Week 12: Dental Implants
1/42
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
43 Terms
What is a dental implant?
a nonbiologic device surgically inserted into the jawbone
What are the parts of a dental implant?
crown, abutment, implant fixture/body
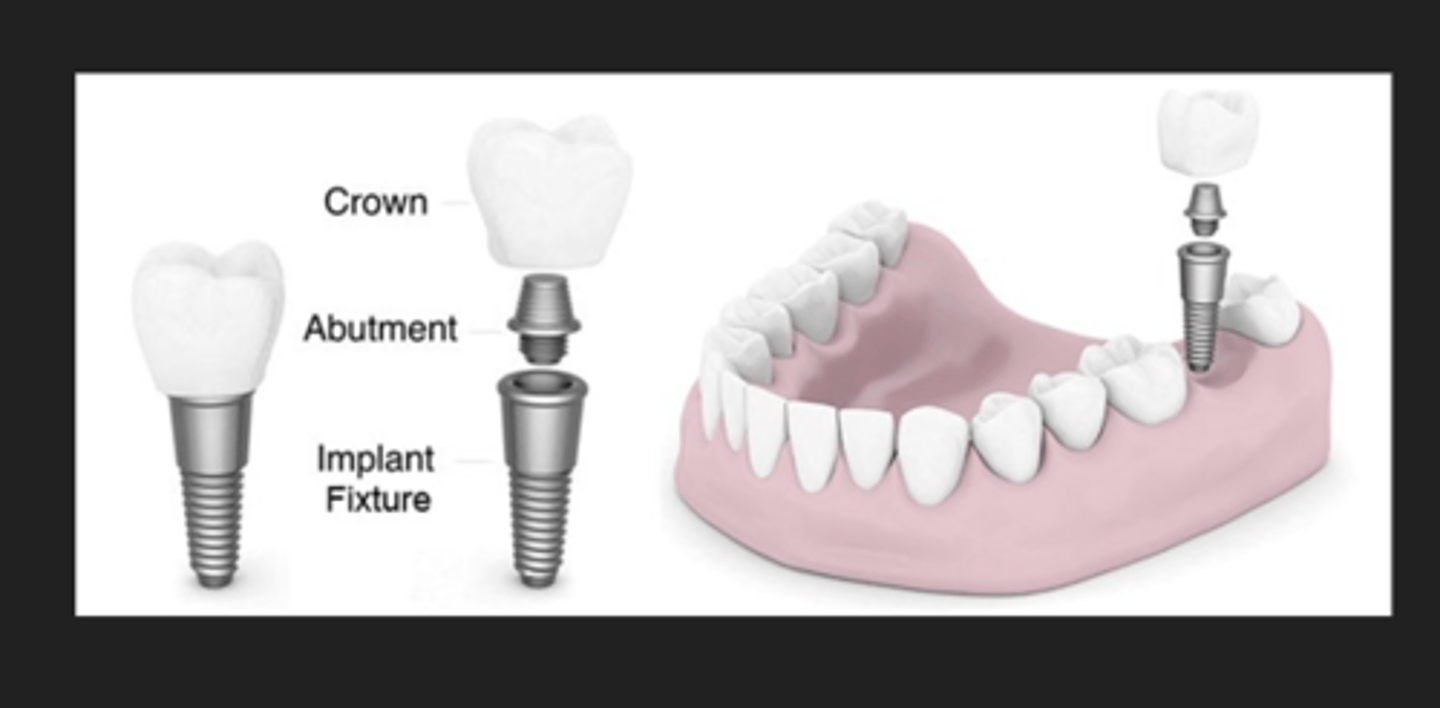
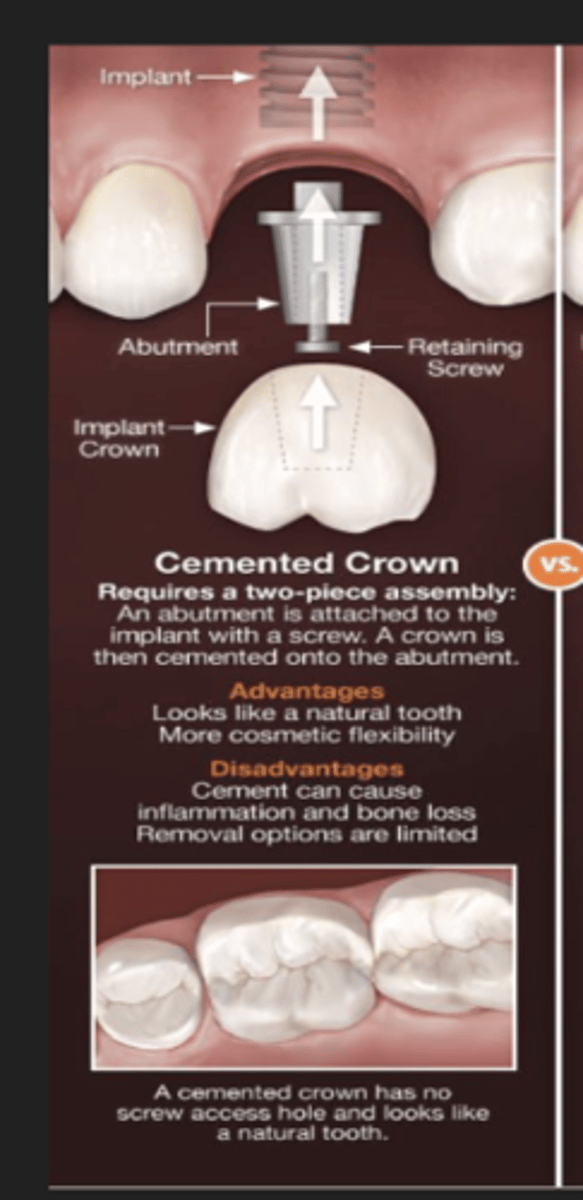
Describe a cement retained implant
