Urinary System (Choi Exam 3, pt. 1)
1/169
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
170 Terms
The bladder can stretch to hold up to ________ of urine.
2 cups
main components of the urinary system:
kidneys, ureters, urinary bladder, urethra
general flow of urine form kidneys to urethra
kidneys filter blood and convert filtrate into urine --> ureters - the liquid waste is transported by the ureters (kidney --> urinary bladder) --> urinary bladder stores urine until it is eliminated from the body --> urethra - urine is eliminated through the urethra
kidneys function/first step in urinary system
filter blood and convert filtrate into urine
ureters function/step 2
the liquid waste is transported by the ureters (kidney --> urinary bladder)
urinary bladder function/step 3
stores urine until it is eliminated from the body
urethra function/step 4
urine is eliminated through the urethra
when the filtrate is converted to urine, different physiological processes occur:
- elimination of metabolic wastes
- regulation of ion levels
- regulation of acid-base balance
- regulation of blood pressure
- elimination of biologically active molecules
elimination of metabolic wastes
the kidneys remove waste within the filtrate (ex. urea, uric acid) so these substances do not reach toxic levels within the blood
regulation of ion levels
the kidneys help control the blood's ion balance, such as sodium, potassium, calcium, and phosphate ions by eliminating them in the urine (filter if have too much, excrete more ions if needed)
regulation of acid-base balance
the kidneys help maintain acid-base balance by altering blood levels of both hydrogen and bicarbonate ions
regulation of blood pressure
- They help regulating BP by excreting fluid in the urine. Regulating fluid lost in the urine helps regulating blood volume.
- The kidneys can also release enzyme "renin" which is used for production of angiotensin II (a hormone that increases BP)
elimination of biologically active molecules
small molecules (ex. hormones, drugs) are filtered, but are not reclaimed, and then becomes part of urine
in addition to filtering _______ and processing __________ to form urine, your kidneys perform/participate in other functions:
blood; filtrate
- formation of calcitriol
- production and release of erythropoietin
- potential to engage in gluconeogenesis (creating glucose)
formation of calcitriol
this hormone increases the absorption of calcium form the small intestine (increased blood calcium concentration)
production and release of erythropoietin
your kidneys can respond to low blood oxygen levels by secreting erythropoietin (EPO) hormone (increased rate of erythrocyte formation)
potential to engage in gluconeogenesis
creating glucose; during fasting or starvation, the kidneys may engage in gluconeogenesis to produce glucose from noncarbohydrate sources to maintain blood glucose levels
TLDR; your kidneys take care of your blood by:
- from the blood
- maintaining
- regulating
- altering
- regulating the number of erythrocytes
- maintaining during fasting or starvation
- removing unwanted materials from the blood
- maintaining blood plasma ions
- regulating blood pH
- altering blood volume
- regulating the number of erythrocytes
- maintaining blood glucose levels during fasting or starvation
healthy kidney --> healthy
blood
the kidneys are , bean-shaped organs
symmetrical
each kidney has a concave medial border called
hilum
the hilum is where...
the vessels, nerves, and the ureter connect to the kidney
an sits on the superior aspect of each kidney
adrenal gland
kidneys are located along the posterior abdominal wall, lateral to the vertebral column ( )
retroperitoneal
the kidney is found between the level of the T12 and L3
left
the right kidney is located to the left kidney (why?)
INFERIOR; b/c liver (2nd largest organ) pushes the right kidney down (spleen on left side does not push down as much)
marks the end of the retroperitoneal organs
duodenum
each kidney is surrounded and supported by several layers. name them innermost to outermost
TISSUE
- fibrous capsule (renal capsule)
- perinephric fat (adipose capsule)
- renal fascia
- paranephric fat
fibrous capsule/renal capsule
- innermost tissue layer
- directly adhere to the external surface of the kidney
- mainly composed of DICT (structural support)
- maintains kidney's shape, protects it from trauma, and prevents pathogens from penetrating the kidney
perinephric fat/adipose capsule
- adipose CT
- provides cushioning and stabilization for the kidney
renal fascia
- third tissue layer
- composed of DICT (structural support)
- anchors the kidney to surrounding structures
paranephric fat
- the outermost layer surrounding the kidney
- composed of adipose CT (cushioning and stabilization)
what causes renal ptosis and hydronephrosis to occur? what is it?
- the loss of adipose CT in very thin elderly or individuals with anorexia
- it's the "dropping" of the kidney
possible consequences of renal ptosis
can cause a "kink" in the ureter, which farther causes...
