ANS 220 Exam 3
1/144
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
145 Terms
How is the estrous cycle divided into 2? And sections within them?
Based on ovarian structures:
1) Follicular Phase
2) Luteal Phase
Based on hormone profiles:
1) Proestrus
2) Estrus
3) Metestrus
4) Diestrus
1 and 2 are in follicular phase with estrogen from follicle
3 and 4 are in luteal phase with progesterone from CL
Dominant structure and hormone during follicular phase?
Dom structure: preovulatory follicle
Dom hormone: estrogen
What starts follicular phase? What ends it?
Regression of corpora luteum (CL)
Ovulation
What percent of cycle is follicular phase?
25-33%
Draw graph of cycle with follicular area boxed in
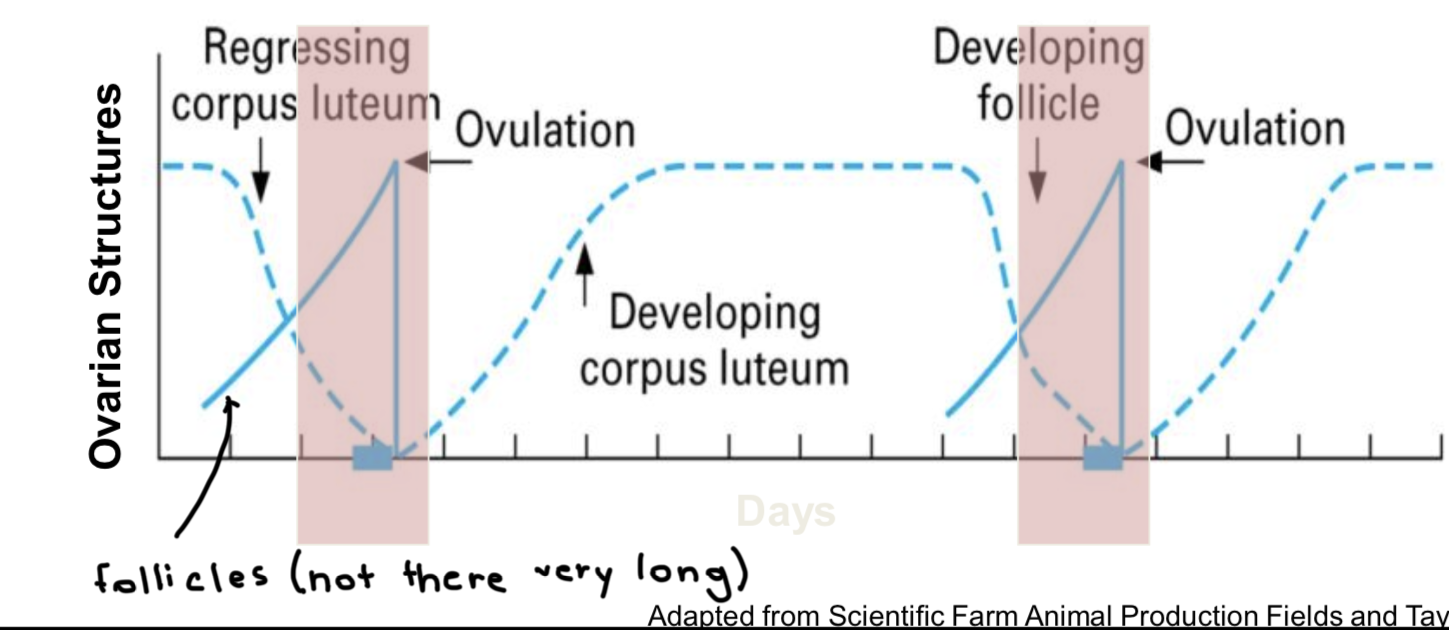
Dominant structure and hormone during luteal phase?
Dom structure: corpus luteum
Dom hormone: progesterone
What starts luteal phase? What ends it?
Starts with ovulation
Ends with luteolysis
What percent of cycle is luteal phase?
66-75%
Draw graph of cycle with luteal area boxed in
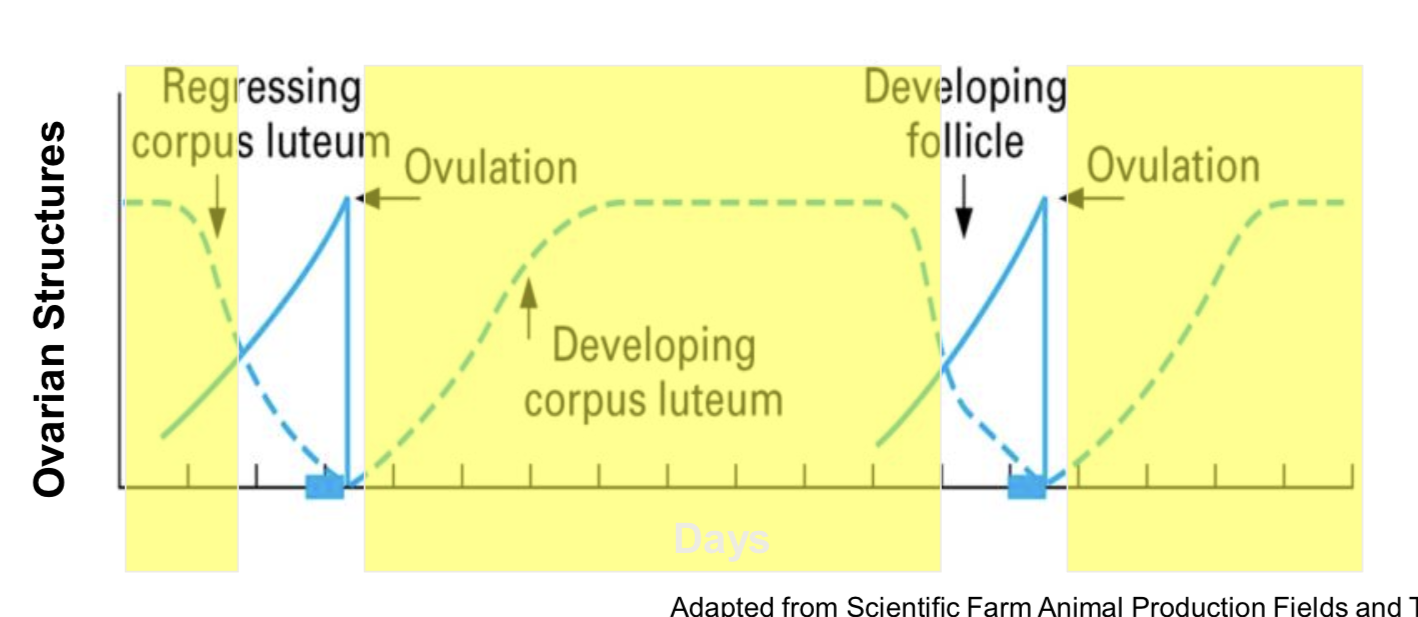
Main goals of follicular vs luteal phase
Growing follicle - preparing to ovulate
Growing CL - preparing for pregnancy
Which phase is target for understanding?
Luteal b/c longest
4 estrous phases graph with E2 and P4 drawn on
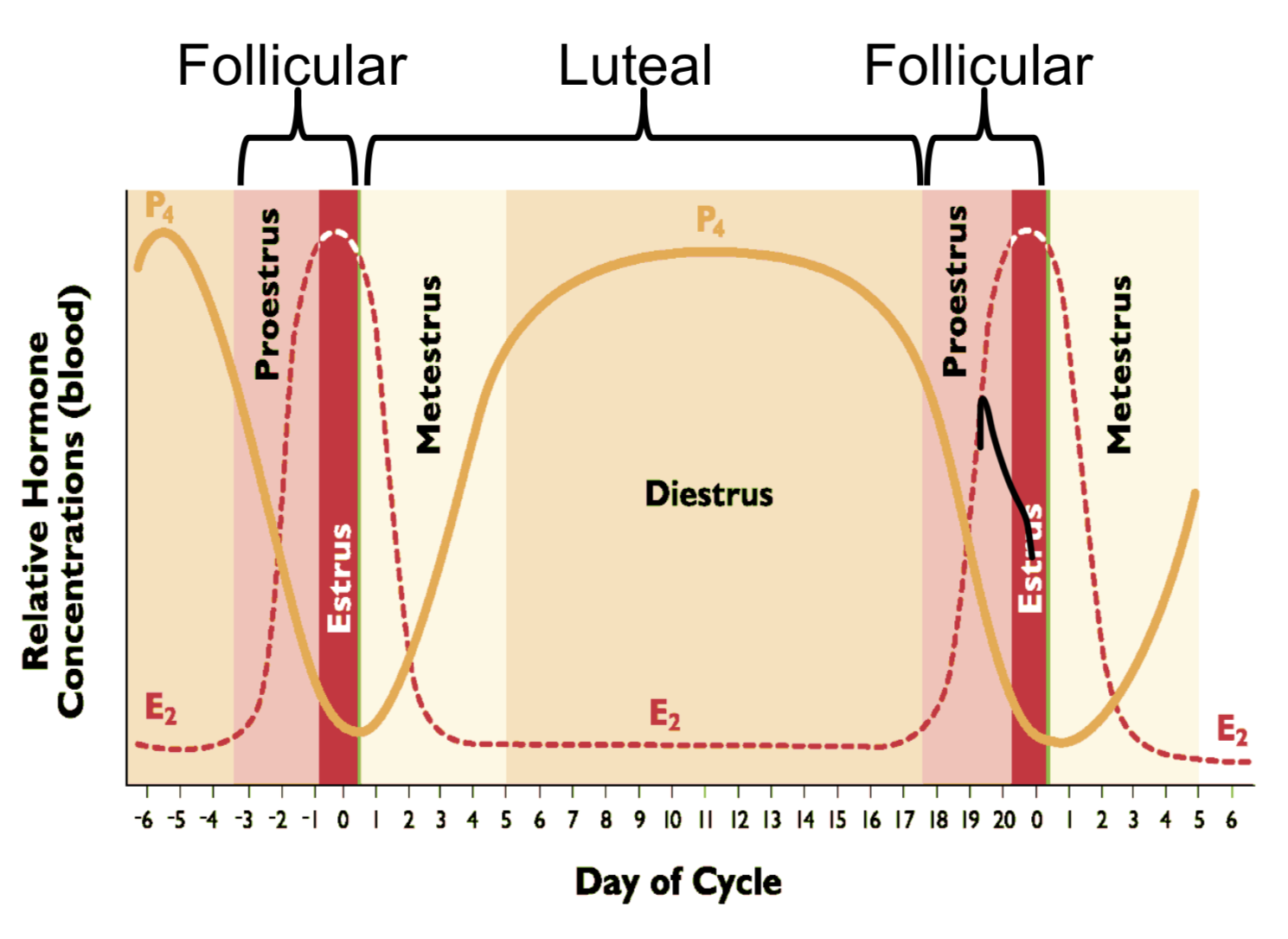
What happens to hormones during proestrus? Draw graph. What is proestrus called?