screw in abutment to connect to body, the crown is cemented to the abutment
usually anterior teeth
Describe a screw retained implant
crown and abutment are fixed together, the screw goes all the way thru the crown, abutment, and body
usually posterior teeth

What are the parts of a screw retained implant?
body, abutment, prosthesis, and screw
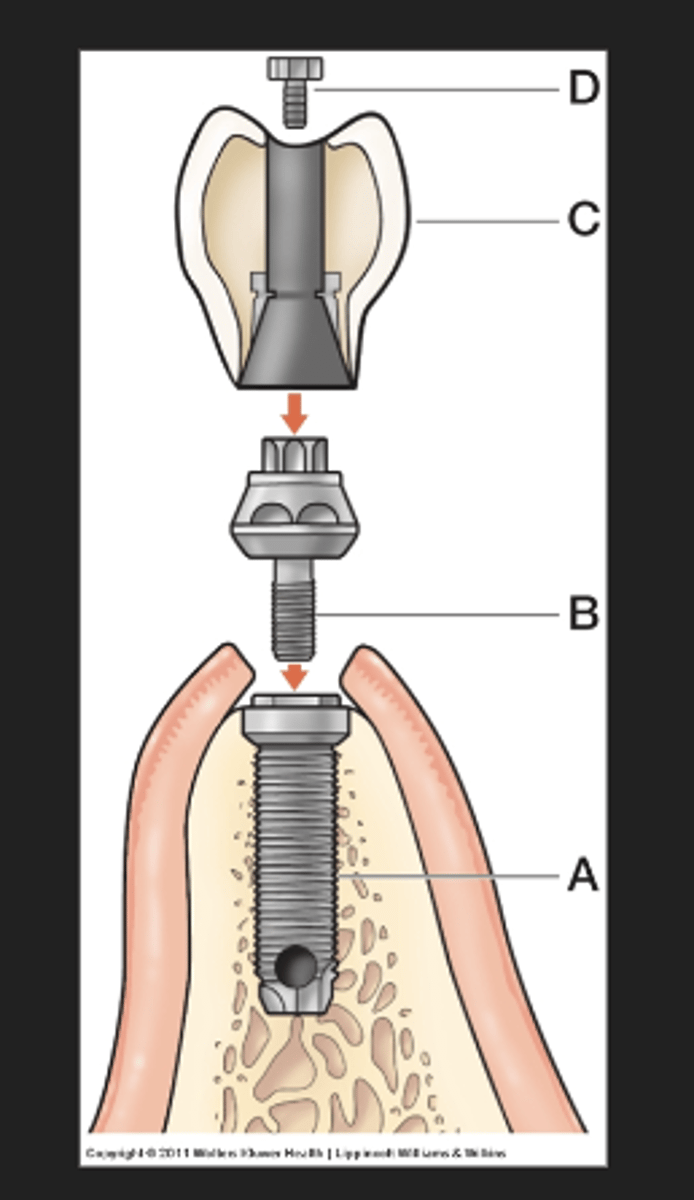
What shape can the body of a implant have?
