloved hand, while foams, jellies, and creams are administered with an applicator.
Why are rectal suppositories shaped with a rounded end?
To prevent anal trauma during insertion.
What preparation might be required before inserting a rectal suppository?
A small cleansing enema.
What is the primary purpose of inhaled medications?
To treat respiratory conditions by delivering small droplets to the lungs via the trachea.
What are the four types of parenteral medication administration?
Intradermal (ID), subcutaneous, intramuscular (IM), and intravenous (IV).
Why is parenteral administration considered a high-risk procedure?
It is invasive, requires aseptic technique, and carries a risk of infection.
How does the speed of action for parenteral routes compare to other routes?
Effects develop rapidly, depending on the specific parenteral route used.
Which syringe size is typically used for IV medications?
5mL syringe
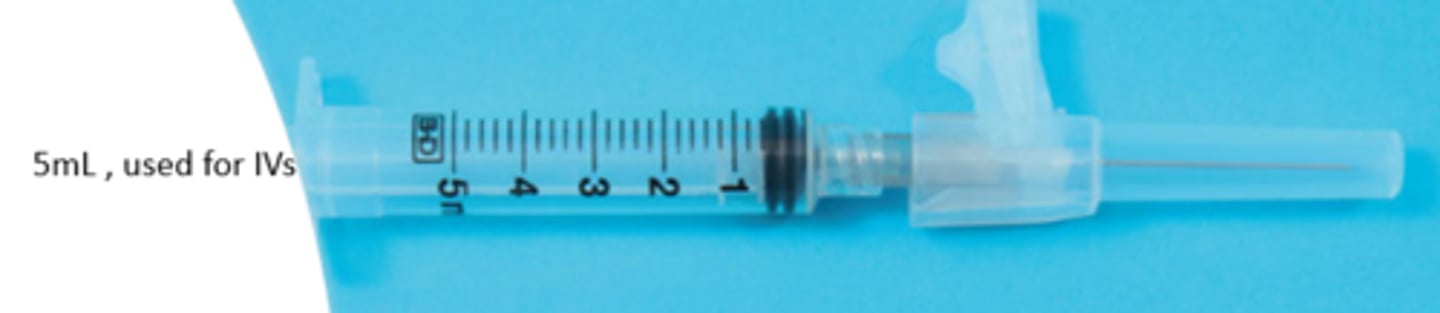
Which syringe size is typically used for intramuscular (IM) injections?
3mL syringe

What type of syringe is used for intradermal (ID) injections like TB tests?
1mL Tuberculin syringe
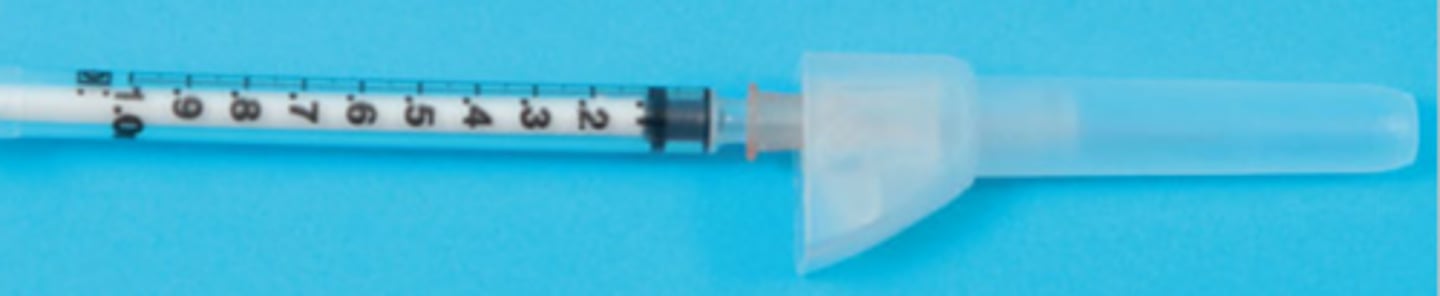
What type of syringe is used for subcutaneous injections into fat tissue?
