Exam 2 Questions
1/207
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
208 Terms
Which physics law have mass and temp as a constant, but when pressure is altered, the volume of gas also changes in an inverse manner?
boyle’s law
What is the PO2 of atmospheric air?
159mmHg
What happens when diffusion distance increases?
diffusion rate decreases
Which of these helps create recoil tendency?
surface tension of alveolar fluid
Which of these is NOT a force thoracic muscles have to overcome for inhalation?
diffusion partial pressure
Which of these is the term for the maze-like passages in the nose?
conchae
Which layer produces the serous secretions?
submucosa
What cells produce surfactant in the bronchi?
clara cells
Which of these means difficulty breathing?
dyspnea
Which of these explain the relationship between ventilation and perfusion?
If the ratio is < normal then perfusion is good but ventilation is not
If the ratio is > normal then perfusion is good but ventilation is exceeding perfusion of tissues
In the trachea, there are (2 words) ______ that produce mucin that forms a mucus barrier to help trap foreign material. There are also (2 words) _____ that push the foreign material out of the respiratory tract.
goblet cells
ciliated cells
With the oxygen extraction fraction, if the volume of O2 in the blood is 20% and there is a 5% yield, then the fraction of O2 that is given up by the blood to the tissues is 1/4 of the volume.
true
At what pressure of PO2 does hemoglobin release oxygen for gas exchange?
40mmHg
The conchae are important for humidifying inhaled air. This is why it is well vascularized.
true
How is physiologic dead space different from residual volume?
Physiologic dead space involves inspired air that isn't involved in gas exchange, while residual volume is the amount of air left in the lungs after expiration.
Which of these are factors the muscle work of the lungs has to overcome?
elastic and surface tension forces
non-elastic forces
airway resistance
The purpose of (2 words) ______ is to help expel air out of the lungs. This is due to the stretched elastin fibers wanting to snap back to a relaxed state.
look at quiz 5
Functional residual capacity is the sum of inspiratory reserve volume and residual volume.
false
Which of these are cells found within the alveoli?
Pneumocytes Type I
Pneumocytes Type II
Dust cells
Hypoxic vasoconstriction response is activated by the PO2 of the alveolar gas, not the PO2 of pulmonary arterial blood
true
When distance of diffusion (1 word) ______ diffusion rate (1 word) ______ due to the change of distance inhibiting efficient exchange
increases
decreases
What is the relationship with intrapulmonic pressure during inspiration and expiration?
During inspiration, the pressure becomes subatmospheric (negative) while expiration becomes higher than atmospheric (positive). This helps the movement of air into and out of the lungs.
Which of these is the term for labored breathing?
Dyspnea
Why is having surface tension with no buffer in the lungs problematic?
The pressure required to inflate the lungs increases with the decrease in radius, making it more difficult to fully inhale
Which is related to decreased ventilation?
hypoventiliation
What activates hypoxic vasoconstriction?
alveolar PO2
At what PO2 do we see 97.5% saturation?
100 mmHg
On the pulmonary side, which directions do bicarb and Cl- go in the RBCs?
