Heart 1
1/61
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
62 Terms
what pumps blood through heart
contraction of cardiac muscle
Functions of the heart (1)
generating blood pressure
What generates blood pressure
contractions of the heart generate blood pressure, which is moving blood through the blood vessels
Heart Function (2)
Routing Blood
what does the heart seperate and ensure through routing blood
seperates pulmonary and systemic circulation and ensures that blood flowing to tissue has an adqueate levels of O2
Heart Functions (3)
ensuring one way blood flow
what causes a one-way flow
valves
Heart Functions (4)
Regulating Blood supply
How does it regulate blood supply
the rate and force of contractions change to meet the metabolic needs of tissues, which vary based on rest, exercise, and changes in body positions
Pericardium
surronds the heart has two layers
Superficial fibrous pericardium
tough fibrous connective tissue that anchors heart within the thoracic cage.
Deep serous pericardium
a thin, two-layered, lubricated membrane forming a closed sac around the heart, crucial for reducing friction during cardiac contractions.
what does the deep serous pericardium consist of
fibrous pareital layer and epicardium
Epicardium (Visceral)
layer of simple squamous epithelium that lines surface of heart
Epicardium
1 thin superficial cell layer forming a smooth external surface and superficial adipose.
Myocardium
Thick middle layer of cardiac muscle tissue responsible for the hearts ability to contract
Endocardium
Deepest layer composed of simple squamous epithelium and connective tissue. The endocardium forms the smooth, inner surface of the heart chambers.
the right side of the heart pumps blood through what
pulmonary circulation
what is pulmonary circulation
which carries blood to the links, where CO2 from the blood into the lungs and O2 diffuses from the lungs into the blood
what side does pulmonary circulation return blood to
left side
what does the left side of the heart pump through
systemic circulation
what does systemic circulation do
which delvers O2 and nutrients to all the remaining tissues of the body.
from the systemic circulation tissues what happens
CO2 and other waste products are carried back to the right side of the heart.
coronary circulation
provides blood flow to the heart via coronary artery
blood returns to the right atria how
cardiac veins
After aorta what is a pathway back to the superior and inferior cava
body tissues
After aorta what is pathway back to the right atrium
coronary arteries to heart tissue to cardiac veins and coronary sinus.
electric properties of the heart
Special cardiac pacemaker cells begin at the Sinoatrial (SA) node
Membrane Potenial
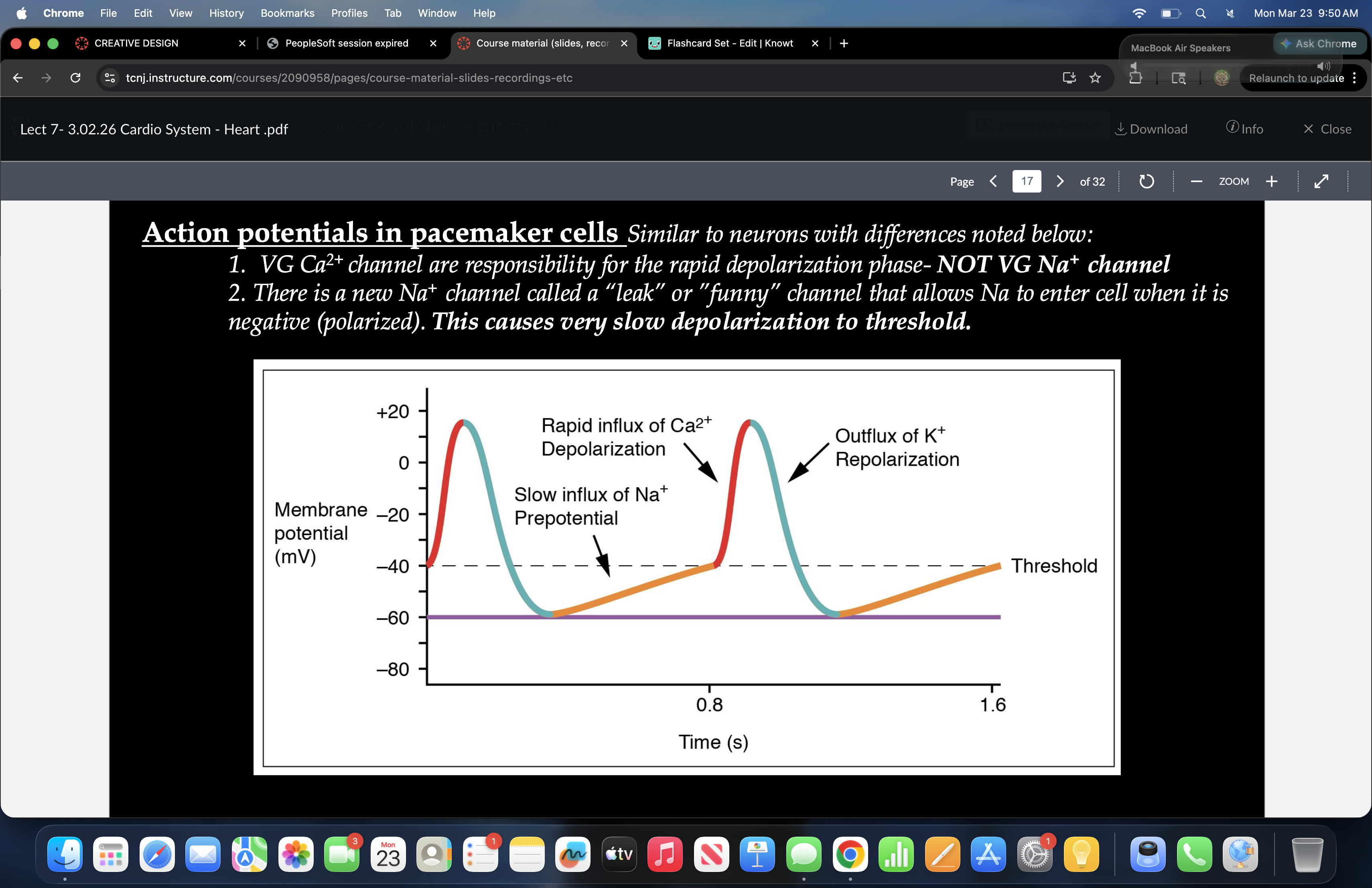
what are responsibile for the rapid depolarzation phase
VG Ca2+ channel
What allows NA to enter the cell when it is negative
a new NA channel called a leak or funny channel
what is spiking in the graph
Ca2+ depolarzation
what comes before the Ca2+
Na+ slow influx
What drops after the Ca2+
K+ repolarzation
Electrocardiogram
measures electrcial activies of heart
with each beat what happens
eletrical impulse is sent to squeeze muscle and pump blood.
a normal heartbeat on the ECG shows what