Insulin syringe
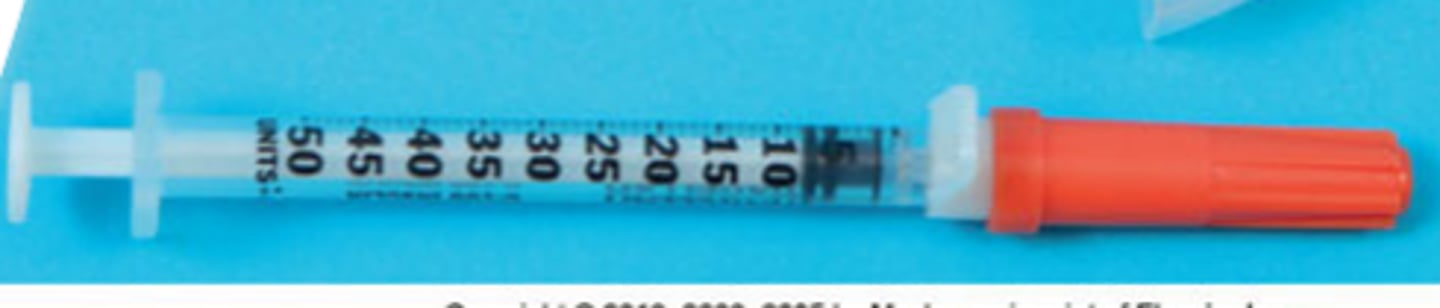
What is an ampule?
A single-dose glass container of medication in liquid form
How do you draw medication from a vial?
Inject an equal amount of air into the vial to maintain a closed system before drawing the medication
What is the primary safety rule for handling used needles?
Engage the safety mechanism and place the needle directly into a sharps container
What is the angle of insertion for an intradermal injection?
5 to 10 degrees with the bevel facing up
What visual indicator confirms a successful intradermal injection?
The formation of a small bleb under the skin
Where is medication placed during a subcutaneous injection?
In the loose connective (adipose) tissue under the dermis
What is the typical angle of insertion for a subcutaneous injection?
Between 45 and 90 degrees, depending on the patient's adipose tissue
How does the absorption rate of IM injections compare to subcutaneous injections?
IM injections have a faster absorption rate
What is the standard angle of insertion for an intramuscular injection?
90 degrees
What factors determine the choice of an IM injection site?
The amount of medication being administered and the size of the muscle
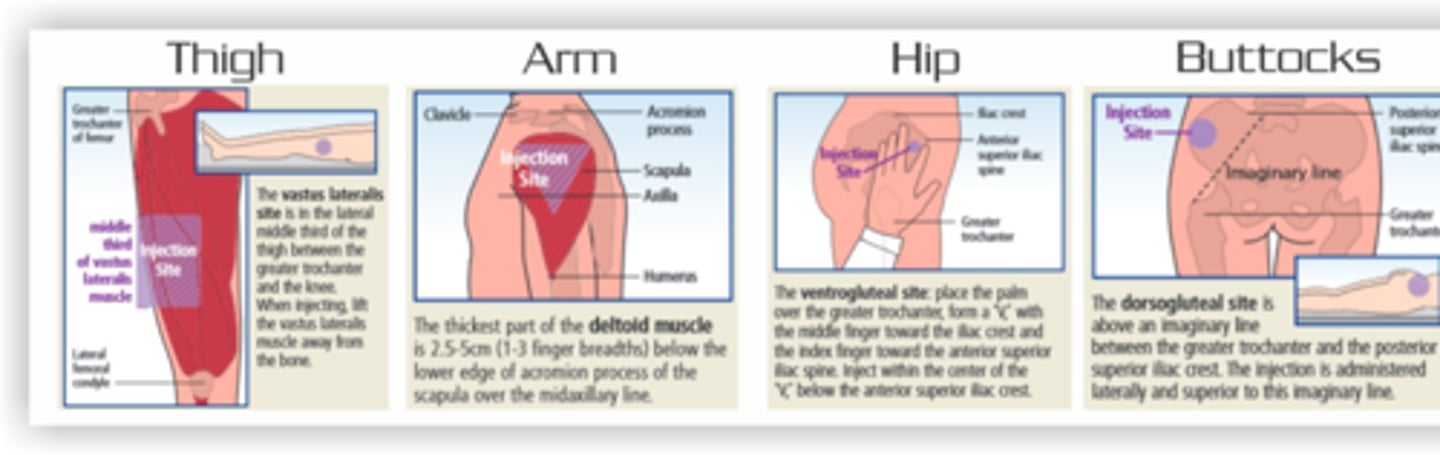
List four common sites for intramuscular injections.