bicarb in, Cl- out
Amount of air breathed in or out during a respiratory cycle
tidal volume
Amount of air that can still be inspired after inhaling the tidal volume
inspiratory reserve volume
Amount of air that can still be expired after exhaling the tidal volume
expiratory reserve volume
Amount of air remaining in the lungs after the most forceful expiration
residual volume
Sum of all volumes
total lung capacity
Sum of all volumes over and above the residual volume; it is the maximum amount of air that can be breathed in after the most forceful expiration
vital capacity
Sum of the tidal and inspiratory reserve volumes
inspiratory capacity
Sum of the expiratory reserve volume and the residual volume
functional residual capacity
Put in order the pathway of air through the respiratory system
nose/mouth →
larynx →
trachea →
bronchi →
primary bronchioles →
terminal bronchioles →
respiratory bronchioles →
alveolar ducts →
alveolar sacs →
alveoli
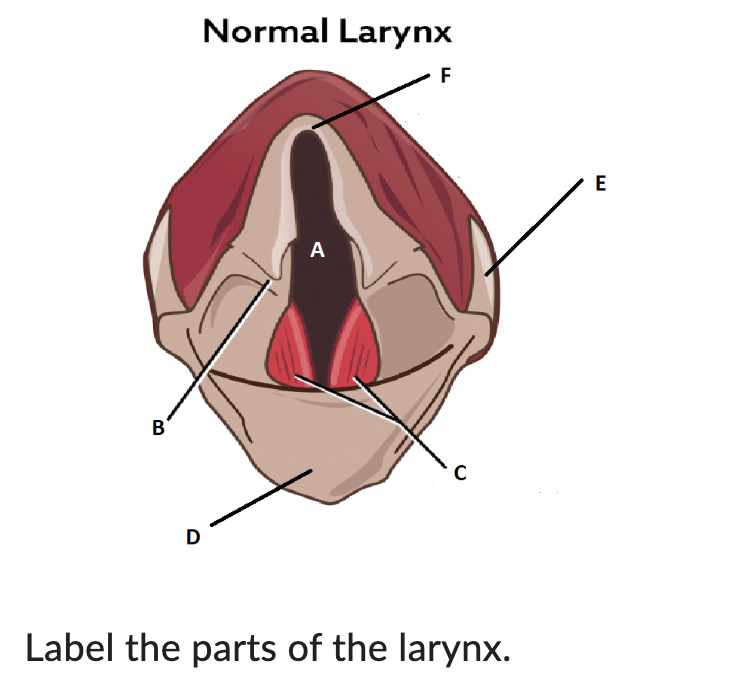
A
glottis
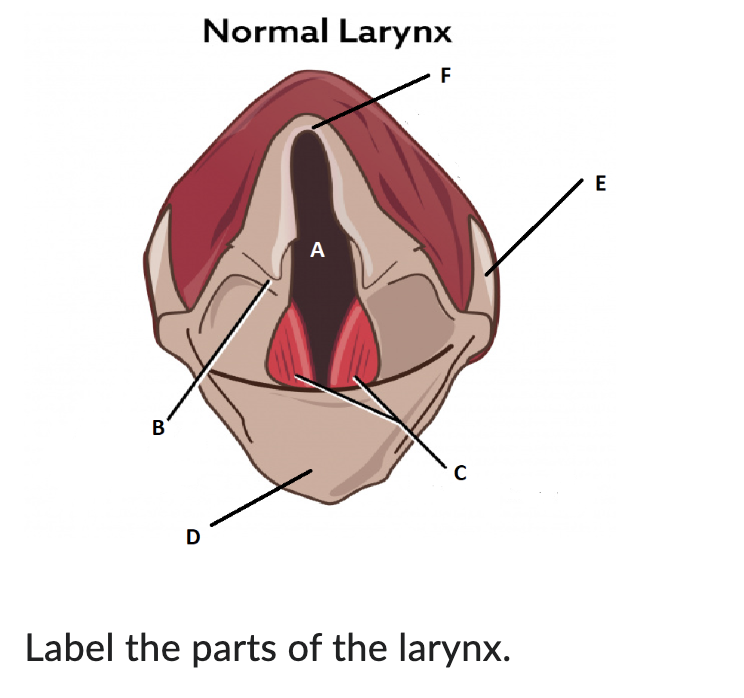
B
arytenoid cartilage
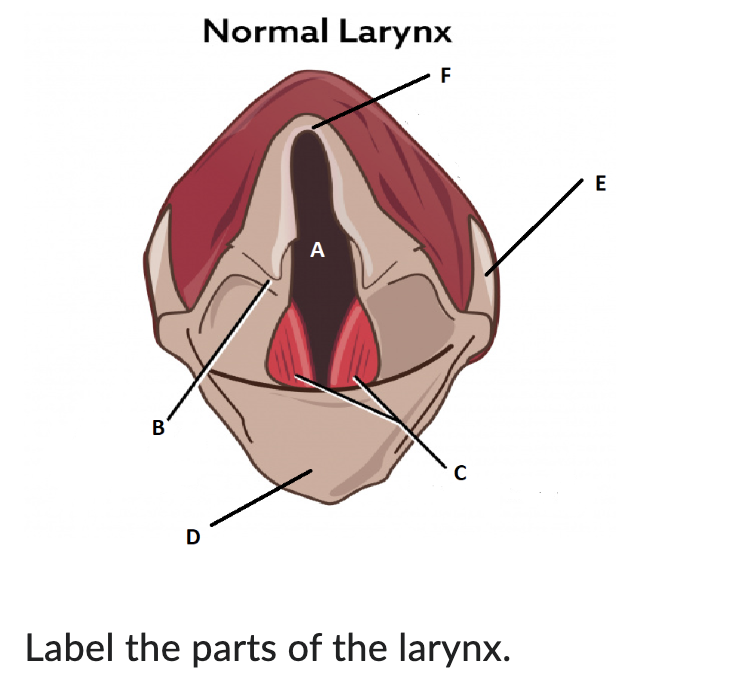
C
vocal cords
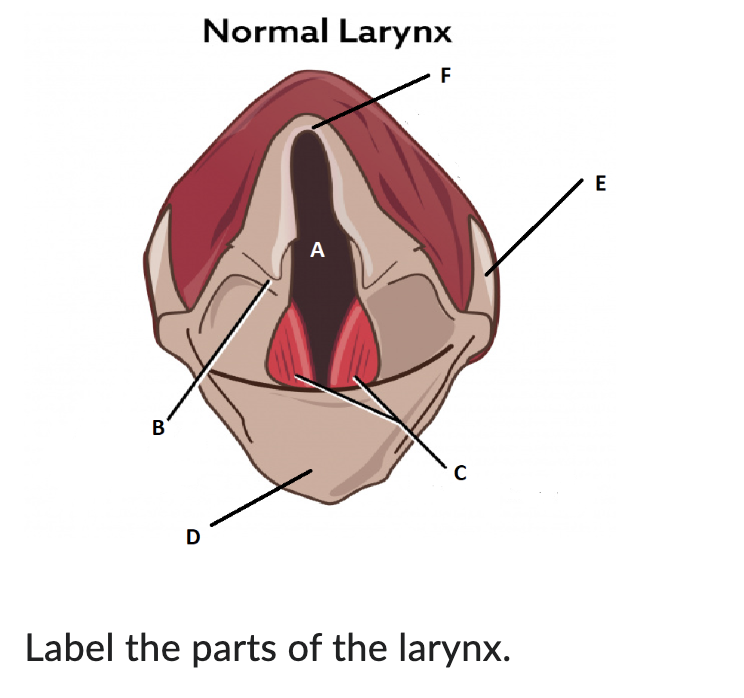
D
epiglottis
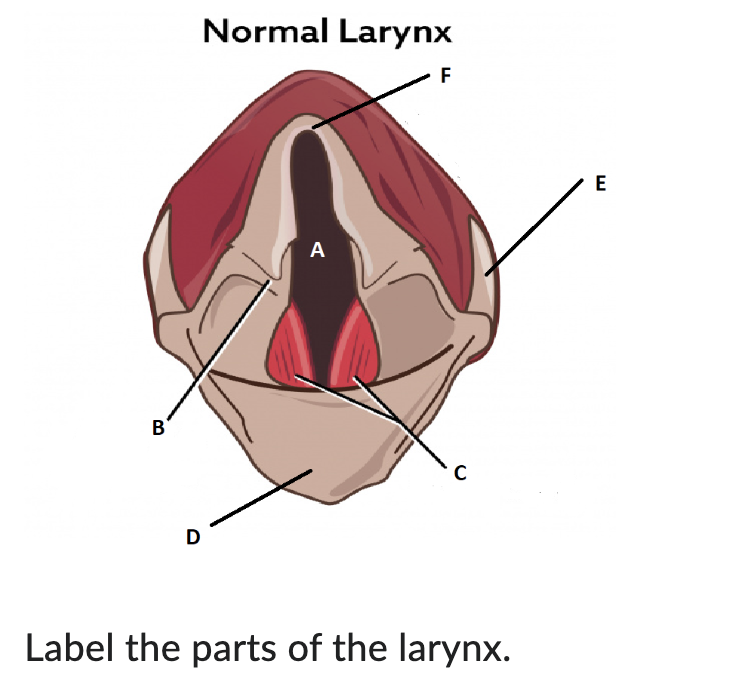
E
thyroid cartilage
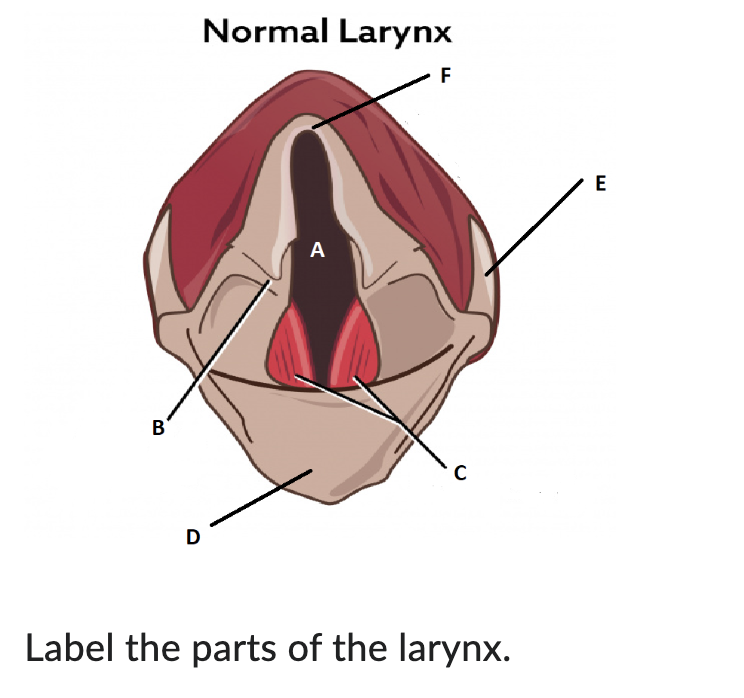
F
cricoid cartilage
Secrete mucin and create a protective mucus layer
goblet cells
Use finger-like projects to help expel foreign material
