W11. Life Support/Monitoring & PFTs - ML
1/303
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
304 Terms
What is the purpose of an Electrocardiogram (ECG/EKG)?
To monitor the heart's rhythm and rate using 10 electrodes to give 12 leads.
If leads fall off the monitor may look like
asystole
What vital signs are usually displayed on an ECG monitor?
Heart rate, body temperature, oxygen saturation, and respiratory rate.
Monitoring Vitals: Every Machine Is Different
Top: Ekg usually Lead 2 Or V5
O2 Saturation Wave
Respiratory Wave
On The Right:
Heart Rate
Body temp
O2 Saturation
Respiratory Rate
Which vital is not measured in real time on the monitor
BP unless it's measure by an internal line
Ekg -Watch For Indications Of Declining Status
St Segment Changes
Multiple Pvcs Or Change In Foci
Onset Of Ventricular Tachycardia Or Ventricular Fibrillation
Progression/Worsening Of Heart Block
A-fib
What does SpO2 measure?
The arterial oxygen saturation expressed as a percentage of oxygen bound to hemoglobin.
SAO2
Invasive arterial blood signal
SaO2 vs SpO2
SaO2 is the oxygen saturation via a blood gas.
SpO2 is oxygen saturation via a pulse oximeter.
What is the threshold level for SpO2 to be considered acceptable?
Above 90%.
Orders For Titrations
maintain levels above 90%
What factors can cause inaccuracies in pulse oximetry readings?
Low perfusion, anemia, nail polish, fluorescent lighting, dark skin, jaundice, and arrhythmias.
Anemia and pulse ox
Not enough RBC or regular pulse to calculate saturation
nail polish and pulse ox
Blocks light from passing through
Fluorescent Lighting and pulse ox
Interferes with infrared signal
Dark Skin and jaundice with SPO2
Melanin
Arrhythmias and pulse ox
Variations in strength and regularity of pulsatile signal making it harder to detect changes in O2 saturation
take pulse
manually
What is the normal range for heart rate (HR)?
50-100 beats per minute.
What is the normal range for SBP
85-140
What is the normal range for DBP
40-90
What is the normal range for RR`
12-20
What is the normal range for O2SAT
>95% FiO2
What is the purpose of invasive arterial lines?
To allow continuous monitoring of blood pressure and hemodynamic status in unstable patients.
What does MAP stand for and what is its normal range?
Mean Arterial Pressure; normal range is 70-110 mmHg.
MAP lower than 60
Poor perfusion
Reasons for A-Line use
Continuous SBP, DBP and MAP Management Or Hemodynamic
Monitoring (Fluid)
Frequent ABGs Taken
Drug Administration
Precautions with arterial lines
Transducers must stay level w/ R atrium
Avoid Dislodging-Large Blood Loss
Radial insertion-Limit Or Avoid WB On Wrist
Femora Insertion-Monitor Closely & Avoid Dislodging!
transducer w/ A-line
stay level at R atrium
Other Potential Arterial Line Placements
Brachial
Radial
Axillary
Ulnar
Femoral
DP Artery
Posterior Tib
What is the function of a central venous line?
To measure central venous pressure (CVP), Right atrial pressure, and provide IV access for medication administration.
What is a PICC line and where is it placed?
A Peripherally Inserted Central Catheter placed in the cephalic, basilic, or brachial vein.
PICC line is used for
long term meds and runs up to SVC
CVP or PICC Precautions
They Need To Remain Sterile.
Usually Well Covered Near Skin Insertion.
Secure Ends Well Before Mobilizing
Be Aware Of The Location And Avoid Dislodging
Use Precautions with ambulation When Femoral Picc Used
Invasive Monitoring
swan Ganz and Pulmonary Artery Catheter
What is the Swan-Ganz catheter used to measure for?
Central Venous Pressure (Cvp)
Right Atrial Pressure
Pulmonary Artery Pressure
Pulmonary Capillary Wedge Pressure
Calculation Of Vascular Resistance
SVo2 And Temporary Pacing
Right atrial pressure with swan ganz
Gives idea of venous return
Why Is The Swan Ganz Catheter So Important?
Measurement Of Left Sided Heart Function
What does pulmonary capillary wedge pressure indicate?
It provides an indirect assessment of left ventricular filling pressure.
Indirect Assessment Of Left Ventricular Function
Elevated PCWP indicates
Pulmonary Htn
Indicates Resistance To Flow Into The Left Ventricle
Uses of swan ganz
Monitoring Heart Function (Post Sx)
Diagnosing Chronic Heart Failure
Differentiating Causes Of Pulmonary Edema
Guiding Diuretic Dosing To Manage Fluid Overload
What are the potential complications of using a Swan-Ganz catheter with mobilization?
Serious Arrhythmias
Pulmonary Artery Rupture
Pulmonary Valve Damage
Infection -Heart
Newer swan ganz mobilization guidelines
Use Of A Standard Dressing And Immobilization Technique Prevents Catheter Dislodgement During Ambulation.
By Increasing Physical Activity, Patients Will Gain Strength To Help Prevent Deconditioning During Prolonged Hospitalizations
Invasive temp monitorring
Swan Ganz
Urinary Catheters
Nasopharyngeal
Rectal Probe
Rectal Probe Only When
Comatose
Intubated
Confused
What is the purpose of monitoring intracranial pressure (ICP)?
Used For Neurological Trauma
Head Injury, Brain Surgery, Hemorrhage, Tumor Meningitis
Increased Icp Causes
Decreased Perfusion Of Brain
Low Co2 Levels Can Help Control
Increased ICP
Drain Or Shunt May Be Placed To Control
ICP
What is the most common device for oxygen delivery?