parallel or tapered
smooth or rough

What are implant-supported prosthesis?
implant bridge
2 implants acting as abutment and middle is the missing tooth
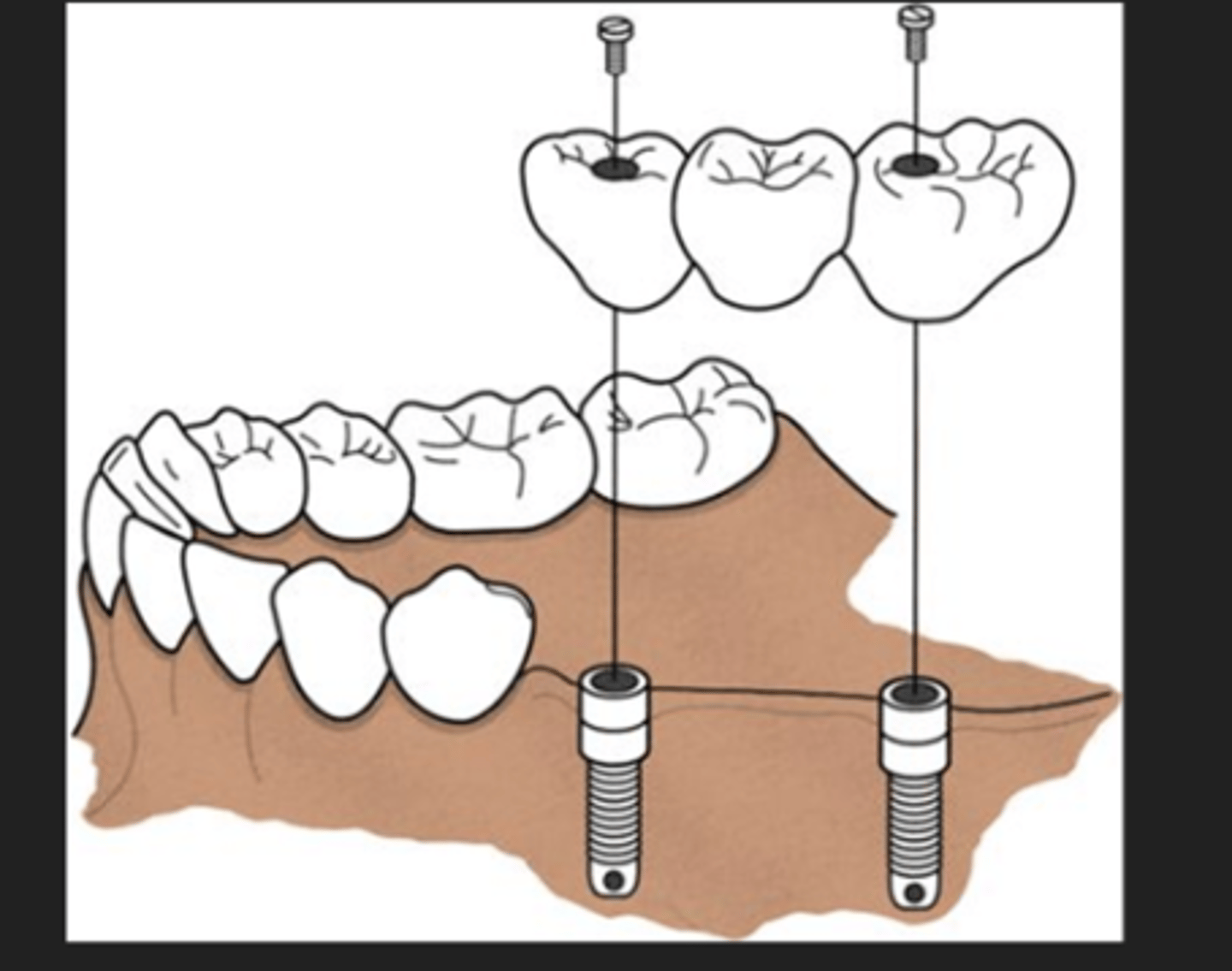
What does a denture implant look like?