Increasing E2 - follicles growing
Decreasing P4 - CL regressing
Transition stage
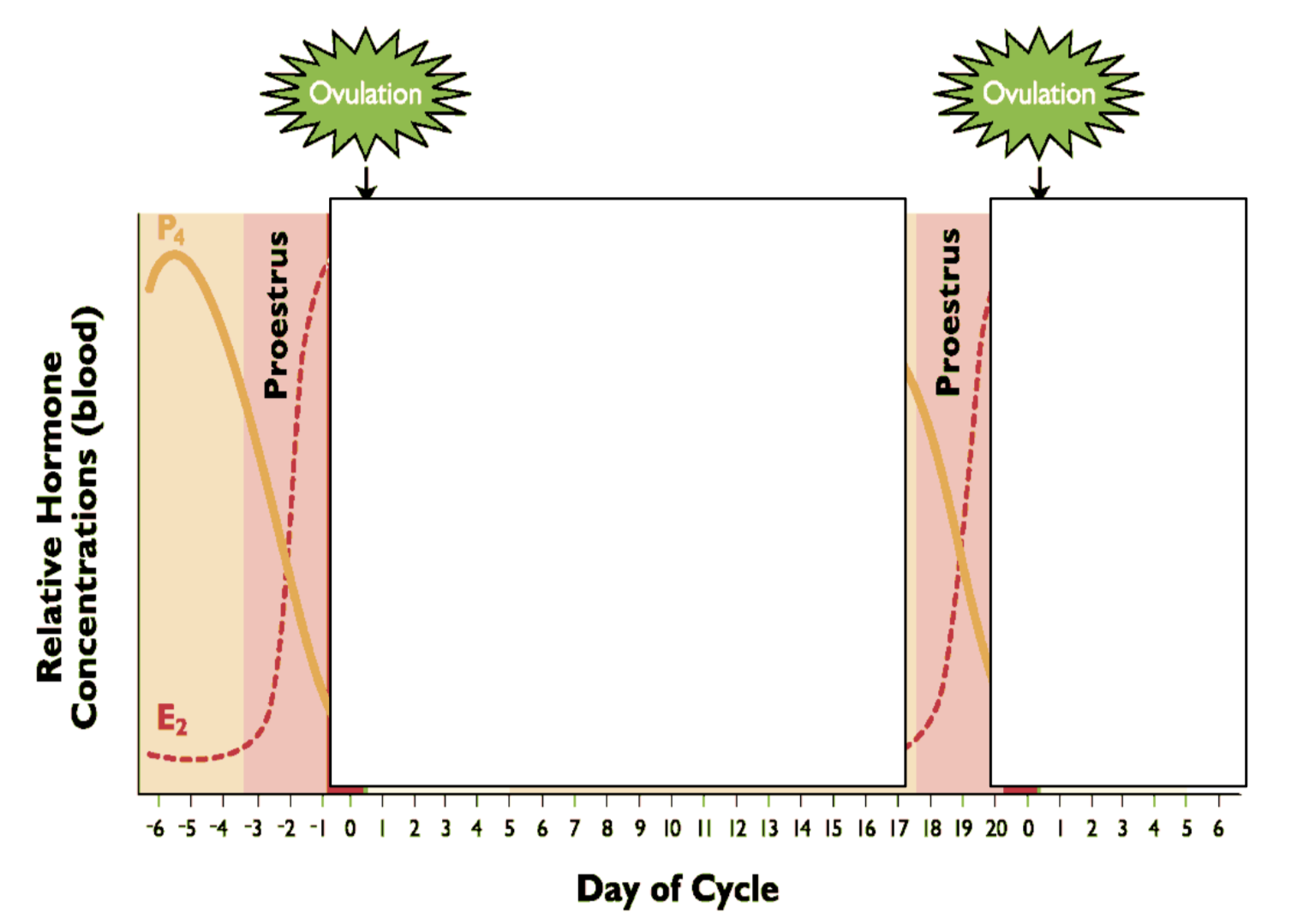
What happens to hormones during estrus? Draw graph. What is estrus called? What is it the period for? LH and FSH? Ovulation?
Peak E2 - max follicle size
Lowest P4
Called heat b/c body temp increases
Period of sexual receptivity
LH and FSH surges due to increased feedback from E2
Ovulation during estrus
-Mare and sow
-Long estrus time
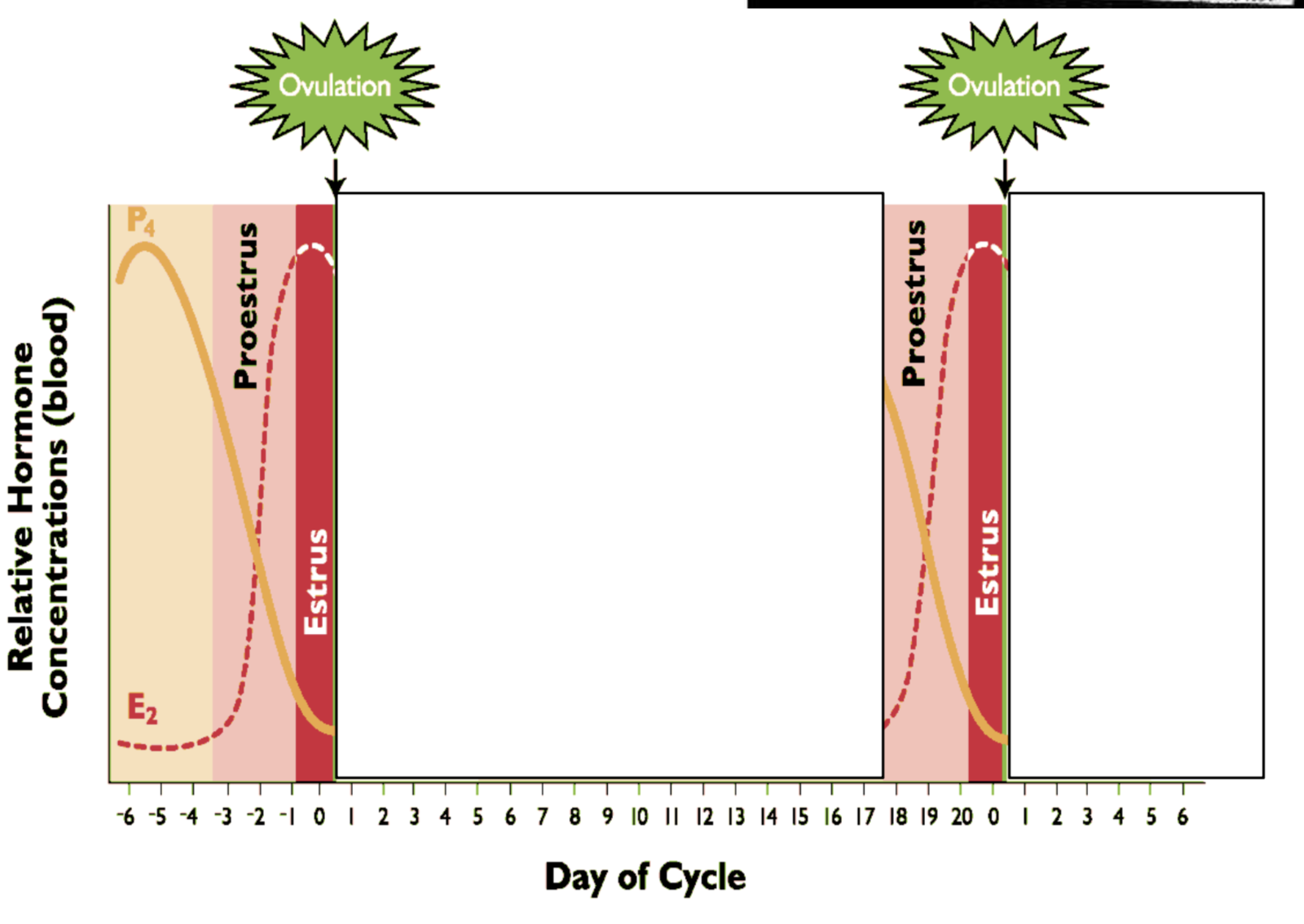
What happens to hormones during metestrus? Draw graph. What is metestrus called? Ovulation?
Increasing P4 - formation of CL following ovulation
Low E2 and LH
Transition stage
Ovulation in metestrus
-Cow and ewe
-Short estrus time (hours); while LH surge has been initiated it takes time to activate system
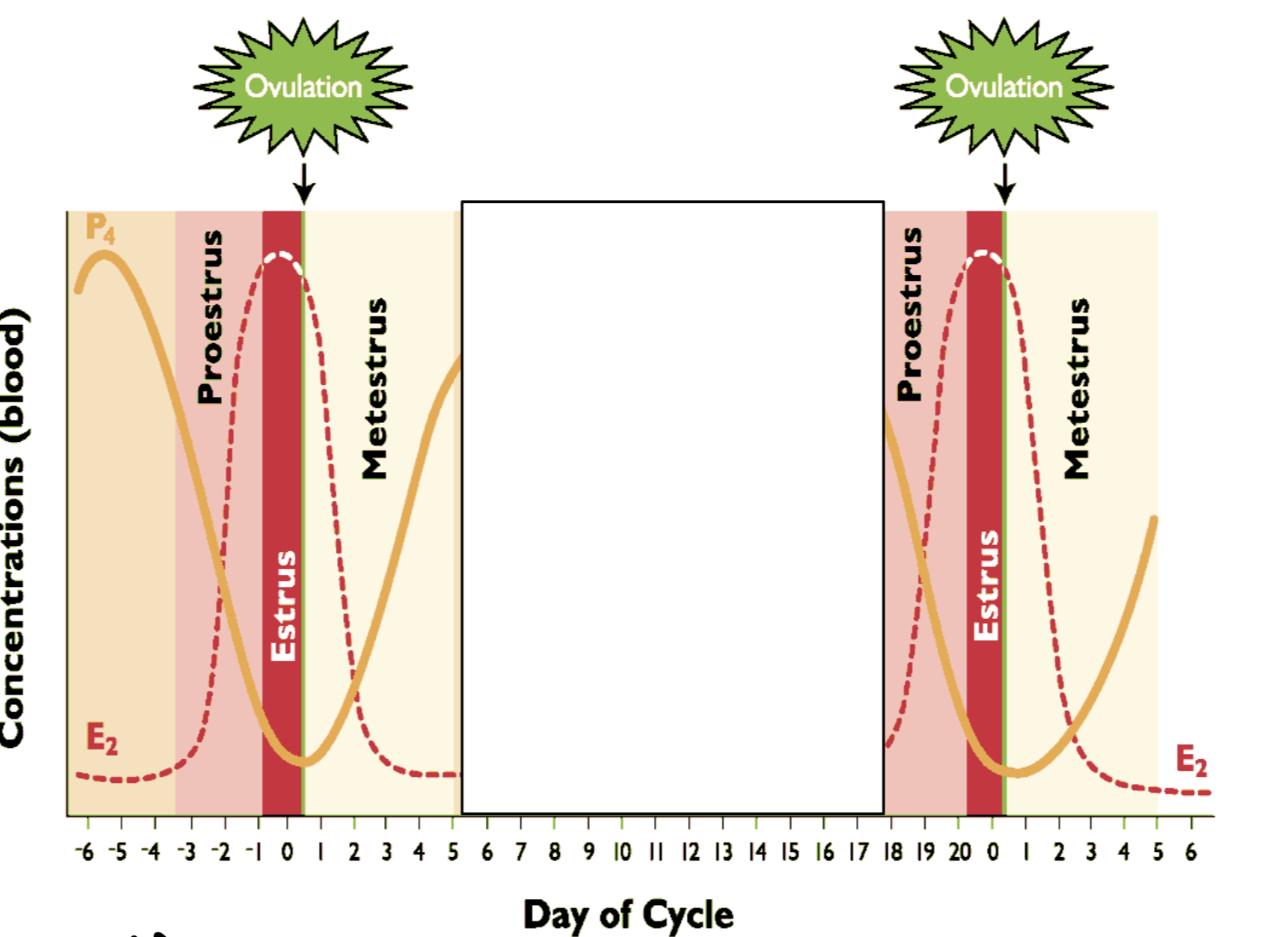
What happens to hormones during diestrus? Draw graph. LH and FSH? How long is diestrus?