Nasal cannula.
Lowest Level Of Oxygen Support
nasal cannula
Nasal cannula flow rate
1-6 L/min
Cannula humidifies when
Rate Is > 4 L/Min because mucus membrane can dry with higher flow rates
What is the FiO2 relation to oxygen flow rates?
For every 1 L/min increase in flow, FiO2 increases by 4%.
face mask flow rate
5-10 L/min
~35 To 56% Fio2
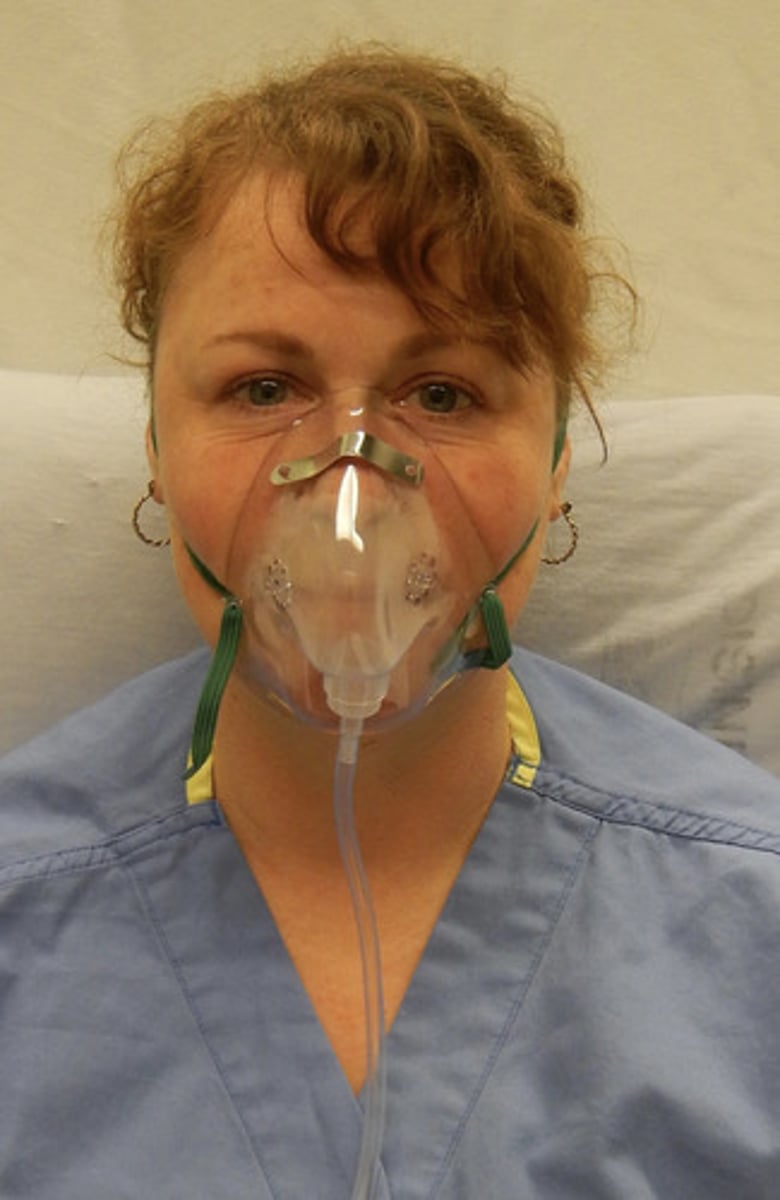
Trach mask
always worn above tracheostomy site
Always Humidified
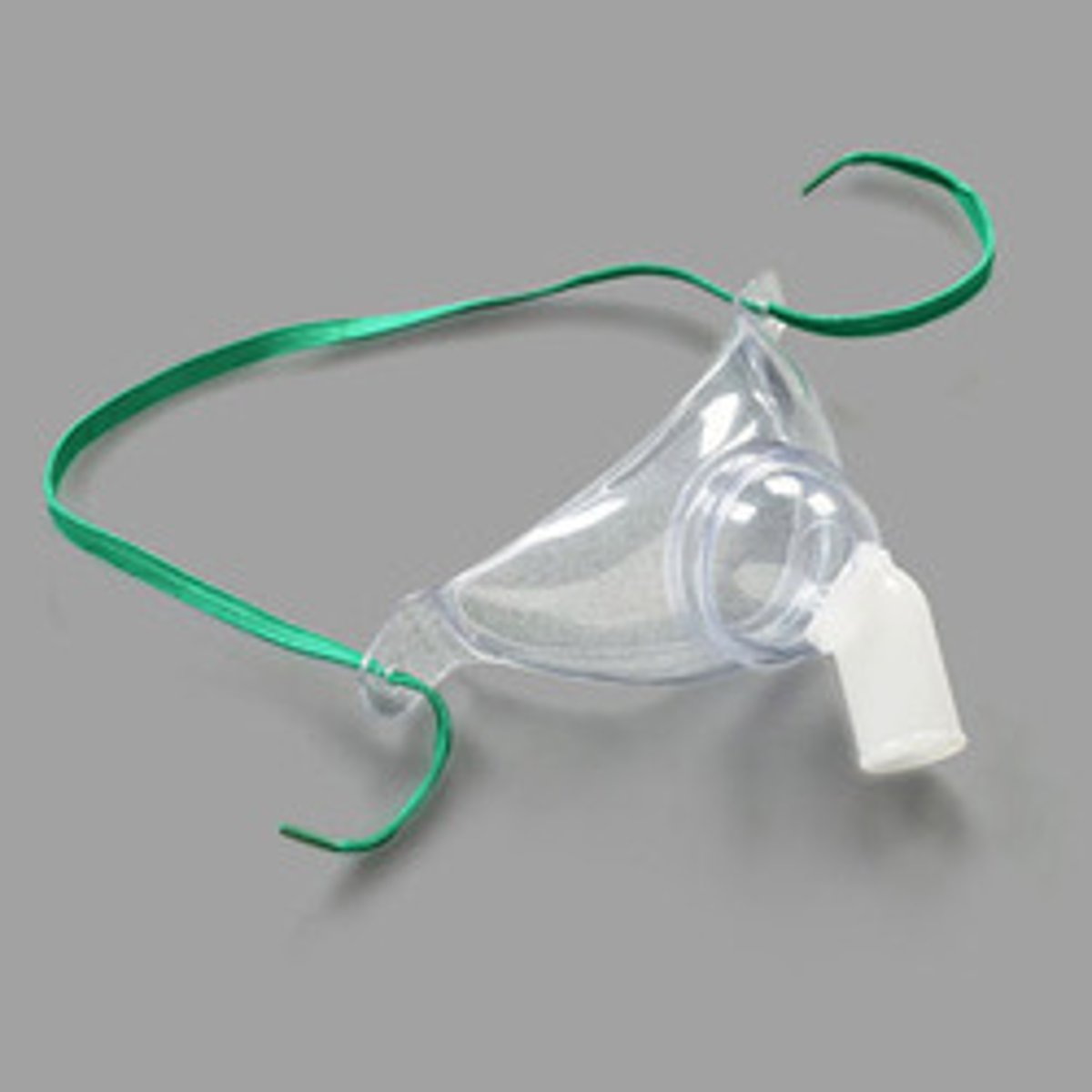
Why Must The Trach Mask Be Humidified?
Humidification Of Air Happens In The Upper Airways, The Trach Is A Bypass of the upper airways and the nose and mouth thus reducing humidification
Venturi Mask
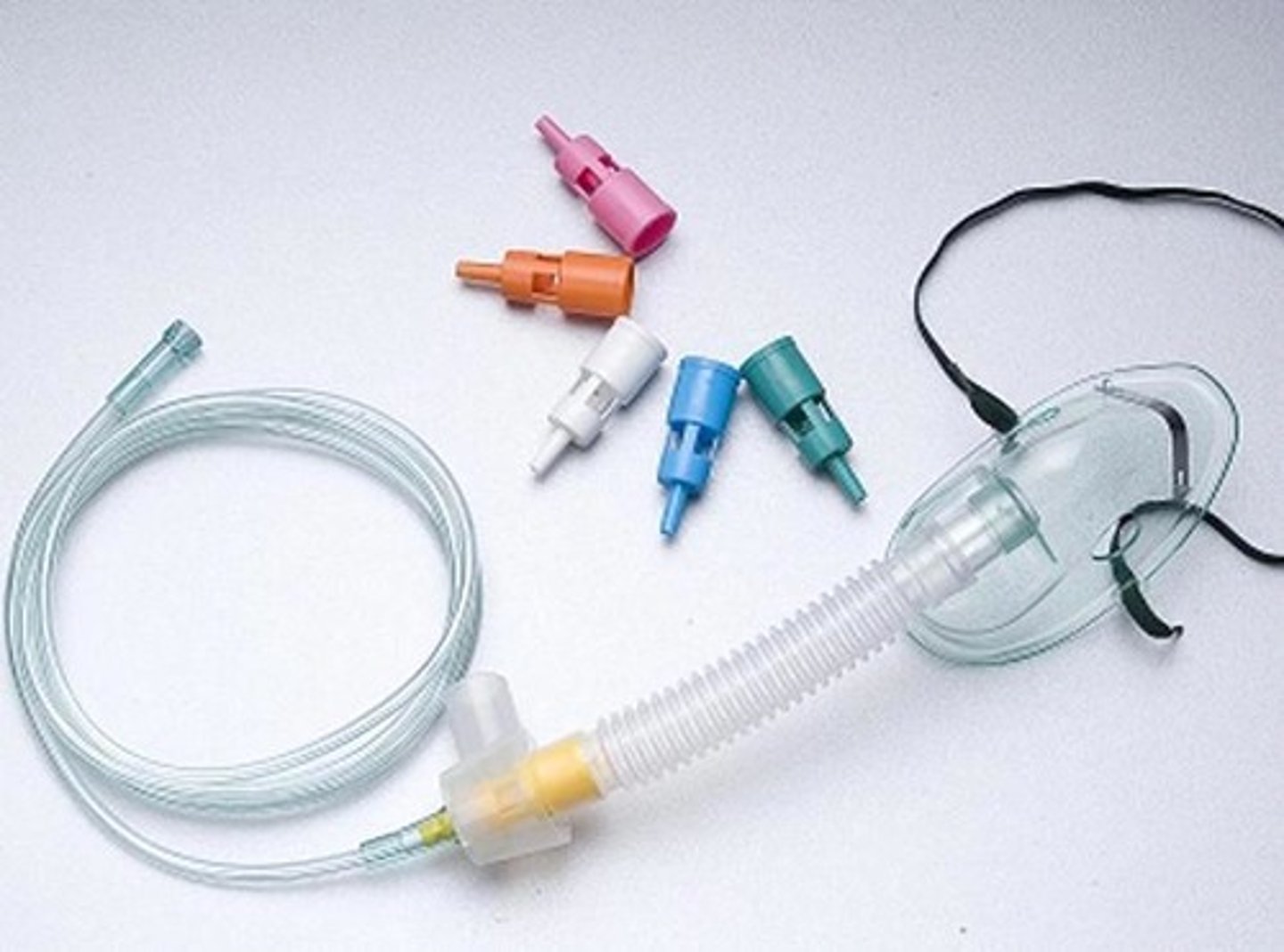
Venturi mask specs
Adapter allow for Much More Specific/Precise Fio2 Delivery
Gain Order For Fio2
Dictates The Liters/Min Setting On The O2 Supply
Non-rebreather mask
Bag Fills From Wall W/ (O2 >15L/Min)
Breathe In Air From Bag
Ensure bag is fully inflated