Vastus lateralis, deltoid, ventrogluteal, and dorsogluteal sites
What is the primary advantage of the IV route for medication administration?
Medications are absorbed quickly into the bloodstream
What is an IV piggyback?
A medication administered alongside continuous IV fluids
What five key areas must a nurse educate a patient on regarding their medication?
Medication effect, indication, side effects, actions to take, and teach-back
Why is it important to assess the muscle before an IM injection?
To ensure proper site identification and verify that the injection is justified
How should you adjust the angle of a subcutaneous injection for a very lean patient?
Use a 45-degree angle to avoid hitting the muscle
What stimulates the active process of inspiration?
Chemoreceptors in the aorta that detect CO2 levels.
What physical change occurs in the thoracic cavity during inspiration?
The diaphragm moves down, creating negative pressure and increasing the size of the thoracic cavity.
What property of the lung makes expiration a passive process?
The elastic recoil properties of the lung.
Define ventilation.
The process of moving gases in and out of the lungs and alveoli.
Define diffusion in the context of respiration.
The movement of respiratory gases through concentration gradients from one area to another.
Define perfusion.
The cardiovascular system's ability to pump oxygenated blood to tissues and return deoxygenated blood to the heart.
What are common objective signs of respiratory diseases like COPD or asthma?
Increased respiratory rate, decreased O2 saturation, and adventitious lung sounds.
What is the function of surfactant in the alveoli?
It keeps the alveoli open and prevents atelectasis (collapse).
What is the consequence of low lung compliance?
Increased airway resistance, increased use of accessory muscles, and higher energy expenditure.
How does increased work of breathing affect metabolic rate?
It increases the metabolic rate, creating a higher demand for oxygen.
What is lung compliance?
The ability of the lungs to distend or expand.
How does increased thickness of the alveolar membrane affect gas exchange?
It impedes diffusion, slowing down the transfer of gases across the membrane.
Name three conditions that can increase alveolar membrane thickness.
Pulmonary edema, pneumonia, and COPD.
Which part of the brain controls the rate, depth, and rhythm of respiration?
The brain stem.
Why can spinal cord injuries inhibit breathing?
Because the brain stem uses the spinal cord to transmit signals for respiratory control.
What is the primary role of coronary artery circulation?
To supply oxygenated blood to the heart muscle itself and remove waste.
What occurs during cardiac diastole?
The heart rests, and the mitral and tricuspid valves permit blood flow into the relaxed ventricles.
What causes the S1 heart sound?
The closing of the AV (mitral and tricuspid) valves during systole.
What causes the S2 heart sound?
The closing of the semilunar valves.
What are the three main components of respiratory gas exchange?
Ventilation, diffusion, and perfusion.
What happens to the thoracic cavity during expiration?
The diaphragm recoils upward, and the thoracic cavity decreases in size.
What factors determine normal lung volumes?
Age, gender, and height.
What is the definition of cardiac output?
The amount of blood ejected from the left ventricle every minute.
What is the formula for calculating cardiac output?
Cardiac Output = Stroke Volume x Heart Rate
Define preload.
The amount of blood in the left ventricle at the end of diastole, representing the pressure in the ventricle before contraction.
What condition causes decreased preload?
Hypovolemia, due to insufficient volume to stretch the ventricle.
Define afterload.
The resistance to the ejection of blood from the ventricle that must be overcome for blood to enter systemic circulation.
What condition causes increased afterload?
High blood pressure, as the heart must work harder to overcome greater resistance.
What is cardiac contractility?
The ability of the heart to squeeze blood out of the ventricles.
What is the primary pacemaker of the heart?
The SA node.
What does the P wave represent on an ECG?
Atrial depolarization (atria contracting).
What does the QRS complex represent on an ECG?
Ventricular depolarization (ventricles contracting) and atrial repolarization (atria relaxing).
What does the T wave represent on an ECG?
Ventricular repolarization.