Max P4 production - CL is dominant structure
Lowest E2 though follicles continue to grow in waves and undergo atresia in domestic livestock so small increases
Tonic secretions of LH and FSH but not surge secretions b/c P4 blocks it
Longest period of cycle
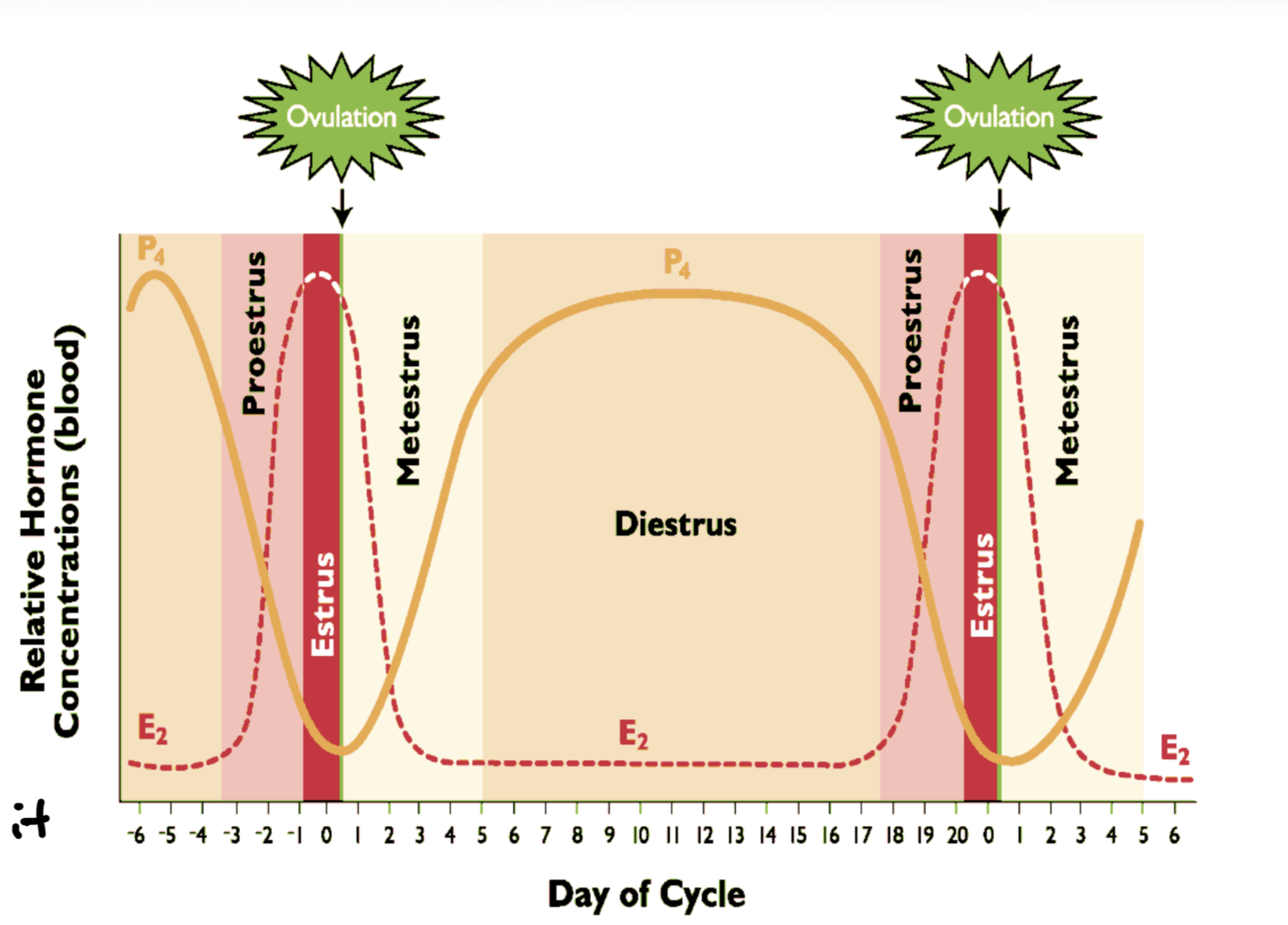
Species Comparison Estrus Length vs Ovulation
Cattle, Sheep, Goats: short estrus, ovulate in metestrus
Swine, Horses: long estrus; ovulate in estrus
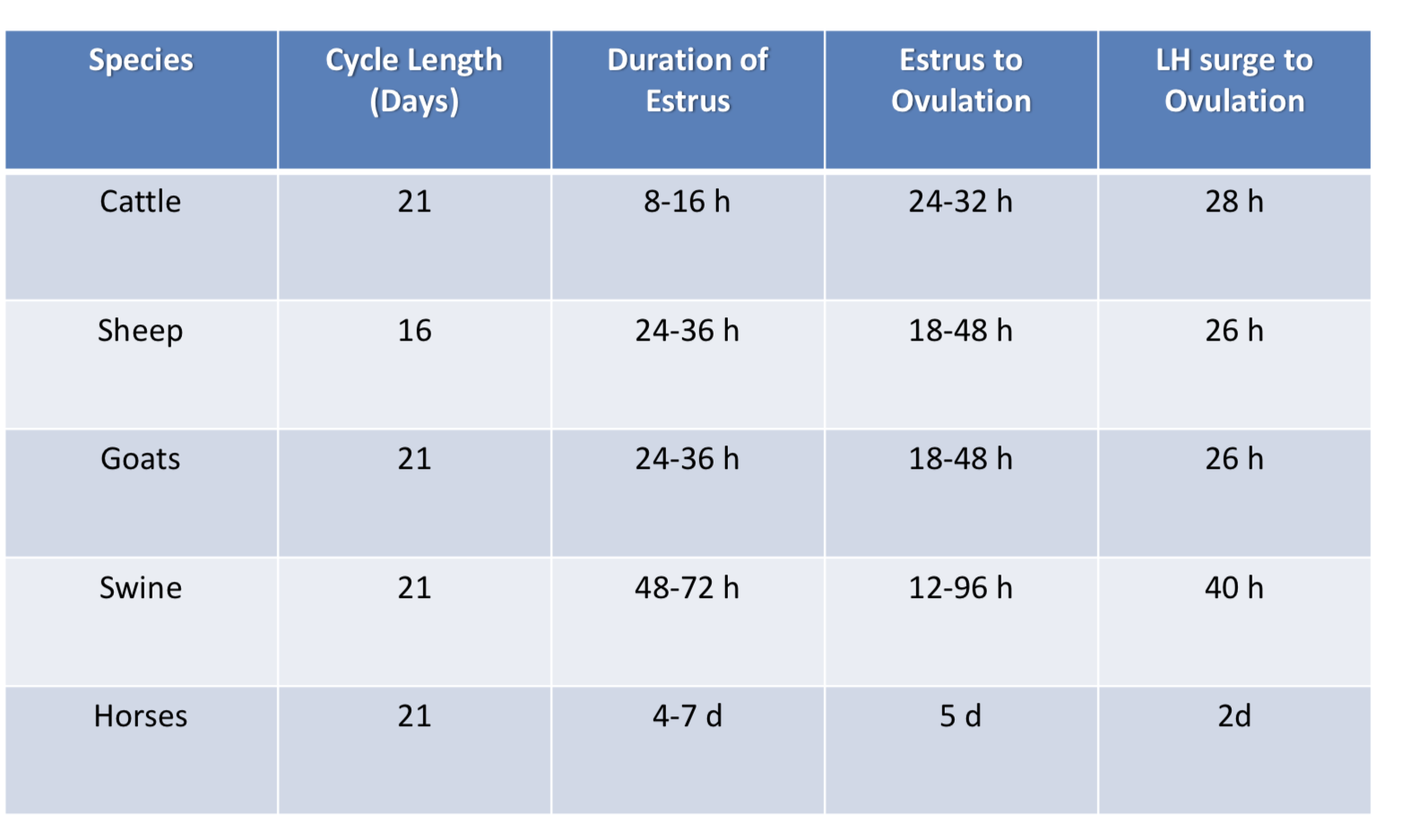
Review types of cycles and ovulators
Cycles:
Polyestrus: cats, swine
Monoestrus: cows, dogs
Seasonally polyestrus: horses, sheep, goats
Ovulators:
Spontaneous: cows, pigs, sheep, horses
Induced: cat, rabbit
Estrous and Menstrual Cycles Difference. Time difference. Ovulation time. What animals is menstrual?
Cycle based on what we see
-Menses (sloughing of endometrial lining) vs estrus (sexual receptivity)
Menstrual: 50 follicular, 50 luteal
Estrous: 25 follicular, 75 luteal
Ovulation on day 14 of 28
Primates
Does menses have clear sexual receptivity period?