Breathe Out-Air Goes Into The Room
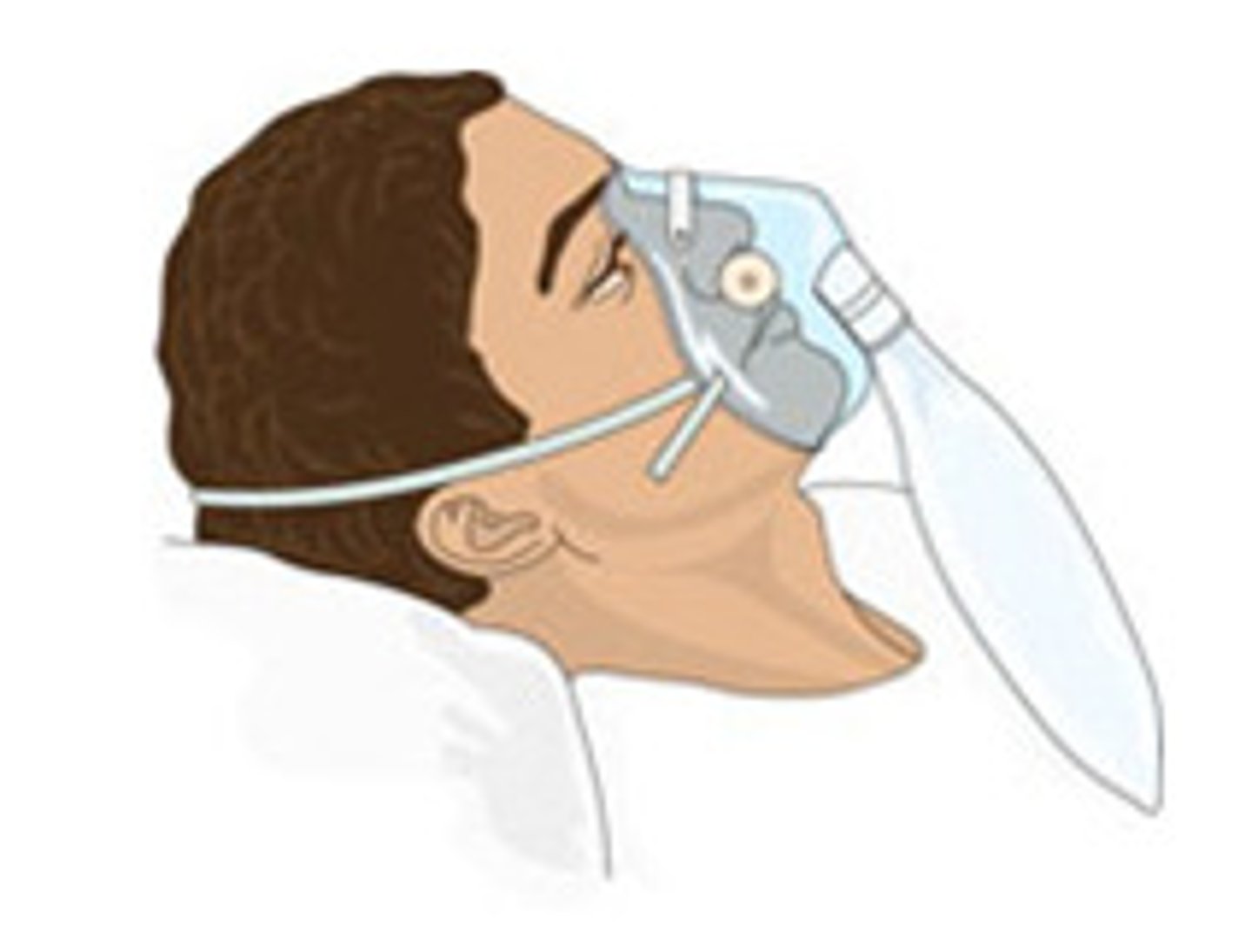
Due To High Flow Rate w/ non rebreather
Need To Start With Full Tank And Bring A Spare when beginning to mobilize patients
High Flow Nasal Cannula
Provides 25-60L/min of O2
Machine gets wall source of air
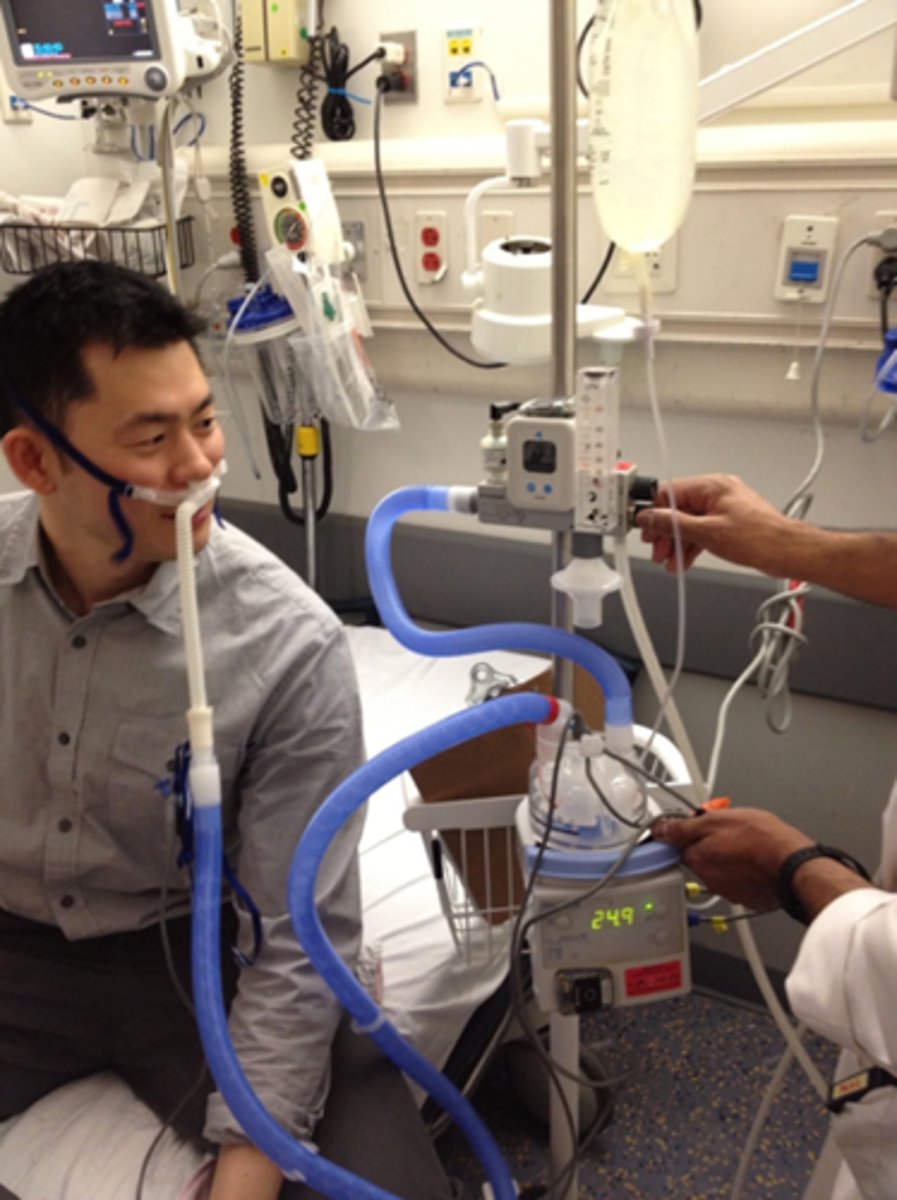
HFNC creates
positive pressure to splint open the airways and remove CO2
What is the function of a non-rebreather mask?
To provide up to 100% oxygen to the patient.
Non invasive ventilation
CPAP/BiPAP
invasive ventilation
- endotracheal tube
- tracheostomy
- mechanical ventilator
What does CPAP stand for and when is it used?
Constant Positive Pressure During Both Inhalation And Exhalation;
commonly used in sleep apnea.
BIPAP
2 Levels Of Pressure, One For Inhalation And One For Exhalation
Used To Wean Off Ventilator Or Prior To Invasive Ventilation
What are the two types of invasive mechanical ventilation?
Endotracheal tube and tracheostomy tube.