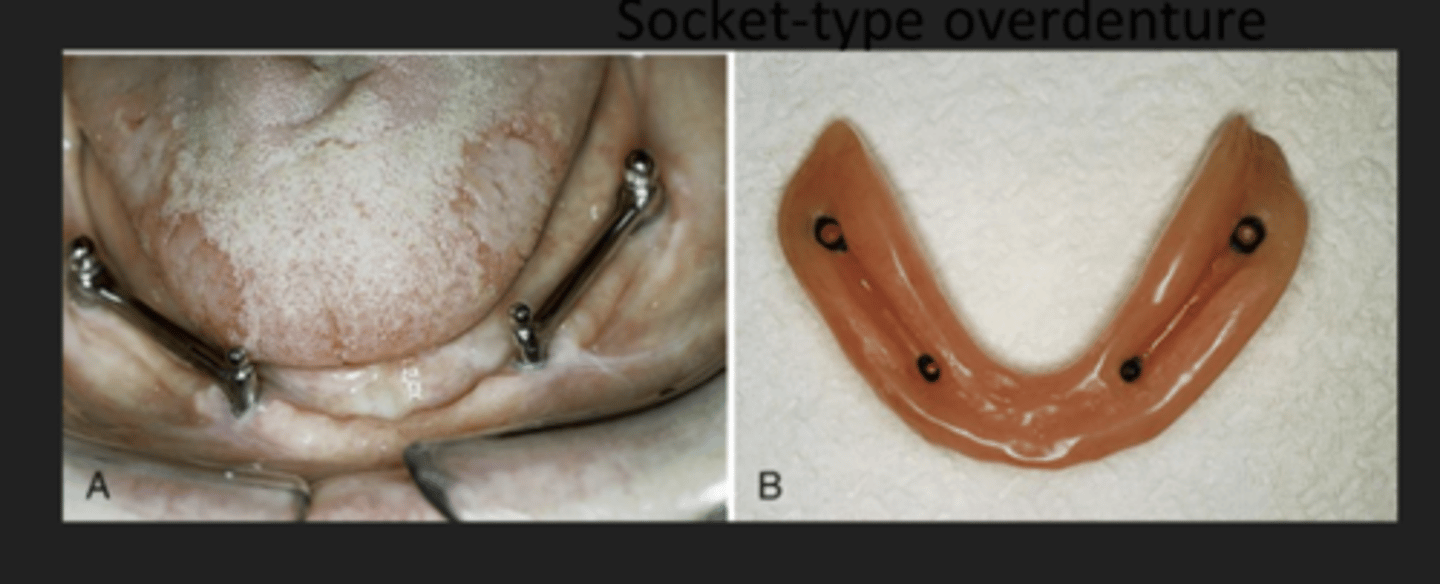
What is a crossbar implant?
