Systemic eye diseases
1/39
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
40 Terms
What is diabetic retinopathy?
damage to the retinal blood vessels due to prolonged high blood sugar
What is the pathophysiology of diabetic retinopathy?
hyperglycaemia damages the retinal small vessels and endothelial cells. Increased vascular permeability leads to leaking vessels, blot haemorrhages and hard exudates.
Damage to the vessel walls leads to microaneurysms and venous bleeding.
Damage to nerve fibres causes cotton wool spots.
Intraretinal microvascular abnormalities refer to dilated and tortuous capillaries in the retina
neovascularisation involves release of growth factors stimulating new vessel development.
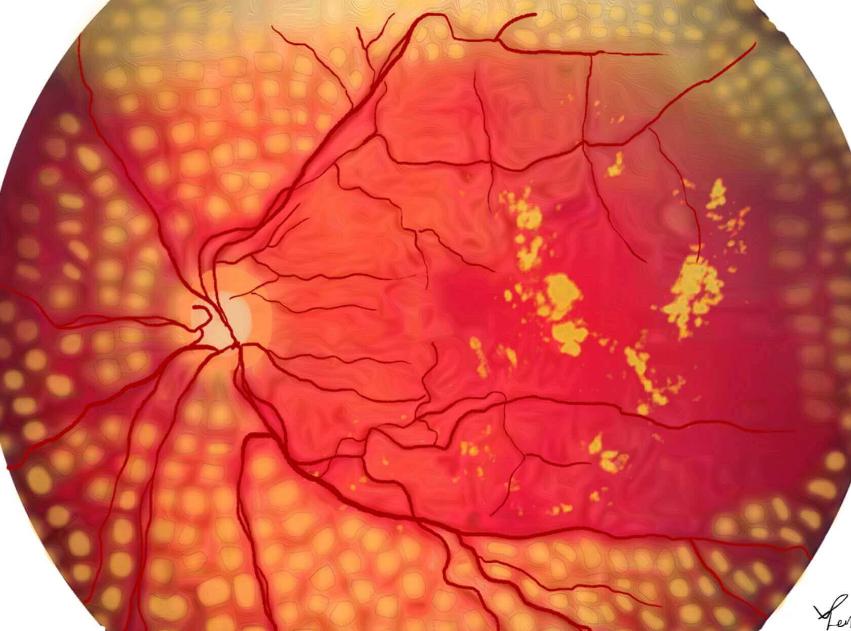
What does a fundoscopy look like in diabetic retinopathy?
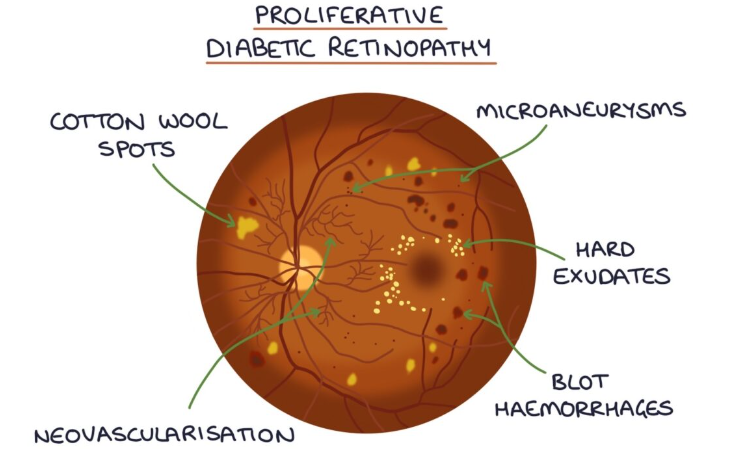
What is background diabetic retinopathy?
microaneurysms, retinal haemorrhages, hard exudates and cotton wool spots
What is pre-proliferative diabetic retinopathy?
venous beading, multiple blot haemorrhages and intraretinal microvascular abnormality (IMRA)
What is proliferative retinopathy?
neovascularisation and vitreous haemorrhage
What are complication of diabetic retinopathy?
vision loss
retinal detachment
vitreous haemorrhage
rubeosis iridis- new blood vessel formation in the iris
cataracts
optic neuropathy
What is the epidemiology of diabetic retinopathy?
most common cause of blindness is adults aged 35-65
What is advice for diabetic retinopathy?
optimise glycaemic control, BP, and hyperlipidaemia
regular ophthalmology review
What is diabetic maculopathy?
has exudates in the macula and macula oedema
based on location rather than severity
check visual acuity
more common in T2
What is the management of non-proliferative diabetic retinopathy?
regular observation
if severe consider pan retinal laser photocoagulation
What is the management for diabetic maculopathy?
if there is a change in visual acuity, then intravitreal vascular endothelial growth factor
What is the management for proliferative diabetic retinopathy?