Causes OF INVASIVE VENTILATION
Failure To Oxygenate
Failure To Ventilate
Combination Of Both
Airway Protection
Endotracheal Tube
short-term artificial airway to administer mechanical ventilation, relieve upper airway obstruction, protect against aspiration, or clear secretions
Tracheostomy Tube
a long-term breathing tube surgically placed through the anterior potion of the neck below the vocal chords
Ventilator Settings
-Tidal volume: amount of air given with each breath
-Rate: number of breaths per minute
-FIO2: oxygen concentration
-Peak inspiratory pressure: pressure needed to deliver set tidal volume
-PEEP: positive pressure exerted during expiration to prevent atelectasis
-Pressure support: positive pressure given during inspiration that eases workload of breathing
Mode-amount of assist
What is tidal volume in the context of ventilator settings?
The amount of air delivered per breath.
What is PEEP in mechanical ventilation?
Positive End Expiratory Pressure; it keeps the airways open at the end of exhalation.
FiO2
Percent Of O2 In Delivered Air
starts at 100% titrated down to 21% which is normal atmospheric
What is the recommended FiO2 level to prevent atelectasis?
Keep FiO2 lower than 50%.
What are the four levels of assist in ventilator settings?
Control mode, assist mode, synchronized intermittent mandatory ventilation (SIMV), and pressure support.
Control mode ventilator
Ventilator Has Complete Control
Volume & RR PRE Set, No Pt Initiation
What is Assist Control (Ac-Vc) in ventilation?
Set Number Of Breaths (Rr)
Every Breath Has Set Volume
Pt Can Initiate More Breaths-Machine Still Gives The Set Volume
What does Synchronized Intermittent Mandatory Ventilation (Simv-Vc) allow?
Set # Of Breaths W/ Set Volume Given
When Pt Takes More Breaths Than Set RR
Tidal Volume Is Not Controlled
In Spontaneous or Pressure Support ventilation, who dictates tidal volume and respiratory rate?
The patient dictates tidal volume and respiratory rate.