No
Menstrual cycle sequence events (6)
1) Menstruation
2) Follicular Growth
3) Ovulation
4) Lutenization - formation of CL
5) Endometrial growth - thickening for embryo
6) Luteolysis - decreases P4 so support for endometrial lining leaves so menses
1-3 are follicular phase and 4-6 are luteal phase
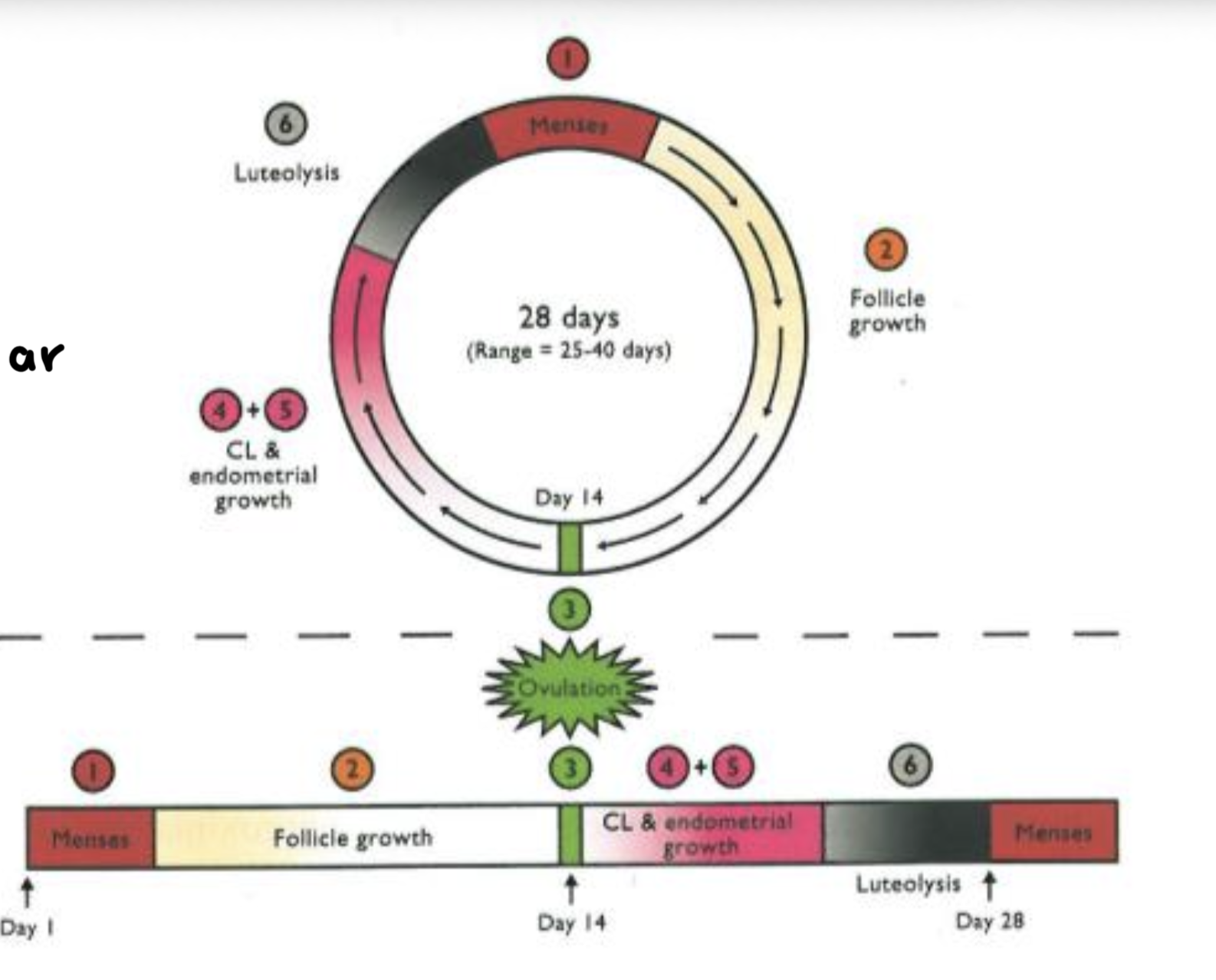
Estrous vs menstrual cycle timeline
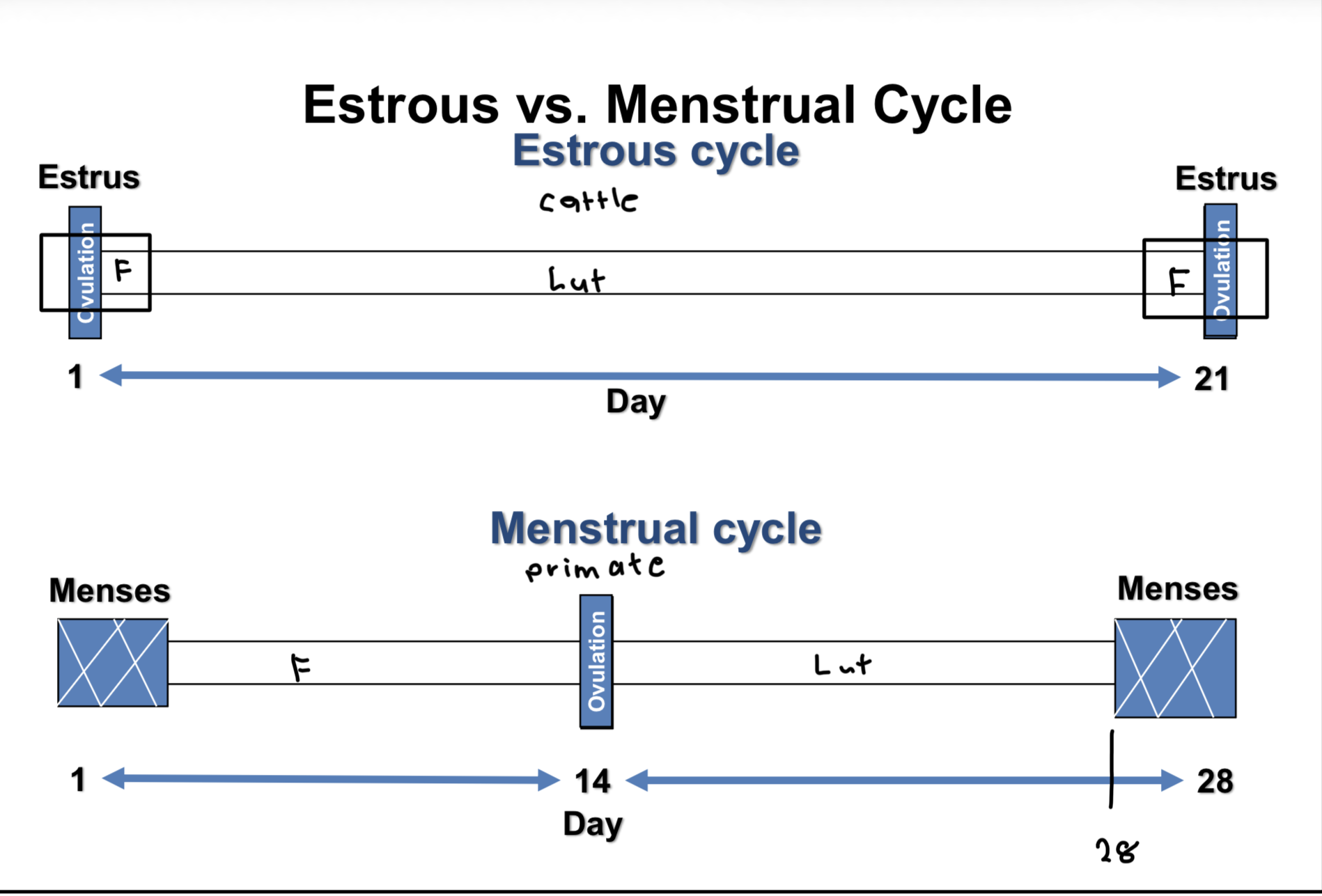
Estrous vs menstrual cycle graphs
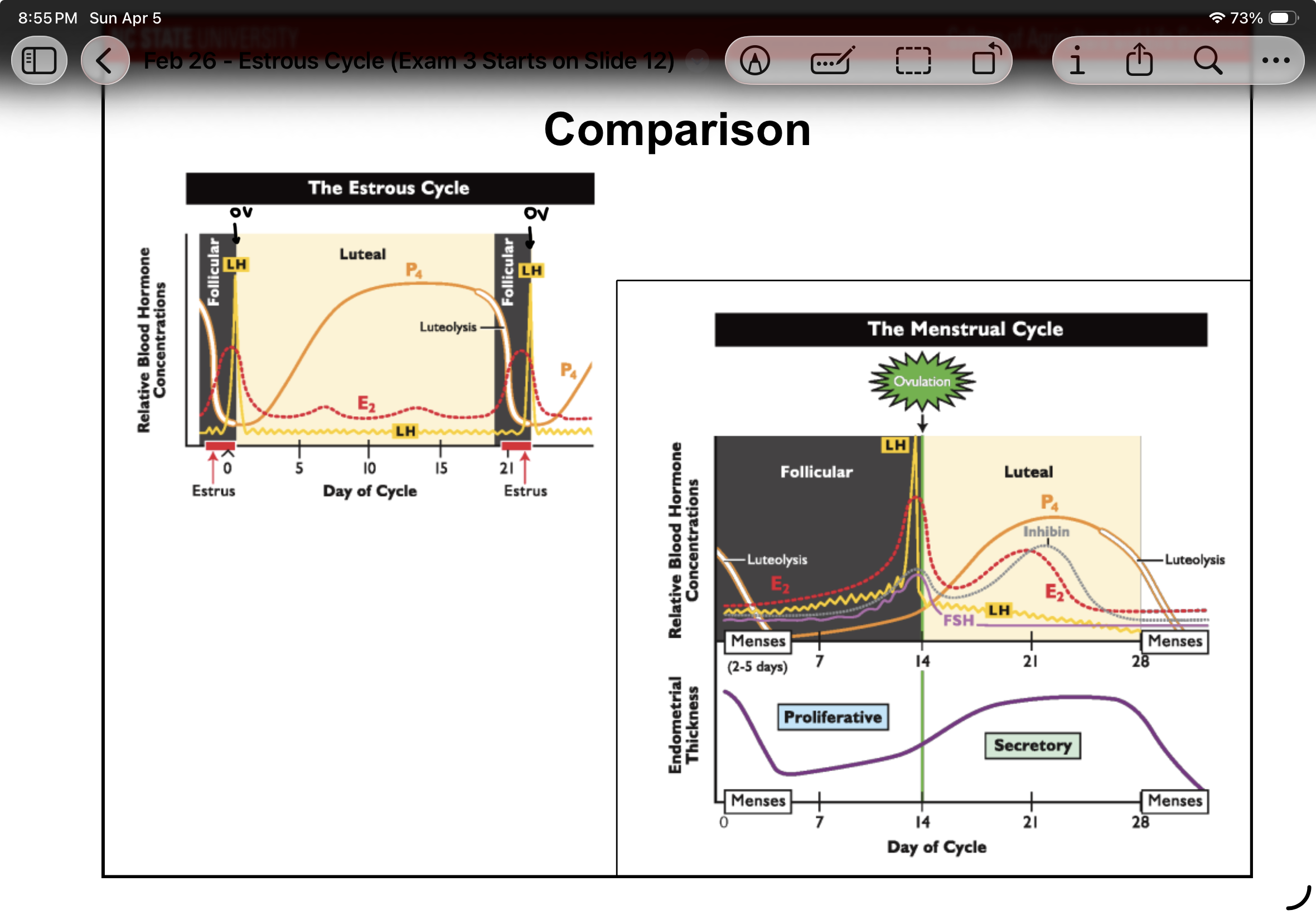
Different estrogen graph curves?
Ruminant: estrogen peak prior to ov
Mare or sow: estrogen higher at ov
What does FSH curve look like? What does it cause?
Tonic release but blip at ov
Increases E2
What does PGF2a do? Where does it come from?