- decreased urine flow
- urine backs up into the proximal part of the ureter
- enlargement of the renal pelvis
when the kidney is sectioned (coronally), the , or "functioning tissue," is visible.
parenchyma
2 distinct regions of the parenchyma include an and an .
outer renal cortex; inner renal medulla
renal columns
- extensions of the cortex
- project into the medulla and subdivide it into renal pyramids (medullary pyramids)
corticomedullary junction
- the wide base of the renal pyramids
- external edge of the medulla, where it meets the cortex
renal papilla
medially directed tip of the renal pyramid
each kidney also contains a medially located space called
renal sinus
renal sinus
- urine drainage area
- minor and major calyces and renal pelvis
the functional anatomy of the kidney includes...
nephrons, collecting tubules, collecting ducts, other associated structures
what is a nephron?**
- microscopic, functional filtration unit of the kidney
two major structures of the nephron
renal corpuscle and renal tubule
where do the two major structures of the nephron reside
almost all reside in the cortex (outer region)
renal corpuscle and 2 major components
- an enlarged, round portion of a nephron housed within the renal cortex
- composed of: glomerulus and glomerular/Bowman's capsule
glomerulus
- thick tangle of capillary loops (glomerular capillaries)
- blood enters the glomerulus by an afferent arteriole and exits by an efferent arteriole
glomerular capsule (Bowman's capsule)
- formed by two layers: visceral and parietal layers
- between the two layers is a capsule space that receives filtrate, which is then modified to form urine
your renal corpuscle also has two opposing poles: the and the poles
vascular and tubular poles
the pole is where the afferent and efferent arterioles are attached to the glomerulus
vascular
the (urinary) pole is where the renal tubule originates
tubular
the renal tubule makes up the remaining part of the nephron and consists of 3 continuous sections:
the proximal convoluted tubule, the nephron loop (loop of Henle), and the distal convoluted tubule
the convoluted tubules usually reside , whereas the loop of Henle typically extends from the to the
in the cortex; cortex to the medulla
UTI's are common in women than men. One of the reasons for this is because they have a urethra (easier for bacteria to reach your bladder)
more; shorter
proximal convoluted tubule (PCT)
- the region of the renal tubule
- originated from the tubular pole (simple cuboidal epithelium with apical ; brush border (increase SA to increase absorption)
- the first region of the renal tubule
- originated from the tubular pole (simple cuboidal epithelium with apical microvilli; brush border (increase SA to increase absorption)
the PCT contains cells packed with --> high ATP demand for active transport
- reabsorbs about 65% of filtrate
cuboidal epithelial cells; mitochondria
main function of the proximal convoluted tubule (PCT)
REABSORPTION; most happens here; called the "workhorse" of the nephron
identify the two different regions of nephron loop (loop of Henle)
descending limb and ascending limb
Loop of Henle/Nephron loop descending limb:
thick or thin? impermeable vs permeable?
- THIN segment (simple squamous epithelium)
- permeable to WATER
- impermeable to solutes (Na+, Cl-)
what happens to filtrate in descending limb?
water moves out into the hypertonic medulla, causing filtrate to become CONCENTRATED
Loop of Henle/Nephron loop ascending limb
thick or thin? impermeable vs permeable?
- THICK segment (cuboidal cells with mitochondria)
- IMpermeable to water
- actively transports Na+, K+, Cl- out into the medulla
what happens to filtrate in ascending limb?
filtrate becomes more dilute as ions leave but water cannot follow
the Nephron loop (Loop of Henle) uses a mechanism, meaning...
COUNTERCURRENT: descending limb loses water; ascending limbs pumps out ions --> creates medullary osmotic gradient
collecting duct is often considered part of the system.
renal tubule system
collecting duct is composed of what types of cells?
- composed of principal cells and intercalated cells
function of principal cells in collecting duct?
respond to ADH (water permeability) and aldosterone (Na+ reabsorption/K+ secretion)
function of intercalated cells in collecting duct?
regulate acid-base balance (H+ or HCO3-)
what are the two types of nephrons?