ciliated cells
Responsible for normal cell replacement and epithelial remodeling upon lung injury
basal cells
Non-ciliated cells that produce and secrete surfactant components
clara cells
Cells that perform gas exchange
Pneumocytes type I
Secretory cells that fuse with the cell membranes and secrete pulmonary surfactant
Pneumocytes type II
Mobile scavengers that engulf foreign particles in the lungs
Alveolar macrophages/ dust cells
Recoil tendency of the lungs is due to fibrous collagen fibers holding lung structure and surface tension of the alveolar fluid.
false
Which of these is NOT a layer of the trachea?
serosa
In the OHDC, a shift to the (1 word) ______means there is an increased affinity for O2, and therefore, less O2 that is yielded into the tissues. A shift to the (1 word) _____ means there is decreased affinity for O2, and therefore, more O2 is yielded into the tissues
left
right
Normal quiet breathing with no deviation in frequency or depth
eupnea
Difficulty breathing, where visible effort is required to breathe
dyspnea
Breathing with increased depth, frequency, or both, and is noticeable after physical exertion
hyperpnea
Rapid shallow breathing, similar to panting
polypnea
A cessation of breathing
apnea
Excessive rapidity of breathing
tachypnea
Abnormal slowness of breathing
bradypnea
When discussing the ventilation:perfusion ratio, why are the naturally different between the dorsal and ventral aspects of the lungs?
Gravity influences the ability of the blood to travel to different sections of the lung. Dorsal aspect has less perfusion but more ventilation and ventral has more perfusion but less ventilation to balance this out.
The (1 word) _____are the next part after the trachea. These have less goblet cells, but still contain a partial cartilage ring. The (1 word) ____ are the next section after that. They don't have any goblet cells and have no cartilage.
bronchi
bronchioles
In normal ventilation, there is (3 words)______ in which some of the air doesn't come in contact with capillaries to allow perfusion. This is a normal event to help cool the body and humidify the air.
physiologic dead space
What is the purpose of hypoxic vasoconstriction?
Redirect blood away from deoxygenated to well oxygenated areas to keep perfusion rate consistent
In the ventilation: perfusion ratio, what does it mean if the ratio is less than normal?
Perfusion is normal but ventilation is not
What is the relationship between intrapulmonic and intrapleural pressures in relation to respiration?
Intrapleural creates the negative pressure system that helps keep the lungs inflated during inspiration when intrapulmonary and atmospheric pressures equalize out.
Which of these is NOT a factor that can lead to the reduction of O2 pressure in the lungs, blood, and tissues?