pan retinal laser photocoagulation- this can cause a reduction in visual fields due to scarring, decrease in night vision due to decrease in rod cells located in the peripheral retina
intravitreal VEGF inhibitors, eg: ranibizumab
vitroretinal surgery
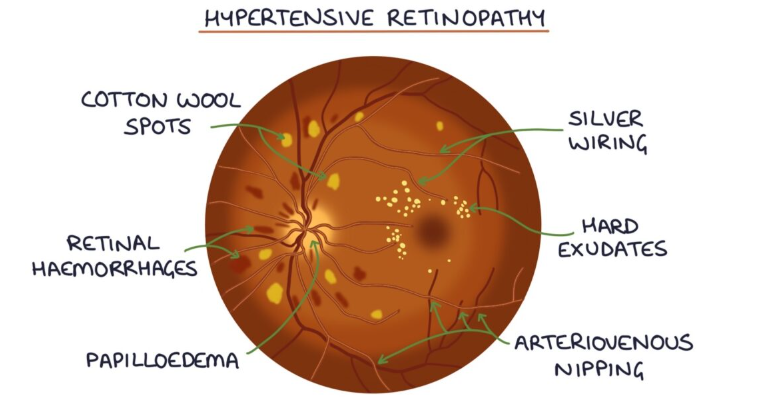
What is hypertensive retinopathy?
damage to the retinal blood vessels relating to hypertension. Changes can happen slowly with chronic HTN or quickly in response to malignant HTN
What are features of hypertensive retinopathy?
silver or copper wiring
arteriovenous nipping
cotton wool spots
hard exudates
retinal haemorrhages
papilloedema
What is silver/copper wiring?
where the walls of the arterioles become thickened and sclerosed and reflect more light on examination
What is Arteriovenous nipping (AV nipping)?
where arterioles cause compression of the veins where they cross due to sclerosis and hardening of the arteries
What are cotton wool spots?
caused by ischaemia and infarction causing damage to nerve fibres
What are exudates?
leakage of lipids from vessels
What are retinal haemorrhages?
caused by damage vessels rupturing and releasing blood to the retina
What is papilloedema?
ischaemia to the optic nerve causing optic nerve swelling
What is the Keith-Wagner classification of hypertensive retinopathy?
1- mild narrowing of arterioles
2- focal constriction of blood vessels and AV nicking
3- cotton-wool patches. exudates, and haemorrhages
4- papilloedema
What is the management of hypertensive retinopathy?
control of BP and manage risk factors (smoking, cholesterol)
What are clinical features of thyroid eye disease?
swelling of the eyelids
oedema and engorgement of vessels of the conjunctiva
exposure of the cornea
exophthalmos
restricted eye movements
optic neuropathy
What is the management of thyroid eye disease?
lid retraction- guanethidine drops to relax smooth muscle
artificial tears
if corneal exposure threatens sight tarsorrhaphy (sewing the eyelids)
What are manifestations of RA on the eye?
episcleritis
scleritis
corneal ulceration
keratitis
How common are ocular manifestation of RA?
25% of patients with RA have eye problems
Which systemic infections can affect the eye?
syphilis
TB
toxoplasmosis
Covid
Ebola
these diseases can present with signs of intraocular inflammation
What haematological conditions can affect the eye?
sickle cell disease
What eye conditions can IBD cause?
episcleritis
uveitis
peripheral ulcerative keratitis
What eye manifestations can MS have?
optic neuritis
optic atrophy
Uhthoff’s phenomenon- worsening of vision following a rise in body temperature
internuclear ophthalmoplegia
What eye manifestations can myasthenia gravis have?
diplopia
ptosis
What dermatological conditions can affect the eye?
acne rosacea
pemphigoid
Steven’s-Johnson
atopic eczema
What can Horner’s present with?
miosis- small pupil
ptosis
enophthalmos- sunken eye
What is optic neuritis?
inflammation of the topic nerve
What are causes of optic neuritis?
multiple sclerosis
diabetes
syphilis
What are presenting features of optic neuritis?
unilateral decrease in visual acuity over hours-days
poor discrimination of colour with red desaturation
pain worse on eye movement
relative afferent pupillary defect
central scotoma- area of depressed vision that interferes with central vision
What investigations are performed for optic neuritis?
MRI of the brain and orbits with gadolinium contrast (a clear colourless fluid used to make images clearer)
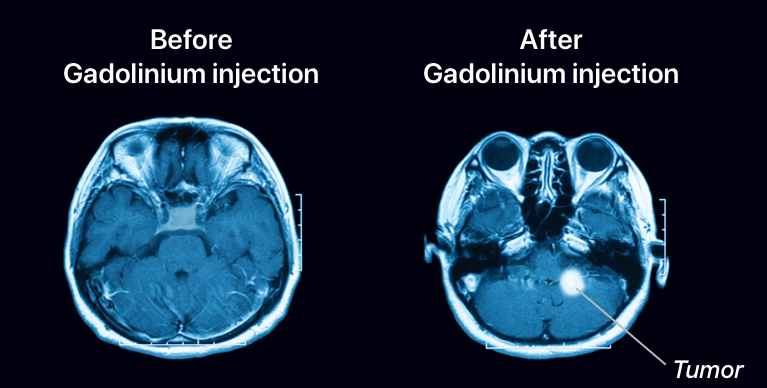
What is the management of optic neuritis?
high dose steroids
recovery can take 4-6 weeks
What is the prognosis of optic neuritis?
if >3 white matter lesions, the 5 year risk of developing MS is 50%