cortical nephron and juxtamedullary nephron
structural differences between two types of nephron
cortical:
- renal corpuscle located near the edge of the cortex
- SHORT loop of Henle that barely penetrates the medulla
-85% of nephrons
juxtamedullary:
- renal corpuscle is adjacent to the corticomedullary junction
- LONG loop of Henle deep into the medulla
- vasa recta (long straight capillaries) run parallel to the loop of Henle
-15% of nephrons
functional differences between two types of nephron
cortical:
- filtration and reabsorption of solutes and nutrients
- produces dilute urine (less water reabsorption)
- efferent arteriole --> forms peritubular capillaries around the PCT and DCT
juxtamedullary:
- key role in concentrating urine via the counterconcurrent multiplier system
- crucial during dehydration, allowing water reabsorption under ADH
Urine formation (not on SG):
nephrons drain into each collecting tubule. Each kidney has thousands of tubules, and they eventually empty into larger ducts. They both project through the renal medulla toward the renal papilla
several; collecting; collecting
Urine formation (not on SG):
- the collecting ducts then drain into a duct (located within the renal papilla
- it is then drained from the papillary duct to the
papillary; minor calyx
What are the two main components of the juxtaglomerular apparatus (JGA)?
macula densa cells of DCT & granular cells of afferent arteriole
granular cells
- modified smooth muscle cells of the afferent arteriole
- act as a baroreceptor (detect BP changes)
- secrete renin when BP drops
macula densa
- modified epithelial cells in the wall of DCT
- they signal granular cells to release renin by detecting changes in NaCl concentration of the DCT
juxtaglomerular apparatus comes into close contact with the arteriole (and sometimes efferent) of the same nephron. It serves as a and that helps the kidney control filtration rate and systemic BP
afferent
sensor and regulator
extraglomerular mesangial cells
- communicate with other cells of the JG apparatus via gap junctions and the release of paracrine hormones
- may influence blood flow
when BP drops... renal perfusion and glomerular filtration rate (GFR)
drops and drops; ALL DROP
from BP, renal perfusion, and GFR dropping, less filtration means less reaches the DCT, so the macula densa senses low . Macula densa signals the JG cells to release . JG cells also directly detect reduces stretch (low pressure) and release .
NaCl; NaCl; renin; renin
about 20-25% of the resting flows through the kidney to remove unwanted substances. a filtrate is formed when the blood flows through the glomerulus, and some components of the plasma enter the .
cardiac output; capsular space
what flows into and out of the kidney?
blood
what flows through the nephron and other urinary structures?
filtrate, tubular fluid, and urine
Describe the pathway of blood flow through the kidney, starting from the renal artery and ending at the renal vein
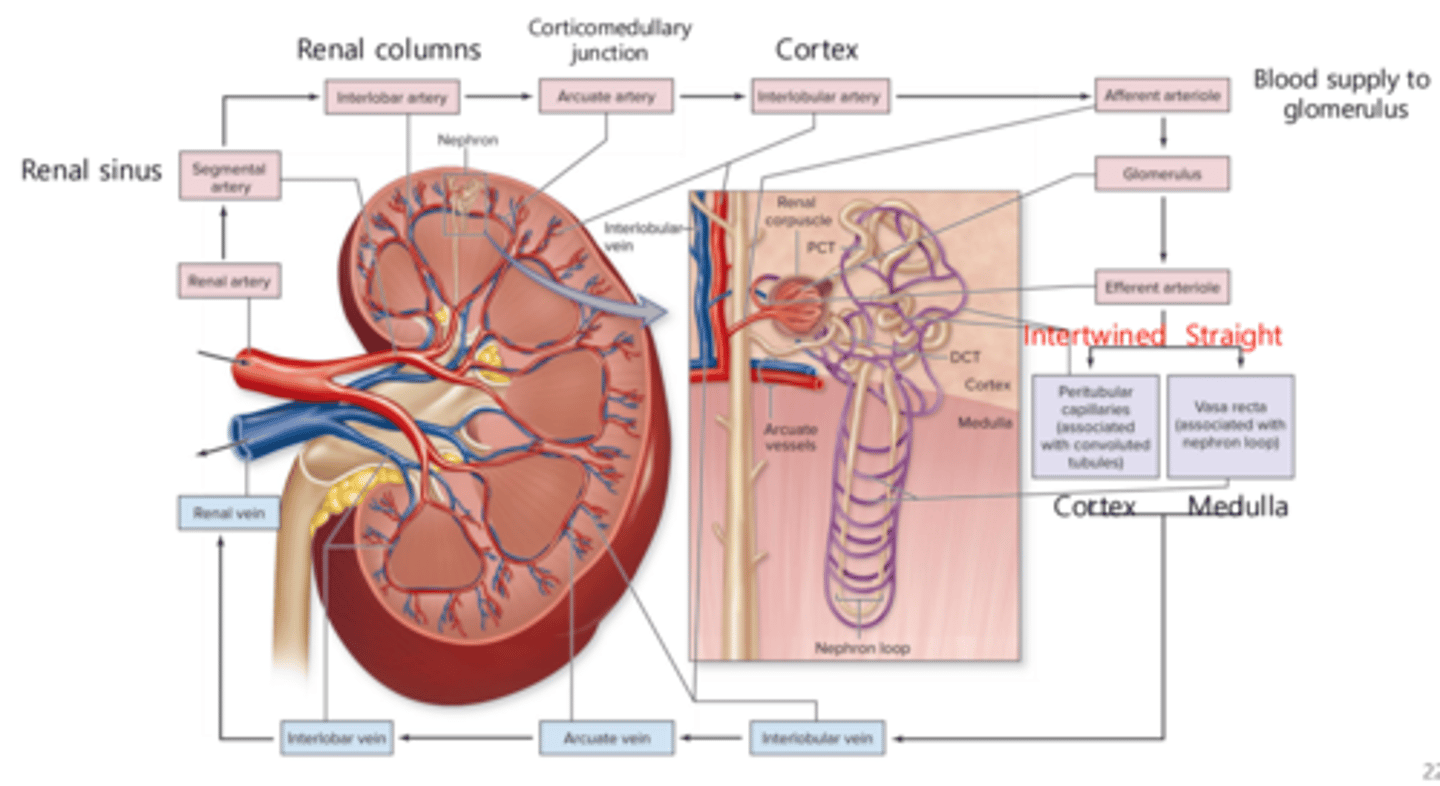
blood flow and filtered fluid flow:
- when blood first enters from the afferent arteriole into the glomerulus, the blood is .
- when the blood reaches the second capillary bed of either the peritubular capillaries or the vasa recta, the occurs.