used for dentures, partial snaps on
lower anteriors
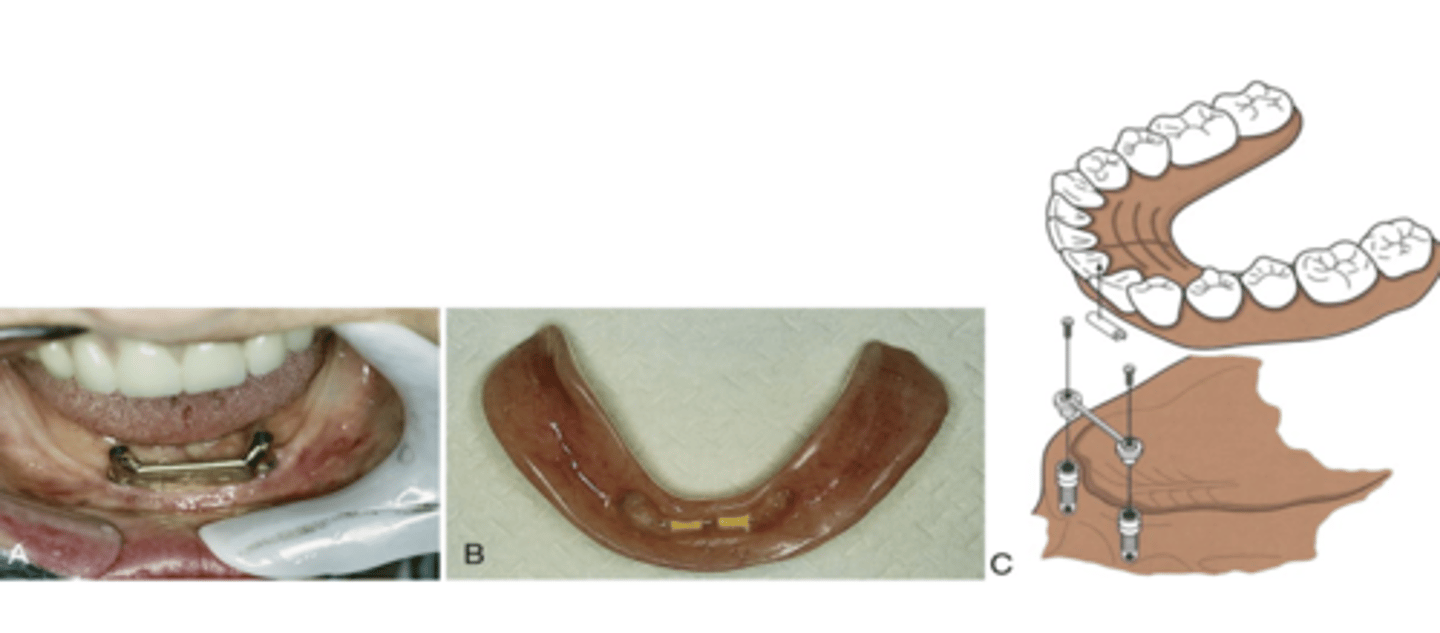
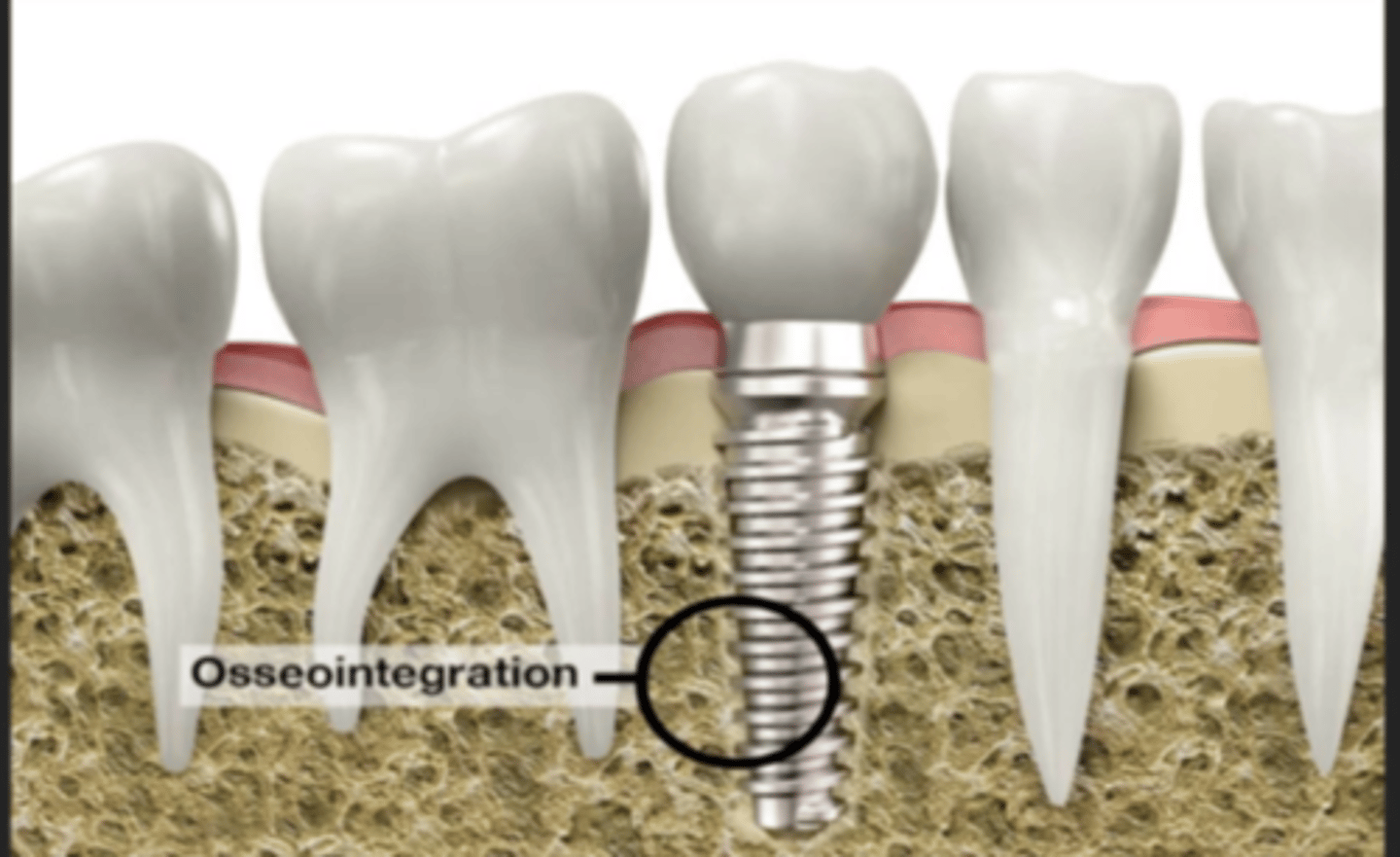
Define osseointegration
direct contact of bone with the implant surface --> another word is ankylose
functionally stable attachment between bone and implant without any CT
bone grows and attaches to threads of the implant
How does healthy mucosal tissues around implants compare to periodontal tissue?
more collagen and less vascular to periodontal tissue
CT resembles scar tissue
they are more susceptible to inflammation and inflammatory cells
What does the implant treatment sequence look like?
1. Presurgical workup - pt should have no dental disease
2. CBCT Scan
3. Tooth extraction (3-6 month healing)
4. Stage 1 surgery: placement of implant (3-6 month healing)
5. Stage 2 surgery: uncovering implant (several days healing)
6. Restorative process - attaching abutment and crown
Describe the clinical characteristics of peri-implant health
No BOP
No inflammation
No suppuration/exudate
Gingival margin follows crestal bone --> bone should be covering the threads
Normal or reduced bone level --> look at baseline after implant is placed to compare
Define remodeling
osteoclast and blast work in harmony
clast makes bone resorb causing some slightly lower levels
Describe the clinical characteristics of peri-mucositis
inflam of gingival soft tissue
BOP
Clinical signs of inflammation
Increase of probing depths (overtime—compare to baseline)
Peri-Implant Crevicular Fluid (PICF)
Increase of cytokins in PICF
What is peri-mucositis caused by?
plaque
reversible
Describe the clinical characteristics of peri-implantitis
inflam of gingival soft tissue and loss of crestal bone
BOP
Suppuration/exudate
Radiographic Bone Loss
Increase of cytokins in PICF
**refer to perio
What is peri-implantitis caused by? (4)
Plaque/calculus
Excess Cement
Genetic Factors
Iatrogenic Factors (from provider)
irreversible
What are the genetic factors that cause peri-implantitis?
cytokine secretion
gene polymorphisms
protein production
What are the iatrogenic factors that cause peri-implantitis?