Large quantity of O2 concentration is consistently exhaled with CO2
Volume of gas moved in or out of airways and alveoli over a certain period of time
total ventilation
Total volume of gas moved in or out of airways and alveoli in 1 min
minute ventilation
Alveolar ventilation increased beyond metabolic needs and a PACO2 below 40 mmHg
hyperventilation
Disturbances of acid–base equilibrium where the pH of blood [H+] is increased or decreased, respectively, from normal
Respiratory alkalosis/acidosis
Normal ventilation in which a PACO2 of about 40 mmHg is maintained
Normoventilation
Made up of alveoli with diminished capillary perfusion, and little or no diffusion of oxygen and carbon dioxide through the membranes of most of the airways
Dead space ventilation
Alveolar ventilation decreased below metabolic needs and a PACO2 above 40 mmHg
hypoventilation
Which of these is NOT part of the right lung?
Caudal part of the cranial lobe
Lipid-soluble substances, such as electrolytes, cannot diffuse freely through the capillary wall. On the other hand, water-soluble lipid-insoluble substances, such as oxygen and carbon dioxide, can diffuse freely through the wall.
false
Abdominal breathing is done when something in the chest is painful. Costal breathing is the normal type of breathing that an animal does when there is no clinical illness.
false
In the oxygen-hemoglobin dissociation curve, when the PO2 has reached its maximum pressure of 100mmHg, the saturation level of hemoglobin is also at max of 97.5%. This means that the blood is fully oxygenated.
true
How is the blood cooled for the brain?
Smaller arteries are bathed in venous blood before they feed into larger vessels for the brain
Which physical force is associated to tiny particles in alveoli?
brownian motion
Which of these is NOT a way a particle is gotten rid of?
Insoluble particle diffusion into blood
What is the purpose of panting?
Heat dissipation
Which term means low O2 content in arterial blood?
Hypoxemia
Which part of the respiratory center system has the primary job of inhibiting inspiration?
pneumotaxic center
Which of these is NOT a location for Hering-Breuer reflex receptors?
heart
What causes respiratory alkalosis?
decreasing PaCO2
What's the purpose of the braking effect?
LOOK AT TOPHAT
What is the purpose of the renorenal reflex?
Balances renal excretory function between kidneys, especially when there is damage to one.
Which of these methods are related to alveolar clearance?
Alveolar macrophages phagocytose foreign material
Foreign material is solubilized by alveolar fluid and drained into lymph tissue
Particles migrated to mucus blanket of tracheobronchial system
The respiratory center has 4 parts. The apneustic center has no known job. The (2 words) ______ limits inspiration. The (3 words) ______ helps set up the respiratory rhythm with the DRG, though it focuses mostly on expiration. The (3 words) ______ also helps set up the respiratory rhythm, but focuses more on inspiration.
pneumotaxic center
ventral respiratory group
dorsal respiratory group
Which term is related to poor O2 saturation due to low PO2 in the atmosphere, usually from being at high altitudes?
Ambient hypoxia
What is the advantage of having receptors in the skin and joints/tendons in relation to the Hering-Breuer Reflex of respiration?
Skin receptor stimulation helps start the breathing cycle of newborns, and joint/tendon receptor stimulation increases respiration rate during exercise.
What is the purpose of the upper air passage reflex?
Protect the respiratory tract from harmful substances that may be inhaled
Which of these is NOT part of the respiratory center?
Rostral ventromedial medulla
What is the difference between corticomedullary and juxtamedullary nephrons?
Corticomedullary has nephrons mostly in cortex with a short loop of Henle. Juxtamedullary has nephrons in cortex close to medulla and have a long loop of Henle
Particle size can dictate where it gets trapped in the respiratory system. Larger particles are more often found deep into the lower respiratory while smaller particles tend to stay more in the upper respiratory
false
What are the specialized cells of the bladder?
Transitional cells
What is the name of the smooth muscle of the urinary bladder?
detrusor muscle
The braking effect promotes the loss of CO2 and H+ to prevent massive changes to the body fluid's pH. It does this by increasing the alveolar respiration.
false
What happens when an animal has atelectasis?
It is a failure of the alveoli to open or remain open and usually involves one or more relatively small areas of lung