Increase amplitude and frequency before ov to kill CL
Uterine endometrium
Full hormone graph
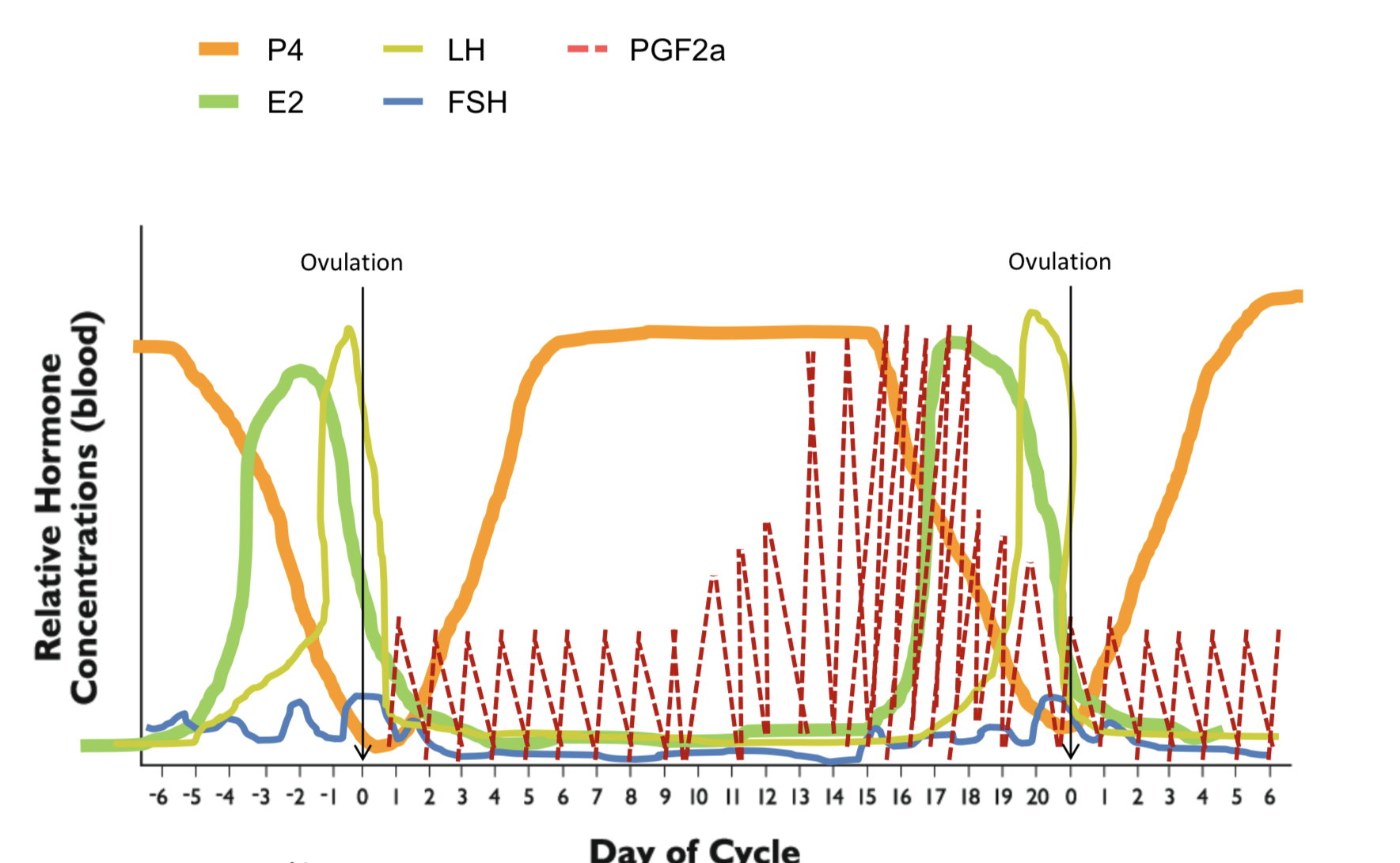
Graph description of order
↑ FSH → ↑ E2 → + feedback loop → LH surge → ovulation → CL forms → ↑ P4 → not pregnant→ ↑ PGF2a → ↓ P4 → beginning
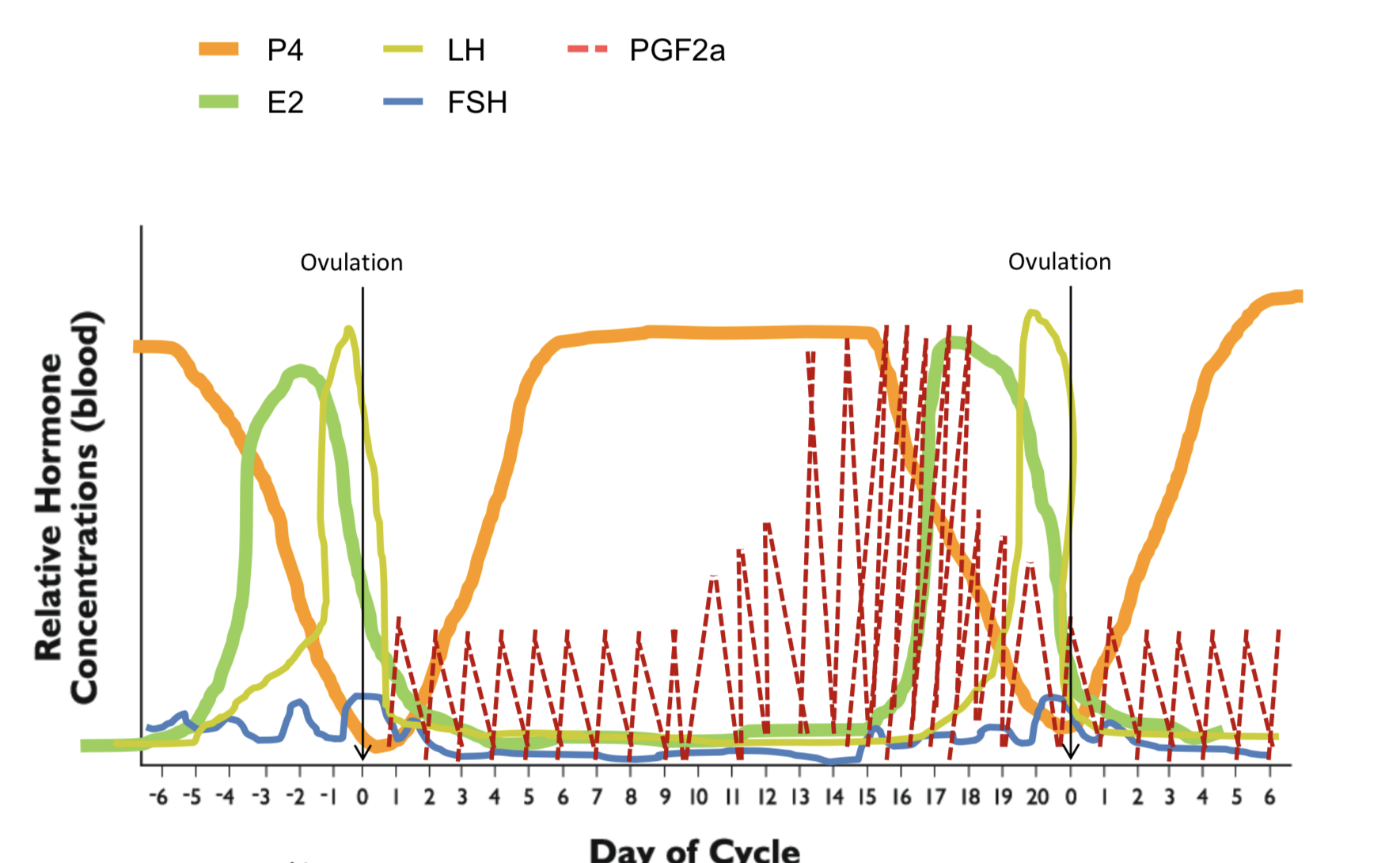
Parts of follicle and process
Oocyte - all follicles have one
-Oogenesis - development of oocyte
Theca cells: produce T that goes into granulosa
Granulosa cells: makes E2 from T
-Cumulus surrounds oocyte
-Mural surrounds other
Follicular fluid
-Nutrients
-Cell communication
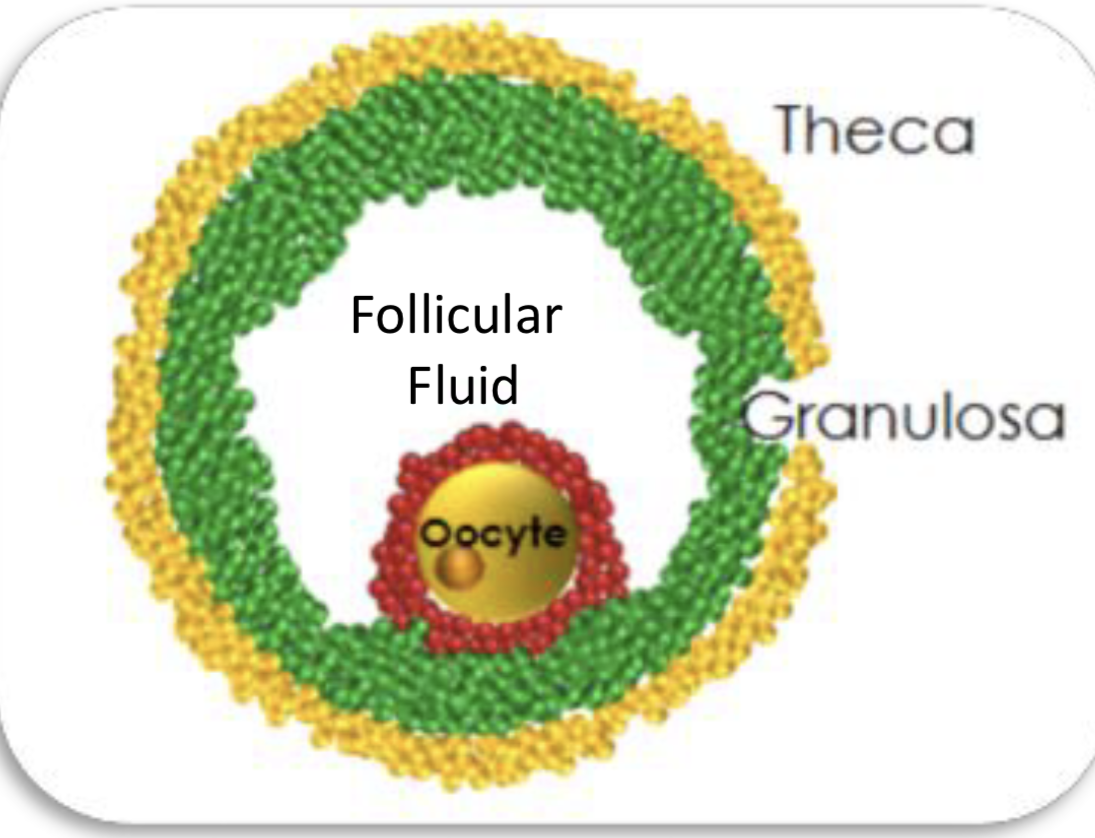
Parts of oocyte
Zona pellucida: thick hardened shell for protection and assists fertilization as sperm cells bind to it
Perivitelline space: air sac buffer btwn two layers
Vitelline/plasma membrane: surface layer of oocyte
Cytoplasm (yolk): contains proteins, enzymes, nutrients, needed for survival of zygote
-Has all needed for mitosis and meiosis
Germinal vesicle: nucleus containing genetic info
What is final stage of embryo development
Zygote
Describe oogenesis and some stages
Oogenesis: formation and development of ovum (egg)/gamete
Primordial germ cells are start
-Fixed # encapsulated in tunica albuginea + loss from medulla region
Oogonium: primordial cell which develops into oocyte
-After mitosis
-Earliest stage
Oocyte: early, not yet fully developed ovum
-Primary oocyte: most prevalent; frozen in meiosis 1
-Secondary oocyte: if activated
Ovum: egg; capable of developing into new individual
What are primary oocytes formed from?
Mitotic divisions of oogonia
What does primary oocytes enter and why?
Enter meiosis 1
Become dormant/frozen to protect them
-Done by surrounding follicular cells
When are max # of primary oocytes formed? What happens once max number is attained?
Mid to late fetal life
Atresia (programmed cell death) or natural degeneration begins and continues for life
Flow map of follicle and oocyte
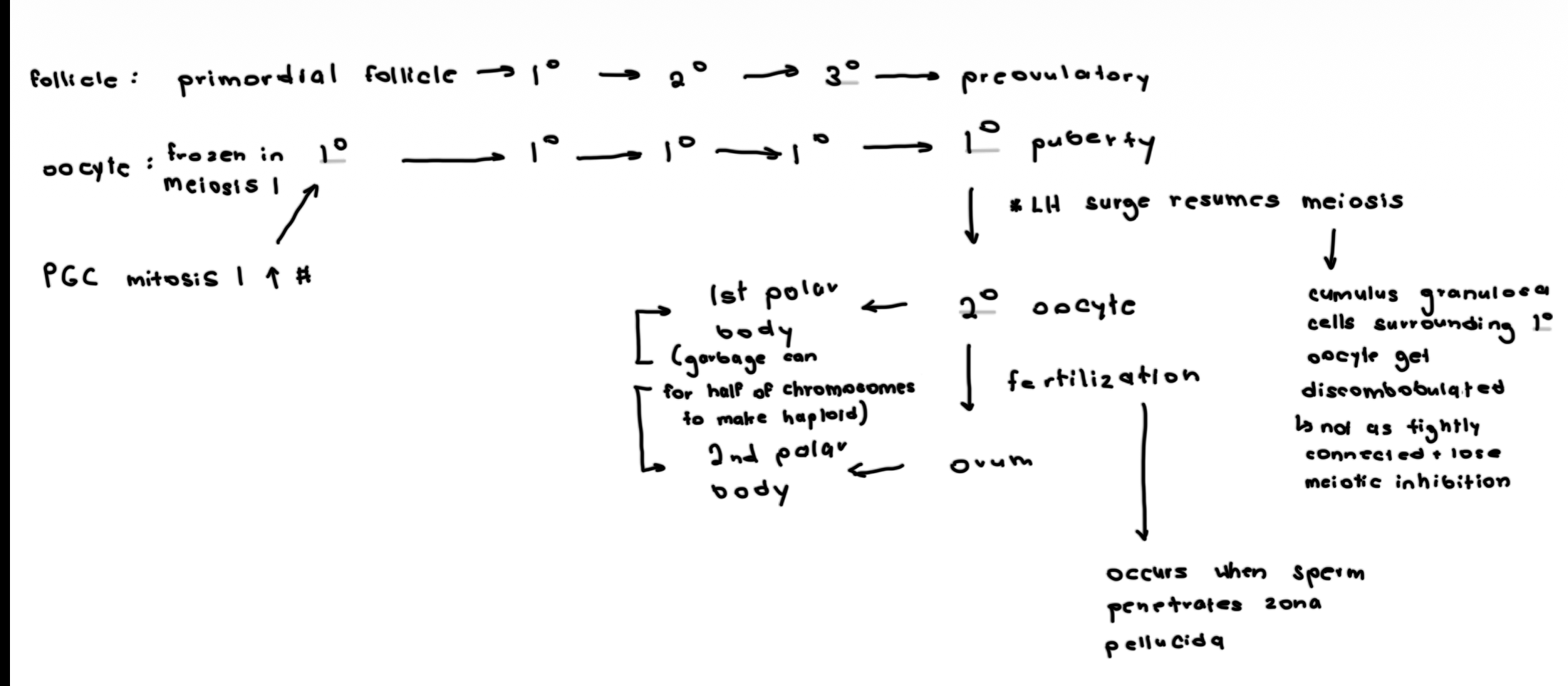
How many primary oocytes stimulated to develop? And when?