Set Pressure, Peep And Fio2
When pt is on a ventilator, the FiO2 is adjusted to attain an Oxygen level goal of
60 mmHg or 90%
How should adjustments be made for CO2 levels in ventilation?
Adjust the respiratory rate (RR) first then tidal volume (TV).
How should adjustments be made for O2 levels in ventilation?
Adjust FiO2 first then PEEP.
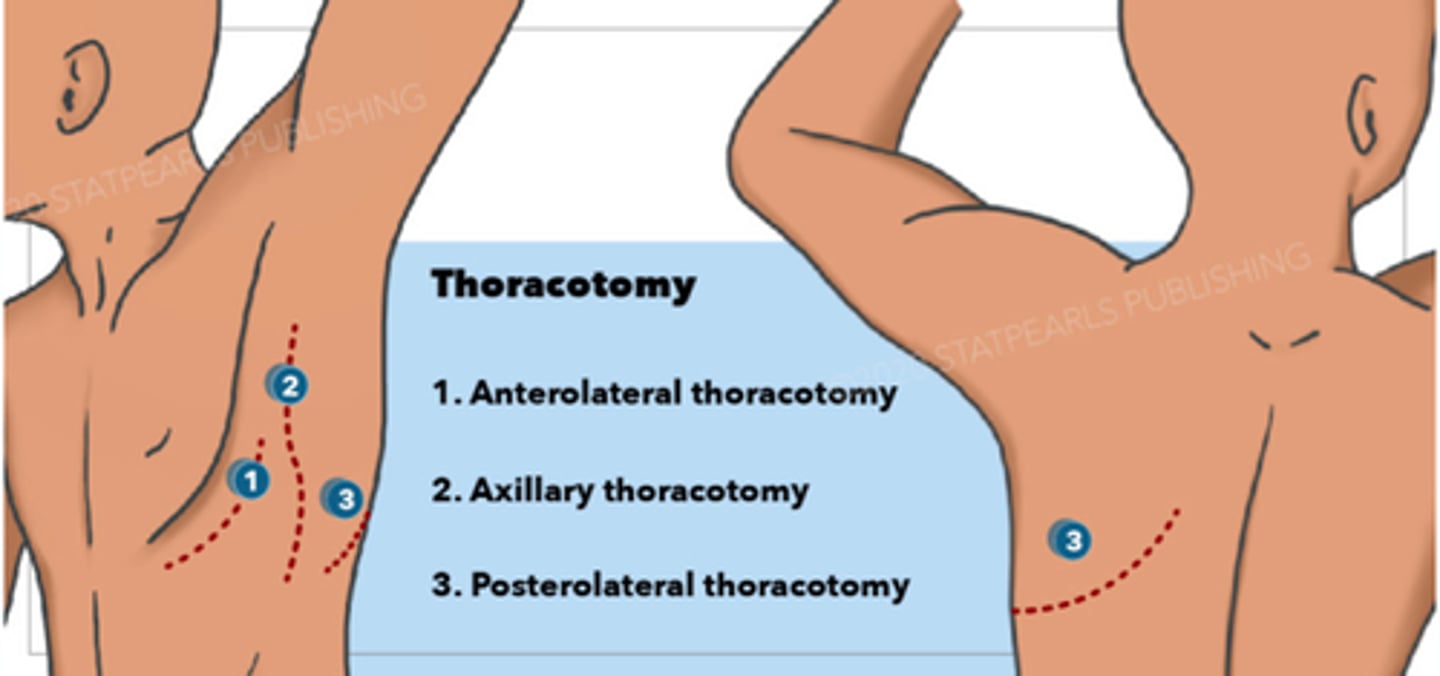
What is the purpose of a thoracotomy?
To access the thoracic cavity for surgical procedures.
What is a Posterolateral Thoracotomy used for?
It is commonly used for pulmonary thoracic procedures,
Used to access lungs for resections, pleuro and pneumothorax sx
What is a Median Sternotomy primarily used for?
It is almost exclusively used for cardiac procedures.
Anterolateral Thoracotomy aka clamshell incisions
Lateral
Subxiphoid Incision
Thoracoabdominal
What is the Anterolateral Thoracotomy incision used for?
It is used for cardiac tamponade, descending thoracic aorta repair, and left pneumonectomy.
Median Sternotomy
Initial Skin Incision Usually Begins Inferior To The Suprasternal Notch And Extends Down Midline Of The Sternum To Below The Xiphoid.
A Sternal Retractor Divides The Sternum Fully And Holds The Incision Open.