rate and rhythm of the contractions in the upper and lower chambers.
P Wave
atrial depolarzation
QRS Complex
ventricular depolarzation
T Wave
ventricular recovery/repolarization/rest
Commotio Cordis
s a phenomenon in which a sudden blunt impact to the chest stops the heart (cardiac arrest)
what is the most common theory for commoto cordios
physical disruption of cardiac plasma membrane causes abnormal ion conductance.
How are heartbeats controlled (1)
Intrinsic regulation (done by cardiovascular system itself without neural or hormonal regulation.)
How are heartbeats controlled (2)
Extrinsic regulation (Involves neural and hormonal control).
Intrinsic regulation of the heart
This is happens due to cardiac muscle cells stretching and generating more force upon contraction.
Starlings Law
states that the stroke volume of the heart increases in response to an increase in the the volume of blood in the ventricle- before
contraction.
How does starlings law happen
This is done by cardiac muscle fibers stretching . Remember muscle fibers are elastic, meaning they spring back to their regular shape after being stretch.
If BP increases, Volume in ventricle increases, and muscle fibers stretch what happens
Stretch muscle fibers contract with more force, This increases the volume of blood ejected (stroke volume) which increases blood
pressure
how are heart rate and blood pressure externally regulated
neurons and hormones
what are baroreceptors and chemoreceptors
specalized sensory neurons
sensors in heart detect what and send where
detect changes and send to CNS
Regulation of heart rate (1)
baroreceptors and chemoreceptors send sensory neurons to CNS
Regulation of heart rate (2)
sensory nerve fibers sent to CNS
Regulation of Heart rate (3)
CNS send parasympatheic and sympathetic nerve fibers back to heart
Regulation of Heart Rate (4)
sympatehic nerves fibers are sent to cardiac nerves while parasympathetic nerve fibers are sent to Vague nerves
Regulation of heart rate (5)
if sympatheic nerve fibers are not sent to cardiac nerves they go to adrenal gland.
Homeostatsis of blood pressure if BP increases (1)
Receptors and control center: Baroreceptors in the carotoid arteries and aorta detect an increase in blood pressure
Homeostatsis of blood pressure if BP increases (2)
Receptors and Control center: the cardioregularty center in brain detect a decrease in sympathetic stimulation of the heart and adrenal medulla increases parasympatheic stimulation of heart.
Homeostatsis of blood pressure if BP increases (3)
Effectors/Reponse: The SA Node and cardiac muscle decrease activity and heart rate and stroke volume decrease (BP restored).
Homeostatsis of blood pressure if BP decreases (1)
Receptors and control center: Baroreceptors in the carotoid arteries and aorta detect an decrease in blood pressure
Homeostatsis of blood pressure if BP decreases (2)
Receptors and Control center: the cardioregularty center in brain detect a increase in sympathetic stimulation of the heart and adrenal medulla decrease parasympatheic stimulation of heart.
Homeostatsis of blood pressure if BP decreases (3)
Effectors/Reponse: The SA Node and cardiac muscle increase activity and heart rate and stroke volume increase (BP restored).