Only a select few and after puberty
Oocyte number in humans at birth then puberty
1-2 mil
300,000
Human oocyte wastage - fetal vs adult
Loss:
99.98% - fetal
97.92% - adult
Primordial follicle: cell type, state, cues to grow, when seen
1° oocyte
Single layer of squamous epithelial
Resting state
Growth factors in ovary: transforming growth factor beta - AMH after puberty
Seen in fetal life and into puberty
Primary follicle: cell type, changes
1° oocyte
Single layer but expand into cuboidal/columnar
Zona pellucida forms
Secondary follicle: cell type: changes
1° oocyte
Multiple granulosa cell layers and theca layer forms (division of cells)
Pre-antral (no follicular fluid)
Describe folliculogenesis
Classification and regulation of follicle growth
Growth and development of 3° follicle with 1° oocyte
What cells provide E2 in follicle?
Mural granulosa
What cells provide meiotic inhibition to oocyte?
Cumulus granulosa
Granulosa and theca: where are they from; responsive to what; convert what to what
Granulosa (mural)
-From cortex
-Responds to FSH
-Convert T to E2
Theca
-From stroma
-Responds to LH
-Convert cholesterol to T
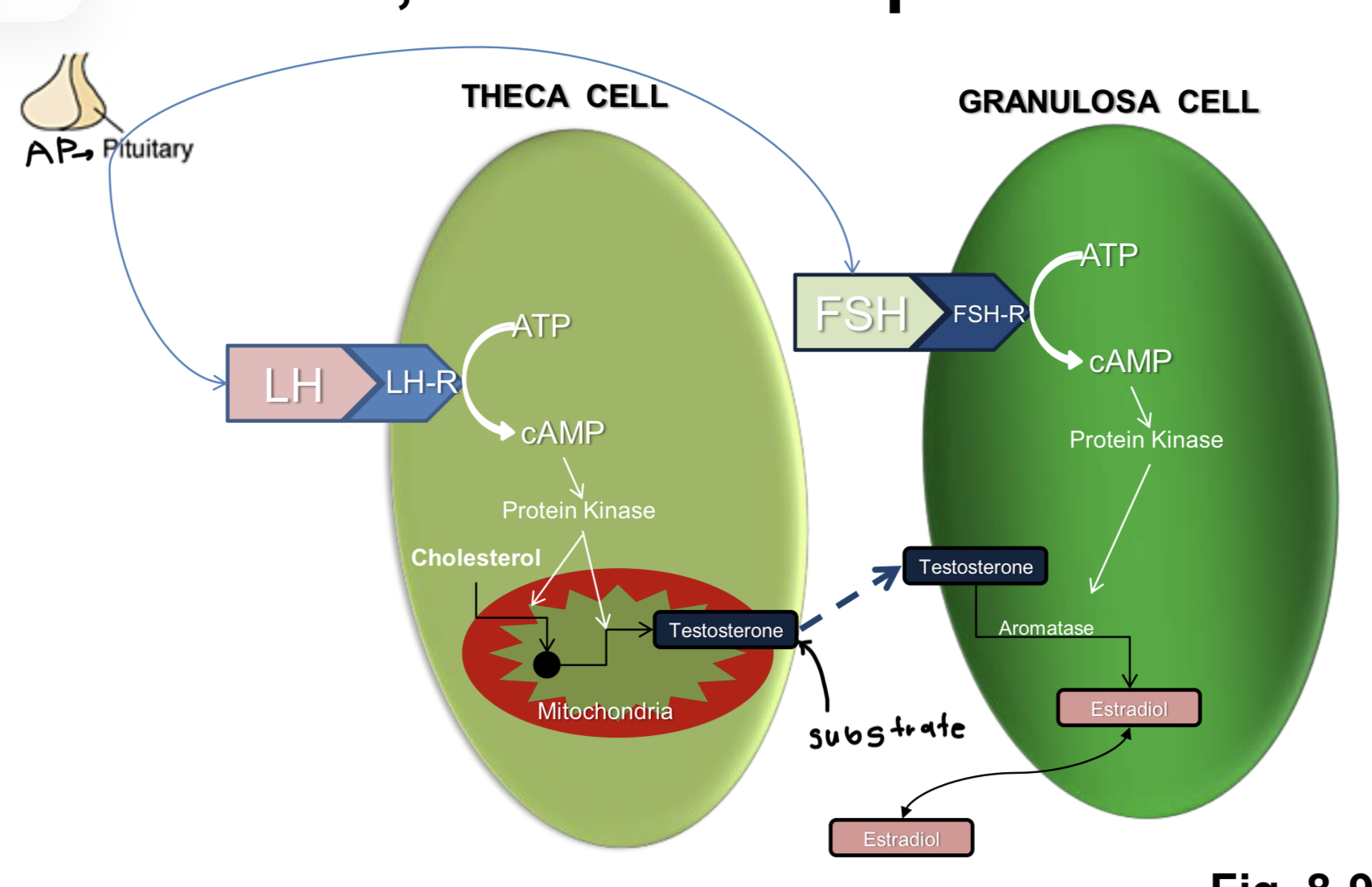
Explain 2-cell-2-gonadotropin model
In Theca/Leydig:
AP → LH → LH receptor → activates g-proteins → adenylate cyclase converts ATP to cAMP → increase in cAMP → activates protein kinases → cholesterol moved into mitochondria → steroidogenesis → testosterone
In Granulosa/Sertoli:
AP → FSH → FSH receptor → activates g-proteins → adenylate cyclase converts ATP to cAMP → increase in cAMP → activates protein kinases → protein kinases increase aromatase (CYP19A1) → test converted to estrogen → estradiol
*Note this is paracrine b/c some of the testosterone that will be converted to estrogen came from theca/leydig cell + test can pass freely through cell membrane b/c lipophilic to become substrate
What transition occurs as follicles grow in regards to FSH and LH
More dependent on FSH to LH as follicle grows
Follicular fluid (antral follicle) components
Hormones
-Steroids (E2, T, P4)
-Gonadotropins (LH, FSH)
-Prostaglandins
Proteins
Enzymes
Carbs
Follicular fluid (antral follicle) function
Supports follicle growth
Aids in oocyte development and health
Mediates granulosa cell functions
Cells live in hypoxic environ b/c no blood supply so follicular fluid keeps them alive
What are the follicular growth stages and what happens in each?
Primordial → 1° → 2° → ovarian follicular pool → 3° →
1) Recruitment: increase number of follicles and low E2 → atresia of many →
2) Selection: decrease number of follicles, increase follicle size, increase E2 b/c granulosa cells increase with follicle size →
3) Dominance: decrease number of follicles until 1 dom prev-ovulatory follicle that is at max size (monovulatory species), high E2
What is follicular growth driven by
LH and FSH support
How long does follicular growth take
45-60 days
Early astral (tertiary)
1° oocyte
Oocyte reaches max size
Granulosa cells expand so more E2
Antrum forms
Theca layer more prominent so more T
-Interna
-Externa
Graafian follicle (preovulatory follicle)
1° oocyte
Last stage of tertiary follicle
Largest domestic follicle
Max # of granulosa cells + follicular fluid
How do follicles grow?
In waves and numbers
What is follicular development regulated by
Gonadotropins (FSH + LH)
Growth factors
Activin: activates FSH from AP from small follicles granulosa
Inhibin: inhibits FSH from AP from large follicles granulosa
Follicle fates
Ovulation: needs low P4
Atresia: follicular death; fate of most
Cysts: diseases causes them not to ovulate or die; produce low E2 +P4
->25 mm in cattle
-Often in high-producing dairy cattle where hormonal regulation from hyp-pit doesn’t always get to follicle
What is PCOS? Affects how many women? What is it? Strong association with? Stuck at what?
Polycystic ovarian syndrome
5-10%
Continuous exposure to E2 blocks LH surge and increases thickness of uterine endometrium
Strong association with obesity
Doesn’t get past small recruitment stage
What happens at dominant stage in litter bearing species
Increased number recruited and selected so co-dom follicles
What does P4 need to be at for dom follicle ovulate
P4 low → ovulate
P4 high → atresia
Different waves of follicular growth. And signals
Ovulatory vs non-ovulatory
Dominant (dom, pre-ov follicle) vs subordinant (recruited + selected follicles)
Signals: LH, FSH, Inhibin (from dom follicle)
Waves description
Non-ov wave when P4 is high so atresia of dom follicle
Ov wave when P4 is lowered so removes inhibition so surge center can be activated by E2 from large dom follicle
Signals for follicle growth
FSH
-Granulosa cell mitosis
-Increases LH receptors
-Steroidogeneis: increase E2
-Effects preantral and antral follicles
LH
-Steroidogeneis: increase T
Effect antral follicles
Surge starts ov
Resumption of meiosis in oocyte
FSH increases LH receptors on granulosa cells
How many follicular waves? Cows? Which is more fertile
1-6
2-3 average in cows
-3 more fertile b/c less P4 exposure in same time frame
What inhibits follicle growth
Presence of dom follicle: large so takes up space + prevents others from growing
Inadequate production of gonadotropins b/c consumed by dom b/c so big
Steroids from dom: E2 and androgens
Inhibin from dom: inhibits follicle growth by decreasing FSH
How to increase number of ova in cow
FSH to keep # recruited follicles high
Two ovulation stimuli
LH surge whether induced or spontaneous
FSH: don’t know why but it surges at ov
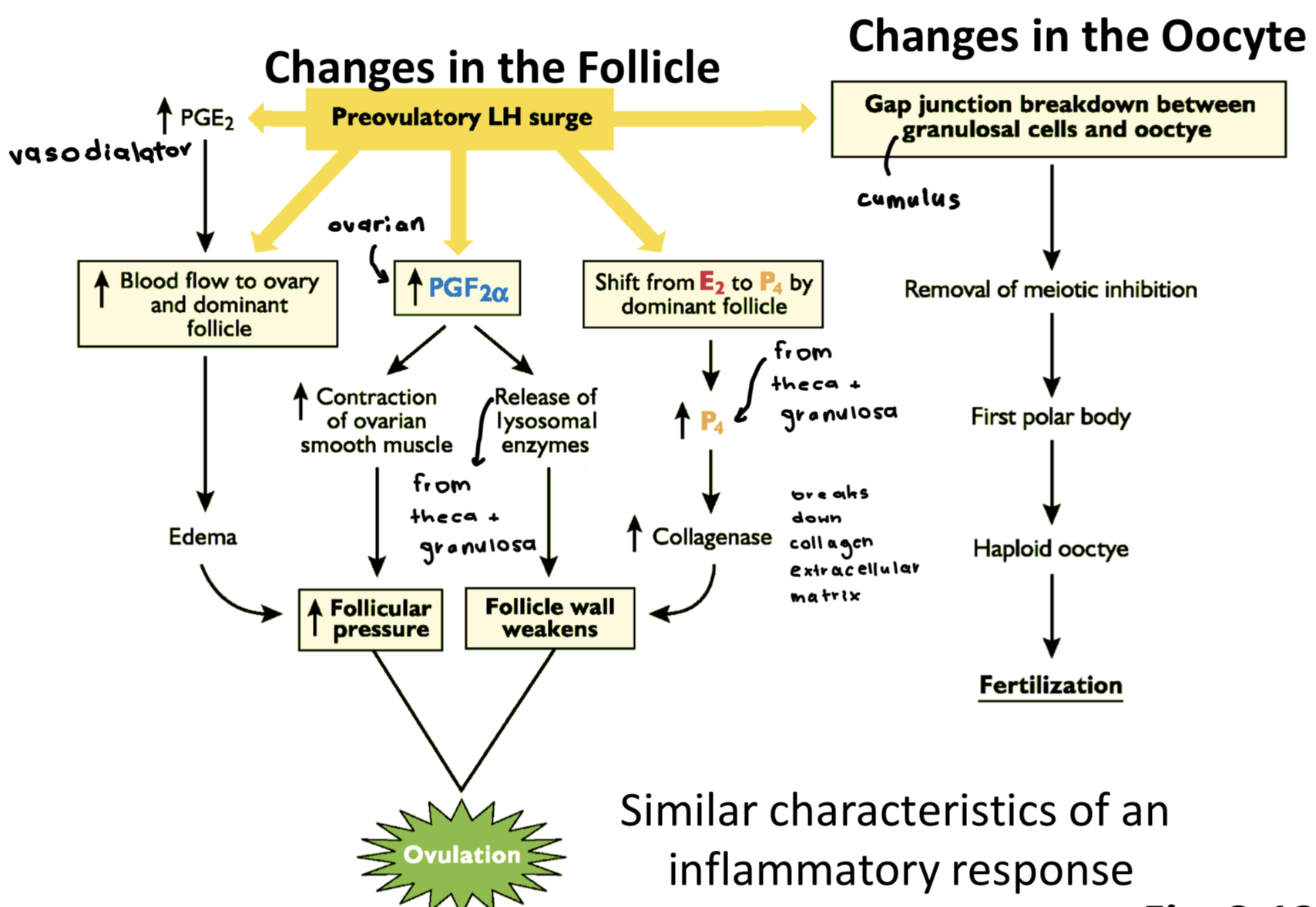
Changes in follicle from LH surge and changes in oocyte
What phase do female reproductive scientists focus on
Luteal phase b/c long
What is characteristic of luteal phase? How long is luteal? How does it end?