Can cause changes to the T-spine
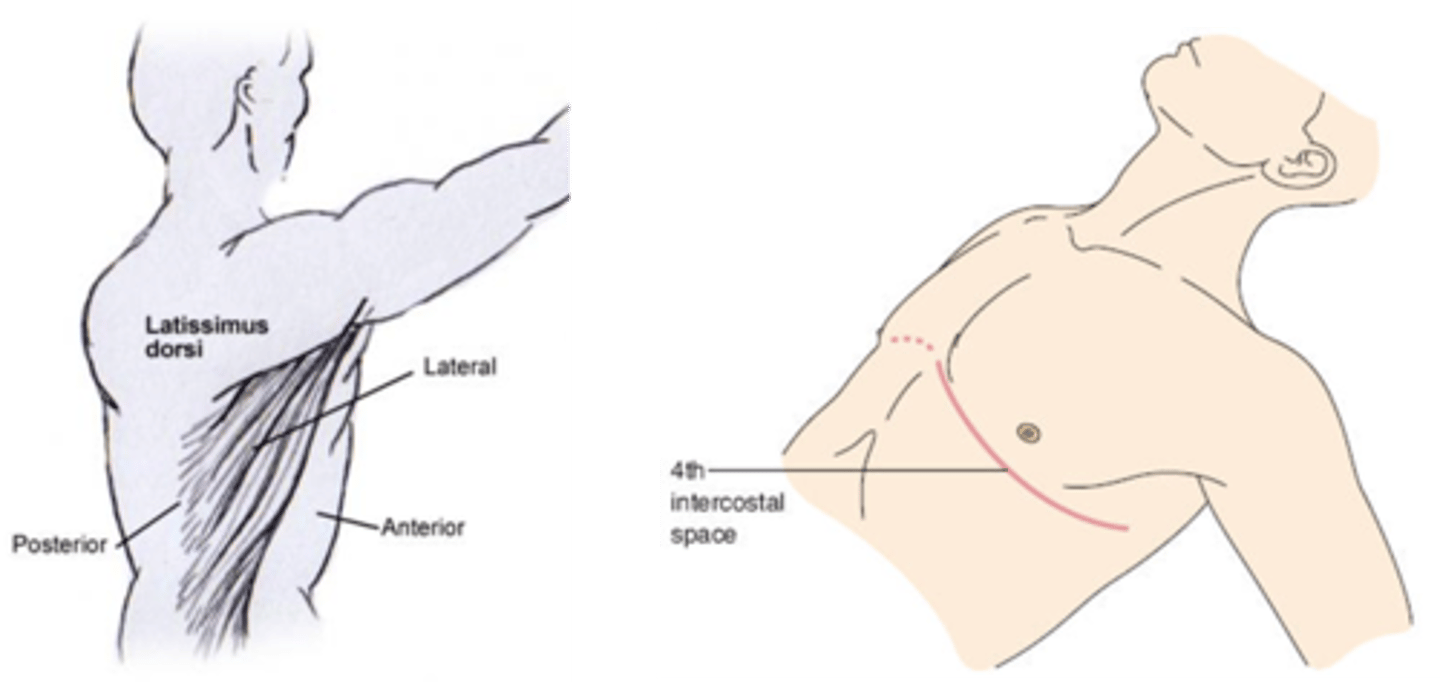
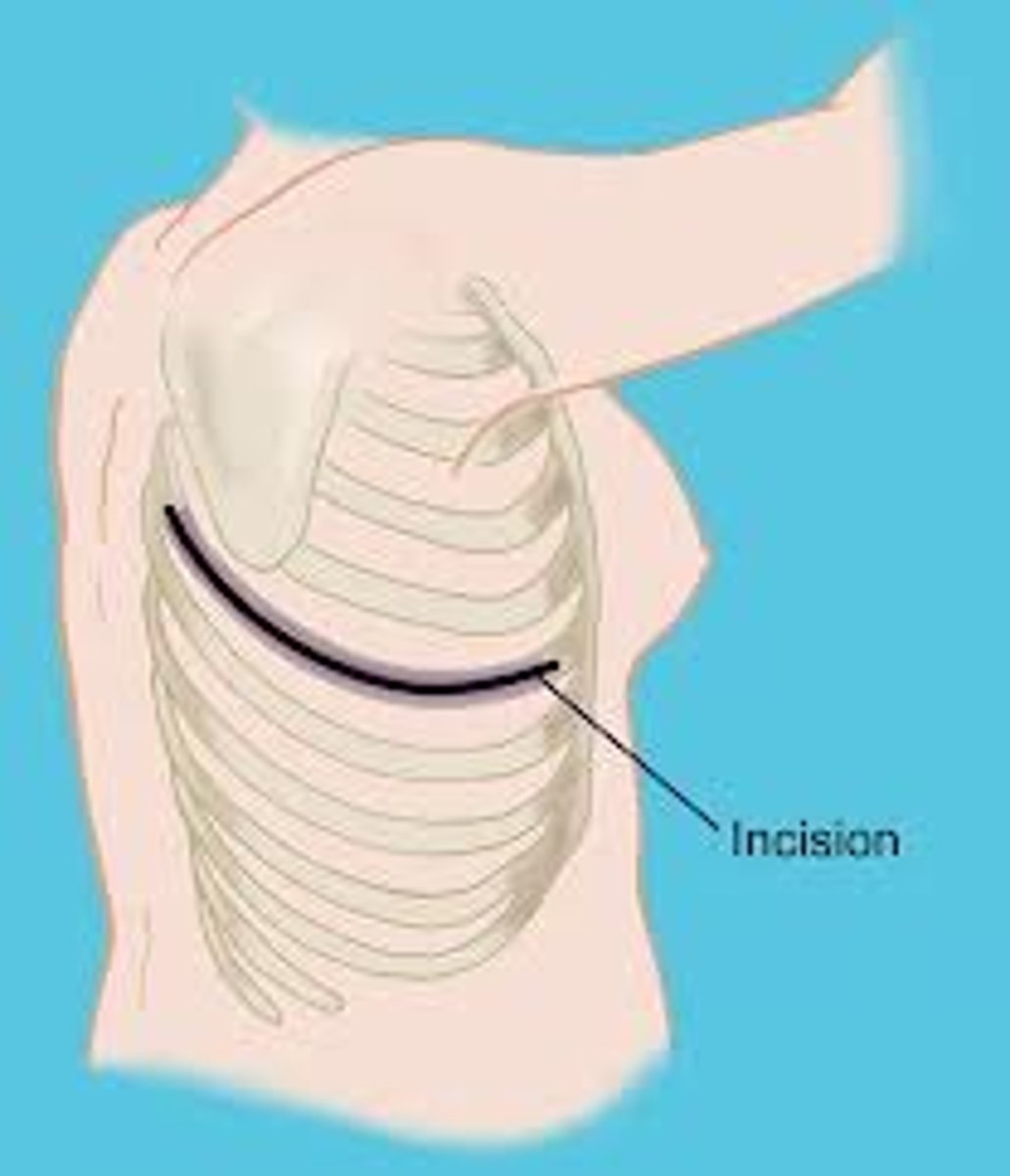
Posterolateral Thoracotomy incision
Extends from T4 medial to scapula to anterior axilla at 5/6th intercostal space
muscles affected with posterolateral thoracotomy
Lower trap, serratus anterior and middle trap can get divided
advantage of posterolateral thoracotomy
Gives Good Visibility
disadvantage of posterolateral thoracotomy
Pain, decreased Mobility And Pulmonary Issues
Anterolateral Thoracotomy
Incision
From Sternal Edge To Midaxillary