- the peritubular capillaries and vasa recta then drain into the network of veins
filtered;
exchange of respiratory gases, nutrients, and wastes occurs
when blood flows through the glomerulus and is filtered:
- both water and solutes move from the blood plasma across the filtration membrane.
- and into the Bowman's capsule to form ( )
- then it enter the (it is now called )
*PCT -> loop of Henle - DCT - collecting tubule - collecting ducts...
once the tubular fluid leaves the collecting ducts, it is now called . it now enters the papillary duct -> minor - major calyx - renal pelvis - ureter - urinary bladder - urethra
when blood flows through the glomerulus and is filtered:
- both water and solutes move from the blood plasma across the filtration membrane.
- and into the Bowman's capsule to form filtrate (plasma - large solutes)
- then it enter the PCT (it is now called tubular fluid)
( *PCT -> loop of Henle - DCT - collecting tubule - collecting ducts...)
- once the tubular fluid leaves the collecting ducts, it is now called urine. it now enters the papillary duct -> minor - major calyx - renal pelvis - ureter - urinary bladder - urethra
at what point does tubular fluid transition to urine
once tubular fluid leaves the collecting ducts
three steps of urine formation
1. filtration
2. reabsorption
3. secretion
glomerular filtration
the movement of substances from the blood within the glomerulus into the capsular space
tubular reabsorption
the movement of substances from the tubular fluid back into the blood
tubular secretion
the movement of substances from the blood into the tubular fluid
where does glomerular filtration take place and what is produced
occurs at the corpuscle (across the glomerular capillaries and Bowman's capsule)
- produces filtrate (separated fluid) (plasma has large solutes)
in glomerular filtration, water and solutes are separated from the within the glomerulus. water and solutes cross the filtration membrane to enter . this separated fluid is called .
blood plasma; Bowman's capsule; FILTRATE
tubular reabsorption occurs...
Along renal tubule and collecting duct, mainly in the proximal convoluted tubule (PCT)
- Also occurs in loop of Henle, DCT, and collecting duct under hormonal control
in tubular reabsorption, substances move from --> into (back to blood)
tubular fluid --> into peritubular capillaries (back to blood)
tubular reabsorption occurs via
• Active transport
• Facilitated diffusion
• Osmosis
• Secondary active transport
in tubular reabsorption, typically, all vital solutes and and most water in the filtrate are
• The excess solutes, water, and waste products remain
reabsorbed; within the tubular fluid
tubular secretion (know in comparison to reabsorption!!)
- The movement of solutes (usually by active transport) out of the blood within the peritubular capillaries and vasa recta into the tubular fluid ; solutes --> tubular fluid
- Materials that are moved into the tubules are to be eliminated (excreted) from the body
- materials in tubules excreted!!
secretion results in
excretion
Reabsorption
substances returned to the blood (kept in the body)
Secretion
substances removed from the blood (excreted from the body)