CL formation
-Lutenization (in metestrus)
P4 production: (-) feedback
66-75%
Ends with luteolysis if not preg
What is lutenization? What is it called? Triggered by what?
Process that turns granulosa and theca cells into luteal cells
Terminal differentiation so can’t switch back
Triggered by LH surge
Describe what happens to follicle after ov
Ovary tissue damaged after ov with ruptured blood vessels to corpus hemorrahgicum forms (blood clot early in metestrus that lasts hours to days)
Then corpus luteum forms and has new blood vessels for more nutrients to come in and P4 to go out
-Heterogenous population of cells meaning small and large luteal cells
Functional capability of CL (P4 produced). 2 components. And match granulosa and theca to slc and llc
Number of luteal cells
-Large cells undergo hypertrophy (3 fold increase) - granulosa
-Small cells undergo hyperplasia (5 fold increase) - theca
Vascularization of CL
-Initiated by angiogenic factors from follicle (luteotropins)
-Vascularity effects CL steroid synthesis and delivery of hormones (more nutrients)
What is insufficient CL function
Failure to maintain luteal phase and/or preg
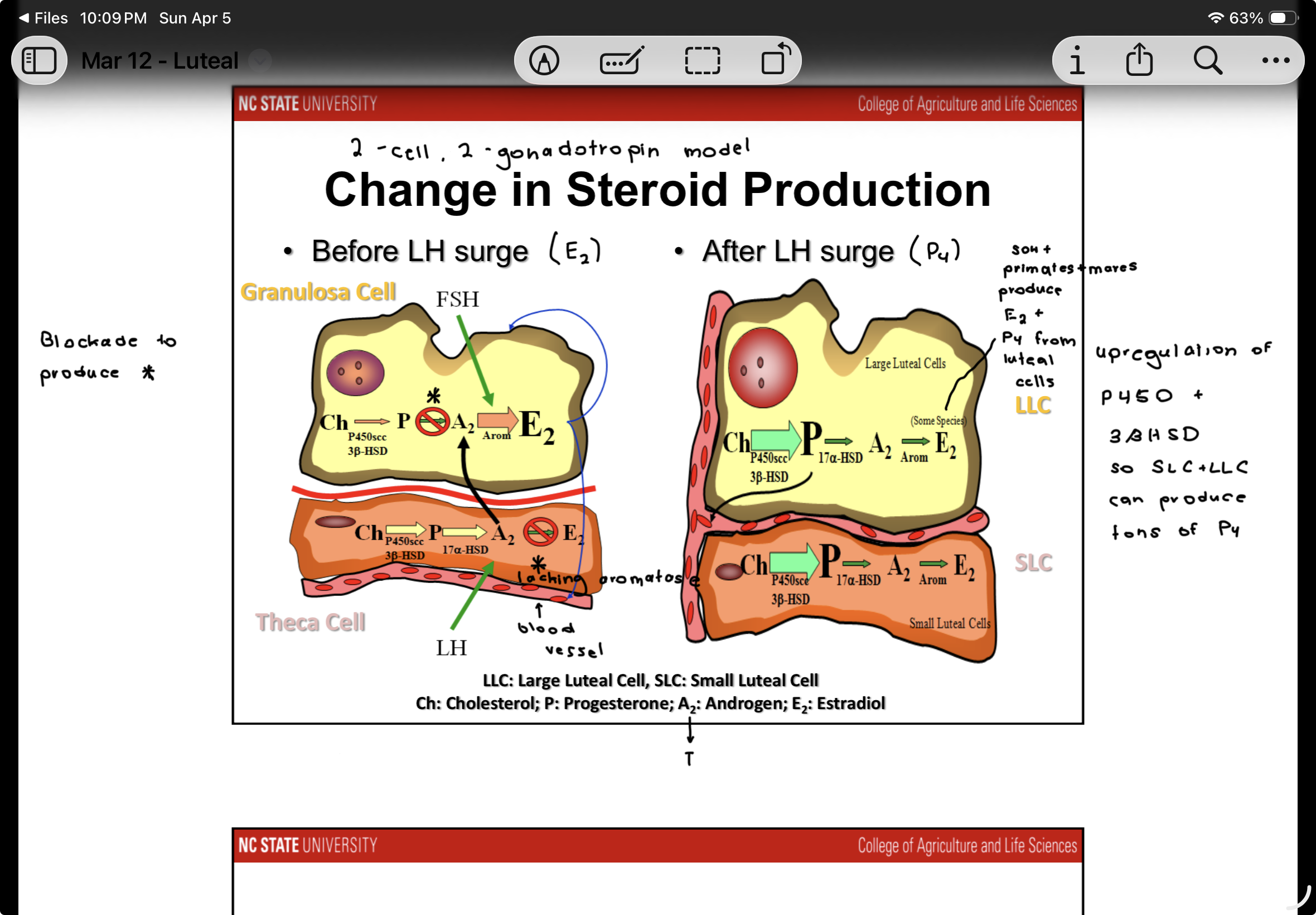
Changes in steroid production before LH surge and after
Before LH surge: E2 is primarily produced - from granulosa cell
-Lacks aromatase to convert T to E2 in theca cell
After LH surge: P4 is primarily produced - from granulosa and theca cells
-Upregulation of P450 and 3BHSD so SLC and LLC can produce tons of P4
Sows and primates and mares produce E2 and P4 from luteal cells
Action of progesterone order
1) Reduces GnRH pulse amplitude and frequency
2) Stops pre-ov LH surge - basis of many hormonal contraceptions
3) Prevents behavioral estrus
4) Reduces myometrial tone to relax uterus
5) Stimulates endometrial gland development and secretion
6) Stimulates alveolar development in mammary gland
-If long term P4 exposure from gestation
What are the luteotropins for each species

What would LH antibodies do?
Antibodies bind to LH + prevent LH from binding to receptor so P4 decreases to prevent ov and pregnancy
Vaccine for LH in wild mares
-Initial + booster lasts 5 years
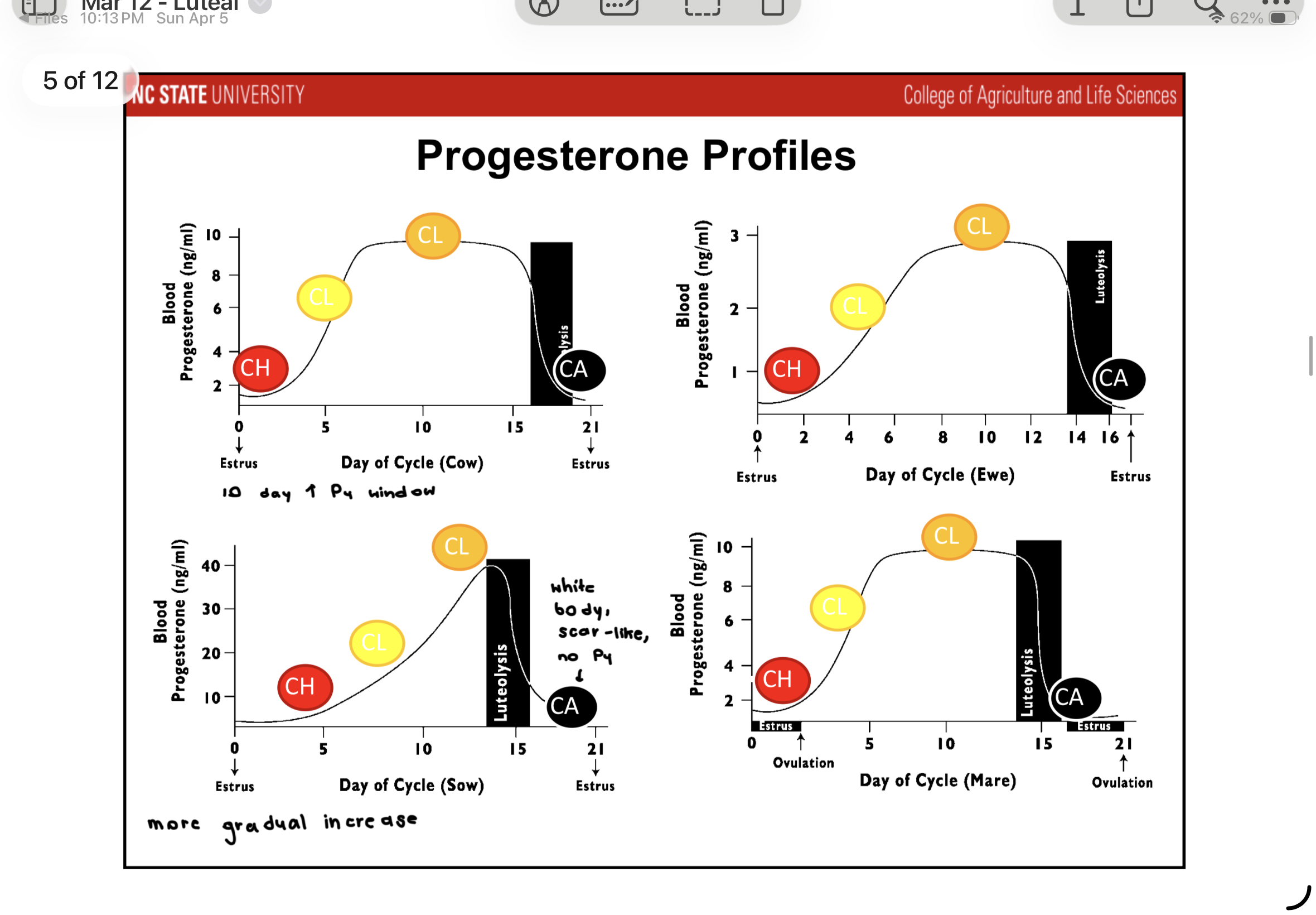
Difference in P4 profiles
Gradual increase in sow
How is progesterone used as diagnostic tool
ELISA assay: recommend sampling 3 times over 21 days
Radioimmunoassay or standard assay: serum concentration of 1ng/ml or higher =cycling
Give different milk assay examples and meanings. And graph

What is needed for her to be cycling
P4 change
What initiates luteolysis/is main luteolytic agent
Prostaglandin F2a secreted by endometrium
Describe PF2a blood flow
Cross current exchange with high to low concentration
Uterine vein (from uterus to heart and body)
Uterine-ovarian artery (heart to ovary+uterus)
Artery wraps around vein
PGF2a in vein moves into artery so it isn’t deactivated in lungs
-In ruminants and swine one pass through lungs can deactivate 90% of PGF2a
Effect of hysterectomy on CL length and its regression. What was found out?