At Level Of 4th or 5th Intercostal Space
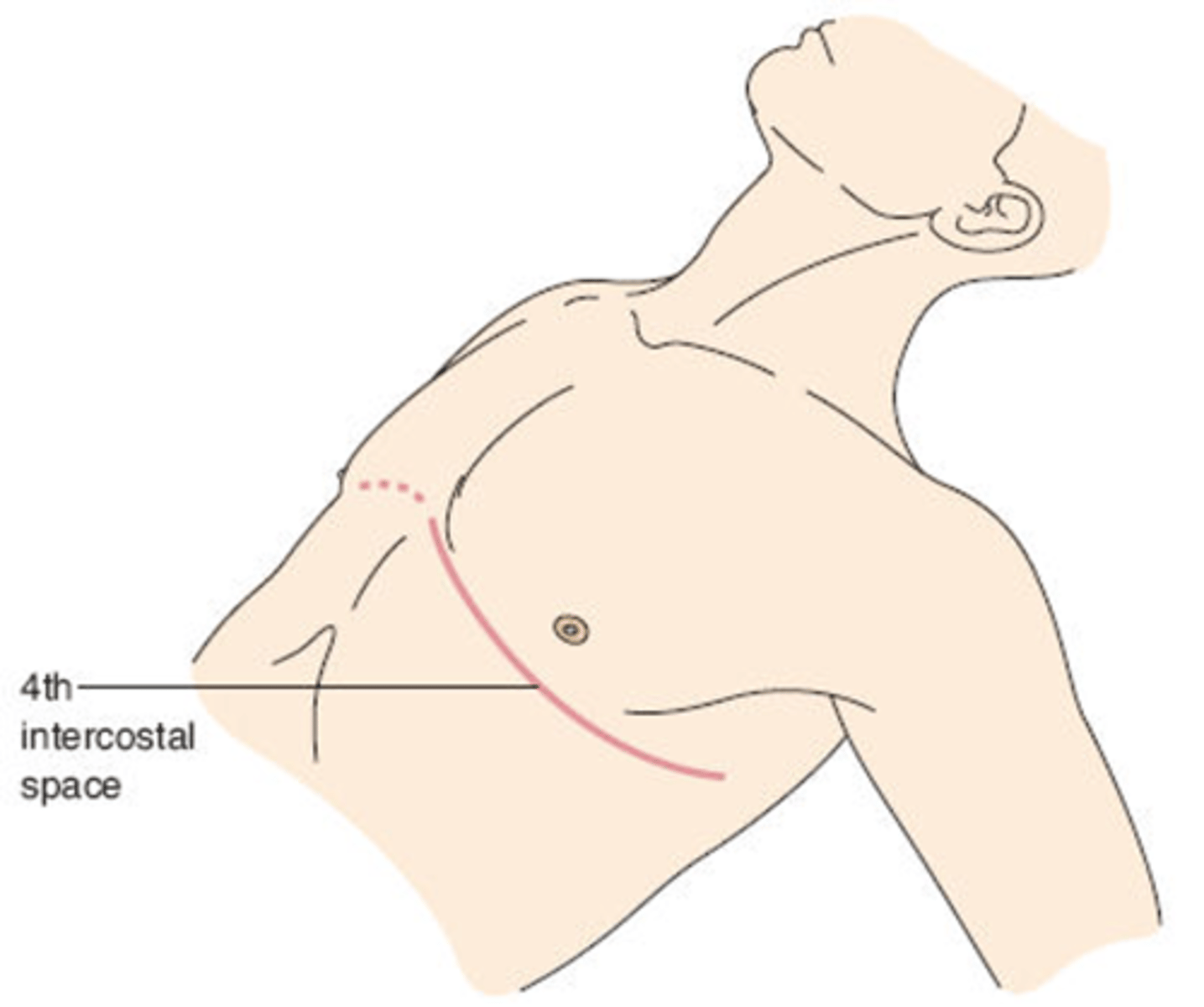
left anterolateral thoracotomy optimal for
Cardiac Tamponade,
Descending Thoracic Aorta Repair,
Pericardial Effusion, Left Pneumonectomy
Right anterolateral thoracotomy optimal for
Right Pneumonectomy
Distal Esophageal Surgeries,
Access To The Hilum
Mitral Valve Repair/Replacement (Minimal Incision)
Anteroloateral approach can affect what muscles
pectorals, serratus and intercostals
Axillary (Lateral) Thoracotomy
Most Frequent Use:
Minimally Invasive Cardiac Procedures And Epicardial Pacemaker Placement