Malpositioned implant body
Over countered implant crown
Poor restoration-abutment seating
What are the the 2 main causes of peri-implantitis? (risk factors)
history or periodontitis
poor plaque control and no regular maintence
What are some other risk factors that cause peri-implantitis? (may need more research)
1. smoking
2. systemic conditions
3. reduced keratinized mucosa
4. occlusal overload
5. titanium particles --> caused by incorrect instrumentation
What are the hard and soft tissue deficiencies that can cause peri-implantitis? (slide images)
Diminished Alveolar Ridge
Extraction trauma
Endodontic Infections/periapical peri-Implantitis
Thin Buccal Plate
Tooth/Root Position
Maxillary Sinuses
What is retrograde peri-implantitis?
overheating of the implant body when it is placed, causing infection
What is periapical endodontic lesions?
pre existing infection in bone was not cleared up and implant was placed regardless
How does an implant become mobile?
1. Usually related to peri-implantitis
2. Loose abutment/fractured abutment
3. Rupture of cement seal on cemented restorations (fistula)
4. Loosening of internal screw
How can a provider ensure a successful maintenance of implants?
1. correct instruments used
2. maintenance protocol
3. standard of clinical practice
What are the factors of an implant that will make it successful?
1. quality of soft tissue
2. inflam response
3. implant position
4. mode of retention
(we don't have control)
How can a patient ensure a successful maintenance of implants?
1. level of compliance
2. level of self care
3. management of risk factors
Who makes up the dental implant team?
patient
surgeon
restorative team (us)
What is the standard of care for dental implant maintenance?
Mechanical plaque control with manual or powered toothbrushes
Professionally administered plaque control procedures
- Oral hygiene instructions
- Mechanical debridement
- Hand or powered instruments with or without polishing tools
What is code 6081?
Scaling and debridement in the presence of inflammation or mucositis of a single implant, including cleaning of the implant surfaces, without flap entry and closure
not performed in conjunction with D1110, D4910, or D4346
only used when treating one implant
How do we probe around an implant?
plastic probe, light pressure
Should be avoided during the initial healing and integration phase (3-6 months (can get baseline readings tho)
What info does probing around an implant provide?
Provides baseline information
BOP
Suppuration
Probing depth
Radiographic bone loss
Implant mobility
Is probing depth as meaningful as it is with natural teeth?
no, longer abutment then greater PD
to interpret probe readings, there must be baseline data
What instruments should we use to remove deposits around an implant?
Plastic instruments (not recommended anymore)
Gold-tipped titanium instruments
Graphite-reinforced nylon scalers
Titanium instruments
Ultrasonic instruments (plastic tips)
Air Polishing with Glycine powder
What is the recall like for implants?
3-6 month professional removal of plaque/biofilm
3 months for periodontally involved patient with dental implants (frequent)
What should you avoid using on implants?
APF fluorides --> .02% NaF recommended
abrasive polishers --> use tin oxide or nonabrasive
What are some adjuncts for cleaning dental implants?
Toothbrushes (ETB)
Interspace brushes (Tuft End)
Power Brushes
Interdental brushes
Rubber tips
Dental floss
Oral Irrigation/Water flossers
Antimicrobial Agents
What is a good rinse to use for peri-mucositits?
CHX rinse
What is a good air polisher for implants?
Glycine powder Hu-Friedy EMS Air-Flow® Perio powder
What are the best adjuncts for implants?
power brushes
water flossers
oral irrigation
What is a dental hygienist measuring and assessing around an implant to determine its health?
BOP
Inflammation (color, contour, consistency)
Suppuration
Probing and Relative
Attachment Loss
Radiographs
Periodontal risk assessment