Found that uterus produced something that regressed CL (except in primate/woman where it regressed even without uterus)
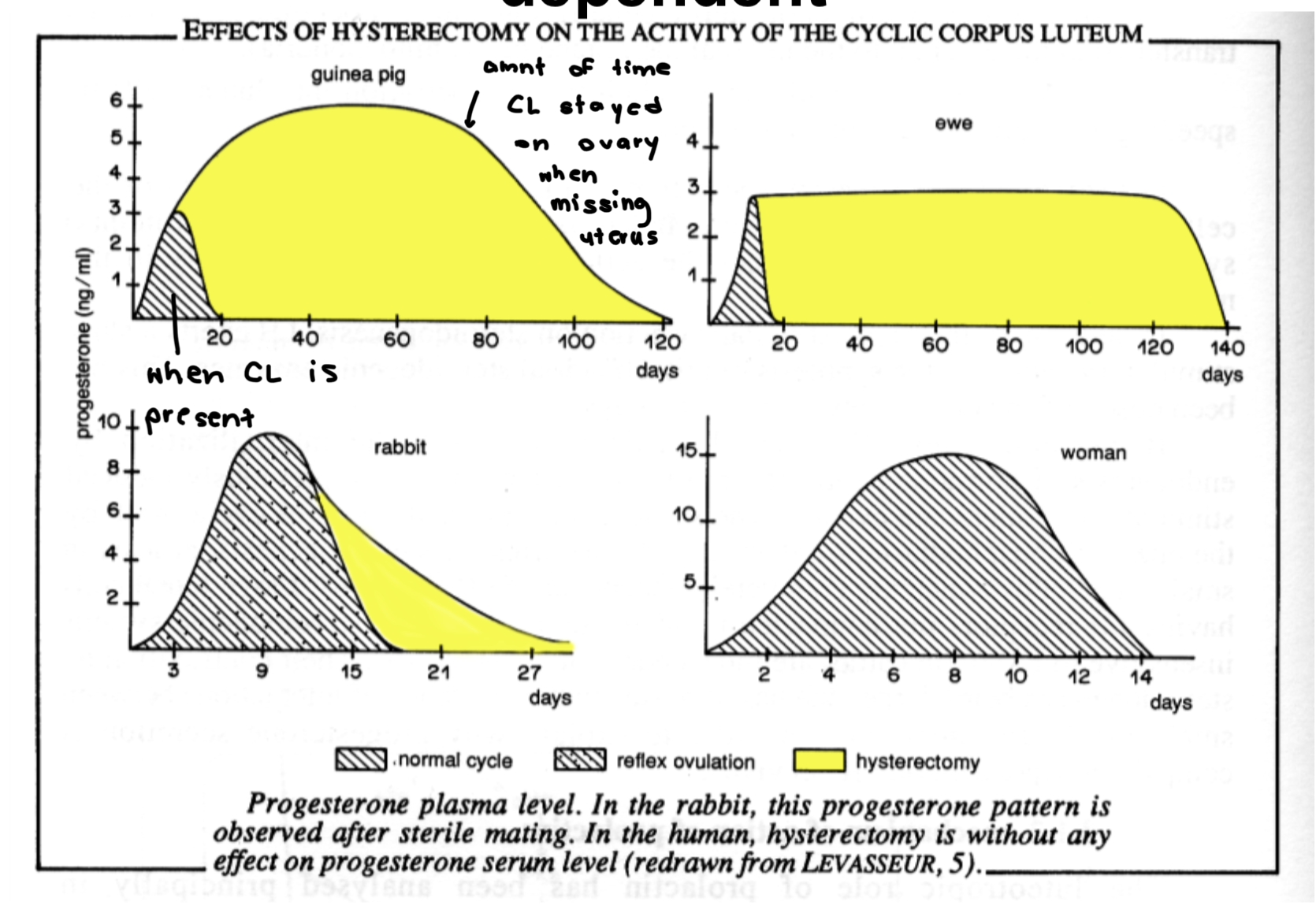
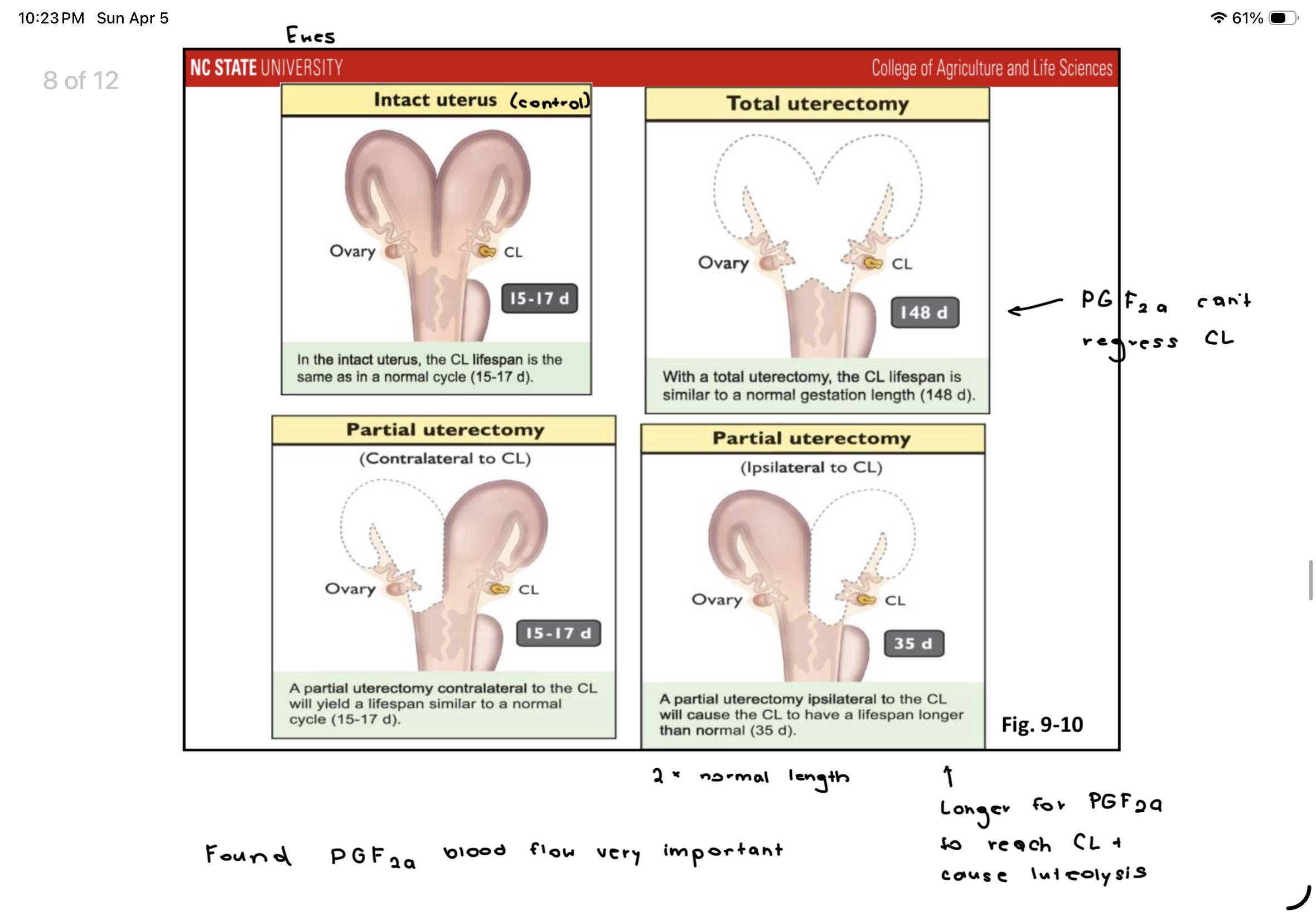
Effect of 4 uterectomy types on CL regression. Found what?
Found that PGF2a blood flow is important in regressing CL
How is luteolysis controlled in primate? CL lifespan?
Doesn’t require uterus
CL lifespan in human is 12-14 days unless preg
In absence of preg, CL produces its own PGF2a
Does PGF2a always induce luteolysis? What days?
Works:
Cattle and sheep: Days 7-17 (10 d effectiveness window)
Swine: Days 12-17 (5 d effectiveness window)
Doesn’t work:
Cattle and sheep: Days 1-6/7 (7 used as safety net)
Swine: Days 1-12
*Because acquisition of luteolytic capacity
-CL has to become sensitive to PGF2a
Doesn’t work:
Days 17-21 b/c already undergoing luteolysis so PGF2a has no effect
2 luteolysis stages
1) Functional regression
-CL can’t make and secrete P4
2) Structural regression
Luteolysis in depth steps
Decreased blood flow due to vasoconstriction from PGF2a
Cellular response
-P4 synthesis decreases
-Apoptosis
Immune response
-Increase in lymphocytes and macrophages that attack tissues
Why is a lot of estrous synchronization work done in cattle first
B/c 9 month gestation so not much room for error with timing
-Only 60 day window to get preg
Non-synchronized percent preg vs synchronized
Non-synch: after 3 cycles 88% are preg
Synch: add extra cycle to breed so after 4 cycles 94% preg
-9 day age advantage so calves from beginning of breeding season weigh more more money
What hormone isn’t used in US?
Estrogen due to carcinogenic effect
Estrous synch advantages
Can shorten breeding season
Shortened time to Breeding
Utilizes labor more efficiently
No heat checking needed
Reduced days to first service
Groups timing of parturition
-Uniform crop of offspring=more valuable
Estrous synch disadvantages
Increased labor costs
Requires skilled labor and periods of intensive management
-Multiple injections
-Timing is everything
Requires adequate facilities
-Less time spent observing animals so can miss detecting non-cyclers in herd
Higher input costs
-Is it worth it
What controls the cycle? Brand names?
Progesterone
Blocks dom follicles from ovulating so they die
Progestins mimic progesterone
-MGA (melengesterol acetate)
-Norgestomet
-PRID (progesterone releasing intravaginal device)
-CIDR (controlled internal drug release)
What does PGF2a do? Brand names
Kills CL to decrease P4 and cause estrus in 72 hrs (cattle)
-Decreases P4 and increases E2
Lutalyse, estimate, prosolvin, bovilene, ETC
Explain prostaglandin protocol in cattle. What does it do?
Regress active CL
-Only effective days 5-17 (grey window days 5-7 b/c CL has to become sensitive to PGF2a)
In estrus 2-5 days after injection
-Heifers: 50 hrs
-Cows: 72 hrs b/c more metabolic strain
Single vs two injections of PGF2a in cattle?
Single injection to random animals
-60-65% will respond - may be in follicular or metestrus in luteal phase
Two injections to synchronized entire herd
-10-14 days after first injection
-All should have CL old enough to respond so 100%